Documente Academic
Documente Profesional
Documente Cultură
Reflectionpaper
Încărcat de
api-273459660Titlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Reflectionpaper
Încărcat de
api-273459660Drepturi de autor:
Formate disponibile
Running head: REFLECTION PAPER
Reflection Paper
Monique Ramirez
University of Arizona
Clinical Systems Leadership Immersion
NURS 660
Mary O'Connell
REFLECTION PAPER
2
Reflection Paper
Overview
When entering the program, I wanted to learn more about the healthcare system and
where I would fit in. I was equipped with the clinical knowledge from working on the floor and
had recently accepted a position in an administrative role as the Transcatheter Aortic Valve
Replacement (TAVR) clinical coordinator. One on my goals was to expand my knowledge about
the administrative and business aspects of healthcare so I could be successful and efficient in my
new role. Healthcare is all about patient care and how we can deliver the most efficient, safe, and
cost effective care without compromising quality. The MSN program was going to prepare me
for future administrative positions while also integrating clinical healthcare knowledge. Pursuing
a degree in Clinical Systems Leadership would provide me with the knowledge and educational
qualifications to advance my career in areas of interest. My overall goal was to use the education
obtained during the MSN program to practice to the full extent of my training in my current
position and also provide an avenue for future endeavors.
One of the most valuable lessons learned was utilizing evidence-based practice and
research to support an argument. This lesson was introduces early in the program and has been
valuable in the work place. The purpose of evidence-based practice is to standardize the
healthcare system using best evidence which reduces variations in care and decreases
unpredictable outcomes (Stevens, 2013). Using evidence-based practice to support new ideas,
renovate a process, or support change can be successfully accomplished with the support of
organizational leaders. The words of Donna Shalala have had a tremendous impact on the way I
think of nursing as a profession. She said nurses and other health care professionals [should be]
able to perform to the top of their education and training (Shalala, 2013). Seeing and
REFLECTION PAPER
experiencing nursing leaders support the future of nursing enables me to practice to the full
extent of my knowledge and training.
Program Outcomes
Design and Lead Innovative Patient-centered Care
My current position is fairly new to the healthcare system. As innovative minimally
invasive programs are introduced to healthcare, my role as a clinical coordinator will become
more defined. The advantage of my position being new is that I am able to design and shape it
the way I deem fit to serve my patient population. Patient care is delivered in the in-patient,
clinic, and out-patient setting, therefore designing a system that compliments each phase of care
can be challenging. Because the patient population that the TAVR program attracts are patients
with multiple comorbidities, I have structured a valve clinic with a team of physicians. This
clinic follows the criteria set forth by the Centers for Medicare and Medicaid Services for
reimbursement and allows for a comprehensive evaluation by a cardiologist, nurse practitioner,
cardiothoracic surgeon, and coordinator in one clinic visit. The clinic structure places the patient
at the center of care, provides available resources, and ensures the patient has a comprehensive
exam by several members of the team. It gives patients information about their in-patient stay
when the procedure is scheduled and provides methods of communication from an out-patient
setting if they need to contact a healthcare professional regarding their care. Designing a valve
clinic allows for collaboration and communication of different specialties to design a clinic that
meets the goals of patient-centered care.
Collaborate with Interprofessional Teams
Collaborating with interprofessional teams is essential for the success of any program.
The knowledge and experience of other specialties ensures that a system and program is
REFLECTION PAPER
developed in its entirety addressing all element for success as seen by evidence-based practice
research. Evidence-based research shows that cardiac rehabilitation prior to surgical intervention
can improve outcomes after surgery. Because of this new found evidence the collaboration of
services with the cardiac rehabilitation staff and the cardiologist caring for the patient is essential
for the best possible outcomes. Facilitating this communication between specialties ensures
patients are receiving quality care that is evidence based. Communicating with various
departments about unique protocols and procedures regarding testing is also crucial to verify that
patients are being tested appropriated and required results are being obtained. This involves
communication with leadership staff in various departments and educational in-services for
proper training of staff.
Evaluate and Apply Evidence-based Healing Strategies
Throughout the program we have researched complementary and alternative therapies for
adoption in patient care. This has expanded my knowledge of available therapies and strategies
for optimal health. Using research to explore the best options for specific patient populations
based on beliefs, physical status, educational background, financial status, and location guided
the introduction to community and hospital resources for healing. The hospital has online
resources, support groups, and health and wellbeing activities patients can explore. Notifying
patients of these services ensures patients are aware of resources for managing stress and
anxiety. Incorporating strategies from lessons learned during the Healing Environments course,
such as the comfort of pillows, personal items from home, music, and activities while in the
hospital also ensures optimal healing during hospital admission.
Incorporates Innovative Healthcare Technology
REFLECTION PAPER
Healthcare technology is on the rise. We recently adopted a new electronic medical
record which allows for easier communication with physicians and other members of the team by
simply searching for the staff members name and sending them a message within the system.
Patients and family members have access to the system called My Chart. They can access test
results and communicate directly with physicians and nurses via the same messaging system.
Patients and families consider this to be a powerful self-advocacy tool as they can be directly
involved in their care. Privacy laws are reviewed before establishing a MyChart account. I
confirm patients are aware of this service and are enrolled in the program if desired.
Coordinate Care Transitions
The current role as TAVR program coordinator allows me to follow patients through the
phases of care to facilitate communication between physicians, prevent duplicate and
unnecessary testing, and ensure all involved are updated on the plan of care. This provides
patients a sense of ease knowing that all involved in their care are communicating. By being an
active member in the coordination of care we have prevented unsafe situations, decreased cost,
and achieved positive patient outcomes by facilitating care through phases of transition from
time of initial consult thru follow-up after a cardiac intervention. Patients are safer when
communication between providers is priority and is being facilitated by a coordinator who
specialized in transitions of care.
Apply Theory and Evidence-based Knowledge
Introduction to theories allowed for the integration into patient care. Having the
evidence-based practice to apply it in the clinical setting increased the effectiveness of adoption.
Strategies to improve quality and safe care such as the chronic care model, the attending nurse
caring model, and the patient care delivery model were incorporated into valve clinic
REFLECTION PAPER
development. These models have been used in evidence based practice and therefore can be
utilized for the design, coordination, and evaluation of patient care systems. Promoting family
involvement in medical decision making, providing resources for self-efficacy, and
comprehensive assessments that address all patient needs focus on elements of the care models
mentioned. Ensuring that the current healthcare system allows for the integration of these models
is an important component of nursing leadership. Nurses can adopt a change in delivery of care
that can later translate into full adoption by the organization. Assessment of the current theories
and evidence-based practice currently used allows for changes or modifications that support
optimal patient-care systems in the clinic, in-patient, and out-patient settings.
Conclusion
By the completion of the program, I feel that I have accomplished all of my personal
goals and learned more than I anticipated. Not only did the material and lessons learned through
each module prepared me for my current role and future employment opportunities, it also taught
me time management, communication skills, and team development skills during group projects.
Personal strengths developed during the program was to appreciate the complexity of the
healthcare system and my role in the nursing professional as a masters prepared registered nurse.
It has given me the knowledge, motivation, and confidence to know that I can promote positivity
and change through evidence based practice. In the future, I plan on expanding my role as the
coordinator to lead more structural heart programs. As a leader, this program has provided me
the knowledge, tools, and resources, to ensure delivery of evidence-based patient-centered care
to all patients. Using the knowledge gained in the business of healthcare, healing environments,
holistic nursing, appraising research, health promotion and risk reduction, and healthcare
technology will enable me to lead the future of nursing.
REFLECTION PAPER
7
References
Shalala, D. (2013, December 11). Back to the future of nursing: A look ahead based on a
landmark IOM report [Video file]. Retrieved from
http://www.iom.edu/Activities/Quality/RosenthalLect/2013-DEC-11.aspx
Stevens, K. R. (2013, May 31). The impact of evidence-based practice in nursing and the next
big ideas. The Online Journal of Issues in Nursing, 18.
http://dx.doi.org/10.3912/OJIN.Vol18No02Man04
S-ar putea să vă placă și
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- Selfreflection 653Document8 paginiSelfreflection 653api-273459660Încă nu există evaluări
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (895)
- ExecutivesummaryDocument5 paginiExecutivesummaryapi-273459660Încă nu există evaluări
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- DocccopdtypicalpatientdescriptionandassessmentguideDocument9 paginiDocccopdtypicalpatientdescriptionandassessmentguideapi-273459660Încă nu există evaluări
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (400)
- M Ramirez Nurs660 TherapeuticstableDocument17 paginiM Ramirez Nurs660 Therapeuticstableapi-273459660Încă nu există evaluări
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (266)
- CopdfastfactsDocument10 paginiCopdfastfactsapi-273459660Încă nu există evaluări
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- M Ramirez Cover LetterDocument2 paginiM Ramirez Cover Letterapi-273459660Încă nu există evaluări
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- M Ramirez ResumeDocument1 paginăM Ramirez Resumeapi-273459660Încă nu există evaluări
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Nursing Board Exam ReviewerDocument32 paginiNursing Board Exam ReviewerRose Anne Mückl100% (9)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (588)
- 30947630Document12 pagini30947630carolinapolotorresÎncă nu există evaluări
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- ADHD: Clinical Practice Guideline For The Diagnosis, Evaluation, and TreatmentDocument18 paginiADHD: Clinical Practice Guideline For The Diagnosis, Evaluation, and TreatmentBen CulpepperÎncă nu există evaluări
- List of Licensed Private and Public Hospital 2011Document7 paginiList of Licensed Private and Public Hospital 2011TJ NgÎncă nu există evaluări
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- Easy Health Insurance Claim FormDocument3 paginiEasy Health Insurance Claim FormJanmejay SinghÎncă nu există evaluări
- PMLS PRESENTATION (Lesson 3&4) (10.5 × 9 CM)Document4 paginiPMLS PRESENTATION (Lesson 3&4) (10.5 × 9 CM)Rhygn SarmientoÎncă nu există evaluări
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2259)
- Human Biology: Edexcel IGCSEDocument28 paginiHuman Biology: Edexcel IGCSEmuhajireenÎncă nu există evaluări
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (73)
- Fee Schedule 2010-2011Document16 paginiFee Schedule 2010-2011Chirag VaidÎncă nu există evaluări
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- Sun Salutations Yoga Lesson PlanDocument8 paginiSun Salutations Yoga Lesson PlanErica Harris100% (1)
- NothingNewUnderTheSun Abdul HamidHughesDocument10 paginiNothingNewUnderTheSun Abdul HamidHughesLuisdaniel Martinez AranaÎncă nu există evaluări
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- How Does Radiation Therapy Work?Document5 paginiHow Does Radiation Therapy Work?mikeadrianÎncă nu există evaluări
- TgaDocument33 paginiTgavarun rajÎncă nu există evaluări
- Drug Interactions With Antibiotics: August 2018Document4 paginiDrug Interactions With Antibiotics: August 2018Komang SubitaÎncă nu există evaluări
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- Vaccination CertificateDocument14 paginiVaccination Certificatemayorga fireÎncă nu există evaluări
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- Henoch Schonlein PurpuraDocument28 paginiHenoch Schonlein PurpuraPhil Adit R100% (1)
- Rad Tech HandbookDocument116 paginiRad Tech HandbookNoah GuilloryÎncă nu există evaluări
- OB PACU Severe PreeclampsiaDocument65 paginiOB PACU Severe Preeclampsiasurbakti_christineÎncă nu există evaluări
- Tugas MedicineDocument2 paginiTugas MedicineRiza Ikhsan MuliaÎncă nu există evaluări
- Biocompactability Testing of Medical DevicesDocument5 paginiBiocompactability Testing of Medical DevicesSathesh Kumar Annamalai100% (1)
- Biologic Width - The No Encroachment Zone: I J D ADocument8 paginiBiologic Width - The No Encroachment Zone: I J D AJinny ShawÎncă nu există evaluări
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (121)
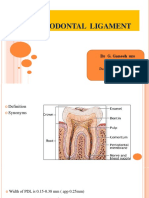
- Periodontal Ligament: Ganesh Ganji 2 Year PGDocument34 paginiPeriodontal Ligament: Ganesh Ganji 2 Year PGNareshÎncă nu există evaluări
- GuidelinesDocument4 paginiGuidelinesChidambaram SeevakanÎncă nu există evaluări
- Field Demonstration ScriptDocument3 paginiField Demonstration ScriptRizabelle Halang HernaezÎncă nu există evaluări
- Presentasi Bio-Strath 2016Document28 paginiPresentasi Bio-Strath 2016Imanluves Amel100% (1)
- Raheem Khan - WikipediaDocument10 paginiRaheem Khan - WikipediaRaheem MahirÎncă nu există evaluări
- GIT Conditions - StudentsDocument57 paginiGIT Conditions - StudentsShamal KoyeÎncă nu există evaluări
- 50 Millesimal Potency Intheory and Practice Harimohon Choudhury.00012 - 2contentsDocument5 pagini50 Millesimal Potency Intheory and Practice Harimohon Choudhury.00012 - 2contentsMd. NazimÎncă nu există evaluări
- AutismScreen AssessDocument42 paginiAutismScreen AssessMelindaDuciagÎncă nu există evaluări
- High Res.Document162 paginiHigh Res.Nando93100% (1)
- Chapter 1Document20 paginiChapter 1luiperdvrouÎncă nu există evaluări
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)