Documente Academic
Documente Profesional
Documente Cultură
Common Case Study-Denise Zaragoza
Încărcat de
api-242880215Descriere originală:
Titlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Common Case Study-Denise Zaragoza
Încărcat de
api-242880215Drepturi de autor:
Formate disponibile
Running Head: CASE STUDY OF LB AND CHRONIC KIDNEY DISEASE
Case Study of Patient LB and Chronic Kidney Disease
Denise Zaragoza
Dietetic Intern
Golden Gate Dietetic Internship Program
Conducted at Novato Healthcare Center
September 22, 2015
CASE STUDY OF LB AND CHRONIC KIDNEY DISEASE
Case Study of Patient LB and Chronic Kidney Disease
Chronic Kidney Disease (CKD) is the progressive and irreversible loss of kidney function
secondary to kidney damage (Nelms, Sucher, Lacey, & Long, 2011). According to the Center
for Disease Control and Prevention, over 10% of adults in the United States have CKD of
varying stages (Center for Disease Control and Prevention, 2014). Type I Diabetes Mellitus
(DM1) causes 3.9% of CKD cases (Nelms, Sucher, Lacey, & Long, 2011). Diabetes and
hypertension are the leading causes of CKD and kidney failure (Center for Disease Control and
Prevention, 2014). Family history, prolonged consumption of non-steroidal anti-inflammatory
drugs, and ethnicity are risk factors for developing CKD (Nelms, Sucher, Lacey, & Long, 2011).
Medical nutrition therapy plays an integral role in preventing malnutrition and protecting against
disease progression in patients with CKD (Academy of Nutrition and Dietetics Evidence
Analysis Library).
Case Study
This case study was conducted 8/20/15 to 8/28/15. The focus of this study is patient LB,
who was admitted to Novato Healthcare Center (NHC) on 8/17/15 with the admission diagnosis
of gangrene of toe, sepsis, and streptococcal infection. LB is a 60 year old female with a past
medical history of DM1, Coronary Artery Disease, Chronic Kidney Disease Stage IV, peripheral
neuropathy, anemia of chronic disease, nicotine abuse, and left ventricular hypertrophy. This
case study focuses primarily on LBs diagnosis and nutrition intervention of Chronic Kidney
Disease Stage IV.
LB was admitted to the hospital with sepsis due to a gangrenous toe. She tripped and
stubbed her toe one week prior to admission. She noticed three days prior to admission that her
great toe had turned black and was draining out a large amount of malodorous pus. She arrived to
CASE STUDY OF LB AND CHRONIC KIDNEY DISEASE
the emergency room with her sister with complaints of fevers, chills, and diarrhea. In the
hospital, the 1st and 2nd digits of her left foot were amputated. She developed a streptococcal
infection following the surgical procedure despite the use of prophylactic antibiotics. She was
discharged with a Foley catheter for recurrent urinary retention. Upon discharged, she was
admitted to NHC for rehabilitation. She is mobile through the use of a wheelchair.
Anthropometric data for LB includes: height 61in, admission weight 54.5kg, reported
usual body weight 50kg, 109% reported usual body weight, ideal body weight 47.7kg, 114%
ideal body weight, BMI 22.7kg/m2. According to chart notes, she had +3 pitting edema in the left
lower extremity. Due to sepsis while at the hospital and active infection, generalized edema is
suspected.
She underwent physical and occupational therapy to increase strength and ability to
perform activities of daily living (ADLs) while at NHC. Extensive assistance was required for all
ADLs, but she was able to feed herself and preferred to eat in her room. The latest labs for her
were collected on 8/19/15; values are recorded in Table 1. A list of medications for LB including
purpose, nutritional implications, and potential side effects are recorded in Table 2.
A nutritional assessment was conducted on 8/20/15 per facility protocol. She was
admitted to NHC on a controlled carbohydrate diet with regular texture and thin liquids. There is
no family history noted. The last bowel movement was recorded on 8/19/15, no constipation or
diarrhea noted. There are no known food allergies. Her oral intake was recorded as 97% since
admission; and she reported good appetite. She does not participate in physical activity as she is
minimally mobile due to neuropathy. At home she lives with her disabled son, who does not
require care from her. LB stated she eats a healthy diet at home but eats out frequently.
CASE STUDY OF LB AND CHRONIC KIDNEY DISEASE
She is a current smoker, smoking a half a pack of cigarettes per day, but she had not
smoked any cigarettes since admission to the hospital three weeks prior. This was of great
concern as smoking significantly delays wound healing and is associated with contributing to
renal damage (Silverstein, 1992), (Orth & Hallan, 2008). In patients with DM1, smoking,
together with poor glycemic control, considerably increases the risk of onset of
microalbuminuria and diabetic nephropathy (Scott et al., 2001).
LB was determined to be of moderate nutritional risk given her various diagnoses
affecting nutritional status, in conjunction with, her surgical procedure and the presence of an
active infection.
Table 1
Patient LB Laboratory Values with NHC Reference Ranges
Lab
Lab Value
Reference Range
Hgb
9.4
12.3-15.3 g/dL
Hct
29.9
36.4-44.9 %
Vit D- 25 Hydroxy
30-100 ng/mL
Glucose, Fasting
267
70-99 mg/dL
BUN
29
7-25 mg/dL
Creatinine
2.5
0.6-1.3 mg/dL
GFR
20
Sodium
132
60-499
90 or more: normal
60-89: mildly reduced
35-59: moderately reduced
15-29: severely reduced
<15: kidney failure
136-145 mEq/L
Potassium
5.4
3.5-5.1 mEq/L
Calcium
7.9
8.6-10.2 mg/dL
CASE STUDY OF LB AND CHRONIC KIDNEY DISEASE
Table 2
LB Medication List Including Purpose, Nutritional Implications, and Potential Side Effects
Medication
Purpose
Nutrition Implications
Potential Side Effects
Vit D3
Vit D deficiency
Ca absorption
Usually none
Cholecalciferol
Overdose can cause:
weight, anorexia,
thirst, dry mouth,
metallic taste, N/V,
constipation, diarrhea
Insulin Lispro
Humalog
BG regulation
Weight
Hypoglycemia
Transient edema
Vision changes
Norco
Hydrocodone
bitartrate &
acetaminophen
Pain management
Anorexia
Ativan
lorazepam
Anxiety
Limit caffeine to
<400-500mg/day
Anorexia
Weight
Appetite
Avoid alcohol
Dry mouth
N/V
Constipation
Drowsiness
Fatigue
Dizziness
Drowsiness
Norvasc
Amlodipine
HTN
Na
Avoid natural licorice
Hypotension
Edema
Toprol-XL
Metoprolol
HTN
Na
Avoid natural licorice
Hypotension
Diarrhea
Insomnia
Flagyl
Metronidazole
Gangrene
(Antibiotic)
Anorexia
Nausea
Diarrhea
Dizziness
Headache
Nicoderm CQ
Smoking cessation
None
Redness or itching on
application site
Headache
CASE STUDY OF LB AND CHRONIC KIDNEY DISEASE
Table 2 continued
LB Medication List Including Purpose, Nutritional Implications, and Potential Side Effects
Medication
Purpose
Nutrition Implications
Potential Side Effects
Senokot
senna
Constipation
Electrolyte imbalance
w/ excessive use
Nausea
Abdominal cramps
Aspirin
MI/CVA
prevention
Anorexia
Dyspepsia
N/V
Platelet aggregation
C-Reactive Protein
Procrit
Epoetin Alfa
Anemia
May need Fe, B12,
Folate supplementation
Weight
Blood Pressure
Headache
Shortness of breath
Fever
Pepcid
famotidine
Gastric reflux
Fe & B12 absorption
Gastric secretions
Gastric pH
Hydralazine
CHF
Anorexia
orWeight
Thirst
N/V
Blood pressure
Angina
Edema
Diarrhea
Headache
Tachycardia
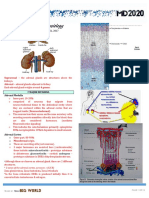
Renal Physiology
The physiological functions of the kidneys are fluid and waste removal, red blood cell
production, maintenance of bone health, electrolyte balance, pH balance, regulation of blood
pressure, and the production of hormones and enzymes (Spoek, 2014). The nephron is the
functional unit of the kidney and is made up of the glomerulus and a series of tubules.
Ultrafiltrate is produced in the glomerulus and products such as amino acids, glucose, sodium,
and potassium are reabsorbed in the tubules (Nelms, Sucher, Lacey, & Long, 2011).
Reabsorption is hormonal dependent.
Vasopressin (antidiuretic hormone) works to increase or decrease water reabsorption.
This works in the maintenance of plasma volume and blood pressure. The release of vasopressin
CASE STUDY OF LB AND CHRONIC KIDNEY DISEASE
increases the reabsorption of water, increasing plasma volume, and thus increasing blood
pressure (Nelms, Sucher, Lacey, & Long, 2011). Blood pressure is also increased through the
rennin-angiotensin-aldosterone system. Decreased sodium, blood volume, or blood pressure
trigger the kidneys to release renin, activating the system. The end product is aldosterone which
causes an increase in sodium and chloride reabsorption, resulting in increased water reabsorption
through diffusion thus elevating blood pressure. Increased blood volume or blood pressure
triggers the excretion of sodium, water follows the sodium through diffusion, resulting in
decreased blood volume and blood pressure (Nelms, Sucher, Lacey, & Long, 2011).
Potassium and sodium are exchanged for one another in the renal tubules. When serum
sodium levels are elevated, potassium is exchanged with sodium in order to maintain electrolyte
balance. Elevated serum potassium results in aldosterone secretion, causing sodium reabsorption
and potassium excretion (Nelms, Sucher, Lacey, & Long, 2011). Waste products including uric
acid, creatinine, and urea are excreted through the urine. The kidneys contribute to the regulation
of pH through the excretion of hydrogen ions or bicarbonate, as well as the reabsorption of
carbonic acid (Matel, 2013).
The kidneys are responsible for activating vitamin D. This is important for the
maintenance of bone health, as the active form of vitamin D increases intestinal absorption of
calcium. This activation is controlled by parathyroid hormone (PTH). PTH causes the kidneys to
reabsorb calcium, excrete phosphorus, and activate vitamin D (Spoek, 2014). Erythropoietin is
synthesized in the kidneys and stimulates the production of red blood cells in the bone marrow.
Pathophysiology of CKD
CKD is a progressive and irreversible loss of renal function. There are five stages of
CKD, detailed in Table 3.
CASE STUDY OF LB AND CHRONIC KIDNEY DISEASE
Table 3
Stages of CKD
Stage
GFR
Signs and Symptoms
90 mL/min
Higher than normal levels of creatinine or
urea in the blood and/or blood or protein in
the urine.
II
60-89 mL/min
Higher than normal levels of creatinine or
urea in the blood and/or blood or protein in
the urine.
III
30-59 mL/min
Fatigue, edema in lower legs, hands, or
around eyes, change in urine such as a foamy
appearance, protein presence in the urine,
darker urine color, problems falling or staying
asleep, back pain where the kidneys are
located.
Complications of kidney disease such as
hypertension, anemia and early bone disease
are more likely to develop.
IV
15-29 mL/min
Fatigue, edema, urination changes such as
foamy urine, dark color, or bloody urine, back
pain where the kidneys are located, trouble
falling or staying asleep, nausea, vomiting,
dysgeusia, uremic breath, loss of appetite,
difficulty concentrating, and numbness or
tingling in the toes and fingers.
<15 mL/min
Loss of appetite, nausea, vomiting, headaches,
fatigue, difficulty concentrating, itching, little
or no production of urine, swelling, muscle
cramps, tingling in hands or feet, increased
skin pigmentation.
Advanced kidney impairment can result in edema, metabolic acidosis, hyperkalemia,
anemia, uremia, azotemia, hyperphosphatemia, oliguria, hypertension, and renal osteodystrophy
(Nelms, Sucher, Lacey, & Long, 2011). Sodium retention results from decreased renal function,
leading to fluid retention and edema, causing hypertension. Anemia results from lack of
erythropoietin and red blood cell production. This is reflected in LBs low Hgb and Hct lab
CASE STUDY OF LB AND CHRONIC KIDNEY DISEASE
values. Hyperkalemia, hyperphosphatemia, uremia, azotemia, and oliguria are caused by
decreased excretion and reabsorption in impaired kidneys. LBs potassium lab values reflect this
effect as well. Although there is no lab for her serum phosphorus levels, it is expected that this
lab value would be elevated.
As kidney function decreases, a deficiency of active form of vitamin D occurs, leading to
impaired intestinal calcium absorption and secondary hyperparathyroidism. The combination of
decreased intestinal absorption of calcium, along with decreased excretion of phosphorus
resulting from impaired renal function, contribute to this. Increased serum phosphorus and
decreased serum calcium elicit PTH secretion (Spoek, 2014). PTH then triggers bone breakdown
in order to increase calcium levels. This is also meant to increase phosphorus excretion in the
kidneys, but this does not occur due to impaired renal function. This develops a cycle of bone
breakdown leading to renal osteodystrophy. Calcium and phosphorus accumulation in the blood
can form hard deposits in the body that can cause tissue hardening. LBs vitamin D level was
incredibly low, indicative of impaired renal vitamin D activation.
Other labs indicative of LBs CKD are her low GFR, high BUN, and high Creatinine.
GFR reflects the rate substances are cleared from the plasma by the glomeruli; therefore,
decreased GFR in CKD is expected and used as a diagnostic criterion. High BUN and Creatinine
lab results are common in patients with impaired renal function, as less filtration is taking place.
In addition to LBs altered renal lab values, her fasting blood glucose was extremely high despite
the use of insulin. This could be a result of infection, as blood glucose levels are elevated in the
bodys response to infection (Nelms, Sucher, Lacey, & Long, 2011). The low sodium value
initially seemed to indicate hyponatremia. Decreased serum sodium can be indicative of
peripheral edema, as noted in LBs chart (Nelms, Sucher, Lacey, & Long, 2011).
CASE STUDY OF LB AND CHRONIC KIDNEY DISEASE
10
Treatment options for CKD Stage V include renal replacement therapies such as
hemodialysis and peritoneal dialysis, and kidney transplant. Hemodialysis works to replace the
function of the kidneys by removing urea and waste by filtering the blood through a dialyzer, or
artificial kidney, through a semipermeable membrane (Nelms, Sucher, Lacey, & Long, 2011).
The patients blood leaves their body via an arteriovenous fistula (AVF) or dual lumen catheter,
is filtered outside the body through a dialyzer, and then returned to the body (Nelms, Sucher,
Lacey, & Long, 2011). A patient with CKD Stage V must go to a clinic three days per week in
order to receive hemodialysis treatments. Hemodialysis patients much adhere to a very strict diet.
In Peritoneal dialysis, a sterile solution called dialysate is instilled into the peritoneal
cavity via a surgically implanted peritoneal catheter. Urea and waste products are removed via
the peritoneal membrane (Nelms, Sucher, Lacey, & Long, 2011). Peritoneal dialysis treatments
are continuous and can be done at home. Patients can learn to exchange the dialysate solution
themselves, as well as use a cycler machine at night to exchange the dialysate solution. The main
draw to peritoneal dialysis for patients would be the independence and ability to conduct
treatments from home. Also, because peritoneal dialysis is continuous, the patient is allowed a
more liberal diet.
Individuals with CKD can live long and relatively normal lives while on renal
replacement therapy, but this therapy is required in order to continue living with the disease.
Customary medical nutrition therapy for patients with CKD not on dialysis, on hemodialysis, and
peritoneal dialysis are outlined in Table 4.
11
CASE STUDY OF LB AND CHRONIC KIDNEY DISEASE
Table 4
Medical Nutrition Therapy for Treatments of CKD
Treatment Energy Protein
Na
K
Not on
30-35
Restriction 1.5-3 Monitor
Dialysis
kcal/kg to delay
g/day serum
progression
levels
0.8-1.1g/kg
Hemodialysis
30-35
1.2g/kg
kcal/kg
Peritoneal 30-35
1.2-1.3
Dialysis
kcal/kg g/kg
Phosphorus
Monitor
serum
levels
Fluid
Unrestricted
with normal
urine output
Supplement
2
2-3
g/day g/day
0.8-1 g/day
1000ml/day
plus urine
output
Renal
vitamin,
B vitamins,
folic acid,
vitamin C,
iron,
vitamin D
2-4
3-4
g/day g/day
0.8-1 g/day
Unrestricted
(Nelms, Sucher, Lacey, & Long, 2011)
Nutrition Care for LB
Two nutrition diagnoses were identified for LB during the nutrition assessment.
1. Impaired nutrient utilization related to CKD Stage IV as evidenced by Potassium,
Sodium, BUN, Creatinine, GFR laboratory values.
2. Increased nutrient needs related to surgical procedure and infection as evidenced by
surgical wound and need for antibiotics.
Energy and protein needs were estimated using kcal/kg and g/kg method per facility
standards. Due to LBs recent surgical procedure and active infection, her energy requirements
were estimated to be 30-35kcal/kg, 1635-1907kcal/day. There were many factors to consider
when estimating her protein needs. She has increased protein needs related to her surgical wound
and infection, but protein restrictions, 0.8-1.1g/kg, have been found to significantly reduce
urinary albumin secretion in type 1 diabetics (Academy of Nutrition and Dietetics Evidence
CASE STUDY OF LB AND CHRONIC KIDNEY DISEASE
12
Analysis Library). Considering LBs wound and infection, along with the benefit of protein
restriction, her protein needs were estimated to be 1.1g/kg, 60g/day.
Nutrition interventions included changing the diet order to controlled carbohydrate 60g
protein renal diet and patient education. LBs renal labs were significantly altered, so she was put
on a renal diet in an attempt to normalize them and limit renal stress. Education consisted of her
nutrition plan of care, including the implementation of renal restrictions to the controlled
carbohydrate diet. The patient was receptive to the information, verbalized understanding, and
agreed to try the renal diet. Smoking cessation and the negative impacts of smoking on her
condition were also discussed. She was very motivated as she had not had a cigarette in three
weeks, and she planned to continue.
Labs were ordered for phosphorus, parathyroid hormone, and Hemoglobin A1C. The plan
was to reassess after repeat labs were drawn for need of further intervention. Goals included
meeting 75% of estimated needs, oral intake greater than 50%, nutrition related lab values within
normal limits, improved skin status, glycemic control, honor the patients food preferences, and
patient verbalizing knowledge of appropriate diet.
LB was visited again on 8/27/15. There were no repeat labs or weight obtained since the
initial assessment. Her oral intake was consistently 90-100% over seven days. She reported good
appetite and tolerance of the current diet order. She verbalized understanding of her diet and
agreed to continue with the current medical nutrition therapy. LB denied any nutrition questions.
The patient was meeting estimated needs with current oral intake. Following up on repeat lab
values will allow for further assessment of the adequacy and appropriateness of the medical
nutrition therapy in place.
CASE STUDY OF LB AND CHRONIC KIDNEY DISEASE
13
NHC allows residents to smoke outside and, unfortunately LB began smoking again.
Counseling for smoking cessation then took place. LB reported that she would work to try to
stop smoking when she was discharged back home. She stated that it was too difficult to quit
smoking while she was not feeling well, and she believed she would have greater success when
she was back at home and life is back to normal. LB seemed to be in the contemplation stage
of change for smoking cessation.
Conclusion
LB was a patient admitted into Novato Healthcare Center on 8/17/15 after a
hospitalization for a gangrenous toe resulting in amputation of the 1st and 2nd digits on the left
foot. She has an extensive medical history including Type 1 Diabetes Mellitus and Chronic
Kidney Disease Stage IV. The nutrition care process was conducted for LB. Due to altered renal
lab values, her diet order was changed from carbohydrate controlled to a carbohydrate controlled
60g protein renal diet. Patient education was conducted on the nutrition plan of care. Counseling
also took place for smoking cessation, though it was not successful. LB tolerated her diet change
very well and maintained an oral intake of 90-100%, meeting her estimated needs. More follow
up is needed with this patient as repeat lab values were not obtained. Update lab values will
allow for assessment of appropriateness and adequacy of the nutrition therapy in place.
Many factors play a role in the nutrition care of a patient in a skilled nursing facility.
While in school, nutrition students are taught medical nutrition therapies for individual disease
states. There is little to no instruction on providing medical nutrition therapy to patients with
multiple disease states requiring nutrition intervention. Finding a balance in order to address all
disease states, yet still provide the patient with a desirable diet, is paramount to providing quality
patient care.
CASE STUDY OF LB AND CHRONIC KIDNEY DISEASE
14
References
Academy of Nutrition and Dietetics Evidence Analysis Library. "Is MNT provided by a
Registered Dietitian for chronic kidney disease (CKD) in adults effective?" Academy of
Nutrition and Dietetics, Accessed 1 September 2015,
https://www.andeal.org/topic.cfm?menu=5303&cat=4487
Academy of Nutrition and Dietetics Evidence Analysis Library. What is the evidence for the
effectiveness of restricted protein intake and nephrotic syndrome? Academy of Nutrition
and Dietetics, Accessed 1 September 2015,
http://www.andeal.org/topic.cfm?menu=5303&cat=1483
Centers for Disease Control and Prevention (CDC). National Chronic Kidney Disease Fact
Sheet: General Information and National Estimates on Chronic Kidney Disease in the
United States, 2014. Atlanta, GA: US Department of Health and Human Services,
Centers for Disease Control and Prevention; 2014
Matel, J. (2013). Fluid, Electrolyte, and Acid Base Balance [PowerPoint slides]. Retrieved from
http://ilearn.sfsu.edu/
Nelms, M., Sucher, K. P., Lacey, K., & Long Roth, S. (2011). Nutrition Therapy and
Pathophysiology (2nd ed.). Belmont, CA: Brooks/Cole Cengage Learning.
Orth, S. R., & Hallan, S. I. (2008). Smoking: a risk factor for progression of chronic kidney
disease and for cardiovascular morbidity and mortality in renal patientsabsence of
evidence or evidence of absence?. Clinical Journal of the American Society of
Nephrology, 3(1), 226-236.
Spoek, K. (2014). Renal [PowerPoint slides]. Retrieved from http://ilearn.sfsu.edu
Scott, L. J., Warram, J. H., Hanna, L. S., Laffel, L. M., Ryan, L., & Krolewski, A. S. (2001). A
nonlinear effect of hyperglycemia and current cigarette smoking are major determinants
of the onset of microalbuminuria in type 1 diabetes.Diabetes, 50(12), 2842-2849.
Silverstein, P. (1992). Smoking and wound healing. The American journal of medicine, 93(1),
S22-S24.
S-ar putea să vă placă și
- Denise Zaragoza ResumeDocument2 paginiDenise Zaragoza Resumeapi-242880215Încă nu există evaluări
- Acute Care Case Study-Denise ZaragozaDocument11 paginiAcute Care Case Study-Denise Zaragozaapi-242880215Încă nu există evaluări
- Denise Zaragoza CN-LMPDocument64 paginiDenise Zaragoza CN-LMPapi-242880215Încă nu există evaluări
- Bowel Care Formulary-1Document1 paginăBowel Care Formulary-1api-242880215Încă nu există evaluări
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (894)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (265)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (119)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- Chemistry InvestigatoryDocument19 paginiChemistry Investigatoryakhilnz06Încă nu există evaluări
- 2 Ligan First MassengerDocument32 pagini2 Ligan First MassengerikhararaÎncă nu există evaluări
- Pro CyclesDocument7 paginiPro Cyclestselentisharris15867% (3)
- GTU 104.2015 Teaching Timetable and Assessment ScheduleDocument9 paginiGTU 104.2015 Teaching Timetable and Assessment ScheduleJebatAl-KelantaniÎncă nu există evaluări
- Metformin in PCOSDocument5 paginiMetformin in PCOSbalaramÎncă nu există evaluări
- Booklet The 8th JAKINUDocument20 paginiBooklet The 8th JAKINUsamuelionardiÎncă nu există evaluări
- Adrenal Cortex DR - GomezDocument13 paginiAdrenal Cortex DR - Gomezvicbart11Încă nu există evaluări
- مراجعة ليلة الامتحان فى مادة «البيولوجي»Document98 paginiمراجعة ليلة الامتحان فى مادة «البيولوجي»Ahmed Ghanam100% (1)
- Managing Diabetes with Diet, Exercise and MedicationDocument25 paginiManaging Diabetes with Diet, Exercise and MedicationaliÎncă nu există evaluări
- Bullous Pemphigoid in Adolescence: Aikaterini Patsatsi MD, MSC, PHD Victoria P. Werth MDDocument5 paginiBullous Pemphigoid in Adolescence: Aikaterini Patsatsi MD, MSC, PHD Victoria P. Werth MDThomas UtomoÎncă nu există evaluări
- Insulin Resistance and PCOS-dr. Hilma Final 11 Juli 2021 FIXDocument48 paginiInsulin Resistance and PCOS-dr. Hilma Final 11 Juli 2021 FIXputrihealthirezaÎncă nu există evaluări
- AACE GuidelinesDocument20 paginiAACE GuidelinesdavekeatsÎncă nu există evaluări
- Evaluation of Infertile CoupleDocument70 paginiEvaluation of Infertile CoupleNdenwaneku OkuwaÎncă nu există evaluări
- EndocrineDocument144 paginiEndocrineaartiÎncă nu există evaluări
- HYPERPARATHYROIDISM On PPDocument26 paginiHYPERPARATHYROIDISM On PPSobia NaseemÎncă nu există evaluări
- Human Physiology MCQSDocument8 paginiHuman Physiology MCQSHaris Qurashi100% (1)
- Adolescence and Puberty PDFDocument318 paginiAdolescence and Puberty PDFjorge torresÎncă nu există evaluări
- Labreportnew 6782Document1 paginăLabreportnew 6782Shahabuddin AnsariÎncă nu există evaluări
- Chapter 15 Student Version The Urinary System 2020.ppt (1402)Document20 paginiChapter 15 Student Version The Urinary System 2020.ppt (1402)S. MartinezÎncă nu există evaluări
- Jurnal PDFDocument15 paginiJurnal PDFElma YuliantiÎncă nu există evaluări
- Congenital Adrenal HyperplasiaDocument42 paginiCongenital Adrenal HyperplasianeysaonlineÎncă nu există evaluări
- Biomarkers of Male Hypogonadism in Childhood and AdolescenceDocument13 paginiBiomarkers of Male Hypogonadism in Childhood and AdolescenceScott LoveÎncă nu există evaluări
- ACTIVITY 1: Nursing Care PlanDocument4 paginiACTIVITY 1: Nursing Care PlanChelsea JardelezaÎncă nu există evaluări
- Strengthening The Global Risk ManagementDocument31 paginiStrengthening The Global Risk ManagementSriNoviantiÎncă nu există evaluări
- Hormonal Therapy in DubDocument20 paginiHormonal Therapy in DubpreethiÎncă nu există evaluări
- Hypothyroidism in Context: Where We've Been and Where We're GoingDocument12 paginiHypothyroidism in Context: Where We've Been and Where We're Going1130017003 AIMMATUL CHANIFAHÎncă nu există evaluări
- Thyrotoxicosis: Presenter: Emiacu Kenneth Facilitator: Dr. Freddie KibengoDocument35 paginiThyrotoxicosis: Presenter: Emiacu Kenneth Facilitator: Dr. Freddie KibengoNinaÎncă nu există evaluări
- 3ES-2 Thyroid and Antithyroid Drugs 1436Document46 pagini3ES-2 Thyroid and Antithyroid Drugs 1436Muath AlqarniÎncă nu există evaluări
- Thyroid SynthesisDocument15 paginiThyroid Synthesistitin indramayaÎncă nu există evaluări
- The Reproductive System: Powerpoint Lecture SlidesDocument175 paginiThe Reproductive System: Powerpoint Lecture SlidesMartin R. GarciaÎncă nu există evaluări