Documente Academic
Documente Profesional
Documente Cultură
Glomerulonephritis
Încărcat de
Matthew RyanDrepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Glomerulonephritis
Încărcat de
Matthew RyanDrepturi de autor:
Formate disponibile
Glomerulonephritis Description/Etiology:
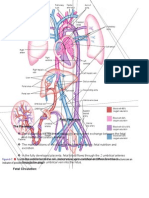
Glomerulonephritis is an inflammation of the glomerulus. There are two types of glomerulonephritis: Acute: This might occur up to 10-21 days following a respiratory tract streptococcal bacterial infection or from a skin infection as a result of antigen/antibody groups trapped in the tubules causing edema that decreases filtering and thus causes urine to be retained. Chronic: An abnormal immune system, bacterial or viral infection, disease or toxin causes progressive dysfunction of the glomerulus over the years and decline of renal function Most causes of acute GN are infectious In children, acute disease is most often a response to a group A betahemolytic streptococcal infection of the skin or pharynx (acute postinfectious glomerulonephritis or APIGN) Highest incidence in children 2-6 years of age More common in boys PATHOPHYSIOLOGY: APIGN: Acute poststreptococcal glomerulonephritis results from entrapment and collection of antigen-antibody complexes in the glomerular capillary membranes after infection with group A hemolytic streptococci. The antigens stimulate the formation of antibodies. Circulating antigen-antibody complexes become lodged in the glomerular capillaries. Glomerular injury occurs when complexes initiate the release of immunologic substances that break down cells and increase membrane permeability allowing RBC and red cell casts to be excreted
Sodium and water are retained leading to edema The severity of glomerular damage and renal insufficiency depends on the size, number, location, duration of exposure, and type of antigen-antibody complexes. Oliguric phase initially seen in glomerulonephritis followed by a diuretic phase. Most individuals with acute glomerulonephritis (AGN) improve dramatically within weeks and recover completely within 1-2 yr Renal damage continues to progress for patients with chronic glomerulonephritis (CGN). CGN is one of the most common causes of chronic renal failure (CRF) CLINICAL MANIFESTATIONS (adults and children the same): Many children are asymptomatic. Abrupt onset of symptoms Flank or mid-abdominal pain Irritability Malaise Fever (AGN) Dyspnea Orthopnea and dyspnea Moist crackles on auscultation Distended neck veins Periorbital edema
Facial edema that is worse in the morning but then spreads to extremities and abdomen with progression of the day Mild to severe hypertension Decreased glomerular filtration rate leading to decreased urine output
Changes in the level of consciousness Anorexia/nausea Headache Back pain Pruritus (CGN) Oliguria (especially with CGN) Uremia (CGN) Azotemia Acidosis (CGN)
LABORATORY/DIAGNOSTIC TESTS Elevated BUN and serum Creatinine
Antistreptolysin-O (ASO) titer: positive indicating the presence of strep antibodies from a recent strep respiratory infection Erythrocyte sedimentation rate (ESR) (elevated indicating active inflammatory response) White blood cell count: elevated indicating inflammation and presence of active strep infection
Urinalysis reveals: proteinuria, hematuria, cell debris (red cells and casts), increased urine specific gravity, urine has a smoky or tea color to it Electrolyte abnormalities: hyperkalemia, hypoalbuminemia, and hyperphosphatemia Antihyaluronidase (AHase), antideoxyribonuclease B (ADNase-B), and streptozyme antibodies may be present.
Serum complement (C3) Decreased initially; increases as recovery takes place; returns to normal at 8 to 10 weeks post glomerulonephritis
X-ray of kidney, ureter, bladder (KUB), and renal ultrasound (to detect structural abnormalities, kidneys may be enlarged with AGN but shrunken and atrophied in CGN) Renal biopsy (to confirm or rule out diagnosis) Chest x-ray may show cardiac enlargement, pulmonary congestion, or pleural effusion during the edematous phase of acute disease. MEDICAL MANAGEMENT: Management consists of general supportive measures and early recognition and treatment of complications.
Patients who have normal blood pressure and a satisfactory urine output can often be treated at home.
Patients with substantial edema, hypertension, gross hematuria, or significant oliguria are hospitalized because of the unpredictability of complications.
Dietary restrictions depend on the stage and severity of the disease, especially the extent of edema. Moderate sodium restriction and even fluid restriction may be instituted for patients with hypertension and edema. Foods with substantial amounts of potassium are generally restricted during the period of oliguria.
Antibiotic therapy is indicated only for those children with evidence of persistent streptococcal infections.
Diuretics such as furosemide (Lasix) to reduce extracellular fluid overload
Antihypertensive such as hydralazine.
Corticosteroids such a prednisone to reduce the inflammatory response.
Severe hypertension is children is a medical emergency and can cause seizures and encephalopathy
Dialysis if the patient goes into uremia or acute renal failure.
NURSING MANAGEMENT: Careful assessment of the disease status, with regular monitoring of vital signs (including frequent measurement of blood pressure), fluid balance, and behavior
Evaluate and record the volume and character of urine, and weigh the patient daily.
Observe for signs of dehydration in children with restricted fluid intake, especially those who are not severely edematous or those who have lost weight.
For most patients a regular diet is allowed, but it should contain no added salt. Foods high in sodium and salted treats are eliminated, and parents/patients and friends are advised not to bring snacks such as potato chips or pretzels.
Fluid restriction, if prescribed, is more difficult, and the amount permitted should be evenly divided throughout the waking hours.
Assess respiratory system for lung sounds, difficulty breathing, crackles in the lungs suggesting fluid overload Assess cardiovascular status, heart rate, heart sounds, presence of S3 suggesting fluid overload.
Assess extremities for edema.
Monitor serum electrolytes, BUN, and creatinine.
If severe hypertension is present monitor the patients neurological status closely and implement seizure precautions if necessary.
Patient and Family Teaching Educate the patient/caregivers about appropriate dietary management/restrictions.
Provide parent/patient education and support in preparation for discharge and home care; include education in home management and the need for follow-up care and health supervision.
Stress to the patient the need for regular blood pressure, urine protein, and renal function assessments during the convalescent months to detect recurrence. Teach the family about administration and side effects of antibiotics, corticosteroids, diuretics and antihypertensive medications.
Advise the patient with a history of chronic upper respiratory tract infections to report immediately signs and symptoms of infection (such as fever or sore throat).
Encourage a pregnant woman with a history of the disorder to have frequent medical evaluations because pregnancy further stresses the kidneys and increases the risk of chronic renal failure.
S-ar putea să vă placă și
- Community Acquired Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDe la EverandCommunity Acquired Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsÎncă nu există evaluări
- Acute Glomerulonephritis: Mohd Zamir Ghouse 060100848Document40 paginiAcute Glomerulonephritis: Mohd Zamir Ghouse 060100848zamirsg100% (1)
- Management of Tuberculosis: A guide for clinicians (eBook edition)De la EverandManagement of Tuberculosis: A guide for clinicians (eBook edition)Încă nu există evaluări
- Acute GlomerulonephritisDocument17 paginiAcute GlomerulonephritisBayanSecond WardÎncă nu există evaluări
- Metabolic Alkalosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDe la EverandMetabolic Alkalosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsÎncă nu există evaluări
- Acute GlomerulonephritisDocument21 paginiAcute Glomerulonephritisbrinda johnÎncă nu există evaluări
- Rheumatic Fever: Causes, Tests, and Treatment OptionsDe la EverandRheumatic Fever: Causes, Tests, and Treatment OptionsÎncă nu există evaluări
- Hyperosmolar Hyperglycemic Nonketotic Syndrome (HHNS)Document8 paginiHyperosmolar Hyperglycemic Nonketotic Syndrome (HHNS)amiraÎncă nu există evaluări
- Chronic Renal FailureDocument28 paginiChronic Renal FailurePatricia Nadine Sarcadio NeffeÎncă nu există evaluări
- Schistosomiasis Case StudyDocument5 paginiSchistosomiasis Case Studyapi-318749549Încă nu există evaluări
- Diabetic KetoacidosisDocument12 paginiDiabetic Ketoacidosispolaris_027Încă nu există evaluări
- Nephroticsyndromeandacasereport 140727015201 Phpapp02Document38 paginiNephroticsyndromeandacasereport 140727015201 Phpapp02TareqhoseinÎncă nu există evaluări
- Lupus Case ReportDocument1 paginăLupus Case ReportMendy HararyÎncă nu există evaluări
- Acute Glomerulonephritis (AGN)Document5 paginiAcute Glomerulonephritis (AGN)smashayielÎncă nu există evaluări
- Liver Cirrhosis: A Case Study OnDocument31 paginiLiver Cirrhosis: A Case Study OnCharmaine del RosarioÎncă nu există evaluări
- Acute GlomerulonephritisDocument7 paginiAcute GlomerulonephritisSel CuaÎncă nu există evaluări
- Diabetic Ketoacidosis Case StudyDocument6 paginiDiabetic Ketoacidosis Case StudyJohn AlcantaraÎncă nu există evaluări
- Acute Glomerulonephritis Case StudyDocument12 paginiAcute Glomerulonephritis Case Study19lyon92100% (6)
- Case Study - Chronic Kidney Disease Treated With DialysisDocument7 paginiCase Study - Chronic Kidney Disease Treated With Dialysisapi-387604918100% (1)
- Cholelithiasis: Group MembersDocument12 paginiCholelithiasis: Group MembersShiela GutierrezÎncă nu există evaluări
- Nephrotic SyndromeDocument61 paginiNephrotic SyndromeRanah Julia Garchitorena AyoÎncă nu există evaluări
- Anemia 130809044630 Phpapp01Document21 paginiAnemia 130809044630 Phpapp01Siddharth Das100% (1)
- Gastro Intestinal Bleeding DR - muayAD ABASSDocument59 paginiGastro Intestinal Bleeding DR - muayAD ABASSMAFADHELÎncă nu există evaluări
- CKD PresentationDocument51 paginiCKD PresentationBasneyatPragyanÎncă nu există evaluări
- Hepatic EncephalopathyDocument3 paginiHepatic EncephalopathyAnonymous GIGXKjfLÎncă nu există evaluări
- Case Study Cirrhosis of The LiverDocument35 paginiCase Study Cirrhosis of The Liverapi-24237671967% (3)
- PancreatitisDocument59 paginiPancreatitisAarif RanaÎncă nu există evaluări
- Diabetic KetoacidosisDocument5 paginiDiabetic KetoacidosisJill Catherine Cabana100% (3)
- Electrolyte Imbalance 1Document3 paginiElectrolyte Imbalance 1Marius Clifford BilledoÎncă nu există evaluări
- SiadhDocument10 paginiSiadhehjing75% (4)
- Pulmonary EmbolismDocument16 paginiPulmonary EmbolismniyigokÎncă nu există evaluări
- Case Study - Acute Glomerulonephritis Sample Case Study Report For PCL Level by Amrit BanstolaDocument15 paginiCase Study - Acute Glomerulonephritis Sample Case Study Report For PCL Level by Amrit BanstolaAmrit Banstola100% (5)
- Addison's DiseaseDocument15 paginiAddison's DiseaseRonald A. Ogania50% (4)
- Acute Glomerulonephritis - CSDocument31 paginiAcute Glomerulonephritis - CSMASIIÎncă nu există evaluări
- Acute Liver FailureDocument24 paginiAcute Liver FailureMohd Johari Mohd ShafuwanÎncă nu există evaluări
- Chronic Kidney Disease Case StudyDocument52 paginiChronic Kidney Disease Case StudyGi100% (1)
- Acute Lymphocytic LeukemiaDocument12 paginiAcute Lymphocytic Leukemiajustin_saneÎncă nu există evaluări
- Syndrome of Inappropriate Secretion of Anti Diuretic HormoneDocument39 paginiSyndrome of Inappropriate Secretion of Anti Diuretic Hormonefarmasi_hmÎncă nu există evaluări
- Predisposing Conditions, Management and Prevention of Chronic Kidney DiseaseDocument52 paginiPredisposing Conditions, Management and Prevention of Chronic Kidney DiseaseSaad MotawéaÎncă nu există evaluări
- Hemodialysis: Carina Joane Villareal-Barroso, R.N.,M.NDocument108 paginiHemodialysis: Carina Joane Villareal-Barroso, R.N.,M.NJune BarsÎncă nu există evaluări
- Liver CancerDocument1 paginăLiver CancerTarantado67% (3)
- Case On ColitisDocument34 paginiCase On ColitisAamer SyedÎncă nu există evaluări
- Chronic Kidney Disease Case PresDocument32 paginiChronic Kidney Disease Case Presnnaesor_1091Încă nu există evaluări
- Chronic Kidney Disease Case PresentationDocument14 paginiChronic Kidney Disease Case Presentationnnaesor_109150% (2)
- Acute Glumerulo NephritisDocument13 paginiAcute Glumerulo NephritisNathan Vince CruzÎncă nu există evaluări
- What Is A Communicable DiseaseDocument3 paginiWhat Is A Communicable DiseaseChrisel D. SamaniegoÎncă nu există evaluări
- Bronchitis ReportDocument34 paginiBronchitis ReportRolinette DaneÎncă nu există evaluări
- Case+Study AGN MINEDocument66 paginiCase+Study AGN MINEJm BernardoÎncă nu există evaluări
- Diabetic Ketoacidosis Written ReportDocument19 paginiDiabetic Ketoacidosis Written ReportEros Victorino100% (2)
- Acute GlomerulonephritisDocument12 paginiAcute Glomerulonephritiskuchaibaru90Încă nu există evaluări
- Case 1 (Pneumonia) ArioDocument26 paginiCase 1 (Pneumonia) ArioJoegie ArioÎncă nu există evaluări
- Group B1 (Cholera)Document66 paginiGroup B1 (Cholera)Krisianne Mae Lorenzo FranciscoÎncă nu există evaluări
- Rheumatic Heart Disease IntroDocument3 paginiRheumatic Heart Disease IntroTrexy LozanoÎncă nu există evaluări
- Case AGNDocument66 paginiCase AGNMohaima PanditaÎncă nu există evaluări
- Buerger DiseaseDocument3 paginiBuerger DiseaseElmer DizonÎncă nu există evaluări
- HyperkalemiaDocument3 paginiHyperkalemiaSergeiÎncă nu există evaluări
- Case Study ReportDocument23 paginiCase Study Reportapi-290866384Încă nu există evaluări
- Case Study: Congestive Heart FailureDocument7 paginiCase Study: Congestive Heart FailureXI-E / 21 / MARY TRIANAÎncă nu există evaluări
- What Is Acute Glomerulonephritis?: Acute Glomerulonephritis (GN) Comprises A Specific Set of Renal Diseases inDocument6 paginiWhat Is Acute Glomerulonephritis?: Acute Glomerulonephritis (GN) Comprises A Specific Set of Renal Diseases inAnnapoorna SHÎncă nu există evaluări
- Urinary Tract DisordersDocument54 paginiUrinary Tract Disorderssharon ocharaÎncă nu există evaluări
- Boot Camp Hemodynamic MonitoringDocument37 paginiBoot Camp Hemodynamic MonitoringTinaHo100% (7)
- DocuNotes Clinical Pocket Guide To Effective ChartingDocument203 paginiDocuNotes Clinical Pocket Guide To Effective ChartingShirlyn Ares Navarro96% (47)
- Cardiovascular DrugsDocument17 paginiCardiovascular DrugsMatthew RyanÎncă nu există evaluări
- Otitis MediaDocument7 paginiOtitis MediaMatthew RyanÎncă nu există evaluări
- FluDocument5 paginiFluMatthew RyanÎncă nu există evaluări
- Acute and Chronic PyelonephritisDocument7 paginiAcute and Chronic PyelonephritisMatthew Ryan100% (1)
- Fetal Perfusion/Congenital Heart DefectsDocument13 paginiFetal Perfusion/Congenital Heart DefectsMatthew RyanÎncă nu există evaluări
- Glucose MonitoringDocument4 paginiGlucose MonitoringMatthew RyanÎncă nu există evaluări
- Nursing Care of The Patient With Seizures and EpilepsyDocument8 paginiNursing Care of The Patient With Seizures and EpilepsyMatthew RyanÎncă nu există evaluări
- Otitis MediaDocument6 paginiOtitis MediaMatthew RyanÎncă nu există evaluări
- Understanding CorticosteroidsDocument4 paginiUnderstanding CorticosteroidsMatthew RyanÎncă nu există evaluări
- Simplifying Neurologic Assessment.5Document4 paginiSimplifying Neurologic Assessment.5Matthew RyanÎncă nu există evaluări
- How To Care For TracheostomyDocument6 paginiHow To Care For TracheostomyMatthew RyanÎncă nu există evaluări
- Acute Respiratory Distress SyndromeDocument9 paginiAcute Respiratory Distress SyndromeMatthew Ryan100% (2)
- SepsisDocument14 paginiSepsislengkong100% (9)
- Making Sense of Abdominal Assessment.5Document4 paginiMaking Sense of Abdominal Assessment.5Matthew RyanÎncă nu există evaluări
- Managing Heart FailureDocument10 paginiManaging Heart FailureMatthew RyanÎncă nu există evaluări
- Breath Sounds Incredibly EasyDocument4 paginiBreath Sounds Incredibly EasyMatthew Ryan100% (3)
- A Look at Standard Medications For LVSD.3Document4 paginiA Look at Standard Medications For LVSD.3Matthew RyanÎncă nu există evaluări
- Nursing Care of The Patient With Seizures and EpilepsyDocument8 paginiNursing Care of The Patient With Seizures and EpilepsyMatthew RyanÎncă nu există evaluări
- Newborn RespirationDocument3 paginiNewborn RespirationMatthew RyanÎncă nu există evaluări
- IV InfiltrationDocument4 paginiIV InfiltrationMatthew Ryan100% (1)
- Nursing Management of Seizures and EpilepsyDocument36 paginiNursing Management of Seizures and EpilepsyMatthew Ryan100% (6)
- Assessing RespirationsDocument5 paginiAssessing RespirationsMatthew Ryan100% (1)
- Assessing Arterial Blood PressureDocument11 paginiAssessing Arterial Blood PressureMatthew RyanÎncă nu există evaluări
- Nursing Management of Seizures and EpilepsyDocument36 paginiNursing Management of Seizures and EpilepsyMatthew Ryan100% (6)
- JaundiceDocument3 paginiJaundiceMatthew Ryan100% (1)
- Neural Tube DefectsDocument2 paginiNeural Tube DefectsMatthew RyanÎncă nu există evaluări
- Assessing Radial PulseDocument4 paginiAssessing Radial PulseMatthew RyanÎncă nu există evaluări
- Bravo Petroleum ProfileDocument8 paginiBravo Petroleum ProfileJacob Thom ZiwahwaÎncă nu există evaluări
- International Standard Paper SizesDocument34 paginiInternational Standard Paper SizesAman KumarÎncă nu există evaluări
- Pengaruh Volume Pemberian Air Terhadap Pertumbuhan Bibit Kelapa Sawit Di Pembibitan UtamaDocument11 paginiPengaruh Volume Pemberian Air Terhadap Pertumbuhan Bibit Kelapa Sawit Di Pembibitan UtamaTahum MatfuahÎncă nu există evaluări
- Patel, Anita - Super Indian Snack and Street Food Recipes PDFDocument117 paginiPatel, Anita - Super Indian Snack and Street Food Recipes PDFBella ImèneÎncă nu există evaluări
- Synthesis of Sentences Is The Opposite ofDocument9 paginiSynthesis of Sentences Is The Opposite ofSpsc AspirantsÎncă nu există evaluări
- The Symbols Found in TarotDocument17 paginiThe Symbols Found in TarotPEdro100% (1)
- Certificado V34aDocument1 paginăCertificado V34aElizabeth Durán SánchezÎncă nu există evaluări
- Method Statement For Boom Barrier Installation (Rev00) ELV2Document38 paginiMethod Statement For Boom Barrier Installation (Rev00) ELV2balajiÎncă nu există evaluări
- Poem Summary - Keeping QuietDocument3 paginiPoem Summary - Keeping QuietVignesh Mohan100% (2)
- L 7 Thermal Death Time DataDocument21 paginiL 7 Thermal Death Time DataVaibhav GuptaÎncă nu există evaluări
- Covid 19Document1 paginăCovid 19Sadiq NaseerÎncă nu există evaluări
- Aspire 7535 ManualDocument220 paginiAspire 7535 ManualinklabsÎncă nu există evaluări
- SBB Product NoteDocument3 paginiSBB Product NoteFilipe MartinsÎncă nu există evaluări
- UD11T4107 English Maritime History Human FactorDocument4 paginiUD11T4107 English Maritime History Human FactorParminder singh parmarÎncă nu există evaluări
- EN 301.908-2 Ver 3.2.1Document37 paginiEN 301.908-2 Ver 3.2.1DHDIDIDÎncă nu există evaluări
- Sound Healing For Health and Well - BeingDocument36 paginiSound Healing For Health and Well - Beingtormenta7azul6225100% (9)
- New Magic Grammar TE3BDocument34 paginiNew Magic Grammar TE3BYume ZhuÎncă nu există evaluări
- 8 - Precast Concrete Structures-Students PDFDocument17 pagini8 - Precast Concrete Structures-Students PDFsitehabÎncă nu există evaluări
- Electric Circuits 1 MSDocument4 paginiElectric Circuits 1 MSEvaÎncă nu există evaluări
- 24 Port - 48 Port CAT6A Patch PanelDocument2 pagini24 Port - 48 Port CAT6A Patch PanelSajid KhanÎncă nu există evaluări
- Euroncap 2017 Audi q5 DatasheetDocument13 paginiEuroncap 2017 Audi q5 DatasheetCosmin AnculiaÎncă nu există evaluări
- Doxiadis, Constantinos (1968) EkisticsDocument556 paginiDoxiadis, Constantinos (1968) EkisticsCelje1234Încă nu există evaluări
- 21 Day Fasting & Prayer 2022Document29 pagini21 Day Fasting & Prayer 2022StephenÎncă nu există evaluări
- PC-FT 403: Lecture (1) byDocument21 paginiPC-FT 403: Lecture (1) byFT 19 Suparno DasÎncă nu există evaluări
- Shell Omala S2 GX 150: Performance, Features & Benefits Main ApplicationsDocument2 paginiShell Omala S2 GX 150: Performance, Features & Benefits Main ApplicationsVelibor KaranovicÎncă nu există evaluări
- Neurology Condition Assessment Methods: Guillain-Barre Syndrome (GBS) Disability ScoreDocument15 paginiNeurology Condition Assessment Methods: Guillain-Barre Syndrome (GBS) Disability ScoreMrinmayeeDeshmukhÎncă nu există evaluări
- Rider's Manual: BMW MotorradDocument136 paginiRider's Manual: BMW MotorradAlex Quintana100% (1)
- Functional Endoscopic Sinus SurgeryDocument3 paginiFunctional Endoscopic Sinus SurgeryDanielicah CruzÎncă nu există evaluări
- Auto CadDocument24 paginiAuto Cadkanchan Redas RedasÎncă nu există evaluări
- Nuitration in Human 3Document2 paginiNuitration in Human 3Usman AmeenÎncă nu există evaluări
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDDe la EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDEvaluare: 5 din 5 stele5/5 (2)
- The Age of Magical Overthinking: Notes on Modern IrrationalityDe la EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityEvaluare: 4 din 5 stele4/5 (28)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionDe la EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionEvaluare: 4 din 5 stele4/5 (404)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeDe la EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeEvaluare: 2 din 5 stele2/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedDe la EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedEvaluare: 5 din 5 stele5/5 (81)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaDe la EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaEvaluare: 4.5 din 5 stele4.5/5 (266)
- Gut: the new and revised Sunday Times bestsellerDe la EverandGut: the new and revised Sunday Times bestsellerEvaluare: 4 din 5 stele4/5 (393)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsDe la EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsEvaluare: 5 din 5 stele5/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisDe la EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisEvaluare: 4.5 din 5 stele4.5/5 (42)
- The Obesity Code: Unlocking the Secrets of Weight LossDe la EverandThe Obesity Code: Unlocking the Secrets of Weight LossEvaluare: 4 din 5 stele4/5 (6)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsDe la EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsÎncă nu există evaluări
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsDe la EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsEvaluare: 3.5 din 5 stele3.5/5 (3)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningDe la EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningEvaluare: 4 din 5 stele4/5 (3)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)De la EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Încă nu există evaluări
- Why We Die: The New Science of Aging and the Quest for ImmortalityDe la EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityEvaluare: 4 din 5 stele4/5 (3)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisDe la EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisEvaluare: 3.5 din 5 stele3.5/5 (2)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryDe la EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryEvaluare: 4 din 5 stele4/5 (44)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeDe la EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeEvaluare: 4.5 din 5 stele4.5/5 (253)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.De la EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Evaluare: 4.5 din 5 stele4.5/5 (110)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisDe la EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisEvaluare: 4 din 5 stele4/5 (1)
- The Marshmallow Test: Mastering Self-ControlDe la EverandThe Marshmallow Test: Mastering Self-ControlEvaluare: 4.5 din 5 stele4.5/5 (58)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsDe la EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsEvaluare: 4.5 din 5 stele4.5/5 (170)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingDe la EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingEvaluare: 4 din 5 stele4/5 (1138)