Documente Academic
Documente Profesional
Documente Cultură
Stridor 1
Încărcat de
DrTarek Mahmoud Abo KammerTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Stridor 1
Încărcat de
DrTarek Mahmoud Abo KammerDrepturi de autor:
Formate disponibile
STRIDOR Stridor is a continuous inspiratory harsh sound produced by partial obstruction in the Etiology region of the larynx or trachea.
Total obstruction cyanosis & death. Acute stridor
Infectious croup
Acute viral laryngitis
Spasmodic laryngitis
Laryngotracheobronchitis Acute bacterial tracheitis Acute bacteria epiglottitis Laryngeal diphtheria
Other causes
Laryngospasm
Laryngeal foreign body
Congenital chronic stridor Tracheomalacia
Chronic stridor
Laryngeal compression (acute)
Laryngeal edema ( allergy, post-extubation)
Laryngomalacia ( most common)
Laryngeal tumors or cyst
Laryngeal web
Acquired chronic stridor Tracheal stenosis
Laryngeal compression ( congenital) Laryngeal stenosis
Laryngeal paralysis
Laryngeal tumors
Laryngeal compression (acquired)
How is the degree of stridor assessed?
The degree of respiratory obstruction is difficult to assess as it may vary from moment to moment. Stridor usually becomes worse if the child cries or becomes agitated. Therefore stridor in a quiet child should be regarded as severe. 1. Inspiratory stridor only, without lower chest wall indrawing (recession or retraction) suggests mild
airway obstruction. These children usually only have stridor when they are upset or crying. There is no stridor when they are sleeping or at rest. 2. The addition of lower chest wall indrawing or stridor during both inspiration and expiration are very
important clinical signs as they indicate worsening airways obstruction. Therefore, expiratory stridor is a sign of severe airway obstruction. Stridor at rest in a quiet child also suggests severe stridor. 3. breathing (tachypnea) are signs of dangerous airway obstruction obstruction. Expiratory stridor is a sign of worsening airway obstruction. The obvious use of chest and abdominal muscles during expiration (active expiration, restlessness or fast
Disappearance or weakening of the peripheral pulse on light palpation during inspiration (pulsus paradoxis), obstruction. Clinical grades of stridor
marked recession, apathy and cyanosis are signs of severe airway obstruction. Stridor becomes softer with severe
Grade 1 (Exertional stridor) : Stridor appears during crying or exercise. < 1 yr of age should be hospitalized. indicated for all cases. indicated.
Grade 2 (Continuous stridor or stridor at rest) : Stridor is present at rest & become worse with exertion. Infants Grade 3 (Stridor with retractions) : Stridor is continuous & accompanied with suprasternal Grade 4 (Stridor with cyanosis) : In addition to continuous stridor & retractions, cyanosis & supraclavicular retractions. The patient looks anxious, irritable, & struggling for breathing. Hospitalization is & altered consciousness occur denoting severe respiratory failure. Urgent hospitalization & ET intubation are
The onset is abrupt or acute & the duration of the illness is short (<1 wk). It is much more common & lifethe larynx or the trachea (infectious croup). However, other causes should be in mind & should be routinely excluded. It includes 5 clinical entities with increasing severity (3 viral & 2 bacterial). Viral infections are more common airway obstruction is severe. Staphylococcus aureus (acute tracheitis) & hemophilus influenza type b (acute epiglottitis) are the 2 main causative bacteria. viruses may be responsible as influenza viruses, adenoviruses, & RSV. With bacterial infections, fever is high & & are usually milder than bacterial infections. Parainfluenza viruses are the principal agents but other Infectious croup threatening than chronic type. Most cases of acute stridor are caused by common viral or bacterial infections of
Acute stridor
illness starts with mild fever, rhinitis, & croupy cough. Stridor appears 1-2 days later & it is usually mild to moderate. Symptoms usually subsides over few or several days. nd cough & stridor that occur principally at night. Stridor is usually moderate in severity & only lasts for several &3 rd 2. Spasmodic laryngitis : It is a viral or propably allergic laryngitis which is characterized by an attack of croupy
1. Acute viral laryngitis : It is a common viral infection which occur mainly in children aging 1-3 yrs. The
hours. The attack may be repeated at nights of the 2 occur.
days but it is usually milder. Recurrence may
3. Laryngotracheobronchitis (croup) : It is a common potentially serious viral infection which mainly hoarseness. Stridor appears 1-2 days later & it is usually moderate to severe inspiratory one. Symptoms are characteristically worse at night & often recur with decreasing intensity for several days & resolve completely & expiratory rhonchi. Rarely, the URT obstruction progresses RR,
occurs in children < 3 yrs of age. The illness starts with mild to moderate fever, rhinitis, barking cough, & reveals slightly RR. There
may be air entry, prolonged expiration,
within a week. Agitation & crying greatly aggravate the illness. Chest examination
presentations & it may be helpful in distinguishing between sever laryngotracheobronchitis & epiglottitis in which the lateral neck X- rays reveals the " thumb sign" due to swollen epiglottis.
(steeple sign). Radiograph should be considered only after airway stabilization in children who have atypical 4. Acute bacterial tracheitis : It is a serious bacterial infection mainly caused by staphylococcuc aureus & principally occurs in children < 3 yrs of age. The illness starts with high fever & gradually progressive stridor.
clinical diagnosis & does not require a radiograph of the neck which may show the typical subglottic narrowing
nasal flaring, suprasternal, infrasternal, & intercostals retractions associated with continuous stridor. Croup is a
epiglottis. Polymorphnuclear leukocytosis is usually present.
Airway obstruction becomes severe & the illness simulates epiglottitis but direct laryngoscopy reveals normal 5. Acute bacterial epiglottitis : It is a very serious & life-threatening infection mainly caused by hemophilus yrs of age (3-7 yrs). The illness starts abruptly with high fever & rapidly progressive stridor. Airway obstruction mouth. The barking cough is rare. Treatment consists of ET-intubation for 2-3 days or tracheostomy followed by IV antibiotics. Management drooling of mouth ( due to inability to swallow) & laboured breathing. The child is leaning forward with open influenza type b bacteria. It has become a rare disease due to immunization. It principally occurs in children > 3 becomes severe within hours. Cyanosis & death rapidly occurs if urgent ET intubation is delayed. Other signs are
can be managed at home.
Most afebrile patients with mild infectious laryngitis, mild laryngotracheobronchitis, or spasmodic laryngitis Worm & moist environment : by taking the child into a bathroom & turning on the hot shower or hot taps.
Home management
Hospital management with grade 3 stridor
moderate cases to need for hospitalization. Expectorants or mucolytics may be used in croup. 3. Suspected bacterial disease (high fever
Drug therapy : Antibiotics (as amoxicillin) & steroids ( as dexmethasone) may be used especially in borderline Hospitalization is indicated in the following condition : 1. Any infant with grade 2 stridor 2. Any child
Inhalation of the hot steam will usually relieve minor obstruction within 30-60 minutes.
& severe obstruction) 4. Grade 4 stridor is an indication of immediate hospitalization & ET- intubation. is very essential to assess the course of the illness & to identify those in need for ET-intubation. minimized. The mother should remain beside the child for reassurance, at least until he sleeps.
Close observation : Frequent monitoring of HR, RR, degree of retractions, colour, & level of consciousness Minimal disturbances : Nursing & medical procedures which disturb the child or anxiety should be Humidification : Warm & moist atmosphere is generally useful. Inhalation of warm water vapor may be soothes inflamed mucosa & 3. provides comfort & reassurance to the child, & anxiety. Drug therapy : It may include : 1. Nebulized epinephrine : This marked in the need for tracheostomy in croup. in : 1. moderate-severe stridor at rest 2. the need for intubation The proposed mechanisms of this cool mist are that it : 1. moistens airways secretions to facilitate clearance helpful in relieving the laryngeal obstruction. This cool mist can be given by nebulizer (cold steam nebulizer). 2.
The mechanism of action may be the constriction of the precapillary arterioles through the - adrenergic receptors fluid resorption from the interstitial space & a in the laryngeal mucousa edema. It is indicated 3.respiratory distress TOF, & ventricular outlet obstruction because of the possible side effects. stridor does not respond to cool mist. It should be used catiously in patients with tachycardia, heart conditions as 4. Hypoxia 5. when
prednisolone 1-2 mg/kg may be used.
(sometimes, a dose as low as 0.15 mg/kg may be effective). Oral dexamethasone is also effective. Oral 3. Antibiotics : They are not indicated in croup (viral) but parenteral antibiotic therapy is important when a bacterial infection is suspected especially in those with high fever. The choices are : Ceftriaxone 50 mg/kg/day
laryngeal mucosa through their anti-inflammatory action. A single IM dose of dexamethasone o.6 mg/kg
2. Corticosteroids : It is the most commonly used & the most essential therapy in croup. This edema in the
single dose (or 100 mg/kg/day in 2 divided doses) or a combination of Ampicillin+Sulbactam. 4. Sedatives are contraindicated because they impair consciousness. children with croup.
5. Preliminary studies with Helium-O2 mixture (Heliox) have shown similar clinical improvement in st O2 therapy : Although it is important to relieve hypoxia, this has 2 disadvantages : 1 ,
rejected by the child & makes him more upset. However, O2 can be used if the patient tolerates it & if the observation is to close. nd Feeding : Maintenance IV fluid is usually needed during the 1 day. st 24 hrs. Careful oral intake is usually the
it delays the appearance of cyanosis which is an important indication for mechanical ventilation, 2
nd , it is usually
initiated from the 2
progression of the degree of the airway obstruction. Prognosis
obstruction. The main indications are : cyanosis, altered consciousness extreme restlessness, or gradual rest, normal air entry, normal color, normal level of consciousness, & given steroids.
previous measures. In 2% of cases, ET-intubation (or tracheostomy) is necessary to relieve the severe
Mechanical relief of obstruction : Fortunately, 98% of cases improve within 48 hrs with
Patients may be safely discharged home after 2-3 hrs period of observation provided there are no stridor at
The outcome of acute laryngotracheobronchitis, laryngitis, & spasmodic laryngitis is excellent. appropriate treatment is initiated at a proper time better prognosis.
Untreated epiglottitis has a mortality rate of 6% in some series (bad prognosis), but of the diagnosis is made &
Most deaths from croup are caused by laryngeal obstruction or due to complications of tracheostomy.
S-ar putea să vă placă și
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5795)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (895)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (121)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (74)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- AP Psychology Chapter 2 Study Guide (W/ Answers)Document24 paginiAP Psychology Chapter 2 Study Guide (W/ Answers)JeremiahUmaleÎncă nu există evaluări
- Digestive System of GoatsDocument4 paginiDigestive System of Goatssoliun2556100% (2)
- The Development of The Middle Ear Spaces and Their Surgical SignificanceDocument15 paginiThe Development of The Middle Ear Spaces and Their Surgical SignificanceDrTarek Mahmoud Abo Kammer100% (2)
- Self Disseminating VaccinesDocument9 paginiSelf Disseminating VaccinesCaesar VranceanuÎncă nu există evaluări
- AP Statistics Final Examination Multiple-Choice Questions Answers in BoldDocument17 paginiAP Statistics Final Examination Multiple-Choice Questions Answers in BoldDrTarek Mahmoud Abo KammerÎncă nu există evaluări
- Practice Guidelines For Family Physicians 4 Infection by MansdocsDocument92 paginiPractice Guidelines For Family Physicians 4 Infection by MansdocsDrTarek Mahmoud Abo KammerÎncă nu există evaluări
- Cochlear Rotation and Its RelevanceDocument7 paginiCochlear Rotation and Its RelevanceDrTarek Mahmoud Abo KammerÎncă nu există evaluări
- StridorDocument3 paginiStridorDrTarek Mahmoud Abo KammerÎncă nu există evaluări
- Eponymous Signs in ENTDocument11 paginiEponymous Signs in ENTDrTarek Mahmoud Abo KammerÎncă nu există evaluări
- CSF LeaksDocument3 paginiCSF LeaksDrTarek Mahmoud Abo KammerÎncă nu există evaluări
- Mastoidectomy and EpitympanectomyDocument18 paginiMastoidectomy and EpitympanectomyDrTarek Mahmoud Abo KammerÎncă nu există evaluări
- History of Leprosy in MaltaDocument5 paginiHistory of Leprosy in MaltacoleiroÎncă nu există evaluări
- Tropical Medicine: Departement of Parasitology Faculty of Medicine USUDocument40 paginiTropical Medicine: Departement of Parasitology Faculty of Medicine USUSartika NapitupuluÎncă nu există evaluări
- Casos Clinicos de Hematopatología IiDocument5 paginiCasos Clinicos de Hematopatología IiRicardo LaraÎncă nu există evaluări
- Chapter XNXXXDocument3 paginiChapter XNXXXclaudette100% (2)
- Cardiac PacemakerDocument24 paginiCardiac PacemakerRitima JainÎncă nu există evaluări
- Mr. Ashish YadavDocument1 paginăMr. Ashish YadavSameer JogasÎncă nu există evaluări
- Mengenal Aspergillosis, Infeksi Jamur Genus Aspergillus Uswatun HasanahDocument10 paginiMengenal Aspergillosis, Infeksi Jamur Genus Aspergillus Uswatun HasanahTiza JulyanÎncă nu există evaluări
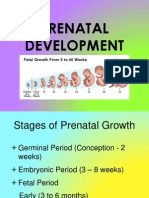
- Prenatal DevelopmentDocument23 paginiPrenatal DevelopmentCelestina TanÎncă nu există evaluări
- Karakteristik Ibu Hamil Dengan Ketuban Pecah Dini Di Rsu Assalam, Gemolong, SragenDocument7 paginiKarakteristik Ibu Hamil Dengan Ketuban Pecah Dini Di Rsu Assalam, Gemolong, SragenaniÎncă nu există evaluări
- Mother's Class BFDocument55 paginiMother's Class BFriz04_fortitudessa5178Încă nu există evaluări
- Class 11 Compiled Chintu Notes ..Document76 paginiClass 11 Compiled Chintu Notes ..Mohammed ArifuddinÎncă nu există evaluări
- Nadi Shodhana (Stage 1)Document3 paginiNadi Shodhana (Stage 1)Béla JózsiÎncă nu există evaluări
- Physical DiagnosisDocument97 paginiPhysical Diagnosisaxmedfare138Încă nu există evaluări
- The Chronicles of NarniaDocument3 paginiThe Chronicles of NarniaSandy TyasÎncă nu există evaluări
- Sex and Sexual FunctionDocument9 paginiSex and Sexual FunctionimanolkioÎncă nu există evaluări
- Public Health and Carrageenan Regulation: A Review and AnalysisDocument26 paginiPublic Health and Carrageenan Regulation: A Review and AnalysisAnnisa Rahma FatmalaÎncă nu există evaluări
- AppendicitisDocument8 paginiAppendicitisPhoebe Corazon Cercado100% (1)
- Early Journal Content On JSTOR, Free To Anyone in The WorldDocument6 paginiEarly Journal Content On JSTOR, Free To Anyone in The Worldnopal10Încă nu există evaluări
- OlfactionDocument12 paginiOlfactionbakex645Încă nu există evaluări
- Cholesterol PresentationDocument28 paginiCholesterol Presentationapi-240098169Încă nu există evaluări
- Fapc Finals ReviewerDocument303 paginiFapc Finals ReviewerC BajamondeÎncă nu există evaluări
- Bmi Lab Viva QuestionDocument7 paginiBmi Lab Viva QuestionnijafancyÎncă nu există evaluări
- Waist-Hip Ratio and Cognitive Ability Is GluteofemDocument10 paginiWaist-Hip Ratio and Cognitive Ability Is GluteofemRyuTatsuharaÎncă nu există evaluări
- Japanese EncephalitisDocument25 paginiJapanese EncephalitisShikhaKoul100% (1)
- Intervention For Voice Disorders PDFDocument14 paginiIntervention For Voice Disorders PDFSiti muhajarohÎncă nu există evaluări
- Supervisi Berjenjang Di Era Pandemi Covid-19 Dalam Manajemen KeperawatanDocument10 paginiSupervisi Berjenjang Di Era Pandemi Covid-19 Dalam Manajemen Keperawatanfebrian rahmatÎncă nu există evaluări
- Journal 1Document2 paginiJournal 1Intan KartikasariÎncă nu există evaluări