Documente Academic
Documente Profesional
Documente Cultură
P.I. Manual, 2nd Ed PDF
Încărcat de
MrsDrHTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
P.I. Manual, 2nd Ed PDF
Încărcat de
MrsDrHDrepturi de autor:
Formate disponibile
THEP.I.
MANUAL
A Handbookof
PodiatricMedicineand Surgery.
2nd Edition
ThePodiatryInstitute
Decatur,Georgia
D. Scot Malay, DPM, MSCE, FACFAS, Editor
PodiatryInstitutePublishing,Inc.
Decatur,Georgia
2008 by The Podiatry Institute, Inc. All rights reserved. This book is protected by
copyright. No part of it may be reproduced, stored in a retrieval system or transmitted
in any form or by any means electronic, mechanical, photocopy, recording, or otherwise
without the prior written consent of the publisher. For information write Podiatry
Institute Publishing, 2675 North Decatur Road, Suite 309, Decatur, GA 30033.
Care has been taken to confirm the accuracy of the information presented and to
describe generally accepted practices. However, the editor and publisher are not
responsible for errors or omissions, or for any consequences from application of the
information in this book, and make no warranty, express or implied, with respectto the
contents of the publication. The reader is urged to check the package insert of all drugs
for current recommendations regarding indications and dosage, and for added
warnings and precautions.
2CXOBl1.08
Contents
Chapter1.SelectedAnatomy&NormalPhysiology
Osteology 1
Arthrology 2
Myology
6
Tendons, Sheathsand Bursae 12
Neurology 13
Angiology 17
Chapter2. BasicPathophysiology
SkinWounds and Healing 22
Bone Healing 24
Cartilage Healing 29
Tendon,Ligamentand JointCapsule Healing 29
Peripherall\lerveWounds and Healing 30
Chapter3.SelectedDiseasesandPathologicalConditions
Dermatosesand Common Skin Pathology 33
Bacterial Infection 40
Acquired ImmunodeficiencySyndrome(AIDS) 51
PeripheralVascularDiseases 52
Diabetes Mellitus 59
Thyroid Disease 60
Hepatitis 61
Arthritides 61
NeurologicalDisorders 68
Neoplasms 71
SelectedEmergencySituations 81
Basic Cardiac Life Support 86
Chapter4. SelectedDiagnosticTechniques
Historyand Physical Examination 89
Diagnostic Imaging 89
Clinical LaboratoryTesting 94
Neurologicaland ElectroneurodiagnosticEvaluation 101
VascularExamination 104
Biomechanics 106
Chapter5.The Peri operativePatient
Preoperative Phase 116
Intra-operativePhase 116
Postoperative Phase 117
iv Contents
Chapter 6. Fundamental Techniques and Procedures
Suture Materials 123
Biopsy Techniques
Plastic Surgery Techniques
Bone Grafting and Orthobiological Agents
Selected Endoscopic Techniques
Laser Surgery
Microsurgery
Selected Tendon Lengthening and Transfer
Internal Skeletal Fixation
External Skeletal Fixation
Hemostasis
Anesthesia
Padding, Straping, Bracing and Prostheses
Chapter 7. Basic Reconstructive Foot and Ankle Surgery
Toenail Surgery
Sunbungual Exostosis
Hammertoes
Bunion Deformity and Hallux Abductovalgus
Hallux Limitus/Rigidus
Hallux Varus
Hallux Interphalangeal Arthrodesis
First Metatarsocuneiform Exostosis
Intermediate (Central) Metatarsalgia & Deformities
Fifth Metatarsal Surgery and the Tailor's Bunion
Heel Surgery
Ankle Equinus
Nerve Entrapments and Acquired Neuropathy
Amputations
Chapter 8. Major Reconstructive Foot and Ankle Surgery
Collapsing Pes Valgo Planus
Pes Cavus
Rheumatoid Foot and Pan Metatarsal Head Resection
Ankle and Pantalar Fusion
Total Ankle Replacement
124
126
131
134
137
140
140
146
152
154
157
161
163
165
166
171
184
191
192
193
194
196
198
204
208
213
214
219
223
225
228
v Contents
Chapter9.Congenital DeformitiesandJuvenileSurgery
Macrodactyly 229
Syndactyly 229
Polydactyly 231
Congenital Hallux Varus 232
Congenital Hallux Abductus Interphalangeus 232
Congenital Curly (Underlapping) Toe 232
Congenital Overlapping (Fifth) Toe 232
Cleft Foot 233
Brachymetatarsia 233
Metatarsus Adductus 234
Talipes Equinovarus 237
Congenital Calcaneovalgus 239
Congenital Vertical Talus 239
Tarsal Coalition 241
Pediatric In-Toe Deformity 242
Pediatric Toe-Walking Gait 242
Micromelia 242
Congenital Hemihypertrophy 242
Ostechondroses 243
Chapter10.ManagementofFootand AnkleTrauma
Selected Soft Tissue Injuries 244
Fractures 257
Chapter11.Footand AnkleDisabilityand Rehabilitation
Disability 282
Chapter12.Evidence-BasedMedicineand ClinicalResearch
Levels of Clinical Evidence and Clinical Research Design Options 285
The Building Blocks of Clinical Evidence 286
Fundamental Elements of Scientific Publication 286
Appendices
Oral Exam TestTaking Algorithm 293
Informed Consent 294
Hospital Admission Orders 294
Hospital Postoperative Orders 295
Hospital Discharge Orders 295
Index 296
Ch.l Selected Anatomy & Normal Physiology
Selected Anatomy & Normal Physiology
OSTEOLOGY
Table 11: LEG AND FOOT OSSIFICATION DATES
PRIMARY EPIPHYSIS OSSIFICAnON
OSSICLE OSSIFICATION CENTER APPEARS CENTERS FUSE
APPEARS (YEARS) (YEARS) (YEARS)
Proximal phalanx Birth 23 1521
Middle phalanx Birth 23 (base) 1521
Distal phalanx Birth 2-3 (base) 1521
1st metatarsal Birth 2-3 (base) 15-18
2nd metatarsal Birth 23Ihead) 1518
3rd metatarsal Birth 23Ihead) 15-18
4th metatarsal Birth 2-3 (head) 15-18
5th metatarsal Birth 2-3 (head) 15-18
Medial cuneiform 3-4
Middle cuneiform 3-4
Lateral cuneiform Birth-1
Cuboid Birth-1
Talus Bith
Calcaneus Birth 5-12 (apophysis) 15-20
Navicular 3-4
Sesamoids 9-11
Fibula Birth (shaft) 2(distal) 11-14
3-4 (proximal) 1421
Tibia Birth (shaft) 2(distal) 1719
Birth (proximal) 19-21
ACCESSORY OSSICLES
These are developmental anomalies, often separations of normal processes or tubercles,
and need to be differentiated from avulsion fractures if there is a history of injury.
2 Pertinent Anatomy & Normal Physiology Ch.1
Table1-2:ACCESSORYOSSICLES
ACCESSORYOSSICLE LOCATION
~ ~ ~ ~ ~ ~ ~ ~ ~ ~
Ostibialeextemum Posteromedial aspecttuberosity of navicular, within insertional
(accessorynavicular) fibers oftibialis posterior.
OsVesalianum Proximal to well-formed tip of the tuberosity of the 5th
metatarsal base; to be differentiated from fracture of the tip of the 5th
metatarsal base, or nonunited or fragmented apophysis.
Osperoneum Sesamoid bone within the peroneus brevis tendon insertion at
the 5th metatarsal base.
Ossupranaviculare Dorsal apsect of tanlonavicular joint
(talonavicular)
Osintermetatarseum Between the medial cuneiform and the 1st and 2nd metatarsal
bases.
Ossustentaculi Posterior aspect of sustentaculum tali.
Oscalcaneus Dorsum anterior process ofthe calcaneus, atthe junction ofthe
secondarius calcaneus, cuboid, head of the talus and the navicular.
Ostrigonum The separated posterolateral tubercle of the talus; to be
distinguished from the intact trigonal process and fracture
thereof (Shepherd's fracture).
Ossubfibulare Distal to the tip of the fibular malleolus; to be distinguished from
an avulsion fracture of lateral malleolus.
Ossubtibiale Distal to the tip of the tibial malleolus; to be distinguished from
an avulsion fracture ofthe medial malleolus.
Oscuneo-'- Plantar aspect ofthe 1st metatarsal-medial cuneiform articulation.
metatarsale-1-plantare
ARTHROLOGY
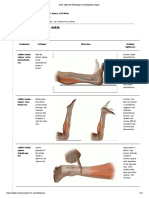
InterphalangealJoints(lPJ)(Fig. 1.1)
Ginglymus (hinge) joints with capsule that is hooded dorsally by the fibrous extensor
expansion and the plantar ligament (flexor plate); reinforced with medial and lateral
collateral ligaments running obliquely from the head of one phalanx to the base ofthe next,
in a proximal-dorsal to distal-plantar direction. A plantar IPJ sesamoid may be present.
Lesser MetatarsophalangealJoints(MTPJ)(Fig. 12)
Spheroidal joints contained within a capsule that is contiguous with the extensor hood
expansion dorsally. and the thickened flexor (plantar) plate. The capsule is reinforced medially
and laterally by collateral and suspensory ligaments. The collateral ligament runs obliquely,
proximal-dorsal to distal-plantar, from the metatarsal head to the phalangeal base. The
suspensory ligament is acontinuation of the extensor hood expansion that descends vertically
to the plantar plate, which is tethered to the adjacent MTPJ flexor plate by the deep transverse
intermetatarsal ligament A plantar sesamoid may be invested within the flexor plate of a
lesser MTPJ.
3 Ch.l Pertinent Anatomy & Normal Physiology
Figure 1.1
Figure 1.2
Extensor
hallie us brevis
Extensor
hallicus longus
Lateral collateral lig
Fib. sesamoid lig.
Transverse
melalarsallig.
Medial collateral lig
lib. sesamoid lig.
Plant. tib .. sesamoid lig.
Figure 1.3
----------------------
4 Pertinent Anatomy & Normal Physiology Ch.1
PaUem 01 dorsal PaUero 01 dorsal Pattern 01 intermetatarsal
tarsometatarsal ligaments intennetatarsalligaments ligaments
Internal
cuneiform
Cuboid Navicular
Plantar tarsometatarsal Pattern of interosseous
ligaments tarsometatarsal ligaments
Figure 1.4
First Metatarsophalangeal Joint (1ST MTPJ) (Fig. 1.3)
The 1st MTPJ is of particular importance because of the sesamoid apparatus and its
relationship to the deformities of hallux valgus and varus. The tibial and fibular sesamoids are
tethered by the intersesamoidal and plantar sesamoidal ligaments, present medially and
laterally, running from each sesamoid to the proximal phalangeal base. The conjoined head of
adductor hallucis inserts plantarlateral into the fibular sesamoid, the 1st MTPJ lateral ligaments,
and the base of the proximal phalanx.
Tarsometatarsal Joints (TMTJ, LlSFRANC'S JOINT) (Fig. 1.4)
Complex consisting of articulations of the metatarsal bases with the cuneiforms and the
cuboid, stabilized by insertion of the base of the 2nd metatarsal (keystone) into the
intercuneiform recess. The complex is arched dorsally in both the frontal and sagittal planes.
There are 3 capsular elements: medial, investing the interface between the 1st metatarsal
base and medial cuneiform; intermediate, investing the interface between the 2nd and 3rd
metatarsal bases and the intermediate and lateral cuneiforms; and lateral, investing the
interface between the 4th and 5th metatarsal bases and the cuboid. The capsule is reinforced
by dorsal intercuneiform and cuneocuboid, tarsometatarsal, intermetatarsal base, and
plantar tarsometatarsal ligaments. Lisfranc's plantar ligament runs obliquely from the medial
cuneiform to the 2nd metatarsal base plantarly.
Calcaneocuboid Joint (CCJ)
Saddle-shaped interface invested in capsule reinforced with dorsal, lateral, and medial
ligaments. The medial ligament is actually the lateral, or calcaneocuboid, portion of the
bifurcate ligament. The joint is also supported by the extracapsular long plantar
calcaneocuboid ligament, which extends from the calcaneal tuberosity to the bases of the
2nd-5th metatarsal bases.
Talocalcaneonavicular Joint(TCNJ)
Commonly referred to as the talonavicular joint, an essentially condylar joint complex that
suspends the head of the talus in the midfoot's acetabulum pedis. The acetabulum pedis
5 Ch.l Pertinent Anatomy & Normal Physiology
consists of the concavity of the posterior surface of the navicular, the anterior and middle
facets of the sustentaculum tali ofthe calcaneus, and the plantar calcaneonavicular (spring)
ligament. The TCNJ's capsule is reinforced by the spring ligament. the calcaneonavicular
portion of the bifurcate ligament. and dorsal talonavicular ligaments. The spring ligament is
crucial to arch support.
Midtarsal Joints (MTJ)
Complex consisting of the talonavicular and calcaneocuboid joints, and functions reciprocally
with the subtalar (talocalcaneal) joint. The STJ and MTJs are generally considered a
reciprocating complex. The transverse (Kite's angle) and sagittal plane radiographic cyma
lines are useful guides to subluxation of the MTJ.
Subtalar Joint (STJ)
A modified ginglymus (hinge) joint displaying triplanar motion that occurs primarily in the
frontal plane, as inversion and eversion. Anatomically, the STJ is defined as the interface
between the posteriorfacets of the calcaneus and the talus. Functionally, the STJ includes
the posterior facets of the calcaneus and talus, as well as the anterior and middle calcaneal
facets of the sustentaculum (an anatomical component ofthe talocalcaneonavicular joint),
and the sinus tarsi. The sinus tarsi consists ofthe dorsal concavity ofthe neck ofthe talus
and the plantar sulcus between the posterior facet and the sustentaculum tali of the
calcaneus. The sinus tarsi is widest laterally, and is reinforced posteriorly by the
talocalcaneal V-ligament, which also envelops the FHL tendon between the posterior
processes of the body of the talus. The posterior facets are stabilized anteriorly, medially,
and laterally by ligaments. The interosseous talocalcaneal ligament is situated posteriorly
in the sinus (just anterior to the posterior facet), and resists supination of the STJ. The
cervical ligament is located atthe anterolateral aspect of the sinus tarsi, between the talus
and calcaneus, and resists supination of the STJ.
Talocrural (Ankle) Joint
Amodified ginglymus (hinge) joint that displays triplanar motion that occurs primarily in the
sagittal plane, as dorsiflexion and plantarflexion. The ankle mortise consists ofthe concave
distal tibial-bearing surface (plafond), the triangular facet of the lateral malleolus,
the comma-shaped facet of the medial malleolus, and the anterior portion of the distal
tibiofibular syndesmotic ligament. The capsule may communicate with the peroneal tendon
sheath, and is reinforced by the deltoid ligament (medial collateral) and the lateral
collateral ligament. The deltoid ligament consists ofthe deep anteriortibiotalar component
and superficial tibionavicular, tibiocalcaneal, and posterior tibiotalar components. The
lateral collateral ligament consists of the intra-capsular anterior talofibular (ATFL), and the
extracapsular calcaneofibular (CFL) and posterior talofibular (PTFL) ligaments. The ATFL
resists ankle plantarfiexion, and anterior subluxation (anterior drawer stress) of the talus out
ofthe mortise. The CFL is deep to the peroneal tendons, and inversion injury often disrupts
both the CFL and the peroneal sheath. Clinically and radiographically, anterior drawer and
inversion stress manipulation of the lateral collateral ligaments, and more commonly MRI,
are used to assess the injured ankle.
Tibiofibular Joints
The tibiofibular joints include the proximal. interosseous, and distal tibiofibular joints. The
proximal joint is planar, and supported by anterior and posterior ligaments. The interosseous
6 Pertinent Anatomy & Normal Physiology Ch.l
membrane (10) consists of obliquely oriented, dense fibrous connective tissue running from
proximal-medial to distal-lateral from the tibia to the fibula. The fibula is also situated slightly
posterior to the tibia, (important when transferring tendon through the 10 membrane). The
distal tibiofibular joint is supported by anterior,lO, and posterior ligaments. The tibiofibular
joints allow motion in frontal and transverse planes, and resists ankle dorsiflexion as the
wider anterior portion of the talar dome engages the mortise.
MYOLOGY
The intrinsic pedal muscles comprise 4 layers in the plantar vault, innervated by the deep
peroneal (EOB; 2nd, 3rd and 4th dorsal 10), medial plantar (FOB, FHB, abductor hallucis,
1st lumbrical), and lateral plantar (OP. abductor digiti minimi, flexor digiti minimi, all 10,
alilumbricals exceptthe 1st. and adductor hallucis) nerves.
Plantar layer I
Abductor Hallucis
origin-medial calcaneal wall.
insertion-tibial sesamoid and medial base of proximal phalanx of hallux (Fig. 1.5).
Flexor Digitorum Brevis
origin-calcaneal tuberosity, divides at base of proximal phalanx.
insertion-plantar surface of middle phalanx (Fig. 1.6).
Abductor Digiti auinti
origin-fateral calcaneal wall.
insertion-lateral aspect base of proximal phalanx (Fig. 1.7).
Figure 1.5
Medial
plantar
nerve
plantar
artery
Figure 1.6
plantar
nerve
Medial
plantar
artery
Figure 1.7
Lateral
plantar
nerve
Lateral
plantar
artery
Ch.l Pertinent Anatomy & Normal Physiology
Plantar Layer II
Quadratus Plantae
origirr--2 calcaneal heads.
insertiorr--lateral aspect of FDL tendon before it divides (Fig. 1.8).
Lumbricales
7
origirr--lst. from medial aspect of FDL to 2nd toe; 2nd, from contiguous aspects of 1st and
2nd FDL tendons; 3rd, from contiguous aspects of 2nd and 3rd FDL tendons; 4th, from
contiguous aspects of 3rd and 4th FDL tendons.
insertiorr--medial aspect of mid-portion of proximal phalanges and fibrous expansion of
the dorsal hood of the 2nd-5th toes (Fig. 1.9),
Figure 1.8
Lateral
plantar
artery
arteries
Deep b r n c h ~
of lateral
plantar nerve
Figure 1.9
plantar
nerve
8 Pertinent Anatomy & Normal Physiology
Plantar Layer III
Flexor Hallucis Brevis
Ch.l
origin-medial arm from tendons of tibialis posterior inserting into the metatarsal bases, and
lateral arm from the cuboid, 3rd cuneiform, peroneus longus tendon, and long and short
plantar ligaments.
insertion-base of proximal phalanx on medial and lateral aspects, after investing 1st MTPJ
sesamoids and plantar plate (Fig. 1.101.
Adductor Hallucis
origin-oblique head arises from 2nd, 3rd, 4th metatarsal bases.
insertion-into fibular sesamoid, plantar plate, and lateral aspect base of proximal phalanx
origin-transverse head arises from plantar plates of 3rd, 4th, 5th MTPJs.
insertiof'l---into fibular sesamoid, plantar plate, and lateral aspect base of proximal phalanx
(Fig. 1.11).
Flexor Digiti Minimi Brevis
origin-plantar aspect of cuboid and 5th metatarsal base.
insertion-plantar aspect base of proximal phalanx of 5th toe (Fig. 1.121.
Figure 1.10
First plantar
metatarsal
artery
Proper
digital
nerve
Superficial
branch of lateral
plantar nerve
Lateral I'm,
plantar
artery
Figure 1.12
Figure 1.11
First plantar
metatarsal
artery
I;.t--Deep branch
of lateral
plantar nerve
Ch.1
Plantar Laver IV
Dorsal Interossei (10)
Pertinent Anatomy & Normal Physiology 9
origin-1st, adjacent surfaces of 1st and 2nd metatarsals; 2nd, adjacent surfaces of 2nd
and 3rd metatarsals; 3rd, adjacent surfaces of 3rd and 4th metatarsals; 4th, adjacent
surfaces of 4th and 5th.
insertion-1 st, base of proximal phalanx of 2nd toe medially; 2nd-4th,lateral aspect of bases
of proximal phalanges of toes 2, 3, and 4 (Fig. 1.13).
Plantar Interossei (/O)
origin-medial aspect of 3rd, 4th, 5th metatarsal shafts and bases.
insertion-medial aspect of bases of proximal phalanges oftoes 3, 4, and 5(Fig. 1.14).
Figure 1.13
Dorsal Intrinsic Muscles
Dorsal
metatarsal
arteries
Extensor Digitorum et Hallucis Brevis
Plantar
metatarsal
arteries
Superficial
branch of lateral
plantar nerve
Figure 1.14
Deep branch
of lateral
plantar nerve
origin-lateral aspect of the calcaneal sulcus and the cervical ligament; forms four slips that
course distally.
insertion-lateral aspect of EDL tendons to 2nd through 4th toes, and dorsal aspect ofthe
proximal phalanx ofthe hallux orthe lateral aspect ofthe EHL tendon. EDB is innervated by
the deep peroneal nerve.
EXTRINSIC PEDAL MUSCULATURE
Anterior Leg Compartment
The anterior leg compartment contains the muscles tibialis anterior (TA), extensor hallucis
longus (EHL), extensor digitorum longus (EDLI. and peroneus tertius (PT). Each of these is
innervated by the deep peroneal nerve and supplied by the anterior tibial artery. The
tendons of these muscles traverse deep to the transverse and cruciate crural ligaments.
10 PertinentAnatomy&NormalPhysiology Ch.1
Tibialis Anterior (TA)
origin-most medialoftheanteriorcruralmuscles,fromthelateralsuperiorcondyleandshaft
ofthetibia,10membrane,deepcruralfascia,andintermuscularseptumadjacenttoEDL
insertion-90% intothemedialcuneiform,10%intothebaseofthe1stmetatarsal
Extensor Oigitorum Longus (EOL)
origin-superiorlateralcondyleofthetibiaandtheproximal;4ofthefibula,10membrane,
cruralfascia,andintermuscularseptaecommontoTAand PL;thetendondividesintofour
majorslipsthatcoursedistally
insertion-into each ofthe4lessertoes.Inthe digit,thetendondividesintoacentralslip
thatinsertsintothedorsalcentralaspectofthebaseof themiddlephalanx;andmedialand
lateral collateral slips that course along the medial and lateral aspects ofthe middle
phalanxbeforetheyreunite and insertas asingletendon intothe dorsalsurface ofthe
distal phalanx. Thetendonsalso yield medial and lateralfibrous expansionsatthe level
ofthehead ofthemetatarsal and MTPJ,creatingthe dorsal hoodthatalso servesas an
insertionpointforthedorsaland plantar10andthelumbricales.
Extensor Hallucis Longus (EHL)
origin-inferiortoTA and EDL,fromthefibula,10 membrane,and adjacentintermuscular
septae.
insertion-dorsal aspectofbaseofthedistalhallucialphalanx
Extensor Hallucis Accessorius
origin-medial aspectofEHLinthedistalleg,ankle,orfoot
insertion-dorsal andmedialaspectsofthebaseoftheproximalhallucialphalanx.
Peroneus Tertius origin-inferior thirdoftheanteromedialsurfaceofthefibulaandthe10
membrane.
insertion-base ofthe5thmetatarsal.
LateralLeg Compartment
The lateral leg (peroneal) compartment contains both the peroneus longus (PL) and
peroneusbrevis(PB).The musclesaresuppliedbytheperonealarteryandthesuperficial
peroneal nerve,andtheytraverse deeptothe peroneal retinaculum distaltothe lateral
malleolus.
Peroneus Longus (PL)
origin-head and proximal half of the fibula, deep cruralfascia, and the anterior and
posterior peroneal septae. The muscle is superficial to the peroneus brevis at the
myotendinous junction proximal to the lateral malleolus, and must be retracted when
harvesting the underlying brevis for some lateral ankle stabilization. The tendon then
coursesaroundthe lateralmalleolus,tothe plantar-lateralaspectofthe cuboid,whereit
turnsmediallyintotheperonealgroovedeeptothelongplantarcalcaneocuboidligament.
insertion-plantar-lateralaspectofthebaseofthe1 stmetatarsal.
Peroneus Brevis (PB)
origin-anterior toPLfromthedistal213of thefibula,andtheanteriorandposteriorperoneal
septae;justdistaltothelateralmalleolus,the PBtendon is superiorand anteriortothe
tendonofPl
insertion-base ofthe5thmetatarsal.
11 Ch. 1 PertinentAnatomy&Normal Physiology
Superficial Posterior Leg Compartment
The superficial posteriorleg compartmentcontainsthetricepssurae,which convergeto
formthetendoAchiliisthatinsertsintothe posterioraspectofthecalcaneus.Themuscles
includegastrocnemiusandsoleus,and areinnervatedbybranchesofthetibialnerve,and
supplied bythe posteriortibial artery.The tricepssurae plantarflexthe ankle,with some
inversion,andextendtheknee byvirtueofthefemoraloriginofgastrocnemius.
Gastrocnemius
origin-as two heads,largermedially,fromthe medial and lateral condyles ofthefemur
posteriorly.
insertion-as Achillestendonintothecentralthirdoftheposteriorsurfaceofthecalaneus.
Soleus
origin-head and proximalthird ofthe fibula andthe middle third ofthe tibia abovethe
poplitealline.
insertion-as Achillestendonintothecentralthirdoftheposteriorsurfaceofthecalaneus.
Plantaris
origin-medial tothelateralheadofthegastrocnemiusatthelateralcondyleofthefemur,
coursinglateraltomedial.
insertion-medial aspectofthetendoAchiliisand,alongwiththeAchilles,intothecalcaneus.
Deep Posterior Leg Compartment
Thedeepposteriorlegcompartmentcontainstibialisposterior(TP),flexordigitorumlongus
(FDL)' andflexorhallucislongus(FHL).Themusclesare innervatedbythetibialnerve,and
supplied bythe posteriortibialartery.Thetendons ofthese musclestraversedeeptothe
flexorretinaculum(laciniateligament)toenterthe plantarvault.
Tibialis Posterior (TP)
origin-from the posteromedialaspectofthefibula,the posterioraspectofthetibiadistal
tothe popliteal line and lateraltothevertical line,the 10 membrane, and adjacentinter-
muscularseptae;FHLandFDLbothoverlapthebellyofTP;andTP passesthroughthefirst
(medial)canalofthetarsaltunnel.
insertion-primarily intothetuberosityofthe navicular,with additionalslipsinsertinginto
theplantaraspectoftheintermediate3metatarsalbasesandeverytarsalexceptthetalus.
Flexor Digitorum Longus (FDL)
origin-from the posterioraspectofthetibiadistaltothesolealline,andfromfascia ofTP;
thetendontraversesthe second canal ofthe tarsaltunnelto enterthefootwhere itfirst
crosses superficialto FHL, and then overTP, where itshares avinculus (masterknotof
Henry)withFDL;thereafter,FDLsplitsinto4slips.
insertion-into the plantaraspectofthedistalphalanxofthelesser4toes.
Flexor Hallucis Longus (FHL)
origin-from thedistal2/3ofthe posteriorsurfaceofthefibula,the posterioraspectofthe
peroneal septum, the anterior surface of the deep transverse intermuscular septum
(separatingthesuperficialanddeepposteriorgroups),andthefasciaaboutTP.Thetendon
coursesthroughthefourth canal ofthetarsaltunnel.
insertion-into theplantaraspectofthe baseofthedistalphalanxofthehallux.
12 Pertinent Anatomy & Normal Physiology Ch.1
TENDONS, SHEATHS AND BURSAE
Tendon Structure
Tendons consist of dense regular connective tissue made up oftropocollagen units, created
by fibroblasts, and organized to form collagen fibers. The fibers are supported within
endotenon, and grouped into fasciculi which are contained within an outer epitenon. The
epitenon defines the anatomical tendon. Golgi tendon organs within tendon fibers inhibit
skeletal muscle contraction when excessive tension is registered. The organized tendon is
further surrounded, outside of the epitenon, by a loose, areolar and highly vascularized
paratenon, wherever the tendon courses a straight line. Paratenon is contained deep to,
and adherent to, the deep fascia (muscle fascia); or it is adherent to a neighboring inter-
muscular septum (fascia) between intact skeletal muscle bellies; or it may be adherent to
deeper periosteum.
Tendon Sheath and the Gliding Mechanism
Atendon sheath exists where atendon changes direction, such as about the ankle deep to
the extensor, peroneal, and flexor retinaculae. The sheath is distinct from paratenon and
consists of afibrous outer septum with asynovial lining, much akin to joint capsule. Synovial
fluid bathes the tendon within the sheath. Within the sheath, on the tendon's deep
(non-friction) surface, asynovium lined fold of connective tissue called mesotenon, conveys
vascularity and further supports the tendon. Mesotenon attaches to the epitenon at the
hilus. At the proximal margin of the tendon sheath a double fold of paratenon, termed a
plicae duplicata, invaginates a short distance into the sheath and adheres to epitenon.
Similarly, at the distal margin of the sheath, a single fold of paratenon, termed a plica
simplex. protrudes into the sheath. As muscle contracts, the plicae unfold and elongate as
the tendon glides within the sheath as the tendon changes direction, or within paratenon
where the course is straight
Tendon Blood Supply
Tendon has three primary sources of blood supply: proximally, atthe myotendinous junction
perimysial blood vessels from the muscle belly; centrally. from paratenon and/or mesotenon;
and distally, insertional periosteal vessels from bone. Synovial fluid within the sheath, and
local lymphatics within the paratenon, also nourish and drain metabolites from the tendon.
Occasionally, a condensed. highly organized fibrous connection, know as avinculus, may
also convey vascularity between closely approximated tendons. The Master Knot of Henry,
between the tendons of FHL and the more superficial (plantar) FOL, at a level consistent
with the distal margin of the sustentaculum. is just such a vinculus. Vinculi also exist
between FHB and FDL neartheir phalangeal insertions.
Subfascial and Subcutaneous Bursae
A variety of bursae occur in the foot and ankle. Bursae protect tendon and muscle from
excessive friction or pressure caused by adjacent muscle, ligament or bone, or external
forces in the case of an adventitious bursa. Subfascial bursae include the retrocalcaneal
or pre-Achilles bursa, those atthe insertions ofTA, TP, and the 10; and those between the
bellies of adductor digiti minimi and the 5th metatarsal, and the belly of FHB and the medial
cuneiform. Subcutaneous bursae are usually adventitious in origin, and may present atthe
13 Ch.1 Pertinent Anatomy & Normal Physiology
head of the 1st and 5th metatarsals, plantar to the tuberosity ofthe calcaneus (present in
about 50% of specimens), at the medial and lateral malleoli, and occasionally posterior to
the insertion of the Achilles tendon.
NEUROLOGY
The lower extremity nerve supply originates in the lumbosacral spine, and specifically
involves spinal nerve roots L4-S3. The spinal nerve roots traverse the lumbosacral plexus
to form the sciatic nerve, which divides into the tibial nerve and the common peroneal nerve
near the junction of the middle and distal thirds ofthe thigh.
Table 1.3. MOTOR INNERVATION TO THE LEG AND FOOT
MUSCLE PERIPHERAL NERVE SPINAL LEVEL
Tibialis anterior Deep peroneal U,5
Extensor digitorum longus Deep peroneal U,5
Extensor hallucis longus Deep peroneal U,5
Peroneus tertius Deep peroneal U,5
Gastrocnemius Tibial Sl,2
Soleus Tibial Sl,2
Plantaris Tibial Sl,2
Popliteus Tibial U,5S1
Fexor hallucis longus Tibial S2,3
Flexor digitorum longus Tibial S2,3
Tibialis posterior Tibial U,5
Peroneus longus Superficial peroneal LsS1,2
Peroneus brevis Superficial peroneal LsS1,2
Extensor digitoum brevis Deep peroneal S1,2
Abductor hallucis Medial plantar S2,3
Flexor digitorum brevis Medial plantar S2,3
First lumbricalis Medial plantar S2,3
Flexor hallucis brevis Medial plantar S2,3
Abductor digiti quinti brevis Lateral plantar S2,3
Quadratus plantae Lateral plantar S2,3
Second, third, fourth lumbricales Lateral plantar S2,3
Adductor hallucis Lateral plantar S2,3
Flexor digiti quinti brevis Lateral plantar S2,3
Plantar interossei Lateral plantar S2,3
First, second doral interossei Deep peroneal, lateral plantar S1,2,3
Third, fourth dorsal interossei Lateral plantar S2,3
14 Pertinent Anatomy & Normal Physiology Ch.1
COMMON PERONEAL NERVE
The common peroneal nerve trifurcates near the head of the fibula, forming the lateral sural
cutaneous nerve, the deep peroneal nerve, and the superficial peroneal nerve.
lateral Sural Cutaneous Nerve
This nerve ultimately anastomoses with the medial sural cutaneous branch of the tibial
nerve, to form the sural nerve.
The Deep Peroneal Nerve (Anterior Tibial) (Fig. 1.15)
This nerve begins atthe peroneal muscular hiatus between the fibula and peroneus longus,
then passes deep to EDL on the 10 membrane to innervate TA, EHL, EDL, and PT. At the
ankle, it divides into medial and lateral terminal branches.
The lateral terminal branch passes deep to, and innervates, EDB and then yields three
interosseous branches which supply the 2nd, 3rd, and 4th dorsal 10.
The medial terminal branch runs parallel and lateral to the DP artery. The nerve divides at
the first interspace into two dorsal digital nerves supplying adjacent sides of the great and
second toes, and the first dorsal interosseous muscle (which is also innervated by the
lateral plantar nerve).
The muscular branches of deep peroneal nerve supply all anterior leg muscles, including
peroneus tertius.
The Superficial Peroneal Nerve
The superficial peroneal nerve supplies both the peroneus longus and brevis muscles, then
divides to form the medial and lateral dorsal cutaneous nerves.
The medial dorsal cutaneous nelVe (Fig. 1.16) divides into two dorsal digital nerves, the
medial dorsal digital branch that communicates with the medial terminal branch from deep
peroneal nerve, to supply the medial aspect ofthe hallux.
The lateral dorsal digital branch supplies the adjacent aspects of the 2nd and 3rd toes
dorsally. The lateral dorsal cutaneous (Lemont's) nerve divides into a medial branch that
supplies the adjacent sides of the 3rd and 4th toes, and a lateral branch that supplies the
adjacent sides of the 4th and 5th toes.
Ch.1 Pertinent Anatomy &Normal Physiology
Dorsal proper
digital nerve
Medial terminal
nerve branch
of the deep
peroneal nerve
Figure 1.15
Abductor hallucis
Figure 1.17
Saphenous
nerve
cutaneous
nerve
Figure 1.16
Proper digHal
nerves
Communicating
branch
Common
E digital nerve
Deep branch
Figure 1.18
Communicating
branch
15
Lateral dorsal
cutaneous nerve
Intermediate dorsal
cutaneous nerve
Proper digital
nerves
Proper digital
nerve
First common
digital nerve
Second common
digital nerve
Medial plantar
nerve
16 Pertinent Anatomy & Normal Physiology Ch.l
TIBIAL NERVE
The tibial nerve traverses the calf deep to the intermuscular septum between the superficial
and deep crural compartments, and in the distal third of leg runs parallel and medial to the
tendoAchillis. The tibial nerve yields the medial sural cutaneous nerve that unites with the
lateral sural cutaneous branch of the common peroneal nerve, to form the sural nerve.
The Sural Nerve
The sural nerve courses distally through the leg, then posterior and inferior to the lateral
malleolus, en route to the lateral aspect of the foot and 5th toe. Just distal to the lateral
malleolus, the sural nerve sends a communicating branch dorsallyto anastamose with the
intermediate dorsal cutaneous nerve. The tibial nerve also provides articular branches
that innervate the knee and ankle. In the calf, the tibial nerve innervates the popliteus,
gastrocnemius, soleus, plantaris, TP, FDL, and FHL muscles. Prior to bifurcation into the
medial and lateral plantar nerves, the tibial nerve yields the medial calcanean branch that
emerges through the laciniate ligament to innervate the skin of the heel medially and
plantarly. (Fig. 1.17)
The medial calcanean nerve can be injured or entrapped in scar tissue following
medial exposure (OuVries incision) ofthe heel, such as in plantar calcaneal spur surgery.
The division ofthe tibial nerve into the medial and lateral plantar nerves usually occurs near
the dorsal margin of the tarsal tunnel, however the bifurcation can occur at any level deep
to the laciniate ligament and occasionally it occurs proximal to the ligament. In many cases
of tarsal tunnel syndrome, operative inspection reveals afar distal bifurcation of the tibial
nerve at the porta pedis where the medial plantar nerve enters the anterior chamber, and
the lateral plantar nerve enters the posterior chamber, of the calcaneal tunnel which is the
distal continuation of the tarsal tunnel deep to abductor hallucis. The anterior and posterior
canals are separated by a fibrous septum coursing from the deep surface of abductor
hallucis to the medial wall of the body of the calcaneus plantar to the sustentaculum tali.
PLANTAR NERVE SUPPLY
Medial Plantar Nerve (Fig. 1.18}
The medial plantar nerve is usually slightly larger than the lateral plantar nerve, and
traverses the 3rd canal ofthe flexor retinaculum along with the medial plantar vessels. The
medial plantar nerve yields cutaneous branches innervating the medial aspect of sale;
muscular branches that supply FOB, FHB, abductor hallucis and the 1st lumbrical; the
proper digital branch to the plantar-medial aspect ofthe hallux; and three common digital
nerves that yield proper digital nerves to the contiguous surfaces ofthe 1st and 2nd, 2nd and
3rd, and 3rd and 4th toes. The 1st common or 2nd proper digital nerve yields a branch to
innervate the 1st lumbrical muscle. The 3rd common or 4th proper digital nerve yields a
branch that communicates with the lateral plantar nerve, and is often the site of Morton'S
neuroma. The proper digital nerves supply the digital pulp, and the tips and sides of the toe,
including the nail matrix.
The lateral Plantar Nerve
The lateral plantar nerve courses through the porta pedis deep to the plantar fascia, and
yields muscular branches to quadratus plantae and abductor digiti minimi; cutaneous
17 Ch.1 Pertinent Anatomy & Normal Physiology
branches to the lateral aspect ofthe sole; asuperficial branch that divides into common and
proper digital branches, and a deep branch. The proper digital branch supplies the lateral
aspect ofthe 5th toe; and the flexor digiti minimi brevis as well as the 3rd plantar and 4th
dorsal 10 muscles. The common digital branch usually communicates with the digital branch
ofthe medial plantar nerve (often the site of Morton's neuroma), before dividing into proper
digital branches to the contiguous surfaces of the 4th and 5th toes. The deep branch of
the lateral plantar nerve supplies all of the 10 muscles except the 4th dorsal and 3rd
plantar in the 4th intermetatarsal space, all of the lumbricales except the 1st lumbrical, and
adductor hallucis.
Saphenous Nerve
The saphenous nerve is the terminal continuation ofthe femoral nerve, and courses through
the thigh to emerge from the adductor canal to become subcutaneous and continue distally
along the anteromedial aspect of the leg and foot. It yields a branch to the skin over the
ankle, and a branch that courses distally to innervate the medial aspect of the tarsus and
greattoe.
ANGIOLOGY
ARTERIAL SYSTEM
The arterial supply to the lower extremities originates with the abdominal aorta, which
bifurcates into right and left common iliac arteries, which then further divides to form internal
and external iliac arteries. The external iliac artery becomes the femoral artery at the
distal margin of the inguinal ligament. The femoral artery is palpable in the groin, and
courses distally through the thigh to become the popliteal artery, which is palpable in the
popliteal fossa. The popliteal artery yields muscular, cutaneous, and articular (knee)
branches. The popliteal artery bifurcates to form the anterior and posterior tibial arteries at
the lower border of popliteus.
The anterior tibial artery courses through the crural 10 membrane to enter the
anterior compartment of the leg where it descends to the ankle, where it becomes the
dorsalis pedis artery. The anterior tibial artery courses between TA and EDL in the superior
third of the leg, between TA and EHL in the middle third, deep to the tendon of EHL just
proximal to the ankle and between the tendons of EHL and EDL atthe level ofthe ankle. The
branches of the anterior tibial artery include:
1. Posterior recurrent tibial artery, posterior to 10 membrane
2. Anterior recurrent tibial artery, which joins the circumpatellar network
3. Muscular branches to TA, EDL, EHL, and peroneus tertius
4. Anterior medial malleolar artery
5. Anterior lateral malleolar artery
The anterior leg muscles are supplied by muscular branches of the anterior tibial
artery. The anterior medial malleolar artery anastomoses with branches of the posterior
tibial and medial plantar arteries. The anterior lateral malleolar artery anastomoses with
the perforating branch of the peroneal and lateral tarsal arteries.
18 PertinentAnatomy&NormalPhysiology Ch.l
Thedorsalispedisartery,thesecondlargestsourcesupplyingthefoot,continuesto
the1stintermetatarsalspace,whereitcoursesasthedeepplantarbranchtojointheplan-
tararchIFig.1.19).Thebranchesofthedorsalispedisarteryinclude:
1. lateraltarsalartery;supplyingEDB
2. medialtarsalartery
3. arcuateartery;yieldingthe2nd,3rd,and4thdorsalmetatarsalarteries
4. 1stdorsalmetatarsalartery
5. deepplantarperforatingbranch
Thedorsalmetatarsalarterieslieinthe correspondingintermetatarsalspaces,deep
to the extensor tendons and dorsal to the dorsal 10 muscles. Exceptthe first dorsal
metatarsalartery,whichyieldsthedeepplantarperforatingartery,themetatarsalarteries
yield posteriorand anteriorperforating branchesatthe levelofthemetatarsal base and
MTPJ,respectively.Thearteriescontinuedistallyascommondigitalarteries,whichdivide
intoproperdorsaldigitalarteriesthatareofsmallerdiameterthantheplantardigitalarteries.
Theposteriortibialartery,thelargestsourcesupplyingthefoot,isaterminalbranch
of the popliteal artery and courses through the leg to the third canal of the flexor
retinaculum,thendividesintomedialandlateralplantararteriesdeeptoabductorhallucis
inthecalcaneal canalsIFig.1.20).Thebranchesoftheposteriortibialarteryinclude:
1. circumflexfibularartery,whichsuppliessoleus
2. peroneal artery,which suppliessoleus,TP, FHL, PL, PB, andthe fibula; andthe
perforatingperonealbranch(thirdlargestsourcesupplyingthefoot)thatpiercesthe
10membraneproximaltotheankletojoinwithbranchesof theanteriortibialartery
3. nutrientarterytotibia,the largestnutrientarteryinthebody
4. muscularbranchestosoleus,TP, FHL, FDL
5. communicatingarterythatanastomoseswithperoneal artery
6. medialmalleolarbranches
7. medialcalcaneanbranches,whichsupplytendoAchiliisandmedialheel
8. medialplantarartery,medialtothemedialplantarnerve
9. lateral plantar artery, which becomes the plantar arch and supplies all ofthe
musclesofthesole,exceptabductorhallucis,FOB,and1stdorsal10muscle.
The plantararch courses lateralto medialtowardthefirstintermetatarsal space,
where itanastomoses with the deep plantar perforating branch ofthe dorsalis pedis
artery.The plantararch separatesthe3rd and 4thmusclelayers,and yields anteriorand
posteriorperforating arteriesthatanastomoseswith corresponding perforatorsfrom the
dorsum.Theplantararchyields4plantarmetatarsalarteries,thefirstofwhichconsistsof
theunionofthelateralplantaranddeepplantarbranches.Theplantarmetatarsalarteries
become common and then properdigitalarteriestothe correspondingtoes. The plantar
digital arteries are largerthanthe dorsal digital arteries. Inthehallux.the lateralplantar
digital arteryisthe largest,while inthe lessertoesthe medial plantardigitalarteriesare
largest. In the hallux,the dorsal digitalarteries extend tothetoe tip, as dothe plantar
digitalarteries,thedorsaland plantarhallucialdigitalarteriessupplyingthehalluxequally
distaltothe interphalangealjoint. Inthe lessertoes, dorsal digital arteriesextend tothe
level ofthe proximal ITPJ,while plantardigital arteries extend tothe toe tip and then
retrogradetosupplythedorsalaspectofthetoe,includingthenailbed(Fig. 1.21).
Ch.l
Figure 1.19
Lateral digital
artery
Figure 1.21
Pertinent Anatomy & Normal Physiology
Common dorsal
digital arteries
artery
Lateral tarsal artery
Distal and
proximal arches
Anterior
perforating
arteries
Figure 1.20
Common
plantar digital
arteries
First plantar
metatarsal
artery
19
20 Pertinent Anatomy & Normal Physiology Ch.l
VENOUS SYSTEM
The dorsal venous system ofthe foot and ankle consists of superficial and deep networks.
The deep dorsal venous plexus converges to form the medial marginal vein. The superficial
dorsal venous plexus is immediately subcutaneous, and contains the dorsal venous arch.
The dorsal veins drain into the greater and lesser saphenous veins. On the plantar aspect,
asuperficial venous plexus drains into the deep venous plexus, which ultimately converges
into the medial and lateral plantar veins, and communicates with the dorsal system via
perforating veins.
LYMPHATIC SYSTEM
Superficial lymphatics drain the skin of the toes, sole and heel, forming a medial system
that drains into the inguinal lymph nodes and a lateral (rays 3-5) system that drains into the
popliteal lymph nodes. The deep lymphatic system forms collecting ducts located dorsally,
laterally (peroneal), and plantarly, and drain into major lymphatics corresponding to the
adjacent anterior tibial, peroneal, and posterior tibial vessels. The deep system drains
primarily into the popliteal lymph nodes.
CUTANEOUS ANATOMY
The skin consists of the epidermis and dermis (Fig. 1.22). The dermis consists of both
reticular and papillary layers, and contains microcirculatory elements (arterioles,
capillaries, venues, glom, and lymphatics), nerves and the annexed. Skin annexed include
echini sweat glands and ducts, hair follicles and arrestor pile muscles, sebaceous glands
at the base of the hair follicle (pilosebaceous gland). and the toenails and perionychium.
Nearthe nail bed, arterioles shunt directly to venules via the Hoyer-Susquet canal, to effect
the glomus body important in temperature regulation, Eccrine glands are present on all
pedal skin surfaces, and are innervated by sympathetic nerves. Pilosebaceous glands are
only present on dorsal skin. Deep in the dermis, near the subcutaneous fat-superficial
fascia junction, lie the Pacinian (Pacini-Vater) corpuscles important in touch-pressure
sensation. The epidermis serves as a barrier, and contains five strata: basale, spinosum,
granulosum, lucidum, and corneum. Melanocytes with dendritic processes exist amongst
the living cells of the stratum basale, and are responsible for melanin production
which serves to protect underlying living cells from the mutagenic effects of UV radiation.
Langerhans immune cells, much like macrophages, as well as Merkel's sensory cells also
exist in the epidermis.
Relaxed Skin Tension Lines (RSTLI (Fig. 1.23)
The skin's intrinsic tension is oriented such that maximum tension is directed parallel to the
long axis of the extremity. Intrinsic skin tension is generated by the forces of underlying
bone and soft tissue prominence, as well as joint motion and extrinsic forces upon the skin.
RSTL are oriented perpendicular to the long axis of the leg and foot, and can be clinically
identified with the pinch test. As arule, elective skin incisions should be made parallel to the
RSTL, as long as the exposure allows access to the underlying target structures and does
not unduly violate vital structures (vessel, nerve, tendon).
Ch. 1 Pertinent Anatomy &Normal Physiology 21
Epidermis ';.-
Papillary-[ -0 0
1
0 '-'
layer r }A / granulosum
layer
Subcutaneous
connective
tissue
Figure 1.22
'
,.. ..... ...
\:::::::'1
'-=7
Plantar
spinosum
Str, basale
Lateral Medial
Figure 1.23
22 Basic Pathophysiology Ch.2
BASIC PATHOPHYSIOLOGY
WOUNDS AND HEALING
This section will describe wounds and healing of avariety of tissues, including skin, bone,
cartilage, tendon, ligament, joint capsule, and nerve. Wound healing relies upon an
adequate vascular supply and angiogenesis. Angiogenesis entails endothelial proliferation
with resultant capillary budding.
SKIN WOUNDS AND HEALING
Healing Phases
Dermal wounds include Punctures, Abrasions, Incisions, and Lacerations (PAIL); as well
as contusions, pressure injuries, mechanically or chemically induced and hypersensitivity
related bullae, burns and frostbite. The epidermis repairs by means of epithelial cell
mitosis that continues until contact inhibition occurs. The underlying dermis heals in three
phases: inflammatory, fibroproliferative, and maturation.
Inflammatory Phase
The inflammatory (substrate or lag) phase begins immediately upon wounding, comprises
approximately 10% of the healing process, and is also referred to as the substrate, or lag
phase because specialized blood cells and proteins necessary for healing are recruited
and migrate to the wound at this time. After initial vasoconstriction, usually lasting several
minutes, vasodilatation and erythema predominate during the inflammatory phase, which
lasts for 3or 4days. Angiogenesis and capillary budding occur while fibroblasts lay down
collagen in a random fashion, and tensile strength begins to return to the damaged skin.
Superficially, epidermal epithelialization occurs concomitantly with dermal inflammation,
and mitosis continues until contact inhibition occurs between epithelial cells, which
ultimately seal the wound surface.
Fibroproliferative Phase
The fibroproliferative (fibroblastic) phase comprises approximately 20% of the healing
process, and lasts from the 3rd to 4th day, until the 14 to 21 day. Granulation tissue, which
consists of new collagen and capillary buds, predominates and continues to form until the
wound contracts and epithelialization is complete. Collagenation rapidly increases during
this phase, and fibroblasts are the primary cell type present in the wound. The tensile
strength of the wound approaches only about 35% of the local skin's original strength after
14 days and, at this point, the wound's main source of tensile strength comes from suture
material used for primary closure.
Maturation Phase
The maturation (remodeling) phase comprises approximately 70% of the healing process
and lasts from approximately 3 weeks until one year post injury. During this phase,
randomly arranged collagen fibers that were laid down during the fibroproliferative phase
are microscopically debrided via macrophage enzymatic breakdown. New fibers are
produced and aligned in response to mechanical forces, and wound contraction occurs in
a centripetal direction (toward the center of the wound). linear scar contraction occurs
23 Ch.2 Basic Pathophysiology
from bothendsofthescartowardthecenter.Thisisimportantwhenplanninganelective
skinincision.Thelongaxisoftheanticipatedscarshouldbeorientedparalleltotheaxisof
motionoftheunderlyingjoint.Ascarthatisperpendiculartothejointaxismaycauseajoint
contractureduetoscarcontraction,oftenseenwithaposteriorlongitudinal ankle ora
dorsallongitudinalMTPjointincision.
Skin Ulcers
Dermalwoundsthatdevelopsecondaryto pressure,(typicallychronic, non- traumatic
weight-bearing or decubitus pressure), can result in ulceration. Technically, skin
ulcerationisdefinedasan openwoundwherethefullthicknessofskinisviolated.
The International Association for Enterostomal Therapy
(classifiespressure-inducedcutaneouscompromise)
Stage I: Epidermis intact,howevererythema remains longerthan30 minutes after
pressurerelieved. Reversiblewithintervention.
Stage II: Partial thickness skin loss, including epidermis and perhaps superficial
dermis.There issurrounding induration,and local bullae orvesicleswith erythema,
tenderness(ifnotinsensitive),andthebaseofwound ismoistand necrosisfree.
Stage III: Full-thickness skin loss, through the dermis into subcutaneous fatand
superficialfascia, effecting acrater. Necroticescharfilling the craterand covering
the base must be debrided in orderto accurately stage the depth and properly
categorizethewound.Thecentralwoundbaseisgenerallynontender. Thereisoften
underminingofthemargin,sinustractformation, local exudate,and asurrounding
halooferythema.Ascendingcellulitisand infectionmayalsobe presentUnderlying
osteomyelitis or, in the presence of an ischemic limb, subcutaneous gas or
necrotizinginfectionshouldalsoberuledout
StageIV:Deepcraterwithpenetrationthroughdeep(muscle)fascia,withassociated
involvementofmuscle,jointand/orbone.Again,thewoundbaseisusuallynontender.
Possibleassociateddissectingabscess,necrotizinginfection,andosteomyelitismust
beruledout.
Wagner Classification of Neurotrophic Ulceration
(categorizesdiabeticandneuropathiculcers)
Grade0: Skinintact,osseousdeformitypresent,atrisk.
Grade I: Localized superficialulcer.
GradeII: Deepulcerextendingtotendon,jointand bone.
GradeIII:Deepabscesswithosteomyelitis.
GradeIV:Gangreneoftoesorforefoot.
GradeV: Gangreneoffootextendingfromforefoottoproximaltomidfoot.
24 Basic Pathophysiology Ch.2
-
Keloids and Hypertrophic Scars
Keloids are reactive fibrous proliferations that develop at sites of cutaneous injury. They
occur more commonly in black individuals and the predilection is hereditary. Fibrous
proliferation extends beyond the area ofthe original skin injury and can be debilitating. The
lesion is thought to develop due to irregular wound granulation associated with abnormal
capillary endothelium, and the presence of excessive myofibroblasts. Excessive
collagenation and decreased collagenase activity may also contribute to fibrous
proliferation. Hypertrophic scars are similarto keloids, however they remain within the area
of the original injury and tend to reduce in size over time. Intralesional injection of
glucocorticosteroid and surface compression, preferably with elasticized silicone polymer,
may reduce keloids and hypertrophic scars. Peptic ulcer, fibromatosis, and enostosis may
be present Elective surgery should be considered cautiously in patients with a history of
hypertrophic scar or keloid formation.
Morphea and Systemic Sclerosis
Morphea is represented by one or more hardened, linear, plaques of atrophic skin. It can
be idiopathic or post-traumatic and develops with an initial purple or pink margin. Morphea
responds to intralesional steroids. Systemic sclerosis (formerly Scleroderma) affects
cutaneous as well as multi-organ connective tissue hardening. In the skin, typically in the
extremities, there is sclerosis, stiffening of small joints, Raynaud's phenomenon, ulceration
and calcinosis (calcinosis cutis). Other findings include esophageal, GI tract, pulmonary,
cardiac, and renal sclerosis.
BONE HEALING
Fractures
Fractures are described according to their location and orientation within the specific bone.
Incomplete fractures, wherein aportion ofthe bone's cortex remains intact, are termed green
stick fractures, and generally develop secondary to flexural deformation of a long bone.
Similarly, astress fracture results in bending without overt radiographic fragment separation.
A bone scan can be useful if diagnosis is in question. Incomplete fractures are diagnosed
primarily by clinical examination, and with subsequent radiographic evidence of secondary
bone callus. Complete fractures can be transverse, oblique, spiral, and comminuted, with
fracture stability and management varying with the fracture pattern. Fracture stability, in
descending order, is as follows:
Transverse> Oblique> Spiral> Comminuted
25 Ch.2 Basic Pathophysiology
Transverse and oblique fractures can be closed-reduced and immobilized, whereas
spiral and comminuted patterns are extremely difficult to adequately reduce and maintain
in a closed fashion. When a fracture violates a joint surface, open reduction and
stabilization is most often the best treatment option. Growth plate injuries and open fractures
also deserve special consideration. Fracture repair is initiated with closed reduction and
immobilization.
Charnley's sequence of closed reduction is as follows: 1st} increase the
deformity, 2nd) distract, 3rd) reverse the deformity and realign, and 4th) maintain
correction with immobilization.
Callus (Secondary) Bone Healing
Bone heals via either callus bone healing or primary bone healing, and requires an intact
vascular supply. Callus bone healing, which may also be referred to as secondary
bone healing, occurs in six phases: hematoma formation, hematoma organization,
fibrocartilaginous callus, primary bone callus, primary bone callus absorption, and
remodeling (maturation). The hematoma phase lasts 1to 3days, and consists of hematoma
formation between fracture fragments. Hematoma organization lasts from 3to 10 days, and
entails inflammation with recruitment of osteoclasts and osteoblasts. The fibrocartilaginous
callus phase lasts from 10 days to 6weeks, depending upon the degree of immobilization
and fragment stability; and consists of osteoclastic phagocytosis of necrotic bone,
chondroblastic and osteoblastic differentiation into cartilage (low oxygen tension) or bone
(high oxygen tension), and neovascularization derived primarily from endosteal, and to a
lesser degree periosteal, blood vessels. Fracture instability leads to progressive irritation
(fibrocartilaginous) callus formation, and delays the development of bone. The primary bone
callus phase lasts from 6to 10 weeks, and includes condensation ofthe fibrocartilaginous
callus into bone that bridges the fracture interface. Primary bone callus absorption lasts
from 2.5 to 4 months, and includes new bone remodeling into secondary bone callus. The
remodeling, or maturation phase entails alteration of bone in response to applied forces in
accordance with Wolff's law, and continues from about 4months post-injury.
Primary Bone Healing
Primary bone healing requires fracture reduction, rigid stabilization, and preservation
of fragment vascularity. When bone fragments are reduced and rigidly stabilized, the
fibrocartilaginous callus phase can be by-passed and new bone formation and remodeling
occur simultaneously via Haversian remodeling. Primary bone healing can occur via either
contact or gap healing. Contact healing involves stabilization of bone-to- bone contact,
while gap healing involves stabilization of the fragments with maintenance of asmall (up to
2mm) gap between the bone ends. Stabilization is enhanced by compression, which
increases friction between bone fragments and promotes rigidity. Fracture stability can be
achieved in avariety of ways (see Internal and External Fixation of Bone).
Haversian remodeling is the underlying process of normal bone healing. When
fracture fragments are reduced and stabilized, capillary budding from Haversian canals
occurs at points of contact, and bridges the fracture interface by means of the cutting cone;
which consists of aleading tip of osteoclasts that phagocytose osteoid, acentral capillary
emanating from the Haversian canal, and osteoblasts that are organized about capillary
margins and lay down lamellar new bone.
26 Basic Pathophysiology Ch.2
Avascular Necrosis
There are many causes of bone necrosis including trauma (accidental and surgical), steroid
therapy, occlusive vascular disease, venous thrombosis, collagen vascular disease
(rheumatoid, arteritis), status-post renal transplant, sickle-cell anemia, pancreatitis and
chronic alcohol abuse, radiation therapy, hyperuricemia and gout, hyperlipidemia,
barotrauma (Caisson's disease), osteoporosis and osteomalacia. The process involves
acute ischemia of bone, necrosis, then revascularization and new bone formation. Bone
scans, if used early and with fine localization, may show a cold spot due to ischemia.
Generally, however, bone scans are hot, which is consistent with new bone accretion
associated with healing. An MRI can be useful in establishing the diagnosis of AVN.
Radiographic Classification ofAVNofths First Metatarsal Hsad (Dr Head ofths Fsmur)
Stage I: Pre-collapse
Early normal density,localized cold bone scan
Intermediate relative sclerosis of dead bone, due to surrounding
hyperemia and disuse osteoporosis
Late: true sclerosis due to new bone accretion,
hot bone scan
Stage II: Collapse
Early: mild step defect, loss of articular sphericity
Late: fragmentation of articular surface and metaphysis
Stage III: Arthritis
Early: joint space narrowing, subchondral cysts and
sclerosis,osteophytosis
Late: sclerosis, ankylosis, articular erosion
Clinical Signs and Symptoms ofAVN
Stage I: usually asymptomatic, or perhaps minimal pain and stiffness
Stage II: usually significant pain and stiffness, occasionally asymptomatic
Stage III: pain and stiffness are most typical
The differential diagnosis of AVN includes arthrosis, RSDS, and infection. The ESR is
usually not elevated due to AVN and RSDS. The medical treatment of AVN consists of
protective or non-weight bearing, electrical bone growth stimulation, vasodilators, NSAlDs
to inhibit platelet aggregation, and avoidance of steroids. Surgical treatment of AVN
includes debridement of necrotic bone or core decompression and replacement with
autogenous bone graft, revascularization with a pedicle muscle graft, and resection with
endoprosthesis or arthrodesis. Rates of AVN of the first metatarsal head following distal
first metatarsal osteotomy have been reported to range from less than 1%to greater than
40%. Steps for the prevention of AVN include preservation of periosteal and capsular
attachments, accurate hemostasis, avoidance of immediately subchondral osteotomies, rigid
stabilization of metaphyseal osteotomies, protective or non-weight bearing, use of sharp
blades and osteotomes, and routine serial radiographs following osteotomy or fracture.
27 Ch.2 Basic Pathophysiology
Delaved Union, Nonunion and Pseudoarthrosis
Following fracture, excessive motion andlor inadequate vascularity can lead to formation
of hypertrophic irritation callus, malunion, delayed union, nonunion, or pseudoarthrosis.
Conditions such as Puget's disease, osteitis fibrosa cystica, rickets, hyperparathyroidism,
osteomalacia and osteoporosis, and debilitated or compromised host (immuno-
compromised, antimetabolite or steroid therapy, anemia, anticoagulation therapy, elderly
patient, chronic cigarette smoker) can also impede bone healing. The presence of irritation
callus rules out primary bone healing, and indicates instability between fragments.
Delayed union simply means the fracture has not healed within a reasonable period, and
can be identified radiographically by the presence of unchanged irritation callus and
persistence of a fracture cleft. Causes of delayed union, and ultimately nonunion, include
inadequate fracture reduction and/or immobilization, overly-aggressive soft tissue
(periosteal) stripping or injury, osteomyelitis, and local vascular compromise. Delayed unions
and nonunions are determined primarily via serial radiographic inspection, combined with
clinical evidence of persistent edema and pain. Depending upon clinical needs and
indicators, a delayed union is treated with continued immobilization and non-weight
bearing, revisional surgery for callus channelization or bone grafting or re-fixation (internal
and external), and employment of electrical bone growth stimulation (EBGSI.
A nonunion is classically defined as failure to achieve stable fracture healing after 8to 9
months of management. It is not necessary to wait 8 or 9 months before intervening
surgically, either revisional or as an initial operation, when treating a delayed union,
however appropriate non-surgical intervention should be applied before deciding to go to
the operating room.
Nonunions are classified as either atrophic or hypertrophic. The atrophic nonunion, also
termed non-reactive, displays radiographic evidence of bone ends rounding off and the
absence of bone callus. Atrophic nonunions are classified as comminuted, with multiple
fragments and gapping; torsion wedge, where a necrotic butterfly fragment impedes
healing; and simply atrophic, where the ends are wasted or markedly rounded. Devitalized
and/or septic bone requires surgical excision and often bone grafting for repair. Hypertrophic
nonunions display radiographic evidence of the bone ends flaring or mushrooming; and
are classified as elephant foot, where there is maximum widening at the interface; horse
hoof, where there is moderate callus flaring; and oligotrophic, where there is minimal
reactive callus.
A pseudoarthrosis is a nonunion with a fibrocartilaginous interface between the fracture
fragments. An articular fracture nonunion may develop into a synovial pseudoarthrosis.
A pseudoarthrosis can also be classified as infected, previously infected or non-infected;
as well as metaphyseal or diaphyseal. A bone scan or MRI can be useful in confirming
vascularity atthe delayed or nonunion site. Diffuse increased uptake of radionuclide is seen
at the hypertrophic nonunion, and may display a biphasic pattern if elephant foot or horse
hoof hypertrophy are present. An Indium-111 labeled white-blood cell scan can also be
useful in the evaluation of suspected infected pseudoarthrosis or nonunion. If the fracture
cleft is large enough, or in the presence of alarge-enough synovial pseudoarthrosis, a bone
scan may reveal a cold cleft. Otherwise, bone scans are not of much use in distinguishing
between delayed and nonunions. CT scans, linear tomography, MRI, stress fluoroscopy,
and intramedullary venography, can also be used to evaluate a delayed Of nonunion of
28 Basic Pathophysiology Ch.2
bone. In regard to noninvasive measures, overall, MRI provides the most diagnostic and
anatomical information regarding asuspected nonunion or pseudoarthrosis. A CT scan is
particularly valuable when trying to identify intervening fracture fragments.
Treatmentof ahypertrophic nonunion involves immobilization and non-weight bearing, bone
growth stimulation (BGS), and continued monitoring. The decision may also be made to
operate. An atrophic nonunion, or an infected or synovial pseudoarthrosis, requires
operative intervention for resection of necrotic or problematic tissue, bone grafting or
reapproximation of bone, followed by application of BGS and immobilization and non-weight
bearing. BGS is ineffective in the treatment of pseudoarthrosis, or, if the gap between
fragments is greater than 1/2 the diameter ofthe bone.
Bone Growth Stimulation (BGS)
Electrical bone growth stimulation (EBGS) and low-intesity ultrasound (UUS) bone
growth stimulation can be used in the treatment of nonunion, failed fusion, congenital
pseudoarthrosis, and fresh fractures (see package insertforthe specific device, for precise
FDA-approved indications and contraindications). EBGS and UUS are not effective in the
presence of acquired synovial or infected pseudoarthroses, when the gap between bone
margins is greater than 1/2 the diameter of the bone, or when sepsis is advanced. BGS is
contraindicated in the presence of neoplastic bone disease. A "hot" bone scan or MRI
should be observed prior to use of BGS. BGS is founded on the fact that areas of bone
growth and fracture healing display electronegativity due to stress-generated (piezoelec-
tric) polarity in collagen. In the presence of electronegativity, low-intesity ultrasound,
and strain-generated potentials, bone forming growth factors are upregulated and new
bone formation induced. BGS can be achieved using any of a number of effective devices
(Table 2.1).
Table 2.1. OPTIONS FOR STIMULATED OSTEOGENESIS
TYPE METHOD USE DEVICE
Invasive Direct current (20 IlA) 24/7* EBI OsteoGen
Noninvasive Pulse electromagnetic 3-10 hrs/ EBI Bone Healing
fields (PEMF) {mVj day System. Orthofix
PhysioStimLite
Combined PEMF (mV) 30 min/day Don Joy Orthologic
Capacitative coupling 24/7* EBI OrthoPak
(9 volt dry cell,
skin patch electrodes)
Low energy ultrasound 20 min/day Smith &
(30 milliwatts/cm2) Nephew Exogen
* 24/7 ; 24 hours/day. 7days/week. or until power source is exhausted.
29 Ch.2 Basic Pathophysiology
The precise method of BGS to be used is determined based on the surgeon's
experience and the patient's needs and ability to properly use the device. The devices vary
in regard to size, weight application, precision with which the energy is directed at the
target bone, and ease of use. Despite technical differences between the individual
stimulators, all of the devices have been clinically proven to work.
In regard to the surgically implantable direct current device, issues of compliance are
obviated by the fact that the stimulator, along with the hermetically sealed power supply,
stimulate bone growth constantly until the battery is exhausted (24-36 months).
Furthermore, with the implantable stimulator, cathode configuration can be varied
according to the specifics of the anatomical site, and the cathode and lead wire should not
contact any hardware used to stabilize the healing bone. The implantable EBGS requires
subsequent surgical retrieval of the power pack and lead wire.
In regard to the capacitative-coupled device, 2 electrodes are affixed (adhesive
patches like EKG leads) to the skin surface on either side of the nonunion, which may
require windowing the cast or using an external fixator to enable access to the target site.
The device runs constantly, as long asthe batteries (supplied by EBI) are changed daily. Like
the capacitative-coupled EBGS, LlUS requires access to the skin surface so that
ultraqsound gel can be applied driectly over the target bone, and this may warrant
windowing the cast or using an external fixator. PEMF devices only need to be secured in
close proximity to the target bone, and they induce electrical current in the bone by means
of asurrounding magnetice field. These devices can be worn outside of a bandage, cast or
immobilizing splint
CARTILAGE HEALING
Hyaline cartilage consists of chondrocytes within aglycosaminoglycan matrix, along with
type II collagen fibers. Fibrocartilage contains type I collagen. Cartilage does not have a
direct blood supply, however it requires synovial fluid for nutrition on its superficial
(articular) surface. Cartilage is viscoelastic due to canals through which synovial fluid flows,
allowing deformation in response to compression and shearing loads. Cartilage wounds
can be partial or full-thickness, and can be difficult to heal. Following articular fracture or
cartilage injury, necrotic cartilage is phagocytosed by macrophages arriving atthe wound
via inflammation. Healing thereafter occurs by means of limited chondrocyte mitosis and,
forthe most part, metaplasia of mesenchymal stem cells into fibrocartilage or near-hyaline
cartilage. Ideal joint repair increases the likelihood of hyaline-like (more type II collagen)
cartilage repair. Undifferentiated stem cells arrive at the cartilage defect via disruption
of the subchondral cortical bone plate, whether via fracture or by means of surgical
perforation, from medullary sinusoids of adjacent epiphyseal and metaphyseal bone.
Healing requires restoration of joint capsule and ligaments, perforation and realignment of
the subchondral bone plate for support and vascularity, and motion under reduced pressure
(non-weight bearing motion). Partial thickness wounds require sculpting (saucerization) of
any jagged or elevated cartilage margins, and perforation of the subchondral plate. Necrotic
fragments should be excised.
TENDON, LIGAMENT AND JOINT CAPSULE HEALING
Tendon, ligament and joint capsule heal by means of lag (substrate), fibroproliferative, and
maturation phases. The lag phase occurs during the first two weeks; is enhanced by
immobilization; and entails inflammation and fibroblastic splinting, with the majority of tissue
strength due to sutures. Fibroplasia and vascularization increase during the 2nd week,
30 Basic Pathophysiology Ch.2
and strength exists primarily due to sutures and immobilization is still required. The fibropro-
liferative (collagenation) phase occurs during week 3, and consists of a marked increase in
fibroplasia. At this time, moderate collagenation strength can sustain gentle passive motion
or isometric (in cast or brace) exercises. The remodeling (maturation) phase begins after 4
weeks, with collagen realignment and remodeling yielding moderate (not full) strength.
Gradual, progressive strengthening occurs with subsequent passive and active exercises.
PERIPHERAL NERVE WOUNDS AND HEALING
Peripheral nerves respond to injury with inflammation, collagenation, and Wallerian
degeneration. Fibroblasts within the connective tissue sheaths respond to inflammation
with increased collagenation.
Seddon's Classification of Nerve Injury
Neuropraxia-the myelin sheath is disrupted by blunt trauma or compression, causing
physiologic blockade of saltatory conduction. Thickly myelinated, large diameter, rapidly
conducting nerve fibers are most susceptible. Adifferential paralysis can develop, wherein
deep tendon reflexes, skeletal muscle function, vibratory and two-point discrimination are
lost, while pain and temperature sensation, and autonomic function persist. Repair can take
days to months, and is usually perfect as the nerve sheaths and axons remain intact, and
only the myelin must regenerate.
Axonotmesis-involves disruption ofaxons, with maintenance of supporting connective
tissue sheaths. Causes include prolonged compression, traction, ischemia, and toxins.
Wallerian degeneration occurs with distal axon degradation via phagocytic Schwann cells,
while the proximal portion of the axon and nerve cell body convert from the production of
neurotransmitter to making macromolecules for axon regeneration. Axonotmesis affects
heavily myelinated fibers equally as well as unmyelinated fibers. Nerve fiber regeneration
occurs at the rate of 1 mm per day from the point of injury. Because the endoneural
scaffold and supportive sheaths remain intact, the budding neurite (new axon) can grow
down its corresponding distal endoneural tube, en route to the nerve's end organ.
Functional recovery is generally good, but diminishes as the distance from the point of
injury to the end organ increases. The more proximal the lesion, the less likely it is that
normal function will return. An injury at the sciatic level is less likely to fully regenerate
compared to injury of the posterior tibial nerve at the level of the ankle. Proximal lesions
affect awider distribution and convey aworse prognosis.
Neurotmesis-involves disruption of nerve fibers as well as the supportive connective
tissue sheaths of the nerve trunk, and is therefore the most devastating form of injury.
Causes include sectioning injuries such as laceration, gunshot wound, open fracture,
severe traction or avulsion. punctures, and injection oftoxin. Because the distal endoneural
tubes are disrupted, it is difficult or impossible for budding neurites to bridge the defect and
grow into corresponding endoneural tubes and properly innervate end organs. Confused
reinnervation is often the case, as neurites that do manage to bridge the defect grow into
endoneural tubes that previously corresponded to other nerve fibers. Even with surgical
intervention to resect necrotic tissue and fibrosis, and to realign fasciculi, regeneration is
imperfect at best and almost impossible without surgical repair. For this reason, nerve-
suturing techniques are essential. Nerve fiber regeneration occurs at 1mm per day, and
axon exhaustion can occur with far proximal lesions. In the case of nerve excision, such as
31 Ch.2 Basic Pathophysiology
in the treatment of Morton's neuroma, the distal segment ofthe nerve trunk is excised and
budding neurites have no chance of achieving reinnervation. Astump neuroma will always
form at the point where the nerve is sectioned, and can be minimized with epineuroplasty
(closure ofthe epineurial cuff).
Entrapment Neuropathy
Nerve entrapment involves impingement of a peripheral nerve trunk by neighboring
anatomic structures, typically where the nerve traverses afibro-osseous tunnel. Classical
impingement sites include the posterior tibial nerve and its branches in the tarsal and
calcaneal tunnels and the plantar common and proper digital nerves in the intermetatarsal
spaces (Morton's neuroma). Injury takes the form primarily of neuropraxia and, in severe
cases, axonotmesis. Prolonged entrapment leads to the development of a neuroma-in-
continuity. Inflammation of surrounding connective tissues can lead to perineural fibrosis.
Signs andsymptomsinclude liners sign, which is pain and paresthesia within the entrapped
nerve's distribution upon percussion or palpation of the nerve trunk at the point of
entrapment. Percussion or palpation of the entrapped nerve may also effect proximal
radiation of paresthesia along the nerves course (Valleix sign). Generally, sensory
abnormalities occur before autonomic (sudomotor, vascular smooth muscle, arrector
pili) dysfunction, and skeletal motor dysfunction is usually last to occur. Electroneuro-
diagnostic testing may show decreased nerve conduction velocity and electromyographic
evidence of fibrillation due to entrapment It is importantto note that electrical testing may
be normal despite functional entrapment with a great deal of symptomatology when the
patient is weight bearing or active. Differential diagnoses include radiculopathy, metabolic
or hereditary polyneuropathy, compartment syndrome, musculoskeletal pathology, and
complex regional pain syndrome (causalgia and RSDS).
Treatment includes protection of the nerve from external forces, anti-inflammatory
medication administered systemically as well as local corticosteroid infiltration about
the nerve trunk, ultrasound therapy, other pharmacological therapy, and surgical
decompression when non-surgical measures have failed to satisfactorily alleviate pain.
Pharmacological approaches are variable, and include:
Capsaicin-topical, to diminish substance Pat C-type fiber terminals
Tricyclic antidepressants-oral. effect selective neurotransmitter blockade; watch
for anticholinergic effects such as dry mucus membranes, insomnia, palpitation,
lightheadedness, and cephalgia; available as: amitriptyline, imipramine, dsipramine,
nortriptyline, paroxetine, and trazodone
Anticonvulsants-oral, effect selective neurotransmitter blockade; with side effects
similar to those noted fortricyclics; available as: carbamazepine, diphenylhydantoin,
gabapentin, pregabalin, and cymbalta
Local anesthetics-such as mexiletine (oral administration) and lidocaine (IV
administration or via transcutaneous patch application)
Adrenergic agonists-such as clonidine transdermal patch
Aldose reductase inhibitors-these can be particularly useful for diabetic
neuropathy, and include: sorbinil, tolrestat, epalrestat
Other agents-including prostaglandin El, and B-complex vitamins
32 Basic Pathophysiology Ch.2
The mainstay of surgical treatment involves external neurolysis, with subsequent nerve
repositioning or excision. Nerve ensheathing in silicone, or capping, is of questionable
benefit and usually effects symptoms of entrapment. External neurolysis alone is often
adequate for symptomatic relief, and is performed using loupe magnification and fine-tipped
instruments. Specific entrapment neuropathies ofthe lower extremity include: saphenous
nerve where it emerges through the adductor canal, common peroneal nerve near the head
of the fibula (Fig. 2.11 (Maisonneuve fracture, constricting BK cast, lateral decubitus
position, traction injury with associated ankle sprain); superficial peroneal nerve where it
emerges through deep fascia proximal to the ankle (compartment syndrome. athlete or
jumper with peroneal muscle herniation through deep fascial hiatus [lienry's hiatus] at
emergence of superficial peroneal nerve (Fig. 2.2) [Henry's mononeuritisll , deep peroneal
nerve deep to the transverse or cruciate crural ligaments (anterior tarsal tunnel), sural nerve
near the lateral malleolus (any ankle sprain, or surgical approach to the lateral aspect
of ankle or heel, tendoAchillis surgery), tibial nerve and its branches deep to the flexor
retinaculum (tarsal tunnel syndrome), and the plantar nerves plantartothe deep transverse
intermetatarsalligaments (Morton's neuroma).
Figure 2.1
Saphenous
nerve and
vein
Figure 2.2
33 Ch.3 Selected Diseases and Pathological Conditions
SELECTED DISEASES AND PATHOLOGICAL CONDITIONS
DERMATOSES AND SKIN PATHOLOGY
The skin forms a barrier to the outside environment, serving as a protective layer from UV
radiation (melanocytes, dendrites and melanin), thermal and mechanical trauma, and
microbiological inoculation. It also retains moisture, participates in the immune response,
and regulates temperature. The epidermis consists ofthe following five strata, (listed from
deep to superficial): st. basale (the basal layer), st. spinosum, st. granulosum, st. lucid urn,
and st. corneum. Melanocytes located in the basal layer expand via dendritic processes
that contain melanin, which absorbs UV-B and thereby protects underlying living cells
from radiation-induced mutation. Merkel cells in the epidermis serve as sensory neuro-
transducers, and Langerhans cells of the epidermis participate in the immune response.
The dermis is composed ofthe papillary and reticular layers. The papillary dermis and basal
layer of the epidermis adhere along an undulating interface of rete ridges and valleys. The
papillary dermis conveys capillaries (responsible forthe pin-point hemorrhages noted upon
debridement of a verruca) and nerve endings; while the reticular dermis contains the skin
adnexae, microcirculatory vessels, and nerves. Deep in the dermis, near the subcutaneous
layer, are also found Pacinian corpuscles (Vater-Pacini units) that participate in deep touch-
pressure sensation. The skin adnexae include: eccrine sweat glands; pilosebaceous units
consisting of sebaceous gland, hair and follicle, and the arrector pili muscle, all of which are
under autonomic control; and the nail unit consisting of matrix, bed, folds and plate. The
glomus body is situated atthe toe tip, partially between the nail bed and distal phalanx, and
consists of an arteriole-to-venule capillary bypass (Susquet-Hoyer shunt) that participates
in thermoregulation, and may become tumorous.
Primary Skin Lesions
Macule-flat, discolored, well circumscribed, up to 1cm diameter
Patch-larger or coalesced macules, > 1 cm diameter
Papule-slightly elevated (due to inflammatory dermal infiltrate), well circumscribed,
up to 1cm diameter
Plaque-larger or coalesced papules, <2 cm diameter
Nodule-well circumscribed, firm elevations, > 2 cm but <3 cm diameter
Tumor-well circumscribed elevation> 3 cm diameter
Vesicle-serous fluid-filled, elevated, < 1cm diameter
Bulla-serous fluid-filled, elevated, > 1 cm diameter (may be hemorrhagic)
Cyst-sterile intradermal mass offluid or other material, contained within a defined
wall, such as a mucus, epidermoid inclusion, or sebaceous cyst
Burrow--intra-epidermal tunnel formed by scabies or other insect/parasite
Secondary Skin Lesions
Scale-thin, plate-like, cornified compact epithelial cells
Excoriation-superficial loss of skin
Erosion-gradual epidermal breakdown, sometimes referred to as a superficial ulcer
that heals without scarring
Ulcer-local excavation or surface defect created by sloughing of inflamed
necrotic skin f
Crust--a scab, caused by surface drying of exudate or secretions
34 Selected Diseases and Pathological Conditions Ch.3
Fissure-abnormal cleft or deep groove, usually hyperkeratotic superficially with an
open or hemorrhagic dermal wound deep in the recess
Scar-cicatrix, or the mark remaining after a dermal. or deeper, defect or other
morbid process has healed (hypertrophic, keloid)
Pustule-visible accumulation of pus within or beneath the epidermis, frequently in
an eccrine duct or hair follicle (pus is a liquid inflammatory product consisting of
leukocytes and serous transudate, along with bacterial and other proteins)
Abscess-a collection of pus in a cavity formed by disintegration of surrounding tissue
Furuncle-an accumulation of pus in the skin and succutaneous tissue, also known
as a boil; typically caused by Staph. entering through a follicle, associated with a
painful, nodular inflammation of skin with corium erythema and subcutaneous edema
Carbuncfe-a cluster of boils (furuncles) affecting skin, associated with subcutaneous
necrosis and multiple draining sinuses
Sinus tract-a cavity or channel connecting an abscess to the skin surface or
adjacent tissue layers (a fistula generally refers to a channel or tract connecting a
deeper organ to another organ or tissue layer, orthe skin surface)
Hyperkeratoses (HPKs)
Non-mechanically induced diffuse keratoses are usually bilateral, symmetrical, plantar
and palmar, and often inherited. Characteristics include 4:1 ratio of stratum (st.) corneum to
st. Malpighii (germinative layers of the epidermis, st. basale and st. spinosum). with the
granular layer, between the st. spinosum and st. lucidum of the epidermis. Common
non-mechanical diffuse HPKs include:
Psoriasis-maculopapulosquamous, silvery scales on erythematous base, Auspitz
sign (bleeds when scale removed!. elbows and knees
Unna Thost disease-bilateral, symmetrical, palms and soles, dominant inheritance
Mal de Maleda-forme fruste (partial expression) of Unna Thost, recessive
inheritance, with nail, ocular and dental involvement.
Vohwinkel's disease (keratoma mutilans hereditarium}-diffuse, honeycombed,
rippled keratosis of soles, star burst keratoma on knees, associated digital
contracture and pseudo ainhum
Keratosis pfantarum sulcatum-status-post immersion foot with Dermatophilus
congolensis
Pachyderma periostosis-keratosis of soles, periosteal hyperostosis, associated
with alveolar cell carcinoma
Alcoholic keratosis-mosaic, honeycomb dystrophic keratosis with sympathetic
component
Hauxthausen's disease (keratosis climactericum}-commonly on heels, erythema-
tous base, in postmenopausal women, associated with hypertension and
hyperuricemia
Moccasin fooE-chronic, dry. hyperkeratotic T. rubrum dermatophytosis
Hyperkeratosis traumaticum marginus as calcis (housewives heel)-secondary to
prolonged weight bearing barefoot or in an open back slipper failing to support the
heel (no counter)
Keratoderma blenorrhagica-chronic inflammatory maculopapular and scaly
dermatosis associated with Reiter'S syndrome (urethritis, iritis, arthritis), usually
in young males, localized to palms, soles and digits
35 Ch.3 Selected Diseases and Pathological Conditions
Mechanically induced diffuse keratoses can be unilateral or bilateral on the soles,
and show a 1:1 ratio of st. corneum to st. Malpighii with the granular layer intact. The
underlying dermis is usually fibrous, with dilated capillaries and eccrine sweat ducts, and
perineural fibrosis. There are typically about400 eccrine ducts per cm
2
of plantar skin. This
is often observed in patients with global anterior pes cavus with callus extending across the
entire ball ofthe foot.
Non-mechanically induced punctate keratoses characteristically display increased st.
corneum, a normal st. Malpighii, an intact st. granulosum, and loose underlying dermis.
Genetically determined forms include keratosis punctata of Hallopeau, which is dominantly
inherited, and displays hundreds of evenly distributed punctate keratoses, bilateral and
symmetrical, with truncated, macular and verrucoid lesions. Acquired punctate keratoses are
generally few in number, asymmetrical, and localized to skin creases. Acquired forms include:
Arsenical keratoses-arsenic intoxication (Cruveiler-Baumgartener disease),
affecting palms/soles, with hepatic failure; associated in past with certain
asthma preparations, wines, and seen in coal miners
Secondary syphilis-palms/soles, maculopapular, evolves to punctate keratoses
Darier's disease-greasy, vegetative lesions, punctiform on palms/soles, external
auditory meatus, cheeks
Aigner's syndrome (form fruste of Albers-Schonberg disease)-punctate keratoses
of palms/soles with osteopetrosis
Hanhart's syndrome-punctate keratoses of palms/soles, with multiple lipomas
Basal cell nevus syndrome-pink (ham colored) pits with ice pick, punctate keratoses
Non-mechanically induced punctate keratoses of unknown etiology include heloma
neurofibrosum, which displays keratinous filaments, typically about the perimeter of the heel,
resembling mosaic verruca, with banana-like projections, single or multiple, and very painful.
Mechanicallyinducedpunctate keratoses characteristically display a1:1 ratio of st. corneum
to st. Malpighii, aparakeratotic plug with atrophy of underlying granular layer, dilated eccrine
sweat ducts, dermal fibrosis, capillary ectasia and perineural fibrosis. Included are:
Parakeratosis plantaris discretum of Steinberg-translucent keratinous plug with
surrounding white (macerated) rim of blocked eccrine duct
Vamp disease-typically overlying EHL., or another extensor, tendon, where shoe vamp
chronically irritates skin resulting in parakeratosis, loss of granular layer, and often a
sinus tract due to draining bursa or tendon sheath
Dermatitides
Dermatitis has many causes and forms, and is typically treated with topical or systemic
corticosteroid, local care, and protection.
Atopic dermatitis-a chronic pruritic eruption common in adolescents and adults,
attributed to allergic, genetic and psychogenic causes; common to tlexor surfaces,
displaying crusts, lichenification, and excoriation
Nummular (coin-like) dermatitis-of unknown etiology, affects extensor surfaces,
buttocks and legs, and displays papulovesicular eruption, forming crusts
Lichen simplex chronicus (localized neurodermatitis)-due to repeated scratching,
most common in temales and Asian individuals, with well-demarcated scaly erythema
36 Selected Diseases and Pathological Conditions Ch.3
Contact dermatitis--an acute inflammation caused by contact with an allergen
effecting delayed hypersensitivity, and usually well-demarcated with araised margin
Dyshidrosis--any disorder of eccrine sweat ducts, such as pompholyx. Pompholyx
("bubbles") is a skin eruption, typically on the sides of fingers and toes, palms and
soles, consisting of discrete 1to 2 mm intra-epidermal vesicles with surrounding
erythema, associated with intense itching, lasting 1to 2weeks intermittently
Id reaction (id rash)-a remote rash associated with a primary lesion caused by
cutaneous sensitization resulting in a distant site allergic reaction to circulating
allergen, such as dermatophytid or syphilid
Stasis dermatitis--affects the distal leg, ankles and hindfoot, secondary to chronic
venous insufficiency (valvular incompetence due to dilation of vein) or lymphedema,
with cyanosis, erythema, pruritus; progressive over years, and may eventually ulcerate
Purpura and otber Hemorrhagic Lesions
Purpura are a group of disorders characterized by brown, red or purple subepidermal
hemorrhages. Petechiae are pinpoint, macular, round, purple or red, intradermal or
submucous hemorrhages. Purpura are larger than petechiae 1 em), but smaller than
ecchymosis (> 1em). Ecchymosis, are large hemorrhages causing black and blue marks or
bruises. Purpura are caused by thrombocytopenia, amyloid, steroids (capillary fragility),
rheumatic vasculitis (leukocytoclastic angiitis)' polyarteritis nodosa, serum sickness, SLE,
Henoch-Schonlein disease, and hemorrhagic fever (Ebola virus). Splinter hemorrhages
occur in the nail bed, and may be indicative of subacute bacterial endocarditis.
Papulosquamous Eruptions
These are characterized by slightly elevated, erythematous and scaly lesions, and include:
Tinea pedis--dermatophyte or other fungal or yeast infection
Psoriasis--chronic, hereditary, recurrent papulosquamous eruption occurring on the
scalp and extensor surfaces, displaying ared macule, papule or plaque covered with
silvery scales, removal of which effects local bleeding (Auspitz sign)
Secondary syphilis--maculopapular and pustular eruption caused by T. pallidum
infection, avenereal disease; the primary stage being ahard chancre, from which the
bacteria spread systemically via lymphatics and blood. Secondary syphilis occurs 6-
12 weeks after initial infection, displays fever, copper-hued multiform papular skin
eruptions (syphilids), iritis, alopecia, mucous patches, and severe arthritis. Tertiary
syphilis is late stage generalized disease affecting the CNS, bones, joints, and
parenchymal organs
Lichen planus--wide, flat, violaceous, itchy skin papules with acharacteristic sheen,
occurring in persistent patches, of unknown etiology (viral or psychogenic are
suspected). The scaling lesion of Uchen planus may demonstrate Wickham's striae
(network of white lines)
Pityriasis rosee-fine, branny, scaling pink oval macules aligned with skin creases
Benign Pigmented Skin Lesions
A nevus is a well-demarcated, stable, malformation of hereditary origin, involving
epidermal, skin adnexal or vascular elements. A nevus containing melanin is said to be
pigmented. Pigmented nevi include:
Junctional nevus--brownish, smooth, hairless, macular or slightly elevated, 1to 8mm
diameter, occurring on any skin surface, histologically displaying nests of melanocytes
"dropping off" into the dermis
37 Ch.3 Selected Diseasesand PathologicalConditions
Compound nevus-raised, flesh-coloredtobrown,oftenpapillomatous,maycontain
hairs,withmelanocytesintheepidermis(newlyformed)and dermis(older)
Intradermal nevus-similar tocompound,typicallymorepapillomatous,withhairs,
and allmelanocytesareinthedermis(older)
Nevievolvefrom epidermistodermis,associated WITh elevation and involvementof
skin appendages(hair). Nevusflammeus(portwine stain, orcapillaryhemangioma)isa
diffuse,poorlydemarcatedareaofpink/red/blue/purplecapillarydilationinotherwisenormal
skin(notmelanocytic).livedo,orlivedoreticularis, isvascularcongestion causing mottled
cyanosis,oftencausedbycoldexposurebutmaybepermanentsecondarytovenulardilation.
Vesicles and Bullae
Table 3.1. CAUSES OF BULLOUS ERUPTIONS
COMMON BULLOUS DISORDERS UNCOMMON BULLOUS DISORDERS
Physical(heat,friction,cold)
ExcesssunorUVexposure
Drug-inducedphotosensitivity
Systemicdrugreaction
Infection(bacterial,fungal,viral)
Contactdermatitis
Eccrinedysfunction(pomphylox)
multiforme
Pemphigus
Epidermolysisbullosa
Dermatitisherpetiformis
Bullouslichenplanus
Toxicepidermalnecrolysis
Diphtheriacutis
Herpes infection-results in clusters of small vesicles, with H. simplex Type I
occurring on skin or perioral. and Type II affecting genitalia. There is often a
prodromalfever, and lesionscan berecurrent. Herpeszosteriscaused bythesame
virusthatcausesvaricella(chickenpox),whichresidesinthedorsalrootganglion,and
eruptsinaunilateral,tensevesicular,usuallytruncal,inflammationinthedermatomal
distribution ofthe affected spinal nerve root,frequentlypainful, and occasionally
associatedwithpost-herpeticneuralgia(shingles).
Erythema multiforme-an urticarial eruption of immune origin, displaying red to
purple,raisedbullae,classicallywithtargetoririslesions,severeformsofwhichare
termedStevens-Johnsonsyndrome,and canbefatal.
Pemphigus-typically occursin middleto olderaged persons ofJewishdescent,
considered autoimmune or viral. with vesicles and bullae on skin and mucus
membranes,treatedwithsteroids,chronic,andoftenwithhighmorbidityordeath.
Epidermolysis bullosa-typicallyoccursearlyinlife(1 to2years)atsitesofprevious
skintrauma,typicallyminor,can be fatal in an infant,andtreatedwithsupportive-
measures.
Dermatitis herpetiformis (Duhring's disease)-a chronic, systemic vesiculobullous
eruptionontheextremitiesandtorso,withassociatedenteritis,largeconcentrationsof
IgA,andconsideredautoimmune.
Toxic epidermal necrolysis (scalded skin syndrome)-can affect all ages with
epidermalnecrosisandsloughorpeeling,oftencausedbystaphylococci,andtreated
inafashionsimilartoburns.Canalsobeadrugreaction,mostnotablywiththeuseof
Allopurinol,NSAlDs,Sulfonamidesandmeaslesvaccine.
38 Selected Diseases and Pathological Conditions Ch.3
Nodular or Granulomatous Lesions
Necrobiosis Jipoidica diabeticorum-displays dermal edema and collagen distortion,
yellow-brown pigmentation, loss of elasticity, well-circumscribed annular pretibial
patches in diabetics, histologically showing palisading granuloma.
Granuloma annulare-annular, hard, reddish, perimalleolar or dorsal, nodular lesion,
benign and recurrent, occasionally related to diabetes, histologically showing
palisading granuloma.
Erythema nodosum-acute inflammatory skin disease with tender red, pretibial
nodules, successive patches over a few weeks, considered an allergic reaction,
frequently seen with tuberculotoxin, streptococcal infection, drug reaction,
coccidiomycosis and psittacosis.
Sarcoidosis-chronic, progressive, systemic granulomatous disease of unknown
etiology, affecting any organ system, a common cause of pulmonary hilar
adenopathy, histologically showing noncaseating epithelioid cell tubercles (tuberculin
negative usually).
Angiolipoma-well vascularized, benign tumor of mature fat cells, often localized
aboutthe tibial plateau and malleoli. Neurilemmoma is aperipheral nerve sheath tumor
of myelin.
Glomus tumor-red dish-blue nail bed lesion displaying myoepithelial cells and
dilation of the Sequet-Boyer canal in the subungual papillary dermis, rarely observed
beyond 25 years of age.
Eccrine spiradenoma-deep, benign, solitary nodule arising from the coil of an
eccrine gland, covered by nonmal appearing skin and associated with paroxysmal pain.
Leiomyoma-benign arrector pili smooth muscle tumor (more commonly, uterine
fibroid).
Leprosy (Hansen's diseaseHue to Mycobacterium leprae infection, causing
asymmetrical, maculopapUlar, hypopigmented, circumscribed skin granulomas that
often progress to digital ainhum and spontaneous amputation. Leprosy is diagnosed
bacteriologically and histologically, and treatment entails diaminodiphenylsulfone
(Dapsone or DDS) combined with rifampin, or clarithromycin and clofazimine.
Ulcerative Skin Lesions
Hypertensive ulcers-localize to the lateral malleolar, digital. and dorsal areas,
are punched-out secondary to occlusion or spasm of arterioles, and are very painful.
Treatment entails control of underlying HTN and local care.
Venous stasis ulcers-localize along the saphenous vein secondary to venous
hypertension caused by valvular incompetence, display stasis dermatitis with
surrounding hyperpigmentation and eczematous vesicles and crusts, and are
irregularly shaped with granular base and may become secondarily infected.
Treatment consists of venous compression, elevation, cleansing, and protection.
Decubitus ulcers-display a well-circumscribed, undermined margin; are
localized to bony prominences and are associated with immobility and pressure. They
are often tender, and respond well to cleansing and pressure relief.
Mal perforans ulcers-punched out, nontender (insensitive), undermined and
related to repetitive pressure. They respond well to supportive measures unless
underlying bone infection develops.
Sickle cell ulcerations-localize perimalleolar, are recurrent due to sludging of
sickled RBCs and infarction. They are associated with hyperpigmentation and
inflammatory infiltrate effecting induration, and are very painful.
39 Ch.3 SelectedDiseasesand Pathological Conditions
Skin Lesions Predisposed to Malignant Transformation or Association
Actinic (solar) keratosis-sharply outlined,red orflesh colored macule, orslightly
raised,verrucousorsquamousgrowthon sun exposedsurfaces.Itmaydevelopinto
acutaneoushorn,orevolveintosquamous cell carcinoma. Itis consideredto be of
UV mutation origin and is seen in the middle aged to elderly, usually in light
skinnedindividuals(alsocalledsolarorsenilekeratosis).
Porokeratosis of Mibelli-rare chronichereditaryskindiseaseofthehandsandfeet,
with hypertrophy of the st. corneum about the eccrine sweat ducts. It may
becomedysplasticandeffectsquamouscarcinoma.
Xeroderma pigmentosum-rare, familial recessive trait, that is often fatal.
affecting skin with atrophy and pigmentation. Itis associated with skin and eye
photosensitivityhasitsonsetin childhoodwithdevelopmentofaffiliates(freckles),
telangiectasia,papilloma,hyperkeratoses,melanomaandcarcinoma.
Ataxia telangiectasia (Louis Bar syndrome)-hereditary progressive ataxia. Itis
associatedwith oculocutaneoustelangiectasia,pulmonarydisease and respiratory
tractinfection,andocularmuscledysfunction.
Malignant Skin Lesions
See selected neoplasms.
Nail Disorders (Onychopathy)
Congenital Defects
Anonychia-absence ofoneormorenailplates,associatedwithichthyosis.
Macronychia-anomalously largenail plate, otherwisenormalin appearance(may
also be acquired secondary to acromegaly, COPD or pulmonary hypertrophy
[clubbingofthedigits]).
Micronychia-anomalously smallnailplates,otherwisenormal.
Onychoheterotopia-nail growth in abnormal location, such as the dorsal or
plantarskin ofthetoeorfoot.
Pachyonychia-abnormally thick,heavilystriatedlongitudinally,occasionallylyticnail
plates(can alsobeacquiredsecondarytorepetitivemicrotrauma).
Polyonychia-extra orsupernumerarynail plate on asingletoe,withone or more
matrices.
Synonychia-a singlenailshared bytwoormoresyndactylizeddigits.
Traumatic Conditions
Hangnail-periungual, filamentousepidermalspicule.
Subungual hematoma-damage tothe nail bed causes hemorrhagethattillsthe
potential space between nail plate and bed, may be associated with simple or
complex bed laceration,open phalangeal fracture, and should be drained (hand
cauteryperforation)ifacuteand painfulorthrobbing,orrequiresremovalofthe nail
plateforrepairofthebedifmorethan25%ofthevisiblenailplatedisplayshematoma
oriftheplateissubstantiallyunstable.
Onychophagia-nail biting.
Onychocryptosis-a late effect of matrix distortion due to acute trauma or
repetitivemicrotrauma,whereintheplategrowsintotheadjacentnailfold,orwhenthe
nailiscutincorrectlyandtheadjacentfoldispushedbyexternalforcesintoandoverthe
plate. Onychophosisrepresentsnailfold hyperkeratosispriorto dermalviolation and
paronychia.
40 SelectedDiseasesand Pathological Conditions Ch.3
Onychogryphosis-distal plantarcurvature,withthickening orclubbing ofthe nail
plate,alateeffectofmatrixand/orbeddisruption,eitheracuteorchronic.
Leukonychia--white spots due to chronic microtrauma effecting plate
separation from the bed, with achange in the refractive index of light; to be
distinguishedfromwhitesuperficialonychomycosis.
Onychia or paronychia--nail fold inflammation,red and swollen,tenderand often
withdrainage,usuallyduetoonychocryptosis.
Onycholysis-separation of theplatefromthebed,canbetraumaticorsecondarytobed
hypertrophyoraccumulationofsubungualdebris,asinonychomycosis.
Metabolic and Systemic Conditions That ANect the Nails
Hyperthyroidism---koilonychia, onycholysis,fingernailsmoresothantoenails.
Psoriatic arthritis-pitting and onycholysis,discoloration,subungualhyperkeratosis,
splinter hemorrhages; usually treated with systemic control of arthritis, local
protectionand palliativecare.
Hypertrophic pulmonary osteodystrophy-digital clubbingduetoperiostealnewbone
formation,IPJarthritis,distaland plantarcurvatureofthenail,paronychia,widening
ofthedistaldigitaltuftand phalanx.ItisassociatedwithCOPO,lungCA.sarcoidosis.
Treatmentlocallyissupportiveinconjunctionwithidentificationandtreatmentofthe
underlyingsystemic disease.
Non-mycotic yel/ow nail disease-usually duetopulmonarydisease.suchaschronic
bronchiectasis, pleural effusion, chronic sinusitis, or chronic lymphedema. It is
associated with slownail growth. absence ofthe cuticle, nail plate hypertrophy,
increasedtransverse curvatureand yellowdiscoloration,avariantofclubbed nail;
and maybetreatedwithintradermaltriamcinolone,oralvitaminE, and identification
andtreatmentofunderlyingsystemicdisease.
Vitamin B12 deficiency-black-gray discoloration duetomelanindeposition inthe
nailmatrixandbed.Mustrule-outmelanoma.
INFECTION
Local signs of infection are those ofinflammation, and include rubor(redness),tumor
(swelling),calor(heat),and dolor(pain).The patientmaydisplayantalgic guardingofthe
infected lowerextremity.Wound drainageshould undergo Gram's stainand cultureand
sensitivitytesting. Constitutional signs and symptoms ofinfection includefever, chills,
malaise,loss ofappetite,and GI distress.The CBC showsa"leftshift"whereinthetotal
WBC countis elevated above 10,000, and granulocytesrise above 70%, and immature
leukocytebandsare identifiedinthe peripheralsmear. Blood culturesareindicatedwhen
theoraltemperatureis102
0
F(37
0
C)orgreater,takenfromthreeseparatesitesat30minute
intervals, if chills and/or hypotension occurs, or whenever septicemia is suspected.
Blood cultures have been reported to be positive in up to 50% of septic arthritis and
osteomyelitiscases.
Avariety of microorganisms can infect the lower extremity. Aerobic organisms
include gram-positive coagulase producing Staph. aureus (the most common infecting
organismofskinandsofttissue),coagulasenegativeStaph. epidermidis, beta-hemolyticgroup
A Strept (usually nonsuppurative with intense cellulitis and lymphangitis); gram
negative aerobes E. coli, Klebsiella, Pseudomonas, Enterobacter, and Serratia.
Anaerobic organisms include Bacteroides, Clostridium, and facultative Staph. and
Peptostreptococcus. Anaerobicinfectionsdevelopwhen aerobicorganismsmetabolize 02,
thereby enhancing conditions for anaerobes. Common synergistic organisms include:
41 Ch.3 Selected Diseases and Pathological Conditions
S. aureus, S. epidermidis, Peptostreptococcus, Corynebacterium, Bacteroides, and Clostridia.
Signs of anaerobic infection include foul smelling (fetid). brown, watery, exudate; necrosis,
subcutaneous gas effecting soft tissue crepitus (readily observed on standard radiographs),
and there is great risk for tissue loss and permanent dysfunction, as well as limb loss.
Identification of infecting organisms requires culture and sensitivity testing (C&S). An
open or draining wound presents exudate that can be swabbed for aerobic and anaerobic
C&S. Clinical suspicion (immunocompromised, chronic or recurrent infection, sickle-cell
anemia, concomitant infection elsewhere in the patient) should guide the practitioner to
obtain special microbiological testing when indicated, including acid fast (mycobacteria)
chocolate agar (Neisseria), and fungal C&S. Specimens can also be obtained via joint or
abscess aspiration, aspiration of sterile saline infiltrated dermis and subcutaneous tissue
when frank pus is absent (rather unreliable), and excisional biopsy with deep swab of
infected bone or sinus tract base. Whenever aspirating for C&S, it is important to try to
obtain the specimen through noncellulitic overlying tissues if possible. This is particularly
true when aspirating a joint. Aspiration requires aseptic skin preparation, and may be
enhanced with fluoroscopy.
Sinus tract cultures are not reliable for identifying actual underlying causative organisms
in cases of osteomyelitis, where it has been reported that a sinus tract C&S growing
Staph. aureus correlates with the underlying causative organism only 50% of the time.
Identification of other organisms from a sinus tract C&S correlates <50% with underlying
causative organism in cases of osteomyelitis. Bone cultures are the most definitive
diagnostic tool in cases of suspected osteomyelitis, and should correlate with bone biopsy.
It is often useful to discuss the matter of biopsy and C&S directly with the pathologist and
infectious diseases specialist whenever aquestion arises regarding diagnosis.
There are several specific types of skin and soft tissue infections. Cellulitis displays
erythema, edema and pain, and is often caused by Strep. Cellulitis can exist as an isolated
infectious process, or in conjunction with deeper and more extensive types of infection.
Pure cellulitis is usually treated without incision and drainage (1&0). The patient can be
treated with appropriate oral or IV antibiotics depending on severity.
Common Cutaneous Bacterial Infections
Ecthyma - Group Astreptococci (5. pyogenes) superficial infection due to minortrauma or poor
hygiene, with pustule formation, crusts and erythema, may ulcerate. The treatment is topical
mupirocin ointment (Bactroban) and 1st generation cephalosporin or erythromycin.
Impetigo- staphylococcus or streptococcus superficial infection, usually in children, pustules
with yellowish purulence, crusts. It is readily spread by contact with purulent lesions.
Usually treated with topical mupirocin ointment and oral 1st generation cephalosporin
or erythromycin.
Erythrasma intertriginous superficial infection caused by Corynebacterium minutissimus,
displaying maceration, scaling, fissuring, and erythema. Wood's lamp reveals coral red
fluorescence. It is treated with dilute povidone iodine soaks and oral erythromycin.
Necrotizing Fasciitis
Necrotizing Fasciitis involves infection dissecting along fascial planes, superficial to
muscle; and most often is caused by peptostreptococcus, S. aureus, Strept pyogenes,
Clostridium, and Bacteroides. Anaerobic muscle infection can cause myonecrosis with
subcutaneous gas, exotoxin release, myoglobinuria and renal failure, and bacteremia.
42 Selected Diseases and Pathological Conditions Ch.3
Myonecrosis (gas gangrene)
Myonecrosis is the most morbid and potentially lethal soft tissue infection of the lower
extremity. Necrotic muscle fails to display the four Cs: contractility (muscle stimulation with
the electrocoagulator causes visible contraction)' capillary bleeding (bright red blood), color
(beefy red), and consistency (firm).
Osteomyel itis
Osteomyelitis is defined as infection of bone and marrow. Osteomyelitis is distinguished
from infectious osteitis, which is suppuration of cortex without marrow involvement; and
infectious periostitis, which is periosteal contamination and inflammation. Osteomyelitis is
confirmed primarily by bone culture and, to a lesser degree, by bone biopsy (inflammatory
biopsy may be false positive). As a rule, osteomyelitis requires surgical debridement
followed by at least six weeks of antibiotic therapy. In some cases, based on clinical
observation, a four week (or less) course of antibiotics may be sufficient following
definitive bone debridement. A variety of classification systems exists for osteomyelitis
including the Waldvogel, Cierny, and Buckholz systems.
Waldvogel Classification of Osteomyelitis Waldvogel described a classification based
loosely upon the pathogenesis of the disease. The categories are Hematogenous
Osteomyelitis, Contiguous Osteomyelitis, and Osteomyelitis 'associated with vascular
insufficiency.
Hematogenous Osteomyelitis - result of bloodstream dissemination of bacteria
emanating from an identifiable focus of infection or developing during transient
bacteremia unrelated to infection. This is most common in patients between the ages
of 1to 20 years, and over 50 years. Blunt trauma to long bone (femur>tibia>humerus)
precedes this form of osteomyelitis in 33% of cases.
Acute Hematogenous Osteomyelitis (AHO) - can be effected by Streptococcal skin
infection, often associated with measles or chicken pox in childhood. Similarly, otitis
media due to Hemophilus, Staph., or pneumococcus can hematogenously spread
to bone. AHO localizes in metaphyseal bone due to the paucity of phagocytes and
sludging venous sinusoids. AHO in the infant (0 to 1 year) can involve the joint, as
capillaries traverse the epiphysis and effusion develops in 60-70% of cases. Group B
Strept., Staph. aureus, and E. coli are the most common organisms in AHO in the
infant. In the child, AHO usually does not involve the joint space and most commonly
localizes around the hip, shoulder, and ankle (distal lateral tibial metaphysis is
intra-articular, and can lead to septic arthritis with osteomyelitis). Extensive cortical
damage and involucrum develop, rarely is there damage to the growth plate or joint,
and Staph. epidermidis is causative in 60-90% of cases of AHO. In patients with
sickle-cell anemia or Sc hemoglobinopathy, Salmonella is most common; and
Hemophilus influenza is most common in children less than two years old. In the adult,
AHO is usually seen in patients older than 50 years of age. Pseudomonas is common
in IV drug abusers developing AHO; and in adults using IV catheters, suffering urinary
tract and pulmonary infection, or within two years following major surgery. Joint
infection may accompany AHO in the adult. Cases of AHO displaying purulence upon
aspiration, or failing to respond favorably within 36 hours of initiating antibiotic
therapy warrant operative intervention.
43 Ch.3 SelectedDiseasesand Pathological Conditions
Contiguous Spread Osteomyelitis - resultsfromdirectcontamination ofbonedueto
spreadofbacteriafrom contiguoustissue,isthemostcommonformofosteomyelitis
observedinpodiatriccases;generallyinvolvespatientsover40yearsofage;andmay
occurfollowingpuncture,laceration,ulceration,orsurgicalintervention.
Postoperative Contiguous Spread Osteomyelitis - includes acute postoperative
osteomyelitis (observed within one month of surgery), delayed postoperative
osteomyelitis (observed between one month and twoyears ofsurgery), and late
postoperative osteomyelitis(notobserved until atleast2years aftersurgery).Most
commonly, postoperativeosteomyelitisisofthedelayedorlatesort,usuallygrowing
Staph. or mixed flora. In allforms ofcontiguous spread osteomyelitis, adjacentsoft
tissue or bone infectionmustbe identified.Athorough searchforanearbyulceror
sinustractisimportant.
Direct Inoculation Osteomyelitis - is caused by contamination of bone without
adjacentsofttissue infection, and is eithertraumaticallyor surgicallyinduced.A
distinctionbetweenpostoperativecontiguousspreadosteomyelitisshould bemade.
Vascular Insufficiency Osteomyelitis - occurs in patientswith peripheralvascular
disease, wherein associated gangrene and ulceration are usually present. May
involve anaerobes, and myonecrosis should be considered. Hasfeatures similarto
contiguous spread osteomyelitis, howeverthe overriding distinguishing factor is
peripheralvasculardisease.
The Cierny-MaderclassificationofOM combinesanatomicand physiologiccategoriesin
an efforttodirecttherapy.Twelve differentstagesofosteomyelitiscan be described by
combiningthedifferentcategories(Table3-2).
TABLE3-2.THECIERNY-MADERCLASSIFICATION OFOSTEOMYELITIS.
Anatomical category PhYSiological category
I.Medullary A.Intactlocalvascularityandsystemicimmunecompetence
II.Superficial B. Compromisedlocalvascularityand!
orsystemicimmunecompetence
III.Localized C. Hostnotasurgicalcandidate,asoperativerisks
IV.Diffuse outweighpotentialbenefits
Bucholtzclassifiedosteomyelrtisusing7categories(Table3-2).
TABLE33.THE BUCHOLTZCLASSIFICATION OFOSTEOMYELITIS.
Category Etiology. anatomical site. and physiological type
A Woundinduced
B Mechanogenic
C PhysealOM
D Ischemiclimb
E Combination ofA-D
F SepticarthritiswithadjacentOM
G Chromic OMwithosteitis
44
A
C
Figure 3.1
Selected Diseases and Pathological Conditions Ch.3
Bone abscess
and
dying bone
(sequestrum)
B
D
Pus
Periosteum
\ '"
, . \
. '.
'f.J
iJ
'
I t.
C". ('. e.
Diagnostic Imaging of Infection-radiographic signs of infection include increased soft
tissue density and volume associated with inflammation and, in cases of OM, include
osteolysis, involucrum, cloaca, and sequestration (Fig. 3.1). Osteolysis is not visible as
radiolucency until 30-50% of osseous mineralization has been washed away by
inflammatory hyperemia. This generally takes 10-14 days after the onset of symptoms.
Thereafter sclerosis and periosteal new bone formation, known as involucrum, surrounds
necrotic and infected bone, known as sequestrum, and ultimately a channel, known as a
cloaca, forms in new bone as bacteria proliferate and exudate drains. Chronic OM involves
the presence of microbes living in dead bone (sequestrum), surrounded and contained
within new bone (involucrum). Eventually, after trauma or some other instigating factor, an
acute flare-up can develop with drainage, and signs and symptoms of acute infection.
Chronic osteomyelitis can lay dormant for many years (reportedly> 50 years) before a
flare-up occurs. In the presence of a chronic draining sinus due to OM (or other causes),
squamous cell carcinoma (SCC) can develop in the epithelium along the sinus tract as a
longterm sequellum. Radionuclide studies can be useful in the evaluation of suspected OM,
and include WBC scans labeled with Tc-99 or In-l11.ln most cases, bone scintigrams
become positive within 48-72 hours. In patients with Charcot neuroarthropathy, or
suspected fibrous nonunion, bone and joint infection may be strongly suggested with
identification of a "hot" In-l11 or Tc-99 labeled WBC scan (Indium and Seratec scans,
respectively). MRI may be the most useful imaging method when considering OM,
however positron emission tomography (PET) scans have been shown to be even more
45
Ch.3 Selected Diseases and Pathological Conditions
sensitive and specific for Charcot neuroarthorpathy, in comparison to MRI scans. None of
the imaging methods can be used to definitively ascertain OM, although alone and in
combination, they can be very helpful. Definitive diagnosis OM is made by means of biospy,
and bone gram stain and C&S.
Treatment of Infection-the treatment of any infection, including OM, entails adherence
to several general principles, including the 5 Os: 1) decompression, 2) drainage,
3) debridement, 4) dressings, and 5) drugs. Decompression is achieved with incision and
drainage (1&0) or removal of operatively-placed sutures, following surgical preparation.
Drainage is achieved with copious lavage, debridement and excision of necrotic and/or
grossly infected tissue, removal of implanted materials or foreign bodies, removal of
unstable internal fixation devices, open packing with fine-mesh gauze, or partial or complete
closure with drain placement. and use of an appropriate dressing. Tourniquets are
generally not used when performing I&D. The extent of infection is thoroughly explored and
drained, and definitive cultures and stains are obtained from the deep tissues. In cases
of OM. a small margin of apparently uninfected bone can be debrided and sent for
pathological inspection. In any infection. drainage is allowed to proceed as long as
necessary. usually aminimum of 48 to 72 hours. with dressing changes consisting of lavage
and debridement as indicated by wound appearance. If necessary, additional debridement
can be carried out by a return to the operating room, which is frequently necessary in cases
involving necrotizing infection. Care should be taken to avoid performing adelayed primary
closure too soon.
Antibiotic Therapy-antibiotics are the primary drugs used in the treatment of infection.
Consideration must be given to the spectrum of coverage, frequency of administration,
toxicity, duration of treatment and cost Prior to ascertaining the microbiological results of
definitive culture specimens, empiric antibiotic therapy is initiated (Table 3-4). In cases of
OM, antibiotic therapy is usually continued for 6 weeks following final debridement. A
Hickman, Broviac or Pice (peripherally inserted central catheter) can be used for longterm
IV therapy. Monitoring the course of treatment of infection requires attention to fever,
antibiotic levels, renal and hepatic function, wound appearance and pain, complete blood
count (CBC) and differential, erythrocyte sedimentation rate (ESRI. insulin requirement in the
diabetic, and C&S results. Antibiotic impregnated calcium sulfate, or polymethyl-
methacrylate (PMMA), beads may be packed in the wound and used in conjunction with IV
antibiotics. Antibiotic beads are usually made in the OR, using gentamycin, vancomycin,
clindamycin, or another antibiotic, and packed in the debrided bone to increase local
concentration of antibiotic. The wound is closed over the beads and, after 10-20 days (or
sooner or later, depending upon wound appearance), the patient returns to the operating
room for bead removal, further debridement, and placement of more antibiotic beads if
needed, or reconstruction and closure. A previously infected wound is ready for closure
after achieving at least one negative culture, and the wound looks clean with beefy red
granulations, no evidence of purulence or sinus tract, and resolution of marginal erythema.
In some cases, delayed primary closure can be undertaken without first ascertaining a
negative wound culture, as a wound that is clinically ready for closure usually has some
degree of surface contamination. Closure may be achieved by means of secondary
intention, or via delayed primary closure, skin graft, orfiap. Previously infected wounds are
generally closed over a drain of some sort, or only partially closed. Depending upon the
specifics ofthe infection, use ofthe wound vacuum, as well as hyperbaric oxygen therapy,
should also be considered.
46 Selected Diseases and Pathological Conditions Ch.3
Diabetic Polyrnicrobiallnfection-diabetic polymicrobial infection can be limb and life
threatening. Plantar space infection may develop, with abscess dissection along fascial
planes of the plantar vault into the posterior compartment of the leg, or through an
intermetatarsal space into the dorsum then into the anterior leg. The patient must be
evaluated for constitutional signs and symptoms of septic shock, including incoherence or
confusion, hypotension, tachycardia, and extreme hyperglycemia and ketoacidosis. Hospital
admission and inpatient management are usually in order. It is useful to obtain a serum
glucose level, CBC and differential, ESR, urinalysis, biochemical levels other than glucose,
EKG, foot/leg and chest X-rays, blood cultures x3 from 3 separate sites 30 minutes apart,
other labs and tests that may be warranted by the patient's individual condition, medical and
anesthesia consultation and co-management, and supportive therapy in preparation for
surgical debridement. Orders should also include NPO, wound and skin isolation, IV LR at
KVO via l8-gauge IV catheter, specific medications (chronic and acute). non-weight
bearing, on call to operating room for I&D. The patient, and/or a family member, must be
informed of the emergent nature of the condition, and possible consequences. Empiric
antibiotic therapy should be initiated prior to identifying definitive culture results, and
coverage should include anaerobic, aerobic, gram (+) and gram (-) organisms. A useful
initial regimen consists of a combination of amoxicillin-clavulonate, clindamycin, and a
quinolone (see Table 3-4). Intravenous antibiotics, such as ticarcillin-clavulonate, could also
be used until definitive cultures are identified. It can be helpful to obtain an infectious
disease consultation, as well as consultation regarding the potential benefits of hyperbaric
oxygen therapy (HBOT).
Incision and Drainage (I&D)-once the patient is prepared for surgery, I&D is performed
in the operating room. The patient should be supine, without a tourniquet, and an orthope-
dic prep ofthe lower extremity performed. The wound or abscess is then probed to deter-
mine its extent and confines, after which awide incision is made in orderto allow drainage.
Exploration entails inspection of all undermined or abscessed areas. In cases of diabetic
plantar vault infection, decompression of the vault requires opening the deep fascia
adequately enough to drain the medial, central, lateral, and deep plantar spaces, as
necessary. Deep specimens are obtained for gram stain and C&S, necrotic and infected
tissues are excised and biopsied, and foreign bodies are removed. IV antibiotics may be
altered based upon the results ofthe gram stain, however empiric therapy usually does not
change until definitive culture results are known. Copious lavage, sometimes using a pulsed,
power-flushing system, is perfomed after initial sharp debridement. Close inspection is paid
to all tissues prior to open packing with fine mesh gauze, then application of sterile
dressing. Subsequent daily or BID dressing changes are performed with lavage and
curettage of the wound, and additional specimens obtained for C&S as indicated by the
appearance of the wound. If the patient and wound are not responding to the treatment,
then there is either persistent abscess orthe choice of antibiotic is incorrect. An MRI could
help detect an unrelieved abscess. A return to the operating room for additional
debridement is performed whenever indicated, based on the patient's progress. The goal is
to achieve a beefy red granular base, with no purulence or malodor, with decreased edema
and erythema and pain, and no residual undermining or tunneling. Closure occurs thereafter
via either continued secondary intention healing, or delayed primary closure, or the use of a
skin graft or flap. In some cases involving aerobic infection, especially those with deep or
large defects, as well as those with considerable drainage, vacuum-assisted wound closure
can be helpful. The wound vacuum can also be used over skin grafts and flaps.
47 Ch.3 Selected Diseases and Pathological Conditions
Chronic Pedal Wound-when a patient presents with a chronic pedal wound, perhaps with
intermittent drainage that has lasted for months, consideration should be given to the
possibility of previous puncture wound or osteomyelitis. Common sites for chronic pedal
wounds include the digits, metatarsal ball, 5
th
metatarsal base, heel, and perimalleolar areas.
Protective sensation should be determined, since chronic ulceration is very commonly
associated with the insensitive foot (mal perforans ulcer). Puncture wounds that have
penetrated the sole of the shoe are likely to involve Pseudomonas aeruginosa, although
Staph. aureus remains the most common pathogen in barefoot punctures and in children.
As with all chronic wound, diagnostic images should be obtained, and consideration should
be given to the potential benefits of wound margin biospy and surgical debridement.
Radiographs are obtained, as are labs (as noted above for the diabetic infection), and
consideration given to a bone scan, or a CT or MRI scan. When indicated, the patient is
taken to the operating room for 1&0 and exploration. Do not dissect through the site of a
chronic draining sinus tract if possible, when exploring bone that may not be infected. A
dorsal approach can be useful in the case of a chronic plantar wound, as long as the nidus
of infection is not obscured from inspection. If there is any concern about compromising
drainage ofthe abscess, then simply excise the entire sinus tract The important point is to
explore the involved area and obtain appropriate samples for gram stain and C&S, as well
as soft tissue and bone biopsy. After obtaining specimens for C&S, then initiate IV antibiotics,
lavage, pack open, and initiate daily wound care.
Fungal Infection-fungal infections are extremely common in the foot and lower
extremities, and must be differentiated from other causes of papulosquamous eruption
(secondary syphilis, psoriasis, pityriasis rosea, contact dermatitis) when localized to the
glabrous skin. Fungi are eukaryotic and reproduce by spore formation, grow as hyphae and
form a mycelium. Some organisms, such as Candida, are dimorphic and grow as either
yeast orfungal hyphae depending upon the host environment. Fungi that infect humans are
categorized as either dermatophytes (superficial) or deep pathogens. The most common
pathogenic fungi affecting humans are the Fungi Imperfecti, although other groups can
infectthe compromised host.
Identification of the infecting fungus is made via skin shaving or nail fragment exam
for hyphae or yeast using KOH (potassium hydroxide) to dissolve keratin from skin
scrapings, or periodiC acid Schiff's (PAS) stain; and by means of fungal C&S using
Sabouraud's dextrose agar (SDA). Superficial mycoses include tinea pedis, candidiasis
(thrush), onychomycosis, tinea corporis, tinea cruris, tinea capitis, tinea axillaris, and tinea
versicolor. linea pedis is usually responsive to topical antifungal cream application for 2-6
weeks, with agents such as terbinafine and econazole proving to be effective. Patients are
encouraged to try over-the-counter antifungal preparations (tolnaftate, undecylenic acid,
miconazole, clotrimazole) for minor conditions of tinea pedis, ifthey have not already done
so. Candida species often infect the nail bed in compromised hosts, and cause paronychia
and pseudo-clubbing due to chronic digital inflammation. Onychomycosis typically
presents as either white superficial onychomycosis (WSO), which is usually caused by
Trichophyton mentagrophytes or yeast and is least common; distal subungual
onychomycosis (OSOI. which is usually caused by I rubrum and is most common; and
proximal subungual onychomycosis (PSO), which is also usually caused by I rubrum and
is rare and usually associated with systemic disease or HIV. Onychomycosis must be
distinguished from mechanically induced nail dystrophy, psoriatic pitting and flaking, lichen
planus and pterygium, COPO induced clubbing, dystrophy due to peripheral vascular
48 Selected Diseases and Pathological Conditions Ch.3
disease, and subungual exostosis. When harvesting nail and nail bed fragments for fungal
tissue examination and C&S, it is imperative to obtain plenty of nail bed fragments from
deep to the nail plate. Palliative treatment of onychomycosis includes nail plate debridement
and regular application of topical antifungal (ciclopirox 8% lacquer or miconazole 2%
solution, or similar agents), however cure rates are usually <75-80% with topical therapy,
although debridement alone is known to improve foot-related quality of life. Cure is more
likely with oral administration of either terbinafine (250 mg PO GO x 3 months) or
itraconazole (200 mg PO GO x 3 months), or perhaps fluconazole (as an adjunct for the
treatment of yeast). It is prudentto check liver enzymes and CBC, current medications, and
past medical history, prior to initiating oral antifungal therapy. Chemically induced
hepatitis has been greatly diminished using the newer systemic antifungal agents, as
therapy is only administered for 3-4 months, generally. Drug interactions (certain
antihistamines, anti-lipid agents, and others) must also be considered priorto initiating oral
antifungal therapy. The active metabolite ofthe agent is maintained in the substance ofthe
nail for 6-9 months, and the ultimate appearance ofthe nail plate cannot be truly assessed
until 6-12 months following initiation of oral therapy. Prevention of recurrent
onychomycosis may require periodic maintenance use oftopical therapy, and concurrent
debridement is a crucial part of any treatment plan. Deep mycoses include mycetoma and
madura foot, sporotrichosis, and blastomycosis; caused by Madurella mycetoma, Sporothrix
schenkii, and Blastomycoses, respectively. Deep fungal infections are granulomatous, with
papular and nodular inflammation of the subcutaneous tissues and overlying skin, sinus
tract formation, foul odor, and secondary bacterial infection may ensue. Treatment may
require excision of infected tissue, including amputation, and systemic administration of
amphotericin-B (sporotrichosis)' sufonamide and other oral antifungal agents (mycetoma,
madura foot, blastomycosis).
Septic Arthritis (see Arthritides)
Antibiotic Therapy-antibiotic therapy varies from community to community, and the
clinician is encouraged to be familiar with the characteristics of the organisms in his/her
own community. The local hospital's antibiotic susceptibility and causative organism
prevalence report can be a useful guide to therapy, and the county health department also
monitors organisms responsible for reported infections. Although it is often necessary to
initiate therapy empirically, it is always adviseable to obtain a culture from the lesion if this
is possible. Once again, appropriate specimens should be obtained for isolation of the
causative organism and determination of its susceptibility to antibiotic therapy. Bacterial
cultures are particularly important in cases of severe infection, in diabetic or compromised
hosts, and for chronic or recurrent infection wherein previous culture and sensitivity has not
been performed. In all cases of infection, ongoing assessment of the response to therapy
must be undertaken. Therapy is generally continued for 10-14 days for soft tissue infections,
and 6weeks for OM, and the treatment should be honed to the individual patients specific
local and systemic requirements. The following information is meant to serve as a general
guide to antibiotic therapy for infections involving the foot, ankle and leg. Since organisms
and antibiotcs evolve and change frequently, the reader is encouraged to check with
appropriate updated literature, such as the drug package insert, for specific indications
and dosages.
49
Ch.3 Selected Diseases and Pathological Conditions
Methicillin-resistant Staphylococcus aureus (MRSA)-community acquired methicillin-
resistant Staphylococcus aureus (MRSA) represents an ever-increasing proportion of
wound infections, particularly in children. MRSA resists the cidal effects of beta lactam
antibiotics such as penicillin and cephalosporin, including cephalexin, ceftriaxone, and
amoxicillin-clavulanate; and the organism may also resist the static effects of
erythromycin, clarithromycin, and azithromycin. Potentially useful oral agents include
clindamycin, trimethoprim-sulfamethoxazole, doxycycline, and linezolid; IV agents include
vancomycin or daptomycin; and mupirocin can be used topically. Rifampin can also be used,
however not as asole antibiotic. For limb- or life-threatening MRSA infection, high-dose IV
antibiotic therapy using vancomycin or daptomycin, perhaps combined with gentamicin,
should be considered. Some strains of MRSA display "inducible resistance" to agents such
as clindamycin, and these can oftern be identified using the "D test." A positive "D test" is
associated with an increased risk of antibiotic resistance, and careful clinical follow-up is
important. In an effortto prevent colonization and relapsing infection, 4-6 weeks oftherapy
may be necessary.
Postoperative Infection-overall, the prevalence of postoperative infection ranges from
1-2% of clean, elective bone surgical cases, and most of these involve Staph. aureus. In
cases involving implant infection, Staph. epidermidis, with its glycocalyx, is also common.
Other causative species associated with postoperative infection include Proteus,
Pseudomonas, 8-hemolytic Streptococcus, Klebsiella, Serratia, Enterobacter, E coli, and
Bacteroides. In general, when stable osteosynthesis implants are present in cases of acute
postoperative infection, metallic fixation devices are left in place unless they are associated
with loose or necrotic bone (hence, loose or unstable). Chronically infected hardware should
be removed and osteomyelitis therapy instituted.
Puncture Wounds-the status of the patient's tetanus prophylaxis should be ascertained
whenever a puncture wound is encountered. Appropriate diagnostic measures combined
with local wound care and antibiotic therapy are basic elements in the treatment of punc-
ture wounds. In general, antibiotic therapy should cover Staph. aureus, and other gram (+)
organisms, with appropriate attention to 1&0 if edema, cellulitis, induration, pain and Hx
suggest abscess. The use of cephalexin, dicloxacillin, or amoxicillin/clavulonate should be
considered. Punctures also convey the risk of anaerobic infection, and radiographs should
be inspected for the presence of subcutaneous gas, primarily hydrogen sulfide. Gas-
forming infections are usually necrotizing and require timely 1&0, and hyperbaric oxygen
therapy may also be useful (see Necrotizing Infection, above). For punctures that involve
penetration through the sole of the shoe, coverage of Pseudomonas sp. should be
considered, and potentially useful agents include aztreonam +clindamycin, or imipenem +
cilistatin, piperacillin +tazobactam, or ampicillin + sulbactam (see Table 3-4).
Empiric Antibiotic Therapy-the following table (Table 3.4) is meantto provide guidelines
for empiric antibiotic therapy, and the reader is encouraged to obtain definitive specimens
for C&S, and to be familiar with the detailed information contained in the package insert for
the specific antibiotic used.
50 Selected Diseases and PathologicalConditions Ch.3
TABLE 3-4. EMPIRIC DRUGS OF CHOICE FOR PREDOMINANT BACTERIA SEEN IN
ADULT FOOT AND ANKLE SURGERY.*
Organism
Gram(+)
Staphylococcus
(methicillinsensitive)
Streptococcus
Staphylococcus
(methicillinresistant)
enterococcus
vancomycinresistant
enterococcus
Therapy of Choice
cephalexin(250mg PO 010)
cefazolin(1-2g IVq8h)
penicillin(penicillin
V0.25-0.5gramsPOTID-OlD.
orpenicillinG1.2-20million
units1M/IVperday)
cephalexin(250mg PO OlD)
cefazolin(1-2g IVq8h)
vancomycin(15mg/kg IVq12h)
ampicillin(250mg-
1gramPOTID)
gentamicin(2mg/kg IVload
followedby1.7mg/kgIVq8h)
Alternate Therapy
clindamycin(300mg PO 010)
vancomycin(15mg/kgIVq12h)
dicloxacillin(250mg PO OlD)
nafcillin(2gramsIVq4h)
azithromycin(500 mg asa
singledoseon day1,followed
by250mg dailyon days2-5)
clindamycin (300mg PO OlD)
vancomycin(15mg/kgq12h IV)
clindamycin(300mg PO 010)
doxycycline(0.1 gramPO/IVq12h)
minocycline(0.1 gram PO q12h)
linezolid(600mg PO/IVq12h)
TMP/SMX(lOStab PO BID)
gentamicin(2mg/kgload
followed by1.7mg/kg IVq8h)[if
limb- orlifethreatening]
amoxicillin-clavulonate
(875/125mg PO q12hx14 days)
vancomycin(15mg/kg IVq12h)
Streptomycin(15mg/kg1Mq24h)
piperacillin/tazobactam(3.375
gramsIVq6h)
combination ciprofloxacin(500-
750mg PO BID).rifampin
(10mg/kg/dayupto600mg/day
PO singledose).gentamicin
(2mg/kgloadfollowed by
1.7mg/kgIVq8h)orceftriaxone
(1-2gramsIVoncedaily)
chloramphenicol(0.25-1 gram
PO/IVq6h upto4grams/day)
51 Ch.3 SelectedDiseasesand PathologicalConditions
GramH
Escherishia cali, Proteus
ECSM group
Pseudomonas
aeruginosis
Anaerobic infection
Bacteroides
Diabetic foot infection
polymicrobial
cephalexin(250mg PO 010)
ciprofloxacin
(500-750mg PO BID)
ciprofloxacin(500-750mg
PO BID)
metronidazole
(500mg PO q6-8h)
amoxicillin-clavulonate
(8751125mg POq12hx14days)
cefazolin(1-2gramsIVq8h)
+metronidazole
(500mg PO/IVq6-8h)
vancomycin
(15mg/kgq12hIV)+
aztreonam(2g IVq8h)+
metronidazole
(5OOmg PO/IVq6-Sh)
ciprofioxacin(500-750mgPOBID)
cefazolin(1 gramIVqBh)
3rdgenerationcephalosporin
(suchasceftriaxone1-2grams
IVoncedaily)
aztreonami1 gramqBh-
2gramIVq6h)
TMP/SMX(lOStab PO BIO)
ceftazidime(2gramsIVqBh)
aztreonam(2g IVqBh)
gentamicin(2mg/kgload
followedby1.7mg/kgIVqSh)
clindamycin(300mg PO OlD)
ampicillinsulbactam(1.5-3
grams IVq6h)
ticarcillinclavulonate(3.1
gramsIVq6h)
piperacillintazobactam(3.375
gramsIVq6hl
Imipenemcilistatin
(500mg IVq6h)
Specific dosages,serum druglevelmonitoring,creatinine and otherappropriate serumlaboratorytests,culture
andsensitivi1y,adjuncttherapy,andclinicalreassessmentsshouldbeindividualizedtothespecificpatientThereader
isencouragedtoconsiderIhefaclthalrecommendedantibiotictherapyoftenvariesovertimeandgeographicarea.
ACQUIRED IMMUNODEFICIENCY SYNDROME (AIDS)
AIDSiscausedbyinfectionwiththecytopathichumanimmunodeficiencyvirus(HIV)retro-
virus(RNAvirus),which causescelldeath.TheCD-4surfaceglycoproteinistheessential
moleculerecognized bytheretrovirus,onthesurfacesofT4lymphocytes,monocytes,and
macrophages.T-helperlymphocytes alsobecomeinfected and destroyed,which greatly
impairsthe immunesystem. Naturalkillerlymphocytesare also destroyed,which impairs
immune surveillance againstneoplasmsand virusinfected cells. Approximately40% to
50%ofpatientsinfectedwithHIV,andpossessinglessthan400T-helpercells,developAIDS
within2yearsofHIVinfection.Eighty-fivepercentofpatientswithT-helpercellslessthan
200,willdevelopAIDSwithin2yearsofinfection.
52 Selected Diseases and Pathological Conditions Ch,3
Four Stages of HIV Infection
Stage 1- manifesting acute HIV, wherein the patient displays general malaise and
"mono-like" symptoms
Stage 11- chronically infected with HIV, often asymptomatic while developing anti-
bodies to HIV
Stage III persistent generalized lymphadenopathy
Stage IV serious manifestations of immunodeficiency, frequent serious infections
and debilitation
Subgroups of Manifestations of HIV Infection
Subgroup A Constitutional symptoms
Subgroup B Neurological syndromes
Subgroup C - Associated with infectious diseases
CO) - Defect in cell mediated immunity (Pneumocystis pneumonia)
C(l) - Less profound infections
Subgroup D - Secondary cancers (e,g, Kaposi's sarcoma)
Subgroup E - Chronic lymphoid interstitial pneumonitis
The treatment of AIDS includes supportive measures, as well as suppressive and
disease modifying agents such as AZT. Therapeutic regimens have been shown to be most
effective when disease modifying agents are used in synergy, Maternal transmission of the
disease to the fetus has been controlled with AZT. Treatment regimens are very expensive,
Any patient suspected of being HIV positive should be counseled regarding the importance
of testing to confirm the presence of antibody, then appropriately referred for infectious
disease consultation, Social services consultation is also important, as various agencies may
be able to assist with therapy, Regardless of whether or not you suspect apatient of being HIV
positive, universal precautions are the standard of care in ALL aspects of health care,
SELECTED PERIPHERAL VASCULAR DISEASES
Raynaud's Phenomenon
Raynaud's phenomenon is an episode of small arterial and arteriole constriction resulting
in acral pallor, cyanosis, or both color changes; with subsequent rubor due to hyperemia
afterthe vasospasm has subsided (white, blue, and red coloration pattern), In severe cases,
prolonged vasospasm can effect cutaneous digital gangrene, The condition is usually
bilateral, however it may rarely be unilateral. It is more common in females, Serious organic
disease (atherosclerosis) is not usually present in the vessel in Raynaud's phenomenon,
When aspecific cause for the vasospasm, such as trauma, connective tissue disease, or
neurogenic, cannot be identified after several years of suffering, then the condition can be
termed Raynaud's disease (also known as primary Raynaud's phenomenon), Secondary
Raynaud's phenomenon can be attributed to trauma, either acute or repetitive microtrauma;
neurogenic due to nerve entrapment such as thoracic outlet, carpal or tarsal tunnel
syndromes; occlusive arterial disease such as thromboangitis obliterans, arteriosclerosis
obliterans, or status-post arterial thrombosis or embolism; thermal injury such as trench
foot (cold and wet); or for miscellaneous conditions such as scleroderma, lupus
erythematosus, RA, dermatomyositis, Fabry's disease, cryoglobulinemia (as in multiple
myeloma or chronic leukemia). hemoglobinuria, myxedema, neoplastic disease, hepatitis B,
pheochromocytoma, and ergotism, Treatment consists of protection, maintaining warmth,
53 Ch.3 Selected Diseases and Pathological Conditions
use of vasodilators (Procardia, alpha-adrenergic blocking prazosin, norepinephrine
depleting methyldopa, and reserpine), topical nitroglycerine and antibiotics.
Frostbite and Cold Injury
Frostbite implies freezing of the skin. Superficial frostbite is also termed chilblains, and is a
mild cold injury.
Classifications offrostbite
1st degree (chilblainsl- skin frozen, no blisters
2nd degree - skin frozen, blisters formed
3rd degree - skin frozen and necrotic, ulceration, subcutaneous exposure
4th degree - skin and subcutaneous tissue frozen and necrotic.
The treatment of chilblains is re-warming in 105-108" Fwhirlpool for 30 minutes, and
administer analgesic (meperidine). Blisters are left intact unless they have ruptured, wherein
they are treated as burns with cleansing debridement, Silvadene and dry sterile dressing.
The treatment of more advanced or deep frostbite is rapid rewarming in 108-110Fwater,
administer antibiotic (cefazolin). tetanus prophylaxis, and analgesic (meperidine). It is
importantto protectthe frozen part until proper thaw and care can be administered, and to
avoid thaw followed by refreeze. Post-freezing sequella include vasomotor instability and
cold hypersensitivity, paresthesia, depigmentation, hyperhidrosis, and atrophy.
Arteriosclerosis Obliterans (Atherosclerosis Obliterans. S ~ S is the primary cause
of occlusive lower extremity vascular disease, with the main lesion being atherosclerotic
plaque occlusion of the superficial femoral or femoral level arteries. It is most common in
males age 50-70 years, and more likely in patients with diabetes mellitus, hypertension.
cigarette smokers, and/or hyperlipidemia. Pathological findings include atheromatous
plaque formation, with secondary thrombosis. Symptoms include intenmittent claudication,
rest pain, cold intolerance, ulceration and gangrene, ischemic neuropathy, disuse atrophy,
joint stiffness and contracture. Aorta or iliac artery occlusion causes buttock, hip and thigh
pain; occlusion of the femoral artery and its branches causes thigh and calf pain; and
popliteal and tibial artery occlusion causes calf, ankle and foot pain. Findings include
diminished peripheral pulsation, discoloration (dependent rubor, pallor, or cyanosis),
exaggerated distal cooling, edema, atrophy, cutaneous compromise, intrinsic atrophy,
ulceration, and gangrene. The ankle-brachial index tABl, Table 3-5), toe pulse pressure and
amplitude, and TcP02 are diminished. Healing is generally anticipated if: ABI >.5, toe
pressure >40 mm Hg, TcP02 >30 mm Hg, and toe pulse amplitude >4 mm. Duplex Doppler ul-
trasound noninvasive vascular testing, magnetic resonance angiography, and perhaps an
arteriogram if surgical care warrants, can assist in the diagnosis. Treatment includes con-
trol of associated systemic disease (HTN, hyperlipidemia, anemia, arrhythmia).
avoiding cold exposure, exercise to tolerance, hemorheologic agent (pentoxifyUine,
cilostazol), antiplatelettherapy{aspirin, clopidogrel, ticlopidine, dipyridamole), vasodilating
agents (a and B-adrenergic blockers, calcium channel blockers), peripheral angioplasty or
vascular reconstruction, or amputation. Operative intervention is warranted whenever
claudication, rest pain, or non-helaing wound is present Peripheral arterial disease is often
associated with carotid, coronary, and renal vascular insufficiency.
54 Selected Diseases and Pathological Conditions Ch.3
TABLE 3-5. ANKLE-BRACHIAL INDEX (ABI) CATEGORIES.*
Ratio Category
20.96 Normal
0.81-0.95 Mild obstruction
0.051-0.8 Moderate obstruction
::;0.05 Severe obstruction
* Misleading, elevated ratios may be observed in cases of noncompressible arteries.
Thromboangiitis Obliterans (TAO, Buerger's Disease)
TAO is a segmental inflammatory, obliterative disease of medium sized arteries and veins
(posterior tibial), most common inthe lower extremities of males who smoke cigarettes, the
cause of which is unknown. TAO results in gangrene. Treatment involves arresting
progression of the disease by avoiding tobacco products, administering anticoagulants and
corticosteroids; followed by effecting vasodialation with Procardia or other agents; and
surgical management of gangrenous wounds.
Monckeberg's Medial Calcific Sclerosis
This is aform of non-atheromatous degenerative arterial disease observed in middle-age
to elderly males. There is fine calcification of the tunica media, which may lead to a
non-compressible vessel. and effect a misleadingly high ankle/arm index. This occurs in
the aorta and other large vessels.
Venous Thrombosis and Pulmonary Embolism-the deep veins of the lower extremity
include the plantar arch, posterior tibial. peroneal, anterior tibial. sural. popliteal. superficial
femoral, and deep femoral. Venous thrombosis, particularly of the deep system at or above
the popliteal fossa, is associated with pulmonary embolism (PEl. and for this reason can be
fatal or extremely morbid. Predisposing factors for venous thrombosis include congestive
heart failure, malignancy, trauma, surgery, pregnancy, and thrombocytosis. Other risk
factors include cigarette smoking, oral contraceptive use, obesity, advanced age, bed rest
or confinement, and paraplegia. Deep venous thrombosis prophylaxis should be instituted
in patients at risk (Tables 3-6 and 3-7).
Lower extremity deep vein thrombophlebitis (DVT, also known as venous thromboembolism,
or VTE) presents with deep, aching pain and tightness in the calf or thigh. Pain upon active
dorsiflexion ofthe ankle, or resistance to ankle dorsiflexion is known as Homan's sign, and
is anonspecific and unreliable clinical diagnostic maneuver. Tenderness upon calf or thigh
muscle compression is amore specific testfor DVT, when associated with edema and local
increase in skin temperature. Superficial thrombophlebitis, which conveys alower likelihood
of PE, more commonly displays local heat, edema, erythema, and a palpable cord
consistent with the thrombosed vein. Application of a tourniquet above the suspected
thrombosis may cause pain at the level ofthrombosis within 30-45 seconds, and is strongly
suggestive of DVT. Comparison of calf circumference will often show enlargement of the
affected side. Constitutional findings may include temperature elevation (39.5-40.5" C), chills,
and malaise. Arterial embolism is usually more painful early on, with less swelling,
exaggerated distal temperature decrease, and early sensory deficit. Severe venous
thrombosis effecting retrograde arterial flow decrease may result in phlegmasia cerulea
dolens, which can result in pedal ischemia and gangrene. Coagulation studies are usually
55 Ch.3 Selected Diseases and Pathological Conditions
normal unless full blown disseminated intravascular coagulation (DICI, familial
antithrombin III deficiency, or lupus erythematosus clotting inhibitors exist The laboratory
diagnosis of DVT hinges on venous non-invasive duplex Doppler examination, and
magnetic resonance venography or contrast venography may be employed if ultrasound is
equivocal. Radioactive 125I-fibrinogen scanning, in conjunction with occlusion impedence
plethysmography is also asensitive combination for DVT ofthe calf. Use ofthe D-dimertest
may also be useful, however combined clinical and venographic tests are more reliable. An
accurate diagnosis of DVT is made upon identification of predisposing factors and clinical
observation, combined with duplex Doppler ultrasound and, perhaps, magnetic resonance
venogram or contrast venography.
Prevention of OVT is recommended, and can be achieved in several different ways (Tables
3-6 and 3-71. Prophylactic therapy in the low-risk patient involves mini-dose subcutaneous
administration of 5000 units of heparin every 8 or 12 hours beginning about 60 minutes
preoperatively. Adjunct physical measures include support hose, intermittent sequential
pneumatic compression of the lower extremity, leg elevation with the knee flexed, and
out-of-bed activity at an early stage after surgery. In high-risk patients, DVT prophylaxis is
administered preoperatively with mini-dose heparinization, however in the postoperative
phase, the heparin dose is adjusted upward to keep the PIT within 4 seconds of high
normal. Despite statistically more postoperative hemorrhage, this form of OVT prophylaxis
appears to be worthwhile in the high-risk patient. Abaseline platelet count is recommended
prior to mini-dose heparinization, and should be monitored periodically if it is observed to
be low. High-risk patients may also be prophylaxed with a combination of mini-dose
heparin and dihydroergotamine, which causes venular constriction and rapid venous return.
Other prophylactic combinations include heparin and antithrombin III administration, and the
use of low molecular weight heparin administered once daily has been shown to be
effective and popular (see risk stratification and guidelines for prophylaxis, below).
Coumadin, which inhibits the vitamin K-dependent clotting factors II, VII, IX, X, and proteins
Cand S, can also be administered preoperatively and during the postoperative phase to
effect DVT prophylaxis.
56 SelectedDiseasesand PathologicalGonditions Ch,3
TABLE 3-6. DVT RISK STRATIFICATION (ASSIGN POINTS BASED ON PROCEDURE,
DISEASE, AND OTHER PATIENT-RELATED FACTORS).
Risk factors
Operatingroomtime>105min
Tourniquettime>90min
Rearfootoranklesurgery
Age40-60years
Pregnancyorpostpartum<1 month
Varicoseveins
Obesity(>20Ibsoveridealbodyweight)
Diabetesmellitus
Hypertension
Hyperlipidemia
Smoker
Polycysticovarysyndrome
Immobilizedin BKorAKcastfor>lweek
Patientconfinedtobedfor>72hours
Centralvenousaccess
Age>60years
Oralcontraceptiveuse
Hormonereplacementtherapy
Inflammatoryboweldisease
Congestiveheartfailure
Ankle,pilonortibialfracture
Severesepsis/infection
Multipletrauma
Acutespinal cordinjury
Cancertreatment
CurrentlytreatedorhistoryofDVTorPE
Risk factor points assigned
2
3
5
Ch.3 SelectedDiseasesand PathologicalConditions 57
TABLE31. DVTRISKSTRATIFICATIONANDGUIDELINESFOR PROPHYLAXIS.
Risk Risk Clinical Prophylaxis
points stratum features
0 Low
<40yearsold Patienteducation
Minorsurgery Earlyambulation
<30minutes
1-2 Moderate - 40-60yearsold Patienteducation,earlyambulation,elastic
+minorsurgery stockings
- Generalanesthesia -Intermittentpneumaticcompression(if
>30minutes NWB)
- Minorsurgery Lowdoseunfractionatedheparin
+1ormoreotherrisks (5000unitssq),orlowmolecularweight
heparin(enoxaparin30mgsQ q12hoursor
40mgsq qd)
- Mechanicaltherapystarting1-2hours
beforesurgery,or12-24hourspostopif
neededtoachieveadequatehemostasis
- Continuetherapywhileinpatientorduring
initialrecovery,thendecidewhetherto
extend7-14days
3-4 High - >60 yearsold+ - Patienteducation,earlyambulation,elastic
minorsurgery+ stockings
nootherrisks -Intermittentpneumaticcompression
>40 yearsold+
(ifNWB)
minorsurgery+ - Lowdoseunfractionatedheparin
anyotherrisk (5000unitssq),orlowmolecularweight
heparin(enoxaparin30mgsq q12hoursor
40mgsq qd)
Mechanicaltherapystarting1-2hours
beforesurgery,or1224hourspostopif
neededtoachieveadequatehemostasis
Continuetherapythroughouthospitalization
andupto7-14days,thendecideduration
basedon degreeofimmobilization,ROM
andWBstatus
25 Veryhigh >PastPE,cancer Patienteducation,earlyambulation,
ormajortrauma elasticstockings
- > 40yearsold+
-Intermittentpneumaticcompression
majorsurgery+ (ifNWB)
anyotherriskfactor Lowmolecularweightheparin(enoxaparin
30mg sq q12hoursor40mgsQ qd),or
fondaparinux,oradjusteddoseheparin
- Warfarin(therapeuticwhenINR2-3)
- Starttherapy1-2hourspreop,or12-24
hourspostopifneededtoachieve
adequatehemostasis
- Continuetherapy10-14daysorentiretime
ofimmobilization
- EncourageearlyROM and/orWB
ifindicated
58 Selected Diseases and Pathological Conditions Ch.3
Treatment of DVT involves assessment of the PT and PIT, followed immediately by IV
infusion of heparin 5000-10,000 units. Thereafter, heparin is infused continuously at arate of
800-1500 units per hour, maintaining the PIT at 2-2.5 times the baseline value, and the INR
at 2.0-3.0. The patient is maintained at bed rest with the lower extremities elevated at 15
degrees to 20 degrees above the level of the heart. It takes approximately one week for
thrombi to become firmly adherent to endothelium and thereby diminish the risk of PE.
Coumadin is started as soon as longterm anticoagulation is planned, and takes 3-5 days to
become therapeutic monitoring the PT. The patient is maintained in an anticoagulated state
for 4-6 weeks for the treatment of isolated calf DVT, and for 3-6 months for more proximal
vein thrombosis. Clinical and/or venographic evidence of clot propagation indicates the
need for vascular surgical consultation regarding the potential benefits of Greenfield filter
(umbrella) placement in the inferior vena cava. Moreover, thrombolytic therapy, or
phlebectomy in rare instances, may be indicated. Postphlebitic syndrome may ensue, and
involves venous insufficiency, chronic venous stasis dermatitis, permanent calf
enlargement and predisposition to recurrent superficial and deep thrombophlebitis,
postphlebitic neuritis, and the need for indefinite use of support hose and perhaps other
physical measures.
Chronic venous insufficiency (postphlebitic syndrome, chronic venous stasis) affects the
skin and subcutaneous tissues of the legs and ankles; and may occur secondary to DVT,
varicose veins, cavernous hemangioma, congenital A-V fistula, or pelvic neoplasm
obstructing venous outflow from the lower extremity. Findings include edema, stasis
dermatitis with hyperpigmentation, eczema, induration, pain, and ulceration. Ulcerations
are usually peri-malleolar, and display sharply demarcated or "punched-out" margins (local
tissue hypertension). Squamous cell carcinoma may develop. Treatment consists of
elevation, application of an Unna-paste bandage, antibiotics as indicated, diuresis, and
protection. Consideration should be given to the potentially beneficial effects of topical
corticosteroid on inflamed, non-ulcerated skin. Atypical skin lesions should be biopsied.
Skin grafting, often in combination with vein surgery wherein varicosities are ligated or
sclerosed, and incompetent perforating veins are bypassed via direct connection of
superficial veins to deeper veins, may also be useful.
Pulmonary Embolism (PEl
PE is very common and aleading cause of death in the US. Lower extremity DVT accounts for
60-80% of PEs. Thrombi embolize from the lower extremities, traverse the pelvis and inferior
vena cava, then enter the right side of the heart, and subsequently obstruct the pulmonary
vessels. Pulmonary infarction ensues thereafter. Clinical signs and symptoms vary with the
degree of pulmonary occlusion and infarction, and include crushing chest pain, dyspnea,
tachypnea, tachycardia, low grade temperature elevation (38
0
C [101
0
Fl), neck vein
distension, ipsilateral diaphragm elevation on standard chest X-ray, a positive ventilation-
perfusion lung scan (
131
1or 51Cr), SoT segment depression (cardiac hypoxia) and other EKG
changes, arterial blood gas abnormalities such as decreased POz and PC02 and Ph, increased
serum LDH and bilirubin in the presence of normal SGOT. The differential includes acute MI
and pneumonia.
Treatmentincludes immediate anticoagulation with IV administration of 5,000-10,000 units
of heparin, followed by continuous infusion of 800-1500 units/hr while monitoring the PIT
Supportive measures include administration of 02, bed rest, and analgesia; while
59 Ch.3 Selected Diseases and Pathological Conditions
-
proceeding with definitive diagnostic measures. Thrombolytic therapy, or surgical
phlebectomy, may be indicated. Septic pulmonary emboli may be observed as a
complication of infected pelvic thrombosis, indwelling catheter, transvenous pacemaker,
arteriovenous or ventriculovenous shunts, or in cases of IV drug abuse.
Fat embolism is most common after long bone or pelvic fracture. Cerebral infarction
symptoms of restlessness, confusion, stupor and coma may accompany pulmonary
symptoms of dyspnea and tachypnea; in conjunction with fever, lipuria, and the
appearance of chest and conjunctival petechiae. The treatment of fat embolism includes
supportive measures identified previously for PE (heparin also activates lipase), in addition
to large doses of corticosteroid.
Cath81er embolism is also possible when central venous catheterization is performed.
Surgical excision is usually indicated in patients that can sustain operative intervention.
Lymphedema
Lymphedema is swelling of soft tissues due to an increased quantity of lymph, which is also
associated with increased tissue fluid found outside of the blood and lymphatic capillaries.
Primary (idiopathic) lymphedema is noted to be present at birth (congenital), seen early in life
(lymphedema praecox)' or observed late in life (lymphedema forme tarde). Congenital
lymphedema can be hereditary (Milroy's disease) or non-familial (simple congenital).
Consideration should be given to congenital or acquired hemihypertrophy. Secondary
lymphedema is of eitherthe obstructive or inflammatorytype. Obstructive lymphedema occurs
secondary to either malignant occlusion, or surgical radiation-induced disruption, of lymphatic
channels and/or nodes. Nontropical inflammatory lymphedema is highlighted by recurrent
lymphangitis and cellulitis, fever and chills, adenopathy, and is attributed most commonly to
streptococcus infection (although trichophytosis, and other microbes may be causative).
Tropical secondary lymphedema is attributed to filariasis. Chronic lymphedema may cause
fibrosis, verrucous dermatitis, ulceration, elephantiasis, and/or lymphangiosarcoma (rare).
The differential diagnosis for lymphedema includes hypothyroid myxedema, CHF, nephrotic
syndrome, and hypoproteinemia. Clinical acumen and historical interview are the mainstays
of diagnosis, and biopsy may be beneficial. Treatment should be instituted as early as
possible, and is primarily medical, although surgery may be indicated rarely. Medical treatment
consists of elevation of the edematous part, diuresis (furosemide), prophylactiC
anticoagulation with subcutaneous heparin, and observation of serum potassium. Antibiotics
may also be indicated. After initial reduction of the extremity, customized support hose
measured and fabricated for regular wear, and longterm diuresis may be maintained. If
medical therapy fails, vascular consultation regarding surgical efforts aimed at improving
lymphatic drainage or excision of edematous tissues may be entertained.
DIABETES MELUTUS
Diabetes mellitus (OM) affects about 10 million people in the US. It is a leading cause of
blindness, renal disease, PVD, peripheral neuropathy, lower extremity ulceration and
amputation, and death. In DM, the ability to oxidize carbohydrates is diminished or lost,
usually due to pancreatic dysfunction, particularly of the islets of Langerhans, with resultant
disruption of insulin function. Classification includes insulin-dependent diabetes mellitus
(100M, Type 1, juvenile-onset [although it can develop in adulthood]), and non-insulin
60 Selected Diseases and Pathological Conditions Ch.3
dependent diabetes mellitus (NIDDM, Type 2, adult-onset). IDDM is caused by autoimmune
destruction of pancreatic beta cells, and must be treated with insulin replacement NIDDM can
be divided into obese and non-obese groups, the obese group displaying the possibility of
returning to euglycemia associated with weight loss and dietary control. Gestational OM is
observed during pregnancy, and usually subsides postpartum. Findings include hyperglycemia,
polyuria, polydipsia, polyphagia, emaciation, weakness, acidosis due to dysfunctional fat
metabolism, dyspnea, ketonuria, and coma. Immunopathy accompanies long-standing
hyperglycemia. Diabetic ketoacidosis or nonketotic hyperosmolar coma may result from
prolonged or severe hyperglycemia. Diabetic retinopathy and nephropathy are the result of
small vessel diseases associated with long-standing hyperglycemia. Diabetic peripheral
neuropathy produces pain and paresthesia, pedal insensitivity, anhidrosis, vasodialation,
brittle hyperkeratosis, mal perforans ulceration, and Charcot neuroarthropathy. All patients
suspected of having OM, or previously diagnosed with the disease, should undergo pedal
monofilament esthesiometer testing to determine whether protective sensation is present.
Diabetic dermopathy creates thin, atrophic, and friable skin in the pretibial region, wounding
of which results in post-inflammatory hyperpigmentation. Necrobiosis lipoidica diabeticorum
also affects the pretibial area as an atrophic plaque with telangiectasia, and microscopically
displays palisading granuloma formation. The laboratory diagnosis of DM hinges on an
abnormal glucose tolerance test, and/or repetitively high fasting blood glucose
measurements. C-peptide assay can be used to distinguish endogenous insulin, and Type 2
DM, from exogenous insulin (administered for therapy). since exogenous insulin doe not
contain C-peptide. The GAD 65 antibody assay can also be used to distinguish Type 1from Type
2DM. Therapy includes efforts to identifythe cause, after which dietary controls and exercise
are instituted (as indicated). Patient education is acrucial part of the managementofDM. Oral
hypoglycemic agents may be used in conjunction with dietary control, and include
sulfonylureas (chlorpropamide, tolbutamide, tolazamide, and acetohexamide), as well as
metformin.lnsulin preparations are indicated when the blood glucose level is not adequately
controlled with diet and oral medication, and in cases of Type 1 DM. Adjusting the
administration of insulin requires close communication between the internist and the patient,
and often entails lifestyle alteration. In the peri-operative period, a sliding scale of insulin,
based on the blood glucose value, can be useful until aregular regimen is resumed. The goal
of therapy in the perioperative phase is to maintain plasma glucose between 150-250 mg%.
Pancreas and islet cell transplantation can also be used in an effort to cure DM.
THYROID DISEASE
Hypothalamic thyrotropin-releasing hormone stimulates pitUitary release of thyroid
stimulating hormone, which activates thyroidal uptake of iodine and production of thyroxine
(T4) and triiodothyronine (T3), which exert negative feedback inhibition of pituitary thyroid stim-
ulating hormone release. Thyroid hormones regulate metabolism. Enlargement of the
thyroid gland is referred to as agoiter, and may be associated with overactive or underactive
function. Hypothyroidism can occur due to surgical or medical (radioactive iodine) ablation,
or inflammation (Hashimoto's disease) ofthe thyroid gland; or secondary to hypothalamic or
pituitary dysfunction (tumor. CVA, trauma, other). Hypothyroidism effects myxedema, which
specifically presents as non-pitting edema, associated with facial changes that include
swelling and a thickened nose, dry or hoarse voice, dry and waxy skin, and mucinous
deposition in tissues. Hypothyroid patients display fatigue, general malaise, weight gain,
bradycardia, and may become comatose (myxedema coma) in severe disease. Thyroid
61 Ch.3 Selected Diseases and Pathological Conditions
supplementation with T4 (Synthroid) and T3 (Cytome/), or natural preparations, as well as
supportive therapy are used as indicated. Hyperthyroidism, or Grave's disease, effects
exophthalmos (lid lag), tachycardia, profuse diaphoresis, nervousness, restlessness, fine
tremors, emaciation, and psychosis. Treatment involves supportive measures and drugs that
alter hormone metabolism or the end-organ effects of the hormone. Thyroid storm is a
medical emergency wherein severe hyperthyroidism effects organ damage and death. Drugs
that inhibit hormone formation and release include thiourea derivatives that block
organification of iodine, iodide which blocks thyroid hormone synthesis, and lithium which
blocks release of thyroid hormone. Propranolol controls the peripheral manifestations of
thyroid hormone. Radioactive iodine destroys thyroid tissue, thereby decreasing thyroid
function and possibly effecting hypothyroidism (which can be treated with thyroid
supplementation).
HEPATITIS
Inflammation of the liver can be caused by trauma, toxins, autoimmune disease, and viral
infection. Liver dysfunction results in inability to detoxify a wide range of substances,
failure to produce blood elements, such as platelets, and inadequate bile production,
resulting in faulty digestion. Acute hepatitis lasts < 6 months, and can result from trauma,
vascular insult, viral infection (cytomegalovirus, Epstein-Barr, Herpes simplex, adenovirus,
hepatitis A virus [infectious jaundice, due to picornavirus], hepatitis E viruses [common
during pregnancy]), bacterial or parasitic infection (Rocky Mountain spotted fever,
Leptospira, toxoplasmosis, and Q fever), toxicity (alcohol, carbon tetrachloride, APAP,
minocycline, isoniazide, ketoconazole, methyl-dopa, nitrofurantoin, chlorambutol, penicillin,
anesthetics, mushroom toxin), collagen vascular disease (SLE), and metabolic or inherited
disorder (Wilson's disease, alpha 1-antitrypsin deficiency). Chronic hepatitis lasts
> 6 months, and can result from any of the conditions that cause acute hepatitis, if the
condition persists ortreatmentfails, orthe most common forms are related to the hepatitis
viruses B, C, and D. Hepatitis B, due to hepadenovirus, results in chronic disease in
approximately 15% ofthose infected; is transmitted via blood transfusion, sexual intercourse
or exchange of body fluids, tattooing, needle sharing, and mother-to-child via breast feed-
ing; is successfully treated (remission) in about 45% of those infected, with alpha-
interferon, pegylated interferon adefovir, entecavir, telbivudine and lamivudine; causes
cirrhosis and hepatocellular carcinoma. A vaccine exists that conveys immunity to
hepatitis Bvirus. Hepatitis C(formerly non-A non-B), due to flavivirus, often results in chronic
hepatitis that evolves to cirrhosis. Hepatitis Cis transmitted through contact with blood,
and it crosses the placenta; and it may remain inactive for 10-20 years. Hepatitis Cviral
loads can be made undetectable with a combination of interferon and ribavarin, and the
response to therapy has been shown to vary with viral genotype. There are other hepatitis
viruses, as well.
ARTHRITIDES
Rheumatoid Arthritis
Rheumatoid Arthritis (RA) is a constitutional disease with inflammatory changes through-
out the connective tissues. It is generally awasting disease with muscle and bone atrophy.
Chronic proliferative inflammation ofthe synovium exists and causes irreversible damage
to joint capsule and cartilage, which are replaced by granulation tissue. Radiographically
62 Selected Diseases and Pathological Conditions Ch.3
there is jointspace narrowing, periarticular demineralization, bone erosion, "punched out"
periarticular lesions, subluxation, deformity (arthritis mutilans), and osteoporosis. RA
primarily affects the small joints of the hands and feet, most commonly the PIPJs and
MTPJs.lt can also present in the hindfoot and ankle, with progressive metatarsal joint and
subtalar joint subluxation and ankle pes valgus. Frequently the posterosuperior process of
the calcaneus is involved.
Clinical manifestations include post-static dyskinesia (pain that is worse after periods of
immobility) and non-weight bearing, as well as stiffness. Post-static dyskinesia is a
hallmark of any type of arthritis. Pain and stiffness often subside somewhat after motion
has proceeded and the joint "warms up." Prolonged activity thereafter can lead to
worsening of pain. Constitutional symptoms of weight loss, fever, coldness, numbness,
tingling, fatigue and malaise are common. The cardinal objective findings are bilateral,
symmetrical small joint swelling (fusiform, sausage fingers and toes), tenderness to
palpation (or even barometric pressure), and pain with motion. Swelling due to synovial
hypertrophy is palpably spongy or rubbery, and often crepitant. Synovitis may lead to
effusion. Umited motion over along period is associated with muscle wasting, contracture,
fibrosis, and ankylosis. Subcutaneous rheumatoid nodules (palisading granulomas) may
form in areas of bony prominence, weight bearing or contact.
Diagnosis ofRA is based on disease characteristics overtime. Classic RA displays 7of the
following symptoms, the first 5 presenting for at least 6 weeks: morning stiffness, painful
range of motion in at least one joint, swelling in at least one joint, swelling of at least one
other joint, symmetrical joint swelling with simultaneous involvement of the same joint on
both sides of the body (except PIPJs), subcutaneous nodules, X-ray changes typical of RA
(peri-articular osteopenia, joint narrowing, bone whittling), positive agglutination test
(rheumatoid factor), poor mucin clot precipitate, characteristic histologic changes in
synovial membrane, characteristic histologic granulomatous nodules. Five of these
findings in combination represent definitive RA,3 represents probable RA. Possible RA is
represented by any 2 ofthe following for 3weeks: tenderness or pain with motion, morning
stiffness, history of joint swelling, subcutaneous nodules, elevated ESR or CRp, or iritis.
Exclusions to RA include:
1. Malar rash typical of systemic lupus erythematosus ISLE)
2. Rash typical of drug reaction
3. High concentration of lupus erythematosus (LEI cells
4. Histologic evidence of polyarteritis nodosa
5. Trunk or neck or pharyngeal weakness or swelling or dermatomyositis
6. Definite scleroderma
7. Rheumatic fever
8. Tophi or gout
9. Septic arthritis
10. Reiter's syndrome
11. Tubercle bacilli in joint
12. Shoulder-hand syndrome
13. Hypertrophic pulmonary osteodystrophy
14. Clinical picture characteristic of neuropathy
15. Homogentisic acid in urine
16. Histological evidence of sarcoidosis
17. Positive Kveim (sarcoid antigen) test
63 Ch.3 SelectedDiseases and PathologicalConditions
18. Multiplemyeloma
19. Characteristicskinlesionsoferythemanodosum
20. Leukemia orlymphoma
21. Agammaglobulinemia
Lab Testing for RA includesCBCwithslighttomoderatenormocytichypochromicanemia,
whitecountdecreasedor,inacutecases,elevated(PMNsmaybeincreasedwithleftshift!.
chronic normalto slightdecrease ESR, moderateto marked increase rheumatoid factor
(RF) withthis agglutinationtestpositive75% afterseveral monthsto ayear, normal uric
acid,alteredplasma proteins(fibrinogenandglobulinincreased,albuminandtotalprotein
and A/G ratio decreased), normal Ca++ and P04, and the synovial fluid is cloudywith
increased WBCs and decreased viscosity. The differential diagnosis includes any
polyarthriticinflammatorydiseasewithconstitutionalsignsand symptoms.
Osteoarthritis
Osteoarthritis (OA) can be idiopathic and defined as primary OA; or the result of
repetitive mechanicalstrain,and definedas secondary OA. SecondaryOAisalsotermed
degenerativejointdiseaseor"wearandtear" arthritis,and is generallynotinflammatory
beyond the confines ofthe joint. Chronic subtalarjointand metatarsophalangeal joint
hyperpronationisacommoncauseofdegenerativejointdiseaseinthefoot,withresultant
pesvalgus,forefootsupinatusandhalluxlimitus/rigidus,plantarfascitis,flexorstabilization
induced hammertoes, and medial Lisfranc breakdown. Any joint can be subject to
degenerative joint disease, particularly when subjected to weight bearing or in the
post-traumaticphase.TherearethreecardinalroentgensignsofOA,includingjointspace
narrowing,subchondral sclerosis, and osteophytosis.The classic dorsal "flag" ofhallux
rigidus (dorsal bunion!. first metatarsal-cuneiform exostosis, and the anterior tibial
exostosis are examples ofadvanced osteophytosis. Clinical manifestationsinclude PSD,
jointpainwithoutacuteinflammation,stiffness,fineand/orcoarsecrepitus,andsymptoms
thatworsen withweight-bearing activity.Although range ofmotion maybe diminished,
thereis rarelyankylosis. OA usuallyaffectsmiddle-aged orolderindividuals,with history
of insidious onset (unless post-traumatic!. with gradual progression. The differential
diagnosisincludesrheumatoid arthritis,gout,and Charcotneuroarthropathy.
GoutyArthritis
Chronichyperuricemiacanresultinmonosodiumuratecrystaldepositioninjointsandsoft
tissues.Thefourmainetiologicalformsofgoutinclude:
1. primarymetabolicgout- chronicover-productionofuricacid,oftendietaryinorigin
2. secondarymetabolic gout- myeloproliferativediseasewith high rate ofcellular
turnovercausing over-productionofuricacid
3. primaryrenalgout- under-excretionofuricaciddueto primarykidneydisease
4. secondaryrenalgout- under-excretionofuricacidduetorenaldiseaseotherthan
primarykidneylesion(certaindiureticmedications).
Serum uricacid levelsof7mg/dlformalesand6mg/dlforfemalesindicateasuper-
saturatedstatewherein crystalsmayprecipitateinjointsandthekidneys.
Clinical forms ofgouty arthritis includeacutegoutyarthritis,intercriticalorquiescent,and
chronic goutyarthritis.Acute goutyarthritispresents asmonoarticular,sudden onsetand
intenselypainfulinflammation(red, hot,swollen,excruciating pain),stiffnessand antalgic
guarding, and overlying cutaneous desquamation. Chronic gouty arthritis presents
64 SelectedDiseasesand PathologicalConditions Ch.3
insidiouslywith gradual, progressivetophusformation;intermittentacutegoutyattacks;
and is associated with indurated tophus formation (advanced monosodium urate
deposition)insubcutaneousand/ortendon,auricularhelix,andthesmalljointsofthehand
and foot; and advanced deformity (bunion, hammertoes, nodular lesions) effecting
cutaneouscompromise.Adrainingtophusrevealsawhite,chalkyexudateofmonosodium
uratecrystals.Thediagnosisofgoutisconfirmedbythepresenceofstronglybirefringent
monosodiumuratecrystalsidentifiedonjointaspiration.The presenceofaphagocytosed
monosodiumuratecrystalwithinagranulocyteispathognomonic,andtermedthe"martini
sign."Serum uricacid,whichischronicallyelevatedin chronic gout, isnormally8mg%;
howeverthe serumvalue can actuallybewithinthenormalrange duringan acute gouty
attack. Roentgen signs of acute goutyarthritisconsistprimarilyof increased softtissue
densityandvolume;whilechronicgoutyarthritisrevealspunchedoutor"ratbite"defects
ofboneatthecapsularattachment.Overtime,chronicerosionandankylosismaydevelop.
The mostcommon locationsofgoutyarthritisarethe firstMTPJ, posteriorheel atthe
Achillesinsertion,the plantarinferiorcalcaneus, otherpedal articulations(lesserMTPJ,
MTJ),the ankle;the hand,wristand elbow, and knee.The differentialdiagnosisincludes
pseudogout;suppurativearthritis,acutebursitis,andrheumatoidarthritis.
Oral therapy consistsofindomethacin50 mg Q6hoursx24hours,followedby50 mg Q8
hoursx24 hours, followed by 25 mg Q8hoursx24 hours. Alternatively, one may use
colchicine(inhibitsPMNmigration)0.5mg Q1houror1mg Q2hoursuntilthe symptoms
subside, or GI distressdevelops,oratotalof6mg has been administeredwithoutrelief.
Colchicinecanalsobeadministeredintravenouslyasaninitial2mgbolusfollowedby1mg
IVQ6hoursfortwoadditionaldoses.Insurgicalortraumatized patientswithahistoryof
acutegoutyarthritis,prophylactictherapyusingcolchicinecanbeadministeredas0.5mg
POQ B hourforoneweek.beginningtwodayspreoperatively. Patientswithhyperuricemia
requiremedicalevaluation,including24hoururineuricacidanalysis,andmaybenefitfrom
longterm anti-hyperuricemictherapy. In such patients,ifthe uric acid excretionisless
than 700 mg/24hourperiod,then probenecid sulfinpyrazone is used; and ifthe uric acid
excretionisover700mg/24hours,thenAllopurinolis usedregularlyforanindefiniteperiod
oftime.
AnkylosingSpondylitis
Thecriteriaforthediagnosisofankylosingspondylitisinclude:
1. Umitedmotionoflumbarspinein anteriorandlateralflexionandextension
2. Historyofpainorpresenceofpainindorsolumbarjunctionorinlumbarspine
3. limitationofchestexpansiontooneinchorless
Definite ankylosing spondylitisis confirmed bythe presence ofbilateralsacroiliitis
associatedwithatleastone clinicalcriteria. Probableankylosingspondylitisexistsinthe
presence of bilateral sacroiliitis associated with none ofthe clinical criteria. Common
symptomsincludelowbackpain,prolongedbackstiffness,ascendingbackpain,heelpain,
peripheraljointpain,fatigue, and diminishedvision and/oreye pain. Roentgen signsvary
with duration ofthe disease. Early signs include sacroiliac joint blurring, joint space
narrowingandwidening,subchondralsclerosis,diffuseosteoporosisofspine,apophyseal
joint sclerosis, and straightening of spine. Advanced ankylosing spondylitis reveals
apophysealjointerosion,squaringofvertebrae,narroweddiscspace,vertebralcollapse,
pelvic whiskering, and pubic symphysis involvement.Terminal roentgen signs include
65 Ch.3 Selected Diseases and Pathological Conditions
intervertebral disc calcification, paravertebral ligament calcification, vertical syndesmo-
phytes, sacro-iliac jointfusion, and bamboo spine.
Reiter's Syndrome
This is a seronegative (no presence of rheumatoid factor), asymmetrical arthritis that
presents with one or more of the following: urethritis, cervicitis, dysentery, inflammatory
eye disease (iriditis), and mucocutaneous disease consisting of balanitis or oral ulceration
or keratoderma blenorrhagica. Characteristics include synovitis, symphysitis and
enthesitis; asymmetrical lower extremity arthritis with predilection for small joints of the
feet and the ankle, pericalcaneal enthesitis, knee and sacroiliac disease; bone erosion with
osteophytosis, and paravertebral ossification. Diagnostic tests suggestive of Reiter's
syndrome include negative rheumatoid factor, demonstration of HLA 8-27 in the serum,
Pekin cells in synovial fluid and neutrophilia in prostatic fluid, and unilateral sacroiliitis.
Psoriatic Arthritis
Psoriatic Arthritis is an often severe polyarthropathy that is more common in females (3:2
M:F ratio), and can affect patients of any age. Patterns of psoriatic arthritis include
polyarthritis with DIPJ involvement and nail disease, symmetrical seronegative
polyarthritis simulating rheumatoid arthritis, monoarthritis or asymmetrical oligoarthritis,
sacroiliitis and spondylitis, and arthritis mutilans. Diagnostic features include papulosqua-
mous skin lesions and nail dystrophy (pitting, onycholysis, flaking, hypertrophy, non-
suppurative paronychia); DIPJ arthritis, fusiform digital swelling (sausage toes), unilateral
sacroiliitis, simultaneous exacerbation of cutaneous psoriasis and arthritis, absence of
subcutaneous nodules, and serum negative for rheumatoid factor. Roentgen signs include
bone resorption with "pencil-in-cup" IPJ osteolysis and mineral resorption (DIPJ
involvement with erosion and expansion of base of distal phalanx with proximal osteolysis),
oligoarthritis, sacroiliitis, and spinal column involvement.
Charcot Neuroarthropathy (Neuropathic Arthropathy)
Causes of Charcot neuroarthropathy include central nervous system defect, such as syphilis
(check fluorescent Treponemal antibody if suspect this with charcot foot), syringomyelia,
meningomyelocele, post-traumatic degeneration, multiple sclerosis, and spinal cord
compression. Peripheral nervous system disorders such as Charcot-Marie-Tooth disease,
diabetic peripheral neuropathy, alcoholic peripheral neuropathy, tuberculous or
lepromatous infection, amyloidosis, pernicious anemia, and steroid-induced neuropathy.
An unusual disorder known as congenital indifference to pain can also effect neuroarthro-
pathic joint disease. Pathologically, Charcot joints have been attributed to, primarily,
autonomic denervation with loss of vasomotor tone, hyperemia, increased bone perfusion
and loss of bone mineralization. The loss of proprioception, joint relaxation and hypotonia,
recurrent microtrauma, possible major injury, resultant malalignment, cartilage fibrillation,
and subchondral plate fragmentation have also been sited as components of the
development of Charcot joint disease. Ankle equinus is a primary deforming influence in
many cases of pedal Charcot degeneration. The foot is usually warm, dry, and swollen.
Other effects of peripheral neuropathy, such as increased hyperkeratosis and keratin
stiffness, loss of sudomotor tone (anhydrosis), protective touch-pressure sensation (5.10 or
red West-Foot monofilament esthesiometer), and intrinsic muscle atrophy (intrinsic minus
foot), also contribute to pedal breakdown. Increased blood flow results in abnormal venous
pooling and edema.
66 Selected Diseases and Pathological Conditions Ch.3
TABLE 3-8. HARRIS AND BRAND CLASSIFICATION OF INSENSITIVE FOOT DEFORMITY.
Pattern Anatomical apex of pedal breakdown
I Calcaneal
II Talar
III Midtarsal
IV Lateral hindfoot (calcaneocuboid)
V Lisfranc (tarsometatarsal)
Harris and Brand have divided tarsal destruction in the insensitive foot into five
patterns. Pattern 1- Calcaneal, Pattern 11- Tatar, Pattern III - Midtarsal, Pattern IV - Lateral
hindfoot, and Pattern V - Lisfranc. As degeneration progresses, cartilage debris is
imbedded in synovium and detritic synovitis develops from deposition of cartilage and
bone fragments, and shards of bone and cartilage can migrate into soft tissue along
the extremity.
Other causes of detritic synovitis include silicone polymer degradation, osteonecrosis,
calcium pyrophosphate deposition (pseudogout). psoriatic arthritis, and osteoarthritis.
Microscopic evidence of shards of cartilage and bone in synovium is diagnostic of
Charcot joints. Extreme angular deformation of the joint leads to ligamentous and capsular
rupture, gross fracture, and progressive deformation. Treatment must encompass systemic
medical management in conjunction with local care. Non-weight bearing using bedrest,
patellar tendon bearing bracing, and total contact casting; as well as antibiotic prophylaxis
or therapy, and surgical management of cutaneous wounds and bone and joint deformity,
are all components in the coordinated treatment of Charcot neuroarthropathy. Prior to
surgery for stabilization of deformed joints and fractured bone, it is necessary to achieve a
state of quiescence. Equinus deformity is addressed, and the mainstay of surgical
reconstruction is arthrodesis in conjunction with electrical bone growth stimulation.
Fixation methods for neuroarthropathic bone include internal fixation, external fixation, and
intramedullary nailing of the tibia. Careful perioperative management is critical.
Septic Arthritis
Septic arthritis usually presents as a monoarticular, erythematous (unless vascular
compromised), lower extremity disease with the knee as the primary site of involvement.
Etiologies include contiguous spread, direct implantation, hematogenous sources, or
surgical contamination. Contiguous spread septic arthritis occurs when osteomyelitis
is present in metaphyseal or epiphyseal bone, with resultant bacterial spread into
subchondral bone leading to eventual joint infection. Hematogenous spread is common
in children, and often the result of otitis media or upper respiratory tract infections. Direct
implantation of bacteria into the joint may occur due to puncture wound. Postsurgical joint
infection is most likely when endoprosthesis are used.
Common infecting organisms include S. aureus, H. influenza, and others. Septic
arthritis correlates with patient age as follows: S. aureus is the most common organism in
all patient populations; Streptococcus and gram negative organisms are most common in
neonates, Hemophilus influenza is most common in children 6 months to 5years of age,
Neisseria is most common in teenagers; and in adults, less than 5% of cases are caused by
coli, Proteus mirabilis, and P. aeruginosa. (P. aeruginosa is common after puncture
injuries); while sickle cell anemia patients are predisposed to Salmonella; and the
compromised host (burn wounds, drug addict, HIV positive, chemotherapy, steroid
therapy) is susceptible to Serratia marcescens. Patients with pyarthrosis present with an
67 Ch.3 Selected Diseases and Pathological Conditions
extremely painful, hot, and swollen joint that they will antalgically guard. The patient may
also exhibit varying signs of septicemia. The onset of symptoms and joint destruction are
frequently rapid and, therefore, timely diagnosis and treatment are necessary in order to
salvage the joint. The differential diagnosis in children includes acute rheumatic fever and/or
a flare up of juvenile rheumatoid arthritis. In adults consideration should be given to the
possibility of joint trauma, gout, pseudogout. or foreign body synovitis.
Useful clinical lab findings include neutrophilia with left shift, elevated ESR, positive
CRP; and blood cultures are positive in 50% of cases. Roentgen signs include increased
soft tissue density and volume, effusion and juxta-articular osteopenia. ATc-99 bone scan,
in combination with a6a-67 scan, may be helpful in making an early diagnosis, despite the
lack of specificity. An In-ll1 labeled leukocytes scan is both specific and sensitive for
infection, and may be used instead of Ga-67.
Joint aspiration should be performed when septic arthritis is considered, however
care should be taken to avoid aspiration through an area of distinct overlying cellulitis
or infection, as this technique may actually inoculate a sterile arthritic joint with bacteria.
Asterile surgical prep ofthe overlying skin is mandatory before joint aspiration is performed.
In order of importance, aspirate should undergo the following studies: C&S (aerobic and
anaerobic, and fungal), gram stain and acid-fast stain, examination for crystals, WBC count
and differential, glucose concentration. In aseptic jointthe WBC will usually be higher than
100,000, with the exception of gonococcal arthritis wherein the WBC count is usually less
than 50,000. In septic arthritis, the differential cell count consists of 90-95% neutrophils. In
additional to lab analysis, the aspirate is grossly inspected for color. consistency. and clarity.
In septic arthritis, the clarity and color will vary from cloudy yellow to creamy white or gray.
The treatment of septic arthritis is much the same as that for an abscess, wherein
incision and drainage, foreign body removal and debridement are performed. Controversy
exists as to whether or not adequate drainage and cleansing can be performed via
multiple repeated needle aspirations and lavage. This technique has also been criticized for
potential cartilage damage due to needle trauma as well as pain and anxiety related to
multiple aspirations (particularly in young patients). Open surgical joint drainage and
debridement allows for direct visualization, lysis of adhesion or scar tissue, removal of
necrotic and infected tissue, placement of drain tube, placement of antibiotic impregnated
PMMA beads if osteomyelitis is present, and thorough inspection of the joint confines.
The criticism of open drainage and debridement is that it promotes arthrofibrosis and
dysfunction due to scar formation. In a child, arthrotomy may be reserved in case of failed
drainage using multiple needle aspirations and lavage. Arthrotomy should be performed in
patients with suspected osteomyelitis, infected endoprosthesis, long-standing infection or
resistance to previous aspiration/lavage, or in the septicemic or endotoxic patient.
Following arthrotomy the wound is initially immobilized and packed open. It is
important to avoid dessication of the joint tissues, and BID wound lavage and fresh
dressing applications are used until the acute inflammatory episode subsides (24 to 48
hours},after which gentle passive range of motion should be initiated. Early motion is
critical in preventing significant arthrofibrosis and limited motion. Presumptive antibiotic
therapy should cover S. aureus (intravenous cefazolin or nafcillin, or clindamycin in
patients sensitive to peN), and any other suspected organisms based on clinical history.
Antibiotic therapy is adjusted in accordance with definitive C&S reSUlts, and should be
continued IV for aminimum of two weeks. Ifthe patient is responding well, then conversion
to oral antibiotics is made at approximately two weeks, and continued until afull antibiotic
course of four weeks is completed (oral antibiotic being administered from the second
through fourth weeks).
68 Selected Diseases and Pathological Conditions Gh.3
SELECTED NEUROLOGICAL DISORDERS
Familial Sensorimotor Polyneuropathy (Charcot-Marie-Tooth Disease)
Familial Sensorimotor Polyneuropathy is also know as Charcot-Marie-Tooth Disease (CMT)
and Peroneal Muscular Atrophy. GMT disease is a progressive, familial, symmetrical,
peripheral polyneuropathy that affects males five times more often than females, and
presents in varying degrees from mild to severe. Severe cases may display significant
cardiac dysrhythmia, Friedreich's Ataxia, and often do not survive beyond adolescence.
CMT involves distal muscle atrophy that begins in the feet and hands then legs and
arms. Lower extremity involvement is often more pronounced, and observed earlier, than is
upper extremity involvement. Classically, the peronii, tibialis anterior,long extensors, pedal
lumbricals and interossei are gradually denervated as the disease progresses, leading to
muscular atrophy and the "stork leg" or "wine goblet" appearance of the legs. Muscle
wasting effects drop foot, pes cavus (more specifically, cavo-adductovarusl. steppage gait,
recurrent lateral ankle ligamentous sprains that eventually develop into chronic instability,
claw toes and MTPJ subluxations, and mechanically induced cutaneous compromise.
Peripheral touch-pressure sensation, deep tendon reflexes, and voluntary muscle function
are diminished.
Electroneurodiagnostic testing will show markedly slowed conduction velocity
(normal conduction 45 to 55 m/sec), while EMG reveals increased fibrillation potentials.
Muscle biopsy reveals atrophy. Neurological consultation and genetic counseling are in
order. Conservative treatment is aimed at increasing stability, and includes cavus-mold
orthoses, digital retainers, ankle sleeve, drop foot bracing (MAFO or similar device), and
palliative skin and nail care.
Reconstructive surgical intervention addresses the pes cavus, digits, and drop foot; and
usually combines stabilization arthrodesis, or sometimes osteotomy, with tendon transfer.
Arthrodesis is generally preferred whenever progressive neuromuscular disease is treated.
Arthrodesis yields astable bone mass upon which the transferred tendons can function. When
heel varus is mild, the Dwyer osteotomy combined with heel cord lengthening and Steindler
stripping (release of plantar intrinsics and fascia from calcaneus) may be adequate; however
triple arthrodesis and tendon transfer from the posterior or medial leg compartment to the
dorsum of the foot (tibialis posterior through the interosseous membrane) offers more
correction and longterm improvement. Digital stabilization, in the form of lessertoe PIPJ and
hallux IPJ arthrodesis, in conjunction with MTPJ relocation, is also very useful. Consideration
may also be given to first metatarsal dorsiflexory base osteotomy.
Dejerine Sottas Disease (Hypertrophic Interstitial Polyneuropathy)
Clinically this disease is similar to CMT, with distal muscle weakness of the lower
extremities with associated sensory deficit, and decreased deep tendon reflexes. Pedal
deformities include pes cavus and claw toes, and the patient may display kyphoscoliosis.
The most distinctive feature ofthis disorder is palpable and sometimes visible enlargement
ofthe peripheral nerves. Nerve biopsy (usually sural nerve) will confirm the diagnosis.
Roussy-Levy Syndrome
Patients with this disease have been compared to patients with CMT disease, with the
addition of an essential tremor that is most prominently expressed in the hands. This is a
familial, slowly progressive, symmetrical neuromuscular disease. Clinical findings include
areflexia, intrinsic pedal muscle atrophy, pes cavus and claw toes, clumsy gait and poor
equilibrium, and the presence of the previously noted essential tremor.
69 Ch.3 SelectedDiseasesand Pathological Conditions
Refsum'sDisease
Thisdiseaseistheresultofabnormallipidmetabolismwhereinphytanicacidaccumulates
in the serum,which resultsin elevation ofserum phytanic acid to levels upto50 times
greater than normal. Associated findings include ichthyosis, night blindness, and a
preceding febrile illness. Peripheralmuscle paresis,areflexia, dropfoot,pes cavus, and
clawtoesarealsoobserved.
Friedreich'sAtaxia
ThisistypicallyamoresevereanddisablingdiseasethanCMTdisease,andtheonsetisnoted
early in life (childhood) and progresses until the patient is essentially incapacitated by
middle-age.Hallmarksofthediseaseareataxia,unstablegait,andpescavuswithclawtoes.
MuscularDystrophv(MD)
Muscle fibers atrophy and become necrotic, resulting in weakness, clinically evident
muscleatrophy(decreased girth), areflexia,and secondarymusclecontracture. Mental
impairmentmayalso bepresent.
TherearethreetypesofMD:
1. Duchenne'spseudohypertrophicMD- mostcommon,musclesappearlargeand
firm because offattyconversion, affectsonly males, and the onsetis between
1-3yearsofagewithsubsequentrapid progression
2. FacioscapulohumeralMD
3. limbgirdleMD Ankle equinus and equinovarusdeformitiesare commonfoot
conditions seen in patients with MD, although pes valgus may also appear.
ClassicallyindividualswithMD displayGauer'ssignwhentheyraisethemselves
from seated or recumbent position, where in they "climb up themselves" by
pushingtheirhands/arms againsttheirknees and thighs,therebypushingthe
torsoupward.
Myelodysplasia(SpinaBifidal
These disorderscomprise agroup ofdevelopmental deformitiesofthe spinal cord and
vertebraethatmostcommonlyaffectthelumbarandsacrallevels,andinclude:
1. spinalbifidawithmeningocele
Themeningealsacprotrudesthroughanopenneuralarchvertebraldefect
and extendstothesubcutaneouslayer.
2. spina bifidawithmyelomeningocele
Otherelementsofthespinalcord and nerverootshavealsoprotruded
3. myelocele
Eventheskinfailstoenclosethecord protrusion,resultinginthemostse-
vereformofspinabifida.
4. spinabifidaocculta
Theneuralarchesofthevertebrahavenotcompletelyclosed,howeverall
oftheneuralelementsremainwithinthespinalcanal.
Pathologically,thespinalcorddefecteffectsmotor,sensoryandautonomicfunctional
deficitsobservedinthelowerextremities.Thedynamicmuscleimbalancetendstoworsen
over time, resulting in equinus, equinovarus, and equinovalgus, and marked rotary
deformitiesofthelowerextremities.Associatedfindingsincludeurinarybladderparalysis
70 SelectedDiseasesand PathologicalConditions Ch.3
(which requires catheterization during operativeintervention)which maybe associated
with chronic urinarytract infection; and profound anesthesia and lack of protective
sensation,oftenwithmalperforansulceration.
Poliomyelitis
The polio virus affectsthe anteriorhorn cells(lowermotorneuron) ofthe spinal cord,
resulting in some degree oflowerextremityflaccid paralysis(areflexia, hypotonia,and
weakness). The central nervous system defect in poliomyelitis is non-progressive,
howeverthediseasecanleadtocontracturethatchangesovertime.Commondeformities
includeequinovalgus,andothers,andtibiocalcanealand pantalarfusioncanbeuseful.
Cerebral Palsy (CP)
Classically,acongenital neuromusculardisordercaused byan intracranialbrain lesion,
andidentifiedearlyon inthepatient'slife.
ThreetypesofCP
1. SpasticCP
Uppermotorneuron diseaseeffectshyperreflexia,clonus, and extensor
plantarresponse,typicallyanteriorlegcompartmentweakness,dropfoot,
pescavus,clawtoes,andsteppagegaitwithcircumduction.Thisisthemost
commonformofspasticCp, andaffectsapproximately65%ofCP patients.
2. AthetoidCP
Thisformaffectsapproximately20% ofpatientswithCp, andisassociatedwith
aslow,worm-likehypertoniaduetouppermotorneurondisease.
3. Ataxic CP
Ataxicaffectsabout15%ofCPpatients,andisassociatedwithtremorandatonia.
UMNdiseasecausesmorespasticityinmusclesthatcrossmorethanonejoint,such
as gastrocnemius. Musclesofflexion,adduction,andinternalrotationtendto overpower
thoseofextension,abduction,andexternalrotation.Talipesequinovalgus,orequinovarus,
iscommon.
Complex regional pain syndrome {CRPS}-Thisis aserious chronic pain condition,the
hallmark symptom being unrelenting, progressively worsening, intense pain out of
proportiontothe severityofthe injuryorinciting event. Patientswith CRPS often display
allodynia,whereintheyrelate pain caused bywhatwould have otherwise been anon-
oxious stimulus, and hyperpathia,wherein astimulusthatwouldtypicallybe considered
painfulismuchmorepainful.CRPS usuallyaffectsan arm,leg,footorhand,and the pain
may evolve to include the entire, dystonic extremity. Although CRPS affects men and
women,itismorecommoninyoungfemales.CRPSisthoughttobetheresultofperipheral
and central nervoussystem dysfunction.CRPS I,often referredto as reflexsympathetic
dystrophy syndrome (RSOS), occurs with tissue injury that does not involve direct,
underlyingnervetrauma.CRPS II,oftenreferredtoascausalgia,isassociatedwithknown
traumainvolvingaknownanatomicalnervetrunk.The clinicalsignsandsymptomsofCRPS
Iand II arethe same. Characteristic signsand symptomsincludecolorand teperature
changes involving the skin, associated with sharp and burning pain, swelling, and
sweating. Associated with these symptoms are exquisite skin sensitivity, vasomotor
instabilitythatcausestheaffectedparttobecolderorwarmerthanthecontralaterallimb,
discolorationthatincludesmottled blue,pallor,purple;texturalchangesthatincludethin,
71 Ch.3 Selected Diseases and Pathological Conditions
shiny skin; hypertrophy or atrophy of digital hair and nail growth; fusiform digital swelling and
stiffness, dystonia that affects the ipsilateral extremity and may extend to other
extremities; symptoms may be heightened by emotional stress, and depression secondary
to chronic pain is common. Although there is no definite cutoff between symptoms and
signs that define distinct stages of CRPS, many clinicians categorize Stage 1as lasting from
1-3 months and characterized by sharp, burning pain, myalgia and dystonia, temperature
and color changes, and increased hair growth. Stage 2 extends from 3-6 months and is
associated with worsening pain, edema, nail dystrophy and diminished hair growth,
muscle atrophy and weakness. Stage 3extends beyond 6months and entails irrevesible skin
and bone atrophy (Sudek's atrophy of bone), and permanent pain and limb contracture. The
pathophysiology of CRPS is notfully understood, although it is believed that the sympathetic
nervous system plays an important role in maintianing the pain, as pain receptors in the
affected limb become sensitive to catecholamines. It has also been theorized that CRPS
represents disruption of the healing process secondary to an abnormal immune response
to injury. Due to the complexity of symptoms and similarities with other conditions, the
diagnosis of CRPS can be difficult to make, especially early in the course of the disease.
There is no single diagnostic testfor CRPS, and it is importantto rule out other conditions
so that the diagnosis can be made by exclusion. AtriphasiC bone scan may be useful, and
often shows a splotchy uptake of radiotracer in cases of CRPS. Supportive therapies
include the use of topical analgesics, anticonvulsant and antidepressant medications,
corticosteroids and opiate analgesics. Physical therapy and movement are encouraged.
Sympathetic nerve blockade, using phentoloamine or local anesthetic; sugical
sympathectomy, only if blockade afforded prolonged and marked relief; spinal cord
stimulation, using an implantable generator with a stimulating electrode along the spinal
cord; and spinal intrathecal local anesthetic and/or analgesic pumps, may be useful. The
prognosis for patients with CRPS varies from person to person, and outcomes range from
permanent pain and disability to spontaneous remision and revovery.
NEOPLASMS
Any enlargement of tissue, whether edematous, hypertrophic or neoplastic, can be referred
to as a tumor. Whenever dealing with neoplasm, a high index of suspicion should be
maintained for potential malignancy. Malignancy of epidermal germ cell origin is termed
carcinoma, whereas those of mesenchymal origin are referred to as sarcoma. Any lesion,
even what is thought to be persistent pyogenic granuloma, chronic onychocryptosis,
resistant verruca, or a diffuse subcutaneous mass that does not respond to reasonable
therapy should be more closely inspected. Closer inspection may involve radiographs or
MRI, lab testing, or biopsy. Consultation may also be helpful. In general, any lesion
suspected of being malignant warrants oncological consultation and systemic evaluation
for lymph node, lung, GI, bone, and other sites of potential metastasis or regional
dissemination. Proper biopsy technique is crucial.
General considerations in the assessment of a neoplasm include coloration, change
in appearance, presence of symptoms such as pain or pruritus, hemorrhage, location
superficial (freely moveable below or within the skin) or deep (fixed) to the deep fascial
lmuscle fascia), sensory or motor disturbance, vascularity or pulsatile nature ofthe lesion,
status of the popliteal and inguinal lymph nodes (tender and/or enlarged), and the presence
of metastatic disease elsewhere in the body.
Diagnostic imaging, such as standard radiographs, MRI and CT scans may be helpful,
and a chest X-ray should be obtained whenever cancer is considered, as the lungs are the
72 Selected Diseases and Pathological Conditions Ch.3
primary site of sarcoma (and many carcinoma) metastasis. Clinical lab testing, including CBC
and differential, biochemical profile, tumor antigen testing, and ESR may be helpful.
Needle biopsy (notfine needle) can be helpful if multiple core specimens are obtained
from different sites within the lesion, and incisional biopsy through the midportion of the
soft tissue mass is routinely performed. Whenever performing an incisional biopsy for
suspected sarcoma (or carcinoma), the biopsy channel to the lesion should be oriented
longitudinally in line with the suspicious mass and within a region to be fully excised with
subsequent definitive surgical excision of the lesion. Moreover. it is important to avoid
dissection into adjacent fascial compartments, in an effort to maintain natural anatomical
barriers to spread of malignant cells. The oncological surgeon can, in many cases of
sarcoma, preserve adjacent intact muscle compartments protected by intact deep fascia,
when appropriate biopsy technique has been used. Attention to such detail may be the
difference between muscle compartment resection from the foot into the leg, versus BK or
AK amputation.
Selected Neoplasms
Epidermal (epidermoid}inclusion cyst- precipitated by skin trauma, wherein epidermis is
forced into underlying dermis and continues to desquamate and build up degenerating
keratin within the dermis. This leads to slow development of a firm, round. subcutaneous
nodule that is often seen on the sole or toes. Pilar and sebaceous cysts are inclusion cysts
around the hair follicle.
Eccrine poroma- asweat gland tumor that is nodular and may drain serous fluid.
Squamous cell carcinoma (SCC)- amalignant epithelial neoplasm with predilection for skin
and mucous membranes. The lesions display erythematous margin. nodules or shallow
ulceration. There are several variations, including verrucous carcinoma, prickle cell
carcinoma, epidermoid carcinoma, and epithelioma cuniculatum. SCC is more common in
light-skinned individuals than in African-Americans, usually localizes to sun-exposed
surface or previously scarred, burned, or irradiated skin; is usually seen in patients over
the age of 40 years, 5% affect the foot and leg, rarely invade deep to bone and rarely
metastasize, and there is a 95% cure rate with adequate excision. SCC can develop in
a chronic, non-healing wound or ulcer. Oncological consultation and possibly adjunct
radiation or chemotherapy may be in order.
Basal cell carcinoma (BCC) - the most common skin cancer, usually observed on sun-
exposed surfaces in the 30 to 50 year-old patient, more common in women,lighter- skinned
individuals, involving basal cells of the epidermis, very slow growing and unlikely to
metastasize unless ignored or neglected. It is also referred to as basal cell epithelioma due
to its failure to metastasize. Four types include superficial, pigmented, nodular, and
morpheaform. BCC has been known to form in scar tissue. Appears as ashiny nodule with
surface telangiectasia. There is a 99% cure rate with adequate excision or ablation via
cryogen, electrodesiccation, or radiotherapy. Routine follow-up is required after
eradication, and there is a35% recurrence rate within 5years.
Bowens Disease (carcinoma in situ) - an in situ squamous cell carcinoma involving skin
and mucocutaneous junctions; appearing as a crusty, nodular looking plaque. When the
superficial crust is curettaged, the lesion appears dull red and moist. It may appear as a
13 Ch.3 Selected Diseases and Pathological Conditions
keratotic lesion on the plantar surface, and pathologically the basement membrane is
intact ICA in situ). Proper excision is curative. Bowen's disease is often associated with
internal malignancy, and oncological consultation is in order.
Dennatofibroma this fibrous skin tumor rarely occurs in the foot. appears flesh-colored,
and may be observed as a periungual angiofibroma which is also referred to as Koenen's
fibroma and associated with tuberous sclerosis, cafe au lait spots and mental retardation.
Plantar fibromatosis - this is a benign and reactive lesion of fibrous tissue (plantar fascia)
affecting the plantar aspect of the foot. The lesions are firm and nodular, and may
resemble a low grade fibrosarcoma due to its fixed nature. Isolated excision is associated
with a 65% recurrence rate, and total excision of the affected band of plantar fascia is
indicated if padding and accommodative insole has failed to yield pain relief when weight
bearing. There is no distinct benefit to injection therapy. Plantar fibromatosis is also known
as Lederhaus disease, and associated with people of a Germanic heritage. These
individuals may also have Dupuytren's palmar contracture or Peronies penile fibromatosis.
Fibrosarcoma - these are firm, fixed small nodular to expansive irregular lesions that
may occur in the lower extremity. Fibrosarcoma may metastasize, and radical excision,
amputation, and oncological management are required.
Lipoma - these are composed of mature fat cells with thin capsular structures, and may
lead to adjacent nerve entrapment They are commonly observed about the malleoli and
knee, and are amenable to excision.
Uposarcoma - amalignant lesion, often with vascular infiltration and termed angiolipoma.
Treatment is excision and oncological management
Ganglion cyst- the most frequently encountered tumor affecting jointtissue, and may also
affect the tendon sheath or nerve connective tissue (usually epineurium). These are
generally of traumatic etiology (perhaps distant incidental trauma), with myxoid
degeneration of connective tissue effecting gelatinous fluid that gels over time. A history
consistent with size change and aggravation by activity is common. The ganglion may
entrap adjacent vital structures and tendon. When in the popliteal fossa, a ganglion is
referred to as a Baker's cyst. Conservative treatment consists of padding and gentle
compression, aspiration of cyst contents and local infiltration of acetate corticosteroid. Lesion
may recur after reduction in size and symptoms, and additional injection therapy or surgical
excision may be effective. Ganglions are seen in all age groups, even in the very young.
Digital mucous cysts - a small cystic lesion overlying a digitallPJ, resembling a ganglion
cyst, and observed in the 30 to 80 year age group (not typical in young individuals). The
lesion stems from myxoid degeneration of the underlying joint capsule, and treatment may
require IP arthroplasty.
Leiomyoma - awell-encapsulated, firm, rubbery-textured smooth muscle tumor arising from
erector pili or vascular smooth muscle. The treatment is usually excision or observation
overtime.
74 Selected Diseases and Pathological Conditions Ch.3
RhabdomyOl118 - a benign tumor of skeletal muscle that occurs usually in young patients.
The treatment is excision.
Rhabdomyosarcoma - a malignant tumor of skeletal muscle that occurs usually in the 5th
to 6th decade of life. The treatment is oncological consultation, adjunct radiation and/or
chemotherapy, and appropriate excision or amputation.
Giant cell tumor of tendon sheath - a true benign neoplasm of synovial structure which is
actually avariation of pigmented villonodular synovitis (PVS). It is usually seen in the 30 to
50 year age group, and isthe second most common tumor oftendon after the ganglion cyst.
Observation or excision is the recommended treatment, and it is importantto note thatthere
is a high rate (25%) of recurrence following excision.
Synovial sarcoma - this malignancy arises from joint capsule, tendon, or bursa; and is
usually seen in youngsters and adolescents, aged 10 to 40 years. The knee and ankle
predominate, and radical excision, or perhaps amputation, is indicated after oncological
consultation and consideration to adjunct radiation and/or chemotherapy. The ankle is
frequently involved with a periarticular synovial sarcoma in the periarticular soft tissues.
Unlike piezogenic papules, synovial sarcoma is present as asubcutaneous nodule even in
the non-weight bearing attitude. The tumor can be of a fibroblastic (spindle cell) or
epithelioid cell type, and tissue specific antigens can aid the pathological diagnosis. Wide
excision, sometimes in conjunction with radiation or chemotherapy, is usually indicated
after biological staging is determined.
Schwannoma - aslow-growing benign, encapsulated tumor that develops within the nerve
sheath, often of traumatic origin. The tumor causes axon compression and nerve fiber
dysfunction. Microsurgical excision under loupe magnification is the indicated treatment
Neurofibroma - a benign, circumscribed, but not encapsulated neoplasm originating in the
nerve trunk, also of Schwann cell origin. The lesions are often multiple, pedunculated, and
nontender. Consideration must be given to von Recklinghausen's disease. Neurofibromas
may undergo malignant transformation.
Hemangioma - the most common benign vascular tumor observed in the feet There are
several distinct types of hemangioma. As with most vascular lesions, they are diascopy
positive (blanch when pressure is applied to the skin surface encompassing the lesion).
The capillary, or strawberry, hemangioma is the most common form. It is observed in the
newborn and may resolve as the child matures. The cavernous hemangioma is a large
lesion consisting of athick, extensive proliferation of vessels which may involve a large
portion of the foot, and thereby pose serious surgical problems relative to excision.
Arteriography is useful in the evaluation of asuspected hemangioma.
Kaposi's sarcoma - is avascular malignancy comprised of a proliferation of capillaries and
connective tissue, seen traditionally in males over the age of 50 years, and of Mediterranean
descent There is also a high incidence in patients suffering with AIDS. The lesions are
bluish, or purple nodules or plaques. Treatment is observation (pending general medical
status) or excision.
75 Ch.3 SelectedDiseasesand Pathological Conditions
Glomus Tumor- abenign,neuro-arterialneoplasmthatisusuallylocalizedtotheperiungual
(nail bed) region,the hallmarkofwhich is extreme pain, and areddish or bluish color.
Treatmentisexcision.
Malignant Melanoma
Melanocyteshavedendriticprocessesandareofepidermalgermcellorigin.Theyfunction
toproduce"sun-protective"melaninpigmentthatguardsthe underlyinglivingcellsofthe
basal layerofthe epidermisfromthemutageniceffectsofUV radiation.Lowerextremity
melanomaismorecommoninwomen,whilemenmorecommonlydisplaymelanomaonthe
torso. Melanoma is mostcommonly seen in the 30to60year age group. Sun exposed
surfacesaremostsusceptible,howeverthepalmsandsoles,particularlyinindividualswith
darkskin,canbeaffected.Anatomicsitespronetosunexposureinclude:"BANS"(back,
arms,neck,scalp).Diagnosticsignsfocusonthesize,shape,color,location,andduration
ofthe pigmented lesion. Benignpigmented skinlesions ofthelowerextremityshould be
lessthan 5mm in diameter, homogenous in color, smooth or regular in contour, and
presentforaslongasthepatientcanremember.Plantarandperiungualpigmentedlesions
warrantan especiallyhighindexofsuspicion.Anylesiononthefootthatisgreaterthan5
mmindiameter,heterogenousincolor,ordisplayinganirregularornotchedbordershould
be biopsiedifithasnotbeenpresentsincebirth.
Melanoma grows in aradial phase and an invasiveorvertical phase.The vertical
growthphasecorrelateswithmetastasis.Melanomainthehorizontalorradialgrowthphase
appearmacular,whilethevertical growth phaseis associatedwith amore aggressive
tumor. Poorprognosticindicatorsincludelesionsdisplayingawhitishoramelanoticcolor,
tumor regression (notched border), progressive nodularity (consistent with deeper
invasionofthedermis),changeinsizeorshape,ulceration,hemorrhage,pain,orpruritus,
shouldbe consideredmalignantandtreatedafteraccurateidentification.
four Main Clincohistolgic Types
1. Superficialspreadingmelanoma (SSM)maydevelop on anyportionofthe body
withpeakincidencearoundthe 5th decade.Comprises about70% ofcutaneous
melanomas.ClassicSSMdisplaysthe"red,white,and blue"ofadvanced malig-
nancyshowingtumorregression.Theseareverycommononthetrunkofmales.
2. Lentigomalignamalignantmelanoma(LMM)istheslowestgrowinglesion,seen
onsunexposedsurfaces.LMMcomprisesabout15%ofMM,andismostcommon
intheelderly(meanage70years).Thelesionismacularwithcolorvariegation.
3. Nodularmelanoma(NM)ishighlymalignant withprimarilyaverticalgrowthphase
only. NM comprises about 12% of cutaneous melanoma, and is seen most
commonlyin males approximately50yearsofage.The appearanceis uniformly
blue,black,ordarkbrown,withanodularappearance.UlcerationisrarewithNM.
4. Acrallentiginousmelanoma (ALM)showspredilectionforplantar,palmar, and
nailbed orgrooves.Hutchinson'ssign(pigmentchangesinthe eponychium of
subungual melanomas), whereas melanotic whitlow involves subungual
melanoma. The peakincidenceofALM isthe7th decade. ALM accountsfor
about3.5% ofcutaneousmelanomas.
76 SelectedDiseasesand PathologicalConditions Ch.3
Staging
StageI
StageII
StageIII
malignantmelanoma involvesaprimarylesion,or onewith localsatellite
within5em
malignantmelanoma entailsintransitmetastasisandregionallymphnode
involvement(identifiedbypalpable adenopathyornodebiopsy)
malignantmelanoma entailsdistantmetastasis. Melanoma can go any-
whereinthebodyincludingthechoroidoftheeyeandinternalparenchyma.
The mostimportantdeterminantofsurvival rateformalignantmelanoma isclinical
staging.SurvivalofaclinicalStageIlesionisfarmorelikelythansurvivalofaclinicalStage
II lesion,whereasclinicalStageIIIlesionsareusuallylethal.
Clark's Levels and Breslow's Thickness Pathological staging systems of malignant
melanomaincludeClark'slevelsandBreslow'sthickness(Tables39and3-10).Thedeeper
the level,orthickerthe lesion,themorelikelyisthereto be metastasis,andthereforethe
prognosisworsens asthe lesion thickensorprogresses deeperintoorthrough the skin.
Identificationofthe Breslowthicknesshas been shownto correlate betterwithsurvival
rate.
TABLE3-9. CLARK'SLEVELS.
Level Microscopicappearanceofmelanoma
I Involvementofepidermiswithnoinvolvement
deeptothebasementmembrane
II Penetratesthebasementmembrane
andentersthepapillarydermis
III Fillsthepapillarydermisandcancercellsline
upagainst,butdonotpenetrateintothereticulardermis
IV Penetratesintothereticulardermis
V Fillsthereticulardermisandenters
thesubcutaneousfatlayer
TABLE3-10.BRESLOWMELANOMATHICKNESSANDCORRESPONDINGSURVIVAL.
Thickness(mm) 5-yearsurvivalrate(010)
0-0.75 83-100
0.761.5 3790
1.51 - 2.25 3783
2.26-3.0 44-72
>3.0 9-55
Themostimportantservicethepodiatristcanprovideinregardtomalignantmelanoma
is timely and accurate recognition and biopsy, thereafter followed by appropriate
consultation and/ordefinitivesurgeryorreferraltoan oncologicalsurgeon.ClinicalStage
Ilesions can be definitivelyexcised bythe podiatric surgeon,whereas ClinicalStage II
lesions,withregionallymph nodeinvolvement,require node dissectionandthe expertise
ofageneralorvascularsurgeonfamiliarwithmelanoma.
77 Ch.3 SelectedDiseasesand PathologicalConditions
Biopsyof asuspectedmalignantmelanomashouldbeperformed,whenpossible,usingan
excisionaltechniquethatprovides1to3mmofnormalappearingskinaboutthelesion,and
thebiopsymustincludesubcutaneousfat(full-thicknessskin).
Forsmalllesions,localanesthesiaisinfiltratedinaproximalV-blockfashioninnormal
appearingtissue.Twosemi-ellipticalincisionsaremadeaboutthelesionfromproximalto
distal,the resultantdimension ofthe lesion being about3:1 length:width.The proximal
normalmarginofskinshould bemarkedwithasutureforpathologicalorientation.
Forlargerlesions,where complete excisionisnotpossiblewithoutcreatingalarge
defect,incisional orpunch biopsyshould be employed. The incisional orpunch biopsy
shouldbeorientedinafashionthatwillallowthebiopsywoundtobeexcisedintotowhen
subsequentdefinitivesurgeryis performed.The incisional orpunch biopsymuststill be
full-thickness skin and include underlying subcutaneousfat. Selectthe most clinically
malignant appearing site of the lesion, and get enough of the lesion for pathological
inspection.Aswithanybiopsyofsuspectedmalignancy,timelydiagnosisand appropriate
follow-up are mandatory. Itis properto perform an incisional biopsywhen indicated,as
long asdefinitivecareissubsequentlyadministered.
Definitivetreatment,basedon clinicalandpathologicalassessment,alwaysincludes
oncological consultation prior to definitive surgical ablation of the lesion. Malignant
melanomacanbeasystemicdisease,thereforechestX-rayandconstitutionalevaluation
are needed. In many cases, it is bestto administer chemotherapy prior to definitive
surgical excision, in an efforttodecreasethetumor and minimizethe riskofmetastasis.
Survivalratesmayincreasewithadjunctpreoperative radiationorchemotherapy. Guide-
linesfordefinitiveexcisionaredepictedinTable3-11.
TABLE 311.GUIDELINES FOR DEFINITIVE EXCISION OF MELANOMA.*
Melanoma depth (mm) Recommended margin of normal
appearing skin (em)about definitive excision
<0.76 2
0.764.0 3
>4.0 5(withexcisionofunderlyingdeepfascia)
*Closuremayrequireuseofaskinflaporgraft.
Thedefinitivetreatmentofasubungualmelanomaisdigitalamputationatthelevelof
the metatarsophalangeal joint.Therapeutic lymph node dissection remains somewhat
controversialforclinicalStageIImelanoma,particularlywithlesionsofClark'sLevelIIand
III,howeverithasbeen recommendedforlesionsofClark's level II .V, andthe decision
hasto be made bytheoncologicalsurgeon afterdiscussion ofadjunctchemotherapy,
prognosisandmorbidityrelatedtoinguinalnodedissection.
BoneTumors
Radiographic Characteristics
Three common radiographic patterns of bone destruction
1. Geographic bonedestructionrepresentstheleastdestructive,slowlydevelop-
ingandusuallybenign process.There isazoneoftransitionthatseparatesthe
lesionfromnormalappearingbone.
78 SelectedDiseasesand PathologicalConditions Ch.3
2. Moth-eatenbonedestructionrepresentsamorerapidlydestructive,malignant
process such as sarcoma orosteomyelitis.The transition betweenthe lesion
and normalboneiswideandlesswell-defined.
3. Permeative bone destruction represents the most aggressive and rapidly
progressive, malignant process. The zone of transition between tumor and
normalboneisverywideandalmostimperceptibleradiographically.
Other importantradiographic characteristics of bone tumors include the type of
trabecularpattern,the periostealreaction,positionofthelesionboth relativetoanatomic
locationaswellasthetransverseplane(crosssectional)locationwithinthebone.
Trabecular patterns ofsome bone tumors
giant cell tumor ofbone - delicate,andthintrabeculae
chondromyxoid fibroma - coarse,andthicktrabeculae
aneurysmal bone cyst- delicate,and horizontal,paralleltrabeculae
non-ossifying fibroma -loculatedtrabeculae
intramedullary hemangioma striated,orradiatingtrabeculae
Periosteal patterns ofnew bone fonnation
solitary bone cyst - amonolayerofnewboneformation adjacenttothetumorand
separatedfrompre-existingcortex
osteogenic and Ewing's sarcoma - multiple,concentric layers("onionskin")ofnew
bone growth, sometimes creating aCodman's triangle wherein periosteal
elevationadjacenttopre-existingcortexradiographicallydepictsananglewith
the apexpointing inthe direction ofnormalbone(also seen in otherexpansile
lesionsofbonecortex,suchas osteomyelitis)
osteogenic sarcoma - radiating spicules,orstarburstpattern ofnewbone growth
multiplemyelomaand Ewing'ssarcoma- hair-on-endradiatingspiculesofnew
bonegrowth.
Transverse plane locations within the bone
enchondroma and solitary bone cyst - centrallylocated
giant cell tumor of bone, osteogenic sarcoma, chondrosarcoma, fibrosarcoma, and
chandromyxaid fibroma - eccentrically located within the medullary canal,
arisingtoonesideofthecentralaxisofalongbone;
nan-assifying fibroma and osteoid osteoma locatedinthecortexperiostealsarcoma
osteochondroma- lesionslocatedintheperiostealregion
Characteristic anatomic sites oftumor development
diaphyseal lesions - solitaryand aneurysmal bone cysts,giantcelltumorofbone,
Ewing's sarcoma, enchondroma, nonossifying fibroma, osteoblastoma,
eosinophilicgranuloma,andfibrousdysplasia
metaphyseal lesions - solitarybone cyst, osteogenic sarcoma, osteochondroma,
chondrosarcoma,non-ossifyingfibroma,andchondromyxoidfibroma
epiphyseal lesions chondroblastoma,intraosseousganglion cystgiantcelltumor
afterepiphysealplateclosure,andhemangioma.
79 Ch.3 Selected Diseases and Pathological Conditions
In general, malignant bone tumors radiographically display moth eaten or permeative
cortical destruction, periosteal new bone formation, and adjacent soft tissue swelling
(increased density and volume). CT scans and MRls can also be helpful in determining the
location, confines, and type oftissue involved in bone tumors. Arteriography can be useful
in determining vascular involvement, and aids in limb salvage planning when compartment
resection or amputation is considered. Laboratory findings consistent with bone tumor
formation and destruction include leukocytosis and anemia, elevated ESR, elevated serum
CaH, elevated alkaline phosphatase (osteoblastic activity), and increased total serum
protein (multiple myeloma). Definitive diagnosis is made with appropriate bone biopsy, which
may involve fine needle aspiration or, more reliably trephine plug(s) or en bloc excision of
representative bone.
Treatment ofbenign bone tumolSvaries from observation to surgical resection and repair,
depending upon symptomatology, the presence of pathological fracture, and prognosis.
The treatment of malignant bone tumors always involves oncological consultation and
management, as adjunct radiation or chemotherapy may be used in conjunction with
appropriate resection or amputation. Longterm (life-long) follow-up is arequired part ofthe
management of malignancy, regardless of tissue type.
Cartilaginous Tumors of Bone
Enchondroma - usually a well-defined, asymptomatic, centrally located medullary lesion,
seen in the 3rd to 4th decade. This tumor often appears as a lytic lesion in fingers and toes,
and pathologic fracture may occur. If pain develops, consider chondrosarcoma. Multiple
enchondromatoses are associated with Oilier's disease.
Periosteal (juxtacortical) chondroma - usually observed in children, wherein the
juxtacortical soft tissue mass erodes or saucerizes the bony cortex.
Chondroblastoma - usually observed in 15 to 30 year-old age group, commonly localized to
the calcaneus or epiphysis of a long bone, with awell-defined osteolytic appearance.
Chondromyxoid fibroma - usually observed in 2nd to 3rd decade, this lesion appears as a
sharply outlined, coarsely trabeculated, round, lytic lesion ofthe metaphysis.
Osteochondroma the most common benign growth of bone occurring anywhere in the
skeleton, typically in the 2nd to 4th decade, originating in the metaphysis, displaying a
cartilaginous cap over new bone proliferation, and rarely associated with malignant
transformation.
Chondrosarcoma a malignant cartilaginous tumor of bone. It can arise from malignant
transformation of an enchondroma, periosteal chondroma, or osteochondroma. It is rare in
children, and is usually observed in the 5th to 6th decade. It is the second most common
malignant tumor of bone, following osteogenic sarcoma. Bone destruction appears moth
eaten, with speckled medullary and soft tissue calcification (in general, soft tissue
calcification in the presence of suspected tumor is an ominous radiographic sign), and
metastasis to the lungs is common. Treatment of this lesion involves oncological
management for radiation and/or chemotherapy, as well as appropriate resection or amputation.
80 Selected Diseases and Pathological Conditions Ch.3
Bone Forming Tumors
Osteoid osteoma - usually observed in children and young adults, marked by nocturnal pain
alleviated with aspirin, displaying a round osteolytic defect surrounding a central
radiodense (sometimes lucent) nidus that is usually no larger than 1 cm in diameter. This
lesion is common in the foot.
Osteoblastoma - usually observed in 2nd to 3rd decade, larger than osteoid osteoma, more
common in males, rapidly growing, metaphyseal or diaphyseal lesion the pain of which is
not responsive to aspirin.
Osteogenic sarcoma -the most common malignant bone lesion, usually appearing in the 2nd
to 3rd decade, often affecting the metaphysis ofthe femur (40%) or tibia (16%). It is rapidly
expansile with astar burst pattern of periosteal new bone formation, cortical erosion, and
formation of Cadman's triangle. It can develop from Paget's disease of bone, which involves
haphazard new bone formation and bone resorption, effecting a "woven bone"
appearance, usually in males over the age of 40 years, and is of unknown etiology (perhaps
viral). Very high levels of serum alkaline phosphatase and urinary hydroxyproline are
observed in Paget's disease.
Connective Tissue Tumors
Non-ossifying fibroma - usually observed in the 1 stto 2nd decade, eccentrically located in
the metaphysis, with asharply demarcated, lobulated osteolytic lesion displaying asclerotic
border.
Fibrosarcoma - usually observed in the medullary canal (67%) of a long bone in a young
male, displaying osteolysis with minimal new bone formation. Speckled soft tissue
calcification may be present.
Locally Aggressive Tumor
Giantcelltumor- usually observed in the 3rd to 4th decade well after growth plates have
closed (skeletally mature), localized to the diaphysis as well as metaphysis and epiphysis
Displays thin, delicate trabeculae that have a "soap bubble" appearance, expanding into
adjacent cortex, and known to undergo malignant transformation.
Tumors of Vascular Origin
Hemangioma - usually observed in the 4th to 5th decade, occurring in any bone. Displays a
cystic lesion surrounded by a"spoke wheel" appearance of periosteal new bone formation.
Glomus tumor- usually observed in the 4th-5th decade, often very painful, localized to the
distal phalanx, and may require IPJ disarticulation.
Tumor and Tumor-Like Bone Lesions of Unknown Origin
Solitarybone cyst- these are simple, or unicameral, cystic lesions of bone, often observed
in the calcaneus or metaphyseal bone, in the 1stto 2nd decade, and contain apinkish fluid
upon aspiration. This is the most common fluid filled cystic lesion of bone.
Epidennoid cyst - usually observed in the 2nd to 4th decade, it is an isolated lytic lesion,
usually of the distal phalanx.
81 Ch.3 Selected Diseases and Pathological Conditions
Aneurysmal bone cyst- a benign, blood-filled lesion that is usually observed in the 1st to 3rd
decade. It is expansile, with horizontal, parallel trabeculae that are readily observed on
MRI. The lesion is difficultto distinguish from malignancy.
Ewing's Sarcoma - usually observed in age group 5 to 25 years. It is a highly destructive
lesion of cortical bone, with both "onion skin" and "hair-on-end" appearance. It displays a
high rate of metastasis. It is the 4th most common malignant tumor of bone, and is rare in
African-Americans. Pathological fracture is common.
Metastatic Bone Disease
Breast and prostate cancer often metastasize to bone, including the bones of the feet.
Any musculoskeletal pain in an individual with history of previous malignancy warrants
a high index of suspicion and careful examination. Leukemia, although rarely arising
primarily in the foot, may effect secondary pedal osteolytic lesions, and is associated with
leukocytosis, anemia, fatigue and malaise, adenopathy and splenomegaly.
SELECTED EMERGENCY SITUATIONS
If alife-threatening event occurs in the office setting, the local emergency medical service
(EMS) should be notified (911) immediately so thattransportto the hospital can be achieved
in atimely fashion. The patient's vital signs should be monitored and recorded throughout
the event, and medications administered during the event should be recorded. Following
emergency treatment of any medical crisis, the patient must undergo immediate systemic
medical evaluation and ongoing treatment should be provided as indicated. Medical emer-
gencies occur, and the best treatment is prevention and preparation.
Syncope
Syncope is caused by temporary cerebral anoxia, often caused by bradycardia secondary
to parasympathetic overtone. It is related to emotional stress and pain, often associated
with injection therapy. Trendelenburg positioning usually serves as adequate prevention.
Signs and symptoms include pallor, hypotension, tachycardia, mydriasis, and diaphoresis
(cool and clammy skin). Treatment consists of Trendelenburg positioning, loosening tight
clothing, cool compress to forehead, aromatic spirits of ammonia, oxygen administered at
4to 6ljmin, and monitor vital signs.
Hypersensitivity Reactions
Hypersensitivity (allergic) reactions are caused by release of histamine, with resultant
vasodilatation and increased vascular permeability, and bronchospasm. If the reaction
progresses, airway constriction, hypotension and shock may ensue. There are four major
types urticarial rash, angioneurotic edema, asthma attack and anaphylaxis.
Urticarial rash presents with wheals, hives and pruritus. Treatment involves removal ofthe
allergen, and administration of 50-75 mg diphenhydramine (Benadryl) 1M, followed by 50
mg PO q 6 h PRN.
Angioneurotic edema presents with marked mucous membrane edema resulting in swelling
of the eyelids, cheeks, lips, pharynx, and larynx. As the upper airway swells, hoarseness
and stridor (laryngospasm), wheezing (bronchospasm) and cyanosis develop. Treatment
involves withdrawal ofthe allergen, and administration of 0.2-0.5 cc epinephrine SC q 15 min
82 Selected Diseases and Pathological Conditions Ch.3
as needed, in addition to 50-75 mg diphenhydramine 1M, and 8 mg dexamethasone
(Decadron) 1M for late effects.
Asthma attack presents with wheezing due to bronchospasm, effecting dyspnea, and
initial flush then cyanosis. Treatment involves administration of 2 puffs of aerosol
bronchodilator (Ventolin, Proventil), which asthmatic patients often carry themselves, or
0.3 - 0.5 cc epinephrine 1:1,000 SC q 15 min x3, in conjunction with aerosol bronchodilator.
Anaphylaxis results in rapid respiratory and cardiovascular collapse, and requires rapid
administration of epinephrine in order to avoid a severely morbid or fatal reaction. Signs
and symptoms include laryngospasm, bronchospasm, hypotension, nausea, diaphoresis,
pruritus, urticaria and angioedema, and unconsciousness. Treatment involves withdrawal
of the allergen, Trendelenburg position, maintain airway, 02, and administer epinephrine
1:1,000 SC or sublingual 1l.3 - 0.5 cc and repeated q5-15 minutes until an adequate response
is observed, try to establish IV access. The sublingual route of administration is acceptable
when IV access is not attainable (inject into posterior ventral portion of the tongue where
it is vascularized with larger vessels). Inject .25 cc 1:1,000 epinephrine about site of
previous injection of allergen, or apply BP cuff proximal to site of allergen injection (release
every 10 to 15 minutes). If hypotension does not respond to epinephrine, administer
metaraminol (Aramine) 1l.5- 5 mg IV. If bronchospasm persists, administer aminophylline
250 mg IV over 10 min. If convulsion occurs, administer diazepam (Valium) up to 10 mg slow
IV infusion titrated until the seizure is controlled, or administer short-acting barbiturate
pentobarbital 100 mg IV . Be prepared to support and maintain respiration whenever IV
diazepam or pentobarbital are administered.
Toxic Reactions to local Anesthetics
Toxic reaction to a local anesthetic involves initial central nervous system (CNS)
stimulation due to inhibition of inhibitory neurons, resulting hypertension, tachycardia, and
skeletal muscle twitching that may progress to convulsion. Treatment consists of
administration of 02 to counter hypoxia and resist convulsion, maintain airway and, in the
office, give diazepam (Valium) 10 mg slow IV titration. Following initial CNS excitation, CNS
depression may develop as the toxic level of local anesthetic proceeds to suppress CNS
function. Pathologic findings include hypotension, weak and rapid pulse, shallow, slow
respiration, loss of speech, confusion, delirium, and coma. Treatment involves airway
maintenance and administration of 02, ephedrine 0.5 cc IV or 1M. If the reaction proceeds
to cardiovascular collapse also administer atropine 0.4 mg IV, and commence BClS and/or
AClS.lt is importantto know the toxic dose of the local anesthetic being administered. The
maximum allowable dose of local anesthetic varies with epinephrine co-administration
(Table 3-12), and readers are encouraged to be familiarwtth the toxic dosages ofthe agents
that they use.
TABLE 312. MAXIMUM I.OeAl ANESTHETIC DOSAGES.*
Local anesthetic Maximum dose (mil)
Plain With epinephrine
Lidocaine 300 500
Bupivacaine 175 225
"'In order to calculate the proper volume of local anestheitc for injection, the following mass per volume proportions
are helpful: there are 2.5 mg/ml in a0.25% solution, 5mg/ml in a0.5% solution, 10 mg/ml in a 1 %solution. and 20 mg/ml
in a2% solution.
83 Ch.3 Selected Diseases and Pathological Conditions
Hypertensive Crisis
Hypertensive crisis can develop as a result of progressive, neglected hypertension, head
injury or encephalitis, drug induced, pheochromocytoma, dissecting aortic aneurysm (will
rapidly drop if aneurysm ruptures), or associated with renal and/or heart failure. Diastolic
pressures of 130-140 mm Hg are considered emergent and require immediate treatment
with diazoxide (Hyperstat) 300 mg IV infused rapidly over 10 seconds. The patient is
transported to the hospital as soon as possible.
Hyperventilation
Hyperventilation is cased by anxiety and emotional stress, perhaps related to anticipation
of pain or injury, and results in blowing off C02 and development of respiratory alkalosis.
Signs and symptoms include rapid, shallow breathing, vertigo, confusion, paresthesia (often
affecting the forearms and hands), and carpopedal spasm. Treatment is to reassure and
have the patient rebreathe into a brown paper bag so that C02 is elevated. Sedation with 5-
10 mg of diazepam PO (or slow IV infusion) may be helpful in a prolonged event.
Seizure
Seizure can result from pre-existing seizure disorder, head trauma, encephalitis, or toxic
effect of medication, such as a local anesthetic. Signs and symptoms include aura, CNS
stimulation, and grand mal epilepsy with tonic-clonic spasms, coma, post-ictal aphasia, and
somnolence. Treatment focuses on protecting the patient from injury during the seizure and
allowing the seizure to run its course. Avoiding head injury as the patient convulses or falls is
important. If easily achieved, a padded tongue depressor may be placed in the mouth to
prevent laceration of the tongue due to jaw compression, however it is not advisable to force
anything into the mouth for fear of inducing injury (dental damage). If the patient becomes
cyanotic or the seizure fails to subside, or status epileptic us occurs (one seizure is
immediately followed by another). then administer diazepam 5-15 mg IV via slow infusion with
attention to respiratory support as indicated. Alternatively, 50 mg (2 ml of 2.5% solution) of IV
sodium thiopental may be administered. Phenytoin (Dilantin) 300 mg IV slow push may also be
administered. 02 should also be administered. The patient should thereafter be transported to
the hospital for neurological evaluation. It is important to know how well-controlled your
patients with epilepsy are, and when the patient's last seizure took place.
Insulin (Hypoglycemic) Shock
Insulin shock is caused by an acute episode of hypoglycemia or hyperinsulinism. Signs and
symptoms include anxiety, confusion, diaphoresis, tachycardia, nausea, convulsion, and
coma. Treatment consists of administration of oral glucose either as an instant glucose
preparation or via fruit juice or a candy bar. An ampule of D50 may also be administered IV
if oral administration has not resolved the crisis. Most experienced diabetic individuals
know the warning signs of hypoglycemia, and take counter-actions in a timely fashion.
Hypoglycemia may occur in a patient who was running late for a morning appointment and
failed to eat breakfast after taking their insulin.
Acute Adrenal Crisis
Acute adrenal crisis can occur as amanifestation of insufficient corticosteroid administration
in a patient who regularly takes steroids for treatment of a steroid-responsive disease, or as
the initial presentation of previously undiagnosed adrenal insufficiency (Addison's disease).
Patients on chronic, regular corticosteroid supplementation or replacementtherapy require
84 Selected Diseases and Pathological Conditions Ch.3
administration of exogenous corticosteroid in the perioperative period. These patients have
suppression or inadequate function of their hypothalamic-pituitary axis for any of avariety of
reasons, often due to the therapeutic use of corticosteroids for the treatment of rheumatoid
arthritis and other auto-immune diseases, asthma and other forms of COPD, or malignancy.
The body's own production of corticosteroid is suppressed after exogenous administration of
just7.5 mg/day of prednisone over a 7 day period.
Symptoms of adrenal insufficiency include hypotension, syncope, nausea and
vomiting. Cardiovascular collapse can develop if corticosteroid is not administered in a
timely fashion. Serum cortisol level should be drawn as soon as possible, without delaying
administration of 100 mg hydrocortisone IV, followed by 100 mg, or 15 mg/kg,lV every 8
hours. The most common complicating effects of steroid therapy, in particular chronic
steroid use, are related to inhibition of WBC function and diminished fibroplasia, both of
which negatively impact soft tissue and bone healing. In the acute postoperative period,
steroid supplementation can decrease the white count and mask infection, and also
diminish epithelialization and wound contraction. Consideration can be given to
supplementing with vitamin A to try to counter some of the detrimental affects of
corticosteroids on wound healing.
All patients requiring daily maintenance corticosteroid administration should continue
on their regular maintenance dose, and receive supplemental corticosteroid during the
perioperative period. For cases involving local anesthesia with or without IV sedation, IV
administration of 100 mg hydrocortisone 30 to SO minutes preoperative, then again
postoperative in the recovery room for cases lasting greater than one hour, is generally
adequate. Alternatively, 15 mg prednisone can be administered orally at 0600 the day of
surgery, then again at 1600 the day of surgery, and afinal supplemental dose of 15 mg orally
at 1600 on postoperative day number one. For patients undergoing general anesthesia, 100
mg hydrocortisone can be administered HS the evening before surgery, then again
preoperative prior to starting the case, and then Q 8 hours over the first 24 hours
postoperative, and continued on a Q 8 hour basis up to the second - fourth postoperative
day, depending upon the physical and mental stress of the surgery. Steroid supplementation
should be tapered down to the regular maintenance level if supplemental steroid has been
administered for more than 3days. Other supplementation regimens may be better suited for
an individual patient, and consultation with the patient's internist is helpful.
Alcohol Withdrawal
Alcohol withdrawal can occur in individuals of all walks of life, and is precipitated by
illness or injury that precludes access to ethanol. Signs and symptoms include
tremulousness, irritability, nausea, anorexia, hallucination, and seizure. These can develop
as early as 3-5 hours or up to 48 hours after the last drink. Delirium tremens is
characterized by autonomic hyperactivity resulting in hyperpyrexia, diaphoresis, and
tachycardia; in conjunction with tremulousness, hallucination, agitation, and confusion.
Delirium tremens conveys serious risk of injury and/or death. Treatment of alcohol
withdrawal consists of chlordiazepoxide (Librium) 25-100 mg PO q6h or diazepam (Valium)
5-20 mg PO q6h; observation, protection, and reassurance. Adjunct therapy for malnutrition
and social service intervention is also indicated.
Airway Obstruction
Airway obstruction is caused by a foreign body in the airway, or angioedema- induced
oropharyngeal occlusion. Signs and symptoms include choking, gagging, violent inspiratory
85 Ch.3 Selected Diseases and Pathological Conditions
effort, suprasternal notch retraction, cyanosis, respiratory arrest, and cardiac arrest.
Treatment involves establishing an airway via inspection and sweeping the oropharynx,
performance of the Heimlich maneuver, placement of an oral airway or endotracheal
intubation, or emergency cricothyrotomy. Once an airway is established, BCLS and/or ACLS
may be indicated. The patient is transported to the hospital as soon as possible.
Respiratory Arrest
Respiratory arrest is caused by airway obstruction or drug toxicity. Signs and symptoms
include apnea, cyanosis, and coma. The so-called "cardinal triad" of barbiturate toxicity or
narcotic overdose consists of apnea, miosis and coma (the patient is usually cyanotic as
well). Respiratory arrest that is not rapidly alleviated will be rapidly followed by cardiac
arrest. Even a brief period of airway obstruction or respiratory arrest in an individual with
coronary artery disease can effect angina pectoris, myocardial infarction, and/or cardiac
arrest. Respiratory arrest is treated with BCLS wherein the airway is established and
artificial respiration (rescue breathing) administered. Transport the patient to the hospital
as soon as possible.
Pulmonary Embolism (PE)
PE can cause acute, crushing chest pain and a sense of impending doom. See Venous
Thrombosis and Pulmonary Embolism
Malignant Hyperthermia
Malignant hyperthermia is a severe, adverse reaction to general anesthesia (intra-
operative) that occurs in approximately 1:20,000 patients, and displays afamilial tendency.
If there is afamily history, the CPK should be assessed preoperatively for elevation (almost
80% correlation). Amide local anesthetics should be avoided in patients with a history of
malignant hyperthermia. The reaction occurs upon exposure to inhalant anesthetic agents,
and results in hypertonicity and skeletal muscle fasciculation, jaw clenching and rigidity,
hyperpyrexia, tachycardia, tachypnea, variable blood pressure, cardiac dysrhythmia,
hyperhidrosis, cyanotic mottling of the chest and extremities, and dark blood observed in
the surgical wound.
Treatment consists of immediate cessation of anesthetic agent, hyperventilation with
100% 02 at 8-10 liters per minute, and IV bolus administration of Dantrolene sodium at 1
mg/kg up to a maximum of 10 mg/kg. The EKG is monitored and procainamide may be
administered to stabilize the myocardium. Physical measures to cool the body are
instituted to counter brain-injuring hyperpyrexia. Cooling efforts include IV administration
of cool saline, application of ice to the groin and axillae, ice water lavage of the stomach,
rectum, and bladder. Administration of sodium bicarbonate may be indicated to counter
acidosis and hyperkalemia. Kidneyfunction is maintained at 2ml/kg/hr using IV furosemide
or mannitol. Insulin may be administered to assist in providing the cells with glucose for
on-going metabolism. Following control of the acute crisis, Dantrolene sodium is
administered orally over the next 2-3 days.
Angina Pectoris
Angina pectoris is caused by coronary artery disease or obstruction. The patient usually has
a family as well as personal history of such crushing chest pain, and may already be
medicated fortheir disease. Anxiety, emotional or physical stress usually precipitate angina
pectoris, and the characteristic crushing chest pain that lasts 3to 5minutes in the presence
86 Selected Diseases and Pathological Conditions Ch.3
of stable vital signs. The pain may radiate to the left arm and wrist. The patient may also
display diaphoresis, dyspnea, nausea, and weakness. Treatment consists of administration
of 100% 02 at Bliters/minute, sublingual nitroglycerine (NTGI 1/150 tablets every 10 minutes
as needed. Loosen tight clothing, sitthe patient in semi-Fowlers position, and transport the
patient to the hospital as soon as possible.
MyocardiallnfarCfion (Mil
MI is caused by respiratory arrest or coronary artery disease, and is usually preceded by
3to 5minutes of angina pectoris with its associated signs and symptoms, as well as asense
of impending doom. Cardiac dysrhythmia may also develop. Treatment consists of
administration of 100% 02 atBliters/minute, morphine sulfate 5-10 mg IV push, or 10-15 mg
1M, while monitoring the BP and securing IV access and initiating infusion of D5W at KVO
(8 hour) rate. Preparation is made to administer BCLS or ACLS, and to transport the patient
to the hospital.
Cardiac Arrest
Cardiac arrest is caused by myocardial infarction and/or respiratory arrest. Signs and
symptoms include unresponsiveness, apnea, and absence of carotid artery pulse, and
clinical death with the pupils fixed and dilated, and facial, acral and chest cyanosis.
Treatment involves BCLS, ACLS, and transportation to the hospital as soon as the patient is
ready. The treatment protocol involves all of the interventions defined previously for MI.
BASIC CARDIAC LIFE SUPPORT
Basic Cardiac Life Support (BCLSI consists of establishment of the airway, rescue
breathing, and circulatory support with external chest compression (cardiopulmonary
resuscitation CPR).Table 3-13).
TABLE 3-13. CARDIOPULMONARY RESUSCITATION (CPR) PROTOCOLS.
Age of victim Number of rescuers Compression-fo-ventilation ratio
Adult 1 15:2
Adult 2 5:1
Child 2 5:1
Infant 2 5:1
If the required equipment and medications are available, additional support can be
administered based on the recuers' level of training and experience. The EKG is observed
in a "quick-look" fashion via the defibrillator paddles, or an Automatic External
Defibrillator reads the rhythm without visual display, and identification of a lethal
dysrhythmia warrants defibrillation in the adult at 200-360 joules delivered (2 joules /kg in a
child) for ventricular fibrillation.
ADVANCED CARDIAC LIFE SUPPORT
Advanced Cardiac Ufe Support (AClS) entails application of algorithms with a degree of
automaticity, however permutations of the algorithms may be helpful on an individualized
basis.
87 Ch.3 Selected Diseasesand PathologicalConditions
Statisticsshowthat:
the majorityofcardiac arrests occurin patientswith pre-existing coronaryartery
disease
20% ofcardiacarrestsarethefirstandlastmanifestationofthedisease
30% ofvictimshaveasecondarrestwithinoneyeariftheysurviveresuscitationbut
donotfollow-upwithtreatment
50% sufferanotherarrestwithinthesecondyearifleftuntreatedthe mostcommon
cause ofarrestisventricularfibrillation(V-fib)
1-2%ofallhospitaladmissionssuffercardiac arrestand50% areresuscitated
33%surviveatleast24hours,butonly15%survivetoleavethehospital
95% die ifthe resuscitation extendslongerthan 15minutesmostcodes are called
(terminated)after30minutesifnosignificantpositiveresponseisnoted
56%ofout-of-hospitalarrestvictimssurviveifACLSisadministeredwithin4minutes
the prognosis for survival worsens in ascending order as follows:
V-tachycardia>V-fib.>bradycardia/asystole;
CPR without appropriate drugs, such as epinephrine, is inadequate to sustain
adequateperfusionofthebrainandheart.
TheABCs(Airway.Breathe.Circulate)ofcardiopulmonaryresuscitation(CPR):
1. Identifyunresponsiveness
2. Callforhelp
3. Positionandestablishairway
4. Checkbreathing
5. Beginrescuebreathingwith2fullbreaths
6.Checkcirculationbypalpatingthecarotidpulse
7.Activateemergencymedicalservice(EMS)
8. Beginchestcompressionsaccordingtovictim'ssize/age
9.Continue basic cardiac lifesupportorimplementadvanced cardiac life support
(ACLS)and/ortransport
Airwayandventilationprotocol:
1.Heimlichmaneuver-ifobstructionissuspected,implementtheHeimlichmaneuver
2. Head back-jawthrust-thisisthe standard approachto establish unobstructed
airwaypatency
3.Rescue breathing-"mouth-to-mouth"ventilation, using appropriate protective
shield(Pocket-maskorsimilardevice)
4. Supplementaloxygen-administer90% 02at 10 liters/minutevia lineto maskor
nasalcannula
5.Ventilation-useanAmbu bag-valve-maskifairwayremainspatent
6. Endotrachealintubationorlaryngealmaskairway(LMA)insertion-resorttomore
secure airway management ifhead back-jawthrust is insufficient; consider a
nasotrachealintubationifcasesinvolvingoraltrauma
7. Spontaneousventilation-ifspontaneouslyventilating, reduceto 20-40% 02via
nasalcannula
88 Selected Diseases and Pathological Conditions Ch.3
Emergency IV access:
Une size-attempt to obtain ;>16 gauge access to facilitate administration of
emergency medications
Site-a central line is preferable to peripheral access
Number of lines-as a rule, 2 sites may be useful, especially in a prolonged
resuscitation effort
Vein options-dorsal hand or antecubital, subclavian or internal jugular vein, and
femoral vein (keep in mind, during CPR there is decreased flow inferior to the
diaphragm)
Catheter methods-Seldinger guide wire and sheath dilator, typically the easiest;
catheter-over-needle (Angiocath), catheter-through-needle (lntracath)
Cut down-as a last resort, sharp dissection to expose and catheterize either the
saphenous or axillary vein can be undertaken
The EKG and cardiac dysrhythmia:
Conduction system-sinoatrial (SA) node, atrioventricular (AV) node, bundle of His,left
and right bundle branches
Electrocardiogram-P wave =atrial depolarization, PR interval = time between atrial
and ventricular depolarization, QRS complex =ventricular depolarization
EKG and cardiac rate-each small grid square =0.04 seconds, there are 5 large
squares/second, 3 large squares approximates 90 beats per minute
EKG tracing-monitor quick-look paddles or lead-2 to determine rate, rhythm, and axis
of the dominant pacer
Dysrhythmias and cardiac life support:
Normal sinus rhythm (NSR)--range 60-100 regular beats per minute
Sinus tachycardia-response to exercise, hypovolemia, fever, anxiety,
hyperthyroidism, sympathomimetic, etc.
Sinus bradycardia-response to vagal overtone or atropine, sinoatrial node defect,
hypotension, ventricular ectopy, local anesthetic toxicity, etc. Premature atrial
contractions
(PACs)--ectopic atrial pacer cause irregular rate; response to sympathomimetic
stimulant or a-agonist, hypoxia, etc.
Atrial tachycardia and fibrillation-atrium fails to effectively contract at 400-700 beats
per minute, as does ventricle at 150-200 beats per minute; due to myocardial infarct or
other disease; requires digitalis and/or cardioversion
Junctional rhythm-AV node acts as latent pacer after 1-1.5 second delay, typically
effects rate of 40-60 beats per minute
Premature ventricular contraction (PVC)-due to ectopic ventricular focus or foci,
runs of PVCs are ominous
Ventricular tachycardia-3 or more ventricular beats, rate> 100 beats per minute
Ventricularfibrillation-this results in no cardiac output and is lethal; coarse waveform
represents recent fibrillation, whereas fine waveform indicates late fibrillation
Ventricular asystole-flat line waveform due to cessation of ventricular contraction.
Atrioventricular block-conduction blockade between the AV node and the bundle
of His, effecting wide QRS segment and decreased cardiac output)
89 Ch.4 Selected Diagnostic Techniques
SELECTED DIAGNOSTICTECHNIQUES
HISTORYAND PHYSICALEXAMINATION
The most importanttool in making an accurate diagnosis is a properly executed history and
physical examination (H&P). The astute practitioner listens to the patient. See Oral Exam Test
Taking Format for a useful H&P form.
DIAGNOSTICIMAGING
Radiation Safety
Radiation safety procedures and an understanding of the effects of ionizing radiation are
important matters for all office personnel participating in preparation of diagnostic images.
X-rays are high energy electromagnetic radiation that can effect mutation of cellular genetic
material. There is no safe dose of ionizing radiation, and therefore exposure must be limited
while maximizing the diagnostic benefit of the image. Pregnant women should not
electively be radiographed, and all subjects should wear protective lead apron, and the
examiner should use a similar apron, thyroid shield, cornea protection, and lead gloves
when manipulating the extremity under examination.
Variable factors in the imaging process include: kV (kilovoltage), mS (milliseconds),
collimation, distance between the foot (part), the film, and the X-ray source. Scatter
radiation must be minimized to reduce environmental radiation not used for creation of
diagnostic images. Fluorescent film screens are used with blue or green light sensitive films
to further decrease the amount of ionizing radiation required to obtain a useful diagnostic
image. Automatic or manual film processing requires exposure of the exposed film to
developer, fixer, and then a water rinse followed by drying. Poor quality images are
unacceptable practice, as useful diagnostic information is compromised atthe expense of
patient and environmental radiation exposure. Use of aradiation dosimetry service enables
one to accurately monitor environmental and personal exposure.
RadiographicViews
Standard pedal radiographic views are taken with the patient weight bearing, with the feet
in the angle and base of gait. This allows reproducible and reliable images, from which
standard angles and relationships can be assessed. Variations can be useful, depending
upon specific needs. The primary views of the ankle include the mortise and lateral
projections. Ankle views do not necessitate positioning the foot in the angle and base of gait.
Contralateral radiographs can be obtained for comparison, particularly when evaluating
the skeletally immature, or when concerned about secondary centers of ossification.
Oorsoplantarloot- the patient standing on film cassette, beam angled 15from vertical and
aimed atthe navicular.
Lateralfoot- the foot is positioned beside (against) the film cassette, which is vertical to the
substrate, beam angled 90from vertical and aimed at the midfoot.
Lateral oblique loot- the patient standing on film cassette, beam angled 45from vertical
and aimed atthe lateral aspect ofthe foot. Useful in assessment of the calcaneus, cuboid,
fifth metatarsal and little toe.
90 jelected Diagnostic Techniques Ch.4
Medial oblique foot - the patient standing on film cassette, beam angled 45" from vertical
and aimed atthe medial aspect ofthe foot. An unconventional view, useful in assessment
of the medial aspect of the foot the first metatarsal and hallux and, in particular, the
plantar medial border of the foot. It is also useful in evaluation of the tuberosity of the
calcaneus, as in the case of suspected plantar heel spur.
Calcaneal axial- the patient standing on film cassette, beam angled 45" to vertical and
aimed at posterior aspect of the heel. Modifications include Harris and Beath prOjections,
wherein the beam angle ranges from 10" above and 10" below the lateral view declination
angle of the posterior facet of the STJ (as determined by a scout lateral view) or, more
simply, 30, 45 and 60" from vertical. Useful in assessment of the posterior aspect of the
calcaneus, suspected calcaneal fracture or inspection of the posterior facet ofthe STJ or
the sustentaculum.
Sesamoidal or metatarsal axial- the patient standing on orthoposer with the film vertical
to the substrate, and the toes dorsiflexed against the film. The hindfoot is supported with
enough radiolucent foam to elevate the heel above the substrate, with the beam angled
from posterior-to-anterior parallel to the substrate and aimed at the metatarsal heads.
Positioning devices are available to aid in stabilizing the patient for these views.
Isherwood views - a rarely used set of three non-weight-bearing views that display the
STJs. The lateral oblique view shows the anterior facet the medial oblique view shows the
middle and posterior facets, and the lateral oblique axial view shows the posteriortacet. CT
and linear tomography are more typically used, as positioning for Isherwood views is
difficult and time consuming. Other sets of radiographic views used to image the STJs,
and generally superseded by linear and axial tomography, include Anthansen and Broden
projections.
Mottise ankle - the heel is backed against the vertical film cassette, with the foot medially
rotated 15, the beam angled parallel to the substrate and aimed at the ankle. This is the
standard view for assessment of the tibiotalar and tibiofibular joints, and the dome of the
talus and tibial bearing surface.
Lateral ankle- the medial aspect ofthe foot is positioned againstthe vertical film, the beam
angled parallel to the substrate and aimed at the ankle.
Anterior-posteriorankle -the heel is backed against the vertical film cassette, with the toes
pointing straight ahead, the beam angled parallel to the substrate and aimed atthe ankle.
The lateral malleolus is rotated posterior to and superimposed behind the tibia in this view,
and the distal tibiofibular syndesmosis is obscured. The mortise view is much more useful
for evaluation of the tibiotalar and tibiofibular joints.
Medial oblique ankle - oriented the same as in the AP or mortise ofthe ankle, however the
foot is medially rotated 45, thereby further opening the tibiofibular syndesmosis.
Lateral oblique ankle - oriented the same as the AP or mortise of the ankle, however the
foot is laterally rotated 45". May be used to assess the medial malleolar cortex and the
medial aspect of the talus.
I
91 Ch.4 Selected Diagnostic Techniques
Stress Radiography
Stress radiography can be performed with static radiographs, or dynamically under
fluoroscopic image intensification. Stress radiographs are used to identify occult fractures
and ligamentous instability, and can be used to evaluate any bone or joint in the leg, foot,
or ankle. The examiner should wear protective gloves, thyroid shield, and body apron
whenever stress films are made.
Antsriordrawerofthe ankle- with the patient supine, the lateral aspect ofthe foot is placed
against the film cassette and the heel is cupped with one hand while the opposite hand
stabilizes the anterior aspect of the tibia. The foot is rotated medially about 15, thereby
allowing visualization ofthe talar dome, while the talus is pulled forward out of the mortise.
The distance between the nearest point on the posterior aspect ofthe dome of the talus and
the most posterior margin ofthe distal tibial bearing surface is measured, and adistance of
>4mm is indicative of disruption of the anteriortalofibular ligament ATelos apparatus can
be useful for applying anterior drawer in a reproducible fashion.
Inversion anklestress (falarult) - with the patient supine, the ankle is oriented in afashion
similar to that used in the mortise view, while the tibia is stabilized medially and the talus
(hindfoot with the STJ stabilized) forced into the tibial malleolus in an effort to stress the
lateral collateral ligaments. The angle created between the plane of the distal tibial
bearing surface and the dome ofthe talus is measured. Angles <5are considered normal.
between 5-20may be normal or abnormal, and larger angles are suggestive of lateral
collateral ligament disruption. Loose bodies may be identified between the tibia and talus.
Stress ankle dorsiflexion (charger) - a weight-bearing lateral view of the ankle is taken
with the ipsilateral knee flexed and the ankle relatively dorsiflexed, This is used to depict
osseous ankle equinus.
Fluoroscopy
Fluoroscopy (image intensification) is used to obtain quick radiographic images of
operative maneuvers and stress manipulation, fracture reduction, fixation placement,
foreign body localization, and trocar or pin placement. The C-arm must be used with a
radiolucent segment in the OR table.
Computerized Axial Tomography (CT)
And Magnetic Resonance Imaging (MRI)
CT and MRI are useful imaging techniques following review of standard radiographs.
Linear tomography (non-axial linear slices) can also be useful. however it is not readily
available currently. Computerized tomography (CT) or computerized axial tomography (CAT
scan) use high-energy ionizing radiation (X-rays). multiple projections, and a computer to
generate images, and is best suited to cortical bone imaging. Magnetic resonance
imaging (MRI) uses low energy radio waves traversing the body within a magnetic field,
and a computer to generate images. T1-weighted (fat) images are dependent on the fat
content of the tissue, while T2-weighted (water, inflammation) images are dependent on
the water content of the tissue and are especially useful in the presence of pathological
inflammation or fluid accumulation. Both CT and MRI can be enhanced when combined
with contrast medium.
92 Selected Diagnostic Techniques Ch.4
Comparison of CT and MRI for Selected Pathological Conditions
Tarsal coalition - MRI is best, as not all coalitions are cortical bone
Arthritis, tendinitis, and other inflammatory processes - MRI is best, as it allows early
visualization of peri-articular and soft tissue changes
Avascular Necrosis - MRI is preferred, and the hallmark MRI sign is a well-defined
region of decreased intensity within medullary bone on both Tl- and T2-weighted
images. CT could be used to show advanced AVN wherein joint space has collapsed
with cortical bone defect
Infection - MRI is sensitive, but not specific, for imaging soft tissue abscess and
osteomyelitis (medullary). MRI does not image subcutaneous gas. CT is useful for
imaging cortical defects, sequestrum, cloaca, involucrum, and intraosseous or
subcutaneous gas.
Neoplasm - MRI is superior for evaluating bone marrow and soft tissue; while CT is
best for cortical bone, calcification, endosteal thinning, and fine periosteal reactions.
Trauma - MRI is preferred for imaging soft tissue injury, in particular tendon, ligament,
and cartilage. CT is superior for imaging cortical bone, especially when comminution
or growth plate (physeal) injury is suspected. Osteochondral lesions may warrant both
CT and MRI. When in doubt as to the preferred imaging technique, simply consult with
the radiologist.
Contrast Imaging
Contrast imaging using radiopaque contrast dye injected into ajoint space ortendon sheath
can be used to assess surface defects such as osteochondral fracture or tendon and sheath
disruption. Hypersensitivity (to the contrast medium). possible sepsis, and the invasive
nature of the procedure, the need for ionizing radiation and limitations related to patient
positioning, are all potential disadvantages of both arthrography and tenography. MRI as
well as CT scanning, despite their cost, offer excellent diagnostic images and have almost
replaced contrast imaging of the ankle and peroneal sheath. Arthroscopy and endoscopy
also offer diagnostic, and therapeutic, modalities applicable in the management ofthe foot
and ankle.
Ultrasonography
Ultrasonography can be used for localization of foreign bodies following puncture wound,
as well as identification of fluid or solid mass in the subcutaneous tissues.
Radionuclide Scans
Radionuclide scans are used to image bone physiology, and are usually performed using
technetium-99, gallium-57, or indium-lll. Most scans show increased SCintigraphy within
48-72 hours after the infection or other osteitis has begun. Tc-99 has a half-life of about 6
hours. Only the technetium scan labels hydroxyapatite crystals in living bone, and is
therefore termed "a bone scan." Ga-67 is used to label white blood cells and plasma
proteins, and is used to identifyWBC accumulation (pus, infection) in bone or other tissues.
Gallium is not used as an isolated study, and is usually combined with a Tc-99 scan
performed about 2472 hours earlier. An increased uptake of Tc-99 without increased
uptake of Ga-67, correlates 85% with the absence of osteomyelitis. If both Tc-99 and Ga-67
scans show increased uptake, then there is about a 70% correlation with osteomyelitis
being present In-lll is used to tag the patient's neutrophils, after first drawing blood and
separating the PMNs. The labeled neutrophils are then infused back into the patient, and
93 Ch.4 Selected Diagnostic Techniques
the scan performed 18 to 24 hours later. In-111 scans are positive in cases of osteomyelitis
and negative in cases of osteoarthropathy. Since In-111 is tagged to neutrophils chronic
osteomyelitis, which is primarily an accumulation of lymphocytes, may present as a false
negative indium scan (infection present despite a negative scan). An In-111 scan may be
useful in trying to distinguish postoperative infection from pseudoarthrosis or nonunion.
Bone Scans
Bone scans (Tc-99) are imaged in atriphasic fashion, wherein ascintigram is made atthree
specified times following administration of the radioisotope. The radio angiogram (first or
immediate phase, blood flow images), is measured immediately following infusion of
radionuclide and shows dynamic flow to the area. The blood pool image (second phase) is
measured about 20 minutes after infusion, and shows increased scintigraphy in the
presence of hyperemia.
The first two phases are "hot" in both bone and soft tissue infection, or other causes
of inflammation and hyperemia. The blood flow image correlates with perfusion ofthe part,
and would not show uptake of radionuclide in the presence of ischemia. The delayed image
(third phase) is measured about three hours after infusion of radionuclide, and correlates
with skeletal uptake of the isotope. The delayed image often identifies activity related to
infection or other persistent bone pathology, such as pseudoarthrosis or hypertrophic
nonunion. Moreover, longer term delayed TC-99 bone scans, imaged at 24 hours (fourth
phase), may be used to image infection in patients with PVD, diabetes mellitus and Charcot
neuroarthropathy. Neuroarthropathy may present "hot" scans in all four phases. Soft tissue
infections are usually "hot" in only the first two phases. Furthermore, aTc-99 labeled WBC
scan (Seratec) can also be used to image bone infection, particularly in patients with
diabetes mellitus or suffering postoperative infection. In any case, a scan is asensitive but
nonspecific imaging technique that must be combined with other diagnostic imaging
techniques and clinical, as well as surgical. diagnostic measures.
Standard Radionuclide Bone Imaging Combinations
Acute Osteomyelitis
Tc - 99m Scan Phase I +
Phase II ++
Phase III +++
Ga - 67 Scan Positive focal uptake
In -111 Scan Positive focal uptake
Inactive Chronic Osteomyelitis
Te - 99m Scan Phase I +/ -
Phase II +
Phase III +++ (persists in longer delayed imaging)
Ga - 67 Scan Negative
In - 111 Scan Negative
94 Selected Diagnostic Techniques Ch.4
Acute Cellulitis
Tc -99m Scan Phase I +++
Phase II ++
Phase III +
Ga 67 Scan Positive diffuse uptake
In -111 Scan Positive
Septic Arthritis
Tc - 99m Scan Phase I +++
Phase II +++
Phase III +1-
Ga - 67 Scan Positive focal uptake
In -111 Scan Positive
CARTILAGE IMAGING
Contrast arthrography-contrast agent (iodine for X-ray or CT, or gadopentetate
dimeglumine for MRI); direct pseudo-direct (via peroneal sheath to ankle joint)' indirect
methods; enhances visualization of articular cartilage margins and small cortical
abnormalities; entails need trauma, possible infection and hypersensitivity to local
anesthetic and contrast agent. High resolution delayed gadolinium-enhanced MRI of
cartilage (HR-MRI-dGEMRIC) with fat suppression is currently the best method of cartilage
imaging short of arthroscopy. The following methods are under development for clinical
use, and are currently experimental research tools that show superb cartilage detail: high
frequency ultrasound, diffraction enhanced imaging (MRI), gradient MRI, T1 rho time
relaxation MRI, T2 time relaxation MRI, optical coherence IR tomography, and positron
emission tomography (PET).
CLINICAL LABORATORY TESTING
Complete Blood Count
Complete blood count (CBC) with differential cell count is ageneral screening for avariety
of conditions. CBC includes:
Hemoglobin (Hgb)- normal range is 13.5-17 gm/l00 ml for males and 12.5-16 gm/l00 ml for
females. Values below 11 gm/100 ml are considered to represent anemia, and should be
evaluated. Elevation above 18 gm/1 00 ml may represent polycythemia, and increases blood
viscosity and increases risk of thrombosis.
Hematocrit(Hct)- normal range is 40-54% for males and 37-47% for females. Varies with the
Hgb.
Red blood cell count- normal range is 5.4 0.8 x lOS Imm3 for males and 4.8 0.6 x lOS/mm
3
for females. The RBC count increases in individuals living at high altitudes, in environmen-
tally hot work places, and in athletically fit individuals.
95 Ch.4 Selected Diagnostic Techniques
Corpuscular indices and anemia
normocytic macrocytic microcyticl
hypochromic
Mean corpuscular
volume 82-92 95-150 50-80
Mean corpuscular Hgb 25-30 30-50 12-25
Mean corpuscular 32-36 32-36 25-30
Hgb concentration
Remember the phrase "90, 30, 30," for normal MCV, MCH, and MCHC values.
Normocytic anemia can be observed with acute hemorrhage, hemolytic anemia, and
abnormal hemopoiesis. Macrocytic anemia occurs with pernicious anemia, sprue,
pregnancy, antimetabolic therapy, and other megaloblastic conditions. Microcytic anemia
occurs with iron deficiency or malabsorption, hemorrhage, and increased iron metabolism.
White bloodcell count- normal range 5,000 -10,000/ mm3. Causes of leukocytosis include:
acute infection, metabolic acidosis, gout, uremia, heavy metal toxicity, tissue necrosis or
injury (burns, gangrene, tumor, myocardial infarction, pulmonary embolism), secondary to
hemorrhage or menstruation, and myeloproliferative diseases. Causes of leukopenia
include: adverse drug reactions to Thorazine, phenylbutazone, various antifungals and
antibiotics; pernicious anemia, aplastic anemia, and certain severe infections (septic shock).
Differential white cell count - segmented neutrophils 40-60%, band neutrophils 0-5%,
lymphocytes 20-40%, monocytes 4-8%, eosinophils 1-5%, basophils 0-1 %. Some causes of
neutrophilia include acute infection, necrosis, pain, exercise or post-convulsion, anoxia,
hemorrhage, sunburn. Some causes of neutropenia include overwhelming infection,
marrow depression, antimetabolite therapy, and autoimmunity. Lymphocytosis may
indicate viral syndrome, hepatitis, chronic TB, and measles. Monocytosis occurs with
leukemia, Hodgkin's disease, collagen vascular diseases and arthritides, sarcoidosis,
subacute bacterial endocarditis, and other infections and wounds. Eosinophilia is
indicative of allergy, asthma, eczema and urticaria; parasitic infection; scarlet fever;
pemphigus and dermatitis herpetiformis; leukemia and pernicious anemia. Eosinopenia is
seen in Cushing's disease, excess ACTH, chronic steroid therapy, postoperative state,
shock, and labor. Basophilia occurs in polycythemia, chronic myelogenous leukemia,
chicken-pox, small-pox, hypothyroid myxedema, and renal disease.
Platelet count- normal range is 140,000 - 340,000 / mm3. Platelets are elevated in collagen
vascular disease, iron deficiency anemia, acute infection or injury, hepatic disease,
cardiac disease, malignancy and polycythemia Vera.
Important Labs in Rheumatoid Disease
Erythrocyte sedimentation rate (ESR) - normal anticoagulated blood shows very little
settling, however, elevated globulin and fibrinogen associated with inflammation leads to
Rouleaux formation and the clumped red cells settle rapidly. An elevated ESR is indicative
of a measurably higher column of red cells settled at the bottom of the tube within a set
time. The ESR can be used to distinguish inflammatory from non-inflammatory conditions,
and is used to monitor resolution of inflammation during the course of therapy.
96 SelectedDiagnosticTechniques Ch.4
The ESR is very sensitive, however, nonspecific. The ESR is elevated in acute
infection,rheumatoid arthritis,polyarteritis,ankylosing spondylitis,septic arthritis,acute
gout,metastasis,andotherconnectivetissuediseases.
C-reactive protein (CRP)- isaglycoproteinthatreactswithC-mucopolysaccharideofmany
pneumococci. Itis commonly produced duringthe acute phase ofinflammation.Itrises
beforetheESR.andnormalizesinthepresenceofNSAtDs,aspirinandsteroids.Itrisesin
acuteflare ofrheumatoid arthritis,Strep. infection,inthe lasthaltofpregnancy,and in
femalesusinganIUDand/ororalcontraceptives.
Antinuclear antibody (ANA) - appearsmonthsafteronsetofconnectivetissue disease,
andmayhaveitsgreatestvalueinmonitoringSLE.ltismoreaccuratethantheLEcelltest
because it is unaffected by steroids. The significance of ANA titers less than 16 is
uncertain,ashealthypersonsmaydisplaytitersinthisrange.ElevatedANAtiterssuggest
connectivetissue disease,while absentorlowtitersdo notrule outconnectivetissue
disorders. High titers are common in SLE, scleroderma, and mixed connective tissue
disorders,andRaynaud'sphenomenon.
Pattern AssociatedAntigens ClinicalConditions
Homogenous Deoxyribonucleoprotein Collagen-VascularDS
Particulated ExtractableNuclear MixedC.T. DS.,scleroderma,
Antigen SLE, Malignancy
Peripheral NativeDNAandHistones ActiveSLEwithNephritis
Nucleolar NucleolarRNA Scleroderma,Raynaud's
Positille ANA is found in the following percentages in the following diseases
Systemiclupuserythematosus (100%,hightiter)
Rheumatoid arthritis (<60%,verylowtiter)
Sjogrensyndrome (75%,lowtiter)
Systemicsclerosis (38%,lowtiter)
Livercirrhosis (45%,lowtiter)
Polymyositis (20%,lowtiter)
Dermatomyositis (20%,lowtiter)
Malignancy (18%,lowtiter)
Bullouspemphigus (rare,lowtiter)
Polyarteritisnodosaorulcerativecolitis (rare,lowtiter)
Waldenstrom'smacroglobulinemia (rare,lowtiter)
Drugreaction (rare,lowtohightiter)
Myastheniagravis (rare,verylowtiter)
Rheumatoid factor (RF) IgM or Ig6 auto-antibodiesthatreact with the Fc portion of
denatured human IgG. There are two methods of measurement latex fixation (75%
sensitive and 75% specific for RA at 1:80 dilution), and sheep cell agglutination (75%
sensitive and 95% specific for RA at 1:160 dilution). RF is found in the following
97 Ch.4 Selected DiagnosticTechniques
percentages: Sjogren syndrome (75-100%), adult RA /70-80%1. juvenile RA (10%), SLE
(20-40%1.scleroderma(5-10%),polyarteritisnodosa anddermatomyositis(0-5%).
Lupus erythematosus (tE) cell - mature polymorphonuclear neutrophil that has
phagocytosed a spherical, homogenous inclusion derived from another neutrophil.
Characteristic of SLE, and observed in the following percentages : SLE 170-80%),
Sjogren syndrome 110-20%), RA (5-10%), scleroderma and polyarteritis nodosa and
dermatomyositis(0-5%).
Serum complement - seriesofenzymatic proteinsthatcombine with antigen-antibody
complexesandeffectlysiswhentheantigenisanintactcell.Complementremainsnormal
inSjogrensyndrome,scleroderma,polyarteritisnodosa,anddermatomyositis;isnormalor
decreasedinSLE;andnormalorslightlyelevatedinacutephaseofRA.
Anti-streptolysin 0(ASO) - antibody againststreptolysin HO" of group Astreptococci
(Strep!.pyogenes).Itispresentin80-85% ofpatientswithacuterheumaticfeverorother
streptococcalinfection.
Ht-A 827- histocompatabilityantigenfound inthefonowing percentagesinthefollowing
diseases: ankylosing spondylitis (90%). Reiter's syndrome (75%). psoriatic arthritis and
juvenileRA(high concentration).
Ht-A 815- histocompatabilityantigenfoundin33% ofpatientswithSLE.
Uric acid (UA) elevatedingout,malignancy,renaldisease,andfamilial hyperuricemia.
Normal is7-9mg% in males, and slightlyless in females. UA may be normal inthe acute
stage(first10days)ofgoutyarthritis,asmuchhasprecipitatedoutoftheserumintotheaf-
fectedjoint.Monosodiumurate(gouty) crystalsare needle-shaped,andformthe"martini
sign"when phagocytosedbyaneutrophil.
Calcium pyrophosphate crystalsarerhomboid,and observed inpseudogout.
JointFluidAnalysis
JointFluid Normal Group-I Group-II Group-III
Volume Increase Increase Increase
Clarity Clear Clear Cloudy Opaque
Color Clear Yellow Yellow Yellow
Opalescent Green
Viscosity High High Low Variable
WBC/mm3< 200 200-2000 2000-100,000 >100,000
%PMNs <25% <25% >50% >75%
Culture
H
(-)
H
(+)
MucinClot Firm Firm Friable Friable
Glucose(mg%) =Serum =Serum <Serum <Serum
98 Selected DiagnosticTechniques Ch.4
Differential Diagnosis Based on the Joint Fluid Analysis Chart
Group-I: Non-inflammatory conditions such as DJD, trauma, osteochondritis
dissecans, osteochondromatosis, neuropathic hypertrophic osteo-
arthropathy (Charcot), resolving or early inflammation, hypertrophic
pulmonaryarthropathy,and pigmentedvilionodularsynovitis.
Group-II: InflammatoryconditionssuchasRA,gout,pseudogout,Reiter'ssyndrome,
ankylosingspondylitis,psoriaticarthritis,arthritisassociatedwithulcerative
colitisorCrohn's regional enteritis,rheumaticfever, SLE, and progressive
systemicsclerosis.
Group-III:Septicarthritisduetobacterialinfection.
Hemarthrosisresultsin ahemorrhagicjointfluid specimen,and can be caused by
hemophilia and otherbleeding diatheses,ligamentoustraumawith orwithoutfracture,
neuropathic arthropathy, pigmentedvillonodularsynovitis,synovioma,hemangioma,and
otherneoplasms.
CoagulationStudies
Partial thromboplastin time (PIT) - normal range is25-35 seconds. Used as areliable
screening test, howevermay not detectsubtle defects. Also used to monitorheparin
anticoagulationtherapy.The PTIcanbeusedtoevaluatethethreestagesofcoagulation,
with the exception of factor VII or platelet factors. The PTI remains normal in von
Willebrand'sdisease,plateletdysfunction,andthrombocytopenia.ThePTIisprolongedby
defectsinclottingfactorsI,ll,V.VIII, IX,X, XI. andXII.
Prothrombin time (PT)- normalrangeis11-16seconds.The PTisusedtomonitorlongterm
Coumadin (Warfarin)anticoagulationtherapy.The PTisprolongedwithdefectsinfactors
I. II,V, VII, andX; aswell asinvitamin-Kdeficiency,fatmalabsorption(steatorrhea,colitis,
jaundice),salicylateorwarfarintherapy,andadvancedhepaticdisease.
Bleeding time - normal range (Duke) is 1-4minutes.The bleeding time is prolonged in
thrombocytopenia,abnormalplateletfunction,andvonWillebrand'sdisease.
Clotting time - normalrange(Lee-White)is3-6minutesinacapillarytube,and6-17minutes
inatesttube.Thisisaroutine,nonspecificscreeningtestusedtodeterminethepresence
ofmajorclottingdeficiencies.
Urinalysis
It ispreferabletoevaluatethefirstmorningspecimen.Physicalandchemicalpropertiesare
assessed.
Color - normal is amberto paleyellow. Black urine is noted in alkaptonuria,malignant
melanoma,andmalaria.Redurineisnotedinhematuria,hemoglobinuria,methemoglobinuria,
andmyoglobinuria.Blueurinemaybenotedinporphyria.Browntogreenurinemayoccurwith
bilirubinuria.Darkbrownurineoccursinsicklecellanemia.Acidicurineappearsorange.
99 Ch.4 Selected Diagnostic Techniques
Odor- normal urine smells like ammonia. A putrid odor may indicate bacteria. Mousy urine
occurs with phenylketonuria (PKU). Asparagus effects a peculiar urine odor.
Clarity - generally the urine is relatively clear, with some sediments. Cloudy urine may
represent infection, crystaluria, hemorrhage, or cellular debris.
Specific gravity- normal range is 1.003 -1.026.
pH - normal is 4.6 - 8.0
Urine chemistries - glucose, ketones, protein, and drug by-products and metabolites can
all be measured.
Microscopic findings - blood and epithelia cells, casts, crystals, and bacteria can be
identified.
Serum Chemistries
Calcium - normal is 8.5-10.5 mg%. Elevated in primary hyperparathyroidism or secondary
to chronic renal failure, metastatic bone disease, lymphoma or multiple myeloma,
sarcoidosis; or lung or renal carcinoma that produce parathormone; or hypervitaminosis
D (excessive intake of cod liver oil), diuretic use, or acidosis. Decreased in
hypoparathyroidism, chronic renal failure (perhaps postoperative, and classically seen with
simultaneous elevation of phosphorous), malabsorption or steatorrhea, alkalosis,
pancreatitis, and when EDTA used to anticoagulate the blood specimen.
Phosphorus - normal is 2.5-4.5 mg%. Elevated in chronic renal failure, diabetic
ketoacidosis, fracture healing, acromegaly, growing children (physiological), and
hypervitaminosis D. Decreased in negative nitrogen balance (simultaneous decreased BUN
and alkaline phosphatase), hepatic disease, Fanconi syndrome, osteomalacia, and with
longterm IV glucose infusion in a non-diabetic patient.
Glucose - normal is 65-110 mg%. Elevated in diabetes mellitus (serum phosphorous remains
normal), Cushing's disease, corticosteroid administration, pheochromocytoma, and brain
injury or tumor. Decreased in hyperinsulinism, pancreatic islet cell tumor, Addison's
disease, bacterial septicemia, and advanced hepatic necrosis.
Blood urea nitrogen (BUN)- normal is 10-20 mg%. Elevated in renal failure (with or without
obstructive uropathy), dehydration, G.I. bleed. Decreased in hepatic failure (urea
production reduced), carbon tetrachloride toxicity, and associated with a negative
nitrogen balance.
Uric acid - normal is 2.5-8 mg%. Uric acid is the end-product of purine metabolism, and
may precipitate out of serum into the tissues as monosodium urate crystals, which is
responsible for acute gouty arthritis as well as chronic tophaceous gout. Elevated in
conditions where there is excessive purine intake (tyramine, cheese, dark beer, game
meats). over-production of uric acid (rapid cell proliferation as in neoplasms such as
lymphoma or leukemia; extensive tissue necrosis), or under excretion of uric acid (renal
disease), eclampsia, starvation, thiazide diuretics, lead poisoning, and metabolic acidosis.
Decreased with use of uricosuric agents, Fanconi syndrome or Wilson's disease.
100 Selected Diagnostic Techniques Ch.4
Cholesterol - normal is 150-275 mg% (this is controversial). Elevated in obstructive
jaundice, hypothyroidism, nephrosis, uncontrolled diabetes, endotoxic shock or gram
negative septicemia, and pregnancy. Decreased in malabsorption syndromes. hepatic
disease (about 2/3 of the cholesterol is esterified in the liver), hyperthyroidism, anemia,
septicemia, and chronic stress.
Albumin - normal is 3.5-5 gm%. Hyperalbuminemia is rare. Decreased in protein
malnutrition, hepatic failure, renal disease (nephrosis), 61 wasting (diarrhea) or
mal-absorption, burn wounds, or extensive exfoliative dermatitis.
Total protein - normal range is 6-8 gm%. Hyperproteinemia is typically caused by an
elevation of globulin, as in collagen vascular disease, chronic infection, or malignancy such
as multiple myeloma. Hypoproteinemia results from the same causes of hypoalbuminemia.
Note the following general formula for total protein:
3gm% globulin +4gm% albumin =7gm% total protein
Lactate dehydrogenase- normal is 90-200 mU/ml. Lactate dehydrogenase catalyzes lactic
acid t pyruvic acid in the citric acid cycle (glycolytic cycle). Increased in cytolysis and
cytonecrosis (acute myocardial, pulmonary, renal, hepatic, skeletal muscle, and major organ
infarction); pernicious anemia, malignant neoplasm, and sprue. Decreased with radiation
therapy.
Bilirubin - normal is 0.1-' mg%. Elevated in jaundice (hepatic, obstructive, or hemolytic),
Crigler-Najjar syndrome and Gilbert's disease. Hemolysis and hemorrhagic or hematoma
due to pulmonary injury or other major trauma will elevate serum bilirubin.
Alkaline phosphatase - normal is 30-85 mU/ml. Elevated in the growing individual; bone
diseases such as sarcoma, fracture healing, Paget's disease, metastatic carcinoma to bone
(usually normal in osteomalacia); other metastatic disease, histiocytosis, pulmonary
embolism, and congestive heart failure. Decreased hypophosphatasia, an inherited
condition similar to rickets however, the alkaline phosphatase and leukocyte counts are
decreased. Also decreased in magnesium deficiency, chronic diarrhea, malabsorption,
uncontrolled diabetes mellitus with magnesium deficient parenteral fluid administration,
malnutrition, and pernicious anemia.
Serum glutamic-oxaloacetic transaminase (SGOT) - normal is 10-50 mU/ml. SGOT is found
in liver> heart> skeletal muscle> kidney, pancreas, red blood cells, and lung. Elevated in
cardiac and hepatic disease (myocardial infarction,liver cancer or injury or hepatitis), acute
tubular necrosis, acute pancreatitis, hemolytic anemia, leukemia, myonecrosis or injury,
pulmonary injury or necrosis, and dermatomyositis. Decreased in conditions with elevated
serum lactate or pyruvate such as beriberi, thiamin deficiency, diabetic ketoacidosis, and
liver disease.
Serum glutamic-pyruvic transaminase (SGPT) - normal is 5-35 mU/ml. SGPT is found
primarily in the liver, and is elevated in liver disease.
Microbiological Testing
Culture and sensitivity (C&S) - used to identify micro-organisms involved in an infectious
process. Standard C&S involves aerobic and anaerobic testing. Acid fast, chocolate agar,
101 Ch.4 Selected Diagnostic Techniques
sheep's blood, fungal culture, and other specific test media may be indicated based on
individual case requirements. Sensitivity of an organism to a particular antibiotic is
determined by Kirby-Bauer disk sensitivity, wherein antibiotic impregnated disks are placed
on the culture medium surface and areas of "no growth" are observed surrounding disks
containing antibiotic that kill the bacteria. Minimal inhibitory concentration (MIC) and
minimal bactericidal concentration (MBC) are also used to test sensitivity to specific
antibiotics, wherein the inhibitory concentration stops cell growth and the cidal
concentration kills the organism.
Gram's stain - used to identify the presence of bacteria, their morphology, and staining
characteristics. Wound exudate suspected of infection should be stained as follows:
1. Gentian violet - H20 rinse
2. Alcohol- H20 rinse
3. Gram's iodine H20 rinse
4. Safranin - H20 rinse.
Microscopic observation should reveal granulocytes indicative of inflammation, and
the presence of bacteria. The combination of granulocytes and bacteria is indicative of
infection. Antibiotic selection is made based upon bacterial morphology and staining.
Gram-positive bacteria appear violet-purple (gentian violet), while gram-negative bacteria
appear red (Safranin). Interpretation of the Gram's stain is particularly important when
considering anaerobic bacteria, as it can be difficultto grow such organisms in the micro-
biology lab.
KOH prep - squamous epithelial cells are dissolved in keratinolytic potassium hydroxide,
leaving microscopically evident fungal hyphae and/or spores and yeast Also known as a
tissue exam for fungus.
PAS - periodic acid Schiff stain for fungal hyphae/spores and yeast
Acidfast staining - for suspected tuberculin infection (Mycobacterium tuberculi).
Bloodagar culture medium - for certain fastidious microbes, such as Neisseria.
Chocolate agar- predisposes to growth of Neisseria.
NEUROLOGICALAND
ELECTRONEURODIAGNOSTICEVALUATION
The basic clinical neurological examination involves sensory, motor, and autonomic testing
and observation. The exam involves touch-pressure (anterior spinothalamic tract and
peripheral sensory organs) monofilament esthesiometer testing of the skin surfaces,
wherein absence of the ability to appreciate touchpressure of 10 kg/cm2 is indicative of
lost protective sensation. Testing lighttouch with cotton or brush stroke is less reliable in
comparison to the use of the monofilaments. (Fig. 4.1)
Position sensation, proprioception, is tested atthe first MTPJ and ankle levels, wherein
the patient notes the position of the joint without looking at the part. Vibratory sensation is
tested with the 128 cycles/second tuning fork. Proprioception and vibratory sensation test
the dorsal column-medial lemniscus pathway. Pain and temperature assessment with pin
prick and awarm or cold water-filled testtube, respectively, tests the lateral spinothalamic
102 Selected Diagnostic Techniques
1. Medial and intermediate femoral cutaneous nerves
2. Posterior femoral cutaneous nerve
3. Lateral sural cutaneous nerve
4. Saphenous nerve
5. Superficial peroneal nerve
6. Sural nerve
7. Medial calcaneal branch 01 tibial nerve
8. Medial plantar nerve
9. Lateral plantar nerve
10. Deep peroneal nerve
Figure 4.1
Ch.4
pathway. Deep tendon reflexes are tested at the patellar (l2-4) and Achilles (S1-2) levels.
The reflexes are graded as
silent or absent (0)
hyporeflexic (+)
normoreflexic (++1
hyperreflexic but not necessarily pathological (3+)
mUltiple clonic contractions (4+)
sustained tonic contraction (5+)
Deep tendon reflexes test the integrity of the spinal reflex and the muscle spindle. The
plantar stroking superficial reflex should effect mild down going contraction of the toes,
whereas hallux dorsiflexion and lesser digital fanning represents the Babinski sign which
is indicative of upper motor neuron immaturity or lesion.
Skin temperature may be increased due to vasodilatation, in conjunction with dryness
due to sudomotor denervation, in the presence of peripheral neuropathy. Generally, sensory
dysfunction is noted before autonomic dysfunction, both of which precede motor
dysfunction, secondary to peripheral neuropathy, injury or nerve entrapment.
The clinical assessment of muscle strength involves inspection for atrophy or hyper-
trophy, and placing the joint acted upon by the muscle-tendon complex in the end range of
motion position, thereby providing the tendon maximum mechanical advantage and
yielding the most accurate clinical test of muscle strength. The grading system for gross
(clinical) manual muscle testing is:
Grade 5"normal" strength, full resistance at end range of motion.
103 Ch.4 Selected Diagnostic Techniques
Grade 4 "good" strength, mild-moderate resistance at end range of motion, often
graded 4+ or 4-
Grade 3 "fair" strength, able to move against gravity only
Grade 2 "poor" strength, able to move only after gravity eliminated
Grade 1 "trace" strength, can visualize or palpate contraction without joint motion
Grade 0 "zero" strength, no clinical evidence of muscle contraction
Muscle strength testing is important when considering tendon transfer. Other
techniques useful in the assessment of muscle strength include biometric testing using
machines such as Cybex or Biodex, which yield information detailing power, endurance, and
strength. Resting muscle tone is idealized to optimize synergistic muscle contractions to
effect movement.
Abnormal, Involuntary Movements
Myoclonus - rapid, abrupt, often cyclic, skeletal muscle contractions resulting in major
movement of the part.
Tremor- more refined, smooth, rhythmic movement, generally of the fingers or toes.
Athetoidmovement- slow, worm-like writhing and twisting movement associated with rest
and intentional motion.
Choreiform movement rapid, jerking movement associated with rest and intentional
motion.
Fasciculation overt twitching of bundles of muscle fiber within a larger muscle belly,
non pathologic when associated with fatigue.
During the gait cycle, biphasic contractions of TA, EHL, ED!., and Peroneus Tertius
occur during the first 10% of contact at heel strike to decelerate, then again at push
off through propulsion and into swing. The peroneii fire at about 15-20% of stance and
throughout propulsion. The FD!., TP, and FHL similarly fire at about 15-20% of stance and
throughout propulsion. A variety of abnormal gait patterns also exist, and are often
associated with specific pathological conditions, including:
Equinus -ankle plantarflexion in swing and, when advanced, stance; associated with
dropfoot, pes cavus, and extensor substitution.
Spastic/Circumducted-the lower extremity is adducted, medially rotated, and flexed atthe
hip and knee, with ankle plantarflexion; associated with cerebral palsy, cerebral vascular
accident, spinal cord lesion, familial diplegia, and other upper motor neuron lesions.
Ataxic - unstable, widened base of gaitto enhance stability, with the single limb widely
swung and then crossing the midline in stance; associated with cerebellar disease,
Friedreich's ataxia, tabes dorsalis, syringomyelia, multiple sclerosis, and diabetic
polyneuropathy.
Steppage - swing phase dropfoot requires high elevation of the thigh and leg, with hip
flexion, in order to have the forefoot clear the ground: associated with CVA, CP, familial
104 Selected Diagnostic Techniques Ch.4
sensorimotor neuropathy (GMT), Landry-Guillain-Barre syndrome, and other paralytic
dropfoot conditions.
Waddling -widened base of stance, lumbar lordosis, external hip rotation, and imbalance;
associated with muscular dystrophy (Duchenne's, Becker's, and limb-girdle), and
congenital dislocated hip.
Trendelenburg- pelvic tilt toward the swing phase side with scoliosis pointing (convexity)
toward the affected side (weight bearing); associated with gluteus medius injury or
paralysis, or dislocated hip.
Festinating - shuffling, shortened and rapid stride, seemingly falling forward, uncoordinated
arm swing, actually moving slowly; associated with Parkinson's disease and similar
conditions.
Major Patterns of Neurological Deficit
Uppermotorneuron disease - (above the anterior horn cell ofthe spinal cord) hyperreflexia,
clonus, superficial plantar response is upward with Babinski's sign, resting skeletal muscle
hypertonicity or rigidity; gait is steppage with spasticity and circumduction.
Lowermotorneuron disease- (at or below the anterior horn cell) deep tendon reflexes are
absent or hyporeflexic, muscle tone is decreased, superficial plantar response is silent; gait
is flaccid.
Ataxia -loss of coordinated skeletal muscle synergy, "drunk" appearance in gait or stance,
or inability to move the contralateral heel along the tibial crest voluntarily.
Neurological consultation, EMG, and NCV testing is usuaUy indicated when a
neurological defect is suspected or identified. Nerve conduction velocity can be measured
for sensory nerves (e.g. sural, saphenous, lateral femoral cutaneous) in an antidromic
fashion; while motor nerves (common peroneal, posterior tibial, medial and lateral plantar)
are measured from proximal to distal and tend to conduct impulses at about 40 meter/
second. Nerve injury, entrapment, or demyelinating disease can decrease nerve
conduction velocity. Electromyography depicts on an oscilloscope skeletal muscle
electrical activity associated with needle electrode insertion. Denervated muscle shows
increased fibrillation potentials. Results in the intrinsic foot musculature are variable.
VASCULAR EXAMINATION
The basic clinical vascular evaluation involves inspection of the skin color, temperature,
turgor, and digital trichosis; as well as palpation of the arterial pulse at the popliteal,
posterior tibial and dorsalis pedis levels. If indicated, arterial pulse at the perforating
peroneal. femoral, and abdominal aortic levels are also assessed. Edema is noted to be
either pitting, brawny or spongy. The skin barrier is inspected for areas of open compromise
or gangrene. Vasospastic instability may elicit livedo reticularis, while arterial insufficiency
may elicit dependent rubor associated with intermittent claudication or even rest pain.
105 Ch.4 SelectedDiagnosticTechniques
Non-Invasive Vascular Examination
The non-invasivevascularexaminationis performedwiththe duplexDopplerultrasound
machine,andcorrelatedwiththeclinicalfindings.Thenon-invasivearterialexammeasures
segmental arterial pressures and waveform analysis. Ipsilateral segmental pressure
differences indicative of a20-30 mmHg pressure drop from the proximal to the distal
segmentarestronglysuggestiveofocclusivedisease.Moreover,arterialpulsationwave-
formsshould betriphasicwith adicroticnotch,oratleastbiphasic.Monophasic Doppler
tracingsand soundsareindicativeofarterialocclusivediseasewithdecreasedflow.
Determiningtheanklesystolicpressureinvolvespneumaticcuffplacementabovethe
ankleandelevateduntilnoarterialpulsationcanbeidentifiedwiththeDopplerultrasound
overthe PT artery.The cuffisthen deflated untilthe ultrasound identifiesflowinthe PT
artery,andthepressurerecorded.Themaneuverisrepeatedwhilemeasuringtheopening
pressureintheDP artery,andthen againfortheperoneal artery.Thehighestofthethree
valuesisusedasthe"ankle"systolicpressure.Forefootanddigitalsystolicpressures,as
well as pulse volume recordings using infrared sensors on the toe pulps can also be
determined.
Transcutaneousoxygentensionandthermographyalsooffertoolsforassessmentof
pedalperfusion.Theankle/armratio(alsoknowas ankle/brachialindexorischemicindex)
iscalculated bydividingthe ankle systolic opening pressure bythe arm systolic opening
pressure.Deceptivelyhighopening pressurescanbemeasuredinthepresenceofmedial
calcificsclerosis.
Ankle/Arm Ratio Guidelines in the Non-Diabetic Patient
Ankle/Ann Ratio Clinical Finding
>0.96 Normal
0.31 - 0.95 Intermittentclaudication
0.25-0.3 RestPain
0-0.3 Impendinggangrene
Ischemic Index Guidelines for Reconstructive Surgery
Foot: Ifankle/armindex<0.75,thengenerallydonotoperate.
Ifankle/armindex>0.75,then checktoe/armindex.
If ankle/armindex>0.75andtoe/armindex<0.65,thengenerallydonotoperate.
Ifankle/armindex>0.75andtoe/armindex>0.65,thenmayoperate.
Ifcan'tgetmeasurementontoebecauseofdeformity,useforefoot/armindex.
Ifankle/arm index>0.75 andforefoot/arm index>0.65,then checkDoppler
flowofdigitalarteries.
Hallux: Ifankle/armindex>0.75,andtoe/armorforefoot/armindex>0.65andtwoof
fourdigitalarteriesidentifiedwithDoppler,thengenerallymayoperate.
LesserToe: Ifankle/armindex>0.75 and toe/arm orforefoot/armindex>0.65 and either
bothdorsalarteriesandoneplantarorboth plantararteriesidentifiedwith
Doppler,then generallymayoperate.
-------
106 Selected DiagnosticTechniques Ch.4
Invasivearterialtesting,intheformofangiographywithradiopaquecontrastmedia,
isusuallyobtainedonlyifreconstructivevascularsurgeryisbeingentertained.Infusionof
contrastmedium is notarisk-free undertaking,and conveysthe riskofhypersensitivity
reaction, as well as renal failure in dehydrated or predisposed individuals. Digital
subtraction angiography can further enhance identification of patent and occluded
vessels.Although noninvasive,MRI can alsobeusedtoevaluatebloodvesselsandyields
considerablyaccurateimages.
Venousnon-invasiveDopplerassessmentisusedwhendeepveinthrombophlebitisis
suspected, and a venogram may further enhance identification of a thrombosis,
particularlyonethatispropagatingorassociatedwithembolismandconsiderationisgiven
tosurgicalintervention.
BIOMECHANICS
Biomechanicsisthestudyofmechanicallawsastheypertaintothehumanmusculoskeletal
systemand,inparticular,bipedallocomotion.
Basictermsinclude:
1. Cardinalbodyplanes sagittal(SP),frontal(FP),andtransverse(TP)
2. Axes frontotransverse, allowingmotioninthe SPfrontosagittal,
allowing motion in the TP sagittotransverse, allowing
motionintheFP
3. Motions- pronationandsupination(triplanar)
inversionandeversion(FPJ
adductionand abduction(TP)
internalrotationandexternalrotation(TP)
dorsiflexionandplantarflexion(SP)
flexionandextension(SP)
4. Positions- pronated,supinated,inverted,everted,abducted,adducted,
externally rotated, internally rotated, dorsiflexed,
plantarflexed.When apositionisfixed,itisreferred to as
flexion, extensus orextension,adductus,abductus,varus,
valgus,elevatus,supinatus,equinus,calcaneus.
Motionisdescribedasoccurringinthecardinalplanesofthebodyortoot,inaplane
90"totheaxisofmotion.Singleplanemotionoccursintheplaneperpendiculartotheaxis
thatliesattheintersectionoftheremainingtwoplanes.Triplanarmotionoccursinaplane
perpendiculartoanaxisthatcoursesthroughallthreecardinalplanes(obliquetoallplanes).
Triplanarmotionofthefootissaidto be pronatory/supinatory(pronatory),andthe axis is
directedfromposterior-lateral-plantartoanterior-medial-dorsal.PureSP motionsinclude
dorsiflexionandplantarflexion,whilepuretransverseplanemotionsincludeadductionand
abduction,and purefrontalplanemotionsincludeinversionandeversion.
Biomechanical Examination
The examination beginswith open chain visual inspection,then patientactive motion,
followed bymanipulationandpalpation,followedbygaitanalysis.Specialtesting,suchas
107 Gh.4 SelectedDiagnosticTechniques
pedobarographic,kinematic,andothermotionanalysismethodsmayalsobeused.Visual
inspection is used toidentifygross positional and structuralfeatures. Examination may
proceed as follows: hip, knee, ankle, subtalar joint, metatarsal joint, 1st ray, 1st
metatarsophalangealjointforefoot-to-hindfootrelationship,thenontootherassessments
ofspecificconcern.
Hip - isadiarthrosisthatallowsenarthrousgliding,rotation,angulation,andcircumduction.
Motionoccursinallthreebodyplanes:
TP(sagittal-frontalaxis):InternalandexternalROM
FP(sagittal-transverseaxis):Abduction/adductionROM
SP(frontal-transverseaxis): Aexion/extensionROM(includinghyperextension).
Themechanicalaxisofthehiprunsfromthecenterofhiptoknee,withthe mechan-
icalaxisofthefemoral shaftrunning from aline betweengreaterand lessertrochanters,
relativetothe planeoffemoralcondyles.
Examinationofthe hipshould revealthefollowing:
Adult Hip Range of Motion - lnt. Rot. =Ext. Rot., with hipflexed orextended.The
neutralhipshouldalignfemoralcondylesontheFP. NormalSPhipflexJext.atbirthis
150, and about100 afterpuberty. Iflimited in extension,then hamstringsare likely
tightiflimited in flexion,theniliopsoasis likelytight;excessiveinternaltoexternal
range ofmotion indicatestightadductors;excessive externalto internalrange of
motionindicatestightabductors;andasymmetricallimitationofmotionmayindicate
congenital orneglected hipdysplasia orlimblength inequity.Total range ofmotion
decreaseswithage.
Knee- motionoccursaboutthisginglymusjointwithonlytwodegreesoffreedom(axes)of
motion: SP flexion-extension, and TP internal and external rotation. 5-60 ofTP motion
occurswithSPtlexion-extensionoftheknee.MotionoccurspredominantlyintheSPabout
afrontal- transverse axis, andto alesserdegree aboutthefrontal-sagittal. FP motion is
indicativeofcollateralligamentdamage.Thepatellaenhancesquadricepsleverage.
In non-weightbearing (open kinetic chain)rotation ofthe knee,thetibia rotates on
thefemur. In weightbearing (closed kinetic chain),the femurrotates on thetibia.The
lateralfemoralcondylerotatesaroundthemedialcondyle,withmotionoccurringbetween
thetibia and meniscus.Therefore,forinternalrotation,the lateraltibial condyle moves
anteriorlyon thelateralmeniscus. Forexternal rotation,thelateraltibial condyle moves
posteriorlyonthe lateralmeniscus.Thegreatestdegreeofrotationisavailablewhenthe
kneeisflexedat90". Examinationofthekneeshouldrevealthefollowing:
1. KneepositionontheFPwhenhipandSTJneutral,withendrangeofmotion180,
andfixed
2. Flexionorhyperextensionmayindicatecompensationforankle equinus.
3. Genuvalgum mayeffectcompensatoryhindfootsupination,butgenerallyover
timeactsas
4. Astrongpronatoryinfluenceonthehindfoot
5. Genuvarummustbedistinguishedfromtibialvarum,andpronatesthehindfoot.
6. Genu recurvatummaybe dueto cruciateligamentouslaxityorcompensationfor
ankleequinus.Thighhamstringsorgastrocnemiuscaneffectgenuflexiondeformity.
108 Selected Diagnostic Techniques Ch.4
Ankle - range of motion occurs about a pronatory axis running from the lateral to medial
malleolus, normal range being 20
0
-30
0
dorsiflexion OF and 30-50PF. The axis is primarily at
the junction of the FP and TP, deviated in the TP by about 12"-15of malleolartorsion, thereby
allowing primarily SP OF (flexion) and PF (extension). The articulation represents amortise
(medial malleolus, distal tibial bearing surface,lateral malleolus) and tenon (talar body) joint
Range of motion is assessed by asking the patient to actively take the ankle joint through
DF/PF range of motion in the sagittal plane, followed by circumduction of the ankle or
figure-of-eight motion.
Examination of the ankle should reveal the following: Ankle range of motion should
allow 25-30 PF, and 100 or more dorsiflexion with the knee extended. Increased ankle
dorsiflexion when the knee is flexed is indicative of limitation by gastrocnemius (equinus if
< 10
0
). The Silfverskiold test is then performed, and the presence or absence of gastrocne-
mius or gastro soleus equinus, or bony (talotibial exostosis) equinus, is determined. Pseudo
equinus, due to plantarflexed forefoot results in functional ankle equinus due to retrograde
ankle dorsiflexion in weight bearing. Compensation for ankle equinus may result in normal
heel-off due to adequate subtalar joint/metatarsal jointhyperpronation, early heel-off if only
partially compensated by hindfoot pronation, or no heel-off whatsoever (no heel contact) if
uncompensated in the foot (usually associated with genu recurvatum or fixed flexion).
Subtalar Joint - range of motion occurs about a pronatory axis deviated 42from the TP
(nearly equidistant from the horizontal TP and the vertical FP), and 160 from the SP. STJ is
minimal in the Sp, as the axis almost lies in this plane. Inversion/eversion and adduction/
abduction motion is greatest and almost equidistant in both the FP and TP, respectively.
A higher pitched subtalar joint axis would allow more TP motion, while a lower pitched
subtalar joint would allow more FP motion. The subtalar joint is an oblique hinge
diarthrosis with triplanar motion. Motion from maximum pronation to maximum supination
defines an are, with 2/3 of the arc supinated from the neutral position, and 1/3 pronated
from the neutral position.
20
Normal subtalar joint range of motion is 30-35
0
, with about 10
0
-15
0
eversion and
0
- 30 inversion. Pronation of the subtalar joint in open kinetic chain (non-weight
bearing) entails abduction, eversion, and dorsiflexion ofthe calcaneus on the talus; whereas
pronation in the closed kinetic chain (weight bearing) attitude entails adduction, inversion,
and plantarflexion ofthe talus on the calcaneus. Range of motion is assessed by observing
normal excursion of 2/3 inversion to eversion with the ankle joint OF and the metatarsal
joint maximally pronated and locked on the hindfoot. It has been estimated that aminimum
subtalar joint range of motion of 8-12is required for normal ambulation. The neutral
position of the subtalar joint, as determined by a posterior bisector ofthe calcaneus, is the
point 1/3 of the way from maximum subtalar joint pronation, and 2/3 of the way from
maximum inversion.
Calculation of subtalar joint (STJ) neutral position (NP) is as follows:
I\IP STJ '" eversion ROM - (total ROM/3).
A positive value indicates avalgus or neutral position
A negative value indicates avarus or neutral position.
109 Ch.4 Selected Diagnostic Techniques
Example
If there is a maximum of 12STJ eversion, and 18maximum inversion, then the
tROM 30".
NP STJ =12" - 30/3 =12" _10=NP STJ of 2varus
To identify STJ NP. we need to know the point from which there is twice as much
supination as there is pronation:
total (STJ ROM / 3) x 2 = inversion from NP. and Onv. from leg) -( inversion from
neutral) NP
Example
If the calcaneus can evert 100 from the leg bisection and invert 200 from the leg
bisection, what is the NP of the STJ?
total STJ ROM 10+20=30, 30/3 x 2 = 20" inversion from NP,
so Onv. from leg) (inv. from neutral) =20- 20=0=NP
Examination of the subtalar jOint should reveal:
Subtalar joint motion, as described previously, ideally 20inversion (supination) and 10
eversion (pronation), with subtalar neutral being 1/3 the range from maximum eversion and
2/3 the range from maximum inversion. The posterior bisector of the heel should be
perpendicular to the ground with the subtalar joint neutral. In a subtalar joint varus
deformity, there is more than 2/3 of the range of motion in the direction of varus (example
25 inversion with supination, 5" eversion with pronation, 5 inversion of calcaneus to
ground), resulting in excessive compensatory subtalar joint/metatarsal joint pronation in
stance (compensated rearfoot varus). Compensated rearfoot varus can also effect
excessive subtalar joint pronation in a subtalar joint varus combined with tibial varum
deformity (eg. 25inversion with supination, 5eversion with pronation, in presence of 5
tibial varum), if the calcaneus is perpendicular to the ground when the subtalar joint is
maximally pronated. A partially compensated rearfoot varus (eg. 30 inversion with
supination, 0" eversion with pronation, 5tibial varuml. when the subtalar joint cannot fully
evertto perpendicular (remains in 5" varus, in this particular example).
Metatarsal joint {MTJ} - range of motion occurs about oblique (OMTJ) and longitudinal
(LMTJ) pronatory axes. The OMTJ axis lies 52" from the TP and 57from the Sp, coursing
from the mid-lateral aspect of the calcaneus to the TNJ. Primary motions are abduction/
adduction and DF/PF, with minimal inversion/eversion. The oblique MTJ (DMTJ) axis allows
predominantly DF/PF and adduction/abduction, with minimal inversion/eversion. The
longitudinal MTJ axis allows predominantly inversion/eversion with minimal DF/PF and
abduction/adduction. Both the OMTJ axis and LMTJ axis allowtriplanar motion. Range of
motion is assessed with the forefoot loaded in DF and eversion atthe 5th metatarsal head,
and the subtalar joint in neutral position. The plantar tangent to the hindfoot should be
perpendicular to the posterior bisector ofthe calcaneus, while allowing the medial column
to seek its own level. Pronation of the STJ will unlock the MTJ and allow hypermobility of
the first ray (forefootsupinatus). The LMTJ (Hicks' axis) lies 9" from the SP and 15from the
TP. coursing from the posterolateral aspect of the calcaneus to the 1st metatarsal-cuneiform
joint. Being so close to the SP and TP. the axis provides a primarily inversion/eversion in
the FP. Normal metatarsal joint range of motion is 4_6. Forefoot supinatus occurs primarily
110 Selected Diagnostic Techniques Ch.4
around Hicks' LMTJ axis. When the 8TJ is pronated, the MTJs become parallel, allowing
the head of the talus to decline plantarly relative to the navicular.
Examination of the MTJ should reveal: MTJ motion with 8TJ pronation, the plantar
aspect of the forefoot everts relative to the hindfoot, as the MTJ unlocks and becomes more
mobile. With 8TJ supination, the plantar aspect of the forefoot inverts relative to the
hindfoot, and MTJ motion is limited. If the forefoot remains inverted to the rearfoot, forefoot
varus exists. If the forefoot remains everted to the rearfoot, forefoot valgus exists. Forefoot
valgus may be rigid orflexible. Forefoot supinatus describes the compensatory inversion of
the forefoot on the rearfoot associated with hyperpronation of the 8TJ and OMTJ, the
inversion of the forefoot occurring around the LMTJ axis.
1st ray- range of motion occurs about an axis coursing 45from the SP and 45from the FP
in a posterior-dorsal-medial to anterior-plantar-lateral direction, allowing motion aboutthe
medial cuneiform-navicular and 1st metatarsal-cuneiform joints. 1st ray range of motion is
assessed with the subtalar joint in neutral position, while manipulating the head of the 1st
metatarsal through its DF/PF 8P excursion.
Examination of the 1st ray reveals: normal 1st ray motion is 5 mm (10) in both dorsal and
plantar directions, as compared to a normal second ray. As the 1st ray dorsiflexes, it
inverts; and when it plantarflexes, it everts, in a 1:1 ratio. This motion is important in
determining hypermobility of the 1st ray. McGlamry has noted that transverse plane
mobility of the 1st ray is comparable to sagittal plane mobility of the 1st ray, and is
indicative of the ability to reverse buckle the 1st MTPJ and thereby reduce the 1st IMA via
Reverdin osteotomy. Moreover, hypermobility of the 1st ray, with resultant forefoot
supinatus, may indicate the need for 1st metatarsal-cuneiform arthrodesis as compared to
1st metatarsal base wedge osteotomy in the correction of metatarsus primus varus and
hallux abducto valgus or other deformities.
A plantarflexed 1st ray reveals maximum dorsiflexion below, or plantar to, the level of
the 2nd metatarsal, resulting in a valgus attitude of the forefoot to the rearfoot. It is
important to assess the relation of the 1st through 5th, and 2nd through 5th, relative to the
rearfoot. The forefoot valgus may be rigid or flexible. A rigid plantarflexed 1st ray effects
forefoot valgus, with retrograde supination of the metatarsal joint and, if severe enough,
even supination of the subtalar joint. Associated deformities include hallux malleus (hallux
hammertoe). with EHL and FH Lmechanically advantaged relative to EHB and FHB; as well
as sesamoiditis (usually tibial), lateral ankle and knee strain, symptomatic Haglund's
deformity (pump bump), and children may display an intoe gait. This also results if a 1st
metatarsal-cuneiform fusion or 1st metatarsal base osteotomy effects too much
plantarflexion.
A flexible plantarflexed 1st ray effects a flexible forefoot valgus, which does not
function plantarflexed when the 1st ray is loaded. The 1st ray may function at the level of
the lesser metatarsals if the MTJ unlocks with hindfoot pronation. Associated findings may
include submetatarsal1 and 5hyperkeratosis, tibial sesamoiditis, and flexor stabilizing lesser
hammertoes.
Metatarsus primus elevatus exists when the 1st ray is positioned above, dorsal to, the
level of the lesser metatarsals, specifically the 2nd metatarsal. and is associated with
hallux limitus/rigidus, hallux equinus, dorsal bunion, lateral dumping of late midstance and
propUlsive phase weight bearing and sub-second metatarsalgia and hyperkeratosis, as
well as 5th toe dorsolateral HD and perhaps 4th interspace HM or HD. The 1st met. may be
elevated relative to the 2nd, even in the presence of overall forefoot varus. An elevated 1st
111 Ch.4 Selected Diagnostic Techniques
ray may be congenital, or acquired secondary to longstanding hyperpronation of the
STJ/MT J (hindfoot), or iatrogenic following fracture or base osteotomy. Hallux limitus may
also be caused by an excessively elongated 1st metatarsal. 1st MTPJ injury, metabolic
arthritis, or sesamoid adhesion. Prolonged metatarsus primus elevatus effects medial
column collapse and pes valgus over time.
5th ray- axis of motion is oblique to all three body planes and is therefore pronatory/supina-
tory, running from proximal-plantar-lateral to distal-dorsal-medial, 20from the TP and 35
from the Sp, and predominately allows SP and FP motion. The 5th ray everts with dorsiflex-
ion and inverts with plantarflexion.
Intermediate rays- consist ofthe 2nd through 4th rays, which have frontal-transverse axes
and therefore allow motion only in the SP. MTPJ function is divided into 1st and lesser
groups, all of the MTPJs functioning primarily, or initially, as ginglymus joints with
predominantly SP dorsiflexion/plantarflexion although TP rotation is also allowed about a
vertical axis. The 1st MTPJ range of motion should display 65 (as measured from a
position parallel to the substrate, or 20-21from the long axis of the 1st metatarsal which is
declined relative to the substrate, in essence making afull range of motion from the long axis
of the metatarsal being 65+20-21=85-86) for normal propulsion, and firm plantarflexion
stabilization ofthe metatarsal (relative plantarflexion) is required in propulsion otherwise 1st
ray hypermobility and lesser digital flexor stabilization will result. The initial 25of 1st MTPJ
dorsiflexion occur with the joint acting strictly ginglymus, however reciprocal 1st metatarsal
plantarflexion is required for dorsiflexion> 25, which causes the frontal-transverse axis to
move proximally and dorsally (path of the evolute) as the joint behaves arthrodial in late
midstance and propulsion.
Lesser MTPJs - should achieve 15 dorsiflexion in propulsion with good plantarflexion
stabilization against the substrate, and similarly require reciprocal metatarsal plantarflexion
and proximal-dorsal migration ofthe transverse axis (evolute) for greater dorsiflexion.
Ontogeny as it Relates to Biomechanics of the Lower Extremity
The femoral segment displays a FP angle of inclination relating the head and neck of the
femurto the long axis of the femoral shaft: birth, 150-160; 6years to adult, 125. The TP angle
of declination relates torsion within the shaft of the femur from the head and neck to the
distal condyles.
Femoral antetorsion refers to twisting ofthe femur such that the condyles ofthe femur
are internally rotated relative to the frontal plane and the head and neck. The angle
between the head and neck of the femur and the femoral condyles is normally 30 - 40of
anteversion at birth and 8-12in the adult, representing a gradual retrotorsion as the femur
untwists with maturation. Concomitant with the retrotorsion is femoral anteversion, or
inward twisting to the thigh segment to counter the more proximal retrotorsion, thereby
keeping the femoral condyles on the FP.
Delayed derotation can effect in-toe, and is often seen in the older female child and
clinical presentation of the "reverse tailor's" sitting position, increased medial femoral range
of motion, and knock-knee. Treatment includes proper sitting habits, Ganley femoral
derotation splint (4 to 8 years), and femoral derotation osteotomy in the older child. Knee
flexion diminishes the therapeutic influence of any pedal splinting directed at the femur,
and appropriate pediatric orthopedic consultation is in order whenever significant deformity
112 Selected Diagnostic Techniques Ch.4
exists. The angle between the head and neck of the femur and the FP is normally 60
0
external
at birth, and 80-1000 external in the adult
Terminology pertaining to the femur includes: antetorsion - internal femoral torsion,
anteversion - internal femoral position, retrotorsion - external femoral torsion, and retro-
version - external femoral position.
The knee alignment- varies with age as follows: birth, genu varum; 1-3 years, straight; 3-6
years, genu valgum; 7 -13 years, straight; 13-18 years, genu valgum, > 18 years, straight; >
60years genu valgum.Tibial varum is aFP inverted angulation ofthe lower leg to the ground
in static stance. Tibial valgum is a FP everted angulation of the lower leg to the ground in
static stance.
The malleoli - form a 0
0
angular relation to the FP at birth, followed by an external growth
torque of 18-23
0
true tibial torsion or 13-18of malleolar position, malleolar position being
about 5 less than true tibial torsion, occurring in the transverse plane. We measure
malleolar position because we can not actually measure tibial torsion clinically. As aguide,
external malleolar position should be as follows 0-100 from birth to 1year, 8-13
0
from 1-5
years, and 13-18from 6years to adulthood.
The hindfoot relationship - oftalus to the calcaneus during fetal development reveals aFP
movement ofthe talus overthe calcaneus from aparallel position (clubfootTEV represents
cessation or limitation ofthe movement away from parallel). The talar head becomes less
plantarflexed relative to body of calcaneus, which is important for development of normal
TP TCA. cyma line, talar declination angle, CIA, and MTJ position.
Growth in length and width ofmetatarsals andphalanges - is ongoing from fetal to adult
stages, and includes FP eversion torsion of metatarsals 1-5, and TP abduction of 1st
metatarsal to lesser metatarsals: fetal- 1 st metatarsal adducted 500, birth - adducted 6, by
4years to adult - 7-9
0
(if> 7-9, get metatarsal primus adductus or varus with juvenile HAV).
The TP relation of the lesser metatarsals to the tarsus reveals: birth 25 adducted,
adult - 15-18adducted. Metatarsus adductus is 15-35at birth, and 15-22in the adult.
Structural and Positional Deformities of the Lower Extremities
Forefoot varus - is a structural deformity of the forefoot in which the plantar plane of the
forefoot is inverted relative to the supporting surface and the vertical posterior bisector of
the calcaneus when the subtalar joint is neutral and the metatarsal joint maximally pronated
and locked. It is associated with compensatory hyperpronation of the STJ/MTJ;
submetatarsal 2-5, especially 4-5, hyperkeratosis; tailor's bunionette, flexor stabilization
induced hammertoes, adductovarus 4th and 5th toes, HAV, metatarsus primus elevatus,
plantar fascitis, and heel spur syndrome, and hallux limitus, medial knee strain and internal
rotation secondary to compensatory hyperpronation of the hindfoot. Biomechanical
treatment generally entails supporting the deformity, thereby nullifying the need for
compensation in the foot, while posting the rearfoot to allow 2-4
0
of motion.
Rexible forefoot valgus- is astructural deformity wherein the plantar plane ofthe forefoot
is everted relative to the supporting surface and the vertical posterior bisector ofthe cal-
caneus when the subtalar joint is neutral and the MTJ maximally pronated and locked. It is
associated with compensation via supination aboutthe LMTJ axis (forefoot supinatus); sub-
113 Ch.4 Selected Diagnostic Techniques
metatarsal 1and 5hyperkeratosis; tibial sesamoiditis, flexor stabilization hammertoes, and
adductovarus 4th and 5th toes. Biomechanical treatment generally entails supporting the
deformity, thereby nullifying the need for compensation in the foot, while posting the
rearfoot to allow 2 to 4of motion.
Rigid forefoot valgus - is a structural deformity wherein the plantar plane of the forefoot is
everted relative to the supporting surface and the vertical posterior bisector of the
calcaneus when the subtalar joint is neutral and the MT.I maximally pronated and locked.
It is associated with compensation via supination about the OMTJ axis and subtalar joint
axis; hallux malleus, tibial sesamoiditis, lateral ankle and knee strain, symptomatic Haglund's
deformity (pump bump), and children may display an intoe gait. Biomechanical treatment
generally entails supporting the deformity and using a 1 st ray cut out, thereby nullifying the
need for compensation in the foot, while posting the rearfoot to allow 2-4of motion.
Rearfoot varus - is a structural deformity wherein the calcaneus is inverted relative to the
substrate when the subtalar joint is neutral and the MTJ maximally pronated and locked. It
is associated with lateral ankle sprain, compensatory pronation of the hindfoot only to
vertical (not a profound degree of pronation), submetatarsal 4-5 hyperkeratosis,
adductovarus 4th and 5th toes, tailor's bunionette, Haglund's deformity, and HAV.
Rearfoot valgus - is a structural deformity wherein the calcaneus is everted relative to the
substrate when the subtalar joint is neutral and the MTJ maximally pronated and locked. It
is associated with submetatarsal2 hyperkeratosis, HAV, plantar fascitis, flexor stabilization.
Metatarsus primus elevatus - is a structural deformity wherein the 1st metatarsal displays
a resting position dorsal to the 2nd metatarsal and plane of the lesser metatarsals. It is
associated with hallux limitus/rigidus, hallux equinus, dorsal bunion, lateral dumping of late
midstance and propulsive phase weight bearing and sub-second metatarsalgia and
hyperkeratosis, as well as 5th toe dorsolateral HD and perhaps 4th interspace HM or HD.
Forefoot supinatus - is a fixed position of supination of the forefoot about the LMTJ axis,
when the subtalar joint is neutral and the MTJ maximally pronated and locked. It is
associated with plantar fascitis, and limited MTJ available range of motion.
Ankle equinus - is the condition of inadequate dorsiflexion range of motion of the foot on
the leg. It is considered present when < 10of ankle dorsiflexion is available, and the
Silfverskiold test is used to determine the influence of the Achilles tendon as a whole and
the gastrocnemius muscle and aponeurosis separately. Osseous talotibial blockade
may also be present. Equinus deformity is associated with early heel off, knee flexion
throughout stance (unless damaging hyperextension-genu recurvatum occurs),
compensatory hyperpronation of the hindfoot with plantar fascitis, flexor stabilization,
adductovarus 4th and 5th toes, HAV, and extensor substitution if the equinus persists as a
dropfootthrough swing phase.
Tibial torsion - is measured as malleolar position with the malleoli forming < 13-18of
external malleolar position, malleolar position being about 5less than true tibial torsion, in
the transverse plane. External malleolar position is as follows 0-10from birth to 1 year,
8-13from 1-5 years, and 13-18from 6 years to adulthood. Internal tibial torsion often
affects the left lower extremity (in utero pressure from maternal vertebral column) in males,
114 Selected DiagnosticTechniques Ch.4
andtreatmentinvolvesserialcastingtoabovetheknee,takingcaretostabilizethehindfoot
andankleinneutralposition.
Genu valgum (knock knee)- isanangulardeformityofthekneeusuallyobservedinobese
female children, and may be associated with coxa vara or uncompensated medial or
compensatedlateralfemoraltorsion,tibialtorsion,pesvalgus,deformation(depression)of
thelateraltibialplateauwithhamstringorquadricepsorcalfpainandDJD intheadult.
Genu varum (bowleg) - is an angulardeformityofthe knee usuallyobservedin casesof
Ricketsduetovitamin-DdeficiencyandabnormalCa andPhmetabolism,orduetoBlount's
osteochondrosisdeformanswhereinthemedialtibialcondyleisflattenedandfragmented
(presentatbirthto24-30months).
Femoral anteversion- referstopositioningofthefemursuchthatthecondylesof thefemur
areinternallyrotated relativetothefrontalplane andtheheadand neckofthefemur.The
anglebetweentheheadandneckofthefemurandthefemoralcondylesisnormally30- 40
ofanteversion atbirthand 8-12inthe adult, representing agradual retrotorsion as the
femuruntwistswith maturation.Delayed derotationcaneffectin-toe,and isoftenseen in
theolderfemalechildwiththeclinicalpresentationofthe"reversetailor's"sittingposition,
increased medialfemoral range ofmotion, and knock-knee. Treatmentincludes proper
sitting habits, Ganley femoral derotation splint(4 to 8years), and femoral derotation
osteotomyintheolderchild.Kneeflexiondiminishesthetherapeuticinfluenceofanypedal
splintingdirectedatthefemur,andappropriatepediatricorthopedicconsultationisinorder
wheneversignificantdeformityexists.
Unequal limb length - maybe structuralwithinthethigh,legorboth femoral andtibiall
fibularsegments;orfunctionalsecondarytoscoliosisinducedpelvictiltwithlowersideof
pelvis effecting functionally longerlimb, unilateral supination or pronation ofthe foot.
Compensation forlimb inequityinvolves pedal pronationon the longerside, along with
ipsilateral inferiorpelvictilt(tilts downward)dueto hyperpronating hindfoot,ipsilateral
shouldertiltdownward,scoliosis,ipsilateralheadtilttowardlongerlimb,increasedstance
phase on the longerside. On theshortside,thehindfootsupinates,pelvisrises,shoulder
rises,andthereislessstancephaseweightbearing.
RadiographicFindingsRelatedtoBiomechanics
Radiographic signs of hyperpronation of the foot include: increased TP and SP
talocalcaneal angles, increased talar declination, decreased calcaneal inclination,
decreasedforefootadductusandincreasedabductusduetounlockedMTJ, anteriorbreak
in the midtarsal cyma line, decreased (<70%) talonaviculararticulation congruity, and
medial column breach in severpes valgus. Radiographic signs ofasupinatedfootare
oppositetothoseseenwithpronation,andincludeabulletsinustarsi,andamore parallel
relation ofthetalus and calcaneus. An acquired rocker bottom foot, dueto equinusor
severepesvalgus,displaysplantararticulargappinganddorsaljamming.
BasicGaitAnalysis
Phasesofthegaitcycleincludestance(62%)andswing(38%).
Thestancephaseissubdividedinto:
115 Ch.4 Selected Diagnostic Techniques
contact - which occurs from heel contact to forefoot contact and entails 27% of the
stance phase and 17% ofthe entire gait cycle, and is associated with the foot serving
as a pronating mobile adapter, with initial vertical force being about 125% of body
weight
midstance- (entails 40% ofthe stance phase) wherein the foot converts to arigid lever
for push-off, and the vertical force decreases to about 75% of body weight;
propulsion - (33% of stance) which consists of heel off and toe off, wherein the
vertical force again reaches about 125% of body weight and the foot is a rigid
supinated, tight-packed lever.
Swing phase - requires external leg rotation and ankle dorsiflexion, and hip and knee
flexion.
At heel contact, we note hip extending, knee flexing, ankle plantarflexing, and
STJ neutral and pronating.
At midstance, we note hip flexing, knee extending, ankle dorsiflexing, STJ
supinating and MTJ pronating.
Double support occurs atthe beginning and end of each stance phase in walk-
ing gait, wherein both feet are on the ground, and this occurs at the 1st 0-12% and
again at 50-62% ofthe gait cycle, or 25% ofthe entire cycle.
Double float, or an airborne phase, occurs in running gait.
The phasic activity of the lower extremity musculature is as follows, relative to the gait
cycle:
hip adductors fire from heel contactto midstance and again from heel off to midswing
hip abductors fire through late swing to prior to heel off
hamstrings fire from late swing to 25% of stance; quadriceps femoris fire from hee
contactto 25% of stance and again from toe off through early swing
triceps surae fire from 15-20% of stance to toe off
peroneal musculature fires from 15-20% of stance to toe off; and the anterior leg
musculature fires from swing to midstance
116 The Perioperative Patient Ch.5
THE PERI OPERATIVE PATIENT
The perioperative period is divided into preoperative, intraoperative and postoperative
phases. Planning asafe and efficacious course forthe patient requires that attention be paid
to many details. Open and frank discussion with the patient and their family, and consult-
ants, is important relative to achieving asmooth operative course.
PREOPERATIVE PHASE
Considerations in the preoperative phase include the history and physical ~ H P ) , accurate
diagnosis and treatment protocol, the decision to operate, and informed consent
Informed Consent Contains:
Review of the diagnosis
Planned surgery or procedure
The possibility of other intervention based upon operative findings
Potential risks and complications
Alternatives to the surgery or procedure
Postoperative course and expectations
Permission for observers in the operating room and for photography
Safe Medical Device Act
Identification that no guarantees have been made
Signature by the patient, awitness, and the surgeon
Appropriate systemic medical evaluation should also be obtained preoperatively, and
discussion with the patient's physician should be undertaken as indicated. Preoperative
consultation, physical therapy, attainment of postoperative medications and/or special
equipment, such as a bone growth stimulator for home use, notification of social services
if home wound care or IV antibiotic administration and testing are anticipated, should also
be considered.
Special medical considerations include thrombophlebitis prophylaxis, corticosteroid
supplementation, prevention of gout, and infection prophylaxis with preoperative
administration of antibiotics. If the procedure is anticipated to last more than 2-3 hours,
urinary catheterization may be performed.
The preferred anesthesia should be discussed with the patient and, if there is a
question, the anesthesiologist. The operating room personnel should be notified ofthe need
for special equipment and studies, such as the C-arm and diagnostic imaging, specific
instruments or implants, power lavage, tubes for aerobic and anaerobic C&S, frozen
section, drains, bandages, and splinting/casting materials. The patient should fully under-
stand the planned postoperative course, analgesia, weight-bearing status, rehabilitation
schedule, time off from work, and prognosis.
INTRA-OPERATIVE PHASE
The intra-operative phase entails those activities that take place once the patient is in the
operating room. The details ofthis period are documented in the operative report, the record
of anesthesia, and the circulating nurses notes. Attention is paid to achieving surgical
117 Ch.5 The Perioperative Patient
anesthesia, patientpositioning,hemostasis,extensile exposure,wound exploration and
inspection of pathological anatomy, alteration of planned procedure if indicated,
intraoperative imagingto assess correction and fixation, wound closure and bandag-
ing/splinting,and controlofanycomplications(hemorrhage, break ofsterilefield, malig-
nanthyperthermia,ischemiaIthatmayhavearisenduringthecourseoftheprocedure.
POSTOPERATIVE PHASE
The postoperative phase entailsthe period commencing in the recoveryroom untilthe
patientisdischargedfromyourcare.Obviouslythe earlypostoperativeperiod(first1to3
dayslismostcriticalrelativetothe possibilityofsystemic complications.The surgeon's
postoperative orders detail planned care ofthe patientonce the anesthesiologist has
transferred the patientfrom the recovery room. The surgeon mustalso documentthe
procedureandfindingsofthesurgeryintheoperativereport
Standard Postoperative Orders Can Include
1. Vitalsigns(VS Qshiftafterreturntofloor)
2. Activity(eBRwithside railsup;absoluteNWBoperatedfootatalltimes;BRP
NWB operated footwith assistance; PT for gait and transfertraining NWB
operatedfootl.
3. IVfluids(maintainIV0%LR atKVO untilfullyreactive/stable.ConverttoHeparin
lockafterD/C IV).
4. Medications,including antibiotics, analgesicsformoderate and severe pain,
anti-inflammatory,anti-emetic,stoolsoftener/bowelstimulant,hypnotic,andthe
patient'sregularmedications.
5. Respiratorytherapy
6. Drain management
7. Diet
8. Dischargeplanning
9. Otherordersspecifictothe case
Postoperative Complications
Postoperativecomplicationsarevariable,andrangefrommild problemstolife- threatening
crises.Complicationscanoccurdespitethebestplanningandtechnique.Itisthesurgeon's
responsibilitytopointout.within reason,the possible complicationsrelatedtoaspecific
procedure,andto beonthelook-outforthedevelopment thereofinthepostoperativephase.
The bestapproachtothe managementofapostoperative complicationisstraight-forward
identificationofthe problem,notificationofthepatientand documentationinthemedical
record,andtreatmentConsultationmaycertainlybeinorder.
Apostoperativecomplicationisdefinedasanyuntowardeventoccurringwithinthirty
daysafterthe surgery. Complicationsmayaffectthe surgicalwound and various organ
systems,including pulmonary, gastrointestinal,cardiovascular,and urinarysystems.The
phraseuwind,water,wound,walk,wonder,"remindsthesurgeonofthemostcommonpost-
operativecomplicationsandthe postoperativedayduringwhichthespecificcomplication
usuallyoccurs.
118 The Perioperative Patient Ch.5
Postoperative Day Complication
firstday pulmonary
second day urinary
thirdday wound
fourthday calfDVT
fifthday anythingispossible
Pulmonary complications include atelectasis, aspiration, and pulmonary embolism.
Pulmonarycomplicationsaremorelikelyfollowinggeneralanesthesia,andinpatientswho
areobeseorthosewithahistoryofCOPOorregularcigarettesmoking.Suchpatientsshould
undergo preoperative pulmonaryfunction testing, and the anesthesiologist should be
notified ofthe results. Postoperative pulmonaryassessmentnotes respiratoryrate and
effort,inconjunctionwithauscultationofthelungfields.
Atelectasis istheconditionofcollapseoftheadultlung,andisusuallyduetobronchial
occlusion (secretions) and subsequent absorption of air as alveolar perfusion
continues.Atelectasismayoccurduringoraftergeneralanesthetic.
Aspiration occurswhengastric contents are admitted intothetrachea, bronchial
passages,andlung,resultinginairwayinflammationand pneumonitis.Aspirationmay
occurin relationtoadministrationofageneral anesthetic,when the patient'sgag
reflexismuted.Atelectasisand aspirationpneumonitiseffectlocalizedpain,dyspnea,
andfever.Auscultationmayrevealabnormalbreathsounds.AchestX-rayshouldbe
obtained.Respiratorytherapytoenhanceventilationisindicatedformildatelectasis,
andwillusuallysuffice.Therapyrangesfromsimple incentivespirometry(Triflow)to
medicated breathingtreatments.Aspirationpneumonitisistreatedwithappropriate
respiratorytherapy,corticosteroids,andantibiotics.
Pulmonary embolism associatedwithlowerextremityDVT, isthemostdevastating
postoperativepulmonarycomplication.See Chapter 3.
Urinary complications include retention and urinary tract infection. Postoperative
assessmentinvolvesobservationoffluid inputand output,blood pressure and heartrate,
andsuprapubicpalpationandpercussion.
Retention iscommon in elderlymalesatbed rest,particularlyifthereisconcomitant
benign prostatic hypertrophy orhistoryofurinarystricture secondaryto previous
traumatic urethral catheterization, infection or surgery. Atropine or other anti
cholinergic in high doses associated with general anesthesia can cause urinary
retention.Similarly,prolongedsurgeryandanesthesia,withadministrationofIVfluids
may lead to bladder distention (average bladdervolume is about500 eel. Cases
anticipatedtolast3ormorehoursshould entail placementofaFoleycatheterafter
generalorspinal anesthesia has been achieved.Ifthe patienthasnotvoided bysix
hours postoperative,examinefor bladderdistention (palpationand percussionland
initiatetreatmentbyencouragingthepatienttostand(workswellinmalesl.Ifpatient
remainsunabletovoid,thenpassastraightcatheteroncetoevacuatethebladderand
measurethevolume.If theurinevolumeis<300cc,discontinuecatheterization.lfthe
urinevolumeis500ccormore,considerplacementofanindwellingcatheteruntilthe
patientismoreambulatoryandcomfortable.
119 Ch.5 The Perioperative Patient
Urinary tract infection can be caused by prolonged urinary retention, or urinary
catheterization. Care should be taken to employ aseptic technique whenever passing a
urinary catheter. Females are more likely to develop urinary tract infection, and many have
previous history of urinary tract infection. Treatment entails adequate hydration, and
antibiotic therapy after obtaining a clean catch, midstream urine specimen for C&S.
Wound complications
Fixation failure or loss of surgical correction usually requires a return to the operating
room to rectify anything butthe minimal deformity.
Circumferential bandage or cast compression. An excessively snug or tight
circumferential bandage or cast can induce pain that is unresponsive to analgesia,
cutaneous compromise and pressure ulceration, neuropraxia; and requires cast and
bandage replacement in order to effect relief.
Hemorrhagewill usually cease with protection, rest, ice, compression, and elevation.
If hemorrhage persists beyond one or two bandage reinforcements, then
consideration should be given to a return to the operating room for exploration and
hemostasis. Hemoglobin and hematocrit levels will decline secondary to significant
hemorrhage, and preparation for transfusion should be considered ifthe hemoglobin
drops below 9 grams. (It is rare and quite problematic for a patient to require
transfusion following foot and/or ankle surgery.) Observation ofthe patient's vital signs
may indicate the need to increase IV fluid administration above the KVO rate.
Dehiscence may be superficial or deep, and can usually be managed with local wound
care and secondary intention healing, as long as hematoma or infection does not
warrant intervention that is more aggressive.
Hematoma and infection warrant, at the least, selected suture removal, swab
specimen of any exudate or drainage for Gram's stain and C&S, CBC with differential,
observation of systemic temperature and blood glucose, close wound monitoring, and
possibly oral antibiotic therapy, for minimal or equivocal findings. If the signs of
inflammation associated with suspected hematoma and/or infection are significantly
advanced, or not responding within 24-48 hours to initial intervention, then a return to
the OR for wound inspection and cleansing debridement may be warranted. Actual
therapy will depend upon the local and systemic merits of the individual case. It is
better to error on the side of over-aggressiveness, rather than miss the diagnosis and
place the patient at more risk.
Infection is highlighted by unusual amounts of pain, often unresponsive to analgesic
medication, on or about the 2nd to 3rd postoperative day. Hemolytic Streptococcus
may cause fever and wound infection within 24 to 48 hours of the surgery.
Consideration should be given to an acute gouty attack in the hyperuricemic patient
with history of gout, and to an excessively tight bandage or cast. Excessive pain at
the operative site always warrants inspection. Nonsuppurative wound infection can
be difficultto identify, even with close observation ofthe surface ofthe well-coapted
incision, and a high index of suspicion should be maintained. Systemic signs of
120 The Perioperative Patient Ch.5
endotoxin release and/or septicemia should be suspected, and include GI distress,
general malaise, cutaneous rash and/or desquamation (toxic shock syndrome),
myalgia, cephalgia, and pyrexia.
Postoperative ischemia usually identified in the digits as a "blue toe." Other common
areas of postoperative ischemia include skin islands (actually isthmuses or bipedicle flaps)
situated between two long, parallel skin incisions. Causes of blue toes include venous
congestion, dissecting hematoma, and arterial occlusion or microcirculatory vasospasm.
Venous congestion effects a cyanotic, often warm, diascopy positive toe that may
respond well to elevation and perhaps loosening of constriction bandages and
flexion of the knee. Ice, nicotine, and caffeine should be avoided whenever dealing
with a blue toe.
The term dissecting hematoma may be amisnomer, however it refers to the condition
wherein hematoma has separated and filled the potential space between intact and
viable dermis and overlying epidermis. The condition has also been described with
intradermal dissection. In this condition, the epidermis displays a dark appearance
consistent with hematoma observed through the thin, translucent epidermis. The basal
layer of the epidermis may also become necrotic, and the epidermis will eventually
slough. The digit may be anesthetic, cool, and stiff. The important clinical distinction,
related to dissecting hematoma, is the possibility of misconstruing the toe as being
gangrenous throughout. It is prudent to carefully inspect and debride the superficial
layers of the skin to ascertain whether deeper tissues are viable. Arterial Doppler
assessment of the digital vessels may also be useful when considering the possibility
of dissecting hematoma.
Occlusive vascularischemia due either to functional vasospasm or organic disruption
of the flow (thrombus, embolism, impingement or laceration), effects a cold toe that
initially displays pallor followed by cyanosis and then gangrene. The ischemic toe
will usually blanch upon application of pressure (diascopy positive), however
subpapillary venous plexus refill time will be greatly delayed. If blood flow is restored
prior to the development of necrosis (3-6 hours), pink or red cutaneous hyperemia will
be observed. Vasospasm can be effected by surgical manipulation, often noted with
vessel traction and pin stabilization across the MTPJ; or seen in patients with a
history of Raynaud's phenomenon and subjected to acool operating room and lavage
fluids; or due to the local use of dilute epinephrine in a patient with Raynaud's
phenomenon or treated with tricyclic antidepressant or MAO inhibitor.
Counter measures include dependency, loosening tight bandages, avoidance of
nicotine and caffeine and ice, adjustment or removal of a pin positioned across the MTPJ,
reflex heat(K-pad) applied to the abdomen and or thigh, posterior tibial nerve or ankle block
with plain bupivacaine, and oral (Procardia) and/or intra-arterial (Priscoline) vasodilator
following vascular consultation.
Postoperative OVT
See Chapter 3
121 Ch.5 The Perioperative Patient
Gastrointsstinal complications - include nausea and vomiting, constipation, gastritis and
reflux esophagitis, fecal impaction, and postoperative jaundice. Severe bowel obstruction
or postoperative paralytic ileus usually only occurs following abdominal surgery.
Postoperative assessment of the belly entails observation, auscultation for bowel sounds,
and palpation for tenderness, guarding, and rebound.
Postoperative nausea and vomiting may be the result of anesthetic or narcotic
influence on the central chemoreceptor trigger lone, or dueto peptic ulcer disease or
gastritis in predisposed patients or those medicated with anti-inflammatory drugs.
Excessive emesis can effect dehydration, and IV fluids should be administered. Drugs
such as Compazine, Tri/afon, Phenergan, Dramamine, ligan, and Emeticon can be
used to control postoperative nausea, and may be administered in suppository form.
Drug interaction with analgesics, sedative/hypnotic, and antidepressants should be
considered whenever administering centrally-acting antiemetics.
Constipation often results from inactivity, and commonly occurs in elderly patients
who are immobilized in bed. Bulk laxatives such as bran Metamuci/ or Senokot, or
stool softeners such as Co/ace, Doxinate and DDS, are preferred over bowel stimulants
such as Milk of Magnesia or Du/co/ax. Encouraging fluids and out of bed activity are
indicated. Rarely is an enema necessary.
Feca/ impaction is rare following foot and ankle surgery and may present as
postoperative diarrhea.lfthe digital rectal examination reveals hard stool, then an oil
retention enema may be helpful. Digital disimpaction may also be necessary.
Gastritis and/or reflux esophagitis is common in patients maintained NPO and
positioned supine with the legs elevated, especially in those with hiatal hernia and/or
previous PUD. Treatment is elevation of the head and oral administration of antacid
(Riopan, Ro/aids, rUMS) and/or HZ receptor antagonist such as Pepcid. Diarrhea can
often be controlled with bismuth (Pepto-bismol).
Postoperative jaundice usually associated with nausea, warrants assessment of
hepatic enzymes and review of the anesthetic record. If right upper quadrant pain is
marked (colic), then general surgical consultation and cholecystogram or ultrasound
is indicated.
Cardiac complications - uncommon in associatIOn with elective foot and ankle
reconstructive surgery, and are most likely to occur in patients with pre-existing coronary
artery disease, dysrhythmia, congestive heart failure, or patients with significant pulmonary
disease. Postoperative cardiac evaluation involves vital sign assessment, and
auscultation. Rarely fluid overload can precipitate congestive heart failure, and pretibial,
perimalleolar, and pedal pitting edema should be observed. Arrhythmias are most
commonly observed during general anesthesia and are usually related to periods of
hypoxia or myocardial sensitivity to the anesthetic agent (halothane, enfluranel.
Consultation with the anesthesiologist is in order in patients with a history of significant
cardiac disease, and a recent chest X-ray and EKG are in order. In patients with acardiac
murmur, prophylactic antibiotics are indicated, and an updated echocardiogram may be
122 The Peri operative Patient Ch.5
useful pending cardiology consultation. In patients with a history of coronary artery
disease or eVA, elective surgery is avoided for at least six months following adocumented
myocardial infarction.
Postoperative nerve entrapment- can occur even after strict attention has been paid to
avoidance and protection of peripheral nerve, secondary to normal wound healing and
fibrosis effecting scar entrapment of the nerve trunk. This generally takes three weeks or
more to become symptomatic, as wound healing and fibroplasia progress. Sharp, burning,
shooting pain and paresthesia noted earlier in the postoperative phase may indicate
specific nerve trunk trauma due to sectioning, traction, or heavy-handed retraction
causing neuropraxia or intraneural hemorrhage.
Postoperative fever - is anticipated early on, especially following general anesthesia.
Fever is defined as a core (rectal) temperature of 37.8e (100Fl, or greater. Temperatures
of 38.3 e (101" F), or higher, indicate a major constitutional problem, and can result in
severe central nervous system damage. In searching for the cause of postoperative
systemic temperature elevation, considerations include: recent general anesthesia;
possibility of pulmonary atelectasis or aspiration, UTI, constipation; catheter sepsis (IV,
urinary); DVT and PE; wound infection or injury; drug reaction or serum sickness.
The physical examination should identify sites of inflammation and potential cause of
the febrile state. In addition to the clinical examination and discussion with the patient,
testing should include eBe with differential; urinalYSis; e&S of wound drainage or exudates,
urine, blood, oropharynx and sputum; and a chest X-ray.
The treatment of hyperpyrexia (fever> 38.5C) involves administration of antipyretic
such as acetaminophen or aspirin (600 mg PO Q6 h PRN)' and use of a cooling blanket. If
the patient remains hyperpyrexic and symptomatic, then consider discontinuing all
medication, consult infectious disease specialist, and re-evaluate the patient.
Chronological Sequence of Postoperative Temperature Alteration
Intraoperative & Elevated temperature due to malignant hyperthermia,
first 12 to 24 hours postop or typically postoperative hypothermia.
1st postop day Postoperative hypothermia, postanesthesia
overshoot, atelectasis I pneumonitis
2nd postop day Benign postoperative fever, urinary tract infection,
pulmonary, DVT
3rd postop day Wound infection, benign postoperative fever, and
constipation.
Any time in the postop phase Drug fever, catheter sepsis, transfusion reaction,
cold, orflu.
123 Ch.6 Fundamental Techniques and Procedures
FUNDAMENTAL TECHNIQUES AND PROCEDURES
SUTURE MATERIALS and WOUND CLOSURE
Sutures are used to reapproximate sectioned tissue, whether it is skin, superficial or deep
fascia, muscle, tendon or ligament, nerve sheath, blood vessel. or bone (stainless steel wire
[SSW]). The ideal suture material is strong enough to resist disruptive tensile forces, non-
allergenic and non-toxic, pliable enough to handle easily and to stay fixed once tied. Sutures
that communicate between the external surface of the skin, and the subcutaneous and/or
intradermal layers should also be inert, non-wicking, and easily removable after the tissues
have healed. The decision to use an absorbable or nonabsorbable suture material varies
with the specific requirements ofthe operative procedure.
Absorbable sutures-these are made of materials that break down in the tissues over
varying time periods, ranging from 1-10 weeks. Since most soft tissues, except tendon, heal
in 3-4 weeks, sutures that degrade at a rate that provides tensile strength up to 3-4 weeks
are commonly used in foot and ankle surgery. Classically, absorbable sutures were made
from sheep or beef intestine, and known as catgut. Plain gut can be strengthened by the
addition of chromium salts that slow down degradation by collagenase, or it can be
heat-treated to increase the rate of degradation (rapid gut). Although it is not likely, disease
transmission, such as bovine spongiform encephalopathy (mad cow disease). is possible
with catgut, which is a xenogeneic material. Although many surgeons prefer the behavior
of gut suture, monofilament or braided multifilament synthetic polymers comprise the
majority of absorbable sutures used nowadays. Synthetic polymers, such as polyglycolic
acid, lactic acid and caprolactone, are relatively inexpensive, non-reactive due to
hydrolysis rather than collagenase degradation, nontoxic and nonallergenic, and they
handle very well. Immunological reaction to synthetic absorbable suture is rare, however
when it occurs asterile abscess can form, and the material may not rapidly or fully absorb.
Monofilament absorbable sutures are often used in the deep tissues during delayed
primary closure of previously infected or contaminated tissues. Sutures range in size
(gauge). as defined by the US Pharmacopeia (USP). from #11-0 (smallest) monofilament
nylon used for ophthalmologic and neurosurgery, to #5 (largest) braided polyester used for
ligament repair. Some suture materials are also coated or impregnated with antimicrobial
agents, to minimize risk of infection.
Non-absorbable sutures-these are made of materials that are not degraded by the body,
such as silk, polypropylene, polyester and nylon, and are often used for skin closure (where
they can readily be removed after the skin has healed), or in tissues where prolonged
strength is require, such as tendon or ligament, or myocardium and blood vessel. Due to the
inert nature of many of these materials, there is less inflammation and less scar formation,
so they are often preferred for skin closure. Stainless steel wire can be used for
intraosseous suture, cerclage, and tension banding.
Suture needles-needles used for suturing are available in a number of shapes, namely:
half curved, quarter circle, 3/8 circle, 5/8 circle, compound curvature, and straight (Keith
needle). Separate needles with eyelets for threading suture are known as traumatic
needles. Atraumatic needles have the suture material swaged to the needle by the
manufacturer. Needles can also be smooth and round or oval. or they may have a cutting
edge on the concave surface of the curve, or on the convex surface of the curve (reverse
124 Fundamental Techniques and Procedures Ch.6
cutting needle). The body of the needle may taper toward the tip, or retain the dimension of
the body and form a blunttip (for friable tissue). The tip ofthe needle can be round, oval, or
diamond-shaped. Generally, a non-cutting, atraumatic needle is used for reapproximation
of friable tissues, whereas a cutting needle is often used for dense and durable tissues
such as fascia and joint capsule.
Suture (stitching) techniques 8nd remov81-some ofthe most common suture techniques
include the simple interrupted stitch (almost always applicable), horizontal and vertical
mattress stitches (excellent margin eversion, however can strangulate!. running and
running lock stitches, figure-of-8 stitch, baseball stitch, and the running subcuticular stitch.
Running subcuticular skin closures are usually reinforced with adhesive skin strips. Skin
sutures that are designed to be removed, are generally taken out according to the
following schedule: face 3-5 days, scalp or trunk 7-10 days, limbs 10-14 days, over a joint
14-20 days, plantar 20-22 days. Care of the operative site varies with anatomical location,
and wound healing progress. Stitch maneuvers suitable for tendon include the Bunnell,
Kessler, and other lateral trapping methods. Nonabsorbable multifilament sutures are often
used to reapproximate tendon to bone, and avariety oftendon anchors are available forthis
(see section on tendon transfers).
TIssue adhesive-cyanoacrylate ("liquid suture" or tissue glue) can be used as an
alternative to suture material for wound margin reapproximation where there is minimal
tendency toward margin disruption. Cyanoacrylate polymerizes when it comes in contact
with tissue fluid, forming aflexible adhesive bond between the wound margins. When used
for skin closure, cyanoacrylate is reinforced with adhesive skin strips.
BIOPSY TECHNIQUES
Incisionsl Biopsy-incisional biopsy removes only a selected portion of the lesion in
question, while an excisional biopsy removes the entire lesion (theoretically). Obviously, a
margin of supposedly "normal" tissue is excised around the lesion in question when an
excisional biopsy is performed. Actual pathological assessment of the margins of the biopsy
is necessary to determine whether a "clean" margin was created. When performing an
incisional biopsy, it is important to select representative portions of the lesion, and more
than one sample may be harvested. It is important to accurately identify the samples
relative to position aboutthe lesion, and adiagram is helpful in this regard. The pathologist
would also benefit from review of the diagram when dealing with a difficult lesion. The
surgeon should not struggle to procure a margin of normal appearing tissue in the
incisional specimen at the risk of missing representative lesion. Scabs, crusts, and
vesicles should be preserved in the specimen, and not destroyed in the surgical
preparation ofthe skin. Most skin biopsies can be performed under local anesthesia, and
dilute epinephrine (1:100,000 or 1:200,000 dilution) may aid hemostasis, if it is not
contraindicated in the particular patient. The local anesthesia should not be infiltrated
directly into the lesion, for fear of spreading potential malignancy or infection, although it
has been shown that direct injection below or through a lesion appears to cause no
significant microscopic alteration. The area is then prepped and draped in the usual s
terile fashion, prior to biopsy.
125 Ch.6 Fundamental Techniques and Procedures
Punch Biopsy-the punch biopsy is aconvenient and effective method of tissue extraction
and may be either incisional (usually), or excisional when dealing with alarge punch and a
smaller lesion. In the lower extremity, the 4-mm punch is typically employed, and standard
punch sets include punches ranging from 2-8 mm. It should be noted that removal of a
specimen <4 mm in diameter might allow the histological confirmation of atumor, however
it is generally considered inadequate for the accurate diagnosis of an inflammatory process.
When using the punch, the skin surrounding the lesion/s should be stretched taut,
perpendicular to the wrinkle lines before the circular punch is inserted. The punch is firmly
pressed downward into the lesion with a rotary back and forth cutting motion until it is well
into the subcutaneous tissue, thereby providing afull-thickness skin biopsy. To remove the
cylindrical specimen from the skin, gently grasp the biopsy plug with forceps, or a27-gauge
needle, and cut the base with scissors or scalpel and then place the sample into 10%
formalin. Simple pressure is adequate for hemostasis. A punch biopsy defect of ~ mm
diameter may require suture closure, whereas a defect <4 mm will heal via secondary
intention with adhesive skin strips and asterile dressing. A linear defect usually heals more
readily than a round defect.
Shave biopsy-the shave biopsy is used to remove that portion of the lesion elevated above
the plane of surrounding tissue and is useful for biopsy or removing many benign
epidermal growths. It is not indicated for biopsies of suspected melanoma, although it can
be used to identify the presence of malignancy without providing adequate tissue for
microstaging of a melanoma. However, it can be used as a convenient procedure for
diagnosis of basal cell epithelioma (basal cell carcinoma). The preparation is as noted
previously for biopsy, and a #15 blade is used to shave the lesion/s and a margin of
apparently normal surrounding tissue. The specimen is retained in 10% formalin. Pressure
is applied to effect hemostasis.
Curettage-curettage is a useful technique, distinguishable from the shave biopsy, for
removal of cutaneous lesions such as warts, seborrheic keratosis, and even malignancies
such as basal and squamous cell carcinomas. The curette is a spoon-like instrument with
a sharp rim. Typically, the 4-mm curette is used. A variation on this technique is
excochleation using a blunt instrument, such as a Freer elevator, when removing a lesion
that has a clear and separable margin with the adjacent normal tissue. An isolated verruca
is ideal for excochleation, as this provides an excellent specimen for biopsy and prepares
the base for ablative surgery (acid, cryogen, or laser).
Surgical excision-excisional biopsy should be considered whenever the lesion displays
active (spreading) margins and the border with normal appearing skin isto be surveyed, or
if the lesion is friable or very sclerotic, or whenever it is necessary to include full-thickness
skin to the level of, and including a portion of, the subcutaneous fat layer (e.g. in suspected
panniculitis, erythema nodosum, or melanoma). In theory, excisional biopsy is curative, and
may be used whenever excision of a lesion is desired. Local anesthesia is achieved as
described previously for incisional biopsy. With the exception of the smallest lesions 4
mm), the planned incisions should be marked on the skin. The most common technique
involves the use of two semi- elliptical incisions to create a wedge of intervening tissue to
be excised. The length of the ellipse should be three to four times the width, with the long
axis of the wedge parallel to crease lines and, therefore, RSTL. Surrounding margins may
be undermined in order to decrease tension with closure, and weight bearing on the
126 Fundamental Techniques and Procedures Ch.6
plantar skin should be avoided for 2-3 weeks, varying with the size of the wound and
progress of healing. When malignancy is suspected, it is importantto avoid contamination
of surrounding tissue planes with cellular elements of the lesion in question. A sarcoma
can often be adequately eradicated with wide excision, compartment resection, or
amputation. Violation of adjacent soft tissue barriers at the time of biopsy may make
subsequent definitive therapy more ablative than it originally need to have been. A frozen
section may be used to identify the presence or absence of tumor in aparticular specimen,
and perhaps yield identification of the specific type of tumor present. It is often difficult to
accurately identify the specific tumor from afrozen section specimen only, however the
presence of dysplasia and anaplasia can usually be determined. Afrozen section must be
planned with the pathologist and OR team. If a local excisional biopsy is performed, and the
frozen section pathology report yields adiagnosis of malignancy, then an adequately wide
excision should only be attempted for very small and well-defined lesions. By definition,
sarcomas are usually invasive and not differentiated from adjacent soft tissues. Carcinomas
localized to the skin may be more readily isolated and amenable to definitive excision and
eradication atthe time of excisional biopsy. Definitive treatment such as wide excision and
coverage with amuscle flap, or amputation, is determined by oncological consultation and
additional testing to ascertain tumor staging. Additional radiographs and CT scans of the
part as well as the lungs, MRI, and other tumor specific tests are often warranted. Adjuvant
radiation and/or chemotherapy may be administered both before and after definitive
excision, and is determined by the oncologist. Definitive surgery is planned and carried out
in a timely fashion. Plastic surgical consultation and co-management is often needed in
order to effectively cover the defect created by wide excision, and a free muscle flap
(serratus, or other suitable donor site) in conjunction with skin grafting may be indicated.
PLASTICSURGERV TECHNIQUES
Elective skin incision planning and execution-elective skin incisions should take into
consideration exposure of underlying target tissues, preservation of vital structures, and
relaxed skin tension lines (RSTL). As long as adequate exposure is not compromised, the
incision should be made parallel to RSTL. An incision made parallel to RSTL will be
subjected to less gapping tendency, and should therefore form less scar. RSTL run
perpendicular to the long axis of the extremity and vital structures. When a transverse
incision fails to yield adequate exposure, an incision that is oblique to RSTL is considered
betterthan one perpendicular to RSTL, with respect to gapping and scar formation. Difficulty
may arise when RSTL are in a transverse direction and the exposure needs to be
longitudinal, as in the case of excision of the plantar fascia for treatment of fibromatosis. In
such acase, azigzag incision can be used to effect longitudinal exposure while remaining
oblique to RSTL over the short segments of the zigzag.
Primary intention closure--involves direct wound margin reapproximation secured with
skin sutures. It results in immediate closure that seals with epithelium after 24-48 hours,
and usually results in afine-line scar. Primary skin closure requires wound margin mobility
that allows approximation ofthe edges.
Secondary intention closure-involves wound granulation, contraction and epithelializa-
tion, and slowly progresses over several days to weeks, depending upon local and
systemic factors. This is often the preferred method of closure following incision and
127 Ch.6 Fundamental Techniques and Procedures
drainage of an abscess or osteomyelitis, or when the wound presents chronic contamina-
tion and necrosis, such as ulceration in a debilitated patient.
Tertiary intention (delayed primary) closure-involves an initial period of secondary
intention healing, followed by additional surgical wound debridement and primary
intention suture closure. Primary, secondary or tertiary intention healing are the preferred
methods of wound closure, and should be attempted whenever clinically indicated.
Indications include a clean wound with beefy red granulations and resolution of
surrounding cellulitis and edema. Generally, other methods of closure, such as skin plasty,
grafts, and flaps, entail a greater risk of dehiscence, dysvascularity, slough or other
complication, and should be reserved for those cases where simpler methods are
deemed inadequate.
Skin Graftin/rskin grafts consist of epidermis and varying thicknesses of dermis. The graft
is said to "take" when it has successfully revascularized and effectively covered the
recipient site. The thicker the graft, the more difficult it is to achieve" graft take." Contrarily,
a thinner graft usually takes more rapidly. Moreover, thicker grafts are more durable and
contract less while healing, whereas thinner grafts are less durable and contract
considerably more. Skin grafts are mostfrequently autogenous, with the patient serving as
his/her own donor. For foot and ankle reconstruction, ipsi- or contralateral leg, thigh,
buttock, orthe anterior aspect of the abdomen, can serve as donor skin graft procurement
sites. Donor skin can be meshed to provide for larger surface coverage atthe recipient site.
Skin grafts can also be allogeneic (from another individual of the same species). xenogeneic
(the donor is of a different species, commonly porcine). or isogeneic (the donor is an
identical twin). By definition, agraft is detached completely when transferred from the donor
site to the recipient bed. There are 3 phases of skin graft healing (Table 6-1).
TABLE 6-1. PHASES OF SKIN GRAFT HEALING.
Phase lime period Key events
Plasmatic 24-48 hours Fibrin adhesion between
graft and recipient site
Inosculation 48-72 hours Microvasculature
traverses fibrin layer
Remodel/reinnervate 3 days to several months Collagenation, collagen
remodeling, reinnervation
Split-thickness skin can be thin, intermediate thickness, or thick. Athin
STSG measures 0.008-0.012 inches in thickness, while an intermediate graft measures
0.012-0.016 inches, and a thick graft measures 0.016-0.020 inches. Thin STSGs contract as
much 50-70%, and are often used as temporary coverage for large wounds. Intermediate
STSGs are most versatile and frequently used in coverage of foot and ankle wounds. Thick
STSGs only contract about 10-15%, however demand markedly increased recipient bed
vascularity, and have a higher risk of failure. Intermediate and thick STSGs can be used to
cover weight bearing and contact areas.
Full-thickness skin graft contains the entire epidermis and dermis,
including dermal appendages such as sweat glands and hair follicles. The subcutaneous
128 Fundamental Techniques and Procedures Ch.6
fat and superficial fascia are not included in a FTSG. FTSGs are very durable and contract
minimally, however take rather poorly in comparison to STSGs. AFTSG can be considered
for coverage of aweight- bearing surface, and can be harvested from apinch of skin over
the sinus tarsi, anterior ankle, or medial arch. The inguinal region and popliteal fossa are also
potential donor sites. Full-thickness pinch grafts consisting of skin from the sinus tarsi are
useful for coverage of small defects in plantar and contact areas of the foot.
The recipient site must be prepared in order to increase the rate of skin graft take,
and this should be done prior to harvesting the graft. The recipient site must be free of
fibrosis, necrosis, infection, and active hemorrhage. A beefy red, confluent granulation
tissue base is the ideal recipient surface. Bare tendon, bone, and cartilage are inadequately
vascularized for graft support, and a period of secondary intention healing is required to
allow for the formation of a granulation tissue surface. In cases involving large or deep
wounds, temporary coverage may be achieved with askin substitute (see below), prior to
subsequent autogenous skin grafting. After the recipient site is prepared, the autogenous
skin graft is harvested (procured) from the donor site manually using a Goulain or Humby
knife, or via use of a pneumatic powered Brown or Pagget dermatome. Although the graft
can be stored for up to 21 days in lactated Ringer's solution at 0-5
0
C. After procurement:,
attention should focus on getting the graft to the recipient site in a rapid (immediate) and
efficient fashion. The graft may be incised in afashion similar to pie crusting, wherein small
incisions are made to allow expansion and seroma drainage. For large recipient sites, the
graft may also be meshed, in a 1 :1.5 ratio using the graft mesher, in order to increase the area
of coverage and enhance drainage of wound transudate through the mesh incisions. Mesh
ratios of 1:3, 1:6, and 1:9 can also be achieved, however these ratios make for sparse
coverage of the recipient site and are only used when a large surface requires coverage.
After meshing, the graft is placed in contact with the recipient bed, maximizing contact and
eliminating dead space. The graft is then secured with several simple interrupted sutures
of 4-0 or 5-0 chromic gut at the margins. A small amount of excess graft may overlap
adjacent intact skin margins. The graft-recipient interface is then secured with atie-over
stent dressing. The tie-over stent dreSSing employs fine-mesh nonadherent gauze placed
directly over the skin graft, followed by coverage with fluffed gauze or mineral oil
impregnated cotton balls, then covered with aflat gauze barrier secured with evenly-spaced
silk sutures that convey gentle pressure overthe graft. In many cases, immobilization and
non-weight bearing are indicated, and the graft is typically not disturbed until 5-7 days. The
graft donor site is dressed with nonadherent gauze, after assuring hemostasis (topical
thrombin spray can be used), and redressed when the recipient site is inspected.
Application of a wound dressing consisting of porcine-derived extracellular collagen,
elastin, glycosaminoglycan, and glycoprotein (such as Oasis), can enhance donor site
healing. Complications related to skin graft healing usually develop secondary to disruption
of the graft-recipient interface with resultant failure to achieve revascularization. Causes
include seroma formation, infection, and inadequate immobilization. A dysvascular
recipient site is doomed to failure. Failure to achieve inosculation results in graft necrosis,
and this usually leads to contamination and subsequent infection if appropriate treatment
(debridement, antibiotic therapy, and revision) is not initiated. Reverse dermal grafts are
sometimes used for nail bed reconstruction, and require inverting an intermediate STSG
prior to application to the recipient bed.
Skin substitutes-a number of options exist for skin coverage that do not involve
harvesting autogenous skin. These materials typically employ combinations of collagen,
129 Ch.6 Fundamental Techniques and Procedures
glycosaminoglycan (GAG), silicon elastomer, and water. One such option (integra) is a
bilayer skin substitute that consists of a biodegradable type I collagen-GAG co-polymer
dermal analog combined with an epidermal analog consisting of a thin silicone polymer
that behaves in afashion similarto normal skin. The cross-linked collagen and GAG matrix
maximizes cellular in growth and degrades in a predictable fashion. After neodermis
formation, the silicone epidermal analog is removed and replaced with athin STSG.ln some
cases, use of the bilayer skin substitute obviates the need for subsequent use of an
autogenous skin graft. Other skin substitutes include combinations of keratinocytes and
fibroblasts, harvested from neonatal foreskin or xenogenic sources, in acollagen matrix, and
these are often used in the treatment of large cutaneous wounds such as those due to
burn injuries.
Skin flaps--f1aps differ from grafts in that avascular pedicle is maintained or, via micro-
surgical reanastomosis, reconstructed. Flaps are defined as either local or distant In the
foot and ankle, defects larger than 2.5 cm
2
are generally covered with a skin graft, while
smaller defects are amenable to use of a local skin flap. Flaps are advantageous for full
thickness defects, poorly vascularized recipient wounds, and coverage of bony prominence
or contact areas. Sensation can also be restored when an innervated flap is used. Skin
flaps are classified according to their blood supply. Random pattern skin flaps are perfused
bythe random dermal-subdermal plexus of vessels, and require apedicle width equal to the
length of the flap. The Z-plasty and V-Y plasty are techniques that create random pattern,
local, rotational or advancement skin flaps. Axial pattern skin flaps are supplied by an
identifiable (Doppler) cutaneous artery, such as the lateral calcaneal artery flap used to
cover heel defects, or the sural artery flap used to cover Achilles tendon defects, and can
be rather long in comparison to the pedicle width. Axial pattern flaps can be of the island
design, or actually distant flaps when the vascular origin is sectioned and later
reanastamosed at the recipient site.
Local flaps-these are mobilized from adjacent skin, and are of either the rotational
or advancement type. Rotational flaps are semicircular and are mobilized about apivot
point where the flap is attached to its pedicle. Alarger semicircle imparts less tension
on the pivot, and tension can be alleviated at the pivot by means of a back cut or
creation of a Burrow's triangle. The single and bilobed rotation flaps are commonly
used for coverage of small pedal skin defects. Advancement flaps are mobilized via
direct extension without rotation, and include the V-V, V-v. single, and bipedicle flaps.
Distant flaps-these originate from a vascular pedicle in one area of the body and,
via maintenance of the pedicle or sectioning with subsequent microvascular
reanastomosis, are used to cover a remote defect For example, a crossed leg flap
uses skin mobilized from the contralateral calfto cover a pedal defect; or asection of
latissimus dorsi, complete with its arterial supply and overlying fascia and skin may be
harvested to cover a pedal defect. In the crossed leg technique, the calf donor skin
remains attached at its pedicle while the legs are skeletally fixated and the flap sutured
to the contralateral pedal recipient site. Once the flap has healed and attached to the
recipient bed, the donor side pedicle is sectioned and the skeletal fixation removed.
Currently, it is more common to use the microvascular free flap, rather than the crossed
leg method. The serratus free flap is commonly used by plastic reconstructive
surgeons to cover large pedal defects, and requires microvascular reanastomosis
and coverage ofthe muscle with aSTSG.
130 Fundamental Techniques and Procedures Ch.6
Skin plastiBtr-these employ local flaps and are used to redirect skin, and alter skin tension
and volume. Scar tissue and contracture can be redirected and lengthened with the
Z-plasty (Figure 6-1), The arms of the Z are of equal length, with the apices forming a 60
angle, in order to achieve approximately 75% increase in skin length with resultant
decreased tension, Multiple Z-plasties, resulting in a W-plasty, can be used to further
elongate skin and relieve tension, The V-V plasty results in skin lengthening after flap
mobilization, The skin defined by the V-incision is mobilized and elongated, and the
resultant wound is sutured closed in the shape of aY. As a rule, the wider the V's base, the
greater the vascular pedicle, Skin can also be shortened or reduced by means of a V-V
plasty. Redundant skin can be excised via the creation of an elliptical wedge using two
semi-elliptical skin incisions, This is often useful in digital surgery, in particular when
derotation of afrontal plant deformity is desired (Figure 6-2), Fasciocutaneous flaps are
useful in the leg, in particular for coverage of defects about the Achilles tendon. Muscle
flaps are useful for coverage of weight bearing or contact areas of the foot and ankle, and
convey excellent vascularity and provide a robust base over which skin can grow.
Identification and preservation ofthe muscle's vascular supply is critical to the success of
the flap, The heel and first metatarsal head area are amenableto coverage with FDB and/or
FHB (Figure 6-31, the medial and lateral malleoli with abductor hallucis and abductor digiti
minimi, respectively,
~
------ ------
60
Figure 6.1
;,'"
Figure 6.2
131 Ch.6 Fundamental Techniques and Procedures
Figure 6.3
BONE GRAFTING AND ORTHOBIOLOGICAL AGENTS
Bone grafting may involve transplantation of viable bone that is expected to remain viable
in the recipient host, whereas implantation implies transfer of non-living bone or tissue
(freeze-dried bone) to the host recipient bed. An autograft originates in the recipient host;
an isograft originates in an identical twin; an allograft or homograft is viable bone
originating in a donor of the same species, while an alioimplant or homoimplant is non-
living bone from the same species; and xenograft or heterograft (or implant) implies bone
from a donor of another species (and are not recommended for general use). Autogenous
bone grafts are advantageous because of immunocompatability and transfer of
osteoconductive (trabeculae and porous channels), osteoinductive (chemotactic and
transformation factors), and osteogenic (viable cells) properties. Disadvantages
associated with autogenous bone grafts pertain to creation of stress risers at the donor
site with potential for fracture, as well as creation of another surgical wound that is
subjectto potential hematoma, infection, or other wound complication. Moreover, the host
may not have adequate bone to donate, and the osteogenic quality varies with site and
age. Autogenous bone is favored for use in the repair of failed unions, previous infection,
or donor site/host morbidity. Allogeneic bone is suitable for orthotopic use, backfill of donor
site void, and in cases wherein donor bone is limited or harvest thereof is contraindicated.
There are 3 physiological elements critical to bone graft healing, including:
1) osteoconduction, 2) osteoinduction, and 3) osteogenesis (Table 6-2). Osteoconduction
pertains to the porous nature of trabecular bone, which provides the scaffold upon which
cells migrate and reside. Osteoinduction pertains to the chemotactic and differentiating
---------------------
132 FundamentalTechniquesand Procedures Ch.6
influencethatbonemorphogeneticprotein,andothergrowthfactors,hasonbonegrowth.
Osteogenesis pertainstothe bone generating properties ofundifferentiatedstem cells,
osteocytes and chondrocytes (via enchondral boneformation). Autogenousbone grafts
can take the form of cancellous, cortical, or corticocancellous bone Table 6-3. More
specifically, bone grafts function in the treatment of delayed union, nonunion and
pseudoarthrosis;to augmentskeletaldefectscreated bytrauma orsurgery,suchastofill
avoid aftercancellous bone biopsyor cystevacuation;tofacilitate arthrodesis andto
effect bone block limitation of motion; and to enhance reconstruction by means of
osteotomy,as withthe Evan'slateralcalcaneal(column)lengthening,orinthe repairof
brachymetatarsia. To acertain degree, restoration of segmental bone defects using
autogenousbonegraftshas beenreplaced bymeansofcallusdistraction,andthe useof
bonegraftsubstitutes.
TABLE 6-2. PHYSIOLOGIC PROCESSES OF BONE GRAFT HEALING.
Process
Osteoconduction
Osteoinduction
Osteogenesis
Elements and function
Pores(10-1000microns)that
mimiccancellousbone;
scaffoldforbone growth
Bonemorphogenetic
proteins2&7, platelet-
andfibroblast-derived
transforminggrowth
factors;recruitand
transformmesenchymal
Livingosteocytes,
osteoblasts,chondrocytes,
chondroblasts,andundifferentiated
mesenchymalstemcells
Source
Cancellousbone,bioceramics
(CaP04,GaS04),hydroxyapatite
(corallineandnaturalcoralgrafts),
extracellularmatrixscaffolds
(collagenorGAG +HA+TGP)'
polymers(PGA),alloys(TI)
Autogenousbone,allogeneic
stemcellsorrecombinant
demineralizedbonematrix,
autogenousplateletrich
plasmaorbonemarrowaspirate
Autogenousbone,fresh
marroworcloned cells
TABLE 6-3. STRUCTURAL TYPES OF BONE GRAFTS.
Structure Graft characteristics
Cortical Dense,compactbonecontainingfewviablecells;providesstable
graftthatcanbesecuredtosurroundingbonewithfixationdevices
Cancellous Spongybonecontainingviablecellstostimulate
osteogenesisandrapidincorporation;nostructuralstrength;
excellentback-fill
Corticocancellous Providesstabilityandosteogenesis;includesgraftssuchas
thoseharvestedfromthecalcanealbodyandiliaccrest;
excellentreconstructivegraft
Harvesting bone graft-whenharvesting an autogenousbone graft,plentyofirrigationis
usedforcoolingduringosteotomyinanefforttopreserveviablecells.Asharposteotome
isidealforharvestingautogenousbonegraft.Thegraftisprocuredand placedin asterile
133 Ch.6 Fundamental Techniques and Procedures
container and covered with asaline moistened sponge. The graft should not be submerged
in saline solution. Prophylactic antibiotic therapy should be used whenever bone grafting
is planned. The graft is usually harvested from the ipsilateral lower extremity. Suitable sites
for harvesting autogenous bone graft material include the iliac crest, greater trochanter,
proximal and distal tibia, calcaneus, fibula (midshah is almost all corticaU. and rib. Donor site
morbidity is anotorious complication. and occurs in up to 25-45% of cases wherein the iliac
crest is used to procure autogenous corticocancellous bone, and pain atthe donor site has
been reported to last up to 5years postoperative. Furthermore, the use of autogenous bone
increases operative blood loss, duration of anesthesia and surgery, wound complications
related to asecond operative site, including nerve entrapment.
Healing ofbone grafts..-.-bone graft healing requires mechanical stability, vascularity, and
close contact between the graft and recipient site. Incorporation takes place by means of
creeping substitution between viable bone and graft. Chondrogenesis and angiogenesis
take place by 5-7 days, and calcification occurs by 10-14 days, and osteoblasts lay down
osteoid from 15-50 days. Vascular in growth occurs over an approximately 2 cm distance
by 6-10 weeks, while mineralization occurs over approximately 1 cm in that same time
period, and it takes about 3-4 months to fully mineralize. Non-weight bearing may be
required for 3-4 months, and electrical or low-intensity ultrasonic bone growth stimulation
may be helpful. Complications of bone grafting include afailure rate reported to be 15-20%.
Failure to incorporate is usually due to inappropriate application or graft selection, and
mechanical instability. Whenever grafting anonunion site, or in cases involving pnorwound
sepsis, an autogenous graft is preferred. Allografts and alloimplants function best as a
spacer for in growth of vessels and new bone. Allografts and alloimplants may convey
immune incompatibility in rare cases, however they are sterile and readily available with-
out creating another wound in the host tissues. Composite bone grafting employs both
autogenous and allogeneic graft materials.
Bonegraftsubstitutes-alternatives to autogenous bone alone include: 1) extenders, which
consist of osteoconductorthatserves to increase the volume of graft in addition to the usual
autogenous graft 2) enhancers, which consist of osteoconductor and
osteoinductor, and serve to expand volume and recruit stem cells; and 3) substitutes, which
convey osteoconduction, osteoinduction, and osteogenesis, and replace bone.
Osteoconductors serve to mimic trabecular bone, with pore sizes that range from 100-1000
microns. These are available in different forms, and vary in strength ranging from weak
tricalcium phosphate and calcium sulfate (more porous, rapidly incorporation) to stronger
(more dense, slower incorporation) coral hydroxyapatite and calcium carbonate. The pores
serve as a scaffold upon which stem cells and blast cells adhere, and capillary in growth
is promoted. These are often sterile and noninfectious and nonimmunogenic, if totally
synthetic. However, they are usually combined with allogeneic material to induce bone
healing. Osteoinductors include demineralized bone matrix (OBM), which contains
chemotactic BMP 7 (osteogenic protein 1) and BMP 3 (osteogenin); as well as
transforming growth factor 13, which converts undifferentiated stem celis to chondro- and
osteoblasts; as well as other growth factors (insulin-like GF, fibroblast GFs, platelet-derived
GF, granulocyte colony stimulating factor, and others). These are antigen-extracted
allogeneic, and treated with either electron beam or gamma ray sterilization. Combinations
of osteoconductor with osteoinductor come in different forms, including crunch (OBM +
cancellous chips), flexible gel strips and sheets, paste, and putty. Osteogenesis requires
134 Fundamental Techniques and Procedures Ch.6
mesenchymal stem cells, chondroblasts (enchondral bone formation), fibroblasts
(collagen), and osteocytes. A bone marrow aspirate, preferably from the proximal tibia,
femur or ilium, can be obtained by aspirating with aJansheedy needle in 4cc increments,
with sequential advancement across the metaphysis; or aspirate 2or more separate sites
and centrifuge to concentrate the MSCs.
SELECTED ENDOSCOPIC TECHNIQUES
Endoscopy involves the use of fiberoptic cameras and small surgical instruments to
evaluate and treatthe intra-articular and periarticular components of a joint as well as
other corporeal spaces. Endoscopy has been shown useful in the ankle, however subtalar
and metatarsophalangeal arthroscopy can also be undertaken. Moreover, endoscopic
plantar fasciotomy has been shown to be useful is certain cases of recalcitrant plantar
fasciitis and heel spur syndrome, and it has been experimentally used for sectioning of the
deep transverse intermetatarsalligament in the treatment of intermetatarsal neuroma, as
well as neurectomy and tarsal tunnel decompression. The value of endoscopy in making an
accurate diagnosis of joint (ankle) pathology is well-established. Arthroscopy is indicated
when CT and MR imaging remain equivocal, or when these studies indicate the need to
biopsy or manipulate intra-articular structures. Endoscopic techniques have advanced a
great deal in the past 35 years, and the application of fiber optics, smaller systems, and
intra-articular laser ablation have contributed to newer approaches to long recognized
pathologies such as joint instability and cartilage degeneration.
Ankle arthroscopy-this can be used in both acute and chronic conditions of the joint. As
with any surgical intervention, proper patient evaluation (H&P) is prerequisite to
arthroscopy. Clinical lab testing, including CBC and differential, ESR, rheumatoid factor, and
other indicators of arthritis may be indicated. Non-invasive imaging and testing includes
standard and stress radiographs (anterior drawer, inversion stress) radiographs, CT scan,
MRI, bone scan and/or other radionuclide imaging, and possibly an arthrogram ortenogram,
may be indicated prior to making the decision to intervene arthroscopically. The potential
benefits of arthroscopic intervention must be weighed against the potential complications,
and the potential benefits of open arthrotomy should be considered. In general,
arthroscopic indications increase with the skill ofthe surgeon, however adequate exposure
and completion of the job at hand should not be compromised by the decision notto open
the joint in atraditional fashion. Complications related to arthroscopy are the same as those
of open surgery, however there is potentially less likelihood of infection and damage to
surrounding vital and connective structures. This, in turn, implies the potential for less joint
fibrosis and a faster rehabilitation. Infection, nerve injury and RSOS, excessive joint
distraction, hematoma, phlebitis, recurrent deformity and/or pain, and painful scar have
been encountered following arthroscopic surgery.
InstrumentBtion for ankle arthroscopy-small joint arthroscopic instruments have improved
a great deal since their introduction in the late 1970s. The arthroscope consists of an
eyepiece and alens that is introduced into the joint Fiberoptic systems enable the confines
of the jointto be explored and viewed videographically. Cannulas serve as portals through
which instruments, the video camera, and a light source are passed. Power instruments
include osteotomes, shavers and abraders; and more recenttythe laser and radiosurgical
instruments. Hand instruments include osteotomes, probes, curettes, knives, punches,
Ch.6 Fundamental Techniques and Procedures 135
rasps, forceps, staplers, suture drivers, and magnetized rods. Adjunct instruments include
distractors, both invasive and noninvasive, and the pressurized distention system.
Atthroscopic ankls anatomy-anatomic considerations pertinent to ankle arthroscopy
include topographical landmarks and internal joint structures. Vital structures, including
vessels and nerves, as well as the tendons and ligaments about the ankle are marked on
the skin surface. Portals of entry for the ankle include: anteromedial, anterolateral,
anterocentral, posterocentral, posterolateral, and accessory portals (Figure 6-4). The
posteromedial portal is avoided for fear of neurovascular injury. The posterocentral portal
perforates the Achilles tendon. Ankle anatomy is subdivided into anterior and posterior joint
pouches. The anterior joint pouch contains the medial, anterior, and lateral gutters. The
medial gutter contains the medial malleolus, medial margin of the talus, anterior talotibial
ligament lthe floor of the medial gutter), and the posterior talotibial ligament (seen upon
application of valgus stress). The anterior gutter (anterior ankle) contains the anterior
tibial margin (lip), medial ankle bend, medial talar shoulder, tibial synovial recess, tibial
plafond, tibial capsular reflection, talar sagittal groove, lateral talar shoulder, tibiofibular
synovial recess and synovial fringe, and the anterior-inferior tibiofibular ligament. The
lateral gutter contains the lateral talar articular surface, medial fibular articular surface,
anterior tibiofibular ligament (ATFL), and the posterior talofibular ligament (seen upon
application of varus stress). The posterior joint pouch, when viewed through the sagittal
groove, contains the posterior tibiofibular ligament, posterior capsular surface, medial ankle
bend, medial gutter, and the posteriortalar dome. When viewed through the posterolateral
portal, the posterior joint pouch contains the posterior tibial margin (lip), posterior talar
dome, talar sagittal groove, posterior tibiofibular syndesmotic ligament. labrum media ankle
bend, medial malleolus, and the posteriortibiotalar ligament.
Ankle arthroscopy allows the surgeon to address awide range of joint pathology (Table
6-4). Soft tissue maladies amenable to arthroscopic inspection and manipulation include
meniscoid ligaments (Collin's lesion), capsular adhesions, fibrous bands, and synovitis.ltis
possible to do an adequate ankle synovectomy in patients with rheumatoid arthritis,
entirely via the arthroscope. The articular surface may be treated for chondromalacia,
subchondral erosion, and other chondral defects. Amenable bone pathologies include
:PlW'lt.iI+-Anteromedial
Anterolateral
Posteromedial
Figure 6.4
136 Fundamental Techniques and Procedures Ch.6
osteochondral lesions and subchondral bone cysts. Other pathological ankle conditions
amenable to arthroscopic intervention include transchondral talar dome injuries, avulsion
fractures of the medial, posterior, and lateral malleoli; ligamentous and capsular repair;
talotibial exostosis, fractures of the tibial bearing surface and margin (lip); foreign body
retrieval, joint biopsy, and ankle arthrodesis (perhaps in conjunction with atrans-Achilles
portal, medial malleolar osteotomy, and cannulated screw fixation), can be undertaken by
means of arthroscopy. Although applicable to the treatment of many conditions of the ankle,
arthroscopy is particularly useful in the treatment of osteochondral defects and torn
cartilage. Because small portals are used to access the joint, recovery after arthroscopy is
often more rapid than that following open arthrotomy, and complications are generally
considered to be less likely. It may be possible to repair talar dome and tibial bearing
surface fractures without osteotomizing the malleoli. Despite the use of smaller incisions,
ankle arthroscopy still conveys a risk of infection, hematoma, nerve injury, and damage to
intact articular structures, and there are associated risks related to anesthesia and
tourniquet use. The postoperative course may involve non-weight bearing and
immobilization, depending upon the specific reconstruction undertaken, however early
return to weight bearing and ROM rehabilitation exercises are the norm.
TABLE 6-4. CLASSIFICATION SYSTEMS FOR CHONDROMALACIA.
System
Collins
Goodfellow
Bauer & Jackson
Subcategories
Grade I
Grade II
Grade III
Grade IV
Superficial Type I
Type II
Type III
Type IV
Deep Type I
Type II
Type III
Type IV
Type 1
Type 2
Type 3
Type 4
Type 5
Type 6
Description of cartilage defect
Fraying
Fi brillation and fissure
Deep, extensive fissure
Full thickness defect
Shallow erosion
Loss of superficial layer
Exposed subchondral bone
Exposed deep matrix
Cartilage softening
Blister formation
Exposed matrix
Exposed bone
Linear crack
Stellate fracture
Rap defect
Avulsion with exposed bone
Fibrillation
Fibrillation & subchondral erosion
Like most surgical maneuvers, arthroscopy requires training and repetition to become
fluent and successful in its application. After achieving satisfactory surgical anesthesia,
instrumentation is delivered into the joint via tubes placed through the small incisions, at
various locations about the ankle. Typically, the arthroscope, various instruments, and
suction are employed simultaneously. Specific operative interventions include joint
inspection, chondroplasty, synovectomy, biopsy, fragment excision, subchondral bone plate
perforation or microfracture, instillation of medications, graft and suture placement,
application affixation devices, and other maneuvers as indicated by the pathology at hand.
137 Gh.6 Fundamental Techniques and Procedures
Specific procedures amenable to arthroscopic application include: debridement and
fragment removal for repair of anterior ankle impingement, excision of osteochondral
fragments, abrasion chondroplasty, excision and repair of anterolateral gutter meniscoid
ligament, and release of posttraumatic arthrofibrosis.
Most ofthe time, patients are positioned supine, with the ipsilateral knee flexed at 90,
for ankle arthroscopy, although the specific position can vary with the needs of the
procedure and anesthesia. The joint is usually distracted H.5 mm) using the sterile
noninvasive foot strap and approximately 25 pounds of tension. Distraction forces >30
pounds, or for periods> 1 hours, may cause dorsal cutaneous and/or anterior ankle
neuropraxia, although this can result from even lesser force and duration, and each patient
should be assessed forthis in follow-up after the anesthesia has subsided. An ingress pump,
setto 45-50 mm Hg pressure, and egress suction can be used to maintain acontinuous flow
of saline through the articular cavity. The egress line may be fitted with a filter to procure
particulate matter flushed from the joint during the arthroscopic procedure. The 2.7 mm
arthroscope is ideal, however a 4 mm arthroscope can also be used. The 3.5 mm shaver
works well in most cases of ankle arthroscopy. The instruments are introduced to the
articular cavity by means of a transdermal incision made with a #15 blade scalpel. The
scope is usually positioned, initially, through an anteromedial portal situated medial to the
tendon of tibialis anterior at the level of the tibiotalar interface. Gare should be taken to
avoid injury to the large saphenous vein and nerve. After penetration of the skin, an
18-gauge needle is used enter the joint, and saline is infused through this cannula. After
instilling saline into the joint, an anterolateral portal, situated immediately lateral to the
intermediate dorsal cutaneous branch of the superficial peroneal nerve and the tendon of
peroneus tertius, is made using the scalpel and 18-gauge needle. It is helpful to tent the
soft tissues and to transilluminate the skin and subcutaneous tissues with the arthroscope,
in order to inspect for the course of any nerve in the area of the planned placement of the
anterolateral portal. After making the standard anterior portals, a systematic inspection of
the articular cavity includes identification ofthe deltoid ligament and medial malleolus, the
joint space between the talar dome and the medial malleolus (medial gutter), the dome of
the talus, the distal tibial bearing surface, the anterior joint cavity (anterior gutter), and the
syndesmosis between the distal tibia and fibula (anterior talofibular ligament, anterior and
posterior tibiofibular ligaments, and the associated talar and fibular articular surfaces).
The endoscope (small arthroscope) can also be used to inspect and manipulate other
joints and cavities in the foot, including the STJs, first metatarsophalangeal joint,
pre-Achilles space, intermetatarsal spaces (sectioning of the deep transverse
intermetatarsalligament)' proximal plantar fascia (endoscopic plantar fasciotomy), and
other areas depending upon the surgeon's skills and the patient's needs. Generally, the
diagnostic and therapeutic benefits related to implementation ofthe endoscope diminish as
the joint or cavity decreases in size, primarily due to technical limitations related to the size
of the instrumentation and the surgeon's skills.
LASER SURGERY
A variety of surgical lasers are used today, however the G021aser remains the mainstay in
cutaneous and musculoskeletal surgery in the foot and ankle. Fundamental physical
properties of laser surgery are based on Planck's quantum mechanics and Einstein's
stimulated emission theories. LASER stands for Light Amplified Stimulated Emission
Radiation. Laser light is monochromatic and coherent, wherein all ofthe light waves line up
138 FundamentalTechniques and Procedures Ch.6
so that the peaks and troughs are equidistant in space and time. The laser beam
(electromagnetic radiation)is characterized byitsfrequency(Hz, or cyclespersecond),
wavelength(nanometers),timeofapplication(millisecondstopicoseconds),powerdensity
(watts per cm2), and amount of energy delivered to the tissues (joules, or watts per
second).The coherent lightis collimated bythe fiberoptic orarticulated arm delivery
system. and can be aimed bythe operator. Thetime ofexposure to the laserbeam is
controlledbygatingthedeliverysystemtoallowpassageoflightas acontinuousbeam,a
single pulse,orrepetitive pulsesvaryingfrom millisecondsto picoseconds.The interval
between pulsesallowsthetissuetodissipate energyas heat,withthe minimalthermal
relaxation ratio being 1:10 on:off.1issueabsorptionvaries primarilywiththewavelength
andtissuetype,whereinlightwithashorterwavelengthhashigherenergy,andtherefore
penetratesdeeperor createsmore heatinthe sametissue. The specificwavelength is
determined bythe specific elementorelements used in the"active lasing media." The
lasing,oractivemediamaybe C02(withheliumandnitrogen),orNd-VAG (neodymiumwith
yttrium,aluminumandgarnet),orotherelementalgases.1issueinteractionwithlaserlight
varies from one tissue type to another. For instance. skin and softtissue may readily
vaporize, while bone and cartilage heat up and their protein content denatures with
resultantnecrosis,in responsetothesame laserbeam.Itisthereforeimportanttoselect
theproperlaserandsettingsforthetissuebeingmanipulated.Infootandanklesurgery,the
avarietyoflasersmaybeuseful(Table6-5).
TABLE 6-5. TYPES OF LASERS USED IN FOOT AND ANKLE SURGERY.
Laser
C02
Holmium-VAG
non-contacttip
Nd-YAG non-contacttip
Nd-VAG contacttip
KTP(potassium,
titanium,phosphate)
non-contacttip
KTP contacttip
Argon non-contacttip
Cu vapor.non-contacttip
Characteristicsand applications
Farinfraredwavelength,readilyabsorbedbywaterand
thereforeonlyusedforsuperficial(0.1 mm)penetrationsuch
ascutting,ablation,andcoagulationofskinandnaillesions
Middleinfraredwavelength,absorbedbyboneand
cartilage.penetrates0.4-0.6 mm,andusedforlesion
ablationinmoredensetissue
Nearinfraredwavelength,poorlyabsorbed,penetrates
6-8 mm,deeplesionablationandcoagulation
Nearinfraredwavelength,penetrates5-200 microns,
superficialcuttingorincision
532micronwavelength,absorbedbydermalvesselsand
superficiallesionssuchasverrucae,penetrates0.5 mmin
pigmented skinandupto4mminnonpigmentedskin,
usedforablation
Penetrates1-2 mm,usedforincisingskin
488-514 micronwavelength,penetrates0.5-1 mm,absorbed
bydermalvesselsandsuperficialskin lesionssuchas
verrucae,usedforablationofdermallesions
478 micronwavelength,penetrates0.5-1 mm,absorbedby
dermalvesselsandsuperficialskinlesions,usedforablation
ofdermallesions
139 Ch.6 FundamentalTechniquesand Procedures
Safety with lasem-Iaser safetyentailsspecialattentiontoinstrumentation,eyeprotection
and personal shielding, vapor evacuation and filtration, and aiming technique. ANSI
publication 136.3 serves as astandard reference for laser safety. Specific eye safety
precautionsvarywiththewavelength ofthe laserbeam asfollows:
Class I-directvisualizationofthebeamdoesnotcauseoculardamage
Class II-prolongeddirectvisualizationwillcauseoculardamage
Class III-directvisualization causesimmediateoculardamage
ClassIV-directvisualizationcausesimmediate,severeoculardamagerangingfrom
corneal burntoretinalablationand blindness
All medicallasersare categorized as Class IV. Theypose afire hazard, damagethe
unprotectedeye,andareharmfultounprotectedskin.Damagingeffectscan be caused by
directorreflectivelaserexposure.Smokeplumeevacuationsystemsshouldentailvacuum
suctionatthepointofcreation,and0.2microndualfiltrationwithcarbon. Personnelinthe
OR shouldwearproperbodyand eye protection,and afiltrationmask.The doortothe OR
mustindicatethe presenceofthemedicallaserpotentialhazard.
Specific laser procedures-surgical lasertechniquesareusedprimarilyforlesionablation
andsofttissuedissection(Table6-6).Aswithanyotherformofdissectionortissueablation
(scalpel, radiosurgery, cryotherapy, coblationl.violation ofthe dermis results in tissue
repairwithscarformation.lncisionsaremadewithafocusedbeamdirectedinarepetitive,
linear fashion. Lesion ablation is achieved with a defocused beam directed in a
cross-hatched linear or back-and-forth fashion, or in an ever-increasing radial circle
fashion beginning centrallyinthe lesion.Periodiccurettagemayassistlesionablation,as
non-vaporizedescharmayaccrue.Itshouldbenotedthat,withtheexceptionofskinlesions,
lasers are generallyused to assistwith dissection and lesion ablation, while standard
techniquesofdissectionand arthroscopyare employedto expose lesionsand underlying
target structures. Patients should understand this concept of "laser assisted" surgery.
Appropriate lesion biopsyshould be obtained priorto laserablation. Appropriate sterile
bandage,withtopical application ofsilversulfadiazine cream, and follow-up are partof
theaftercare.
TABLE 6-6. COMMON LESIONS AND PROCEDURES AND APPLICABLE LASERS.
Lesion
Verruca
Cavernoushemangioma
Hypertrophicscarorkeloid
Tattooremoval
Cutaneousgranulomatouslesion
Nailmatrixablation
Synovitis,scar,chondromalacia,osteophyte
Laser
C02, Argon,Nd-Vag,KTP
Nd-VAG barefiber
C02
C02
C02
C02,Argon,Nd-VAG
Holmium-VAG
140 Fundamental Techniques and Procedures Ch.6
MICROSURGERY
Microsurgical techniques are valuable when manipulating peripheral nerves, veins and
arteries. These techniques can be used in cases of trauma, peripheral neurosurgery
(neuroma, tarsal tunnel, nerve entrapment), plastic reconstructive surgery (flaps), or
whenever magnification ofthe surgical field is desired. Magnification can be achieved with
the operating microscope (4-30x) or, more typically, by means of loupe magnification
(2.5-16x). Loupes also enhance inspection of the surgical field when foreign body
exploration is undertaken. Microsurgical instruments, namely forceps, scissors, and
needle holders, enhance the surgeon's ability to manipulate structures under magnification.
Typical suture gauges include 7-0 to 9-0 nylon. Specific vascular and neurological repair
techniques are learned and practiced in residency and fellowship training, and
microsurgical techniques courses.
SELECTED TENDON LENGTHENING AND TRANSFER PROCEDURES
Balance of muscle power-all of the joints of the foot and ankle are influenced by the
muscle-tendon units that cross each joint The ultimate position of afunctional joint, both
at rest and during function, is determined primarily by the forces created by the muscle-
tendon units acting upon the joint. An accurate clinical assessment ofthe strength ofthe
muscle(s) in question must be documented. Every time a muscle-tendon unit is
manipulated (transferred), there is a change in the overall balance of the joint. To
effectively restore function, deforming influences must be removed and it may be
necessary to stabilize (arthrodesis) deformed or dysfunctional joints upon which the
transferred tendons can work (e.g. it is common to combine triple arthrodesis with major
tendon transfers crossing the ankle). Furthermore, there is only a fixed amount of power
available to influence a joint, and the total amount of power cannot be increased via
transfer. One can expect at least 1/2 grade decrease in strength fol/owing tendon transfer
(see manual muscle strength testing, in the section describing diagnostic techniques).
Rarely would a muscle weaker than grade 4 be considered for transfer, unless another
tendon transfer augments it. Only a muscle-tendon unit of satisfactory strength and range
of contraction is suitable for transfer.
Muscle and tendon anatomic and physiologic factors-see Chapter 1
AtraumBt;c tendon surgical methods exist for handling tendon, all of
which are meant to enhance healing and ultimate function. These include:
A. Maintain tendon moisture (avoid desiccation)
B. Prepare the recipient site for transfer prior to harvesting the tendon;
C. Establish physiological tension in the transferred tendon (See Blix curve);
o. Use available, naturally occurring tendon sheaths and retinaculae to direct and
maintain the course of the transferred tendon;
E. Preserve the vascular supply to the transferred tendon by avoiding excessive
traction on the muscle belly, or overcrowding tendons within a sheath or fibro-
osseous tunnel or hiatus in the interosseous membrane ofthe leg; and
F. Enhanced rehabilitation based upon an understanding oftendon healing.
Ch.6 Fundamental Techniques and Procedures 141
Blix CUIVe-depicts the relationship between muscle length and strength of contraction,
and shows that physiologically a muscle's ideal resting length allows for optimum strength
of contraction (Figure 6-5). In Blix's contractile force curve, the actual contractile force of
muscle is greatest at about 120% of its resting length. Tension falls off markedly in both
directions, indicating that muscle must have optimum length for function, and deviations
from this length will reduce the contractile force of the muscle. A muscle subjected to
excessive resting tension will undergo fiber degeneration, while inadequate tension
predisposes to muscle weakness. Muscle tensile strength is approximately 75 psi, while
tendon tensile strength is 8,600-18,00 psi. Comparing tension versus length, as the length
increases beyond resting length, tension increases up to a point after which tension
decreases as the muscle belly fails to sustain force. Thereafter, tension actually rises as the
strength of the tendon, notthe muscle, sustains the load. In some cases, it may be desirable
to use the transferred tendon as a sling or suspensory ligament, and not a gliding,
functional tendon.
Direction ofpull-the direction of pull determines the influence ofthe transferred tendon
on affected joints. The effect of various tendons on the foot and ankle can be
schematically summarized in Figure 6-6. Tendon anchors and reattachment techniques
include the hole and button, hole and bone plug, 3-hole intraosseous, 2-hole intraosseous,
side-to-side, Bunnell, lateral trap, and various commercially available anchors (Statak
T
.,
Mytek, Permanent Bone Anchor, and Tenodesis Screw System (interference screw), to
name afew).
Complications-complications of tendon transfer may include muscle spasm (diazepam is
useful in the early postoperative phase), stenosing tenosynovitis and adhesion,
overcorrection, under- correction or weakness, loss of correction, bowstringing, and nerve
entrapment.
t
c
o
'w
c:
{!!
Total
Figure 6.5
I
I "
I ", 1
: contraCtile;"'\ /
force .. I
I >-,
g': Passive '.,/ \
"iii I strength / \
Q) I/'\
cr:: I/'\
\
Length_
)
EVerSIon
,"-- EHl EDL
" 0 0 /
Dorsiflexion
AJ '\
""
Plantarflexion
Figure 6.6
.gy
", 7
'0.
AJ
'DPB
DPL 00
.... ,
'STJ
":>
TSO
142 Fundamental Techniques and Procedures Ch.6
Tendon lengthening procedures-these include the open Z-tenotomy, which is commonly
used on the long digital extensor when correcting a hammertoe with a significant MTPJ
contracture. Ankle equinus is corrected using the gastrocnemius recession or lengthening
of the entire tendoAchiliis. The Baker tongue-in-groove gastrocnemius recession is used
when the Silverskiold test reveals limited dorsiflexion only when the knee is extended,
indicative of gastrocnemius tightness. The tendoAchiliis lengthening (TAL) is used when
the Silverskiold test reveals limitation of ankle dorsiflexion with the knee extended and
flexed, indicative of gastrosoleus equinus. The TAL is commonly performed as an open
frontal plane Z-Iengthening.
Common Tendon Transfers
Jones Suspension (Figure 6-7)
Goals-eliminate cock-up hallux, enhance ankle dorsiflexion
Indications-cock-up hallux, weak tibialis anterior, loss of sesamoid function
Adjunct procedures-hallux IP arthrodesis, Heyman-Jones pan metatarsal
suspension
Complications-recurrence of deformity due to tendon regeneration
Aftercare-BK weight bearing cast 2-3 weeks
Hibbs Suspension (Figure 6-B)
Goals-decrease MTPJ buckling and increase ankle dorsiflexion
Indications-anterior weakness (mild), flexible anterior cavus with extensor
substitution, claw toes often with associated IPK
Contraindications-posteriorweakness, weak interossei, gross EDL weakness,
structural rigidity, osseous instability
Aftercare-BK weight bearing cast 4-6 weeks
Tibialis Anterior Tendon Transfer (TAm (Figure 6-9)
Goals--decrease forefoot supinatory twist increase true ankle dorsiflexion
Indications-recurrent clubfoot, flexible anterior cavus, dropfoot (CMT)
Contraindications-excessivelv weak TA 4), pes valgus, weak PL, severe
anterior cavus with clawtoes
Aftercare-BK weight bearing cast 3-4 weeks
Split Tibialis Anterior Tendon Transfer (STArn (Figure 6-10)
Goals-increase true ankle dorsiflexion, decrease long extensor swing phase
overload, and decrease adductocavovarus forefoot deformity
Indications-flexible anterior cavus, extensor substitution, clawtoes; spastic
posterior ankle equinus, equinovarus (CP), anterior weakness dropfoot, flexible
cavovarus, overpowering inverters
Contra indications-excessively weak TA 4). pes valgus, weak PL, severe
anterior cavus with clawtoes
Aftercare-BK weight bearing cast 3-4 weeks
6'9 am!:i!::1
L'9 am!:i!::1
144 Fundamental Techniques and Procedures
10. Atraumatic
technique
3. Supple local
tissue
2. Understanding
the anatomy
c
11. Preserve blood supply
and innervation
6. Select
suitable
tendon
D l
12. Adequate tendon
upon fixation
13. Secure fixation
9. Preserve the
gliding mechanism
E
Ch.6
necessary
14. Careful
postoperative
management
Figure 6.10
Tibialis Posterior Tendon Transfer (TPTT) (Figure 6-11)
Goals-eliminate dropfoot, eliminate flexor substitution (triceps surae weakness)
Indications-anterior muscle weakness, dropfoot, non-spastic equinovarus,
recurrent clubfoot, peroneal nerve palsy (CMT), and triceps surae weakness
Contraindications-spastic TP, pes valgus, rigid clubfoot
Technical considerations-interosseous window aperture, phase conversion,
often combined with arthrodesis
Aftercare-BK cast 3weeks non-weight bearing, then additional 3weeks weight
bearing, begin ROM at 4weeks
Peroneus Longus Tendon Transfer (PLTT) (Rgure 6-12)
Goals-increase ankle dorsiflexion, eliminate PL cavus influence
Indications-anterior muscle weakness, dropfoot and flexible cavus
Technical considerations-easy phase conversion, caution sural and
intermediate dorsal cutaneous nerves
Contraindications-posterior weakness, pes valgus
Aftercare-same as for TPTT (above)
saJnpaOO.ld pUll sanb!U40alllllUaWllpUn::l
9 '4::1
146 Fundamental Techniques and Procedures Ch.6
Peroneus Brevis into Talus Tendon Transfer (PBTT)
Goals-suspend talar neck, eliminate flexible vertical talus
Indications-type I vertical talus, severe pes valgoplanus
Contraindications-rigid pes valgoplanus, immature talus, or compromised talar
neck circulation
Technical considerations-may be combined with closing adductory wedge
osteotomy of talar neck, medial arch tendosuspension (McGlamry-Young), and
Evans lateral column lengthening
Aftercare-up to 8weeks, BK cast, non-weight bearing
MurphyAnteriorAdvancement ofthe TendoAchillis (Figure 6-13)
Goals-eliminate spastic posterior ankle equinus, shortens ankle lever arm 48%
and MTPJ lever arm only 15%
Indications-CP induced dropfoot with triceps surae contracture ankle equinus
Contraindications-osseous ankle equinus
Technical considerations-heel prominence, routing deep to FHL, McGlamry
modification involves medial-to-Iateral intraosseous suture through calcaneus,
recurrent deformity, and weak propulsion
Aftercare-up to 5-6 weeks, BK non-weight bearing cast with ankle and STJ
neutral
Figure 6.13
147 Ch.6 Fundamental Techniques and Procedures
INTERNAL SKELETAL FIXATION
Fracture, or osteotomy stability is determined by intrinsic and extrinsic factors. Intrinsic
factors include fracture configuration, and bone composition and quality. Certain fracture
configurations are intrinsically more stable than others. Atransverse fracture is said to be
intrinsically stable, whereas agreenstick or torus fracture is said to be potentially stable, and
a spiral or comminuted fracture is said to be unstable. Unstable fractures tend to
displace when subjected to an axial load, resulting in shortening. Metaphyseal cancellous
bone fractures are generally more stable than cortical diaphyseal fractures due to the
composition of metaphyseal bone yielding more friction between the fragments. Healthy
bone stock without osteoporosis, provides intrinsic bone quality that enhances internal
fixation device purchase and fragment stability.
Extrinsic factors that affect stability relate to surrounding soft tissues, including:
1) tendons, ligaments and periosteum-which either aid manipulation and reduction of a
fracture, or prevent successful reduction due to interposition between fragments; 2) when
multiple fractures exist, soft tissue attachments between larger fragments can be
instrumental in providing satisfactory realignment and stabilization; 3) vassal rule
(phenomenon)----fixation of the dominant fracture affords stabilization of the subordinate
fracture, as classically depicted with reduction and stabilization of the lateral malleolus and
subsequent spontaneous reduction of the posterior malleolus in certain ankle fractures;
and 4) extrinsic mechanical forces that affect fracture stability include bending, torsion,
shear, and axial tension and compression. Cortical bone tends to fail (fracture) on its
tension surface. The goals of internal fixation include anatomic reduction, stable internal
fixation, atraumatic technique with vascular preservation, and active mobilization in the
postoperative phase in an effort to avoid cast disease and fibrosis. Internal fixation devices
do not effect faster bone healing, however they create compression between fracture
fragments which, in turn, increases friction and enhances stability, the result of which is
improved healing without complication (less likely not to heal).
Biomal9rials usedfor skeletal fixation-a number of biomaterials are suitable for skeletal
fixation. Key features of metallic biomaterial alloys include strength, ductility and malleability,
and corrosion resistance. The basic composition of surgical stainless steel (316L [low
vacuum] or316 LVM [low vacuum remelt]) consists of iron, with carbon added for hardness
(carbon steel), and molybdenum, nickel, and chromium added to enhance workability and
application to bone fixation (these elements make the alloy less brittle), and to impart
resistance to corrosion. Chromium oxide forms the surface passive layer that resists loss
of metallic ions in the aqueous environment of the tissues. Specifically, most of the
implantable fixation metals come in the form of Austenitic stainless steel. Cutting edges and
some wear surfaces are composed of Martensitic stainless steel, which is harder and less
malleable and less ductile. Cobalt-chromium alloys are also particularly resistant to
compression and shearing wear and, as such, are often used in the fabrication of he wear
surfaces of joint endoprostheses. 1itanium (99% pure) also serves as a useful metallic
implant, due to its ductility and malleability, a Young's modulus that is suitable for skeletal
fixation, and apassive titanium oxide passive layer that readily forms and resists corrosion.
Although surgical stainless steel and titanium implants are both considered appropriate for
permanent implantation, titanium is generally considered more appropriate for such use
due to its inert nature. As arule, dissimilar metals should not be placed in direct contact. due
to the risk of galvanic corrosion. Other forms of corrosion include fretting between hardware
148 Fundamental Techniques and Procedures Ch.6
components that are in direct contact, such as the interface between the land of a screw
head and screw hole of ametal plate. Resorbable forms of fixation are often composed of
poly iL-lactide) acid (PLLA) or poly-p-dioxanone (PDS).
Splintage-this is commonly used to effect fracture or osteotomy stability. Splintage
generally does not create rigidity, and secondary or callus healing is usually noted. K-wires
and Steinmann pins, as well as stainless steel wire suture and staples are usually used for
splintage. K-wires range in diameter from 0.035-0.062 inches, with the 0.045 and 0.062 inch
wires being used most commonly in the forefoot. Steinmann pins are larger, with the most
frequent sizes used in the hindfoot and ankle being 0.078 inches or larger. Advantages of
single pin fixation incfude application when dealing with small fragments and physeal plates.
Disadvantages include poor resistance to distraction and rotary forces, however this can
be diminished by using additional pins in divergent directions; and the tendency for smooth
pins to migrate upon weight bearing or motion. Pin stability can be enhanced with proper
bending and burying, or with bandaging when the pin exits the skin. Threaded K-wires offer
resistance to distraction and pull out, but care must be taken to prevent separation of the
fracture fragments as the far fragment is penetrated. This is accomplished by compress-
ing the fragments together (preloading) prior to positioning the wire across the fracture or
osteotomy. Repetitive three-point bending, or pin flexure, can cause metal fatigue and wire
failure. This is more likely in narrower and threaded K-wires. Use of abuilt-up surgical shoe,
or non-weight bearing, may be needed to prevent pin failure.
Stainless steel wire suture can also be used to effect splintage. Wire size is
measured in gauges from 18to 30 (larger numbers smaller gauges). with 18 and 24gauge
wire being commonly used in foot and ankle surgery. Wire fatigue and failure can occur with
repetitive or excessive twisting or bending. Proper instrumentation, including use of awire
twister, decreases the likelihood of inadvertent wire breakage. Application of an
intraosseous wire loop can be used to stabilize small fracture fragments in bones with thick
cortical walls (to prevent pull through). Wire loops should be placed perpendicular to the
fracture and at 90to each other for maximum stability (double box wire loops). Cerclage
wire is used to prevent telescoping of an oblique diaphyseal fracture, or as a gathering
influence to control small fragments when used with other forms of fixation (plates and
screws). Stainless steel wire suture can be used for: 1) intraosseous wire fixation, 2)
cerclage wiring (circumferential placement around a diaphysis)' and 3) tension banding.
Staple fixation can also be used to effect splintage. Staples are designed to be used
almost exclusively in cancellous bone, and cortical bone should be predrilled to avoid
fracture during staple placement. Staples resist distraction forces across the osteotomy or
fracture, but do not withstand shearing or bending forces very well. Two staples oriented
at 90 apart provide excellent stability. During staple insertion, the surgeon should use a
minimum of mallet strikes in an effort to prevent loss of contact between the bone and
staple. A staple extractor set is needed to remove a staple that has been properly seated
against the cortex.
Absorbable fixation pins can also be used to achieve splintage. Bioabsorbable fixation
devices have become popular and they are particularly useful for treatment of
osteochondritis and chondral fragments, as well as for use in metatarsal osteotomy fixation.
Poly-p-dioxanone (PDS), and poly (L-Iactide) acid (PLLA). are useful bioabsorbable
materials that come in a variety of forms for bone fixation in the foot and ankle. These
materials have been shown to be biocompatible and safe, even in the phalanges when used
for arthrodesis and fracture stabilization. They are radiolucent and can be used in
149 Ch.6 Fundamental Techniques and Procedures
diameters that yield an elastic modulus similar to that of bone (PLLA), enable loading in
standard wire drivers, allow for cutting with a bone sectioning forceps or scalpel, and
degrade in apredictable fashion with creeping bone substitution. OrthoSorb pins (DePuy
division of Johnson & Johnson, New Brunswick, NJ) are made of PDS, and they are
available as straight pins in 1.3 mm and 2.0 mm diameters, as well as atapered pin that is
swaged to ametallic guide pin. The ArthreXTrim-lt Pin' and Trim-It Drill Pin"" (Arthrex, Inc.,
Naples, Florida) are made of PLLA, and are available as a 1.5 mm pin, and a2.0 mm pin with
a metal cutting tip.
Rigid internal fixation-rigid fixation provides absolute stability and promotes primary
(non-callus) bone healing. Rigid internal fixation can be achieved with interfragmental
compression screws, plates, and tension band wires.lnterfragmental compression is either
static or dynamic. Static interfragmental compression is achieved when tension is placed
upon a prestressed implant that in turn converts the tension to compression at the
osteotomy or fracture interface, and is best represented by the interfragmental
compression screw. Contact of the screw head with the near cortex, and purchase of the
distal cortex with the screw threads, places tension along the screw shaft as the threads
try to pull (lag) the head into the bone. The screw resists this axial tensile force and, in turn,
imparts compression across the bone interface. Dynamic interfragmental compression
employs a combination of static force in conjunction with physiologic loads that naturally
occur about the part in question, thereby effecting compression across the fracture
interface. The classic example of this is the fractured patella, wherein atension band wire
is place across the transverse fracture on the anterior (tension) surface and the knee slightly
flexed to convert the tension in the wire to compression between the fracture fragments.
Lag screw-this fixation device is used to achieve static interfragmental compression. A
lagged screw is one that engages only the far fragment with its threads. Compression
occurs as the head of the screw contacts the near cortex and the threads purchasing the
far fragment pull the fragments together. The screw itselfthen sustains tension throughout
its mass, as the thread end and head are relatively pushed apart by the bone cortices. The
tension within the screw is, in turn, converted to compression between the fragments. There
are different types of lag screws, including partially and fully threaded cortical screws and
cancellous screws. Cortical screws have a finer thread pitch, thereby increasing the
number of threads purchasing bone per unit length of screw. Increased thread purchase
increases friction between the screw and bone and, in turn, between the bone fragments.
Increased friction enhances rigidity, and promotes primary bone healing. In orderto create
the lag effect using a fully threaded screw, it is necessary to overdrill the near cortex to
create a gliding hole.
The Swiss AO (Arbeitsgemeinschaft fUr Osteosynthesefragen, or Association for
Osteosynthesis) screws display an asymmetrical (buttress) thread design, which increases
purchase and minimizes pullout Ascrew's size is determined by the diameter of its threads,
with the core diameter actually being less than that of the threads. Cortical screws are
available in 1.5 mm, 2.0 mm, 2.1 mm, 3.5 mm, and 4.5 mm sizes. Cancellous bone screws are
only partially threaded so that overdrilling of the near cortex is not necessary to produce
interfragmental compression. The first rule of fixation states that all of the purchasing
threads of a lag screw must purchase only bone of the distal (far) fragment Threads that
cross the osteotomy or fracture line can distract the fragments and maintain a gap.
Cancellous screws display awider pitch and athinner core diameter, and sizes include 4.0
150 Fundamental Techniques and Procedures Ch.6
mm, 4.5 mm, and 6.5 mm long and short thread pattern screws. Various companies make
both cortical and cancellous bone screws that are cannulated, which makes for ease of
placement and obviates the need to place temporary stabilization pins that can often impede
placement of permanent fixation.
Scr8W plac8m8nt-this should ideally be perpendicular to the fracture or osteotomy
interface. In reality, this orientation is not always practical. When a lag screw is placed
perpendicular to an oblique fracture line, axial loading can cause telescoping and
shortening (Figure 6-14). When asingle screw is used, it is often helpful to orientthe screw
midway between perpendicular to the long axis ofthe shaft ofthe bone and perpendicular
to the fracture/osteotomy interface. Long oblique or spiral fractures, wherein the fracture
length is 2-3 times the width ofthe bone, are amenable to multiple screw fixation with each
screw being placed perpendicular to the fracture interface at each level along the shaft The
first screw should be placed centrally and perpendicular to the long axis of the bone.
Secondary screws are placed on each side of the initial screw and perpendicular to the
fracture line (Figure 6-15).
Scr8W ins8rtion-this proceeds in aspecific fashion that, as arule, should not be altered.
To achieve the lag effect with afully threaded screw, the following sequence is used:
1. Guide hole is drilled through both fragments with a K-wire or adrill bit.
2. The near cortex is then overdrilled to the diameter of the screwto be inserted, which
allows the threads to pass through the near cortex without purchasing.
3. The far cortex thread hole is then enlarged to adiameter that is less than that of the
threads, and just slightly larger than the core diameter of the screw's shaft. This
requires use of the concentric drill guide (T-sleeve).
4. Countersink the near cortex to fit the undersurface of the screw head and minimize
the development of a stress riser.
5. Depth gauge measurement to determine proper screw size, and add 1-2 mm to
assure at least 1-2 thread purchase of the far cortex.
6. Tap (cut) the thread pattern into the far cortex to enhance buttress thread purchase,
using an alternating method of 3 clockwise rotations followed by 1/2 counterclock-
wise rotation to periodically clear the tap flutes of cortical bone. Appropriate drill
guides and tap sleeves should be used to assure proper orientation and prevent soft
tissue injury (the tap has a predilection to becoming wrapped with adjacent soft
tissues).
7. Insert screw to 2-finger tightness.
Rgure 6.14 Figure 6.15
Ch.6 Fundamental Techniques and Procedures 151
When inserting apartially threaded screw, the sequence is the same as just described
for the fully threaded screw, with the exception of not overdrilling. Variations on the
sequence of instrumentation can be effective, however the surgeon is cautioned against
this, as each step in the sequence is meant to maximize stability.
Plates-these offer another means of
achieving rigid internal fixation and, in certain
applications, can be used to achieve axial
compression. In most cases, plates are used
to effect splintage and to provide protection of
a reduced and fixated fracture/osteotomy
that is already stabilized with interfragmental
compression provided by lag screws. In this
way, the plate acts as a neutralization shield
that sustains forces and protects the reduced
and stabilized fracture from bending, torque,
axial tension and compression, and shear
forces. Axial interfragmental compression
Figure 6.16
. . ~
can only be achieved with a plate if the plate is prestressed, and the fracture is relatively
transverse in orientation. An oblique fracture will shorten and displace under axial
compression. In order to effect axial compression using the plate, standard 1/3 tubular
plates must be eccentrically drilled (load screw principle), so that when the undersurface
(countersink) of the screw head engages the plate, the plate is pushed away from the
osteotomy!fracture as the screw seats into the bone and through the plate. A 1/3 tubular
plate must be pre-bent prior to achieving axial compression via load screw placement.
Pre-bending involves bending the plate away from the bone cortex, so that as the screws
seat and lag the plate to the bone, there is no tendency to gap the far cortex as the near
cortex is placed under greater axial load (Figure 6-16).
Dynamic compression plate-this is thick and will not allow gapping of the far cortex, and the
hole/slots in the plate are designed to allowthe creation of axial compression as the screws
seat Whenever possible, the plate should be applied to the Tension side ofthe bone. When
using the load screw technique, the first plate hole away from the fracture, after lagging the
plate to the bone on the other side of the fracture, is offset drilled away from the fracture
interface. Once this screw is seated, axial compression is achieved, and the remaining drill
holes may be concentrically drilled. It may be possible to get a bit more axial compression by
offset drilling the next distal screw, however it is necessary to first loosen the first load screw
priorto securing final purchase with the distal load screws. Neutralization is a method by
which a relatively unstable fracture can be afforded more stability while subjected to axial
compression, despite the long oblique or spiral fracture orientation. Some fractures, such as
long spiral, oblique, or comminuted fractures, are simply not amenable to axial compression.
Interfragmental compression can be obtained between certain fragments using lag screws.
Once lag screw interfragmental compression is achieved, the fixation is protected from shear,
flexure, and torsion about the fracture with the use of aplate to neutralize force applied to the
bone. A neutralization plate can be applied using any size plate, as long as the plate is well
molded. Tubular plates work bestforthis application. When applying aneutralization plate, all
screw holes are drilled concentrically. You can use aseparate interfragmental screw and you
can use alag screw through the neutralization plate.
152 Fundamental Techniques and Procedures Ch.6
Buttressplating-this is used in the fixation of unstable fractures, wherein the strong (thick)
buttress plate is used to maintain alignment of the fragments despite the lack of intrinsic
stability(either tensile or compressive) within the injured bone. Buttressing precludes the
use of interfragmental compression, and gap healing may occur. The buttress plate
essentially serves as abridge between larger fragments with intervening small fragments
"leaning against" the plate. Devitalized bone fragments should be removed and replaced by
cancellous bone graft under protection of abuttress plate.
Tension band wire fixation-this usually combines the splintage afforded by two smooth
K-wires with stainless steel wire tension, to effect dynamic interfragmental compression.
The tension in the stainless steel wire is converted to compression at the fracture
interface. This is useful at the fifth metatarsal base, malleolar fractures, and the patella.
Classically, dynamic interfragmental compression is created with an eccentrically
positioned tension wire used in conjunction with a load beam that converts the tension in
the eccentric wire to compression across the fracture interface, usually requiring joint
positioning that effects wire tension (Figure 6-111. A plate placed on the tension side of a
fracture also acts as atension band.
Figure 6.17
EXTERNAL SKELETAL FIXATION
Extemal skeletal fixation-an external fixator can be used to achieve static interfragmental
compression, as long as the fracture/osteotomy/arthrodesis interface is relatively
transverse. A variety of external fixators are available for use in the leg, ankle and foot. In
general, these devices are of uniplanar, multiplanar or circular designs. They can also be
miniaturized for use in the metatarsus and toes, or for focal use in the tarsus. Hybrid
systems, combining uniplanar and multiplanar elements are also available. The devices can
be used to distract and elongate bone, and to correct deformity. External fixation (EXFX)
devices yield a great deal of stability, while allowing periodic adjustment of the
compressive or distraction load. EXFX can be useful in the acutely injured patient when
temporary skeletal stabilization of the traumatized extremity is required while other injuries,
including head trauma, are managed. The external fixator can be used to provide
interfragmental compression, or it can be used to splint or maintain distraction of an open,
comminuted fracture. EXFX can also be used to span a joint or osseous segmentthat has
153 Ch.6 Fundamental Techniques and Procedures
been debrided or resected for the treatment of infection or neoplasm. These devices are
also used for limb-lengthening by means of corticotomy and callus distraction and other
reconstructive interventions for deformity correction, and have been shown is some case
series to be useful in cases of Charcot reconstruction. EXFX can be achieved with
unilateral (eccentric), and multiplane and circular frames. In some cases, such as those
involving pilon fracture repair, EXFX can be combined with limited dissection internal
fixation to effect satisfactory results.
The frame is applied to the bones via pins or wires, or half pins (pin-screws). that are
positioned proximal and distal to, and as close to the fracture/osteotomy!fusion interface as
is possible. EXFX stability can be enhanced, and pin/wire loosening at the metal-bone
interface can be reduced, by maximizing pin diameter and radial preload, avoiding
overdrilling of the pin tract, and using pins coated with hydroxyapatite. Pin diameters
ranging from 4,5-6 mm are usually sufficient for fixation of the adult tibia, and the diameter
ofthe bone should be >2/3 the diameter ofthe pin in order to minimize the risk of fracture.
Most tibial segments can be adequately stabilized with 2-3 pins separated as far as
possible within the segment, with one pin being placed as close as possible to the
fracture/nonunion, bone graft interface. As a rule, 3 pins provide more stability to an
osseous segment than do 2pins; and, pins oriented in different planes maximize stability. The
distance of the extremity to the frame should also be minimized, without compromising the
adjacent cutaneous barrier. External fixators are also used to effect dynamization, wherein
cyclic micromovement is produced with a lever arm at 3-6 weeks after initial stabilization,
thereby stimulating callus formation (secondary bone healing) while maintaining alignment.
When dynamization is desired, consideration should be given to the optimal length of the
frame at the time of initial application, so that shortening can be achieved when adequate
bone healing has occurred.
Disadvantages of EXFX include the bulky size of the devices, and the rather high rate
of pin tract infection. It can also be difficult to properly place the fixation pins, or pin-screws
(halfpins), so that they do not span adjacent joints or violate neurovascular structures. As
a rule, it is important to use safe zones for pin placement so that neurovascular structures
are not damaged. It is also importantto try and minimize placementthrough muscle bellies,
although this becomes necessary at certain locations. Pin and wire placement can be
enhanced with the use of intraoperative image intensification fluoroscopy,
In the tibia, proximal to the tibial tubercle and>1cm distal to the knee joint, asafe zone
extends from the posteromedial to posterolateral border of the proximal tibia. Care should
be taken to avoid violation of the space immediately adjacent and posterior to the head of
the fibula, wherein lies the common peroneal nerve, and the space posterior to the tibia,
wherein lies the posterior tibial nerve, artery and vein. Transfixation wires can be inserted
through the anterior portion of the fibular head, aiming approximately 30 lateral-to-
medial into the proximal tibia to exit just medial to the patellar tendon. A second
transfixation wire can then be placed from lateral-to-medial in the frontal plane, anterior to
the head ofthe fibula and the medial collateral ligament. When halfpins are used, they can
be positioned obliquely through the medial or lateral portions of the anterior half of the
proximal tibia, or through the head of the fibula into the proximal tibia.
Immediately inferior to the tibial tubercle, the anterior and posterior tibial arteries are
vulnerable to impalement if placement of medial-to-Iateral transfixation pins is attempted,
or if a pin is directed into the distal aspect of the popliteal fossa or the posterior leg,
therefore these methods are not recommended at this level. A transfixation wire can be
directed through tibialis anterior and the anterolateral aspect of the tibia, taking care to
154 Fundamental Techniques and Procedures Ch.6
avoid injuring the saphenous vein and nerve. Halfpins can also be positioned obliquely
through the medial portion of the proximal tibial metaphysis.
At the midshaft level of the tibia, to the junction of the middle and distal thirds of the
tibia, care should be taken to avoid injuring the tibial artery, venae commitans, and nerve
located medial to the midline along the posterior surface ofthe tibia. Here, atransfixation
pin can be directed posteromedially through the crest of the tibia, avoiding violation of the
posterior surface of the tibia. Again, it is important to avoid violating the saphenous vein
and nerve medial to the crest of the tibia. It is also safe to place an additional wire through
the anterior muscle compartment, from lateraI-to-medial, just posteriorto the tibial crest It
is best to align these pins carefully, so as not to redirect and repetitively perforate skeletal
musculature.
Just proximal to the ankle, care should be taken to avoid injuring the deep peroneal
nerve and the anterior tibial artery, adjacentto the lateral surface of the tibia. Placement of
transfixation pins through the fibula should be limited to the anterior portion of the fibula, and
avoid the perforating peroneal nerve lateral to the tibia, and the saphenous nerve and vein
medial to the tibia. Atthis level, it is also useful to position atibiofibular transfixation halfpin
through the tibia into the fibula, once again taking into consideration the pOSition of the
perforating peroneal artery.
It can also be helpful to stabilize the relationship of the foot to the leg, particularly
when fracture/dislocations warrant stabilization ofthe foot, or when reconstructive efforts
require immobilization of the ankle or protection of the foot from plantar weight bearing.
Purchase of the talus can be achieved with halfpins or transfixation pins, and it is best to
position these through the neck of the talus, between the talonavicular joint and the
anterior margin of the posterior facet of the talus. Purchase of the calcaneus, either with
halfpins or transfixation pins, should be localized to the tuberosity and take into
consideration the contents of the tarsal tunnel. the STJs, and the insertion of the Achilles
tendon, all of which should be avoided.
When using the lIizarov technique, pins/wires are positioned obliquely, and this
requires elongation of the half ring with afootplate, or plates, and the addition of adistal half
ring oriented perpendicular to the substrate. The foot frame can be constructed of 2half
rings that can be stabilized with atranstarsal fixation pin situated dorsal to the plantar vault
and plantar to the dorsal neurovascular bundle; or, the first and fifth metatarsals can be
purchased with 2-3 halfpins.
Pin (or wire) tract infections are not uncommon when many pins/wires are used, and
the EXFX frame is left in place for >3-4 weeks. If the pin remains stable, and there is no
radiographic evidence of radiolucency about the pin, then the pin is usually left in place
and local pin tract care and, at the surgeon's discretion, oral antibiotic therapy can be
useful. If the pins/wires display loosening and radiolucency, then removal and bone
curettage, and implantation of vancomycin- or gentamicin-impregnated calcium sulfate (or
PMMA) beads, as well as IV antibiotic therapy, may be useful therapies.
HEMOSTASIS
Anatomic dissection-anatomic dissection is the foundation upon which target structures
and pathological anatomy are identified, tissues manipulated, and hemostasis achieved in
foot and ankle surgery. Anatomic dissection enables the surgeon to avoid tourniquet
application in almost any forefoot surgical case. The majority of bleeders are identified in
the subcutaneous layer, superficial to the deep fascia. The process involves skin incision,
155 Ch.6 Fundamental Techniques and Procedures
transdermal dissection, separation of the superficial fascia and subcutaneous fat layer,
deep fascial incision, then joint capsular and/or periosteal incision. Specific capsular and
deep muscular vessels are generally few and well known, and attention should be focused
upon these vessels when necessary. Hemostasis is achieved via ligature application
using a hand tie or instrument tie, when the lumen of the vessel is grossly visible.
Electrocoagulation can be readily used tor vessels with asmaller lumen diameter. Anatomic
dissection is usually performed using the scalpel, however limited sectioning can be
achieved with the radiosurgical electro-sectioning unit.
Dilute vasoconstrictor (epinephrine}-rlilute epinephrine can be used to enhance
hemostasis in certain cases when indicated. Epinephrine diluted 1:200,00-1: 400,000 in the
local anesthetic solution can be infiltrated in the subcutaneous tissues about the surgical
site. Contraindications include any evidence of ischemia or PVO, organic occlusive or
vasospastic (Raynaud's phenomenon). connective tissue disease such as scleroderma,
vasculitis, concomitant use of MAO inhibitor or tricyclic antidepressant agent, pregnancy
(which usually contraindicates any elective surgical intervention), or distal tissue injury,
Tourniquets-these can be used, in conjunction with anatomic dissection, to achieve
hemostasis. Application ofthe pneumatic cuff is performed in a smooth and even fashion,
over a well-padded limb, after exsanguination via three minutes of elevation at 45, or
distal-to-proximal application of an Esmarch bandage. The cuff is applied at the ankle
(supramalleolar) or thigh (junction of proximal and middle thirds) level for foot and
hindfoot/ankle surgery, respectively. Sterile tourniquets are available, although proper
draping will allow application of a nonsterile ankle cuff for forefoot surgery.
Inflation pressure-there are 3 variables used to determine tourniquet inflation
pressure: patient age, systolic blood pressure, and the size of the extremity. The usual
pressure range for athigh tourniquet is 300-375 mmHg. The usual pressure range for
an ankle tourniquet is 70100 mm Hg above the preoperative systolic blood pressure,
or approximately 225250 mm Hg torthe average size adult, or approximately 125150
mm Hg for children. Insufficient pressure may effect a "venous tourniquet" that only
inhibits venous return, while allowing arterial perfusion, congestion and stagnation of
the blood in the extremity, which can be problematic. The pneumatic tourniquet
pressure register should be checked regularly with the mercury manometer to assure
proper pressure measurement. The tourniquet should remain inflated no longer than
90 minutes on the ankle, or 120 minutes on the thigh. The tourniquet can be re-inflated
after a20 minute "breathing period," however for most foot and ankle surgery, this is
usually not necessary. The "breathing period" enables hyperemic limb perfusion and
restoration of normal pH, pCOz, and pOz. If it becomes necessary to deflate the
tourniquet additional times during a prolonged case, each tourniquet inflation period
should be shorter and each "breathing period" should be longer (15 minute
increments). Potential complications of tourniquet application include paralysis,
ischemia, clotting dysfunction, thrombophlebitis, and cutaneous compromise,
Paralysis may result from neuropraxia induced by excessive pressure or prolonged
inflation, inadequate pressure allowing creation of a venous tourniquet that allows
perfusion of the vasonervorum and intraneural hemorrhage; or prolonged ischemia.
Limb ischemia lasting greater than three hours effects some degree of sublethal
muscle damage. Tourniquet induced alteration ofthe clotting mechanism hinges on the
156 Fundamental Techniques and Procedures Ch.6
liberation of plasminogen activators secondary to non-physiological pressure applied
to venous walls and limb hypoxia that, in turn, results in fibrinolysis. Increased
fibrinolytic activity peaks at approximately 15 minutes post-deflation, and normalizes
at approximately 30 minutes post-deflation. The combination of post-deflation
hyperemia and increased fibrinolytic activity effects increased hemorrhage in the first
30 minutes following tourniquet deflation. Thrombophlebitis is rarely seen following
proper use of the pneumatic cuff in patients with no previous history of
thrombophlebitis or venous stasis. Chemical irritation of the skin can occur if the
tourniquet padding becomes soaked with povidone iodine or any other antiseptic
solution used to prepare the skin for surgery.
Topical hemostatic agents-these topical agents, when placed in contact with blood,
effect clotting.
Topical thrombin-bovine-derived prothrombin that is activated by tissue
thromboplastin. It catalyzes conversion of fribrinogen to fibrin monomers and
polymers and, ultimately, afibrin clot. Can induce hypersensitivity due to bovine origin.
Used to cause rapid, direct coagulation of capillaries and small vessel (minor)
bleeding. Available in a spray bottle, or blotted on bleeding surfaces. Not for
intravascular use.
Absorbable gelatin (GeUoanfP)-sterile, purified porcine skin collagen gelatin that is
H20 soluble, pliable, and non-antigenic. It is not intrinsically hemostatic, however
absorbs many times its weight in blood, providing tamponade and pressure, thereby
slowing bleeding. Once clot forms, the gelatin serves as aframework for granulation.
The gelatin is absorbed in 4-6 weeks. Used for small vessel (minor), capillary, and
venous bleeding. It is deal for small dead space control, however it can interfere with
bone and dermal healing.
Oxidized cellulose (Surgicef)-when impregnated on a knitted fabric, oxidized
cellulose can be used to rapidly clot capillary, venous, and small arterial bleeding
impregnated knitted fabric. It is removed after the clot forms, and any residue left in
the tissues is absorbed via liquefaction in about 2weeks. It is non-antigenic, non-toxic,
and also antibacterial. It will inhibit bone healing if placed interfragmental.
Microfibrillar collagen (Aviteng@)-this is the dry, sterile, HCI acid salt of purified
bovine corium collagen, and it rapidly causes clot formation via the extrinsic clotting
pathway. It can be antigenic due to bovine origin. It can be used to stop brisk
bleeding, and is applied with gentle compression. It is more expensive than the other
topical hemostats described, above. It is not to be used between bone fragments, as
it will inhibit osteosynthesis.
Drains and dressingHt is advisable to use an appropriate wound drain, whenever closure
entails reapproximation of deep layers, in particular those layers deep to the deep fascia.
Drains are of 2 basic types: gravity and closed-suction. Gravity drains include fine-mesh
gauze and latex or non-latex, or silicone, rubber drains in various sizes and shapes. These
are typically pulled from the wound after several days, usually at the time of the first
dressing change. and may be appropriate following delayed primary closure. Closed
suction drains, using either a vacutainer or bellows chamber, are appropriate for deep
wounds with considerable muscle oozing, or when larger volumes of drainage are expected.
Negative pressure wound closure (Wound VAC) is often useful in achieving closure of
open wounds, and is not indicated for use in wounds closed by primary intention.
157 Ch.6 Fundamental Techniques and Procedures
Wound dressings should also serve to absorb any drainage, serous or hemorrhagic,
that exude from the closed wound. To this end, the bandage should splintthe healing tissues,
absorb drainage, and avoid excessive pressure or strangulation of circumferentially
wrapped tissues. For almost every tendon or osseous surgery performed on pedal
structures, bringing the bandage materials above the ankle can help to stabilize the tissues,
as well as preventthe bandage from coming loose.
ANESTHESIA
Local Anesthetics-these agents are either esters or amides. Esters are formed from an
alcohol and acid by removal of water, and amides are formed from an acid by replacing the
hydroxide group with the amide group (NH3). Amides are detoxified in the liver and
consequently their effects last longer. Esters are metabolized in the blood stream by
pseudocholinesterase and are more quickly detoxified, and they display a high potential
for hypersensitivity. When using local anesthesia, it is important to convert the
concentration of the solution (% solution) to milligrams of local anesthetic agent (Table 6-7).
TABLE 6-7. CONVERTING CONCENTRATION (% SOLUTION) TO MASS (MILLIGRAMS)
OF LOCAL ANESTHETIC.
Percent (%) solution Milligrams (mg) of local anesthetic
0.25% 2.5
0.5% 5
1% 10
2% 20
General guidelines for the use of local anesthesia include: " having knowledge ofthe
patient's medical and allergy history, 2) knowledge ofthe toxic dose ofthe particular local
anesthetic being used, 3) use the smallest concentration of local anesthetic necessary to
effect anesthesia (a higher concentration does not last longer), 41 a larger volume of local
anesthetic may be necessary to anesthetize alarger diameter nerve, 5) allow enough time
for the anesthetic to take effect (each anesthetic agent has an intrinsic time lag before
anesthesia sets in), 6) concomitant use of dilute epinephrine is helpful when alarge volume
of local anesthetic would otherwise be necessary (when epinephrine is not contraindi-
cated), 7) infiltration should be done with frequent aspiration to assure avoidance of in-
travascular infusion ofthe local anesthetic, 8) patients who are scheduled for procedures
using local anesthesia should be maintained NPO preoperatively so that conversion to se-
dation or general anesthesia can be undertaken if deemed necessary, 9) avoid local infil-
tration into an infected or traumatized area since local anesthetic onset is delayed by lower
pH (inflammation and/or infection), and 10) each foot should be injected separately when
long duration bilateral cases are planned. Local anesthesia used in conjunction with IV se-
dation is usually adequate for many forefoot surgeries. The local anesthetic dose can be ad-
justed under certain circumstances, including: 1) use half of the standard adult dose for
debilitated or elderly patients, 2) use Clark's rule for children, where the child's weight in
pounds is divided by 150 and multiplied by the adult dose, and 3) use Fried's rule for infants,
where the infant's age in months is divided by 15 and multiplied bythe adult dose. Standard
local anesthetic dosages are depicted in Table 6-8.
158 FundamentalTechniquesand Procedures Ch.6
TABLE 6-8. STANDARD LOCAL ANESTHETIC DOSAGES FOR USE IN AN AVERAGE
ADULT(:::: 25YEARS OFAGE,70KG MALEOR60KG FEMALE).
Local Proprietary Duration Class Maximumsingledose(mg)
anesthetic name ofaetion Plain With epinephrine
Procaine Novocaine 0.75-1 hour Ester 750 1000
Tetracaine Pontocaine 2-3hours Ester 75 100
Lidocaine Xylocaine 1-2hours Amide 300-350 500
Mepivacaine Carbocaine 1-3hours Amide 400 500
Bupivacaine Marcaine 3-12hours Amide 175 225
GeneralAnesthesia
GeneralanesthesiacausesreversibleunconsciousnessviaCNSdepressionstartingatthe
cerebralcortex,andproceedingthroughthebasalganglia,cerebellum,medullaoblongata,
and finally, the spinal cord. The anesthesiologist must look for several potentially
complicating factors in patients anticipating general or IV sedation anesthetics, in
particularcardiovasculardisease such as hypertension,coronaryarterydisease,valve
dysfunction or arrhythmia; endocrine disorders such as diabetes mellitus, adrenal
insufficiency,orthyroid disease; pulmonarydisorders such as COPO, regular cigarette
smoking,orchronic cough;GI concerns such asthelasttimethepatientate ordrank,or
whetherornotdentureplatesare present;historyofhepatitis;and historyofpersonalor
familialneuromusculardisorderoranesthesia-relatedadversereactions,suchasmalignant
hyperthermia.ThestagesofanesthesiaaredepictedinTable6-9.
TABLE6-9.STAGESOFANESTHESIA.
Stage
1-amnesia
andanalgesia
2-delerium
3-surgicalanesthesia
4-medullaryparalysis
Plane
1
2
3
1
2
3
4
1
2
Physiologicaleffects
Preanalgesia,memoryandsensationintact
Partialamnesiaandanalgesia
Totalamnesiaandanalgesia
Unconscious,mydriasis,irregularbreathing,
involuntaryskeletalmusclemovement
Sleeping,residuallidreflex,eyesfixedcentrally,
regularbreathing
Pupilsdilating,fullanalgesia,heartrateandBP
stable
Partialintercostalparalysis,tachycardiaandhy
potension,hypotonia
Complete intercostalparalysisand respiratory
arrest,requiresartificialventilation
Reversiblerespiratoryparalysis
Irreversiblecardiovascularandrespiratory
arrest
Anesthetic agents are used with such frequency that they are improved upon
regularly, and newagentsbecome availablewith regularity. Inhalationalagentsusedto
159 Ch.6 Fundamental Techniques and Procedures
achieve general anesthesia historically include diethylether, methoxyflurane, and
chloroform. More recently, the following agents have been used:
fnflurane-supports the cardiovascular system, can be used with epinephrine, does
not induce emesis, however can be hepatotoxic.
IsoBurane-maintains heart rate, allows rapid induction and emergence, can be used
with epinephrine, does not induce emesis, may be hepatotoxic, however often induces
shivering.
Halothane-allows rapid indUction, acts as a bronchodilator, is nonematic, however
can be negative inotropic, arrhythmogenic and it sensitizes the myocardium to
catecholamines, can be hepatotoxic, often induces postoperative shivering, and is
associated with malignant hyperthermia.
Sevoflurane-very fast onset and offset, minimal mucus membrane irritation,
excellent cardiovascular stability, an agent that replacing isoflurane and halothane in
everyday general anesthesia.
Desflurane-extremely fast onset and offset due to very high volatility, however may
be associated with tachycardia, limited potency, and relatively high cost.
Nitrous oxide-a low-potency inhalant gaseous anesthetic that has little effect on the heart,
liver, kidneys, and lungs, as long as hypoxia does not develop. Nitrous oxide provides
profound analgesia, without sensitizing the myocardium, and allows rapid induction and
emergence. There is, however, no muscle relaxation and nitrous oxide has been associated
with fatal agranulocytosis and spontaneous abortion after prolonged administration. The
patient receiving nitrous oxide should be ventilated with 100% 02 during emergence, in
order to prevent postanesthetic delayed-diffusion hypoxia.
Sedative and hypnotic agents are usually administered as induction and maintenance
agents before or in addition to an inhalational anesthetic, in an effort to diminish anxiety,
initiate, and maintain CNS depression. Traditionally used agents include barbiturates,
benzodiazepines, and narcotics. Neuroleptanalgesia effects somnolence, psychological
indifference, amnesia, analgesia, and loss of voluntary movement. As with all IV sedative-
hypnotic agents, careful assessment of the patient's respiration is mandatory, and
supportive measures are often necessary.
Fentany#-a short-acting narcotic that depresses respiration, effects analgesia, and
is reversed by naloxone. Fentanyl is administered 0.05-0.1 mg 1M 30-60 minutes
pre-procedure, then titrated as indicated.
Droperido#-a sedative-tranquilizer that effects peripheral vasodilatation,
somnolence, mental dissociation (perhaps dysphoria), and serves as a strong
antiemetic. The sedative dose of droperidol is 2.5-10 mg 1M 30-60 minutes pre-
procedure. The combination of droperidol and fentanyl combines the analgesic
effects of fentanyl with the tranquilizing and antiemetic effects of droperidol in a 1:50
(fentanyl: droperidol) ratio.
160 Fundamental Techniques and Procedures Ch.6
Propofol-an IV sedative hypnotic agent used for induction and maintenance of
anesthesia or sedation, and can be used in conjunction with local anesthesia.
Midazolam-a short-acting benzodiazepine eNS depressant often used in
conjunction with analgesia to achieve IV conscious sedation. Midazolam is titrated
IV starting with 1mg, then increasing up to 2.5 mg over at least two minutes, then via
small increments (not to exceed 5mg) while monitoring the degree of sedation.
Other medications used in abalanced anesthesia protocol may include phenothiazine
tranquilizers such as promethazine and prochlorperazine. Atropine (atropa belladonna) and
scopolamine are premedications used to minimize respiratory secretions and to counter
parasympathetic overtone by blocking the vagus nerve whenever a positive chronotropic
cardiac effect is desired. Ondansetron is aselective 5-HT3 receptor antagonist with strong
antiemetic properties, originally used in patients undergoing cancer chemotherapy, and
now regularly used following general anesthesia. Ondansetron is administered 4mg IV slow
infusion over 3-5 minutes, in the treatment of postoperative nausea and vomiting. Paralytic
agents such as succinylcholine are used to paralyze the body and facilitate endotracheal
intubation, cause afast onset and short duration depolarizing skeletal muscle blockade.
Depolarization can be associated with marked increase intragastric and intraocular
pressures, and a rise in serum K+. The rise in K+ can be arrhythmogenic in patients
predisposed to high serum K+, such as patients with burn, tetanus, trauma, uremia, or lower
motor neuron disease (paraplegia, quadriplegia, and muscular dystrophy, Landry-Guillain-
Barre syndrome). Depolarization may be associated with rhabdomyolysis, masseter spasm,
malignant hyperthermia, and dysrhythmia. Atracurium-besylate is a non-depolarizing
neuromuscular blocker that competitively binds with the cholinergic receptor sites on the
motor endplate, and is often used when depolarization is contraindicated. Muscle relaxants
not only facilitate intubation ofthe trachea, but aid in ventilation and abdominal dissection
by diminishing muscle tone. Skeletal muscle paralysis does not cause amnesia or
analgesia, and these conditions must first be achieved via administration of rapid onset IV
agents before paralyzing the patient.
I
Spinal andEpidural Anesthesia-these methods should be considered whenever general
anesthesia poses greater risk. Spinal anesthesia should not be attempted in the presence
of hypovolemia, anticoagulanttherapy or bleeding diathesis (peridural hematoma and spinal
compression), asthma or other COPD, obesity, pre-existing neuromuscular disease (MS,
myasthenia gravis, poliomyelitis, spinal metastasis), pre-existing lumbosacral disk disease
or DJD, local or systemic sepsis, or in the debilitated host. Lumbar epidural anesthesia is
achieved by injecting local anesthesia into the spinal epidural space, usually below G.
Epidural anesthesia prevents spinal headache, can be maintained 24-48 hours for ongoing
anesthesia, rapidly resolves after discontinuing anesthetic, is not associated with
hypotension and allows segmental blockade. Spinal anesthesia may propagate proximally
and effect spinal headache or anesthetize a broader-than-desired area; however the
technique uses less local anesthetic than does an epidural block, and is generally easier to
perform than an epidural block. The most common acute complication of spinal
anesthesia is hypotension caused by sympathectomy. Late complications include postural
headache, lumbago, meningitis, spinal neuralgia, cauda equina syndrome (very rare and due
to fibrosisi, and epidural hematoma.
161 Ch.6 Fundamental Techniques and Procedures
Intravenous Block (Bier Block}-Bier block is commonly used for hand surgery, however
it is applicable to the lower extremity, as long as the surgeon and anesthesiologist are
prepared to handle a possible toxic reaction to local anesthesia. Two pneumatic
tourniquets are placed side-by-side proximal to the operative site after obtaining IV access
in the upper extremity. A butterfly needle is then introduced to the dorsal venous arch,
secured, and connected to a 10 ml syringe. The extremity is exsanguinated to the distal
tourniquet, and the proximal cuff inflated. Lidocaine, or carbocaine, is then infused using 3
mVkg of body weight of a0.5% solution (5 mg/ml), through the butterfly catheter. This effects
surgical anesthesia regionally in about 5 minutes, and lasts for 60-90 minutes. When the
patient begins to complain of proximal cuff tenderness, inflate the distal cuff over the now
anesthetized portion of the extremity, and deflate the proximal cuff only after the distal cuff
is inflated. Do not deflate both cuffs at the same time. At about 30-40 minutes after infusion
ofthe local anesthetic agent, slow deflation of the tourniquets can be safely performed as
enough of the anesthetic has been bound by local tissues and metabolized to avoid atoxic
dose in the systemic circulation. Even if the surgical procedure is finished before 30-40
minutes of elapsed time, the tourniquet must remain inflated at least this long before
deflation. Patient positioning and safety in the OR are the responsibility of the anesthesiol-
ogist and surgeon, and care must be taken to avoid traction nerve palsy, neuropraxia,
injury secondary to pinching or crushing small parts (fingers, skin and other appendages)
in equipment and the operating room table.
PADDING. STRAPING, BRACING AND PROSTHESES
Padding with the use of felt, rolled cotton, felted-foam, various foams and sponge
materials, can be very useful whenever mechanical pressure is associated with pain or
skin compromise (lichenification, hyperkeratosis, or wound). Standard pads include the
metatarsal projection, toe crest, medial longitudinal arch pad, heel cobra pad, heel counter
pad, heel lift, aperture or pontoon pads, and bunion and bunionette flange padding.
Strapping can be used to support musculoskeletal and ligamentous structures, and include
standard applications such as the low Dye strap, digital sling-down strap, the Gibney ankle
boot, and variations that combine different methods. A number of arch binders, and bunion
and hammertoe shields can be customized or obtained commercially. Similarly, avariety of
ankle and Achilles braces (McDavid-type lace-up, Aircast'" stirrup, Malleotrain and
Achilliotrain) can be obtained from surgical supply services or via online services.
A wide range of braces is available for support and substitution of lost function. The
use of accommodative foot orthoses, an extra depth shoe that is anatomically fitted with a
roller sole or metatarsal bar can be used for many conditions, in particular the rheumatoid
or insensitive foot. Simple adjustments for limb length and gait imbalance can be readily
applied. Reverse, adduction and straight shoe last, and custom-made shoes are also
available. Surgical shoes, forefoot-relief and heel-relief orthoses, healing sandals,
removable cast boots (fixed and adjustable, low- and high-top), ankle-foot orthoses (AFOsl.
Charcot Restraining Orthotic Walkers (CROW), and total contact casts can be used in the
post-traumatic, postoperative and chronic settings. Of particular use in cases of dropfoot
are molded ankle foot orthosesthatfit into the shoes, and the heavier double upright brace
with metal stays that are affixed directly to the shoe. The double upright (contoured
aluminum) brace is preferable when ankle edema or deformation prohibits the use of a
hinged AFO (Richie brace, or similar device). a gauntlet-style brace (Arizona AFO), or a
polypropylene molded AFO. The patellar tendon bearing brace, usually of a clamshell
162 Fundamental Techniques and Procedures Ch.6
design, can also be used to diminish weight-bearing load transfer through the foot. Of
course, off-loading can be achieved using appropriately fitted crutches or a walker to aid
ambulation. Off-loading of the lower extremity can be enhanced with the use of a
wheelchair, aRoll-A-Bout or Turning leg Caddy'M, or, as a lastresort, bed rest. Braces and
shoe gear need to be periodically inspected, along with the patient's lower extremities, in
order to monitor for the possibility of cutaneous compromise, especiany in those with
neuropathy and/or vasculopathy, immunocompromise or steroid dependence, and
collagen disorders.
163 Ch. 7 Reconstructive Surgery of Basic Conditions and Deformities
RECONSTRUCTIVESURGERY:
BASICCONDITIONSANDDEFORMITIES
NAILSURGERY
The ingrown toenail (onychocryptosis) involves nail pathology wherein the nail plate has
grown into the ungual labia, with or without concomitant infection. Paronychia lalso termed
whitlow or run-around) consists of nail fold erythema, edema, and pain. Ingrown toenails
are commonly classified as self-inflicted or iatrogenic. Self-inflicted is where the patient
chronically cuts the nail too short or incorrectly angulates the nail nipper deep to the nail
fold. Other causes of ingrown toenails include congenital abnormalities where the matrix
is maligned and produces an incurvated plate; primary soft tissue hypertrophy wherein the
primary pathology involves the adjacent nail fold, which is enlarged and overlaps the plate;
and combinations of incurvated nail plate and nail fold hypertrophy. Nail fold hypertrophy
can also develop secondary to chronic plate incurvation and repetitive wound irritation
with the formation of a pyogenic granuloma. Treatment options include:
Avulsion -treatment should involve education as to proper nail trimming technique, as well
as acute intervention to alleviate paronychia and allow the wound to heal. No amount of
antibiotic will cure an infected ingrown toenail until the offending nail border is
satisfactorily removed. The mainstay of treatment for onychocryptosis is avulsion of the
offending nail border. This effects temporary removal of the margin, and allows subsequent
regeneration over the ensuing months. Avulsion can be performed with, or without, local
anesthetic digital blockade, depending upon the extent of plate removal necessary to
alleviate the condition and other factors, such as peripheral sensory status. Avulsion is
followed by local wound care, perhaps concomitant use of oral antibiotics if paronychia
and/or systemic factors warrant doing so. Re-evaluation should be performed between 2
and 3 weeks after avulsion, at which time proper nail trimming technique is reviewed with
the patient. Temporary removal of the offending border is generally recommended in a
first-time case of ingrown toenail, whereas recurrent onychocryptosis may be best treated
with permanent matrix ablation via either chemical or surgical matrixectomy.
Phenol and Alcohol (P &A) and Sodium Hydroxide (NaOH) matrix ablation-these
techniques of permanent partial or total nail matrix ablation are rather simple, and inflict
minimal pain. The P& A involves three 30-second applications (causing the nail bed and
matrix to appear ashen gray) of 90% phenol followed by rinsing with alcohol (70-90%
isopropyl or ethyl), then copious saline lavage and application of silver sulfadiazine cream
and a sterile bandage. The NaOH procedure involves application of 10% NaOH until the
matrix and nail bed tissues appear ashen gray-brown (about 20-30 seconds); followed by
acetic acid (vinegar) rinse, then copious saline lavage, silver sulfadiazine cream, and a
sterile bandage. It is importantto avoid excessive hemorrhage during application of either
chemical cauterant, as dilution could inactivate the chemical agent. A digital tourniquet
can be useful in this regard, and must be removed after applying the chemical. The main
disadvantage to both the PM and NaOH procedures is the creation of achemical injury that
denatures proteins much as a thermal burn would do. The wound remains open and
draining for 3-4 weeks. Chemical matrixectomy is generally not performed in the presence
of advanced paronychia, and it is recommended that the patient undergo avulsion of the
offending border/s followed by local wound care, and perhaps oral antibiotic therapy
164 Reconstructive Surgery of Basic Conditions and Deformities Ch.7
(cephalexin), with planned matrix ablation to be performed any time after resolution ofthe
paronychia and before recurrence of onychocryptosis. It is also advisable to have the
patient initiate oral antibiotic therapy 24 hours before the planned matrixectomy.
Matrixectomy techniques !true "open" matrix excisions) employing eponychial and nail
fold incision are numerous, and include:
Modified Steindler Matrixectomy-a useful technique for incurvated or iatrogenic
chronically ingrown toenails. This is often employed after failed chemical matricectomy, or
when an "open" excision is desired. The procedure is used to excise the matrix, and does
not address nail fold hypertrophy.
Frost Partial Matrixectomy-employs a right angle incision into the nail fold allowing
reflection of the fold and exposure of the underlying corner of the matrix, following nail plate
avulsion (Figure 7-1. The involved area of nail bed is also excised. The right angle incision is
actually rounded gent/yto avoid slough of the apex.
Winograd Partial Matricectomy-uses 2 inCisions, one longitudinal through the nail bed,
and asecond semi-elliptical incision through the adjacent nail fold, to create awedge of nail
fold and bed that are excised after avulsion ofthe nail plate (Figure 7-2). Hypertrophic un-
guallabium is readily excised.
Ungual Labioplasty-involves awedge-shaped excision ofthe hypertrophic labium, and is
useful only for reduction of nail fold hypertrophy.
Suppan Panhypertrophy Matrixectomy-uses afish mouth incision through the nail folds
surrounding the entire nail plate, allowing excision of surrounding hypertrophic folds and
underlying matrix and bed.
'FJ.
Figure 7.1
Figure 7.2
165 Ch.7 Reconstructive Surgery of Basic Conditions and Deformities
l
Figure 7.3
Zadik (Quenu) Matrixectomy-an H-shaped incision is made with the two vertical arms
through the nail medial and lateral folds, and the transverse arm through the proximal nail
fold (Figure 7-3). The proximal nail fold is then reflected proximally and the underlying
matrix and proximal bed excised. The exposure allows removal of subungual exostosis if
necessary. Closure involves proximal advance ofthe distal nail bed flap, allowing closure
without shortening ofthe distal phalanx.
SUBUNGUAL EXOSTOSIS
Dorsal proliferation of the distal phalanx into the overlying nail plate can effect plate
deformation, often described as a pincer nail, with or without associated onychocryptosis
(Figure 7-4). Subungual exostosis can be of traumatic origin or, when capped with
fibrocartilage, congenital due to osteochondroma. Osteochondroma is usually observed
early in life, between 10-25 years of age, onset on or before puberty, and most commonly is
observed in females (F: M ratio 2:1). Eradication of a symptomatic subungual exostosis or
osteochondroma is via nail plate avulsion, and exposure of the phalangeal lesion with a
distal fish mouth incision, or via longitudinal or semi-elliptical nail bed incision or excision,
respectively. The semi-elliptical incisions are used to create awedge excision of associated
nail bed, when the pathology has caused nailed scar or other lesion. It may not be
necessary to perform nail plate avulsion when the exostosis is small, however exposure of
the exostosis should not be compromised by trying to preserve nail plate attachment.
Osteotripsy may be a useful method for reduction of the osseous prominence. The excised
lesion should be submitted en bloc for pathological inspection, and specimens should be
obtained for bacterial C&S, as well.
Figure 7.4
166 Reconstructive Surgery of Basic Conditions and Deformities Ch.7
HAMMERTOES
Digital contraction deformities include hammertoes, clawtoes, and mallet toes. The
deformities can be flexible or rigid, and the Kelikian push-up test is used to assess the
degree of flexibility. Anatomic considerations include extrinsic and intrinsic musculature,
with emphasis on the MTPJ extensor hood expansion (Figure 7-5).
Metatarsal head
Plantar interosseous
Flexor tendons
Figure 7.5
Dynamic etiologies of digital contracture include:
Capsule
Dorsal interosseous
Transverse metatarsal
ligament
Flexor Stabilization-the most common cause of pathological digital contracture (>70%),
itself caused by late stance and propulsion phase hyperpronation; the FDl and FOB fire
earlier and longer to stabilize the hypermobile forefoot, thereby overpowering the
interossei with resultant dorsal subluxation of the MTPJ; associated with adductovarus
fourth and fifth digital deformities.
Extensor Substitution-this is associated with pes cavus, foot drop, and anterior
compartment weakness, wherein the Eol overpowers the lumbricales during swing phase,
and causes dorsiflexion of the MTPJs; results in a high degree of MTPJ subluxation and
retrograde plantar buckling ofthe metatarsus.
Flexor Substitution-this is the least common cause of digital contracture, and occurs due
to weakness ofthe triceps surae wherein the deep posterior leg muscles compensate and
thereby overpower the interossei during stance phase, particularly during propulsion; the
digits are seen primarily in the sagittal plane, with minimal varus rotation; a calcaneus gait
may develop and this may be observed following over-lengthening (TAL) of the heel cord.
A mallet toe involves sagittal plane plantarflexion ofthe DlPJ, and may be associated with
along toe. Acongenital curly (varus) toe involves adduction contracture and varus rotation
of the DlPJ, usually toes 3-5, and radiographs (upon reaching skeletal maturity) may show
a delta-shaped middle phalanx. Hammertoes involve dorsiflexion of the proximal phalanx
and plantarflexion of the middle phalanx, perhaps with transverse plane deviation in the
direction of flexor plate subluxation. The clawtoe involves plantarflexion of both the PIPJ and
the DIPJ, and is often seen in cases of extensor substitution (Figure 7-61.
Ch. 7 Reconstructive Surgery of Basic Conditions and Deformities 167
MPJ extension
Clawtoe
Mallet toe
Figure 7.6
Symptoms associated with advanced digital contracture deformity include painful PIPJ
motion, painful hyperkeratotic lesion(s), inability to wear regular shoes, contracted painful
toe that is short, and possibly dorsiflexion deformity of the DIPJ. Radiographic findings
include joint narrowing and superimposition at the contracted joint levels, gun-barrel sign
on the AP view due to long axis imaging of the phalanx in either dorsiflexion (proximal) or
plantarflexion (middle), shortened contracted toe, DJD of the PIPJ and MTPJ, and
periarticular osteoporosis. Biomechanical signs of digital contraction deformity include the
presence of hypermobile first ray and other hyperpronation findings (flexor stabilization), or
Stage I pes cavus as seen in anterior cavus and dropfoot related extensor substitution.
Postoperative management involves the use of a wooden or stiff-soled surgical shoe,
perhaps with build-up when the pins cross the MTPJ, and may involve casting depending
upon other procedures performed.
Avariety of nonsurgical options are available fortreatment of symptomatic digital contractures,
including the use of larger shoes with an extra-depth toe box, digital retainers such as dorsal
(early. flexible defonmity) and/or plantar (advanced, rigid defonmities) toe crests, sling-down
toe-MTPJ splints (Budin splint), sling-down or predislocation taping, pads and shields, and
periodic debridement of hyperkeratoses. The use of a supportive insole with a metatarsal
projection pad can also help to realign the MTPJs, and enhance nonsurgical treatment of
hammertoes. When nonsurgical efforts fail to effect satisfactory relief, then a variety of
surgical interventions can be considered. like the nonsurgical interventions, operative
measures also take into consideration the alignment ofthe MTPJ as well as that of the IPJs.
Surgical procedures for repair of contracted digital deformities include:
Flexor tenotomy-operative procedures for correction of digital deformities will vary
depending on the degree of toe and MTPJ flexibility. The reducible lesser digital
deformity may be responsive to flexor tenotomy, both long and short (flexor set),
however the use of this as an isolated procedure is rarely indicated and does not
provide a long lasting correction in most cases. Indications include plantarflexion
deformity atthe PIPJ or DlPJ that is completely reducible with manipulation. Attention may
168 ReconstructiveSurgeryofBasic Conditions and Deformities Ch.7
onlybe requiredatthelongflexorandtheIPJcapsuleproximallyand distally.Generallya
plantarstabincisionisindicated,howeveramildcontracturemaybeapproachablethrough
amedial or lateral exposure. This procedure can be useful in conjunction with PIPJ
arthrodesisinthe presence ofpersistentmallettoe,whenthetoe is pin-stabilized in a
positionofslightDIPJ dorsiflexion.
Extensor tenotomy and capsulotomy-these are also rarely indicated as isolated
procedures,andarecommonlyusefulinconjunctionwithPIPJstabilizationandMTPJre-
location(seesequentialrelease).
Resection arthropiasty-a varietyofhammertoe procedures can be used,includingthe
Post arthroplasty wherein the head of the proximal phalanx is resected
transversely at the level of the metaphyseal flare. Resection of the base of the
proximal phalanx(Gotch and Kreuz) iswroughtwith complicationsdueto destructionof
theintrinsicmuscleattachmentstothe base,andmustbecombinedwithadjacentdigital
stabilizationandsyndactylyin ordertoavoidfloatingorflailtoe.
,
Digital stabilization-in general,multiple digital stabilizations, conSisting ofPIPJ fusion
and MTPJrelocation,areindicatedforcorrectionofadvanced,dynamicallyinduceddigi-
tal deformities.Such deformitiesareusuallyassociatedwith lessermetatarsalgia,con-
comitant plantar hyperkeratosis (intractable plantar keratoma [lPK] or diffuse plantar
tyloma),dorsalPIPJanddistaldigitaltipandhyponychiumhyperkeratosis,mechanicalony-
cholysisandnaildystrophythatpredisposestofugalinfection,andrigidityorincompletere-
locationwithpush-uploading.Transverseplanedeformitymayalsobepresent,inparticular
whenthesecondtoe crossesoveror,lesscommonly,underthe halluxinthepresenceof
associated HAVand bunion deformity.The crossoversecond toe is particularlyhardto
completelyrealign. Isolatedinterphalangealarthroplastycan beusefulinthe presenceof
anunusuallylongdigitthatiscontractedsecondarytoshoecrowding,howeveritisrarely
indicated for the treatment of multiple, dynamically-induced hammertoes. Moreover,
multipleadjacentPIPJ arthroplastymayleadtodigitalinstabilityand recurrentdeformity,
in the postoperative phase. Itcan be useful to approach the deformity by means of
sequentialrelease.Thesequentialreleaseforadvancedhammertoedeformity(Figure7-7)
includesthefollowingsteps:
1. Long extensorhoodrecession,
2. Long extensortenotomy(openZ-tenotomyortransverse),
3. PIPJ capsulotomyandarthroplastyorarthrodesis,
4. MTPJ capsulotomy,and
5. MTPJ flexor plate release (made easy using the McGlamry metatarsal
elevator)and repair.
The Kelikian push-uptest(applyadorsally-directedforceto the plantarsurface ofthe
metatarsalhead,tosimulategroundreactiveforce)isperformedbetweeneachstepinthe
sequentialrelease,andprogressiontothenextlevelofreleaseisnotnecessaryifthedigit
and MTPJ properlyaligninarelaxedattitudewithsimplepush-uploading.Full sequential
release is used inthe correction ofadvanced clawtoe orhammertoe deformities. Itis
necessaryto performthe Z-tenotomywhen advanced dorsal contracture iscorrected,
otherwiseitmaybe difficulttoreapproximatethetendonupon closure.Medial orlateral
Ch.7
c
E
G
Figure 7.7
Reconstructive Surgery of Basic Conditions and Deformities
?t
Figure 7.8
B
EDL
undermined
Phalangeal head
,
D
,
F
,q;; ..
H ?t
169
170 Reconstructive Surgery of Basic Conditions and Deformities Ch. 7
dislocation of the flexor plate will cause a medial or lateral deviation of the digit upon
push-up loading, and is usually related to chronic synovitis and subluxation of the flexor
plate to the side of deviation. Flexor plate subluxation must be addressed at the time of
sequential release, and an anchor suture may be necessary in order to maintain correct,
balance alignment. In some cases, persistent deformity may require MTPJ capsulorrhaphy
with wedge excision of redundant capsule, or metatarsal osteotomy (medial or lateral
transpositional and/or shortening) for satisfactory correction.
Interphalangeal arthrodesis-this entails several modifications, including end-to-end
(non-fixated, described by Soule; K-wire stabilization, described by Taylor and Selig); and
peg-in-hole (pike, described by Higgs; or rounded, described by Young) techniques.
Arthrodesis is generally indicated in cases of multiple lesser digital deformities, which is the
typical presentation when treating dynamically induced (flexor stabilization, extensor
substitution, or flexor substitution) contractures ofthe toes and MTPJs. Either peg-in-hole
or end-to-end fusion can be used, based on surgeon's preference. If shortening is a
concern, then the end-to-end fusion may be used, as less shortening is encountered. The
peg-in hole may more reliably achieve radiographic fusion mass consolidation, however, the
functional result of afibrous pseudoarthrosis of an end-to-end arthrodesis has been shown
to function as well as the radiographically solid fusion in many cases. After resection ofthe
articular surfaces, arthrodesis is completed with pin stabilization, starting the 0.045" (or
0.062" if desired) K-wire atthe base of, or hole in, the middle phalanx and driving it distally
across the dorsiflexed and straightened DlPJ, then out the tip of the digit centrally. Care is
taken to avoid perforation of the nail bed. The K-wire is then retrograded
proximally across the PIPJ to the base of the proximal phalanx, then across the
realigned MTPJ if indicated by persistent upon push-up loading. Stabilization of the MTPJ
is performed with the toe situated half way between the horizontal substrate (parallel to
the bottom of the foot), and in line with the metatarsal declination angle.
Digital alignment is slightly over-corrected in plantarflexion, and the pin crossing the MTPJ
maintained for 3-6 weeks. The PIPJ fusion is stabilized for 5-6 weeks, or until
radiographic and clinical evidence of fusion is observed. PlaCing the pin across the MTPJ
requires use of a built-up surgical shoe postoperatively, in order to avoid
repetitive mechanical flexure and pin breakage in the MTPJ (Figure 7-8). Interphalangeal
arthrodesis can also be achieved using bioabsorbable fixation pins or screws, and other
devices made to press-fit or snap-fit once seated in either the proximal and/or middle
phalanges. It is important to keep in mind that if absorbable fixation, or a device that is
limited to just the interphalangeal joint/s, is used to achieve digital fusion, attention to the
alignment of the corresponding MTPJ may require separate fixation or metatarsal
osteotomy, if the push-up test fails to display satisfactory MTPJ realignment. After
realignment of the toe and MTPJ, the long extensor tendon is re-approximated in corrected
alignment, followed by subcutaneous and then skin closure.
Flexor tendon transfer (Girdlestone, Foerster and Brown}-can also be useful for the
correction of hammertoes and clawtoes, however care must be taken to transfer the
sectioned flexor tendon slips from plantar to dorsal on the phalanx in a subperiosteal
fashion (to avoid constriction of digital vessels), or through adrill hole in the phalanx, and it
is possible to effect a PIPJ rocker-bottom deformity unless arthrodesis is performed
(obviating the need for flexor tendon transfer). Sgarlato's modification of the Girdlestone
procedure can be used for the correction of hammertoes and clawtoes with MTPJ
171 Ch. 7 Reconstructive Surgery of Basic Conditions and Deformities
subluxation, and serves to redirect the long extensor tendon's pull to that of a stabilizing
influence on the toe and MTPJ. Two incisions are used, 1medial or lateral aspect at the
proximal phalanx, and an adjunct dorsal incision more to the side opposite the medial or
lateral incision. The long flexor tendon is split and transferred dorsally in a subfascial
fashion and sutured to itself and the dorsal hood expansion as a sling dorsally atthe level
of the proximal phalangeal shaft. Care must be taken to transfer the split tendon segments
in a subfascial (deep fascia) fashion, in order to avoid circumferential constriction of the
subcutaneous neurovascular elements coursing to the toe tip. The transfer results in
decreased PIPJ range of motion. Dockery and Kuwada modified the transfer by use of a
dorsal-to-plantar drill hole in the anatomic neck ofthe proximal phalanx. Moreover, arocker
bottom PIPJ or swan-neck deformity can be created iftoo much tension is placed within the
transferred long flexor. PIPJ arthrodesis is generally considered a more effective and
lasting method to stabilize the digit and convert the long flexor to astabilizing influence on
the MTPJ, particularly for the intermediate lesser digits. A flexor tendon transfer may be
applicable to the fifth toe, or in the presence of congenital absence ofthe middle phalanx.
BUNION DEFORMITY AND HALLUX ABDUCTO VALGUS
First metatarsal anatomy pertinentto the bunion deformity and hallux abductovalgus (HAV,
hallux valgus) surgery includes the proximal physeal plate, which closes at about 15-18
years of age, the primary nutrient artery situated laterally about 2 cm proximal to the
articular surface, and the peri-articular soft tissue sleeve and sesamoid apparatus. When
the hallux abducts and the first metatarsal adducts (metatarsus primus varus), the
dorsomedial eminence of the first metatarsal head becomes clinically prominent, and is
termed a "bunion." The term bunion basically refers to a bump, traditionally, from the old
French buignon, from buigne or "bump on the head." (Similarly, aprominent fifth metatarsal
head is often referred to as a bunionette.)
Radiographic Angular and Anatomic Relationships Related to HAV-there are a number
of angular relationships useful in the assessment of HAV, including:
HalluxAbductusAngle (HAA}-the angle formed by the intersection ofthe bisection of the
shaft of proximal phalanx and the bisection of the shaft of first metatarsal,
normally 15, and representative of the relative position of the hallux to the first metatarsal
(Fig 7-9).
Distal Articular Set Angle (DASA}-the angle formed by the intersection of a line
perpendicular to the effective cartilage of the base of the proximal phalanx and the
bisection of the shaft of the proximal phalanx, normally 7.5, and representative of the
relative position of the effective cartilage to the shaft of the proximal phalanx. An increase
in DASA may indicate lateral deviation in the shaft of the proximal phalanx (Fig 7-10).
Proximal Articular Set Angle (PASA}-the angle formed by the intersection of a line
perpendicular to the effective articular cartilage of the metatarsal head and the
bisection of the shaft of the first metatarsal. normally 7.5", and representative of the
relative position ofthe effective cartilage to the shaft of the metatarsal. An increase in PASA
indicates lateral deviation (adaptation) of the cartilage surface (Fig 7-11).
172 Reconstructive Surgery of Basic Conditions and Deformities Ch. 7
Figure 7.9 Figure 7.10 Figure 7.11 Figure 7.12
Metatarsus PrimusAdductus orFirst Intermetatarsal Angle (first IMA)-the angle formed
by the intersection of the bisection of the shaft of the first metatarsal and the bisection
of the shaft of the second metatarsal, normally 8, and representative of the angular
relationship between the first and second metatarsals. An increase in the first IMA makes
the head ofthe first metatarsal more prominent medially, and predisposes to HAV (Fig 7-12).
Hallux InterphalangeusAngle (HIA)-the angle formed by the intersection ofthe bisection
of the shaft of the proximal phalanx and the bisection of the distal phalanx, normally 10,
and representative of hallux interphalangeal joint (HIPJ) or phalangeal deformity (Fig 7-13).
Metatarsal Protrusion Distance-the distance between two arcs which, respectively,
represent the lengths of the first and second metatarsals. A line representing the
bisection of the first metatarsal is extended to intersect with a line representing the
bisection of the second metatarsal. A compass is placed atthe point of intersection and an
arc drawn from the distal portion of the first metatarsal and another arc is drawn from the
distal portion of the second metatarsal. A positive millimeter distance is used to indicate a
longer first metatarsal. Anegative distance is used to indicate the second metatarsal being
longer than the first. Normal is 2mm, and represents the relative length between the first
and second metatarsals. A longer first metatarsal may be associated with hallux limitus,
while shortening may correlate with lesser metatarsalgia (Fig 7-14).
Metatarsus Adductus Angle (MAA)-the angle formed by the intersection of the
bisection of the lesser tarsus and the bisection ofthe second metatarsal. The lesser tarsus
is bisected by obtaining the midpoint between the anterior-medial corner of the first
cuneiform and the posterior-medial corner of the navicular, and the midpoint between the
anterior-lateral corner of the cuboid and the posterior-lateral corner of the cuboid. The
midpoints are then connected and a perpendicular is drawn to this line. The MAA is
normally 10-20"; and represents the degree of adduction ofthe metatarsus. As the MAA
increases, the foot becomes more adducted and there is greater chance for development
of HAV. Moreover, the first IMA becomes pathologically significant at alower degree in the
presence of increased MAA (Rg 7-15).
Tibial Sesamoid Position (TSP)-the position the tibial sesamoid is compared to the
bisection of the first metatarsal shaft, and designated as position 1-7; normally 1-3, and
traditionally representative of the need to remove the fibular sesamoid. TSP 4
predicts erosion of the tibial sesamoid against the plantar central crista of the metatarsal
173 Ch. 7 Reconstructive Surgery of Basic Conditions and Deformities
Figure 7.13 Figure 7.14 Figure 7.15 Figure 7.16
head, and relative deviation of the metatarsal head medially so thatthe fibular sesamoid is
positioned in the first intermetatarsal space. When the first metatarsal plantarflexes, a
relative distal position of the sesamoids may appear, whereas dorsiflexion causes relative
proximal positioning (Fig 7-16).
Shape 01 the Metatarsal Head--the intrinsic stability ofthe MTPJ varies with the shape of
the metatarsal head. A round head is theoretically most unstable and likely to deviate into
HAV; a square head is considered stable, and a square head with a central ridge is
considered most stable and may be seen in cases of hallux rigidus (Fig 7-17).
First MTPJ Position (Congruous, Deviated or SubluxatedHrst MTPJ alignment can be
congruous, deviated or subluxated. In the congruous joint, a parallel relationship exists
between the effective articular cartilage of the metatarsal head and the phalangeal base.
The deviated joint displays extra-articular intersection of the lines representing the
effective articular surfaces of the metatarsal head and phalangeal base. The subluxated
(subluxed) joint displays intra-articular intersection of the lines representing the effective
articular surfaces of the metatarsal head and phalangeal base (Fig 7-18).
Figure 7.17
174 ReconstructiveSurgeryofBasic Conditionsand Deformities Ch.7
Figure7.17
Figure7.18 Congruous Deviated Subluxated
Structural, Positional, and Combined HAV Deformities-HAV can be classified as to
whetherornotthefirstMTPJ deformityisstructural,positional,oracombined deformity
basedontheformulaedepictedinTable7-1.
Table 1-1. FORMULAE FOR STRUCTURAl., POSmONAI.,AND COMBINED FIRST MTPJ
DEFORMITIES.
TYPEOF ANGLE PASAANDI FlRSTMTPJ
DEFORMITY FORMULA ORDASA AUGNMENT
Structural PASA+ DASA=HM PASAorDASA Abnormal,congruent
Positional PASA+ DASA< HM PASAandDASA Normal,deviated
orsubluxed
Combined PASA+ DASA< HM PASAorDASA Abnormal,deviated
orsubluxed
Example1:
HM=35, DASA 3, PASA =5(3 + 5<35, so MTPJ displayspositional deviation or
subluxation,asPASAand DASAarenormal).
Example2:
HM 35, DASA=7", PASA 2SO (7 + 28=35,so MTPJdisplaysacongruous structural
deformity,and PASAisabnormal).
Example3:
HM=35", DASA 1, PASA=18"(1 +18<35,so MTPJ displaysacombined deviatedor
subluxateddeformity,and PASAisabnormal).
175 Ch.7 Reconstructive Surgery of Basic Conditions and Deformities
Bunionectomies-specific procedures for bunion repair vary a great deal, and it is the
surgeon's responsibility to select the best procedure for the patient in question. Procedure
selection varies with patient expectations, bone stock, local and systemic tissue status, the
degree of deformity relative to the anatomic relationships, and the surgeon's skills. Repair
options are categorized as soft tissue manipulations, hallux osteotomies, and distal, shaft
and base metatarsal osteotomies, and combinations thereof.
Soh tissue manipulations used for correction of HAY include:
McBride Bunionectomy---this is a versatile and powerful
component of many bunion repairs, and focuses on muscle-
tendon balance that addresses the underlying pathologic
influences in the development of HAV. Preoperative criteria include
mild to moderate pain associated with the sesamoid apparatus, first
MTPJ range of motion that is essentially free of crepitus or
significant articular degeneration, mild-moderate axial rotation
(valgus) of the hallux, prominent dorsomedial bunion, medial
bursitis; and radiographic signs such as relative hypertrophy ofthe
medial eminence, deviated to subluxated first MTPJ, and a tibial
sesamoid position of 4or greater. Specific surgical maneuvers used
in the true McBride bunionectomy include medial exostectomy, Figure 7.19
excision of the fibular sesamoid, medial capsulorrhaphy, and
transfer ofthe adductor hallucis tendon to the deep surface ofthe
medial capsular flap (Figure 7-19). The modified McBride procedure involves preservation
of the fibular sesamoid, with adductor tendon transfer following complete plantarlateral
soft tissue release (Figure 7-20). The primary limitation of the McBride procedure is an
inability to correct a structural deformity of the metatarsal head. The modified McBride
procedure serves as the foundation for many bunionectomies, and is usually combined with
first metatarsal osteotomy for the correction of HAV with metatarsus primus varus. Over-
aggressive manipulation ofthe soft tissues using the McBride procedure can over-correct
and predispose the patient to the development of hallux varus. Proper execution of soft
tissue release and realignment about the first MTPJ, in conjunction with distal metatarsal
osteotomy, can be carried out safely and withoutthe development of capital fragment AVN.
B
Figure 7.20
Keller Bunionectomy---this joint destructive procedure is a time-honored technique for
alleviation of debilitating pain related to severe, advanced HAV, usually with concomitant
DJD and/or hallux rigid us. Indications include apropulsive gait, pain in the first ray and lesser
metatarsalgia (lateral dumping) that presents a constant impediment to ambulation,
--------
176 Reconstructive Surgery of Basic Conditions and Deformities Ch.7
stiffness, and inhibition of weight bearing or motion. The Keller procedure classically
involves resection of the base of the proximal phalanx of the hallux. A number of
modifications of the Keller procedure have come to be appreciated in order to prevent
complication, including: re-attachment ofthe flexor apparatus to the phalangeal shaft, use
of a long medial capsular flap that serves as a sling to resist hallux abduction, and
lengthening of the EHL (and brevis). Other variations include usa oftha medial capsular flap
as a biological trellis over the metatarsal head (Ganley modification), K-wire nailing for
temporary stabilization, and purse string capsular interposition. The main complications
related to the Keller procedure are shortening of the hallux, recurrent hallux abductus,
hallux elevatus, lesser metatarsalgia secondary to proximal retraction of the sesamoid
apparatus, and sub-second metatarsal head IPK. The development of complications is
reduced with implementation of the modifications.
Silver (Simple) Bunionectomy-may be used in cases where bump pain and medial
cutaneous compromise predominate, especially in the elderly or debilitated host. It does not
address sesamoid pain, deep joint pain, or dynamic MTPJ imbalance. Preoperative
criteria include a satisfactory first MTPJ range of motion, no crepitus, and often a medial
adventitious bursa is present. Surgery focuses on simple resection of the dorsomedial
eminence of the first metatarsal head while preserving the plantar sesamoidal shelf.
Caution should be taken to use a digital retainer postoperatively, so that rapid advance of
hallux abductus due to loss of medial capsular-ligamentous tethering of the hallux, is
countered. The procedure may convey poor long-term results, and recurrence may occur
because the etiology of the deformity is not addressed. The combination of first metatarsal
head medial exostectomy and Akin osteotomy for correction of significant HAV,
particularly in ayoung or active patient wherein systematic disarticulation and first MTPJ
reconstruction are not addressed, can convey a high rate of recurrent deformity.
Hallux osteotomies used for correction of HAV include:
Standard Akin Osteotomy-a closing adductory osteotomy of the
proximal metaphysis of the proximal phalanx of the hallux,
indicated for correction of true hallux interphalangeus or an
increased DASA. The Akin osteotomy is rarely indicated as an
isolated procedure, and is usually used in conjunction with more
proximal intervention that addresses first MTPJ muscle-tendon
balance and/or structural deformity. The Akin osteotomy itself does
not directly address a bunion deformity or HAV. Inadequate
correction ofthe first MTPJ cannot be adequately corrected with a
"cheater Akin," which creates the clinical appearance of a
straightened hallux even in the presence of adeviated or subluxated
first MTPJ. The Akin procedure employs a wedge osteotomy in the
proximal phalangeal proximal metaphysis, the distal arm of the
osteotomy being perpendicular to the long axis of the phalanx and
the proximal arm being parallel to the articular surface of the phalanx F 721
(Figure 7-21'. Caution should be practiced if the proximal phalanx is Igure.
short, and the physis should be closed in a young patient. The
osteotomy is stabilized using a nonabsorbable suture, wire suture, a K-wire, an
absorbable pin, or astaple. The Akin is an adjunct procedure to MTPJ realignment.
Ch. 7 Reconstructive Surgery of Basic Conditions and Deformities
Cylindrical Akin Osteotomy-a cylindrical resection of the proximal
phalanx, usually at the junction of the diaphysis and proximal
metaphysis, to correct abnormally high DASA and/or HIA in a very
long proximal phalanx. The epiphysis should be closed, and delayed
diaphyseal healing is arisk. The Akin is an adjunct procedure to MTPJ
realignment (Figure 7-22).
Distal Akin Osteotomy-a closing adductory proximal phalangeal
osteotomy positioned in the distal metaphysis, and indicated for the
correction of HIA >10-12, in the presence of a congruous first MTPJ
(corrected), and an adequately long phalanx. It can be used even when
the proximal physis is open. The Akin is an adjunct procedure to MTPJ
realignment (Figure 7-23).
Distal first metatarsal osteotomies used for correction of HAV:
Reverdin Osteotomy-a useful technique for correction of high PASA,
when used in conjunction with appropriate muscle-tendon balancing
ofthe first MTPJ. The Reverdin can be performed in young patients,
however it is most frequently used in conjunction with atrue McBride
procedure in an elderly patient with an advanced, yet
flexible HAV. The osteotomy is an intra-articular closing adductory
wedge osteotomy, at the level of the sesamoid apparatus, that
preserves an intact lateral cortical hinge. The distal cut is made
proximal and parallel to the residual articular cartilage of the
metatarsal head, and the proximal cut is made perpendicular to the
long axis of the first metatarsal (Figure 7-24), The osteotomy is
oriented perpendicularto the substrate (weight-bearing surface), and
positioning the osteotomy distal to the sesamoid apparatus may
theoretically decrease weight bearing load on the capital fragment.
Removal of the medially based wedge of bone decreases articular
cubic content, and may enhance range of motion in cases involving
hallux limitus. Placement of the osteotomy distal to the weight
bearing level of the sesamoids increases the risk of capital fragment
AVN. The osteotomy is ideally fixated with 1or 2diverging segments
of bioabsorbable pin. Alternative fixations include stainless steel wire
suture or 2-0 absorbable suture. AK-wire may also be used. The main
complications of the Reverdin osteotomy include AVN, sesamoiditis,
and first MTPJ stiffness. The Reverdin osteotomy enables first IMA
reduction via reverse buckling, wherein the hallux applies an
abductory force on the head of the flexible first metatarsal when
bandaged in slight overcorrection.
Green-Modified Reverdin Osteotomy (distalL}-a useful
modification of the classical Reverdin osteotomy, wherein ahorizontal
plantar osteotomy is made through the metatarsal head, dorsal to the
sesamoid, so that the Reverdin cuts do not penetrate the plantar
corte)( and violate the sesamoidal articular surfaces (Figure 7-25),
Figure 7.22
Figure 7.23
Figure 7.24
177
178 Reconstructive Surgery of Basic Conditions and Deformities Ch.7
-----------------------_...._-
Laird-Modified Revert/in Osteotomy-combines the Green-modified Reverdin with
completion ofthe osteotomy through the lateral cortex, eliminating the intact cortical hinge
and allowing transverse plane translocation of the capital fragment toward the second
metatarsal in an effort to decrease the first IMA. A K-wire or other fixator is required to
stabilize the capital fragment, and AVN is a risk (Figure 7-26).
Todd-Modified Reverdin Osteotomy-combines the Laird-modified Reverdin with
penetration of the plantar cortex to enable sagittal plane correction in addition to
transverse plane correction.
Peabody Osteotomy-addresses ahigh PASA using the same osteotomy as described for
the traditional Reverdin, however the osteotomy is positioned at the anatomic neck of the
first metatarsal. Bone healing is traditionally slower due to a higher degree of cortical bone
atthe more proximal location.
Wi/son Osteotomy-an oblique, through-and-through osteotomy of the surgical neck of
the metatarsal. usually oriented from distal-medial to proximal-lateral to allow reduction of
the first IMA with shortening of the metatarsal. The orientation of the osteotomy can be
reversed to elongate the metatarsal, or oriented perpendicular to the long axis of the
second ray to avoid shortening or lengthening. The Wilson osteotomy, in the past. was often
employed in minimal-incision surgery, and conveys a high risk of malunion, delayed
union, and recurrent deformity or transfer metatarsalgia when not adequately controlled
and stabilized.
Mitchell Osteotomy-a popular distal metaphyseal. step-down osteotomy wherein the
distal arm of 2parallel cuts does not penetrate the lateral cortex while the proximal arm does.
Completion of the osteotomy allows both transposition and angulational correction of the
capital fragment. It is used for correction of mildly increased first IMA, and dorsal
displacement of the osteotomy can be problematic (Figure 7-27).
.......
~
Figure 7.25
Figure 7.26 Figure 7.27
179 Ch.7 Reconstructive Surgery of Basic Conditions and Deformities
Austin Osteotomy-perhaps the single most commonly used osteotomy for correction of
moderate HAV, wherein the first IMA is usually no more than 16, and the joint is not
degenerated. The procedure consists of a through-and-through, sagittal plane
V-osteotomy (chevron), with base proximal and apex distal, situated atthe first metatarsal
metaphysis. The osteotomy allows triplanar correction. The apex of the osteotomy is
positioned at the center of the imaginary circle of the metatarsal head, and application of
a smooth K-wire as an apical axis guide, for many surgeons, enhances control of the saw
and predetermines the direction of displacement ofthe capital fragment. The arms of the
V-cut usually intersect to form a 60angle, however an offset-V, such as the Vogler and
Kalish modifications, with the dorsal arm extending proximally to the proximal (Vogler
osteotomy) or midshaft (Kalish osteotomy) level of the metatarsal can be used to achieve
interfragmental screw fixation and, perhaps correct a higher degree of metatarsus primus
adductus by virtue of additional angular correction made available by swiveling the distal
fragment upon the proximal portion of the metatarsal. An offset-V osteotomy positioned
through the shaft, with the dorsal arm exiting near mid-diaphysis, namley Kalish's
modification of the Austin, is readily stabilized with 2interfragmental compression screws.
An offset-V osteotomy positioned through the shaft, with the dorsal arm exiting near the
proximal metaphysis, namley Vogler's shaft osteotomy, is ideally suited to enable a
significant amount of transverse plane swivel of the dorsal fragment to reduce PASA
(Figure 7-28), and may be used to correct rather large degrees of HAA and first IMA. The
degree of displacement of the capital fragment in the Austin procedure, and its variations,
is dependent upon the width of the metatarsal and orientation of the osteotomy. The
plantar arm of the osteotomy creates a shelf that resists weight bearing, and the
osteotomy is very stable when soft tissues are properly preserved. Fixation of the
traditional Austin osteotomy is via buried or percutaneous K-wires, absorbable pins, or lag
screws. Although originally described as an unfixated osteotomy, the addition of fixation
decreases the likelihood of delayed union, loss of correction, and AVN of the capital
fragment. Postoperative care involves weight bearing in a surgical shoe and early return
{3-4 weeks) to a soft shoe or sneaker.
Figure 7.28
Oerotational Abductory Transpositional Osteotomy (ORATO)-a relatively difficult and
infrequently used osteotomy of the metatarsal head that addresses valgus rotation, PASA,
metatarsus primus varus, and sagittal plane (usually elevatus) deformity. The DRATO
osteotomy is performed through the cortical bone of the anatomic neck, and requires cast
immobilization and K-wire stabilization. Complications, including AVN and delayed union, as
well as technical difficulties which have limited the use of this procedure.
180 Reconstructive Surgery of Basic Conditions and Deformities Ch.7
Shaft osteotomies of the first metatarsal used for correction of HAV:
Off-set V Osteotomy weight bearing,
sagittal plane V-osteotomy (described above in the
discussion of the Austin osteotomy) that extends
through the shaft of the metatarsal (Fig 7-29), allowing
correction of a moderate to high first IMA, PASA via
swiveling ofthe dorsal fragment, and application of lag
screws or a K-wire or Steinmann pin for stabilization.
Gudas-scarf Osteotomy-this Z-plasty osteotomy
accomplishes the same goals as does the Vogler
off-set V osteotomy, however it employs 3 bone cuts
whereas the V-osteotomy employs just 2 cuts
(Fig 730). The osteotomy, and its shortened variation,
the short Z-osteotomy, is amenable to lag screw or
pin fixation.
LudloffOsteotomy-this osteotomy involves astraight oblique transection ofthe metatarsal
shaft from dorsal-proximal to plantar-distal, and is typically fixated with lag screws and
maintained for 6-8 weeks non-weight bearing. The Ludloff design can be used to elongate
the metatarsal 1-2 mm when indicated (Figure 7-31).
Mau Osteotomy-this osteotomy involves a straight oblique transection of the metatarsal
similar to the Ludloff, however the orientation of the osteotomy is reversed (dorsal-distal to
plantar-proximal) (Figure 7-32).
Figure 7.29
Figure 7.30
B
Figure 7.31
Figure 7.32
181 Ch. 7 Reconstructive Surgery of Basic Conditions and Deformities
Proximal osteotomies of the first metatarsal and medial cuneiform, and metatarso-
cuneiform arthrodesis, for correction of HAV:
Juvara Oblique Base Wedge Osteotomy-employs the hinge axis concept (Figure
7-33) to create an oblique, closing abductory base wedge osteotomy that enables
correction in the transverse and sagittal planes. The osteotomy is oblique and
measures about twice the width of the metatarsal base. The Juvara is suitable for
correction of a first IMA of >16, as long as the bone stock is satisfactory and the metatarsal
base not too narrow. It can be used in the presence of an open proximal physis, as long as
the osteotomy is positioned distal to the growth plate. A dorsomedial hinge allows
reduction of the first IMA with plantar declination of the distal fragment. Use of a pure
medial (vertical) hinge only allows reduction ofthe first IMA, whereas aplantarmedial hinge
allows dorsal excursion along with reduction of the first IMA, and a dorsomedial hinge
allows plantar excursion along with reduction of the first IMA. The osteotomy is ideally
suited for fixation using an anchor and lag, 2-screw arrangement. Potential complications
include delayed or nonunion,shortening and/or elevatus with transfer metatarsalgia, and
medial dorsal cutaneous neuritis (Figure 7-34). There are 3variations of the Juvara oblique
base osteotomy:
Type A-nblique osteotomy directed from distal-lateral to proximal-medial,
with an intact medial cortical hinge, the arms of the osteotomy creating an
approximately 15wedge resection.
Type 8---proceeds as described for Type A, however the medial hinge is sectioned
after wedge resection and a greater degree of sagittal plane manipulation can be
achieved, as well as shortening or lengthening by means of swiveling or sliding the
fragments upon one another.
Type C-an oblique osteotomy without wedge resection, completing the hinge thereby
allowing swiveling and sliding manipulations as in Type B.
Figure 7.33
Figure 7.34
182 Reconstructive Surgery of Basic Conditions and Deformities Ch,7
Tmnsverse Base Wedge (Louisan-Balacescu) Osteotomy-involves atransverse, closing
abductory, base wedge osteotomy of the proximal metaphysis, and maintains an intact
medial cortical hinge. The osteotomy is not amenable to lag screw fixation, and crossed
K-wires or stainless steel wire suture are applicable, in conjunction with immobilization and
non-weight bearing up to 6-8 weeks.
r',I'
,,41
--
Crescentic Base Osteotomy-uses a crescent shaped saw blade
to create a crescentic osteotomy in primarily the transverse plane
(TPI, offering easy manipulation of the distal segment into a
corrected alignment in the TP. Sagittal plane (SP) correction must
be addressed via orientation of the osteotomy to include motion in
the SP. Minimal shortening occurs with this osteotomy if stability is
maintained. Delayed union is the most likely complication, and
crossed K-wire, lag screw and stainless steel wire suture fixation
can be used in conjunction with immobilization and non-weight
bearing for 6-8 weeks (Figure 7-35).
Figure 7.35
Proximal Chevron Osteotomy-a chevron osteotomy can be
positioned at the base of the metatarsal, and may be useful in regard to correction of the
first IMA, and asmall to moderate amount of angulational correction can also be achieved
by means of swiveling. The osteotomy can be fixated in a nuber of ways, including
interfragmental compression screw or screws, or splintage methods, and non-weight
bearing and immobilization for up to 6-8 weeks are indicated.
Opening Wedge (Trethoan) Osteotomy and Bone Gmb-this
repair can be performed on a short metatarsal, and
traditionally packs a medial base cortical osteotomy with the
resected bone of the medial eminence (autogenous bone graft)
to lengthen the medial cortex of the metatarsal. Consideration
should be given to harvesting autogenous corticocancellous graft
from the calcanean body, as the medial exostectomy may not
provide adequate graft material. Alternatively, the use of a suit-
able bone graft substitute can work well. Astaple or K-wire may
be used to stabilize (non-compressive splintage) the graft, and
immobilization and non-weight bearing up to 6-8 weeks are in
order (Figure 7-36). Specialized locking fixation plates (Darco""
Figure 7.36
plates) are ideally suited to this procedure.
Lapidus Procedure (First Metatarsal-Cuneiform Arthrodesis}-applicable when there is
DJD, pain and/or instability atthe first metatarsal cuneiform articulation in conjunction with
ahigh first IMA and bunion deformity, often observed with around first metatarsal head. The
Lapidus procedure may shorten the first ray, and it is combined with a bone graft for this
reason. Fixation is usually via lag screws and a neutralization or load-screw plate applied
to the medial-plantar aspect ofthe metatarsal and, as with the opening wedge procedure,
specialized locking fixation plates (Darco' plates) are also suited to this procedure. Care
must be takentto accurately manipulate the intercuneiform and intermetatarsal articulations
as desired, and avoidance of excessive shortening is also important. Immobilization and
non-weight bearing for up to 10-12 weeks may be in order (Figure 7-371.
183 Ch,7 Reconstructive Surgery of Basic Conditions and Deformities
A B
Figure 7,37
Figure 7,38
Cotton Procedure (Medial Cuneiform Opening Wedge Osteotomy and Graft}-this
procedure addresses excessive first metatarsal-cuneiform adductus, and employs
application of the resected medial exostosis of the first metatarsal head or, more
typically abone graft substitute perhaps combined with ipsilateral calcaneal or distal tibial
donor bone, as an autogenous graft placed into the opening medial cuneiform
osteotomy, The osteotomy preserves the lateral cortex of the medial cuneiform, Pin or
staple splintage, or locking fixation plates, along with immobilization and non-weight
bearing are also employed, Complications include cuneiform AVN, medial dorsal cutaneous
neuritis, and TA tendinitis, This procedure may be applicable in the correction of
metatarsus adductus, when combined with aclosing wedge osteotomy ofthe cuboid,
Epiphysiodesis for Juvenile HAV-this may be applicable for correction of mild
juvenile HAV, wherein the first IMA is not greatly increased, Epiphysiodesis represents an
effort to control the final position of the first metatarsal by either staple fixation or bone graft
interposition at the lateral aspect of the first metatarsal base physis (Figure 7-38), The
staple can be removed at a later date, however bone graft consolidation of the physis is
permanent Attention must be paid to standard growth charts, so that adaptation and
subsequent growth can be anticipated,
Combination Procedures for Correction of HAY:
Logroscino Procedure-application of a closing abductory base wedge osteotomy with
the Reverdin osteotomy, for correction of a high first IMA and PASA, comprises the
Logroscino procedure, Use of an Austin-type chevron osteotomy has also been described
in conjunction with a base wedge osteotomy, Obviously, double osteotomy is associated
with extensive disruption of periosteal and epiphyseal blood supplies, and conveys a
higher risk of bone healing complications, There have been cases reported of AVN of
the intervening segment of first metatarsal. usually associated with loss of osteotomy
stability proximally,
Stamm Procedure-this procudure involves application of an opening base wedge
osteotomy and graft with the Keller procedure, and may be of historical importance only,
184 Reconstructive Surgery of Basic Conditions and Deformities Ch.7
90
Dorsal and proximal
migration 01 instant
center of motion of
1sl MPJ as hallux
dorsiftexes.
Neutral
A
B
Figure 7.39
HALLUX L1MITUS AND HALLUX RIGIOUS
Hallux Iimitus/rigidus (HllHR) traditionally implies limitation of first MTPJ motion to less than
65of dorsiflexion, with excessive compressive load of the proximal phalangeal base upon
the dorsal aspect of the first metatarsal head as the end range of motion is approached
(Figure 7-39). More recently, it has been appreciated that at least 35 of first MTPJ
dorsiflexion is typically needed for normal walking, and less motion will usually result in
pain and inhibited ambulation. Some surgeons refer to any limitation of 1st MTPJ
dorsiflexion, in general, as hallux rigid us. Others distinguish between limitus and rigid us,
wherein rigidus is reserved for those cases that display minimal to no dorsiflexion. In this
manual, we will refer to the condition as hallux limitus/rigidus (HI./HR). Etiologies of HlIHR
include metatarsus primus elevatus related to hypermobile first ray, forefoot supinatus, or
iatrogenic metatarsal elevatus following base wedge osteotomy; a long first metatarsal,
which may be associated with a distal metaphyseal epiphysis (pseudoepiphysis);
immobility of the first ray due to lisfranc DJD or tarsal coalition; first MTPJ DJD due to
osteoarthritis, longstanding HAV, or systemic arthritic involvement of the joint; status-post
trauma or iatrogenic deformity; and even a short first metatarsal wherein the hallux
vigorously plantarflexes (hallux equinus) to stabilize the first ray in stance. Signs and
symptoms include pain and swelling, stiffness and crepitus, dorsal bony prominence
(dorsal bunion) and HIPJ overload with plantar hyperkeratosis, and lateral metatarsalgia due
to antalgic guarding of the painful first ray, apropulsive gait and fifth toe heloma durum
formation. Radiographic signs include subchondral sclerosis, joint space narrowing,
flattening of the metatarsal head, and osteophytosis with exostosis Idorsal flag sign)
formation. In some cases, the metatarsal.head displays a central ridge. It is importantto
ascertain the status and function of the sesamoids by loading the plantar aspect of the joint
while dorsiflexing the hallux. Nonsurgical treatment of HlIHR involves use of ametatarsal
bar or tapered rocker-sole, orthosis control of hypermobility, and range of motion physical
therapy; and these measures are combined with anti-inflammatory intervention, intra-
articular chondroprotective agent (chondroitin sulfate and glycosaminoglycan
preparations), and alteration of activities. The surgical treatment of HlIHR is founded upon
adequate chielectomy in conjunction with reconstructive osteotomy. Procedures include:
First MTPJ Chielectomy-involves removal of osteophytic proliferation via a
dorsomedial, longitudinal capsulotomy. It is necessaryto remove osteophytes and spur for-
Ch.7 Reconstructive Surgery of Basic Conditions and Deformities 185
mation from the dorsal, medial and lateral aspects ofthe joint, including the metatarsal head
and the phalangeal base. The metatarsal elevator can be used to release capsular and
sesamoidal adhesion plantarly atthe flexor plate. Loose or degenerated cartilage should be
debrided and sculpted to an intact and smooth surface, and exposed subchondral cortical
bone should be perforated with multiple 1.5 mm or 0.045" K-wire holes. Fenestration of the
cortex enables mesenchymal stem cells from the medullary sinusoids to cover the
articular surface and, under conditions of motion with reduced compression, convert to
functional fibrocartilage. It is important to understand that chielectomy does not address
structural deformity or the etiology that may have contributed to the condition in the first
place. First MTJ range of motion is initiated early in the postoperative phase. Chielectomy
is usually used in conjunction with metatarsal osteotomy and MTB, and serves as the
foundation upon which almost all repairs of HLJHR are based.
Watennann Osteotomy-a dorsally based trapezoidal wedge resection atthe surgical neck
of the metatarsal. designed to rotate plantar cartilage dorsally and decrease first MTPJ
cubic content. Complications associated with the Watermann osteotomy include capital
fragment instability, loss of correction, sesamoiditis, delayed and/or nonunion, AVN, and
inability to truly rotate the articular surface without creating a transverse angular ridge at
the apex of rotation. Excessive shortening of the first metatarsal may also predispose to
lesser metatarsalgia. The McGlamry-modified Watermann osteotomy preserves a plantar
cortical hinge, while resecting adorsally based, pie-shaped wedge of metatarsal head that
also rotates plantar cartilage dorsally and decreases internal cubic content of the joint
(Figure 7-40). Fixation is via absorbable pins or suture, or metallic splintage wires or screws.
The hallux may initially be splinted in dorsiflexion for a few days, however early passive and
active range of motion is desirable. The Watermann and McGlamry-modified Watermann
are used in conjunction with chielectomy.
Modified Green-Watermann Osteotomy-this involves chielectomy, and osteotomy of the
metatarsal neck wherein a rectangular section of bone is excised from the dorsal aspect
ofthe surgical neck, while a plantar arm (much like that used forthe Austin osteotomy) exits
the joint parallel to the substrate posterior to the articular surface (Fig 7-41). An axis guide
A__ ~ ~ ______
Figure 7.40
B ~ ~
Figure 7.41
186 Reconstructive Surgery of Basic Conditions and Deformities Ch.7
can be used to orient the arms of the osteotomy, and the first IMA can be reduced if
necessary. This procedure enables shortening of the metatarsal while simultaneously
allowing plantar declination of the capital fragment, thereby decreasing the risk of lesser
metatarsalgia. The osteotomy also avoids violation of the articular surface with the
osteotomy, decreasing both the risks of sesamoiditis and AVN. Fixation of the osteotomy is
performed with lag screws, smooth orthreaded K-wires, or absorbable pins. When threaded
K-wires are used, they are cut flush to the cortical surface and retained indefinitely.
Austin Osteotomy and Variations--this osteotomy has been described above, and is
applicable for correction of certain cases of H/HR. The apical axis guide is oriented
to effect primarily plantar declination of the capital fragment. which also limits
reduction of the first IMA. In the presence of concomitant HAV and HLJHR, the Green-
Watermann and Austin osteotomies enable simultaneous reduction of the first IMA,
although the Green-Watermann osteotomy generally enables greater plantar declination
without excessive shortening. The Youngswick modification of the Austin osteotomy
entails removal of atrapezoidal wedge of bone from the dorsal arm of the proximal segment
of the metatarsal, thereaby allowing plantar declination and some shortening of the first
metatarsal. This procedure is versatile and readily stabilized with tapered absorbable pins,
aK-wire, or an interfragmental compression screw.
Lambrinudi and Other First Metatarsal Plantarflexory Osteotomies-this employs an
oblique wedge osteotomy directed from plantar-distal to dorsal-proximal in the metatarsal
base, with the base distal and the apex proximal, and is designed to correct structural
metatarsus primus elevatus (Figure 7-42). Instability of the first metatarsal-cuneiform joint
contra indicates efforts at structural correction distal to the joint, and medial column
Lisfranc arthrodesis (such as the Lapidus) may be indicated. The osteotomy is fixated with
lag screws. Excessive shortening ofthe first ray may complicate the lambrinudi, however
concomitant over-aggressive plantar declination usually results in weight bearing
sesamoiditis. Various modifications of oblique base wedge osteotomy, abductory if
reduction of the first IMA is indicated, can also be used to achieve plantar declination ofthe
distal segment of the first metatarsal. Furthermore, osteotomy through the cortical hinge
allows plantar displacement ofthe distal segment via swiveling in the sagittal plane (Figure
7-43). Oblique and step-down (Giannestras) shaft osteotomies can also be used to effect
shortening and plantar declination of the distal segment of the first metatarsal
(Figure 7-44).
Opening PJantarflexory First Metatarsal Osteotomy-this can be used to correct
metatarsus primus elevatus, and involves adorsally based wedge graft of bone placed into
an osteotomy of the dorsal portion of the proximal metaphysis of the first metatarsal base.
Autogenous corticocancellous bone graft, or asuitable substitute, is used.
Mayo Procedure and Stone involve varying degrees of first metatarsal
head resection. The Mayo procedure involves oblique resection, from dorsal-proximal to
plantar-distal in the sagittal plane, of the dorsal aspect of the metatarsal head. The
osteotomy penetrates the articular surface centrally in the sagittal plane, and includes
resection of any medial osteophytosis. The Stone procedure more aggressively resects the
dorsal portion of the metatarsal head, and penetrates the articular surface just distal to the
Ch.7 Reconstructive Surgery of Basic Conditions and Deformities
A ~
B ~ S 7 i 7
Figure 7.42
Figure 7.43
Figure 7.44
187
sesamoids.ln effect, the Stone procedure attempts to preserve the plantar cortical surface
of the metatarsal head, while eliminating dorsal blockade to hallux dorsiflexion.
Heuter Procedure-this involves complete excision of the first metatarsal head, and may
be useful for the treatment of osteomyelitis, or as a component of pan metatarsal head
resection. This procedure irreversibly destroys the weight bearing function of the first ray,
and is of historical interest only in regard to the treatment of HL/HR.
Bonney-Kessel Osteotomy-this procedure involves resection of adorsally based wedge
of bone from the proximal metaphysis ofthe proximal phalanx of the hallux. however there
is very little indication for this procedure as it does not address metatarsus primus
elevatus, degenerative changes of the first MTPJ, or length of the first metatarsal. It has
been said that this procedure may be indicated in young patients without DJD, however it
must be stressed that failure to definitively address the biomechanical and structural causes
of HL/HR may result in progressive first MTPJ degeneration even after apparently correct-
ing lack of hallux dorsiflexion with a hallucial osteotomy. This criticism is analogous to that
of the isolated Akin osteotomy in the treatment of HAV.
Base enclavement (Regnauld procedure}-employs creation of a hat-shaped
osteocartilaginous proximal phalangeal base graft, in an effort to, theoretically decrease first
MTPJ tension and enhance range of motion (Figure 7-45). The hat-shaped graft is harvested,
and the proximal phalanx shortened via cylindrical resection of cortical bone, after which
the graft is implanted into the residual medullary canal of the phalanx. Care must be taken
to avoid proximal retraction ofthe sesamoids, which are the true weight-bearing level of the
first ray, and to this end actual relaxation of tension through the first MTPJ may be
compromised. The procedure has been shown most useful in repair of the traumatically or
iatrogenically deformed first ray with metatarsus primus varus aggravated by concomitant
proximal phalangeal elevatus. Fixation of the graft, despite its peg-in-hole arrangement,
can be tenuous, and crossed K-wires may be used.
188 ReconstructiveSurgeryofBasic Conditionsand Deformities Ch.7
ll
"'<>
, . ~ : : )
r1
~
J1
ll
t.
..~
i . ~
W
~
J1
Figure7.45
Keller Arthroplasty-the Kellerprocedure,whichhasbeendescribedabove,canalso be
usedtotreatHl/HR.
First Metatarsophalangeal Arthrodesis (McKeeverFus;on}-a rthrodesisofthefirstMTPJ
is aversatileandtime-honored method ofachieving astable, pain-freealignmentinthe
treatment of painful, inhibiting arthrosis (pain, decreased function, and deformity).
Indications for arthrodesis include apropulsive gait, flail toe, neuromuscular disease
(spastic orflaccid)'failed implant,failed Keller, previous bone and/orjointsepsis,and
previousintra-articularfracture.Thetechniqueisalsoapplicableforrheumatoidforefoot
reconstruction when combined with lesser metatarsal head resections and digital
stabilizations,anditcanalsobeusedtorepairlongstandinghalluxvarusorsevereHAY,or
CharcotdegenerationofthefirstMTPJ. Contraindicationsinclude limited and/orpainful
HIPJmotion,andinadequatebonestock.ItmaybecombinedwithHIPJfusionwhentheIPJ
isalreadyarthriticordeformed.Theoptimumpositionaffusionisparalleltothesecondtoe
inthetransverse plane, approximately 15-20ofsagittal plane dorsiflexion(varies with
anticipated heel height of shoes/boots), and a neutral frontal plane position.
McKeeveroriginallydescribed apeg-in-holetechnique,and modificationsofthiscan be
employed based on operative findings. However, effort should be made to
minimize bone resection and shortening, and the technique of cartilage removal via
curettageandperforationofthesubchondralplatetoexposecancellousboneworkswell,
as long as adequatetrabecularboneis exposed.Stabilizationofthe arthrodesis can be
achievedwithcrossedK-wires(0.045and/or0.062"),asingleaxialretrograded3/32"or5/64"
Steinmannpin,lagscrews,Herbertscrews,tensionbandwire,cerclagewire,oraplateand
screws, and there are specialized locking plates availableforthis procedure, as well.
Immobilizationandnon-weightbearingmaybehelpfulpostoperatively,howeveritmaybe
necessaryto use aremovable, modified walking castor brace thatfloatsthe hallux, in
patients with rheumatoid arthritis or neuroarthropathy. Advantages of first MTPJ
arthrodesis includepreservation ofintrinsicattachmentstothe phalanx,stability,good
cosmesis,improvedweightbearingfunctionofthefirstray,andspontaneousreductionof
the first IMA. Disadvantages include technical difficultiesthat relate to achieving the
optimalpositionoffusion;and post-fusiondifficultykneeling, potentialHIPJ overload and
degeneration,andpotentialdelayedornonunion.Abonegrowthstimulatormaybehelpful
incasesofdelayedunionoranticipatedbonehealingdifficulties.
189 Ch. 7 Reconstructive Surgery of Basic Conditions and Deformities
First Metatarsophalangeal Endoprosthesis (Implant Arthroplasry}-patlents suitable for
first MTPJ endoprosthesis implantation should display adequate neurovascular status, skin
coverage, bone stock, and adequate capsular and tendinous structures, as well as an
understanding and acceptance of the procedure. Indications also include apropulsive gait,
previous joint trauma, stiffness, and pain that inhibit weight bearing. Contraindications to
endoprosthesis implantation include dense peripheral neuropathy, advanced
osteoporosis, excessively short proximal phalanx, inadequate joint and/or cutaneous
coverage, and allergy to implant materials. Relative contraindications include previous
septic arthritis, or a young and active patient. The goals of endoprosthesis implantation
include the classic triad of reconstructive surgical goals: 1) decrease pain, 2) increase
function, and 3) reduce deformity. Patients undergoing endoprosthesis placement should
be informed ofthe subsequent need for prophylactic antibiotic therapy whenever they are
subjected to invasive procedures and dental work. Implant design has improved greatly
over the past 10-15 years, and use of a silicone polymer (Silastic) joint spacer has given
way to functional deSigns that enhance motion and bear weight during propulsion.
Technical refinements related to endoprosthesis of the first MTPJ include reattachment of
FHB and the sesamoid apparatus to the proximal phalanx, lengthening of EHL, sectioning
FHL, and proper angulation of bone resection. Alternatives to joint implantation for the
treatment of HL/HR with OJO include Keller arthroplasty and first MTPJ arthrodesis.
Complications associated with implants include stress-induced plastic deformation,
osseous and implant stress fracture, and microscopic shard production (wear debris) that
causes detritic synovitis with marked synovial thickening. Softer implant materials,
especially silicone polymer, are subject to wear-induced shard formation, although all
biomaterials will eventually show microscopic wear-and-tear breakdown. Implant
arthropathy consists of detritic synovitis, subchondral bone cyst formation, ectopic new
bone proliferation, and aseptic necrosis. Host soft tissue inflammatory reactions are ofthe
foreign body granuloma type, as shards are phagocytosed with resultant capsular
fibroplasia and encapsulation. (Silicone polymer has also been used in the production of
interphalangeal implants and as metatarsal caps following head resection.) Basic implant
designs include hemi-implant endoprostheses and total joint replacement models.
Hemi-implant arthroplasty-silicone polymer hemi-implant functions as a spacer
(not an endoprosthesis) and is rarely used in the first MTPJ. Indications for the
hemi-implant included joint space narrowing, osteophytosis, joint subluxation, and
preservation of a satisfactory first metatarsal articular surface, if the subchondral
bone plate has good contour and direction and if resection of metatarsal head
exostosis will not destroy functional articulating surface. The technique of hemi-
implantation involved dissection of the first MTPJ in a fashion consistent with that
described for the Keller bunionectomy. It is possible to perform aReverdin or Austin
osteotomy when hemi-implanting. The proximal phalangeal base is transected
perpendicular to the long axis of proximal phalanx (5 - 10 degrees of abductus is
physiologic). and the hub of the implant should be wider than the cortical width of the
phalanx. An excessively wide implant may limit range of motion. The medial capsular
flap, which is made long via avertical incision at about the mid-diaphyseal level (as is
done when performing the Keller) of the proximal phalanx, is reattached following
implant sizing and placement. The capsular flap is attached via drill holes in the
phalanx positioned dorsomedial and plantar medial. while a central plantar drill hole
is used to reattach the intersesamoidal ligament or the FHB directly, using 2-0
190 ReconstructiveSurgeryofBasic Conditionsand Deformities Ch.7
nonabsorbable suture.The Weil angulated hemi-implantincorporates a15lateral
deviation of the phalangeal base surface, designed to compensate for
deviationofthefirstmetatarsalarticularsurface(increasedPASA).
Total implant arthroplasty (total replacement arthroplasty}-the total implantis
applicable, in limited situations,wheresevere DJO ofboth articularsurfaces has
t
caused hallux rigidus. The Swanson-designed total implant, manufactured by
Dow-Corning Wright is made of Silastic silicone polymer. Contraindications
include ahigh first IMA and excessive HM,as the implant cannotstand up to
angular deforming forces over time. Prolonged angular deformation of the
implantwillresultin implantdegradation,and/orosseous erosion and/orfracture.
Metatarsallength ispreserved in an efforttoavoidtransfermetatarsalgia,andthe
majority of bone is resected from the phalanx. litanium grommets are
availabletofitovertheimplantstems,andfunctiontoshieldthesiliconepolymerfrom
wear at the bone interface. Sutter Biomedical's lawrence-designed total
implantdisplaysaproximalstemthatisangulated 15dorsally,to correspondtofirst
metatarsal declination; and theirlaPorta-designedtotal implantsdisplayright. left,
and neutraltransverse plane sided angulatedstems.Whenperformingtotalimplant
arthroplasty,thefirstIMAiscorrectedvia closingabductorybasewedge osteotomy
when indicated,orvia aggressive distal and dorsal firstmetatarsal resection using
the Mayo partial head resection. Complications oftotaljointimplantation include
floating ornon-purchasing hallux,iftoo muchmetatarsalhead is removed dorsally;
limited dorsiflexion and transfer metatarsalgia, iftoo much metatarsal head is
removedplantarly.
Multicomponent First MTPJ Endoprosthesis-these are designed to resist
wear-induced degradation while providing a degree of functional weight
bearingandmotioninthefirstray.Theycombinehighdensitypolyethylene(HOP)and
cobalt-chromium(CoCr) and/ortitanium alloy.Wearsurfaces are made ofHOP and
CoCr, while scintered sternsoftitanium provide aYoung's modulus compatiblewith
bone.Polymethylmethacrylatebonecementmaybeusedasaleutingagenttosecure
theimplantstems,howeverisusuallynotnecessarywhenappropriatebroachesare
used to seatthe device. These systems also employ osteotomy jigs (guides) for
preparation ofthe metatarsal and phalangealsurfacesto assure properfitwithout
excessiveboneloss,andallownear-physiologicalrangeofmotionwhilemaintaining
theweight-bearing level ofthe sesamoid apparatus.Accumet's greattoe implant
employsanextendeddorsalflangethattheoreticallyallowsanatomicrangeofmotion
asthefirstmetatarsal plantarflexesandthe halluxglidesdorsally.The Biomettwo
component endoprosthesis combines HOP and CoCr atthe wear surfaces. The
Bioactiontotalendoprosthesisisanothertwo-componentsystemmadeofHOp'CoCr
and titanium. and employs aplantarflangethatarticulateswiththe sesamoids and
theoreticallyenhancesweightbearingthroughthefirstray.
Autologous Cartilage Transplant Procedures (OATS and ACT}-osteoarticular
transfersystem(OATS) is asurgical procedure usedtotreatfocal cartilagedefects.An
osteochondral graft is usually harvested as multiple plugs procured from a
non-weight bearing surface of the knee, or the head of the talus, or some other
non-contactarticularsite. Once procured,the plugs aretransplantedtothe recipeintsite
191 Ch.7 Reconstructive Surgery of Basic Conditions and Oeformities
in amosaic fashion. Care must be taken to try and match subchondral cortical contour and
cartilage thickness between the donor and recipient sites. The donor site usually heals by
secondary intention, and the recipient site heals by means of graft incorporation and
fibrocartilage regeneration. It is important to maintain range of motion under reduced
pressure, during the healing phase. Another potentially useful method is that of autologous
chondrocyte transplant (ACT), which is a procedure that entails collection of normal
cartilage cells from, typically, inside the knee and are then sent to a laboratory to grow for
several weeks in tissue culture. Once they are grown in the laboratory, the chondrocytes
are then transplanted to the recipient site and secured by means of articular
reconstruction that will enable reduced weight bearing motion in the postoperative phase.
Asummary of the surgical options for the treatment of HlJHR is depicted in Table 7-2.
TABLE 7-2. ASTEPWISE APPROACH TO HALLUX LlMITUS/RIGIDUS.
Amountoffirstmetatarsalhead Surgicaloptionstobeusedalone
atticulardegeneration orincombination
<50% of central third of distal surface
250% of central third of distal surface
Arthroplasty
Cheilectomy and cartilage sculpting
Subchondral drilling (or cultured,
autogenous cartilage cell transplant)
Arthrodiastasis
Reconstructive osteotomy
Plantar and proximal displacement
(decompression)
Arthrodesis
Keller-type arthroplasty
Endoprosthesis
Autologous cartilage transplant (OATS)
Cultured cartilage cell transplant
HALLUX VARUS
Hallux varus involves an adductus and/or varus deviation ofthe hallux atthe first MTPJ, and
is usually observed as a complication of hallux valgus surgery. Contributing iatrogenic
influences include excessive resection of the medial eminence (staking the metatarsal
head), excision of the fibular sesamoid, overcorrection of the intermetatarsal angle,
over-tightening of the medial capsule, and overcorrection ofthe PASA. The condition can
also occur post-traumatically, congenitally or secondary to neuromuscular imbalance.
Symptoms include difficulty wearing conventional shoes, pain along the medial aspect of
the hallux secondary to shoe pressure, medial arch pain due to abductor hallucis spasm,
and pain and crepitus and limitus due to first MTPJ OJD. Clinical signs include adduction
and/or varus of the hallux, plantarflexion contracture ofthe hallux IPJ, and EHL contracture
effecting dorsiflexion ofthe MTPJ. Radiographic signs include hallux adductus, a reduced
or negative first IMA, possibly staked first metatarsal head and/or absentfibular sesamoid,
the presence of a previous osteotomy ofthe first metatarsal, a negative PASA, and MTPJ
OJO (narrowing, sclerosis, irregular contour). Non-surgical treatment includes counter-
192 Reconstructive Surgery of Basic Conditions and Deformities Ch.7
Figure 7.46
bandaging, padding, and shoe wear. Not every hallux varus requires surgical repair,
however significant deformity should be corrected as early as possible to prevent
resultant DJD. There is no single surgical procedure, but rather the causative factor must
be determined and corrected along with any secondary deformities that may have
developed. Surgical repair entails complete soft tissue release, correction of structural
deformity (reverse negative IMAl. tendon transfer about the first MTPJ (Figure 7-46), tibial
sesamoidectomy, and arthroplasty or fusion in severe or degenerative cases. Arthrodesis
is preferred in cases of neuromuscular imbalance or spasticity.
HALLUX INTERPHALANGEAL ARTHRODESIS
Hallux interphalangeal arthrodesis is usually used as an adjunct procedure in cavus foot
reconstruction, or following excision of the hallucial sesamoids. The deformity of hallux
malleolus, or cock-up hallux, can be repaired with hallux interphalangeal arthrodesis.
Indications for HIPJ arthrodesis include the presence of partially or nonreducible HIPJ
contracture, painful hyperkeratotic or ulcerative lesion overlying the IPJ, transverse or
frontal plane hallux deformity, hallux hammertoe, or an abnormally short or long hallux.
Signs and symptoms include painful and/or limited HIPJ motion; lichenification, keratoma,
or ulceration; and inability to wear regular shoes. Radiographic findings include the
contracted IPJ,jointspace narrowing, osteophytosis, and subchondral sclerosis; abnormal
hallux interphalangeal abductus angle; abnormal hallux length; and adequate bone stock
should be present when arthrodesis is considered. Biomechanical observations
associated with the need to fuse the HIPJ include instability of first ray and/or MTPJ
causing an abnormal weight-bearing position of the hallux, and severe pronatory
imbalance effecting forefoot supinatus, or loss of sesamoid stabilization ofthe hallux.
Surgery should be considered if a digital retainer and balanced inlay with aroller sole
have not satisfactorily alleviated symptoms. The surgical approach to the HIPJ is via either
alazy-S, L-shaped, or two semi-elliptical incisions. The joint is resected with attention paid
to angulation and length, and planned fixation method. Avariety of fixation methods can be
used, including stainless steel monofilament wire (single or double box loops of 20 or 22
gauge stainless steel wire), two crossed 0.045" K-wires, a single 4.0 mm cancellous lag
screw,a single 3.5 mm cortical lag screw, and a2.7 mm cortical lag screw.
Advantages of the stainless steel wire suture technique include relatively easy
application and minimal instrumentation, no need for intraoperative radiographs, can be used
193 Ch. 7 Reconstructive Surgery of Basic Conditions and Deformities
in conjunction with first MTPJ endoprosthesis, and it can be used when a sagittal plane
deformity of the hallux is maintained. Disadvantages of the stainless steel wire technique
include pull-through in osteoporotic bone, requires intact cortical bone adjacentto the fusion,
difficulty achieving uniform interfragmental compression, and the wire becomes a permanent
fixation device. Advantages of the K-wire technique include easy application and minimal
instrumentation, and affords effective splintage even in osteoporotic bone, and it need not be
permanent if placed percutaneously, and it can be used when asagittal plane deformity of the
hallux is maintained. Disadvantages of the K-wire include frequent need to confirm alignment
radiographically, pin tract infection, difficulty when used in conjunction with first MTPJ
endoprosthesis, and inability to generate interfragmental compression. Advantages of screw
fixation for HIPJ fusion include interfragmental compression, typically rapid primary bone
healing ensues, and earlier mobilization ofthe firstMTPJ is possible. Disadvantages of the lag
screw technique include technical difficulties with screw purchase and instrumentation,
prominence of the screw head distally at the hyponychium, screw removal is usually
indicated (and quite easy), intra-operative radiographs should be taken, not amenable to
concomitant first MTPJ endoprosthesis placement with stem of the implant secured in the
proximal phalanx, and sagittal plane hallux deformity must be corrected in orderto enable the
screw to seat properly in the phalanges. Postoperative management includes use of a
built-up surgical shoe, cast, and/or non-weight bearing for reduction of push-off loading of
the hallux for 6-8 weeks. Percutaneous pins can be removed at about 6-8 weeks pending
radiographic and clinical evidence of consolidation. A lag screw inserted from distal to
proximal should usually be removed at approximately 8weeks postoperative, unless the screw
head has not caused any distal irritation.
FIRST METATARSOCUNEIFORM EXOSTOSIS
This degenerative process generally accompanies chronic first ray hypermobility and
dorsal jamming at the metatarsocuneiform joint (MCJ).lt can be seen in anterior cavus, as
well as forefoot supinatus, and is overall a component of Lisfranc DJD. Over time, the
dorsal aspect of the MCJ becomes prominent, while plantar gapping occurs. Signs and
symptoms include cutaneous erythema, difficulty fitting shoes, medial dorsal cutaneous
neuritis, MCJ bursitis, EHL tendinitis and/or vamp disease. Anatomic considerations
relating to surgical intervention include the EHL and TA tendons, and the neurovascular
bundle. First MCJ exostosis is categorized as depicted in Table 7-3.
TABLE 7-3. FIRST METATARSOCUNEIFORM EXOSTOSIS.
Type of metatarsocuneifonn Clinical description of exostosis
exostosis
I Localized dorsal exostosis
II Dorsal exostosis with MCJ arthritis
III Dorsal exostosis with angular deformity, such as
adduction of the cuneiform and first metatarsal
IV Hyperostosis that extends across the
entire Lisfranc joint complex
Pseudoexostosis of anterior cavus,
wherein an actual exostosis is not present, although
the dorsum ofthe articulation is relatively prominent
V
194 Reconstructive Surgery of Basic Conditions and Deformities Ch.7
Exposure of the exostosis can be approached from the medial aspect via a curvilinear
incision situated between the EHL and TA tendons, and this will allow retraction of the dorsal
neurovascular elements while providing access to the dorsal exostosis. Exostectomy is
performed with osteotome and mallet or power instrumentation, followed by hand rasping.
The articular margins should be saucerized. If articular degeneration is extensive, then
arthrodesis should be considered, and is usually achieved with a combination of lag screws
and a neutralization or load-screw plate situated on the medial-plantar aspect of the
metatarsocuneiform fusion interface. Specialized locking plates are also available for this
fusion. Postoperative care involves application of acompression dressing and mobilization and
weight bearing to tolerance following exostectomy, or immobilization and non-weight
bearing following arthrodesis.
INTERMEDIATE (CENTRAL. Second-through-Fourth RAYS) METATARSALGIA and
DEFORMITIES
The primary causes of lesser ray pathology are dynamic in nature, and include retrograde
buckling of contracted digits (flexors stabilization, extensor substitution, and flexor
substitution). hypermobile first ray and hallux limitus/rigidus effecting lateral dumping of
weight bearing, and various forms of ankle equinus and dropfoot. Isolated structural
deformities affecting the intermediate rays are less common, but certainly exist and must
be considered when evaluating the patient with lesser metatarsalgia. Isolated structural
deformities may be congenital, post-traumatic, or iatrogenic; and include hypertrophic
plantar condyle, elongated metatarsal or adjacent brachymetatarsia, isolated metatarsal
equinus, or adjacent elevatus. Radiographic inspection of the intermediate lesser
metatarsals should include the lateral oblique projection, as this allows comparison ofthe
sagittal plane relationship of the central metatarsals. The metatarsal axial view, and
measurement of relative metatarsal protrusion on the weight bearing A-P view, may also be
helpful. Signs and symptoms include metatarsalgia, IPK, diffuse tyloma, and MTPJ
enthesitis. The differential diagnosis entails functional and structural etiologies, as well as
systemic arthritis, intermetatarsal neuroma, MTPJ enthesitis and/or bursitis, stress
fracture, thrombocytosis and erythromelalgia. Treatment involves attention to the dynamic
etiology, and conservative protection of the metatarsus, as well as anti-inflammatory
measures both systemic and local, and physical measures. Application of a metatarsal
projection pad to the insole proximal to the metatarsal heads, in conjunction with digital
retainers and supportive shoes, perhaps with a roller sole, can be helpful. A forefoot
extension with aperture padding may also be used. Surgical intervention usually entails
digital stabilization and MTPJ relocation via the sequential release. Isolated metatarsal
osteotomy may be used if digital surgery and supportive measures prove inadequate.
Caution is practiced when considering intermediate lesser metatarsal osteotomy, as the
incidence of recurrence, transfer lesion, floating toe, delayed and/or nonunion are
relatively high, especially when osteotomy fixation is not pursued.lntermetatarsal osseous
bridging may develop in cases wherein multiple adjacent metatarsal osteotomies are
performed, even when fixation, immobilization, and non-weight bearing are employed.
Selected lesser metatarsal surgical procedures include plantar condylectomy, distal and
proximal osteotomies, shaft osteotomies, and adjunct techniques such as syndactyly and
bone grafting. It is important to understand the need for appropriate digital stabilization and
MTPJ alignment when it comes to successful management of lesser metatarsalgia, and
the foundation role that digital stabilization plays relative to metatarsal surgery. A number
of surgical procedures are useful for treatment of intermediate metatarsalgia, and include:
195 Ch.7 Reconstructive Surgery of Basic Conditions and Deformities
Plalltar cOlldylectomy-used to reduce a hypertrophic or prominent plantarlateral
metatarsal head condyle, and is rarely indicated as an isolated procedure. The procedure
is usually performed via adorsal longitudinal incision over the MTPJ and is often combined
with arthrodesis of the corresponding and adjacent central PIPJ and sequential release of
the MTPJs, and syndactyly of the corresponding toe to the adjacent stabilized digit.
Syndactyly is an important adjunct procedure, as condylectomy results in decreased MTPJ
cubic content that in turn, allows the toe to float dorsally due to loss of plantar tethering.
The MTPJ capsulotomy enables plantar displacement of the toe and exposure of the
plantar condyles of the metatarsal head. Use ofthe metatarsal elevator may expedite this
exposure and delivery of the metatarsal head into view. The hypertrophic condyle is then
resected with the osteotome and mallet, and the remaining bone smoothed with the rasp.
Atemporary K-wire may be used to stabilize the toe and MTPJ if necessary. Layer closure
ensues, with attention paid to avoiding excessive EDL tension. A built-up surgical shoe will
be necessary if the MTPJ is pinned.
Weil osteotomy-this is a powerful procedure for shortening and elevating the
capital fragment of the metatarsal by means of a dorsal-distal to plantar-proximal oblique
osteotomy that can be fixated with asingle 2.0 or 2.7 mm interfragmental compression screw
from dorsal to plantar. Caution should be taken in regard to the prevention of a
postoperative floating toe, which can accompany any shortening or elevating metatarsal
osteotomy, or procedure that decreases the internal cubic content of the MTPJ, such as
plantar condylectomy.
Jacoby V-osteotomy-involves a transverse plane chevron osteotomy, through-and-
through from dorsal to plantar at the surgical neck, with base proximal and apex
distal. The approach entails dorsal dissection, digital stabilization, and MTPJ relocation.
This osteotomy can also be used to plantar declinate the capital fragment when indicated.
The osteotomy is stabilized with a K-wire, either from proximal to distal or through the
stabilized digit and MTPJ in an axial (medullary nail) fashion.
Dorsiflexorywedge osteotomy (DFWD}-there are several variations of dorsiflexorywedge
osteotomy (DFWOI. including distal metaphyseal (surgical neck) osteotomies such as the
transverse tilt-up and oblique wedge osteotomies; and the oblique base wedge osteotomy.
Distal osteotomies are readily fixated with an axial K-wire used to simultaneously stabilize
the corresponding digital arthrodesis and MTPJ relocation. The dorsal-distal to
plantar-proximal oblique distal DFWO at the anatomic neck usually involves resection of
only a thin wedge (thickness ofthe saw blade) of bone, and can be fixated with a K-wire or
alag screw (Figure 7-47). The same dorsal-distal to plantar-proximal oblique DFWO can be
placed atthe metatarsal base, and stabilized with K-wires or a lag screw.
Lesser metatarsal shalt osteotomy-a variety of shaft osteotomies can be used, often in
conjunction with bone grafting. The Giannestras step-down osteotomy is classically used
to shorten ametatarsal, however it can also be used to elongate. The step-down osteotomy
isthrough-and-through, and involves complete exposure of the metatarsal. The osteotomy
consists of three cuts oriented in the transverse plane. The proximal and distal transverse
arms exit opposite sides (medial or lateral) of the cortex, and are united by a longitudinal
central arm. When shortening is desired, an additional proximal and distal transverse cut
is made from the shaft segments. The osteotomy can be oriented somewhat in the sagittal
196 Reconstructive Surgery of Basic Conditions and Deformities Ch.1
Figure 1.41
plane, in an effort to facilitate lag screw fixation. Variations on the Ludloff and Mau, Gudas-
scarf Z-plasty, and offset V-osteotomy, oriented in both the transverse and sagittal planes,
have all been used for lesser metatarsal shaft reconstruction. The sliding osteotomies are
more suitable to interpositional bone grafting with lag screw fixation.
FIFTH METATARSAL SURGERY AND THE TAILOR'S BUNION
The tailor's bunion deformity is observed in the uncompensated or partially compensated
rearfoot or forefoot varus foot types, which predispose to hypermobility of the fifth ray in
response to ground reactive forces. The plantarflexed fifth metatarsal will adduct, evert
and dorsiflex in response to the ground reactive force; and may present with a plantar-
lateral bursitis, hyperkeratosis, and pain. A congenitally dorsiflexed fifth ray may also result
in tailor's bunion symptoms, usually with a dorsolateral or lateral lesion. Weight bearing
radiographic analysis of the tailor's bunion deformity will usually display rotation of the
plantarlateral tubercle to amore lateral position, consistent with pronatory eversion of the
metatarsal. There will often be an increase in both the fourth IMA above 6.5, and the
lateral deviation (bowing) angle above 2.1". There is often adumbell-shaped and enlarged
fifth metatarsal head, and arthritic changes with osteophytosis may be present When the
foot clinically appears to be very wide, the combination of first IMA >120 and afourth IMA
>8is consistent with splayfoot deformity, and the tailor's bunion is often the primary area
of patient concern. Surgical goals in the treatment of tailor's bunion focus on elimination of
prominent lateral exostosis, either dorsal or plantar; along with correction of structural
deviations such as excessive fourth IMA and/or lateral bowing. Adjunct procedures may
include correction of an adductovarus fifth hammertoe. Specific procedures for correction
of tailor's bunion deformity include:
Lateral exostsctomy-this procedure (Fig 7-481. performed performed on mild tailor's bunions
as an isolated procedure, or in conjunction with other structural corrections and avariety of
fifth metatarsal osteotomies. If an over-aggressive lateral exostectomy is performed
(staking the metatarsal head) in the presence of structural bowing or a high fourth IMA,
excessive fifth MTPJ laxity will lead to adductovarus fifth toe contracture and retrograde
MTPJ buckling with recurrence and worsening of deformity.
fifth metatarsal head excision-a radical procedure that involves head resection at the
anatomic neck and usually well tolerated in less ambulatory individuals due to the fifth ray's
independent axis of motion; it may be indicated too, in cases of fifth metatarsal head
osteomyelitis, tumor or avascular necrosis.
197 Ch. 7 Reconstructive Surgery of Basic Conditions and Deformities
Hohmann
Reverse Wilson
Figure 7.48
Figure 7.49
Figure 7.50
Mitchell
Thomasen's
Figure 7.51A
Figure 7.51 B
Hohmann osteotomy-a transverse through-and-through osteotomy atthe anatomic neck,
usually stabilized with a K-wire (Fig 7-49).
Reverse Wilson osteotomy-an oblique osteotomy from distal-lateral to proximal-
medial often floated but better to be stabilized with aK-wire (Fig 7-50).
Mitchell osteotomy-a variation of the first metatarsal osteotomy that may be limited by a
narrow fifth metatarsal neck; this osteotomy is at risk for dorsiflexion if subjected to early
weight bearing (Figure 7-51A).
Thomasen's osteotomy-a peg-in-hole variation of the Hohmann osteotomy, usually
stabilized with aK-wire (Fig 7-51 B).
198 Reconstructive Surgery of Basic Conditions and Deformities Ch. 7
==---
Figure 7.52 Figure 7.53 Figure 7.54
Reverse Austin osteotomy-a sagittal plane chevron limited by the width ofthe metatarsal
neck and stabilized with a K-wire or absorbable pin (Fig 7-52).
Closing adductoryosteotomy at neck (Mercado)-distal transverse plane medially based
wedge osteotomy with an intact lateral cortical hinge, stabilized with either a K-wire or
stainless steel wire suture, or both (Fig 7-53).
Closing adductory base wedge osteotomy (Gerbert)-a transverse plane medially based
wedge osteotomy with an intact lateral cortical hinge, fixated with aK-wire and or stainless
steel wire suture, or made oblique to facilitate lag screw fixation
Oblique wedge osteotomy-located at the apex of the bowing deformity, fixated with aK-
wire and or stainless steel wire suture, or lag screws (Fig 7-54).
HEEL SURGERY
Approximately 15% of all adult foot complaints are related to disorders of the heel. The
circulation to the heel entails the medial calcaneal branches of posterior tibial artery
medially, the communicating branches of the peroneal and lateral malleolar arteries
laterally and plantarly, and communicating branches posteriorly. The neutral or vascular
triangle, of the calcaneus is the radiolucent area observed in the lateral radiograph,
inferior to the sustentaculum tali within the body of the calcaneus, where the subtalar
pressure trabeculae combine with traction trabeculae formed in response to the pull ofthe
plantar fascia and Achilles tendon are seen under sustentaculum tali.
Plantar Fascitis and Heel Spur Syndrome-this condition results from prolonged,
excessive tension in the plantarfascia, usually secondary to hyperpronation of the STJ/MTJ,
and eventually leads to fasciosis at or near the attachment of the plantar fascia to the
calcaneus. Over time, an elongated plantar spur may also develop atthe attachment of the
fascia. Stress fracture may lead to development of a prominent plantar protrusion. Chronic
inflammation of the fascia, with or without spur formation, may also be associated with
distal tarsal (calcaneal) tunnel syndrome. The diagnosis is made based on localization of
199 Ch.7 Reconstructive Surgery of Basic Conditions and Deformities
focal, deep tenderness to the fascial attachment to the calcaneus, the presence of similar
pain upon activation of the plantar windlass (simultaneous dorsiflexion of the MTPJs and
ankle, with the knee extended); post-static dyskinesia, and radiographic evidence of a
plantar spur in about 75% of cases. A distinct plantar spur need not be present to effect
pain. Differential diagnostic considerations for plantar heel pain include lumbosacral
radiculopathy, systemic arthritis, tarsal tunnel syndrome, subcalcaneal bursitis, contusion
or local trauma, stress fracture, entrapment neuropathy of the lateral plantar nerve and its
muscular branch, diffuse idiopathic skeletal hyperostosis (DISH) syndrome, Paget's
disease, and heel neuroma. A bone scan may be helpful in resistant cases when stress
fracture is suspected. Conservative treatment combines biomechanical. pharmacological.
physical. and surgical therapies (Table 7-4).
TABLE 7-4. TREATMENT HIERARCHY FOR PLANTAR FASCIITIS AND HEEL SPUR
SYNDROME.
Intervention Stage I Stage II Stage III Stage IV
Pharmacological NSAID NSAID
Local steroid
Oral steroid
Biomechanical Low Dye strap Custom orthotic Immobilization
Prefabricated Roller sole
orthotic
Physical Ice Iontophoresis Night splint
Flexibility Dynamic splint
Surgical ESWT Cold ablation
microdebridement.
fasciotomy,
spur resection;
bursectomy
Extracorporeal Shockwave Therapy (ESWT)-shockwaves consist of high amplitude, fast
rising, asymmetrical. low frequency (>500 bar in 33 nanoseconds) sound energy that
imparts intense pressure to the target tissues, namely the plantar fascia. Shockwaves can
be generated by means of piezoelectric crystals or ceramics, electromagnetic energy, and
electrohydraulic vaporization of water. Shockwaves have been used in the treatment of
tendinosis calcarea (shoulder). lateral epicondylitis (tennis elbow). cedial epicondylitis (golf
elbow), chronic calcifications (thigh, apophysis), patellartendinitis, ossoue nonunions and
pseudarthrosis, nephrolithiasis, and microscopic studies into the potential use in the
treatment of cancer and CNS lesions are alos underway. In order to treat plantar fasciitis,
shockwaves must deliver 0.26-0.32 mJ/mm2 of energy to the target fascia. This causes
physical alteration of small axons, inhibiting impulse conduction, chemical alteration of pain
receptor neurotransmitter, and hyperstimulation analgesia (gate control); as well as
neovascularization. Resultant tissue absorption and deformation create a wound healing
response that, in 3-6 weeks, may relieve chronic pain related to plantar fasciitis. Weight
bearing is immediate following ESWT. Potential complications of ESWT include
subcutaneous hematoma, skin erosion, swelling, petecchial hemorrhage, pain and
200 Reconstructive Surgery of Basic Conditions and Deformities Ch.1
paresthesia, and vasovagal syncope. Contraindications to ESWT include pregnancy,
children, nerve damage, tarsal tunnel syndrome, tarsal tunnel syndrome, osteoporosis,
rheumatoid arthritis, peripheral vascular disease, infection or tumor, bleeding diasthesis,
cardiac pacemaker, and healing fracture.
Radiofrequency coldablation (Coblation"') microdebridement-the plantar fascia can be
debrided in an open fashion by means of a small incision over the proximal portion of the
fascia, and application of 15-20 high voltage radiofrequency impulses in asaline medium that
creates a plasma layer between the concentric electrodes at the tip of the probe, and
disrupt the molecular bonds in the target tissue, thereby effecting localized fascia
debridement with minimal collateral tissue destruction. Non-weight bearing, or partial
weight bearing is employed following cold ablation debridement of the plantar fascia,
varying with the nature of the plantar skin incision, surgeon's preference, and the amount
of debridement undertaken.
Plantar Fasciotomy and Calcaneal Spur Resection-exposure of the attachment of the
plantar fascia to the calcaneus, and the plantar spur, can be achieved through a plantar
transverse, longitudinal, or oblique incision. Of historical interest is the distally-based
U-shaped pedicle flap Griffith incision, which can be used to expose the entire plantar
aspect of the calcaneus. The medial DuVries approach can also be used, however this
incision makes the medial calcanean nerves vulnerable to post-incisional entrapment. The
deep plantar fascia is identified and sectioned from the calcaneal tuberosity, and the
plantar spur resected. A small segment of the most proximal fibers of the plantar fascia is
retained for pathological inspection. It is importantto re-establish anormal cortical contour
when the spur involves prominent plantar protrusion, even if fascitis has been essentially
resolved with conservative measures. Care must be taken to avoid injury to the lateral
plantar nerve and its branches, and over-aggressive resection of bone as this could weaken
the calcaneus and predispose it to fracture. Other complications include recurrence,
hematoma, scar pain, and chronic plantar enthesitis. A compressive dressing is applied,
and early ankle range of motion and 3 weeks non-weight bearing ensue. Non-weight
bearing is necessary in order to allow the plantar skin wound to heal. A wide range of
techniques have been used over the years for the treatment of recalcitrant plantar heel
pain, some of which are of historical interest only while others show useful application.
Variations on the general theme of fasciotomy and spur resection include minimal incision
or semi-closed approaches wherein the fascia is released and the spur remodeled under
fluoroscopic guidance, or via topographical guidance and identification of palpable
landmarks. Instep plantar fasciotomy, localized to the midportion ofthe medial band ofthe
plantar fascia, and not addressing the calcaneus, can also be useful in some cases.
Historically, spur reduction has been addressed with a countersinking osteotomy, or a
rotational osteotomy combined with tendoAchiliis lengthening.
Endoscopic Plantar Fasciotomy (EPFJ---fmdoscopic plantar fasciotomy has been shown
to be a useful option for releasing the fascia, and is based on the theorythatthe spur need
not be remodeled in order to alleviate plantar heel pain. The procedure is performed under
local or general anesthesia, and uses a blunt obturator to channel from medial to lateral
across the heel after initially making an incision through which the obturator is passed. The
deep fascia is visualized by passing aslotted cannula with obturatorfrom medial to lateral
and rotating the slot toward the fascia. An L-shaped blade is then inserted from lateral to
Ch.7 Reconstructive Surgery of Basic Conditions and Deformities 201
medial while viewing through the endoscope, which is inserted from medial to lateral. The
blade is turned dorsally at the medial margin of the fascia, and then pulled laterally.
Fasciotomy is directly viewed, and several passes of the blade are usually necessary to
adequately section the fascia. Care is taken when inserting and removing the L-shaped
blade through the lateral incision. The wound is lavaged and skin closure performed,
followed by application of a compressive dressing. It is also possible to reduce bony
prominence endoscopically with the rota-osteotome and shaver, however this is generally
not done.
External Neurolysis-if the cause of plantar heel pain is thought to be entrapment
neuropathy ofthe lateral plantar nerve and/or its muscular branch (inferior calcaneal nerve
and calcaneal tunnel syndrome), then external neurolysis of the nerve trunks may be in
order. External neurolysis, however, is usually performed in conjunction with fasciotomy
and spur reduction. External neurolysis is best performed with the use of fine-tipped
instrumentation and loupe magnification.
CalcanealOecompression--decompression of calcaneal intramedullary pressure, via
multiple small drill or K-wire holes aligned obliquely from posterior-proximal to anterior-
distal (dorsal cortex to plantar cortex) through the cortex of the calcaneal body, has also
been espoused as a treatment for plantar calcaneal pain. Currently, this procedure is
primarily of historical interest only, although there is some basis to its use. In essence, the
decompression holes result in cortical fracture when subjected to the pull of the Achilles
tendon and plantar fascia, thereby reducing tension in these soft tissues after resumption
of weight bearing. Calcaneal joint depression fracture is an obvious risk of the
decompression technique.
Haglund's Oefonnity-this deformity consists of prominence ofthe posterosuperior aspect
(bursal projection) of the calcaneus. It can be structural or positional, or a combination of
both. A variety of radiographic observations (Figure 7-55) are used to assess the posterior
aspect of the calcaneus. The Fowler and Philip angle (FPA) normally ranges from 44
0
-69",
and an FPA >75
0
will often present with posterior swelling, cutaneous compromise and
prominence just superior to Achilles insertion. Prominence of the posterior aspect of the
calcaneus predisposes to the development of retrocalcaneal bursitis, as the constant
pre-Achilles bursa becomes repetitively irritated with ankle dorsiflexion (Figure 7-56). Ruch
has pointed out that the total angle is a more reliable assessment of the likelihood of the
T ~ k ,
1) Angle of Fowler & Philip
2) Calcaneal inclination angle
3) Total angle
A
Figure 7.55 Figure 7.56
202 Reconstructive Surgery of Basic Conditions and Deformities Ch.7
posterior aspect ofthe heel to irritate the retrocalcaneal bursa, as this measurementtakes
into accountthe calcaneal inclination angle (CIA) and posterior structural prominence (FPA).
A total angle> 90" correlates highly with retrocalcaneal bursitis and Haglund's deformity.
Parallel pitch lines (PPL) have also been used to assess the prominence of the
posterosuperior prominence of the body of the calcaneus. An adventitious superficial
calcaneal bursa may develop superficial to the Achilles tendon secondary to repetitive
mechanical irritation. Kager's triangle is demarcated by the long flexor tendons anteriorly,
the Achilles tendon posteriorly, and the superior surface ofthe calcaneus inferiorly, and is
visualized in the lateral radiograph as adark, radiolucent triangle with apex pointed dorsally.
Kager's triangle represents the pre-Achilles fat pad. Thickening of the Achilles, which is
usually about 9 mm wide in the lateral radiograph, due to retrocalcaneal bursitis and/or
tendinitis will encroach on Kager's triangle and blur the usually sharp interface with the
pre-Achilles fat pad. The calcaneal apophysis usually closes at 14-16 years of age.
Biomechanical foot types associated with increased motion between the posterior aspect
of the heel and the shoe counter, thereby aggravated by Haglund's deformity, include
compensated rearfootvarus, compensated forefoot valgus, and rigid plantarflexed first ray.
Symptomatic Haglund's deformity is most commonly observed in young to middle-
aged females; with pain and cutaneous irritation at the posterior aspect of the heel,
radiographic evidence of acortically intact bursal projection, loss of the pre-Achilles recess
indicative of retrocalcaneal bursitis, Achilles tendon widening> 9 mm indicative of
tendinitis, and loss of distinction of the posterior margin of Kager's triangle. A tender
superficial Achilles bursitis may be present, and causes the classic "pump bump"
aggravated by shoes with a tight counter and elevated heel height. Treatment of the
symptomatic Haglund's deformity, due either to a prominent bursal projection, a normal
posterior contour with a high CIA, or acombination of both, involves initial use of a heel lift
inside the shoe and aheel counter pad to shield the tender posterior aspect of the heel. The
use of NSAIDs, calf and arch flexibility exercises, orthotic control of hyperpronation, and
local infiltration of corticosteroid combined with gel-cast or similar immobilization can be
useful for persistent cases. Recalcitrant cases may warrant surgical intervention for
excision of chronic superficial and/or retrocalcaneal bursitis, and remodeling of the
prominent bursal projection. The treatment of Haglund's deformity and posterior calcaneal
spur are summarized in Table7-5.
203 Ch.7 Reconstructive Surgery of Basic Conditions and Deformities
TABLE 75. TREATMENT HIERARCHY FOR HAGLUND'S DEFORMITY OR POSTERIOR
CALCANEAL EXOSTOSIS.
Intervention Stage I Stage II Stage III StagelY
Pharmacological
NSAID
Local steroid*
Oral steroid
NSAID
Biomechanical
Heel lift
Heel counter pad
Prefa bricated
orthotic
Custom orthotic
Roller sole
Immobilization
Continued
immobilization
Physical Ice
Rexibility
Iontophoresis Night splint
Dynamic splint
Surgical Remodel
posterosuperior
process or spur
resection; preserve
Achilles or detach;
bursectomy
* Support ofthe ankle and partial immobilization (gel cast and surgical shoe, cast boot (cam walker), BK cast) with
weight bearing are advised whenever corticosteroid is infiltrated about the Achilles tendon.
Surgical repair of Haglund's deformity of the heel involves alateral paratendinous incision
with the patient prone or in the contralateral decubitus position. The procedure is readily
performed under local anesthesia with IV sedation, and anatomic dissection yields
adequate hemostasis. The sural nerve must be protected within its subcutaneous bed. The
deep fascia is incised in aparatendinous fashion, in line with the overlying skin incision. Care
should be taken to avoid excessive reflection of the fibrous expansion of the Achilles
tendon at its insertion. Plantarflexion of the ankle enhances retraction of the Achilles. The
prominent posterosuperolateral process is resected with an osteotome and mallet, and the
remaining calcaneal surface is then rasped. "Chasing the bump" prevents creation of a
new prominence due to over aggressive resection. It is possible to remodel the entire
posterior aspect from the lateral approach, however a second medial paratendinous
incision can be used if necessary, however a distance of at least 2.5 cm should be
maintained between the two parallel incisions. Acurvilinear or lazy-S incision could also be
used. Generally, with Haglund's deformity the single lateral incision will suffice. In the
symptomatic, structural cavus foot with a pathologically high CIA, in the presence of a
normal posterior contour and bursal projection, the Kelly and Keck osteotomy may be used
to resect a dorsally based wedge from the calcaneal body. This procedure brings the
posterosuperior aspect of calcaneus anteriorly. The osteotomy is fixated with Steinmann
pins, staples or lag screws.
Retrocalcaneal Exostosis with Calcification in the Achilles-the retrocalcaneal
exostosis differs from the Haglund's deformity in that it is usually seen in older individuals,
is situated distal to the posterosuperior process, and it generally traverses the entire
posterior aspect from lateral to medial. The patient should be positioned prone or in the
contralateral decubitus position, and the procedure can be performed under local
204 Reconstructive Surgery of Basic Conditions and Deformities Ch.7
anesthesia if desired. Incisional approaches are variable, including two paratendinous
incisions, acentral longitudinal posterior or an oblique curvilinear (Dickinson) incision, and
it is often necessary to create a central longitudinal tendon-splitting incision in order to
remove intratendinous calcification (Figure 7-57). The tendon splitting incision enables
the surgeon to expose the posterior surface of the calcaneus while preserving distal
attachments medially and laterally. After remodeling the posterior surface of the calcaneus
and debriding the Achilles, the tendon is reattached with multiple intraosseous tendon
anchors and nonabsorbable sutures. Following layered closure, acompressive dressing and
short leg cast are applied. The patient is maintained non-weight bearing for 2-4 weeks, and
immobilization is discontinued at 5-6 weeks followed by gradual rehabilitation. The duration
of non-weight bearing and immobilization is determined by individual factors and the extent
oftendon reflection. Downey has advocated the use of an inverted V-tenotomy for debride-
ment of the Achilles tendon and removal of aposterior calcaneal spur, noting thatthis method
enables the surgeon to readily access the calcaneus and easily reapproximate the tendon.
Figure 7.57
Calcaneus
Figure 7.58
ANKLE EQUINUS
52%
Anterior
Medial Lateral
Posterior
35%
Medial ") Lateral
3 ~ ~
Medial ~ Lateral
The triceps surae consist ofthe medial and lateral heads of gastrocnemius, plantaris, and
soleus. The medial head of gastrocnemius is thicker and broader than the lateral head, and
it extends further distally and attaches to the lateral aspect of the tendoAchillis. Soleus
attaches to the medial 2/3 ofthe deep surface of the tendoAchiliis (Fig 7-58). Plantaris arises
from the lateral femoral condyle, and is absent 7% of the time. Plantaris attaches medially
along the Achilles. The tendoAchiliis averages 15 cm in length and originates near the
middle ofthe leg. Gastrocnemius traverses three joints: knee, ankle, and STJ; while soleus
traverses two joints: ankle, and STJ. The gastrosoleus complex functions in late contact
through midstance and into early propulsion, and causes knee flexion and heel lift via
ankle plantarflexion.
205 Ch.7 Reconstructive Surgery of Basic Conditions and Deformities
Muscular Forms of Ankle Equinus-the muscular forms are caused by skeletal muscle
spasm, congenital shortness, and acquired conditions. Spastic equinus is the oldest
recognized form of ankle equinus, and is caused by upper motor neuron disease such as
cerebral palsy, CVA, and head and spinal trauma. Spastic equinus presents with
hypertonicity, hyperreflexia, and steppage gait. Congenital equinus usually presents with toe
walking until about 15-18 months of age (usually the first 3-6 months after initial walking), and
thereafter the equinus subsides. Acquired ankle equinus may develop in response to
prolonged casting in plantarflexion, such as following Achilles tendon repair, or due to
chronic use of high-heeled shoes. Chronic equinus contracture results in tightness of the
deep flexors and peroneal tendons, posterior ankle and subtalar ligaments and capsule.
The Silverskiold test indicates gastrocnemius equinus if ankle dorsiflexion is <10
0
with
the knee extended, but ~ 1 with the knee flexed; or gastrosoleal equinus if <10
0
of
dorsiflexion with the knee extended or flexed. Gastrocnemius equinus can be addressed
with gastrocnemius recession, while gastrosoleus equinus warrants tendoAchiliis length-
ening (TAL). The end range of motion should be smooth and "soft tissue," as compared to
an abrupt, bony end range consistent with osseous equinus. The standard lateral ankle and
charger (stress dorsiflexion) radiographs should be checked for talotibial exostosis, which
could cause bony blockage to dorsiflexion. Distal tibiofibular synostosis following trauma
can inhibitthe wider anterior portion ofthe dome ofthe talus from gliding through the ankle
mortise, thereby blocking ankle dorsiflexion without the presence of talotibial exostosis.
Hamstring tightness can also cause ankle equinus, and the knee should be checked for
flexion contracture while plantarflexing the ankle (eliminates pull of gastrocnemius on the
knee) and passively extending the knee to end range. Pseudoequinus may be present when
the cavus foot (anterior equinus) uses available dorsiflexion atthe ankle, simply to stand with
the forefoot loaded, thereby limiting available dorsiflexion range of motion and functionally
inducing equinus deformity.
Combined forms of equinus may involve gastrocnemius or gastrosoleus equinus, with
bony blockade and/or pseudoequinus. Distal pedal compensation for ankle equinus occurs
as hyperpronation of the STJ and MTJ with associated forefoot supinatus, flexor
stabilization induce hammertoes and HAV, and serves as one of the most forceful and
common deforming influences acting on the foot. Failure to compensate with pedal
hyperpronation results in genu recurvatum or overt toe walking/standing. Uncompensated
equinus also presents as pes cavus, with equinovarus, fixed STJ supination, extensor
substitution, and dropfoot. In the neuropathic (insensitive, Charcot) patient, equinus
deformity leads to tremendous Lisfranc fracture and luxation. Neurological consultation is
in order whenever UMN or spastic equinus is noted. Nonsurgical efforts to manage
significant equinus deformity are generally not very successful. Efforts include stretching
and flexibility for nonspastic forms, and possible acceptance ofthe deformity and use of a
heel lift, orthosis, and roller sole.
206 Reconstructive Surgery of Basic Conditions and Deformities Ch.7
Figure 7.59 Figure 7.60
Gastrocnemius Equinus-gastrocnemius equinus has been treated with selective
dennervation of the gastrocnemius muscle bellies, as well as proximal recession via
transection of the medial and lateral heads near their femoral origins. Vulpius and Stoffel
described a distal transverse recession of the gastrocnemius aponeurosis, and they later
converted the technique to an inverted V-shaped lengthening of the aponeurosis without
suturing to underlying soleus muscle. Strayer described atransverse aponeurotic incision
with suturing of proximal portion to underlying soleus. Baker described a distally based
tongue-in-groove recession of the aponeurosis (Fig 7-59), and sectioned the central soleus
aponeurosis deep to the gastrocnemius aponeurosis. Fulp and McGlamry modified the
tongue-in-groove distal recession by basing the tongue proximally (Fig 7-60), however
Downey and Banks later noted this to associate with atrophy of the medial head of
gastrocnemius due to the natural rotation of the gastrocnemius fibers. Gastrocnemius
recession is used most effectively in cases of nonspastic gastrocnemius ankle equinus.
Distal gastrocnemius recession (Baker) is carried out on the prone or lateral decubitus
patient using an approximately 6-7 cm longitudinal incision, originating at the palpable
myotendinous junction, and positioned just medial to the midline on the posterior aspect of
the calf. The incision is deepened through the dermis into the subcutaneous fat, where the
sural nerve and lesser saphenous vein are preserved in their soft tissue bed laterally. The
deep fascia and paratenon are incised in line with the overlying skin incision, and reflected
as a single layer. Plantaris is transected on the medial aspect of the wound (originates
laterally and traverses from lateral to medial as it propagates distally), and a segment is
excised to assure release. The ankle is then slightly plantarflexed to enhance access to the
most distal fibers of the aponeurosis, and the tongue-in-groove aponeurotomy is initiated
by transecting the medial and lateral thirds of the aponeurosis distally. The ankle is then
slightly dorsiflexed to make the remaining intact fibers taut, and the central third of the
aponeurosis is transected proximally. The aponeurosis is then lengthened (recession) by
dorsiflexing the ankle with the knee extended until 100 of motion is achieved with the
subtalar joint neutral. The central soleal aponeurosis is then sectioned. The wound is the
lavaged and the central tongue portion of the aponeurosis is sutured to the medial and
Ch.7 Reconstructive Surgery of Basic Conditions and Deformities 207
lateral thirds in the corrected length, using 2-0 nonabsorbable, buried knot sutures
reinforced with 2-0 absorbable sutures to reapproximate the medial and lateral thirds
centrally. Paratenon and deep fascia are closed with 3-0 absorbable running lock suture,
and smooth gliding function deep to the fascia/paratenon layer is assessed by moving the
ankle through its range of motion. The subcutaneous layer and skin are then closed. A BK
cast or immobilizing splint is then applied with the knee extended and STJ neutral, and
maintained for 3-4 weeks before rehabilitation is initiated.
Gastrosoleal Equinus-gastrosoleal equinus has been treated with a variety of
tendo-Achillis lengthening (TAL) procedures. The frontal plane Z-lengthening (Fig 7-61) is a
commonly used technique for TAL, and provides excellent control of length and avoidance
of suture irritation of the overlying deep fascia and skin posteriorly. The procedure is
performed on the prone or lateral decubitus patient via a 6-8 cm longitudinal incision
medial to the posterior midline, terminating atthe insertion of the Achilles. Deep fascia and
paratenon a.re then incised longitudinally, and the entire Achilles tendon isolated for a
distance of 5-7 cm from its insertion. A #11 (bayonet) blade is then used to hemisect the
tendon in the frontal plane, creating anterior and distal hemisections. The hemisection is
converted to a Z-tenotomy by sectioning the posterior hemisection proximally, and the
anterior hemisection distally. The plantaris tendon is sectioned at the medial aspect of the
Achilles (or alternatively it can be Z-Iengthened itself). Attention is directed to residual
contracture, and posterior ankle and/or STJ capsulotomy or deep flexor or peroneal tendon
lengthening is performed as necessary. The ankle is placed in corrected position, with the
STJ neutral, and the tendon sections reapproximated with a combination of 1-0 and 2-0
nonabsorbable and absorbable sutures taking care to bury the knots. Paratenon and deep
fascia are then reapproximated with 3-0 running lock absorbable suture, followed by
closure of the subcutaneous layer and skin. A BK cast is then applied with the knee
extended and the STJ in neutral position.
Figure 7.61
Osseous Ankle Equinus--an anterior talotibial exostosis can be addressed via an open or
arthroscopic technique, and involves removal of impeding osteophytosis and spurring until
adequate range of motion is achieved. If tibiofibular synostosis inhibits ankle dorsiflexion,
then mortise reconstruction may be in order.
Murphy Anterior Advancement of the Achilles Tendon-this procedure has been described
in Chapter 6, and is indicated in the treatment of spastic triceps sume equinus.
208 Reconstructive Surgery of Basic Conditions and Deformities Ch.7
Selected Peripheral Nerve Entrapments and Acquired Neuropathy
Kopel and Thompson have defined peripheral nerve entrapment as an area of nerve trunk
impingement due to the surrounding "stress anatomy" at apoint where the nerve traverses
afibro-osseous tunnel or constricting soft tissue hiatus. In the lower extremity, anumber of
entrapment sites are commonly symptomatic, and any peripheral nerve can become
entrapped. Most notable among the common entrapments inferior to the knee are tarsal
tunnel syndrome (medial), Morton's intermetatarsal neuroma, and superficial peroneal nerve
entrapment atthe deep fascial hiatus proximal to the ankle.
Tarsal Tunnel Syndrome (TTS)-tarsal tunnel syndrome is classically described as
entrapment or compression neuropathy of the posterior tibial nerve and/or its terminal
branches, the medial and lateral plantar and medial calcanean nerves. The surgical
anatomy of interest includes the flexor retinaculum (laciniate ligament) extending from the
medial malleolus to the medial process of the calcaneal tuberosity and the plantar
aponeurosis. The porta pedis at the distal aspect of the medial tarsal tunnel is the canal
created by the abductor hallucis muscle belly and its deep fibrous septal attachment to the
periosteum of the medial wall of the calcaneus, through which the medial and lateral
plantar nerves pass and enter the plantar vault. The division of posterior tibial nerve into its
three terminal branches most commonly occurs proximal to the laciniate ligament, however
it may divide deep to the laciniate ligament, or even at the distal margin of the tunnel. The
distal bifurcation into medial and lateral plantar nerves is often identified in cases of TIS,
as the subabductorfibrous septum encroaches on the crotch ofthe division, and is termed
distal tarsal tunnel, or calcaneal tunnel, syndrome. This is often associated with
longstanding, recalcitrant plantar fascitis and medial heel pain. The medial calcanean nerve
usually emerges through the laciniate ligament, and is primarily a sensory branch. The
medial plantar nerve provides sensory innervation to the plantar aspect of the hallux,
second and third toes, medial half of the fourth toe, and medial half of plantar aspect of the
foot. The lateral plantar nerve provides sensory innervation to the plantar-lateral half ofthe
fourth toe, plantar aspect of the fifth toe, and the plantar-lateral aspect of the foot. The
plantar nerves provide motor innervation to the intrinsic muscles, and autonomic
innervation to sweat glands and vascular smooth muscle.
The etiology of medial TIS is generally thought to be due to overuse or repetitive
microtrauma, consistent with impingement of the nerve by the surrounding "stress
anatomy." Operative inspection may reveal no particular gross abnormality of the
structures, unless a distal bifurcation, or tumor within the tunnel is identified. In the
typical case, longstanding hyperpronation of the STJ and MTJ has effected chronic
constriction of the contents of the tunnel. The existence of dilated and tortuous
posterior tibial veins within the tunnel may lead to engorgement and concomitant chronic
stasis, which can result in peripheral nerve compression and severe nocturnal discomfort
which is often associated with calf cramping. Traumatic causes of medial TIS include ankle,
talar or calcaneal fracture; recurrent ankle and/or subtalar sprain and subluxation; both of
which may lead to chronic, recurrent hemorrhage and fibrosis. Systemic diseases such as
rheumatoid arthritis, hypothyroid myxedema, and even diabetes mellitus predispose to TIS.
Space occupying lesions such as lipoma, neurofibroma. neurilemmoma, ganglion. and
synovial cyst (often associated with rheumatoid arthritis), have also been implicated as
causes of entrapment within the tunnel. Even hypertrophy ofthe abductor hallucis muscle
belly has been implicated as acause of TIS. The clinical symptoms associated with medial
TIS include forefoot pain with symptoms localizing to the metatarsal ball and digits plantarly,
209 Ch.7 Reconstructive Surgery of Basic Conditions and Deformities
as well as medial and plantar heel pain and paresthesia. Early symptoms include intermittent
burning pain, numbness, and paresthesia overthe medial side ofthe heel, the toes and the
plantar aspect of the foot. As the condition worsens, late symptoms include paresis that
will develop into paralysis of the pedal intrinsic muscles (intrinsic minus foot). Proximal
radiation of pain (Valleix sign) may propagate upthe posterior calf. Pain and paresthesia are
generally proportional to the amount of weight-bearing activity sustained during the day. The
diagnosis of TIS is not always sharply defined. Important aspects ofthe diagnosis include
history of progressive symptomatology, unless there is a traumatic event relevant to the
tunnel; the presence of unilaterallinel's IHoffman-linel's) sign upon gentle percussion or
moderate-deep palpation of the tunnel's contents and, similarly, the presence of a
unilateral Valleix sign; application of a venous tourniquet proximal to the ankle will elicit
pain and paresthesia on the affected side secondary to venous occlusion with a
temporary passive congestion in the presence of intra-tunnel varix; forced eversion of the
STJ may elicit symptoms on the affected side in cases related to prolonged hyperpronation;
radiographs may provide evidence of previous injury; and appropriate lab testing may be
useful in establishing the presence of RA, myxedema, or OM. It is important to rule-out
lumbosacral radiculopathy or plexopathy, employing the straight leg raise, Achilles and
patellar deep tendon reflexes, and extrinsic muscle strength testing. EMG and NCV testing
may be helpful, however need not necessarily be positive for nerve entrapment atthis level
even in the presence of overwhelmingly suggestive clinical findings. For this reason,
treatment decisions are not made solely on the results of electrodiagnostic testing.
Conservative treatment of medial TIS entails local anesthetic block of the posterior
tibial nerve and local infiltration of corticosteroid into the third canal of the tarsal
tunnel, followed by rest and gentle flexibility exercises of the ankle and foot Support hose
may be indicated in case involving dependency-related venous congestion. Functional
orthotics may be useful for those patients displaying weight-bearing hyperpronation.
Surgical management of medial TIS can be enhanced by avoiding use of atourniquet, as
this allows visualization of the posterior tibial artery and the tortuous veins that may require
ligation. Atourniquet may be used ifthis is the surgeon's preference. Extensile esposure is
gained via a curvilinear incision extending posterior and plantar to the medial malleolus.
The incision should be placed at least 1em posterior to the malleolus. The laciniate ligament
is identified, and vessels and nerves in the superficial fascia and subcutaneous fat are
observed and protected. The medial calcanean branch, which may pierce the flexor
retinaculum atthis level and may display multiple branches, should be identified. The flexor
retinaculum is then incised and opened in line with the overlying skin incision and the
contents identified and documented; afterwhich external neurolysis of the posterior tibial
nerve and its branches is performed. Nerve retraction is maintained with a latex drain or
vessel loop. The nerve trunks are identified from proximal to distal through the tunnel,
including inspection of the porta pedis. Dilation of the porta pedis is enhanced with loupe
magnification and microsurgical instrumentation. Abductor hallucis is examined for
hypertrophy and hypertrophic tissue may be excised. The posterior tibial veins may reveal
varicosities that require ligation and excision. The wound is then flushed, and the laciniate
ligament is realigned but generally not sutured directly. The superficial fascia is then
reapproximated with absorbable suture of choice, followed by skin closure and
application of a gently compressive, sterile dressing. The foot and ankle are allowed to
move freely, however weight bearing is avoided for 2-3 weeks, depending upon wound and
patient progress. A gradual resumption of activity is thereafter undertaken. Complications
of TIS treatment include recurrence of symptoms secondary to fibrosis, and consideration
210 Reconstructive Surgery of Basic Conditions and Deformities Ch.7
should be given to burying the nerve in the calcaneus or tibia in cases of severe disability
due to recurrent nerve entrapment. This is obviously a serious undertaking, as plantar
insensitivity and loss of intrinsic muscle function ensues. Severing the posterior tibial artery,
which provides 80% of the arterial supply to the foot, is a potential complication that would
require microsurgical repair. Other potential complications include nerve laceration,
tenosynovitis, hematoma, and possible infection, as well as dehiscence.
Deep transverse,
intermetatarsal
ligament
Figure 7.62
A B
c
Morton's Neuroma-this condition is a common cause of metatarsalgia, and must be
considered in cases involving pain in the ball ofthe foot. It is most frequently encountered
in the fourth to 6th decades of life and, although any intermetatarsal space can be affected,
it is usually localized to the third intermetatarsal sapce. The patient relates sharp, shooting
pain with associated aching, broughton byweight-bearing load of the forefoot, insidious in
onset, progressively worsening, and intermittent in nature, and seemingly relieved by sitting
and massaging the unshod foot for a brief time. Hyperpronating individuals, the obese, and
those that wear high-heeled or tight-fitting shoes are prone to entrapment irritation of the
common plantar nerve and/or its branches in the intermetatarsal space, just plantar to the
transverse intermetatarsalligament (Figure 7-62). The mechanism of nerve entrapment in
the intermetatarsal space involves repetitive irritation of the nerve by the neighboring
ligament. Identification entails focal tenderness and paresthesia to direct deep palpation,
apositive Mulder's strum-click sign, and localization of anesthesia to the contiguous sides
of the adjacent toes. Differential diagnoses include MTPJ enthesitis, intermetatarsal
bursitis, diabetic peripheral neuropathy, neoplasm, trauma, TIS, and radiculopathy.
Nonsurgical treatment measures involve the use of a metatarsal projection pad
(proximal to the metatarsal heads), orthoses, local infiltration of corticosteroid, ultrasound
with MTPJ range of motion exercises, use of asneaker with roller sole, NSAIDs, ice after
strenuous activity, and rest. Surgical intervention evolves around adequate external
neurolysis ofthe involved plantar nerve and, traditionally, excision ofthe common plantar
nerve proximal to the proximal margin of the DTIL Approaches include: 1) the plantar
211 Ch.7 Reconstructive Surgery of Basic Conditions and Deformities
longitudinal interspace incision, which yields optimal exposure ofthe plantar nerve without
disruption ofthe DTIL; 2) the transverse plantar incision, which yields exposure to adjacent
interspaces; 3) the web-splitting incision, 4) the dorsal longitudinal, which is satisfactory
for an interspace into which no previous dissection has been undertaken; and 5) the
plantar zig-zag or lazy-S incision, which affords exposure of the plantar metatarsus and
vault whenever revisional neurectomy is necessary. Sectioning the DTIL readily exposes the
plantar nerve and its branches, and makes it easy to excise the neuroma, which is typicaly
present at the distal margin of the DTI L After identification of the common plantar digital
nerve trunk and its proper digital branches to the contiguous surfaces ofthe adjacenttoes,
the nerve is inspected for coloration and texture and, usually, resected proximal to the
proximal margin of the DTIL. Some surgeons do not excise the nerve, and limit the
procedure to sectioning the DTIL or, less commonly, translocating the nerve from plantar to
dorsal to the DTIL The latter intervention entails sectioning the ligament, transposing the
nerve, and then repairing the ligament It is also possible to section the DTIL by means of
endoscopic identification and sectioning using specialized instrumentation, however such
intervention neither excises the neuroma nor translocates the nerve trunk. If the nerve is
section and the neuroma excised, the proper branches are procured as far distal as
- possible in each toe, and the common nerve trunk is sectioned as far proximal to the
proximal margin of the DTIL as possible. This can be difficult when the dorsal incisional
approach is used, however this method of surgical treatment is commonly used. After the
common trunk is sectioned, the proximal nerve stump is allowed to retractfurther proximally
in the intermetatarsal space, where it can reside amidst intact intrinsic skeletal muscle
bellies. In an effort to further diminish the potential risk of developing asymptomatic stump
neuroma, closure of the common trunk's epineurium with 8-0 nylon suture can be
undertaken, prior to allowing the stump to retract proximally. All plantar incisions require
approximately 3 weeks of non-weight bearing thereafter. Complications of plantar
neurectomy include hematoma in dead space, and this is most often associated with the
dorsal longitudinal incisional approach. Hematoma predisposes to infection, and may
require suture removal and drainage. Vascular ischemia may also develop after neurectomy,
and is particularly likely following adjacent interspace dissection. If postoperative ischemia
is noted, avoid ice and elevation, nicotine and caffeine, excessive weight bearing, loosen
bandage, and administer bupivacaine posterior tibial nerve block, and consider using reflex
abdominal or popliteal heat (K-padl, as well as isoxsuprine IV 5 mg- 10 mg with careful
assessment of vital signs. Venous congestion may cause cyanosis, and elevation in this
case would be helpful. Recurrent intermetatarsal neuroma, also known as amputation or
stump neuroma, occurs in all cases of nerve resection. A symptomatic stump neuroma,
however, occurs in only about 10-15% of cases following excision of an intermetatarsal
neuroma. Efforts to minimize the risk of symptomatic stump neuroma formation include
sectioning the nerve proximal to the proximal margin ofthe DTIL, epineurial closure over a
clot of thrombin or cyanoacrylate (not FDA approved) using 8-0 nylon simple interrupted
sutures. One may also bury the nerve stump in an adjacent metatarsal shaft. Silicone
capping and entubulation have not proven to be reliably effective in preventing
symptomatic stump neuroma formation. The ideal location for a sectioned nerve stump is
within well-vascularized, protected, intact skeletal muscle bellies, as is the condition within
the intrinsics of the foot wherein the plantar nerve retracts proximal to the DTIL. Permanent
numbness of the contiguous surfaces ofthe involved digits and plantar interspace, as well
as loss of sudomotor and vascular smooth muscle tone, are anticipated.
-----
212 Reconstructive SurgeryofBasic Conditionsand Deformities Ch.7
TerminalSymeoperation
lortotalnailremoval
Halluxamputation
Fourthandfifth
rayresection
.
Uslranc'samputation Chopart'samputation
Syme'samputation
Figure7.63
213 Ch.7 Reconstructive Surgery of Basic Conditions and Deformities
Superficial Peroneal Nerve Entrapment (Henry's Mononeuritis)-this is most frequently
seen in active individuals, often involved in jumping sports or physically strenuous
occupations. or in older individuals who were once regular participants in such activities.
The pathology is localized to the deep fascial hiatus proximal to the ankle where the
superficial peroneal nerve emerges to enter the subcutaneous fayer. It is usually
aggravated by peroneal muscle herniation through the hiatus, thereby impinging the nerve
and causing localized pain and paresthesia over the ankle and pedal distribution of the
nerves. Treatment involves local corticosteroid and nerve block, attention to any potential
causes of compartment syndrome, and recalcitrant symptoms may require surgical repair
of the skeletal muscle herniation and transposition of the intact nerve trunk. The branches
of the superficial peroneal nerve, namely the intermediate dorsal cutaneous nerve (lDCN,
Lemont's nerve) and the medial dorsal cutaneous nerve (MDCN), can also become
entrapped and, being located on the anterior aspect of the ankle and the dorsum of the foot,
these are particularly vulnerable to direct contusion as well as traction injury associated
with ankle inversion. Morever, they are vulnerable to iatrogenic involvement in association
with surgical dissection of these areas.
Amputations
The essential element in determining amputation level is tissue viability. Clinical
assessment, duplex Doppler ultrasound, and transcutaneous oxygen tension (Tc-p02) are
primary methods used to assess tissue viability, perfusion, and predisposition to healing. The
skin is warmed to 44 C, and aClark electrode is used to measure Te-p02. Amputations are
likely to heal if the Tc-p02 is at least 40 mmHg, are questionable if the Tc-p02 is between
26-40 mm Hg, and likely to fail if the Te-p02 is < 26 mmHg. Surgical principles specific to
amputations include gentle handling of the skin, adequately wide flap pedicle, and
avoidance of skin tension or bony prominence. Bone resection and remodeling can be
performed with both power and hand instrumentation. Moreover, muscle insertions should
be maintained or recreated to avoid contracture deformity and severe muscular imbalance.
Preservation of muscle balance usually requires intraoperative decision making on the part
of the surgeon. Preservation of TA and PB tendons prevents equinovarus deformity.
Isolated digital amputation predisposes to adjacent digital transverse plane drift, and HAV
is likely following second toe removal. Hallux amputation predisposes to apropulsive
(pedestal) gait. During amputation, stump (amputation) neuroma formation should be
prevented by sharp sectioning under tension, with subsequent retraction proximally into
well-vascularized and protective skeletal muscle bellies. Epineurial closure may be helpful
on large nerve trunks. Planning should include use of a robust, sensate flap to cover the
stump. Hemostasis is critical. and vessels with lumens large enough to grossly visualize
should be ligated as compared to electrocoagulated. In general, transtibial amputations
are regarded as major amputations, and those distal to the tibia are considered minor
amputations. Pedal amputations include the following techniques: terminal Syme's
amputation, digital amputation and disarticulation, ray resection, transmetatarsal
amputation (TMA), Lisfranc amputation, Chopart amputation, Pirogoff amputation,
and Symes (ankle) amputation (Figure 7-63). The Symes amputation entails ankle
disarticulation with removal ofthe malleoli and proximal rotation ofthe heel pad to cover the
distal surface of the tibia. The Pirogoff amputation entails sectioning the talus and
calcaneus in line with the anterior margin of the tibia, thereby preserving the posterior portion
of the calcaneus, heel weight bearing surface, and the insertion of the Achilles tendon.
214 Reconstructive Foot and Ankle Surgery Ch.8
RECONSTRUCTIVEFOOTANDANKLESURGERY:
COMPLEXCONDITIONSANDMAJORDEFORMITIES
Complex conditions requiring majorfoot and ankle reconstruction often require combination
surgery. Repair may require major hindfoot or midfoot, or ankle, arthrodesis and adjunct soft
tissue manipulations such as tendon lengthening andlortransfer. These procedures can be
used to correct acquired, degenerative, or post-traumatic conditions, as well as neurologically
induced and congenital defects. Selected deformities amenable to major pedal recon-
structive intervention include advanced pes valgus, pes cavus, degenerative arthrosis, and the
rheumatoid toot Congenital deformities will be discussed elsewhere. Deformities may be rigid,
or flexible and unstable. Selected procedures include triple arthrodesis, ankle and pantalar
arthrodesis, and Usfranc arthrodesis. At times, it may be applicable to perform isolated
intertarsal arthrodesis, or variations on midtarsal and intercuneiform fusion, as well as partial
tarsometatarsal fusion, based upon the needs of the individual case.
Collapsing Pes Valgoplanus (CPVP, Flexible Flatfoot}-it is important to note that not all
flatfeet are pathological. Isolated sagittal plane arch depression, in the presence of a
perpendicular or minimally everted resting calcaneal stance position, is usually
asymptomatic and well tolerated throughoutthe individual's life with the exception of post-
traumatic degeneration or neuropathy. On the other hand, the presence of hindfoot
eversion, or pes valgus, is a strong destructive force during weight bearing and is
associated with steadily progressive articular subluxation and degenerative joint disease,
TP dysfunction, abnormal shoe wear, and difficulty walking or standing. A variety of
etiologies exist for CPVp, including: tibialis posterior muscle weakness, accessory
navicular (Kidner foot), and chronic TP dysfunction; ligament weakness and laxity;
prolonged FF supinatus secondary to hyperpronation of the STJ and MTJ IFF and RFvarus,
flexible FF valgus, ankle equinus, and other pronating biomechanical foot types);
congenital or acquired calcaneovalgus; lower extremity torsional abnormalities such as
femoral anteversion; and Charcot collapse in its early stages.
Radiographic Findings Associllted with CPVP-standard radiographs include: AP view
Kite's angle (Kite's talocalcaneal angle) 30-50reducing to 17-21by age 5years, with 75%
articulation of TNJ; lateral view CIA 1821, talar declination angle 21, and lateral
talocalcaneal angle of 35 - 50. Planal dominance of deformity in flatfoot: transverse plane
dominance with increased Kite's angle, increased cuboid abduction, decreased FF
adduction; frontal plane dominance with superimposition of metatarsals, decreased first
met declination, decreased height of sustentaculum tali, midtarsal and STJ; sagittal plane
dominance with increased talar declination, navicular-cuneiform breach, and increased
T-e angle on lateral view.
Cliniclll Signs of CPVll-these include evidence of the Hubscher maneuver (toe test of
Jack), indicative of flexibility. The Hubscher maneuver should cause the flexible flatfoot to
reform amedial longitudinal arch when the hallux is dorsiflexed and the patient externally
rotates the ipsilateral hip and leg, causing the heel to go into varus. Alateral radiograph can
be taken with the heel elevated to see if the medial column reduces, if not, there is aneed
for medial column work in addition to other reconstructive procedures. In the young child,
simply have them attempt raise up on the ball of the foot and observe the heel go into varus,
which indicates aflexible deformity that will often respond well to supportive therapy while
the skeleton matures.
Ch.8 Reconstructive Foot and Ankle Surgery 215
Surgical Repair of CPVP-indications for flatfoot surgery include: midfoot and tarsal
instability with associated FF hypermobility (HA'I, flexor stabilizing HTs, MTPJ subluxation),
metatarsalgia, and plantar fasciitis; postural symptoms extending from the foot to the low
back; midfoot and arch pain, especially along TP and TNJ, as well as sinus tarsi; tight heel
cord with calf pain and inability to stand for long periods of time; difficulty walking/running,
or performing other weight bearing activities; decreased activity level of youngster due to
symptomatic feet; failed non-surgical treatment such as foot orthoses and calfflexibility and
TP exercises. Contraindications to flexible flatfoot reconstructive efforts include rigid
flatfoot (convex pes valgus, tarsal coalition, paralytic); osseous equinus and extreme obesity.
Congenital gastrocnemius or gastrosoleus equinus often accompanies CPVp, and may be
contributory in the development of the deformity, and must be addressed with either
gastrocnemius recession or TAL, respectively, when the flatfoot is reconstructed. Similarly,
metatarsus adductus must be considered whenever medial arch enhancement, with or
without lateral column lengthening, is undertaken. Repair of epvp effects FF adductus as
the medial arch elevates and TP becomes more effective. Therefore, it may become
necessary to address metatarsus adductus deformity in addition to repair of the CPVP
Reconstruction of epvp typically addresses the triad of deformities including the medial arch,
lateral column, ankle equinus, and usually combines osseous and soft tissue manipulations.
As a rule, isolated soft tissue manipulations in the medial arch are inadequate without
associated osseous stabilization or lateral column lengthening. Surgical options include:
Extra-Articular STJ Bone Block Procedures Useful in Young Patients-a variety of
extra-articular blocking procedures are available for patients wherein arthrodesis is
not desireable.
Chambers procedure-indicated for children <8 years of age, wherein bone graft is
placed in the calcaneal sulcus of the sinus tarsi to inhibit adduction and plantar-
flexion of the talus on the calcaneus (Figure 8.1).
Baker and Hill procedure-calcaneal osteotomy and elevating bone graft under
posterior facet, to decrease vertical alignment of STJ and minimize adduction and
plantarflexion of talus.
Selakovichprocedure-opening osteotomy and graft of sustentaculum tali, inhibiting
talar declination and adduction.
Subtalar Arthroereisis-ST J arthroereisis is also useful in young patients 4-8 years of age,
with epvp displaying atransverse plane (TP) Te angle >30and 50% TN articular congruity,
heel eversion of 8-10", and FF varus of >10with superimposition of the metatarsals on the
Figure 8.1
216 Reconstructive Foot and Ankle Surgery Ch.8
lateral radiograph. This procedure can also be used in adults with CPVp, and is often used
in conjunction with other reconstructive procedures addressing the medial columnn and
triceps surae. Arthroereisis uses synthetic polymer or metallic implant, rather than bone
graft, to block STJ pronation by impinging on the anterior margin of the leading edge of
posterior talar facet. The implanted blocking plug is usually removed after the child has
achieved skeletal maturity and avoided the destructive, adaptive changes related to patho-
logical STJjMT J hyperpronation during the formative years. Specific techniques include:
polymer {Silastic) plug positioned from lateral to medial in the sinus
tarsi, thereby elevating the floor of the sinus (calcaneal sulcus) and blocking talar
adduction-plantarflexion. The polymeric plug has been criticized for instability,
displacement, and implant degradation.
StaPeg"'-polyethylene plug positioned in the sinus tarsi, and noted to be more
stable and durable in comparison to the LeLevre procedure.
Villadot-an hour glass-shaped Silastic implant, also considered by manyto be more
stable than the LeLevre design.
Valente-polyethylene plug with screw thread surface that actually screws into the
sinus tarsi using appropriately sized guides, designed to allow just 4-50 of STJ
pronation thereafter.
Maxwell-BrancheauMBA'" Titanium Subtalarlmplant-one of several highly refined
arthroereisis implants, the MBA'" probably has the longest record of clinical
successful. It is abarrel-shaped, slotted implant made oftitanium alloy that is readily
implanted by means of limited dissection and accurate sizing. The instrumentation
and surgical technique are well-developed. The implant is also easily assessed on
standard radiographs. Weight bearing in an immobilizing cast-bootfor approximately
2-3 weeks is commonly undertaken in the early postoperative phase. The implant can
be removed at a later date, or it can be retained permanently, depending upon the
requirements ofthe clinical course.
Medial Column Procedures-these focus on restoring joint stability, TP function, and arch
height (eliminate TN or NC fault), and include:
Kidnel'-exciseos tibiale externum and transpose TP to plantar aspect of the
navicular.
Young-used to correct TN and/or NC fault in a flexible flatfoot with FF supinatus.
wherein the TA is rerouted through akeyhole slot in the navicular. McGlamry and Ruch
(Figure 8-2) have enhanced this procedure by specifically including advancement ofthe
spring ligament, TP, and combining lateral column lengthening using the Evans open
calcaneal graft
Lowman-TN arthrodesis combined with rerouting TA under the navicular and
suturing ilto the spring ligament.
217 Ch.8 Reconstructive Foot and Ankle Surgery
Figure 8.2
Miller-navicular-medial cuneiform combined with cuneiform-first metatarsal
arthrodesis, further combined with soft tissue reefing. This procedure results in much
shortening and it is difficult to achieve satisfactory bone-to-bone apposition without
interposition of corticocancellous bone graft.
Hoke-navicular to first and second cuneiform arthrodesis.
Cotton-dorsally-based opening wedge osteotomy of medial cuneiform, packed with
truncated corticocancellous bone graft; used to plantarftex the medial column.
Lateral Column Lengthening-lateral column lengthening enhances the stability and
longevity of medial arch reconstruction, and has proven to be highly reliable, readily
achieved, and associated with low morbidity and complication. The Evan's calcaneal
osteotomy and bone graft, or bone lengthening using corticotomy and callus
distraction with an external fixator, are the mainstays of lateral column lengthening.
Bone graft extension calcaneocuboid arthrodesis can also be employed. The highly
trabecular anterior portion of the body of the calcaneus readily heals, accepts
allogeneic corticocancellous bone graft and bone transport manipulation, and is
ideally positioned to influence forefoot adduction (correct forefoot abduction by
reducing the calcaneocuboid abductus angle). Once again, attention must be paid to
pre-existing metatarsus adductus skewfoot deformity, and the metatarsus adductus
may require concomitant correction.
Evans Calcaneal Osteotomy and Bone Grah-this is the primary osteotomy used to
reduce forefoot abduction in the transverse plane (Figure 8-3). The procedure involves
an opening osteotomy approximately 1.5 cm proximal to the calcaneocuboid joint
(CCJ)' preserving the ligaments and capsule of this joint, and directed from lateral to
medial through-and-through the anterior portion of the body of the calcaneus. The
osteotomy is distal to the posterior facet of the STJ, and it is extra-articular. A
trapezoidal block of allogeneic corticocancellous bone graft is then wedged into the
osteotomy, advancing the distal aspect of the calcaneus and CCJ, and adducting the
forefoot. Autogenous bone graft could also be used, however the site is amenable to
alogeneic graft, and a secondary donor site wound is not necessary. Alternatively,
corticotomy and gradual distal transport ofthe anterior portion of the calcaneus can
be achieved, after an initial '10-14 days of stabilization, using an adjustable external
fixator employing the principles of callus distraction osteotaxis.
218 Reconstructive Foot and Ankle Surgery Ch.8
Figure 8.3
VarusProducing Calcaneal Osteotomies-varus-producing calcaneal osteotomies are
performed in the posterior aspect of the calcaneus, in patients >3 years of age. Fixation of
calcaneal osteotomies, both with and without bone graft, can be achieved with staples,
interfragmental compression screws, or absorbable pins (preferably without bone graft);
and postoperative non-weight bearing and immobilization are crucial. Lateral approaches
to the calcaneus require that attention be paid to the course of the sural nerve, lesser
saphenous vein, and the peroneal tendons. Specific procedures include:
Gleich-an oblique calcaneal osteotomy anterior to the posterior cortex that allows
medial shift of the posterior segment and relative adduction of the tuberosity and
posterior os calcis.
Owyer-a lateral opening wedge oriented
obliquely from the dorsal-to-plantar margins of
the calcaneus, midway between the posterior
margin of the posterior STJ facet and the
Achilles attachment, incorporating allogeneic
or autogenous corticocancellous bone graft
insertion. It has also been described as a
medial closing calcaneal osteotomy, however
the contents of the tarsal tunnel can complicate Figure 8.4
the dissection, and the procedure is not
commonly done in this fashion. The lateral
closing Dwyer osteotomy is amainstay of pes cavus reconstruction (Figure 8-4).
SilvBl'-an opening wedge bone graft performed via alateral approach, wherein the
posterior aspect of the calcaneus and tuberosity are shifted plantarly, and medially.
Koutsogiannis-a versatile, frontal plane osteotomy through the body ofthe calcaneus
midway between the posterior lip of the STJ and the Achilles insertion, allowing
triplanar correction of the posterior calcaneus and tuberosity via primarily medial and
plantar displacement.
219 Ch.8 ReconstructiveFootand Ankle Surgery
PesCavus-theetiologyofpescavusincludes:
1. Musculardiseasessuchasmusculardystrophy,
2. Peripheralorspinalnervelesions,suchasDejerineSottas,CharcotMarieTooth
(familialsensorimotorneuropathy,peronealmuscularatrophy),and polyneuritis
and/ortraumatoperipheralnerves,
3. Spinal cord defectssuch as poliomyelitis(ofteneffectsparalyticflatfoot,also),
spina bifidawithmyelomeningocele,diastematomyelia,andspinaltumors,
4. Spino-cerebellardefects,which are usuallyhereditary, including Roussy-Levy
syndrome,andFriedreich'sataxia,
5. Pyramidal and extrapyramidal tract lesions effecting spastic and athetoid
cerebralpalsy,
6. Supratentorialconditionssuchashysteria,
7. Congenitaldefectssuchastalipesequinovarus,and
8. Idiopathicpescavus.
Etiopathogenesishingesonmuscleimbalances,oftenwithspastictricepssuraeand
deep posteriormusculature,and anteriorand peroneal compartmentweakness causing
dropfoot.Thefirstrayisusuallyplantarflexedas peroneuslongusisunopposed.Extensor
substituionresultschronicMTPJsubluxation,clawtoes,metatarsalgia,andinabilitytoget
the heeltothe ground. Itis postulatedthatthe extrinsic digital extensors overpowerthe
lumbricales.TPoverpowersandsupinatesthefootandpiantarflexesthe ankle.
Classification of Pes Cavus-the classification of pes cavus can be confusing and
cumbersome,and severalsystemsexist,including:
Apex of the Cavus Oeformity-a commonclassificationinvolvesidentificationofthe
apexofthecavusdeformity.AnteriorpescavuscanbedescribedbytheSagittalPlane
(SPI shape ofthefootas itrelatestothe dorsal apexofthedeformity,asfollows:
metatarsal, tarsometatarsal, lesser tarsal, and forefoot or midtarsal cavus.
Subcategoriesofanteriorcavusincludeisolatedmedialorlateralcolumncavus,first
and fifth ray respectively. orglobal cavuswherein all ofthe metatarsalrays bear
weightmoreorlessequallyduetotransverseplanesymmetryoftheplantarlydeclined
structuresdistaltothe apex. Combinations ofanteriorcavus can also exist Lower
extremitycompensationforanterior cavus includesdigital and MTPJ contraction,
effectinghammerand clawtoesand associatedsubluxationoftheMTPJs;dropfoot
thatoften catchesorscuffsacrossthe substrate,andmetatarsalgiawithorwithout
plantarkeratomaformation.lfthedeformityisflexible,thenloadingtheforefootresults
in acertain degreeofmetatarsalandtarsaldorsiflexionthat,overtime,can become
degenerative.Moreover,acertaindegreeofanklejointdorsiflexionwillalso be used
to compensate forresidual anteriorcavus,thereby limiting available dorsiflexion
required forlate stance propulsion.Thisrelative limitation ofankle dorsiflexion is
referredtoaspseudoequinus,andfunctionstofurtherloadpedalstructuresandlead
to symptomatology. Pseudoequinus is more pronounced in rigid forms ofanterior
cavus.Posteriorpescavusresultsfromstructuralincreaseinthecalcanealinclination
angle,usuallywithadductionandvarusofthehindfootCombinedpescavustypically
entailsfixedfrontalplanevarusandanon-reduciblerearfoot.
220 Reconstructive Foot and Ankle Surgery Ch.8
Three-Stage Classification of Pes Caws-perhaps the most useful classification involves
3stages of pes cavus, and focuses on options for surgical repair after failed non-surgical
efforts. The system includes:
Stage I Pes Cavus-entails clawtoes and subluxated or dislocated MTPJs. Repair
evolves around digital stabilization with PIPJ arthrodesis and MTPJ relocation with pin
fixation. Adjunct procedures involve the Hibbs and Jones tendosuspensions, and
perhaps tendon transfer (STATT) to enhance ankle dorsiflexion.
Stage II Pes C8ws-entails those deformities of Stage I cavus, as well as heel varus
and more significant cavoadductovarus localized primarily to the distal to the midfoot
Reconstructive options are determined by the degree of flexibility, as determined by
the Coleman block test for heel varus and plantarflexed first ray. Failure to establish a
perpendicular relationship of the posterior bisector of the heel to the ground when
the lateral column is elevated on a block, to eliminate the varus influence of a rigid
plantarflexed first rayon the hindfoot, indicates the presence of fixed heel varus that
will require corrective osteotomy. Corrective procedures include the Dwyer closing
lateral wedge osteotomy of the calcaneus, dorsiflexory wedge osteotomy (DFWO) of
the first ray, Jones and/or Hibbs suspension, and tendon transfertothe dorsum ofthe
foot to enhance straight ankle dorsiflexion.
Stage III Pes Cavus-entails marked, rigid, cavoadductovarus deformation, often of
neurological etiology, associated with adaptive arthrosis and serious dropfoot, and
typically requires Cole midfoot osteotomy or triple arthrodesis for correction. The Cole
procedure involves athrough-and-through, dorsally based wedge resection of bone
positioned through the tarsal navicular and cuneiforms, and the cuboid, thereby
elevating the forefoot out of an equinus alignment. The osteotomy, after reduction, is
stabilized with Steinmann pins or staples, and maintained non-weight bearing for up
to three months. The triple arthrodesis is a versatile procedure for correction of the
most severe cavus deformities.
Assessmentofthe Patient with Pes Caws-assessment ofthe patient with pes cavus
requires athorough family history that includes inquiry about parents, siblings, and
other blood relatives. Neurological examination, typically with neurology consultation
prior to surgery, should identify the presence or absence of spasticity, flaccidity,
muscular dystrophy, spinal and other eNS defects; as well as familial diseases that
may require genetic and social counseling. Nerve conduction velocity and EMG may
be in order. Pedal and ankle, as well as spinal radiographs if spina bifida or other
defect is suspected, should be obtained. Radiographically, the apex of the cavus
deformity should be identified and the deformity classified in this regard. The
radiographic evaluation of pes cavus should be performed weight bearing, and
include AP. lateral and lateral oblique projections, with consideration given to ankle
films. The lateral radiograph will show increases CIA >30", normal to posterior break
in the SP cyma line, accentuated or bullet-hole sinus tarsi, SP long axis of the neck of
the talus passes superior to the long axis of the first metatarsal, and dorsally based
wedge shaped cuneiforms. An axial view ofthe calcaneus at 45should be obtained
to rule out astructural heel varus.
221 Ch.8 Reconstructive Foot and Ankle Surgery
Surgical Procedures for Correction of Pes Cavus-procedures for the correction of pes
cavus vary depending upon the degree of flexibility.
Flexible Pes Cavus--procedures useful for correction of flexible pes cavus include the
Steindler stripping, wherein the plantar fascia and intrinsic musculature is reflected from
the plantar calcaneal cortex, and may be useful only ifthe deformity is flexible and not of
bony rigidity. A Hibbs suspension may also be combined with the Steindler stripping in a
flexible deformity. Tendon transfers such as the STATT and Pln. or TPn. are often used to
balance inverter/everter imbalance in flexible deformity. Digital fusion and MTPJ relocation
are crucial to the treatment of both flexible and rigid pes cavus.
Rigid Pes Cavus--for rigid deformity, where the Coleman block test failed to eliminate heel
varus orthe medial column is rigidly plantarflexed, a first metatarsal base DFWO combined
with a Dwyer lateral closing osteotomy of the calcaneus, perhaps with the STAn. is a
useful combination (Stage II pes cavus). It may also be useful to transfer TA dorsally into
the base of first metatarsal and perform a plantar opening wedge osteotomy with bone
graft of the medial cuneiform, along with a Jones suspension of the first ray. If fixed bony
equinus is localized to the lesser tarsus and midfoot. the Cole osteotomy is indicated
(Figure 8-5). The Cole osteotomy is performed as adorsally based wedge resection of bone
and joint throughthe navicular-cuneiform and cuboid level. A first metatarsal DFWO may
also be necessary, and adductovarus deformity can be addressed by manipulating the
forefoot on the hindfoot at the level of the osteotomy. The Cole should only be performed
on askeletally mature foot. as shortening will ensue. The Japas osteotomy can be used for
less severe, rigid pes cavus, and involves atransverse plane V-osteotomy with the apex in
the navicular and the wings diverging distally through the cuneiforms and cuboid on the
medial and lateral aspects, respectively (Figure 8-6). The Japas causes less shortening
than does the Cole, however it is difficult to address adducto varus deformity. In
youngsters with open growth physes, in the presence of pan metatarsal global equinus, first
metatarsal-cuneiform dorsal opening wedge osteotomy with bone graft, along with pan-lesser
metatarsal DFWO may be used. In the adult. pan metatarsal DFWOs may be considered. The
triple arthrodesis remains the most versatile and powerful reconstructive procedure for
repair of severe pes cavus, which is often of neurological etiology (Figure 8-7).
Charcot Foot Reconstruction-Charcot deformity and treatment are described in Chapter 3.
Rheumatoid Foot Reconstruction and Panmetatarsal Head Resection-when treating the
patient with rheumatoid arthritis, it is necessary to consider the patient's physiologic age,
general medical status, immunocompromise status, bone stock, wound healing capacity,
systemic corticosteroid supplementation, and current as well as anticipated weight-
bearing activity level. The combination of deformities caused by rheumatoid arthritis
mutilans is generally referred to as the rheumatoid foot. The rheumatoid foot will usually be
symptomatic in either the forefoot or hindfootlankle. The majority of symptomatic
presentations involve the forefoot. which displays claw or hammertoes, subluxated to
dislocated MTPJs, plantar metatarsalgia with or without IPK and/or rheumatoid nodules.
Excessive mechanical overload can effect ulceration and underlying bone infection.
Hindfoot and ankle involvement usually entails TP synovitis and chronic dysfunction,
rheumatoid nodules of the plantar and posterior heel, retrocalcaneal enthesitis, and
severe pes and ankle valgus deformity. The patient often adapts apedestal gait with antalgic
fSaJnB!:I
g'S aJnB!.:J
8
223 Ch.8 Reconstructive Foot and Ankle Surgery
guarding. Fundamental non-surgical treatments include periodic, palliative skin and nail
care, accommodative foot orthoses, extra-depth shoes with an external roller sole, and
other supportive measures that hinge upon adequate systemic disease modulation under
a rheumatologist's guidance.
Rheumatoid Foot Reconstructive Surgical Techniques-techniques useful for repair ofthe
rheumatoid foot include: synovectomy, excision of rheumatoid nodules, digital stabilization,
Keller arthroplasty, pan metatarsal head excision, first MTPJ fusion along with lesser
metatarsal head excision, MTPJ and/or IPJ endoprosthesis, and arthrodesis of the greater
and/or lesser tarsus and ankle. Systemic corticosteroid supplementation and prophylactic
antibiotics are in order. Postoperative non-weight bearing can be difficult, and
immobilization can be detrimental to subsequent joint movement. Occupational and
physical therapy should also be considered. (Note: digital arthrodesis, Keller arthroplasty,
endoprosthesis implantation, and first MTPJ fusion have been described elsewhere in this
manual). In regard to the use of first MTPJ endoprosthesis in rheumatoid patients,
multicomponent total joint replacement is common, although the use of silicone polymer
total hinged implants can also be useful. In these patients, however, endoprosthesis
probably offers little more in comparison to Keller arthroplasty. Importantly, implantation
requires the presence of adequate bone stock, and perhaps metatarsal osteotomy to
correct angular deformity. Other useful procedures include:
Panmetatarsal Head Resection-this is performed to eliminate pain and cutaneous
compromise, and maintain apedestal gait Hoffman described excision of all five metatarsal
heads, while Clayton recommended excison of aportion if not all ofthe proximal phalangeal
bases if they were large or osteophytic. Proximal phalangeal base resection is wrought
with subsequent digital instability and may require syndactylization to effect stability.
Incisional options include transverse plantar, or five or three dorsal longitudinal incisions.
The more severely dislocated MTPJs and clawtoes invite atransverse plantar incision with
an elliptical excision of redundant plantar skin and postoperative non-weight bearing. The
subcutaneous fat layer should remain attached to the skin, and intermetatarsal dissection
should be avoided. The five incision approach includes a wound over each metatarsal,
while three dorsal incisions are localized to the first ray, between the second and third and
between the fourth and fifth toes respectively. Separate dorsal incisions are used to
perform PIPJ arthrodesis of the second through fourth and arthroplasty of the fifth. The
preferred length pattern after metatarsal head resection is: 2=1 > 3 >4 >5. The metatarsals
are transected distally from dorsal to plantar and the plantar cortex rasped smooth. The
first metatarsal is also angulated from distal lateral to proximal medial, while the third-fifth
metatarsals are angulated from distal medial to proximal lateral. Most commonly, fusion of
the PIPJs 2 through 4 and arthroplasty of the fifth toe are performed along with the
metatarsal head excision, and for added stability a K-wire is directed through the PIPJ
fusion and into the metatarsals. The combination of first MTPJ fusion with lesser
panmetatarsal head excisions can be very useful. Postoperatively, a protective cast boot
works well. Some shortening of the foot can be expected, but the patient should maintain
an apropulsive gait.
Usfranc Arthrodesis-arthrodesis of all or part ofthe tarsometatarsal joint (TMJ, Usfranc's
joint) is useful in the treatment of post-traumatic or degenerative arthritis, Charcot foot
associated with ankle equinus, and other maladies localized to this level (Figure 8-8).
224 Reconstructive Foot and Ankle Surgery Ch.8
Isolated first metatarsal-medial cuneiform arthrodesis (Lapidus procedurel. as previously
noted. can be used to stabilize the medial column and may be used to correct severe HAV
deformity with associated metatarsal-cuneiform instability, hypermobility of the first ray and
long-standing forefoot supinatus. Arthrodesis of Usfranc's joint complex usually involves 3
dorsal incisions, the first medially over the medial column, the second and third between the
second and third, and fourth and fifth metatarsals, respectively. Fixation is achieved with a
plate and interfragmental compression screw placement across the first metatarsal-medial
cuneiform fusion site, Steinmann pins or crossed K-wires or single interfragmental screws
across the lesser metatarsal-cuneiform and cuboid fusion, or perhaps a plate and screws
across the fifth metatarsal-cuboid site. Specialized locking plates may also be used atthis
site. Furthermore, achieving primary rigid internal compression fixation of the medial
column, in conjunction with splintage of the lesser TMJs, is an example of the vassal rule
of internal fixation and serves as acommon approach to Usfranc arthrodesis.
Triple Arthrodesis-this is a versatile procedure that is applicable in cases that include
collapsing pes valgo planus, tarsal coalition, convex pes valgus, tarsal arthritis, pes cavus,
residual clubfoot, neuromuscular disease, and others. Triple arthrodesis enables the
surgeon to orientthe foot in relation to the leg and ankle, and to manipulate the relationship
of the forefoot to the hindfoot. It also affords a stable hindfoot upon which the tendons of
the extrinsic pedal musculature can function. The classic Oilier incision can be used for
the triple arthrodesis, and courses from the tip of the fibular malleolus, across the sinus
tarsi then on to the dorsal aspect of the talonavicular joint. The Oilier incision is applicable
in the cavus foot, however predisposes to difficulty exposing the TNJ in the valgus foot. In
the valgus foot, a 2-incision approach is preferred, and most surgeons use the 2-incision
approach even for pes valgus correction. The lateral incision extends from the tip ofthe
lateral malleolus to the dorsum of the junction between the fourth and fifth metatarsal bases,
and provides excellent exposure of the ST.I and CCJ. The medial incision extends from the
anterior margin of the medial malleolus longitudinally to the first metatarsal-medial
cuneiform joint, and provides excellent exposure of the TNJ and neck of the talus. The
lateral dissection proceeds through the superficial fascia to the deep fascia, which is incised
longitudinally between EDB and the PB tendon Care is taken to preserve the peroneal
sheath. EDB is reflected away from the CCJ, and the intertarsal talocalcaneal ligament and
sinus tarsi are evacuated. The lateral aspect of the head and neck of the talus are exposed,
and the peroneal tendons are retracted plantarly to expose the posterior facet of the STJ.
Medially the dissection should avoid the medial marginal vein, and the deep fascial incision
is made medial to the tendon afTA. Amedial periosteal and capsular incision exposes both
the TNJ and the anterior margin afthe ankle. The technique of osseous resection is crucial
A
B
Figure 8.8
225 Ch.8 Reconstructive Foot and Ankle Surgery
when performing the triple arthrodesis (Figure 8-9). Preoperative assessment of the
relationship between the foot and leg enables the surgeon to take into consideration knee
and ankle positions so that proper placement of the hindfoot can be achieved. The hindfoot
should be positioned in slight valgus, and varus should be avoided at all costs. A varus
hindfootfusion is destined to marked weight bearing difficulties, pain, and ankle instability
postoperatively. The foot should be positioned in about 12-15of pes abductus, when the
knee is on the frontal plane. Less pes abductus is needed ifthe knee is externally rotated,
and more may be useful in the presence of medial knee position or tibial torsion.
Resection proceeds from the MTJs to the STJs, as MTJ resection enables easier
access to the STJ. The foot is held in areduced attitude and the CCJ and TNJ are resected
with the blade parallel to the articulations in most cases. Severe adductus or abductus may
warrant transverse plane wedging, however a flush resection preserves bone mass and
correction can usually be satisfactorily achieved via translocation of the forefoot on the
hindfoot without the ne!)d for specific wedge resection. Similarly, anear-parallel resection
ofthe STJs (posterior,medial and anterior facets) is usually adequate, as only slightvalgus
positioning will suffice. STJwedging may be more pronounced ifthe frontal plane deformity
is severe. The calcaneus is translocated medial/yfor correction of pes valgus, and laterally
for correction of pes cavus. Sagittal plane correction is also corrected primarily via
translocation of the forefoot on the hindfoot, after achieving the desired talocalcaneal
alignment The calcaneus can also be shifted posteriorly to increase the lever arm for the
tendoAchiliis and to increase sagittal plane talar declination and thereby increase arch
height. Contrarily, sliding the calcaneus anteriorly relative to the talus dorsiflexes the talus
and decreases arch height Achilles function. The desired alignment is temporarily stabilized
with cannulated screw guide pins, and intraoperative radiographs in the Ap, lateral, and
calcaneal axial projections are obtained and reviewed. The order of stabilization generally
proceeds from STJ to TNJ to CCJ, and is usually achieved with three 6.5-7.0 mm
interfragmental compression screws (Figure 8-10). The TC fusion is achieved with a lag
screw directed from the neck of the talus dorsally, into the body of the calcaneus. In a
similar fashion, the TNJ and CCJ are stabilized with distal to proximal lag screws.
Care is taken to avoid the following fixation hazards: violation of the medial cortex of
the body of the calcaneus and entrance of the fixation device into the tarsal tunnel when
fixating the TC interface, entrance of the TN fixation into the ankle, and fracture of the
dorsolateral cortex ofthe cuboid with the screw head. Additional intraoperative radiographs
should be used to reassess final fixation if any questions exist The Te lag screw can also
be directed from the apex of the calcaneus postero-plantarly into the body and neck ofthe
talus. The MTJs can also be satisfactorily stabilized, each with two staples oriented 90to
each other. Closure proceeds in layers following placement of drains medially and laterally,
and the foot is secured in a BK Jones compression immobilizing dressing. Aftercare
involves drain removal after 24 to 72 hours, redressing between 3to 5 days, and BK cast
immobilization without weight bearing for up to 3to 4months. Mobilization ofthe ankle and
MTPJs can be undertaken in a non-weight-bearing attitude as soon as desired, and
immobilized partial weight bearing can be initiated by 10 to 12 weeks pending clinical
and radiographic findings. Full weight bearing ensues thereafter, as does conversion to
desired shoes.
Ankle and Pantalar Fusion---the most common indication for ankle fusion is post-traumatic
arthrosis following ankle fracture, wherein a small proximal and lateral shift of the lateral
malleolus has produced mortise incongruity resulting in articular cartilage degeneration. It
226 Reconstructive Foot and Ankle Surgery Ch.8
Figure 8.9
Figure 8.10
has been shown that a 1 mm shift can result in greater than a40% decrease in tibiotalar
congruity. The most common predisposing causes of the need for pantalar fusion is severe
cavo adducto varus deformity with chronic ankle instability, and avascular necrosis ofthe
talus for whatever reason. Other indications for ankle and pantalar fusion include
destructive bone tumors, infection, and failed ankle endoprosthesis. Evaluation of the
patient requires inspection of the knee, leg, ankle, STJ and MTJ, and the relationship of the
forefoot to the hindfoot and leg. The ideal position of fusion is 90" of the foot relative to the
leg, with slight ankle and/or hindfoot valgus, and approximately 10-12of pes abductus. If
tibial varum is present, increase the amount of valgus to adjust for the added varus
deformity. The surgical approaches to ankle fusion include Charnley's transverse anterior
incision, extending from one malleolus to the other, which is rarely used currently because
of risk of injury to anterior neurovascular and tendinous structures. The lateral
transmalleolar hockey stick incision is most commonly used, and begins over the junction
ofthe middle and distal thirds ofthe fibula, then curves distally toward the sinus tarsi forthe
ankle fusion, and onward toward the junction of the bases ofthe fourth and fifth metatarsals
for pantalarfusion. This approach yields anterior, lateral, and posterior exposure for fibular
osteotomy. An accessory medial incision over the anterior margin ofthe medial malleolus
is usually combined with the transfibular incision to provide anteromedial exposure for
resection of the cartilage of the medial malleolus and enables hardware placementthrough
the tibial pilon. When performing ankle fusion, we are looking to position the large
cancellous mass of the tibial metaphysis in rigid apposition to the trabecular bone of the
body of the talus.
227 Ch.8 Reconstructive Footand AnkleSurgery
TechniquestoAchieveAnkleFusion
1. Curettageofcartilagewithinterpositionalbonegraft;
2. Slidinginlaygraftfromtheanteriorsurfaceofthetibialmetaphysisintothetalar
neck/body;
3. ModifiedGalliefusionwhereinallogeneic graftis inserted anterolaterallyand
stabilizedwithastaple;
4. Transmalleolar(eitherfibularortibiaUwithosteotomytoenhancevisualizationof
thetibiotalarinterface;
5. The subtotalfusion fordebilitated patientsthatcannotsustain extensive bone
resectionandtrephineplugjointresectionwithdowelgraftfusionwillsuffice;
6. Compression arthrodesisusing anyofavarietyofexternalfixation devicesor
interfragmentallagscrews;and
7. The Blairtibiocalcanealfusionwhichcanbeusefulpost-poliooraftercollapse
ofthetalus.
Aswithallfusion procedures,Glissane'scriteriamustbe metforsuccessfularthrodesis:
1. Removal of cartilage, fibrous tissue, or other material hindering raw bone
contact;
2. Accurateandclosefittingofsurfaces;
3. Optimalposition offusion;and
4. Maintenanceofappositioninundisturbedfashionuntilfusioniscomplete.
ThePodiatryInstitutetechniqueofankleandpantarlarfusionsentailtheuse of:
1. Alateralhockeystickincision;
~ Preservationofthefibula(avoidosteotomy);
3. Cartilageresectionwithpreservationofasmuchofthetalarbodyaspossible;
4. Ancillary medial approach for removal of medial malleolar and talar body
cartilage;
5. Temporarystabilizationwithcannulatedscrewguidepins;
6. Fusionalignmentof90"ofthefoottotheleg;
7. 10-12pesabductusandslightankle/hindfootvalgus;
8. IntraoperativeradiographsintheAP. lateral,and calcanealaxialviews;
9. Interfragmental compression fixation with crossing 6.5-7.0 mm cancellous
screws;
10. Placementofthefibularonlaygraftwithinterfragmental compression screws
purchasingthetibiaandtalus(andcalcaneusin pantalarfusion);
11. Be sure to allow agap between the proximal and distal segments of the
osteotomizedfibula inordertoavoid pseudoarthrosisornonunion;
12. Repeatintraoperativeradiographstoascertainfixationand bone alignment
13. Place and activateclosedsuctiondrains,bandage andimmobilize;
14. Plantoleavehardwareinindefinitelyoratleast6to12months;and
15. Besurenotto penetratetheSTJwithfixatorsifonlyanklefusionisperformed.
228 Reconstructive Foot and Ankle Surgery Ch.8
Complications of ankle and pantalar fusion include infection (reported as high as 20% in the
literature); nonunion, malunion, and pseudoarthrosis; malposition due to operative
misadventure (most often varus or calcaneus); stress transfer to MTJ and STJ (may need
triple later if only ankle fusion originally performed); and limb shortening if bone graft is
not used.
Total Ankle Replacement (TAR) Arthroplasty-chronic ankle pain that is not responsive to
other treatments, as well as the potential complications related to ankle arthrodesis, have
prompted the questfor atotal ankle replacement (TAR) that is reliable and effective. Severe
ankle pain, deformity and dysfunction that serves as a constant impediment to weight
bearing ambulation, often due to arthritis secondary to rheumatoid disease, trauma, joint
sepsis, or osteoarthritis, can be treated by means of TAR. There are basically 2types of
ankle endoprostheses: 1) 2-part prostheses that are either constrained, semi constrained
or nonconstrained; and 2) multi-axial 3-part prostheses that include a free gliding
interpositional core. These devices have been under development since the 1970s and have
yet to be perfected, and the long term results have not be promising for any particular
device, so far. Earlier models were secured with cement, however most surgeons prefer
cementless models. Common complications of TAR include loosening withoutthe presence
of infection, and postoperative dehiscence. Ankle geometry and soft tibial metaphyseal
bone contribute to aseptic loosening, and this complication is most common when a
constrained system is used. Unconstrained systems, on the other hand, are associated with
instability, ankle deformation and subsequent loosening. Difficulties mimicking ankle
geometry stem from the factthatthe ankle is not atrue ginglymus (hinge) joint, and the path
of the center of motion evolves as the ankle goes through its range of motion. Current goals
of ankle endoprosthesis design focus attention on the normal contours ofthe talar dome and
the distal tibial bearing surface, and minimization of the amount of bone resection required
to secure the implant. A number of options exist for TAR, including the Scandinavian
Total Ankle Replacement (STAR) (Waldemar Link GmbH & Co., Hamburg, Germany), a
3-component device; the Agility"" Total Ankle System (DePuy, Inc., Warsaw, IN), a
2-component device; the TNK Ankle (Kyocera Corporation, Kyoto, Japan). a2-component
device; and the Buechel-Pappas Ultra Total Ankle Replacement (Endotec, South Orange,
New Jersey), a3-component device. The main alternative to TAR is ankle fusion, and both
procedures aim to alleviate pain while TAR also aims to improve function. While both
procedures are designed to reduce pain, TAR is also intended to improve function. IfTAR
fails, then consideration is given to arthrodesis, the standard therapy option for ankle
arthrosis and the mainstay of salvage following failed TAR. Salvage after failed TAR often
requires the use of substantial amounts of bone grafting. To date, unlike the results of hip
and knee arthroplasty, the long-term results otTAR have not been as successful. Although
there are many case series describing the benefits and shortcomings of different types of
TAR, further investigation is necessary to determine the best options for patients with
recalcitrant ankle arthrosis.
229
-.
B
Ch.9 Congenital Deformities and Juvenile Surgery
CONGENITAL DEFORMITIES AND JUVENILE SURGERY
Congenital deformities can be familial, inherited traits, or they may present without aknown
family history. The condition may be idiopathic; or a known etiology such as an identified
genetic defect intrauterine or birth trauma, hypoxia, teratogenic drug or toxin exposure,
tumor or other cause may exist. Some defects present as a component of a known
syndrome and other defects, both physical and mental. may be identified.
Macrodactyly (Localized Gigantism)-this idiopathic, rare. usually unilateral, congenital
defect displays abnormal largeness of a single or multiple adjacent toes. It may be related
to or caused by hyperplastic lymphatic or vascular elements, or neurofibromatosis; and
usually occurs as an isolated defect without familial inheritance. In static macrodactyly,
the giant digit(s) display a growth rate proportional to the remaining normal parts. In
progressive macrodactyly. the giant digit(s) display a more rapid growth rate than normal
tissues. Treatment consists either of partial or total amputation of the giant part, or
sequential operations to reduce excess soft tissue and bone in a staged fashion (Figure
9-'). Reconstructive efforts can be difficult and convey a high rate of complication.
A ~ ~
D ~
&
c ~
Figure 9.1
Syndactyly-this is the most common congenital deformity of the foot and hand, and is
marked by partial or complete persistence ofthe interdigital web. The condition is familial,
and can occur unilaterally or bilaterally. The defect occurs during the sixth to eighth
intrauterine week, and most commonly localizes to the second-third toes. Simple syndactyly
involves only fusion of the skin and soft tissues of the adjacent toes, while complex
syndactyly involves fusion of the soft tissues, nails, and bone. Single syndactyly involves two
toes and one web, double syndactyly involves three toes and two webs, and triple
syndactyly involves four toes and three webs. Treatment is usually based not on physical
dysfunction, but rather on psychological or emotional concerns of the older child or adult.
Surgical desyndactylization can be difficult, and techniques involve creation of dorsal and
plantar skin flaps or use of dorsal and plantar W-plasties (Figure 9-2Al. or application of a
FTSG (Figure 9-2B) after incisional separation. Osteotomy may be necessary in cases of
complex syndactyly.
Ii'll:>
3
Ch.9 Congenital Deformities and Juvenile Surgery 231
Polydactyly-this is a common congenital anomaly consisting of an accessory
(supernumerary) digit or digits. The condition is idiopathic and an irregular autosomal
dominant inheritance has been suggested. Preaxial polydactyly involves duplication of the
hallux, while postaxial polydactyly involves duplication of the fifth toe. Postaxial polydactyly
occurs in approximately aO% of cases, preaxial in about 15% of cases, and central ray
duplication occurs in about 5% of cases. Mixed polydactyly involves pre- and postaxial
duplication, and is observed most often in black individuals. Duplication can be either of an
entire extra digit complete with bone (Type A). or of a rudimentary or vestigial toe (Type B).
Polydactyly occurs bilaterally in about 50% of cases. Six radiographic patterns are seen with
extra digits, including the short block metatarsal, V-shaped metatarsal, T-shaped metatarsal,
normal metatarsal shaft with wide head, partial or complete ray duplication, and normal
metatarsal with distal phalangeal duplication (Figure 9-3). Syndactyly can occur in addition
to polydactyly (synpolydactyly). Surgical treatment entails identification of the digit that has
the most potential for normal growth and function, as duplication can involve bone, tendon,
vessels, and nerves. Amputation should allow the foot to assume the most normal contour
and facilitate wearing a shoe. Usually, the most medial digit is amputated in preaxial
polydactyly while the most lateral digit is amputated in the postaxial state. Amputation for
preaxial polydactyly, involving disarticulation of the extra medial toe is associated with the
development of postoperative hallux varus, and K-wire stabilization across the MTPJ with
recession of abductor hallucis are recommended. In cases of postaxial polydactyly,
preserve robust skin (usually plantar) for coverage and closure overthe lateral aspect of the
new fifth ray. In case of an abnormal metatarsal configuration (V or T), the prominent portion
of bone should be osteotomized flush with the metatarsal shaft, and awide metatarsal head
should be made more narrow with osteotomy perpendicular to the growth physis in an
effort to avoid growth disturbance. Central ray duplication can be managed with a dorsal
racquet shaped incision at the base of the toe, and disarticulation and/or osteotomy at the
appropriate level
Figure 9.3
Complete
duplication
232 Congenital Deformities and Juvenile Surgery Gh.8
Congenital Hallux Varus-this deformity involves an adductus and/or varus deviation of
the hallux at the first MTPJ, and is usually observed as a complication of hallux valgus
surgery. Congenital hallux varus can be observed as a consequence of neuromuscular
disease, and often accompanies metatarsus primus adductuslvarus. The Thompson
procedure involves abductor hallucis recession and tendon lengthening, or actual excision
of the muscle, and may be used inthe infant or juvenile with congenital hallux varus due to
non-spastic contracture of this muscle. This technique conveys risk of overcorrection and
hallux valgus.
Congenital Hallux Abductus Interphalangeus (Ungual Phalanx Valgus}-this rare
congenital anomaly displays abduction and valgus positioning ofthe hallux, with the apex
of the deformity at the hallux IPJ. Radiographically, the phalangeal primary centers
appear at birth, and the secondary center between 2-3 years. By 2-3 years of age,
enlargement ofthe medial aspect of the distal phalangeal base can be observed. Surgical
treatment entails excision of the medial aspect of the distal phalangeal base and growth
plate arrest, or Akin osteotomy.
Congenital Curly (Underlapping) Toe--this familial. idiopathic anomaly can involve any of
the lesser toes and occurs uni- or bilaterally. Adductovarus underlapping of a lateral toe
beneath its medial neighbor is most common, however abduction and valgus can also occur.
Treatment entails interphalangeal arthroplasty and derotational skin wedge plasty (Figure
9-4 A, B, and C).
Congenital Overlapping Fifth Toe-this anomaly usually affects the fifth toe overriding the
fourth, with adduction and varus, and dorsal soft tissue contracture in a proximal and
medial direction. The second toe overriding the first is the next most common form of
congenital overlapping toe. As the individual matures, IPJ plantar contracture and hammer
or claw toe ensues. Nonsurgical treatment includes taping or use of adigital retainer to try
to redirect the digit in the infant or youngster. Surgical options include amputation, (which
Figure 9.4A
A
A B
B
Figure 9.4B
Figure 9.4C
233 Ch.9 Congenital Deformities and Juvenile Surgery
A
B
c I ~ ~
Figure 9.5
is a rather undesirable approach)' as well as sequential release of the deformity and
reconstruction. The Butler procedure entails use of racquet-shaped incision, EDL
lengthening, MTPJ capsulotomy (Figure 9-5). The McFarland procedure involves excision
of skin of the web between the fourth and fifth toes, EDL lengthening, MTPJ and PIPJ
capsulotomy, and syndactyly of the fifth-to-fourth toe. The Podiatry Institute technique
involves a dorsal Z-plasty, EDL lengthening, MTPJ capsulotomy, PIPJ arthroplasty,
excision of redundant plantar skin wedge, and K-wire stabilization.
Cleft Foot (Lobster Foot, Claw Foot)-this rare, familial, congenital anomaly displays
absence of part or all ofthe central rays, effecting a claw-like foot. The defect can present
either unilaterally or bilaterally. Associated defects include syndactyly, polydactyly, cleft
palate, deafness, and many others. Surgical treatment focuses on establishing afunctional
limb, and afoot that can be shod. Each case is unique and no specific procedure is always
applicable. Surgery usually combines soft tissue and bone surgery, such as skin and bone
grafting, arthrodesis and osteotomy.
Brachymetatarsia-this hereditary anomaly is characterized by premature closure of the
epiphyseal plate of one or more metatarsals, and most commonly affects the fourth
metatarsal although any or multiple metatarsals can be affected. Associated maladies
include Down's syndrome, pseudohypoparathyroidism, and poliomyelitis. The defect is
usually not recognized at birth, however becomes evident between 4-15 years of age.
Although usually unilateral, brachymetatarsia can occur bilaterally. Surgical treatment has
traditionally hinged on one-stage autogenous bone graft elongation of the affected
metatarsal. This technique, as well as elongating osteotomy such as the Giannestras
step-down, and other sliding shaft deSigns, are limited by skin and neurovascular
compromise secondary to excess lengthening. Skin plasty and Z-Iengthening ottendon, as
well as staging and soft tissue expansion techniques can be useful in this regard. More
recently, bone transport with the mini external fixation has proven to be most effective and
very safe as the soft tissues can gradually elongate along with the bone. Postoperative non-
weight bearing is used for up to 2-3 months pending radiographic evidence of bone healing.
234 Congenital Deformities and Juvenile Surgery Ch.8
Metatarsus Adductus-this transverse plane deformity displays medial deviation of the
metatarsals with the apex of the deformity at lisfranc's articulation. Metatarsus adductus
(MAdd) occurs in lout of every 1,000 live births, is familial, and the presence of the
deformity conveys a 1 in 20 chance that asibling will also have the anomaly, and it occurs
bilaterally in 55% of cases. Clinical findings include aC-shaped foot with convex lateral and
concave medial borders in the transverse plane, adducted metatarsals with the more
medial metatarsals being more adducted (1)2>3>4>5), a high arch if there is no STJ
compensatory pronation, a skewfoot (toes abducted, metatarsals adducted, tarsus
abducted) with heel valgus if compensatory STJ pronation is available, separation between
the first and second digits, inability to abduct the metatarsals past midline of the foot,
hypertonicity and spasm of tibialis anterior in gait or upon striking in open chain, and
possible hyperactivity of abductor hallucis. Ifthe hindfoot is in rigid equinus and varus, rule
out clubfoot. Total MAdd involves all five metatarsals, whereas atavistic MAdd localizes to
the first ray, and is termed congenital metatarsus primus adductus or varus. MPV displays
a first intermetatarsal angle of 10 or greater. Radiographic assessment of MAdd is
necessary to quantifythe degree of deformity. The AP view is used, and the long axis of the
lesser tarsus or that of the second cuneiform can be compared to the long axis of the
second metatarsal (Fig 9-6). Using the long axis of the lesser tarsus, the normal met-add
angle is 15-21, and 25when using the middle cuneiform reference. The Podiatry Institute
radiographic classification system employs the long axis of the lesser tarsus, and defines
met-add as follows: normal (rectus foot) 0-15, mild 16-25, moderate 26-35, and severe
>35. In the AP view, long-term compensation will show moderate-severe hallux abductus,
cuboid abduction, and digital abductus as toes align with rearfoot, and increased Kite's
talocalcaneal angle as the talus adducts medial to the navicular. In the lateral view of
the compensated deformity, an anterior break in the cyma line indicates hyperpronation
and is usually associated with a decreased CIA. The uncompensated foot will display
characteristics of pes cavus.
LTAx
Points plotted for deremination of
logitudinal bisection of lesser tarsus.
Figure 9.6
Lesser tarsal axis (LTAx) represents
perpendicular to bisector of lesser
tarsus. Line "EF" is bisector of
lesser tarsus. Line "G" is bisection
of second cuneiform.
235 Ch.9 Congenital Deformities and Juvenile Surgery
Conservative treatment can be effective if instituted in atimely fashion. For patients <3
months of age, manipulation, taping or casting, can be effective. For patients <3 years of age,
altering sleeping habits to avoid adduction, use of the Ganley splint or corrective casting are
useful. Cast therapy involves three point bending of the foot in the transverse plane (Figure
9-7l. and should be maintained an additional period of time equal to half ofthe time that was
required to eliminate the deformity. If cuboid abduction increases, then over correction is
occurring and casting should be discontinued. The BK cast should entail limited padding,
and effect abductory force at the first metatarsal head and medial aspect ofthe heel, with
an adductory force applied to the cuboid-fifth metatarsal junction. The hindfoot and ankle
are maintained in neutral position. Medial tibial torsion, if present, can simultaneously be
addressed with an AK derotating cast. The cast is changed every 1-2 weeks. Following
correction, a reverse last shoe may be useful for up to 6-12 months.
Surgical treatment is indicated in patients >2 years of age who have reached an
impasse with nonsurgical methods, and offer treatment options for patients up to 8 years
of age. The Heyman, Herndon and Strong (HHS) procedure is performed through either a
transverse or three longitudinal incisions, and entails sectioning of the medial 2/3 of the
capsule and ligaments ofthe tarsometatarsal jOints, followed by K-wire stabilization and
casting. The Thompson procedure can be used in the infant or youngster to correct hallux
varus associated with metatarsus primus adductus or varus. Johnson's chondrotomy
technique entails laterally based (medial apex) wedge resection (2.5 mm) of the
cartilaginous metatarsal base of the lesser metatarsals and a closing abductory base
wedge, distal to the physis, on the first ray; in addition to lengthening abductor hallucis. The
Lange procedure involves first metatarsal-cuneiform capsulotomy with recession of
abductor hallucis, followed by serial casting. The Lichtblau procedure entails sectioning of
a hyperactive abductor hallucis, much like Thompson's procedure, and is indicated in the
equinovarus foot with metatarsus adductus Brown described transfer of tibialis posterior
into the navicular from anomalous insertion, combined with medial cuneiform-navicular
capsulotomy. Ghali described an anterior-medial release of the first metatarsocuneiform
and naviculocuneiform joints with division of tibialis anterior atthe medial aspect of medial
cuneiform. Osseous procedures are indicated in patients 8years of age or older. McCormick
and Blount described arthrodesis ofthe first metatarsocuneiform joint with lateral closing
wedge osteotomy of the second, third, and fourth metatarsals and the cuboid. Peabody and
Muro described mobilization of the first metatarsocuneiform joint combined with excision
of the second, third, and fourth metatarsal bases and lateral closing wedge osteotomy of
the fifth metatarsal. Steytler &VanDerWaIt described pan metatarsal oblique laterally based
closing wedge osteotomies. The Berman-Gartland procedure is a popular technique that
employs lateral closing base wedge osteotomies of all five metatarsals distal to the growth
plates (Figure 9-8). The Lepird procedure (Figure 9-9) is a refinement on the Berman-
Gartland technique that varies with the use of through-and-through rotational osteotomies
of the intermediate metatarsals, combined with lateral clOSing base wedge osteotomies of
the first and fifth metatarsals. The through-and-through osteotomies are made parallel to the
substrate and are initially made with preservation ofthe dorsal-distal-medial cortex, which
is completed only after interfragmental screw placement has been positioned and prior to
achieving final screw purchase after swiveling the metatarsals into corrected alignment.
Fowler described an opening wedge osteotomy of the medial cuneiform, and Ganley
refined the technique to address adeformed LASA (Lisfranc articular set angle) that displays
a severely oblique first met-cuneiform articular interface directed from proximal-medial to
distal-lateral. Ganley performed a medial cuneiform opening wedge osteotomy with
236 Congenital DeformitiesandJuvenileSurgery Ch.8
A
B
Metatarsusadductusangle. Correctionisgainedbycompressing
thereartoot. Metatarsalsarethen
abductedonstableresrfoot.
Figure9.7
Figure9.8
Figure9.9
237 Ch.9 Congenital Deformities and Juvenile Surgery
autogenous bone graft in conjunction with alaterally based closing wedge osteotomy ofthe
cuboid. The resected corticocancellous cuboid bone is harvested for transplant into the
medial cuneiform. The osseous work is combined with appropriate soft tissue releases and
subsequent casting. Bankhart described excision of the cuboid, and Tachdjian-Grice
described a combination of hindfoot extra-articular arthrodesis with forefoot soft tissue
release for correction of skewfoot.
Talipes Equinovarus (lEV, Clubfoot)-this is an idiopathic, triplanar deformity that typically
includes ankle equinus, hindfootvarus, and forefoot adduction; in addition to subluxation of
the TNJ. Although TEV is the most common form of clubfoot equinovalgus can also occur.
Clubfoot occurs in 1:1,000 live births, with a 2:1 male: female ratio. 50% of cases are
unilateral, with the right foot being more commonly involved. The condition is familial, and
siblings display 20-30 times the chance of having clubfoot than the general public. Acquired
forms of clubfoot can be neuromuscular in origin and associated with Cp, CVA, meningitis,
cord lesion, and post-polio; or post-traumatic following burns, ischemic contracture, and
fracture malunion ortendon injury. In clubfoot the head and neck ofthe talus are adducted
60-90" to the body in the transverse plane, whereas the normal relationship is 15-20". In the
sagittal plane, the head and neck ofthe talus are plantarflexed 25-30in clubfoot whereas
the normal relationship is 45-65. Recenttheory embraces medial rotation offoot under the
talus, with the talus staying aligned with the leg (Ganley). The anterior aspect of the
calcaneus is observed to be rotated beneath the talus in a medial direction, while the
posterior aspect of the calcaneus is rotated laterally. There is associated tightness of the
anterior deltoid, tibialis posterior and long flexors, and medial TNJ and NCJ and first
metatarsocuneiform joint; as well as tightness of the CFL laterally. Tethering of the tibialis
posterior tendon pulls the navicular medially and forces articulation with the medial
malleolus. The cuboid, tethered to the navicular by ligament, follows the navicular. Equinus
in clubfoot affects the ankle, and is due to tightness of the heel cord, long flexors, and
posterior AJ and STJ capsules. The wider anterior portion ofthe talar dome does not reside
in ankle mortise, and may pose difficulty in late term realignment due to tightness of the
mortise. Contracted ligaments in clubfoot include: posteriorly, the calcaneofibular, posterior
talofibular ligament and medially, the deltoid, tibionavicular, and calcaneonavicular. Tendon
contractures include: posteriorly, the Achilles; medially, TP, FDL, FHL, and abductor
hallucis; and laterally, the peroneal tendons. Radiographically, clubfoot displays, in the AP
view (Figure 9-10), Kites talocalcaneal angle reduced to 0-15(normal 20-30), the talar-first
metatarsal angle >15, which is indicative of TN subluxation. In the lateral view, the
sagittal plane TCA 0-35(nonmaI35-55) with decrease upon dorsiflexion stress (this angle
will increase in the normal foot).
The Ponsetti method of corrective casting is the mainstay of conservative treatment.
Much like metatarsus adductus, initial efforts are directed at reducing adductus until the
cuboid is anterior to the calcaneus and the navicular is anterior to the talus. Secondly, the
varus is reduced until the calcaneus is no longer medial to and inverted in relationship to
the talus. Lastly, the equinus is reduced after satisfactory reduction of the adductus and
varus components. If a dorsiflexory force is applied before reduction of the adductus and
varus, the STJ and MTJ will hyperpronate and SUbluxation will effect a rocker bottom foot.
If the equinus resists manipulative reduction, and anutcracker compression ofthe midfoot
is likely, then posterior release should be performed before continuing to force dorsiflexion.
Serial cast therapy should be initiated as early as possible, even in the infant. Neonates
may respond to taping alone. Casting is ideal before 6-8 months of age, but can be attempted
238 CongenitalDeformitiesand JuvenileSurgery Ch.8
Normalfoot Clubfoot
Talocalcaneal L20-40 TalocalcanealL15
Figure9.10
eveninolderchildren.Clubfootbecomesmoreresistanttocorrectivecastingafterthechild
beginswalking.Thetypical duration ofcasttherapyis6weeksto 3monthsin patients
<1 yearold, andfrom3-5 monthsin olderchildren.Casting can be continued as long as
progressive correction occurs, howeversurgical intervention should be entertained if
impasse is reached. Serial casts are changed approximately every two weeks. The
durationofcastingisproportionaltothedegreeofrigidity,and growthmustoccurforthe
deformitytoreduce.
Surgeryentailssofttissue release intheinfantand young child.Correction entails
releaseofthosestructuresthataretight,andvariesfrompatienttopatient.Goalsinclude
restorationof theTN,TC,andCCrelationships.Considerationshouldbegiventostagingthe
repairinolderchildren andadults,toavoidneurovascularcompromise.Turcopopularized
theonestageposteromedialand circumferentialreleases(Turco procedure)forclubfoot
repair. The Cincinnati incision, or amedial hockey stick approach can be used. The
Cincinnati incision may limit posterior exposure. The posteromedial release involves
releaseand/orlengtheningofthefollowing:AchillestendonZ-plasty;posteriorankle and
STJ capsulotomy; section CFL and posterior syndesmotic ligament; TP, FDL and FHL
Z-Iengthening;TN, NC, cuneiform-metatarsal capsulotomy;sectioningthe interosseous
talocalcaneal (cervical) ligament; abductor hallucis recession; and smooth K-wire
stabilization of the relocated TN and TC joints. Circumferential release includes the
posteromedialreleasewithadditionalreleaseofplantarandlateralstructures.Theplantar
releaseinvolvesreflectionoftheplantarfascia andintrinsicmusculaturefromtheplantar
cortex of the calcaneus. Lateral release involves sectioning the bifurcate ligament
IV-ligament,orcalcaneonavicular-calcaneocuboidligament),and perhapsZ-plastyofthe
peronealtendonsifindicated.Transferoftibialis anteriorintothe lateral cuneiform may
also be auseful adjunct. Osseous procedures,performedin conjunctionwithsofttissue
releases, include lateral column shortening techniquessuch as the lichtblau anterior
239 Ch.9 Congenital Deformities and Juvenile Surgery
calcaneal lateral closing wedge osteotomy, the Evans calcaneocuboid wedge resection
and fusion, and Ganley's closing abductory cuboid osteotomy. It may be necessary to
osteotomize the lateral cuneiform as well. In case of neglected clubfoot, triple or pantalar
arthrodesis may be useful, however talectomy with tibiocalcaneal-tarsal arthrodesis is the
most frequently used reconstruction.
Congenital Calcaneovalgus-this congenital anomaly presents the foot in an acutely
extended position with the dorsal surface in contact with the anterolateral surface of the
leg. The entire foot, including the heel. is in complete valgus to the point that when the
neonatal foot is pulled into plantarflexion, the following are noted: flexion is limited to the
neutral position, or perhaps slightly beyond; skin and subcutaneous tissues are stretched
tightly due to contracture that reveals a prominent, tight band that blanches in comparison
to surrounding normal skin; the underlying tendons usually not contracted; the calcaneus
(heel) is in valgus with the rest of the foot and there is no frontal plane deviation of the
forefoot in relation to the hindfoot; and the foot is fairly flexible so that the heel and midfoot
can be brought into acorrected varus position (a nonrigid deformity). Normal neonatal ankle
dorsiflexion is approximately 45", unlike the calcaneovalgus foot that can dorsiflex to
become flush with the pretibial surface of the leg. Normal neonatal ankle plantarflexion is
about 50, whereas the calcaneovalgus foot only gets to neutral or a few degrees of
plantarflexion. Increased plantarflexion of talus will be visible on the lateral radiograph,
and Kite's angle will be >35
0
in the AP view.
TABLE 9-1. COMPARISON OF THE NORMAL FOOT VS. THE CALCANEOVALGUS FOOT.
Normal foot Calcaneovalgus foot
Talus sits on top of calcaneus Talus is plantarflexed and the talar head
without overlap of the anterior overlaps the anterior edge of the calcaneus
edges of the bones Bisection of the talus falls plantar to the
Bisection of the talus passes through cuboid on the lateral radiograph
the superior half of the cuboid, If the defonmity is severe, the talus lies
on the lateral radiograph in avertical position
As with many pedal misalignments, the parents usually do not seek an opinion or care
until the child is 6-8 months of age, when the child first stands. In weight bearing, a
complete absence of the arch and severe valgus are noted. Conservative treatment
employs corrective casting using two layers of cast padding after applying skin adherent
(tincture of benzoin). An assistant holds the foot by the toe tips and maintains as much of
an equinus position as possible, while maintaining a neutral relationship of the FF to the
hindfoot, and adduction of the FFto correctthe TN alignment. The cast is then applied from
the toe tips to below-the-knee, molding into the arch and about the heel. A lateral X-ray is
obtained to confirm reduction, and correction is maintained for 2-3 weeks, changing the cast
every 3-4 days in the neonate.
Congenital Vertical Talus (Congenital Convex Pes Valgus, Rocker Bottom Foot)-this
idiopathic anomaly, aform of clubfoot, is characterized by afoot that may actually contact
the pretibial surface at birth. The plantar surface is convex (rocker bottom), and the talar
head can be identified on the medial plantar aspect of the longitudinal arch, with the
hindfoot in equinovalgus. Deforming muscle groups displaying contracture include
240 Congenital Deformities and Juvenile Surgery Ch.8
gastrosoleus complex (ankle equinus); ankle dorsiflexors (TA, EOL, EHL,) and the peroneal
tendons; and the peroneii and tibialis posterior are relatively more anteriorly migrated than
normal. Ligamentous shortening involves the dorsal talonavicular, tibio-navicular,
calcaneofibular, calcaneal-cuboid, interosseous talocalcaneal ligaments; and the
posterior AJ and STJ capsules are tightened. The spring ligament, conversely, is elongated.
Radiographic evaluation employs use of the AP, lateral and forced plantarflexion views
(Figure 9-11 ).In the lateral view, the long axis ofthe talus appears vertical and parallel to that
of the tibia while the calcaneus is in equinus and the forefoot dorsiflexed. In the AP view,
the TCA is increased to >40". The navicular cannot be radiographically evaluated until 3-4
years of age, when it ossifies. When it has ossified, the navicular is identified in a dorsally
dislocated position. The stress plantarflexion lateral view allows comparison of the first
metatarsal on standard lateral and the stress view, so that rigidity of the deformity can be
determined. Normally, the talar and first metatarsal axes are parallel; however in the
presence of arigid plantarflexed talus, the talar axis passes through sale offoot and the first
metatarsal axis passes dorsal to head of talus. In the forced plantarflexion view, this
relationship will not be reduced. Convex pes valgus is categorized as either Type I or Type
II. Type I involves dislocation ofthe TNJ, subluxation of the TCJ, and a normal CCJ. Type II
is more rigid and involves dislocation of the TNJ, subluxation of the TCJ and CCJ, and ankle
equinus. The differential diagnosis for calcaneovalgus includes talipes calcaneovalgus,
severe pes valgoplanus with gastrosoleus equinus, paralytic pes valgoplanus,
myelomeningocele, polio, and rigid pes valgus due to tarsal coalition. Associated
deformities include cleft palate, arthrogryposis, and spastic equinus due to CP and others.
Treatment of congenital vertical talus focuses on restoring the normal TN, Te, and
CCJ relationship as soon as possible. This condition is notoriously resistant to nonsurgical
treatment. As with talipes equinovarus, manipulation and serial corrective casting
(Ponsetti method) are useful. At birth, gentle manipulation is used to stretch the contracted
soft tissues. Manipulation entails stretch of triceps surae and calcaneofibular ligament via
distal and medial traction, plantarflexion and adduction ofthe FFto stretch dorsiflexors and
everters, and distal traction ofthe FF and TNJ to effect adductus and varus stretch ofthe
tibionavicular and talonavicular ligaments. The stretch is held for 15 seconds and then
released, and the exercise is continued for 15 minutes after which the cast is applied. The
cast is changed twice per week for six weeks. As correction ensues, focus more on TN
reduction by means of distal FF traction until the head of the talus dorsiflexes and the
calcaneus is pulled under the talus. It may become necessary to maintain the closed
reduction with percutaneous pin stabilization. If, after 4-6 months of closed reduction,
Figure 9.11
241 Ch.9 Congenital DeformitiesandJuvenileSurgery
impasse is reached, then open reduction should be performed. The longer the TN
dislocationpersists,the morethe softtissue contracturedeforms bone and surrounding
joints. Surgical repair of congenital vertical talus employs amedial, curvilinear skin
incisionextendingfromthemedialaspectoftheAchillestendonatapoint4-6cmproximal
totheankle,aroundthetipofthemedialmalleolus,andonwardtothejunctionofthefirst
metatarsal and medialcuneiform.The neurovascularbundleisretracted,afterwhichthe
Achilles,TA, EHl, and peronealtendons areZ-plastylengthened.Thetibionavicular,TN,
bifurcate,and dorsalcalcaneocuboid,calcaneofibularandTCinterosseousligamentsare
then sectioned. The talarhead is manipulated dorsally and the navicularmoved in a
plantardirectionwith inversion.Asmooth 0.062" K-wire isthen drivenfromthe posterior
aspectofthetalusacrossthereducedTNJ,andcontinuedanteriorlyacrosstheNCJ.The
spring ligamentisthen reefedtightly,and anAKcastusedtomaintainthe correctionfor
12-16weeks.TheK-wirecanberemovedaround6weekspostop.Avascularnecrosisofthe
talusisapossiblecomplication.Excisionofthenavicularhasbeeneffectiveinthetreatment
ofrigidarthrogryposisinpatients3-6yearsofage. Inchildren>6yearsold,rigid boneand
jointadaptationmayindicatetheneedfortriplearthrodesis.
Tarsal Coalition-thisconditionoccursduetofailureofdifferentiationand segmentation
ofprimitivemesenchymewithresultantlackofjointformation.Typesofcoalitionsinclude:
syndesmosis or fibrous, synchondrosis or cartilaginous, and synostosis or osseous.
The middle facettalocalcaneal (TC) coalition occurs mostfrequently, followed bythe
calcaneonavicular(eNbar),andthen bythetalonavicluar(TN)coalition.The ageofonset
ofsymptomsvariesasfollowswiththesiteofthecoalition:TN coalition,3-5years;CN bar,
8-12years;TCcoalition,12-16years.The3predominantsymptomsinclude:
1. Tonic peroneal muscle spasm, hencetheterm peroneal spasticflatfoot,with
antalgiceversionguardingagainstSTJmotion;
2. LimitationofSTJand possiblyMTJmotion;and
3. Pain uponweightbearing orattemptedhindfootmotion.
Classically, arigid flatfootdeformitydisplaysthe combination ofperoneal spasm,
stiffness,and pain.Radiographicevaluationoftarsalcoalition,inthe lateralview, reveals
talarbeaking,increased halo effectorscleroticappearance ofsustentaculumtali and
crucialangleareaofthecalcaneus,broadeningandflatteningoflateraltalarprocess,and
diminished orabsentjointspace ofmiddleand posteriorfacets.Themedial obliqueview
(lateral projection)isthe bestviewtovisualize aCN bar. Isherwood views andthe 60
0
medial oblique are bestforvisualization ofthe anteriorfacetofthe STJ. Asingle 45
0
calcanealaxialorasetofHarrisandBeathviewswillrevealtherelationshipofthemiddle
andposteriorfacets,whichshouldbeparallel.ThepresenceofaTCcoalitionwillmakethe
relationship oblique or obliterate the involved, usuallymiddle or medial, facetspace.
Secondary articular changes are those of joint space narrowing, osteophytosis, and
subchondralsclerosis.TheseareclassicallyobservedatthedorsalaspectoftheTNJinthe
formofdorsalexostosis,ortalarbeaking,inassociationwithaTC coalition;orintheform
ofthe parrot beak sign (anteater sign, calcaneal beak) in association with aCN bar.
Wide-anglelineartomography,makingimagesacrosstheSTJsat5mmintervalsbeginning
atthe lateralmalleolus, can also be usefuL CT scanning and MRI can also be used to
identify coalitions, and MRI is particularly useful in cases of fibrous or cartilaginous
bridging. Conservative treatmentoftarsal coalition entailsstabilization ofthe STJ using
242 Congenital Deformities and Juvenile Surgery Gh. B
strapping, foot orthoses, and cast immobilization in acutely painful cases with marked
peroneal spasm. Corticosteroid infiltration into the sinus tarsi may also yield symptomatic
relief. Surgical intervention for persistently painful CN bar involves resection of the
coalition and is best performed before 14 years of age. The bar is excised via an Oilier or
similar approach to the sinus, and Bagley described transplantation of the EDB muscle
belly into the excision site in an effortto avoid the development of rigid fibrosis in the cleft
(Figure 9-12). Postoperative non-weight bearing and immobilization are used for 4-6 weeks.
In cases of Te coalition in ayoungster with no secondary arthrosis, consideration can be
given to resection of the coalition, and arthrodesis may become necessary in the future. In
the adult without significant secondary arthrosis, isolated TC fusion is indicated. In any
patient with significant secondary arthrosis, triple arthrodesis is indicated.
Figure 9.12
Pediatric In-toe Deformity-a variety of conditions can cause an in-toe, or medially
adducted gait. The most common causes are femoral anteversion, which usually self-
corrects by 3 years of age, and metatarsus adductus. Talipes equinovarus, metatarsus
primus varus, juvenile hallux varus, and medial tibial torsion also display in-toe.
Asymmetry pronounced deformity, pain, or gait imbalance all warrant evaluation.
Treatment may range from simple observation to manipulation, reverse last shoe, casting,
night splints, or surgery depending upon the cause and degree of deformity.
Pediatric Toe-walking Gait-a variety of causes can lead to an equinus or toe-walking
stance and gait, including: CP, delayed myelinization ofthe corticospinal tracts, muscular
dystrophy, GMT and other peripheral neuropathies, disease of the basal ganglia such as
dystonia musculorum, spinal cord defects such as spina bifida, talipes equinovarus,
gastrocnemius or gastrosoleus equinus, prancer syndrome where the child mimics toe
walking seen in adults or older children, autism and conditions of mental retardation
Micromelia-this rare congenital defect has been associated with hypoxia, maternal
thalidomide intake during gestation, and involves pathological smallness of the limb. The
condition is usually associated with other defects. No specific treatment is recommended
for the extremity.
Congenital Hemihypertrophy-this rare, idiopathic anomaly usually displays enlargement
of the ipsilateral upper and lower extremities or parts thereof. Possible causes include
neurofibromatosis, vascular or lymphatic hyperplasia, AV fistula, malignancy, or benign
243 Ch.9 Congenital Deformities and Juvenile Surgery
tumor. When indicated, treatment is directed at the identified primary defect, or ablative
intervention on the involved limb. Shortening osteotomy, arthrodesis, and soft tissue
debulking techniques can be used in one stage or multi-staged procedures.
Osteochondroses-these acquired diseases affect growth centers, both primary and
secondary, and have been attributed to vascular disturbance and/or trauma. Systemic
arthritis, infection, certain medications and toxins, and tumors can also disturb the growth
center, however the osteochondroses are generally observed as idiopathic, insidious
conditions that occur in active youngsters and cause diffuse aching and guarded
ambulation. Radiographic inspection may reveal irregularity and fragmentation of the
growth center and adjacent physis, and increased soft tissue density and volume. Treatment
usually entails rest, ice, compression, and elevation, and appropriate oral anti-inflammatory
medication can be helpful. Gel casting and use of a surgical shoe, cast or splint
immobilization, protected weight-bearing and follow-up use of foot orthoses may also be
used. Specific osteochondroses include:
Freiberg's infraction-osteochondritis that usually affects the second metatarsal head,
more common in females 2:13 years of age, resulting in flattening and widening of the
metatarsal head, and attributed to traumatic disruption ofthe physeal blood supply.
Lushke's disease--osteochondritis of the fifth metatarsal base, observed in children 5-11
years of age.
Kohler's disease-osteochondritis ofthe tarsal navicular, most common in boys 3-6 years
of age.
Sever's disease--osteochondritis ofthe calcaneal apophysis, observed in children 8-14
years of age and most common in boys.
Osgood-Schlatter's disease-osteochondritis of the tibial tuberosity, most common in
athletic boys aged 11-15 years. It is important to rule-out osteosarcoma in this age group
and location.
244 Management of Foot and Ankle Trauma Ch.10
MANAGEMENT OF FOOT AND ANKLE TRAUMA
Basic principles of the management of trauma include athorough assessmentofthe injured
patient, triage, and appropriate treatment of specific injuries. Priorities include basic and
advanced life support (described elsewhere in the manual), which entail maintenance of
an airway, CPR, identification and control of hemorrhage, monitoring vital signs (BP, pulse,
respiration, temperature, and level of consciousness). and fluid management. Blood should
be obtained for typing and cross matching, if the potential for substantial volume depletion
exists. While waiting for compatible whole blood, an IV infusion of glucose and water,
plasma, plasma expanders, or lactated Ringer's solution may control shock temporarily.
Ideally, whole blood should be administered for severe blood loss. Specific injuries of soft
tissues and bone should then be determined. Injuries include punctures, abrasions,
incisions, and lacerations (PAIL). as well as burns, penetrating trauma, fractures, and
dislocations. Tetanus prophylaxis is aconsideration in every form of trauma that results in
cutaneous compromise. In general, the injured lower extremity should receive protection,
rest, ice, compression, and elevation (PRICE). after assessment of the neurovascular
status to the injured limb.
SELECTED SOFT TISSUE INJURIES
Cutaneous Wounds-After ascertaining the systemic status of the patient, local tissue
factors may be evaluated. Inspection enables identification of pathological anatomy and the
presence of foreign body. An open wound is considered "old" and contaminated if care
has not been administered within 6 hours afterthe onset ofthe injury. The status ofthe skin,
vessels and nerves, tendons, bones and joints must all be documented based on the
merits of each individual injury. Local, regional, and even general anesthesia may be
necessary in order to thoroughly identify pathology. The procedure may take place in the
office, emergency department, orthe operating room. Intravenous conscious sedation with
local or proximal field block often suffices for foot and ankle injuries. Local anesthesia
should only be infiltrated after assessment of the peripheral neurovascular status, and then
only proximal to the injured tissues. A proximal tourniquet is usually preferred as compared
to dilute vasoconstrictor in the local block. Normal sterile saline, warm or room
temperature, a bulb syringe or 18-gauge needle with a 20-50 cc syringe, and aseptiC
technique are used for lavage, inspection and local debridement. TIssue forceps, scalpel,
curette, and other probes may be helpful. Adequate debridement entails removal of all
necrotic or heavily contaminated tissue, including small fragments of bone, and foreign
bodies. Skin viability is ascertained clinically by a pink dermal coloration, warmth, and
capillary bleeding. If necessary, IV administration of 10-15 mg/kg of fluorescein dye
followed by observation of the tissues under Wood's light will reveal dye uptake in the
tissues by means of fluorescence. Fascia is relatively expendable due to its diminished
vascularity compared with other tissues, and it is also prone to infection. For tendon to
remain or become viable, it must be covered with intact skin or graft, flap, muscle, or a
suitable skin substitute. Muscle viability is determined by the presence of the 4 Cs: color
(beefy red), contractility (upon electrical stimulation), capillary bleeding (bright red blood),
and consistency (firm, elastic). Specimens should be obtained for C&S, as well as for
histopathological inspection of appropriate tissues. Following initial debridement,
definitiVe therapy can be determined, or additional debridement may be in order.
Specialized vascular and/or neurological consultation may be indicated following initial
245 Ch.10 ManagementofFootandAnkleTrauma
debridement,priortodefinitivereconstructiveefforts.Similarly,infectiousdisease,internal
medicineandanyotherappropriatedconsultationthatisindicated,couldbe obtained.
Tetanus Prophvlaxis-the specific action to be taken is determined by the patient's
immunizationhistory,asfollows:
1. Ifimmunizationwascompleted previously, andthe lastboosterwaswithin 1
year;thenthereisnoneedtoadministertetanustoxoidorimmuneglobulin.
2. Ifimmunizationwascompletedwithinthepreceding10yearswithoutsubsequent
booster,thenadminister0.5mltetanusanddiphtheriatoxoid(adultTd).
3. Ifimmunizationwas completed>10years ago,andthelastboosterwaswithin
the preceding10years;thenadminister0.5ml ofTd.
4. Ifimmunizationwas completed>10years ago, andthere has been no booster
withintheprevious10years,andthewoundisminor,relativelycleanandtreated
promptly;thenadminister0.5mlofTd.
5. Ifimmunizationwas completed>10years ago, and therehas been no booster
withinthe preceding 5years, and the wound is dirtyor>6-8hours old;then
administer0.5mlofTdand250-500unitsofhumantetanusimmuneglobulin(TIG
[h]).The5OO-unitdosageisusedifthewoundisconsideredpronetoclostridial
contamination, otherwise 250 units is sufficient. The Td and TIG[h] are
administeredusingseparatesyringesandneedles,atdistantsites(deltoid and
contralateralglutei).
6. Ifthere is no history of immunization, and the wound is minor, clean, and
treatmentisprompt;theninitiateanimmunizationprogramwith0.5mlofT dand
schedulethefollow-upboosterseries.
7. Ifthere is no history ofimmunization and the wound isdirtyortreatmentis
delayed;then administer0.5 mlTd and250 unitsTIH[h] andfollow-upwiththe
boosterseries.Give500unitsTIG[h]ifthewoundisclostridia-prone.Inaddition
to Td and TIG[h], 10-20 million units of aqueous penicillin-G should be
administered IV for a tetanus- prone wound, and appropriate cleansing
debridementandwound care undertaken.
Nail Trauma-traumaticconditionsthataffectthe nailandassociatedstructuresinclude
subungual hematoma, and hematoma with underlying phalangealfracture; simple and
complex nail bed lacerations; and nail bed tissue loss injuries such as partial digital
amputation,degloving andavulsion.Themajorityofnailinjuriesresultfrom blunttrauma,
eitherstubbing ordroppingsomething heavyon thetoe.Treatmentcan be enhanced by
digitalormetatarsalrayblockwithlocalanesthetic infiltratedinto normal-appearingskin
proximaltothedefect.Subungualhematomacausesthrobbingpainashemorrhagethrough
the nail bed accumulatesinthe potential space betweenthe plate and bed, and usually
requires no moretreatmentthan reassurance and observation. Hematoma will slowly
migrate forward with nail growth, and takes 7-9 months in the adult for complete
regenerationofatoenail.Painfulhematomaintheacutephasemaybenefitfromdrainage
byperforatingthenailplatewithahandcautery,oranarrowrotaryburor#11 scalpelblade.
The toe isprepped with antiseptic beforedrainage,then antibiotic cream and asterile
coverletafterwards.lfthesubungualhematomainvolvesgreaterthan25%ofthevisiblenail
plate, andthe plateisunstableuponthe nail bed,then serious considerationshould be
giventoavulsionofthenailplateandinspectionofthedamagednailbed(Zook'srule).Nail
246 Management of Foot and Ankle Trauma Ch.10
----"
bed lacerations are either simple transverse, oblique or longitudinal lesions; or complex
(stellate, crushing), perhaps with apices that will eventually undergo necrosis.
Approximately 20% of subungual hematomas are associated with distal phalangeal
fracture, which can technically be considered an open fracture after either traumatic or
therapeutic nail plate avulsion in the presence of nail bed laceration. After cleansing
debridement, the nail bed is sutured with 4-0 or 5-0 absorbable suture in fresh, clean
wounds; or nonabsorbable suture in heavily contaminated or longstanding (>6 hours)
wounds. The nail bed is bandaged with nonadherent gauze preserving the cui de sac
nature of the proximal nail fold, and appropriate supportive measures are used. Nail bed
tissue loss injuries are defined by the Rosenthal classification system, which describes the
level of tissue loss as either distal to the bony phalanx (zone 1), distal to the lunula (zone 2),
or proximal to the distal margin of the lunula (zone 3); and according to the direction of
tissue loss as either dorsal oblique, plantar oblique, transverse guillotine, tibial or fibular
axial, or central gouging (Fig 10-1). Treatment includes cleansing debridement, and
coverage with local transport of adjacent skin by means of the Atasoy flap (plantar-to-tip
V-V flap) or Kutler flap (medial and lateral V-V plasties) after reduction of any prominent
distal phalanx. Split- and full-thickness skin grafts can also be used to cover broad defects.
Lesions proximal to the OIPJ may require disarticulation. Complications of nail bed injury
include delayed nail regeneration; matrix disturbance with Beau's transverse line or ridge,
A
o
B
c
E
Figure 10.1
Ch.lO Management of Foot and Ankle Trauma 247
onychocryptosis, and nail dystrophy with onycholysis and secondary fungal infection,
canaliformis or split-nail deformity, and an unstable nail.
Burns and Frostbite-burns are caused by thermal injury, both hot and cold, and chemical
and electrical injury. The severity of a burn depends upon the extent of surface area and
depth of skin penetration. Tissue damage is caused by protein denaturation, fluid
extravasation, and edema. The extent of a burn is designated as a percent of total body
surface area (TBSA), and the rule of nines is applicable. The body is divided into multiples
of 9% (Fig. 10-2). Partial-thickness burns include first and second degree wounds.
Full-thickness burns are designated as third degree. First-degree burns involve only the
epidermis, show erythema and no blisters, and are painful. The most common form is
sunburn. Second-degree burns are either superficial or deep. Asuperficial second-degree
burn involves injury to the epidermis and a portion of the dermiS; and they are
erythematous, moist with blister formation and serous drainage, and are very painful.
A deep second-degree burn injures the epidermis and most of the dermis, leaving skin
appendages intact. It mayor may not show blister formation and can be dry and it might
display scattered anesthesia. Athird degree burn involves full-thickness skin and aportion
of the subcutaneous layer, destroying all skin appendages, thrombosing vessels, and
appearing dry, anesthetic, whitish and leathery (eschar). Athird degree burn can extend to
bone. Fourth degree burns are caused by low voltage 1000 volts) electrical injury, and
fifth degree burns are caused by high voltage electricity or radiation injury. Fourth and fifth
degree burns involve muscle and bone.
Minor burns can be treated outpatient and include all first-degree, second-degree
<15% total body surface area (TBSA), and third-degree <2% TBSA wounds. Moderate burns
may be treated either in or out of the hospital, based on specific merits of each case, and
include second-degree >15% TBSA and third-degree <10% TBSA. Severe burns require
inpatient treatment and entail any third-degree burn of the foot, hand or face; second-
degree >30% TBSA, third-degree>10% TBSA, or any burn with associated sepsis,
Figure 10.2
,
t\
' ~ J ~
} I
~
248 Management of Foot and Ankle Trauma Ch.1O
fracture, or systemic complication such as shock or cardiopulmonary disorder. The goals
of treatment are to stop the burn process, prevent infection, and enhance healing.
Fundamentals include airway management, fluid management (IV lactated Ringer's
solution or fresh frozen plasma, monitor urine output; along with tetanus prophylaxis, IV
and topical antibiotic, analgesia, and escharotomy. Silver sulfadiazine and sulfamyalon
(anti-pseudomonal [nosacomial)}, sterile water lavage, and porcine heterograft or
biosynthetic skin substitutes may be used. First-degree burns respond well to topical lotions
to moisturize and diphenhydramine and methylprednisolone in adose pack may be helpful
in some cases. Second-degree burns are managed much like abrasions, cleansed,
blisters that are very large or already show drainage are debrided, followed by application
of topical antibiotic cream and sterile bandage. Third degree, or full-thickness burns
require excision of necrotic eschar followed by autogenous split-thickness skin graft (STSG)
or temporary coverage with porcine heterograft or skin substitute until the patient can be
prepared both locally and systemically for definitive skin grafting or other plastic
reconstruction. Compressive dressings, splints, and early physical therapy for range of
motion are crucial therapeutic measures that minimize contracture and edema.
Complications of burns include hypertrophic scar, contracture deformity, syndactylization,
ischemia, and vasomotor instability.
Frostbite is also categorized based on the depth of penetration. First-degree frostbite
displays freezing of the epidermis with subsequent pain, erythema and exfoliation, but no
blister formation. Second-degree frostbite involves freezing of the entire epidermis and a
portion of the dermis, and pain develops after thawing. Third-degree frostbite involves
freezing of the entire thickness of skin and displays localized ulceration. Fourth-degree
frostbite also involves full-thickness skin freezing, however the extent of injury is more
extensive in the extremity, encompassing an entire hand or foot, leg or arm. Superficial
frostbite, first- and second-degree, is also termed chilblains. Trench foot implies freezing or
near freezing in a wet environment, with vasospastic hypoxia, necrosis and subsequent
edema. Systemic hypothermia is described as a core body temperature <90
0
F, with
dehydration, and cardiogenic shock can ensue.
Treatment of frostbite entails protection of the part, avoiding friction rubbing to try to
stimulate warming frozen tissues, and getting to a place where rewarming and
assessment of the core body temperature can be achieved in a definitive fashion.
Refreezing is particularly destructive. Rewarming of the frozen part is done in afootbath with
water at 38-44
0
Cin 15-20 minutes. Administration of IV dextran counters the osmotic
imbalance due to local tissue dehydration in the frozen part. Tetanus and antibiotic
prophylaxis, analgesia, and subsequent sterile bandaging are also in order. Sequelae
include cold sensitivity, Raynaud's phenomenon, paresthesia and pain, and contracture.
Puncture Wounds (see Chapter 3)
Gunshot Wounds (GSW) and Penetrating Trauma-gunshot wounds are a form of
penetrating trauma associated with awide range of defects, both local and systemic. In the
lower extremity, low velocity injuries are most common. The projectile creates a path and
cavity in the tissues, which varies with projectile mass, velocity, and tissue density and
volume. Kinetic energy is equal to half of the mass times its velocity (KE 1/2 mv2),
therefore both velocity and mass greatly influence the amount of energy sustained by the
bodypart. A low velocity projectile, shot from most handguns, effects a straight and
narrow, orfocused path and cavity; whereas ahigh velocity projectile, shot from ahunting
249 Ch.10 Management of Foot and Ankle Trauma
rifle or military weapon, will yaw, tumble and create a large cavity as it traverses the body
part. Soft nose or hollow point, as well as jacketed bullets, are designed to deform and
fragment upon impact, thereby creating more projectiles that result in more damage. Low
velocity projectiles frequently do not create an exit wound, even when bone is not involved.
High velocity bullets create entry and exit wounds. Exit wounds are usually larger than the
entry defect, since the projectile deforms and fragments, along with the tissues, as it
penetrates and traverses the part. When a low velocity projectile encounters bone in the
foot, a typical udrill hole" defect can be observed radiographically where the bullet
traverses the bone. High velocity bullets shatter small bone into fragments that are often too
small to repair. Treatment of GSWs entails triage, identification of the systemic and local
tissue status, attention to neurovascular compromise, tetanus and antibiotic prophylaxis,
cleansing debridement and removal of necrotic soft tissue and bone, foreign body bullet
removal, skeletal stabilization and reconstruction, often requiring bone grafting. Definitive
reconstruction may be performed on a delayed basis. Completion of a police report is
usually required.
Knife wounds represent a form of low velocity penetrating trauma. The path and
cavity are very narrow and distinct. Identification of systemic and local pathology proceeds
in a fashion similar to that for gunshot wounds, and the management protocol is
essentially the same.
Animal and Human Bite Wounds-these are crushing injuries that convey special
microbiology related to a wide range of organisms and tissue necrosis. Anaerobes and
both gram-negative and positive organisms may be present. Cleansing debridement with
identification of pathological anatomy proceeds in the standard fashion.
Peroneal Tendon Dislocation, Stenosis, and Rupture-dislocating peroneal tendons can
be caused by forced eversion of the hindfoot with ankle dorsiflexion, a direct blow to the
lateral aspect of the hindfoot and/or ankle, or due to congenital absence or defect of the
peroneal groove in the lateral malleolus. Symptoms include hindfoot and ankle pain and
edema due to peroneal tendinitis, palpable crepitus, and aclicking sensation as the tendon
subluxates from behind the fibula and displaces anteriorly. Radiographs may show an
avulsion fracture fragment from the lateral malleolus or defect in the peroneal tubercle of
the calcaneus. MRI can also be useful, and may reveal a split-tear of the peroneal tendon,
tenosynovitis of the peroneal sheath, as well as any associated osseous lesion. Treatment
involves cast immobilization in the acute phase for 3-6 weeks, or ankle bracing during
strenuous activity in the chronic state. Surgical reconstruction of the peroneal retinaculum
(Fig. 10-3) or ofthe peroneal groove in the fibula (Fig. 10-4) may be indicated in recalcitrant cases.
Stenosing peroneal tenosynovitis can be caused by direct, acute trauma sustained
during fibular, talar, or calcaneal fracture; or by chronic microtrauma due to an enlarged
peroneal tubercle or constricting retinaculum. Symptoms include pain upon hindfoot/ankle
inversion, and stiffness. Signs include point tenderness along the tendon at the point of
entrapment, and thick, boggy edema. Diagnostic studies include lateral and calcaneal
axial radiographs, peroneal tenogram, or MRI. Treatment involves supportive bracing,
corticosteroid infiltration, and perhaps physical therapy; or surgical repair of bone, sheath,
and tendon. Postoperative physical therapy may also be in order.
Peroneal tendon rupture is uncommon, and may result from laceration, severe
hindfoot/ankle fracture/dislocation or, more typically, chronic degeneration. Signs and
symptoms include edema and pain in addition to associated injury, as well as absence of
250 Management of Foot and Ankle Trauma Ch.10
.\ Y!.;
Figure 10.3 Figure 10.4
Figure 10.5
eversion function and inability to plantarflex the first ray. MRI is essential to making the
diagnosis, and has replaced the use of the peroneal tenogram in most cases. Longitudinal
split-tears may be identified. Treatment entails surgical repair, perhaps with tendon graft,
postoperative immobilization, and gradual rehabilitation.
Ankle Ligamentous Injury-collateral ligament injury involving the ankle is very common.
It should be noted thatthe calcaneofibular ligament (eR) runs anterior to posterior in the
sagittal plane and angulates 20-40 from the long axis of the fibula, while the anterior
talofibular ligament (ATFL) courses lateral to medial in the frontal plane (Fig. 10-5). The
orientation of the ligaments can be difficult to recreate with secondary surgical repairs,
and nonphysiologic motion may follow such treatment Causes of ankle instability include
post-traumatic ligamentous disruption, osteochondritis dissecans (OeD) ofthe talar dome,
DJD with ligamentous laxity, peroneal subluxation, muscle weakness or paralytic dropfoot,
talofibular meniscoid (defective ligament trapped between articulating surfaces),
tibiofibular diastasis, nonunion of previous ankle fracture or poorly reduced yet healed
fracture (shortened fibula), fixed calcaneal varus, tibial varum, rigid plantarflexed first ray,
pes cavoadductovarus, or femoral anteversion ortibial torsion effecting pronounced in toe.
Acute Ankle Ligament Disruption (lnstability)-acute disruption of the lateral
collateral ligaments causes immediate ankle instability, and may lead to chronic
251 Ch.10 Management of Foot and Ankle Trauma
instability and arthrosis. Most cases of acute disruption are treated with non-
operative functional therapy that involves temporary immobilization for up to 4weeks,
weight bearing ambulation, and gradual rehabilitation for strength and flexibility.
Aspiration of hematoma or hemarthrosis may be indicated. Acute ankle instability is
determined by the presence of pain, edema, antalgic gait, and clinical and
radiographic evidence of anterior drawer and/or talar tilt. In many cases, chronic
instability conveys minimal chronic pain despite frequent inversion sprain. Instability
can be identified with the stress lateral (anterior drawer) and stress AP (talar tilt)
radiographs. Classification of the acute injury is based on the presence or absence of
ligament disruption and resultant instability. Afirst-degree sprain correlates with ATFL
rupture, while a second-degree sprain correlates with ATFL and CFL rupture, and a
third degree-sprain correlates with ATFL, CFL and posteriortalofibular ligament (PTFL)
rupture, although this classification system can be confusing and difficult to
accurately determine. Crucial to the diagnosis, however, is the determination that
ankle instability is or is not present. Anterior drawer of 5-8 mm suggests rupture of
the ATFL, 10-15 mm suggests rupture of the ATR and CFL, and>15 mm suggests
rupture of the ATFL, CFL, and PTFL Talar tilt of >1()" suggests of rupture of the CFL
Surgical intervention may be considered after acute disruption in the patient with an
active/strenuous occupation/avocation, positive stress radiography indicative of at
least ATFL and CFL rupture, and adequate local and systemic findings to sustain
surgery. Primary collateral ligament repair, in the acute or delayed (months to years
after disruption) setting, involves a lateral curvilinear incision extending from the
posterior margin of the fibular malleolus to the lateral margin of the EDL anteriorly.
Dissection should occur between the sural and intermediate dorsal cutaneous nerve
trunks. Immediately upon penetration of deep fascia, capsule and ligament will be
evident Hematoma is evacuated in the acute phase, and scar dissected in the chronic
scenario. Ligament is repaired with suitable suture, and intra-osseous anchors or
fracture fragment repair in the case of ligament avulsion, may be indicated.
Intraoperative stress anterior drawer and talar tit!: should be negative. Postoperative
immobilization in aweight-bearing attitude, with the ankle in a neutral alignment, for
3-4 weeks followed by bracing and rehabilitation is undertaken.
Chronic Ankle Ligamentous Disruption (lnstability)--secondary ankle ligamentous
reconstruction can be useful in the treatment of chronic instability, and entails
reconstructive procedures that approximate rather than truly restore ligaments to
their native state. It is difficult to recreate ligaments that mimic the ankle's normal
orientation and physiologic motion, despite restoring stability. Traditionally, peroneus
brevis has been harvested for ligament reconstruction, however peroneus longus is
now more frequently used as the supinatory influence ofthe first rayon the ankle can
be diminished by eliminating the pull of peroneus longus while preserving the everter
function of peroneus brevis. There are many options, and the surgeon should pursue
a reconstruction that best suits the patient's needs. The use of intraosseous tendon
anchors and nonabsorbable suture materials are useful in these repairs. Procedures
that recreate 1ligament, namely the ATFL, include:
Watson-Jones (Fig. TO-6)-detach peroneus brevis (PB) proximally and suture
its belly to peroneus longus, then reroute the distal portion through 2drill holes
that course transversely through the fibula and asingle drill hole in the neck/head
of the talus. The tendon is first directed from posterior to anterior through the
252 Management of Foot and Ankle Trauma Ch.lO
proximal fibular channel, then from superior to inferior through the talus, then
back through the distal fibular channel from anterior to posterior and sutured
upon itself and periosteum at the posterior aspect of the lateral malleolus.
Lee (Fig. 1O-7Hetach PB tendon as proximal as possible and suture its belly to
peroneus longus, then reroute the harvested distal portion of the PB tendon from
posterior to anterior through a drill hole in the distal fibula, then suture the
tendon to itself distal to the lateral malleolus.
Nilsonne (Fig. 1O-8}--detach PB proximally and suture its belly to peroneus
longus. Create a subcortical trough with a gouge in the lateral malleolus while
preserving an anterior cortical hinge, then place the tendon into the trough and
flap the cortex over the tendon and suture periosteum to stabilize both cortex
and tendon.
Evans (Fig. 1O-9}--detach PB proximally and suture its belly to peroneus longus,
reroute the distal portion of the tendon through a drill hole in the fibula from
anterior-inferior to posterior-superior, then suture the tendon to periosteum at
both ends of the osseous tunnel.
Figure 10.7
Figure 10.8
Figure 10.9
253 Ch.10 Management of Foot and Ankle Trauma
Procedures that recreate 2 ligaments (ATFL and CFL), include:
Christman-Snook (Fig. lD-TO)-detach asplit portion of PB proximally (PB is deep
to peroneus longus (PL) at the proximal level of sectioning), then split PB to the
vicinity of the fifth metatarsal base, then reroute the split portion in asubperiosteal
and subcapsular fashion to the anterior surface of the lateral malleolus. Next,
route the tendon from anterior to posterior through a drill hole in the fibula, then
course inferiorly superficial to the peroneal tendons posterior to the lateral
malleolus toward the lateral wall ofthe calcaneus. Route the tendon through a
small channel created in the calcaneus from posterior to anterior and suture the
tendon to periosteum and the PB and PL tendons posterior to the fibula.
Split Peroneus Brevis Lateral Ankle Stabilization (SPBLAS) (Fig. TO-11)-this is
a modification of the Christman-Snook procedure that involves simply
transplanting the split portion of PB into atrephine hole in the lateral aspect of
the calcaneus and packing the site with the trephine bone plug rather than
suturing the tendon to PB and PL after channeling through the calcaneus.
Having converted to the use of PL, this technique is now referred to as the
SPLLAS, and proceeds as described previously with the only significant
variation being use of a split portion of PL.
Elmslie (Fig. 1O-12)-fascia lata is harvested and used as afree graft anchored
through a channel in the calcaneus and one in the talar neck, routed through a
drill hole in the fibula.
A variety of other secondary ankle ligament repairs have also been described,
including use of free tendon graft and synthetic ligament substitutes. Over time,
however, the delayed primary repair has offered the best physiologic result and should
be the surgeon's first choice if enough ligament can be identified and sutured.
Figure 10.10 Figure 10.11
254 Management of Foot and Ankle Trauma Ch.10
Figure 10.12
Achilles Tendon Rupture-this injury is most commonly seen in males, aged 25-40
("weekend warrior"), and typically occurs in the least vascularized portion of the tendon
2-6 mm proximal to its insertion in adults >25 years of age. The Achilles tendon is surrounded
by a richly vascularized paratenon, however has no true tendon sheath (a sheath is only
present where tendon changes direction). The mechanism of acute rupture in apreviously
asymptomatic heel cord is severe traction sustained during weight bearing push-off with
the knee extended, or less commonly secondary to severe ankle dorsiflexion (downhill
skiing). Chronic degenerative tendinitis, with a long history of pain and inflammation, can
predispose to rupture near the insertion and is often associated with calcification of the
insertional fibers and a prominent posterior calcaneal step defect. Acute rupture may
effect apopping sensation, orthe sensation of being struck across the tendon. Pain, edema,
and an apropulsive gait with inability to stand on the toes with the heet elevated on the
affected side are common findings. Palpation of the tendon reveals adefect or rent in the
tendon, surrounding tenderness and induration, loss of active open chain ankle
plantarflexion, and the presence of the Thompson-Dougherty sign. The Thompson-
Dougherty test involves squeezing the ipsilateral triceps surae and noting absence of
passive ankle plantarflexion. Even asmall amount of intact tendon, despite partial rupture,
is enough to make the Thompson-Dougherty test negative. Standard radiographs display
increased soft tissue density and volume obliterating Kager's triangle. MRI reveals tendon
disruption, and may be useful when partial rupture is suspected. Conservative treatment is
indicated for cases of partial rupture, and in patients with limited function or inadequate
local tissue factors. Nonsurgical care entails application of aJones compression dressing
to splintthe ankle for 24-72 hours, followed by AK cast application with the knee slightly
flexed and the ankle in plantarflexion for up to 4 weeks, then conversion to a less
plantarflexed cast for an additional 4weeks. Additional cast or removable walking boot
therapy, in addition to physical therapy to improve flexibility is thereafter used as needed.
Functional therapy, which can be very effective, entails the use of aplantarflexed brace that
is gradually converted to a right ankle orientation of the foot to the leg, enabling weight
bearing as tolerated by the patient. Many cases of complete rupture warrant operative
repair, preferably in the acute setting with end-to-end reapproximation or other methods
that permit reconstruction. Tendon reapproximation requires the use of aBunnell or other
lateral trapping suture technique to substantially purchase longitudinal tendon fibers and
resist tension. Good results have also been obtained with functional recovery using
gradually decreasing degrees of weight bearing plantarflexion splinting. Dissection via a
255 Ch. 10 Management of Foot and Ankle Trauma
posterior incision just medial to the midline, taking care to avoid the sural nerve, and
preserving the paratenon for reapproximation over the repaired tendon is standard. A
number of repair techniques are notable, including:
Lynn Achilles tendon repair-this technique involves reapproximation ofthe 2ends re-
inforced with aflap offree plantaris graft harvested from the same wound and fanned
out over and around the repair for reinforcement. Schuberth has
recommended lengthening the tendon at the time of repair, to avoid posttraumatic
equinus and to hasten rehabilitation. V-to-Yplasty at the myotendinous junction eases
reapproximation and decreases traction across the repair.
Lindholm Achilles tendon repair-this technique of delayed primary Achilles repair
employs two proximal, longitudinal flaps from the aponeurosis that are rotated
distally and sutured to the distal segment, and themselves, to bridge a fibrotic gap.
Transfer of a portion of tibialis posterior and peroneus longus to the distal portion of
the Achilles, as well as techniques using free tendon grafts, fascia lata, and synthetic
tendon mesh have also been described.
Compartment Syndromes-increased intracompartmental pressure can cause local
muscular and neurovascular damage. The compartment is that area defined by overlying
deep muscle fascia, surrounding intermuscular septae, and/or underlying bone and
periosteum. The contents of the compartment are skeletal muscle bellies, tendons,
bursae, and neurovascular structures. A compartment syndrome develops when the
intracompartmental pressure increases to a pathological level, thereby damaging the
contents of the compartment and distal structures dependent on blood flow through the
compartment. In the foot, there are 3 main longitudinal compartments: 1) medial
compartment-containing abductor hallucis and FHB; 2) superficial compartment-which
is plantar central and contains FOB; and 3) lateral-which contains abductor digiti minimi
and flexor digiti minimi brevis. The forefoot also houses 5 smaller compartments:
4 intermetatarsal Hnterosseous) spaces containing the interossei; and the adductor
hallucis compartment plantarly. The hindfoot houses a single deep compartment, referred
to as the calcanean compartment, which contains the quadratus plantae. In the leg, the
peroneal, anterior, and posterior deep and superficial compartments are of concern
(Fig. 10-13). Compartment pressure increases due to enlargement of intracompartmental
volume, or external pressure that causes a decrease in the compartment volume. The nor-
mal lower extremity intracompartmental pressure, in the normotensive patient, is 4 4
mmHg. During exercise, the intra compartmental pressure may exceed 50 mmHg.
Immediately post-exercise, the pressure should be <30 mmHg; and within 5 minutes after
cessation of exercise, the pressure should normalize. In the normotensive patient,
compartment pressures approaching 100 mm Hg are necessary to occlude arterial
pulsatile flow. Any condition resulting in sustained intracompartmental pressure of ;;:30
mmHg, in a patient who presents 28 hours after injury or the inciting event, and who
demonstrates clinical signs and symptoms, should undergo emergency fasciotomy to
alleviate compartment syndrome. Signs and symptoms include allodynia, exquisite pain,
paresthesia, and pulselessness (the 3 "P's"). Soft tissue and osseous injury may be
present, along with edema, pallor or cyanosis, decreased skin temperature, and
sensorimotor deficit. The neurological and vascular deficits must be documented prior to
256 Management of Foot and Ankle Trauma Ch.10
Figure 10.13
surgical intervention. Distal arterial pulsation may be appreciated even when compartment
syndrome causes pain and paresthesia, as the initial vascular compromise occurs at the
microcirculatory (arteriolar) level distally. Predisposing injuries include comminuted
fracture or crush defect, contusion, Volkmann's ischemic contracture (post-ischemia!.
intracompartmental hemorrhage or hematoma, burn wounds, decubitus stasis secondary
to drug overdose and coma, circular bandages and/or casting, abscess and tumor.
Diagnosis is confirmed via transcutaneous wick catheter measurement of the
intracompartmental pressure, with values of mmHg. Pressure measurements <10 mmHg
are indicative of neuropraxia (pulses will usually be palpable). Values of 10-20 mmHg should
be remeasured 30-60 minutes after observation, and administration of analgesic, systemic
corticosteroid (methylprednisolone or prednisone), and rest.lfthe condition is thoughtto be
related to circumferential bandaging or casting, remeasure the compartment pressure
30-60 minutes after cast and bandage removal. Fasciotomy is performed after sterile prep,
and may be done in the emergency room or OR, depending upon the merits of the specific
case. Compartment decompression in the foot is achieved using 2 dorsal longitudinal
incisions located overthe second and fourth metatarsals. Dissection is carried through the
deep fascia to periosteum, then medially and laterally into the adjacent intermetatarsal
spaces where the interosseous musculature is reflected from the corresponding metatarsal.
In asimilarfashion, other compartments in the foot and leg are opened via fasciotomy. The
wounds are then packed open and maintained with local care for 3-5 days, keeping the
extremity at bed level with slight knee flexion, after which delayed primary closure or skin
grafting is undertaken.
Ch.10 Management of Foot and Ankle Trauma 257
FRACTURES
The principles of fracture management include:
Reduction and Immobilization-fractures are described according to their location and
orientation within the specific bone. Fractures are caused by pathological bending,
twisting, and shearing forces that are applied either directly (direct blow) or indirectly
(twisting). Fractures are either closed or open injuries. Radiographic inspection requires at
least two or three (preferably). or more views, as well as comparison views of the
contralateral extremity in questionable cases involving sesamoids, growth plates, or
suspected supernumerary bones. Incomplete fractures, wherein a portion of the bone's
cortex remains intact, are termed greenstick fractures and generally occur secondary to
flexural deformation of a long bone. Similarly, a stress fracture results in bending without
overt radiographic fragment separation. A bone scan can be useful if diagnosis is in
question. Incomplete fractures are diagnosed primarily by clinical examination, and with
subsequent radiographic evidence of secondary bone callus. Complete fractures can be
transverse, oblique, spiral, and comminuted, with fracture stability and management
varying with orientation. Fracture stability, in descending order, is as follows:
transverse> oblique> spiral> comminuted
Transverse and oblique fractures may be amenable to closed reduction and
immobilization, whereas spiral and comminuted patterns are extremely difficult to
adequately reduce and maintain in a closed fashion. When a fracture violates a joint
surface, open reduction and stabilization is most often the best treatment option. Growth
plate injuries and open fractures deserve special consideration.
Fracture repair is initiated with closed reduction and immobilization, regardless of
whether the injury is open or closed. Closed reduction, as described by Charnley, entails the
following sequential maneuvers: 1) increase the deformity; 2) distract; 3) reverse the
deformity and realign; and 4) maintain correction with an immobilizing splint (Fig. 10-14).
These general rules apply to all fractures, and may be used as definitive treatment in
amenable injuries, or as a temporary intervention to improve neurovascular status in
preparation for open reduction and fixation in the OR. Closed reduction can be impeded by
soft tissue interposition, such as the tibialis posterior tendon at the medial malleolus.
Maintenance of the reduction with acast or brace is indicated when closed reduction and
immobilization are the mainstays of treatment If open reduction and internal fixation (ORIF)
caval t. II
C'711
II)
:;:/
Figure 10.14
-iui
Convex
258 Management of Foot and Ankle Trauma Ch.l0
or use of external fixation is employed, the brace may be removable or nothing more than
a posterior, sugar tong (medial and lateral stirrup), or anterior splint. The usual
fracture-healing phase lasts at least 68 weeks, and protection should be maintained
during this period. As a rule, the bone should be stabilized with immobilization extended to
one joint above the fractured ossicle. If internal or external forms of skeletal fixation are
used, the "one joint above" rule becomes less important. Fractures sustained distal to the
MTPJs are usually satisfactorily stabilized with a rigid sole trauma/surgical shoe (such as
the Darco shoe). Stress fractures of the metatarsals respond well to a gel-cast and
surgical shoe, and digital fractures can be managed with gauze dressings and a surgical
shoe. Acute metatarsal fracture is best treated with below-the-knee (BK) immobilization.
Only very stable fractures, due either to fracture pattern, location, or surgical fixation, can
sustain weight bearing during the healing phase (compare the fracture to surgical
osteotomy design and fixation to help decide how to protect during healing). For this
reason, non-weight bearing immobilization is the general rule for foot and ankle fractures.
Ambulation with crutches, a walker, or wheel chair or another protective device are
standard. Follow-up radiographic inspection is required after initial reduction, and perhaps
a few days later (initial follow-up), based on clinical progress, to assure maintenance
of alignment, then at about 68 weeks, or any time as indicated based on clinical signs
and symptoms.
Open Fracture Management-open fractures may be associated with severe limb and/or
life threatening injuries. Locally, the extent of soft tissue injury must be evaluated. Open
fractures convey a60-70% incidence of bacterial contamination and growth atthetime of
initial inspection. Open fractures that have gone without treatment for 68 hours are
considered infected. The Gustilo classification of open fractures is depicted in Table 10-1.
TABLE 10-1. THE GUSTILO CLASSIFICATION OF OPEN FRACTURES.
---..
Type Description of the fracture
I Fracture with open wound <1 cm, clean, minimal soft tissue necrosis, and the
fracture is usually transverse or short oblique with minimal or no comminution
II Fracture with open wound >1 cm, clean, minimal soft tissue necrosis, and
fracture is usually transverse or short oblique with minimal or no comminution,
commonly associated with crush injuries sustained in motor vehicle accidents,
farm or industrial machinery mishaps, and gunshotwounds
III Fracture with extensive open wound, contamination, and/or necrosis of skin,
muscle, neurovascular and surrounding soft tissues; and the fracture is often
comminuted
The principles of open fracture treatment follow those stated previously for wound
debridement, tetanus and antibiotic prophylaxis, in addition to skeletal stabilization.
Appropriate antibiotic therapy entails initial administration of cefazolin 1 or 2 grams IV,
followed by 1 gm IVPB Q 8 hr thereafter until definitive cultures are available, depending
upon the specifics of the case. It the injury occurred in a farm or similar tetanus-prone
environment, then cover for Clostridia by administering aqueous penicillinG 10-20 million
units IV daily in divided doses every 6 hours. Alter antibiotic therapy based on allergy
history, and other systemic factors. Use antibiotics for at least 3 days, and continue
therapy for 3 additional days in the noninfected wound if management warrants delayed
Ch.10 Management of Foot and Ankle Trauma 259
primary closure, secondary intention closure, ORIF or in the event that internal or external
fixations require alteration. Skeletal stabilization in an anatomic alignment enhances
tissue viability, wound healing, and diminishes the risk of infection. Initial treatment varies
with fracture stability and neurovascular status, and focuses on manipulative (closed)
reduction as described above. Temporary andlor permanent fixation can be achieved with
K-wires and Steinmann pins, external fixation, and interfragmental compression screws as
deemed indicated based on the specific merits of each fracture. It is preferable to minimize
periosteal reflection. If bone grafting is indicated, this can be done immediately in aType I
open fracture, however is best performed on adelayed basis after initial stabilization of the
wound. In Type II open fractures, the bone graft is best applied at the time of delayed
primary closure when there is no evidence of infection. Application of an external fixator
obviates the need to effect stability with a bone graft at the time of initial intervention. If
infection does occur after graft transplantation, the autogenous graft may still take. Gustilo
recommended autogenous cancellous bone grafting in type III open fractures at
approximately 3 months after initial therapy, when reactive bone callus formation has
diminished. The decision to close the wound is based on factors previously described.
Digital Fractures and Dislocations-digital fractures usually occur secondary to dropping
aheavy object on the toe, which usually damages the distal phalanx; or by stubbing the toe
into a rigid object, which usually fractures the distal phalanx of the hallux or the proximal
phalanx of a lesser toe. Hyperplantarflexion injuries often result in IPJ dorsal avulsion
fracture. The fifth toe is the most commonly fractured digit, followed by the hallux and then
the intermediate toes. Intermediate phalanx fractures are rare in the lesser toes. The
medial oblique projection is useful for evaluating the hallux, as is isolation of the toe by
elevating it on foam or similar material to eliminate superimposition of adjacent digits.
Digital fractures should be stabilized with gauze bandaging, stabilizing the injured toels to
adjacent healthy digits (buddy splint), and a surgical shoe, much as would be used
following digital arthroplasty. Displaced or unstable fragments that are large enough,
particularly if intra-articular, can be stabilized via ORIF with K-wires or small lag screws.
Distal phalangeal tuft fractures, particularly if comminuted, may require surgical nail plate
avulsion, repair of any nail bed defect, and excision of displaced fragments. Distal
phalangeal fractures that heal with hypertrophy may require subsequent reduction of
prominent bone to eliminate subungual exostosis. Proximal phalangeal base fractures,
particularly of the hallux, can predispose to digital floating, and transverse plane
misalignment. If hallux abductus develops, consideration should be given to surgical
treatment. Hallux interphalangeal joint (HIPJ) dislocation is the essential differential
diagnosis in cases of suspected phalangeal fracture, as it can also result from the same
pathological force. In the lesser toes, IPJ dislocation rarely involves the DIPJ, and most
commonly affects the PI PJ of the fifth toe. Treatment is closed reduction and buddy splint-
ing usually, unless the reduction is unstable or prevented by protrusion of the phalanx
through the IPJ capsule. In this case, open reduction and capsular repair are required.
Metatarsophalangeal Joint Fractures and Dislocations-turf toe is atraumatic condition
of the hallux and first MTPJ, wherein repetitive hyperdorsiflexion, hyperptantarflexion,
hyperadduction, or hyperabduction results in MTPJ sprain without gross change in joint
alignment. The injury usually affects athletes, in particular those playing on artificial turf
surfaces, although tennis and basketball players can also be affected. Clinically the joint,
as well as the HIPJ, appears swollen, indurated, and tenderto palpation and motion. Often
-------
260 ManagementofFootandAnkleTrauma Ch.lO
thereisanassociatedsubungualhematomaand/ordigitalecchymosis.Radiographsshould
be obtained to rule out dislocation, osteochondral or avulsion fracture, or sesamoid
fracture. TreatmentconsistsofPRICEwith use ofagauze bandage and surgical shoe.
Gradualresumptionofstrenuousactivityisinitiatedin7-10days.andathleticshoesshould
be evaluated forproperfitOrthosesmaybe helpful. Oral anti-inflammatoryagents are
generallyindicated.andcorticosteroidinjectionshouldbe avoided.
FirstMTPJ dislocation-thisoccurssecondaryto hyperdorsiflexionforce. and is
categorizedasdepictedinTable 10-2.
TABLE10-2.CLASSIACATIONOFARSTMETATARSOPHALANGEALJOINTDISLOCATION.
Type Description
I Atransversecapsularruptureplantartothemetatarsalhead/neckwiththe
proximal phalanx, plantarcapsule, and sesamoids displaced dorsally on
metatarsalhead.Theretrogradeplantardirectedforceof thephalanxdrives
the metatarsalheadin aplantardirection,andthe HIPJ becomesfixed in
plantarflexion.Thisinjuryisusuallynotamenabletoclosedreduction.
II A Same as Type Iexceptthatratherthan the entire plantar capsule and
sesamoidapparatusdislocating distallyand dorsally,the intersesamoidal
ligamentrupturesandthesesamoidssubluxtoeachsideofthemetatarsal
head. Radiographs readilyshowthe sesamoids medial and lateraltothe
metatarsalhead.Thisinjuryisamenabletoclosedreduction,howeverthe
softtissuedisruptionshouldberepairedwithsuture.
B Thisinjuryalso displaysthesesamoids displacedmedial andlateraltothe
metatarsal head. however rather than rupture of the intersesamoidal
ligament, there is avulsion fracture of one of the sesamoids. Closed
reductionofthefirstMTPJdislocationentailsMayoblockofthefirstray,then
distraction, followed by pushing the proximal phalanx into acongruous
relationwiththemetatarsalhead.Correctionismaintainedwith aslipperor
BK cast for 3-4 weeks,then asurgical shoe for an additional 3weeks.
Resistantdeformityrequiresoperative repair.TheType liBinjuryshould be
casted BK for6weeks non-weightbearing. lateterm sequelae include
sesamoidnonunionand/orsesamoiditis,andsurgicalexcisionofthepainful
ossiclemaybenecessary.
Lesser MTPJ dislocation-this occurslessoftenthan doesfirstMTPJ dislocation,
and dorsal dislocation ofthe phalanxon themetatarsal head isthe usual pattern.
ClosedreductionissimilartothatperformedforTypeIfirstMTPJdislocations.
Osteochondral fractures ofthe first MTPJ-these canaffecteitherthephalanxbaseor
metatarsalhead.Phalangeal osteochondralfracturesusuallyoccurduetostubbing
withforcedtransverseplanemotionthatavulsestheintrinsicattachmentsto thebase.
Metatarsalhead osteochondralfracturesusuallyoccurdueto hyperdorsiflexionthat
causesimpactionwith high shearstrainatthe dorsalaspectofthe head.Treatment
entailsclosedreductionand6weeksofimmobilizationinaslipperorbootcastforsmall
fragments,orORIFandimmobilizationfor6weeksin acastforlargerfragments.Very
smallfragments can betreatedmuchlikeadislocation,withearlierreturntoweight
261 Ch.10 Management of Foot and Ankle Trauma
bearing and motion. When the joint is opened, loose or torn cartilage should be
remodeled and the subchondral cortical bone fenestrated with a 0.035" K-wire. Late
term sequelae include post-traumatic DJD, and arthrodesis or multicomponent
endoprosthesis may be indicated.
Sesamoid fractures-these can occur after afall from aheight wherein direct dorsally
directed force pushes the sesamoids into the plantar surface of the metatarsal head
while the hallux forcefully dorsiflexes. Cumulative microtrauma can also cause
sesamoidal stress fracture, and is associated with dancing, basketball, tennis and
other strenuous activities. The condition is often misdiagnosed and mismanaged. The
tibial sesamoid is more commonly fractured, and rarely are both the tibial and fibular
fractured in the same joint. Moreover, bilateral sesamoid fractures are rare.
Symptoms include pain upon direct palpation or first MTPJ range of motion, in
particular with dorsiflexion. The differential diagnosis is extensive, and includes:
Joplin's neuroma, sesamoiditis, osteochondritis dissecans of the sesamoid,
osteochondrosis of the sesamoid, bi- or multipartite sesamoid DJD or rupture, turf toe,
HAV with eroded crista, and prominent or hypertrophic sesamoid with plantarflexed
first ray painful plantar callus. Radiographic evaluation can be difficult particularly
when a bipartite sesamoid is present 75% of which occur unilaterally. Medial and
lateral oblique, sesamoidal axial views, and contralateral comparison views are often
helpful. When in doubt order abone scan or MRI. Treatment entails aslipper or boot
cast or immobilizing splint and non-weight bearing for 6-8 weeks, followed by
transition back to asneaker using asurgical shoe until asymptomatic. The prognosis
for complete healing is guarded, and primary as well as delayed excision of the
fracture fragment(s) should be considered. Remember that sesamoidectomy, even
partial. conveys the risk of valgus orvarus deformity for the tibial and fibular ossicles,
respectively, especially in cases involving a round metatarsal head. Appropriate
muscle-tendon balancing should be performed whenever sesamoidectomy is
performed. Removal of both sesamoids will decrease intrinsic muscle strength and
hallux purchase, causing a hallux hammertoe or cock-up hallux. Prophylactic fusion
ofthe HIP,I should be performed whenever both sesamoids are excised.
Metatarsal Fractures-the principles for management of metatarsal fractures, whether of
the first or lesser metatarsals, at the head, shaft or base, are the same as those stated
previously in the general management offracture discussion. Afew points of interest should
be noted. It is importantto try and restore the weight bearing balance ofthe metatarsus, and
attention should be paid to length and sagittal plane relations. Transverse and short oblique
metatarsal fractures, particularly of the shaft, are amenable to closed reduction and
immobilization, and difficult lesions can be pinned either percutaneously or via open
dissection. Multiple metatarsal fractures often display spontaneous reduction ofthose of
the intermediate rays upon ORIF of either or both of the first and fifth metatarsals, and
fixation of the intermediate metatarsals can be adequately achieved with asingle K-wire or
no fixation other than casting. This is an example of the vassal rule. A number of different
types of metatarsal fractures can be incurred, including:
Fifth metatarsal fractures-these are very common injuries. Keep in mind that the
apophysis of the fifth metatarsal styloid appears at 9-14 years and fuses at 12-15 years
of age. The physis is oriented almost parallel to the long axis of the fifth metatarsal
262 Management of Foot and Ankle Trauma Ch.10
shaft The accessory ossicle, os Vesalianum, appears in the tendon of peroneus
brevis near the base. Of particular interest is the Jones fracture (Fig 10-15), which is
caused by medial or lateral cutting or pivoting movement that produces atransverse
fracture distal to the junction of the fourth and fifth metatarsals. This is actually a
proximal diaphyseal fracture that is not produced by inversion of the foot and ankle.
The Jones fracture is notorious for nonunion, and meticulous fracture management is
crucial. In the patient without great physical demands, closed reduction and
immobilization for 6-8 week in a BK non-weight bearing cast is indicated. In the
athlete or individual that participates in strenuous daily activity, ORIF and BK
non-weight bearing cast 5-6 weeks followed by weight-bearing castfor an additional
2-3 weeks is indicated. If delayed union is suspected, maintain non-weight bearing
and immobilization and add electrical bone growth stimulation (EBGS). If a nonunion
develops, repair with autogenous cancellous bone graft, electrical stimulation, and
cast non-weight bearing. The base of the fifth metatarsal can also fracture into the
metatarsal-cuboid joint secondary to forced inversion and traction applied through
the tendon of peroneus brevis or the lateral slip of the plantar fascia. The result is an
avulsion fracture that enters the tarsometatarsal joint (TMJ). If the fracture is
displaced, the ORIF followed by weight- bearing BK cast for 6weeks. If the fracture is
nondisplaced, then closed reduction and immobilize in a non-weight bearing castfor
6weeks. The fifth metatarsal base can also fracture atthe styloid process (Fig 10-16),
which is an extra-articular fra cture caused by the same force described above forthe
intra-articular fracture. Treatment is the same as that described above for the
articular fracture at the fifth metatarsal base.
Metatarsal stress fracture--this is also known as a march or fatigue fracture, and
develops secondary to cumulative that surpasses the bone's ability to respond to
repetitive load. This is frequently observed when a person initiates a new exercise
program, undergoes basic training in the military (march fracture), suffers with a
specific biomechanical abnormality wherein there is loss of adjacent metatarsal
support (hypermobile first ray dumping force on the second ray, or following adjacent
metatarsal fracture or osteotomy). The onset of pain is usually gradual, but
Figure 10.15
Figure 10.16
263 Ch.l0 Management of Foot and Ankle Trauma
exacerbated by recent increased activity. The pain is localized to the affected
metatarsal, with associated edema and local heat Stress fracture usually localizes to
the metatarsal neck, and most commonly involves one of the intenmediate rays. The
differential diagnosis includes neuroma, MTPJ enthesitis, arthritis, and extensor
tenosynovitis. Charcot fractures, pathological fracture, and osteoporosis should also
be considered. Radiographic findings initially may reveal asmall cortical break at site
of maximum clinical tenderness. Periosteal reaction usually develops at the stress
fracture site, and may become evident at about 10 days or longer from onset of pain.
Repeat radiographs at 2-3 weeks after the onset of pain may be needed to confirm
diagnosis. A bone scan or MRI should be obtained if standard films are equivocal.
Treatment of metatarsal stress fracture entails a gel-cast and surgical shoe or a
removable cast-boot for 3-5 weeks, and orthoses may be useful to address
biomechanical abnormalities thereafter.
Lisfranc Fracture Dislocation-this injury constitutes 1% of all reported fractures,
however the diagnosis is missed in almost 20% of cases. Anatomical considerations
include the "keystone" nature of the second metatarsal base in the intercuneiform recess,
which provides asignificant amount of stability to the midfoot complex. The tarsometatarsal
joint (TMJ) is bound together by aseries of transverse dorsal and plantar ligaments, as well
as intermetatarsalligaments. There is a distinct absence of an intermetatarsalligament
between the first and second metatarsals. The plantar ligaments are thicker, and dorsal
displacement is most common. The ligament attaching the medial cuneiform to the first
metatarsal is the largest ligament at this level. The most important ligament of the TMJ is
Lisfranc's interosseous ligament, which attaches the base of the second metatarsal
medially to the lateral aspect of first cuneiform. Lisfranc's ligament is often involved in
avulsion fracture of the second metatarsal base. The Hardcastle classification (also know
as Queno and Kuss) is the standard system for identifying TMJ fracture/dislocations
(Fig. 10-11), and categorizes these injuries as depicted in Table 10-3.
TABLE 10-3. THE HARDCASTlE CLASSIACATION OF USFRANC FRACTURE DISLOCATIONS.
A
Type
(total. homolateral
dislocation)
B (partial
dislocation)
C (divergent)
Description of injury
The most common TMJ fracture/dislocation, it
displays disruption of the entire TMJ in the sagittal or
transverse plane. This injury usually involves lateral
displacement of all of the metatarsal
1. Medial displacement of the first metatarsal alone
or with metatarsals 2, 3, 4, not 5
2. Lateral displacement of one or more of the lesser
metatarsals (not the first metatarsal)
Displays the first metatarsal dislocated medially and
the lesser metatarsals either partially or totally dislocated
laterally in the sagittal andlortransverse planes
Although the Hardcastle classification is most commonly used, Wilson also classified
Lisfranc joint fracture/dislocations, as depicted in Table 10-4.
264 Management of Foot and Ankle Trauma Ch.10
Type A
Lateral dislocation
Figure 10.17
Medial
dislocation
TypeB
2
Partial Incongruity
TypeB1
TABLE 10-4. THE WILSON CLASSIFICATION OF LlSFRANC FRACTURE DISLOCATIONS.
Class Stage
Plantar-flexion-
supination-most common I
II
Plantarflexion pronation I
Description of the fracture
Dorsolateral dislocation of metatarsals 2-5
Dorsolateral dislocation of metatarsals 1-5
Medial dislocation of first metatarsal
" Medial dislocation offirst metatarsal, dorsolateral
dislocation of metatarsals 2-5
Plantarflexion Dorsal dislocation of second metatarsal base and/or
fracture dislocation base of first metatarsal
The mechanism of TMJ injury is usually a crushing force applied to the forefoot with
the ankle plantarflexed. The second metatarsal must be dislocated first, either by
transverse base fracture or medial avulsion by Lisfranc's ligament, in order to disrupt the
TMJ. Clinical findings include localized signs and symptoms of fracture/dislocation, and it
is critical to assess the neurovascular status to the forefoot The foot may appear grossly
shorter than the contralateral limb. Radiographs can be difficult to assess, and attention
should be directed at the first metatarsocuneiform interfaces, as well as the base of the
second metatarsal. Dne should also look for a compression fracture of the cuboid.
Transverse and sagittal plane stress views can add information, and the CT scan has
Ch.10 ManagementofFootand AnkleTrauma 265
becomeamainstayofdiagnosticaccuracyin regardtothisinjury.Treatmentbeginswith
attemptedclosedreductionandimmobilization,ifindicated.Distaltractioncanbeachieved
bysuspendingthefootabovethetablewithChinesefingertrapsuntiladequatesofttissue
relaxation ensues. Counterweightsstrapped aroundthe ankle can be used to enhance
distraction. An external fixation frame can also be used to effect distraction and
stabilization.Attentionisdirectedattryingtorelocatethesecondmetatarsalbaseintothe
intercuneiform recess,then to reduction ofthe firstmetatarsal-medial cuneiform joint
depending on the fracture/dislocation pattern. Percutaneous pin stabilization may be
attemptedafterreduction,howeverthisisnotoriouslydifficultIfclosed reductionfails,it
may be due to tibialisanterioror peroneuslongusinterposition,ordueto the avulsion
fragmentofthe second metatarsal base. ORIFmaybe performed via 3dorsalincisions:
1) dorsomedial first met-cuneiform. 2) between second and third metatarsals and
correspondingcuneiforms.and3)betweenfourthandfifthmetatarsalsandthecuboid.The
firstmetatarsalisgenerallyfixedfirst,followed bythe remaining metatarsalsfrom medial
tolateral.Pin stabilizationisrecommendedasfollows:
TypeA-1wirestabilizingfirstmetatarsal-cuneiformandasecondstabilizingthefifth
metatarsal-cuboidjoints.
TypeB{medialtypef--.2pinsstabilizingthefirstmetatarsal-cuneiform.
Type C-2pinsmedialandonelateral.
ABKcastisthen usedfor8-12weeks.thefirst6-8weeksbeingnon-weightbearing.
Thepinsareremovedafter6-8weeks.
Calcaneal Fractures-this injuryismostcommonlyobservedinmenaged35-45years,and
themaletofemaleratiois5:1.Calcanealfracturesareassociatedwithspinalfractures20%
oftime,withT12-l2themostcommonvertebralrangeand L 1themostcommon vertebra
fractured.Themostcommonmechanismisafallfromaheight,followedbymotorvehicle
accident.Clinicalfindings include Mondor'ssign,which is plantarecchymosisextending
fromthe heel intothe plantarvault.The heelalso appearswide and shortened,andthe
patientisantalgicandunabletobearweightontheinjuredfootBohler'sangleismadeby
theintersectionofalineextendingfromtheposterosuperiorprocessof thecalcaneustothe
posteriormarginoftheposteriorfacetoftheSTJ, andthelineextendingfromthe posterior
margin ofthe posteriorfacetofthe STJ tothetip ofthe anteriorbeakofthe calcaneus
(Fig. 10-18). Bohler'sangleis usually25-40,and is depressedoreven negativewhenthe
posterior facet is depressed by the talus into the body of the calcaneus in ajoint
depressionfracture.Radiographicsignsincludedisruptionofthecalcaneocuboidjointon
theAPview;depressionoftheposteriorfacetoftheSTJand Bohler'sangleonthelateral
view;disruptionoftheposteriorfacetandwideningof thecalcaneuswithlateralwallblow
outonthecalcanealaxialview;andfractureoftheanteriorprocessonthemedialoblique
view. Radiographs ofthe ankle,legs, and vertebral column mayalso be indicated,and a
CT scan ofthe hindfootcan be very useful priorto operative intervention. The Rowe
classification(Table10-5)dealsprimarilywithextra-articularcalcanealfractures(Fig.10-19).
266 Management of Foot and Ankle Trauma
Lateral talar process
Figure 10.18
la Ib
~
~
Ie
~
.'- Break
~
l I a
~
fracture
, lib
Avulsion
II" fracture
Figure 10.19
Gissane's crucial angle
~
III
Gf),v
v
Ch.10
267 Ch.10 Management of Foot and Ankle Trauma
TABLE 10-5. THE ROWE CLASSIFICATION OF CALCANEAL FRACTURES.
Type Description
I A Fracture of the calcaneal tuberosity
sustained in afall with the heel everted
or inverted; can result in splaying and
widening that may interfere with the
peroneal tendons
B Fracture of sustentaculum tali, sustained
from fall with twist on a supinated foot
tenderness upon passive or active
flexion and extension of the hallux due
to FHL; axial calcaneal X-ray is the
best view.
C Fracture of anterior process (most
common Type I fracture); only cal-
caneal fracture where females have
higher incidence; this is an avulsion in-
jury of bifurcate ligament force is
plantarflexion on a supinated foot;
seen clearly on lateral or medial
oblique views; may need tomograms
to visualize ifthe fragment is small
II A Beak or avulsion fracture of calcaneus
that does not affect Achilles insertion
B Avulsion fracture with pull off at
Achilles attachment
III Fracture of body without involvement of
STJ (most common extra-articular frac-
ture); results from fall with edge of talus
going into calcaneus; lateral X-ray and
axial views most helpful; axial view deter-
mines STJ involvement
IV Fracture of body of calcaneus involving
STJ; this is actually an articular fracture,
however fractures in the Rowe
classification are still considered as
primarily extra-articular
V Central depression fracture with a
degree of comminution (also, an
articular fracture)
Treatment
Closed reduction immobilization
with BK cast, 6 weeks, weight
bearing if non-displaced. ORIF if
displaced or unstable
Closed reduction immobilization
with BK cast 6 weeks if non-
displaced. ORIF if displaced or
unstable
Closed reduction and immobiliza-
tion with BK walking cast for
6 weeks. Excise or ORIF the
fragment if symptoms persist
Non-weight bearing BK cast for
about6weeks in plantarflexion if
non-displaced. Must reduce if
large and/or displaced; percuta-
neous pin may work, or ORIF if
unstable
AK Non-weight bearing cast with
knee flexed. ORIF if displaced or
unstable
Closed reduction, percutaneous
pinning. or ORIF
268 Management of Foot and Ankle Trauma Ch.10
The Essex-Lopresti classification (Table 10-6) describes intra-articular calcaneal
fractures (Fig. 10-20). The Essex-Lopresti system of intra-articular fractures describes
approximately 75% of all calcaneal fractures that usually result from along fall from ahigh
place. When the victim hits the ground feet first, the talus is driven down into the
calcaneus, crushing the posterior facet into the body of the os calcis and splitting the bone
like awedge. Essex-Lopresti Types A and Bare differentiated bythe secondary fracture line
and the shape of the resultantfragments.
Tongue Type JOint depression type
Figure 10.20
269 Ch.l0 ManagementofFootandAnkleTrauma
TABLE10-6.THEESSEX-LOPRESTICLASSIFICATION OFCALCANEALFRACTURES.
Type
A(tonguefracture)
B(jointdepression)
Primaryfractureline
Coursesfromsuperiorto
inferior,extendingfrom
Gissane'scriticalangleat
thejunctionoftheposterior
facetandthecalcaneal
sulcus,totheplantar
aspectofthecalcaneus
The sameasdescribed
aboveforthetongue-
typefracture
Secondaryfractureline
Propagatesfromtheprimary,
posteriorlytoexitthe
posteriorcortex,usually
proximaltotheAchilles
insertion
Surroundstheposteriorfacet
thatisdrivenlikeacolumninto
thecancellousboneofthebodyof
thecalcaneus,explodingthe
bonemediallyandlaterally
intocomminutedfragments
The Sanders classification of calcaneal fractures is probablythe most useful in
regardto directingsurgical intervention(Table 10-7).To classifythefracture usingthis
system,thefrontalplane CTscan is used,andthe posteriorfacetofthe subtalarjointis
dividedinto3equal segments,from.lateraltomedial,withthefinal line collinearwiththe
verticalmarginofthesustentaculumtali.TheTypeIfracturearenondisplacedandinvolve
afractureofeitherthelateral.central,ormedialsegmentoftheposteriorfacetFractures
localizedtothemedialsegmentaremostdifficulttovisualizeandreduceprimarily.TypeII
fractures involve 2-part split fracture of the posterior facet, and Type III injuries
involve3-partsplitfractureswith depression ofthe posteriorfacetintothe bodyofthe
calcaneus.Type IVfracturesinvolvesevere comminution ofthe posteriorfacetandthe
bodyofthe calcaneus.
TABLE10-7.THESANDERSCLASSIFICATION OFCALCANEALFRACTURES.
Type DescriptionofthefrontalplaneCTappearanceofthefracture
I Nondisplacedfractureoftheposteriorfacet
II 2-part(split)displacedfracture
III 3-part(split)displacedfracturewithjointdepression
IV Severelycomminutedfracturewithjointdepression
Mechanicallyspeaking,thecalcanealtuberosityissituatedlateraltothecenterofthe
talus.Whenaverticalcompressiveforceisapplied,2primaryfracturefragmentsdevelop:
')superomedial or sustentacularfragment (sustentaculum tali), and 2) the tuberosity
fragmentthatcontainsthelateral1/3to 1/2oftheposteriorfacet.Ifthe pathologicalforce
continues,thetalusandsustentaculumtaliaredrivenplantarand medial. Iftheforce still
continues,thenthe posterolateraledgeofthetalusisdrivenintothesuperolateralaspect
oftheposteriorfacet,whichissupportedbycancellousbonethatiscrushedandimpacted.
A lateral wall blowout fracture may also occur, with possible extension into the
calcaneocuboid joint. Palmer's three constant components of intra-articularfracture
include: 1)verticalshearingfracture,2)fracture ofthe lateral cortex,and,3) depression
270 ManagementofFootand AnkleTrauma Ch. 10
fracture ofthe posterolateral STJ. Pedal deformityrelatedto calcanealjointdepression
fracture includes: increased calcaneal width making shoe wear difficult, decreased
calcanealheightandlengthadverselyaffectinglimblengthandgait,intra-articular fracture
oftheSTJwithresultantDJD,andsuralnerveandperonealtendonentrapmentalongthe
lateral wall ofthe calcaneus. Initial managementinvolves neurovascularassessment,
PRICE, and attempted closed reduction and immobilization if indicated. Simple
immobilization,oftencombinedwithearlyweightbearing,eliminatessurgicalrisksandmay
be indicatedin certain patientswho are lessactive and perhaps athigh riskforsurgical
complication.Limitedweightbearingafter1week,progressingtofullweightbearingat6-
12weekscanbeundertaken.Essex-Loprestidescribedmanipulationwithskeletalfixation
using apinthatentersthe bodyofthe calcaneusfromthe posterioraspectthatisthen
pulledinaplantardirectiontotryandlifttheposteriorfacetoutofthebodyofthecalcaneus.
Thiscanalsobeundertakenwithmorethan1pin.Thepinorpinsis/arethensecuredinthe
surroundingplasterthatisappliedAKwiththekneeflexed.Thismethodisapplicableonly
intonguefractures, and isnotused much because ofinaccurate STJ realignment, and
subcutaneouscompromiseatthepintract.Palmerdescribedaclamp(Palmerclamp)used
tosqueezethe medialandlateralcorticestogether,howeverthisdidverylittleto improve
the STJ. Palmeralso described ORIFwith elevation ofthe posteriorfacetunderdirect
visualization and manipulation, followed by packing beneath the raised facet with
autogenousbonegraft.followedbypinstabilizationandBKnon-weightbearingcastfor12
weeks. Galie described earlytriple arthrodesis,and indeedthisis often alastresortfor
patientswhohavedevelopedpost-traumaticarthrosisfollowingfracture.If fractureblisters
arepresent,thensurgicalinterventionshouldbepostponeduntiltheskinbarrierishealthy.
Operativeintervention isideallyperformed withinthefirst2-6hoursofinjury.The Zwipp
incisionpreservesthe peronealtendons and the suralnerve in an intactsofttissueflap.
ThePodiatryInstitutetechniqueentailsalateralapproachwithsectioningorpreservation
ofthe peronealtendons,reconstructionofthe posteriorfacetwithsupportingbone graft,
andacombinationofbuttressplateandlagscrewandcerclagewirefixation,asnecessary.
Anumberofspecialtylocking and non-locking plates are availableforreconstruction of
the fractured calcaneus. Complications of calcaneal fracture, and its repair, include
post-traumatic STJ arthritis, ankle jointarthritis,tenosynovitisofperoneals,plantarheel
painduetodiminishedcushioningeffectoffatpad,suralorPTnerveentrapment,shuffling
gaitwith shortened stride, and stiffness. Late salvage ofarthrosisfollowing calcaneal
fracture often entailstalocalcanealfusion,triplearthrodesis,orextra-articularbone bloc
distractionarthrodesistorestoretheheightoftheheel.
Talar Neck Fractures-anatomically,2/3ofthetalus is covered with articularcartilage,
therefore mostfractures ofthetalusare intra-articular.Nomusclesortendons originate
fromorinsertintothetalus.Theextendedneckwithitstenuousbloodsupplyisvulnerable
toinjury.Thebloodsupplytothetalusentails:
Body-artery oftarsalcanalfromtheposteriortibialanddeltoidbranch.
Head and neck-artery oftarsalsinusfromperforatingperonealandDP.
Posterior talus-calcaneal branchesofPT.
Avascularnecrosis(AVN) is likelytooccurwhen 2/3 ofthevascularchannels are
disrupted. Hawkins notedthatittakes until6-8weeks afterthe injuryto recognizethe
presence of AVN, and it may not appear until 1-4 months have passed. Signs and
271 Ch.10 Management of Foot and Ankle Trauma
symptoms of talar AVN include intractable pain, relative radiographic sclerosis, or opacity
of the dead bone, best observed on the AP view of the ankle. Hawkins noted the presence
of subchondral bone revascularization as radiolucency in the dome of the talus on the AP
view, and this is referred to as Hawkins' sign and is indicative of healing. The treatment of
AVN is non-weight bearing in BK cast for 6-8 months until revascularization occurs, with
electrical bone growth stimulation. The Hawkins classification (Table 10-8) of talar neck
fractures can be useful in regard to anticipating the development of avascular necrosis
(Fig. 10-21).
TABLE 10-8. THE HAWKINS CLASSIFICATION OF TALAR NECK FRACTURES.
Type Fracture Clinical characteristics
I Vertical non-displaced Occurrence is 20%, only the blood supply
fracture of talar neck to the neck disrupted, 0-15% incidence of AVN
II Vertical fracture through Occurrence is 42%, with 2areas of disrupted
neck with dislocation blood supply, neck and body; 15-50%
of STJ (not ankle) incidence of AVN
III Vertical fracture of neck Occurrence is 34%, and all 3sources of
with dislocation of talar blood supply are disrupted; 90-100 %
STJ and ankle incidence of AVN
IV Vertical fracture of neck Occurrence is 4%, disrupts all 3areas of talar
with dislocation of blood supply; 90-100% incidence of AVN
STJ, ankle, and TNJ
Figure 10.21
272 Management of Foot and Ankle Trauma Ch.10
The treatment of talar neck fractures is based on the degree of injury and blood
supply. Hawkins Type I fractures are managed in a BK non-weight bearing cast for 6-8
weeks. Alternatively, an AK castwith the foot plantarflexed for 3-4 weeks followed by aBK
cast neutral for an additional 4 weeks can be used. Weight bearing and motion are not
initiated until adequate signs of healing are observed radiographically. Hawkins Type II, III,
and IV fracture/dislocations are initially closed reduced, however ORIF with lag screw
fixation of the neck is most effective. Immobilization and WB status are the same as
described previously for non-surgical treatment. Complications of talar neck fractures
include AVN, degenerative arthritis of the ankle and STJ, nonunion or mal-union, and
infection related to open fracture or surgery.
Os trigonum Syndrome and Shepherd's Fracture-os trigonum syndrome and Shepherd's
fracture can be very painful and debilitating. The os trigonum is present in 10% of the
population. The posterior aspect of the talus displays 2 processes that form agroove through
which the FHL tendon courses. The lateral process, also known as Stieda's process or the
trigonal process, is the larger of the 2and develops from asecondary center of ossification
atB-l1 years of age. Ossification with closure ofthe physis will usually occur within one year
thereafter. The os trigonum represents failure of the secondary center to unite with the
posterolateral process ofthe body. Fracture of Stieda's process is referred to as Shepherd's
fracture, and must be differentiated from a painful os trigonum. Both the os trigonum and
Stieda's process are injured by means offorced plantarflexion. The os trigonum may occur
bilaterally, so contralateral radiographs may be informative. Afractured posterior process
will be jagged with rough edges in the early phase, while the margins of the os trigonum
should be smooth. Ankle and first MTPJ range of motion may be painful in both cases.
Treatment for both os trigonum syndrome and Shepherd's fracture entails alocal anesthetic
block, BK weight bearing cast immobilization for 6 weeks, followed by range of motion
physical therapy. Recalcitrant cases require surgical excision of the os trigonum or the
Shepherd's fracture fragment, via a posterolateral incision that parallels the peroneal and
is anterior to the Achilles tendon.
Talar Dome Fractures-talar dome defects can develop secondary to ankle sprain or
fracture, and are known to be debilitating in all age groups. The Berndt and Harty
classification (Table 10-9) is the standard system for identification of talar dome lesions.
Talar dome osteochondral defects develop as aresult of shearing under compressive load
between the distal tibial bearing surface and the dome. The injury causes AVN of
the subchondral trabecular and cortical bone. which eventually heals with cortical
irregularity, and resultant development of post-traumatic arthritis.
TABLE 10-9. THE BERNDT AND HARTY CLASSIFICATION OF TALAR DOME LESIONS.
Stage Description of the injury
I A small area of subchondral bone compression
II A partially detached osteochondral fragment
III A completely detached fragment. remaining in its crater
IV A displaced osteochondral fragment
The incidence of posteromedial talar dome defect is 56%, while anterolateral defects
occur in 44% of cases. Medial lesions are caused by ankle inversion and plantarflexion,
273 Ch.l0 Management of Foot and Ankle Trauma
while lateral lesions are caused by ankle inversion with dorsiflexion (Figs. 10-22 and 10-23).
Treatment for all Stage r, II, and medial Stage III lesions is 6-12 weeks of BK non-weight
bearing cast immobilization, with consideration to use of a patellar tendon bearing brace and
partial weight bearing; and surgical intervention for recalcitrant pain. Stage IV and lateral
Stage III lesions are treated surgically by means offragment excision, saucerize the crater,
drill hole fenestration of the subchondral bone to aid revascularization and enhance
fibrocartilage production. Medial lesions may require medial malleolar osteotomy and
subsequent replacement with lag screw fixation. Lateral lesions may be combined with
secondary repair of chronic lateral ankle instability if this condition exists. Very large
fragments may be amenable to reduction and fixation with either absorbable pin or screw
fixation. The use of autogenous osteochondral plug grafts (OATS) harvested from non-
contact articular cartilage from the head of the talus, or the knee, as well as allogeneic
grafts, and/or autogenous cultured cartilage cells, provide other reconstructive options.
Early postoperative range of motion in a non-weight bearing fashion is indicated, with
resumption of weight bearing at about 2-3 weeks postop. Salvage by means of ankle fusion,
or total ankle replacement may also be considered (explained elsewhere in this manual).
Ankle Fractures-the anterior inferior tibiofibular ligament attaches to the tibia at the
tubercle of lillaux. Avulsion fracture of the tibia at this location is termed a lillaux-Chaput
fracture. Avulsion of the fibula at the attachment of this ligament is termed a Wagstaffe
fracture. The Lauge-Hansen classification (Table 10-10) of ankle fractures provides a
functional description ofthe mechanism of injury. The first word in the system describes the
position of the foot at the time of injury, and the second word denotes the pathological
motion of the foot relative to the ankle.
Stage I Stage II
Anterolateral
lesions
Key
Sites 01 osteochondrallractures
Stage III Stage IV
Figure 10.22 Figure 10.23
----------------
274 ManagementofFootandAnkleTrauma Ch.10
TABLE 10-10. THE LAUGE-HANSEN CLASSIFICATION OF ANKLE FRACTURES.
Class
Supination-
adduction
(Figure 10-241
Pronation-
abduction
(Figure10-25)
Supination-
eversion
(external
rotation)
(Figure 10-26)
Pronation-
eversion
(external
rotation)
(Figure10-27)
Mechanism
Pure
inversionof
footinthe
anklemortise
Pureeversion
ofthefootin
the anklemortise
Thetalus
externally
rotatesabout
an axis
comprised of
themedial
malleolusand
deltoidligament
External
rotationof
thetalus
aboutan axis
consistingof
the lateral
malleolusand
lateralcollateral
ligaments
Stage
I
II
II
III
II
III
IV
II
III
IV
Description of the pathology
Ruptureoflateralcollateralligamentsortrans-
verseavulsionfractureoflateralmalleolus
Talusimpactsthe medialmalleoluscausinga
vertical (oblique) fracture of the tibia; the
tibiofibularsyndesmosis remains intactand
diastasisdoesnotoccur
Ruptureofthe deltoidligament(medial clear
space),ortransverseavulsionfractureofthe
medialmalleolus
Ruptureoftheanteriorand posteriorinferior
tibiofibular ligaments, or Tillaux-Chaput or
Wagstaffeavulsionfracturefromthetibia or
fibula,respectively
Shortobliquefractureofthelateralmalleolus
originating atthelevelofthe ankle joint;on
thelateralview,thefibularfracture appears
transverse
Disruptionofthe anterior-inferiortibiofibular
ligamentor avulsionfractures ofWagstaffe
(fibula)orChaput-Tillauxtibia)
Classicspiralfractureofthelateralmalleolus,
beginning atthejointline;the fracture line
runs laterally from anterior-inferior to
superior-posterior
Disruption of posterior-inferior tibiofibular
ligamentoravulsionfracture ofVolkmann's
posteriormalleolus
Rupture of deltoid ligaments or transverse
fractureofmedialmalleolus
Disruption ofdeltoid ligamentortransverse
avulsionfractureofmedialmalleolus
rupture of anterior-inferior tibiofibular
ligament or Wagstaffe (fibulal or Tillaux-
Chaput(tibia)avulsionfracture
Interosseous membrane torn above
syndesmosis and below fibular head,
followed byhighfibularfracture atanylevel
starting above jointline, all the wayto the
proximal neck of the fibula (Maisonneuve
fracture)
Disruption of posterior-inferior tibiofibular
ligaments or avulsion fracture of tibia
(Volkmann)orfibula
Ch.10 Management of Foot and Ankle Trauma 275
Stage 1
Figure 10.24
Figure 10.25
Stage 1
Rgure 10.26 Fig ure 10.27
The Danis Weber classification (Table 10-11) focuses on the level of the fibular
fracture line relative to the ankle joint, and serves as a guide to repair of the fibula. The
fibular fracture is considered dominant, and restoration of its anatomic length takes
precedence over repair of the inferior tibiofibular syndesmosis. The goals of ankle fracture
repair are realignment of the ankle mortise, inspection of the talar dome and tibial plafond,
and reapproximation of supporting soft tissue structures.
276 Management of Foot and Ankle Trauma Ch.10
TABLE 10-11. THE DANIS WEBER CLASSIFICATION OF ANKLE FRACTURES.
Type Fracture pattern Pathological anatomy Corresponding
Lauge-Hansen
classification
A Fibular fracture Transverse avulsion fracture Supination-
distal to the joint line of fibula at or distal to level adduction
of ankle joint
Inferior tibiofibular ligaments
remain intact
May see associated medial
malleolar vertical fracture
B Fibular fracture Spiral or oblique fibular fracture Supination-
atthe joint line beginning at inferior tibiofibular eversion or
syndesmosis pronation-
Tibiofibular ligaments are abduction
usually disrupted but interosseous
membrane remains intact
May have disruption of deltoid
ligament or transverse medial
malleolar fracture
C Fibular fracture Fibular fracture above the Pronation-
above the joint line level of the tibiofibular eversion
syndesmosis up to the fibular head
Rupture oftibiofibular syndesmosis
and interosseous membrane
Deltoid rupture or transverse
medial malleolar fracture
Treatment in all cases begins with attempted closed reduction and immobilization, and
certain fractures are amenable to closed reduction and immobilization as the mainstay of
management Patients with minimal displacement, debilitated hosts, and patients with
limited ambulatory capacity may do best with closed reduction and immobilization, and
supportive therapy for post-traumatic arthrosis afterwards. Conscious sedation usually aids
closed reduction and immobilization. After closed reduction, immobilization in a curved
plaster cast with 3-point pressure (minimal padding) is continued 6-8 weeks non-weight
bearing. The radiographic criteria for adequate reduction of displaced ankle fractures include:
1. No widening of medial clear space;
2. No displacement of malleoli on AP view;
3. <2 mm of posterior displacement of lateral malleolus on lateral view;
4. No angular deformity of the ankle; and
5. Posterior malleolar fracture involvement of less than 25-30% ofthe tibial plafond.
Open reduction and fixation is best performed as soon as possible after injury, before
severe edema and hematoma form, as long as the patient is medically able to sustain
operative intervention. After 6-8 hours, edema with hematoma may prevent wound closure,
and fracture blisters may form. In such cases, therapy entails protection and rest, ice,
compression and elevation (PRICE) with closed reduction and application of a Jones
Ch.10 ManagementofFootandAnkleTrauma 277
immobilizing dressing, and waiting 4-14 days until the skin barrier is intact and edema
reduced.
SuggestedtechniquesforORIFofanklefractures(thereareotherusefulfixationmethods,
andthefollowingaretimehonoredguidelines)include:
Supination-Adduction (Type A)
1. Usetwo0.062 inch K-wires with 22-gauge tension band wirefortransverse
fibularfracture.
2. Usetwo4.0mmcancellousscrewsperpendiculartofracturelineandparallelto
eachothertofixverticalmedialmalleolarfracture.
Pronation-Abduction (Type B)
1. Fixtheshortobliquelateralmalleolarfracturewitha5- or6-hole1/3tubularaxial
compression platewith3.5 mm corticalscrewstosecurethe plate abovethe
fracture line(through bothfibularcortices)butnotbelowthefracture line,as
thiscoulddamagethetalus.Onlypurchasethelateralfibularcortex.
2. Repairinferiortibiofibularligaments with O-gauge non-absorbable suture. If
Tillauxfractureispresentuse4.0mm cancellouslagscrew/so
3. Transversemedialmalleolarfractureisfixedwithtwo4.0mmcancellousscrews
perpendiculartofracturelineandparalleltoeach other.
Supination-Eversion (Type B)
1. Spiralfracture offibulaisfixedwithinterfragmental4.0mm cancellousscrews
or3.5mm corticalscrews.Supplementwith 1/3tubular5-6-holeneutralization
plate placedperpendicularto planeoftheinterfragmentalscrews.The plateis
anchoredwith3.5mmcorticalscrewslaterally,oraposterioranti-glideplate is
usedtoboth reduceandstabilizethelateralmalleolarfragment.
2. Repairofanterior-inferiortibiofibularsyndesmosisoravulsions,asnotedabove.
3. Ifsmall posteriormalleolarfracturefragmentoccurs,itshould spontaneously
reducewithreductionofthefibulasincetheposteriorinferiortibiofibularligament
isintact(vassal rule).
4. Ifthere is alarge tibia fragment posteriorly (greater than 25% of posterior
malleolus)itmustbereduced.Use4.0cancellousscrewsposteriortoanterior.
5. Two 4.0 mm cancellous screws perpendiculartotransverse avulsion medial
malleolarfractureandparalleltoeachother.
Pronation-Eversion (Type C)
1. For fibular fractures mid-diaphyseal level or lower, use interfragmental
compression,with4.0mmcancellousor3.5mmcorticalscrews,thenaugment
with1/3tubularneutralization plate. Usetibiofibulartransfixingscrewthrough
orabovetheplateforfractureddistaldiaphysis.Alternatively,absorbablescrews,
or anonabsorbabletension suture(TightRope), could be used fortibiofibular
transfixation.
2. InMaisonneuvefractures,donotopenreduceduetopotentialcomplicationwith
commonperonealnerve,andadequacyoftibiofibulartransfixation.
3. First,fitdistalfibula intofibularnotchon tibia andtemporarilytransfixtibiaand
fibulawith5164SteinmannpinsandX-raytovisualizemortiseandlengthoffibula.
_ Is
': g
~ ; ; ; ~ Dividingcells
1 ~ ~ ~ l . i . Restingcells
278 ManagementofFootand AnkleTrauma Ch.lO
Ifsatisfactory,sutureinterosseousmembrane and then usefinalfixation with
two 3.5 mm cortical screws. Goal is to stabilize the tibiofibular relationship
withoutcompression ofthemortise.
4. Removetransfixingscrewsat6-8weeksandhardwareat4-6months.
Tibial Pilon Fractures-thedistaltibialmetaphysis(pilon)can be seriouslydisruptedin a
varietyofinjurypatterns,andrepairofthisstructureisdifficultand requiresconsiderable
experience.Pilonfracturesentertheankle,andmaybeassociatedwithfibularfractureas
well.Repairentailsanatomicreduction,autogenouscorticocancellousbonegrafting,and
internalaswellas externalfixation.Ahighrateofpost-traumaticarthrosis,osteomyelitis,
delayed and nonunion,limb angularand length misalignment.and difficultywalking can
ensue.Revisionalsurgery,bonetransport,ankleandpantalararthrodesis,andamputation
are not uncommon. Although several classification systems are available, the most
straightforwardisthatofRuediandAllgower(Table10-121.
TABLE 10-12. THE RUEDI-ALLGOWER CLASSIFICATION OF PII.ON FRACTURES.
Type Description of the pilon fracture
I Pilonfracturewithminimaldisplacement
II Pilonfracturewithsignificantdisplacement
III Pilonfracturewithsignificantdisplacementandlossofcancellousbone
Epiphyseal Plate Fractures-theepiphysealcomplexconsistsoftheepiphysis,physis,and
themetaphysis.Epiphysesare eitherofthe pressureortractiontype.Pressureepiphyses
are located atthe end ofalong bone and provide rapid longitudinal growth.Traction
epiphysesarenon-articular,andlocatedwheremuscleortendonattachestobone,anddo
not contribute to axial growth. Anatomicallythe physis displays three distinct zones
(Fig.10-28).Thezoneofgrowthisclosesttotheepiphysisandcontainsrestingchondrocytes
thatprogresstodividing cellsthatarrangein columns.Thenextcomponentisthezone of
cartilagematuration,whichistheweakestregionduetolossofintracellularmatrix.Finally,
---,
Ossification
Zoneof
Transformation
Vascular
penetration
Calcifcation }
Zoneof
IHypertrophy Maturation
COlumalion}
Zoneof
Growth
Figure10.28
Figure10.29
279 Ch. 10 ManagementofFootandAnkleTrauma
thezone ofcartilagetransformationdisplays cartilage convertingto bone. Periosteum is
morevascularized,thicker,and strongerinthe child.The cartilageisstronglyattachedto
themetaphysis,andmorelooselyattachedtothediaphysis.Theperiosteumalsoactsasa
checkrein to resist fracture displacement. The vascular supply to the growth plate
complexisasfollows:metaphysis-suppliedbythenutrientarteryofthediaphysis,vessels
from periosteum and perichondrium, and these sources extend to the zone of
hypertrophiedcelis;epiphysis-suppliedbynutrientepiphysealvessels;physis-supplied
by nutrient arteries from both the metaphysis and the epiphysis, as well as direct
perichondrialvesselstothephysis.lfthemetaphysealsupplyiscompromisedorlost,there
is usuallyverylittle change in physeal perfusion. If, however, eitherthe epiphyseal or
perichondrialsupplyislost,thephysismaydieand prematurepartialortotalclosure may
ensue.Theepiphysealvesselssupplythephysealzoneofgrowth.Partialclosuremaycause
angulardeformity.TheosseousringofLacroixisan extensionofmetaphysealcorticalbone
that stabilizesthe physis atthe zone of Ranvier, where the physis interfaceswiththe
metaphysis(Fig. 10-29). Evaluation ofphyseal injuryrequires atleastthree radiographic
viewsandcomparisonwiththe uninjuredextremity.Epiphysealfracturesare categorized
bySalter-Harris(Table10-13)andAiken-Mueller(Table 10-14).
TABLE 10-13.SALTERHARRIS (SH)CLASSIFICATION OF EPIPHYSEAL PLATE FRACTURES.
Type
I(Fig. 10-30)
II(Fig, 10-31)
III(Fig.10-32)
IV(Fig. 10-33)
V
VI (Fig.10-341
VII(Fig.10-35)
Description
1. Separation of epiphysis from metaphysis between layers of
hypertrophyandcalcification
2. Restingcellsremainwiththeepiphysis
3. Minimaldisplacementusuallyduetostrongperiosteum
1. Mostcommonacutephysealinjury
2. Separation of epiphysis from metaphysis between layers of
hypertrophyandcalcification
3. Fracturelinerunsthroughphysisthenthroughmetaphysis
4. Thurston-Holland sign-metaphyseal fragment where the
periosteumisintactadjacenttothemetaphysealfragment
5, Werenskiold sign-smallfragmentofmetaphysealfragmenton
X-ray
1. Fracture beginsin joint,runs uptothe physisthen makesa90
turnthroughthelayerofhypertrophiedcellsto periphery
2. Area of concern for blood supplyto free fragment as well as
congruityofjointsurface
3. Mostgerminalcellsremainintact
1. Injuryrunsfromjoint,through epiphysis,through physis and out
throughmetaphysis
1. Crushinginjurythatdestroysalllayersofphysis
2, Prematureclosureusuallyensues
1. Injury associated with removal of bone loss at the zone of
Ranvier,duetotraumasuchas aburnordeglovinginjury
1. Avulsionfractureoftheepiphysis,notinvolvingthe physis
280 Management of Foot and Ankle Trauma Ch.10
W
~
Type IA fracture Type IB fracture Type IC fracture
Figure 10.30
g g
~
Type IIA fracture Type liB fracture Type IIC fracture
Type liD fracture
Figure 10.31
brJ-
Jj
b6
t
Type iliA fracture Type IIiB fracture
Figure 10.32
y
6
~
Q
1M
~
/-/-
Type IVA fracture Type IVB fracture Type IVD fracture
Figure 10.33
281 Ch.10 ManagementofFootandAnkleTrauma
B
Type VI fracture
TypeVIIfracture
Figure10.34 Figure10.35
Atriplanefractureisspecial distaltibial epiphysealfracturethatusuallyoccursin
olderchildren, about1yearpriorto closure ofthe epiphysis,and resultsfrom external
rotation. The 2-parttriplane fracture occurs when the medial part of the distal tibial
epiphysishasalreadyclosed,andthelateralradiographdisplaysaSH IVfracture,andthe
posteriortibialplafondfragmentextendstothemetaphysis,andmaybecomminuted.The
3-parttriplanefracture consists ofacombination ofaSH II and aSH III fracture, and
occurs when the middle portion of the distal tibial epiphysis has closed. The lateral
radiographdisplaysaSH IIfracture,whilethemortiseviewshowsaSHIIIfracture.Thetibia
displaysalargeposteriorfragmentconsistingofalargeposteriorfragmentofposteriorand
medialportionsofthemetaphysis,whilethemedial1/3-1/4ofthetibialplafond andmedial
malleolusremainsintact.Thefibulaisalsousuallyfractured.Treatmentrecommendations
forepiphysealplatefracturesentailthefollowingguidelines:
TypesIand II
1. Usuallyrespondwelltoclosed reduction,especiallyifseenearly.
2. Ifseen7days afterinjury,the attemptat closed reduction maydo more
harmthangood duetofasthealingthatoccursatthissite.
TypesIII,IV,V, andVI
1. Should attemptclosed reductionfirst, butusuallyrequires ORIF. 2. Must
anatomicallyreducethephysisandpreservejointcongruity.
3. TrytokeepthreadedK-wiresorscrewsoutofphysis.
4. Tryand maintainfixationdevicesin metaphysis.
TABLE 10-14.
THEAIKEN-MUELLEREPIPHYSEALPLATE FRACTURE CLASSIFICATIONSYSTEMS.
Aiken Mueller
1=SalterII A=SalterI,II
2=SalterIII B=SalterIII,IV,VI
3 SalterlV C=SalterV
-----------------------------------
282 Foot and Ankle Disability and Rehabilitation Ch.11
FOOT AND ANKLE DISABILITY AND REHABILITATION
WORKABILITY, DISABILITY, AND REHABILITATION
Rehabilitation of the foot and ankle following injury or surgery, or as apart of the treatment of
disease, ranges from straightforward and simple intervention such as walking and range of
motion (ROM) exercises, to complicated diagnostic and therapeutic regimens that require
specialized training and equipment. Specialization has developed due to an ever-increasing
number of work-related injuries, workers' compensation and disability lawsuits, costs, and
regulatory agencies and the Americans with Disabilities Act. Occupational therapy or
industrial medicine consultation and referral can be helpful, in such cases.
Work is defined as any and all forms of productive activity, regardless of whether or
not there is reimbursement. Work levels, as defined by the US Department of Labor, are
depicted in Table 11-1. Cumulative trauma disorders often develop secondary to repetitive
strain, vibration or cold exposure, and include plantar fasciitis and heel spur syndrome,
tarsal tunnel syndrome, stress fracture, and chronic tendonitis and/or capuslitis. Physical
therapy entails exercise and other physical modalities used in primarily the acute and
subacute phases oftreatment. Workability may be determined using afunctional capacity
assessment (FCA), which entails a standardized questionnaire to assess appropriate
behavior and symptom magnification; direct measurements of strength, power, endurance,
coordination, balance and mobility; and job simulation. Patients who have been out of work
or incapacitated for greater than 3-6 months, despite accurate diagnosis and treatment,
including physical therapy, may benefit from functional capacity assessment. Individuals
incapacitated >6 months may require work conditioning in an effort to reestablish strength,
flexibility, and aerobic capacity, without work simulation. Work hardening involves real and
simulated conditioning tasks, designed to enable productive, safe, and tolerable re-entry to
the work place after temporary incapacitation. Job modification may be recommended
based on the functional capacity assessment and efforts at work hardening, and may
entail work aids (a stool to sit upon, a cushioned floor mat, special shoes, etc.), alteration
of labor category (job description), and measures to assure safety and prevent reinjury. Not
all physical therapists are equipped to perform aFCA, or to undertake work conditioning or
work hardening programs.
TABLE 11-1. WORK LEVELS DEFINED BY THE US DEPARTMENT OF LABOR *
Work level Maximum lift Frequently lifts Ambulation
Sedentary 10 lb. None Infrequentwalkin or standing
Light work 20lb 101bs. Frequent walking and/or standing
Medium work 50 lb. 251bs. Frequent walking and/or standing
Heavy work 100 lb. 501bs. Frequent walking and/or standing
Very heavy work >100 lb. >50Ibs. Frequent lifting and carrying
website last visited 10/27/2007.
Such reports may also be useful in legal matters where disability determination is in
question. Occupational therapy and social service intervention will often enhance the
patient's progress and lifestyle. For patients with chronic pain, or suspected RSDS/CRPS,
referral to the pain clinic can also be helpful. Categories for the industrial rehabilitation pre-
scription are depicted in Table 11-2.
283 Ch.11 FootandAnkleDisabilityand Rehabilitation
TABLE11-2.INDUSTRIALREHABILITATION PRESCRIPTIONS.
Phase Prescription
acuteandsubacute3months) Accuratediagnosis,protectionoftheinjuredpart
rest.ice,compressionandelevation,medications
andphysicaltherapy
~ months FCAandworkhardening
Prolongedrehabilitation(>6months) FCA,workconditioning,workhardening
Anexampleofaprescriptionforphysicaltherapyfollowingan anklesprainfollows:
RxPhysicaltherapyfor: 1)strengthening,2)flexibility/rangeofmotion,and3)
proprioception,rightankle;6-8sessionsover3-4weeks,evaluateandtreat.
Diagnosis:status-postanklesprain(lCD9xxx.xx)
Anexampleofaprescriptionforworkhardeningfollowing an anklefracturefollows:
RxWorkhardeningstatus-postORIFanklefracture(lCD9xxx.xxl.please
send report
Activities of dailyliving (ADLs) include feeding, grooming, dressing,toileting, bathing,
continence, transfers, and communication. Some examples ofcomplex ADLs include:
cooking, cleaning,laundering,shopping, housekeeping,telephone,moneymanagement,
care giving,traveling,andtaking medications. Functional capabilities includeself-care
(fundamentalandcomplexactivitiesofdailyliving),work,playandleisure.Disabilitystatus
canbe categorizedusingtheKarnofskyscale(Table 11-3).
TABLE11-3.
DISABILITYSTATUSACCORDINGTOTHEKAMOFSKYSCALEOFPERFORMANCE.
ScoreDisability
100 Normal,nocomplaintorapparentdisease
90 Normal,minorsignsandsymptomsofdisease
80 Normalwithextraeffortmoderatesignsandsymptomsofdisease
70 Unabletocarryonnormalactivitiesoractivelywork,cancareforself;markedsigns
andsymptomsofdisease
60 Requiresoccasionalassistance,primarilycaresforself;marked signs andsymp-
tomsofdisease
50 Requires considerable assistance and frequentmedical care; marked signs and
symptomsofdisease
40 Disabled,requiresspecialcareandassistance;markedsignsandsymptomsofdis-
ease
30 Severe disability,hospitalized orinstitutional care indicated;marked signs and
symptomsofdisease
20 Verysick,hospitalizationwithactivesupportivecareisnecessary
10 Moribund,fatal processesprogressing
o Death
284 FootandAnkle Disabilityand Rehabilitation Ch.11
Rangel00-80-thepatientisabletocarryonnormalactivity,andnospecialcareisneeded.
Range70-50-thepatientisunableto work,butisabletolive athome and careformost
personalneeds,withavarying amountofassistanceasneeded.
Range4O-10-thepatientisunableto careforselfandrequiresequivalentofinstitutional,
orhospitalcare,anddiseasemaybeprogressingrapidly.
285 Ch.12 Evidence-BasedMedicine(EBM)and Documentation
EVIDENCE-BASED MEDICINE (EBM) AND DOCUMENTATION
EVIDENCE-BASED MEDICINE (EBM)
Evidence-basedmedicine(EBM)entailsthe applicationof3elementsofinformationused
to makeclinicaldecisions.The3componentsofEBM are:1)the clinician'sexperience,2)
theindividualpatient'sneeds,and3)thescientificevidencerelatedtotheclinicalquestion
athand.There isahierarchyofevidence relatedtohuman clinical scientificknowledge
(Table 12-1).
TABLE 12-1. lEVELS OF HUMAN CLINICAL EVIDENCE.
ACFAS* Score
1a
lb
1c
2a
2b
2c
3a
3b
4
5
Level of Clinical Evidence
SystematicreviewofhomogenousRCTst
IndividualRCTwithnarrowconfidenceintervals
"All-or-none"observationalstudy
Systematicreviewofhomogenouscohortstudies
Singlecohortstudy,orpoorqualityRCT
Outcomesresearchorecologicalstudy
Systematicreviewofhomogenouscase-controlstudies
Singlecase-controlstudy
Case reportorseries,orpoorqualitycase-controlstudy
Expertopinion,animalphysiology,benchstudy
*ACFAS=AmericanCollege ofFootandAnkleSurgeons(http://WWIIIlacfas.org)
tReT=randomizedcontrolledtrial
Furthermore,humanclinicalresearchfollowsahierarchyofresearchdesignoptions(Table
12-2).
TABLE 12-2. HUMAN CLINICAL RESEARCH DESIGN OPTIONS.
Analytical
hypothesis-
testing
Descriptive
hypothesis-
forming
Research Design Options*
RCn(interventionalexperiment)
Prospectivecohortstudy(observational)
Retrospectivecohortstudy(observational)
Case-controlstudy(observational)
Analysisofseculartrends(groupcorrelational)
Crosssectional(individualpoint-in-time)
Case series
Casereport(raredisease,noveltreatment)
Animalphysiology,cadaver,syntheticorcomputermodelstudy
*Thetableisarrangedfromtopto bottom,beginningwiththe research designthatismostlikelyto producevalid
results(andconclusions},thatbeingtherandomizedcontrolledtrial,to theresearchdesignthatisconsideredto be
leastlikelyto produce valid results in regard to human clinical outcomes, that beingthe animal orbench-top
investigation.
tRCT randomized controlledtrial
286 Evidence-Based Medicine (EBM) and Documentation Ch.12
The elements of ascientific investigation that contribute to the validity ofthe conclusions
gleaned from the study are depicted in Table 12-3.
TABLE 12-3. THE BUlI.DlNG BLOCKS OF GOOD CLINICAL EVIDENCE.
Building Blocks of Clinical Evidence*
1. Explicitly defined research question, population, and end points
2. Randomized treatment allocation and intention-to-treat analysis
3. Participants and outcomes assessors blind to treatment allocation
4. Use of avalid health measurement (quality of life) instrument
5. Power and sample size determined a priori
6. Statistical analyses compatible with type and distribution ofthe data
7, Point estimate and 95% confidence interval reported
'Turlick MA, Kushner D, Stock D. J Am Podiatri Med Assoc 93: 392-8,2003.
FUNDAMENTAL ELEMENTS OF SCIENTIFIC PUBLICATION
When reporting scientific information, or submitting a manuscript to a peer-reviewed
journal, the following information can be used to develop the report,
Abstract Submit an abstract of s 250 words summarizing the contents of the article, The
Abstract canbe no longer than 250 words, since the National Library of Medicine (via
Pubmed) truncates longer abstracts at 250 words, resulting in loss of information. The
Abstract can be written as continuous prose, or with subheadings for each section of the
manuscript, depending on the specific journal's preference. The Abstract for a report of
research should reflect the format ofthe manuscript itself, describing pertinent information
for each section of the manuscript. It should briefly introduce the research problem,
explain methods, summarize results, and provide a conclusion, The Abstract for a case
study should state the condition of interest, and include a brief summary of the specific
clinical situation, the uniqueness or rarity of the diagnosis orthe novelty of the intervention,
and a statement regarding the clinical significance of the case. Do not use any
abbreviations or bibliographic reference citations in the Abstract, since electronic
searching may limit the space not all abbreviations will be recognizable to all readers. If
necessary, parts of the Abstract may be written as phrases, rather than as complete
sentences, The level of clinical evidence (Table 12-1) should be noted in the last sentence
of the Abstract
Key Words: Provide 3-5 key words or phrases for electronic indexing purposes, Keep in
mind that electronic searches ofthe biomedical literature depend to alarge degree on key
words. Refer to the National Library of Medicine's (via Pubmed) Medical Subject Heading
(MeSH) webpage (http://www.ncbi,nlm,nih.gov)for help selecting key words. Key words
are to be spelled in small case letters, unless representative of a proper name, and listed
in alphabetical order separated by a comma between each word/term, Avoid abbreviations
in the key words, unless aproprietary name uses an abbreviation, In general, proper names
are not used as key words.
Introduction: This section should provide a concise overview of the state of knowledge
regarding the specific problem being studied, It should begin with a statement of the
287 Ch.12 Evidence-Based Medicine (EBM) and Documentation
problem and its clinicaVsocial importance, followed by an explanation of recent and
important research related to the topic, supported by reference citations. The importance
of the topic is best conveyed by means of statistics that indicate the prevalence and/or
economic impact of the condition in the population/society. After an explanation of what is
known, and what remains unknown in regard to the focus of the study, the author should
concisely state the specific research question or hypothesis for the current investigation.
Generally, the last sentence of the introduction should include a statement that describes
the specific study design (see Table 12-2) and reiterates the research question.
PatientsIMaterials and Methods: If the study is a clinical investigation involving living,
human participants (patients, subjects), then the heading for this section should
be "Patients and Methods." If the investigation involves animals, cadavers, or in vitro
models of any sort, including computer models, then this section should be termed
"Materials and Methods." In general, the methods section should describe the following
elements of the investigation: aims, assessors and other members of the investigational
team, population or sample, intervention, endpoints (measured variables), and the
statistical methods used to determine the meaning of the results (see details below).
Ideally, this section should provide enough detail to allow subsequent researchers to
replicate the study. When reporting randomized controlled trials, a study flow diagram in
CONSORT format as well as all of the information required by the CONSORT checklist,
should be provided. The CONSORT statement, checklist, and study flow diagram are
available at http://www.consort-statementorg. For observational investigations, the STROBE
statement (http://Www.strobe-st8tementorg) guidlelines and checklist can be used.
Aims: The primary aim of the investigation, as well as any secondary aims, should also be
clearly stated. A distinction should be made between primary and secondary aims. As a
rule, the sample size should be adequate to identify astatistically significant difference in
regard to the primary aim, if such a difference exists. Power and sample size calculations
can be determined using any of a number of software programs, such as that found at:
http://biostatmc. vanderbiltedu/tWiki/bin/view/M8in/PowerSampleSize. In describing th e
primary aim, many authors will restate, in some fashion, their hypothesis and research
question, emphasizing that they undertook to answer the question.
Assessors: Members of the investigational team should be described in regard to their
participation in the study; namely, if they served as outcome assessors or if they performed
an intervention or, in the case of aretrospective study, if they abstracted data from medical
records. For studies in which subjective measurements are determined, such as
measurements of radiographic angles, amethod should be described for breaking ties and
determining an outcome when indecision or uncertainty exists. If outcomes assessors were
blind to treatment allocation, this must be stated. If outcomes assessors were participants
in the intervention, such as members of the surgical team or treating clinicians, this must
also be stated.
Study population: The methods section should provide readers with an explicit description
ofthe participant/patient population and the time period from which they were selected. The
time period should delineate the day, month and year that the period started; and the day,
month and yearthatthe period ended (MM/DD/VYYY-MM/DD/VYYY.lfthe daythatthe time
period started is not known, then it is acceptable to state just the month and year that
288 Evidence-Based Medicine (EBM) and Documentation Ch.12
initiated and ended the period (MM!YYYY-MM!YYYY). It is also important for the author to
state whether or not treatment allocation was determined in arandom fashion, and whether
or not participants in a clinical trial were blind to treatment allocation. The method of
randomization should be described (random number table, electronic random number
generator, sealed envelopes, other). For case series and cohort studies, the author should
state whether or not the participants were enrolled consecutively. The inclusion and
exclusion crrteria must be clearly stated, and it is best to simply list these.
Intervention: In any investigation, the intervention needs to be explicitly described. If
participants were randomized to an active therapy that was compared to standard
therapy, or placebo, each treatment arm needs to be described. Authors are encouraged
to avoid presenting a detailed narrative report of an operative intervention for a standard
procedure that can be referenced in any of anumber of textbooks. Reference can be made,
wrth an appropriate citation, to a standard procedure as rt is described in atextbook; and
variations on the procedure should be described in detail. Novel interventions, notable
variations on standard procedures, decision points related to an intervention, and adjunct
procedures should be thoroughly described.
Endpoints (outcomes): Outcome measures should be explicitly defined in terms of how the
variable was measured, who made the measurement, and whether or not the assessor was
blind to the intervention (for an intervention trial). Authors should clearly state if outcomes
were based on physical examination, chart review, telephone interview, questionnaire or
radiographic films. As a rule, any variable that a reasonable clinician would consider
important in regard the treatment of a patient, as it pertains to the investigation, should be
considered in the analysis. In addition to the intervention/s or outcome/s of interest, typical
independent variables include such things as age and age category, gender, activity level,
body mass index (BM!) or BMI category, comorbidities, medications, duration oftreatment,
surgeon or clinical site, adjunct therapies, frequency and duration of follow-up, and
post-intervention management procedures (immobilization, physical therapy, etc.). Items
such as those just listed above should be referred to as "variables" and not as
"parameters," since the term "parameter" should be reserved for statistical expressions
that describe the data, such as the mean and standard deviation, or beta coefficients
derived from a regression analysis. Whenever possible, it is preferable that "hard"
endpoints be used, such as analytical measurements. clinical or microbiology laboratory
results, and the like. Whenever "soft" endpoints, such as quality of life (QOl), are
considered. it is preferable to use health measurement instruments that have previously
been shown to be reliable and valid. QOl instruments should be specific to the foot and
ankle (ACFAS, AOFAS, Bristol Foot Score, Foot Function Index, etc')' as well as measures
of general health (SF-36, etc). Investigator derived questionnaires should be described in
terms of reliability and validity, if such testing was undertaken. For scales that rank
categories (mild, moderate, severe, for example) an aggregate score should be used. For
measurements of pain, the lO-cm Visual Analog Scale (VAS) is recommended.
Statistical Methods: The statistical plan should be clearly described, and every investigation
should include at least descriptive and inferential, as well as univariate and multiple variable,
statistical analyses. The descriptive statistical analysis should define parameters such as the
measure of central tendency (mean or median average), and measures of dispersion
(standard deviation or range). The parameter, as well as the statistical test, should be selected
289 Ch.12 Evidence-Based Medicine (EBM) and Documentation
based on the type and distribution of the data. In short, continuous numeric data that are
normally distributed are suitable for representation using the mean and standard
deviation, and may be analyzed using mean-based statistical tests (such as Student's
Hest). Categorical data, and data that are non-normally distributed, are suitable for
representation using the median and range, and may be analyzed using median-based
methods such as the Wilcoxon matched-pairs signed-ranks test, sign test, Wilcoxon
rank-sum test, and the Kruskal-Wallis equality-of-populations rank test, and other null
hypothesis tests and methods of estimation. For categorical data, Fisher's exact method should
be used as much as possible. Univariate analyses should describe the association of
independent variables with the outcome of interest (dependent variable!. whereas
multiple variable analyses should describe the association of all of the clinically important
variables with the outcome of interest
Results should be presented with only as much precision as is of scientific value. For
example, measures of association (odds ratios, relative risks, risk differences, etc.) should
typically be reported to two significant digits. As a rule, the terms "significant" and
"significantly" should be reserved for use when describing statistical differences. The
statement "no significant difference was found" between two groups should not be made
unless apower analysis was done and the value of alpha (level of significance, typically 5%)
or beta (the power to detect a statistically significant difference, usually 80% or 90%) is
reported. Use of the word "significant" requires reporting of a P-value (probability), orthe
95% confidence interval about a point estimate. It is preferable to report the 95%
confidence interval (CI) rather than the P-value, since the 95%CI describes whether or not
the result was statistically significant, while also showing just how precise the estimate
was. Except when l-sided tests are required by study methodology, such as in
noninferiority trials, 2-sided P-values should be reported. By convention, P-values larger
than 0.01 should be reported to two decimal places, those between 0.01 and 0.001 to three
decimal places, and P-values smaller than 0.001 should be reported as P<0.001. P-values
should not be reported as "P = O."Furthermore, use of the word "correlation" or the term
"correlates with" requires that a correlation coefficient (Cronbach's alpha) be calculated
and reported. The results of a sensitivity analysis, such as that described by Greenland
(Maldonado G, Greenland S: Simulation study of confounder-selection strategies. Amer J
Epidemiol. 1993; 138: 923-936.), or that described by Rosenbaum (Rosenbaum PR.
Sensitivity analysis for matched case-control studies. Biometrics. 1991 Mar; 47(1): 87-100;
and, Rosenbaum PRo Discussing hidden bias in observational studies. Ann Intern Med. 1991
Dec 1; 115(11): 901-5.), should be presented for retrospective studies where unmeasured
independent variables may have potentially influenced the results.
Additional references that may be useful in regard to the description of the methods
and the presentation of a statistical plan include:
Bailar JC III, Mosteller F. Guidelines for statistical reporting in articles for medical
journals: amplifications and explanations. Ann Intern Med1988; 108: 266-73.
Altman DG. Machin D, Bryant TN, Gardner MJ (eds). Statistics with Confidence.
second edition. london: BMJ Books, 2000.
Malay DS. Some thoughts about data type, distribution, and statistical significance.
J Foot Ankle Surg 45: 57-9,2006.
Malay DS. Levels of clinical evidence. J Foot Ankle Surg 46: 63-4, 2007.
290 Evidence-Based Medicine tEBM) and Documentation Ch.12
------------------------....
Results: The results section should presents quantitative information on the data collected,
in the form of descriptive and inferential statistics. Relevant information on the study
population includes demographic information for each subgroup (control group and study
groups), exclusions and attrition. Inferential statistics should be used to compare groups
using appropriate statistical tests based on the size ofthe study population, type of variables
under study (discrete vs. continuous), and the distribution of the data collected.
Quantitative information should be summarized in the text, and readers should be referred
to relevant tables for more detailed information. As a rule, three results tables should be
presented, and designated Tables 1, 2, and 3. Table 1 typically depicts the baseline
demographic characteristics of the sample population, often categorizing the patients/
participants by intervention or outcome, and showing whether or not statistically
significant differences existed between the groups. For randomized controlled trials, it is not
necessary to depict statistically significant differences at baseline, since randomization
distributes the characteristics by chance. Table 2 generally depicts the results of the
univariate analyses, and Table 3 generally depicts the results of the multiple variable
analyses. Additional tables can be helpful when the data warrant such detail.
Discussion: The discussion section should offer the authors' interpretation ofthe results of
their investigation. Authors should consider how their results fit into the general state of
knowledge on the subject, as well as their clinical relevance. In addition, authors should
acknowledge the limitations of their investigation that may have introduced bias, and they
should discuss how the results may have been affected by bias. It is adviseable that authors
tell the readers all of the shortcomings that they (the authors) understand to have
influenced their results and conclusions, rather than leave this criticism solely up to the
readers. Investigations that show a statistically significant difference between treatment
groups should not be criticized for having too small a sample. Finally, suggestions for
clinical applications and/or further research may be appropriate. Do not include a
separate "Conclusion" subsection, as the final paragraph ofthe discussion should describe
the authors' conclusions.
Acknowledgement In general, acknowledgments should be made to those who have
informally contributed their expertise or assisted in the investigation, ratherthan to those who
have contributed to the manuscript while performing the role oftheir regular occupation.
References: References are cited in the body of the text by means of numeric citations
listed parenthetically in the appropriate sentence, prior to the end of the sentence (usually
just before the period ending the sentence). Reference citations are to appear in
sequential numeric order, beginning with the number "1" and continuing in sequential
numeric order the first time that a particular reference is cited, until the last citation is noted.
In other words, supply references numbered in the exact order they appear in the text (not
alphabetically). Sources not identified in the text should be listed as Additional References.
Unpublished sources must be included in parentheses within the body of the text, not in
the Reference Section. Abbreviations for journal titles should conform to those used by
Medline (www.ncbi.nlm,nih.gov/sites/entrez?db=pubmed). If Medline does not index a
journal, then spen out the entire journal name in addition to listing the author name/s, title
of the article, volume number, page numbers, and year of publication. Always list all
authors, and do not use "et al" when listing your references. The term "et al" may be used
in the body of the text; however, it is generally reserved for mentioning papers written by
291 Gh.12 Evidence-Based Medicine (EBM) and Documentation
more than 3 authors. Whenever atextbook is referenced, it is necessary to include the
specific page or pages used. Whenever aweb reference is cited, it is necessary to include
the date when the site was last accessed.
~ m p l e s of reference citations include:
Journal article: 1. Mendicino RW, Orsini Re, Whitman SE, Cantanzariti AR. Fibular
grove deepening for recurrent peroneal subluxation. J Foot Ankle Surg 40:252-263,
2001.
Textbook: 2. Trevino SG. Disorders of the hallucal sesamoids. In Foot and Ankle
Disorders, pp 379-398, edited by MS Myerson, WB Saunders, Philadelphia, 2000.
Electronic version of a print journal: 3. Gardner MJ, Boraiah S, Hentel KD, Helfet DL,
Lorich DG. The hyperplantarflexion ankle fracture variant J Foot Ankle Surg [serial on
the Internet146:256-60, 2007.tiSlAvailable at http://www.jfas.org/issues!contents.
Web page: 4. Clinical Practice Guideline Heel Pain Panel. Diagnosis and Treatment of
Heel Pain. American College of Foot and Ankle Surgeons Web site. September/
October 2001. Available at: http://www.acfas.org/pubresearch/cpg/heelpain-cpg.htm.
Accessed mm/dd/yyyy.
Figures: Photographs and illustrations should be clear and support the specific points
mentioned in the text. Figures and their accompanying legends should be able to stand
alone, communicating the meaning ofthe information without reference to the main text. In
the text, figures should be cited using parentheses about the figure-reference being cited.
For example: "(Figure 1"'. Each figure should be titled, and accompanied by afigure legend.
The figure title should be formatted as in the following example: "Figure 1. The
gastrocnemius recession." Do not use abbreviations in either the figure title or the figure
legend, unless the abbreviation is defined in the legend. Abbreviations or footnotes should
be explained in lower case alphabetical superscripts beneath the figure. Ifthe figure reports
astatistical result, such as a P-value, then the statistical test used to determine the P-value
needs to be described in the legend or elsewhere in the figure. Rgure titles and legends must
be submitted for each figure, and should be typed in consecutive order, double-spaced, on
a separate page from the text Each figure must be submitted as a separate page
(electronic file). Images should be provided in TIF, GIF or EPS format, per the specific
journal's instructions. Manuscripts that describe a pathological entity should be
accompanied by a photomicrograph, with the type of stain and magnification indicated.
Radographic images should be submitted in grayscale format. Black and white line
drawings are acceptable only if they are of professional-quality. All figures must be
original. unless indicated otherwise. A letter should accompany figures that have already
been published in other sources, indicating that the previous publisher and author have
granted permission for their use. Keep in mind that hardcopy lIustrations and figures are
usually not returned to authors.
Tables: Tables should be clear and support the specific points mentioned in the text. Black
and white lines and text are preferred, and the "insert table" function ofthe toolbar of most
292 Evidence-Based Medicine (EBM) and Documentation Ch.12
word processors works well for this. Tables and their accompanying legends should be
able to stand alone, communicating the meaning of the information without reference to the
main text In the text tables are cited using parentheses about the table-reference being
cited. For example: "(Table 1)." Each table should be titled, and accompanied by a table
legend. The table title should be formatted as in the following example: "Table 1. The
dataset." Do not use abbreviations in either the title or the table legend, unless the
abbreviation is defined in the legend. Abbreviations or footnotes should be explained in
lower case alphabetical superscripts beneath the table. If the table reports a statistical
result, such as a P-value, then the statistical test used to determine the P-value needs to be
described in the legend or elsewhere in the table. Table titles and legends must be
submitted for each figure, and should be typed in consecutive order, double-spaced, on a
separate page from the text Each table must be submitted as a separate page (electronic
file). Tables should be provided in either .doc, TIF, GlF or EPS format, per the journal's
instructions for online submission. All tables must be original, unless indicated otherwise.
A letter should accompany tables that have already been published in other sources,
indicating thatthe previous publisher and author have granted permission fortheir use.
Registered trademarks and copyrights: As arule, generic terminology is preferred. Any and
every time that a proprietary substance (such as a medication), device, equipment, or
software program is mentioned in the manuscript, it must be accompanied by either of the
following symbols: "" or "f"", indicating that the substance or device is a registered
trademark; and the following information must be provided in parentheses, immediately
following mention ofthe proprietary item: proprietor's name (the name ofthe company that
owns the registered trademark), city and state wherein the proprietor's headquarters are
located, and the country if other than the United States. If copyrighted material is
mentioned, then the "" symbol should accompany the item. Furthermore, the use of
copyrighted material requires that the author obtain explicit permission from the owner of
the copyright (publisher), and the author, for such use. As arule, proprietary names should
not be used in the manuscript's title, and once a proprietary name is used to describe an
intervention or diagnostic test, generic terminology should be used thereafter. In an effort
to remain scientific, and to avoid the appearance of proprietary bias, generic terminology
is generally preferred by peer reviewers and editors.
Abbreviations: Do not use abbreviations in the litle, Abstract, or Key Words section of the
manuscript because information from these portions ofthe paper is used in the process of
electronically indexing biomedical literature. If a proper or proprietary name entails the use
of an abbreviation, only then can it be used in the Title, Abstract or Key Words sections.
Abbreviations can be used in the Introduction, as well as any area of the manuscript
thereafter. Abbreviations are notto be used unless the term has first been spelled in full, and
the abbreviation noted in parentheses immediately following the full term. For example:
" ... deep peroneal nerve (DPN)." Abbreviations that are part of a proprietary name are to
be used in accordance with the guidelines noted for registered trademarks and copyrights.
EBM web sites: Much of the information described above can be found in greater
detail at a number of evidence-based medicine websites, such as the Centre for
Health Evidence (http://www.cche.net/). the Centre for Evidence-based Medicine
(http://www.cebm.utoronto.ca/). and the Oxford Centre for Evidence-based Medicine
(http://www.cebm.net/).
Appendices 293
APPENDICES
ORAL EXAM TEST-TAKING ALGORITHM
Do notdeviatefrom this algorithm unless prompted bythe examiner. You may ask ifa
specificsegmenthas beenadequatelycovered,howeverdonotassumeanythingunless
theproctorindicatesso.Startwiththehistoryandphysical(H&P)examination,thenmake
adiagnosisanddescribeatreatmentplanandfollow-up.
History and Physical
Chiefcomplaint
Natureofsignand!orsymptom
Locationofsignand/orsymptom
Durationofsignand/orsymptom
Onsetofsignand/orsymptom
Courseofsignand/orsymptom
Aggravatedby(activitiesorcircumstances)
Treatment(whathasbeentried,helpfulornot)
PreviousMedicalHistory,Medications,Allergies
SurgicalHistory
SocialHistory,Occupation/Avocation,FamilyHistory
PhysicalExam
VitalSigns(Temp,Pulse,Respiration,BP)
Vascular
Neurological
Dermatological
Orthopedic
Biomechanical
X-ray,andotherclinicalordiagnostictesting
Differentialdiagnosis
Considerconfirmatoryconsultationorothertesting
Diagnosis
TreatmentOptionsand Plan
Non-surgicaltreatment
Pharmacological
Biomechanical
Physicaltherapy
Surgicaltreatment
Preoperativepreparation
Intra-operativeplan
Postoperativeplan
Altercareinaccordancewithclinicalresponse
294 Appendices
INFORMED CONSENT
Informed consentisacrucial partofadequate patientpreparation foranyprocedureor
operation,and should be written,signed bythe surgeonorperson explaining the case,
witnessed,dated, andtimed.The components ofinformed consentinclude, butare not
limitedto,anexplanation,inlayman'sterms,ofthefollowingpoints:
1. Goalsandobjectivesoftheplannedprocedureoroperation.
2. DiagnosiS(whatyouaretreating).
3. Planned procedureandanesthesia.
4. Potential risks and complications (such asinfection,recurrence ofpain &lor
deformity,newand/orpermanentpain&lor deformity,overcorrection,stiffness,
weakness, instability, scar pain or disfigurement, nerve &lortendon injury,
hematoma, phlebitis and pulmonaryembolism, bone orhardware breakage,
prolongedswellingorslowwoundhealing,difficultywalking,andotherconcerns
pertinenttotheindividual'sspecificcase(cardiacarrest,severebloodloss,etc.).
5. Postoperative course and rehabilitation(ambulatorystatus,bandages, casts,
shoes,timeofffromworkorschool,ordriving).
6. Therapeuticalternativesandsurgicaloptions.
7. Noguaranteesaregivenregardingan outcome.
8. Otherpointsmaybemadedependinguponthespecificmeritsofthecase.When
using anew or experimental drug or technique (not FDA labeled for the
application),thisfactshould benotedinthewrittenconsent
9. Intenttohaveobserversintheoperatingroom,ortoimagethecase(photo,video)
shouldbenoted.
HOSPITAL ADMISSION ORDERS
Standardadmissionordersmayinclude:
1. AdmittoserviceofDr.
2. Dr.__formedical management(admissionto aspecific service mayvary
depending upon hospital bylaws, rules and regulations, and staff privilege
delineation).
3. Diagnosis:__.
4. Condition:_(stable,guarded,criticalorurgent,emergent).
5. Resuscitationstatus:__(full.orotherwise).
6. IVaccessand fluids("IVD5LR atKVO [keepvein open]via 18 gaugevenous
catheter[specifypreferencesl."
7. Shave andprep[specify]preop.
8. ActivityandWBstatus[specify).
9. Diet[specify].
10. NPO after2400preop[coordinatewithdietary).
11. Labsandancillarytesting[specify].
12. Medications[specify].
13. Consultations[specify).
14. Suppliestobedside[specify].
15. Socialservicesfordischargeplanning[specify).
16. Otheritemsspecifictothecaseathand[woundandskinisolation,etc.].
Appendices 295
HOSPITAL POSTOPERATIVE ORDERS
Standardinitialpostoperativeordersmayinclude:
1. Vitalsignsj"VSqshiftafterreturntofloor").
2. Activity("CBR(complete bed rest)withside rails up";"absolute Non-weight
bearing operatedfootatalltimes";n BRP Non-weightbearing operated foot
with assistance" ; " PT for gait and transfer training Non-weight bearing
operatedfoot";"AssistwithfirstOOB (outofbed) activity";Danglefeetover
bedsidewhileseated3-5minutesbeforefirstOOB activity").
3. IVfluids("maintain IVD5LR[orotherIVfluid asindicated]atKVO [orfasterrate
asindicated]untilfullyreactive/stable";"converttoheparinlockafterDIC IV").
4. Medications, considerations include antibiotics, analgesics formoderate and
severepain,anti-inflammatory,musclerelaxant,anti-emetic,stoolsoftener/bowel
stimulantsedative/hypnotic,otherindicatedmeds.aswellasthepatient'sregular
meds.
5. RespiratorytherapyrTriflowincentivespirometryq1hourwhileawake,instruct
andencourage").
6. Drain management("monitor drain/s [TLS, Hemovac or Jackson-Pratt] and
record outputchangewhen2/3fulloratleastqshift").
7. Diet(regular,diabetic,restrictedcalorie,lowsodium,asindicated).
8. Discharge planningrsocialservicesforhome antibiotic [specify],labtesting
[specify],P.T. [specify],andwoundcare[specify]").
9. Radiographs (specifyviews,weightbearing statusand anyspecial attention
items).
10. Other orders, such as supplies to bedside, consultations, physical therapy,
notification ofthe attending internistor general practitionerof the patient's
postoperativestatus,andanyotheritemsthatarespecifictothecaseathand.
HOSPITAL DISCHARGE ORDERS
Standarddischargeordersmayinclude:
1. Discharge__(specifywhen,or"atthediscretionof"whomever).
2. Dispensewritten and oral postoperativeinstructions(separateform detailing
activities,medications,homeorspecialcare,problemstobe awareoforonthe
lookoutfor,follow-upappointments,homehealthcare,etc.).
3. Dispenseprescriptions(specify).
4. Ambulatorystatus(specify).
5. Otherpertinentitems.[AED1]
296 Index
A
Abdomen 120,127
Abduct 234
Abduction 70,106-9,112,176,214,217,232,
234-5,274,276-7
Abductor
digitiquinti 6,13
hallucis 6,13,16,18,130,191,208-9,231-2,
234-5,237-8,255
Abductorhallucis
musclebelly 208
recession 231-2,235,238
AbductorhallucisMedial 13
Abductus IDS, 114,171,176,189,192,217,
225-7,232,234,259
pes 225-7
ABI(ANKLE-BRACHIALINDEXI 53-4
Ablation 60,72,138
Absorbablefixation 148,170
Absorbablesuture 123,177,207,209,246,m
Absorption,primarybonecallus 25
Accommodativefootorthoses 161,223
Achilles 11,102,202-4,207,209,237,241,255
tendon 11,13,113,129-30,135,154,198,
201-5,207,213,238,241,254-5,272
Acid
fast 41,100-1
uricacid 63-4,97,99
Acidosis 60,85,95,99
AClS(AdvancedCardiaclifeSupportl 82,
85-7
Acrallentiginousmelanoma 75
Acrallentiginousmelanoma(AlMI 75
Acromegaly 39,99
Actinic 39
Activitiesofdailyliving(ADLs) 283
Acuteadrenalcrisis 83
Acutegoutyarthritis 63-4,99
Acutemetatarsalfracture 258
Addison'sdisease 83,99
Adduct 196
Adduction 70,106-9,161.166,172,191,193,
214-9,232,235,237,239-40,274,276-7
Adductor
canal 17,32
hallucis 6,8,13,17,175,255
tendon 175
Adductovarus 112-3,166,196
Adductus 106,112,114,172,179,183,191,215,
217,225,232,234-7,240,242
Adenopathy 38,59,76,81
Adherent 12,58
Adhesion 67,111,127,141,185
Adhesiveskinstrips 124-5
Adjacentmetatarsalfracture 262
Adjunct
procedures 176-7,192,195-6,220,288
radiation 72,74,79
ADLs(Activitiesofdailyliving) 283
Administration 31,45,55,58,60,81-6,88,93,
118,122,160,244,248,256
Admission 46,294
Adnexae 33
Adrenal 83-4,158
Adrenergic 31,53
Advancedcardiaclifesupport(ACLS) 86-7
Aerobic 40-1,46,67,100,116,282
Aerosolbronchodilator 82
Aftercare 139,142,144,146,225
Age 37-8,42-3,56,65-6,69,72,74-5,80,107,
112,131,158,165,171,202,205,214-5,218,
232-3,235,237,239-43,254,261,272,288
Agents 31,47-9,54,82,157-60
Agglutination 62-3,96
Agranulocytosis 159
AHO(AcuteHematogenousOsteomyelitis) 42
AIDS(AcquiredImmunodeficiencySyndrome)
51-2,74
Aigner'ssyndrome 35
Aiken-MuellerEpiphysealPlateFracture
ClassificationSystems 281
Ainhum 34,38
Airway 81-2,84-7,118,244,248
obstruction 84-5
Akin
osteotomy 176-7,187,232
procedure 176
Albumin 63,100
Alcoholwithdrawal 84
Alcoholickeratosis 34
Alkalinephosphatase 79,80,99,100
Allergen 36,81-2
Allergic 35-6,38,81
Allergy 95,157,189,258
Allodynia 70,255
Allogeneic 127,131-3,217-8,227,273
Allograft 131,133
Alloimplant 131
Alloimplants 131.133
Allopurinol 37,64
ALM(Acrallentiginousmelanoma) 75
Alopecia 36
Ambubag 87
Ambulation,early 57
AmericanCollegeofFootandAnkleSurgeons
285,291
Amide 85,157-8
Aminophylline 82
Amphotericin-B 48
Ampicillin 49-51
Amputation,transmetatarsal 211.213
Index 297
Amyloid 36
Anaerobic 40-1,46,49,51,67,100-1,116
Anaerobicinfections 40-1,49,51
Anaerobicmuscleinfection 41
Analgesia 58,116,119,158-60,199,248
Anaphylaxis 81-2
Anastomoses 14,18
Anatomicdissection 154-5,203
Anemia,pernicious 65,95,100
Anesthesia
general 57,84-5,118,121-2,157-60,200,244
spinal 118,160
Anesthesiologist 116-8,121,158,161
Aneurysmalbonecyst 78,81
Anginapectoris 85-6
Angiofibroma 73
Angiogenesis 22,133
Angiography 53,106
Angiolipoma 38,73
Angiology 17
Angioneuroticedema 81
Angle
intermetatarsal 172,191,234
talar-firstmetatarsal 237
total 198,201-2
Angulardefonmity 114,193,276,279
Anhydrosis 65
Ankle 5,10-2,14,16-8,20,30,32,36,42,48,53-
4,56,58,62,64-5,74,89-92,94,105,107-8,
114,121,129-30,134-7,140-1,146,148,152,
154-5,157,161, 199,203-9,212-4,219-20,
223-8,235,237,241,249-51,254,262,264-5,
270-6,278, 282, 288
arthrodesis 136,228
arthroscopy 134-7
dorsiflexion 6,54,113,115,142,144,201, 205,
219-20,249,254
equinus 65,69,91,107-8,113,142,146,194,
204-7,214-5,223,237,240
osseous 146,207
spasticposterior 142,146
fracture 225,249-50,275,283,291
repair 275
fractures 147,225,250,258,273-4,276-7,283
displaced 276
status-postORIF 2B3
fusion 225-8,273
instability 225-6,250-1,273
inversion 212,272-3
joint 94,108,219,270,274-6
labrummedia 135
medialoblique 90
mortise 5,205,237,274-5
plantarflexing 115
plantarflexion 5,103,204
activeopen chain 254
sprain 32,113,272, 283
surgery 50,56,119,121,123,138,148,154-5,
214-5,217,219,221,223,225,227
systolicpressure 105
Ankle-brachialindex 53-4
ANKLE-BRACHIALINDEX(ABO 534
AnkleDisability 282-4
AnkleligamentousInjury 250
Ankle andPantalarFusion 225
Ankle/armindex 105
Ankylosingspondylitis 64,96-8
Ankylosis 26,62-4
Anonychia 39
Anorexia 84
Anoxia 81,95
Antacid 121
Antalgicgait 251
Anterior 5,6,10,16-8,64,135,137,149,153,
204,207,219,226,237,239,250-3,255-6,272,
274,277
cavus 142,167,193,219
flexible 142
drawer 5,91,134,251
lateralmalleolarartery 17
margin 154,213,216,224,226
muscleweakness 144
portion 5,6,15H,205,217,237
andposteriortibialarteries 17,153
talofibularligament(ATFL) 250
tibialartery 9,17-8,154
courses 17
Anteromedial 135
Anteversion 111-2,114,214,242,250
Anti-inflammatory 31,117,121.184,194,243,
260,295
Anti-streptolysin0(ASO) 53,97
Antibiotic 42,45-6,48-9,51.53,66-7,101,116,
119,128,133,154,163-4,189,245,248-9,258,
295
beads 45
prophylaxis 66,248-9,258
therapy 42,45,48-9,67,119,128,154,258
empiric 45-6,49
oral 119,154,16H
Antibiotics 41-2,45-7,49,53,58-9,67,95,101,
116-B,163,258,295
oral 67,163
Anticoagulation 27,58-9,98
Antiemetic 159-60
Antimetabolite 27,95
Antiplatelet 53
Antitrypsin 61
Anxiety 67,83,85,88,159
Aorta 17,53-4
AP SO, 220,225,227,240
view 167,234,237,239-40,265,271,276
298 Index
Apex 164,179,185,198,202,219-21,225,232,
234
Aplasticanemia 95
Apnea 85-6
Aponeurosis 113,205-6,255
Apophysis 1,2,199,202,243,261
Application 28-9,46,54,58,85-6,120,128,133-6,
138,147-8,151,155,163,179-80,183,192-4,
200-1,209,229,248,254,259,276,285,294
Apropulsive 175,184,188-9,213,223,254
Ar 7,15,19,21.32,169
Arc 108,172
Arch 5,18,20,54,69,128,146,161,191,202,
214-7,225,234,239
Arcuateartery 18
Areflexia 68-70
Argon 138-9
Aromaticspiritsofammonia 81
Arrectorpili 31,33,38
Arrest 87
respiratory 85-6,158
Arrhythmia 53,121,158
Arsenical 35
Arterial
doppler 120
pulse 104
Arteries 17-8,53-4,105,140,153,198,270,279
dorsalispedis 17-8
externaliliac 17
lateraltarsal 17-8
Arteriography 74,79
Arteriosclerosisobliterans 52-3
Artery 9-11,14,17-8,53,85-7,105,121-2,129,
153-4,158,171,198,209-10,270,279
Arthritis 26,34,36,40,42-3,48,61-7.84,92,94,
96-9,111,134-5,188-9,193-4,199,200,208,
221,223-4,228,243,263,270,272
Arthrodesis 26,66,68,110,132,136,140,142,
144,148,152,168,170-1.181-2,186,168-9,
191-2,194-5,214-7,220-1,223-5,227-8,233,
235,237,239,241-3,261,270,278
bonegraftextensioncalcaneocuboid 217
cuneiform-firstmetatarsal 217
interphalangeal 170
metatarsocuneiform 181
stmetatarsal-cuneiform 11
Arthrofibrosis 67, 137
Arthrogram 134
Arthrogryposis 240-1
Arthrology 2
Arthropathy 65,98,189
Arthroplasty 73,168,188-92,223,228,232-3,
259
Arthroscope 134-1
Arthroscopic 134-7,207
Arthroscopy 92,94,134,136,139
metatarsophalangeal 134
Arthrosis 26,188,214,220,225,228,242,251,
270,276,278
secondary 242
Arthrotomy 61,134,136
Articularsurface 26,135,170-1,176,185-6,190
Articulations,stmetatarsal-medialcuneiform
2
Aseptic 41,119,189,228,244
ASO (Anti-streptolysin0) 53,97
Aspirate,bone marrow 132,134
Aspiration 41-2,64,67,73,79,80,118,122,157,
251
Aspirin 53,80,96, 122
Assessment 48,58,11,89,90,103,105,101,
121,159,171,212,220,244,248
functional capacity 282
Assessors 287-8
Assistance 117,283-4,295
Asthma 35,81-2,84,95,160
AtasoyfJap 246
Ataxia 39,68-9,103-4,219
Ataxic 70, 103
Atelectasis 118,122
ATFl 5,135,250-1,253
Athetoid 70,103,219
cerebralpalsy 219
Atopic dermatitis 35
Atracurium-besylate 160
Atraumatic
needle 124
technique 144,147
Atropa belladonna 160
Atrophicnonunion 21-8
Atrophic nonunions 27-8
Attachment 198,200,273
Atypical 58
Aureus 40-2,41,49,66-7
Auscultation 118,121
Auspitzsign 34,36
Austeniticstainlesssteel 141
Austin 179-80,183,185-6,189,198
osteotomy 179-80,185-6,189,198
procedure 179
Authors 287-8,290-2
Autogenous 26,127-9,131-3,182-3,186,191,
217-8,233,237,248,259,262,270,273,278
Autonomic 30-1,33,65,69,84,101-2,208
AVfistula 242
Avascularnecrosis 26,92,196,226,241,210-1
AVN (Avascularnecrosis) 26,92,177-9,183,
185-6,196,226,241,270-2
Avulsion 1,2,30,136,163-5,245-6,249,251,
259-60,262-7,273-4,276-7,279
fracture 1,2, 136,260,262-3,266-7,273-4,279
Axes 106-7,109,111,240
Index 299
Axis 20,23,78,84,88,106-13,125-6,150,167,
176-9,181,185-6,189,196,220,234,240,250,
261,274
frontal-transverse 107,111
long 20,23,111,125-6,150,176-8,189,220,
234, 240, 250, 261
mechanical 107
ofmotion 23, 106
pronatory 108-9
Axon 30,74
Axonotmesis 30-1
Axons 30,199
Azithromycin 49,50
AZT 52
Aztreonam 49,51
B
Babinskisign 102
Bacteria 36,42-4,50,66-7,99,101
Bacterialinfection 98
Bacteroides 40-1,49,51
Baker
and Hill procedure 215
tongue-in-groovegastrocnemiusrecession
142
Bamboospine 65
Bankhart 237
Barbiturate 82,85
Barometric pressure 62
Basal
cell nevussyndrome 35
ganglia 158,242
Basalcellcarcinoma 72, 125
Basalcellcarcinoma(BCC) 72, 125
Base 1,2,4,9-11,20,23,65,125,130,168,
170-1,176,182,201,226,231,260-4
enclavement 187
metatarsalosteotomies 175
wedgeosteotomies 182-4,235
Basiccardiaclifesupport(BClS) 86
Basic Pathophysiology 22-3,25,27,29,31
BCC(Basalcellcarcinoma) 72,125
BCLS(Basic CardiacLife Support) 82,85-7
Beads 45,67, 154
Beam 89,90,139
laser 138-9
Beats 88
Bed 33,39,40,56,121,164,245,295
recipient 127-9
Bedside 294-5
Beefy 42,45-6,127-8,244
Belly 11-2,121,251-2
Benign 38,73-5,81,242
Berman-Gartland procedure 235
Berndtand Hartyclassification 272
Beta-hemolytic 40
Bilirubin 58,100
Bioabsorbable 148,170,177
Biomechanical 106,112-3,167,187,192,199,
202-3,214,262-3,293
Biomechanics 106,111,114
Biopsy 41-2,47,59,68,71-2,76-7,79,124-6,
132,134,136,139
incisional 72,77,124-5
punch 77, 125
shave 125
BiopsyTechniques 71-2,124
Bipartitesesamoid 261
Birth 1,59,75,107,111-4,232-3,239-40
Bisection 171-2,234,239
Bite 64,249
BK
cast 144,146,203,206-7,235,260,262,265,
267,271-2
non-weight 146,262,270,272-3
weight 142,272
Bladder 69,85,118
Blairtibiocalcanealfusion 227
Blastomycoses 48
Blind 287-8
Blister 136,247-8
Blisters 53,247-8
Blixcurve 140-1
Blood 36,59,61,92,99,122,155-6,244
cell 27,94-5
pressure 85, 118,155
supply 12,129,144,270-2,279
urea nitrogen(BUN) 99
Bluetoe 120
Body 5,16,18,62,71,75-6,84-5,91,106,112,
123-4,129,139,160,198,202,217-8,225-6,
237,247,265,267-72,290
foreign 45-6,84,92,244
massindex(BMI) 288
weight 56,115, 161
Bohler'S 265
Bone 12,20,22-9,36,42-4,47,64,66,71-2,
77-81.91-3,100,123-4,128,131-3,138,
148-51,153,156,180,185-6,188,190,195,
200,217,229,231,233,241,244,247,249,
255,257-9,268-9,278-9,294
atrophy 61,71
autogenous 131-3
basedwedgeresectionof 220-1
biopsy 41-2,47,79
block 132,215
callus 24-5,27,257,259
destruction 77-9
fixation 147-8
fractured 66
fragments 25,66,149,156
giantcelltumorof 78
300
Index
graft 26,131-3,152-3,182-3,186,215-8,221,
227-8,233,237,259,262,270
allogeneiccorticocancellous 217
autogenous 26,131-2,182,217,237,270
healing 131-3
substitute 182-3
substitutes 132-3,182-3
grafting 27-8,131,133,194-5,228,233,249,
259
growth 28-9,132
new 78
stimulation 26-8,66,133,262,271
electrical 26-8,66,262,271
healing 24-5,27-8,84,133,147,149,153,156,
178,183,188,193,233
callus 25
primary 25,27,149
secondary 25, 153
infection 38,42-3,221
long 24,42, 59,78-80,257, 278
non-living 131
normal 78
osteoporotic 193
resection 188-9,213,227-8
scans 24,26-8,47,93,134,199,257,261,263
stock 175,181,189,192,221,223
target 29
tumors 77-9
Bonecultures 41-2
BoneGrowth Stimulation 26-9,66,133,262,
271
Bonney-Kesselosteotomy 187
Booster 245
Border,plantarmedial 90
Bowen'sdisease 72-3
Bowleg 114
Braces 30,161-2,188,257-8,273
Brachymetatarsia 132,194,233
Bradycardia 60,81,87-8
Braininjury 99
Branches 11,16-8,31-2,53,198,200,207,
209-10,212
medialcalcanean 16,18,209
muscular 14,16-8,199,201
properdigital 16-7,210
Breathsounds 118
Breathing
period 155
rescue 85-7
Bridges 25,30,152,255
Bronchial 118
Bronchospasm 81-2
Brownpaperbag 83
Bucholtzclassification 43
Budinsplint 167
Buechel-PappasUltraTotalAnkle
Replacement 228
Buerger'sdisease 54
Bulla 33
Bullet 114,220,249
Bullous 37,96
Bunion 63-4,110,113,161,168,171,175-6,182,
184,196
deformity 168,171,176,182
tailor's 196
Bunionectomies 175-6
Bunionectomy 175-6,189
Bunionette 112-3,161,171
Bunnell 124,141,254
Bupivacaine 82,120,158,212
Bum 66,100,129,139,160,163,247-8,256,279
Burning pain 70-1
Burrow 33,129
Bursae 12,255
Bursalprojection 201-3
Bursitis 64,175,193-4,196,199,201-2,210
retrocalcaneal 201-2
Butlerprocedure 233
Buttress
piate 152,270
plating 152
C
Caffeine 120,212
Caisson'sdisease 26
Calcaneal 47,9,16,18,31,66,90,114,129,
132,183,198,200-4,208,214-9,221,225,227,
239-41,243,249-50,254,265,267-70
axial 90,225,227,241,249,265
osteotomies 215,218
varus-producing 218
sulcus 9,215-6
tuberosity 4,6,200,208,267,269
tunnel 16,201.208
CALCANEAL FRACTURES 208,249,265,267-8,
270
extra-articular 265
suspected 90
Calcaneocuboid 4,5,10,66,217,238-9,241,
265,269
joint 4,217,265,269
Calcaneofibular 237,240-1
ligament 240,250
Calcaneovalgusfoot 239
Calcaneus 1,2,5,11,13,16,62,64,68,79,80,
89,90,106,108-9,112-4,133,146,154,166,
198-204,208,210,213,215,217-8,220-1,225,
227-8,23741,249,253,265,267-70
plantar 16
Calcium 45,66,97,99,133,154
carbonate 133
Index 301
pyrophosphate 66,97
Calf 16,53-5,58,114,118,129,202,206,208-9,
215
Callus 24-5,27,35,132,148-9,153,217,257,
259,261
distraction 132,153,217
fibrocartilaginous 25
painfulplantar 261
Canal 11.16,29,208
Cancellousbone 132,148,269,278
screws 149-50
Cancer 56-7,71-2,76,81.100,160,199
Candida 47
Capacitativecoupling 28
Capillaries 20,25,33,42,74,133,156,244
Capillary 22,24-5,33,35-7,42,74,98,133,156,
244
fragility 36
Capping 32,212
Capsaicin 31
Capsule 2,4,5,205,217,235,251
Capsulotomy 168,184,195,207,233,235,238
Carbontetrachloride 61,99
Carbuncle 34
Carcinoma 34,39,44,58,61,71-2,99,100,125
in situ 72
Cardiac
arrest 85-7,294
lifesupport
advanced 86-1
basic 86-7
output 88
Cardinalbodyplanes 106
Cardiogenicshock 248
Cardiopulmonaryresuscitation(CPR) 86-1
Cardiovascular 82,84,117
C-arm 91,116
Carotid 86-7
Carpopedalspasm 83
Cartilage 22,25,29,61,65-7,92,94,128,134,
136,138,171,173,171,185,188,190-1,225-7,
261,270,273,278-9
effective 171
CartilageHealing 29
Cartilageimaging 94
Cast 29,30,32,56,119,142,144,146-7,161,179,
188,193,202-4,206-7,216,223,225,235,237-
43,249,254,256-8,260-3,265,267,270-3,276
bearing 142,146,262,267,270,272
boot 260-1
immobilization,bearing 212-3
plantarflexed 254
Casting 66,114,116,167,205,235,237-40,242-
3,256,261
Casts 99,161,238,294
Catheter 45-6,59,88,118-9,122,161.256,294
Cathode 29
Cauda equinasyndrome 160
Causalgia 31,70
Caution 176,194-5
Cavernoushemangioma 58,74,139
Cavity 34,137,248-9
articular 137
Cavoadductovarus 220,250
Cavus
deformity 219-20
foot 192,203,205,224
Cc 82,118
CCJ 4,217,224-5,240
CO-4 51
Cefazolin 50-1,53,67,258
Ceftriaxone 49-51
Cells,viable 131-2
Cellulitis 41,49,59
Cellulose 156
Cement 190,228
Central nervoussystem 65,70,82,122
Cephalexin 49-51,164
Cephalgia 31,120
Cerclage 123,148, 188,270
Cerebral palsy 70, 103,205,219
Cervicalligament 5,9
CFL 5,237,25D-l,253
Channel 34,44,200,253
Charcot 44-5,60,63,65-6,88,93,98,153,161,
188,205,214,219,221,223,263
foot 65,221,223
Charcot-Marie-Toothdisease 65,68
Charnley 25,226,257
Chasingthebump 203
Cheeks 35,81
Chemoreceptortriggerzone 121
Chemotherapy 66,72,74,77,79,126,160
ChestX-ray 46,58,71,77,118,121-2
Chevron 179,182-3,195,198
osteotomy 182-3,195
Chickenpox 37,42
Chielectomy 184-5
Chilblains 53,248
Child 42,61,67,74,86,111,114,157,214,216,
229,238-9,242,279
Childhood 39,42,69
Children 41-2,47,49,66-7,79,80,99,110,113-4,
155,157,200,215,238,241-3,281
older 238,242,281
Chloroform 159
Chocolateagar 41,100-1
Cholesterol 100
Chondrocyte 29,191
Chondroma 79
Chondromalacia 135-6,139
Chondromyxoidfibroma 78-9
302 Index
Chondroplasty 136-7
Chondrosarcoma 78-9
Chopartamputation 213
Choreiform 103
Christman-Snook 253
Chronic pain 71,199,282
Ciclopirox 48
Cierny-Maderclassification 43
Cigarette 27,53-4,118,158
Cilistatin 49.51
Cilostazol 53
Cincinnatiincision 238
Ciprofloxacin 50-1
Circumflexfibular artery 18
Cirrhosis 61,96
Clarithromycin 38,49
Class,oculardamage 139
Clawfoot 233
Clawtoes 70,142,166-7,170,219-20,223
Clayton 223
Cleft 27,34,233,240,242
foot 233
Clindamycin 45-6,49-51,67
Clinicalevidence 27,103,170,193,285-6,289
ClinicalStage 76-7
Cloaca 44,92
Clonidine 31
Closed reduction 25,240,257,259-62,265,267,
270, 276,281
Closedreductionimmobilization 267
Closedsuction 156,227
Closing adductory
basewedgeosteotomy 198
osteotomy 176, 198
Clostridia 41, 245.258
Clostridium 40-1
Closure 31,45-6,77.125-7.156,165, 168,207,
212, 225, 231,272,281
Clotting 55,98,155-6
factors 55,98
time 98
Clubbing 39,40,47
Clubfoot 112,142,144,224,234,237-9
CMT 68, 104,142,144,242
disease 68-9
C-mucopolysaccharide 96
CN bar 241
C02 83,137-9
Coagulation 54,98,138
Coalition 92,184,215,224,240-2
Coalitions 92,241-2
Cobalt 147,190
Cock-uphallux 142,192,261
CoCr 190
Codliveroil 99
Codman'striangle 78,80
Colchicine 64
Coldinjury 53
Cole
osteotomy 221
procedure 220
Colitis 96,98
Collagen 12.22,26,28-30,38,61,95-6,100,
127-9,132,134,156,162
vasculardisease 26, 61,95, 100
Collagenation 22,24,30,127
Collataralligament 2,5,91.107,153,250-1
Collin'slesion 135
Color 42,67,70,75,98,244
Column 65,95,101,109,111,113-4,132,146,
186,214-7,219-21,224,238,265,269,278
lateral 146,215-7,220
Coma 59,60,82-3,85,256
Comatose 60
Comminution 92,258,267,269
Commoniliacarteries 17
Commoninfectingorganisms 40,66
Common peronealnerve 13-4,16,32,153,277
trifurcates 14
Community 48-9
Compartmentsyndrome 31-2,212,255-6
Compartments 10,255-6
posteriorleg 11
Compensation 107-8,112-4,282
Complement 97
Completebloodcount(CBC) 45,94
Completefractures 24,257
Complexregionalpainsyndrome(CAPS) 70
Complication 59,117-8,127,131,133,147,160,
176,182,191,210,217,228-9,232,241,248,
270,277
Compound nevus 37
Compression 25,29,30,119,147,149,151-2,
243-4,276,27B,283
axial 151
Compressions 87
Conditions 27,46,52,61,71,94,99,100,104,
113,118,120,136,160-1,163,184-5,191,
209-10,212,229,231,237,240-2,255-6,261,
273,286-7,294
Condyle 10-1.107,114,194-5,204
Condylectomy 194-5
Confusion 46,59,82-4
Congenital 58-9,104,107,111,165,194,214,
232,240-1
calcaneovalgus 239
curly(underlapping)toe 232
halluxvarus 232
hemihypertrophy 242
overlappingfifthtoe 232
verticaltalus 239-41
Index 303
Congenital Deformities 214,229
andJuvenile
Surgery 229,231,233,235,237,239,241,243
SurgeryCh 230,232,234,236,238,240,242
Congenitalhalluxabductus 232
CongenitalHalluxAbductusInterphalangeus
232
Congruous 173-4,177
Conjunction 40-1.45,55,59,50,66,68,74,79.
82,84,102,118,126,136,149,152,155,157,
160,168,175-7,182-5,193-6,201,216,224,
237-8
Connectivetissue 6,12,24,30,52,61,73-4,80,
96,155
disease 52,96, 155
Consent,informed 116,294
Conservativetreatment 68,73,199,209,235,
237,239,241,254
ConservativetreatmentofmedialTIS 209
Constipation 121-2
Consult 92,122
Consultation 46,52,58-9,68,71-4,76-7,79,84,
104,III,114,116-7,120-2,126,205,220,
244-5.282,293
Consultations
infectiousdisease 46,52
oncological 71-4,77,79.126
Contact 22,25,29.36-7,41,47.61-2.66,103,
108,115.124,127-30,133,138,147-9,156,
161,190,204,227,239,273
areas 127-30
dermatitis 36-7,47
Contract 88,127-8
Contracture 23.34.53.62,69-71.73,130,142,
146,166-8.170,191-2,196.205,207,213,232,
237,239,241.248,256
Contraindications,intermediatedorsal
cutaneousnerves 144
Contrastmedium 91-2,106
Convexpesvalgus 215,224,239-40
Convulsion 82-3,95
Coolingblanket 122
Coralhydroxyapatite 133
Core 26,72,122,149-50,228,248
Corneum 20,33-5,39
Coronary 85-7,121-2,158
arterydisease 85-6.122,158
Correction 25,68,110,117.141.167-8.170.
176-83.185-6,192.196.220-1,225,235-41.
257,260
ofHAV 175-7,180-1
Correctivecasting 235.237-40
Corrosion 147
Cortex 24,42,78-80.90,148-51,158,177-8,
182-3,185,195,201,218.221,223,225,235,
238, 252, 257, 269,277
far 150-1
plantarcalcaneal 221
Cortical
bone 81,92,147-8,150,178-9.187,272
intactmedial 181-2
screws 149,277-8
Corticosteroid 31,35,58-9,73,83-4.99,116,
202-3,209-10,212,221.223,242,249,256.
260
Corticotomy 153,217
Cortisol 84
Corynebacterium 41
minutissimus 41
Cotton 101.128.161.183.217
procedure 183
Coumadin 55,58,98
Countersink 150-1
Coverage 45-6,49,126-30,231,246
Coxa 114
CP(CerebralPalsy) 70,103.142,146,205,219,
237, 240, 242
CPpatients 70
C-peptide 60
CPR,CARDIOPULMONARYRESUSCITATION)
86-8.244
CPVP 214-6
Crater 23.272-3
C-reactiveprotein 96
Creepingsubstitution 133
Crescenticbase osteotomy 182
Crest,iliac 132-3
Cricothyrotomy 85
Crigler-Najjarsyndrome 100
Crisis 81,83,85
CRPS(Complexregional painsyndrome) 31,
70-1
Crust 33,72
Cruveiler-Baumgartenerdisease 35
Cryotherapy 139
Crystals 83-4,67,92,97,99,199
C&S 41.45-9,67.100.119.244
C-shapedfoot 234
CT(Computerizedtomography) 47.90-2,94
CTscans 27-8.126.134.264-5
Cuboid 1,2.4.8.10.89.172,183.214.220-1.
224-5,234-5,237,239-40.262,264-5
Culture 40-1,48,51.97.100
and sensitivity(C&S) 100
Cuneiform 1. 2,4,8.10,12.63,109-10,172,
181-3,186,193.214,217,221,224,234-5,
237-9,241.263, 265
arthrodesis,metatarsal-medial 224
Cuneiforms 4,8,172,193.220-1.234,263,265
lateral 4.238-9
metatarsal-medial 224,265
Curettage 46,125,139,154,188.227
304 Index
Curette 125,244
Curly(underlapping)toe 232
Curvilinearincision 194,209,251
Cushing'sdisease 95.99
Cutdown 88
Cutaneousmelanomas 75
Cutting cone 25
Cuttingneedle 124
Cyanoacrylate 124.212
Cyanosis 36-7.52-3,81-2.85-6,120.212.255
CylindricalAkin osteotomy 177
Cyst 33,72-4.78.80-1,132,189.208
Cysticlesions 80
D
DANISWEBERCLASSIFICATION ofANKLE
FRACTURES 276
Dantrolene 85
Daptomycin 49
Darco 258
Darier'sdisease 35
DASA(DistalArticularSetAngle) 171,174
Days 22,25,30,44-5,48.50-1,57-8,64,84-5.97,
117-8,124,126-8,133,156,185,209,217,225,
239,256,258,260,263,277,281,287
Debridement 26,33,45-6,48,67,128,137,200,
204,244-5
cleansing 53, 119,245-6,249
Debris 40,66,99, 189
Decade 74-5,79-81
Decompression 26,31,45-6,134,191,201,256
Deepfascia 12,32,46,72,77,123,154,156,171,
200,203,206-7,224,251,256
Deepperoneal L4 13
Defects 30,34,52,98,125-6,128-30,220,229,
233,242,245-6,248-9,254
Deformity 4,25,62,105,110-4,142,163,166-8,
176,179,188-9,192,194,196,201,205,214-5,
219-21,228,232-5,238-40,257,294
equinovarus 69,213
flexible 167,214,221
pre-existingmetatarsusadductusskewfoot
217
sagittalplane 193
structural 112-3,174-6,185,192
Degeneration 30,65-6,73,134,141,175,187-8,
191,194,214,225,249
Degree 45,53,58,68,70,86,107,113,132,155,
160,167,172,178-9,181,186,189-90,219,
238-9,267,272
burns 247
Dehiscence 119,127,210,228
Dehydration 99, 121,248
DejerineSottasdisease 68
Delayed union 27,132,178-9,182,188,262
Delirium 82,84
tremens 84
Deltoidligament 5, 137,274,276
Demineralizedbonematrix(DBM) 133
Dendritic 20,33,75
Depicts 78,141,290
Depolarization 88.160
Depression 58,71.82,95,114,158-9,201,214,
265.267-70
fracture,joint 201,265,270
joint 269
Depthgauge 150
Dermal 22-3,33-5,38-9,127-9,138,156,244
Dermatitides 35
Dermatitis 35-8,47,58-9,95, 100
Dermatofibroma 73
Dermatome 128
Dermatomyositis 52,62,96-7,100
Dermatophiluscongolensis 34
Dermatophyte 36
Dermis 20,22-3,33,35-8,41,72.75-6,120,127,
139,206,247-8
reticular 33,76
Derotation 111,114,130
Derotationalabductorytranspositional
osteotomy(DRATO) 179
Desflurane 159
Desquamation 63,120
Deviations,standard 288-9
Devices 28-9,68,87,152-3,161,170,190,228,
292
Dextran 248
Dextrose 47
DFWO (Dorsiflexorywedgeostaotomy) 195,
220-1
Diabetes 38,53,56,59,50,93,99,lOa, 158,208
mellitus 53,56,59,60,93,99, 100,158,208
Diabetic 23,31,38,45-8,51,60,65,83,99,100,
103,105,210,295
peripheralneuropathy 60,65,210
Diagnosis 24,26,41,45,53,55,59,60,62-4,
67-8,71,74,77,79,89.98,116,119,125-6,
134,194,198,209,240,250-1,256-7,259,
261,263,282-3,286,291,293-4
DiagnosisandTreatmentofHeel Pain 291
Diagnostic
images 47,89
imaging 44,71.89,93,116
Diameter 18,28,33,36,75,80,125,148-50,153
Diaphoresis 61.81-4,86
Diascopy 74, 120
Diastolic 83
Diazepam 82-4, 141
Differential 26,30-1,45-6,58-9,63-4,67,72,
94-5,98,119,122,134,194,199,210,240,
259,261,263,293
Differentialcell count 67,94
Index 305
Differentialdiagnosis 26,59,63-4,67,194,240,
259,261,263,293
Differentialparalysis 30
Digitalarteries 18,105
Digt\:alnerves 14
proper 16,31
Digitalstabilization 68,168,188,194-5,220,223
Digits 10,15,34,39,47,68,120,166,168,170-1.
208,231-2,234,289
Diphenhydramine 81-2,248
Diphtheriacutis 37
DIPJ 166-7,246,259
Directvisualization 67,139,270
Direction,tendonchanges 12,254
DisalJility 71,210,282-4
Discharge 117,294-5
Disease 42,48,52,54,56,60-1,64,68-71,85,
87-8,96-7,242,2824
infectious 52,245
renal 59,63,95,97,99,100
symptomsof 283
Dislocation 170,240-1,244,249,259-60,263-5,
271
Disorders 36,65,68-9,198,291
Displacement 179,216,276,278
Disruption 29,30,59,71.91,128,183,210,251,
263,265,274,276
acute 250-1
Dissectingaortic aneurysm 83
Dissection 72,139,210,218.224,251,254,256
anatomic 154-5,203
Disseminatedintravascularcoagulation(Dlel
55
Distal I,10-1,16,18,26,40,42,77,104, 149,
153-4,168,175,177,186,193-5.209-10,213,
217,220,223,225,235,240,246,252,276
Akinosteotomy 177
metatarsalosteotomy 175
phalangealbase 232
phalangealtuftfractures 259
phalanx 10-1,33,65,80,165,172,246,259
portion 172,251-2,255
tibialepiphysis 281
Distalphalangealfractures 246,259
Distribution 30,286,289-90
Diuresis 58-9
Diuretic 63,99
OM (Diabetesmellitus) 53,56,59,60,93,99,
100,158,208-9
DNA 96
Dome 90-1,137,205,271-2
Donor 127,131,191
site 126-8,131,133,191,217
Doppler 53,55,105-6,120,129,213
Dorsal 4,10,14,17-8,38-9,110,167,170,177,
184-5,190,195-6,210,223,229,232,240
arm 179,186
bunion 63,110,113,184
exostosis 193-4,241
incisions 223-4,265
interossei 9,13
10 muscles 17-8
metatarsalarteries 18
Dorsal-distal 180,195
Dorsalispedisartery 17-8
Dorsiflexion 5,6,54,91.102,106,108,lID-I,
113,115,142,144,166-8,173,184-5,187-8,
190-1,197,199,201,205,207,219-20,237,
239,249,254, 261, 273
Dorsiflexors 240
Dorsiflexorywedgeosteotomy 195,220
Dorsolateral dislocationofmetatarsals 264
Dorsomedial 181,184,265
eminence 171,176
Dorsoplantarfoot 89
Downey 204,206
Doxycycline 49,50
Drain 12,20,45-6,67,72,117,156,209,225,295
Drainage 40-1,44-7,59,67,119,122,127-8,
156-7,212,245,247-8
Drains 20,45-6,116,156,225
DHATO (DerotationalAbductoryTransposi-
tionalOsteotomyl 179
Drill 149-51.170-1.189,201,249,251-3,273
holes 151,170,189,251-3
Droperidol 159
Dropfoot 69,70,103-4,113,142,144,146,161,
167,194,205,219-20,250
Drug reaction 37-8,62,95-6,122
otest 49
DTIL 210,212
Duhring'sdisease 37
Duplication 231
Dupuytren'spalmarcontracture 73
Duvries 16,200
DVT 54-6,58,122
prophylaxis 55
Dwyer 68,218,220-1
Dynamiccompressionplate 151
Dynamization 153
Dysfunction 31,37,39,41,59-61,67,70,74,98,
102,155,158,214,221,228-9
Dyshidrosis 36
Dyskinesia 62, 199
Dyspnea 58-60,82,86,118
Dysrhythmia 68,85-6,88,121,160
Dystonia 71.242
musculorum 242
E
EBGS(Electricalbonegrowthstimulation) 26-8,
66,262,271
306 Index
EBM(Evidence-BasedMedicine) 285-92
Ebolavirus 36
Ecchymosis 36,260,265
Eccrine 20,33-9,72
poroma 72
spiradenoma 38
Eclampsia 99
Econazole 47
Ecthyma 41
EDB 6,9,14,224
Edema 27,34,38,41.46,49,53-4,58,60,65,71,
81,104,121.127,161,163,247-9,251,254-5,
263,276-7
EDL(ExtensorDigitorumLongus) 9,10,13-4,
17,103,233,240,251,256
Effects,stmetatarsalbaseosteotomy 110
EHL
andTAtendons 193-4
tendon 9,17
EHL(ExtensorHallucisLongus) 9,10,13-4,17,
103,110,176,189,240-1,256
Elastin 128
Electricalbonegrowthstimulation(EBGS)
27-8,262
Electrocardiogram 88
Electrocoagulation 155
Electrode 71,104,213
Electronegativity,fracturehealingdisplay 28
Electroneurodiagnostic 68
Elevatingmetatarsalosteotomy 195
Elevation 33,37-8,58-9,69,85,94,100,119-21,
155,212,243-4,270,276,283
Elevatus 106,110-3,176,179,181,184,186-7,
194
Elmslie 253
Embolism 52,54,58-9,85,95,100,106,118,120,
294
Emergence 32, 159
Emergency 61,81,85,87-8,244,255-6
medicalservice(EMS) 81,87
Emesis 121,159
Empiricantibiotictherapy 45-6,49
Encephalitis 83
Enchondroma 78-9
End-to-end 170,254
Endocarditis 36,95
Endoneural 30
Endoprosthesis 26,66-7,189-91,193,223,226,
228,261
implantation 189,223
Endoscope 137,201
Endoscopic 134,137,200,210
plantarfasciotomy(EPF) 134,137,200
Endoscopy 92, 134
Endotenon 12
Endotoxic 67,100
shock 100
Endotoxin 120
Endotrachealintubation 85,81,160
Endpoints 287-8
Enema 121
Energy 26-9,89,91,138,199,248
Enflurane 121,159
Enoxaparin 57
Ensheathing 32
Enterobacter 40,49
Enthesitis 65, 194,200,210,221,263
Entrapment 31-2,52,73,102,104,122,133,
140-1,199-201,208-10,212,249,270
peronealtendon 270
Eosinopenia 95
Eosinophilia 95
Epalrestat 31
EPF(Endoscopic PlantarFasciotomy) 134,137,
200
Epidermal 22,33,36-7,39,71-2,15,125,129
Epidenmis 20,22-3,33-4,37,12,75-6,120,127,
247-8
Epidermoid 33,72,80
Epidermolysis 37
bullosa 37
Epiduralanesthesia 160
Epilepsy 83
Epinephrine 81-2,87,120,124,155,151-9
Epineurium 13,212
Epiphysealplatefractures 278-9,281
Epiphysiodesis 183
Epiphysis 1,42,79,80,177,184,278-9,281
Epitenon 12
Epithelialcell 22
Epithelioid 38,74
Equinovalgus 69,10,237,239
Equinovarus 69,70, 142,144,205,213,219,235,
231,240,242
foot 235
talipes 219,237,240,242
Equinus 65-6,69,91,103,106-8,110,113-4,142,
146,184,194,204-7,214-5,220-1,223,234,
231,239-40,242,255
deformity 66,113,205
gastrosoleal 205,201
,
gastrosoleus 142,205,215,240,242
isolatedmetatarsal 194
Ergotism 52
Erosion 26,33,62,84-5,80,135-6,172,190,199
Erythema 22-3,34-8,41,45-6,54,63, 125, 163,
193,247-8
muttiforme 37
nodosum 38,63,125
Erythrocyte 45,95
sedimentationrate(ESR) 45,95
Erythromycin 41,49
Index 301
Esmarchbandage 155
ESR(Erythrocytesedimentationrate) 26,45-6,
63,72,95-6,134
Essex-Lopresticlassification 268-9
ESSEX-LOPRESTICLASSIFICATIONof
CALCANEALFRACTURES 269
Ester 158
Esters 157
Esthesiometer 80,65,101
ESwr(ExtracorporealShockwaveTherapy)
199,200
Etiologies,unknown 35-6,38,80
Etiopathogenesis 219
Euglycemia 60
Evans 132,146,216-1,239,252
EvansCalcanealOsteotomyand BoneGraft
217
Eversion 5,106,108-9,112,124,196,209,214-5,
241,249-50,274,216-1
Evert 109-10,196
Ewing'ssarcoma 18,81
Ewing'ssarcoma 78
Exacerbation 65
Examination 67,81,89,106-10,293
Excision 27,30,32,45,48,59,12-5,71.79,
125-6,131H,164-5,170,175,181,191-2,
196,202,209-10,212,223,232-3,235,237,
241-2,248,259-61,272-3
definitive 77,126
radical 73-4
Excisionalbiopsy 41,124-6
Excochleation 125
Excoriation 33,35
Excretion 63-4,99
Exercise 53,60,88,95, 240,255,262,282
EXFX(Externalfixation) 25,66,152-3,227,
233, 258-9,265,278
Exostosis 48,63,108,136,165,183-4,189,
193-4,196,203,205,207,241,259
retrocalcaneal 203
talotibial 108,136,205
Exotoxin 41
Exposure 20,85,89,126,134,138,164-5,194-5,
200,210
Extension 64,70,106-8,129,184,194,217,267,
269,279
Extensor 2,9,10,12-3,18,35-6,70,103,113,
142,166-8,170-1,194,205,219,256,263
digitorum
ethallucisbrevis 9
longus 9, 10,13,256
hallucis
accessorius 10
longus 9,10,13,256
substitution 103,113,142,166-7,170,194,205
Extent 45-6,163,204,247-8,258
Externalfixation 25,66,152,227,233,258-9,
265,278
Externalfixation(EXFX) 152
Externalfixator 29,152,217,259
Externalneurolysis 32,201,209-10
Externalrotation 70,106-7,281
ExtracorporealShockwaveTherapy(ESwr)
199,200
Extrapyramidal 219
F
Fabry'sdisease 52
Factors 54-5,98,132-3,163,204,259
Facultative 40
Familial 39,68,103,229,232-4,237
Fanconisyndrome 99
Fascia 10-2,16,20,23,32,46,68,71-3,77,
123-4,126,128-9,137,154-6,171,198-201,
203,206-7,209,221,224,238,244,251,253,
255-6,262
crural 10
Fasciculation 85, 103
Fasciculi 12,30
Fasciitis 41,134,199,282
Fasciosis 198
Fasciotomy 134,137,199-201,255-6
endoscopicplantar 134,137,200
Fastidious 101
Fatembolism 59
Fatal 37,39,54
Fatiguefracture 262
FCA 282-3
FDL(FlexorDigitorumLongus) 7,11-3.16,18,
103,141,166,237.256
FDLtendons 7
Febrile 69, 122
Females 35,52,63,65,68,94,96-7,119,165,
243,267
Femoral 53-4,104,114
artery 17,53
condyles 107,111,114
Femur 11,26,42,80,107,111-2,114,134
Fentanyl 159
Fever 36-7,40.45,59,61-2,67,88,95,97-8,
118-9,122
FHL(FlexorHallucisLongus) 11-2,18,103,
110,146,237,256,267
Fibrillation 31,65,68,86-8,104,136
ventricular 86-8
Fibrinogen 55,63,95
Fibro-osseous 31.208
Fibroblast 132-3
Fibrocartilage 29,165,185,191,273
Fibroma 73,78-80
Fibromatosis 24,73,126
Fibroplasia 29,30,84,122,189
308 Index
Fibroproliferative 22,29,30
phase 22
Fibrosarcoma 13,18,80
Fibrosis 30-1,35,59,62,122,128,134,147,160,
208-9,242
Fibula 1,6,10-1,14,18,32,133,137,153-4.
226-7,249-53,273-1,281
Fibular
fracture 274-5.278
sesamoid 4,8.172-3,175.191
Fig 2,4,6-9,14,16,18,20,32,44,101,247,
249-53,255,257,263,265,268.271,278-9
Figure-of-eight 108
Figuretitles 291
Film 89-91
cassette 89-91
Fine needleaspiration 79
Firstintermetatarsal 18,172-3,234
Firstmetatarsal 90.130,171-2,176-8,180-1,
183,185-7,191,193,220-1,223,240-1,263-5
articular 189-90
axes 240
head 26, 171,176,182-4,181,235
plantarflexes 173,190
FirstMetatarsal-CuneiformArthrodesis 182
FirstMetatarsal PlantarflexoryOsteotomies
186
FirstMetatarsocuneiformExostosis 193
Firstmetatarsophalangealarthrodesis 188
FirstMetatarsophalangealEndoprosthesis
189
FirstMetatarsophalangealJoint 4
FirstMetatarsophalangealJointDislocation
260
Firstray 109,167,175,182,184,186-8,190,192,
194,219-21,223-4,234-5,250-1,260
plantarflexed 202,220,250,261
Fissure 34,136
Fistula 34,58,242
Fixatedfracture/osteotomy 151
Fixation 25,27,45,49,66,91,96,117,119,129,
132,136,144,147-54,170,177,179-83,185-7,
192-4,196,198,218,220,224-5,227,233,
257-9,261,265,270,272-3,276-8,281
external 66, 152,233,258-9,278
skeletal 129,147,258,270
Fixators,external 29,152-3,217
Flag 63,184
Flaking 47,65
Flaps 45-6,127,129-30,140,244,246,252,255
Flatfoot 214-6,219,241
flexible 214-6
Flexibleflatfoot 214-6
Flexion 64,70.103,106-8,111,113-5,120,184,
204-5,239,256,267
Flexor
digiti minimi brevis 8,17,255
digitorum
brevis 6, 13,207
longus 11,13,256
hallucisbrevis 8,13
hallucislongus 11,256
plate 2,166,168,170,185
retinaculum 11. 16,18,32,208-9
set 167
stabilization 63,111-3,166-1,170,205
substitution 144,166,170,194
tendontransfer 170-1
FlexorhallucisbrevisMedial 13
Floatingtoe 194-5
Flora 43
Fluids 33,61,92,117-8,120-1,294-5
Fluorescein 244
Fluorescence 41,244
Follicle 20,33-4,72
Foot
charcot 65,223
elephant 27
insensitive 47,66,161
intrinsicminus 65,209
madura 48
medialoblique 90
normal 237,239
operated 117,295
orthoses 215,242-3
accommodative 161,223
molded ankle 161
pain 53
rheumatoid 214,221,223
supinated 114,267
trench 52,248
FootandAnkle
Disability 283
and RehabilitationCh 282,284
Disorders 291
FootAnkleSurg 289,291
Forceps 125,135,140,149,244
Forefoot 23,63,103,105,107-10,112-5,142,
148,154-5,157,161,166,184,188,192-4,196,
202,205,208,210,217,219-21,224-6,237,
239-40,255,264
pain 208
supinatus 63,109-10,112-3,184,193
surgeries 155,157
valgus 110,113
compensated 202
flexible 110,112
rayeffects 110
varus 110,112
foottypes 196
Formation, blister 136,247-8
Index 309
Fowlerand Philip 201
angle(FPA) 201-2
FP 106-12
motion 107-8
FPA(Fowlerand Philipangle) 201-2
Fracture 2,24-30,32,39,56,59,66,79,81,90-2,
98-100,111,131,136,147-54,188-90,194,
198-201,205,208,225,237,244-6,248-51,
256-83,291
articular 262,267
blisters 270,276
cleft 27
comminuted 147,151-2.256,269
configurations 147
digital 258-9
displaced 269
fragments 25,27,147-9,261
healing 99, 100
stable 27
interface 25, 149-52
line 149-50,274,277,219
pathological 79,81,263
pattern 24, 258
reduction 25,91
inadequate 27
repair 25,257
stability 24-5,141,257,259
tongue 269-70
transverse 147,149,214
Type 280
unstable 141,151-2
Fractureofbodyofcalcaneus 267
Fractured calcaneus 270
Fracture/dislocations 264,272
hindfoot/ankle 249
Fragments 25,27-8,147-52,181,244,249,260,
267-8,279
capital 177-9,186,195
metaphyseal 279
Frame 153-4,265
Freckles 39
Freeflap 129
Freeze-driedbone 131
Freiberg'sinfraction 243
Fried'sruleforinfants 151
Frontalplane 5,106,111,114,142,153,188,
192,207,214,218-9,225,239,250,269
Frostpartialmatrixectomy 164
Frostbite 22,53,247-8
Frozensection 116,126
FTSG (Full-thicknessskingraft) 127-8,229,246
Full-thicknessskingraft(FTSG) 127
Function 5,68,75,110,140-1,170,184,187-90,
219,224,228,231
Functionalcapacityassessment(FCA) 282
Functionaltherapy 251.254
FundamentalTechniques 123,125,121,129,
131,133,135,137,139,141.143,145, 147,149,
151,153,155,157,159,161
andProceduresCh 124,126,128,130,132,
I ~ U 1 ~ 1 ~ 1 ~ 1 ~ I . 1 ~ 1 ~ 1 ~
154,156,158,160,162
Fungallnfection 47
FungiImperfecti 41
Furosemide 59,85
Furuncle 34
Fusion 28,65,70,110,153,168,170,188,192-4,
214,221,223-9,239,242,261,270,273
end-to-end 170
stmetatarsal-cuneiform 110
varushindfoot 225
G
Ga 93-4
Ga-67 61,92
Gabapentin 31
Gadolinium 94
Gadopentetatedimeglumine 94
Gait 68-70,89,103-4,106,110,113-5,117,161,
166,175,184,188-9,205,213,221,223,234,
242,251,254,270,295
analysis 106,114
cycle 103,114-5
Galie 270
Gallium 92
Gamma raysterilization 133
Ganglion 31,73-4,78,208
cyst 73-4,78
Gangrene 53-4,95,104,120
Ganley 111,114,176,235,237,239
splint 235
Gap 25,28,149,151,227
healing 25,152
Gas 23,41-2,49,58,92
Gastritis 121
Gastrocnemius 11,13,16,70,108,113,142.
204-6,215,242,256,291
aponeurosis 205-6
equinus 205
medial headof 204,206
recession 142,205-6,215,291
Gastrosoleus 142,204-5,215,240,242
equinus 142,205,215,240,242
Gauer'ssign 69
Gauge 46,88,123,125,137,148,150,192,
244,277, 294
Gelatin 156
Generalanesthesia 57,84-5,118,121-2,
151-60,200,244
Generalanesthetic 118
Genericterminology 292
Geneticdefect 229
310 Index
Genitalia 37
Genotype 61
Gentamicin 49-51,154
Gentianviolet 101
Genu 107-8,112-4,205
valgum 107,112,114
varum 107,112,114
Geographicbonedestruction 77
Gestational 60
Ghali 235
Giantcelltumor 74,78,80
Gibneyankleboot 161
Gigantism 229
Gilbert'sdisease 100
Ginglymus 2,5,107,111,228
Girdlestone 170
procedure 170
Gissane's 269
Gland 20,33,38,60,72
Gleich 218
Glidingmechanism 12,144
Globulin 63,95,100,245
Glomus 20,33,38,75,80
Glycocalyx 49
Glycolyticcycle 100
Glycoprotein 51,96,128
Glycosaminoglycan(GAG) 129
Gm 94,100
Goals 46,60,142,144,146-7,180,189,196,228,
238,248,275,278,294
Gonococcalarthritis 67
GotchandKreuz 168
Gout 26,62-4,67,95-9,116,119
Goutyarthritis 63-4,97
chronic 63-4
Grade 23,102-3,136
Graft 26,45-6,77,127-9,131-3,136,152-3,
182-3,186-7,190-1,215-8,221,227-8,233,
237,244,248,250,253,255,259,262,270
autogenous 133,183,259
freeplantaris 255
freetendon 253,255
take 127-8
thinner 127
transplantation 259
Gram 40,45-7,49-51,66-7,100-1,119,249
negative 40,66,100
stain 46-7,67
Gram'sstain 40,101,119
Granuloma 38,60,71,78,163,189
annul are 38
Granulomatous 38,48,62,139
Grave'sdisease 61
Greaterandlessersaphenousveins 20
Green-modifiedReverdinosteotomy 177
Green-Watermannosteotomy 185-6
Greenfieldfilter 58
Groin 17,85
Ground 103,109,112,115,196,219-20
Groups 36,41-2,47,69,97,289-90
Growth 101,112,129,133,183,238,258,278-9
centers 243
factor 133
GSWs(GunshotWoundsl 248-9,258
Gudas-scarfosteotomy 180
Gutter 135,137
H
HAA(HalluxAbductusAngle) 171,174,179
Haglund'sdeformity 110,113,201-3
Haglund'sdeformity 113,202-3
Hairs 33,37
Halfpins 153-4
Hallucination 84
Hallux 4,6.9,11,14,16,18,63,68,90.102,105,
110-3,142,166.171-3,175-7,184-5,187-8,
190-4,208,211,213-4,231-2,234-5,242,259,
261,267
abductovalgus 171
abductus
angle(HAAI 171
interphalangeus 232
dorsiflexion 102,187
equinus 110, 113,184
interphalangeal 172,259
arthrodesis 192
limitus 63,110-3,172,177,184,191.194
limitus/rigidus 63,110,113,184,191
malleus 110,113
osteotomies 175-6
rigidus 63,173,175.184,190
valgus 4,171,191.232
varus 175,188,191-2,231-2,235,242
HalluxInterphalangeusAngle(HIA) 172,177
Halothane 121,159
Hammertoes 63-4.110,112-3,142,166-8,170,
196,205,221
Hamstrings 107,114-5
Hangnail 39
Hanhart'ssyndrome 35
Hansen'sdisease 38
Hardcastleclassification 263
Harris
andBeath projections 90
andBrand classification 66
Hauxthausen'sdisease 34
HAV 112-3,111-7,180-1,183-4,187-8,205,213,
215,261
Hawkins 270-1
classification 271
HawkinsType 272
HDP 190
Index 311
Head 1,2,4,101,13-4,26,32,110-2,114,121,
149,153,168,1723,177,190,205,224,231,
237,240,260-1,270, 273
back-jawthrust 87
Heal 29,123,125,147,163,200,213,259
Healing 22,24-30,46,53,71-2,84,99,100,119,
122,124,126-8,131-3,140,147-9,152-3,
156-7,161,177-8,183,188,191,193,199,200,
213,221,233,248,258-9,261,271-2,281. 294
fracture 200
gap 25,152
process 22,71
secondaryintention 46,119,127-8
Heartfailure, congestive 54,56.100,121
Heat 37,40,138
Heel 16,18,20,32.34-5,47,64,68,90-1,103-4.
108-9,112-3,115.129-30.134,146,161,166,
188,198-205,208-9,213-5,219-21,234-5,237,
239,254,265,267,270,282.291
contact 108,115
lift 161.202-5
pain 64,291
recalcitrantplantar 200
spursyndrome 112,134,198-9,282
varus 68. 220-1
Heimlichmaneuver 85,87
Hemangioma 31,58,14,78,80,98,139
Hemarthrosis 98.251
Hematocrit 94,119
HematogenousOsteomyelitis 42
Hematoma 25,39,100,119-20, 131,134,136,
160,199,200,210.212,245,251,256,260,
276.294
dissecting 120
Hemoglobin 94,119
Hemoglobinuria 52,98
Hemolysis 100
Hemophilus 42,66
Hemopoiesis 95
Hemorrhage 39,55,71,75,95,99,117,119,122,
128.155-6,163,199,208,244-5,256
Hemorrhagic 33-4,36,98,100,157
Hemostasis 26,57,117,119,124-5,128,154-5,
203,213
adequate 57,203
Henoch-Schonleindisease 36
Henry's 32,212
hiatus 32
mononeuritis 32,212
Heparin 55,57-9,98,117,295
lowmolecularweight 55,57
Hepatic 35,45,95,98-100,121
disease 95,99,100
Hepatitis 48.52,61.95,100,158
Hepatotoxic 159
Heterograft,porcine 248
Heuterprocedure 187
Hg 53,83,155,213.255
HIA(HalluxInterphalangeusAngle) 172,177
High-riskpatients 55
Hightiters 96
Hindfoot 36,62,66.90-1,107-14,148,155,214,
219-21,224-7,234-5,237,239,241,249,255,
265
pronation 108,110
varus 237
Hip 42,53.103-4,107,115,214.228
HIPJ (Halluxinterphalangealjoint) 172,192,
259-61
Histamine 81
Histopathological 244
History 1,24,56,62-4,73,81,85,89,116.
118-22,156,158,209,293
and physical(H&P) 116,293
HIV 47,51-2,66
HUHR 184-8
Hoarseness 81
Hockeystick 226-7,238
Hohmannosteotomy 197
Hoke 217
Holmium 138-9
Horizontal plantarosteotomy 177
Hormone 56,60-1
Hospital 81.83.85-7,247,284
Hospitalization 57,283
Hours 42,44-5,55-8,64,67,84,86-7,92-3.116,
118-20,126,137,160,164,216,225.244-6,
254-5,258, 270,276.295
Amide 158
postop 57,122
Hubschermaneuver 214
Human immunodeficiencyvirus(HIV) 51
Humbyknife 128
Humerus 42
Hyaline 29
cartilage 29
Hydrocortisone 84
Hydrogen sulfide 49
Hydrolysis 123
Hydroxyapatite 92, 132-3,153
Hyperbaricoxygentherapy(HBOT) 46
Hyperdorsiflexion 260
Hyperemia 26,44,52,65,93.120,156
Hyperglycemia 46.60
Hyperhidrosis 53,85
Hyperinsulinism 83,99
Hyperkeratoses 34,39,167
Hyperkeratosis 34,39,40,60,65,110,112-3,
161,167-8,184,196
Hyperlipidemia 26,53,56
Hyperosmolar 60
Hyperostosis 34.193,199
312 Index
Hyperparathyroidism 27,99
Hyperpronation 63,108,110-4,166-7,198,202,
205,208-9,214,216,234
compensatory 112-3
Hypersensitivity 22,36,53,81.92,94,106,156-7
Hypertensive 38,83
crisis 83
Hyperthermia 85,117,122,158-60
Hyperthyroidism 40,61,88,100
Hypertrophic
nonunion 27-8,93
pulmonaryosteodystrophy 40,62
scar 24,139,248
scars 24,248
Hyperuricemia 26,34,63-4,97
Hypervitaminosis0 99
Hyphae 47,101
Hypnotic 117, 121, 159-60,295
Hypoglycemia 83
Hyporeflexic 102,104
Hypotension 40,46,81-2,84,88,160
Hypothalamic 50,84
Hypothermia 122,248
Hypothesis 285,287
Hypotonia 65,70,158
Hypovolemia 88, 160
Hypoxia 58,82,121,156,159,229,242,248
Hysteria 219
Iatrogenic 111,163-4,184,191,194,212
Ice 35,85,119-20,210,212,243-4,276,283
Ichthyosis 39,69
1&0 41.45-7,49
Id reaction 36
Identicaltwin 127,131
Idiopathic 24,59,63,199,219,229,231-2,237,
239,242-3
IgA 37
IgM 96
llizarov 154
1M 81-2,86
IMA 178,180,182-3,190-1,196
first 172,178-9,181-3,186,188,190,196
Images 89-92,106,241,291,294
Imipenem 49,51
Imipramine 31
Immobilization 25,27-30,57,128,136,154,182-
3,188,194,202-4,218,223,242,257-8,260-2,
265,267,270,276, 288
Immunity 52,61
Immunization 245
Immunocompromise 162,221
Immunopathy 60
Implant 116,131,189-90,193,216,228
arthroplasty 189-90
degradation 190,216
infection 49
interphalangeal 189
metallic 147,216
stems 190
stressfracture 189
total 190
Implantablefixation metals 147
Implantation 131,154,223
In-111 44,67,92-3
In-toe 111,114,242
Incision 16,23,41,45-6,67,119,126,130,137-8,
154-5,164-5,168,171,178,189,194-5,200-1,
203-7,209-10,223-4,226-7,231,233,238,
241.251,255,270,272
2-incisionapproach 224
Incisionanddrainage(1&0) 41,45-6
Incisional 77,125,223
biopsy 72.77,124-5
Incisions 41,45-6,67,126,128,136,139,164,
171,200,203-4,206,209-10
electiveskin 20,23,126
longitudinaltendon-splitting 204
medialparatendinous 203
plantar
longitudinalinterspace 210
stab 168
rightangle 164
semi-elliptical 77,164-5,192
tendonsplilting 204
transverseplantar 210,223
Inclusioncyst 72
Incompletefractures 24,257
Increasedplantarflexionoftalus 239
Index
ankle-brachial 53-4
forefootlarm 105
ofsuspicion 71,75,81,119
Indications 28,48,127,134.142,144,146.167,
175,188-9,192,215,226
Indiumscan 93
Induction,rapid 159
Infant 37,42,86,157,232,235,237-8
Infection 23,26,36-49,51-2,56,59,61,65-7,70,
84,92-101.116,118-9,122-4,128,131,134,
136,153,157,163,168,193,200,210,212,221,
226,228,243-4,247-8,259,272.294
acute 44,95-6
concomitant 41,163
diabetic
foot 51
plantarvault 46
polymicrobial 46
joint 42,44,66
neerotizing 23,45,49
parasitic 61,95
Index 313
pintract 153,193
plantarspace 46
recurrent 41,48
riskof 123,136,259
streptococcal 38,97
treatmentof 45, 153
viral 61
Inflammation 25,29,30,37,40,42,44,60-1.91,
93,95-6,101,119,122-3,157,254
Influenza 42,66
Information 48-9,103,264,285-7,290-2
Infusion 58,82-3,93,161
Ingrowntoenails 163-4
Injuring 154
Injury I,5,22, 24-5,27,29-32,52-3,56,65,70-1,
83-4,92.95,99,100,102,104,111,122,134-7,
150,152,155,161,163,200,209,212,226,237,
244,246-51,254-60,263-5,267,269-70,272-3,
276,278-9,281-2,294
electrical 247
growthplate 25,257
hyperplantarflexion 259
nailbedtissueloss 245-6
pulmonary 100
Inlay 192,227
Innervate 14,16-7
Inosculation 127-8
Insertion 4,6-13,87,154,203,207,213,254
peroneusbrevistendon 2
Instability 25,27,53,68,70,91,104,133-4,142,
168,182,185-6,192,215-6,223-6,228,248,
250-1,273,294
Insulin 45,59,60,83,85, 133
Integra 129
Intention 45-6,119,125-8,156,191,259,286
Intercuneiform 4,182,214,263,265
Interest,historical 187,200-1
Interface 4,5,27,148
fracture/osteotomy 150
fracture/osteotomy/arthrodesis 152
fracture/osteotomy/fusion 153
graft-recipient 128
metatarsocuneifonmfusion 194
Interferencescrew 141
Interferon 61
Interfragmental 149,151-2,156,179,182,186,
193,195,218,224-5,227,235,259,277
compression 149,151-2,179,182,186,193,
195,218,224-5,227,259,277
screw 149.182,186,195,224
screws 149.179,182,186,195,218.225,
227,259
screw 151,179,235
Intermediategraftmeasures 127
Intermediatemetatarsalgia 194
Intermediatephalanxfractures 259
Intenmediaterelativesclerosisofdeadbone
26
Intenmetatarsalligaments 4
Intermetatarsalspace 17-8,31,46,137,173,
210,212
Intenmittentpneumaticcompression 57
Internaland externaliliacarteries 17
Internalfixation 45,66,147,149,151,153,224,
257
Internalrotation 70,106-7,112
InternationalAssociationforEnterostomal
Therapy 23
Interossei 9, 13,68,142,166,255
Interosseousmembrane 68, 140,274, 276, 278
Interphalangeal
arthrodesis 170,192
joint 18,170,112,259
InterphalangealJoints(IPJI 2,167.188,192
Intersection 106,171-2.265
Interstitial 52,68
Intervention 23,86,116,210,282,286-8,290,
292
Intra-articular
calcanealfractures 268
fracture 188,262,268-70
Intra-operative 85,116,193,293
Intracompartmentalpressure 255-6
Intradermalnevus 37
Intralesional 24
Intramedullaryhemangioma 78
Intrauterine 229
Intrinsic 6,9,20,53,65,68,104,147,152,157,
166,168,173,188,208-10,212,221,238,
260-1
Inv 109
Inversion 5,11,91,106,108-10,134,212,241,
249,251,262,272-4
maximum 108-9
Inversion/eversion 108-9
Investigation 228,287-8,290
Involucrum 42,44,92
10(Interossei) 6,9,12-3,68,142,166,255
10membrane 6, 10-1,14, 17
Iodine 41,60-1,94,101,156
Ion 3,141,167
Ionizingradiation 89,91-2
lor 19
IPJ(InterphalangealJointsl 2.167,188,192
Iritis 34,36,62
Iron 95,147
deficiency 95
Ischemia 26,30,54,93,117,120,155,212,
248,256
Ischemicindex 105
Isoflurane 159
Isolatedmetatarsalosteotomy 194
314 Index
Isolatedstructuraldeformities 194
Isopropyl 163
J
JacobyV-osteotomy 195
Jansheedyneedle 134
Japasosteotomy 221
Jaundice 61,98,100,121
Jawclenching 85
Jointline 274,276
Jointpouch 135
Joints 2,24,36,62-5,137,140-1,204,244
tibiofibular 5,6,90
Jones
fracture 262
suspension 142,221
Joplin'sneuroma 261
Junctional
nevus 36
rhythm 88
Juvaraobliquebasewedgeosteotomy 181
Juvenilerheumatoidarthritis 67
K
Kager'striangle 202,254
Kager'striangle 202
Kalish osteotomy 179
Kaposi'ssarcoma 52,74
Karnofskyscale 283
Keithneedle 123
Kelikianpush-uptest 166,168
Keller
arthroplasty 188-9,223
procedure 176,183,188
Keloid 24,34,139
Keloids 24,34
Keratoderma blenorrhagica 34,65
Keratoma 34,168,192,219
Keratosis(seealsohyperkeratosis) 34-5,39,
125
climactericum 34
plantarumsulcatum 34
punctataofHallopeau 35
Kessler 124
Ketoacidosis 46,60,99, 100
Ketones 99
Ketonuria 60
Keywords 286,292
Kidner 214,216
Kinetic energy 248
Kirby-Bauerdisk 101
Kite'sangle 5,214,239
Klebsiella 40,49
Knee 11,16-7,34,55,64-6.69,73-4.91,103,
107-8,110-5.120.137,142,149,153,190-1.
199,204-8,225-6.228.239,254.256,258.267.
270,273
Knife 128,249
Knockknee 114
Koenen'sfibroma 73
Kohler'sdisease 243
KopelandThompson 208
Koutsogiannis 218
KTP 138-9
Kutierflap 246
Kveim 62
K-wire 150,170,176-8.180,182,186,192-3,195,
197-8.223.241,259,261,277
crossed 182,187-8,224
stabilization 170,179,231,233,235
Kyphoscoliosis 6B
l
Labrum 135
Labs 46-7,71,209,294-5
Laceration 30,39.43.83,120.210,246,249
Lactatedehydrogenase 100
Lacticacid 100,123
Lag
phase 22,29
screw 149-51,180,182,192-3,195-6,198,225,
270,272-3,277
fixation 182,196,198,272-3
screws 149-51,179-80.182,186,18B.193-5,
19B,203,225,259,270
Laird-modifiedReverdinosteotomy 178
Lambrinudi 186
Lantar 7,8
Landry-Guillain-Barresyndrome 104
Lapidus 182,186,224
procedure 182,224
Laryngospasm 81-2
Larynx Bl
Lasers 125,134,137-9
Lat 3,6,102
Lateralaspect 7,9,16-7,32,89.91,171,183,
204,224,231,249,253,263
lateralcollateralligaments 2. 5,91.250,274
lateralcolumn 146,215-7,219-20.238
Lateraldecubituspatient 206-7
Lateralheads II,204-5
Lateralhindfoot 66
Lateralmalleolus 2,5,10,13.16,32,90,lOB,
130,136,147.224-5,241,249.252-3,274,276
Lateralplantar
artery 18
nerve 14,16-7,199-201,207-8
courses 16
supplies 17
nervespass 20B
Lateral plantarS2 13
Lateralradiograph 198,202.214,216,220.239.
281
Index 315
Lateralsuralcutaneousnerve 14
Lateraltarsalartery 18
Lateralthirds 206
Lateraltibialcondyle 107
Lateral-to-medial 153-4
Lateraltrappingsuture 254
Lateralview 90,214,234,237,240-1,265,274,
276
LAUGE-HANSEN CLASSIFICATION ofANKLE
FRACTURES 274
Lavage 45-7,61,85,116,120,163,244,248
Lawrence-designedtotalimplant 190
Laxity 107,196,214,250
layers
basal 33,75,120
granular 34-5
Lazy-Sincision 203,210
LE (Lupuserythematosus) 52,55,62,96-7
Lead 27,29,31,42,54,62,70,73,88-9,99,118,
168,196,198,208,219,242,250
Lee 98,252
Leg 1,13,16-8,20,35,46,46,58,68,70,72,91,
103,109,113-4,121.129-30, 140,152,154,
204,214,224-7,237,239,246,254-6,265
Legends 291-2
Leiomyoma 38,73
LeLevre 216
procedure 216
Lengthen 182
Lengthening 68,130,132,140,142,146,153,
166,176,178,181,189,200,205,207,214-7,
232-3,235,238,255
Lentigomaligna malignantmelanoma(LMM)
75
Lepird procedure 235
Lepromatous 65
Leprosy 38
Leptospira 61
Lesion 24,30,36-7,46,53,71-81,102,124-6,
138-9,165,261,273
ablation 138-9
lateral 196,273
Lesion/s 125
Lessermetatarsalshaftosteotomy 195
Lessermetatarsals 110,112-3,235,261,263
intermediate 194
LesserMetatarsophalangealJoints 2
Lesserpanmetatarsalheadexcisions 223
Lessertarsalaxis(LTAx) 234
Lessertarsus 172,221,223,234
Leukemia 52,63,81,95,99,100
Leukocyte 40, 100
Leukocytosis 79,81,95
Leukonychia 40
Leukopenia 95
Li 3
lichen
planus 36-7,47
simplexchronicus 35
lichenification 35,161.192
Lichtblau procedure 235
Lidocaine 31.82,158,161
Ligament 2,4,5,9-12,16-7,22,29,65,91-2,107,
123,134-5,137,141,153,189,207-10,214,
216,224,237-8,240-1,250-1,253,260,263-4,
267,273-4,276-7
ligaments 5,12,16,22,29,92,123,135,147,
210,217,235,237-8,250-1,253,263,273
anterior-inferiortibiofibular 135,274
intennetatarsal 263
interosseoustalocalcaneal 5,240
laciniate 11,16,208-9
long plantarcalcaneocuboid 4, 10
plantar
sesamoidal 4
tarsometatarsal 4
spring 5,216,240-1
suspensory 2,141
Ught 39,40,138
limb 23,41,43,46,49,50,69-71,79, 103-4,107,
114,124,153,155-6,161,228,233,242-4,258,
264, 270, 278
lengthinequity 107
salvage 79
lindholmAchillestendonrepair 255
linezolid 49,50
lip 81,135-6,218
lipase 59
lipid 46,69
lipoma 73,208
liposarcoma 13
Lisfranc 4,66,193,211,223-4
lisfrancArthrodesis 223-4
lisfranc'sjoint 4,223-4
lisfranc's
ligament 263-4
plantarligament 4
liters/minute 86-7
lithium 61
LlUS 28-9
Livedo 37,104
reticularis 37,104
liver 48,61,96,99,100,157,159
LMM (Lentigomalignamalignantmelanoma)
75
LMTJ axis 110,112-3
Loading,push-up 168,170
Lobsterfoot 233
Localanesthesia 77,84,124-5,157,160-1,203,
244
Localanesthetic 31,71,82-3,85,88,94,155,
157-8,160-1,163,209,245,272
316 Index
Lockingfixationplates,specialized 182
Logroscino 183
procedure 183
Longflexors 168,171,2r7
longitudinalincisionmedial 2IfI
Lordosis 104
LouisBarsyndrome 39
Loupe 32,74,140,201,209
Loupes 140
LowDyestrap 161,199
Lowerextremities 17,32,40,42,46-7,54-5,58,
68-9,73,75,103,111-2,125,133,161-2,20B,
242,248
Lowermotorneuron 70, 104,160
Lowman 216
LTAx(Lessertarsalaxis) 234
Ludloffosteotomy 180
Lumbago 160
Lumbar 64,69, 104,160
Lumbosacral 13,160,199,209
Lumbricales 7,10,13,17,166,219
Lung 40,58,71,99,1 DO, 118
Lupuserythematosus(LE)cell 97
lushke'sdisease 243
lymphnode 71,76-7
Lymphadenopathy 52
Lymphatic 20,59,229,242
Lymphedema 36,59
Lymphoma 63,99
lynnAchillestendonrepair 255
lyticlesion 79
M
MAA(MetatarsusAdductusAngle) 172,236
Maceralion 41
Macrocyticanemia 95
Macrodactyly 229
Macronychia 39
Macrophage 22
Macular 35-6,75
Macule 33,36,39
Madurellamycetoma 48
Magnesium 100
Magneticfield 91
Magnification 32,74,140,201,209,282,291
Maisonneuve
fracture 32,274
fractures 32,274,m
Mal
de Maleda 34
perforansulcer 47
Malabsorption 95,98-100
Malaise 40,52,54,60,62,81,120
Males 54,63,68-9,74-5,80,94,97,113,118,
158,237, 254, 265
Malignancy 54,73-4,79,81,84,95-7,100,
125-6,242
Malignant 39,59,71-81,85,98,100,117,122,
158-60
bonetumors 79
hyperthermia 85,117,122,158-60
melanoma 757,98
transformation 39,74,79,80
Malleolarposition 112-3
exlernal 112-3
Mallet 148,166-8,194-5,203
toe 166-8
Malpighii 34-5
ManagementofFootandAnkle
Trauma 245,247, 249,251,253,255,257,259,
261,263,265,267,269,271,273,275,277,
279,281
Trauma Ch 244,246,248,250,252,254,256,
Z58,260,262,264,266, 268,270,272,274,
276,278,280
Manifestations 52,83,87
Manuscript 286,290-2
MAOinhibitor 120,155
Martensiticstainlesssteel 147
Martinisign 64,97
Masseterspasm 160
MasterknotofHenry 11-2
Matrix 16,29,33,39,40,129,132-3,136,139,
163-5,246,278
Matrixectomy 163-5
Maturation 22,25,29,30,111,114,278
phase 22,25
Mauosteotomy 180
Mayo 186, 190,260
Mayoblock 260
Mayoprocedure 186
McBride 175,In
procedure 175,177
McFarlandprocedure 233
McKeeverfusion 188
Medial 1,2,4-14,16-8,20,46,54,63,68,90,101,
104-12,114,128,130,135-7,146,153-4,161,
165,168,170-2,175-6,178,181-3,185-6,189,
191,193-5,197-8,200-1,203-9,212,214-9,
221,223-7,231-2,234-5,237-42,246,250,
255,257-65,267,269-70,272-4,276-7,281
ankle 135
arch 128,146,191,215,217
pain 191
tendosuspension 146
aspect 7,9-11,14,16-7,90,191,194,206-7,
232,235,241
basecorticalosteotomy 182
calcaneal
branches 198
wall 6
Index 317
calcaneannerve 16,208
calcificsclerosis 54, 105
capsularflap 115-6,189
capsular-ligamentoustethering 176
collateralligament 153
column 109,111,114,186,214,216-7,221,224
Lisfranc arthrodesis 186
cortex 182,225
cuneiform 1,2,4,10,12,181,183,217,221,
235,237,241,263
dorsalcutaneous
nerve 14,212
neuritis 181,183,193
eminence 175,182,191
exostectomy 175-6,182
gutter 135,137
heel 18
pain 208
incision 224
accessory 226
and lateralplantarveins 20
lesions 272-3
ligaments 4
malleolarosteotomy 136,273
malleolus 2,5,108,135,137,208-9,224,226,
237,241,257, 274, 281
margin 135,201
marginalvein 20, 224
metatarsals 234
nerve 154
oblique 90,241,259,265,267
view 90,241,265
plantar 6,18
arteries 17-B
artery 18
aspect 239
plantarnerve 16-B,207-B
segment 269
suralcutaneousnerve 16
tarsalartery 18
tibialtorsion 235,242
TIS 208-9
wall 16,208
MedialCuneiformOpeningWedgeOsteotomy
and Graft 183
Medialdirection 232,237
Medialdislocationoffirstmetatarsal 264
Medial-plantaraspect 182,194
Medications 46,48,81,83,86,117,122,136,
160,243,283,288,292-5
Mediterraneandescent 74
Medullaoblongata 158
Medullary 29,43,78-80,92,158,185,187,195
Megaloblastic 95
Melanin 20,33,36,40,75
Melanocytes 20,33,36-7,75
Melanoma 39,40,75-7,98,125
Members 287
Meniscoid 135, 137,250
Meniscus 107
Mentalretardation 73,242
Meperidine 53
Mepivacaine 158
Mesenchyme 241
Mesh 45-6,128,156,255,286
Mesher 128
Mesotenon 12
Metaphyseal 26-7,29,42,66,78,80,147,168,
178,184,195,228,279
cancellousbonefractures 147
Metaphysis 26,42,79,80,134,154,176-7,179,
182,186-7,226-7,278-9,281
Metaraminol 82
Metastasis 71-2,75-7,79,81,96,160
Metastasize 72-3,81
Metastatic 71,81,99,100
Metatarsal 1,2,4,8-12,18,26,47,62-3,68,89,
90,107-13,130,148,152,161.167-8,170-3,
175-91,193-8,208,210,212,217,219-21,
223-4,231,233-5,237-8,240-1,243,245,253,
256, 258, 260-5
arteries lB
ball 47,208
bar 161,184
bases 2,4,8,11.18,47,152,181,186,195,224,
235,243.253,262
Birth 2-3 1
elevator 185,195
fracture 258,262
fractures 261
head 2,90,109,168,171,173,175-7,179,
184-7,190-1.194-6,210,223,231,243,260-1
excision 196.223
lesser 223
pan 223
osteochondralfractures 260
neck 185,197-8,263
osteotomy 170,185,196,223
first 26, 175,177,197
fixation 148
intermediatelesser 194
multiple adjacent 194
plantarflexion 111
reciprocal 111
projectionpad 167,194,210
protrusiondistance 172
shafts 9, 180,231
first 171-2
stressfracture 262-3
surgery 194,196
Metatarsal-cuneiform 186,265
Metatarsal-medialcuneiformfusionsite 224
318 Index
Metatarsale-l-plantare 2
Metatarsalgia 110,113,168,172,175-6,178,
181,184-6,190,194,210,215,219,221
intermediate 194
lesser 168,172,175-6,185-6,194
sub-second 110,113
Metatarsals 9, 10,12-3,107-13,171-2,178-80,
182,185-6,190.194-6.214-5.219. 223.233-6,
256. 258,263-5
fifth 89.154,224,226,235,261-2.265
intermediate 235,261
normal 109,231
second 172,178,234,263-4
Metatarsocuneiform 193
arthrodesis 181
first 235,237
joint 193,235,237
Metatarsophalangeal 2,4,63,77,107,134,
137,188-9,259-60
MetatarsophalangealJointFracturesand
Dislocations 259
Metatarsus 110-3,152,166,171-2,175,179,
183-4,186-7,194,210,215,217,232,234-7,
242,261
adductus 112,172,183,215,217,234-7,242
angle 172,236
angle(MAA) 172,236
primus
adductus 172,179,235
adductuslvarus 232
elevatus 110.112-3,184,187
Methicillin-resistantStaphylococcusaureus
(MASA) 49
Methyldopa 53
Mexiletine 31
Mg/kg 50-1,84-5,244
load 50-1
Mg/ml 82,161
MI (Myocardial Infarction) 85-6,95,100,122
Miconazole 47-8
Microbiology 249,288
Microcyticanemia 95
Microfibrillarcollagen 156
Microfracture 136
Micromelia 242
Microscopic 66,76,99,101,124,189,199
Microsurgery 140
Microtrauma 39,40,52,65,208,249,261
Microvascularfreeflap 129
Midazolam 160
Themiddlefacettalocalcaneal(TC) 238,240-1
Middle phalanx 6,10,166,170-1
Midfoot 23,89,214-5,220-1,237.239,263
Midpoints 172
Midstance 110-1,113,115,204
Midtarsal 66,214
Miller 217
Milroy'sdisease 59
Mineralization 44,65,133
Minimalbactericidalconcentration(MBC) 101
Minimalinhibitoryconcentration(MIC) 101
Minorsurgery 57
Minutes 22-3,46,53,55,57,82,85-7,93,98,
155-6,159-61,240,248,255-6,295
Mitchellosteotomy 178,197
MI 83,94
Mm Hg 53,83,137,155.213,255
Mm3 94-5,97
MmHg 155,213,255-6
Modifications 90,170,176-7,186,188,253
Molybdenum 147
Mondor'Ssign 265
MononeurITis 32,212
Morphea 24
Mortise 5,6,89-91,108,205,207,225.237,
274-5,277-8,281
Morton'sneuroma 16-7,31-2,210
Morton'sneuroma 16-7,31-2
Mosaicverruca 35
Moth-eatenbonedestruction 78
Motion 5,6,20,23,27,29,30,62-4,67,102-3,
106-14,125,132.148,167,171,175-7,182,
184-5,187-92,196,200,202,205-7,210,228,
241,248,250-1,259-61,272-3,282-3
allowing 106,110
attemptedhindfoot 241
firstMTPJ rangeof 175-6,261,272
increasedmedialfemoral rangeof 111,114
intentional 103
jointrangeof 108-9
-rangeof 109-10
triplanar 5,106,108-9
Motor 13,31,69-71.101-4,160,205,208,258,
265
MAl (Magnetic ResonanceImaging) 5,26-8,
44,46,71,81,91-2,94,106,126,134,241,
249-50,254, 261, 263
MASA(Methicillin-resistantStaphylococcus
aureus) 49
MTJ(MidtarsalJoints) 5,64,109-10,112-3,
205,208,214,225-6,228,237
MTJmotion 110,241
MTPJ
arthrodesis 188-9
dislocations 260
fusion 223
muscle-tendonbalance 176
realignment 170,176-7
relocation 68,194-5,221
MTPJs(MetatarsophalangealJoints) 2,8,10,
18,62,111,120,166-8,170-1,173-6,191-2,
195,199,219,223,225,231,258
Index 319
MTPJs,first 64,101,175-7,187-9,191-3,232,
259-60
Mucinclot 62,97
Multiplemetatarsalfractures 261
Multiplemyeloma 52,63,78-9,99,100
MU/ml 100
Mupirocin 41.49
Muscle 10-4,16,18,23,26,30-3,38-9,41-2,54,
61-2,65,68-74,82,85,100,102-4,113,123,
126,129-30,140-1,144,153-6,158-60,168,
175-7,205,208-10,212-4,219,232,239,241-
2,244,247,250,255,258,261,270,278,295
atrophy 69,71
belly 12,103,140-1,153
fascia 12,71,255
intrinsic 208-9
skeletal 74,100,104
spasm 141,205,241
spindle 102
strength 102-3
MUSCLEPERIPHERALNERVESPINALLEVEL
13
Muscle-tendon 102,177,261
balance 175
unit 140
units 140
Musclestraverse 9,11
Musculardystrophy 69,104,160,219-20,242
Mutation 33,39,89
Myalgia 71,120
Myastheniagravis 96, 160
Mycetoma 48
Mycobacterium 38,101
leprae 38
tuberculi 101
Mydriasis 81,158
Myelin 30,38
Myelocele 69
Myelodysplasia 69
Myeloma,multiple 52,63,78-9,99,100
Myelomeningocele 69,219,240
Myeloproliferative 63,95
Myocardialinfarction 85-6,95,100,122
Myocardium 85,123,159
Myoclonus 103
Myoglobinuria 41,98
Myology 6
Myonecrosis 41-3,100
Myotendinousjunction 10,12,206,255
Myxedema 52,59,50,95, 208-9
N
Nafcillin 50,67
Nail 34,39,40,48,68,163,223,229,245
bed 18,20,33,36,38-9,47-8,75,128,163-5,
170,245-6,259
biting 39
fold 163-4
hypertrophy 163-4
plate 39,40,48,163-4,245
avulsion 164-5
Naloxone 159
NaOHprocedure 163
Nausea 82-4,86,121,160
Navicular 1,2,5,11,89,110,172,214,216-7,
220-1,234-5,237,240-1,243
Nc 15,19,238
Nd 3,4,6-9,14,16,18,25,29,79,80,110-1,119,
166
metatarsal 4,9,110,113
bases 2,4
Nd-YAG 138-9
Neck 5,62,75,111-2,114,154,198,220,224-5,
237,270-2
anatomic 171,178-9,195-7
Necrobiosislipoidicadiabeticorum 38,60
Necrosis 23,26,34,37,41,92,95,99,100,120,
127-8,138,189,198,226,241,246,248-9,258,
270-1
Necrotic 23,25-30,33,42,44-6,49,53,67,69,
120,244,248-9
bone 25-6,49
Necrotizing 23,41,45,49
fasciitis 41
Needle 61,67,72,79,8B,97,104,123-5,134,
137,140,161,244
Needles 61,72,123-4,161,245
Neisseria 41,66,101
Neonatal 129,239
Neoplasms 51,71,92,98-9,153,210
Nephrosis 100
Nephroticsyndrome 59
Nerve 9-11,13-4,16-8,20,22,30-3,37-8,52,68-
71,73-4,102,104,120,122-3,133-4,136-7,
140-1,144,153-4,157,160-1.199-201,203,
206-10,212-3,218-20,251,255,270,277,292,
294
conductionvelocity 104
entrapment 31,52,73,102,122,133,140-1,
208-10,212,270
fiber 30,74
fibers 30
injury 30,104,134,138
proximal,commonplantar 210
sheaths 30,74, 123
traverses 31,208
trunk 30-1,74,122,201,209-10
intermediatedorsalcutaneous 251
Nerves 6, 14,20,22,31,33,73,135, 137,154,
208-10,212,231,244,294
commonperoneal 13-4,16,32,153,277
deepperoneal 9,14,32,154,292
320 Index
inferiorcalcaneal 201
intermediatedorsalcutaneous 16
intermediateddorsalcutaneous 212
lateralsuralcutaneous 14
medial
calcanean 16,200,208
dorsal cutaneous 14,212
suralcutaneous 16
perforatingperoneal 154
saphenous 17,32,154
superficialperoneal 10,14,32,137,212
tibial 11,13-4,16,32
Nervoussystem 65,70-1.82,122
Neuralgia 37,160
Neurilemmoma 38,208
Neurites,budding 30-1
Neuroarthropathy 44,60,63,65-6,93, 188
Neurodermatitis 35
Neurofibroma 74,208
Neuroleptanalgesia 159
Neurological 52,68,83,101,104,140,205,
220-1,244,255,293
Neurology 13,220
Neurolysis 32,201,209-10
Neuroma 16-7,31-2,134,140,194,199,208,
210,212-3,261,263
intermetatarsal 134,194,212
Neuromuscular 68,70,158,160,188,191-2,
224,232, 237
disease 68,160,188,224,232
Neuron 70,102-4,160,205
Neuropathy 31,53,59,60,62,65,102,104,162.
189,199,201,208,210,214,219
Neuropraxia 30-1,119,122,137,155.161,256
Neurotmesis 30
Neurotransmitter 30-1,199
Neurovascularbundle 154,193,241
Neutral 107-10,112-5,146,184,188,190,198,
206-7,235,239,251,266,272
Neutral position 108-10,114,207,235.239
Neutralizationplate 151,277
Neutrophil 97
Neutrophilia 65,67,95
Nevus 35-7
Newbone
accretion 26
formation 25-6.28,40,44,78-80
Newborn 74
Nickel 147
Nilsonne 252
Nitroglycerine 53,86
Nitrousoxide 159
Nodular 34,38,48,64,72-3,75
Nodule 33,38,72,74
Non-ossifyingfibroma 78,80
Non-weight 26-9,46,62,66,74,107-8,128,133,
136,144,146,148,180,182-3,188,190,193-4,
200,204,212,258,260-2,265,267,271,273,
276
bearing 26-9,46,62,66,74,107-8,128,133,
136,144,146,148,180,182-3,188,190,193-4,
200,204,212,218,220,223,233,242,258,
260-2,265,267,270-3,276,295
Nonabsorilablesuture 123,176,190,246,251
Noncaseating 38
Noninvasive 28,53,106,135,137
Nonsuppurative 40,65, 119
Nonsuppurativewoundinfection 119
Nonunion 27-9,44,93,132-3,153,181,185,188,
194,227-8,250,260,262,272,278
Norepinephrine 53
NormalfootCalcaneovalgusfoot 239
Normal neonatalankle plantarflexion 239
Normal range 64,94-5,98-100,108
Normocytic anemia 95
NP 108-9
NP STJ 108-9
NSAID 199,203
Nt 3,6,19
Nullifying 112-3
Nutrientarteries 18,279
Nutrition 29
o
OA(Osteoarthritis) 63,66,184,228
Oasis 128
OATS 190-1,273
Obese 60,114,118,210
Obesity 54,56,160,215
Oblique 24,106,108-9,111,126,151,178,181,
186,198,235,246,257,274
fractures 25, 151,257
osteotomy 181,197
plantar-proximal 195
wedgeosteotomy 186,198
Observation 59,73-4,79,84,101,118-9,121,
242, 244-5,256
Observational 285
Ocular 34,39,139
Oculocutaneous 39
Off-setVosteotomy 180
Oligoarthritis 65
Oilier'sdisease 79
OM 44-5,48
OMTJ 109-10
Oncological 71-4,76-7,79,126
Ondansetron 160
Onionskin 78,81
Ontogeny 111
Onychia 40
Onychocryptosis 39,40,71,163-5,247
Index 321
Onychogryphosis 40
Onychoheterotopia 39
Onycholysis 40,65,168,241
Onychomycosis 40,47-11
Onychopathy 39
Onychophagia 39
Onychophosis 39
Openfracture 30,246,258-9,272
Openfractures 25,30.246,257-9,272
Openreduction 25,241,251,259,276
Opening
medialcuneiformosteotomy 183
plantarflexoryfirstmetatarsalosteotomy 186
wedge(Trethoan)osteotomy 182
Operatingroom 27,45-7,116,119,244,294
ORtable 91
Oralexam 89,293
Oraltemperature 40
Organ 30,34
Organification 61
Organisms 41,48-9,101.249
causative 41,48
Orientation 24. 150-1,118-80,182,250,257
ORIF 257,259-62,265,267,272,281
Origin 6-12,63,237
Orthopedic 46,111.114,293
Orthoses,ankle-foot 161
Orthosis 184,205
Orthosorb 149
Os
calcis 34,218.266
intermetatarseum 2
peroneum 2
subfibulare 2
subtibiale 2
supranaviculare 2
sustentaculi 2
tibialeexternum 2,216
trigonum 2,272
syndrome 272
Vesalianum 2.262
Osgood-Schlatter'sdisease 243
Osseous
equinus 205,215
ringoflacroix 278-9
Ossification 1.65.89,272,218
Osteoarthritis 63,65,184,228
Osteoarticulartransfersystem(OATS) 190
Osteoblastic 25,79
Osteoblasts 25,133
Osteochondral 92,136-7,190,260,272-3
fractures 92, 260. 213
phalangeal 260
graft 190
Osteochondritis 148.243
dissecans(OCD) 250
Osteochondroma 18-9,165
Osteochondroses 243,261
Osteochondrosis 114,261
Osteoconduction 131-3
Osteoconductor 133
Osteogenesis 28,131-3
Osteogenic 18-80,131,133
sarcoma 18-80
Osteoid 25,78,80,133
osteoma 78.80
Osteoinduction 131-3
Osteoinductor 133
Osteology 1
Osteolysis 44. 65,80
Osteomalacia 26-7,99.100
Osteomyelitis 23,21,40-4,47,49,66-7,78.92-3,
127.187.196.278
Osteonecrosis(seealsoavascularnecrosis) 66
Osteopenia 62.61
Osteoporosis 26-7.62,64,147,167.189.200,263
Osteosarcoma 243
Osteotomes 26,134.194-5,203
Osteotomy 26.66.132.148-9.176-83.185-7.191.
195.197.203.217,220-1,227,229.231-3.262
distal 117
stability 141-8,183
step-down 178,195
OsteotomyandBoneGraft 182
Osteotomy/fracture 151
Osteotripsy 165
Otitismedia 42.66
Outcomes 287-8,290,294
Overdrill 149
Overlyingskin incision 203,206. 209
p
Pacemaker 59.200
Pachyderma periostosis 34
Padding 73,161,192
Page 291-2
Paget'sdisease 80,100,199
PAil 22.244
PAil(Punctures.Abrasions.Incisions.and
lacerations) 22.244
Pain 26-7.30-1.38,40-1,45-6,49,53-4.58,60,
62-5,67.70-1,13.15.79-81.83.85-6,95,101,
104-5,114,117-9,121-2,133-4,161,163,115-
6,182,184.188-9.191,196,199-202,208-10,
212,215,223,225,228,241-2,245.248-9.251.
254-6.261-3,210-1,213,282,288,291,294-5
calf 53,114,215
chest 58,85
joint 63-4, 116
localized 118,212
minimal 26,163
permanent 71,294
322 Index
plantar calcaneal 201
rest 53, 104-5
shooting 122,210
Palisading granuloma 38,60
Pallor 52-3,70,81, 120,255
Palmer 269-70
clamp 270
Palms 34,36,75
Palms/soles 35
Palpation 31,62,104,106,118,121,209-10,
254,259,261
Pan metatarsal head resection 187
Pancreas 60,100
Pancreatic 59,60,99
Pancreatitis 26,99,100
Panmetatarsal 142,221,223
Pantalar 70,214,225-8,239,278
arthrodesis 214,239,278
fusion 70,225-8
Papillary dermis 33,76
Papilloma 39
Pa pule 33,36
Papulosquamous 36,47,65
Parallel 14,16,20,110,112,126,170,176-8,
188,235,240-1,261,272,277
angled 90
pitch lines (PPl) 202
Paralysis 30, 69, 70, 104, 155, 158, 160, 209
Paraplegia 54,160
Parasympathetic 81,160
Paratendinous incision 203
Paratenon 12,206-7,254-5
Parentheses 290-2
Paresis 69,209
Paresthesia 31,53,60,83,122,200,209-10,212,
248,255-6
Parkinson's disease 104
Paronychia 39,40,47,65, 163-4
Partial thromboplastin time (PIT) 98
Participants 286-8,290
PASA (Proximal Articular Set Angle) 171, 174,
179-80,183,191
Passive
ankle plantarflexion 254
layer 147
Patella 107,149,152
Patellar 66,102,153,161,199,209,273
Path 111, 228, 248-9
Pathological fracture 79,81,263
Patient
age 66,155
education 57,60
positioning 92, 117, 161
standing 89, 90
supine 91
Patients 24,29,31,35,40-8,51-4,56,56-60,
64-72,74-5,81,83-7,89,90,92-3,97,106,
108,116-22, 124, 127, 135, 137, 139, 156-64,
175,188-9,194,196,203-5,209-10,214-5,
218,220-1,223,226,228,235,238,241-2,
244,248,251,254-5,262,265,270,276,282,
284-5, 287-8, 290, 295
active 176,189
debilITated 127, 227
elderly 27,121,157,177
injured 152, 244
non-diabetic 99, 105
normotensive 255
Patient's progress 46,282
Patients, young 67,74, 176-7,187,215
Pattern 4,66
PB (Peroneus Brevis' 2,10,13,18,146,251,
253,262
PB tendon 10,224,252
PDS (Poly-p-dioxanone' 148-9
PE (Pulmonary Embolism) 54,56,58-9,85,95,
100,118,122,294
Peabody
and Muro 235
osteotomy 178
Pedal 6,9,20,47,54,60,64-6,68,81,89,105,
111,114,121,129,157,205,209,212-4,
219-20,224,239,270
Pediatric 111, 114, 242
Pedicle 26,129-30,200,213
Peg-in-hole 170,187-8,197
Pemphigus 37,95-6
Pencil-in-cup 65
Penicillin 49,50,61,245,258
Pentobarbital 82
Peptostreptococcus 40-1
Percentages 96-7
Percussion 31,118,209
Perforating veins 20, 58
Perimalleolar 38,47,121
Perioperative 60,66,84,116-22
Perioperative Patient 116-7,119,121
Perioperative Patient Ch 116,118,120,122
Periosteal 12,25-7,34,40,42,44, 78-SO, 92, 155,
183, 224, 259, 263
Periosteal (juxtacorticall chondroma 79
Periosteum 12,147,208,252-3,255-6,279
Peripheral
nerves 30,68,122, 208, 219
nervous system 65
neuropathy 59,60,65, 102, 189,210,242
Peripheral Nerve Wounds 30
Permeative bone destruction 78
Pernicious anemia 65,95,100
Index 323
Peroneal 5,6,9-14,16-8,20,32,54,68,92,94,
104-5,115,137,144,153-4,198,205,207-8,
212,218-9,224,237-8,240-2,249-50,253,
255,267,270,272,m,291-2
artery 10,18,105,154
groove 10,249
muscle herniation 32,212
nerve
entrapment 208,212
palsy 144
retinaculum 10,249
sheath 5,92,94,224,249
spasm 241-2
tendon 5,207,249,270
tendonsheath 5
tendons 5,205,207,218,224,237-8,240-1,
249,267,270
dislocating 249
posterior 253
tenogram 249-50
PeronealTendonDislocation 249
Peroneus 2,8-10,13-4,17,103,137,144,146,
219,251-3,255-6,262,265
brevis 2,10,13,146,251,253,262
intotalustendontransfer 146
longus 8,10,13-4,144,219,251-3,255-6,265
tendontransfer 144
PeroneuslongusTendonTransfer(PLTI) 144,
221
Peroneustertius 9,10,13-4,17,103,137
Peroniespenilefibromatosis 73
Perpendicular 23,109,125-6,150,172.176-7,
214,234
cancellousscrews m
PertinentAnatomy&Normal
Physiology 3,5,7,9,11,13,15,17,19,21
PhysiologyCh 2,4,6,8,10,12,14,16,18,20
Pes
cavoadductovarus 250
cavus 35,68-70,103,166-7,205,214,218-21,
224-5,234
valgus 62-3,69,111,114,142,144,214-5,
224-5,239-40
Petechiae 36,59
PF 108
Phagocytosis 25
Phalangeal 2,4,12,39,165,171-3,176-7,184-5,
187,189-90,223,231-2,245-6,259-60
base 2,l73,185
fracture 245
open 39
suspected 259
Phalanx 1-4,6,8-11,33,4O,65,80,165-8,l70-2,
l76-7,187-90,193,232,246,259-60
Pharynx 81
Phases 22,25,30,93-4,114,127
acute 96-7,245,249,251
fibrocartilaginouscallus 25
fracture-healing 258
Phenol 163
Phenothiazine 160
Phenylketonuria(PKU) 99
Phenytoin 83
Pheochromocytoma 52,83,99
Phosphorous 99
Photosensitivity 37,39
Physeal 43,92,148,171,243, 279
Physicaltherapy 71,116,184,223,249,254,
272, 282-3,288,293,295
PHYSIOLOGIC PROCESSESofBONEGRAFT
HEALING 132
Physis 176-7,181.183,231,235,243,261,272,
278-9,281
Piezoelectric 28,199
Piezogenic 74
Pigmentation 38-9
Pigmented 36,72,74-5,98,138
Pilon 56,153,226,278
fracture 153,278
Pilonfractures 278
Pilosebaceous 20,33
Pins 120,148-9,153-4,167,170,176,179,183,
185-6,198,218,265,270,273
Piperacillin 49-51
PIPJs 62,68,166-7,170,195,223,259
Pirogoffamputation 213
Pittingedema 60,121
Pityriasisrosea 36,47
PLlPeroneusLongus) 8,10,13-4,18,144,219,
251-3,25&-6,265
Placement 45,58,67,85,118,150,153,177,189,
225,227
Planaldominance 214
Plantar 2,4-14,16-8,20,31-2,34-5,39,40,46-7,
54,63-4,68,70,73,75,90,102,104-6,109-14,
124,126,128,134,137,154,166-8,170-2,
176-82,184-7,189-91,193-6,198-201,207-10,
212,215-6,218-9,221,223,229,231-3,238-9,
241,246,255,260-5,269-70,282
arch 18,54
arm 179,185
arteries,lateral 18
aspect 8,11,20,73,110,184,200,208-9,216,
269
branches 18
calcaneonavicular 5
capsule 260
condylectomy 194-5
cortex 177-8,201.223.238
declination 181,186
direction 241.260,270
displacement 186,195,218
324 Index
fascia 16,73,126,137,198-201,221,238,262
fasciitis 134,199,282
fibromatosis 73
hallucial 18
heelpain 199-201,209,270
incisions 212
inferiorcalcaneus 64
interossei 9, 13
lateral 6, 18,104,208
ligaments 2,263
short 8
medial 189
metatarsalarteries 18
metatarsalgia 221
metatarsus 210
nerve 208,210,212
common 210
involved 210
perforatingbranch 18
plane 112-3
plantarnerves 32
plate 2,8
protrusion 198,200
release 238
response 104
skin 35,39,126
incision 200
spur 199,200
surface 6,73,168,239,261
vault 6,11,46,154,208,265
Plantar-distal 180,186
PlantarFasciotomyandCalcanealSpur
Resection 200
Plantarfascitis 63,112-3,215
PlantarFascitisandHeelSpurSyndrome 198
Plantar-lateralaspect 10,208
PlantarLayer 6-9
Plantar-medialaspect 16
PLANTARNERVESUPPLY 16
Plantarflexes 110,184,217,219,250
Plantarflexion 5,103,106,108,110-1,166-7,
170,191,203-5,215-6,239-40,254,260,264,
267,272
forced 240,272
stabilization 111
Plantaris 11,13,16,35,204,206-7,255
Plantarlateralmetatarsalheadcondyle 195
Plantarmedial 181
Plaque 33,36,53,60,72
Plasma 50,63,92,132,200,244,248
Plate 2,8,25, 29,33,39,40,42,48,65,78,92,
136,148-9,151-2,154,163-6,168,170-l,
181-2,185,188-9,194,224,232-3,245-6,
257,259,270,277-9,281
buttress 152,270
subchondralbone 29,189
tubular 151
Plica 12
simplex 12
Plicae 12
PLLA 148-9
PLTT(PeroneusLongusTendonTransfer) 144,
221
Pneumonia 52,58
Pneumonitis 52, 118,122
PO BID 501
PO OlD 50-1
Poliomyelitis 70,160,219,233
Poly(L-Iactide)acid(PLLA) 148
Poly-p-dioxanone(PDS) 148-9
Polyarteritisnodosa 36,62,96-7
Polycythemiavera 95
Polydactyly 23U33
Polydipsia 60
Polyester 123
Polyglycolicacid 123
Polymer 24,66,129,189-90,216,223
Polymethylmethacrytate(PMMA) 45
Polyneuropathy 31,68,103
Polyonychia 39
Polyphagia 60
Polypropylene 123,161
Pompholyx 36
Ponsettimethod 237,240
Popliteal
artery 17-8
fossa 17,54,73,128.153
Porakeratosis 35,39
ofMibelli 39
plantarisdiscretum 35
Poroma 72
Porta pedis 16.208-9
Position,relative 171
Positional 174,201
Positronemissiontomography(PET) 44,94
Postaxial 231
Posterior 6,13,16-8,68,135-6,153-4,202,204,
209,218.225,250-3,255,258,281
aspect 11,90-1,201-3,206,218,237,241,252,
270, Ll2
bisector 108-9,220
vertical 112-3
facet 5,90,154,215,217,224,241,265,268-70
ligaments 5,6
peronealseptae 10
surface 5,11,154,204
talardome 135
tibial 17,54,104,270
artery 11.17-8,153,198,209-10
nerve 30-1.120,153,207-9
Posterior-inferiortibiofibularligaments 274
Posteromedial 135,153
Index 325
Posting 112-3
Postoperative 43,49,55,84,93,95,99,116-22,
133,136,141,144,147,159-61,167-8,179,
185,191.193-5,212,216,218,223,228,231,
233,242,249-51,273, 293-5
day 84,117,119
halluxvarus 231
immobilization 250-1
infection 49, 93
ischemia 120,212
jaundice 121
nerveentrapment 122
non-weight 218,223,233,242
phase 55,116-7,122,147,168,185,191
PostoperativeComplications 117
Postpartum 56,60
Postphlebitic 58
syndrome 58
Potency 159
Povidone 41.156
Power 103,140,213,282,286-7,289
Prancersyndrome 242
Prazosin 53
Preaxial 231
Pregabalin 31
Pregnancy 54,56,60-1,95-6,100,155,200
Pregnant 89
Prematureventricularcontraction(PVCs) 88
Preoperative 77.84,116,118,155,175-6,225,
293
Preservation 25-6,126.130,175,188-9,227,
235,270
Pressure 12,23,38,53,74,105,120,125,156,
255,278
compartment 255-6
Pretibial 38,60,121,239
PRICE 244,260,270,276
Primarybonehealing 25,27,149,193
Primaryclosure,delayed 45-6,123,256,259
Primaryfractureline 268-9
Primaryintention 126-7,156
Probenecid 64
Procaine 158
Procedures
isolated 167-8,176,195-6
standard 288
Procurement 127-8
Projectile 248-9
Prolongedmetatarsusprimuselevatuseffects
medial 111
Pronated 106,108-10,112-3
Pronatingmobile adapter 115
Pronation 106,108-10,113-4,216.234,264,274,
276-7
Prone 75,203,206-7,210,244-5,258
Prophylactic 55,59,64,121,133,189,223,261
Prophylaxis 49,53-5,57,66,116,244-5,248-9,
258
Propofol 160
Proprietaryname 292
Proprioception 65,101,283
Propulsion 103,111,115,146,166,189,204,219
Prostaglandin 31
Prostatecancer 81
Protective 26,33,47,60,65,70,75,87,89,91,
101,213,223,258
Protein 63,79,96,99,100,132-3,138,247
Proteins,total 63, 100
Prothrombintime (PT) 98
Protocol 86-7,116,160,249
Proximal 1,5,10-1,16-7.23,30,77,104-5,133,
153-5,165,167,170-1,177,179,193,195,
208-10,212,217,223,225,227,232,241,244,
246,252,254-5
articularsetangle(PASA) 171
chevronosteotomy 182
lesions 30
margin 12,210,212
metaphysis 176-7,179,182,186-7
phalangealbasefractures 259
phalanx 4,6,8,9,166,168,170-2,176-7,187,
189,193,259-60
base of 6,8,9
lateralaspectbaseof 6,8
tibia 134,153
Proximal-medial 6,181,197,235
Pruritus 36,71,75,81-2
Pseudoarthrosis 27-8,93,132,170,227-8
Pseudoequinus 205,219
Pseudogout 64,66-7,97-8
Pseudomonas 40,42,47,49,51
Psoriasis 34,36,47,65
Psoriatic 40,47,65-6,97-8
arthritis 40,65-6,97-8
Psychogenic 35-6
Psychosis 61
PT(Prothrombintime) 9,14,58,98,117,270,
295
PTartery 105
PIT(Partialthromboplastintime) 55,58,98
Publisher 291-2
Pull 141,144,148-9,198,201,205,251,267
Pulmonary 24,38-40,42,54,58-9,62,85,95,98,
100,117-8,121-2,158,294
embolism 54,58,85,95,100,118,294
Pulse 28,53,82.86-7,104-5,138,244,293
Pump bump 110,113,202
Punched-out 38,58
Punctatekeratoses,induced 35
Punctures,Abrasions,lncisions,and
Lacerations(PAIL) 22,244
Purchase 149,154,277
326 Index
Purpura 36
Pus 34,41,44,92
Pustular 36
Pustule 34,41
P-values 289,291-2
PVCs(Prematureventricularcontraction) 88
Pyogenicgranuloma 71,163
Pyramidal 219
Pyrexia 120
Pyruvicacid 100
Q
Qd 57
Qfever 61
Quadratusplantae 7,13,16,255
Quadriceps 107,114-5
QuenoandKuss 263
Quinolone 46
R
RA(RheumatoidArthritis) 52,61-5,67,84,96-8,
135,188,200,208-9,221
Radiation 20, 26,31,33,59,72,74-5,77.79,89,
91-2,100,126,137-8,209,247
Radiculopathy 31,199,209-10
Radioactive 55,60-1
Radiograph 198,202,214,216,220,239,281
Radiographic 5,24,26-7,44,77-9,89-91,114,
154,167,170-1,175,184,191-4,196, 199,
201-2,214,220,225,231,233-4,240-1,243,
251,257-8,261,263,265,271,276,279,287-8
characteristics 77-8
Radiographs 47,49,71,126,134,166,205,209,
249,251,260,263-5,295
intraoperative 192,225,227
Radionuclide 27,44,92-3,134
Radiopaque 92, 106
Radiosurgery 139
Randomized controlledtrial 285,287,290
Range 26,61,63,88,96,102-3,107-9,111,113,
117,133,135,140,161,177,184,187,189,191,
200,205-7,228,242,248-9,272,282, 288-9
ofmotion(ROMI 282
Rash 36,62,81,120
Raynaud'sphenomenon 24,52,96,120,155,
248
Rays 20,110-1,178,196,219,231,233,262
intermediate 111,194,261,263
Reartoot 56.109-10,112-3,196,202,219,234,
236
varus,compensated 109,202
Recipientsite 127-9,133,140,191
ReconstructiveFootandAnkle
Surgery 215,217,219,221,223,225,227
SurgeryCh 214,216.218,220,222,224,226,
228
ReconstructiveSurgeryofBasic Conditions
163,165,167,169,171,173,175,177,179,181,
183,185,187,189,191,193,195,197,199,201,
203,205,207,209.211,213
and DeformitiesCh 164.166,168.170,172,
1 ~ 1 ~ 1 ~ 1 . 1 ~ 1 ~ 1 . 1 . ~ 1 ~
194,196,198.200,202,204,206,208.210,212
Recoveryroom 84,117
Rectal 121-2
Recurrent 37-8,58,68
clubfoot 142,144
Red bloodcell 94
Reduction 25,27,59,73,91.147,164-5, 177-8,
181,186,188,193,200-1,220,237,239-41,
246,257-62.265,267,270,273,276-8.281
open 25,241,257,259,276
References 288-92
Reflexsympatheticdystrophysyndrome
(RSDS) 70
Reflux 121
Refractiveindex 40
Refsum'sdisease 69
Regeneration,nervefiber 30
Registeredtrademarks 292
Regnauldprocedure 187
Rehabilitation 116,134,136,140,204,206,
250-1,255, 282-4,294
Reiter'ssyndrome 34,62,65,97-8
Reiter'ssyndrome 34,62,65,97-8
Relaxedskintensionlines 20,126
Release
posteromedial 238
sequential 168,170,194-5,233
Relocation 68.168.194-5,220-1
Remodeling 22,25.30,127,202,204,213
Renal 24,26,41,45.59.63,83,95,97,99,100,
106
failure,chronic 99
Repair 27,30,39,79,131-2,137,167-8,175,182,
185,187-8.214-5,220-1,223,238,249,251,
255,259,262,270,275,278
surgical 30,192,203,212,220.249-50
Replacement,totalankle 228.273
Reroute 251-3
Rescuebreathing 85-7
Rescuers 86
Researchquestion 287
Resection 26,28,79,168,170,176,186-7,189,
195,203,225-6,242
Reserpine 53
Respiration 82,85,159,244,293
Respiratory 39,66,82-3,85-6,117-8,158,160,
295
alkalosis 83
arrest 85-6, 158
therapy 117-8,295
Index 327
Retinaculum 10-1,16,18,32,208-9,249
Retinopathy 60
Retrocalcanealexostosis 203
Retrotorsion 111-2,114
Retrovirus 51
Return 22,30,45-6,117,119,260,295
Revascularization 26.128,271,273
Revardin 110,177-8,183.189
osteotomy 110,177-8,183
Reverse
Austinosteotomy 198
lastshoe 235,242
Wilsonosteotomy 197
Rewarming 53,248
RF(Rheumatoidfactor) 62-3,65,96,134
Rhabdomyoma 74
Rhabdomyosarcoma 74
Rheumatoid 26,61-5,67,84,95-6,134-5,161,
188,200,208,214,221,223,228
arthritis 61,63-5,67,84.96.135,188,200,
208,221
factor 62-3,65,96,134
Rheumatoid FootReconstructionand
PanmetatarsalHead Resection 221
Rheumatoidnodules 221,223
Ribavarin 61
Richie brace 161
Rickets 27,100,114
Rifampin 38,49,50
Rigid internalfixation 149,151
Ringer'ssolution 128
Rinse 101,163
RNA 51,96
Ro 15,19,166
Rockerbottomfoot 114,237,239
Roentgen 63-5,67
Roll-A-Bout 162
Rollersole 161,192,194,199,203,205,210,223
Rosenthalclassification 246
Rotation 70,104,106-7.111-2,115,129,150,
166,175,179,185,196,206,213,237,274,281
external 70, 106-7,281
Rouleauxformation 95
Roussy-Levysyndrome 68,219
Roweclassification 265,267
ROWE CLASSIFICATION ofCALCANEAL
FRACTURES 267
RSTL{RelaxedSkinTensionLines) 20,125-6
Ruleofnines 247
Rupture 66,249,251,254,260-1,274, 276
partial 254
peronealtendon 249
Ry 6,19
S
Sabouraud'sdextroseagar(SDAI 47
Sacroiliac 64-5
Sacroiliitis 64-5
Safety 89,139,161,282
Sagittalplane 4,5,108.110,166,178-82,186,
188,193-4,196,198,214,225,237,250,261,
264
V-osteotomy 179-80
Saline 41,85,133.137.163,200,244
Salmonella 42,66
Salter 281
Sample 47,124-5,287,290
Sandersclassificationofcalcanealfractures
269
SANDERSCLASSIFICATION ofCALCANEAL
FRACTURES 269
Saphenousnerve 17,32,154
Sarcoidosis 38,40,62,95,99
Sarcoma 52,71-2,74,78-81,100,126
osteogenic 78-80
Scabies 33
Scaldedskin 37
syndrome 37
Scale 33-4,60,283,288
ScanPhase 93-4
ScanPositive 93-4
ScandinavianTotalAnkleReplacement(STAR)
228
Scans 44,93
Scar 16,22-4,34,67,72.122-3,126,130,134,
139,165,200,248,251,294
pain 200,294
Scatterradiation 89
SCC (Squamouscellcarcinoma! 39,44,58,
72,125
Schuberth 255
Schwanncell 74
Schwannoma 74
Scissors 125,140
Scleroderma 24,52,62,96-7,155
Sclerosis 24,26,44.54,63-5,73,96,98,103,
105,184,191-2,241,271
Scoliosis 104,114
Screwhead 148-51,193,225
Screws 148-51,170,182,185,188,193,216,
224,277,281
threaded 149-51
Sculpting 29, 191
Sebaceous 20,33,72
cyst 33
gland 33
Seborrheickeratosis 125
Second-degreeburns 247-8
Secondmetatarsalbase 263-5
Secondarybone
callus 24-5,257
healing 25,153
328 Index
Secondaryfractureline 268-9
Secondaryintention 45-6,119,125-8,191,259
Secondarysyphilis 35-6,47
Seconds 54-5,83,88,98,163,240
Sectioning 122,129,134,137,207,210,212-3,
235,238,253,270
Sedation 83-4,157-8,160,203, 244, 276
Sedative 121,159-60,295
Seddon'sclassificationofnerveinjury 30
Sedentary 282
Seizure 82-4
Selakovichprocedure 215
SelectedAnatomy&Normal Physiology 1
SelectedDiagnosticTechniques 89,91,93,95,
97,99,101,103.105,107,109.111.113,115
SelectedDiagnosticTechniquesCh 90.92,94,
96,98,100,102,104,106,108.110,112.114
SelectedDiseasesand Pathological
Conditions 33,35,37.39.41,43,45,47,49,51.
53,55,57,59,61.63.65,67,69,71,73.75.77.
79,81,83,85,87
ConditionsCh 34,36,38,40.42.44,46.48,50,
52,54,56,58.60.62.64,66,68,70,72.74.76,
78,80,82.84.86,88
Self 283-4
Sensitivity 40-1.48.51,70,100-1,121,248.289
Sensorimotor 68,104,219,255
Sentence 286-7,290
Separation 1,24,40,148,155,229,234,257,279
Sepsis 28.56,92.122,133.160,188,228,247
Septicarthritis 40,42-3.48.62,66-7,94,96,98,
189
Septicemia 40,67,99,100,120
Septum 10-2.16,208
Sequence 150-1
Sequentialrelease 168.170,194-5,233
Sequestrum 44,92
Serratia 40,49,66
Serum 36,4S,51.58-9,63-5,69,79,BO.84.97,
99,100.122,160
glutamic-oxaloacetictransaminase(SGOT)
100
glutamic-pyruvictransaminase(SGPT) 100
sickness 36.122
Sesamoid 2,4,6,8,111.142,171-3.175-7,
189-92,260-1
apparatus 4,171,175-7,189-90
fracture 260
Sesamoidfractures 260-1
Sesamoidal 4,90,176-7,185.261
axial 261
Sesamoidectomy 192,261
Sesamoiditis 110,177.185-6,260-1
Sesamoids 4,173,177,184,187,190,257.260-1
Sever'sdisease 243
Sevoflurane 159
SGOT(Serumglutamic-oxaloacetic
transaminase) 100
SGPT(Serumglutamic-pyruvictransaminase)
100
SH (SALTER-HARRIS) 279,281
Shaft 1,10,111,150,171-2,175.179-80,261-2
osteotomies lBO, 186,194-5
Sheath 5. 12,30,35,38,73-4,86,92,94,123,
140,224.249.254
Sheep'sblood 101
Shepherd'sfracture 2, 272
Shepherd'sfracture 2,272
Shingles 37
Shock 46,81,83,95.100,120,244,248
Shockwave 199
Shockwaves 199
Shoe 35,47,49,148,161-2,167-8,170.179,
191-3,195,202-3,214.231,235,242-3,
258-61,263,270
Shoes 47,49.161.167-8.191,202,225,231,
235,242.258, 294
Shortobliquemetatarsalfractures 261
Shortening 147.150.153,165,170,172,176,
178,181,186.188,195,217,221,223
excessive 182,185-6
Sicklecell 38,66,98
anemia 66,98
Significantdifferences,statistically 287,
289-90
Signs 31,44,67.71.81-6,117,119,184,192-4,
209-10,212,244.249,255,270-2.293,295
marked 283
Silicone
polymer 189-90,21S,223
polymer(Silastic) 189,216
Silk 123,128
Silversulfadiazine 139.163.248
Silverskioldtest 142.205
Simpleinterruptedstitch 124
Sinus 5,23,34-5,41.43-5,47-8,88,114.128,
215-6,220.224,226,242,270
tarsi 5,128.215-6,224,226,242
tract 23,34-5,41,43-5,47-8
Sjogrensyndrome 96-7
Skeletal 12,30-1.74,82.85,93.100,103-4,129,
132,147,152,154,158,160,166,199.205,
212-3,216,249,255,258-9,270
Skeletalfixation 129,147,152.258,270
Skeletalmuscle 12,30,74,82,85,100,103-4,
158,160,205.212-3,255
Skeletalstabilization 249,258-9
Skevvfoot 217,234,237
Skin 16-7,20.22-4,34,37-41,53,58,69-72,
76-7,120,123-6,128-30,137-8,148,156,161.
206-7,213,223,229,233,239,244,258
adnexae 33
Index 329
appendages 37,247
closure 123-4,170,201,209
flap n, 129
full-thickness 77,125,247-8
graft 45-6,127-9,248
healing 127-8
grafting 58,126-7,256
grafts 45-6,127-9
autogenous 128-9
lesions 138-9
plasties 127,130
plasty 127,233
substitute 128-9,244,24B
substitutes 128-9,244,248
surface 29,34,36,74,101,135
Skinflaps 77,129
SkinWounds 22
SI 3
SLE 36,61-2,96-8
Slipper 34,260-1
Slough 37,120,127,164
Smoking 54,118,15B
Smoothmuscle 31,38,73,20B, 212
Socialservice 84,282
Sodiumhydroxide(NaOH) 163
Softtissue
infections 41-2,48,93
manipulations 175,214-5
release 175,237-8
Solealline 11
Soles 34-6,75
Soleus 11,13,16,18,108,204-5,256
Solitarybonecyst 78,SO
Solution 48,82-3,157,161
Somnolence 83,159
Sorbinil 31
Soule 170
SP(Sagittal plane) 4,5,106-11,166,178-82,
186,188,193-4,196,198,214,219-20,225,
237,250,261,264
Spasm 38,83,141,160,191,205,234,241-2
Spastic 70,103,142,144,146,188,205,207,219,
232,240-'
equinus 205,240
SPBLAS(SplitPeroneusBrevislateralAnkle
Stabilization) 253
Species 127,131
Specificgravity 99
Specify 294-5
Specimens 13,41,46,48,124-6,165,244
Spicule 39
Spina bifida 69,219-20,242
Spinal 13,37,56,65,69-71,102-4,118,158,160,
205, 219-20,242,265
anesthesia 118,160
column 65
cord 69-71,104,158
level 13
Spine 13,64-5
Spinosum 20,33-4
Spiral 24-5,147,257
Splenomegaly 81
Splint 29,111,114,152,157,167,199,203,206,
235,243, 254,257-9,261
Splintage 148,151-2,182-3,185,193,224
Split-nail 247
Splitperoneusbrevislateralanklestabilization
(SPBLAS) 253
Split-thicknessskingraft(STS6) 127.248
Splittibialisanteriortendontransfer 142
SplitTibialisAnteriorTendonTransfer(STATT)
142,220-1
Spondylitis,ankylosing 64,96-8
Spore 47
Sporothrixschenkii 48
Sprain 32,113,208,251.259,272,283
Springligament 5,216,240-1
Sprue 95, 100
Spur 16,90,112,134,184,198-204,282
reduction 200-1
suspectedplantarheel 90
Sputum 122
Squamouscellcarcinoma 39,44,58,72,125
St 2,6,7,9,13,16,19,25,33-5,39,SO-I,110-1,
115
metatarsal 10,110-3
metatarsophalangeal 107
ray 107,110,113
Stability 103,132,147,151-3.182,188,217,223,
263
Stabilization 10,25-6,63,66,68,111-3,120,147-
8,150,152-4.166-8,170,176,179-SO,188,192,
194-5,205,215,217,220,223,225,227,231,
233,235,238,240-1,249,253,257-9,265,270
Stainlesssteel 123,147-8,152,177,182,192-3,
198
Stammprocedure 183
Stance 103-4,109,113-5,184
phase 114-5,166
Staph 34,42,47,49
Staphylococci 37,41
Slaphylococcusaureus 49
Staple 148,176,182-3,227
Staples 148,176,182-3,203,218,220,225,227
STAR (ScandinavianTotalAnkleReplacement)
228
Starvation 99
Stasisdermatitis 36,38,58
Slate 66,286-8,290,292
Statement 286-7,289
STATT(SplitTibialisAnteriorTendon
Transfer) 142,220-1
330
Index
Steatorrhea 98-9
Steinberg 35
Steindlermatrixectomy 164
Steinmannpin 180,188
Step 26,151,168,178,186,195,233,254
Steppagegait 68,70,205
Sterile 33,41,46,53,67,117,123,125,132-3,
137,139,155-6,163,209,244-5,248,256
Sterilization 133
Steroids 26,36-7,83,96
Stevens-Johnsonsyndrome 37
Steytler&VanDerWalt 235
Stiffness 26,62-4,71,176,184,189,241,249,
270,294
Stimulant 88,117,295
Stirrup 161,258
Stitch 124
STJ(SubtalarJoint) 5,62,90-1,107-10,112-3,
115,137,146,154,204-9,214-5,217-8,224-8,
234,237,241,265,267,269-72
Stoneprocedure 186-7
Stoolsoftener 117,295
Storkleg 68
Strain-generatedpotentials 28
Stratum 20,34,57
bassIe 20
Strength 22,30,103,140-1,147,251,282
tensile 22,123,141
Strept 40-2,97
Streptococci 41,66,97
Streptomycin 50
Stress 5,24,27-8,71,81,83-5,91,100,131,
134-5,150,189,194,198-9,205,208,228,
237,240,251,257-8,261-4,282
emotional 71,81,83
fracture 24,189,194,198-9,257-8,261-3,282
radiography 91,251
riser 150
Stretch 240
Stridor 81
STRUCTURALTYPESofBONEGRAFTS 132
Stump 212-3
neuroma 31,212
symptomatic 212
Styloidprocess 262
Subacutebacterialendocarditis 36,95
Subchondral 26,29,83-6,135-6,184-5,188-9,
191-2,241,261,271-3
sclerosis 63-4,184,192,241
Subcutaneous 12,17,20,23,33-4,41,48-9,53,
55,58-9,62,64-5,69,71-2,74,76-7,92,123,
125,127,137,154-5,170-1,199,203,206-7,
209,212,223,239,247,270
bursae 12
fat 20,23,76-7,125,155,206,209,223
nodules 62,65,72,74
Subgroup 52,290
Sublingual 82,86
Subluxation 5,62,166,170-1,174,189,208,
214-5,219,237,240,250,291
Submetatarsal 110,112-3
Subsequentradiographicevidenceof
secondarybone callus 24,257
SubstanceP 31
Substitute 128-9,182-3,186,244,248
Substrate 22,29,89,90,111,113,154,177,219,
235
Subtalar 5,62,107-10,112-3,134,206,269
Subungual 38-40,47-8,75,77,165,245-6,259-60
debris 40
exostosis 48, 165,259
hematoma 39,245-6,260
melanomas 75,77
Sudomotor 31,65,102,212
SuggestedtechniquesforORIFofankle
fractures 277
Sulbactam 49, 51
Sulfamethoxazole 49
Sulfinpyrazone 64
Sulfonamides 37
Sunburn 95,247
SuperficialperonealL5Sl 13
Superficialperonealnerve 10,14,32,137,208,
212
Superficialreflex 102
Superficialspreadingmelanoma 75
Supinated 106,108,114-5,267
Supination 5,106-10,112-4,205,274,276-7
Supinatus 63,106,109-10,112-3,184,192-3,
205,214,216,224
Supine 46,91,121,137
Suppanpanhypertrophymatrixectomy 164
Supplies 14,18,294-5
peronealnerve 14
Supratentorial 219
Suralnerve 14,16,32,68,203,206,218,255,
270
Surfaces
adiacent 9
contiguous 16-7,210,212
Surgeon 116-7,123-4,134-5,148,151,154,161,
179,184,204,210,213,224-5,228,251,253,
288,294
Surgery 43,46,54-5,57,59,66,84,116-9,132-3,
156,171,176,192,220,233,238,242,272,282
halluxvalgus 191,232
plantarcalcanealspur 16
Surgical
excision 27,59,72-3,77,125,260,272
neck 178,185,195
shoe 148,161,167,170,179,193,195,203,
243,258-61,263
Index 331
stainlesssteel 147
Survival rates 767
Susquet-Hoyershunt 33
Sustentaculum 2,5,12,16,90,198,214-5,241,
269
tali 2,5,16,198,214-5,241.269
Suture 22,77. 119,12J.5,127,135-6,140,146,
148,170,176-7,182,185,190,192,198,206-7,
209,212,246,251-4,260,277-8
materials 22, 123-4
Sutures 29,30,77,123-4,185,251-3,260
absorbable 123,177,206-7,209,246
Sweat 20,33,35-6,39,72,127,206
Swing 103,114-5
phase 103-4,113,115,142,166
Swiveling 179-82,186,235
Symesamputation 213
Sympathectomy 71,160
Sympathomimetic 88
Symptoms 26,31,40,44,46,52-3,58,62-3,67,
70-1,73,81-6,167,184,191-4,209,241,249,
255,258,261,264,267,271,293
Syncope 81,84,200
Syndactylization 223,248
Syndactyly 1GB, 194-5,229, 231,233
Syndesmosis 90,137,241,274-1
Syndrome 16,3H,34-5,37,39,51,56,58-9,
62,65,68,70,95-100,104,112,120,134,160,
198-201,208,212,219,229,233,242,255-6,
272,282
complexregional pain 31,70
postphlebitic 58
Synergistic 40, 103
Synonychia 39
Synostosis 205,207,241
Synovial 12,27-9,62-3,65,74,135,189,208
fluid 12,29,63,65
sarcoma 74
Synovitis 62,65-7,74,98,135,139,170,189,221
detritic 66,189
Synovium 12,61,86
Synpolydactyly 231
Syphilis 35-6,47,65
Syringomyelia 65, 103
Systemic 24,35,37-8,40,43,47-8,53,62,66,71,
77,81,96,98,116-7,119,122,126,160-1,163,
175,184,194,199,208,221,223,243-4,248-9,
251,256,258
lupuserythematosus 62,96
sclerosis 24,96,98
Systemicdiseases 40,47,77,208
Systolic 105,155
T
Tl-weighted 91
T2-weighted 91-2
TA (TibialisAnterior) 9,10,12-3,17,GB, 103,
137,142,153,213,216,224,234-5,238,240-1.
256,265
Tabesdorsalis 103
Tables 13,28,31,49,91,265,285,290-2
Tachdjian-Grice 237
Tachycardia 46,58,61,81-5,87-8,158-9
Tachypnea 58-9,85
Tailor'sbunion 196
TAL(ThetendoAchiliislengthening) 142,166,
205,207,215
Talar 6,66,91,lOB, 112,114,135-7,146,208,
214-6,225,227-8,237,239-41,249-51,253,
266,270-2,275
beaking 241
dome 6,91,135-7,228,237,250,272,275
lesions 272
head 112,239,241
neckfractures 270-2
sagittalgroove 135
tilt 91,251
Talipes 70,219,237,240,242
equinovalgus 70
equinovarus 219,237,240,242
Talocalcaneonavicular 4,5
TalocalcaneonavicularJoint(TCNJ) 4,5
Talus 1,2,4,5,11,90-1,108,110,112,114,135,
137,146,154,190,205,213,215,220,224-7,
234,237,239-41,251-2,265,267-74,277
adductsmedial 234
plantarflexed 240
TalusTendonTransfer 146
Tamponade 156
TAO 54
Tap 150
TAR(TotalAnkle Replacement) 228,273
Tarsal
coalition 92,184,215,224,240-1
tunnel 11,16,32,52,134,140,154,199,200,
208-9,218,225,282
syndrome 16,32,52,199,200,208,282
Tarsometatarsal 4,66,219,262
joint(TMJ) 262-3
TAIT(TibialisAnteriorTendonTransfer) 142
Tattoo 139
Tattooing 61
Tazobactam 49-51
TBSA 247
Te 93-4
Te(Themiddlefacettalocalcaneal) 238,240-1
Tc-99 44,67,92-3
TC coalition 241-2
Tc-p02 213
TCNJ(TalocalcaneonavicularJoint) 4,5
Td, ml of 245
Technetium 92
332 Index
Techniques 67,103,117,124-5,129,139-40,
163-4,170,177,188-9,200,205,207,213,216,
223-4,229,232-3,235,253,255,294
Telangiectasia 39,60,72
Temperature 20,30,33,40,54,58,71,101-2,
104,119,122,244,248,255
Tendinitis 92,183,193,199,202,249,254
Tendinosis 199
TendoAchiliis 11,16,18,32,142,146,200,
204-5,207,225
Tendon 2,5-13,17,20,22-3,29,30,35,64,66,
68,73-4,92,102-4,113,123-4,128-30,135,
137,140-2,144,146-7,153-4,157,161,168,
170-1,175-7,192,198,201-5,207,209,213-4,
220-1.224,231-3,237-9,241,244,249-55,
257,261-2,270,272-3,278,294
adductorhallucis 175
anchors 124,141
courses 11-2
graft 250
healing 140
injury 237,294
longflexor 171,202
patellar 66,153,161,273
ofperoneusbrevis 262
peroneuslongus 8
plantaris 207
reflexes 30,68,102,104,209
sheath 5,12,35,73-4,92,140,254
transfer 68,103,124,140-2,144,146,170-1,
175,192,220-1
flexor 170-1
transferred 68, 140-1
Tendonitis 282
Tenon 108
Tenosynovitis 141,210,249,263,270
Tenotomy 142,167-8,204,207
Tension 125,129,137,141,149,152,171,187,
213
band 149, 152,188,277
Teratogenic 229
Terbinafine 41-8
Terminal branches 14,18,208
Tertiaryintention 127
Tetanus 49,53,160,244-5,248-9,258
prophylaxis 53,244-5,248
Tetracaine 158
Text 290-2
Textbook 288,291
Therapy 45,48-9,52,57,60-1,66,11,95,118-9,
154,258,276
Thigh 13,17,53-4,69,103,Ill,114,120,127,
155,199
Thiopental 83
Thomasen'sosteotomy 191
Thompson-Dougherty
sign 254
test 254
Thompson procedure 232,235
Threads 149-50
Thrombin 128,156,212
Thrombolytic 58-9
Thrombophlebitis 58,155-6
Thrombosis 26,52-4,58-9,85,94,106
Thrombus 120
Thrush 47
Thurston-Hollandsign 279
Thyroid hormones 60-1
Tibia 1,6,10-1,18,42,66,80,90-1,107,133-4,
137,153-4,210,213,227,240,273-4,277,281
distal 11
Tibial 2,4-6,9,11,13-4,16-8,20,30-2,38,42,
53-4,56,63,90-1,104,107-10,112-4,120,
135-7,153-4,172,175,183,192,198,207-10,
212,225-8,235,242-3,246,250,261.270,272,
275-6,278,281
metaphysis 226-7
nerve 11,13-4,16,30-2,120,153,207-9,212
plafond 135,275-6,281
sesamoid 6,172,261
position 172,175
sesamoiditis 110, 113
torsion 112-4,225,235,242,250
tubercle 153
varum 107,109,112,226,250
Tibial SesamoidPosition(TSP) 172,175
Tibialis 2,8-11,13,68,137,142,144,153,214,
234-5,237-8,240,255-7,265
anterior 9,10,13,68,137,142,153,234-5,238,
256,265
tendontransfer 142
TibialisAnteriorTendonTransfer(TATT) 142
Tibialisposterior 2, S,11,13,68,144,214, 235,
237,240,255-7
tendon 237,257
transfer 144
TibialisPosteriorTendonTransfer(TPTT) 144,
221
Tibiofibular
joint 6
transfixation 277
Tibiotalar 90
Ticarcillin 46,51
clavulonate 51
Tie-overstentdressing 128
TIG 245
Tight-packed 115
lightness 54,205,237
TightRope 277
Tillaux-Chaputfracture 273
Timeperiod 123,133,287
Tinctureofbenzoin 239
Index 333
linea 36,47
axillaris 47
capitis 47
corporis 47
cruris 47
pedis 36,47
versicolor 47
linerssign 31
lip 2,16,18,25,33,124,149,170-1.200,224,
239,241,265
lissue
glue 124
type 79,138
lissues 22,28,45-6,60,71,74,77,79,91-2.,99,
120,123-5,131,138,147,154,156-7,244,248-9
litanium 138,147,190,216
Title 290, 292
TMJ(Thetarsometatarsaljoint) 223,235,262-4
TN 216,238,241
TNJ 109,214-5,224-5,237,240-1,271
TNKAnkle 228
Tobacco 54
Todd-modified Reverdinosteotomy 178
ToetestofJack 214
Toe-walking 242
Toe/armindex 105
Toenail 163,245
Toes 9,11, 14,16-8,20,23,36,62, 72,79,90,
102-3,112-3,152,166,170,209,223,229,
233-4,254
claw 68-9,142
lesser 10,18,232,259
proximalphalangesof 9
Tolazamide 60
Tolnaftate 47
Tolrestat 31
Tongue 82-3,142,205-6,268-70
Tophaceousgout 99
Tophi 62
Tophus 64
Topicalthrombin 128,156
TotalanklereplacementfTAR) 228
Total bodysurfacearea(TBSA) 247
Totalprotein 63, 100
Touch-pressure 20,33,65,68,101
Tourniquet 45-6,54,56,136,154-6,161,163,
209,244
Toxic 37,82-3,120,123,156-7,161
Toxic epidermalnecrolysis 37
Toxic shocksyndrome 120
Toxin 30,61.229
TP(libialisPosterior) 2,8,11-3,16,18,68,103,
106-9,111,141,144,182,214-6,235,237-8,
240,255-7
TPmotion 107-8
TPTT(libialisPosteriorTendonTransfer) 144,
221
Traction 30,122,240,254-5,262
Transchondral 136
Transcutaneous 31,105,213,256
Transfer 131,140,170-1,175,214,255,263
metatarsalgia 178,181,190
Transfixation 153-4,277
pins 154
medial-to-Iateral 153
Transfixationwires 153
Transforminggrowthfactor 133
Transfusion 61, 119,122
Transition 77-8,261
Transport 81,85-7
Transverse 5,9,24-5,32,106,151-2,168,181-2,
192,196,235,246,257-8,261,264,274
avulsion
fracture 274
medialmalleolarfracture 277
basewedge(Louisan-Balacescu)osteotomy
182
intermetatarsalligament 2,32,134,137,207,
210
medialmalleolarfracture 276-7
plane 6,78,106,110,112-3,166,168,178-9,
la2,188, 190,195, 198,213-5,217,219,221,
225,234-5,237,259-60,263
Trauma 26,44,52,54,57,60-1,70,92,94,98,100,
132,140,160,205,210,219,228,243-4,279
penetrating 244, 248-9
Treatment
biomechanical 112-3
definitive 77,126,257
inpatient 247
openfracture 258
surgical 32,184,210,231-3,235,259,293
Treatmentallocation 286-8
Treatmentofbenign bonetumors 79
Treatmentofmetatarsalstressfracture 263
Tremor 61,68,70,103
Tremulousness 84
Trenchfoot 52,248
Trendelenburg 81-2, 104
positioning 81
Trephineplug 79,227
Triage 244,249
Triamcinolone 40
Tricepssurae 11,115,144,146,166,204,207,
216,219,240,254
Trichophyton 47
mentagrophytes 47
Tricyclic 31,120,155
antidepressant 120,155
Trigonum 272
syndrome 272
Trim-Itpin 149
334 Index
Trimethoprim 49
Trimming 163
Triphasic bonescan 71
Triplanarmotion 5,106,108-9
Triplanefracture 281
Triplearthrodesis 68,140,214,220-1,224-5,
241-2,270
TSP(TIbialSesamoid Position) 172,175
TIS(TarsalTunnelSyndrome) 16,32,52,199,
200,208-10,282
Tubercle 2,62,153,196,249,213
Tuberculin 38,101
Tuberosity 2,11,13,90,154,218
Tuberoussclerosis 73
Tumor 33,38,40,60,71-5,77-81,95,99,125-6,
196,200,208,229,243,256
regression 15
Tuningfork 101
Tunnel 11,16,31-3,52,134,140,154,198-201,
208-9,218,225,252,282
Turco procedure 238
Turftoe 259,261
Type 37,59,60,136,181.193,231,240,259-60,
264-5,269,277,280-1
TypeDescription 258,260,267,269,278-9
Tyramine 99
U
UA(Uric acid) 63-4,97,99
Ulcer 23-4,33,43,47,72,121
Ulceration 23-4,43,47,53,58-60,65,70,72,75,
119,121,192,221,248
Ultrasonography 92
Unconsciousness 82,158
Undecylenicacid 47
Unequallimb length 114
Ungual 163-4,232
labia 163
labioplasty 164
Union 18,27,132,178-9,182,188,262,272
Units 57-8,245,258
Universal precautions 52
UnnaThostdisease 34
Uppermotorneuron 70,102-4,205
Uptake 93-4
increased 27,92
Urate 63-4,97,99
Urethritis 34,65
Uric acid 63-4,97,99
Urinalysis 46,98, 122
Urinary 42,69,70,80,116-9,122
bladder 69
catheterization 116,119
retention 118-9
tractinfection 118-9,122
Urine 62,64,98-9,118-9,122,248
Urticaria 82,95
Urticarial 37,81
US DepartmentofLabor 282
US Pharmacopeia(USP) 123
V
Vaccine 37,61
Valente 216
Valgus 4,62-3,69,106,108,110-4,135,142,144,
171,175,179,191,202,214-5,221,224-7,232,
234, 239-40,261
ankle/hindfoot 221
foot 224
halluxabducto 110,171
Valleixsign 31,209
Valve 87,158
Valvular 36,38
Vamp 35,193
disease 35,193
Vancomycin 45,49-51,154
Variant,hyperplantarflexionanklefracture 291
Variations 72,74,89,125,151,161,176,179,
181,186,195-7,200,214,253,288
Varicella 37
Varicose 56,58
Varix 209
Varus 4,68,106,108-10,112-3,135,166,171,175,
179,187-8,191-2.196,202,214-5,218-21.225-
6,228,231-2,234-5,237,239-40,242,250,261
metatarsusprimus 110,171,175,179,187,242
Vascularpedicle 129-30
Vasculitis 36,155
Vasoconstriction 22
Vasodilator 120
Vasomotor 53,65,70,248
instability 53,70,248
tone 65
Vasospasm 52,120
Vassal rule 147,224,261,277
Vater-Paciniunits 33
Veins 20,36,54,56,58,140,153,208-9,294
Velocity 31,68,104,220,248-9
Venogram 55,106
Venous 20,26,36,38,42,54--6,58-9,65,85,106,
120,155-6,161,209,212,294
stasisdermatitis 58
thromboembolism 54
thrombosis 26,54,85
Ventilation 58,86-7,118,158,160
Ventilation-perfusionlungscan 58
Ventricular 86-8
Venule 33
Verruca 33,35,71,125,139
Verrucae 138
Verticalfracture 271, 276
ofneckOccurrence 271
Index 335
Verticalmedialmalleolarfracture 277
Verticaltalus 146,240-1
Vesicle 33
Vesicles 23,37,124
Vesicular 37
Vessel 20,52,54,60,120,123,155-6,209
Vessels
dermal 138
medialplantar 16
Vibration 282
Vibratorysensation 101
Vinculus 11-2
Vinegar 163
Vitalsigns 81,86,117,119,212,244,293,295
Vitamin 40,55,84,98, 114
A84
B 40
Vitamins 31
Voglerosteotomy 179
Vohwinkel'sdisease 34
V-osteotomy 179-80,195-6,221
V-Yflap 246
W
Wagstaffefracture 273
Waldenstrom'smacroglobulinemia 96
Walleriandegeneration 30
Warfarin 57,98
Water 53,85,89,91,101,117,129,138,157,199,
244,248
Watermannosteotomy 185-6
Watson-Jones 251
Waveforms 105
Wavelength 138-9
infrared 138
micron 138
Weakness 60,62,68-71,86,141-2,144,166,
214,219,250,294
Wearsurfaces 147,190
Web 210,229,233,291
Webs 229,233
Wedge
osteotomy 176, 183,221,235,237,239
based 198
dorsiflexory 195,220
medialcuneiformopening 235
plantaropening 221
stmetatarsalbase 110
resection 181,225,235
Weight 29,31,62-3,73,104,107-8,125,127-8,
130,136,144,148,156,176-7,179-80,186-7,
189-90,194,196,199,203,209,214-6,219,
225,228,239,241,251.254,260-2,265,267,
270,272,295
bearing 26-9,31.34,46,62-3,66,13-4,89,104,
107-8,110,113-4.125,121-8,130,133,136,
142,144,146,148,154,176-7,179-80,182-3,
186-91,193-4,196-7,199-201,203-4,209,
212-6,218,220,223,225,228,233,239,241-2,
251, 254,258,260-2,265,267,270-3,276,295
Weilosteotomy 195
Werenskioldsign 279
Wheezing 81-2
Whiskering 64
Whiteblood cell 95
Whitespots 40
Whitlow 75, 163
Wickcatheter 256
Wilsonosteotomy 178,191
Wilson'sdisease 61,99
Winegoblet 68
Wire 29,148-9,153-4,193
suture,stainlesssteel 148,177,182,198
Withdrawal 81-2,84
Wood'slamp 41
Words 273,286,289-90
Work
conditioning 282-3
hardening 282-3
levels 282
Workability 147,282
Wound 22-4,29,30,34,40-1,43,45-7,49,66-7,
12,77,84-5,92,95,101,116-9,122-4,126-8,
130-1,133,156-7,161,163,199-201,206,209,
217,221,223,244-6,249,255-6,258-9,276,
294-5
appearance 45
base 23
chronicpedal 47
chronicplantar 47
complications 119,131,133
dermal 22-3
exit 249
gunshot 30,248-9,258
healing 22,84,122,259
infected 45
infections 49,119,122
postopday 122
local 49,119,163
open 23, 156,244, 258
plantarskin 200
puncture 47,49,66,92,248
vacuum 45-6
Wovenbone 80
X
Xenograft 131
Xeroderma pigmentosum 39
336
Index
V
YAG 138-9
Yaw 249
Yearagegroup 73-5
Yeast 47-8,101
Yellownaildisease 40
Young 34,67,70,73-4,80,146-7,170.176-7,187,
189-90,202,214-6,238
Z
Zadik(Quenu)matrixectomy 165
Zigzagincision 126
Zone 77-8,121,153,246,278-9
ofcartilage
maturation 278
transformation 279
ofgrowth 278-9
ofRanvier 279
Zwippincision 270
S-ar putea să vă placă și
- Hand Conditions and Examinations: a Rheumatologic and Orthopaedic ApproachDe la EverandHand Conditions and Examinations: a Rheumatologic and Orthopaedic ApproachÎncă nu există evaluări
- Review - ACFAS Surgical Review BookDocument90 paginiReview - ACFAS Surgical Review BookAndrew Bernhard50% (2)
- Coughlin & MannDocument4.539 paginiCoughlin & MannNicholas CampitelliÎncă nu există evaluări
- Movements and Orthopedic Tests: quick, easy, and reliableDe la EverandMovements and Orthopedic Tests: quick, easy, and reliableÎncă nu există evaluări
- Module 4 MedicineDocument50 paginiModule 4 Medicinepjanu86Încă nu există evaluări
- Chapter 4d Podiatric Infectious DiseasesDocument20 paginiChapter 4d Podiatric Infectious DiseasespodmmgfÎncă nu există evaluări
- Classification SystemsDocument11 paginiClassification SystemsKelli StevensÎncă nu există evaluări
- Handbook of Foot and Ankle Orthopedics (Rational Prescription of Foot and Ankle Orthotics) PDFDocument6 paginiHandbook of Foot and Ankle Orthopedics (Rational Prescription of Foot and Ankle Orthotics) PDFAbdallah Jaber100% (2)
- ABPS Exam Study GuideDocument37 paginiABPS Exam Study Guidepodjones100% (2)
- Module 2 OrthopedicsDocument50 paginiModule 2 Orthopedicspjanu86Încă nu există evaluări
- Practical Biomechanics for the Podiatrist: Book 1De la EverandPractical Biomechanics for the Podiatrist: Book 1Încă nu există evaluări
- Foot & Ankle PearlsDocument167 paginiFoot & Ankle PearlsPamela Hong100% (3)
- Pod EssentialDocument60 paginiPod EssentialAmar AlkhafajiÎncă nu există evaluări
- ABFAS Study GuideDocument368 paginiABFAS Study GuideMohammed FarhanÎncă nu există evaluări
- Hershey Board Certification Review Outline Study Guide: Jonathan M. Singer, D.P.MDocument9 paginiHershey Board Certification Review Outline Study Guide: Jonathan M. Singer, D.P.MpoddataÎncă nu există evaluări
- Des Moines Landmark ReviewDocument147 paginiDes Moines Landmark ReviewD.j. HaramieÎncă nu există evaluări
- Presby ManualDocument432 paginiPresby Manualpoddata100% (3)
- Forefoot Study GuideDocument22 paginiForefoot Study GuideArchibald J. Loch83% (6)
- Exam Table For Foot and AnkleDocument14 paginiExam Table For Foot and AnkleLouie Okay100% (1)
- Watkins Manual of Foot and Ankle Medicine and Surgery 2016Document931 paginiWatkins Manual of Foot and Ankle Medicine and Surgery 2016Karolina100% (7)
- Orthobullets Foot and AnkleDocument88 paginiOrthobullets Foot and AnkleStevent Richardo100% (1)
- Biomechanical Foot Function - A Podiatric PerspectiveDocument7 paginiBiomechanical Foot Function - A Podiatric PerspectiveFisioterapi Kumala SurakartaÎncă nu există evaluări
- Antibacterial Cheat SheatDocument1 paginăAntibacterial Cheat Sheatnkarimova2Încă nu există evaluări
- Fractures of The Foot and Ankle 2018Document240 paginiFractures of The Foot and Ankle 2018okida192100% (2)
- Pediatric Foot DeformitiesDocument27 paginiPediatric Foot DeformitieszeshmaÎncă nu există evaluări
- Shortcut to Orthopaedics: What's Common and What's Important for Canadian Students and Primary Care PhysiciansDe la EverandShortcut to Orthopaedics: What's Common and What's Important for Canadian Students and Primary Care PhysiciansÎncă nu există evaluări
- Nbpme Part II Rapid ReviewDocument147 paginiNbpme Part II Rapid Reviewpudding350% (2)
- Ankle Arthrodesis - Screw FixationDocument26 paginiAnkle Arthrodesis - Screw FixationChristopher HoodÎncă nu există evaluări
- Foot and Ankle Anatomy and Physical Examination PART 1Document49 paginiFoot and Ankle Anatomy and Physical Examination PART 1eric sivaneshÎncă nu există evaluări
- Calcaneus Fracture: Randy SusantoDocument32 paginiCalcaneus Fracture: Randy SusantoRandy SusantoÎncă nu există evaluări
- @MedicalBooksStore 2013 ExternalDocument431 pagini@MedicalBooksStore 2013 ExternalОлександр ШендераÎncă nu există evaluări
- Foot and Ankle Injuries Kylee Phillips - 0Document74 paginiFoot and Ankle Injuries Kylee Phillips - 0Charlez OhanuÎncă nu există evaluări
- ABFAS - Trauma Section Flashcards - QuizletDocument21 paginiABFAS - Trauma Section Flashcards - Quizletpjanu86Încă nu există evaluări
- Orthopedic Inpatient Protocols: A Guide to Orthopedic Inpatient RoundingDe la EverandOrthopedic Inpatient Protocols: A Guide to Orthopedic Inpatient RoundingÎncă nu există evaluări
- AAOS Spine 2009 PDFDocument174 paginiAAOS Spine 2009 PDFDr-fadi AlkhasawnehÎncă nu există evaluări
- OrthopedicsDocument42 paginiOrthopedicsJubir Feat Divisi Operasional100% (1)
- SCPM Surgery Study GuideDocument41 paginiSCPM Surgery Study GuideKyle TemplinÎncă nu există evaluări
- 20 Orthopedic EmergenciesDocument48 pagini20 Orthopedic Emergenciesfzee13Încă nu există evaluări
- AAOS Essentials of MusculoskeletalDocument1.295 paginiAAOS Essentials of MusculoskeletalОлександр Шендера100% (5)
- Trauma Plating Systems: Biomechanical, Material, Biological, and Clinical AspectsDe la EverandTrauma Plating Systems: Biomechanical, Material, Biological, and Clinical AspectsEvaluare: 5 din 5 stele5/5 (2)
- Foot and Ankle TreatmentDocument59 paginiFoot and Ankle TreatmentKonstantinosKontouvalisÎncă nu există evaluări
- Kenny's Boards 2 ReviewsDocument254 paginiKenny's Boards 2 ReviewsHuguette Marie NseleÎncă nu există evaluări
- Chapter 3e Pathological GaitDocument8 paginiChapter 3e Pathological GaitpodmmgfÎncă nu există evaluări
- 019 Foot and Ankle ClassificationsDocument13 pagini019 Foot and Ankle ClassificationsOh Deh100% (1)
- Chapter 4e Internal MedicineDocument19 paginiChapter 4e Internal MedicinepodmmgfÎncă nu există evaluări
- Hip Neck Fracture, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDe la EverandHip Neck Fracture, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsÎncă nu există evaluări
- Evidence-Based Evaluation & Management of Common Spinal Conditions: A Guide for the Manual PractitionerDe la EverandEvidence-Based Evaluation & Management of Common Spinal Conditions: A Guide for the Manual PractitionerEvaluare: 5 din 5 stele5/5 (1)
- Foot and AnkleDocument40 paginiFoot and AnkleAhmed Salman100% (2)
- Orthopedic Emergencies-Springer International Publishing (2017)Document555 paginiOrthopedic Emergencies-Springer International Publishing (2017)Leonardo Tillieci Minnetti100% (1)
- Aaos 2012Document190 paginiAaos 2012Yusufa ArdyÎncă nu există evaluări
- Ultrasound Guided Musculoskeletal Procedures in Sports Medicine: A Practical AtlasDe la EverandUltrasound Guided Musculoskeletal Procedures in Sports Medicine: A Practical AtlasEvaluare: 5 din 5 stele5/5 (1)
- AANA Advanced Arthroscopy The Foot and Ankle PDFDocument223 paginiAANA Advanced Arthroscopy The Foot and Ankle PDFsuny007_bond100% (2)
- The Foot and AnkleDocument17 paginiThe Foot and Ankletimmaber100% (1)
- AAOS2012 Foot and AnkleDocument103 paginiAAOS2012 Foot and AnkleAmmar HilliÎncă nu există evaluări
- 2004, Vol.23, Issues 1, Athletic Foot and Ankle InjuriesDocument165 pagini2004, Vol.23, Issues 1, Athletic Foot and Ankle InjuriesAndrei Gianina100% (3)
- ABPM Fall2014 ExamDocument200 paginiABPM Fall2014 Exampudding35Încă nu există evaluări
- Chapter 5 Pediatric PodiatryDocument88 paginiChapter 5 Pediatric Podiatrypodmmgf100% (1)
- Chapter 6b Digital SurgeryDocument18 paginiChapter 6b Digital SurgerypodmmgfÎncă nu există evaluări
- Ultrasonography of the Lower Extremity: Sport-Related InjuriesDe la EverandUltrasonography of the Lower Extremity: Sport-Related InjuriesÎncă nu există evaluări
- Innervation: The of The Joints of TheDocument8 paginiInnervation: The of The Joints of ThemitroisergiuÎncă nu există evaluări
- Study of Collagenase and Metronidazole in The Topical Management of Diabetic Foot UlcersDocument112 paginiStudy of Collagenase and Metronidazole in The Topical Management of Diabetic Foot UlcersSHREYA MAHESHWARI100% (1)
- Vasc., 6.lymph.& 7. Inn. of The Foot 209-10Document46 paginiVasc., 6.lymph.& 7. Inn. of The Foot 209-10Ameet ThakrarÎncă nu există evaluări
- Pocket PodDocument656 paginiPocket PodchristineÎncă nu există evaluări
- P.I. Manual, 2nd Ed PDFDocument342 paginiP.I. Manual, 2nd Ed PDFMrsDrH88% (8)
- Inervatia Membrului InferiorDocument73 paginiInervatia Membrului InferiorMihai AndreeaÎncă nu există evaluări
- Roblin HealyDocument6 paginiRoblin HealyMiguel JohnsonÎncă nu există evaluări
- Workshop E - Bundle 2019 - Electro-274-295Document22 paginiWorkshop E - Bundle 2019 - Electro-274-295adaptacion neonatal100% (1)
- Nerve of The Lower Limb Edited LagiDocument159 paginiNerve of The Lower Limb Edited Lagifathizu100% (1)
- 19 Tibial NerveDocument38 pagini19 Tibial Nerverodrigocorcino899959Încă nu există evaluări
- (PPT) Anatomy 2.5 Lower Limbs - Blood and Nerve Supply - Dr. Tan PDFDocument110 pagini(PPT) Anatomy 2.5 Lower Limbs - Blood and Nerve Supply - Dr. Tan PDFPreeti Joan BuxaniÎncă nu există evaluări
- Medial Plantar Flap For Hand ReconstructionDocument7 paginiMedial Plantar Flap For Hand ReconstructionMiguel JohnsonÎncă nu există evaluări