Documente Academic
Documente Profesional
Documente Cultură
Gastro PDF
Încărcat de
Ari Syuhada PutraTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Gastro PDF
Încărcat de
Ari Syuhada PutraDrepturi de autor:
Formate disponibile
Gastroenterology Reference Guide
GASTROENTEROLOGY REFERENCE GUIDE
Gastroenterology Reference Guide
ACKNOWLEDGEMENTS: Clinical review and editing was provided by George Pavlou, M.D. of Laneve, Bellardini, Kosc, and Pavlou. Text development, overall composition, and project direction were accomplished by Patricia Vendely, MSMT, ASCP of Quest Diagnostics Medical Information Department.
II
TABLE OF CONTENTS
Gastroenterology Reference Guide
PART 1. GASTROENTEROLOGY DISEASES: SUMMARY INFORMATION CHAPTER 1. NUTRITIONAL AND MALABSORPTION DISORDERS
1 10 15 20 27 32 35 43 54 63 64 71 75 Section 1. Celiac Disease Section 2. Food Allergies Section 3. Lactose Intolerance Section 4. Irritable Bowel Syndrome Section 1. Gastroesophageal Reflux Disease Section 2. Barretts Esophagus Section 3. Esophageal Cancer Section 1. Peptic Ulcer Disease (Helicobacter pylori Infection) Section 2. Gastric Cancer Introduction Section 1. Bacterial Gastroenteritis Section 2. Viral Gastroenteritis Section 3. Parasitic Gastroenteritis
CHAPTER 2. ESOPHAGEAL DISORDERS
CHAPTER 3. STOMACH DISORDERS
CHAPTER 4. GASTROENTERITIS
CHAPTER 5. INFLAMMATORY INTESTINAL DISORDERS
81 86 96 Section 1. Diverticular Disease Section 2. Inflammatory Bowel Disease (Ulcerative Colitis and Crohns Disease) Section 3. Microscopic Colitis (Collagenous and Lymphocytic Colitis) Overview Section 1. Hepatitis Section 2. Primary Biliary Cirrhosis Section 3. Liver Cancer
CHAPTER 6. COLORECTAL CANCER
99 115 127 133
CHAPTER 7. LIVER DISORDERS
III
Gastroenterology Reference Guide
PART 2. GASTROENTEROLOGY TEST LISTING
145 Gastroenterology Test Listing
PART 3. TEST APPLICATION AND INTERPRETATION
191 192 196 196 198 198 200 202 202 225 226 230 234 238 241 244 245 252 252 256 257 258 258 273 278 290 292 293 295 1. Alpha-fetoprotein 2. Alpha-fetoprotein and AFP-L3 3. CA 19-9 4. CA 72-4 5. Carcinoembryonic Antigen 6. CD117, IHC 7. Celiac Disease Comprehensive Panel 8. Colorectal Cancer 8.1 Laboratory Support of Diagnosis and Management 8.2 Carcinoembryonic Antigen 8.3 Fecal Globin 8.4 Microsatellite Instability 8.5 MLH1, MSH2, and MSH6 Mutations 8.6 UGT1A1 Gene Polymorphism 9. E coli Shiga Toxins 10. Epidermal Growth Factor Receptor 11. Food Allergy Guidelines 12. Helicobacter pylori Infection 12.1 Laboratory Support of Diagnosis and Management 12.2 H pylori Antigen 12.3 H pylori Urea Breath Test 13. Hepatitis 13.1 Viral Hepatitis: Laboratory Support of Diagnosis and Management 13.2 Hepatitis B 13.3 Hepatitis C 13.4 Hepatitis E 14. IgA 15. Inflammatory Bowel Disease 16. Lactoferrin
IV
Gastroenterology Reference Guide
Part 1. Gastroenterology Diseases: Summary Information
PART 1. GASTROENTEROLOGY DISEASES: SUMMARY INFORMATION
Gastroenterology Reference Guide
VI
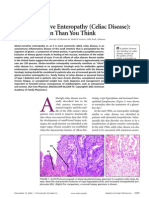
CHAPTER 1. NUTRITIONAL AND MALABSORPTION DISORDERS SECTION 1. CELIAC DISEASE OVERVIEW Celiac disease is caused by an immune response to gluten in genetically susceptible individuals. Gluten is a generic term for the storage proteins that are found in grains (gliadin in wheat, secalin in rye, hordein in barley, avenin in oats). Patients who have an immune response to gluten may develop partial to complete villous atrophy of the small intestine, crypt hyperplasia, and lymphocytic infiltration of the epithelium and lamina propria. Onset of celiac disease may occur at any age from infancy to adulthood. If left untreated, celiac disease may be accompanied by progression of villous atrophy and development of other autoimmune diseases (eg, thyroid disease and insulin-dependent diabetes mellitus), osteoporosis, and neoplasia, including T-cell lymphoma and adenocarcinoma of the small intestine. Dermatitis Herpetiformis (DH)1 DH is a related disorder in that it too is caused by gluten sensitivity. DH manifests as an intensely pruritic papulovesicular skin disease that affects the extensor surfaces of the limbs and trunk and back of the scalp. Onset is usually in the second to fourth decades of life. The spectrum of histopathologic changes in DH resembles the spectrum of changes seen in the small intestine of patients with celiac disease. About 10% to 20% of patients with DH have symptoms of malabsorption, about 20% have atypical symptoms, and the remainder have silent celiac disease.2
Gastroenterology Reference Guide
Chapter 1: Nutritional Disorders
Gastroenterology Reference Guide
Chapter 1: Nutritional Disorders
DH Diagnosis Diagnosis of DH requires a skin biopsy and direct immunofluorescence staining, which reveals the accumulation of granular IgA and C3 deposits in the dermal papillary tips. Note that the abnormal deposits of IgA are found in apparently normal skin near the lesions, but may not be found in the lesions themselves. Biopsies should be taken accordingly. DH Treatment and Prognosis Strict adherence to a gluten-free diet usually results in symptom resolution. Dapsone can be prescribed to relieve symptoms. PREVALENCE Estimated prevalence of celiac disease in the United States is 1:133 people (roughly 1% of the US population or 3 million Americans), which is much greater than previous estimates.3,4 Celiac disease may also occur in patients with Down syndrome, Turner syndrome, Williams syndrome, and selective IgA deficiency. Table 1. Populations with an Increased Prevalence of Celiac Disease4
Population First-degree relatives of individuals with biopsy-proven celiac disease Second-degree relatives of individuals with biopsy-proven celiac disease People with type 1 diabetes mellitus People with Down syndrome Prevalence (%) 4 -12 Undetermined 3-8 5 -12
Gastroenterology Reference Guide
SYMPTOMS Clinical symptoms of celiac disease in adults and children vary widely and depend on the extent of intestinal damage and the duration of nutrient malabsorption. Depletion of a single nutrient may be the only symptom, often manifested as iron or folate deficiency, osteomalacia, and edema from protein loss. Secondary conditions may occur without gastrointestinal symptoms. Nearly 50% of patients may be asymptomatic (silent celiac disease). DIAGNOSIS AND LABORATORY TESTING Prompt diagnosis is important, as the disease can stunt growth and development in children and lead Table 2. Symptoms of Celiac Disease
Primary Gastrointestinal Symptoms Abdominal cramping/ distention Chronic diarrhea* Abdominal pain Foul stools Vomiting (in children) Secondary Malabsorption-Related Manifestations Amenorrhea Hyperparathyroidism Anemia Bone-related symptoms: Pain and fractures Osteoporosis Osteopenia Osteomalacia (vitamin D depletion) Edema (due to hypoalbuminemia) Electrolyte depletion Excessive appetite Fatigue: lack of energy/ general weakness Growth-related symptoms: Delayed puberty Short stature
*Diarrhea lasting >4 weeks.
Infertility and miscarriages Neurological changes (peripheral neuropathy, ataxia) Night blindness (due to vitamin A depletion) Mouth sores or cracked lips Muscle cramping, especially in the hands and legs Reduced padding on the feet and buttocks Smooth tongue Tooth enamel defects Very dry skin Weight loss
Chapter 1: Nutritional Disorders
Gastroenterology Reference Guide
to autoimmune diseases and other complications. Presumptive diagnosis of celiac disease is based upon a combination of symptoms, positive serology, and biopsy of the small intestine.4 Serologic assays can be used to help identify patients who require biopsy and should be performed while the patient is on a glutencontaining diet. Diagnosis is confirmed when symptoms resolve subsequent to a gluten-free diet. A demonstration of normalized histology following a gluten-free diet is no longer required for a definitive diagnosis of celiac disease unless the patient was asymptomatic at the time of initial diagnosis (ie, diagnosis was based solely on biopsy and serology). Testing should be considered for patients with4: Autoimmune disease (thyroiditis, type 1 diabetes mellitus) Cerebellar ataxia Delayed puberty Dental enamel hypoplasia Infertility Iron-deficiency anemia Irritable bowel syndrome Recurrent fetal loss Peripheral neuropathy Persistent aphthous stomatitis Short stature Unexplained gastrointestinal symptoms Unexplained transaminase elevations Celiac disease prevalence is increased in the following and testing may be considered in selected patients4: Down syndrome First- and second-degree relatives with celiac disease Type 1 diabetes mellitus
Chapter 1: Nutritional Disorders
Gastroenterology Reference Guide
Turner syndrome Williams syndrome Serology Tissue transglutaminase (tTG; IgA) antibody is an excellent first-line marker, with high sensitivity and specificity in untreated individuals.5 The endomysial antibody (EMA; IgA) assay has high specificity for celiac disease and is usually used to confirm positive IgA anti-tTG results. It should also be considered in cases in which the IgA anti-tTG result is negative but clinical suspicion remains high. The IgG anti-tTG is usually performed when the total IgA is low. Some patients with limited villous atrophy have been reported to lack EMA and tTG antibodies, and testing for IgA antigliadin antibody (AGA) may help detect celiac disease in such patients.6 Total serum IgA is measured to identify selective IgA deficiency, present in about 2% to 10% of celiac disease patients. Such patients would have negative results on IgA anti-tTG and EMA assays but may have positive IgG anti-tTG results. Because levels of anti-tTG and EMA tend to wane in the absence of gluten ingestion, these markers are useful to monitor adherence to a gluten-free diet. Tests can be performed individually or as a comprehensive panel. Biopsy4,7 Biopsy of the proximal small bowel is indicated in individuals with a positive celiac disease antibody test and for those whose symptoms and other laboratory tests indicate malabsorption. Multiple biopsies should be obtained from the descending part of the duodenum or beyond (as histologic changes may be focal). The pathology report should specify the degree of crypt hyperplasia and villous atrophy as
Chapter 1: Nutritional Disorders
Gastroenterology Reference Guide
well as the number of intraepithelial lymphocytes. Some degree of villous atrophy (Marsh type 3) is considered necessary for a positive biopsy.4 Patients with silent, atypical, or occult celiac disease and those who have DH may exhibit normal or mild villous atrophy; thus, histopathology may not be diagnostic. An infiltrative change with crypt hyperplasia (Marsh type 2) is consistent with celiac disease, but not diagnostic.7 Hyperplasia alone (Marsh type 1) is not specific for celiac disease. In patients with Marsh type 1 or 2, positive serology strengthens the diagnosis. HLA typing, repeat biopsy and/or serology, and a trial of gluten-free diet may be helpful when the diagnosis is still in question.7 Genetic Markers When serology and biopsy results are indeterminate, HLA haplotype testing can be helpful by stratifying an individual into a low- or high-risk category.4 Greater than 97% of people with celiac disease have the DQ2 and/or DQ8 variant; thus, an individual who lacks both is highly unlikely to have celiac disease. However, since about 40% of the general population carry these variants, presence of the variant(s) is not diagnostic of celiac disease.3 TREATMENT Strict adherence to a gluten-free diet is the only treatment for celiac disease and DH. A gluten-free diet is defined by the National Institutes of Health as one that excludes wheat, rye, and barley.4 The glutenfree diet recommendations of the Celiac Sprue Association also exclude spelt, Kamut', and oats. While the information on oats is inconclusive, it should also be excluded due to the potential for gluten contamination during processing.4
Chapter 1: Nutritional Disorders
Gastroenterology Reference Guide
PROGNOSIS Strict adherence to a gluten-free diet usually results in prompt symptom resolution. In most cases, the small intestine heals and returns to normal function. Rarely, people with celiac disease have refractory disease and continue to have symptoms even after theyve eliminated gluten from their diet. Others may develop refractory sprue after an initial, often lengthy, improvement on gluten-free diet. Some people with refractory disease have collagenous sprue in which a layer of collagen-like material is seen below the basement membrane.3 Treatment with immunosuppressive agents may help, though the prognosis is poor.8 The most significant complication of celiac disease is development of gastrointestinal and nongastrointestinal cancers, enteropathy associated T-cell lymphoma (EATL), and other lymphomas. A gluten-free diet may diminish the risk of developing lymphoma.4 A lymphoma should be suspected in patients whose disease was previously controlled by a gluten-free diet and in other patients with refractory disease.3,9 The all-cause mortality for patients with celiac disease is twice that of controls.4 RESOURCES National and regional educational and supportive resources are available. For more information, contact: American Dietetic Association (ADA) Dietary Support Coalition Internet: http://www.eatright.org/Public
Chapter 1: Nutritional Disorders
Gastroenterology Reference Guide
Chapter 1: Nutritional Disorders
Association of Gastrointestinal Motility Disorders Inc. (AGMD) Phone: 781-861-3874 Internet: http://www.agmd-gimotility.org Celiac Disease Foundation (CDF) Phone: 818-990-2354 Internet: http://www.celiac.org Celiac Sprue Association/USA Inc. Phone: 877-CSA-4-CSA (272-4272) Internet: http://www.csaceliacs.org Digestive Disease National Coalition Phone: 202-544-7497 Internet: http://www.ddnc.org Gluten Intolerance Group of North America (GIG) Phone: 206-246-6652 Internet: http://www.gluten.net Intestinal Disease Foundation Phone: 877-587-9606 Internet: http://www.intestinalfoundation.org National Digestive Diseases Information Clearinghouse Phone: 800-891-5389 Internet: http://digestive.niddk.nih.gov/ddiseases/ pubs/celiac/index.htm National Foundation for Celiac Awareness Phone: 215-325-1306 Internet: http://www.celiacawareness.org
Gastroenterology Reference Guide
REFERENCES
1. Yancey KB, Lawley TJ. Immunologically mediated skin diseases. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGrawHill; 2005:311-318. 2. Zone JJ. Skin manifestations of celiac disease. Gastroenterology. 2005;128:S87-S91. 3. Binder HJ. Disorders of absorption. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1763-1776. 4. National Institutes of Health. NIH Consensus Development Conference Statement on Celiac Disease [June 28-30, 2004]. Available at: http://consensus.nih.gov/2004/2004CeliacDisease118html.htm. Accessed October 18, 2006. 5. Farrell RJ, Kelly CP. Diagnosis of celiac sprue. Am J Gastroenterol. 2001;96:3237-3246. 6. Green PH, Jabri B. Coeliac disease. Lancet. 2003;362:383-391. 7. Hill ID, Dirks MH, Liptak GS, et al. Guideline for the diagnosis and treatment of celiac disease in children: recommendations of the North American Society for Pediatric Gastroenterology, Hepatology and Nutrition. J Pediatr Gastroenterol Nutr. 2005;40:1-19. 8. Murray JA. The widening spectrum of celiac disease. Am J Clin Nutrition. 1999;69:354-365. Available at: http://www.ajcn.org/cgi/content/full/ 69/3/354. Accessed October 13, 2005. 9. Celiac disease [MedicineNet website]. Available at: http://www.medicinenet.com/celiac_disease/page11.htm. Accessed October 13, 2005.
Chapter 1: Nutritional Disorders
Gastroenterology Reference Guide
Chapter 1: Nutritional Disorders
SECTION 2. FOOD ALLERGIES OVERVIEW
Food allergy is an immunologically based hypersensitivity to 1 or more foods. Sensitization may occur from ingestion of the substance, from breathing in proteins that are similar to the ones in IgE (Immunoglobin E) the food(s), or through the skin when the barrier function is impaired. This hypersensitivity can involve Also known as reagin, or multiple clinical syndromes and may result in severe reaginic antibody, antigenspecific IgE is 1 of 5 classes and sometime fatal anaphylaxis upon second and of human immunoglobins. It subsequent exposures to the particular food(s). interacts with mast cells and Symptoms can manifest locally in the GI tract or in eosinophils to protect the remote organs.
host against invading parasites. The same antibody-cell combination is also responsible for immediate hypersensitivity allergic reactions such as hay fever, asthma, hives, and anaphylaxis.
Food allergy can manifest as: 1) an immediate, anaphylactic, fixed reaction (typical IgE mediated) or 2) a delayed, chronic, cyclic reaction. The symptom severity of the latter is related to both the quantity and frequency of food ingested. Food allergies occur in people of all ages, though the patterns differ in adults versus children. Children sometimes outgrow their allergies (especially to milk, egg, soy, and wheat); adults do not. Allergies to peanuts, tree nuts, fish, and shellfish are usually enduring. Food allergies should be differentiated from other reactions to foods, including food intolerance and food idiosyncrasy. These adverse reactions to a food or additive involve difficulty with the digestion or metabolism of the substance and are generally localized, temporary, and rarely life threatening.
10
Gastroenterology Reference Guide
PREVALENCE Food allergies are relatively uncommon, affecting 2% to 5% of the general population.1 They occur more often in children (~8%) than in adults (~2%).1 People at risk for food allergies include those with a personal or family history of allergies, especially food allergies. Environmental factors (eg, exposure to tobacco smoke) may also be involved. PREVENTION The American Academy of Pediatrics provides the following recommendations1 to prevent development of a food allergy: Continuation of breastfeeding for 1st year of the infants life Supplement breastfeeding with hypoallergenic formulas if infant at risk Avoidance of peanuts and tree nuts and, possibly, eggs, cows milk, and fish while breastfeeding Introduce solid foods only after 5 months of age in high-risk infants Delay feeding infants dairy products until 1 year of age, eggs until 2 years, and peanuts, nuts, and fish until 3 years The effectiveness of these recommendations, however, is not yet proven.1 SYMPTOMS Symptoms may be mild or severe and may develop gradually or progress rapidly to life-threatening anaphylaxis. Symptoms may involve the skin, gastrointestinal tract, respiratory system, vascular system,
Common Causes of Allergic Food Reactions The most common causes of allergic food reactions in children and adults include: Eggs (hen) Milk (cow) Children Soy Wheat Fish Fruit Shellfish (shrimp, lobster, crab) Vegetables
Chapter 1: Nutritional Disorders
Adults
All
Peanuts Tree Nuts (walnut, cashew, Brazil, pistachio)
11
Gastroenterology Reference Guide
Chapter 1: Nutritional Disorders
or the larynx. Anaphylactic reactions occur more commonly in response to milk, eggs, peanuts, tree nuts, fish, and shellfish than in response to other allergens. Symptoms may include the following: Anaphylaxis (urticaria and angioedema [flushing], bronchospasm) Rhinoconjunctivitis (nasal congestion, runny nose, sneezing) Edema of lips, tongue, palate, throat (difficulty swallowing) Asthma (bronchospasm: difficulty breathing, shortness of breath, wheezing) Hypotension (light-headed, fainting) Nausea, abdominal pain, vomiting, diarrhea Atopic dermatitis (eczema, hives, rash, itching) DIAGNOSIS AND LABORATORY TESTING Diagnosis begins with a relevant history and physical, focusing on: List of suspect foods Quantity of food consumed prior to reaction Repeatability of reaction to particular food Time between exposure (eg, ingestion or inhalation) and reaction Symptoms (type and duration) Examination of target organ systems When the history and physical are consistent with an IgE-related allergy, the next step is usually food-specific IgE testing to determine the presence or absence of an IgE-mediated immune reaction to the suspected food(s). A positive food-specific IgE test is considered diagnostic when consistent with the patients history. If a positive IgE test is not consistent with the history, either an oral food challenge (see below) or a trial
Food-specific IgE Tests Traditionally, food-specific IgE skin tests were performed to diagnose or rule out IgE mediated food allergies. Percutaneous skin tests (PSTs) are recommended over intracutaneous skin tests because intracutaneous tests are overly sensitive, and thus have a high rate of false-positive results, and are associated with risk of anaphylaxis and death. Food-specific IgE serum tests have roughly the same sensitivity and specificity as the skin tests and consequently have the same clinical application. Serum tests are especially useful when the patient has a history of a life-threatening reaction or a medical condition that prevents accurate skin testing (eg, extensive atopic dermatitis or dermatographism) and when the patient is known to have a nonreactive histamine control or is known to be pregnant.
12
Gastroenterology Reference Guide
elimination diet is the recommended next step depending on whether the symptoms are episodic or chronic, respectively.1 In a trial elimination diet, suspected foods are eliminated from the patients diet for several weeks and then gradually reintroduced one at a time while the patient is observed for signs of an allergic reaction. If the IgE test is negative, further evaluation using a double blind, placebo controlled food challenge may be warranted. The patient swallows capsules that contain either the suspected food or a placebo. A third party keeps records of the capsules contents and thus enables the patient and the physician to judge reactions objectively. TREATMENT Dietary avoidance of the implicated food is the primary treatment. However, vague or inaccurate labeling or cross-contamination may result in accidental exposure to the implicated food. If an anaphylactic reaction results, epinephrine should be administered (injected). Individuals subject to anaphylactic reactions should carry injectable epinephrine. PROGNOSIS Prognosis is excellent when dietary avoidance is successful. However, individuals subject to anaphylactic reactions should always carry injectable epinephrine for emergency use. In some cases, dietary avoidance may lead to future tolerance, or partial tolerance, of the food.
Radioimmunoassay procedures (radioallergosorbent test [RAST]) are no longer used. Current methods use a foodspecific allergen bound to a solid phase to detect IgE in the patients serum. World Health Organization-based standards are used to quantify results, which are reported in kIU/L.
Chapter 1: Nutritional Disorders
13
Gastroenterology Reference Guide
Chapter 1: Nutritional Disorders
Additionally, children often outgrow their allergy to substances such as milk, eggs, and wheat. RESOURCES National and regional educational and supportive resources are available. For more information, contact: FDA Center for Food Safety and Applied Nutrition Information About Food Allergies Internet: http://www.cfsan.fda.gov/~dms/ wh-alrgy.html US Food and Drug Administration 5600 Fishers Lane Rockville, MD 20857-0001 Phone: (888) INFO-FDA (463-6332) National Institute of Allergy and Infectious Diseases Phone: 301-496-5717 Internet: http://www.niaid.nih.gov NIAID Office of Communications and Public Liaison 6610 Rockledge Drive, MSC 6612 Bethesda, MD 20892-6612 The Food Allergy & Anaphylaxis Network Phone: 800-929-4040 Internet: http://www.foodallergy.org REFERENCE
1. American College of Allergy, Asthma, and Immunology. Food allergy: a practice parameter. Ann Allergy Asthma Immunol. 2006;96(Suppl 2):S1-S68.
14
Gastroenterology Reference Guide
SECTION 3. LACTOSE INTOLERANCE OVERVIEW Lactose intolerance results from a deficiency in lactase. Individuals who are deficient in this enzyme cannot adequately digest lactose, a carbohydrate present in dairy products. Undigested lactose osmotically attracts water, leading to diarrhea. Furthermore, bacteria in the intestines ferment the lactose, producing gas, which leads to bloating and abdominal pain. Primary Lactose Intolerance Although lactase disappears following the postnatal period in most animals, it is retained in some human ethnic groups and lost in others. Symptoms develop as lactase disappears, usually in the adolescent or adult years. Such individuals are deemed to have primary lactose intolerance, an inherited condition in which lactase is decreased or absent while other digestive enzymes are not. Other aspects of intestinal absorption are usually normal. The amount of dairy products that can be consumed asymptomatically depends on the degree of lactase deficiency; many people are asymptomatic. Secondary Lactose Intolerance Secondary lactase deficiency stems from disorders that damage the small-bowel mucosa (eg, celiac sprue, tropical sprue, and intestinal infection). Other digestive enzymes may be deficient, and the patient may have difficulty absorbing many nutrients. Resolution of the underlying disorder can lead to resolution of the lactase deficiency.
Chapter 1: Nutritional Disorders
15
Gastroenterology Reference Guide
Chapter 1: Nutritional Disorders
Congenital Lactose Intolerance Rarely, infants will be born without lactase. The condition may be either secondary and temporary due to premature birth or primary and permanent. PREVALENCE Since gradual loss of the lactase enzyme is a normal process, many people are affected. The enzymatic loss is more pronounced in African Americans (>85%), Asian Americans (>90%), Hispanics (~80%) and Native Americans (>50%).1,2 In white people of Northern European descent, however, less than 20% are affected.1,2 SYMPTOMS Not all people with lactose intolerance are symptomatic since development of symptoms depends on the degree of lactase deficiency and the amount of dairy products consumed, the speed at which the stomach and small intestines are emptied, and use of antibiotics that affect intestinal microflora. Those who are symptomatic may have: Bloating Abdominal pain or cramps Diarrhea Flatulence Nausea Symptom onset is about 30 minutes to 2 hours after eating or drinking foods containing lactose. Severity varies depending on the amount of lactose each individual can tolerate.
16
Gastroenterology Reference Guide
DIAGNOSIS AND LABORATORY TESTING Diagnosis begins with a review of symptoms, medical history, and physical exam. If lactose intolerance is then suspected, several tests can be used to support the diagnosis. Fecal pH Acidic stool (low pH) is associated with carbohydrate malabsorption; this test is not specific for lactose intolerance, however, so follow-up testing is needed. Lactose Breath Test The amount of exhaled hydrogen is measured before and after ingesting 50 g of lactose. The amount of hydrogen exhaled increases in affected patients subsequent to bacterial fermentation of the lactose. Gas, including hydrogen, is released during fermentation, absorbed into the bloodstream, and carried to the lungs, from which it is expelled. Sensitivity and specificity for lactose intolerance are above 95%.2 Lactose Challenge Blood glucose is measured before and after the patient ingests a lactose load (1.0 to 1.5 g/kg body weight).2 Affected patients develop symptoms and have only a minimal rise in glucose level. This test is less specific than the breath test.2 Therapeutic Trial The patient eliminates dairy products from his/her diet for a period of time prior to undergoing a lactose challenge (eg, 1 quart of milk). If symptoms
Chapter 1: Nutritional Disorders
17
Gastroenterology Reference Guide
Chapter 1: Nutritional Disorders
abate during the period of abstinence and return with the lactose challenge, a presumptive diagnosis of lactose intolerance is made. If symptoms persist while the patient is on a strict lactose deficient diet, inflammatory bowel disease should be suspected since the symptoms of these disorders are similar. TREATMENT There is no cure for lactose intolerance but ingesting either limited amounts or no dairy products can prevent symptoms. Small amounts of milk (<12 oz per day) or yogurt are well tolerated in some patients. Lactase supplements are available in tablet or liquid form and may facilitate lactose digestion in some patients. Calcium supplements should be considered for those restricting their intake of dairy foods. PROGNOSIS Prognosis is excellent. A carefully chosen diet is the key to reducing symptoms and protecting future health. RESOURCES National and regional educational and supportive resources are available. For more information, contact: American Dietetic Association (ADA) 120 South Riverside Plaza, Suite 2000 Chicago, IL 60606-6995 Phone: 800- 366-1655 or 800-877-1600 Internet: http://www.eatright.org
18
Gastroenterology Reference Guide
International Foundation for Functional Gastrointestinal Disorders (IFFGD) PO Box 170864 Milwaukee, WI 53217-8076 Phone: 888-964-2001 Email: iffgd@iffgd.org Internet: http://www.aboutibs.org http://www.iffgd.org REFERENCES
1. Binder HJ. Disorders of absorption. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1763-1776. 2. Gastrointestinal disorders. In: Beers MH, Porter RS, Jones TV, Kaplin JL, Berkwits M, eds. The Merck Manual of Diagnosis and Therapy. 18th ed. Merck Publishing Group; 2006. Available at: http://www.merck.com/ mmpe/sec02/ch017/ch017c.html?qt=lactose%20intolerance&alt=sh. Accessed November 15, 2006.
Chapter 1: Nutritional Disorders
19
Gastroenterology Reference Guide
Chapter 1: Nutritional Disorders
SECTION 4. IRRITABLE BOWEL SYNDROME OVERVIEW Irritable bowel syndrome (IBS), sometimes referred to as spastic colon, is an intestinal motility disorder that interferes with normal function of the colon. IBS manifests with abdominal pain or discomfort, constipation, diarrhea, or both. Usually either constipation or diarrhea is predominant in an individual patient. Structural abnormalities are absent. The colon can be more sensitive and reactive than usual to certain foods and stress. While IBS causes a great deal of discomfort and distress, it does not damage the intestines or lead to any serious complications. Most patients (70%) have mild disease while others (25%) have disease of moderate severity. The remainder (5%) have severe disease.1,2 ETIOLOGY The cause of IBS is not clear. There appears to be a complex interaction between genetics, the environment, psychosocial factors (eg, life stress, psychologic state, coping mechanisms, social support), and physiology (eg, gut motility, visceral hypersensitivity). Symptoms may occur following gastrointestinal infection, increased fat or alcohol intake, traveling, vigorous physical activity, or psychologic stress. PREVALENCE IBS is a relatively common disorder that affects 10% to 20% of people in the United States.2 The disorder occurs twice as often in women than in men,2 and
20
Gastroenterology Reference Guide
80% of those with severe symptoms are women.1 Prevalence is similar in whites and African Americans, but may be lower in Hispanics.2 Patients usually first present in the third to fifth decades of life.2 SYMPTOMS Symptoms usually occur during the day, but not at night. They are episodic, lasting an average of 5 days and may occur several times a month.2 Periods of constipation may be followed by a period of diarrhea. Symptoms wax and wane over the years.2 Symptoms of IBS include: Abdominal pain, often relieved by defecation or passing of gas Bloating Perceived flatulence Constipation and/or diarrhea due to altered rate of stool movement through the intestinal tract Mucus in the stool Sensation of incomplete evacuation after defecation Rectal urgency and/or incontinence Dyspepsia Heartburn Nausea, vomiting If the above symptoms occur without pain, alternative diagnoses should be sought. Factors that exacerbate IBS symptoms include: Eating, especially when rapid; especially lipids Emotional/psychiatric stress Premenstrual and menstrual phases Particular foods (patient specific)
Chapter 1: Nutritional Disorders
21
Gastroenterology Reference Guide
Chapter 1: Nutritional Disorders
DIAGNOSIS AND LABORATORY TESTING Diagnosis is primarily based on clinical features and exclusion of other disorders and thus begins with a complete medical history and physical examination. The Rome III diagnostic criteria (Table 1) define the disorder. When a patient meets the Rome criteria but presents with alarm signs (ie, those suggesting another diagnosis) (Table 2), further testing is recommended. If alarm signs are absent, another diagnosis is rarely made and further testing may not be warranted. Diagnostic algorithms are presented in references 4 and 2 for the primary care physician and gastroenterologist, respectively. The following diagnostic tests may be employed, depending on a particular patients situation: Complete blood count (CBC) Hemoccult (stool blood test) Sedimentation rate (ESR) Serum chemistries TSH Ova and parasites (O&P) Colonoscopy or sigmoidoscopy Endomysial and tissue transglutaminase IgA antibodies to rule out celiac sprue Table 1. Rome III Diagnostic Criteria1-3
At least 3 months, which need not be consecutive, in the preceding 6 months of abdominal discomfort or pain associated with 2 of the following 3 features: 1. Relieved by defecation 2. Onset associated with a change in frequency of stool 3. Onset associated with a change in form (appearance) of stool
22
Gastroenterology Reference Guide
Table 2. Primary Features Suggesting Non-IBS Diagnosis
Absence of concurrent psychosocial symptoms Family history of colon cancer or inflammatory bowel disease Onset at an older age Persistent diarrhea after a 48-hour fast Presence of nocturnal diarrhea or steatorrheal stools Progressive course of disease Vomiting Weight loss Anemia Increased sedimentation rate Leukocytes or blood in stool Stool volume >200 to 300 mL/d
Chapter 1: Nutritional Disorders
Differentiating IBS and Inflammatory Bowel Disorder (IBD) Patients with IBD may develop rectal bleeding and permanent intestinal damage. Additionally, they frequently require long-term steroid therapy and immunosuppressive agents. Consequently, distinguishing IBS from IBD is critical for patient management. Fecal Lactoferrin Increased in active IBD Not increased in IBS 86% sensitive and 100% specific in distinguishing IBD from IBS5
Fecal lactoferrin to rule out inflammatory bowel disorder H. pylori test to rule out peptic ulcer disease Hydrogen breath test or therapeutic trial to rule out lactose intolerance Therapeutic trials for constipation (fiber or osmotic laxative), diarrhea (loperamide, diphenoxylateatropine, cholestyramine), pain/gas/bloating (anticholinergic, antidepressant, psychologic treatment) Imaging studies (GI tract, gallbladder) TREATMENT Therapy varies depending on the type of symptoms (eg, predominant constipation vs diarrhea) and their severity and on the presence of psychosocial problems. All patients should be educated about the disorder. Regular physical activity helps alleviate stress and improve bowel function. Some patients may benefit from dietary changes if certain substances exacerbate symptoms. These
23
Gastroenterology Reference Guide
substances may include fatty foods, beans and other gas-producing foods (eg, apples, grape juice, bananas, nuts, raisins, cabbage), alcohol, caffeine, and lactose. High fiber diets and stool bulking agents may be helpful in some but not others; data regarding efficacy is controversial. Certain types of sugar (eg, sorbitol, mannitol, fructose) might also be problematic for some patients. Medications may include the following: Antispasmodics (anticholinergics) for pain and bloating Antidiarrheal agents (loperamide [Imodium'], diphenoxylate, cholestyramine) Osmotic laxatives (milk of magnesia, sorbitol, polyethylene glycol) for constipation Antidepressants (eg, tricyclics, selective serotonin reuptake inhibitors [SSRIs]) 5-HT3 receptor antagonists (cilansetron) for diarrhea and pain 5-HT4 receptor agonists (tegaserod) for constipation Biofeedback, acupuncture, yoga, and meditation may help some patients. PROGNOSIS IBS is a lifelong condition with exacerbations and remissions, but most people can control their symptoms with diet, stress management, and medication. For others, IBS can be severe and disabling.
Chapter 1: Nutritional Disorders
24
Gastroenterology Reference Guide
RESOURCES Association of Gastrointestinal Motility Disorders (AGMD) 11 North Street Lexington, MA 02420 Phone: 781-861-3874 Email: AGMDInc@aol.com Internet: http://www.agmd-gimotility.org International Foundation for Functional Gastrointestinal Disorders (IFFGD) PO Box 170864 Milwaukee, WI 53217-8076 Phone: 888-964-2001 Email: iffgd@iffgd.org Internet: http://www.aboutibs.org http://www.iffgd.org REFERENCES CITED
1. Owyang C. Irritable bowel syndrome. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1789-1793. 2. Drossman DA, Camilleri M, Mayer EA, et al. AGA technical review on irritable bowel syndrome. Gastroenterology. 2002;123:2108-2131. 3. Drossman D. The launching of Rome III. Available at: http://www.romecriteria.org/launch.pdf#search=%22Rome%20Criteria %20III%20IBS%22. Accessed: September 22, 2006. 4. Fass R, Longstreth G, Pimentel M, et al. Evidence- and consensus-based practice guidelines for the diagnosis of irritable bowel syndrome. Arch Intern Med. 2001;161:2081-2088. 5. Kane SV, Sandborn WJ, Rufo PA, et al. Fecal lactoferrin is a sensitive and specific marker in identifying intestinal inflammation. Am J Gastroenterol. 2003;98:1309-1314.
Chapter 1: Nutritional Disorders
ADDITIONAL REFERENCE
1. Irritable bowel syndrome (IBS). In: Beers MH, Porter RS, Jones TV, Kaplin JL, Berkwits M, eds. The Merck Manual of Diagnosis and Therapy. 18th ed. Merck Publishing Group; 2006. Available at: http:// www.merck.com/mmpe/sec02/ch008/ch008e.html?qt=inflammatory%20 bowel%20syndrome&alt=sh. Accessed November 16, 2006.
25
Gastroenterology Reference Guide
Chapter 1: Nutritional Disorders
26
CHAPTER 2. ESOPHAGEAL DISORDERS
Gastroenterology Reference Guide
SECTION 1. GASTROESOPHAGEAL REFLUX DISEASE OVERVIEW Gastroesophageal reflux disease (GERD) is a highly variable chronic condition that is characterized by periodic episodes of gastroesophageal reflux, classically accompanied by heartburn. Incompetent barriers at the gastroesophageal junction enable the backflow of gastric acid and other gastric contents into the esophagus, pharynx, larynx, and tracheobronchial tree, which in turn causes the symptoms of GERD. Over time, the acid may damage the lining of the esophagus. Untreated, GERD can progress to esophagitis. Severe reflux esophagitis can be complicated by Barretts esophagus, a risk factor for cancer. ETIOLOGY Reflux occurs when the pressure gradient between the lower esophageal sphincter (LES) and the stomach is either lost or inadequate. This may be due to unexplained muscle weakness or loss of tone in the LES as well as a myriad of other causes such as myopathy, pregnancy, smoking, and medications, to name a few. Ineffectiveness of the diaphragmatic crural muscle can also set the stage for GERD. Factors that may contribute to reflux include: Increase in gastric volume (eg, after meals) Increase in proximity of gastric contents to the gastroesophageal junction as occurs when lying or bending down or with a hiatal hernia
Chapter 2: Esophageal Disorders
27
Gastroenterology Reference Guide
Increase in gastric pressure caused by obesity, pregnancy, tight clothing, and ascites Ingestion of certain substances including alcohol, caffeine, carbonated beverages, fatty foods, chocolate, and mint
Chapter 2: Esophageal Disorders
PREVALENCE The published prevalence figures vary depending on the source; however, one thing is clear: GERD is relatively common. It may affect as many as 40% of adults in the United States.1-3 SYMPTOMS The most common symptoms include: Regurgitation of gastric contents (sour material) into the mouth Heartburn (burning sensation due to irritation of the esophagus by acidic gastric contents) Less common symptoms include: Chronic cough Bronchoconstriction Pharyngitis Laryngitis Bronchitis Pneumonia Morning hoarseness Wheezing (asthma) Angina-like or atypical chest pain Dysphagia Some patients are asymptomatic and do not seek treatment until severe complications occur.
28
Gastroenterology Reference Guide
Infants may also present with irritability, vomiting, and anorexia. DIAGNOSIS AND LABORATORY TESTING Most people with GERD can be diagnosed based on their symptoms. Diagnostic tests (Table 1) may be helpful for patients who have either no response or inadequate response to treatment and those with evidence of complications. TREATMENT The goals of treatment are to provide symptom relief, heal erosive esophagitis, and prevent further complications. Table 2 details therapeutic options. PROGNOSIS Treatment is usually effective in suppressing acid reflux and heartburn. Standard doses of PPI therapy can heal esophageal erosion within 8 weeks in about Table 1. Diagnostic Tests for GERD1,2,4
Test Barium esophagram (ie, barium swallow radiograph, an X-ray study of the esophagus) Endoscopy with biopsy, if indicated Esophageal pH (ie, ambulatory reflux monitoring) Purpose Diagnose peptic stricture or esophageal ulcer; relatively low sensitivity and specificity compared with endoscopy Diagnose erosive esophagitis, peptic stricture, ulcer, Barretts esophagus, or adenocarcinoma Document and quantitate acid reflux in symptomatic patients who are unresponsive to treatment and have an unremarkable endoscopy Ensure accurate placement of pH probes (see above); determine degree of competence of the LES and esophageal motor function prior to surgical treatment
Chapter 2: Esophageal Disorders
Esophageal manometry (motility study)
29
Gastroenterology Reference Guide
Table 2. GERD Therapy1,2,4
Lifestyle changes* Weight reduction, if indicated Elevate head while sleeping (4-6 inches) Avoid tobacco, fatty foods, coffee, alcohol, chocolate, mint, orange juice
Chapter 2: Esophageal Disorders
Avoid certain medications (eg, anticholinergics, smoothmuscle relaxants, calcium channel blockers) Avoid large fluid intake with meals Avoid eating within 2 to 3 hours of bedtime Avoid tight clothing Medications Antacids o Useful in mild cases o Available over-the-counter o Include: Alka-Seltzer', Maalox', Mylanta', Pepto-Bismol', Rolaids', Tums' Proton pump inhibitors (PPI) o Acid suppressor (provides symptomatic relief and heals esophagitis) o Include: Prilosec', Prevacid', Nexium', Protonix', Aciphex') H2 receptor blocking agents o Acid suppressor (provides symptomatic relief and heals esophagitis) o Less effective than PPIs, but may be useful in less severe cases o Include: Tagamet HB', Pepcid AC', Axid AR', Zantac 75') Promotility agents o Used in conjunction with acid suppressor for selected patients o Side effects are common o Include: metoclopramide, bethanechol, cisapride, domperidone tegaserod, baclofen Surgery Endoscopic therapy
*Of uncertain efficacy.4
Fundoplication (gastric fundus is wrapped around the LES to increase LES pressure) Radiofrequency application (eg, Stretta') Endoscopic sewing techniques
30
Gastroenterology Reference Guide
90% of patients.1 Therapy may have to be prescribed long-term, however, to keep symptoms from returning. In untreated or refractory patients, GERD may cause serious complications: Reflux esophagitis occurs when acid, pepsin, and bile damage the mucosa. o Mild esophagitis is characterized by infiltration of the mucosa with eosinophils or granulocytes, basal cell hyperplasia, and elongation of dermal pegs. o Erosive esophagitis involves more severe mucosal damage that can result in esophageal bleeding ulcers. Peptic stricture occurs when fibrosis causes constriction of the lumen (frequency: ~10% of untreated cases). Barretts esophagus, a rare premalignant condition, occurs in some patients with erosive esophagitis. REFERENCES
1. Goyal RK. Diseases of the esophagus. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1739-1746. 2. Gastroesophageal reflux disease (GERD). In: Beers MH, Porter RS, Jones TV, Kaplin JL, Berkwits M, eds. The Merck Manual of Diagnosis and Therapy. 18th ed. Merck Publishing Group; 2006. Available at: http://www.merck.com/mmpe/sec02/ch012/ch012f.html?qt=gerd&alt= sh. Accessed November 21, 2006. 3. Delaney BC. Review article: prevalence and epidemiology of gastrooesophageal reflux disease. Aliment Pharmacol Ther. 2004;20(Suppl 8):2-4. 4. DeVault KR, Castell DO. Updated guidelines for the diagnosis and treatment of gastroesophageal reflux disease. Am J Gastroenterol. 2005;100:190-200.
Chapter 2: Esophageal Disorders
31
Gastroenterology Reference Guide
SECTION 2. BARRETTS ESOPHAGUS OVERVIEW The American College of Gastroenterology (ACG) defines Barretts esophagus as a change in the esophageal epithelium of any length that can be recognized at endoscopy and is confirmed to have intestinal metaplasia by biopsy of the tubular esophagus and excludes intestinal metaplasia of the cardia.1 Barretts esophagus is characterized by replacement (metaplasia) of esophageal squamous epithelium with columnar epithelium during healing of acute esophagitis. Columnar epithelium is more resistant to damage by acid and pepsin than is squamous epithelium. Short-segment Barretts (<2-3 cm in length) appears to be less severe than long-segment Barretts (>2-3 cm). The metaplasia in both, however, can lead to dysplasia and esophageal adenocarcinoma. ETIOLOGY Barretts esophagus is a complication of severe reflux esophagitis, which is a complication, in turn, of gastroesophageal reflux disease (GERD) (see Chapter 2, Section 1). PREVALENCE About 0.5% of people develop long-segment Barretts while about 15% develop short-segment Barretts.2 The disorder occurs more frequently in white men than in women or in men of other ethnicities. Prevalence increases with increasing age. More importantly, Barretts esophagus is most prevalent in those who have chronic (10 years) GERD symptoms.1
Chapter 2: Esophageal Disorders
32
Gastroenterology Reference Guide
SYMPTOMS Most people with Barretts esophagus have symptoms of GERD; some people, however, are asymptomatic. There are no clinical symptoms that differentiate people who have GERD without Barretts esophagus from those who have GERD with Barretts esophagus. DIAGNOSIS AND LABORATORY TESTING Since people with chronic GERD symptoms are more likely to have Barretts esophagus, the ACG recommends upper endoscopy for such patients after reflux symptoms are controlled with therapy.1 Biopsy of abnormal esophageal mucosa should then be taken to document intestinal metaplasia (eg, replacement of squamous epithelium by columnar epithelium) and to detect dysplasia, which is the first step in the neoplastic process.1 TREATMENT When active esophagitis is present, patients are treated with acid suppression therapy and, possibly, with surgery. Although such treatment can control GERD symptoms and maintain a healed mucosa, it does not reduce the grade of Barretts esophagus nor eliminate the risk of cancer. Endoscopic surveillance (Table 1) is instituted to monitor the patient for dysplasia and early adenocarcinoma. Endoscopic mucosal resection (esophagectomy) may be advisable for patients with multifocal dysplasia and/or mucosal irregularity.1 Such an approach may prevent frank cancer and the associated risk of metastasis.
Chapter 2: Esophageal Disorders
33
Gastroenterology Reference Guide
Table 1. Endoscopic Surveillance of Patients with Barretts Esophagus1
Degree of Dysplasia No dysplasia* Low-grade
Chapter 2: Esophageal Disorders
Surveillance Endoscopy at 3-year interval Endoscopy and biopsy yearly until dysplasia no longer detected Endoscopy and biopsy every 3 months
High-grade, focal
*On 2 consecutive endoscopies with biopsy.
Other treatments include photodynamic therapy and surgical esophagectomy. PROGNOSIS Control of GERD symptoms and periodic monitoring of patients with Barretts esophagus, followed by surgical resection when clinically indicated, is the best hope of survival for these patients. REFERENCES
1. Sampliner RE and the Practice Parameters Committee of the American College of Gastroenterology. Updated guidelines for the diagnosis, surveillance, and therapy of Barretts esophagus. Am J Gastroenterol. 2002;97:1888-1895. 2. Goyal RK. Diseases of the esophagus. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1739-1746.
34
Gastroenterology Reference Guide
SECTION 3. ESOPHAGEAL CANCER OVERVIEW Cancer of the esophagus is a lethal cancer as evidenced by the equivalence between the yearly number of cases diagnosed and the number of deaths.1 Esophageal cancers are either squamous cell carcinomas or adenocarcinomas. Squamous cell esophageal carcinoma arises in squamous cells lining the esophagus and usually occurs in the upper (cervical) and middle part of the esophagus. Adenocarcinoma usually develops in the glandular tissue in the lower (distal) part of the esophagus. Adenocarcinomas account for more than 50% of all esophageal cancers.2
Esophageal Cancers2 15% occur in the cervical esophagus 35% occur in the midesophagus RISK FACTORS 50% occur in the lower Risk factors associated with esophageal carcinoma are esophagus
Chapter 2: Esophageal Disorders
listed in Table 1. Alcohol and tobacco use are the strongest risk factors for squamous cell disease, while Table 1. Esophageal Carcinoma Risk Factors2,3
Squamous cell Alcohol consumption (excess)* Cigarette smoking* Chronic achalasia Diet deficient in molybdenum, zinc, vitamin A Esophageal irradiation Extremely hot tea (long-term ingestion) Adenocarcinoma Barretts esophagus Chronic GERD Fanconis anemia Ingestion of nitrites or lye Obesity Plummer-Vinson or Paterson-Kelly syndrome Tylosis (congenital hyperkeratosis and pitting of palms and soles) Cigarette smoking Obesity
GERD, gastroesophageal reflux disease. *Risk increases with increasing use; these 2 factors increase risk synergistically.
35
Gastroenterology Reference Guide
Barretts esophagus is the strongest risk factor for adenocarinoma. PREVALENCE The American Cancer Society estimates there will be 14,550 new cases and 13,770 deaths from esophageal cancer in the United States in 2006.1 It affects more African Americans than whites and approximately 3 times as many men as women.2,3 Most cases occur in older people (ie, 65-74 years of age).3 SYMPTOMS In the early stages of esophageal cancer, patients are asymptomatic. Symptoms usually do not manifest until the disease is incurable. The first 2 symptoms listed in Table 2 are classic and affect most patients. Patients have difficulty swallowing solid food when first presenting with dysphagia. As the disease progresses, the patient will have difficulty swallowing semi-solid foods and, finally, liquids (including saliva). Weight loss occurs in 75% of patients.3 SCREENING General population screening is not recommended for either type of esophageal cancer; however, the American Gastroenterological Association (AGA) Table 2. Symptoms of Esophageal Carcinoma
Progressive dysphagia Weight loss Aspiration pneumonia Cough Gastrointestinal bleeding Hiccups Hoarseness Pain in the chest or back Pain when swallowing Regurgitation Vocal cord paralysis Vomiting
Chapter 2: Esophageal Disorders
36
Gastroenterology Reference Guide
supports endoscopic screening for a subgroup of patients with gastroesophageal reflux disease (GERD).3 This subgroup consists of white males over 50 years of age. Other high-risk groups that may be suitable for screening include those with tylosis, lyeinduced strictures, Fanconis anemia, achalasia, and prior head-and-neck cancer as well as those with chronic tobacco and alcohol use.3 SURVEILLANCE The AGA supports periodic monitoring of patients with Barretts esophagus.3 Four-quadrant biopsies of Barretts mucosa (every 1-2 cm, depending on degree of dysplasia) may be performed. The AGA recommendations are similar to those of the American College of Gastroenterology (Table 3). Patients with confirmed high-grade dysplasia may be treated with surgical resection and mucosal ablation with photodynamic therapy (PDT) to prevent cancer development. DIAGNOSIS AND LABORATORY TESTING During an endoscopic procedure, biopsies are taken from any suspicious areas. A cytologic examination is then performed on the tissue. Cytology of tumor
Chapter 2: Esophageal Disorders
Table 3. Frequency of Monitoring Patients with Barretts Esophagus3,4
Degree of Dysplasia None Low-grade High-grade AGA Recommendations 5-year intervals 1 to 2 year intervals 3-month intervals for 2 years, then every 6 months ACG Recommendations 3-year intervals Yearly until dysplasia no longer detected Every 3 months
AGA, American Gastroenterological Association; ACG, American College of Gastroenterology.
37
Gastroenterology Reference Guide
brushings may be indicated to complement biopsies. Inspection of the larynx, trachea, and bronchi, in addition to the esophagus, may be advisable in patients with a history of smoking and alcohol use. Since treatment decisions are based on the stage of disease, the following procedures should be considered to assess stage: computed tomography (CT) of the chest and upper abdomen, endoscopic ultrasonography (EUS), fine-needle aspiration, and positron emission tomography (PET). STAGING The American Joint Committee on Cancer (AJCC) has outlined terminology for staging esophageal Table 4. TNM Staging of Esophageal Cancers3
Tumor staging T0 Tis T1 T2 T3 T4 Nodal staging N0 N1 Metastasis M0 M1 M1a M1a M1b M1b X No evidence of primary tumor Carcinoma in situ Tumor invades lamina propria or submucosa Tumor invades muscularis propria Tumor invades adventitia Tumor invades adjacent structures No evidence of metastasis to regional lymph nodes Evidence of metastasis to regional lymph node(s) No evidence of distant metastasis Evidence of distant metastasis Metastasis to celiac nodes (tumor in lower thorax) Metastasis to cervical nodes (tumor in upper thorax) Metastasis to nonregional or other nodal groups (tumor in midthorax) Distant metastasis (tumor in lower esophagus or upper thorax) Unable to assess metastasis presence/absence
Chapter 2: Esophageal Disorders
38
Gastroenterology Reference Guide
Table 5. Definition of Esophageal Cancer Stages3
Stage 0 1 2a 2b 3 3 4 4a 4b Definition Tis, N0, M0 T1, N0, M0 T2-3, N0, M0 T1-2, N1, M0 T3, N1, M0 T4, any N, M0 Any T, any N, M1 Any T, any N, M1a Any T, any N, M1b
Chapter 2: Esophageal Disorders
cancers (Tables 4 and 5).3 Tumor staging may be further divided as shown in Table 6. TREATMENT Endoscopic resection is commonly used for squamous cell cancers confined to the mucosa or upper third of the submucosa. Endoscopic resection with or without photodynamic therapy (PDT) is used to treat adenocarcinomas detected in an early stage (stages 1 and 2a). Patients with more advanced disease (stage 2b or 3) might be treated with radiation and chemotherapy (neoadjuvant therapy) before undergoing surgery. This helps lower the stage of the cancer prior to surgical resection, thereby improving the chance of survival. Patients
Table 6. Sub-categorization of T1 Stage3
T1m T1sm T1sm1 T1sm2 T1sm3 T1 confined to the mucosa T1 penetrating the submucosa T1sm in upper third of submucosa T1sm in middle third of submucosa T1sm in lower third of submucosa
39
Gastroenterology Reference Guide
with stage 4 disease are treated with either radiation/chemotherapy or palliative therapy. PROGNOSIS If diagnosed and treated at an early stage, patients with esophageal cancer have a good chance of 5-year survival. However, if not diagnosed and treated until a later stage, prognosis is poor. Thus, screening and monitoring of high-risk individuals is critical to management of this cancer. RESOURCES National and regional educational and supportive resources are available. For more information, contact: American Cancer Society Phone: 800-ACS-2345 (227-2345) Internet: www.cancer.org Cancer Care, Inc. Phone: 800-813-HOPE (813-4673) or 212-221-3300 Email: info@cancercare.org Internet: www.cancercare.org Cancer Hope Network Phone: 877-HOPENET (467-3638) or 908-879-4039 (New Jersey Residents) Email: info@cancerhopenetwork.org Internet: www.cancerhopenetwork.org Cancer Information Service (CIS) Phone: 800-4-CANCER (422-6237) TTY: 800-332-8615 (for deaf and hard of hearing) Internet: http://cis.nci.nih.gov/
Chapter 2: Esophageal Disorders
40
Gastroenterology Reference Guide
National Cancer Institute Phone: 800-422-6237 or 301-496-6631 Internet: www.cancer.gov www.nci.nih.gov NCI's Facing Forward Series Phone: 888-4-CANCER (422-6237) Internet: www.nci.nih.gov/cancerinfo/ life-after-treatment National Coalition for Cancer Survivorship Phone: 877-622-7937 or 301-650-9127 Email: info@canceradvocacy.org Internet: http://www.canceradvocacy.org The Cancer Information Network Internet: www.cancerlinksusa.com/stomach/ index.asp The Wellness Community Executive Office Phone: 888-793-WELL (793-9355) or 202-659-9709 Email: help@thewellnesscommunity.org Internet: www.thewellnesscommunity.org REFERENCES
1. American Cancer Society. Cancer Facts and Figures 2006. Atlanta: American Cancer Society; 2005. Available at: http://www.cancer.org/ docroot/STT/stt_0.asp. Accessed November 21, 2006. 2. Mayer RJ. Gastrointestinal tract cancer. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:523-533. 3. Wang KK, Wongkeesong M, Buttar NS. American Gastroenterological Association technical review on the role of the gastroenterologist in the management of esophageal carcinoma. Gastroenterology. 2005;128:14711505. Also available at: http://scholar.google.com/scholar?hl=en&lr=&q= cache:DL2IvPLiS7wJ:www.spg.pt/docspdfs/ AGAesofago.pdf+. Accessed November 22, 2006. 4. Sampliner RE and the Practice Parameters Committee of the American College of Gastroenterology. Updated guidelines for the diagnosis, surveillance, and therapy of Barretts esophagus. Am J Gastroenterol. 2002;97:1888-1895.
Chapter 2: Esophageal Disorders
41
Gastroenterology Reference Guide
Chapter 2: Esophageal Disorders
42
CHAPTER 3. STOMACH DISORDERS
Gastroenterology Reference Guide
SECTION 1. PEPTIC ULCER DISEASE ( HELICOBACTER PYLORI INFECTION) OVERVIEW Peptic ulcer disease (PUD) is characterized by ulcers within the stomach and/or duodenum. Such ulcers may be caused by Helicobacter pylori infection, ingestion of a non-steroidal anti-inflammatory drug (NSAID), or, rarely, Zollinger-Ellison syndrome. H pylori accounts for most PUD (~70% of gastric ulcers and up to 90% of duodenal ulcers).1 NSAIDs are the second most common cause of PUD. Subsequent to the withdrawal of some COX-2 inhibitors (eg, rofecoxib, valdecoxib), NSAIDinduced PUD may be on the rise, especially in the elderly. Like NSAIDs, COX-2 inhibitors reduce inflammation, but without irritating the stomach as do the NSAIDs. With the diminished availability of the COX-2 inhibitors, doctors must again rely on NSAIDs to treat inflammatory conditions in spite of the damaging side effects. Since H pylori accounts for such a large proportion of PUD, it will be the focus of the discussion in this section. H pylori infection is a gram-negative bacterium that colonizes the stomach. It is suited to living in a highly acidic environment owing to its ability to produce urease. Urease stimulates production of ammonia from urea, and the ammonia damages the epithelial cells lining the stomach wall, making it susceptible to gastric acid. The bodys inflammatory response leads to further epithelial cell damage, and other enzymes produced by H pylori damage the mucosa. Damage can lead to gastritis, PUD, mucosal-associated lymphoid-type (MALT) lymphoma, and gastric cancer.
Chapter 3: Stomach Disorders
43
Gastroenterology Reference Guide
Another important factor in H pylori infection is the ability of the bacterium to move from the antrum of the stomach to more proximal segments of the stomach. Location of the bacterium is associated with clinical disease: antral-predominant infection is most closely linked with increased acid secretion and duodenal ulcers, whereas infection primarily in the body of the stomach (corpus-predominant) is linked with decreased acid secretion, gastric ulcers, and development of gastric cancer. ETIOLOGY AND RISK FACTORS
Chapter 3: Stomach Disorders
H pylori is acquired via oral-oral and fecal-oral routes. Risk of acquiring the infection is associated with: Poor socioeconomic status Less education Birth or residence in a developing country Domestic overcrowding Unsanitary living conditions, including unclean food and water Exposure to gastric contents of infected individual (eg, vomit, contaminated endoscope) Other factors contributing to ulcer development include NSAIDs, cigarette smoking, and selected chronic disorders (eg, systemic mastocytosis, pulmonary disease, renal failure, cirrhosis, nephrolithiasis, alpha1-antitrypsin deficiency). Evidence implicating a role for genetic predisposition, personality type, psychological stress, certain foods, alcohol, or caffeine is inconclusive.
44
Gastroenterology Reference Guide
PREVALENCE Acid peptic disorders affect about 4 million people per year in the United States.2 This equates to a 10% to 12% lifetime prevalence of PUD.2 Overall, about 30% of the U.S. population is infected with H pylori.2 Some of these infections are asymptomatic or mild; not all progress to PUD. H pylori prevalence increases with increasing age and is more prevalent in African Americans and Hispanics. The prevalence of both PUD and H pylori infection is declining owing to improved sanitation and medical intervention. SYMPTOMS PUD is characterized by dyspepsia. Burning or gnawing epigastric pain that is worse when fasting and relieved by eating is common, but not seen in all patients. Alternatively, the patient may experience an ill-defined, aching or hunger sensation. Some patients experience no symptoms until they have a bleeding ulcer. In patients with gastric ulcer, pain may be precipitated, rather than relieved, by eating. Bloating, nausea, vomiting, and weight loss may also occur and may suggest more complicated disease. In patients with duodenal ulcer, patients may awake with abdominal pain in the middle of the night. They are more likely to experience relief 2 to 3 hours after eating or after ingesting an antacid. Signs of complicated PUD (gastrointestinal bleeding, perforation, gastric outlet obstruction) include:
Chapter 3: Stomach Disorders
45
Gastroenterology Reference Guide
Variation in intensity or distribution of abdominal pain Consistent pain, not relieved by food or antacid Pain radiating to the back Sudden onset of severe, generalized abdominal pain Nausea, vomiting Weight loss Bloody or black stools Vomit with appearance of coffee grounds Anemia
Chapter 3: Stomach Disorders
DIAGNOSIS AND MANAGEMENT Endoscopy enables visualization of the ulcer; it is the method of choice for definitive diagnosis of PUD, being preferred over barium radiography.1 Additionally, endoscopy enables early detection of gastric cancer and Barretts esophagus. However, since endoscopy is expensive, other options may be preferable for managing patients with upper abdominal pain (dyspepsia). Options include: Empirical acid suppression Noninvasive H pylori test followed by endoscopy if positive Noninvasive H pylori test followed by eradication therapy if positive (ie, "test and treat") Empirical H pylori eradication therapy (no testing) Early endoscopy The American Gastroenterological Association (AGA) recommends H pylori test and treat (followed by acid suppression if symptoms persist) for patients with dyspepsia who are <55 years of age and have no alarm symptoms (eg, weight loss, dysphagia, signs of blood loss).3 This approach is cost-effective and may prevent distal gastric cancer; however, empirical acid
46
Gastroenterology Reference Guide
suppression may be a good choice when the prevalence of H pylori is 10%.3 For older patients and those with alarm features, the AGA recommends early endoscopy.3 A biopsy should be taken during endoscopy for H pylori testing. If positive, eradication therapy can be instituted to reduce the risk of PUD and gastric cancer.3 LABORATORY TESTING FOR DIAGNOSIS Invasive and noninvasive tests are available for H pylori: Upper gastrointestinal tract biopsy, histologic exam, rapid urease testing (RUT), and culture Antibody detection Antigen detection Urea breath test (BreathTek' UBiT') employing 14 C- or 13C-urea When endoscopy is not indicated, the preferred methods for H pylori testing are the 13C-urea breath test and the stool antigen tests, because serology (antibody detection) is less accurate and does not differentiate active from resolved infection.3 When endoscopy is indicated, histology is the test of choice. Culture is not very sensitive but may be useful for antibiotic resistance testing in patients unresponsive to therapy. Rationale Against the Use of Serologic Tests4 Serologic tests are not suitable for diagnosis of H pylori infection. They detect the presence of antibodies to H pylori rather than the bacterium itself. H pylori antibody levels may persist for years after eradication of infection (ie, the H pylori bacterium).
Chapter 3: Stomach Disorders
47
Gastroenterology Reference Guide
Presence of antibody could indicate an active infection or a resolved, cured infection. Treating uninfected, cured people o Is ineffective (ie, no treatment response) o Contributes to the growing problem of antibiotic resistance o Adds needless cost. Antibody tests are relatively insensitive (ie, more false-negative test results). Conversely, urea breath and stool antigen tests can distinguish between active and resolved infection. H pylori bacteria must be present to get a positive test result: Urea breath test indirectly detects urease produced by H pylori bacteria. Stool antigen test uses anti-H pylori antibody to detect H pylori antigen. Thus, both urea breath and stool antigen tests can be used for diagnosis. Moreover, the higher sensitivity and specificity of these tests lead to even better performance when prevalence is low. This is particularly important since the prevalence of H pylori infection is declining in the U.S. Urea Breath Test5 H pylori bacteria produce the enzyme urease which hydrolyzes urea to produce ammonia and carbon dioxide (CO2). The CO2 is then exhaled in the breath and can be measured using an infrared spectrophotometer. This chemical reaction is the basis of the UBiT test:
Chapter 3: Stomach Disorders
48
Gastroenterology Reference Guide
1. An initial, baseline breath sample is tested to determine the ratio of 13CO2 to 12CO2. This ratio will be low because almost all naturally occurring urea in the body is 12C-urea. 2. After the patient ingests 13C-urea, a synthetic urea comprised of stable, naturally occurring, nonradioactive carbon-13, the ratio of 13CO2 to 12 CO2 is determined again. 3. An increased ratio is consistent with the presence of H pylori bacteria. Patient Preparation and Sample Collection
Chapter 3: Stomach Disorders
The patient should have fasted for a minimum of 1 hour and should have abstained from antimicrobials, proton pump inhibitors, and bismuth preparations in the 2 weeks prior. To collect the first sample, the patient inhales, holds his/her breath for 4 to 5 seconds, and then exhales into the bag provided in the sample collection kit. The patient then drinks, without stopping, all the 13 C-urea solution provided in the kit (powder must be reconstituted in water). After 15 minutes, during which there is no eating, drinking, or smoking, the patient exhales into a second bag using the procedure detailed above. Both bags should be capped tightly after collection and stored or transported at room temperature. The sample should be tested within 7 days of collection. Stool Antigen Test6,7 Stool antigen tests such as HpSA' (Meridian Bioscience) use antibodies to H pylori to determine if H pylori is present in the stool. Specimens can be tested immediately, stored for 3 days in the refrigerator, or frozen. Test results are available
49
Gastroenterology Reference Guide
within 5 minutes (point-of-care test) or 90 minutes (laboratory test) of test initiation. Table 1 summarizes the laboratory tests for H pylori. Refer to Part 3, Test Application and Interpretation Table 1. Tests Available for Detecting H pylori Infection
Test Description Invasive Tests Histologic exam
Chapter 3: Stomach Disorders
Accuracy*
Comments Also provides other histologic information, eg, presence/absence of cancer, etc. False-negatives caused by antibiotics, PPI, or bismuth compounds; suitable for test of cure Useful to determine alternative treatment for nonresponders; expensive; slow turnaround time
Uses modified Giemsa Sensitivity: or silver stain to visualize 80% to 90%2 H pylori bacteria Specificity: >95%2 Sensitivity: 80% to 95%2 Specificity: 95% to 100%2 Sensitivity: 70% to 80%8 Specificity: 100%8
Rapid urease Colorimetric test that (CLO test) detects urease in biopsy specimen Bacterial growth followed by identification and antibiotic susceptibility (if desired) Non-invasive Tests Antibody detection See text Culture
Sensitivity: 85%4 Specificity: 79%4
Simple, low cost; no longer recommended due to lower accuracy; not suited for proof of cure or to differentiate between active and past infection Useful for diagnosis and proof of cure; false-negatives caused by antibiotics, PPI, or bismuth compounds Useful for diagnosis and proof of cure; false-negatives caused by antibiotics, PPI, or bismuth compounds
Antigen detection
See text
Sensitivity: 93%4 Specificity: 93%4
Urea breath test
See text
Sensitivity: 95%4 Specificity: 96%4
CLO, Campylobacter-like organism; PPI, proton pump inhibitor. *Data represents approximate sensitivity and specificity; not based on side-by-side studies. Results subject to sampling error.
50
Gastroenterology Reference Guide
for additional information on the UBiT and stool antigen tests. TREATMENT Treatment goals include relief of symptoms, healing of the ulcer, and prevention of recurrence and complications. Documented eradication of H pylori infection is associated with substantially decreased rates of recurrence and complications; thus, physicians aim for an initial eradication rate of 85% to 90%.2 Triple therapy for 7 to 14 days duration is the typical treatment regimen and may include 2 antibiotics and 1 acid suppressor. The 14-day regimen is thought to be more efficacious than shorter regimens.1,2 Quadruple therapy may be used in patients who do not respond to triple therapy. Such patients may have an antibiotic resistant strain. If the patient still fails to respond, culture and sensitivity should be considered. Table 2 lists medications used for H pylori treatment. LABORATORY TESTING POST THERAPY H pylori testing is performed 4 or more weeks after the end of treatment. Such testing is appropriate for: Patients with a history of ulcer complications Patients with MALT lymphoma Patients with early gastric cancer Patients with recurrent symptoms post-treatment The urea breath test and the stool antigen test are the recommended noninvasive tests for confirming eradication of H pylori. Serologic tests are not suitable because they cannot distinguish between active and
Chapter 3: Stomach Disorders
51
Gastroenterology Reference Guide
Table 2. Medication Options Used for H Pylori Therapy
Drug Class Antibiotics Action Eradicate H pylori infection Examples Amoxicillin Clarithromycin Metronidazole Tetracycline Antacids (eg, Mylanta', Maalox', Tums', Gaviscon') H2 receptor antagonist (eg, cimetidine, ranitidine, famotidine, nizatidine) PPI (eg, omeprazole, lansoprazole, rabeprazole, pantoprazol, esomeprazole)* Bismuth-containing compound (eg, Pepto-Bismol') Prostaglandin analogue (eg, misoprostol) Sucralfate
Acid suppressors Relieve symptoms; heal the ulcer
Chapter 3: Stomach Disorders
Mucosal protective agents
Prevent further damage; heal the ulcer
PPI, proton pump inhibitor. *Acid suppressor drug class of choice.
resolved infection. When endoscopy is indicated, the rapid urease test results can be used as proof of cure. PROGNOSIS Triple therapy is effective in more than 80% of patients. Once H pylori infection is eradicated, most patients become symptom-free, and only about 4% to 6% of patients will have recurrent PUD.2 Therapy can still be successful when treatment is delayed until after development of complications (eg, in those who were previously asymptomatic) as evidenced by complete remission in >50% of patients with MALT lymphoma.2
52
Gastroenterology Reference Guide
REFERENCES
1. Talley NJ, Vakil NB, Moayyedi P. American Gastroenterological Association technical review on the evaluation of dyspepsia. Gastroenterology. 2005;129:1756-1780. 2. Del Valle J. Peptic ulcer disease and related disorders. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGrawHill; 2005:1746-1762. 3. Talley NJ for the American Gastroenterological Association. American Gastroenterological Association medical position statement: evaluation of dyspepsia. Gastroenterology. 2005:129:1753-1755. 4. Vakil N, Fendrick AM. How to test for Helicobacter pylori in 2005 [review]. Cleve Clin J Med. 2005;72(suppl 2):S8-S13. Also available at: http://www.ccjm.org/PDFFILES/Vakilsuppl5_05.pdf. Accessed January 5, 2007. 5. BreathTek UBiT [package insert]. Lafayette, Colorado: Meretek Diagnostics Inc; 2005. Available at: http://meretek.com/downloads/ 2215NOV05_cropped.pdf. Accessed January 8, 2007. 6. H pylori Stool Antigen Test Medical Information. Meridian Bioscience Europe Web site. Available at: http://www.mdeur.com/hpsa-doctor.htm. Accessed January 8, 2007. 7. Premier Platinum HpSA Plus. Meridian Bioscience Europe Web site. Available at: http://www.mdeur.com/products/601348.htm. Accessed January 8, 2007. 8. Meurer LN, Bower DJ. Management of Helicobacter pylori infection. Am Fam Phys. 2002;65:1327-1336. Available at: http://www.aafp.org/afp/ 20020401/1327.html. Accessed January 8, 2007.
Chapter 3: Stomach Disorders
53
Gastroenterology Reference Guide
SECTION 2. GASTRIC CANCER OVERVIEW Gastric cancers include gastric adenocarcinoma (85% of all gastric cancers), primary gastric lymphoma (12% to 14%), and nonlymphoid gastric sarcoma (ie, gastrointestinal stromal tumors [GIST]; 1% to 3%).1 ETIOLOGY AND RISK FACTORS The following factors appear to be involved in development or risk of gastric cancer: H pylori infection Familial mutation in the E-cadherin gene Diet low in fresh fruits and vegetables Gastric polyps Ingestion of large amounts of nitrates, commonly found in dried, smoked, and salted food High salt intake Tobacco smoking Mntriers disease (extreme hypertrophy of gastric rugal folds) The following factors are associated with decreased risk of gastric cancer: Diet high in vitamin C Diet high in whole grain foods Diet high in carotenoids Diet high in allium compounds Diet high in green tea INCIDENCE The American Cancer Society estimated there would be about 22,000 new cases of gastric cancer and
Chapter 3: Stomach Disorders
54
Gastroenterology Reference Guide
11,000 deaths in patients with gastric cancer during 2006.2 It is the 13th most common cancer, ranking well below prostate, breast, lung, and colon cancer. Incidence in distal tumors is declining along with the declining incidence of H pylori infection, whereas the incidence of proximal tumors in the cardia is increasing in the United States (Table 1). SYMPTOMS In the early, curable stage of gastric cancer, the patient is usually asymptomatic. As the tumor progresses, the patient may have the following: Upper abdominal discomfort of varying intensity A feeling of fullness after eating a small amount of food Occult blood in the stool Iron deficiency anemia Anorexia Nausea, vomiting (especially in the middle of the night) Weight loss DIAGNOSIS AND LABORATORY TESTING Evaluation of a symptomatic patient may begin with a double-contrast barium swallow radiograph, followed by an esophagogastroduodenoscopy (EGD) if gastric cancer is not ruled out.3 Alternatively, evaluation can Table 1. Gastric Cancer Site of Origin1
Location Distal stomach Mid-stomach Proximal third of the stomach Entire stomach % of All Gastric Cancer 30 20 37 13
Chapter 3: Stomach Disorders
55
Gastroenterology Reference Guide
begin with the EGD. Multiple biopsies from suspicious sites should be taken; diagnosis is based on microscopic examination of tissue. Following diagnosis, the patient should be evaluated further to determine extent of the disease (eg, presence or absence of lymph node, liver, or lung metastasis). This workup may include the following: Computed tomography (CT) scan Positron emission tomography (PET) scan Endoscopic ultrasonography (EUS)
Chapter 3: Stomach Disorders
Other tests may also be used to evaluate the patient: Complete blood count (CBC) Chemistry tests Coagulation studies Immunohistochemistry (IHC) tests The c-kit protein (CD117) test, performed by IHC, is used to differentiate GISTs from glomus tumors of the stomach. GISTs are c-kit positive, while glomus tumors are negative. Additionally, glomus tumors tend to be positive for smooth muscle actin and vimentin.4 STAGING The American Joint Committee on Cancer (AJCC) has outlined terminology for staging gastric cancers (Tables 2 and 3).3 TREATMENT Selection of treatment regimens depends on the type of gastric cancer, extent of disease, and general health of the patient. The National
56
Gastroenterology Reference Guide
Table 2. TNM Staging of Gastric Cancers3
Tumor staging T0 Tis T1 T2 T2a T2b T3 T4 Nodal staging N0 N1 N2 N3 Metastasis M0 M1 No evidence of primary tumor Carcinoma in situ Tumor invades lamina propria or submucosa Tumor invades muscularis propria or subserosa Tumor invades muscularis propria Tumor invades subserosa Tumor penetrates serosa (visceral peritoneum) Tumor invades adjacent structures No evidence of metastasis to regional lymph nodes Metastasis in 1 to 6 regional lymph node(s) Metastasis in 7 to 15 regional lymph nodes Metastasis in >15 regional lymph nodes No evidence of distant metastasis Evidence of distant metastasis
Chapter 3: Stomach Disorders
Table 3. Definition of Gastric Cancer Stages3
Stage 0 Ia Ib II Definition Tis, N0, M0 T1, N0, M0 T1, T2, M0, T2a or T2b, N0, M0 T1, N2, M0 T2a or T2b, N1, M0 T3, N0, M0 T2a or T2b, N2, M0 T3, N1, M0 T4, N0, M0 T3, N2, M0 T4, N1, 2, or 3, M0 T1, 2, or 3, N3, M0 Any T, any N, M1
IIIa
IIIb IV
57
Gastroenterology Reference Guide
Comprehensive Cancer Network (NCCN) recommendations for gastric adenocarcinoma are outlined in Table 4. Components of supportive care are outlined in Table 5. PROGNOSIS Prognosis varies based on the extent of disease (stage) at time of diagnosis and treatment and the type of gastric cancer. Patients with early stage cancer are potentially curable (5-year survival up to 80%);6 however, only about one-third of patients are diagnosed when the cancer is in an early stage. Prognosis for late stage is poor (<15% 5-year survival rate).6 Prognosis is much better for patients with primary gastric lymphoma (eg, MALT lymphoma) than with adenocarcinoma because antibiotic therapy, aimed at eradication of H pylori infection, has a 75% response rate.1 Surgery, radiation, and chemotherapy may not even be necessary for these patients. Patients with localized, high-grade lymphomas who are treated with surgery have a 40% to 60% 5-year survival rate.1
Chapter 3: Stomach Disorders
Table 4. NCCN Recommendations for Treatment of Gastric Cancer5
Patient Characteristics Medically fit with stage I to III gastric cancer Medically fit with unresectable tumor* Distant metastasis (M1) Post surgery, select individuals Therapy Surgery: partial (for distal tumors) or complete (for proximal tumors) gastrectomy Radiation or chemotherapy Salvage therapy Adjuvant radiation or chemotherapy
Medically unfit with locoregional cancer Radiotherapy or salvage chemotherapy
*Evidence of peritoneal or major blood vessel involvement or distant metastasis. Stage I to III or M0. Consisting of supportive care, chemotherapy, or clinical trial participation.
58
Gastroenterology Reference Guide
Table 5. Components of Supportive Care5
Stent placement, laser surgery, photodynamic therapy, radiotherapy, surgery, or combination of these* Surgery, endoscopic therapy, radiotherapy Nutritional support PEG tube Counseling Pain management Radiotherapy Medications
PEG, percutaneous endoscopic gastrostomy. *For patients with luminal obstruction. For patients with significant bleeding.
Chapter 3: Stomach Disorders
Patients with nonlymphoid gastric sarcoma (eg, GIST) may also have a better prognosis than those with adenocarcinoma. About 50% of patients with c-kit positive GIST tumors respond to imatinib mesylate (Gleevec') therapy. RESOURCES National and regional educational and supportive resources are available. For more information, contact: American Cancer Society Phone: 800-ACS-2345 (227-2345) Internet: http://www.cancer.org Cancer Care, Inc. Phone: 800-813-HOPE (813-4673) or 212-221-3300 Email: info@cancercare.org Internet: http://www.cancercare.org
59
Gastroenterology Reference Guide
Cancer Hope Network Phone: 877-HOPENET (467-3638) or 908-879-4039 (New Jersey residents) Email: info@cancerhopenetwork.org Internet: www.cancerhopenetwork.org National Cancer Institute Phone: 800-422-6237 or 301-496-6631 Internet: http://www.cancer.gov http://www.nci.nih.gov Cancer Information Service Building 31, Room 10A16 31 Center Drive, MSC 2580 Bethesda, MD 208922580 NCI's Facing Forward Series Phone: 888-4-CANCER (422-6237) Internet: http://www.nci.nih.gov/cancerinfo/ life-after-treatment National Coalition for Cancer Survivorship Phone: 877-622-7937 or 301-650-9127 Email: info@canceradvocacy.org Internet: http://www.canceradvocacy.org The Cancer Information Network http://www.cancerlinksusa.com/stomach/index.asp The Wellness Community Executive Office Phone: 888-793-WELL (793-9355) or 202-659-9709 Email: help@thewellnesscommunity.org Internet: http://www.thewellnesscommunity.org
Chapter 3: Stomach Disorders
60
Gastroenterology Reference Guide
REFERENCES CITED
1. Mayer RJ. Gastrointestinal tract cancer. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:523-533. 2. American Cancer Society. Cancer facts and figures 2006 graphs and figures. Available at: http://www.cancer.org/docroot/MED/content/ MED 1 1 Most-Requested Graphs and Figures 2006.asp. Accessed January 12, 2007. 3. Layke JC, Lopez PP. Gastric cancer: diagnosis and treatment options. Am Fam Physician. 2004;69:1133-1140. 4. Hwang JH, Rulyak SD, Kimmey MB. American Gastroenterological Association Institute Technical Review on the management of gastric subepithelial masses. Gastroenterology. 2006;130:2217-2228. 5. Ajani J, Bekaii-Saab T, DAmico TA, et al. National Comprehensive Cancer Network clinical practice guidelines in oncology v.1.2006: gastric cancer. Available at: http://www.nccn.org/professionals/physician gls/PDF/ gastric.pdf. Accessed January 12, 2007. 6. Stomach cancer. In: Beers MH, Porter RS, Jones TV, Kaplin JL, Berkwits M, eds. The Merck Manual of Diagnosis and Therapy. 18th ed. Merck Publishing Group; 2006. Available at: http://www.merck.com/mmpe/ sec02/ch021/ch021d.html?qt=gastric%20cancer&alt=sh. Accessed January 12, 2007.
Chapter 3: Stomach Disorders
ADDITIONAL REFERENCE
1. Gastric Cancer (PDQ'). National Cancer Institute Web site. Available at: http://www.cancer.gov/cancertopics/pdq/prevention/gastric/ healthprofessional. Accessed January 12, 2007.
61
Gastroenterology Reference Guide
Chapter 3: Stomach Disorders
62
CHAPTER 4. GASTROENTERITIS
Gastroenterology Reference Guide
INTRODUCTION Gastroenteritis is an acute inflammation of the stomach and/or intestinal lining. It can be caused by bacteria, viruses, parasites, and irritating substances in food or drinks (eg, capsaicin, found in hot peppers, or ciguatera found in barracuda, snapper, jack, and grouper fish). Common symptoms include loss of appetite, nausea, diarrhea, abdominal pain, and weakness. Since these symptoms are nonspecific, gastroenteritis differential diagnosis includes consideration of drug toxicity and inflammatory bowel disease as well as the causes just listed. Gastroenteritis is a very common disease worldwide, second only to acute respiratory illness.1 Morbidity ranges from mild to severe: mild cases may require no medication, whereas severe cases may be lifethreatening (eg, due to dehydration). Some infections causing gastroenteritis may become chronic (>2 weeks duration) and may lead to malnutrition. Many of these infections are transmitted via a fecal/oral route (ie, contaminated water and food, food poisoning). This chapter will focus on bacterial, viral, and parasitic gastroenteritis. REFERENCE
1. Butterton JR, Calderwood SB. Acute infectious diarrheal diseases and bacterial food poisoning. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:754-759.
Chapter 4: Gastroenteritis
63
Gastroenterology Reference Guide
SECTION 1. BACTERIAL GASTROENTERITIS OVERVIEW Bacterial gastroenteritis is caused by food poisoning (ie, ingestion of contaminated food or water). When such poisoning occurs in people who have recently or are traveling in another country, it is termed Table 1. Bacterial Causes of Gastroenteritis1
Incubation Disease Toxin Transmission Period Duration Producing Aeromonas Swimming, drinking water Bacillus 1-6 h <12 h Yes, Fried rice, pork cereus emetic Bacillus 8-16 h Yes, Beef, pork, cereus entero chicken, vanilla sauce Campylobacter 16-72 h 1 wk Uncooked jejuni poultry, unpasteurized milk, infected pet (eg, reptiles, dogs, cats) Clostridium Few d Yes, Fecal-oral, difficile to 2 mo entero or person-to-person, cytopathic during or following antibiotic therapy Clostridium 8-16 h 24 h Yes, alpha, Meat, poultry, perfringens beta, or gravy, hash, entero stew Escherichia coli 72-120 h 1 wk Yes Undercooked (E coli O157:H7) (Shiga ground beef, (enterohemorrhagic) toxin) unpasteurized milk and juice, water, person-to-person Escherichia coli 16-72 h ? Developing (enteroinvasive) countries Escherichia coli
(enteropathogenic)
Bacteria
Symptoms Sporadic, nonbloody diarrhea Nausea, vomiting, abdominal cramping Abdominal cramping, watery diarrhea Fever, headache, myalgia, abdominal cramps, watery or bloody diarrhea that may include WBCs
Chapter 4: Gastroenteritis
Ranges from none to lifethreatening colitis
Abdominal cramps, watery diarrhea Bloody diarrhea, abdominal cramps, hemolytic uremic syndrome (5%-10% of patients) Watery diarrhea; blood, mucus, and/or WBCs in stool; fever; cramps Watery diarrhea, fever, vomiting, mucus in stool
No
Nursery outbreak
64
Gastroenterology Reference Guide
travelers diarrhea. There are many different species of bacteria that can be involved in bacterial gastroenteritis (Table 1). RISK FACTORS Travel to endemic regions, especially those with poor sanitation or hygiene
Table 1. (Continued)
Bacteria Escherichia coli
(enterotoxigenic)
Listeria
Salmonella
Shigella
Staphylococcus aureus
Vibrio cholerae
Vibrio parahaemolyticus Yersinia enterocolitica
Incubation Disease Toxin Transmission Symptoms Period Duration Producing 16-48 h Yes, Contaminated meat, Watery diarrhea, entero vegetables, fruit; cramps, nausea person-to-person Uncooked chicken, Fever, diarrhea* beef, vegetables, milk, cheese 16-72 h Few d Yes, Uncooked fruits, Nausea, vomiting, to 1 wk endotoxin vegetables, oysters, diarrhea, fever, malaise, shellfish, eggs, muscle aches, poultry, pork, abdominal pain dairy products, water, pets (turtles) 16-72 h 1 wk Yes Primarily Fever, abdominal (Shiga person-to-person; cramping, watery toxin) food (egg salad, diarrhea followed by vegetables) bloody diarrhea less commonly 2 to 6 h Yes, Custard-filled Nausea, vomiting, enterotoxin baked goods, abdominal cramps, canned food, watery diarrhea processed meat, potato salad, ice cream 16-48 h Yes, Uncooked or Vomiting, watery entero undercooked food diarrhea with mucus (eg, shellfish), water 16-72 h Undercooked Diarrhea seafood 16-72 h Pork chitterlings, Fever, abdominal pain, tofu, milk, water diarrhea
Chapter 4: Gastroenteritis
h, hours; wk, weeks; d, days; mo, months; WBC, white blood cell. *More commonly a cause of meningitis.
65
Gastroenterology Reference Guide
Hemolytic Uremic Syndrome (HUS) Overview HUS primarily affects young children between the ages of 1 and 10 years. It is a vascular disorder that may lead to acute renal failure. It can occur following a minor febrile or viral illness (eg, enterohemorrhagic E coli). Although there is no effective treatment, only 10% to 50% of patients develop chronic renal disease and <10% of children die.2 Symptoms Fever Thrombocytopenia Microangiopathic hemolytic anemia Hypertension Varying degrees of acute renal failure
People with lowered immunity Children in day care centers Those who are in the hospital or a long-term care facility (eg, the elderly) INCIDENCE Although relatively common, bacterial gastroenteritis occurs less often than viral gastroenteritis. It occurs more often in developing countries or regions with poor sanitation and is more common in the summer or rainy months. The overall incidence is difficult to determine because many self-limiting cases are not reported. SYMPTOMS See Table 1 for typical symptoms associated with each bacterium. These symptoms range from mild to severe. Severe symptoms such as profuse watery diarrhea (and the resultant dehydration) can be life threatening. Complications can occur. For example, enterohemorrhagic E coli can lead to hemolytic uremic syndrome in 5% to 10% of patients.1 Arthritis may develop following Campylobacter, Salmonella, Shigella, or Yersinia infection. DIAGNOSIS Diagnostic evaluation begins with a medical history and physical examination. The patient should be evaluated for: Symptom onset, intensity, frequency, duration Stool characteristics o Presence or absence of blood
Chapter 4: Gastroenteritis
66
Gastroenterology Reference Guide
o Presence or absence of leukocytes o Consistency (bulky vs watery) Frequency of bowel movements Quantity of stool Recent antibiotic use (may raise suspicion of C difficile infection) Additionally, the following epidemiologic risk factors can be considered: Potential ingestion of contaminated food or water (especially during a known outbreak) Travel history Contact with similarly ill people Contact with animals and reptiles Daycare center attendance or employment Occupation as a food handler or caregiver Underlying medical conditions likely to predispose patient to infectious diarrhea (eg, AIDS)
Chapter 4: Gastroenteritis
The differential diagnosis should also include consideration of viral or parasitic gastroenteritis, drug toxicity, irritable bowel syndrome, inflammatory bowel disease, appendicitis, cholecystitis, and ulcerative colitis. Celiac disease, lactose intolerance, and other forms of malabsorption should be considered in patients with chronic diarrhea. Table 2 illustrates how specific symptoms can be used to suggest a possible diagnosis. A specific diagnosis (ie, identification of the causative bacterium) is not always necessary to determine the course of treatment. LABORATORY TESTING Laboratory tests may be helpful in selected cases. These tests include:
67
Gastroenterology Reference Guide
Tests for serum electrolyte, blood urea nitrogen (BUN), and creatinine levels to assess the severity of disease (ie, dehydration and acid-base balance) Gram stain Fecal lactoferrin test to detect the presence of fecal leukocytes which indicate an inflammatory process; elevated lactoferrin levels may be associated with inflammatory bowel disease, C difficile, C jejuni, enterohemorrhagic or enteroinvasive E coli, Salmonella, Shigella, V parahaemolyticus, or Y enterocolitica, and Entamoeba histolytica Bacterial culture of stool specimens Shiga toxin EIA to help diagnose Shigella or enterohemorrhagic E coli (O157:H7) infection Y enterocolitica antibody Analysis of suspected food to detect bacterial presence and/or toxin Table 2. Symptom Driven Differential Diagnosis3
Chapter 4: Gastroenteritis
Symptom Diarrhea of >2 weeks duration Fever Fecal leukocytes, blood, mucus
Possible Cause Causes of acute diarrhea unlikely Invasive disease, malaria Inflammatory disorder (invasion or cytoxin) rather than noninflammatory disorder (enterotoxin) Enterohemorrhagic E coli Small intestine disorder causing malabsorption Cholera or other toxigenic process Campylobacter, Shigella, cholera, necrotizing toxins Yersinia enterocolitica Shigella Toxin-producing bacteria, malaria, intestinal obstruction C difficile, Salmonella
Bloody stools without leukocytes Bulky white stools Profuse watery diarrhea with small pieces of mucus Severe abdominal pain Appendicitis-like syndrome Tenesmus* Vomiting Diarrhea coincident with or following antibiotic therapy
*Little stool produced in spite of strong urge to defecate and painful rectal spasms.
68
Gastroenterology Reference Guide
TREATMENT Most bacterial gastroenteritis cases are mild and selflimiting; thus, the focus is on bed rest and hydration rather than on antibiotic therapy. Oral rehydration solutions (ORS) containing electrolytes and glucose, rice, or cereal may be prescribed. ORS are often sold over-the-counter and include, among others, Lytren', Rehydralyte', and Pedialyte'. Sports drinks, soda, and juice are not recommended because they may result in additional fluid loss owing to lack of optimal balance between carbohydrate and sodium concentrations. If dehydration is severe, intravenous fluids such as Ringers lactate may be prescribed. Bismuth subsalicylate, antiperistaltic agents, and antimicrobial agents may shorten the duration of symptoms in patients with enterotoxigenic E coli infection. However, antibiotics that increase the production of Shiga toxins are contraindicated for treatment of enterohemorrhagic E coli infection. Antibiotics are sometimes recommended for patients with Shigella, V cholerae, or C difficile infection. RESOURCES National and regional educational and supportive resources are available. For more information, contact: American Dietetic Association Phone: 800-366-1655 or 800-877-1600 Internet: http://www.eatright.org U.S. Department of Agriculture Meat and Poultry Hotline Phone: 888-MPHotline (674-6854) Internet: http://www.usda.gov
Chapter 4: Gastroenteritis
69
Gastroenterology Reference Guide
US Department of Health and Human Services Phone: 877-696-6775 or 202-619-0257 Internet: http://www.os.dhhs.gov US Environmental Protection Agency (EPA) Phone: 202-272-0167 Internet: http://www.epa.gov US Food and Drug Administration FDA (HFE-88) Phone: 888-INFO-FDA (463-6332) Internet: http://www.fda.gov Center for Food Safety & Applied Nutrition Phone: 888-SAFEFOOD (723-3366) Internet: http://vm.cfsan.fda.gov/list.html Centers for Disease Control and Prevention (CDC) Phone: 800-311-3435 or 404-639-3534 Internet: http://www.cdc.gov
Chapter 4: Gastroenteritis
Gateway to Government Food Safety Information Internet: www.FoodSafety.gov REFERENCES
1. Isada CM, Kasten BL, Goldman MP, Gray LD, Aberg JA. Infectious Diseases Handbook. 4th ed. Hudson (Cleveland), OH: Lexi-Comp, Inc; 2001. 2. Handin RI. Disorders of the platelet and vessel wall. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGrawHill; 2005:673-680. 3. Butterton JR, Calderwood SB. Acute infectious diarrheal diseases and bacterial food poisoning. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:754-759.
70
Gastroenterology Reference Guide
SECTION 2. VIRAL GASTROENTERITIS OVERVIEW Viral gastroenteritis, commonly misnamed as stomach flu, is caused by rotavirus (group A); caliciviruses, which include norovirus (formerly Norwalk virus) and sapovirus; astrovirus; and adenovirus (types 40 and 41). Table 1 details some characteristics of these viruses. Mortality is a rare sequelae among healthy young adults, but elderly persons, particularly those in fragile health, are at risk of severe dehydration and death. INCIDENCE Viral gastroenteritis is a common disease that occurs more often in winter than other times of the year in the United States. Unlike bacterial gastroenteritis, the incidence of viral gastroenteritis is similar in industrial and developing countries. Viral gastroenteritis is much more common than bacterial. Most adults have antibodies to the Norwalk and related human caliciviruses, and
Chapter 4: Gastroenteritis
Table 1. Characteristics of Gastroenteritis-causing Viruses1-5
Virus Rotavirus, group A Norovirus Sapovirus Astrovirus Adenovirus, types 40 and 41 3-4 d 3-10 d 2-4 d Incubation Period Infants: <2 d Adults: 2-4 d 24-48 h Disease Primary Population Duration Affected 3-9 d Children aged 6 mo to 2 y 24-60 h All ages Infants, young children Children <5 y Infants, children <4 y Relative Severity +++ ++ + + +/++
d, days; mo, months; y, year; h, hours.
71
Gastroenterology Reference Guide
nearly all children are infected with rotavirus by age 5 years. TRANSMISSION Transmission of these viruses is predominantly via a fecal-oral route. Ingestion of contaminated food or water, person-to-person contact, vomit, aerosol, respiratory secretions, and contaminated surfaces or objects may be involved. SYMPTOMS Although patients are sometimes asymptomatic, nonbloody, noninflammatory, watery diarrhea is more likely to be manifested. The patient may also experience nausea, vomiting, abdominal pain, fever, chills, headache, and myalgia. Severe illness may be complicated by life-threatening dehydration.
Chapter 4: Gastroenteritis
Rotavirus typically causes the most severe illness, but it may be relatively mild in the neonatal period owing to maternal antibodies. Severity decreases with each reinfection. Severity of illness caused by norovirus is typically less than that caused by rotavirus but greater than that caused by sapovirus and astrovirus. Severity of adenovirus infection can be the same as sapovirus and astrovirus or similar to that caused by norovirus. DIAGNOSIS The diagnostic evaluation is essentially the same as that for bacterial gastroenteritis. If antibiotic therapy is being considered, laboratory testing should be used to differentiate viral from bacterial disease because differentiation based on clinical and epidemiologic characteristics is difficult. Parasitic
72
Gastroenterology Reference Guide
gastroenteritis, drug toxicity, and inflammatory bowel disease should also be considered. A specific diagnosis (ie, identification of the causative organism) is not always necessary to determine the course of treatment. LABORATORY TESTING The following tests are available to confirm a viral etiology: Rotavirus antigen detection using enzyme immunoassay (EIA) Norovirus RNA detection using reversetranscriptase polymerase chain reaction (RT-PCR) Adenovirus antigen detection using EIA Adenovirus culture Stool collection during the 1st week of symptoms provides the best recovery of rotavirus; however, viral shedding may continue longer in immunocompromised patients. Stool specimens for norovirus testing should be collected within 48 to 72 hours of onset of symptoms for best results; however, viral recovery can occur up to 2 weeks after resolution of symptoms. TREATMENT Specific antiviral therapy is not available and generally not required since viral gastroenteritis is self-limiting. Supportive therapy to prevent or treat dehydration may be needed, however. For details, see the section describing treatment of bacterial gastroenteritis. Antibiotic therapy is contraindicated.
Chapter 4: Gastroenteritis
73
Gastroenterology Reference Guide
PROGNOSIS Most people recover from viral gastroenteritis without any complications. However, viral gastroenteritis can be serious if severe dehydration develops. RESOURCES Centers for Disease Control and Prevention Phone: 800-311-3435 or 404-639-3534 Internet: http://www.cdc.gov REFERENCES
1. Isada CM, Kasten BL, Goldman MP, Gray LD, Aberg JA. Infectious Diseases Handbook. 4th ed. Hudson (Cleveland), OH: Lexi-Comp, Inc; 2001. 2. Centers for Disease Control. CDC technical fact sheet about noroviruses. Available at: http://www.cdc.gov/ncidod/dvrd/revb/gastro/norofactsheet.pdf. Accessed January 31, 2007. 3. Public Health Agency of Canada. Adenovirus types 40 and 41 material safety data sheet. Available at: http://www.phac-aspc.gc.ca/msds-ftss/ msds4e.html. Accessed January 31, 2007. 4. Parashar UD, Glass RI. Viral gastroenteritis. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1140-1143. 5. Matsui SM, Greenberg HB. Astroviruses. In: Knipe DM, Howley PM, eds. Fields Virology. 4th ed. Philadelphia, PA: Lippincott Williams and Wilkins; 2001:875-893.
Chapter 4: Gastroenteritis
74
Gastroenterology Reference Guide
SECTION 3. PARASITIC GASTROENTERITIS OVERVIEW Parasitic gastroenteritis is caused by infection with Giardia lamblia, Cryptosporidium parvum, Cyclospora cayetanensis, Isospora belli, Entamoeba histolytica (amebiasis), and microsporidia (eg, Enterocytozoon bieneusi, Encephalitozoon intestinalis). Characteristics of these protozoan parasites are listed in Table 1. Table 1. Parasitic Causes of Gastroenteritis1,2
Infective Incubation Disease Transmission Form Period Duration Cryptosporidium Oocyst 2-14 d 2 wk Fecal-oral, person-toparvum person; water; food; animal-human Cyclospora cayetanensis muscle Oocyst 1 wk 6 wk Fecal-oral [not person-to-person]; water, food Entamoeba histolytica Giardia lamblia Cyst 7-10 d 1-4 wk Contaminated food or water; fecal-oral Contaminated water or food; fecal-oral; oral-anal sexual contact Contaminated food or water Birds Parasite Symptoms Watery diarrhea, malaise, abdominal cramping or pain, fever Intermittent watery diarrhea, abdominal cramping, Chapter 4: Gastroenteritis aches, anorexia, fever, nausea, vomiting Asymptomatic (90%); abdominal pain; bloody diarrhea Asymptomatic (50%); watery diarrhea, abdominal pain, bloating; chronic malabsorption Watery diarrhea, abdominal cramps, anorexia, weight loss, occasional fever Gradual onset of diarrhea, weight loss, nausea, abdominal cramps, anorexia Gradual onset of diarrhea, weight loss, nausea, abdominal cramps, anorexia
Cyst
1-14 d
1-3 wk
Isospora belli
Oocyst
weeks
Enterocytozoon bieneusi*
Spore
Chronic
Encephalitozoon Spore intestinalis*
Chronic
Domestic and wild animals
*Opportunistic infections occurring predominantly in immunocompromised patients.
75
Gastroenterology Reference Guide
RISK FACTORS Travelers to endemic areas (Table 2) and campers are at risk of parasitic gastroenteritis. Other risk factors include recent immigration, institutionalization, and homosexuality. People with IgA deficiency or diverticulosis are at increased risk of severe or relapsing giardiasis. DIAGNOSIS Diagnosis is frequently based on an ova and parasites (O&P) test, which includes concentration of a fecal specimen (via centrifugation) followed by examination of the concentrate under a microscope. A trichrome, acid-fast, or other stain may be used to help visualize and identify the parasite. Other tests may be appropriate depending on the suspected organism (Table 3).
Chapter 4: Gastroenteritis
Identification of Cyclospora cayetanensis, though infrequent, is important since treatment is available. The oocytes are twice as large as Cryptosporidium oocytes and appear deep red or pink when using an Table 2. Geographic Distribution of Protozoan Parasites1
Parasite Cryptosporidium parvum Cyclospora cayetanensis Entamoeba histolytica Giardia lamblia Isospora belli Enterocytozoon bieneusi Encephalitozoon intestinalis Distribution Worldwide Worldwide, especially in Nepal, Peru, Mexico, Morocco, India, Pakistan Mexico, India, West and South Africa, portions of Central and South America Worldwide, especially in wilderness and mountainous areas Tropical and subtropical climates Worldwide Worldwide
76
Gastroenterology Reference Guide
Table 3. Diagnosis of Parasitic Gastroenteritis1
Parasite Cryptosporidium parvum Cyclospora cayetanensis Entamoeba histolytica Giardia lamblia Isospora belli Enterocytozoon bieneusi Laboratory Tests Acid-fast stain on 2 or more separate samples; DFA; EIA O&P, modified acid-fast stain, phase microscopy, UV microscopy O&P, antigen detection, sigmoidoscopy or colonoscopy O&P with or without staining, duodenal biopsy aspiration, string test O&P, acid-fast stain Microscopic examination of trichrome-stained stool smear; other stains may also be used; PCR (select research laboratories) Microscopic examination of trichrome-stained stool smear; other stains may also be used; PCR (select research laboratories)
Encephalitozoon intestinalis
DFA, direct immunofluorescence assay; EIA, enzyme immunoassay; O&P, ova and parasites test; UV, ultraviolet; PCR, polymerase chain reaction.
Chapter 4: Gastroenteritis
acid-fast stain. Nonrefractile hyaline cysts can be seen using phase microscopy, while neon blue fluorescence can be seen using ultraviolet microscopy. Stool specimens, duodenal aspirate, or small bowel biopsy specimens can be submitted for testing. Sensitivity of O&P for diagnosis of Entamoeba histolytica is 80% to 90% when 3 stool specimens are examined, each within 20 minutes of collection.1 Detection of E histolytica antigen, using enzyme immunoassay (EIA), is 60% to 90% 7 days after exposure.1 Sigmoidoscopy or colonoscopy can be used to differentiate parasitic gastroenteritis from inflammatory bowel disease in patients with chronic colitis.
77
Gastroenterology Reference Guide
TREATMENT Therapeutic regimens employed are listed in Table 4. Supportive care to prevent or treat dehydration may be needed. For details, see the section describing treatment of bacterial gastroenteritis. RESOURCES National and regional educational and supportive resources are available. For more information, contact: Centers for Disease Control and Prevention / Division of Parasitic Diseases (CDC /DPD) Phone: 800-311-3435 or 404-639-3534 Internet: http://www.cdc.gov/ncidod/dpd/
Chapter 4: Gastroenteritis
Table 4. Therapeutic Regimens for Parasitic Gastroenteritis1,2
Parasite Cryptosporidium parvum Cyclospora cayetanensis Entamoeba histolytica Treatment Supportive care; clarithromycin and nitazoxanide may be useful, but more studies needed Drug of choice is co-trimoxazole, a combination of trimethoprim and sulfamethoxazole (orally for 7 days) Metronidazole (3 times/day for 10 days) followed by diloxanide furoate; alternatively, treat with metronidazole followed by paromomycin or iodoquinol Many self-resolving, but treatment with metronidazole is recommended; other options include quinacrine, tinidazole, and nitazoxanide Co-trimoxazole (4 times/day); alternatively treat with sulfadoxine and pyrimethamine or with ciprofloxacin Supportive care, albendazole Supportive care, albendazole
Giardia lamblia
Isospora belli Enterocytozoon bieneusi Encephalitozoon intestinalis
78
Gastroenterology Reference Guide
REFERENCES
1. Isada CM, Kasten BL, Goldman MP, Gray LD, Aberg JA. Infectious Diseases Handbook. 4th ed. Hudson (Cleveland), OH: Lexi-Comp, Inc; 2001. 2. DPDx Laboratory identification of parasites of public health concern. [Centers for Disease Control and Prevention, National Center for Infectious Diseases, Division of Parasitic Diseases Web site]. Available at: http://www.dpd.cdc.gov/dpdx/Default.htm. Accessed February 12, 2007.
Chapter 4: Gastroenteritis
79
Gastroenterology Reference Guide
Chapter 4: Gastroenteritis
80
CHAPTER 5. INFLAMMATORY INTESTINAL DISORDERS SECTION 1. DIVERTICULAR DISEASE OVERVIEW Diverticular disease includes diverticulosis and diverticulitis. Diverticulosis is characterized by diverticula affecting any part of the gastrointestinal (GI) tract; the sigmoid colon is most commonly affected, accounting for 95% of cases.1 False, or pseudodiverticulum, is the most common type of diverticulum in the colon; this sac-like projection or hernia extends through the muscularis propria, but not all layers of the intestinal wall. True diverticula contain all layers of the intestinal wall. Diverticulitis is the most common complication of diverticulosis. It is characterized by inflammation of the diverticulum, which is caused by trapped fecal material. Infection, bleeding, and perforation may follow. ETIOLOGY Diverticula are most likely caused by an increase in pressure (higher amplitude contraction) within the GI tract in combination with weak sections of the wall. Since the sigmoid colon is the narrowest part of the colon and has the highest pressure between segments, it is the most likely location for diverticula formation. A low-fiber diet (low-bulk stool) is thought to contribute to the increased pressure and is considered the probable cause of diverticular disease. Diverticula of the right side of the colon are thought to be congenital.1
Gastroenterology Reference Guide
Chapter 5: Inflammatory Intestinal Disorders
81
Gastroenterology Reference Guide
PREVALENCE Diverticular disease affects about 50% of people over the age of 60 in western populations.2 It is much less common in underdeveloped countries in which highfiber diets are common. It is relatively rare in people younger than 40 years of age, but prevalence increases with increasing age thereafter. Although men usually present at a younger age than women do, both genders are equally affected. SYMPTOMS About 20% of people with diverticulosis develop symptoms.2 Primary symptoms include painless rectal hemorrhage or those associated with diverticulitis. Patients with diverticulitis may present with: Fever Abdominal pain Nausea Vomiting Abdominal distention Diarrhea or constipation Anorexia
Chapter 5: Inflammatory Intestinal Disorders
Diverticulitis complications include abscesses, peritonitis, pneumaturia, or recurrent urinary tract infections in patients with a fistula between the bladder and bowel. Fistulas may also occur in other adjacent structures such as the small bowel, vagina, and uterus. Fistulas are uncommon, however, occurring mostly in patients with recurrent attacks of diverticulitis.
82
Gastroenterology Reference Guide
DIAGNOSIS AND LABORATORY TESTING Asymptomatic diverticulosis is detected during procedures (eg, imaging studies, endoscopy, or colonoscopy) that are performed to evaluate another ailment or as part of colon cancer screening. In patients presenting with rectal bleeding, colonoscopy or mesenteric angiography is used to localize the site of bleeding. When diverticulitis is suspected, computed tomography (CT) scan of the abdomen and pelvis is used. The differential diagnosis includes irritable bowel sydrome, appendicitis, and colon or ovarian cancer. To assist in diagnosis, other procedures such as ultrasonography, barium enema, and laparoscopy may be employed. Laboratory tests may show leukocytosis, increased erythrocyte sedimentation rate (ESR), or increased C-reactive protein (CRP) levels. TREATMENT The asymptomatic patient, diagnosed incidentally, is treated with a high-fiber (15 to 30 gm/d) diet. Fiber supplements such as Metamucil', Citrucel', and Fibercon' may be used. Diverticular bleeding stops spontaneously in the majority of patients. However, heat or laser coagulation of vessels can be employed during colonoscopy for patients with mild to moderate bleeding. In patients with more extensive bleeding, coil embolization techniques can be used during angiography with an 80% success rate.2 Alternatively, vasopressin infusion can be used to stop bleeding. Both procedures are associated with side effects and/or recurrence.
Chapter 5: Inflammatory Intestinal Disorders
83
Gastroenterology Reference Guide
Diverticulitis should be treated initially with a 7- to 10-day course of antibiotics and bowel rest (nothing by mouth or a clear liquid diet) until abdominal pain ceases. This is successful in nearly 75% of cases.2 Antibiotic choices include trimethoprim/ sulfamethoxazole, ciprofloxacin, metronidazole, ampicillin, amoxicillin, ceftazidime, and piperacillin. Surgical resection (segmental or total abdominal colectomy) is sometimes required; for example, surgery is offered to patients who have had 2 episodes of diverticular disease and to those who do not respond rapidly to other therapy. Surgery is also required for patients with complicated disease (eg, abscesses, fistulas, obstructed bowel). Segmental resection is performed more often than total abdominal colectomy. PROGNOSIS Diverticular disease is successfully treated in most cases. A small percentage will have recurrent disease. RESOURCES
Chapter 5: Inflammatory Intestinal Disorders
National and regional educational and supportive resources are available. For more information, contact: Digestive Disease National Coalition 507 Capitol Court NE, Suite 200 Washington, DC 20002 Phone: 202-544-7497 National Digestive Diseases Information Clearinghouse (NDDIC) Phone: 800-891-5389 Internet: http://digestive.niddk.nih.gov/index.htm
84
Gastroenterology Reference Guide
REFERENCES CITED
1. Joffe S, Kachulis A, Horowitz M. Colon, diverticulitis. [EMedicine Web site]. Available at: http://www.emedicine.com/radio/topic183.htm. Accessed February 13, 2007. 2. Gearhart SL, Bulkley G. Common diseases of the colon and anorectum and mesenteric vascular insufficiency. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1795-1803.
ADDITIONAL REFERENCE
Gastrointestinal disorders: diverticular disease. In: Beers MH, Porter RS, Jones TV, Kaplan JL, Berkwits M, eds. The Merck Manual of Diagnosis and Therapy. 18th ed. Merck Publishing Group; 2006. Available at: http://www.merck.com/mmpe/sec02/ch019/ch019a.html. Accessed February 13, 2007.
Chapter 5: Inflammatory Intestinal Disorders
85
Gastroenterology Reference Guide
SECTION 2. INFLAMMATORY BOWEL DISEASE (ULCERATIVE COLITIS AND CROHN'S DISEASE) OVERVIEW Inflammatory bowel disease (IBD) is a chronic inflammation of the intestine characterized by diarrhea and abdominal pain. There are 2 main types: ulcerative colitis (UC) and Crohns disease. UC usually involves the rectum and may extend to part or all of the large intestine (colon) in a continuous and contiguous pattern. Damage to the lining of the intestine is usually limited to the mucosa. Crohns disease can involve any part of the gastrointestinal (GI) tract, from the mouth to the anus. Damage usually affects all layers of the intestine. Moreover, unlike UC, areas of healthy bowel alternating with regions of diseased bowel characterize Crohns disease. ETIOLOGY AND RISK FACTORS IBD is an idiopathic disorder in which inflammation is thought to develop subsequent to interaction between the patients genetics, physiology, and environment. In genetically susceptible individuals, endogenous intestinal microorganisms (normal flora) may somehow trigger an autoimmune (inappropriate) response. This response is exacerbated by environmental factors. Epidemiology studies show about 10% of IBD patients have an affected first-degree relative.1 Prevalence along ethnic lines also indicates a genetic link: prevalence is highest in those of Jewish ethnicity and decreases progressively in Caucasian, AfricanAmerican, Hispanic, and Asian ethnicities.1 IBD is
Chapter 5: Inflammatory Intestinal Disorders
86
Gastroenterology Reference Guide
also associated with some inherited disorders (eg, Turners syndrome, Hermansky-Pudlak syndrome).1 Gene mapping has identified a genetic link between 3 mutations in the NOD2 gene located on chromosome 16 and Crohns disease susceptibility.2 This gene is also called CARD15. Up to 50% of western Caucasian patients with Crohns disease have a NOD2/CARD15 mutation.2 These 3 mutations have not been found in Chinese or Japanese people with Crohns disease, though. The 3 NOD2/CARD15 mutations do not appear in patients with other inflammatory disorders, including UC. To date, a causative infectious agent has not been identified. Lifestyle risk factors include cigarette smoking and oral contraceptive use. Cigarette smokers are twice as likely to have Crohns disease than nonsmokers; conversely, smokers are less likely to have UC than nonsmokers.1,3 Women who use oral contraceptives are at increased risk (RR 1.9) of Crohns disease, but not UC.1 INCIDENCE
Chapter 5: Inflammatory Intestinal Disorders
UC incidence in the United States is about 11:100,000, and Crohns disease incidence is about 7:100,000.1 Additional cases of IBD also occur since UC and Crohns disease cannot be differentiated in about 10% of affected people. Such people are said to have indeterminate colitis. UC incidence is similar in men and women; however, Crohns disease occurs more frequently in men. Onset peaks in people aged 15 to 30 years and in people aged 60 to 80 years (ie, 2 peak periods).1 As discussed previously, incidence is highest in people of Jewish ethnicity.
87
Gastroenterology Reference Guide
SYMPTOMS Ulcerative Colitis Symptom severity correlates with the extent of disease. The patient presents with: Bloody diarrhea Rectal urgency Tenesmus Rectal bleeding Passage of mucus Crampy abdominal pain In severe disease, the patient may also have: Fever Malaise Anemia Anorexia Weight loss Joint pain Symptoms may be exacerbated by recent or past cigarette smoking cessation or nonsteroidal antiinflammatory drug use. Crohns Disease Characteristic symptoms of Crohns disease include: Chronic or nocturnal diarrhea Abdominal pain Weight loss Fever Rectal bleeding
Chapter 5: Inflammatory Intestinal Disorders
88
Gastroenterology Reference Guide
Other symptoms vary depending on the location of disease within the GI tract: Anorexia Nutritional deficiency Malaise Nausea Vomiting Incontinence Bowel obstruction Upper respiratory tract and enteric infections, cigarette smoking, and use of nonsteroid antiinflammatory drugs may exacerbate symptoms. Extraintestinal manifestations of IBD IBD may manifest a multitude of extraintestinal conditions, including: Skin disorders (eg, erythema nodosum, pyoderma gangrenosum) Peripheral arthritis Ankylosing spondylitis (in HLA-B27 positive patients) Sacroiliitis Ocular inflammation (eg, conjunctivitis, uveitis, episcleritis) Hepatic steatosis Cholelithiasis Kidney stones Ureteral obstruction Fistulas Thromboembolic disease
Chapter 5: Inflammatory Intestinal Disorders
89
Gastroenterology Reference Guide
DIAGNOSIS AND LABORATORY TESTING Owing to the non-specific symptoms, the differential diagnosis of IBD is lengthy. Disorders to be considered include: Gastroenteritis/infectious colitis Ischemic, radiation-induced, medication-induced, or other inflammatory bowel disease (eg, lymphocytic or collagenous colitis) Celiac disease Irritable bowel syndrome Neoplasia Refer to the appropriate sections of this manual to review tests that may be useful to rule out these disorders. Additionally, UC differentiation from Crohns disease may be helpful for: 1) determining prognosis and cancer risk, 2) medical and surgical therapy selection, and 3) patient counseling.4 Features useful for UC differentiation from Crohns disease are listed in Table 1. Diagnostic tools include endoscopy, sigmoidoscopy or colonoscopy, computerized tomography (CT), magnetic resonance imaging (MRI), and pathology. Laboratory testing is also employed. Complete blood count (CBC) to assess leukocytosis and anemia is helpful in diagnosis and determining the severity of disease, respectively. Erythrocyte sedimentation rate (ESR) helps determine the severity of disease, as do liver function tests. ESR is also useful to assess a patients response to therapy. Perinuclear antineutrophil cytoplasmic antibodies (pANCA) and anti-Saccharomyces cerevisiae antibody (ASCA) tests can help differentiate UC from Crohns disease in the majority of patients.4
Chapter 5: Inflammatory Intestinal Disorders
90
Gastroenterology Reference Guide
Table 1. Differentiating Features of Ulcerative Colitis and Crohns Disease1
Feature Fistula Cobblestoning mucosa Significant small bowel abnormality Segmental colitis Asymmetric colitis Granuloma on biopsy Perianal disease Abdominal mass Obstruction Rectal sparing ASCA-positive ANCA-positive Bloody stools Mucus Continuous disease Abnormal terminal ileum Systemic symptoms Pain Stricture Ulcerative Colitis /+ /+ /+ /+ ++ + + + +/ +/ +/ +/ Crohns Disease + + + + + +/ ++ + ++ ++ ++ /+ +/ +/ +/ + ++ ++ ++
Chapter 5: Inflammatory Intestinal Disorders
, not present; +, present; +/, occasionally present; ++, frequently present; /+, rarely present; ANCA, perinuclear antineutrophil cytoplasmic antibodies, pANCA; ASCA, anti-Saccharomyces cerevisiae antibody.
TREATMENT Inducing and maintaining remission of symptoms, promoting the highest possible quality of life, is the primary goal of therapy. IBD treatment is selected, in part, on the basis of anatomic extent and clinical severity of the acute attack (eg, disease location, severity, extraintestinal complications). The American College of Gastroenterology has recommended treatment for the various categories of UC severity (Table 2).4 Patients are treated medically
91
Gastroenterology Reference Guide
Table 2. Ulcerative Colitis Disease Management4
Disease Severity Mild Criteria for Classification <4 stools/d with or without blood, no systemic toxicity, normal ESR Therapeutic Options Distal colitis: topical mesalamine (preferred), oral aminosalicylates, or topical steroids; oral prednisone if refractory Extensive colitis: daily oral sulfasalazine or aminosalicylate; if refractory, oral steroids (prednisone); if still refractory, 6-mercaptopurine or azathioprine The combined use of oral and topical aminosalicylates is more effective than use of either alone. Moderate Severe >4 stools/d with minimal toxicity Same as for mild disease
>6 bloody stools/d with Hospitalization, daily intravenous steroid (eg, fever, tachycardia, anemia, hydrocortisone, methylprednisolone); if or increased ESR refractory, IV cyclosporine (alternatively, colectomy); consider CMV and C difficile infection Same as for severe disease with addition of broad-spectrum antibiotics and small bowel decompression tube (if small bowel ileus present), keep NPO, rotate frequently into prone or knee-elbow position; if deterioration occurs, perform immediate colectomy
Fulminant >10 stools/d, continuous bleeding, toxicity, abdominal tenderness and distension, anemia requiring blood transfusion, and colonic dilation
IV, intravenous.
Chapter 5: Inflammatory Intestinal Disorders
with anti-inflammatory drugs (aminosalicylates such as mesalamine, corticosteroids such as prednisolone), immunosuppressives (mercaptopurine, azathioprine, cyclosporine), and antibiotics (metronidazole, ciprofloxacin). Additionally, the FDA approved use of infliximab for inducing and maintaining remission in patients with refractory disease in 2005 and 2006, respectively. Surgery (partial or total colectomy) is recommended if there is exsanguinating hemorrhage, frank perforation, or documented or strongly suspected carcinoma.4 Patients with less severe, but medically intractable disease, may also be considered for surgery. Surgery is performed within
92
Gastroenterology Reference Guide
the first 10 years of illness for about half of the patients with extensive chronic UC.1 Since patients with UC are at increased risk of colon cancer, annual or biannual colonoscopy should be performed in patients who have been affected for >8 to 10 years. Evidence of dysplasia warrants consideration of colectomy to prevent cancer and metastasis. The American College of Gastroenterology has recommended treatment for the various categories of Crohns disease severity (Table 3).5 Patients are treated medically with anti-inflammatory drugs (aminosalicylates such as mesalamine and sulfasalazine, corticosteroids such as prednisolone and budesonide, and infliximab), immunosuppressives (cyclosporine, tacrolimus), and antibiotics (metronidazole, ciprofloxacin). Corticosteroids are contraindicated for long-term maintenance; however antibiotics can be used. Surgery is recommended to Table 3. Crohns Disease Management5
Disease Severity Mild-moderate Criteria for Classification Ambulatory, no dehydration, fever, rigor, prostration, abdominal tenderness, painful mass, obstruction or >10% weight loss Therapeutic Options Oral mesalamine, sulfasalazine, metronidazole, or ciprofloxacin
Chapter 5: Inflammatory Intestinal Disorders
Moderate-severe Refractory to treatment for mildmoderate disease or presence of fever, significant weight loss, abdominal pain, intermittent nausea or vomiting, or anemia Severe-fulminant Symptoms persist despite outpatient steroid therapy or presence of high fever, persistent vomiting, intestinal obstruction, rebound tenderness, cachexia, or abscess
Oral steroid therapy (eg, prednisone, budesonide), antibiotic therapy, percutaneous or surgical drainage of abscess, infliximab infusion Hospitalization with percutaneous or surgical drainage of abscesses, parenteral corticosteroids, nutritional support, and/or surgery as clinically indicated
93
Gastroenterology Reference Guide
treat complications or medically refractory disease.5 Most patients with Crohns disease require surgery at some point.1 PROGNOSIS While IBD is a serious chronic disease, most people with the illness may continue to lead full, active, and productive lives, even though they may be hospitalized from time to time or need to take medications. In between flare-ups of the disease, many individuals may be relatively free of symptoms. RESOURCES National and regional educational and supportive resources are available. For more information, contact: The Crohn's and Colitis Foundation of America (CCFA) Phone: 800-932-2423 Internet: http://www.ccfa.org
Chapter 5: Inflammatory Intestinal Disorders
94
Gastroenterology Reference Guide
REFERENCES
1. Friedman S, Blumberg RS. Inflammatory Bowel Disease. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGrawHill; 2005:1776-1789. 2. Russell RK, Wilson DC, Satsangi J. Unravelling the complex genetics of inflammatory bowel disease. Arch Dis Child. 2004;89:598-603. 3. Gastrointestinal disorders: inflammatory bowel disease (IBD). In: Beers MH, Porter RS, Jones TV, Kaplan JL, Berkwits M, eds. The Merck Manual of Diagnosis and Therapy. 18th ed. Merck Publishing Group; 2006. Available at: http://www.merck.com/mmpe/sec02/ch018/ ch018a.html?qt=inflammatory%20bowel%20disease&alt=sh. Accessed February 14, 2007. 4. Kornbluth A, Sachar DB. Ulcerative colitis practice guidelines in adults (update): American College of Gastroenterology, Practice Parameters Committee. Am J Gastroenterol. 2004;99:1371-1385. 5. Hanauer SB, Sandborn W and the Practice Parameters Committee of the American College of Gastroenterology. Management of Crohns disease in adults. Am J Gastroenterol. 2001;95:635-643.
Chapter 5: Inflammatory Intestinal Disorders
95
Gastroenterology Reference Guide
SECTION 3. MICROSCOPIC COLITIS: COLLAGENOUS AND LYMPHOCYTIC COLITIS OVERVIEW Microscopic colitis causes chronic watery diarrhea in spite of a normal appearing colorectum on endoscopy. Histologic examination of a biopsy, however, reveals microscopic inflammation. There are 2 types of microscopic colitis: collagenous colitis and lymphocytic colitis. ETIOLOGY Although no precise cause has been found for collagenous colitis or lymphocytic colitis, multiple etiologic theories exist, including that it is an autoimmune, infectious, or medication-induced disease. PREVALENCE Collagenous colitis occurs primarily in women (female to male ratio is 9:1), and the age of onset is 60 to 80 years.1 People with lymphocytic colitis present at the same age; however, the disorder affects women and men equally. Both collagenous and lymphocytic colitis are rare disorders. SYMPTOMS Symptoms of microscopic colitis include: Chronic, nonbloody, watery diarrhea Dehydration Fatigue
Chapter 5: Inflammatory Intestinal Disorders
96
Gastroenterology Reference Guide
Weight loss Abdominal cramping Patients may also exhibit signs of malnutrition. DIAGNOSIS AND LABORATORY TESTING Microscopic colitis is considered when other, more common causes of watery diarrhea have been excluded. Diagnosis is based on histologic appearance of biopsy specimens acquired during sigmoidoscopy or colonoscopy. Collagenous colitis shows increased subepithelial collagen deposition and intraepithelial lymphocytes. Lymphocytic colitis shows increased intraepithelial lymphocytes, but no subepithelial collagen deposition. TREATMENT Symptoms may disappear without treatment in about 20% of patients.2 Avoidance of nonsteroidal antiinflammatory drugs (NSAIDS) may be successful in eliminating symptoms in some patients. A low-fat diet devoid of caffeine and lactose-containing foods may be helpful. Medical treatment options including antidiarrheals, antibiotics, 5-aminosalicylates, steroids, and immunosuppressants are shown in Table 1. Table 1. Medical Treatment Options for Microscopic Colitis2
Therapy First line Second line Third line Fourth line Options Loperamide (Imodium') or diphenoxylate/atropine (Lomotil') Bismuth subsalicylate, mesalamine, or cholestyramine Budesonide, prednisone Azathioprine, 6-mercaptopurine
Chapter 5: Inflammatory Intestinal Disorders
97
Gastroenterology Reference Guide
Surgery may be considered in the few cases refractory to medical therapy or in patients who cannot tolerate medical therapy. PROGNOSIS Some patients become asymptomatic with no treatment, while others become asymptomatic after 6 months of treatment. More than 80% of patients will become asymptomatic within 3 years.2 RESOURCES National and regional educational and supportive resources are available. For more information, contact: Digestive Disease National Coalition 507 Capitol Court NE, Suite 200 Washington, DC 20002 Phone: 202-544-7497 National Digestive Diseases Information Clearinghouse (NDDIC) Phone: 800-891-5389 Internet: http://digestive.niddk.nih.gov/index.htm REFERENCES
1. Friedman S, Blumberg RS. Inflammatory Bowel Disease. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGrawHill; 2005:1776-1789. 2. Goosenberg E, Chaudhary A. Collagenous and lymphocytic colitis. [EMedicine Web site]. Available at: http://www.emedicine.com/med/ topic1351.htm. Accessed February 14, 2007.
Chapter 5: Inflammatory Intestinal Disorders
98
CHAPTER 6. COLORECTAL CANCER
Gastroenterology Reference Guide
OVERVIEW Colorectal cancer is a common cancer affecting the colon (large intestine) and/or rectum. It usually develops from adenomatous polyps; almost all cases are adenocarcinomas. Colorectal cancer may be preventable in patients who undergo routine screening and is often curable when detected early. If not detected and treated early, colorectal cancer may metastasize to the regional lymph nodes, liver, lung, or abdominal peritoneum. ETIOLOGY AND RISK FACTORS About three-quarters of colorectal cancer cases result from environmental factors, diet, and aging. The remaining 25% of cases are associated with a family history of colorectal cancer.1 Risk factors include2: Age (>50 years) Previous colorectal cancer Previous colorectal polyps Inflammatory bowel disease (especially ulcerative colitis) Family history of colorectal cancer Diet high in animal fat (meat and dairy products) Obesity Physical inactivity Cigarette smoking Heavy alcohol intake Genetics and Colorectal Cancer Hereditary colorectal cancer is 1 of 2 types: the rare familial adenomatous polyposis (FAP) and the less rare hereditary nonpolyposis colorectal cancer
Chapter 6: Colorectal Cancer
99
Gastroenterology Reference Guide
(HNPCC). FAP is characterized by the presence of thousands of adenomatous polyps in the large bowel. Polyps typically develop after puberty but before age 25 years. If untreated, almost all patients develop colorectal cancer by the age of 40 years. FAP is caused by mutations in the adenomatous polyposis coli (APC) gene. These mutations are transmitted in an autosomal dominant fashion; thus, children of an affected parent have a 50% chance of inheriting FAP. Children should be routinely screened with proctosigmoidoscopy and, once the polyps appear, should undergo colectomy to prevent development of the cancer. HNPCC, also known as Lynch syndrome, is transmitted in an autosomal dominant fashion, as is FAP. Unlike FAP, huge numbers of polyps do not develop. Cancer usually arises in the proximal large bowel before the patient is 50 years old. Affected women may also develop primary ovarian or endometrial cancer. Microsatellite instability (MSI) testing can identify individuals who may have inherited HNPCC. If MSI testing is positive, identification of a causative mutation confirms the diagnosis of HNPCC. Such mutations are found in the MLH1, MSH2, MSH6, or PMS2 genes. Individuals meeting the Amsterdam criteria (Table 1) or the Bethesda criteria (Table 2) are suitable for testing. More often, multiple members of a family will have colorectal cancer, but no identifiable hereditary cause can be found. These patients are said to have familial colorectal cancer. PREVALENCE Colorectal cancer is the second leading cause of cancer death in the United States, with projections of
Chapter 6: Colorectal Cancer
100
Gastroenterology Reference Guide
55,000 deaths and 149,000 new cases (colon: 107,000; rectum: 42,000) diagnosed in 2006.2
Table 1. Amsterdam Criteria3
3 relatives with an HNPCC-associated tumor* 1 is a first-degree relative of the other 2 2 successive generations affected 1 diagnosed at <50 years of age FAP should be excluded in the patients with colorectal cancer Tumor should be verified by pathologic examination
FAP, familial adenomatous polyposis. *Endometrial, stomach, ovarian, pancreas, ureter and renal pelvis, biliary tract, and brain tumors; sebaceous gland adenomas and keratoacanthomas in Muir-Torre syndrome; and carcinoma of the small bowel.
Table 2. Bethesda Criteria4
Colorectal tumors should be tested for MSI in individuals meeting any of the following: Colorectal cancer diagnosed at age <50 years Presence of synchronous colorectal cancers (multiple cancers 6 months after initial tumor removal), metachronous colorectal cancer (cancer recurrence >6 months after initial tumor removal), or other HNPCCassociated tumors* Colorectal cancer with the MSI-H histology diagnosed at age <60 years Colorectal cancer in 1 first-degree relative with an HNPCC-related tumor with 1 of the cancers diagnosed at age <50 years Colorectal cancer diagnosed in 2 first- or second-degree relatives with HNPCC-related tumors
*Endometrial, stomach, ovarian, pancreas, ureter and renal pelvis, biliary tract, and brain tumors; sebaceous gland adenomas and keratoacanthomas in Muir-Torre syndrome; and carcinoma of the small bowel. Presence of tumor infiltrating lymphocytes, Crohns-like lymphocytic reaction, mucinous/signet-ring differentiation, or medullary growth pattern.
Chapter 6: Colorectal Cancer
101
Gastroenterology Reference Guide
PREVENTION Screening for colorectal cancer is an important step in prevention. Removal of polyps found during screening helps prevent some colorectal cancers from developing. Additionally, early detection of colon cancer enables treatment that may cure the patient. Although reduction and/or elimination of lifestylebased risk factors has not been proven to prevent colorectal cancer, it is reasonable to recommend such reduction and/or elimination.5 Thus, patients should be counseled to: Reduce animal fat Ingest >30 to 35 grams of fiber per day by eating fruits, vegetables, legumes, and whole grains5 Avoid obesity Exercise daily Stop smoking Drink alcohol in moderation or not at all Dietary supplements (eg, folic acid, calcium) and medications (eg, aspirin, nonsteroidal antiinflammatory drugs [NSAIDs], estrogen-replacement therapy) may reduce risk of colorectal cancer. Their use to prevent colorectal cancer is not currently recommended, however. SYMPTOMS
Chapter 6: Colorectal Cancer
Symptoms vary based on the location of the cancer and extent of disease (Table 3).
102
Gastroenterology Reference Guide
Table 3. Colorectal Cancer Signs and Symptoms
Location Signs and Symptoms Cecum and ascending Chronic, insidious blood loss leading (right) colon to fatigue, weakness, unexplained iron deficiency anemia; occult blood Transverse and descending colon Abdominal cramping, constipation and increased stool frequency or diarrhea, stool streaked or mixed with blood, focal pain or tenderness signifying perforation Bloody stools, rectal bleeding, tenesmus, sensation of incomplete evacuation, pain
Rectosigmoid
SCREENING Screening for colorectal cancer can detect adenomatous polyps, the precursors of most colorectal cancers. Removal of these polyps may prevent cancer from developing. Additionally, screening can detect colorectal cancer before outward signs and symptoms are observed. Such early detection enables treatment that is likely to be successful in curing the patient. Screening recommendations vary according to the individuals risk (Tables 4-6).
Table 4. Screening Options for Adults of Average Risk*6
Annual FOBT or FIT Flexible sigmoidoscopy every 5 years Annual FOBT and flexible sigmoidoscopy every 5 years Double contrast barium enema every 5 years Colonoscopy every 10 years
FOBT, fecal occult blood test; FIT, fecal immunochemical test. *Begin screening at age 50 years.
Chapter 6: Colorectal Cancer
103
Gastroenterology Reference Guide
Table 5. Screening Recommendations Based on Personal History6
History of Inflammatory bowel disease Screening Recommendation Consider monitoring with colonoscopy and biopsy beginning 8 to 10 years after onset
1 to 2 tubular Colonoscopy in 5 years adenomas (<1 cm) >3 or advanced adenoma Colorectal cancer Colonoscopy in 3 years; if normal or only 1-2 adenomas <1 cm, repeat in 5 years Colonoscopy at diagnosis or 6 months following surgery if obstructed preoperatively; repeat in 3 years if normal; repeat again every 5 years if normal
Table 6. Screening Recommendations Based on Family History6
History of 1st degree relative with colorectal cancer or adenomatous polyp at age >60 years 2 1st degree relatives with colorectal cancer or 1st degree relative with adenomatous polyps at age 60 years 1st degree relative with HNPCC or carrier of known MMR gene mutation Screening Recommendation Screen as for average risk individuals, but start at age 40 years Colonoscopy every 5 years, beginning at age 40 years or 10 years before age of diagnosis in affected relative, whichever occurs earlier Colonoscopy every 1-2 years, beginning at age 20-25 years or 10 years before age of diagnosis in affected relative, whichever occurs earlier
Chapter 6: Colorectal Cancer
1st degree relative with FAP Colonoscopy annually or carrier of known APC beginning at age 10-12 years gene mutation
MMR, mismatch repair.
104
Gastroenterology Reference Guide
DIAGNOSIS AND LABORATORY TESTING Colorectal cancer is diagnosed based on histologic examination of biopsied tissue, which is usually obtained during sigmoidoscopy or colonoscopy. Laboratory tests are useful for screening, diagnosis, selecting therapy, and monitoring patients with colorectal cancer. Fecal Occult Blood (FOBT) and Fecal Immunochemical Tests (FIT) These tests are non-invasive screening tests performed on stool samples. Positive results indicate the presence of blood, which is associated with colorectal cancer, polyps, trauma, benign tumors, hemorrhoids, anal fissures, inflammatory bowel disease, and colonic angiodysplasia. Positive results should be followed by colonoscopy for a definitive diagnosis. A negative test means that colorectal cancer is unlikely; however, a negative test does not rule out colorectal cancer. Intermittent bleeding or nonuniform distribution of blood in the stool can cause negative tests. Table 7 outlines the differences between these 2 tests. FIT is considered more specific for colorectal cancer because diet and medication do not cause falsepositive or false-negative results and because it measures only the globin portion of the hemoglobin molecule. Globin does not survive passage from the upper gastrointestinal (GI) tract, thus ruling out upper GI causes of blood in the stool (eg, bleeding esophageal varices, esophagitis, gastritis, peptic ulcer). In a recent clinical study comparing an FIT (InSure') with an FOBT, the FIT had a colorectal cancer true-positive rate of 87.5% vs 54.2% for the FOBT.7
Chapter 6: Colorectal Cancer
105
Gastroenterology Reference Guide
Table 7. Differentiating Characteristics of FOBT and FIT
Method FOBT FIT Oxidation of guaiac by hemoglobin Immunochemistry targeting globin peroxidase; detects the human and portion of hemoglobin non-human heme portion of hemoglobin Detects upper* and lower GI bleeding Detects lower GI bleeding associated with colorectal cancer, adenomas, polyps, and other lower GI conditions
Specificity
Patient Avoid ingestion of red meat, some Diet and medication restrictions not preparation raw fruits, and uncooked vegetables required for 3 days prior to stool sample collection; may also need to avoid non-steroidal anti-inflammatory drugs, aspirin, and >250 mg/day vitamin C Sample collection Patient defecates into a clean, dry container (not toilet bowel); patient smears a portion of the stool on a slide or card. Patient repeats procedure for a total of 3 consecutive bowel movements. InSure': Toilet water is collected by gently disturbing surface of stool with a supplied brush and then dabbing the water onto a specimen card. Patient performs the procedure for a total of 2 consecutive bowel movements. Other products: 3 consecutive stool samples as described for FOBT Examples Hemoccult', Seracult', Coloscreen' InSure', HemeSelect', FlexSure'
*Not associated with colorectal cancer; includes bleeding in the esophagus and stomach.
Flexible Sigmoidoscopy Sigmoidoscopy allows inspection of the rectum and the sigmoid (descending) colon. The patient takes a laxative the night before and has an enema on the morning of the test. During the procedure, polyps and tissue samples (biopsies) can be removed by inserting tools through the sigmoidoscope. If adenomatous polyps or colorectal cancer is diagnosed, a colonoscopy should be performed to inspect the entire colon.
Chapter 6: Colorectal Cancer
106
Gastroenterology Reference Guide
Double-Contrast Barium Enema A double-contrast barium enema is used to optimize X-rays of the lining of the colon. The patient takes a laxative the night before and has an enema on the morning of the test. If positive, this procedure should be followed by a colonoscopy. Colonoscopy Colonoscopy allows inspection of the entire colon (ascending, transverse, and descending colon) and the rectum. The patient consumes a clear liquid diet for 1 to 3 days before the exam. Additionally, the patient takes a laxative the night before and has an enema on the morning of the test. During the procedure, polyps and tissue samples (biopsies) can be removed by inserting tools through the colonoscope. Histologic Exam Tissue removed from the colon or rectum is examined under a microscope by a pathologist. This examination is the only sure way to determine if cancer is present or not. MSI, MLH1, MSH2, MSH6 These tests are useful for screening (MSI) and diagnosis of HNPCC. See Part 3. Test Application and Interpretation for more information. Complete Blood Count (CBC) This laboratory test may be used to determine if anemia is present. Presence of anemia suggests chronic bleeding. The patient might need to be
Chapter 6: Colorectal Cancer
107
Gastroenterology Reference Guide
treated for the anemia prior to surgical treatment of the cancer. Carcinoembryonic Antigen (CEA) This laboratory test is used to monitor a patient being treated for colorectal cancer. An initial, baseline test is performed before treatment. The result of this baseline test is then compared with the result of tests performed during or after treatment. If the level of CEA increases or stays the same as the baseline level, the patient is not responding to treatment and an alternative therapy can be tried. A decreasing CEA level indicates the patient is responding to treatment. After successful treatment, an increasing level means the cancer is recurring. CEA can detect recurrence before other signs or symptoms of recurrence are evident. CA19-9 and CA72-4 These tumor markers might be helpful for the 25% of patients whose cancer does not produce CEA. If the patients cancer produces either marker, that marker can be used in the same manner as CEA. Additional Procedures Other procedures such as CT of the abdomen, chest, and pelvic area may be used to determine if the cancer has metastasized. Liver function tests may help evaluate possible liver metastasis. UGT1A1 and DPYD mutation analysis can be used to predict toxicity to irinotecan and pyrimidine-based chemotherapeutic agents (5-fluorouracil, capecitabine), respectively. UGT1A1 can also be used to assist in selecting an optimal initial dose of irinotecan.
Chapter 6: Colorectal Cancer
108
Gastroenterology Reference Guide
STAGING The American Joint Committee on Cancer (AJCC) has outlined terminology for staging colorectal cancers (Tables 8 and 9). The corresponding Dukes stage is provided in Table 9. Table 8. TNM Staging of Colorectal Cancer8
Tumor staging T0 Tis T1 T2 T3 T4 Nodal staging N0 N1 N2 Metastasis M0 M1 No distant metastasis Distant metastasis No evidence of metastasis to regional lymph nodes Metastasis to 1-3 regional lymph nodes Metastasis to 4 regional lymph nodes No evidence of primary tumor Carcinoma in situ Tumor invades submucosa Tumor invades muscularis propria Tumor invades subserosa or non-peritonealized pericolic or perirectal tissues Tumor invades other organs or structures and/or perforates visceral peritoneum
Table 9. Definition of Colorectal Cancer Stages8
AJCC Stage 0 I IIA IIB IIIA IIIB IIIC IV Dukes Stage A B B C C C Definition Tis, N0, M0 T1 or 2, N0, M0 T3, N0, M0 T4, N0, M0 T1 or 2, N1, M0 T3 or 4, N1, M0 Any T, N2, M0 Any T, any N, M1
Chapter 6: Colorectal Cancer
109
Gastroenterology Reference Guide
TREATMENT Treatment options depend on the stage and histologic grade (degree of differentiation) as well as the general health of the patient. Options are presented in Table 10. Radiation therapy may also be used for patients with rectal cancer.9 PROGNOSIS Early detection and treatment is the key to surviving colorectal cancer (Table 11). Surgery is often curative when the tumor has not metastasized. Additionally, surgical patients rarely (colon) or infrequently (rectum) need a colostomy. RESOURCES National and regional educational and supportive resources are available. For more information, contact: American Society of Colon and Rectal Surgeons Phone: 847-290-9184 Email: ascrs@fascrs.org Internet: http://www.fascrs.org Table 10. Therapeutic Options for Patients with Colorectal Cancer1,8,9
Option Curative surgery Non-curative surgery Comments Appropriate for nonmetastatic cancers; may include surgical resection of the tumor or colectomy and removal of regional lymph nodes Appropriate for patients with metastatic disease with GI bleeding or obstruction; less extensive than curative surgery. Also appropriate to treat metastatic disease in selected cases
Chapter 6: Colorectal Cancer
Adjuvant Not indicated for patients with stage I cancer; options include chemotherapy 5-fluorouracil, leucovorin, oxaliplatin, irinotecan, capecitabine, bevacizumab, cetuximab, panitumumab
110
Gastroenterology Reference Guide
Table 11. Colorectal Cancer Survival Rates2
Stage at Treatment All Early, localized cancer Regional metastasis* Distant metastasis
*Lymph nodes or adjacent organs.
5-Year Survival Rate (%) 64 90 68 10
American Cancer Society Phone: 800-ACS-2345 (227-2345) TTY: 866-228-4327 Internet: http://www.cancer.org Cancer Care, Inc. Phone: 212-221-3300 or 800-813-HOPE (813-4673) Email: info@cancercare.org Internet: http://www.cancercare.org Cancer Hope Network Phone: 877- HOPENET (467-3638)or 908-879-4039 (New Jersey residents) Internet: http://www.cancerhopenetwork.org Cancer Information Service (CIS) Phone: 800-4-CANCER (422-6237) TTY: 800-332-8615 Internet: http://cis.nci.nih.gov Colon Cancer Alliance (CCA) Phone: 877-422-2030 Internet: http://www.ccalliance.org Association of Cancer Online Resources Colon Cancer Discussion List Internet: http://www.acor.org/colon.html
Chapter 6: Colorectal Cancer
111
Gastroenterology Reference Guide
Colorectal Cancer Network Phone: 301-879-1500 Email: CCNetwork@colorectal-cancer.net Internet: http://www.colorectal-cancer.net American Gastroenterological Association Foundation for Digestive Health and Nutrition Phone: 301-222-4002 or 866-337-FDHN (337-3346) Email: info@fdhn.org Internet: http://www.fdhn.org Gilda's Club Phone: 888-GILDA-4-U (445-3248) Email: info@gildasclub.org Internet: http://www.gildasclub.org National Cancer Institute Phone: 800-4-CANCER (422-6237) or 301-496-6631 Internet: http://www.nci.nih.gov NCI's Facing Forward Series Phone: 888-4-CANCER (422-6237) Internet: http://www.nci.nih.gov/cancerinfo/ life-after-treatment National Coalition for Cancer Survivorship Phone: 877-NCCS-YES (622-7937) or 301-650-9127 Email: info@canceradvocacy.org Internet: http://www.canceradvocacy.org
Chapter 6: Colorectal Cancer
The Cancer Information Network Internet: http://www.cancerlinksusa.com/colorectal/ index.asp
112
Gastroenterology Reference Guide
Collaborative Group of the Americas on Inherited Colorectal Cancer (CGA-ICC) Phone: 847-290-9184 Internet: http://www.cgaicc.com United Ostomy Associations of America, Inc. Phone: 800-826-0826 Email: editor@uoaa.org Internet: http://www.uoaa.org The Wellness Community Phone: 888-793-WELL (793-9355) or 202-659-9709 Email: help@thewellnesscommunity.org Internet: http://www.thewellnesscommunity.org REFERENCES CITED
1. Mayer RJ. Gastrointestinal tract cancer. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:523-533. 2. American Cancer Society: Cancer facts and figures 2006. Available at: http://www.cancer.org/downloads/STT/CAFF2006PWSecured.pdf. Accessed February 15, 2007. 3. Vasen HF, Watson P, Mecklin J-P, et al. New clinical criteria for hereditary nonpolyposis colorectal cancer (HNPCC, Lynch syndrome) proposed by the International Collaborative Group on HNPCC. Gastroenterology. 1999;116:1453-1456. 4. Umar A, Boland CR, Terdiman JP, et al. Revised Bethesda guidelines for hereditary nonpolyposis colorectal cancer (Lynch syndrome) and microsatellite instability. J Natl Cancer Inst. 2004;96:261-268. 5. American Gastroenterological Association medical position statement: impact of dietary fiber on colon cancer occurrence. Gastroenterology. 2000;118:1233-1234. 6. Winawer S, Fletcher R, Rex D, et al for the U.S. Multisociety Task Force on Colorectal Cancer. Colorectal cancer screening and surveillance: clinical guidelines and rationaleUpdate based on new evidence. Gastroenterology. 2003;124:544-560. 7. Smith A, Young GP, Cole SR, et al. Comparison of a brush-sampling fecal immunochemical test for hemoglobin with a sensitive guaiac-based fecal occult blood test in detection of colorectal neoplasia. Cancer. 2006;107:2152-2159. [This study was funded in part by Enterix Inc. (through Enterix Australia Pty. Ltd), the manufacturer of InSure FIT. Enterix is now owned by Quest Diagnostics Incorporated. However, neither Enterix nor Quest Diagnostics participated in the data analysis or influenced the conclusions reached by the authors.]
Chapter 6: Colorectal Cancer
113
Gastroenterology Reference Guide
8. Engstrom PF, Benson AB III for the National Comprehensive Cancer Network'. NCCN Clinical Practice Guidelines in Oncology'. Colon Cancer, v.1.2007. Available at: http://www.nccn.org/professionals/physician_gls/ PDF/colon.pdf. Accessed February 20, 2007. 9. Engstrom PF, Benson AB III for the National Comprehensive Cancer Network'. NCCN Clinical Practice Guidelines in Oncology'. Rectal Cancer, v.1.2007. Available at: http://www.nccn.org/professionals/physician_gls/ PDF/rectal.pdf. Accessed February 20, 2007.
ADDITIONAL REFERENCES
1. Colorectal Cancer. In: Beers MH, Porter RS, Jones TV, Kaplan JL, Berkwits M, eds. The Merck Manual of Diagnosis and Therapy. 18th ed. Merck Publishing Group; 2006. Available at: http://www.merck.com/mmpe/ sec02/ch021/ch021h.html?qt=colorectal%20cancer&alt=sh. Accessed February 21, 2007. 2. Fecal Occult Blood Test (FOBT). [MedlinePlus Web site]. Available at: http://www.nlm.nih.gov/medlineplus/ency/article/007008.htm. Accessed February 21, 2007.
Chapter 6: Colorectal Cancer
114
CHAPTER 7. LIVER DISORDERS
Gastroenterology Reference Guide
SECTION 1. HEPATITIS OVERVIEW Hepatitis is characterized by inflammation of the liver and can be caused by a variety of things, including viruses, bacteria, alcoholism, autoimmune disease, medications, and an inherited disorder called Wilsons disease. Viral hepatitis is relatively common and can be caused by cytomegalovirus (CMV), Epstein-Barr virus (EBV), and human immunodeficiency virus (HIV) as well as by the hepatitis viruses A, B, C, D, and E. Of these, hepatitis A, B, and C are the most common, occurring at a rate of 4.3 per 100,000 individuals in 2004.1 Hepatitis C is the most serious of the 3 because the majority of infections become chronic, it accounts for a substantial proportion of serious liver disease, and there is no vaccine for prevention. Viral hepatitis caused by hepatitis A, B, C, and D will be the focus of the discussion in this section. ETIOLOGY The hepatitis viruses can be transmitted in a variety of ways (Table 1).
Chapter 7: Liver Disorders
Table 1. Primary Transmission Routes of the Hepatitis Viruses2
Hepatitis Virus A B C D Fecal-oral X Parenteral X X X Perinatal X X Sexual X X* X
Bold reflects most common transmission route. *Possibly, but barrier protection is nevertheless advised.
115
Gastroenterology Reference Guide
Chapter 7: Liver Disorders
RISK FACTORS Risk factors for transmission of the hepatitis viruses are listed in Table 2. People with certain disorders (eg, hemophilia, chronic renal failure, cancer requiring chemotherapy) are at increased risk for hepatitis infections transmitted parenterally. Healthcare workers in hospitals or other institutions are at increased risk of infections transmitted parenterally or through a fecal-oral route. Contaminated needles are a risk for healthcare workers (accidental needle sticks), for those injecting drugs of abuse, and for those getting a tattoo or having acupuncture. Transmission risk increases for people who travel to endemic areas. Table 3 lists the most common risk factor for HAV, HBV, and HCV as reported to the Centers for Disease Control in 2004.1
Table 2. Transmission Risk of the Hepatitis Viruses2
Transmission Route Fecal-oral Risk Factors Poor personal hygiene Overcrowding Contaminated water Contaminated food (eg, milk, raspberries and strawberries, shellfish) Close contact with infected person(s) Repeated blood or blood product transfusions Contact with bodily fluids (eg, blood) of infected person Drug abuse (injection with contaminated needles) Hemodialysis Organ transplantation HBV infection (including carrier status) during pregnancy (risk to fetus) Hepatitis-infected sex partner Multiple sex partners Men having sex with men
Parenteral
Perinatal Sexual
116
Gastroenterology Reference Guide
Table 3. Most Common Risk Factor for Hepatitis A, B, and C Infection1
Hepatitis Virus A B C Most Common Risk Factor International travel to endemic area Sexual contact Drug abuse (injection with contaminated needles)
Chapter 7: Liver Disorders
PREVALENCE The overall prevalence of viral hepatitis attributed to HAV, HBV, and HCV has decreased in the United States since 1998.1 This decrease is due, in part, to the use of HAV and HBV vaccines and improvements in the screening of blood donors. Table 4 lists prevalence statistics for HAV, HBV, and HCV. PREVENTION Immunization (passive and active) is used to help prevent viral hepatitis infection (Table 5). Other prevention measures include screening blood donors and implementation of behavioral changes designed to limit exposure. Table 4. Hepatitis Virus Prevalence1
Prevalence Estimated new cases in 2004* Age-related Hepatitis A 56,000 Similar among all age groups Hepatitis B 60,000 Highest in ages 25 to 44 years; lowest in ages <15 years Hepatitis C 26,000 Highest in ages >15 years
Gender-related Similar in males and 1.7 times higher in females except higher males than females in males 35-44 years of age
*Asymptomatic infection and underreporting were taken into account.
Slightly higher in males than females
117
Gastroenterology Reference Guide
Chapter 7: Liver Disorders
Table 5. Immunization for Prevention of Viral Hepatitis2
Hepatitis Immunization Virus Availability A Immunoglobulin administered before or up to 2 weeks after exposure Appropriate Individuals Individuals in intimate contact* with an affected person Children (and their family members) and staff at day-care centers with an infected individual Travelers to endemic areas if <4 weeks from date of travel Age >2 years Children living in area of high frequency Day-care center employees Intravenous drug users Laboratory (health care) workers Men having sex with men Military personnel Patients requiring frequent doses of clotting-factor concentrates Patients with chronic liver disease (including chronic HCV infection) Primate handlers Travelers to endemic areas Effective Period Short term
Vaccine
20 years
Vaccine
Children <18 years of age Unclear; Health care workers exposed to blood probably 5 Hemodialysis center patients and staff to 10 years Household and sexual contacts of HBV carriers Intravenous drug users People in endemic areas (living or travelers) People with hemophilia People with multiple sex partners Prison inmates Unvaccinated person exposed to HBV Unclear (eg, needle stick, sex with affected person, etc) Infants born to HBsAg-positive woman Susceptible people Unclear
Vaccine + HBIG
C D
None HBV vaccine
HBIG, hepatitis B immune globulin. *Household, sexual, institutional.
118
Gastroenterology Reference Guide
SYMPTOMS The hepatitis viruses produce clinically similar illnesses and cannot be differentiated based solely on the patients presentation. While some patients are asymptomatic, others experience sudden, intense symptoms (ie, fulminant disease). Chronic infections (ie, those of 6 months duration) can progress to liver cirrhosis and hepatocellular carcinoma. Symptoms of acute viral hepatitis include: Anorexia Nausea Vomiting Malaise Arthralgias Myalgias Headache Fever Dark urine Clay-colored stools Jaundice Weight loss Abdominal pain Symptoms typically appear 2 to 26 weeks after exposure (Table 6).
Chapter 7: Liver Disorders
Table 6. Incubation Periods for the Hepatitis Viruses2
Hepatitis Virus A B C D Incubation Period (weeks) 2 to 6 4 to 26 2 to 23 4 to 26
119
Gastroenterology Reference Guide
Chapter 7: Liver Disorders
Patients with chronic viral hepatitis may be asymptomatic or may have the same symptoms as those with acute stage disease. Additionally, patients with chronic viral hepatitis may have: Fatigue Ascites Edema Bleeding gastroesophageal varices Hepatic encephalopathy Coagulopathy Hypersplenism Leukocytoclastic vasculitis Immune-complex glomerulonephritis Polyarteritis nodosa Sjgrens syndrome Lichen planus Porphyria cutanea tarda DIAGNOSIS AND LABORATORY TESTING The differential diagnosis of viral hepatitis includes: Leptospira, Candida, Brucella, Mycobacteria, and Pneumocystis infections Medication- or anesthesia-induced hepatitis Alcoholism Cholecystitis Common duct stone Ascending cholangitis Pancreatic cancer Primary parenchymal liver disease Certain vascular disorders Acute fatty liver, cholestasis, eclampsia in a pregnant patient Wilsons disease 1-antitrypsin deficiency
120
Gastroenterology Reference Guide
Liver function tests (Table 7), along with clinical features, help diagnose hepatitis. Liver function tests are not specific, however. Abnormal results are found in many conditions. Serologic and molecular tests are specific for the particular type of viral hepatitis. Table 8 lists tests associated with HAV, HBV, HCV, and HDV. Tests specific for HEV, CMV, EBV, HIV, herpes simplex, and coxsackievirus are also available. See Part 2 and 3 of this manual for test availability, testing algorithms, and detailed interpretive information. Liver biopsies are usually not required for diagnosis, but may be helpful to rule out certain conditions (eg, alcoholic hepatitis) and assess the extent of disease (ie, stage of fibrosis) prior to treatment in patients with chronic hepatitis. HepaScore is a newly developed, non-invasive laboratory test that also may assist with diagnosis and staging of liver fibrosis in patients with hepatitis C. TREATMENT Acute Viral Hepatitis Antiviral medication is not required for most cases of acute hepatitis A and B. Since untreated hepatitis C very often progresses to chronic disease, the decision to treat hepatitis C with antiviral therapy in the early Table 7. Liver Function Test Results in Patients with Hepatitis
Test Alanine aminotransferase (ALT) Albumin Alkaline phosphatase Aspartate aminotransferase (AST) Bilirubin (total, direct) Result Normal or Normal or
Chapter 7: Liver Disorders
121
Gastroenterology Reference Guide
Chapter 7: Liver Disorders
Table 8. Laboratory Tests for the Differential Diagnosis of Viral Hepatitis
Viral Hepatitis Type Test Hepatitis A HAV antibody (IgM) Hepatitis B Hepatitis C HBV surface antigen HCV antibody (EIA) HCV antibody (RIBA) HCV RNA Hepatitis D HDV antibody HDV antigen
*Consistent with type-specific viral hepatitis.
Result* Reactive Reactive Reactive Positive 5 IU/mL Reactive Reactive
HBV core antibody (IgM) Reactive
days following onset is dependent on HCV RNA and ALT levels and the stage of liver fibrosis. Patients are generally advised to restrict physical activity, eat a high-calorie diet (primarily in the morning owing to afternoon nausea), avoid alcoholic drinks, and avoid medications that may cause cholestasis and those that are metabolized by the liver. Patients with fulminant disease require special treatment including maintenance of fluid balance, circulatory and respiratory support, control of bleeding and glycemic state, and restricted protein intake. Laboratory tests can be used to determine recovery from acute infection (Table 9). Chronic Viral Hepatitis Antiviral therapy (Table 10) is commonly used to treat chronic viral hepatitis. The goal is to reduce the viral load (level of viral DNA or RNA in the blood) to undetectable levels. Thus, viral load testing is an important tool for monitoring therapy. Additional indicators of successful therapy are listed in Table 9.
122
Gastroenterology Reference Guide
Table 9. Indicators of Recovery from Viral Hepatitis
Viral Hepatitis Type Test Hepatitis A ALT Hepatitis B HBV envelope antigen HBV envelope antibody HBV surface antigen HBV DNA Result* Normal Nonreactive Reactive Nonreactive Not detected <100 IU/mL (<160 copies/mL) Negative Negative <5 IU/mL
Chapter 7: Liver Disorders
Hepatitis C
HCV antibody (RIBA) HCV RNA
ALT, alanine aminotransferase. *Consistent with recovery.
Genotyping can predict the response to antiviral therapy. For example, some HBV-associated mutations diminish response to one medication but not to another. Thus, knowing the HBV genotype can help in selecting appropriate medication for an individual patient. Since the genotype may change over the course of treatment, periodic monitoring of non-responders may be helpful.
Table 10. Antiviral Therapy for Treating Chronic Viral Hepatitis3
Hepatitis B Approved Interferon Lamivudine Adefovir dipivoxil Entecavir Under development Telbivudine Clevudine Emtricitabine Pegylated interferon
*Pegylated interferon combined with ribavirin is the most effective regimen.
Hepatitis C* Interferon Ribavirin Pegylated interferon-2a Pegylated interferon-2b
Hepatitis D None effective; treatment of choice is liver transplantation at time of liver failure
123
Gastroenterology Reference Guide
Chapter 7: Liver Disorders
Patients with HCV genotype 2 or 3 are more likely to respond to therapy than are patients with HCV genotype 1. Additionally, patients with genotype 1 require a longer course of treatment. More detailed information, including test availability, testing algorithms, and interpretive information can be found in Part 2 and 3 of this manual. PROGNOSIS Most patients with hepatitis A recover from their infection within 6 months; however, the infection is fatal in a small percentage of infected people (Table 11). Hepatitis A does not progress to chronic disease, and patients who recover are immune to recurrent infection. Most patients with acute hepatitis B also recover within 6 months and are immune for life. In those who do not, the infection is fatal in some and becomes chronic in others. Patients with chronic disease may develop hepatocellular carcinoma. Those who develop a superinfection or coinfection with hepatitis D also have a poorer prognosis. Although most patients with hepatitis C develop chronic disease, their prognosis is relatively good. A Table 11. Viral Hepatitis Prognosis2,3
Viral Hepatitis Type A B C Mortality Rate (%) 1 1 to 2 1 to 5 Likelihood of Carrier State None 10% (adults) 90% (infants) 50%-80% 80%-90% Yes Likelihood of Chronic Disease None 1%-10% Association with Hepatocellular Carcinoma No Yes
124
Gastroenterology Reference Guide
small proportion develops serious complications such as type II cryoglobulinemia and hepatocellular carcinoma. RESOURCES National and regional educational and supportive resources are available. For more information, contact: American Liver Foundation (ALF) Phone: 800-GO-LIVER (465-4837) or 888-4HEP-USA (443-7872) or 212-668-1000 Email: info@liverfoundation.org Internet: http://www.liverfoundation.org Centers for Disease Control (CDC) Phone: 800-CDC-INFO (232-6348) Email: cdcinfo@cdc.gov Internet: http://www.cdc.gov/ncidod/diseases/ hepatitis/ National Digestive Diseases Information Clearinghouse (NDICC) Phone: 800-891-5389 Email: nddic@info.niddk.nih.gov Internet: http://www.cdc.gov/ncidod/diseases/ hepatitis/ The following links are provided by the American Liver Foundation: HCV Advocate Internet: http://www.hcvadvocate.org/ Hep C Alert Internet: http://www.hep-c-alert.org/index.htm
Chapter 7: Liver Disorders
Hepatitis D Infection Hepatitis D virus (HDV) can only infect patients who have a hepatitis B infection (ie, no HBV infection, no HDV infection). There are 2 types of HDV infection: coinfection and superinfection. A patient is said to have HDV coinfection when the HDV infection was acquired at the same time as the HBV infection. Conversely, a patient is said to have an HDV superinfection when the HDV infection was acquired after the HBV infection.
125
Gastroenterology Reference Guide
Chapter 7: Liver Disorders
Hep C Connection Internet: http://www.hepc-connection.org/ Hepatitis B Foundation Phone: 215-489-4900 Email: info@hepb.org Internet: http://www.hepb.org Hepatitis Foundation International Phone: 800-891-0707 or 301-622-4200 Email: hfi@comcast.net Internet: http://www.hepfi.org/ REFERENCES
1. Centers for Disease Control and Prevention. Hepatitis Surveillance Report No. 61. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, 2006. Available at: http://www.cdc.gov/ncidod/diseases/hepatitis/resource/PDFs/ hep_surveillance_61.pdf. Accessed: February 23, 2007. 2. Dienstag JL, Isselbacher KJ. Acute viral hepatitis. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGrawHill; 2005:1822-1838. 3. Dienstag JL, Isselbacher KJ. Chronic hepatitis. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:1844-1855.
126
Gastroenterology Reference Guide
SECTION 2. PRIMARY BILIARY CIRRHOSIS OVERVIEW Primary biliary cirrhosis (PBC) is characterized by a slow, progressive destruction of the bile ducts within the liver, leading to cholestasis (impaired flow of bile), fibrosis, cirrhosis, and eventual liver failure. In stage 1, there is chronic inflammation and necrosis of intrahepatic bile ducts. In stage 2, bile ductules proliferate; there is infiltration of mononuclear cells in portal areas; and mild fibrosis may be seen. In stage 3, there is less inflammatory infiltrate in portal areas; bile ducts are absent from portal triads; and there is increased fibrosis. In stage 4, there is biliary cirrhosis with few remaining bile ducts. ETIOLOGY AND RISK FACTORS PBC is thought to be an autoimmune disorder because it is frequently associated with other autoimmune disorders (eg, sicca syndrome [dry eyes and mouth], autoimmune thyroiditis, type 1 diabetes, rheumatoid arthritis, CREST syndrome, Raynauds syndrome). Moreover, >90% of patients have an antimitochondrial antibody (AMA) that is rare in other forms of liver disease.1 INCIDENCE/PREVALENCE PBC occurs most often in women over the age of 20 years.2 Among patients with symptomatic disease, 90% are women between the ages of 35 and 60 years.1
Chapter 7: Liver Disorders
127
Gastroenterology Reference Guide
Chapter 7: Liver Disorders
SYMPTOMS About 50% to 60% of patients with PBC are asymptomatic at time of diagnosis.2,3 The first sign may be an abnormal liver function test that is found during a routine physical or as part of a work-up for another disorder. Symptomatic patients may have: Pruritus (itchy skin) Fatigue Jaundice Hyperpigmentation (melanosis) Hyperlipidemia Steatorrhea (excessive fat in feces) Malabsorption of fat-soluble vitamins Xanthomata (lipid-filled nodule or plaque) Variceal hemorrhage (portal hypertension) Ascites Osteoporosis Osteomalacia Finger clubbing Hepatic insufficiency DIAGNOSIS AND LABORATORY TESTING Diagnosis is based on laboratory tests (Table 1), ultrasound of the liver and biliary tree, and liver biopsy results. Cholangiography may be needed for some patients. The differential diagnosis includes primary sclerosing cholangitis and remediable extrahepatic biliary tract obstruction. An otherwise unexplained increase in the alkaline phosphatase (ALP) level should prompt consideration of PBC diagnosis. The patient may be tested for gamma glutamyl transpeptidase (GGT), conjugated bilirubin, and total cholesterol. An elevated GGT level confirms liver origin of the
128
Gastroenterology Reference Guide
increased ALP. Alkaline phosphatase isoenzymes can also be used to confirm liver origin. Bilirubin and cholesterol levels may or may not be elevated depending on the stage of disease. Bilirubin is usually elevated in the later stages and suggests a worse prognosis. Almost all patients (>90%) with PBC have a positive AMA result.1,3 An ultrasound is recommended for patients with evidence of cholestasis.2 A liver biopsy may be performed to confirm the diagnosis, but is not always necessary.2,3 The most important diagnostic criteria include increased liver enzymes for >6 months, a positive AMA result, and compatible liver biopsy (histologic) findings.3 If the diagnosis is questionable, other tests may be performed, including an immunoglobulin profile and a serum antinuclear antibody (ANA) test.2 An elevated IgM fraction is supportive of a PBC diagnosis, as is a positive ANA test result; however, these results are not specific for PBC.
Chapter 7: Liver Disorders
Table 1. Laboratory Test Results Consistent with Primary Biliary Cirrhosis2,3
Test Alkaline phosphatase (ALP) Gamma glutamyl transpeptidase (GGT) Bilirubin, conjugated Cholesterol, total Immunoglobulins or normal or normal IgG: normal IgM: IgA: normal or deficiency Antimitochondrial antibody (AMA) Antinuclear antibody (ANA) if coincident IgA Result
Positive, titer 1:40 Positive (50% of patients)
129
Gastroenterology Reference Guide
Chapter 7: Liver Disorders
TREATMENT Two treatments are available for PBC: ursodiol (ursodeoxycholic acid) and liver transplantation. Ursodiol therapy (13 to 15 mg/kg/day) slows the progression of PBC but does not cure it. ALP, GGT, bilirubin, and cholesterol levels tend to decrease. Some symptoms may be improved while others are not. For example, ursodiol has no effect on fatigue or osteoporosis but has variable effect on pruritus and portal hypertension. Side effects are rare. Liver transplantation is an effective therapy: recurrence is uncommon and, if it does happen, the progression is very slow. Timing of liver transplantation is based in part on the Mayo risk score, which includes consideration of the patients age, serum albumin and bilirubin levels, edema score, and prothrombin time test results. The American Association for the Study of Liver Diseases recommends transplantation for liver failure and in some patients with uncontrollable pruritus or severe osteoporosis.2 Immunosuppressive therapy is not currently recommended. Prior to liver transplantation, symptomatic and preventative treatment is often employed (Table 2). PROGNOSIS Although PBC progresses slowly, people with it do not live as long as those without it. Progression is highly variable, taking months to years. However, as stated above, liver transplantation is very successful.
130
Gastroenterology Reference Guide
Table 2. Management of Primary Biliary Cirrhosis1,2
Symptom Pruritus Options Cholestyramine (1st choice) Rifampicin (2nd line therapy) Opioid antagonists such as nalmephene and naltrexone (resistant patients only) Steatorrhea Fat soluble vitamin deficiency Portal hypertension Osteoporosis Low-fat diet Supplementation with vitamins A, D, E, and K Beta blockers with or without nitrates when varices are visualized endoscopically Calcium and vitamin D supplementation Exercise, smoking cessation Hormone replacement therapy Bisphosphonate therapy (eg, alendronate)
Chapter 7: Liver Disorders
RESOURCES National and regional educational and supportive resources are available. For more information, contact: American Liver Foundation (ALF) Phone: 800-GO-LIVER (465-4837)or 888-4HEP-USA (443-7872) Email: info@liverfoundation.org Internet: http://www.liverfoundation.org National Digestive Diseases Information Clearinghouse (NDICC) Phone: 800-891-5389 Email: nddic@info.niddk.nih.gov Internet: http://digestive.niddk.nih.gov/ddiseases/ pubs/primarybiliarycirrhosis/index.htm
131
Gastroenterology Reference Guide
Chapter 7: Liver Disorders
REFERENCES
1. Chung RT, Podolsky DK. Cirrhosis and its complications. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGrawHill; 2005:1858-1869. 2. Heathcote EJ. Management of primary biliary cirrhosis. The American Association for the Study of Liver Diseases practice guidelines. Hepatology. 2000;31:1005-1013. 3. Kaplan MM, Gershwin ME. Primary biliary cirrhosis. N Engl J Med. 2005;353:1261-1273.
132
Gastroenterology Reference Guide
SECTION 3. LIVER CANCER OVERVIEW Primary liver cancer includes hepatocellular carcinoma (HCC), fibrolamellar carcinoma, cholangiocarcinoma, and papilla of Vater carcinoma. Hepatocellular carcinoma is by far the most frequent of these and will be the focus of discussion in this section. Metastatic liver cancer is about 20 times more frequent than primary liver cancer and ranks second only to cirrhosis as a cause of fatal liver disease.1 Primary cancers of the gastrointestinal tract, breast, and lung are the most common types of cancer that metastasize to the liver. However, all primary cancers, except those in the brain, may spread to the liver. Patients may present with weight loss, anorexia, fever, sweating, and fatigue. Other symptoms occur in more advanced stages. Evaluation for liver metastasis usually occurs before treatment of the primary cancer. Definitive diagnosis is based on liver biopsy results following discovery of an elevated alkaline phosphatase level and/or a mass shown on an ultrasound, CT, or MRI of the liver. Therapy is usually palliative. Surgery or systemic chemotherapy may prolong life in some cases. ETIOLOGY AND RISK FACTORS HCC is a complication of cirrhosis and, as such, is caused by chronic liver disease of any type (Table 1). In the United States, chronic hepatitis B and C infections are the greatest risk factors. Hormones may also play a role since prevalence is greater in men than in women.1,2
Chapter 7: Liver Disorders
133
Gastroenterology Reference Guide
Chapter 7: Liver Disorders
Table 1. Hepatocellular Carcinoma Risk Factors in the United States1
Hepatitis C infection Hepatitis B infection Alcoholic liver disease 1-antitrypsin deficiency Hemochromatosis Tyrosinemia Primary biliary cirrhosis Nonalcoholic steatohepatitis Environmental carcinogens (eg, thorium dioxide, vinyl chloride)
INCIDENCE The American Cancer Society estimates there will be about 19,000 new cases of liver and intrahepatic bile duct cancer in the United States during 2007.2 More than half of these will be in men and more than half of the estimated 16,800 deaths will also be in men.2 SYMPTOMS Patients present with nonspecific symptoms including: Upper abdominal pain Anorexia Weight loss Malaise Jaundice Additionally, a paraneoplastic syndrome may occur and include: Erythrocytosis Hypercalcemia Hypercholesterolemia
134
Gastroenterology Reference Guide
Hypoglycemia Polymyositis Porphyria Dysfibrinogenemia Cryofibrinogenemia Vasoactive peptide-associated diarrhea SCREENING Screening the general population for HCC is not recommended; however, the National Comprehensive Cancer Network (NCCN) recommends patients at high risk be monitored with alkaline phosphatase, albumin, alpha-fetoprotein (AFP), and liver ultrasonography every 3 to 6 months.3 High-risk individuals include those with chronic hepatitis C virus infection. The frequency of monitoring should increase to every 3 months when the AFP is rising but the ultrasound remains negative.3 It is unclear whether such monitoring results in detection of HCC at a curable stage. Others recommend screening every 6 months to 1 year with AFP and ultrasound. The cost-effectiveness of this strategy is also questionable.4 DIAGNOSIS AND LABORATORY TESTING The diagnostic work-up includes a medical history, physical examination, laboratory tests, imaging studies, and biopsy. Laboratory Tests Laboratory tests include: AFP AFP-L3
Chapter 7: Liver Disorders
135
Gastroenterology Reference Guide
Des--carboxy prothrombin protein (DCP) Glypican-3 Complete blood count (CBC) and platelets Hepatitis screen Liver function tests, including alanine aminotransferase (ALT), total protein, albumin, globulin, alkaline phosphatase, aspartate aminotransferase (AST), and bilirubin (total, direct, indirect) Prothrombin Blood urea nitrogen (BUN) Creatinine Lactate dehydrogenase (LDH) The first 4 tests listed above are tumor markers that are used in the diagnosis and management of HCC.5 AFP is the most widely used of these tumor markers. It is an oncofetal protein that is elevated in patients with HCC, cirrhosis, hepatitis, nonseminomatous germ cell tumors, and other conditions. Levels >500 g/L (ie, >500 ng/mL), however, are highly suggestive of HCC and occur in 70% to 80% of patients.1 Like AFP, each of these tumor markers are elevated in some patients with HCC as well as in patients with other conditions. Their sensitivity and specificity for HCC vary with the population studied and the cut-off value (ie, reference range) used. Since they are independent markers, their combined use improves the diagnostic sensitivity and specificity. Tumor markers are also important for assessing prognosis and monitoring therapy. When monitoring therapy: A sustained level post therapy indicates residual disease
Chapter 7: Liver Disorders
136
Gastroenterology Reference Guide
Rising levels indicate recurrent and/or progressive disease Falling levels indicate therapeutic response The other tests listed above help assess the liver reserve and comorbid conditions and are considered when making management decisions. Imaging Studies
Chapter 7: Liver Disorders
AFP-L3
AFP has 3 different forms, called glycoforms. The AFPImaging studies enable visualization of the tumor and L1 glycoform is the major form found in patients with may include: nonmalignant liver disorders such as cirrhosis and viral Ultrasound hepatitis infection. AFP-L2 is found primarily in yolk-sac Computed tomography (CT) tumors. AFP-L3 is produced Magnetic resonance imaging (MRI) by liver cancer cells; it is the Hepatic artery angiography major glycoform found in people with HCC. AFP-L3 CT and MRI help define the extent and number of might therefore be more specific for HCC than total lesions, vascular anatomy, vessel involvement, and AFP measurements and may metastasis; this information is considered when help differentiate between making treatment decisions. malignant and nonmalignant liver disease. People with an Biopsy increased percentage of AFP-L3, relative to total AFP, are at greater risk of HCC. AFP and imaging studies can be sufficient for Additionally, people with diagnosis; however, definitive diagnosis is based on HCC and increased AFP-L3 biopsy and histologic examination. Biopsy is may have a worse appropriate for patients with potentially resectable prognosis.5
disease who have: <400 ng/mL AFP and a non-reactive hepatitis B surface antigen test result <4,000 ng/mL AFP and a reactive hepatitis B surface antigen test result3
137
Gastroenterology Reference Guide
Chapter 7: Liver Disorders
Table 2. Histologic Grading of Hepatocellular Cancer3
Grade G1 G2 G3 G4 Definition Well differentiated Moderately differentiated Poorly differentiated Undifferentiated
Additionally, a biopsy sample is used to determine the histologic grade of the tumor (Table 2). STAGING The American Joint Committee on Cancer (AJCC) has outlined terminology for staging liver cancer (Tables 3 and 4). Other scoring systems (eg, Cancer of the Liver Italian Program [CLIP]) can be used for predicting prognosis for patients with unresectable tumors. Table 3. TNM Staging of Liver Cancer3
Tumor staging T0 T1 T2 T3 T4 Nodal staging N0 N1 Metastasis M0 M1 No evidence of primary tumor Solitary tumor without vascular invasion Solitary tumor with vascular invasion or multiple tumors 5 cm Multiple tumors >5 cm or tumor involving major branch of portal or hepatic vein Invasion of adjacent organs other than gallbladder or perforation of visceral peritoneum No evidence of metastasis to regional lymph nodes Metastasis to regional lymph nodes No distant metastasis Distant metastasis
138
Gastroenterology Reference Guide
Table 4. Definition of Liver Cancer Stages3
Stage I II IIIA IIIB IIIC IV Definition T1, N0, M0 T2, N0, M0 T3, N0, M0 T4, N0, M0 Any T, N1, M0 Any T, any N, M1
Chapter 7: Liver Disorders
TREATMENT Treatment options (Table 5) vary based on the tumor stage, grade, liver reserve, and comorbid conditions. Surgery that includes a liver transplantation is the only cure for HCC. Patients who are candidates for liver transplantation include those for whom resection is not an option and who have the following: A single tumor 5 cm or 2 to 3 tumors each 3 cm No macrovascular invasion No extrahepatic spread to lymph nodes, lungs, abdominal organs, or bone
Table 5. Therapeutic Options for Hepatocellular Cancer3
Surgical resection with or without ablation Surgical resection with liver transplantation Ablation with radiofrequency, alcohol, cryotherapy, or microwave Embolization (vessel occlusion) including chemoembolization or radioembolization Chemotherapy Radiation therapy Palliative therapy (ie, supportive care)
139
Gastroenterology Reference Guide
Chapter 7: Liver Disorders
PROGNOSIS The 5-year survival in liver transplant recipients is as high as 75%.3 The 3-year survival for patients diagnosed before symptoms occur and who receive surgical resection without a liver transplant is 28%.1 Most patients diagnosed when symptomatic die within 3 to 6 months.1 RESOURCES National and regional educational and supportive resources are available. For more information, contact: American Cancer Society Phone: 800-ACS-2345 (227-2345) TTY: 866-228-4327 Internet: http://www.cancer.org American Liver Foundation (ALF) Phone: 800-GO-LIVER (465-4837) or 888-4HEP-USA (443-7872) or 212-668-1000 Email: info@liverfoundation.org Internet: http://www.liverfoundation.org Cancer Care, Inc. Phone: 800-813-HOPE (813-4673) or 212-221-3300 Email: info@cancercare.org Internet: http://www.cancercare.org Cancer Hope Network Phone: 877-HOPENET (467-3638) or 908-879-4039 (New Jersey residents) Email: info@cancerhopenetwork.org Internet: http://www.cancerhopenetwork.org
140
Gastroenterology Reference Guide
National Cancer Institute Phone: 800-4-CANCER (422-6237) or 301-496-6631 TTY: 800-332-8615 Email: cancergovstaff@mail.nih.gov Internet: http://cancer.gov NCIs Facing Forward Series Phone: 888-4-CANCER (422-6237) Internet: www.nci.nih.gov/cancerinfo/life-aftertreatment National Coalition for Cancer Survivorship Phone: 877-NCCS-YES (622-7937) or 301-650-9127 Email: info@canceradvocacy.org Internet: http://www.canceradvocacy.org The Cancer Information Network Internet: http://www.cancerlinksusa.com The Wellness Community Executive Office Phone: 888-793-WELL (793-9355) or 202-659-9709 Email: help@thewellnesscommunity.org Internet: http://www.thewellnesscommunity.org
Chapter 7: Liver Disorders
141
Gastroenterology Reference Guide
Chapter 7: Liver Disorders
REFERENCES
1. Dienstag JL, Isselbacher KJ. Tumors of the liver and biliary tract. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Harrisons Principles of Internal Medicine. 16th ed. New York, NY: McGraw-Hill; 2005:533-536. 2. American Cancer Society: Cancer facts and figures 2007. Available at: http://www.cancer.org/docroot/STT/stt_0.asp. Accessed March 07, 2007. 3. Benson AB III, Curley SA, Sigurdson ER for the National Comprehensive Cancer Network'. NCCN Clinical Practice Guidelines in Oncology'. Hepatobiliary cancers. V.1.2007. Available at: http://www.nccn.org/ professionals/physician_gls/PDF/hepatobiliary.pdf. Accessed March 6, 2007. 4. Daniele B, Bencivenga A, Megna AS, et al. Alpha-fetoprotein and ultrasonography screening for hepatocellular carcinoma. Gastroenterology. 2004;127(Suppl 1):S108-S112. 5. Zhou L, Liu J, Luo F. Serum tumor markers for detection of hepatocellular carcinoma. World J Gastroenterol. 2006;12:1175-1181
142
Gastroenterology Reference Guide
Part 2: Gastroenterology Test Listing
PART 2. GASTROENTEROLOGY TEST LISTING
143
Gastroenterology Reference Guide
144
Gastroenterology Reference Guide
Table 1: Food Allergens Table 1a Alphabetical by Allergen
Food Almond Alpha-lactalbumin Apple Apricot Asparagus Avocado Banana Barley Basil Beef Beta-lactoglobulin Black pepper Blackberry Blue mussel Blueberry Brazil nut Broccoli Buckwheat Cabbage Carrot Casein Cashew nut Cauliflower Celery Cheddar cheese Cheese, mold type Cherry Chestnut Chicken meat Chili pepper Cinnamon Phadia Code f20 f76 f49 f237 f261 f96 f92 f6 f269 f27 f77 f280 f211 f37 f288 f18 f260 f11 f216 f31 f78 f202 f291 f85 f81 f82 f242 f299 f83 f279 f220 Test Code 2820 2851 2849 2563 2626 8928 8926 2806 2564 2827 2852 2561 2630 2837 2568 2818 2631 2811 2632 2831 2853 2608 2635 2860 2858 2859 2609 2636 2857 2610 2637
Table 1b By Phadia Code
Phadia Code f1 f2 f3 f4 f5 f6 f7 f8 f9 f10 f11 f12 f13 f14 f15 f17 f18 f20 f23 f24 f25 f26 f27 f31 f33 f35 f36 f37 f40 f41 f44 Food Egg white Milk Codfish Wheat Rye Barley Oat Corn Rice Sesame seed Buckwheat Pea Peanut Soybean White bean Hazel nut Brazil nut Almond Crab Shrimp Tomato Pork Beef Carrot Orange Potato Coconut Blue mussel Tuna Salmon Strawberry Test Code 2801 2802 2803 2804 2805 2806 2807 2808 2809 2810 2811 2812 2813 2814 2815 2817 2818 2820 2823 2824 2825 2826 2827 2831 2833 2835 2836 2837 2840 2841 2844
Part 2: Gastroenterology Test Listing
145
Gastroenterology Reference Guide
Table 1a Alphabetical (cont.)
Food Clam Cocoa Coconut Codfish Coffee Corn Crab Cucumber Egg mix Egg white Egg yolk Eggplant Garlic Ginger Gluten Goat milk Grape Grapefruit Green bean Green pepper Halibut Hazel nut Honey Kiwi fruit Lamb Lemon Lentils Lettuce Lime Lobster Mackerel Malt Phadia Code f207 f93 f36 f3 f221 f8 f23 f244 f245 f1 f75 f262 f47 f270 f79 f300 f259 f209 f315 f263 f303 f17 f247 f84 f88 f208 f235 f215 f306 f80 f206 f90 Test Code 8929 2875 2836 2803 2915 2808 2823 2639 2919 2801 2856 2642 2847 2644 2854 2922 2675 2923 2680 2931 2998 2817 8930 2884 2888 2708 3010 2862 2709 2855 2713 2863
Table 1b By Phadia Code (cont.)
Phadia Code f45 f47 f48 f49 f54 f75 f76 f77 f78 f79 f80 f81 f82 f83 f84 f85 f86 f87 f88 f89 f90 f91 f92 f93 f94 f95 f96 f201 f202 f203 f204 f206 Food Yeast Garlic Onion Apple Sweet potato Egg yolk Alpha-lactalbumin Beta-lactoglobulin Casein Gluten Lobster Cheddar cheese Cheese, mold type Chicken meat Kiwi fruit Celery Parsley Melons Lamb Mustard Malt Mango fruit Banana Cocoa Pear Peach Avocado Pecan nut Cashew nut Pistachio Trout Mackeral Test Code 2845 2847 2848 2849 2555 2856 2851 2852 2853 2854 2855 2858 2859 2857 2884 2860 2861 2887 2888 2889 2863 23860 8926 2875 8884 8405 8928 2864 2608 2726 3063 2713
146
Gastroenterology Reference Guide
Table 1a Alphabetical (cont.)
Food Mandarin Mango fruit Melons Milk Milk, boiled Mushroom Mustard Nutmeg Oat Onion Orange Oregano Oyster Papaya Paprika Parsley Passion fruit Pea Peach Peanut Pear Pecan nut Pine nut Pineapple Pistachio Plum Poppy seed Pork Potato Rabbit Rice Rye Phadia Code f302 f91 f87 f2 f231 f212 f89 f282 f7 f48 f33 f283 f290 f293 f218 f86 f294 f12 f95 f13 f94 f201 f253 f210 f203 f255 f224 f26 f35 f213 f9 f5 Test Code 2714 23860 2887 2802 3044 8931 2889 2718 2807 2848 2833 3045 8932 2720 3047 2861 2724 2812 8405 2813 8884 2864 2725 3048 2726 2728 3050 2826 2835 2730 2809 2805
Table 1b By Phadia Code (cont.)
Phadia Code f207 f208 f209 f210 f211 f212 f213 f214 f215 f216 f218 f220 f221 f222 f224 f231 f234 235 f237 f242 f244 f245 f247 f253 f255 f256 f258 f259 f260 f261 f262 f263 Food Clam Lemon Grapefruit Pineapple Blackberry Mushroom Rabbit Spinach Lettuce Cabbage Paprika Cinnamon Coffee Tea Poppy seed Milk, boiled Vanilla Lentils Apricot Cherry Cucumber Egg mix Honey Pine nut Plum Walnut Squid Grape Broccoli Asparagus Eggplant Green pepper Test Code 8929 2708 2923 3048 2630 8931 2730 3054 2862 2632 3047 2637 2915 6805 3050 3044 3244 3010 2563 2609 2639 2919 8930 2725 2728 3489 2745 2675 2631 2626 2642 2931
Part 2: Gastroenterology Test Listing
147
Gastroenterology Reference Guide
Table 1a Alphabetical (cont.)
Food Salmon Scallop Sesame seed Shrimp Soybean Spinach Squid Strawberry Sweet potato Swordfish Tea Tomato Trout Tuna Vanilla Walnut Wheat White bean Yeast Phadia Code f41 f338 f10 f24 f14 f214 f258 f44 f54 f312 f222 f25 f204 f40 f234 f256 f4 f15 f45 Test Code 2841 273 2810 2824 2814 3054 2745 2844 2555 3055 6805 2825 3063 2840 3244 3489 2804 2815 2845
Table 1b By Phadia Code (cont.)
Phadia Code f269 f270 f279 f280 f282 f283 f288 f290 f291 f293 f294 f299 f300 f302 f303 f306 f312 f315 f338 Food Basil Ginger Chili pepper Black pepper Nutmeg Oregano Blueberry Oyster Cauliflower Papaya Passion fruit Chestnut Goat milk Mandarin Halibut Lime Swordfish Green bean Scallop Test Code 2564 2644 2610 2561 2718 3045 2568 8932 2635 2720 2724 2636 2922 2714 2998 2709 3055 2680 273
148
Gastroenterology Reference Guide
Table 14. Food Allergy Profile, Adult (test code 10715)
States 50 States Test f1 f2 f3 f4 f8 f13 f14 f24 f207 f256 f338
*Additional Food offerings can be found on page 00
Prevalent Test Allergens* Egg white Milk Codfish Wheat Corn Peanut Soybean Shrimp Clam Walnut Scallop
Part 2: Gastroenterology Test Listing
Test Code
10715
149
Gastroenterology Reference Guide
Acid Fast Stain
4503X
CPT Code(s): 87206 Preferred Specimen(s) Raw specimens as recommended for Mycobacterium culture. Specimens should be delivered to the laboratory within one day of collection. Transport Container Slide carrier or sterile plastic screw-cap container Transport Temperature Slides: Room temperature Raw specimen: Refrigerated (cold packs) Reject Criteria Raw specimens greater than 5 days old Pooled specimens Blood in EDTA (lavender-top) tube Specimens in formalin Methodology Decontamination and concentration as needed and microscopic examination by fluorochrome stain (auramine rhodamine) Clinical Significance Positive smears indicate the presence of acid fast organisms
Instructions Collect fresh stool in sterile, leak-proof container without media, preservative or metal ion. For patients requiring the use of diapers, first line the diaper with clean plastic to prevent absorption. Then transfer 2 grams or 2 mL of the stool specimen from the plastic lined diaper to the sterile container. Do not submit the diaper itself. Cap securely. Do not use M4 transport media. Do not use any preservative, media or additive. Transport Container Plastic screw-cap container Transport Temperature Refrigerated (cold packs) Shipping frozen acceptable Reject Criteria Received room temperature Methodology Enzyme Immunoassay (EIA)
Alanine Aminotransferase (ALT)
CPT Code(s): 84460 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Anticoagulants other than heparin Methodology Spectrophotometry Reference Range(s)
823X
Adenovirus Antibody
686X
CPT Code(s): 86603 Preferred Specimen(s) 1 mL serum Instructions Clinical interpretation of complement fixation test results requires comparison of an acute serum sample to a convalescent serum sample. The convalescent sample should be obtained 2-3 weeks later. The acute sample should be stored at (or below) 4 C until the convalescent sample is obtained. Both samples should be submitted together for testing, clearly identified and dated. Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Reject Criteria Hemolysis Methodology Complement Fixation (CF) Reference Range(s) Serum <8 Clinical interpretation of complement fixation test results requires comparison of an acute serum sample to a convalescent serum sample. The convalescent sample should be obtained 2-3 weeks later. The acute sample should be stored at (or below) 4 C until the convalescent sample is obtained. Both samples should be submitted together for testing, clearly identified and dated. A four-fold rise in titer during convalescence is indicative of recent infection. Clinical Significance Adenovirus causes respiratory tract infections, conjunctivitis, and diarrhea. Infections are most common in individuals who are immunocompromised and in young children. A four-fold rise in titer during convalescence is indicative of recent infection.
<1 Month 1-11 Months 1-3 Years 4-12 Years 13-15 Years 16-19 Years 20 Years
Male 3-25 U/L 4-35 U/L 5-30 U/L 8-30 U/L 7-32 U/L 8-46 U/L 9-60 U/L
Female 3-25 U/L 3-30 U/L 5-30 U/L 8-24 U/L 6-19 U/L 5-32 U/L 6-40 U/L
Clinical Significance Alanine aminotransferase (ALT) measurements are useful in the diagnosis and treatment of heart disease and certain liver diseases, e.g., viral hepatitis and cirrhosis. ALT activity in tissue is generally much lower than aspartate aminotransferase (AST) activity and is found in highest concentrations in the liver. Significant elevations of ALT occur only in diseases of the liver. ALT is often measured in conjunction with AST to determine whether the source of the AST is the liver or the heart. ALT is normally not elevated in cases of myocardial infarction, i.e., a normal ALT, in conjunction with an elevated AST, tends to suggest cardiac disease. However, slight elevations of ALT may occur if an infarct destroys a very large volume of heart muscle.
Adenovirus Antigen Detection, Gastroenteritis, EIA 38945X
CPT Code(s): 87301 Preferred Specimen(s) 2 grams fresh stool
150
Gastroenterology Reference Guide
Albumin
223X
CPT Code(s): 82040 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Hemolysis Methodology Spectrophotometry Reference Range(s) 3.6-5.1 g/dL Clinical Significance Serum albumin measurements are used in the monitoring and treatment of numerous diseases involving primarily the liver and kidney. Its main value lies in the follow-up therapy where improvement in the serum albumin level is the best sign of successful medical treatment. There may also be a loss of albumin in the gastrointestinal tract, in the urine by the damaged kidney or direct loss of albumin through the skin. More than 50% of patients with gluten enteropathy have depressed albumin. The only cause of increased albumin is dehydration; there is no naturally occurring hyperalbuminemia.
Alkaline Phosphatase Isoenzymes
231X
Part 2: Gastroenterology Test Listing
CPT Code(s): 84075, 84080 Includes Alkaline Phosphatase, Intestinal Isoenzymes, Bone Isoenzymes, Liver Isoenzymes, Placental Isoenzymes, Macrohepatic Isoenzymes Patient Preparation Overnight fasting is preferred Preferred Specimen(s) 2 mL serum Instructions Centrifuge within 30 minutes of collection. Transfer serum to a clean plastic transfer vial and freeze immediately. Must note patients age and sex on requisition. Results are sex and age specific. Transport Container Plastic screw-cap vial Transport Temperature Frozen Clinical Significance When the Total Alkaline Phosphatase activity is increased, the Isoenzymes may be useful in determining the source of the increased activity
Alkaline Phosphatase
CPT Code(s): 84075 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Hemolysis Anticoagulants other than heparin Methodology Spectrophotometry Reference Range(s)
234X
Alpha-Fetoprotein (AFP) and AFP-L3
CPT Code(s): 82105 Preferred Specimen(s) 1.5 mL serum Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Methodology Liquid-phase Binding Assay System Reference Range(s) AFP AFP-L3
19529X
1.6-4.5 ng/mL 0.5-9.9 %
<1 Month 1-11 Months 1-3 Years 4-6 Years 7-9 Years 10-12 Years 13-15 Years 16-19 Years 20 Years 20-49 Years 50 Years
Male 75-316 U/L 82-383 U/L 104-345 U/L 93-309 U/L 47-324 U/L 91-476 U/L 92-468 U/L 48-230 U/L 40-115 U/L
Female 48-406 U/L 124-341 U/L 108-317 U/L 96-297 U/L 184-415 U/L 104-471 U/L 41-244 U/L 41-176 U/L 33-115 U/L 33-150 U/L
Clinical Significance This assay is intended for use in the assessment of risk for the development of hepatocellular carcinoma (HCC) in patients with chronic liver disease
Clinical Significance Serum alkaline phosphatase levels are of interest in the diagnosis of hepatobiliary disorders and bone disease associated with increased osteoblastic activity. Moderate elevations of alkaline phosphatase may be seen in several conditions that do not involve the liver or bone. Among these are Hodgkins disease, congestive heart failure, ulcerative colitis, regional enteritis, and intra-abdominal bacterial infections. Elevations are also observed during the third trimester of pregnancy.
151
Gastroenterology Reference Guide
Alpha-Fetoprotein, Tumor Marker
237X
CPT Code(s): 82105 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemic EDTA or heparinized plasma Methodology Immunoassay Reference Range(s)
<1 Month 12 Months 3 Years >3 Years
Male 0.5-16387 ng/mL 0.5-28.3 ng/mL 0.5-7.9 ng/mL <6.1 ng/mL
Female 0.5-18964 ng/mL 0.5-77.0 ng/mL 0.5-11.1 ng/mL <6.1 ng/mL
Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemic Methodology Immunofluorescent Assay (IFA) Reference Range(s) ANCA-IBD Screen Negative P-ANCA Titer <1:20 Clinical Significance Testing for anti-neutrophil cytoplasmic antibodies (P-ANCA and/or C-ANCA) has been found to be useful in establishing the diagnosis of suspected vascular diseases (e.g., crescentic glomerulonephritis, microscopic polyarteritis and Churg-Strauss syndrome), bowel disease (Crohns Disease, ulcerative colitis, primary sclerosing cholangitis, and autoimmune hepatitis) as well as with other autoimmune diseases (drug-induced lupus, SLE, Feltys syndrome).
Clinical Significance Elevation of serum AFP above values found in healthy individuals occurs in several malignant diseases, most notably nonseminomatous testicular cancer and primary hepatocellular carcinoma. AFP is not recommended as a screening procedure to detect cancer in the general population.
Antinuclear Antibody Screen, EIA, with Reflex to Titer, IFA 249X
CPT Code(s): 86038 Includes If the Antinuclear Antibodies (ANA) Screen is positive, ANA titer and pattern will be performed at an additional charge (CPT code(s): 86039). Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemic Methodology Screen: Enzyme Immunoassay (EIA) Titer: Indirect Immunofluorescence (IIF) Reference Range(s) ANA Screen
Amylase
243X
CPT Code(s): 82150 Preferred Specimen(s) 1 mL serum Transport Container Red-top tube, serum separator tube (SST), plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Hemolysis Lipemic Methodology Enzymatic Reference Range(s) 21-101 U/L Clinical Significance The major sources of amylase are the pancreas and the salivary glands. The most common cause of elevation of serum amylase is inflammation of the pancreas (pancreatitis). In acute pancreatitis, serum amylase begins to rise within 6-24 hours, remains elevated for a few days and returns to normal in 3-7 days. Other causes of elevated serum amylase are inflammation of salivary glands (mumps), biliary tract disease and bowel obstruction. Elevated serum amylase can also be seen with drugs (e.g., morphine) which constrict the pancreatic duct sphincter preventing excretion of amylase into the intestine.
Negative
Antinuclear Antibodies <1:40 Negative 1:40-1:80 Low antibody level >1:80 Elevated antibody level
Clinical Significance This screening test with reflexive testing to the traditional IFA procedure is useful for the diagnosis of SLE and other autoimmune disorders. The descriptive IFA pattern may suggest a specific disease entity or autoantibodies.
ANCA Inflammatory Bowel Disease with Reflex to Titer 10054X
CPT Code(s): 86021 Includes If the screen is positive, P-ANCA Titer will be performed at an additional charge (CPT code(s): 86021).
152
Gastroenterology Reference Guide
Aspartate Aminotransferase (AST)
CPT Code(s): 84450 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Anticoagulants other than heparin Methodology Spectrophotometry Reference Range(s)
822X
Bilirubin, Fractionated
7286X
CPT Code(s): 82247, 82248 Includes Direct Bilirubin, Indirect Bilirubin (calculated), Total Bilirubin Preferred Specimen(s) 2 mL serum Transport Container Light protected container Transport Temperature Room temperature Reject Criteria Gross hemolysis Anticoagulants other than heparin Methodology Spectrophotometry Reference Range(s) Bilirubin, Direct 0.2 mg/dL
Part 2: Gastroenterology Test Listing
<1 Month 1-11 Months 1-3 Years 4-6 Years 7-19 Years 20-49 Years 20-44 Years 50 Years 45 Years
Male 3-51 U/L 3-65 U/L 3-56 U/L 20-39 U/L 12-32 U/L 10-40 U/L 10-35 U/L
Female 3-49 U/L 3-79 U/L 3-69 U/L 20-39 U/L 12-32 U/L 10-30 U/L 10-35 U/L
Bilirubin, Indirect 1 Day 2 Days 3-5 Days 6 Days-9 Years 10-19 Years 20 Years Bilirubin, Total 1 Day 2 Days 3-5 Days 6 Days-9 Years 10-19 Years 20 Years
5.1 mg/dL (calc) 7.2 mg/dL (calc) 10.3 mg/dL (calc) 0.2-0.8 mg/dL (calc) 0.2-1.1 mg/dL (calc) 0.2-1.2 mg/dL (calc) 5.1 mg/dL 7.2 mg/dL 10.3 mg/dL 0.2-0.8 mg/dL 0.2-1.1 mg/dL 0.2-1.2 mg/dL
Clinical Significance AST is widely distributed throughout the tissues with significant amounts being in the heart and liver. Lesser amounts are also found in skeletal muscles, kidneys, pancreas, spleen, lungs, and brain. Injury to these tissues results in the release of the AST enzyme to the general circulation. In myocardial infarction, serum AST may begin to rise within 6-8 hours after onset, peak within two days and return to normal by the fourth or fifth day post infarction. An increase in serum AST is also found with hepatitis, liver necrosis, cirrhosis, and liver metastasis.
Bilirubin, Direct
285X
CPT Code(s): 82248 Preferred Specimen(s) 1 mL serum Transport Container Amber plastic screw-cap vial or foil-wrapped plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Anticoagulants other than heparin Methodology Spectrophotometry Reference Range(s) 0.3 mg/dL Clinical Significance The assessment of direct bilirubin is helpful in the differentiation of hepatic disorders. The increase in total bilirubin associated with obstructive jaundice is primarily due to the direct (conjugated) fraction. Both direct and indirect bilirubin are increased in the serum with hepatitis.
Clinical Significance The assessment of direct bilirubin is helpful in the differentiation of hepatic disorders. The increase in total bilirubin associated with obstructive jaundice is primarily due to the direct (conjugated) fraction. Both direct and indirect bilirubin are increased in the serum with hepatitis. In the newborn patient with hemolytic jaundice and neonatal jaundice, the increase in the total bilirubin is primarily due to the indirect (unconjugated) bilirubin fraction. This jaundice may be caused by Rh, ABO, or other blood group incompatibilities, by hepatic immaturity, or by hereditary defects in bilirubin conjugation.
153
Gastroenterology Reference Guide
Bilirubin, Fractionated, Pediatric
6631X
CPT Code(s): 82247, 82248 Includes Direct Bilirubin, Indirect Bilirubin (calculated), Total Bilirubin Preferred Specimen(s) 0.3 mL serum - protect from light, avoid hemolysis Transport Container Amber plastic screw-cap vial or foil-wrapped plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Anticoagulants other than heparin Methodology Spectrophotometry Reference Range(s) Bilirubin, Direct 0.3 mg/dL
Reference Range(s) 1 Day 2 Days 3-5 Days 6 Days-9 Years 10-19 Years 20 Years
5.1 mg/dL 7.2 mg/dL 10.3 mg/dL 0.2-0.8 mg/dL 0.2-1.1 mg/dL 0.2-1.2 mg/dL
Clinical Significance Levels of bilirubin are used in the diagnosis and treatment of liver, hemolytic, hematologic, and metabolic disorders, including hepatitis and gallbladder obstructive disease
Bilirubin, Total, Pediatric
20381X
Bilirubin, Indirect 1 Day 2 Day 1 Week 3 Months >3 Months Male >3 Months Female Bilirubin, Total 1 Day 2 Days 1 Week 3 Months >3 Months Male >3 Months Female
6.0 mg/dL (calc) 8.0 mg/dL (calc) 12.0 mg/dL (calc) 1.3 mg/dL (calc) 1.5 mg/dL (calc) 1.3 mg/dL (calc) 0.2-6.0 mg/dL 0.2-8.0 mg/dL 0.2-12.0 mg/dL 0.2-1.3 mg/dL 0.2-1.5 mg/dL 0.2-1.3 mg/dL
CPT Code(s): 82247 Preferred Specimen(s) 0.3 mL serum - protect from light, avoid hemolysis Transport Container Amber plastic screw-cap vial or foil-wrapped plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Anticoagulants other than heparin Received unprotected from light Methodology Spectrophotometry Reference Range(s)
Clinical Significance The assessment of direct bilirubin is helpful in the differentiation of hepatic disorders. The increase in total bilirubin associated with obstructive jaundice is primarily due to the direct (conjugated) fraction. Both direct and indirect bilirubin are increased in the serum with hepatitis. In the newborn patient with hemolytic jaundice and neonatal jaundice, the increase in the total bilirubin is primarily due to the indirect (unconjugated) bilirubin fraction. This jaundice may be caused by Rh, ABO, or other blood group incompatibilities, by hepatic immaturity, or by hereditary defects in bilirubin conjugation.
1 Day 2 Days 3 Days-1 Week 2 Weeks-3 Months 4 Months-2 Years 3 Years
Male 0.2-6.0 mg/dL 0.2-8.0 mg/dL 0.2-12.0 mg/dL 0.2-1.3 mg/dL 0.2-1.5 mg/dL 0.2-1.5 mg/dL
Female 0.2-6.0 mg/dL 0.2-8.0 mg/dL 0.2-12.0 mg/dL 0.2-1.3 mg/dL 0.2-1.3 mg/dL 0.2-1.3 mg/dL
Clinical Significance Elevated in jaundice of the newborn, obstructive jaundice
CA 19-9
4698X
Bilirubin, Total
287X
CPT Code(s): 82247 Preferred Specimen(s) 1 mL serum Transport Container Amber plastic screw-cap vial or foil-wrapped plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Anticoagulants other than heparin Methodology Spectrophotometry
CPT Code(s): 86301 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Methodology Immunoassay Clinical Significance A large percentage of patients with gastrointestinal tumors (such as pancreatic, liver, gastric, colorectal tumors) and some other malignancies have been shown to have elevated serum or plasma CA 19-9 levels. The serum or plasma CA 19-9 levels may be useful for monitoring disease activity predicting relapse following treatment. CA 19-9 should not be used as a screening test.
154
Gastroenterology Reference Guide
CA 19-9, IHC with Interpretation
CPT Code(s): 88342 Preferred Specimen(s) Formalin fixed paraffin embedded tissue Transport Container IHC specimen transport kit Transport Temperature Room temperature Methodology Immunohistochemical Stain
19138X
Clinical Significance Campylobacter is considered a pathogen when isolated from clinical specimens. Its identification is important for control and treatment. Campylobacter jejuni is the most common pathogenic Campylobacter isolated from stool. Other Campylobacter species have also been associated with gastroenteritis.
Part 2: Gastroenterology Test Listing
Carbon Dioxide
310X
CA 72-4
15583X
CPT Code(s): 86316 Preferred Specimen(s) 1 mL serum collected in a red-top tube (no gel) Transport Container Plastic screw-cap vial Transport Temperature Frozen Reject Criteria Fibrotic Highly lipemic Received room temperature Received refrigerated Methodology EIA-Based Fluorescence Reference Range(s) <4 U/mL Clinical Significance Tumor Associated Glycoprotein (Tag) 72 is a high-molecular weight, mucin-like complex which is predominantly expressed in malignant tumors. It has been found expressed in tissue sections in over 90% of colorectal, gastric and ovarian carcinomas and in approximately 70% of breast carcinomas. Tag-72 has also been found in many other malignancies including non small cell lung carcinoma and pancreatic carcinoma. Tag-72 is found in greatly reduced amounts the most normal adult tissues with the exception of endometrial tissue during the secretory phase.
CPT Code(s): 82374 Preferred Specimen(s) 5 mL whole blood collected in a red-top, gel barrier tube and spun - Do not open tube Instructions Centrifuge 30 minutes after drawing Transport Container 1 full, unopened spun gel barrier tube Transport Temperature Room temperature Reject Criteria Hemolysis Plasma Methodology Spectrophotometry Reference Range(s) 21-33 mmol/L Clinical Significance Measurements are used in the diagnosis and treatment of numerous potentially serious disorders associated with changes in body acid-base balance
CBC (includes Differential and Platelets) 6399X
CPT Code(s): 85025 or if manual differential is performed, 85025 will be changed to 85027 and 85007. Includes WBC, RBC, Hemoglobin, Hematocrit, MCV, MCH, MCHC, RDW, Platelet Count, MPV and Differential.If abnormal cells are noted on a manual review of the peripheral blood smear or if the automated differential information meets specific criteria, a full manual differential will be performed at an additional charge. Preferred Specimen(s) Whole blood full EDTA (lavender-top) tube Instructions Maintain specimen at room temperature. If multiple draw, collect EDTA (lavender-top) tube last. Traumatic tap can introduce thromboplastin and trap WBC and platelets. Refrigeration can precipitate fibrin and trap WBC and platelets. Do not refrigerate. Transport Container EDTA (lavender-top) tube Transport Temperature Room temperature Reject Criteria Hemolysis Clotted Received frozen Methodology Electronic Cell Sizing, Sorting/Cytometry/Microscopy Reference Range(s) See Medical Report Clinical Significance A complete blood count is used as a screening test for various disease states including anemia, leukemia and inflammatory processes
Campylobacter, Culture
4475X
CPT Code(s): 87046 Includes If culture is positive, identification will be performed at an additional charge (CPT code(s): 87077 or 87147 or 87143 or 87149 or 87140). Preferred Specimen(s) Stool submitted in Cary-Blair stool culture transport medium Instructions Cary-Blair transport (or appropriate stool transport medium). Fluid level should reach line on vial. Transport Container Cary-Blair stool culture transport medium Transport Temperature Room temperature. Do not refrigerate Reject Criteria Unpreserved, at any temperature Frozen specimens in Cary-Blair transport medium Expired transport medium Specimen in diaper or parasitology transport vials Methodology Bacterial culture Aerobic isolation and identification procedures Antibiotic susceptibility testing (when appropriate)
155
Gastroenterology Reference Guide
CD117 (c-kit), IHC with Interpretation
11230X
Celiac Disease Comprehensive Panel with Reflex 15981X
CPT Code(s): 83516 (x2), 82784 Includes Tissue Transglutaminase IgA, Gliadin Antibody IgA, and Total IgA, Serum
CPT Code(s): 88342 This test was developed and its performance characteristics have been determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) Formalin-fixed paraffin embedded tissue block Transport Container IHC specimen transport kit Transport Temperature Room temperature Reject Criteria Received frozen Methodology Immunohistochemistry (IHC) Clinical Significance Testing for CD117/c-kit expression may be a useful tool for the identification of several malignant neoplasma expressing c-kit, including gastrointestinal stromal tumors (GISTS), mast cell diseases, acute myeloid leukemia (AML), small cell lung carcinoma (SCLC), and Ewings sarcoma. It may also aid in differentiating gastrointestinal stromal tumors (GISTS) from other intra-abdominal mesenchymal tumors. Recent studies have indicated that the tyrosine kinase inhibitor, STI571 (Gleevac), may be effective in treating CD117/c-kit positive tumors. Therefore, testing tumors for CDcd117/c-kit immunoreactivity can assist in both diagnosis and the prediction of drug sensitivity to tyrosine kinase inhibitor STI571 treatment.
If the Tissue Transglutaminase IgA is positive, Endomysial Antibody Screen (IgA) will be performed at an additional charge (CPT code(s): 86255) and, if appropriate, Endomysial Antibody Titer (CPT code(s): 86256) will be performed at an additional charge. If the Total IgA is less than 11 mg/dL then, Tissue Transglutaminase IgG will be performed at an additional charge (CPT code(s): 83516). Preferred Specimen(s) 5 mL serum Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Methodology Immunoassay Immunofluorescence Assay (IFA) Immunoturbidometry Clinical Significance This panel assists in differentiating celiac disease from other inflammatory bowel diseases and helps avoid progression of celiac disease, particularly in children, through early identification of gluten sensitivity.
Celiac Disease Panel
15980X
CEA
978X
CPT Code(s): 82378 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Note: Room temperature acceptable if received within 24 hours of collection. Frozen acceptable. Methodology Immunoassay Reference Range(s) Non-Smoker Smoker
<2.5 ng/mL <5.0 ng/mL
CPT Code(s): 82784, 83516 (x2) Includes Tissue Transglutaminase IgA, Total IgA, Gliadin Antibody IgA Preferred Specimen(s) 2 mL serum Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Methodology Immunoassay Immunoturbidometry Clinical Significance Patients with celiac disease display a hypersensitivity to gluten (wheat) in their diet. This panel helps differentiate patients with celiac disease from patients with other inflammatory bowel diseases.
Clinical Significance Increased serum CEA levels have been detected in persons with primary colorectal cancer and in patients with other malignancies involving the gastrointestinal tract, breast, lung, ovarian, prostatic, liver and pancreatic cancers. Elevated serum CEA levels have also been detected in patients with nonmalignant disease, especially patients who are older or who are smokers. CEA levels are not useful in screening the general population for undetected cancers. However, CEA levels provide important information about patient prognosis, recurrence of tumors after surgical removal, and effectiveness of therapy.
156
Gastroenterology Reference Guide
Celiac Disease Panel without Gliadin 17612X
CPT Code(s): 82784, 83516 Includes IgA, Total, Tissue Transglutaminase Antibody, IgA Preferred Specimen(s) 5 mL serum Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Methodology Immunoassay Immunofluorescence Assay (IFA) Immunoturbidometry Reference Range(s) See individual analytes Clinical Significance This panel assists in differentiating celiac disease from other inflammatory bowel diseases and helps avoid progression of celiac disease, particularly in children, through early identification of gluten sensitivity.
Transport Temperature Room temperature Reject Criteria Gross hemolysis Plasma Methodology Ion Selective Electrode (ISE) Reference Range(s) 98-110 mmol/L Clinical Significance Serum chloride is the major extracellular anion and counter-balances the major cation, sodium, maintaining electrical neutrality of the body fluids. Two thirds of the total anion concentration in extracellular fluids is chloride and it is significantly involved in maintaining proper hydration and osmotic pressure. Movement of chloride ions across the red blood cell membrane is essential for the transport of bicarbonate ions in response to changing concentrations of carbon dioxide. Chloride measurements are used in the diagnosis and treatment of electrolyte and metabolic disorders such as cystic fibrosis and diabetic acidosis.
Part 2: Gastroenterology Test Listing
Cholesterol, Total
CPT Code(s): 82465 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Anticoagulants other than heparin Methodology Spectrophotometry Reference Range(s) <20 Years 20 Years
334X
Ceruloplasmin
CPT Code(s): 82390 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Methodology Nephelometry Reference Range(s)
326X
Age 30 Days 11 Months 3 Years 6 Years 9 Years 12 Years 15 Years 18 Years >18 Years
Male 8-25 mg/dL 15-48 mg/dL 25-56 mg/dL 29-56 mg/dL 25-52 mg/dL 21-51 mg/dL 20-50 mg/dL 20-45 mg/dL 18-36 mg/dL
Female 3-28 mg/dL 15-43 mg/dL 29-54 mg/dL 26-54 mg/dL 23-48 mg/dL 21-48 mg/dL 21-46 mg/dL 22-50 mg/dL 18-53 mg/dL
125-170 mg/dL 125-200 mg/dL
Clinical Significance Total cholesterol, in conjunction with LDL and HDL cholesterol and triglyceride determination, provide valuable information for the risk of coronary artery disease. Total serum cholesterol analysis is useful in the diagnosis of hyperlipoproteinemia, atherosclerosis, hepatic and thyroid diseases.
Clinical Significance Decreased levels of ceruloplasmin are found in Wilsons Disease, fulminant liver failure, intestinal malabsorption, renal failure resulting in proteinuria, chronic active hepatitis and malnutrition. Elevated levels are found in primary biliary cirrhosis, pregnancy (first trimester), oral contraceptive use and in acute inflammatory conditions since ceruloplasmin is an acute phase reactant.
Chloride
CPT Code(s): 82435 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial
330X
157
Gastroenterology Reference Guide
Clostridium difficile Culture, with Reflex to Toxin 4407X
CPT Code(s): 87081 Includes If culture is positive, identification and toxin studies will be performed at an additional charge: Identification (CPT code(s): 87076 or 87140 or 87143 or 87149); Toxin Studies (CPT code(s): 87158). Antibiotic susceptibilities are only performed when appropriate (CPT code(s): 87181, 87184, 87185, 87186). Preferred Specimen(s) 5 grams or 5 mL stool Transport Container Anaerobic transport vial or swab, stool in clean leak-proof container Transport Temperature Raw stool: Refrigerated (cold packs) Anaerobic transport device: Room temperature Reject Criteria Raw stool received at room temperature Specimens from children less than 1 year of age Specimens exceeding stability Specimens in expired transport media Specimens in non-bacteriological transport media Methodology Bacterial culture, anaerobic Routine isolation and identification techniques Toxin (EIA) assay testing performed on all isolates of C. difficile Clinical Significance Clostridium difficile has been associated with lower gastrointestinal complications of antimicrobial therapy.
Reject Criteria Swabs and samples submitted in stool transport media Methodology Tissue Culture, Neutralization of Cytopathic Effect of Clostridium difficile Cytotoxin Clinical Significance Clostridium difficile has been associated with lower gastrointestinal complications of antimicrobial therapy. The tissue culture assay for detecting cytotoxin (toxin B) is the standard reference method for the laboratory diagnosis of C. difficile-associated disease.
Comprehensive Metabolic Panel with Glomerular Filtration Rate, Estimated (eGFR) 10231X
CPT Code(s): 80053 Includes Albumin, Albumin/Globulin Ratio (calculated), Alkaline Phosphatase, ALT, AST, BUN/Creatinine Ratio (calculated), Calcium, Carbon Dioxide, Chloride, Creatinine, GFR Estimated, Globulin (calculated), Glucose, Potassium, Sodium, Total Bilirubin, Total Protein, Urea Nitrogen Patient Preparation Fasting specimen Preferred Specimen(s) 2 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Hemolysis Methodology See individual analytes Reference Range(s) See individual analytes
Clostridium difficile Toxin A and B, EIA 37212X
CPT Code(s): 87324 Preferred Specimen(s) 5 grams (5 mL) stool Transport Container Clean plastic screw-cap, leak-proof container Transport Temperature Refrigerated (cold packs) Reject Criteria Stools submitted in transport media or swab Unfrozen stools greater than 72 hours old Methodology Immunoassay Clinical Significance This test offers maximum sensitivity as it detects both toxin A and toxin B produced by C. difficile. Clostridium difficile has been associated with colitis secondary to antimicrobial therapy.
C-Reactive Protein (CRP)
4420X
Clostridium difficile Toxin B Screen
4408X
CPT Code(s): 87230 Preferred Specimen(s) 3 grams or 3 mL feces (single or multiple freshly passed fecal specimens) Transport Container Plastic screw-cap, leak-proof container Transport Temperature Frozen preferred
CPT Code(s): 86140 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Lipemia Methodology Nephelometry Clinical Significance Increased CRP levels are found in inflammatory conditions including: bacterial infection, rheumatic fever, active arthritis, myocardial infarction, malignancies and in the post-operative state. This test cannot detect the relatively small elevations of CRP that are associated with increased cardiovascular risk.
158
Gastroenterology Reference Guide
Creatinine with Glomerular Filtration Rate, Estimated (eGFR) 375X
CPT Code(s): 82565 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Hemolysis Plasma Methodology Spectrophotometry Reference Range(s)
Culture, Stool (Salmonella and Shigella) 10019X
Part 2: Gastroenterology Test Listing
Creatinine Female Male GFR Estimated Female Male
0.5-1.2 mg/dL 0.5-1.3 mg/dL 60 mL/min/1.73m2 60 mL/min/1.73m2
Clinical Significance Serum creatinine is useful in the evaluation of kidney function and in monitoring renal dialysis. A serum creatinine result within the reference range does not rule out renal function impairment: serum creatinine is not sensitive to early renal damage since it varies with age, gender and ethnic background. The impact of these variables can be reduced by an estimation of the glomerular filtration rate using an equation that includes serum creatinine, age and gender.
CPT Code(s): 87045 Includes If culture is positive, identification will be performed at an additional charge (CPT code(s): 87077and/or 87147 or 87140 or 87143 or 87149). Antibiotic susceptibilities are only performed when appropriate (CPT code(s): 87181 or 87184 or 87185 or 87186). Preferred Specimen(s) Stool submitted in Cary-Blair stool culture transport medium Transport Container Cary-Blair transport vial Transport Temperature Room temperature. Do not refrigerate. Reject Criteria Unpreserved, at any temperature Frozen specimens in Cary-Blair transport medium Expired transport medium Specimen in diaper or parasitology transport vial Methodology Bacterial culture. Aerobic routine isolation and identification procedures. Antibiotic susceptibility testing (when appropriate). Clinical Significance Salmonella and shigella are considered pathogens when isolated from clinical specimens. Identification of these organisms is important for treatment and infection control.
Culture, Stool (Salmonella/Shigella/ Campylobacter) 10045X
CPT Code(s): 87045, 87046 Includes If culture is positive, identification will be performed at an additional charge (CPT code(s): 87077 and/or 87147 or 87140 or 87143 or 87149). Antibiotic susceptibilities are only performed when appropriate (CPT code(s): 87181 or 87184 or 87185 or 87186). Preferred Specimen(s) Stool submitted in Cary-Blair stool culture transport medium Transport Container Cary-Blair transport (or appropriate stool transport medium) Transport Temperature Room temperature. Do not refrigerate Reject Criteria Unpreserved, at any temperature Frozen specimens in Cary-Blair transport medium Expired transport medium Specimen in diaper or parisitology transport vials Methodology Bacterial culture. Aerobic isolation and identification procedures. Antibiotic susceptibility testing (when appropriate).
Cryptosporidium Antigen, Stool
37213X
CPT Code(s): 87015, 87272 Includes Concentration and Cryptosporidium antigen Preferred Specimen(s) 5 grams (5 mL) stool Instructions Transfer stool within 30 minutes of collection into formalin vial. Fill to the line on the transport vial. Transport Container 10% formalin transport vial Transport Temperature Room temperature Reject Criteria Unpreserved stool Stool in polyvinyl alcohol (PVA) Received frozen Raw stool Methodology Fluorescent Microscopy Clinical Significance Cryptosporidiosis is a disease which produces watery diarrhea and which can be life threatening in immunosuppressed patients.
159
Gastroenterology Reference Guide
Culture, Viral, Comprehensive
689X
CPT Code(s): 87252 Preferred Specimen(s) Respiratory tract specimens, lesion swabs, stool, CSF, body fluids, tissues or urine in VCM medium or microtest (M4) microbe transport (blue-cap/label) tube, or equivalent. Instructions Use only Dacron or rayon-tipped swabs with plastic or metal shafts for specimen collection. Whole blood and bone marrow must be submitted in a sodium heparin (green-top) tube, not in M4. Do not freeze blood. Transport Container Respiratory tract specimens, lesion swabs, tissues or stool: Submit in VCM or M4 (blue-cap/label) transport vial. CSF and Body fluids: Submit in an equal volume of VCM or blue-cap M4 medium or in a sterile tube with a leak-proof cap. Transport Temperature Refrigerated (cold packs) Reject Criteria Wooden shaft and calcium alginate swabs Dry swabs Transwabs or swabs in bacterial gel based transport medium DNA probe transports Tissues in formalin or other fixatives Transports for antigen detection by EIA Received room temperature or refrigerated specimens more than 3 days old Methodology Tissue culture Clinical Significance Viral isolation in tissue culture remains the most sensitive method or Gold Standard for the detection of many common viruses. Successful isolation depends on the selection of the appropriate cell lines based on provisional diagnosis or symptoms and source of infection.
Dihydropyrimidine Dehydrogenase (DPD) Gene Mutation Analysis 15538X
CPT Code(s): 83891, 83896 (x2), 83898, 83908, 83912 This test was developed and its performance characteristics have been determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 5 mL whole blood collected in an EDTA (lavender-top) or ACD solution B (yellow-top) tube Instructions Whole blood: Normal phlebotomy procedure. Specimen stability is crucial. Store and ship ambient immediately. Do not freeze. Transport Container EDTA (lavender-top) tube Transport Temperature Room temperature Reject Criteria Received frozen Methodology Polymerase Chain Reaction (PCR) Oligonucleotide hybridizations Chemiluminescent detection Clinical Significance Partial or complete deficiency of DPD activity has been associated with an increased risk for severe adverse reactions when treated with pyrimidine-based chemotherapeutic agents, such as 5-fluorouracil (5-FU). This test can also be used to confirm the clinical diagnosis of dihydropyrimidine dehydrogenase (DPD) deficiency in affected patients and for the detection of the IVS14 + 1GA mutation in asymptomatic carriers.
Cyclospora and Isospora Examination
10018X
E. coli 0157 Culture
8631X
CPT Code(s): 87015, 87207 Includes Cyclospora Examination, Isospora Examination, Concentration. Preferred Specimen(s) 5 grams (5 mL) stool. Transfer stool within 30 minutes of collection into formalin vial. Fill to the line on the transport vial. Transport Container 10% formalin transport vial Transport Temperature Room temperature Reject Criteria Unpreserved stool Methodology Microscopic exam of modified acid fast stain Clinical Significance Cyclospora cayetanensis and Isospora belli are coccidian parasites which cause malaise, low grade fever, and diarrhea. Fatigue, anorexia, vomiting, myalgia and weight loss occur. The clinical presentation for those patients infected with either disease is similar.
CPT Code(s): 87046 Preferred Specimen(s) Fresh stool in Cary-Blair transport Transport Container Stool transport tube-modified Cary-Blair Transport Temperature Room temperature Reject Criteria Raw stool not in transport tube Received refrigerated Received frozen Methodology Conventional Culture Reference Range(s) None isolated Clinical Significance Infection by Shiga toxin producing Escherichia coli (STEC) can cause self-limiting diarrhea due to hemolytic uremic syndrome (HUS). Serotype 0157: H7, the most frequently isolated, has been isolated in large food outbreaks and sporadic cases.
160
Gastroenterology Reference Guide
Endomysial Antibody Screen (IgA) with Reflex To Titer 15064X
CPT Code(s): 86255 Includes If the Endomysial Antibody Screen (IgA) is abnormal, Endomysial Antibody Titer is performed at an additional charge (CPT: 86256). Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Methodology Immunofluorescence Assay (IFA) Reference Range(s) Negative Clinical Significance A positive IgA endomysial antibody result supports the diagnosis of celiac disease
Methodology Immunohistochemistry (IHC)
Part 2: Gastroenterology Test Listing
Fecal Globin by Immunochemistry (InSure) 11290X
CPT Code(s): 82274 Patient Preparation No special diet or avoidance of drugs or supplements is required for the InSuretest Preferred Specimen(s) Fecal specimen collected from toilet water and brushed on the InSure FOBT test card Transport Container InSure FOBT test card Transport Temperature Room temperature Reject Criteria Stool submitted in any container InSure FOBT cards with stool applied to the sample windows will be rejected Any test card with obvious blood present Methodology Immunochromatography Clinical Significance The fecal occult blood test is an immunochromatographic fecal occult blood test that qualitatively detects human hemoglobin from blood in fecal samples. This is a useful screening aid for detecting primarily lower gastrointestinal (G.I.) disorders that may be related to iron deficiency anemia, diverticulitis, ulcerative colitis, polyps, adenomas, colorectal cancers or other G.I. lesions that can bleed. It is recommended for use by health professionals as part of routine physical examinations and in screening for colorectal cancer or other sources of lower G.I. bleeding.
Entamoeba histolytica Antibody, IgG, EIA 30262X
CPT Code(s): 86753 Preferred Specimen(s) 1 mL serum Instructions Separate serum from cells as soon as possible Transport Container Plastic screw-cap vial Transport Temperature Frozen Reject Criteria Received Room temperature Plasma Methodology Immunoassay Reference Range(s) <0.90 0.90-1.10 >1.10
Negative Equivocal Positive
Clinical Significance Entamoeba histolytica is a parasitic protozoan that can infect the digestive tract and occasionally other tissues. Antibody IgG is useful in differentiating amebiasis from other causes of liver cysts and parasitic infection.
Epidermal Growth Factor Receptor (EGFR), Immunohistochemical Stain 10479X
CPT Code(s): 88342 Preferred Specimen(s) Tissue, formalin fixed, paraffin embedded tissue block Transport Container Formalin Fixed Tissue: Plastic screw-cap container Paraffin Embedded Tissue Block: Paraffin block bag Transport Temperature Room temperature Reject Criteria Received frozen
161
Gastroenterology Reference Guide
Fecal Globin by Immunochemistry (InSure), Medicare 11293X
CPT Code(s): 82274 or HCPCS: G0328 When diagnostic testing for a Medicare Patient is required for Fecal Globin by Immunochemistry (InSure) testing, please order test code 11290, Fecal Globin by Immunochemistry (InSure) Patient Preparation No special diet or avoidance of drugs or supplements is required for the InSure test Preferred Specimen(s) Fecal specimen collected from toilet water and brushed on the InSure FOBT test card Transport Container InSure FOBT test card Transport Temperature Room temperature Reject Criteria Stool submitted in any container InSure FOBT cards with stool applied to the sample windows will be rejected Any test card with obvious blood present Methodology Immunochromatography Clinical Significance The fecal occult blood test is an immunochromatographic fecal occult blood test that qualitatively detects human hemoglobin from blood in fecal samples. This is a useful screening aid for detecting primarily lower gastrointestinal (G.I.) disorders that may be related to iron deficiency anemia, diverticulitis, ulcerative colitis, polyps, adenomas, colorectal cancers or other G.I. lesions that can bleed. It is recommended for use by health professionals as part of routine physical examinations and in screening for colorectal cancer or other sources of lower G.I. bleeding.
Gamma Glutamyl Transferase (GGT)
CPT Code(s): 82977 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Hemolysis Plasma Methodology Spectrophotometry Reference Range(s)
482X
<6 Months 6-11 Months 1-12 Years 13-15 Years 16-19 Years 20-29 Years 30-39 Years 40-54 Years 40-49 Years 50-59 Years 55-59 Years 60 Years
Male 12-122 U/L 39 U/L 3-22 U/L 8-32 U/L 9-31 U/L 3-70 U/L 3-90 U/L 3-95 U/L 3-85 U/L 3-70 U/L
Female 15-132 U/L 39 U/L 3-22 U/L 7-18 U/L 6-26 U/L 3-40 U/L 3-50 U/L 3-55 U/L 3-70 U/L 3-65 U/L
Fecal Leukocyte Stain
3930X
CPT Code(s): 89055 Preferred Specimen(s) Stool in PVA to fill line on collection vial Instructions Mix contents thoroughly until homogenous. Specimens submitted in formalin cannot be processed by this method. Transport Container PVA vial Transport Temperature Room temperature Unpreserved specimens must be refrigerated within 1 hour from the time of collection and transported to the lab within 24 hours Reject Criteria Unpreserved stool more than 24 hours old Stool in Cary-Blair transport medium Received frozen Specimens containing barium or received in preservatives other than PVA Methodology Microscopy Clinical Significance The presence of leukocytes is an indicator of inflammation. Generally, inflammation is a product of bacteria-host interaction.
Clinical Significance Elevated GGT is found in all forms of liver disease. Measurement of GGT is used in the diagnosis and treatment of alcoholic cirrhosis, as well as primary and secondary liver tumors. It is more sensitive than alkaline phosphatase, the transaminases, and leucine aminopeptidase in detecting obstructive jaundice, cholangitis, and cholecystitis. Normal levels of GGT are seen in skeletal diseases; thus, GGT in serum can be used to ascertain whether a disease, suggested by elevated alkaline phosphatase, is skeletal or hepatobiliary.
Giardia Antigen, EIA, Stool
8625X
CPT Code(s): 87329 Preferred Specimen(s) 5 grams (5 mL) stool Instructions Transfer stool within 30 minutes of collection into formalin vial. Fill to the line on the transport vial. Transport Container Formalin transport vial Transport Temperature Specimens in formalin: Room temperature Specimens in Carey Blair: Refrigerated (cold packs) Reject Criteria Specimens in Poly Vinyl Alcohol (PVA) Methodology Immunoassay Clinical Significance A positive giardia antigen test indicates that Giardia lamblia is present. Giardia is considered to be a pathogen when detected in clinical specimens. Its identification is important for control and treatment of giardiasis.
162
Gastroenterology Reference Guide
Giardia/Cryptosporidium Antigen Panel 39480X
CPT Code(s): 87015, 87272, 87329 Includes Concentration Preferred Specimen(s) 5 g stool or 5 mL, preserved in 10% formalin Instructions Transfer stool within 30 minutes of collection into formalin vial. Other acceptable transport media are merthiolate-iodine-formalin (MF) and sodium acetate-acetic acid formalin (SAF). Transport Container Formalin vial Transport Temperature Room temperature Reject Criteria Received in PVA Specimen other than stool Shipping frozen unacceptable Methodology Enzyme Immunoassay (EIA) for Giardia Direct Immunofluorescence Assay (DFA) for Cryptosporidium
Clinical Significance Celiac Disease is characterized by the presence of Gliadin Antibody. Such patients display a hypersensitivity to gluten (wheat) in their diet. The antibody is undetectable when patients with hypersensitivity are placed on gluten-free diets. Antibody IgA is more specific and IgG is a more sensitive assay to Celiac Disease.
Part 2: Gastroenterology Test Listing
Gliadin Antibody Panel (IgG, IgA)
CPT Code(s): 83516 (x2) Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Reject Criteria Gross hemolysis Hyperlipemic Plasma Methodology Enzyme Immunoassay (EIA) Reference Range(s) <11 U/mL 11-17 U/mL >17 U/mL
8889X
Gliadin Antibody (IgA)
CPT Code(s): 83516 Preferred Specimen(s) 1 mL serum Instructions Avoid lipemia Transport Container Sterile screw-cap vial Transport Temperature Refrigerated (cold packs) Reject Criteria Gross hemolysis Lipemic Methodology Immunoassay Reference Range(s) <11 U/mL 11-17 U/mL >17 U/mL
11228X
Negative Equivocal Positive
Clinical Significance Celiac disease is characterized by the presence of Gliadin Antibody. Such patients display a hypersensitivity to gluten (wheat) in their diet. The antibody is undetectable when patients with hypersensitivity are placed on gluten-free diets. Antibody IgA is more specific and IgG is more sensitive to Celiac Disease.
Glypican 3
16157X
Negative Equivocal Positive
Gliadin Antibody (IgG)
11212X
CPT Code(s): 83516 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial, serum separator tube (SST) or red-top tube Transport Temperature Refrigerated (cold packs) Reject Criteria Gross hemolysis Hyperlipemic Plasma Methodology Immunoassay Reference Range(s) <11 U/mL 11-17 U/mL >17 U/mL
CPT Code(s): 83520 This test was performed using a kit that has not been approved or cleared by the FDA. The analytical performance characteristics of this test have been determined by Quest Diagnostics. This test should not be used for diagnosis without confirmation by other medically established means. Preferred Specimen(s) 1 mL serum collected in a no additive (red-top) tube Transport Container No additive (red-top) tube Transport Temperature Frozen Reject Criteria Hemolysis Lipemia Icteric Methodology Immunoassay Reference Range(s) 180 pg/mL Clinical Significance Glypican 3 is a serum biomarker for the early detection of hepatocellular carcinoma. The glypican 3 test is an ELISA-based assay for the quantitative determination of human GPC3 concentration in serum.
Negative Equivocal Positive
163
Gastroenterology Reference Guide
Gram Stain
497X
CPT Code(s): 87205 Preferred Specimen(s) Specimen, any source. Air-dried smear. Instructions Indicate source of specimen on both the test request form and specimen transport device Transport Container Specimen in sterile, leak-proof container or air-dried smear in slide transport device Transport Temperature Room temperature Reject Criteria Broken slide Methodology Gram Stain Microscopy Clinical Significance Varies with source. The gram stain is a critical test for the rapid, presumptive diagnosis of infectious agents and also serves to assess the quality of clinical specimens.
Clinical Significance Colonization with H. pylori is associated with increased risk of patients developing gastritis, peptic ulcer disease, and gastric adenocarcinoma. Antibodies IgG, IgA, and IgM provide higher sensitivity than any single antibody test alone.
Helicobacter pylori Antibody (IgG), Quantitative 29408X
CPT Code(s): 86677 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Reject Criteria Gross hemolysis Methodology Chemiluminescence (CL) Reference Range(s) <0.9 0.9-1.0 >1.0
Helicobacter pylori Antibodies (IgG, IgA) 37695X
CPT Code(s): 86677 (x2) Preferred Specimen(s) 2 mL serum Instructions Sample collected aseptically by venipuncture. Prompt separation of serum from clot to avoid hemolysis. Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Reject Criteria Plasma Methodology Immunoassay Clinical Significance Colonization with H. pylori is associated with increased risk of patients developing gastritis, peptic ulcer disease, and gastric adenocarcinoma. Antibody IgA may be elevated for years in infected individuals.
Negative Equivocal Positive
Clinical Significance A positive serological response to H. pylori antigens has been determined in individuals with duodenitis, chronic gastritis, and gastric or duodenal ulcers. Further, many people without clinical symptoms are seropositive for H. pylori Ab, with the prevalence increasing with age. Therefore, while H. pylori serology is a sensitive method to determine colonization, differentiation between colonization and active disease is not possible.
Helicobacter pylori Antibodies (IgG, IgA, IgM) 20325X
CPT Code(s): 86677 (x3) Preferred Specimen(s) 2 mL serum Instructions Allow specimen to clot at room temperature and then centrifuge. Separate serum from cells as soon as possible. Refrigerate at 2-8 C. Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Reject Criteria Received room temperature Reference Range(s) See individual analytes
164
Gastroenterology Reference Guide
Helicobacter pylori Antigen, EIA, Stool 34838X
CPT Code(s): 87338 Patient Preparation Patient should be off antimicrobials, proton pump inhibitors and bismuth at least two weeks prior to specimen collection.
Note: This assay should be negative four weeks following successful treatment with antibiotics. Preferred Specimen(s) Collect 0.5 mL of semi-solid stool or 20 mm diameter solid stool and transfer to properly labeled sterile, leak-proof container. Do not place stool in preservative, transport media or swab. Watery, diarrheal stool is not acceptable. Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) up to 3 days; frozen if delay exceeds 3 days Reject Criteria Watery, diarrheal stool Stool in preservative, transport media or swab Methodology Immunoassay Reference Range(s) Not detected A result of H. pylori Detected indicates H. pylori antigen is present. A result of Not Detected indicates the absence of H. pylori antigens or the level of antigen is below the sensitivity of the assay. This test result is intended to aid in the diagnosis of H. pylori infection in adult patients. It is also intended to aid in monitoring the efficacy of antimicrobial therapy. The sensitivity and specificity of this test are 96%. In populations with disease prevalence ranging from 34% to 69% (average 52%), the positive and negative predictive values were found to be 96%. The performance characteristics of this assay have not been established for use in individuals younger than 18 years of age, in asymptomatic individuals, or on watery diarrheal stools. Clinical Significance Colonization with H. pylori is associated with increased risk of patients developing gastritis, peptic ulcer disease, and gastric adenocarcinoma. Stool antigen testing provides a sensitive measure of infection including during and after treatment.
Keep each pair of breath samples together reusing the plastic kit pouch provided. Transport Temperature Room temperature Reject Criteria Specimen types other than Breath Tek UBiT bags Specimen from patients <18 years old Methodology Infra-red Spectrophotometry Reference Range(s) Not detected Clinical Significance The urea breath test detects active H. pylori infection and can document post-therapy cure. H. pylori infection can cause chronic gastritis, peptic ulcer disease and gastric cancer.
Part 2: Gastroenterology Test Listing
Helicobacter pylori, Culture
8395X
CPT Code(s): 87081 Includes If culture is positive, identification will be performed at an additional charge (CPT code(s): 87077 or 87140 or 87143 or 87147 or 87149). Preferred Specimen(s) Antral or gastric biopsy Instructions Indicate source of specimen on both requisition and specimen transport device. Transport to the laboratory and culture as soon as possible. Transport Container Sterile leak-proof container with small amount of sterile saline (2 mL or less) Transport Temperature Refrigerated (cold packs) Reject Criteria Stool Methodology Bacterial Culture, Microaerophilic Special Isolation and Identification Procedures Clinical Significance Helicobacter pylori has been identified as a cause of gastroduodenitis, gastric and duodenal ulcers and non-ulcer dyspepsia. H. pylori has also been associated as a co-factor in the development of gastric cancer.
Helicobacter pylori Urea Breath Test, Infra-red (UBiT) 14839X
CPT Code(s): 83013 Patient Preparation Please call laboratory for availability. Patient should fast one hour before collection of baseline breath sample. Patient must be off antibiotics, proton-pump inhibitors (i.e., Prilosec, Nexium, Protonix, Aciphex) and bismuth preparations two weeks prior to administration of test. Pranactin-citric contains a small amount of aspartame sweetener. Test may not be suitable for patients with phenylketonuria whose dietary phenylalanine should be restricted. Preferred Specimen(s) Human breath Paired breath samples (pre and post) collected in Meretek kit bags and must be submitted together. Follow instructions provided with kit. Transport Container Capped blue and pink bags. Bags may leak if cap is not attached.
165
Gastroenterology Reference Guide
Hemoquant, Stool
4947X
CPT Code(s): 84311 Patient Preparation Patient should exclude red meat from the diet for 3 days prior to specimen collection. Preferred Specimen(s) 3 grams of stool from a timed (24, 48, or 72 hour) stool collection
Hepatitis A Antibody, Total with Reflex to IgM 36504X
CPT Code(s): 86708 Includes If Hepatitis A Antibody total is reactive, Hepatitis A IgM Antibody will be performed at an additional charge (CPT code(s): 86709). Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemia Methodology Immunoassay Clinical Significance Hepatitis A Virus (HAV) antibodies indicate prior or acute infection with, or immunization to, Hepatitis A virus.
Special instructions: Record total specimen weight and total collection time on the test requisition and container. Seal container in a plastic bag to avoid leakage and ship frozen. Transport Container Sterile screw-cap container Transport Temperature Frozen Reject Criteria Received thawed Stool specimens received in paint cans Received room temperature Received refrigerated Methodology Conversion of heme to porphyrins Quantitation by fluorometry Clinical Significance Detection of total hemoglobin present in feces is useful in aiding the diagnosis of gastrointestinal ulcers and cancers
Hepatitis A IgM Antibody
512X
Hepatic Function Panel
10256X
CPT Code(s): 80076 Includes Total Protein, Albumin, Globulin (calculated), Albumin/Globulin Ratio (calculated), Total Bilirubin, Direct Bilirubin, Indirect Bilirubin (calculated), Alkaline Phosphatase, AST, ALT Preferred Specimen(s) 2 mL serum Transport Container Serum separator tube or plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Hemolysis Methodology See individual analytes Reference Range(s) See individual analytes
CPT Code(s): 86709 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemia Methodology Immunoassay Clinical Significance IgM antibodies to Hepatitis A suggest a current, acute or recent Hepatitis A infection.
Hepatitis B Core Antibody, Total
501X
Hepatitis A Antibody, Total
CPT Code(s): 86708 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemia Methodology Immunoassay Clinical Significance HAV antibody indicates prior or acute infection with, or immunization to, Hepatitis A virus.
508X
CPT Code(s): 86704 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemia Methodology Immunoassay Clinical Significance This assay does not distinguish between Total B core antibody IgG and IgM detected before or at the onset of symptoms; however, such reactivity can persist for years after illness, and may even outlast anti-HBs. Occasionally Hepatitis B core antibody may be the only marker of either current or past Hepatitis B infection.
166
Gastroenterology Reference Guide
Hepatitis B Core Antibody, Total, with Reflex to IgM 37676X
CPT Code(s): 86704 Includes If Hepatitis B Core Antibody Total is reactive, Hepatitis B Core IgM Antibody will be performed at an additional charge (CPT code(s): 86705). Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Gross lipemia Methodology Immunoassay Clinical Significance Hepatitis B core-specific IgM class antibody has been detected in most acute infections and is a reliable marker for acute disease. In some cases, Hepatitis B core IgM antibody may be the only specific marker for the diagnosis of acute infection with Hepatitis B virus.
10 mIU/mL as per CDC guidelines, please order Hepatitis B Surface Antibody, Quantitative.
Part 2: Gastroenterology Test Listing
Hepatitis B Surface Antibody, Quantitative
8475X
CPT Code(s): 86706 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Sodium citrate (light blue-top) tubes Methodology Immunoassay Reference Range(s) Values 10 mIU/mL indicate immunity Clinical Significance This assay is used to determine immune status for Hepatitis B as 10 mIU/mL as per CDC Guidelines.
Hepatitis B Core IgM Antibody
Hepatitis B Surface Antibody, Quantitative to Endpoint 34000X
CPT Code(s): 86706 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemia Methodology Immunoassay Reference Range(s) Values 10 mIU/mL indicate immunity
4848X
CPT Code(s): 86705 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Gross lipemia Methodology Immunoassay Clinical Significance Hepatitis B core-specific IgM class antibody has been detected in most acute infections and is a reliable marker for acute disease. In some cases, hepatitis B core IgM antibody may be the only specific marker for the diagnosis of acute infection with hepatitis B virus.
Hepatitis B Surface Antibody, Qualitative
499X
CPT Code(s): 86706 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemia Methodology Immunoassay Clinical Significance The detection of anti-HBs is indicative of a prior immunologic exposure to the antigen or vaccine. To determine immune status as
167
Gastroenterology Reference Guide
Hepatitis B Surface Antigen with Reflex Confirmation 498X
CPT Code(s): 87340 Includes Positive samples will be confirmed based on the manufacturers FDA approved recommendations at an additional charge (CPT code(s): 87341).
Note: When only a single test, Hepatitis B Surface Antigen, is ordered to diagnose Hepatitis B in a pregnant woman and the result is positive, additional tests such as liver enzymes should be ordered to confirm the diagnosis. Preferred Specimen(s) 2 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Gross lipemia Methodology Immunoassay Clinical Significance Surface antigen usually appears in the serum after an incubation period of 1 to 6 months following exposure to Hepatitis B virus and peaks shortly after onset of symptoms. It typically disappears within 1 to 3 months. Persistence of Hepatitis B surface antigen for greater than 6 months is a prognostic indicator of chronic Hepatitis B infection.
Methodology Real-Time Polymerase Chain Reaction Reference Range(s) <100 IU/mL (<160 copies/mL) Clinical Significance Chronic carriers will persist in producing detectable HBV. Patients with chronic liver disease of unknown origin most commonly have HBV that is detected by viral DNA testing. Quantitative measurement of HBV viral DNA may be used to monitor progression of disease.
Hepatitis B Virus DNA, Qualitative, PCR 34181X
CPT Code(s): 87516 This test was developed and its performance characteristics determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 2 mL plasma collected in a PPT-Potassium EDTA (white-top) tube Instructions Plasma: Collect blood in sterile tubes containing EDTA anticoagulant, either 0.15% solution v/v final EDTA K3 (standard EDTA tube) or 9 mg spray dried EDTA K2 (plasma preparation tube or PPT tube with plasma separator-gel, preferred). Blood collected in tubes containing ACD anticoagulant are acceptable but will yield results approximately 15% lower when compared to EDTA tubes due to the dilution effect of the 1.5 mL of anticoagulant used in the tube. Blood collected in tubes with heparin anti-coagulant are unsuitable for this test. Store whole blood at room temperature and separate plasma from cells within 2 hours of collection. Transfer plasma to sterile, plastic, screw-capped, aliquot tubes and store at -20 C or colder. Do not clarify plasma by filtration or further centrifugation. Avoid repeated freezing and thawing of specimen. Serum: Collect blood in sterile tube with no anticoagulants, serum separator tubes (SSTs) are recommended. Allow blood to clot at room temperature and separate serum from cells within 2 hours of collection. Transfer serum to sterile plastic screw-capped, aliquot tubes and store at -20 C or colder. Avoid repeated freezing and thawing of specimen. Transport Container Plastic screw-cap vial Transport Temperature Frozen Reject Criteria Received room temperature Methodology Real Time Polymerase Chain Reaction (RT-PCR) Reference Range(s) Not detected Clinical Significance The level of HBV DNA in serum or plasma is thought to reflect more accurately the replicative state of HBV. Concentration of HBV DNA in serum is an excellent indicator of disease status because HBV enters the blood when there is active viral replication in the liver. As chronic hepatitis activity fluctuates, the amount of HBV DNA changes in parallel much more quickly and reliably than do serologic markers. The current qualitative HBV DNA test would also be useful in assessing potential infectivity of problematic cases of donated blood units and for assessing whether asymptomatic chronic carriers are contagious.
Hepatitis B Viral DNA, Quantitative, PCR 8369X
CPT Code(s): 87517 This test was developed and its performance characteristics determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 2 mL plasma collected in a PPT-Potassium EDTA (white-top) tube. Instructions Specimen may be collected in an SST red-top glass tube and transferred to a plastic transport tube for submission to the laboratory. Do not submit glass tubes.
PPT or SST: Separate plasma or serum by centrifugation within 6 hours of collection. Then freeze the plastic PPT or SST tube at -20 C or colder. Ship frozen. EDTA plasma: Separate plasma within 6 hours of collection, transfer plasma to a sterile, screw-capped plastic aliquot tube. Freeze immediately at -20 C. Ship frozen. Serum: Collect blood in a sterile tube without anticoagulant and allow to clot completely. Separate serum from the clot within 6 hours of collection, transfer to a sterile, screw-capped plastic tube. Freeze immediately at -20 C. Ship frozen. Transport Container Plastic screw-cap vial Transport Temperature Frozen Reject Criteria Received room temperature SST (red-top/glass)
168
Gastroenterology Reference Guide
Hepatitis B Virus Genotype
10529X
CPT Code(s): 83891, 83894, 83900, 83904 (x4), 83912 This test was developed and its performance characteristics determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 1 mL plasma collected in a PPT (white-top EDTA) tube Instructions Plasma: Separate plasma from cells by centrifugation within 2 hours and freeze. The PPT tube gel barrier will maintain separation of plasma from cells. Store at -18 C or colder, if necessary.
Reference Range(s) Non-Reactive Clinical Significance Persistence of HBeAg for greater than 6 months is a prognostic indicator of a chronic hepatitis B virus carrier state.
Part 2: Gastroenterology Test Listing
Hepatitis C Antibody
8472X
Serum: Collect blood in sterile tubes with no anticoagulants; plastic serum separator tubes (SSTs) are recommended. Allow blood to clot at room temperature and separate serum from cells within 2 hours of collection. Transfer serum to sterile, plastic screw-capped, aliquot tubes and store at -18 C or colder. Ship frozen. Transport Container PPT (white-top EDTA) tube Transport Temperature Frozen Reject Criteria Received room temperature Received refrigerated Methodology Polymerase Chain Reaction (PCR), Sequencing Reference Range(s) 500 copies/mL
CPT Code(s): 86803 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Gross lipemia Methodology Immunoassay Reference Range(s) Non-Reactive Clinical Significance Hepatitis C Virus (HCV) is the major cause of hepatitis. Approximately 1% of blood donors are seropositive for anti-HCV. The clinical symptoms of a HCV infection are variable. Exposure to HCV results in a chronic infection in 50 to 80% of cases. The window between infection and seroreactivity is highly variable, up to 12 months.
Hepatitis C Antibody Supplemental Testing 8739X
CPT Code(s): 86804 Preferred Specimen(s) 1 mL serum collected in no additive red-top tube Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Methodology RIBA 3.0 Strip Immunoblot Assay (SIA) Reference Range(s) Negative Clinical Significance HCV Antibody Supplemental testing is used as a follow-up to rule out false positive HCV Antibody test results
Hepatitis Be Antibody
556X
CPT Code(s): 86707 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemic Plasma Methodology Immunoassay Reference Range(s) Non-Reactive Clinical Significance Anti-HBe in the blood following exposure to the Hepatitis B virus suggests a good prognosis for patients with Hepatitis B infection.
Hepatitis Be Antigen
CPT Code(s): 87350 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemic Plasma Methodology Immunoassay
555X
169
Gastroenterology Reference Guide
Hepatitis C Antibody with Reflex to HCV RIBA 37677X
CPT Code(s): 86803 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Gross lipemia Methodology Immunoassay Reference Range(s) Non reactive Clinical Significance Hepatitis C Virus (HCV) is the major cause of parenterally transmitted non-A or non-B hepatitis. Approximately 1% of blood donors are seropositive for anti-HCV. The clinical symptoms of an HCV infection are variable. HCV establishes a chronic infection in 50 to 80% of cases. The window between infection and seroreactivity is highly variable, up to 12 months. The specificity of HCV screening Immunoassay may be increased by retesting positive sera by the HCV Immunoblot assay (RIBA).
Hepatitis C Viral RNA, Qualitative, TMA 37273X
CPT Code(s): 87521 Preferred Specimen(s) 3 mL frozen plasma collected in a PPT (white-top EDTA) tube Instructions Separate plasma from cells by centrifugation within 2 hours and freeze. The PPT tube gel barrier will maintain separation of plasma from cells. Store at -18 C or colder, if necessary. Transport Container PPT (white-top EDTA) tube Transport Temperature Frozen Reject Criteria Received thawed Received room temperature Received refrigerated Lithium heparin (green-top) tube Methodology Transcription-Mediated Amplification (TMA) Clinical Significance Qualitative RNA by TMA is useful in confirming HCV infection and to assess response to therapy. Limit of detection is 10 IU/mL.
Hepatitis C Viral RNA Genotype, LiPA 37811X
CPT Code(s): 87902 This test was developed and its performance characteristics determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 2 mL collected in a PPT (white-top EDTA) tube Instructions Plasma: Separate plasma from cells by centrifugation within 2 hours and freeze. The PPT tube gel barrier will maintain separation of plasma from cells. Store at -18 C or colder, if necessary. Serum: Collect blood in sterile tubes with no anticoagulants; serum separator tubes (SSTs) are recommended. Allow blood to clot at room temperature and separate serum from cells within 6 hours of collection. Transfer serum to sterile, plastic, screw-capped, aliquot tubes and store at -18 C or colder. Avoid repeated freezing and thawing of specimen. 2 mL is the preferred specimen volume. Transport Container PPT (white-top EDTA) tube Transport Temperature Frozen Methodology Multi-Probe Reverse Hybridization Clinical Significance Hepatitis C genotype is a predictor of response to interferon alfa-2b (non-type 1 are better responders) and to combination therapy with interferon and ribavirin (all types respond but dosage and duration of treatment is dependent on genotype; Type 1 requires extended treatment).
Hepatitis C Viral RNA, Quantitative, Real-Time PCR with Reflex to Genotype LiPA 11348X
CPT Code(s): 87522 This test was developed and its performance characteristics determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Includes If Hepatitis C Viral RNA, Quantitative, Real-Time PCR is >300 IU/ML, Hepatitis C Viral RNA Genotype, LiPA will be performed at an additional charge (CPT code(s): 87902). Preferred Specimen(s) 3 mL plasma collected in a PPT-Potassium EDTA (white-top) tube Instructions Separate plasma from cells as soon as possible, but no later than 6 hours after collection and freeze at -18 C or colder. Avoid thawing. Separated plasma can be kept refrigerated if testing is performed less than 72 hours after collection. Transport Container Frozen centrifuged PPT EDTA (white-top) tube Transport Temperature Frozen Refrigerated (cold packs) up to 72 hours from collection. Reject Criteria Received room temperature Received refrigerated later than 72 hours from collection Methodology Real-Time Polymerase Chain Reaction Multi-Probe Reverse Hybridization Reference Range(s) <50 IU/mL (<1.70 log IU/mL)
170
Gastroenterology Reference Guide
Hepatitis C Viral RNA, Quantitative, TMA 10073X
CPT Code(s): 87522 This test was developed and its performance characteristics determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 2 mL frozen plasma collected in a PPT (white-top EDTA) tube Instructions Separate plasma from cells by centrifugation within 2 hours and freeze. The PPT tube gel barrier will maintain separation of plasma from cells. Store at -18 C or colder, if necessary. Transport Container PPT (white-top EDTA) tube Transport Temperature Frozen Reject Criteria Received thawed Received room temperature Received refrigerated Serum Methodology Transcription-Mediated Amplification (TMA) Reference Range(s) <5 IU/mL (<0.7 log IU/mL) Clinical Significance Quantitative RNA by TMA is useful in confirming HCV infection, assessing prognosis (prior to the initiation of therapy), prescribing individualized therapy, predicting response to therapy, and monitoring response to therapy. Reportable range is 5 to 7,500 IU/mL.
by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Includes If Hepatitis C Viral RNA, Qualitative, PCR is positive, the HCV Quantitative PCR will be performed at an additional charge (CPT code(s): 87522) Preferred Specimen(s) 3 mL frozen plasma collected in a PPT (white-top EDTA) tube Instructions Separate plasma from cells by centrifugation within 2 hours and freeze. The PPT tube gel barrier will maintain separation of plasma from cells. Store at -18 C or colder, if necessary. Transport Container PPT (white-top EDTA) tube (preferred) or plastic screw-cap vial Transport Temperature Frozen preferred Refrigerated (cold packs) acceptable within 72 hours Reject Criteria Received room temperature Methodology Polymerase Chain Reaction (PCR) Clinical Significance Predict likelihood of therapeutic response and determine the duration of treatment.
Part 2: Gastroenterology Test Listing
Hepatitis C Virus RNA, Quantitative, bDNA 29271X
CPT Code(s): 87522 Preferred Specimen(s) 3 mL frozen plasma collected in a PPT (white-top EDTA) tube Instructions Separate plasma from cells by centrifugation within 2 hours and freeze. The PPT tube gel barrier will maintain separation of plasma from cells. Store at -18 C or colder, if necessary. Transport Container PPT (white-top EDTA) tube (preferred) or plastic screw-cap vial Transport Temperature Frozen Reject Criteria Gross hemolysis Heparin (green-top) tube ACD (yellow-top) tube Received thawed Received room temperature Received refrigerated Methodology Nucleic Acid Amplification by Branched DNA (bDNA) Reference Range(s) <615 IU/mL (<2.79 log IU/mL) Clinical Significance Quantitative RNA by bDNA is useful in confirming HCV infection, assessing prognosis (prior to the initiation of therapy), prescribing individualized therapy, predicting response to therapy, and monitoring response to therapy. Reportable range is 615 to 7,700,000 IU/mL.
Hepatitis C Virus RNA, Qualitative, PCR 34024X
CPT Code(s): 87521 Preferred Specimen(s) 3 mL frozen plasma collected in a PPT (white-top EDTA) tube Instructions Separate plasma from cells by centrifugation within 2 hours and freeze. The PPT tube gel barrier will maintain separation of plasma from cells. Store at -18 C or colder, if necessary. Transport Container PPT (white-top EDTA) tube (preferred) or plastic screw-cap vial Transport Temperature Frozen preferred Refrigerated (cold packs) acceptable within 72 hours Reject Criteria Received thawed Received room temperature If heparin collection tube is used Methodology Polymerase Chain Reaction (PCR) Clinical Significance Confirm Hepatitis C infection and demonstrate resolution of infection. Limit of detection is 50 IU/mL.
Hepatitis C Virus RNA, Qualitative, PCR, with Reflex to Quantitative, PCR 36559X
CPT Code(s): 87521 This test was developed and its performance characteristics determined by Quest Diagnostics. It has not been cleared or approved
171
Gastroenterology Reference Guide
Hepatitis C Virus RNA, Quantitative, Real-Time PCR 35645X
CPT Code(s): 87522 This test was developed and its performance characteristics determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 3 mL frozen plasma collected in a PPT (white-top EDTA) tube or EDTA (lavender-top) tube Instructions Separate plasma from cells by centrifugation within 2 hours and freeze. The PPT tube gel barrier will maintain separation of plasma from cells. Store at -18 C or colder, if necessary. Transport Container PPT (white-top EDTA) tube (preferred) or plastic screw-cap vial Transport Temperature Frozen Refrigerated (cold packs) up to 72 hours from collection Reject Criteria Received refrigerated later than 72 hours from collection Received room temperature Methodology Real-Time Polymerase Chain Reaction Reference Range(s)
Hepatitis Delta Antigen
23880X
CPT Code(s): 87380 Preferred Specimen(s) 1 mL serum collected in no additive (red-top) tube Instructions Serum should be removed from cells promptly after collection and transferred to a plastic tube Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Methodology Immunoassay Clinical Significance Diagnose Hepatitis D Viral (HDV) infection in patients with (1) newly diagnosed HBV infection; (2) chronic HBV infection with acute exacerbation; (3) fulminant HBV infection
Hepatitis E Antibodies (IgG, IgM)
15085X
HCV RNA, QL, Real-Time PCR HCV RNA, QN, Real-Time PCR
<1.70 log IU/mL <50 IU/mL
Clinical Significance Useful in monitoring therapy and disease progression. Reportable range is 50 to 50,000,000 IU/mL.
Hepatitis Delta Antibody
4990X
CPT Code(s): 86692 This test was performed using a kit that has not been cleared or approved by the FDA. The analytical performance characteristics of this test have been determined by Quest Diagnostics. This test should not be used for diagnosis without confirmation by other medically established means. Preferred Specimen(s) 1 mL serum collected in serum separator tube Instructions Collect blood in sterile tubes with no anticoagulants. Serum separator tubes (SSTs) are recommended. Allow blood to clot at room temperature and separate serum from cells within 1 hour of collection. Transfer serum to sterile, plastic, screw-capped aliquot and store refrigerated or frozen. Transport Container Sterile screw-cap vial Transport Temperature Refrigerated (cold packs) Methodology Immunoassay Reference Range(s) Non reactive
CPT Code(s): 86790 (x2) This test was performed using a kit that has not been cleared or approved by the FDA. The analytical performance characteristics of this test have been determined by Quest Diagnostics. This test should not be used for diagnosis without confirmation by other medically established means. Preferred Specimen(s) 1 mL serum collected in a no additive (red-top) tube Instructions Serum should be removed from cells promptly after collection and transferred to a plastic tube Transport Container Plastic screw-cap vial Transport Temperature Frozen Reject Criteria Received room temperature Methodology Immunoassay Reference Range(s) Non reactive This test is not to be used in the diagnosis or prognosis of disease, for donor screening, as a confirmatory test, as a supplemental test, or to counsel donors. Clinical Significance Hepatitis E causes an acute, self-limiting infection. Antibody IgG is detected after Antibody IgM is detected, typically 1 month post-infection. Antibody IgM is detected 1-4 weeks post-infection.
172
Gastroenterology Reference Guide
Hepatitis E Antibody (IgG)
36583X
CPT Code(s): 86790 This test was performed using a kit that has not been approved or cleared by the FDA. The analytical performance characteristics of this test have been determined by Quest Diagnostics. This test should not be used for diagnosis without confirmation by other medically established means. Preferred Specimen(s) 1 mL serum collected in a red-top tube (no gel) Instructions Serum should be removed from cells promptly after collection and transferred to a plastic tube. Do not submit the sample in a glass tube. Transport Container Plastic screw-cap vial Transport Temperature Frozen Reject Criteria Received room temperature Methodology Immunoassay Clinical Significance Resolution of HBV can be assessed with the disappearance of HBeAg and the appearance of HBeAb
If Hepatitis B Surface Antigen is positive, confirmation by neutralization will be performed at an additional charge (CPT code(s): 87341). Preferred Specimen(s) 5 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Methodology Immunoassay
Part 2: Gastroenterology Test Listing
HEPTIMAX HCV RNA
10565X
Hepatitis E Antibody (IgM)
36582X
CPT Code(s): 86790 This test was performed using a kit that has not been approved or cleared by the FDA. The analytical performance characteristics of this test have been determined by Quest Diagnostics. This test should not be used for diagnosis without confirmation by other medically established means. Preferred Specimen(s) 1 mL serum collected in a tube with no additives (red-top) Instructions Serum should be removed from cells promptly after collection and transferred to a plastic tube Transport Container Plastic screw-cap vial Transport Temperature Frozen Reject Criteria Received room temperature Methodology Immunoassay Reference Range(s) Non reactive This test is not to be used in the diagnosis or prognosis of disease, for donor screening, as a confirmatory test, as a supplemental test, or to counsel donors. Clinical Significance Hepatitis E causes an acute, self-limiting infection. Antibody IgG is detected after Antibody IgM is detected, typically 1 month post-infection. Antibody IgM is detected 1-4 weeks post-infection.
CPT Code(s): 87522 This test was developed and its performance characteristics determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 3 mL frozen plasma collected in a PPT (white-top EDTA) tube Instructions Separate plasma from cells by centrifugation within 2 hours and freeze. The PPT tube gel barrier will maintain separation of plasma from cells. Store at -18 C or colder, if necessary. Transport Container PPT (white-top EDTA) tube Transport Temperature Frozen Do not thaw Reject Criteria Received thawed Received room temperature Methodology TaqMan Real-Time Polymerase Chain Reaction, Transcription-Mediated Amplification (TMA) Clinical Significance HCV RNA quantitative assays are used to confirm HCV Antibody and to document persistent infection. The Veterans Affairs Guidelines recommend HCV RNA assays for patients receiving treatment. Heptimax C provides the broadest linear range available for HCV. The reference interval for this assay is 5-50,000,000 IU/mL.
Hepatitis Panel, Acute with Reflex Confirmation 10306X
CPT Code(s): 80074 Includes Hepatitis A IgM (Acute), Hepatitis B Surface Antigen with Reflex Confirmation, Hepatitis B Core IgM Antibody, Hepatitis C Antibody
173
Gastroenterology Reference Guide
HEPTIMAX HCV RNA with Reflex to HCV Genotype, LiPA 19702X
CPT Code(s): 87522 This test was developed and its performance characteristicshave been determined by Quest Diagnostics.It has not been cleared or approved by the U.S. Food and Drug Administration.The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Includes If the HEPTIMAX HCV RNA result is >300, then the Hepatitis C Viral RNA Genotype, LiPA will be performed at an additional charge (CPT(s) 87902.) Preferred Specimen(s) 3.2 mL PPT Potassium EDTA (white-top) plasma Instructions Plasma: Collect blood in sterile tubes containing EDTA anticoagulant, either 0.15% solution v/v final EDTA K3 (standard EDTA tube) or 9 mg spray-dried EDTA K2 (plasma preparation tube or PPT tube with plasma separator-gel, preferred). Blood collected in tubes containing ACD anticoagulant are acceptable but will yield results approximately 15% lower when compared to EDTA tubes due to the dilution effect of the 1.5 mL of anticoagulant used in the tube. Blood collected in tubes with heparin anticoagulant are unsuitable for this test. Store whole blood at room temperature and separate plasma from cells within 6 hours of collection. Transfer plasma to sterile, plastic, screw-capped aliquot tubes and store at -18 C or colder. Do not clarify plasma by filtration or further centrifugation. Avoid repeated freezing and thawing of specimen. Note: If blood is collected in a PPT tube, centrifuge within 6 hours of collection as before, but it is not necessary to transfer the plasma to aliquot tubes. Following centrifugation, a gel barrier maintains separation of plasma from cellular components during specimen transport and storage, and unlike standard Vacutainer brand blood collection tubes, the PPT tube is plastic and hence the plasma can be shipped and stored frozen in the original tube. Serum: Collect blood in sterile tubes with no anti-coagulants; serum separator tubes (SSTs) are recommended. Allow blood to clot at room temperature and separate serum from cells within 6 hours of collection. Transfer serum to sterile, plastic screw-capped, aliquot tubes and store at -18 C or colder. Avoid repeated freezing and thawing of specimen. Transport Container Plastic screw-cap vial Transport Temperature Frozen Reject Criteria Received thawed Received room temperature Methodology TaqMan Real-Time Polymerase Chain Reaction, Transcription-Mediated Amplification (TMA) Multi-Probe Reverse Hybridization
Transport Temperature Refrigerated (cold packs) Reject Criteria Received frozen Methodology Polymerase Chain Reaction Amplification followed by Sequence Specific Oligonucleotide Probes (PCR-SSO) Clinical Significance Celiac disease is a multigenic immune-mediated enteropathy triggered by dietary proteins, commonly known as glutens, present in wheat, barley, and rye. Varied clinical manifestations begin either in childhood or adult life. Its prevalence in the united states ranges from 0.5 to 1%. Celiac disease is strongly associated with the HLA genetic region. Approximately 90% of celiac patients express the HLA-DQ2 molecule. Most of the DQ2 negative patients express the HLA-DQ8 molecule. Gluten peptides presented by these HLA molecules induce an abnormal mucosal immune response and tissue damage. The HLA-DQ molecules are heterodimers of an alpha and a beta chain. The beta chain of HLA-DQ2 is coded by HLA-DQB1 * 02 and of DQ8 by HLA-DQB1 * 0302. HLA-DQB1 genotyping allows clinicians to evaluate the genetic predisposition for celiac disease in a patient.
HNPCC, MLH1 and MSH2 Mutations
14986X
HLA Typing for Celiac Disease
17135X
CPT Code(s): 86817 Preferred Specimen(s) 10 mL whole blood collected in a ACD-A or ACD-B (yellow-top) tube Transport Container ACD-A or ACD-B (yellow-top) tube
CPT Code(s): 83891, 83892 (x2), 83898 (x40), 83904 (x40), 83909 (x40), 83912 This test was developed and its performance characteristics have been determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 5 mL whole blood collected in an EDTA (lavender-top) tube or ACD Solution B (yellow-top) tube Instructions Whole blood: Normal phlebotomy procedure. Specimen stability is crucial. Store and ship room temperature immediately. Do not freeze. Transport Container EDTA (lavender-top) tube or ACD Solution B (yellow-top) tube Transport Temperature Room temperature Reject Criteria Received frozen Received refrigerated Methodology Polymerase Chain Reaction (PCR) Dye Terminator Sequencing Reaction Clinical Significance This test should be offered to patients with colorectal cancer who meet the Bethesda criteria established by National Cancer Institute (NCI), and/or that their tumors display Microsatellite Instability (MSI) or Replication Error Phenotype. Detection of a germline mutation in one of the two mismatch repair genes (MSH2 and MLH1) helps establishing a clinical diagnosis of hereditary nonpolyposis colorectal cancer (HNPCC) in affected patients. Mutation detection in at-risk family members allows predicative diagnosis of the disease and thus intensive screening and early intervention of cancer.
174
Gastroenterology Reference Guide
HNPCC, MLH1 Mutation, One Exon 14984X
CPT Code(s): 83891, 83892, 83898, 83904, 83909, 83912 This test was developed and its performance characteristics have been determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 5 mL whole blood collected in an EDTA (lavender-top) tube or ACD Solution B (yellow-top) tube Instructions Whole blood: Normal phlebotomy procedure. Specimen stability is crucial. Store and ship room temperature immediately. Do not freeze. Transport Container EDTA (lavender-top) tube or ACD Solution B (yellow-top) tube Transport Temperature Room temperature Reject Criteria Received frozen Received refrigerated Methodology Polymerase Chain Reaction (PCR) Dye Terminator Sequencing Reaction Reference Range(s) Not detected Clinical Significance Single exon sequencing should be offered to patients who have family history of a specific MLH1 mutation associated with hereditary nonpolyposis colorectal cancer (HNPCC). Detection of the familial mutation in MLH1 helps to establish a predicative diagnosis or rule out the diagnosis of HNPCC in at-risk family members of affected patients. This will allow intensive cancer screening and early intervention of the disease in HNPCC families.
family history of a specific MSH2 mutation associated with hereditary nonpolyposis colorectal cancer (HNPCC). Detection of the familial mutation in MSH2 helps to establish a predicative diagnosis or rule out the diagnosis of HNPCC in at-risk family members of affected patients. This will allow intensive cancer screening and early intervention of the disease in HNPCC families.
Part 2: Gastroenterology Test Listing
HNPCC, MSH6 Mutation
14982X
HNPCC, MSH2 Mutation, One Exon 14981X
CPT Code(s): 83891, 83892, 83898, 83904, 83909, 83912 This test was developed and its performance characteristics have been determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 5 mL whole blood collected in an EDTA (lavender-top) tube or ACD Solution B (yellow-top) tube Instructions Whole blood: Normal phlebotomy procedure. Specimen stability is crucial. Store and ship room temperature immediately. Do not freeze. Transport Container EDTA (lavender-top) tube or ACD Solution B (yellow-top) tube Transport Temperature Room temperature Reject Criteria Received frozen Received refrigerated Methodology Polymerase Chain Reaction (PCR) Dye Terminator Sequencing Reaction Clinical Significance Single exon sequencing should be offered to patients who have
CPT Code(s): 83891, 83892, 83898 (x18), 83904 (x18), 83909 (18), 83912 This test was developed and its performance characteristics have been determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 5 mL whole blood collected in an EDTA (lavender-top) tube or ACD Solution B (yellow-top) tube Instructions Whole blood: Normal phlebotomy procedure. Specimen stability is crucial. Store and ship room temperature immediately. Do not freeze. Transport Container EDTA (lavender-top) tube or ACD Solution B (yellow-top) tube Transport Temperature Room temperature Reject Criteria Received frozen Received refrigerated Methodology Polymerase Chain Reaction (PCR) Dye Terminator Sequencing Reaction Clinical Significance This test should be offered to patients with colorectal cancer who meet the Bethesda criteria established by National Cancer Institute (NCI), and/or that their tumors display Microsatellite Instability (MSI) or Replication Error (RER) phenotype. Detection of a germline mutation in the MSH6 gene helps in establishing a clinical diagnosis of hereditary nonpolyposis colorectal cancer (HNPCC) in affected patients. Mutation detection in at risk family members will allow predicative diagnosis of the disease and thus monitoring and early intervention of the disease.
175
Gastroenterology Reference Guide
HNPCC, MSH6 Mutation, One Exon 14983X
CPT Code(s): 83891, 83892, 83898, 83904, 83909, 83912 This test was developed and its performance characteristics have been determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 5 mL whole blood collected in an EDTA (lavender-top) tube or ACD Solution B (yellow-top) tube Instructions Whole blood: Normal phlebotomy procedure. Specimen stability is crucial. Store and ship room temperature immediately. Do not freeze. Transport Container EDTA (lavender-top) tube or ACD Solution B (yellow-top) tube Transport Temperature Room temperature Reject Criteria Received frozen Received refrigerated Methodology Polymerase Chain Reaction (PCR) Dye Terminator Sequencing Reaction Clinical Significance Single exon sequencing should be offered to patients who have family history of a specific MSH6 mutation associated with hererditary nonpolyposis colorectal cancer (HNPCC). Detection of the familial mutation in MSH6 helps to establish a predicative diagnosis or rule out the diagnosis of HNPCC in at-risk family members of affected patients. This will allow intensive cancer screening and early intervention of the disease in HNPCC families.
Clinical Significance Increased IgA is associated with monoclonal IgA myeloma, respiratory and gastrointestinal infections, and malabsorption; decreased IgA is found in selective IgA deficiency and in ataxia telangiectasia.
IgG
CPT Code(s): 82784 Preferred Specimen(s) 2 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemic Methodology Immunoturbidimetric Reference Range(s) Cord Blood 1 Month 5 Months 9 Months 12 Months 3 Years 6 Years 9 Years 11 Years 13 Years 15 Years >15 Years
543X
553-1360 mg/dL 213-765 mg/dL 170-595 mg/dL 187-765 mg/dL 247-910 mg/dL 533-1078 mg/dL 592-1723 mg/dL 673-1734 mg/dL 821-1835 mg/dL 893-1823 mg/dL 842-2013 mg/dL 694-1618 mg/dL
IgA
CPT Code(s): 82784 Preferred Specimen(s) 2 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemic Methodology Immunoturbidimetric Reference Range(s) Cord Blood 1 Month 5 Months 9 Months 12 Months 3 Years 6 Years 9 Years 11 Years 13 Years 15 Years >15 Years
539X
Clinical Significance Increased IgG is associated with acute and chronic inflammations, monoclonal IgG myeloma, autoimmune diseases; decreased IgG is found in selective IgG deficiency, Brutons Disease, and acquired immune deficiency.
1-3 mg/dL 2-43 mg/dL 3-66 mg/dL 7-66 mg/dL 12-75 mg/dL 24-121 mg/dL 33-235 mg/dL 41-368 mg/dL 64-246 mg/dL 70-432 mg/dL 57-300 mg/dL 81-463 mg/dL
176
Gastroenterology Reference Guide
IgM
CPT Code(s): 82784 Preferred Specimen(s) 2 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemic Methodology Immunoturbidimetric Reference Range(s) Cord Blood 1 Month 5 Months 9 Months 12 Months 3 Years 6 Years 9 Years 11 Years 13 Years 15 Years >15 Years
545X
Lactate Dehydrogenase (LD)
593X
<17 mg/dL 13-54 mg/dL 17-67 mg/dL 23-84 mg/dL 27-101 mg/dL 26-218 mg/dL 36-314 mg/dL 47-311 mg/dL 46-368 mg/dL 52-367 mg/dL 23-281 mg/dL 48-271 mg/dL
CPT Code(s): 83615 Preferred Specimen(s) 1 mL serum Instructions Do not refrigerate or freeze Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Received frozen Anticoagulants other than heparin Received refrigerated Methodology Spectrophotometry Reference Range(s) 100-250 U/L Clinical Significance Elevations in serum lactate dehydrogenase occur from myocardial infarction, liver disease, pernicious and megaloblastic anemia, pulmonary emboli, malignancies, and muscular dystrophy
Part 2: Gastroenterology Test Listing
Lactoferrin, Qualitative, Stool
10156X
Clinical Significance Increased IgM is associated with Waldenstrms macroglobulinemia, infectious mononucleosis, viral infections, nephrotic syndrome, and estrogen therapy; decreased IgM is found in selective IgM deficiency, Brutons Disease, and acquired immune deficiency.
Inflammatory Bowel Disease Differentiation Panel
10457X
CPT Code(s): 86671 (x2), 86021 Includes Saccharomyces cerevisiae Ab (ASCA) IgG, Saccharomyces cerevisiae Ab (ASCA) IgA, ANCA-IBD Screen with Reflex to Titer If the ANCA-IBD screen is positive a P-ANCA Titer will be performed at an additional charge (CPT code(s): 86021). Preferred Specimen(s) 3 mL serum Transport Container No additive (red-top tube) Transport Temperature Refrigerated (cold packs) Reject Criteria Received room temperature Methodology Immunoassay Reference Range(s) See individual analytes Clinical Significance For the detection of Saccharomyces cerevisiae IgG and IgA antibodies in human serum. These tests are intended to aid in the diagnosis of patients with Crohns Disease.
CPT Code(s): 83630 Preferred Specimen(s) 1 g frozen stool collected in a screw-cap container Instructions From collection time to the time stool is frozen must not exceed 48 hours. Patients may collect stool and hold at room temperature until it can be properly frozen. Specimens can be delivered to Patient Service Center (PSC) or physicians office for freezing and delivery to the laboratory. Transport Container Plastic screw-cap container Transport Temperature Frozen Reject Criteria Received room temperature Methodology Immunoassay Clinical Significance The Lactoferrin IBD-CHEK is a qualitative (QL) Enzyme Linked Immunosorbent Assay (ELISA) for measuring concentrations of fecal lactoferrin, a marker for leukocytes. A positive level is an indicator of intestinal inflammation. The test can be used as an in vitro diagnostic aid to distinguish patients with active inflammatory bowel disease (IBD) from those with non inflammatory irritable bowel syndrome (IBS).
177
Gastroenterology Reference Guide
Lactoferrin, Quantitative, Stool
Lipase
606X
17321X
CPT Code(s): 83631 Preferred Specimen(s) 1 g stool Instructions Collect undiluted feces in clean, dry, sterile, leak-proof container. Do not add fixative or preservative. From collection time to the time stool is frozen must not exceed 48 hours. Patients may collect stool and hold at room temperature until it can be properly frozen. The time held at room temperature must not exceed 48 hours from time of collection. Specimens can be delivered to Patient Service Center (PSC) or physicians office for freezing and delivery to the laboratory. Transport Container Plastic screw-cap container Transport Temperature Frozen Reject Criteria Specimen collected in formalin, MF, SAF, or PVA Cary-Blair media Received room temperature Received refrigerated Methodology Immunoassay Clinical Significance This is an Enzyme-Linked Immunosorbent Assay (ELISA) for measuring concentrations of fecal lactoferrin, a marker for leukocytes. An elevated level is an indicator of intestinal inflammation. The test can be used as an in vitro diagnostic aid to distinguish patients with active inflammatory bowel disease (IBD) from those with noninflammatory irritable bowel syndrome (IBS).
CPT Code(s): 83690 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Hemolysis Lipemia Methodology Spectrophotometry Reference Range(s) 7-60 U/L Clinical Significance Confirmatory evidence for diagnosis of pancreatitis
Listeria Antibody, Serum, CF
CPT Code(s): 86609 Preferred Specimen(s) 1 mL serum Methodology Complement Fixation (CF)
34329X
Liver Fibrosis Panel (HepaScore)
19647X
Lactose Tolerance Test, 5 Specimens (50g) 7675X
CPT Code(s): 82951, 82952 (x2) Includes Fasting specimen, 1/2-hour, 1-hour, 2-hour, and 3-hour specimens Preferred Specimen(s) 1 mL plasma collected in five separate gray-top tubes (fluoridated, oxalated) Instructions 1st specimen obtained fasting*. Immediately thereafter, the adult patient is given a 50 gram dose of lactose (supplied by patients physician) and specimens are obtained 1/2, 1, 2 and 3 hours later. Specimens must be labeled accordingly for each submission. * Fasting is defined as no consumption of food or beverage other than water for at least 8 hours before testing. Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Hemolysis Methodology Spectrophotometry, Hexokinase Clinical Significance Results may be used to evaluate deficiency of small bowel mucosal lactate, which may be associated with intolerance to lactose, manifested by diarrhea and other symptoms following ingestion of milk
CPT Code(s): 82977, 82247, 83520, 83883 *This test was developed and its performance characteristics have been determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Includes HepaScore, GGT, Bilirubin, Total; Hyaluronic Acid*, Alpha 2 Macroglobulin Preferred Specimen(s) 3.6 mL serum collected in a no additive (red-top) tube Transport Container Plastic screw-cap vial Transport Temperature Frozen Reject Criteria Received room temperature Hemolysis Lipemia Patients <20 years old Methodology Spectrophotometry Colorimetric Immunoassay Fixed Rate Time Nephelometry Reference Range(s) See individual analytes Clinical Significance HepaScore has been developed to assist with the non-invasive diagnosis and staging of liver fibrosis in patients with Hepatitis C
178
Gastroenterology Reference Guide
Methicillin Resistant Staphylococcus aureus, PCR 17656X
CPT Code(s): 87798 Preferred Specimen(s) Nasal swab Instructions Swab must be inserted into nostril up to 2.5 cm (1 inch) from edge of the nare and rolled 5 times. Repeat using same swab in the other nostril. Return swab to its container. Nasal swab collect in: Liquid Amies, Single Swab Copan Venture Transystem. Liquid Stuart, Single SwabCopan Venture Transystem Transport Container Nasal swab Transport Temperature Refrigerated (cold packs) Reject Criteria Received room temperature Received frozen Specimens exceeding stability Specimens in leaking or broken containers Non-validated specimen types Amies gel collection tubes Methodology Polymerase Chain Reaction (PCR) Clinical Significance This assay is used to detect the presence of Methicillin-Resistant Staphylococcus aureus (MRSA) DNA in a patients nasal swab specimen. The use of real-time PCR to detect the presence of MRSA DNA in clinical specimens allows for rapid patient testing.
Microsporidia Spore Detection
3562X
Part 2: Gastroenterology Test Listing
CPT Code(s): 87015 (if performed), 87207 Includes Smear and Concentration (if performed) Preferred Specimen(s) 5 grams (5 mL) stool Instructions Transfer stool within 30 minutes of collection into formalin vial. Fill to the line on transport vial. Transport Container Sterile screw-cap container with 10% formalin Transport Temperature Refrigerated (cold packs) Reject Criteria Unpreserved stool Stool in Cary-Blair or PVA Frozen specimens Methodology Light Microscopy: Modified Trichome Stain Reference Range(s) None detected Clinical Significance Microsporidia infection was first recognized as a cause of chronic diarrhea in patients infected with HIV. Microsporidia may also cause pneumonia, acute bilateral keratoconjunctivitis, and infection of the biliary and pancreatic ducts.
Microsatellite Instability (MSI), HNPCC 14989X
CPT Code(s): 83890 (x2), 83900 (x2), 83901 (x6), 83907, 83909 (x2), 83912 This test was developed and its performance characteristics have been determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 5 mL whole blood collected in an EDTA (lavender-top) tube and formalin-fixed, paraffin embedded tissue block Instructions One formalin-fixed paraffin embedded tissue with representative tumor AND one EDTA whole blood from the same patient must be submitted for testing. Both sample types are required for testing. Avoid hemolysis. Transport Container EDTA (lavender-top) tube and Paraffin Block Bag Transport Temperature Room temperature Reject Criteria Received frozen Avoid hemolysis Methodology Polymerase Chain Reaction (PCR) Capillary Electrophoresis Clinical Significance Patients with early onset and family history of colon cancers are suggestive of Hereditary Nonpolyposis Colon Cancer (HNPCC) syndrome. Microsatellite instability analysis on tumor tissue is recommended as a screening test to identify individuals eligible for germline mutation analysis of mismatch repair genes.
Mitochondrial Antibody with Reflex to Titer 259X
CPT Code(s): 86255 Includes If screen is positive, Mitochondrial Antibody titer will be performed at an additional charge (CPT code(s): 86256) Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemia Methodology Immunofluorescent Assay (IFA) Reference Range(s)
<1:20 Negative 1:20-1:80 Intermediate level. May be present in autoallergic or other liver diseases. >1:80 Elevated level. Strongly suggestive of primary biliary cirrhosis.
Clinical Significance A high anti-mitochondrial (AMA) titer supports the diagnosis of primary biliary cirrhosis; low titers of AMA may be detected in other liver disorders which include chronic active hepatitis and cryptogenic cirrhosis.
179
Gastroenterology Reference Guide
MLH1 and MSH2 Mutations (Deletion and Duplication), HNPCC 16051X
CPT Code(s): 83891, 83900, 83901 (x39), 83909 (x2), 83912 This test was developed and its performance characteristics have been determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 5 mL whole blood collected in an EDTA (lavender-top) tube Instructions Whole blood: Normal phlebotomy procedure. Specimen stability is crucial. Store and ship room temperature immediately. Do not freeze. Provide family history. Contact the laboratory for other sample types. Transport Container EDTA (lavender-top) tube Transport Temperature Room temperature Reject Criteria Received frozen Methodology Multiplex Polymerase Chain Reaction (PCR), Capillary Electrophoresis Clinical Significance This test should be offered to patients with colorectal cancer who meet the Bethesda criteria, established by National Cancer Institute (NCI), and/or that their tumors display microsatellite instability (MSI), in conjunction with direct sequencing analysis of the MLH1/ MSH2 genes. It greatly enhances the sensitivity of MLH1/MSH2 germline mutation detection, which helps in establishing a clinical diagnosis of HNPCC in affected patients. Mutation detection in at risk family members allows predicative diagnosis of the disease and thus intensive screening and early intervention of cancer.
Methodology Enzymatic Clinical Significance Positive results in patients who have followed the prescribed pre-test diet are suggestive of gastrointestinal bleeding from causes that include colorectal cancer, polyps, peptic ulcers, and hemorrhoids
Occult Blood, Stool, Qualitative, Medicare 35306X
CPT Code(s): 82270 When diagnostic testing for a Medicare Patient is required for Occult Blood, Stool, Qualitative testing, please order test code 35301, Occult Blood, Stool, Qualitative Preferred Specimen(s) Hemoccult SENSA slide inoculated with a thin smear of stool. Transport Container Hemoccult SENSA card Transport Temperature Room temperature Reject Criteria Bulk stool Specimens not received on Hemoccult SENSA cards All other specimen types Specimens older than 14 days Methodology Enzymatic Clinical Significance Positive results, in patients who have followed the prescribed pre-test diet, are suggestive of gastrointestinal bleeding from causes that include colorectal cancer, polyps, peptic ulcers, and hemorrhoids
Ova and Parasites
681X
Norovirus RNA, RT-PCR
CPT Code(s): 87798 Preferred Specimen(s) 1 g stool Transport Container Sterile leak-proof container Transport Temperature Frozen Methodology Real-time Polymerase Chain Reaction
19098X
Occult Blood, Stool, Qualitative
35301X
CPT Code(s): 82270 if two or three specimens. 82272 if one specimen. Preferred Specimen(s) Hemoccult SENSA slide inoculated with a thin smear of stool. Transport Container Hemoccult SENSA card Transport Temperature Room temperature Reject Criteria Bulk stool Specimens not received on Hemoccult SENSA cards All other specimen types Specimens older than 14 days
CPT Code(s): 87177, 87209 Includes Ova and Parasites Concentrate Result, Trichrome Result Preferred Specimen(s) Stool in 10% formalin and polyvinyl alcohol (PVA) transport vials Transport Container 10% formalin and polyvinyl alcohol transport vials may be submitted in a sterile container Transport Temperature Stool: Room temperature Reject Criteria Unpreserved specimens Specimens containing barium Stool preserved in medium other than 10% formalin and PVA, Sodium Acetate-Acetic Acid Formalin (SAF) or Merthiolate Iodine Formalin (MIF) Stool in 10% formalin received frozen Methodology Concentration of treated fecal sediment or urine by centrifugation and microscopic exam, trichrome stain and microscopic exam Clinical Significance Diseases caused by human parasites remain on a worldwide basis among the principle causes of morbidity and mortality. Correct diagnosis of intestinal parasitic infection depends on proper collection, transport, detection and identification of parasites in stool specimens. Symptoms range from malaise to death. Treatment is dependent upon examining multiple stool exams due to the erratic shed rates of some parasites.
180
Gastroenterology Reference Guide
Ova and Parasites, 3 Specimens
6652X
CPT Code(s): 87177 (x3), 87209 (x3) Includes Ova and Parasite Concentrate Results, Trichrome Results Preferred Specimen(s) Stool in 10% formalin and in polyvinyl alcohol (PVA) transport vials Transport Container 10% formalin and polyvinyl alcohol (PVA) transport vials Transport Temperature Stool: Room temperature Reject Criteria Unpreserved specimens Specimens containing barium Stool preserved in medium other than 10% formalin, SAF or MIF Stool in 10% formalin received frozen Stool submitted in expired transport vial Methodology Concentration of treated fecal sediment or urine by centrifugation and microscopic exam, trichrome stain and microscopic exam Clinical Significance Diseases caused by human parasites remain on a worldwide basis among the principle causes of morbidity and mortality. Correct diagnosis of intestinal parasitic infection depends on proper collection, transport, detection and identification of parasites in stool specimens. Symptoms range from malaise to death. Treatment is dependent upon examining multiple stool exams due to the erratic shed rates of some parasites.
Transport Temperature Room temperature Reject Criteria Unpreserved specimens Specimens obtained within 7 days of treatment with mineral oil, barium, antibiotics, and laxatives Methodology Microscopic and Macroscopic Examination and Conventional Identification Techniques Clinical Significance Some parasitic diseases can be diagnosed by recovering the intact parasite in adult, immature or larval form. The symptoms of the diseases caused by each parasite varies, dependent upon the type of parasite.
Part 2: Gastroenterology Test Listing
Parietal Cell Antibody with Reflex to Titer 262X
CPT Code(s): 86255 Includes If the Parietal Cell Antibody Screen is positive, a Parietal Cell Antibody Titer will be performed at an additional charge (CPT code(s): 86256) Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemic Methodology Immunofluorescent Assay (IFA) Reference Range(s) <1:20 1:20-1:40 >1:40
Parasite Exam, Stool, Trichrome Stain 5408X
CPT Code(s): 87209 Preferred Specimen(s) Feces: 1 g of stool in a polyvinyl alcohol (PVA) vial Instructions Fluid level should reach line on vial. Mix specimen with the preservative. Indicate on vial label whether stool is formed (soft or hard) or diarrheal. Do not freeze. For other fluids, contact the laboratory for instructions. Transport Container Polyvinyl Alcohol (PVA) Transport Vial Transport Temperature Room temperature Reject Criteria Unpreserved specimens Received frozen Methodology Microscopic Examination and Trichrome Stain Clinical Significance Clinical significance depends upon the organism identified. Some organisms are of little or no significance in humans, while others may be associated with significant disease states.
None detected Weakly Positive Positive. Suggestive of pernicious anemia or atrophic gastritis.
Clinical Significance Parietal cell antibodies are present in about 80% of patients with pernicious anemia and are rarely present in gastric ulcer, gastric cancer, or in association with antinuclear antibodies
Parasite Identification, Intestinal
3950X
CPT Code(s): 87169 or 87999 Preferred Specimen(s) Collect specimen (suspect nematode, cestode, trematode or other parasite) in a clean container and transfer to 70% alcohol as soon as possible. Transport Container Clean, plastic, leak-proof container
181
Gastroenterology Reference Guide
pH, Stool
1304X
CPT Code(s): 83986 Preferred Specimen(s) 5 mL frozen, random liquid stool Instructions Place into any plastic container with tightly fitting cover. Seal container in plastic bag before shipping. Store and ship frozen. Transport Container Plastic screw-cap vial Transport Temperature Frozen Reject Criteria Received room temperature Received thawed Fecal specimens received in paint can Methodology Potentiometry Clinical Significance As a screen for carbohydrate and fat malabsorption, and is also used to evaluate small intestinal disaccharidase deficiencies
Clinical Significance Potassium measurements are useful in monitoring electrolyte balance in the diagnosis and treatment of disease conditions characterized by low or high blood potassium levels. Potassium is elevated in adrenal cortical insufficiency, acute renal failure and in some cases of diabetic acidosis. Potassium is decreased in diuretic administration and renal tubular acidosis.
Protein, Total
CPT Code(s): 84155 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Plasma Methodology Spectrophotometry Reference Range(s)
754X
Pinworm Identification
4496X
CPT Code(s): 87172 Preferred Specimen(s) One pinworm paddle consisting of a clear plastic spatula with adhesive on one side Instructions Press without smearing onto the folds of the perianal area. Collect specimen first thing in the morning. Transport Container Plastic tube containing pinworm paddle Transport Temperature Room temperature Reject Criteria Stool specimens Frosted tape preparations Methodology Microscopic Examination Clinical Significance Diagnosis of pinworm infestation is based on the observation of typical thick-walled, football-shaped eggs. The eggs are usually deposited around the anus and are not commonly seen in feces.
<1 Month 1-5 Months 6-11 Months 1-19 Years 20 Years
Male 4.1-6.3 4.7-6.7 5.5-7.0 6.3-8.2 6.2-8.3
g/dL g/dL g/dL g/dL g/dL
Female 4.2-6.2 g/dL 4.4-6.6 g/dL 5.6-7.9 g/dL 6.3-8.2 g/dL 6.2-8.3 g/dL
Clinical Significance The total serum protein level is the sum of all circulating proteins that are major components of blood. Serum total protein measurements are useful in the diagnosis and treatment of a variety of diseases involving the liver, kidney, or bone marrow as well as other metabolic or nutritional disorders.
Prothrombin
331X
Potassium, Serum
733X
CPT Code(s): 84132 Preferred Specimen(s) 1 mL serum. Separate from cells as soon as possible after clotting. Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Methodology Ion Selective Electrode (ISE) Reference Range(s) 1 Week 8-30 Days 1-5 Months 6 Months-1 Year 2-19 Years 20 Years
3.2-5.5 3.4-6.0 3.5-5.6 3.5-6.1 3.8-5.1 3.5-5.3
mmol/L mmol/L mmol/L mmol/L mmol/L mmol/L
CPT Code(s): 85210 Preferred Specimen(s) 3 mL platelet poor 3.2% sodium citrate-anticoagulated plasma (collected in light blue-top tube), separated and frozen immediately. Instructions Draw blood in light blue-top tube containing 3.2% sodium citrate, mix gently by inverting 3-4 times. Centrifuge 15 minutes at 2500-3500 rpm. Using a plastic pipette, remove plasma, taking care to avoid the WBC/platelet buffy layer and place into a plastic vial. Centrifuge a second time and transfer platelet-poor plasma into a new plastic vial. Plasma must be free of platelets (<10,000/ microliter). Transport Container Plastic screw-cap vial Transport Temperature Frozen Reject Criteria Received thawed Received refrigerated Hemolysis Methodology Photometric Clot Detection
182
Gastroenterology Reference Guide
Rotavirus Antigen Detection
706X
CPT Code(s): 87425 Preferred Specimen(s) Stool specimen or rectal swab in a clean, dry container without preservatives or media Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Reject Criteria Transport systems containing media, serum, preservatives or detergent Methodology Immunoassay Clinical Significance Rotavirus infection is the major cause of gastroenteritis in children from six months to two years. Infection occurs in both sporadic and epidemic forms and is responsible for approximately half the cases of diarrhea in infants that require hospitalization worldwide. The peak of rotavirus disease in temperate climates occurs during the cooler months of the year. Rotavirus has also emerged as a cause of enteritis in adults, particularly in elderly immunosuppressed patients.
Reject Criteria Gross hemolysis Lipemia Methodology Immunoassay Reference Range(s)
Part 2: Gastroenterology Test Listing
20 U 20.1-29.9 U 30 U
Negative Equivocal Positive
Clinical Significance Antibodies to Saccharomyces cerevisiae are found in approximately 75% of patients with Crohns disease, 15% of patients with ulcerative colitis, and 5% of the healthy population. High titers of antibody increase the likelihood of disease, and specifically Crohns disease, and are associated with more aggressive disease.
Salmonella, Total Antibody, EIA
10582X
Saccharomyces cerevisiae Antibody (ASCA) IgA 10295X
CPT Code(s): 86671 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Reject Criteria Gross hemolysis Lipemia Methodology Immunoassay Reference Range(s)
20 U 20.1-24.9 U 25 U
Negative Equivocal Positive
CPT Code(s): 86768 (x5) Includes Salmonella O Type D, Salmonella H Type d, Salmonella H Type a, Salmonella H Type b, and Salmonella O Type Vi Preferred Specimen(s) 1 mL serum Instructions Blood collected by venipuncture should be allowed to clot at room temperature and then centrifuged, following National Accrediting Agency for Clinical Laboratory Scientists guidelines. Serum should be separated as soon as possible and refrigerated or stored frozen if not tested within one week. Transport Container Plastic screw-cap vial Transport Temperature Frozen Reject Criteria Hemolysis Lipemia Received room temperature Methodology Enzyme Immunoassay (EIA) Clinical Significance Salmonella, Total Antibody, detects antibodies to Salmonella typhi, a common cause of gastroenteritis, diarrhea, and dysentery. Antibody results should be confirmed with stool or blood cultures.
Clinical Significance Antibodies to Saccharomyces cerevisiae are found in approximately 75% of patients with Crohns disease, 15% of patients with ulcerative colitis, and 5% of the healthy population. High titers of antibody increase the likelihood of disease, and specifically Crohns disease, and are associated with more aggressive disease.
Saccharomyces cerevisiae Antibody (ASCA) IgG 10294X
CPT Code(s): 86671 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs)
183
Gastroenterology Reference Guide
Sedimentation Rate (ESR), Modified Westergren 809X
CPT Code(s): 85652 Preferred Specimen(s) Whole blood: Full EDTA (lavender-top) tube Instructions Maintain specimen at room temperature. If multiple tests are ordered, please submit a separate tube for this test. Transport Container EDTA (lavender-top) tube Transport Temperature Room temperature Reject Criteria Hemolysis Samples >24 hours old Clotted Insufficient quantity Methodology Modified Westergren Reference Range(s)
Transport Temperature Room temperature Methodology Immunoassay
Smooth Muscle Actin, IHC with Interpretation 19271X
CPT Code(s): 88342 This test was developed and its performance characteristics have been determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) Formalin fixed paraffin embedded tissue Transport Container IHC specimen transport kit Transport Temperature Room temperature Methodology Immunohistochemical Stain
50 Years >50 Years
Female 20 mm/h 30 mm/h
Male 15 mm/h 20 mm/h
Clinical Significance Useful in differentiating inflammatory and neoplastic diseases and as an index of disease severity. CRP is also useful in monitoring inflammatory disease states.
Smooth Muscle Antibody (IgG)
15043X
Shiga Toxins, EIA
30264X
CPT Code(s): 87427 Preferred Specimen(s) Stool in Cary-Blair transport, rectal swab in transport medium or culture isolate Transport Container Cary-Blair transport vial, transport swab, or bacteriologic media slant in a double-walled container Transport Temperature Room temperature Reject Criteria Unpreserved stools Dry swabs Stools in diapers Methodology Immunoassay
CPT Code(s): 83516 Preferred Specimen(s) 0.5 mL serum Transport Container Plastic screw-cap vial Transport Temperature Frozen Reject Criteria Gross hemolysis Lipemic Received room temperature Methodology Immunoassay Clinical Significance Actin is the major antigen to which smooth muscle antibodies react in autoimmune hepatitis. F-Actin IgG antibodies are found in 52-85% of patients with autoimmune hepatitis (AIH) or chronic active hepatitis and in 22% of patients with primary biliary cirrhosis (PBC). Anti-actin antibodies have been reported in 3-18% of sera from normal healthy controls.
Shiga Toxins, EIA and Culture, Stool 10108X
CPT Code(s): 87045, 87046, 87427 Includes Shiga Toxins (including E. coli), EIA; Culture, Salmonella and Shigella; Culture, Campylobacter If culture is positive, identification will be performed at an additional charge (CPT code(s): 87077 or 87140 or 87143 or 87147 or 87149). Antibiotic susceptibilities are only performed when appropriate (CPT code(s): 87181 or 87184 or 87185 or 87186). Preferred Specimen(s) Stool in Cary-Blair transport, rectal swab in transport medium or culture isolate Transport Container Cary-Blair transport vial, transport swab, or bacteriologic media slant in a double-walled container
184
Gastroenterology Reference Guide
Smooth Muscle Antibody Screen with Reflex to Titer 263X
CPT Code(s): 86255 Includes If Smooth Muscle Antibody Screen is positive, a Titer will be performed at an additional charge (CPT code(s): 86256) Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Hyperlipemic Methodology Immunofluorescent Assay (IFA) Reference Range(s) <1:20 1:20-1:40
Transport Temperature Refrigerated (cold packs) Methodology Immunoassay Reference Range(s) IgG <7 U/mL 7-10 U/mL >10 U/mL
Part 2: Gastroenterology Test Listing
Negative Equivocal Positive Negative Equivocal Positive
IgA <5 U/mL 5-8 U/mL >8 U/mL
>1:40
Negative Weakly Positive. May be present in acute viral hepatitis, lupoid hepatitis, infectious mononucleosis and malignancy High Positive. Highly suggestive of active chronic hepatitis
Clinical Significance Tissue Transglutaminase Antibody, IgA, is useful in diagnosing gluten-sensitive enteropathies, such as Celiac Sprue Disease, and an associated skin condition, dermatitis herpetiformis. The IgG test is useful in patients who are IgA-deficient. The IgG test also provides support for gluten-sensitive enteropathies beyond IgA the test.
Tissue Transglutaminase (tTG) Antibody (IgA) 8821X
CPT Code(s): 83516 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Refrigerated (cold packs) Methodology Immunoassay Reference Range(s) <5 U/mL 5-8 U/mL >8 U/mL
Clinical Significance Smooth muscle antibodies are detected in 85% of patients with chronic active hepatitis and in less than 50% of patients with primary biliary cirrhosis. Smooth muscle antibodies are usually negative in extrahepatic biliary obstruction, drug induced liver disease, viral hepatitis and hepatoma.
Sodium
836X
CPT Code(s): 84295 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Gross hemolysis Anticoagulants other than heparin Methodology Ion Selective Electrode (ISE) Reference Range(s) 135-146 mmol/L Clinical Significance Sodium measurements are useful in the diagnosis and treatment of aldosteronism, diabetes insipidus, adrenal hypertension, Addisons Disease, dehydration, inappropriate antidiuretic hormone secretion, or other diseases involving electrolyte imbalance
Negative Equivocal Positive
Clinical Significance Tissue Transglutaminase Antibody, IgA, is useful in diagnosing gluten-sensitive enteropathies, such as Celiac Sprue Disease, and an associated skin condition, dermatitis herpetiformis.
Tissue Transglutaminase (tTG) Antibodies (IgG, IgA) 11073X
CPT Code(s): 83516 (x2) Preferred Specimen(s) 1 mL serum Transport Container Sterile screw-cap vial
185
Gastroenterology Reference Guide
Tissue Transglutaminase (tTG) Antibody (IgG) 11070X
CPT Code(s): 83516 Preferred Specimen(s) 1 mL serum Transport Container Sterile screw-cap vial Transport Temperature Refrigerated (cold packs) Methodology Immunoassay Reference Range(s) <7 U/mL 7-10 U/mL >10 U/mL
TSH
CPT Code(s): 84443 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Methodology Immunoassay Reference Range(s)
899X
Negative Equivocal Positive
Birth-13 Days Premature Infants (28-36 Weeks) 1st Week of Life Term Infants (>37 Weeks) Cord Blood 2 Days 4 Days 13 Days 5 Months 20 Years >20 Years Pregnancy First Trimester Second Trimester Third Trimester
0.70-27.00 IU/L 2.30-13.20 IU/L 3.20-34.60 IU/L 0.70-15.40 IU/L Not established 1.70-9.10 IU/L 0.70-6.40 IU/L 0.40-5.50 IU/L 0.30-4.50 IU/L 0.50-4.60 IU/L 0.80-5.20 IU/L
Clinical Significance Tissue Transglutaminase Antibody, IgG, is useful in diagnosing gluten-sensitive enteropathies, such as Celiac Sprue Disease, and an associated skin condition, dermatitis herpetiformis in patients who are IgA-deficient.
Tissue, Gastrointestinal Pathology Report 14517X
CPT Code(s): CPT Code(s) varies based on complexity of case as follows: 88300 Surg Path Level I, Gross Examination Only 88302 Surg Path Level II, Gross and Microscopic Examination 88304 Surg Path Level III, Gross and Microscopic Examination 88305 Surg Path Level IV, Gross and Microscopic Examination 88307 Surg Path Level V, Gross and Microscopic Examination 88309 Surg Path Level VI, Gross and Microscopic Examination Includes Preparation of each submitted sample and microscopic interpretation by a pathologist. The fee for service will vary depending upon the number of specimens submitted, the size and complexity of the specimen and difficulty of diagnosis. Specimens requiring a decalcification procedure will be performed at an additional charge (CPT: 88311). Special stains (CPT: 88312 (each stain) or 88313 (each stain)) and/or IHC Immunohistochemistry stains (CPT: 88342 each antibody)) may be ordered at the discretion of the pathologist. These services will be performed at an additional charge. Preferred Specimen(s) Provide all patient information using the Tissue Pathology requisition form Reject Criteria Unlabeled container(s) Leakage of sample during transport Mismatch between name of patient on container(s) and name on test request form Methodology H & E Staining Microscopy Clinical Significance The nature of possible underlying disease states can often be detected by microscopically visualizing histologic changes in tissue biopsies
Clinical Significance For differential diagnosis of primary, secondary, and tertiary hypothyroidism. This assay is a third generation product capable of detecting values as low as 0.01 IU/L. Also useful in screening for hyperthyroidism. This assay allows adjustment of exogenous thyroxine dosage in hypothyroid patients and in patients on suppressive thyroxine therapy for thyroid neoplasia.
186
Gastroenterology Reference Guide
UGT1A1 Gene Polymorphism (TA Repeat) 17813X
CPT Code(s): 83891, 83900, 83909, 83912 This test was developed and its performance characteristics have been determined by Quest Diagnostics. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Preferred Specimen(s) 5 mL whole blood collected in an EDTA (lavender-top) tube Instructions Record the draw time and date on the tube. Ship immediately to maintain sample stability. Transport Container EDTA (lavender-top) Transport Temperature Room temperature Reject Criteria Gross hemolysis Lipemia Clotted blood received frozen Methodology Fluorescent Polymerase Chain Reaction Clinical Significance This assay is intended for selection of colorectal cancer patients who would benefit most and experience the least toxicity from 5-fu, oxalipatin and irinotecan chemotherapy by determining the individual patient genotypes to guide chemotherapy choices in advanced stage colorectal cancer
Vancomycin Resistant Enterococci, Culture 37129X
Part 2: Gastroenterology Test Listing
CPT Code(s): 87081 Includes If culture is positive, identification will be performed at a an additional charge (CPT code(s): 87077 or 87147). Antibiotic susceptibilities are only performed when appropriate (CPT code(s): 87181 or 87184 or 87186). Preferred Specimen(s) Stool in transport medium Transport Container Cary-Blair transport medium or red or blue-cap swab in Amies transport medium Transport Temperature Room temperature Reject Criteria Ova and parasite Para-Pak transport system containing formalin and PVA Frozen or unpreserved stool Expired transport device Methodology Bacteriologic culture, aerobic Special isolation procedure on bile esculin azide agar with 6 mcg/mL vancomycin Identification and antibiotic susceptibility testing when appropriate Clinical Significance Vancomycin resistance in enterococci (VRE) limits antimicrobial therapy. The VRE culture screen permits rapid detection of those patients who are infected or colonized with VRE. An increased risk of VRE infection has been associated with previous vancomycin therapy, severe underlying disease or immunosuppression, and intra-abdominal surgery.
Urea Nitrogen (BUN)
CPT Code(s): 84520 Preferred Specimen(s) 1 mL serum Transport Container Plastic screw-cap vial Transport Temperature Room temperature Reject Criteria Hemolysis Anticoagulants other than heparin Methodology Spectrophotometry Reference Range(s)
294X
Vibrio, Culture
4489X
<1 Month 1-11 Months 1-3 Years 4-19 Years 20 Years
Male 4-12 mg/dL 2-13 mg/dL 3-12 mg/dL 7-20 mg/dL 7-25 mg/dL
Female 3-17 mg/dL 4-14 mg/dL 3-14 mg/dL 7-20 mg/dL 7-25 mg/dL
Clinical Significance Urea is the principle waste product of protein catabolism. BUN is most commonly measured in the diagnosis and treatment of certain renal and metabolic diseases. Increased BUN concentration may result from increased production of urea due to (1) diet or excessive destruction of cellular proteins as occurs in massive infection and fevers, (2) reduced renal perfusion resulting from dehydration or heart failure, (3) nearly all types of kidney disease, and (4) mechanical obstruction to urine excretion such as that caused by stones, tumors, infection, or stricture. Decreased urea levels are less frequent and occur primarily in advanced liver disease and in overhydration.
CPT Code(s): 87046 Includes If culture is positive, identification will be performed at an additional charge (CPT code(s): 87077 or 87140 or 87143 or 87147 or 87149). Antibiotic susceptibilities are only performed when appropriate (CPT code(s): 87181 or 87184 or 87185 or 87186). Preferred Specimen(s) Stool submitted in stool culture transport device Transport Container Cary-Blair transport device Transport Temperature Room temperature Reject Criteria Unpreserved Frozen Expired media Specimens in diapers Parasitology transport vials Methodology Bacterial Culture, Aerobic Routine Isolation and Identification Procedures Antibiotic Susceptibility Testing when appropriate Clinical Significance Vibrio species are usually associated with infection when isolated. Infections caused by Vibrio species fall into three categories: intestinal, wound and systemic infections in persons with pre-existing diseases.
187
Gastroenterology Reference Guide
Vimentin, IHC with Interpretation
CPT Code(s): 88342 Preferred Specimen(s) Formalin fixed paraffin embedded tissue Transport Container IHC specimen transport kit Transport Temperature Room temperature Methodology Immunohistochemical Stain
19279X
Yersinia, Culture
4487X
CPT Code(s): 87046 Includes If culture is positive, identification will be performed at an additional charge (CPT code(s): 87077 or 87140 or 87143 or 87147 or 87149). Antibiotic susceptibilities are only performed when appropriate (CPT code(s): 87181 or 87184 or 87185 or 87186). Preferred Specimen(s) Stool submitted in stool culture transport device Transport Container Cary-Blair transport device Transport Temperature Room temperature Reject Criteria Unpreserved Frozen Expired media Specimens in diapers Parasitology transport vials Methodology Bacterial Culture Aerobic Routine Isolation and Identification Procedures Antibiotic susceptibility testing when appropriate Clinical Significance Yersinia is usually considered a pathogen when isolated. Yersinia enterocolitica and Yersinia pseudotuberculosis may cause gastroenteritis. Yersinia fredericksenii is a potential human pathogen when isolated from extra-intestinal sites.
188
Gastroenterology Reference Guide
Part 3: Test Application and Interpretation
PART 3: TEST APPLICATION AND INTERPRETATION
189
Gastroenterology Reference Guide
190
Gastroenterology Reference Guide
1. ALPHA-FETOPROTEIN (AFP)
Part 3: Test Application and Interpretation
Clinical Use: This test is used to distinguish between seminomatous and nonseminomatous testicular germ cell cancer, monitor therapy and detect recurrence in individuals with nonseminomatous testicular germ cell cancer, determine prognosis in individuals with fulminant hepatitis, monitor therapy in individuals with hepatocellular carcinoma, and monitor hepatitis B carriers for evidence of liver cancer. Clinical Background: AFP is an oncofetal protein produced by the fetal yolk sac and liver. Levels in maternal blood are relatively elevated, with peak concentrations early in the second trimester of pregnancy. After birth, blood concentrations diminish rapidly to adult levels. AFP serves as a marker for testicular nonseminomatous germ cell cancers (embryonal carcinoma, choriocarcinoma, teratomas). The presence of increased AFP levels in blood indicates yolk sac tumor elements. Thus, AFP measurements are useful to distinguish between seminomatous and nonseminomatous testicular germ cell cancer. AFP, as well as lactic dehydrogenase (LDH) and beta-hCG, is recognized by the International Germ Cell Consensus Classification as an independent prognostic factor that can categorize nonseminomatous germ cell tumors into prognostic groups ( J Clin Oncol. 1997;15:594-603). AFP levels are increased in patients with primary hepatocellular carcinoma; increased concentrations may precede clinical evidence of liver cancer. Thus, serial measurements have been recommended in hepatitis B carriers, who have an increased risk of liver cancer. Interpretive Information: AFP concentrations are increased in patients with liver cancer, hepatitis, and
191
Gastroenterology Reference Guide
liver cirrhosis (Table 1). Increased levels in severe hepatitis indicate liver cell regeneration. Thus, the absence of AFP in patients with fulminant hepatitis is considered a poor prognostic sign. AFP concentrations decline to normal levels with effective therapy. Persistently elevated levels suggest residual disease; rising levels suggest disease progression or recurrence. 2. ALPHA-FETOPROTEIN (AFP) AND AFP-L3 Clinical Use: This test is used to determine risk of hepatocellular carcinoma (HCC), diagnose HCC, determine prognosis for individuals with HCC, and monitor HCC therapy.
Table 1. Distribution of AFP
Number of Subjects Healthy Subjects Men Women Malignant Disease Testicular Seminomatous Nonseminomatous Liver Other Other (Women) Nonmalignant Disease Cirrhosis Hepatitis Other Other (Women) Number with AFP Levels <5 IU/mL 118 0 6 14 3 36 18 3 19 5 15 515 IU/mL 1 0 0 8 0 1 0 1 4 0 0 15100 IU/mL 0 0 0 15 2 0 1 0 1 0 1 >100 IU/mL 0 0 0 23 5 3 1 0 0 1 0
119 29 6 60 10 40 20 4 24 6 16
All data were derived from men except where noted. Source: IMMULITE 2000 AFP package insert (DPC).
192
Gastroenterology Reference Guide
Clinical Background: HCC is the fifth most common cancer in the world, with an incidence of >20 per 100,000 in China and eastern Asia and 8 to 10 per 100,000 in the United States.1,2 The most significant risk factors for HCC are chronic infection with hepatitis B or C virus (HBV and HCV, respectively) and hepatic cirrhosis. Individuals at risk for HCC are typically monitored with serial hepatobiliary ultrasounds, as well as other imaging techniques (eg, CT scans), and serial measurements of alphafetoprotein (AFP). AFP is a glycoprotein synthesized by the fetal yolk sac, fetal liver, testicular non-seminomatous germ cell cancers, and malignant hepatic cells. It is the most established marker of HCC. Reliance on AFP levels to detect HCC, however, is confounded by the fact that AFP may be elevated in individuals with chronic HBV or HCV infection and hepatic cirrhosis. The sensitivity and specificity of AFP for diagnosing HCC vary with the population studied and the cut-off value above which AFP is considered positive. They range from 52% to 80% and 90% to 98%, respectively.3 Measurement of an AFP glycoform may prove to be clinically superior to measuring AFP. Three glycoforms, determined by the degree of fucosylation of the N-acetylglucosamine-linked sugar chain, have been identified. The glycoforms are separated in vitro by their ability to bind the lectin Lens culinaris agglutinin (LCA), a carbohydrate binding protein isolated from lentil seeds. AFP-L1 is non-LCA binding and the major glycoform found in individuals with nonmalignant hepatopathy (eg, cirrhosis or chronic HBV infection). AFP-L2 has an intermediate LCA binding capacity and is primarily produced by yolk sac tumors. AFP-L3 is produced by malignant liver cells, binds to LCA with high affinity, and is the major glycoform found in individuals with HCC.4,5
193
Part 3: Test Application and Interpretation
Gastroenterology Reference Guide
AFP-L3 levels 10% are associated with a 7-fold increased risk of developing HCC within the next 21 months and can be elevated 3 to 21 months before HCC is detected by standard imaging techniques.6,7 The diagnostic sensitivity and specificity ranges from 36% to 66% and 77% to 95%, respectively.8,9 Because AFP-L3 is produced by malignant hepatocytes, its measurement helps distinguish non-malignant hepatic disease from HCC.6,8-12 Malignant liver cells that produce AFP-L3 have an increased tendency for rapid growth, early invasion, and intra-hepatic metastasis, thus making AFP-L3 an indicator of poor prognosis in affected individuals.6,8-12 Individuals Suitable for Testing include those at risk for HCC and those with primary or recurrent HCC. Method: This immunofluorescent liquid-phase binding assay simultaneously measures AFP-L3 and non-AFP-L3 forms of AFP. Ion exchange chromatography is used to separate AFP-L3 and the non-AFP-L3 glycoforms, followed by fluorescence detection of the 2 chromatography fractions. Total AFP and the percentage of AFP-L3 are reported. The analytical sensitivity is 0.8 ng/mL for AFP and 0.5% for AFP-L3. There is no interference from vitamins B1, B6, and B12 or from alpha, beta, and gamma interferon; ibuprofen; acetaminophen; and acetylsalicylic acid. 6 Reference Range AFP: 1.6 4.5 ng/mL AFP-L3: 0.5 9.9% These ranges apply to non-pregnant adults only. Interpretive Information: Individuals with an increased percentage of AFP-L3 (AFP-L3%), relative to total AFP present in serum, are at increased risk of
194
Gastroenterology Reference Guide
developing HCC. AFP-L3-secreting hepatocytes have an increased tendency for rapid growth, early invasion, and intra-hepatic metastasis, thus leading to a poorer prognosis in affected individuals. AFP and AFP-L3 levels decline to normal levels with effective therapy; rising levels suggest disease progression or recurrence.5 Not all hepatic cancers secrete AFP or AFP-L3. AFP and AFP-L3% may be elevated in individuals with germ cell tumors and other cancers including those of the gastric and biliary tract, lung, pancreas, and testes.8 AFP may also be elevated in individuals with viral infections, liver diseases other than HCC, women who are pregnant, and children less than 18 months of age. Decreased AFP-L3% may occur if free and conjugated bilirubin are >20 mg/dL.6 Results should be interpreted in conjunction with other laboratory and clinical findings. References
1. Bosch FX, Ribes J, Borras J. Epidemiology of primary liver cancer. Semin Liver Dis. 1999;19:271-285. 2. American Cancer Society: Cancer Facts and Figures 2006. Atlanta, Ga: American Cancer Society, 2006. Available at http://www.cancer.org/ downloads/STT/CAFF2006PWSecured.pdf. Accessed April 19, 2006. 3. Lopez JB, Thambyrajah V, Balasegaram, et al. Appropriate cut-off levels for serum alpha-fetoprotein in hepatocellular carcinoma. Diagnostic Oncology. 1994-1995;4:287-291. 4. Sato Y, Nakata K, Kato Y, et al. Early recognition of hepatocellular carcinoma based on altered profiles of alpha-fetoprotein. N Engl J Med. 1993;328:1802-1806. 5. Li D, Mallory T, Satomura S. AFP-L3: a new generation of tumor marker for hepatocellular carcinoma. Clin Chim Acta. 2001;313:15-19. 6. LBA AFP-L3 Manufacturers Package Insert, Rev. #1/0505DDD00K, Wako Pure Chemical Industries, Ltd., (1/05/05) 7. Kumada T, Nakano S, Takeda I, et al. Clinical utility of Lens culinaris agglutinin-reactive alpha-fetoprotein in small hepatocellular carcinoma: special reference to imaging diagnosis. J Hepatol. 1999;30:125-130. 8. Taketa K, Endo Y, Sekiya C, et al. A collaborative study for the evaluation of lectin-reactive -fetoprotein in early detection of hepatocellular carcinoma. Cancer Res. 1993;53:5419-5423. 9. Oka H, Saito A, Ito K, et al. Multicenter prospective analysis of newly
Part 3: Test Application and Interpretation
195
Gastroenterology Reference Guide
diagnosed hepatocellular carcinoma with respect to the percentage of Lens culinaris agglutinin-reactive -fetoprotein. J Gastroen Hepatol. 2001;16:1378-1383. 10. Tada T, Kumada T, Toyoda H, et al. Relationship between Lens culinaris agglutinin-reactive -fetoprotein and pathological features of hepatocellular carcinoma. Liver Int. 2005;25:848-853. 11. Yoshida S, Kurokohchi K, Arima Keiji, et al. Clinical significance of Lens culinaris agglutinin-reactive fraction of serum -fetoprotein in patients with hepatocellular carcinoma. Int J Oncol. 2002;20:305-309. 12. Toyoda H, Kumada T, Kiriyama S, et al. Prognostic significance of simultaneous measurement of three tumor markers in patients with hepatocellular carcinoma. Clin Gastroenterol Hepatol. 2006;4:111-117.
3. CA 19-9 Clinical Use: This test is primarily used to monitor therapy in individuals with pancreatic cancer. It is also useful for monitoring therapy in selected individuals with gastric and colon cancer. Clinical Background: CA 19-9 is a mucin-glycoprotein derived from a human colorectal carcinoma cell line. It is related to the Lewis blood group protein and is present in epithelial tissue of the stomach, gall bladder, pancreas, and prostate. Blood levels may be increased modestly in patients with pancreatitis, biliary tract disease, inflammatory bowel disease, and cystic fibrosis. The distribution of CA 19-9 in healthy individuals, benign disorders, and malignant disease is reflected in Tables 2 and 3. Interpretive Information: CA 19-9 concentrations are increased in patients with pancreatic, gastric, and colon cancer as well as in some non-malignant conditions (Table 2). Increasing levels generally indicate disease progression, whereas decreasing levels suggest therapeutic response. 4. CA 72-4 Clinical Use: This test is used to monitor therapy and
196
Gastroenterology Reference Guide
Table 2. Distribution of CA 19-9
Patient Group Healthy Subjects Benign Disease Pancreatic Inflammatory Bowel Disease Polyps Other Diseases Malignant Disease Pancreatic Adenocarcinoma Gastric Adenocarcinoma Colorectal Adenocarcinoma Advanced Localized Inactive 164 25 21 46 8 0 80 24 79 50 21 56 27 219 0 2 0 2 Number of Patients 1020 % with CA 19-9 >37.0 U/mL 0.6
Part 3: Test Application and Interpretation
Reference: DelVillano BC, et al. Clin Chem 1983;29:549-552.
detect recurrence in patients with CA 72-4-positive cancer (eg, gastrointestinal cancers). Clinical Background: CA 72-4 (TAG-72) is a highmolecular-weight mucin glycoprotein derived from a tumor cell line. It is most useful as a marker for gastrointestinal cancer, but blood levels may be increased in other malignancies (eg, lung cancer) and in non-malignant disorders involving gastrointestinal tissues. Method: This enzyme immunoassay uses a capture antibody specific for tumor associated glycoprotein 72 (TAG-72) and a biotin-conjugated detection antibody that binds to a different epitope of the TAG72 molecule. Addition of a streptavidin-labeled fluorescent tag initiates a fluorescent signal that is measured in a flow cytometer.
197
Gastroenterology Reference Guide
Table 3. Distribution of CA 19-9
Patient Group Nonmalignant Disease Abdominal Pain Jaundice Malabsorption Pancreatic Renal Failure Malignant Disease Pancreas 37 89 86
Reference: Steinberg WM, et al. Gastroenterology. 1986;90:343-349.
Number of Patients 34 58 7 48 10
% with CA 19-9 >37 U/mL >75 U/mL 3 19 0 19 20 3 12 0 6 0
Interpretive Information: Elevated levels (4 U/mL) are associated with multiple tumor types and some non-malignant disorders (Table 4). Increasing levels are associated with tumor progression, whereas decreasing levels are associated with therapeutic response. 5. CARCINOEMBRYONIC ANTIGEN (CEA) See section 8.2. 6. CD117, IHC Clinical Use: This test is used to determine eligibility for Gleevec' (imatinib mesylate; STI571) treatment in patients with c-kit-positive gastrointestinal stromal tumors (GISTs). Clinical Background: The transmembrane glycoprotein c-kit (CD117), a member of the receptor tyrosine kinase subclass III family, has been implicated in a number of malignancies: GISTs, mast cell diseases, acute myeloid leukemia, small cell lung carcinoma, and Ewings sarcoma. Imatinib mesylate,
198
Gastroenterology Reference Guide
Table 4. Distribution of CA 72-4
Subject Group Number of Subjects 744 75 59 17 199 77 104 41 165 28 60 61 16 92 15 66 50 25 29 % with CA 72-4 in Indicated Range >6.0 U/mL >10.0 U/mL 3.5 0.5 5 8 0 42 55 38 54 16 36 17 11 19 24 53 12 20 4 3 1 3 0 34 47 29 39 12 25 10 7 19 20 40 11 10 0 3
Part 3: Test Application and Interpretation
Disease Free Benign Disease Stomach Colorectal Miscellaneous Malignant Disease Gastric Stage IV Colorectal Stage IV Lung Adenocarcinoma Squamous Cell Small Cell Non-Small Cell Ovarian Stage IV Breast Advanced Prostatic Squamous Sarcoma
Reference: Gero EJ, Colcher D, Ferroni P, et al. J Clin Lab Analysis. 1989;3:360-369.
a tyrosine kinase inhibitor, appears to be effective in treating GISTs and other tumors that express c-kit. Therefore, testing tumor tissue for c-kit immunoreactivity can help predict sensitivity to tyrosine kinase inhibitor therapy. Method: This immunohistochemical (IHC) assay uses a polyclonal rabbit anti-human CD117/c-kit antibody, along with the Dako EnVision' + Peroxidase detection kit (DakoCytomation), to detect CD117/c-kit
199
Gastroenterology Reference Guide
expression on tissue sections and cell preparations. The EnVision+ detection system is a 2-step IHC staining technique employing a horseradish peroxidase-labeled polymer conjugated with secondary antibodies.
This test was developed and its performance characteristics determined by Quest Diagnostics Nichols Institute. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test.
Interpretive Information: A positive result indicates tumor expression of CD117/c-kit and eligibility for Gleevec therapy. 7. CELIAC DISEASE COMPREHENSIVE PANEL Clinical Use: This test is used to diagnose celiac disease, differentiate celiac disease from irritable bowel syndrome, and monitor adherence to a glutenfree diet in patients with celiac disease. Clinical Background: Celiac disease is caused by an immune response to gluten in genetically susceptible individuals. Patients may develop partial to complete villous atrophy of the small intestine, crypt hyperplasia, and lymphocytic infiltration of the epithelium and lamina propria. This disease is more common than once thought, affecting as many as 1 in 133 not-at-risk Americans (ie, those without family history or gastrointestinal symptoms); rates are even higher among first- and second-degree relatives of patients.1 Untreated, celiac disease may be accompanied by progression of villous atrophy and development of other autoimmune diseases (eg, thyroid disease and insulin-dependent diabetes mellitus), osteoporosis, and neoplasia, including T-cell lymphoma and adenocarcinoma of the small intestine.
200
Gastroenterology Reference Guide
Diagnosis is based on biopsy of the small intestine, but serologic assays help identify patients who require this invasive procedure. Tissue transglutaminase (tTG; IgA) antibody is an excellent first-line marker, with high sensitivity and specificity in untreated individuals.2 The endomysial antibody (EMA; IgA) assay has high specificity for celiac disease and is used to confirm positive IgA anti-tTG results. Although this panel tests for EMA only when IgA anti-tTG results are positive, EMA testing can be ordered separately if the anti-tTG result is negative but clinical suspicion remains high. Some patients with limited villous atrophy have been reported to lack EMA and tTG antibodies; testing for IgA antigliadin antibody (AGA) may help detect celiac disease in such patients.3 Total serum IgA is measured to identify selective IgA deficiency, present in about 2% to 10% of celiac disease patients. Such patients would have negative results on IgA anti-tTG and EMA assays but may have positive IgG anti-tTG results. Because levels of anti-tTG and EMA tend to wane in the absence of gluten ingestion, these markers are useful to monitor adherence to a gluten-free diet. Method: This panel includes tests for tTG IgA, gliadin IgA, and total IgA. Additional tests are performed, at an additional charge, as follows: An EMA screen is performed when the tTG IgA is positive, and, if positive, an endomysial antibody titer is performed. Further, a tTG IgG test is performed when the total IgA is low. References
1. Fasano A, Berti I, Gerarduzzi T, et al. Prevalence of celiac disease in atrisk and not-at-risk groups in the United States: a large multicenter study. Arch Intern Med. 2003;163:286-292. 2. Farrell RJ, Kelly CP. Diagnosis of celiac sprue. Am J Gastroenterol. 2001;96:3237-3246. 3. Green PH, Jabri B. Coeliac disease. Lancet. 2003;362:383-391.
Part 3: Test Application and Interpretation
201
Gastroenterology Reference Guide
8. COLORECTAL CANCER 8.1 Laboratory Support of Diagnosis and Management Clinical Background: Colorectal cancer (CRC) is the second leading cause of cancer death in the United States, with projections of 55,000 deaths and 149,000 new cases diagnosed in 2006.1 About three-quarters of CRC cases are sporadic, apparently resulting from environmental factors, diet, and aging (Table 5). The remaining 25% are familial or inherited. Familial CRC is not well understood and is characterized by increased risk of CRC and an unclear pattern of inheritance. Inherited CRC, on the other hand, exhibits a clear pattern of inheritance and includes hereditary nonpolyposis colorectal cancer (HNPCC) and familial adenomatous polyposis (FAP) as well as Table 5. Probability of Developing Colorectal Cancer2,3
Etiology Sporadic CRC Familial CRC % of New Cases 75 15 to 20 Probability of Developing CRC 4% by age 79 1 first-degree relative with CRC: 9% by age 79 More than 1 first-degree relative with CRC: 16% by age 79 1 first-degree relative with CRC before age 45: 15% by age 79 1 first-degree relative with colorectal adenoma: 8% by age 79 80% by age 75 90% by age 45 Attenuated FAP: 69% by age 80 MYH-associated neoplasia: unknown Peutz-Jeghers syndrome: 39% by age 64 Juvenile polyposis syndrome: 17% to 68% by age 60
Hereditary CRC HNPCC FAP Other
5 1 Rare
CRC, colorectal cancer; HNPCC, hereditary nonpolyposis colorectal cancer; FAP, familial adenomatous polyposis.
202
Gastroenterology Reference Guide
the more rare MYH-associated neoplasia, PeutzJeghers, and juvenile polyposis syndromes. Determining the type of CRC has important implications for screening and follow-up of patients and family members. Molecular Characteristics of CRC The natural progression of CRC from benign adenoma to carcinoma to metastatic disease is associated with 1 of 2 distinct molecular pathways. The most common pathway, chromosomal instability, occurs in 80% to 85% of cases and is characterized by allelic loss (loss of heterozygosity), chromosomal rearrangements, or loss of whole chromosomes. Such characteristics are associated with most sporadic CRCs and FAP. The remaining 15% to 20% are associated with impairment of nucleotide mismatch repair (MMR) that normally occurs during DNA replication or recombination. In tumor tissue, MMR defects are characterized by microsatellite instability (MSI), defined as insertions or deletions of nucleotides within repeated DNA nucleotide sequences known as microsatellites. The MMR defect pathway is exemplified by HNPCC, an autosomal dominant syndrome also known as Lynch syndrome. Individuals with HNPCC typically inherit 1 copy of a defective MMR allele; subsequent somatic mutations may cause loss of the normal allele, leading to defective DNA repair. Approximately 51% of the mutations occur in MLH1, 38% in MSH2, 10% in MSH6, and 2% in PMS2.4 Germline mutation of the adenomatous polyposis coli (APC) gene, a tumor suppressor gene, causes FAP, an autosomal dominant disorder with a prevalence of approximately 1 in 8000.
Part 3: Test Application and Interpretation
203
Gastroenterology Reference Guide
Screening for CRC The American Cancer Society (ACS) recommends screening average-risk individuals with one of several options beginning at age 50 years (Table 6).5 Screening options should be chosen based on individual risk, personal preference, and access. Of these screening tests, the fecal occult blood test (FOBT) or fecal immunochemical test (FIT) are the only non-invasive tests; FOBT has led to the detection and surgical excision of precancerous polyps thereby significantly reducing the incidence of CRC and related mortality.6 Flexible sigmoidoscopy is also associated with reduced mortality for CRC,7 and combining FOBT with flexible sigmoidoscopy is more effective than either test alone.5 Although less commonly used, double contrast barium enema has the advantage of examining the entire colon, but is less sensitive than colonoscopy in detecting polyps.7 The American Gastroenterology Association recommends that high-risk individuals be screened at a younger age and that screening be performed more frequently (Table 6).7 Differential Diagnosis of CRC and Risk Assessment Because HNPCC is the most common of the hereditary CRCs, criteria to identify families with the disorder have been developed by the National Cancer Institute (Bethesda guidelines)8 and the International Collaborative Group on HNPCC (Amsterdam criteria).9 HNPCC is characterized by a high lifetime cancer risk and early age at onset (mean 45 years). Because HNPCC progresses rapidly, early detection is critical for affected individuals and their first-degree relatives; close surveillance of affected family
204
Gastroenterology Reference Guide
Table 6. CRC Screening Recommendations
Population Average-risk men and women* Screening Options Age to Begin Screening Annual FOBT or FIT 50 years Flexible sigmoidoscopy every 5 years Annual FOBT and flexible sigmoidoscopy every 5 years Double contrast barium enema every 5 years Colonoscopy every 10 years Same as for those with 50 years average risk Same as for those with 40 years average risk Same as for those with average risk Colonoscopy every 5 years 40 years 40 years or 10 years younger than the earliest diagnosis in the family, whichever comes first 20 to 25 years or 10 years younger than the earliest diagnosis in the family, whichever comes first 10 to 12 years
Part 3: Test Application and Interpretation
1 second- or any thirddegree relative with CRC First-degree relative of an individual with CRC or AP at age 60 years 2 second-degree relatives with CRC 2 first-degree relatives with CRC, or 1 first-degree relative with CRC or AP at age <60 years High risk for HNPCC (firstdegree relative with HNPCC or carrier of known MMR gene mutation) High risk for FAP (firstdegree relative with FAP or carrier of known APC gene mutation)
Colonoscopy every 1 to 2 years
Annual sigmoidoscopy
FOBT, fecal occult blood test; FIT, fecal immunochemical test; AP, adenomatous polyp; HNPCC, hereditary nonpolyposis colorectal cancer; FAP, familial adenomatous polyposis; APC, adenomatous polyposis coli gene. *Recommended by the American Cancer Society5 Third-degree relatives include great-grandparents and cousins. Recommended by the American Gastroenterology Association.7
members can reduce overall mortality by 65%.10 Additionally, women with HNPCC are at high risk for endometrial cancer (40% to 70%) and ovarian cancer (10% to 12%),4 and early detection of HNPCC or familial MMR mutations allows close monitoring for these cancers. FAP is characterized clinically by the presence of
205
Gastroenterology Reference Guide
hundreds to thousands of colorectal polyps identified at an early age (<30 years). FAP will progress to colon cancer unless colectomy is performed. It is also associated with an increased lifetime risk of other cancers, including duodenal cancer (5% to 11% risk).11 Selection of Therapy for Patients with CRC Pharmacogenomics, the study of genetic influences on drug response, is becoming increasingly important in the selection of therapeutic agents. Genetic polymorphisms are partially responsible for inter-patient variability in drug efficacy and/or toxicity; detecting such polymorphisms prior to treatment may help optimize drug selection and dosage. Individuals Suitable for Testing Screening, Differential Diagnosis, and Risk Assessment Individuals suitable for testing include those recommended for CRC screening (Table 6), those with CRC who meet any of the Bethesda criteria (Table 7), those who meet the Amsterdam II criteria (Table 8), and first-degree relatives of individuals with a known MMR gene mutation. Determine Prognosis, Select and Monitor Therapy Individuals suitable for testing include those diagnosed with CRC. Test Availability Table 9 lists tests used to assess risk, screen, diagnose, determine prognosis, and select and monitor therapy for CRC.
206
Gastroenterology Reference Guide
Table 7. Bethesda Guidelines for Testing Colorectal Tumors for MSI8
Colorectal tumors should be tested for MSI in individuals meeting any of the following: CRC diagnosed at age <50 years Presence of synchronous CRC (multiple CRCs 6 months after initial tumor removal), metachronous CRC (CRC recurrence >6 months after initial tumor removal), or other HNPCC-associated tumors* CRC with the MSI-H histology diagnosed at age <60 years CRC in 1 first-degree relative with an HNPCC-related tumor with 1 of the cancers diagnosed at age <50 years CRC diagnosed in 2 first- or second-degree relatives with HNPCC-related tumors
*Endometrial, stomach, ovarian, pancreas, ureter and renal pelvis, biliary tract, and brain tumors, sebaceous gland adenomas and keratoacanthomas in Muir-Torre syndrome, and carcinoma of the small bowel. Presence of tumor infiltrating lymphocytes, Crohns-like lymphocytic reaction, mucinous/signet-ring differentiation, or medullary growth pattern.
Part 3: Test Application and Interpretation
Test Selection and Interpretation FOBT Screening In 2003 the ACS guidelines for stool blood tests were expanded to include fecal immunochemical tests (FITs).5 The traditional guaiac-based FOBTs (eg, Hemoccult') suffer from false-positive results due to ingestion of red meat, some raw fruits and uncooked vegetables, non-steroidal anti-inflammatory drugs, and aspirin. Additionally, ingestion of vitamin C (>250 mg/day) from supplements or citrus fruits may lead to false-negative results. Thus, dietary and medication restrictions are required prior to sample collection. Conversely, FITs such as InSure' are more specific and consequently do not require dietary and Table 8. Amsterdam II Criteria for Identifying Families with HNPCC9
3 relatives with an HNPCC-associated tumor* 1 is a first-degree relative of the other 2 2 successive generations affected 1 diagnosed at <50 years of age FAP should be excluded in the patients with CRC Tumor should be verified by pathologic examination
FAP, familial adenomatous polyposis. *Defined in the first footnote of Table 7.
207
Gastroenterology Reference Guide
Table 9. Tests Available for Diagnosis and Management of Colorectal Cancer
Test Code Assay Screen 11290X Fecal Globin, Immunochemistry (InSure) Method Description Immunochemistry targeting globin portion of hemoglobin; colorimetric detection Oxidation of guaiac by hemoglobin peroxidase; colorimetric detection Hematoxylin and eosin stain; microscopy Clinical Use Screen for lower GI bleeding associated with CRC, adenomas, polyps, and other lower GI conditions Screen for upper and lower GI bleeding
Not Applicable
Hemoccult
Diagnose or Assess Risk 14517 Tissue, Gastrointestinal Pathology Report 14989X Microsatellite Instability (MSI), HNPCC*
Diagnose CRC
14986X
16051X
Multiplex PCR amplification of 5 NCIrecommended microsatellites; fluorescent fragment analysis MLH1 and MSH2 PCR amplification of Mutations, HNPCC* MMR gene regions; DNA sequencing MLH1 and MSH2 Multiplex PCR Mutations (Deletion amplification of MMR and Duplication), gene regions; fluorescent HNPCC* fragment analysis MSH6 Mutation, HNPCC* PCR amplification of MMR gene regions; DNA sequencing
Differential diagnosis of CRC; assess risk of HNPCC in patients with CRC
Confirmation of clinical diagnosis of HNPCC; identification of familial mutations in affected individuals
14982X
14984X 14981X
14983X
MLH1 Mutation, One Exon, HNPCC* MSH2 Mutation, PCR amplification of One Exon, HNPCC* MMR gene regions; DNA sequencing MSH6 Mutation, One Exon, HNPCC*
Identify MMR gene mutation in family members when the family mutation is known
208
Gastroenterology Reference Guide
Table 9. Tests Available (Continued)
Test Code Assay Determine Prognosis 978X Carcinoembryonic Antigen (CEA) 14603X Chromosome Analysis, Solid Tumor 36158X DNA Cell Cycle Analysis, Paraffin Block 14989X Microsatellite Instability (MSI), HNPCC* Method Description Immunochemiluminometric assay Culture, microscopy, karyotype Flow cytometry Clinical Use
Part 3: Test Application and Interpretation
Predict prognosis pretreatment Assess prognosis in patients with CRC Predict overall survival in patients with CRC Predict overall survival in patients with CRC
36162X
p53 Oncoprotein*
Multiplex PCR amplification of 5 NCIrecommended microsatellites; fluorescent fragment analysis Immunohistochemical assay Hematoxylin and eosin stain; microscopy
14517
Tissue, Gastrointestinal Pathology Report Select and Monitor Therapy 4698X CA 19-9 15583X CA 72-4
Predict recurrence-free survival in patients with CRC Predict survival in patients with CRC
Immunochemiluminometric assay EIA, fluorometric quantitation
Monitor therapeutic response; detect residual disease, detect recurrence
978X 16109X
Carcinoembryonic Antigen (CEA) Colorectal Cancer (CRC) Pharmacogenomic Panel*
Immunochemiluminometric assay PCR amplification followed by fluorescent fragment analysis or single Includes UGT1A1, nucleotide primer TYMS, XRCC1, ERCC1, extension
GSTP1, XPD, and DPYD gene analysis.
15538X
Dihydropyrimidine Dehydrogenase (DPYD) Gene Mutation Analysis*
PCR amplification of target regions followed by hybridization with mutant and wild-type oligonucleotides
Guide chemotherapy selection (5-fluorouracil, oxaliplatin, and irinotecan) to minimize toxicity in advanced CRC; predict survival in patients receiving these chemotherapeutic drugs Predict toxicity from pyrimidine-based chemotherapeutic agents (5-fluorouracil, capecitabine)
209
Gastroenterology Reference Guide
Table 9. Tests Available (Continued)
Test Code Assay 10920X Epidermal Growth Factor Receptor (EGFR), ELISA 10479X Epidermal Growth Factor Receptor (EGFR), IHC 19041X FISH, EGFR* 17813X UGT1A1 Gene Polymorphism (TA Repeat)* Method Description Immunoassay Clinical Use
Immunohistochemical assay Fluorescence in situ hybridization PCR amplification of promoter region of UGT1A1; fluorescent detection
Determine suitability for EGFR-targeted drugs
Predict irinotecan toxicity; assist in selecting initial dosage for patients with metastatic or recurrent CRC
CRC, colorectal cancer; GI, gastrointestinal; HNPCC, hereditary nonpolyposis colorectal cancer; NCI, National Cancer Institute; MMR, mismatch repair. *This test was developed and its performance characteristics determined by Quest Diagnostics Nichols Institute. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. See reference 12 for more details. This test is performed pursuant to a license agreement with Roche Molecular Systems Inc. This test was performed using a kit that has not been approved or cleared by the FDA. The analytical performance characteristics of this test have been determined by Quest Diagnostics Nichols Institute. This test should not be used for diagnosis without confirmation by other medically established means.
medication restrictions.13 Furthermore, InSure is more specific for occult bleeding in the colon and rectum thus making it less likely that bleeding is from the upper gastrointestinal tract.13 In a recent clinical study comparing InSure with a guaiac-based FOBT, InSure had a better true-positive rate for early stage CRC (92.3% vs 30.8%, n = 13 stage I patients), all stages of CRC (87.5% vs 54.2%, n = 24), and significant adenoma (42.6% vs 23.0%, n = 61).14 False-positive rates were 3%. Positive FOBT or FIT results generally reflect the presence of blood in the stool and may be associated with CRC. The ACS recommends colonoscopy as follow-up to a positive test; flexible sigmoidoscopy or repeat testing are not indicated.5 Negative results do
210
Gastroenterology Reference Guide
not rule out CRC; false-negative results can occur because of uneven distribution of blood in the feces or intermittent bleeding. Differential Diagnosis of CRC and Risk Assessment of Relatives Since patients with CRC present with non-specific symptoms (eg, change in bowel habit, unexplained weight loss, abdominal pain, mucous discharge, or rectal bleeding) or with no symptoms, diagnosis is based on colonoscopy and pathologic examination of the suspicious tissue. Once CRC is diagnosed, it is important to determine if the cancer is hereditary. If HNPCC is diagnosed, or if family members have an HNPCC-associated mutation, increased surveillance is required. Figure 1 depicts a suggested testing algorithm for the differential diagnosis of CRC and risk assessment of family members. Details regarding these tests follow. Microsatellite Instability The diagnosis of HNPCC begins with consideration of MSI testing. Colorectal tumors should be tested for MSI when any of the Bethesda criteria are met (Table 7). In a study of 1222 patients with CRC, combining Bethesda criteria with MSI testing was more effective in determining which patients should be tested for MMR mutations than the use of either alone.15 The combination resulted in a sensitivity of 81.8%, a specificity of 98.0%, and an overall accuracy of 97.9% for identifying patients with MLH1 or MSH2 mutations. Furthermore, combining Bethesda criteria with MSI testing was more cost effective. Results are reported as MSI-high (MSI-H), MSI-low (MSI-L), or negative for MSI (microsatellite stable,
211
Part 3: Test Application and Interpretation
Gastroenterology Reference Guide
Patient with CRC who meets 1 Bethesda criterion (Table 7)
Family Member Risk Assessment
Microsatellite Instability (MSI) testing [14989X]* Family MMR mutation is unknown and Amsterdam II criteria (Table 8) are met
MSI not detected
MSI-L detected
MSI-H detected HNPCC diagnosis likely
Family MMR mutation is known
HNPCC diagnosis unlikely Consider MLH1, MSH2, MSH6 mutation testing if strong suspicion of HNPCC
MLH1 and MSH2 testing (mutation analysis [14986X] and deletion/duplication [16051X])
Single exon mutation testing (MLH1 [14984X], MSH2 [14981X], or MSH6 [14983X])
Mutation detected
No mutation detected HNPCC less likely
No mutation detected Average risk of CRC
Patient with CRC: HNPCC diagnosis confirmed
Screened family member: high risk of HNPCC
MSH6 mutation testing [14982X]
Mutation detected High risk of HNPCC
Mutation detected
No mutation detected HNPCC unlikely
*Test codes are included in brackets.
Figure 1. Differential diagnosis of CRC and risk assessment for HNPCC 8,11
MSS). A MSI-H result is reported if 2 of the 5 National Cancer Institute-recommended markers show instability and requires follow-up with MMR gene mutation testing (Figure 1). Although an MSIH result is the hallmark of HNPCC, it is also found in 15% to 20% of sporadic CRC cases.11 An MSI-L result, reflecting instability in 1 marker, is found in <10% of HNPCC cases and in most MSI-positive sporadic CRCs. Since MSI results do not rule out
212
Gastroenterology Reference Guide
HNPCC, MMR gene mutation testing should be considered regardless of MSI status in families with a strong suspicion of HNPCC.8 MMR Gene Mutation Testing For patients with suspected HNPCC and no known familial mutation, begin MMR gene testing with MLH1 and MSH2. MLH1/MSH2 mutation testing should include DNA sequence changes, which are more commonly identified, and also deletion/ duplication mutations, which are found in 27% of families with HNPCC.16 If no MLH1/MSH2 mutations are detected, MSH6 mutation testing should be performed (Figure 1). Detection of an MMR gene mutation in a patient with CRC is diagnostic of HNPCC. Failure to identify a relevant mutation makes HNPCC unlikely but does not rule it out. Once a diagnosis of HNPCC is established and an MMR gene mutation is identified, first-degree relatives should be tested for the mutation using a single-exon assay (Table 9; Figure 1). Relatives who carry the family mutation are at high risk for HNPCC and should be monitored closely (Table 6). For firstdegree relatives of HNPCC patients who meet the Amsterdam criteria but do not know the family mutation, MLH1 and MSH2 mutation testing should be performed first; MSH6 mutation testing should then be considered for patients with negative results (Figure 1). Because not all HNPCC families meet the Amsterdam criteria, MMR mutation testing should also be considered when there is a strong suspicion of HNPCC.3,16 Detection of an MMR gene mutation is associated with high risk for HNPCC, whereas negative results are consistent with average risk but do not rule out HNPCC.
Part 3: Test Application and Interpretation
213
Gastroenterology Reference Guide
Determining Prognosis Tumor Staging Tumor staging using either the American Joint Committee on Cancer (AJCC) system17 or the Dukes system has historically been a powerful tool for determining the prognosis of patients with CRC. Tumor staging reflects the extent of CRC and provides prognostic information, as demonstrated by the data in Table 10. The data were derived by correlating AJCC stage with survival in more than 119,000 colon cancer patients.18 Interestingly, stage IIIa CRC had a better prognosis than stage IIb (P <0.001); this may be due to the current practice of initiating chemotherapy for patients with stage III but not stage II disease.18 The Dukes stage that corresponds to the AJCC stage is provided to give the reader estimated survival times for the various Dukes stages.
Table 10. CRC Prognosis by Disease Stage18
AJCC Stage I Ila IIb IIIa IIIb IIIc IV Dukes Stage A B B C C C D TNM T1 or T2, N0, M0 T3, N0, M0 T4, N0, M0 T1 or T2, N1, M0 T3 or T4, N1, M0 Any T, N2, M0 Any T, Any N, M1 Pathologic Description 5-year Survival* 93.2% 84.7% 72.2% 83.4% 64.1% 44.3% 8.1%
Cancer limited to submucosa or muscularis Cancer extends into serosa Cancer extends through serosa Cancer extends to regional lymph nodes Cancer extends beyond the muscularis Cancer extends to increased number of lymph nodes Distant metastases (eg, liver, lung, bone)
AJCC, American Joint Committee on Cancer; TNM, tumor-node-metastasis. *Colon cancer specific.
214
Gastroenterology Reference Guide
Microsatellite Instability
Part 3: Test Application and Interpretation
Tissue testing for MSI may be used to assess prognosis independent of CRC tumor stage. In a meta-analysis combining the results from 32 studies including 7,642 cases, overall survival was more favorable with MSI than with MSS tumors (hazard ratio [HR] = 0.65, 95% confidence interval [CI] 0.590.71).19 The survival advantage of patients with MSI tumors was maintained when HRs were pooled for stage II and stage III CRC patients (n = 2,935). However, the use of microsatellite status to assess prognosis has not been investigated in a prospective clinical trial. DNA Cell Cycle Analysis DNA cell cycle analysis is used to determine ploidy, specifically aneuploidy (an abnormal complement of chromosomes), in CRC tissue. Because of conflicting data on the association of aneuploidy with a poor outcome, the American Society of Clinical Oncology (ASCO) does not recommend routine testing for ploidy.20 p53 Oncoprotein Overproduction of p53 oncoprotein serves as a surrogate marker of p53 oncogene mutation, which is a common event in tumorigenesis. Although some studies have found an association between p53positive tumor tissue and poor prognosis in patients with CRC, results have been inconsistent.20 Carcinoembryonic Antigen (CEA) Elevated pretreatment CEA levels (>5 ng/mL) are associated with poor prognosis and predict eventual tumor recurrence.20
215
Gastroenterology Reference Guide
Selecting and Monitoring Therapy Carcinoembryonic Antigen (CEA) A CEA level, if elevated preoperatively, can be used to detect residual disease following curative intent surgery in patients with primary CRC. If tumor removal was complete, the CEA level should return to normal within 6 weeks following surgery; persistently elevated levels suggest residual or metastatic disease.21 Approximately 50% of patients who undergo surgery with curative intent develop recurrent or metastatic disease.21 Serial CEA monitoring post surgery is useful for detecting these conditions: the sensitivity and specificity are 80% and 70%, respectively.21 Sensitivity is higher (100%) for detecting liver metastasis, which accounts for about 80% of CRC recurrences, than for detecting locoregional recurrence (sensitivity 60%).21 ASCO recommends testing every 3 months for at least 3 years following diagnosis of stage II or III disease, providing the patient is a candidate for further surgery or systemic therapy.20 While stable or falling CEA levels suggest no disease progression, elevated levels, if confirmed by retesting, are associated with disease progression and warrant reevaluation for recurrent and metastatic disease. Stage IV CRC (distant metastases) and locoregional recurrence may be treated with surgical resection, chemotherapy, or radiation, depending on the site and extent of the metastases or recurrence. In this setting, CEA levels are useful for evaluating the success of surgical removal of the metastasis and for monitoring chemotherapy. ASCO considers CEA to be the marker of choice for monitoring chemotherapy and recommends measurement
216
Gastroenterology Reference Guide
before treatment and every 1 to 3 months during treatment.20 While decreases in CEA levels during chemotherapy suggest a favorable treatment response, persistently rising values above pretreatment levels suggest disease progression. Rising values should prompt reevaluation and consideration of alternative treatment.20,21 However, transient increases in CEA can occur with chemotherapy that are not associated with disease progression (eg, within 2 weeks following 5-FU-based treatment and within 4 to 6 weeks after oxaliplatin therapy).20,22 Thus, timing of sample collection for CEA determination should be considered in context with the therapy prescribed. Although there is no universally accepted definition of what constitutes a clinically significant change in CEA levels, guidelines have been proposed: 1) 30% increase over the previous value, confirmed by a second sample collected within 1 month; or 2) >15% increase maintained over 3 successive samples.21 Since 25% of patients with CRC do not have elevated levels of CEA, monitoring treatment with alternative tumor markers such as CA 19-9 or CA 72-4 may be of benefit.21 ASCO does not recommend the routine use of these markers, however.20 Epidermal Growth Factor Receptor (EGFR) Cetuximab (Erbitux') is a recombinant, human/mouse chimeric monoclonal antibody that blocks signal transduction and cell growth when bound to the extracellular domain of EGFR. Thus, EGFR expression was assumed to be a prerequisite for response to cetuximab, and the clinical trials conducted to demonstrate drug efficacy required a positive EGFR immunohistochemical (IHC) stain for patient inclusion. Later studies, however, showed that
217
Part 3: Test Application and Interpretation
Gastroenterology Reference Guide
patients with EGFR-negative tumors might also respond. 23,24 Nevertheless, the Erbitux package insert states that a positive EGFR IHC stain is a prerequisite for use of the drug.25 Clinical trials have shown no correlation between efficacy of treatment and the intensity (ie, 1+ to 4+) of EGFR IHC staining.26 Determination of EGFR gene copy number by FISH or EGFR protein expression by ELISA (using serum rather than tissue) have been proposed as alternatives to IHC testing. Although preliminary results suggest FISH results predict response to cetuximab-based therapy,27 confirmatory studies are required. Pharmacogenomic Testing The goal of pharmacogenomic testing is to improve patient outcome by enabling optimal patient-specific drug selection and dosing. Theoretically, genetic markers can identify patients who will 1) respond to a specific medication using standard doses, 2) respond only with increased doses, or 3) have a toxic reaction that either requires a reduced dose or selection of an alternative therapy. To date, most studies correlating genetic markers with CRC treatment outcomes are retrospective, derived from small sample sizes, and often originate from a single research group. The information presented below and in Table 11 summarizes the available literature and classifies the clinical utility of each test. 5-Fluorouracil (5-FU) DPYD Polymorphism Deficiency of dihydropyrimidine dehydrogenase (DPD), the rate-limiting enzyme in the catabolism of pyrimidine-based chemotherapeutic agents (eg, 5-FU and capecitabine), has been linked to severe myelosuppression and death in patients treated with standard doses.28 Approximately 50% of DPD218
Gastroenterology Reference Guide
Table 11. Prediction of Chemotherapy Outcome in Patients Treated for Advanced CRC
Therapy 5-Fluorouracil Test DPYD IVS14+1GA TYMS 3'-UTR TYMS 5'-UTR Favorable Result Negative for IVS14+1GA Negative for 6bp deletion 2R (2 tandem repeats of a 28bp sequence) Outcome Clinical Predicted Utility of Test* Reduced 2 toxicity28-30 Reduced disease 3 progression31,32 Improved 3 response rate33 Improved 3 survival31,32 Reduced 1 toxicity34-36 Improved 2 survival32,37 Improved 2 survival32,38 Reduced disease 3 progression32 Reduced toxicity39 3 Improved 2 survival32,40 Reduced disease 3 progression32,40 Improved 3 response rate40 Improved 3 response rate41
Part 3: Test Application and Interpretation
Irinotecan Oxaliplatin
UGT1A1 TA repeat ERCC1-118 GSTP1 Ile105Val
Negative for TA repeat Negative for C118T Val105Val
XPD-751
Negative for Lys751Gln
XRCC1 Arg399Gln
Negative for Arg399Gln
UTR, untranslated region; bp, base pair. *1, currently defined; 2, potential for future use; 3, not currently defined.
deficient patients have 1 or 2 copies of a DPYD allele containing the IVS14+1GA mutation; roughly onethird of patients with grade 3 or 4 toxicity due to 5FU treatment have this mutation.28-30 Consequently, presence of this mutation suggests an increased risk of severe myelosuppression in patients
219
Gastroenterology Reference Guide
treated with 5-FU; however, a negative test result (lack of mutation) does not rule out this risk. TYMS Polymorphism 5-FU exerts its effect primarily by inhibiting thymidine nucleotide production catalyzed by thymidylate synthase (TS). Polymorphisms in the 5'and 3'-untranslated regions (UTRs) of the gene that encodes TS (TYMS) influence the activity of the enzyme and may, therefore, affect patient response to 5-FU-based treatment as detailed in Table 11.31-33 Irinotecan UGT1A1 Polymorphism Irinotecan (Camptosar') therapy can result in doselimiting toxicity manifesting as neutropenia, diarrhea, and asthenia. The risk of toxicity can be assessed by testing for an additional TA repeat in the promoter region of the gene encoding uridine diphosphate glucuronosyltransferase 1A1 (UGT1A1).34,35 This hepatic enzyme metabolizes SN38, the active form of irinotecan and the cause of drug toxicity. The presence of an additional TA repeat (ie, positive for TA repeat) is consistent with reduced UGT1A1 enzyme activity and SN-38 metabolism, leading to increased likelihood of irinotecan toxicity. Consequently, the irinotecan product insert suggests a reduced initial dose for patients homozygous for the TA repeat.36 Heterozygous patients have intermediate enzyme activity and may be at increased risk for neutropenia; however, such patients have been shown to tolerate normal initial doses.35 Patients negative for the TA repeat are the least likely to suffer from dose-limiting toxicity. The UGT1A1 TA repeat assay does not detect other mutations in the
220
Gastroenterology Reference Guide
UGT1A1 gene that may affect UGT1A1 enzyme activity. Oxaliplatin ERCC1-118 Polymorphism Excision repair cross-complementation group 1 (ERCC1) is an excision nuclease within the nucleotide excision repair (NER) pathway. Polymorphisms in the ERCC1 gene may increase DNA repair activity via the NER pathway, resulting in resistance to platinum-based chemotherapeutic drugs such as oxaliplatin.37 A single-nucleotide polymorphism (CT) in codon 118 was shown to result in worse survival when advanced CRC patients were treated with 5-FU/oxaliplatin.32,37 Median survival was improved in patients homozygous for the 118C genotype (C/C) relative to those with 1 or more thymine alleles (Kaplan-Meier analysis, P = 0.021).37 GSTP1 Ile105Val Polymorphism The activity of glutathione S-transferase P1 (GSTP1), an enzyme involved in inactivation of platinum-based chemotherapeutic agents, is decreased with GSTP1 polymorphisms that lead to an amino acid change at codon 105. Homozygosity for the 105Val allele has been associated with improved survival, slower disease progression, and less cumulative peripheral neuropathy in patients treated with oxaliplatin.32,38,39 Shorter median survival associated with a dosedependent presence of Ile genotype was significant in 1 study (Ile/Ile, 7.9 months; Ile/Val, 13.3 months; Val/Val >24.9 months, P < 0.001),38 but not in another after multivariate analysis (P =0.072).32 Whereas median survival data are conflicting, the risk of disease progression was significantly higher (2 times) in patients with the Ile/Ile genotype than in those with the Val/Val genotype (95% CI 0.854.71, P =0.018).32
221
Part 3: Test Application and Interpretation
Gastroenterology Reference Guide
Preliminary results indicate that risk of dose-limiting toxicity manifesting as cumulative peripheral neuropathy is increased with the combined Ile/Ile and Ile/Val genotypes compared to the Val/Val genotype (odds ratio, 5.75; 95% CI 1.0830.74; P=0.02).39 XPD-751 Polymorphism Xeroderma pigmentosum group D (XPD), another enzymatic component of the NER pathway, is also involved with DNA repair resulting in resistance to platinum-based drugs. K751Q polymorphisms in the XPD gene (Lys/Gln and Gln/Gln) have been associated with reduced response to 5-FU/oxaliplatin treatment and reduced median survival.32,40 Among patients (n = 70) with advanced CRC treated with 5-FU/oxaliplatin, the Lys/Lys genotype was associated with longer median survival (17.4 months, 95% CI 7.926.5) than was the Lys/Gln (12.8 months, 95% CI 8.525.9) or Gln/Gln (3.3 months, 95% CI 1.46.5) genotype.40 XRCC1 Arg399Gln Polymorphism The X-ray cross-complementation group 1 (XRCC1) enzyme is another DNA repair enzyme associated with resistance to platinum-based treatment.41 In a small study of XRCC1 polymorphisms, homozygosity for the 399Arg allele (Arg/Arg) predicted successful 5-FU/oxaliplatin treatment in patients with advanced CRC.41 Patients with at least 1 Gln allele (Arg/Gln or Gln/Gln) were at a 5.2-fold increased risk (95% CI 1.2122.07) of not responding to 5-FU/oxaliplatin chemotherapy. References
1. American Cancer Society: Cancer facts and figures 2006. Available at: http://www.cancer.org/downloads/STT/CAFF2006PWSecured.pdf. Accessed June 12, 2006.
222
Gastroenterology Reference Guide
2. Engstrom PF. Colorectal Cancer. In: Lenhard RE, Osteen RT, Gansler T, ed. Clinical Oncology. Atlanta, GA : American Cancer Society Inc; 2001:361-371. 3. Genetics of Colorectal Cancer (PDQ). Available at: http://www.cancer. gov/cancertopics/pdq/genetics/colorectal/HealthProfessional/page1. Accessed August 11, 2006. 4. Lynch HT, de la Chapelle A. Hereditary colorectal cancer. NEJM. 2003;348:919-932. 5. Smith RA, Cokkinides V, Eyre HJ. American Cancer Society guidelines for the early detection of cancer, 2006. CA Cancer J Clin. 2006;56:11-25. 6. Mandel JS, Church TR, Bond JH, et al. The effect of fecal occult-blood screening on the incidence of colorectal cancer. NEJM. 2000;343:16031607. 7. Winawer S, Fletcher R, Rex D, et al. Colorectal cancer screening and surveillance: Clinical guidelines and rationale-update based on new evidence. Gastroenterology. 2003;124:544-560. 8. Umar A, Boland CR, Terdiman JP, et al. Revised Bethesda guidelines for hereditary nonpolyposis colorectal cancer (Lynch syndrome) and microsatellite instability. J Natl Cancer Inst. 2004;96:261-268. 9. Vasen HF, Watson P, Mecklin J-P, et al. New clinical criteria for hereditary nonpolyposis colorectal cancer (HNPCC, Lynch syndrome) proposed by the International Collaborative Group on HNPCC. Gastroenterology. 1999;116:1453-1456. 10. Jarvinen HJ, Aarnio M, Mustonen H, et al. Controlled 15-year trial on screening for colorectal cancer in families with hereditary nonpolyposis colorectal cancer. Gastroenterology. 2000;118:829-834. 11. Cruz-Correa M, Giardiello FM. Diagnosis and management of hereditary colon cancer. Hematol Oncol Clin N Am. 2003;17:539-551. 12. Bardi G, Fenger C, Johansson B, et al. Tumor karyotype predicts clinical outcome in colorectal cancer patients. J Clin Oncol. 2004;22:2623-2634. 13. Levin B, Brooks D, Smith RA, et al. Emerging technologies in screening for colorectal cancer: CT colonoscopy, immunochemical fecal occult blood tests, and stool screening using molecular markers. CA Cancer J Clin. 2003;53:44-55. 14. Smith A, Young GP, Cole SR, et al. Comparison of a brush-sampling fecal immunochemical test for hemoglobin with a sensitive guaiac-based fecal occult blood test in detection of colorectal neoplasia. Cancer. 2006;107:2152-2159. 15. Pinol V, Castells A, Andreu M, et al. Accuracy of revised Bethesda guidelines, microsatellite instability, and immunochemistry for the identification of patients with hereditary nonpolyposis colorectal cancer. JAMA. 2005;293:1986-1994. 16. Lynch HT, Riley BD, Weismann S, et al. Hereditary nonpolyposis colorectal carcinoma (HNPCC) and HNPCC-like families: problems in diagnosis, surveillance, and management. Cancer. 2004;100:53-64. 17. AJCC Cancer Staging Manual, 6th ed. New York, NY: Springer; 2002. 18. OConnell JB, Maggard MA, Ko CY. Colon cancer survival rates with the new American Joint Commission Committee on cancer sixth edition staging. J Natl Cancer Inst. 2004;96:1420-1425. 19. Popat S, Hubner R, Houlston RS. Systematic review of microsatellite instability and colorectal cancer prognosis. J Clin Oncol. 2005;23:609-618.
Part 3: Test Application and Interpretation
223
Gastroenterology Reference Guide
20. Locker GY, Hamilton S, Harris J, et al. ASCO 2006 update of recommendations for the use of tumor markers in gastrointestinal cancer. J Clin Oncol. 2006;24:5313-5327. 21. Duffy MJ, vanDalen A, Haglund C, et al. Clinical utility of biochemical markers in colorectal cancer: European Group on Tumour Markers (EGTM) guidelines. Eur J Cancer. 2003;39:718-727. 22. Sorbye H, Dahl O. Transient CEA increase at start of oxaliplatin combination therapy for metastatic colorectal cancer. Acta Oncologica. 2004;43:495-498. 23. Chung KY, Shia J, Kemeny NE, et al. Cetuximab shows activity in colorectal cancer patients with tumors that do not express the epidermal growth factor receptor by immunohistochemistry. J Clin Oncol. 2005;23:1803-1810. 24. Hebbar M, Wacrenier A, Desauw C, et al. Lack of usefulness of epidermal growth factor receptor expression determination for cetuximab therapy in patients with colorectal cancer. Anticancer Drugs. 2006;17:855-857. 25. Erbitux [package insert]. Branchburg, NJ:ImClone Systems Inc; March 2006. 26. Cunningham D, Humblet Y, Siena S, et al. Cetuximab monotherapy and cetuximab plus irinotecan in irinotecan-refractory metastatic colorectal cancer. N Engl J Med.2004;351:337-345. 27. Moroni M, Veronese S, Benvenuti, et al. Gene copy number for epidermal growth factor receptor (EGFR) and clinical response to antiEGRF treatment in colorectal cancer: a cohort study. Lancet Oncol.2005;6:279-286. 28. Raida M, Schwabe W, Hausler P, et al. Prevalence of a common point mutation in the dihydropyrimidine dehydrogenase (DPD) gene within the 5-splice donor site of intron 14 in patients with severe 5-fluorouracil (5-FU)-related toxicity compared with controls. Clin Cancer Res. 2001;7:2832-2839. 29. Van Kuilenburg AB, Meinsma R, Zoetekouw L, et al. High prevalence of the IVS14+1G>A mutation in the dihydropyrimidine dehydrogenase gene of patients with severe 5-fluorouracil-associated toxicity. Pharmacogenetics. 2002;12:555-558. 30. Van Kuilenburg AB, Meinsma R, Zoetekouw L, et al. Increased risk of grade IV neutropenia after administration of 5-fluorouracil due to a dihydropyrimidine dehydrogenase deficiency: high prevalence of the IVS14+1G>A mutation. Int J Cancer. 2002;101:253-258. 31. Hitre E, Budai B, Adleff V, et al. Influence of thymidylate synthase gene polymorphisms on the survival of colorectal cancer patients receiving adjuvant 5-fluorouracil. Pharmacogenet Genomics. 2005;15:723-730. 32. Stoehlmacher J, Park DJ, Zhang W, et al. A multivariate analysis of genomic polymorphisms: prediction of clinical outcome to 5FU/oxaliplatin combination chemotherapy in refractory colorectal cancer. Br J Cancer. 2004;91:344-354. 33. Marsh S, McKay JA, Cassidy J, et al. Polymorphism in the thymidylate synthase promoter enhancer region in colorectal cancer. Int J Oncology. 2001;19:383-386. 34. Massacesi C, Terrazzino S, Marcucci F, et al. Uridine diphosphate glucuronosyl transferase 1A1 promotor polymorphism predicts the risk
224
Gastroenterology Reference Guide
35.
36. 37.
38.
39.
40.
41.
of gastrointestinal toxicity and fatigue induced by irinotecan-based chemotherapy. Cancer. 2006;106:1007-1016. Rouits E, Boisdron-Celle M, Dumont A, et al. Relevance of different UGT1A1 polymorphisms in irinotecan-induced toxicity: a molecular and clinical study of 75 patients. Clin Cancer Res. 2004;10:5151-5159. Camptosar [package insert]. New York, NY: Pfizer Inc; 2006. Park DJ, Zhang W, Stoehlmacher J, et al. ERCC1 gene polymorphism as a predictor for clinical outcome in advanced colorectal cancer patients treated with platinum-based chemotherapy. Adv Hematol Oncol. 2003;1:162-166. Stoehlmacher J, Park DJ, Zhang W, et al. Association between glutathione S-transferase P1, T1, and M1 genetic polymorphism and survival of patients with metastatic colorectal cancer. J Natl Cancer Inst. 2002;94:936-942. Lecomte T, Landi B, Beaune P, et al. Glutathione S-transferase P1 polymorphism (Ile105Val) predicts cumulative neuropathy in patients receiving oxaliplatin-based chemotherapy. Clin Cancer Res. 2006;12:30503056. Park DJ, Stoehlmacher J, Zhang W, et al. A Xeroderma Pigmentosum Group D gene polymorphism predicts clinical outcome to platinumbased chemotherapy in patients with advanced colorectal cancer. Cancer Res. 2001;61:8654-8658. Stoehlmacher J, Ghaderi V, Iobal S, et al. A polymorphism of the XRCC1 gene predicts for response to platinum based treatment in advanced colorectal cancer. Anticancer Res. 2001;21:3075-3079.
Part 3: Test Application and Interpretation
8.2 Carcinoembryonic Antigen (CEA) Clinical Use: This test is used to monitor persistent, metastatic, or recurrent adenocarcinoma of the colon following curative surgery. Clinical Background: CEA is an oncofetal glycoprotein present in the gastrointestinal tract and body fluids of the embryo and fetus. This 180kilodalton antigen is also present in certain adult gastrointestinal cells, including the mucosal cells of the colorectum, and small amounts are present in blood. Although its physiological role is not clear, CEA is a useful tumor marker. Blood levels are usually not increased in localized or primary disease, but are often elevated in patients with disseminated cancers and in some patients with non-malignant disease.
225
Gastroenterology Reference Guide
CEA is useful for detecting recurrence of colon cancer; increased levels may precede clinical evidence of recurrence by as much as 6 months. The sensitivity for detecting recurrence is 97% in patients whose CEA was elevated preoperatively, but only 66% in those with normal preoperative levels. CEA is not recommended for screening because of low sensitivity and specificity, particularly in the early stages of neoplastic disease. The American Society of Clinical Oncology (ASCO) has recommended the use of CEA testing for staging/prognosis, detecting recurrence, monitoring therapy, and screening for hepatic metastases in patients with colon cancer ( J Clin Oncol. 2001;19:1865-1878). Interpretive Information: Normal CEA concentrations (<2.5 ng/mL) are seen in about 97% of apparently healthy individuals. Elevations may be seen in 19% of heavy smokers and 7% of former smokers, individuals with inflammatory diseases of the gastrointestinal tract (eg, peptic ulcer, diverticulitis, etc), liver diseases including cirrhosis and chronic active hepatitis, advanced renal disease, and fibrocystic disease of the breast. Levels can also be increased in as many as 30% of patients with breast, lung, hepatocellular, and pancreatic carcinoma (Table 12). About 30% of patients with metastatic colon cancer have normal CEA levels. 8.3 Fecal Globin, Immunochemistry (InSure) Clinical Use: This test is used to screen for lower gastrointestinal bleeding associated with colorectal cancer, adenomas, polyps, and other lower gastrointestinal conditions. Clinical Background: Colorectal cancer is the third most common form of cancer and the third leading
226
Gastroenterology Reference Guide
Table 12. Distribution of CEA
Part 3: Test Application and Interpretation
Subject Group No. of Subjects % with CEA in Indicated Range 02.5 ng/mL 2.65.0 ng/mL 5.110.0 ng/mL 10.020.0 ng/mL >20.0 ng/mL
Healthy Subjects Non-smokers Smokers Malignant Disease Colorectal Lung Breast Gastric Ovarian Pancreatic Liver Lymphoproliferative Other* Non-Malignant Disease Cirrhosis Other benign liver Ulcerative colitis Benign polyps Colon and intestinal Gastrointestinal Breast Kidney and bladder Lung Other 53 5 11 23 15 21 53 12 29 117 42 40 91 65 67 76 96 83 69 86 13 20 9 22 20 14 0 8 24 8 32 0 0 13 0 0 2 0 7 4 13 40 0 0 13 5 0 8 0 1 0 0 0 0 0 5 2 0 0 0 250 158 221 35 35 43 6 15 40 38 46 68 60 83 44 50 80 75 11 16 15 17 11 21 17 20 10 7 11 8 9 3 16 0 0 10 6 7 2 6 3 7 33 0 5 38 20 7 9 0 12 0 0 0 225 150 98 87 2 8 0 5 0 0 0 0
Source: Bayer Corporation. *Other cancerous diseases include bladder, prostate, esophagus, head and neck, sarcoma, and kidney cancer. Other non-malignant diseases include benign uterine, cervical and vaginal, benign ovary, and benign male genital as well as other benign conditions.
cause of cancer death in the United States. According to American Cancer Society (ACS) estimates, 145,290 new cases of colorectal cancer were expected to be
227
Gastroenterology Reference Guide
diagnosed and more than 56,000 people were estimated to die of this disease in 2005, accounting for 10% of cancer deaths in each sex.1 The most common risk factor is age: >90% of colorectal cancers are diagnosed in people >50 years of age.1 Screening and early detection are crucial, as survival rates decrease dramatically with increasing cancer stage: 5-year survival ranges from >90% for Dukes stage A to <5% for Dukes stage D. Moreover, detection and removal of precancerous polyps can reduce the incidence of colorectal cancer by 76% to 90%.2 Although routine screening is recommended for average-risk individuals 50 years of age,3-5 fewer than half of age-eligible adults receive appropriate screening.6,7 Because cancerous and precancerous colorectal lesions tend to cause low-level bleeding, assays for occult blood in feces have become an important screening tool. Annual screening with a fecal occult blood test (FOBT) can decrease colorectal cancer mortality by up to 33%.8 ACS guidelines indicate that a yearly FOBT is an acceptable screening method for average-risk individuals 50 years of age; combining an annual FOBT with flexible sigmoidoscopy every 5 years is preferred over the annual use of either test alone.3 One drawback to the most common currently used FOBTs is that they are guaiac based; they detect heme peroxidase activity and are not specific for human hemoglobin. Thus, hemoglobin from red meat, peroxidase from fruits and vegetables, and certain medications can cause false-positive reactions and need to be avoided for several days before the test. In addition, vitamin C (in excess of 250 mg/day) from supplements or citrus fruits and juices may cause a false-negative guaiac test result. While these FOBTs are non-invasive and specimens can be collected at home, strict dietary and medication restrictions may decrease
228
Gastroenterology Reference Guide
adherence.7,9 Newer immunochemical assays such as InSure do not react with non-human hemoglobin or peroxidase, so food restrictions are not necessary. Immunochemical FOBTs are also more specific for lower gastrointestinal bleeding because they target the globin portion of hemoglobin, which does not survive passage through the upper gastrointestinal tract. Based on these features and published performance characteristics of immunochemical FOBTs, ACS guidelines suggest that immunochemical FOBTs such as InSure are more patient-friendly, and are likely to be equal or better in sensitivity and specificity relative to guaiac-based tests.3,10 Individuals Suitable for Testing include those undergoing routine screening for colorectal lesions or other sources of bleeding in the lower gastrointestinal tract. Samples should not be collected 1) during, or 3 days before or after, a menstrual period; 2) if bleeding hemorrhoids are present; 3) if there is visible blood in the urine or toilet bowl; 4) if there are bleeding cuts on the hands; or 5) if the toilet contains rust or saltwater. Toilet freshener should be removed and the toilet flushed prior to sample collection. Dietary roughage may increase test sensitivity, but no dietary changes or restrictions are required. Method: This immunochemistry assay uses monoclonal, mouse anti-human hemoglobin-coated chromatography test strips with colorimetric detection. The analytical sensitivity of the assay is 50 g Hb/g feces.11 It is specific for colorectal bleeding and does not detect blood from the upper gastrointestinal tract.9 Interpretive Information: Positive results indicate occult blood in the feces and should be followed up
Part 3: Test Application and Interpretation
229
Gastroenterology Reference Guide
with physician consultation and possible endoscopic evaluation. Negative results indicate the absence of fecal blood; however, false-negatives can occur because of uneven distribution of blood in the feces or intermittent bleeding. References
1. American Cancer Society. Cancer facts and figures 2005. Available at: http://www.cancer.org/docroot/STT/stt_0.asp. Accessed Sept. 20, 2005. 2. Winawer SJ, Zauber AG, Ho MN, et al. Prevention of colorectal cancer by colonoscopic polypectomy. The National Polyp Study Workgroup. N Engl J Med. 1993;329:1977-1981. 3. Smith RA, Cokkinides V, Eyre HJ. American Cancer Society guidelines for the early detection of cancer, 2003. CA Cancer J Clin. 2003;53:27-43. 4. US Preventive Services Task Force. Screening for colorectal cancer: recommendations and rationale. AHRQ Pub. No. 03-510A. July 2002. Available at: http://www.ahcpr.gov/clinic/3rduspstf/colorectal/ colorr.pdf. Accessed July 18, 2003. 5. Winawer S, Fletcher R, Rex D, et al. Colorectal cancer screening and surveillance: clinical guidelines and rationaleupdate based on new evidence. Gastroenterology. 2003;124:544-560. 6. Centers for Disease Control and Prevention. Colorectal cancer test use among persons aged 50 yearsUnited States, 2001. MMWR. 2003; 52:193-196. 7. Vernon SW. Participation in colorectal cancer screening: a review. J Natl Cancer Inst. 1997;89:1406-1422. 8. Mandel JS, Bond JH, Church TR, et al. Reducing mortality from colorectal cancer by screening for fecal occult blood. Minnesota Colon Cancer Control Study. N Engl J Med. 1993;328:1365-1371. 9. Robinson MH, Pye G, Thomas WM, et al. Haemoccult screening for colorectal cancer: the effect of dietary restriction on compliance. Eur J Surg Oncol. 1994;20:545-548. 10. Levin B, Brooks D, Smith RA, et al. Emerging technologies in screening for colorectal cancer: CT colonography, immunochemical fecal occult blood tests, and stool screening using molecular markers. CA Cancer J Clin. 2003;53:44-55. 11. InSure Product Instructions. Falmouth, ME: Enterix Inc; 2000.
8.4 Microsatellite Instability (MSI), HNPCC Clinical Use: This assay is used to assess the need to test individuals or their family members for hereditary nonpolyposis colorectal cancer (HNPCC)associated mutations.
230
Gastroenterology Reference Guide
Clinical Background: HNPCC, an autosomal dominant condition caused by mutations in mismatch repair (MMR) genes, accounts for about 3% to 5% of colorectal cancers. In individuals with an MMR mutation, the lifetime risk of developing colorectal cancer is about 80%;1 these mutations may also predispose to endometrial, ovarian, stomach, and other forms of cancer. Although HNPCC may have a somewhat better prognosis than other forms of colorectal cancer, it is characterized by rapid progression from adenomatous polyps to malignant lesions. Identifying HNPCC in affected individuals is important, as close surveillance of at-risk family members has been found to reduce the rate of colorectal cancer and overall mortality by >60%.2 Family members with an MMR mutation require aggressive follow-up (colonoscopy every 12 years), while those without the familial mutation are at the same risk as the general population and do not require intensive screening. HNPCC can be diagnosed on the basis of clinical and family history,3,4 as well as by direct detection of MMR mutations. In suspected HNPCC patients without a known familial mutation, the first step in the genetic diagnosis is identifying microsatellite instability (MSI) in tumor cells. Microsatellites are sequences of repetitive DNA with repeating units of 1 to 7 base pairs. These regions are prone to replication errors, which are normally repaired by MMR enzymes. If one of the MMR enzymes is impaired, the microsatellites become unstable and will have varying repeat numbers at specific loci. Although MSI does not seem to have any clinical effect, it is a marker of faulty DNA repair; cancer arises when faulty DNA repair leads to mutations in tumor suppressor or oncogenes. MSI is found in most HNPCCs but only about 15% of sporadic colorectal tumors,5,6 and therefore cannot be used alone for diagnosis of HNPCC. However, a
231
Part 3: Test Application and Interpretation
Gastroenterology Reference Guide
finding of MSI strongly indicates the presence of MMR mutations and the need for further genetic testing.7 The National Cancer Institute has recommended a panel of 5 microsatellites for MSI screening: BAT 25 and BAT 26 (mononucleotide repeats), D2S123, D5S346, and D17S250 (dinucleotide repeats). Individuals Suitable for Testing include those who meet any of the Bethesda criteria (Table 7) and in whom a familial mutation is not known. Method: This assay detects microsatellite instability in tumor tissue. Paraffin sections containing 30% tumor cells are processed with selective scraping of the tumor-rich area, whereas those containing <30% tumor cells are processed with laser capture microdissection. Whole blood is used as control (non-tumor) tissue. Microsatellite instability is detected in a multiplex polymerase chain reaction (PCR)-based assay in which 5 STR loci (BAT 25, BAT 26, D2S123, D5S346, D17S250) are amplified from tumor and normal tissue. One primer from each set of PCR primers is labeled with either 6-FAM (blue) or HEX (green) fluorescein; the 5 markers are distinguished by peak size and fluorescent labels. Amplification products are separated by capillary electrophoresis, followed by data analysis with GeneMapper' software to detect peaks and determine allele size. The tumor and normal peaks are visually compared to detect MSI. Aliases for this test are HNPCC, Lynch syndrome, and replication error (RER+).
This test was developed and its performance characteristics determined by Quest Diagnostics Nichols Institute. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test.
232
Gastroenterology Reference Guide
Interpretive Information: The presence of 2 or more unstable microsatellite loci indicates MSI; instability at 1 locus indicates absence of MSI. Individuals with MSI tumors should be screened for germline mutations in MLH1 and MSH2, and in MSH6 if no MLH1 or MSH2 mutations are found. Because most HNPCCs exhibit MSI, germline MMR mutation analysis is generally not necessary in patients without MSI-H. However, MSI is frequently absent in tumors associated with MSH6 mutations.9 References
1. Vasen HF, Wijnen JT, Menko FH, et al. Cancer risk in families with hereditary nonpolyposis colorectal cancer diagnosed by mutation analysis. Gastroenterology. 1996;110:1020-1027. 2. Jarvinen HJ, Aarnio M, Mustonen H, et al. Controlled 15-year trial on screening for colorectal cancer in families with hereditary nonpolyposis colorectal cancer. Gastroenterology. 2000;118:829-834. 3. Vasen HF, Mecklin JP, Khan PM, et al. The International Collaborative Group on Hereditary Non-Polyposis Colorectal Cancer (ICG-HNPCC). Dis Colon Rectum. 1991;34:424-425. 4. Vasen HF, Watson P, Mecklin JP, et al. New clinical criteria for hereditary nonpolyposis colorectal cancer (HNPCC, Lynch syndrome) proposed by the International Collaborative group on HNPCC. Gastroenterology. 1999;116:1453-1456. 5. Giardiello FM, Brensinger JD, Petersen GM. AGA technical review on hereditary colorectal cancer and genetic testing. Gastroenterology. 2001;121:198-213. 6. Terdiman JP, Gum JR Jr, Conrad PG, et al. Efficient detection of hereditary nonpolyposis colorectal cancer gene carriers by screening for tumor microsatellite instability before germline genetic testing. Gastroenterology. 2001;120:21-30. 7. Winawer S, Fletcher R, Rex D, et al. Colorectal cancer screening and surveillance: clinical guidelines and rationale-update based on new evidence. Gastroenterology. 2003;124:544-560. 8. Rodriguez-Bigas MA, Boland CR, Hamilton SR, et al. A National Cancer Institute Workshop on Hereditary Nonpolyposis Colorectal Cancer Syndrome: meeting highlights and Bethesda guidelines. J Natl Cancer Inst. 1997;89:1758-1762. 9. Berends MJ, Wu Y, Sijmons RH, et al. Molecular and clinical characteristics of MSH6 variants: an analysis of 25 index carriers of a germline variant. Am J Hum Genet. 2002;70:26-37.
Part 3: Test Application and Interpretation
233
Gastroenterology Reference Guide
8.5 MLH1, MSH2, and MSH6 Mutations for HNPCC Clinical Use: This test is used to differentiate hereditary nonpolyposis colorectal cancer (HNPCC) from non-HNPCC colorectal cancer (CRC) and to assess the risk of HNPCC in family members of individuals with HNPCC. Clinical Background: HNPCC, which accounts for about 3% to 5% of CRCs, is caused by defects in mismatch repair (MMR) enzymes. These defects may also increase the risk of endometrial, cervical, stomach, ovarian, and other forms of cancer. About 90% of individuals with identifiable HNPCC mutations have mutations in the MLH1 or MSH21 MMR gene. Mutations in MSH6, PMS1, and PMS2 have also been implicated. HNPCC is an autosomal dominant condition with variable penetrance. Individuals with HNPCC typically inherit 1 copy of a defective MMR allele; mutations in somatic tissue may cause loss of the normal allele, leading to an increased rate of mutations in affected cells. Mutations in oncogenes or tumor suppressor genes then lead to carcinogenesis. The lifetime risk of CRC in individuals with an MMR gene mutation is about 80%.2 Diagnosis of HNPCC is based on clinical features and familial cancer patterns,3,4 or on detection of mutations in MMR genes. Although HNPCC appears to have a slightly more favorable prognosis than nonHNPCC CRC, the often rapid progression from adenomatous polyps to malignant lesions necessitates aggressive follow up for individuals with HNPCC and their first-degree relatives; close surveillance of family members can reduce the rate of CRC and overall mortality by >60%.5,6 Detection of MMR mutations is
234
Gastroenterology Reference Guide
important for counseling individuals with HNPCC and their families, as family members without a known familial mutation are at the same risk as the general population and do not require intensive screening. If a familial mutation is not known, testing suspected HNPCC tumors for microsatellite instability (MSI) can help determine the need for MMR mutation analysis. Microsatellites are regions of repetitive DNA with repeating units of 1 to 7 base pairs. These regions are prone to replication errors, which can be detected as heterogeneous repeat numbers at specific microsatellite regions. Because MMR enzymes normally repair such errors, detection of MSI in tumor tissue suggests the presence of MMR defects. MSI is found in most HNPCCs7,8 but only about 15% of sporadic colorectal tumors. Because of the relative frequencies of MMR mutations, MLH1 and MSH2 should be examined first; if no mutations are found, mutations in MSH6 should be sought. If the family mutation is known, only the relevant exon in the affected gene should be tested. Individuals Suitable for Testing include individuals with CRC who meet the Amsterdam criteria for diagnosis of HNPCC3; individuals with documented MSI in a colorectal tumor; first-degree relatives of individuals who have a known MMR mutation; and, if the familial MMR mutation is not known, first-degree relatives of individuals who Meet the Amsterdam criteria; or Have 2 HNPCC-related cancers, including synchronous and metachronous CRCs or associated extracolonic cancers (endometrial, ovarian, gastric, hepatobiliary or small bowel
235
Part 3: Test Application and Interpretation
Gastroenterology Reference Guide
cancer or transitional cell carcinoma of the renal pelvis or ureter); or Have CRC and have a first-degree relative with CRC and/or HNPCC-related extracolonic cancer and/or a colorectal adenoma; one of the cancers diagnosed at age <45 years, and the adenoma diagnosed at age <40 years.9 Method: In this assay, relevant MMR gene coding regions and splice junction sites are amplified by polymerase chain reaction (PCR). Both strands of each amplified product are then sequenced, with automated fluorescence detection. The test report lists nucleotide changes in coding sequences and known splice sites. This assay detects heterozygous point mutations, small deletions, and insertions in the relevant MMR gene(s), with an analytical sensitivity of >98%. Aliases include Lynch Syndrome Mutation and HNPCC Mismatch Repair Gene Mutation.
This test was developed and its performance characteristics determined by Quest Diagnostics Nichols Institute. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test.
Interpretive Information Individuals with CRC: Detection of an MMR gene mutation in an individual with colon cancer suggests the need for aggressive screening for recurrent CRC and, possibly, other cancers associated with HNPCC (eg, endometrial and ovarian cancer). American Gastroenterological Association (AGA) guidelines recommend colonoscopy every 1 to 2 years for individuals with a clinical or genetic diagnosis of HNPCC.6 Genetic counseling should be offered to
236
Gastroenterology Reference Guide
the patient and first-degree family members, who may benefit from germline mutation testing. If mutations are not found in MLH1 or MSH2, mutations in MSH6 should be sought. Mutations not identified in these assays may also be associated with HNPCC. At-risk Family Members: If the familial mutation is known, detection of that mutation implies an increased risk of HNPCC and associated cancers. AGA guidelines recommend colonoscopy every 1 to 2 years for those at increased risk of HNPCC, beginning at age 20 to 25, or 10 years before the earliest age of CRC diagnosis in the family.6 Individuals without the mutation are not at increased risk and can be followed up according to screening recommendations for the normal-risk population. If the familial mutation is not known, negative MLH1 and MSH2 findings should be followed with tests for mutations in MSH6. References
1. Lynch HT, de la Chapelle A. Genetic susceptibility to non-polyposis colorectal cancer. J Med Genet. 1999;36:801-818. 2. Vasen HF, Wijnen JT, Menko FH, et al. Cancer risk in families with hereditary nonpolyposis colorectal cancer diagnosed by mutation analysis. Gastroenterology. 1996;110:1020-1027. 3. Vasen HF, Mecklin JP, Khan PM, et al. The International Collaborative Group on Hereditary Non-Polyposis Colorectal Cancer (ICG-HNPCC). Dis Colon Rectum. 1991;34:424-425. 4. Vasen HF, Watson P, Mecklin JP, et al. New clinical criteria for hereditary nonpolyposis colorectal cancer (HNPCC, Lynch syndrome) proposed by the International Collaborative group on HNPCC. Gastroenterology. 1999;116:1453-1456. 5. Jarvinen HJ, Aarnio M, Mustonen H, et al. Controlled 15-year trial on screening for colorectal cancer in families with hereditary nonpolyposis colorectal cancer. Gastroenterology. 2000;118:829-834. 6. Winawer S, Fletcher R, Rex D, et al. Colorectal cancer screening and surveillance: clinical guidelines and rationale-update based on new evidence. Gastroenterology. 2003;124:544-560. 7. Giardiello FM, Brensinger JD, Petersen GM. AGA technical review on hereditary colorectal cancer and genetic testing. Gastroenterology. 2001;121:198-213.
Part 3: Test Application and Interpretation
237
Gastroenterology Reference Guide
8. Terdiman JP, Gum JR Jr, Conrad PG, et al. Efficient detection of hereditary nonpolyposis colorectal cancer gene carriers by screening for tumor microsatellite instability before germline genetic testing. Gastroenterology. 2001;120:21-30. 9. Rodriguez-Bigas MA, Boland CR, Hamilton SR, et al. A National Cancer Institute Workshop on Hereditary Nonpolyposis Colorectal Cancer Syndrome: meeting highlights and Bethesda guidelines. J Natl Cancer Inst. 1997;89:1758-1762.
8.6 UGT1A1 Gene Polymorphism (TA Repeat) Clinical Use: This test is used to predict toxicity from irinotecan therapy, assist in selection of initial irinotecan dosage, and support diagnosis of Gilberts syndrome. Clinical Background: Irinotecan (Campostar', Pfizer Inc, New York, NY) is a topoisomerase-I inhibitor widely used for treatment of metastatic and recurrent colorectal cancer. The most common doselimiting adverse effects of irinotecan are neutropenia, diarrhea, and asthenia. Variations in the gene encoding uridine diphosphate glucuronosyltransferase 1A1 (UGT1A1) may help predict which patients are most likely to develop these adverse effects. UGT1A1 is a hepatic enzyme primarily responsible for conjugation of bilirubin. UGT1A1 also catalyzes the glucuronidation of SN-38, the active metabolite of irinotecan and the main source of treatmentrelated toxicity. Glucuronidation is thought to protect against the toxicity of SN-38.1 However, the presence of an additional TA repeat in the TATA region of the UGT1A1 promoter (ie, 7 TA repeats; UGT1A1*28) markedly decreases UGT1A1 production, leading to reduced glucuronidation.2,3 Patients homozygous for the UGT1A1*28 allele therefore accumulate higher levels of SN-38 and are more likely to experience severe adverse effects
238
Gastroenterology Reference Guide
during irinotecan chemotherapy.46 Thus, knowledge of the UGT1A1 polymorphism status could help guide the selection of appropriate starting dosages, reducing the risk of severe toxicity and improving the chances that therapy could be maintained. Homozygosity for this allele is also associated with Gilberts syndrome, a mild form of unconjugated hyperbilirubinemia. Roughly 10% of the US population is homozygous for UGT1A1*28. The frequency of the UGT1A1*28 allele varies among ethnicities,7 being highest in those of African (43%) or European (39%) descent and lowest in those of Asian (16%) descent.8 Variants with 5 or 8 repeats occur at much lower frequencies, primarily in individuals of African descent. The presence of 8 TA repeats has been associated with Gilberts syndrome and with decreased glucuronidation in vitro.8 Other variations in the genes encoding UGT1A1 and other uridine diphosphate glucuronosyltransferases may also influence glucuronidation and have been reported at varying frequencies across ethnicities. Individuals Suitable for Testing include patients being considered for treatment with irinotecan and individuals with suspected Gilberts syndrome. Method: This fluorescent polymerase chain reaction (PCR) method uses primers specific for the 5' untranslated region of UGT1A1 and automated detection of PCR products. Results reported as negative, heterozygous, or homozygous for the UGT1A1*28 allele. Interpretive Information: Absence of the UGT1A1*28 allele usually indicates a wild-type genotype, although some individualsespecially
Part 3: Test Application and Interpretation
239
Gastroenterology Reference Guide
those of African descentmay have 5 or 8 TA repeats. Patients with a wild-type UGT1A1 genotype have a low risk of severe toxicity from standard starting dosages of irinotecan. Similarly, in patients with 1 copy of the UGT1A1*28 allele (heterozygous), the other copy is most likely wild-type. These patients are at increased risk of irinotecan toxicity but may still tolerate normal initial dosages. Individuals with 2 copies of the UGT1A1*28 allele (homozygous) are at increased risk of severe toxicity from irinotecan. Irinotecan product information indicates that a reduced initial dosage should be considered for such patients.9 Other chemotherapeutic options may also be considered. This assay does not detect other polymorphisms or mutations in the UGT1A1 gene that may impair irinotecan detoxification, nor does it examine other modifiers of irinotecan metabolism such as CYP3A4 activity. Since genetic variation can affect the accuracy of direct mutation testing, the results should be interpreted in light of other clinical and laboratory findings. In symptomatic patients, homozygosity for UGT1A1*28 is consistent with a diagnosis of Gilberts syndrome. Because other UGT variants have been associated with Gilberts syndrome, absence of the UGT1A1*28 allele does not rule out this condition. References
1. Gupta E, Lestingi TM, Mick R, et al. Metabolic fate of irinotecan in humans: correlation of glucuronidation with diarrhea. Cancer Res. 1994;54:3723-3725. 2. Iyer L, King CD, Whitington PF, et al. Genetic predisposition to the metabolism of irinotecan (CPT-11). Role of uridine diphosphate glucuronosyltransferase isoform 1A1 in the glucuronidation of its active metabolite (SN-38) in human liver microsomes. J Clin Invest. 1998;101:847-854.
240
Gastroenterology Reference Guide
3. Iyer L, Das S, Janisch L, et al. UGT1A1*28 polymorphism as a determinant of irinotecan disposition and toxicity. Pharmacogenomics J. 2002;2:43-47. 4. Massacesi C, Terrazzino S, Marcucci F, et al. Uridine diphosphate glucuronosyl transferase 1A1 promoter polymorphism predicts the risk of gastrointestinal toxicity and fatigue induced by irinotecan-based chemotherapy. Cancer. 2006; [Epub ahead of print] 5. Rouits E, Boisdron-Celle M, Dumont A, et al. Relevance of different UGT1A1 polymorphisms in irinotecan-induced toxicity: a molecular and clinical study of 75 patients. Clin Cancer Res. 2004;10:5151-5159. 6. Innocenti F, Undevia SD, Iyer L, et al. Genetic variants in the UDPglucuronosyltransferase 1A1 gene predict the risk of severe neutropenia of irinotecan. J Clin Oncol. 2004;22:1382-1388. 7. Innocenti F, Grimsley C, Das S, et al. Haplotype structure of the UDPglucuronosyltransferase 1A1 promoter in different ethnic groups. Pharmacogenetics. 2002;12:725-733. Erratum in: Pharmacogenetics. 2003;13:183. 8. Beutler E, Gelbart T, Demina A. Racial variability in the UDPglucuronosyltransferase 1 (UGT1A1) promoter: a balanced polymorphism for regulation of bilirubin metabolism? Proc Natl Acad Sci U S A. 1998;95:8170-8174. 9. Campostar [package insert]. New York, NY: Pfizer Inc; 2005.
Part 3: Test Application and Interpretation
9. E C O L I SHIGA TOXINS, EIA, STOOL Clinical Use: This test is used to diagnose Shiga toxinproducing Escherichia coli infection. Clinical Background: Escherichia coli Shiga toxins are in the same toxin family as that produced by Shigella dysenteriae type 1.1 The main types of Shiga toxins produced by E coli are Stx1 and Stx2. The bacteria that produce these toxins are transmitted to humans via E coli-contaminated food (undercooked meat, raw milk, vegetables, or fruit) and water, as well as by person-to-person and animal contact. Shiga toxin production in vivo may lead to asymptomatic infection or mild to severe gastrointestinal disease characterized by abdominal pain, watery or bloody diarrhea, and hemorrhagic colitis. Five to ten percent of cases progress to hemolytic uremic syndrome (HUS),2 a life-threatening complication that includes acute renal failure, microangiopathic hemolytic anemia, and severe thrombocytopenia and purpura.
241
Gastroenterology Reference Guide
Although HUS mortality is <10%, 30% of HUS survivors have significant sequelae, including chronic renal insufficiency, hypertension, diabetes, and neurologic defects.2 Children and the elderly are the most often affected. Treatment is primarily supportive, but early diagnosis may prevent unnecessary invasive diagnostic procedures (eg, appendectomy for severe abdominal pain) or inappropriate antibiotic therapy.3-5 Infected patients may be monitored for complications, enabling early intervention. Early diagnosis also helps limit further spread of the organism. Individuals Suitable for Testing include patients with diarrhea. Testing is strongly recommended for patients with bloody diarrhea or a history of bloody diarrhea; those with severe watery diarrhea and no evidence of other intestinal pathogens; those with HUS; and individuals epidemiologically linked to cases of Shiga toxin-producing E coli infection.2,6 Method: This test utilizes an enzyme immunoassay (EIA) that detects Stx1 and Stx2. The stool specimen is preincubated in GN broth for optimal sensitivity. The EIA uses monoclonal Stx1 and Stx2 capture antibodies, a polyclonal Shiga-like toxin antibody, and an enzyme-conjugated polyclonal IgG antibody for toxin detection. The analytical sensitivity is 7 pg/well for Stx1 and 15 pg/well for Stx2. The clinical sensitivity is 89%8 to 100%.9 The specificity for O157:H7 serotype is 99.7%, while the specificity for non-O157 serotype has not been evaluated.9 Synonyms for this test include Shiga-like toxin (SLT), verotoxin (VT), and Premier EHEC. Interpretive Information: A positive result (toxin detected) indicates the presence of Shiga toxin produced by E coli or Shigella dysenteriae type 1. Since Aeromonas hydrophila, A caviae, and Enterobacter cloacae
242
Gastroenterology Reference Guide
are known to produce Stx1 and since Citrobacter freundii may produce Stx2, presence of these organisms may also result in a positive test (studies not yet performed).2 Positive results have been obtained from several Pseudomonas aeruginosa strains.10 A negative result (not detected) indicates the absence of Shiga toxins or a level of toxin below that which can be detected by the test. Neither a positive nor a negative result precludes the presence of other infectious agents. References
1. McBrien AD, Karmali MA, Scotland SM. A proposal for rationalizing the nomenclature of the Escherichia coli cytotoxins. In: Karmali MA, Goglio AG (eds). Recent Advances in Verocytotoxin-Producing Escherichia coli Infections. Amsterdam: Elsevier Science BV. 1994; pp. 353-356. 2. Paton JC, Paton AW. Pathogenesis and diagnosis of Shiga toxinproducing Escherichia coli infections. Clin Microbiol Rev. 1998;11:450-479. 3. Walterspiel JN, Ashkenazi S, Morrow AL, et al. Effect of subinhibitory concentrations of antibiotics on extracellular Shiga-like toxin I. Infection. 1992;20:25-29. 4. Carter AO, Borczyk AA, Carlson JA, et al. A severe outbreak of Escherichia coli O157:H7associated hemorrhagic colitis in a nursing home. N Engl J Med. 1987;317:1496-1500. 5. Pavia AT, Nichols CR, Green DP, et al. Hemolytic-uremic syndrome during an outbreak of Escherichia coli O157:H7 infections in institutions for mentally retarded persons: clinical and epidemiologic observations. J Pediatr. 1990;116:544-551. 6. Karch H, Bielaszewska M, Bitzan M, et al. Epidemiology and diagnosis of Shiga toxin-producing Escherichia coli infections. Diagn Microbiol Infect Dis. 1999;34:229-243. 7. Tarr PI, Neill MA, Clausen CR, et al. Escherichia coli O157:H7 and the hemolytic uremic syndrome: importance of early cultures in establishing the etiology. J Infect Dis. 1990;162:553-556. 8. MacKenzie AM, Lebel P, Orrbine E, et al: Sensitivities and specificities of Premier E coli O157 and Premier EHEC enzyme immunoassays for diagnosis of infection with verotoxin (Shiga-like toxin)-producing Escherichia coli. J Clin Microbiol. 1998;36:1608-1611. 9. Kehl KS, Havens P, Behnke CE, et al. Evaluation of the premier EHEC assay for detection of Shiga toxin-producing Escherichia coli. J Clin Microbiol. 1997;35:2051-2054. 10. Beutin L, Zimmermann S, Gleier K. Pseudomonas aeruginosa can cause false-positive identification of verotoxin (Shiga-like toxin) production by a commercial enzyme immune assay system for detection of Shiga-like toxins (SLTs). Infection. 1996;24:267-268.
Part 3: Test Application and Interpretation
243
Gastroenterology Reference Guide
10. EPIDERMAL GROWTH FACTOR RECEPTOR (EGFR), IHC Clinical Use: This test is used to determine eligibility for cetuximab (Erbitux') treatment in patients with advanced metastatic colorectal cancer. Clinical Background: EGFR is a 170-kd receptor tyrosine kinase encoded by the c-erb-B (HER-1) protooncogene. It is expressed in various solid tumors, including colorectal, prostate, head and neck, and lung cancer, as well as in certain normal tissues. When bound by ligands such as epidermal growth factor (EGF) and transforming growth factor-, EGFR undergoes conformational changes that activate its intracellular tyrosine kinase activity, initiating autophosphorylation and downstream signal transduction pathways. Activation can mediate a variety of cellular responses, including gene expression, cell proliferation, and cell survival. Dysregulation of the EGFR signaling pathway due to EGFR overexpression, genetic aberrations, or other causes leads to malignant transformation. Thus, EGFR has become an important target for anticancer drug development; cetuximab is the first EGFR inhibitor to receive FDA approval for treatment of colorectal cancer. Cetuximab is a humanmouse chimeric monoclonal antibody directed against the extracellular ligandbinding domain of EGFR. This drug competitively inhibits binding of EGFR by EGF and transforming growth factor-, thereby blocking downstream signal transduction pathways and arresting cell growth. Cetuximab is indicated for treatment of advanced metastatic colorectal cancer resistant to irinotecanbased therapy, and as a single agent in patients who cannot tolerate irinotecan. Pre-treatment testing for
244
Gastroenterology Reference Guide
EGFR expression in tumor tissue is required, as only patients with EGFR-expressing tumors are eligible for cetuximab therapy. However, levels of EGFR expression do not appear to correlate with clinical response to cetuximab. Method: This immunohistochemical assay uses a mouse monoclonal anti-human antibody specific for the extracellular region of EGFR. Results are reported as positive or negative for detection of EGFR; values >0 (ie, 1+, 2+, or 3+) are considered positive. No cross-reaction with HER-2, HER-3, or HER-4 has been noted. Aliases include EGF Receptor, HER-1, cetuximab sensitivity, and Erbitux' sensitivity. Interpretive Information: A positive result indicates the presence of EGFR on cell membranes of tumor tissue and eligibility for treatment with cetuximab. A negative result suggests that the patient is not suitable for cetuximab treatment. Specimens from individuals with hepatitis B virus infection with HBsAg may exhibit non-specific staining with horseradish peroxidase. 11. FOOD ALLERGY: JOINT TASK FORCE GUIDELINES FOR DIAGNOSIS AND MANAGEMENT Introduction: Guidelines for diagnosis and management of food allergy have been developed by the Joint Task Force on Practice Parameters representing the American Academy of Allergy, Asthma, and Immunology; the American College of Allergy, Asthma, and Immunology; and the Joint Council of Allergy, Asthma and Immunology.1 Here we provide a summary of these guidelines with a particular focus on the use of laboratory testing for the diagnosis and management of food allergy (IgE245
Part 3: Test Application and Interpretation
Gastroenterology Reference Guide
mediated). It is important to bear in mind, however, that the majority of adverse reactions to food are not caused by IgE-mediated allergies. Refer to the complete Practice Parameter1 for more information on the differential diagnosis of non-IgE-mediated adverse food reactions. Clinical Background: It is important to diagnose food allergies to avoid unnecessary dietary restrictions that could negatively affect quality of life, nutritional status, and, in children, growth. The diagnostic algorithm developed by the Joint Task Force (Figure 2) begins with a relevant clinical history provided by the patient. This includes a list of suspected foods and the amount consumed, the time between ingestion and reaction, the type and duration of symptoms, repeatability of the reaction to the suspect food, requirement for cofactors (eg, exercise), and the time from last reaction. The second step is performance of a relevant physical examination including inspection of the upper and lower respiratory tract and the cutaneous and gastrointestinal (GI) systems. Third, determine if clinical and physical findings are consistent with an IgE-mediated reaction, which is characterized by a short time (ie, usually within minutes, rarely up to a few hours) from ingestion of the food to symptom onset, a severe reaction resulting from small amounts of food, an adverse reaction occurring with reexposure, and symptoms of pruritus, urticaria or angioedema, GI disturbance, rhinoconjunctivitis, bronchospasm, and anaphylaxis. Fourth, perform food-specific IgE testing when the history is consistent with an IgE-mediated food reaction. In vivo or in vitro tests can be used. Finally, perform an oral food challenge or trial elimination diet as indicated by food-specific IgE test results and clinical symptoms (see Figure 2).
246
Gastroenterology Reference Guide
Patient with adverse reaction to food
Part 3: Test Application and Interpretation
Relevant clinical history; physical examination including cutaneous, respiratory, and gastrointestinal systems
History consistent with IgEmediated food reaction
Yes Food-specific IgE Testing
No Further evaluation for non-IgE-mediated immunologic or nonimmunologic reactions
Negative Tested foods likely to be tolerated; consider open challenge
Positive with history of anaphylaxis Avoidance of problem food
Positive without history of anaphylaxis
Symptoms resolve
Symptoms persist
Episodic symptoms
Chronic symptoms
Oral Challenge
Trial Elimination Diet
Positive Avoidance of problem food
Negative Tested foods likely to be tolerated
Symptoms persist
Symptoms resolve Probable food allergy; consider oral challenge
Periodic reassessment if clinically indicated
Reprinted with permission from the American College of Allergy, Asthma, and Immunology.
Figure 2. Diagnosis and management of food allergy. 1
Individuals Suitable for Testing include individuals who have a history consistent with an IgE-mediated food reaction as described above. Test Availability: Available tests include food-specific IgE tests such as in vivo skin prick or puncture tests (intracutaneous or percutaneous) and in vitro (serum) tests (eg, ImmunoCAP', AlaSTAT', HY-
247
Gastroenterology Reference Guide
TEC') as well as oral food challenge tests and a trial elimination diet. In vivo food-specific IgE testing has a high negative predictive value (95%) but a low positive predictive value ( 50%). These tests are useful, therefore, as an initial test to rule out an IgE-mediated reaction to a highly suspected food. Percutaneous skin tests (PSTs) are recommended over intracutaneous tests because intracutaneous tests are overly sensitive, and thus have a high rate of false-positive results, and are associated with risk of anaphylaxis and death. In vitro IgE tests have roughly the same sensitivity and specificity as in vivo IgE tests and consequently have the same clinical application. In vitro tests are especially useful when the patient has a history of a life-threatening reaction or a medical condition that prevents accurate skin testing (eg, extensive atopic dermatitis or dermatographism) and when the patient is known to have a nonreactive histamine control or is known to be pregnant. Radioimmunoassay procedures (radioallergosorbent test [RAST]) are no longer used. Current methods use a foodspecific allergen bound to a solid phase to detect IgE in the patients serum. World Health Organizationbased standards are used to quantify results, which are reported in kIU/L. Oral food challenge tests and trial elimination diets (Table 13) may lead to or confirm a diagnosis of food allergy and may be useful for patient management. Interpretive Information: A negative food-specific IgE test result generally indicates lack of an IgE-mediated food reaction and probable tolerance of the food. However, results may be affected by the patients age, the reagents used, and the testing techniques used. For example, tests that use extracts from foods with
248
Gastroenterology Reference Guide
Table 13. Non-cutaneous In Vivo Tests Used in Diagnosis and Management of Food Allergy*
Food Challenge Test Definition
Open challenge Uses either suspect food in its natural form or a placebo; not blinded to patient or physician Uses either suspect food (given in gradually increasing amounts) or a placebo disguised and blinded to the patient; reactions are judged by patient and physician Uses either suspect food (given in gradually increasing amounts) or a placebo disguised and blinded to the patient and the physician; reactions are judged independently by patient and physician Eliminates suspected foods from the diet for several weeks and then gradually reintroduces them one at a time with reactions observed
Part 3: Test Application and Interpretation
Advantages
Disadvantages
Simplest to perform; Subject to patient best when several and physician bias; foods are suspect positive result may require blinded confirmation testing Eliminates patient Test interpreter bias and need for potentially biased test interpreter to be blinded; offers protocol flexibility
Oral challenge Single-blind
Double-blind
Gold standard for diagnosis of food allergy
Requires a third person to prepare the blinded food
Trial elimination diet
Best when symptoms are chronic; replaces individual food challenges when several suspect foods have been identified
Positive result requires compelling supportive evidence for a definitive diagnosis
*Anaphylaxis is a risk and thus food challenges should be performed where emergency treatment is readily available.
stable proteins (eg, peanut, milk, egg, tree nuts, fish, and shellfish) are more reliable than those that use extracts from foods with labile proteins (eg, some
249
Gastroenterology Reference Guide
fruits and vegetables). In vitro tests and PSTs use purified antigen that may differ from food challenge antigen that is raw, cooked, or otherwise processed resulting in seemingly inconsistent results. Furthermore, in vivo skin tests are affected by the skin test devices used, the location of test placement, and the mode of measurement. In the event of a severe reaction and a negative test result, an open food challenge may be appropriate to rule out a food allergy. Preparation for a possible anaphylactic response should be made prior to the food challenge. A positive food-specific IgE test result in a patient with a history of anaphylactic response to that food is considered diagnostic. There is no need for further testing. Since a positive test alone does not necessarily indicate ingestion of the food will result in a clinical response, further testing is required (Figure 2) in patients without an anaphylactic response to rule out cross-reacting proteins or other causes of a falsepositive result (eg, eosinophilic gastroenteropathy). A larger PST response size or greater concentration of IgE correlates with a greater likelihood of a clinical reaction to the food, but does not correlate with the type or severity of that reaction. Interpretation of these and other available diagnostic tests is summarized in Table 14. Patient Management: The following steps may be taken when managing a patient with a food allergy. First, educate and advise the patient to avoid the specific food allergen. Educational topics include how to read food labels, including an awareness of risk imposed by unfamiliar terms and crosscontamination during food processing; available dietary alternatives, including supplements; and how
250
Gastroenterology Reference Guide
Table 14. Interpretation of Tests Used for Diagnosis of Food Allergy
Tests Food-specific IgE testing Positive Test Results With history of anaphylaxis: diagnostic; no further testing needed Without history of anaphylaxis: suggestive, but not diagnostic; further testing needed Open oral food challenge Single blind oral food challenge Double blind oral food challenge Reaction is suggestive of food allergy, but results are prone to bias Reaction is suggestive of food allergy, but results are prone to bias Reaction is highly suggestive of food allergy Negative Test Results Tested foods are likely to be tolerated (negative predictive value 95%) Consider open challenge in some cases with severe reaction Tested foods are likely to be tolerated Tested foods are likely to be tolerated irrespective of foodspecific IgE test results Tested foods are likely to be tolerated irrespective of food-specific IgE test results Perform oral challenge when chronic symptoms persist
Part 3: Test Application and Interpretation
Trial elimination Food allergy is probable when diet chronic symptoms resolve
to avoid unintentional food allergen exposure (eg, in schools or restaurants. Second, educate and advise the patient on treating an anaphylactic response (eg, use of injectable epinephrine with or without antihistamine and seeking medical care for a systemic reaction). Third, perform periodic testing to determine newly-developed tolerance. Avoidance of the food allergen may lead to future tolerance. Additionally, children are likely to outgrow some types of food allergies (eg, cows milk, wheat, and egg). A subsequent negative food-specific IgE test is likely to indicate tolerance to the food; however, a positive test is inconclusive since these tests may remain positive even when the patient no longer has clinical symptoms. An oral food challenge may be helpful in determining current tolerance status.
251
Gastroenterology Reference Guide
Reference
1. American College of Allergy, Asthma, and Immunology. Food allergy: a practice parameter. Ann Allergy Asthma Immunol. 2006;96:S1-S68.
12. H E L I C O B A C T E R P Y L O R I INFECTION 12.1 Laboratory Support of Diagnosis and Management Clinical Background: Helicobacter pylori has been associated with duodenal and gastric ulcers and chronic active, chronic persistent, and atrophic gastritis in adults and children. Infected persons have a 2- to 6-fold increased risk of developing gastric cancer and mucosal-associated-lymphoid-type (MALT) lymphoma. About 70% to 90% of infected individuals respond to a multiple-drug regimen over a 1- to 2-week period. Individuals Suitable for Testing: Testing is appropriate for symptomatic individuals with active peptic ulcer disease, a history of documented peptic ulcer, or MALT lymphoma, and to confirm eradication post-therapy. Diagnostic testing is not recommended for asymptomatic individuals without a history of peptic ulcer disease or those on longterm proton pump inhibitor (PPI) therapy for gastroesophageal reflux disease (GERD). Testing is also not recommended for patients with dyspeptic symptoms due to use of non-steroidal antiinflammatory drugs or Cox-2 inhibitors.1 Testing should be performed only when treatment is intended, or to document H pylori eradication. Children under age 18 may be tested with the stool antigen assay.
252
Gastroenterology Reference Guide
Test Availability
Part 3: Test Application and Interpretation
Several methods can be used to diagnose H pylori infection: 1) upper gastrointestinal tract biopsy with histologic exam, rapid urease testing (RUT), or culture; 2) urea breath test employing 14C- or 13Curea; 3) antigen detection in stool; and 4) antibody detection. Biopsy-Based Assays When endoscopy is indicated, RUT or histologic examination is useful to determine the presence of H pylori infection.1 Culture is not very sensitive but may be useful for antibiotic resistance testing in patients unresponsive to therapy.1,2 Non-Invasive Assays The urea breath test (UBT) and stool antigen test are recommended by both the American Gastroenterological Association (AGA) and the American College of Gastroenterologists (ACG) as the preferred non-invasive tests for diagnosis and confirmation of eradication.1,3 Both methods are highly sensitive and specific and are useful for diagnosis, therapeutic monitoring, and test of cure (Table 15). Serology-based methods cannot distinguish between active and resolved infection. Thus, they are not recommended for monitoring infection or confirming eradication of the organism.2-4 They are also not the first choice for diagnosis.1,2,4
253
Gastroenterology Reference Guide
Table 15. Characteristics of Non-invasive Tests for H pylori
Clinical Utility Urea Breath Test (UBT)5 Diagnose current infection Assess treatment response Document cure 13 CO2 release Infrared spectrometry 13 C-urea Antigen Detection6 Diagnose current infection Assess treatment response Document cure H pylori antigen Enzyme immunoassay Polyclonal anti-H pylori antibody 96 (95% CI, 9099) 95 (95% CI, 7499.9) 96 (95% CI, 9099) 96 (95% CI, 9099) None known Very low antigenic levels Proton pump inhibitors Antibiotics Bismuth-containing compounds Cleared Stool 24 hours 3 days 3 days Frozen
Measures Method Primary reagent Sensitivity, %* For diagnosis For eradication* Specificity, % For diagnosis For eradication* False positives False negatives
95 (95% CI, 9397) 97 (95% CI, 9399) 90 (95% CI, 7398) 95 (95% CI, 8998) Achlorhydria; other urease-producing organisms (eg, H heilmannii) Proton pump inhibitors Antibiotics Bismuth-containing compounds
FDA status Sample type Sample stability Ambient Refrigerated Frozen Sample handling
Cleared Breath 3 days Not applicable Not applicable Room temperature
CI, confidence interval. *Testing performed at least 4 weeks after end of therapy for H pylori eradication.
Test Selection and Interpretation Diagnosis Patients >55 Years of Age or with Alarm Features Prompt esophagogastroduodenoscopy is recommended for symptomatic patients >55 years of age and younger patients with alarm features (eg, anemia, gastrointestinal bleeding, family history of
254
Gastroenterology Reference Guide
gastrointestinal cancer, early satiety, unintended weight loss of >10%, history of esophagogastric malignancy, previous documented peptic ulcer, progressive dysphagia, odynophagia, persistent vomiting, palpable mass or lymphadenopathy, or jaundice).1,3,4 Biopsy samples obtained during endoscopy may be used for diagnosis of H pylori infection using RUT, histology, or culture; patients with positive results should be offered H pylori eradication therapy. Patients 55 Years of Age Without Alarm Features Although current guidelines differ somewhat, 2 main approaches are used for diagnosis of H pylori infection in patients 55 years of age without alarm features1,3: 1) Test and treat: First, test with a noninvasive assay for H pylori infection (eg, UBT or stool antigen). Positive results indicate the need for treatment to eradicate H pylori, followed by a trial of acid suppression if symptoms persist after successful eradication. Negative results are followed by a 4- to 8-week empiric trial of acid suppression therapy with a PPI. 2) Empiric treatment: A 4- to 8-week trial of empiric acid-reducing therapy with a PPI. If the PPI trial fails or the patient relapses after the end of treatment, the test-and-treat strategy should be pursued before contemplating endoscopy.1 Post-therapeutic Testing Follow-up testing with a non-invasive assay (UBT or stool antigen), or an endoscopy-based assay if endoscopy is indicated, has been recommended to confirm eradication of H pylori infection after therapy.2 If endoscopy is performed, culture may be
255
Part 3: Test Application and Interpretation
Gastroenterology Reference Guide
useful to assess H pylori antibiotic sensitivity after failed eradication therapy.1 UBT and antigen-based testing should be performed no sooner than 4 weeks post-therapy. References
1. Talley NJ; American Gastroenterological Association. American Gastroenterological Association medical position statement: evaluation of dyspepsia. Gastroenterology. 2005;129:1753-1755. 2. Malfertheiner P, Megraud F, OMorain C,et al. Current concepts in the management of Helicobacter pylori infectionthe Maastricht 2-2000 Consensus Report. Aliment Pharmacol Ther. 2002;16:167-180. 3. Talley NJ, Vakil N; Practice Parameters Committee of the American College of Gastroenterology. Guidelines for the management of dyspepsia. Am J Gastroenterol. 2005;100:2324-2337. 4. Talley NJ, Vakil NB, Moayyedi P. American Gastroenterological Association technical review on the evaluation of dyspepsia. Gastroenterology. 2005;129:1756-1780. 5. BreathTek UBT for H pylori [package insert]. Lafayette, Colorado: Meretek Diagnostics Inc; 2005. 6. Premier Platinum HpSA [package insert]. Cincinnati, Ohio: Meridian Bioscience Inc; 2001.
12.2 Helicobacter pylori Antigen Clinical Use: This test is used for differential diagnosis of peptic ulcer disease and chronic active gastritis, and for therapeutic monitoring and documentation of cure in patients with H pylori infection. Method: This enzyme immunoassay employs a polyclonal anti-H pylori capture antibody adsorbed to microwells and a peroxidase-conjugated polyclonal detection antibody. Based on the intensity of color developed, results are reported as H pylori antigen not detected, equivocal, or detected. Performance characteristics have not been established for watery diarrheal stools or for asymptomatic individuals.
256
Gastroenterology Reference Guide
Interpretive Information: A positive result (antigen detected) is indicative of H pylori presence (96% sensitivity); however some individuals may have H pylori antigen but no disease. A negative result (antigen not detected) indicates absence of H pylori or an antigenic level below the assay limit of detection (184 ng H pylori protein/mL of stool) (96% specificity). False-negative results may be obtained on specimens from patients who have ingested selected compounds (antimicrobials, proton pump inhibitors, bismuth preparations) within the 2 weeks prior to specimen collection. In populations with disease prevalence ranging from 34% to 69% (average 52%), the positive and negative predictive values were 96%. A positive result 7 days post-therapy is indicative of treatment failure. A negative result 4 weeks posttherapy indicates eradication of the infection. 12.3 Helicobacter pylori Urea Breath Test (UBiT) Clinical Use: This test is used for differential diagnosis of patients with peptic ulcer disease and chronic active gastritis and for therapeutic monitoring in patients with Helicobacter pylori infection. Method: This urea breath test indirectly detects the presence of H pylori-associated urease by measuring CO2 in the patients breath. A baseline breath sample is collected before the patient ingests 13C-urea, ie, urea labeled with a naturally occurring, nonradioactive carbon isotope. A second sample is collected shortly after the ingestion. H pyloriassociated urease degrades the urea, producing ammonia and CO2. The resultant CO2 is absorbed in the blood and then exhaled. An increase in the ratio
Part 3: Test Application and Interpretation
257
Gastroenterology Reference Guide
of 13CO2 to 12CO2 between the pre- and post-ingestion samples indicates presence of H pylori-associated urease. Interpretive Information: A negative result indicates the absence of H pylori-associated urease but does not rule out the possibility of H pylori infection. Falsenegative results may be due to antimicrobials, proton pump inhibitors (PPIs), and bismuth preparations ingested by the patient within 2 weeks prior to testing or due to collection of a test sample before the recommended interval following 13C-urea ingestion. When clinical signs warrant, a repeat test should be considered with this, or an alternative, test method. Children under age 18 may be tested, but sex, age, and weight are required to interpret results. A positive result is associated with the presence of H pylori infection, other gastric spiral organisms such as H heilmannii, and achlorhydria. 13. HEPATITIS 13.1 Viral Hepatitis: Laboratory Support of Diagnosis and Management Clinical Background: Viral hepatitis is a relatively common disease (25 per 100,000 individuals in the United States) caused by a diverse group of hepatotropic agents that lead to liver inflammation and cell death. Five hepatitis viruses have been well characterized (A, B, C, D, and E; Table 16), and others have been identified (F and G). Hepatitis A and E viruses (HAV, HEV) are transmitted through the fecal-oral route and manifest as acute or asymptomatic disease. There is no chronic carrier state and serious sequelae are rare. Hepatitis
258
Gastroenterology Reference Guide
Table 16. Clinical Spectrum of Viral Hepatitis
Part 3: Test Application and Interpretation
Hepatitis Transmission Virus A B C D E Fecal-oral Parenteral, perinatal, sexual Incubation Mortality Likelihood of Likelihood of Association with Period (%) Carrier State Chronic Disease Hepatocellular (weeks) Carcinoma 2-6 1 None None No 4-26 1-2 1-5 2-20 1-2 10% (adults) 90% (infants) 50%-80% Variable None 1%-10% 80%-90% 80% in superinfection* None Yes Yes Yes* No
Parenteral, perinatal 2-23 & possibly sexual Parenteral, sexual, perinatal Fecal-oral 6-26 2-9
*Requires coinfection with HBV. Simultaneous infection with HBV is associated with severe acute disease and low likelihood of chronic infection (<5%); superinfection of HBV carries high likelihood of fulminant disease (2%-20%), chronic HDV infection (up to 80%), and cirrhosis (60%-70%), and may progress to hepatocellular carcinoma. 15%-20% in pregnant women.
B, C, and D viruses (HBV, HCV, HDV) establish persistent infections with significant morbidity and mortality. All 3 are transmitted parenterally. HBV and HCV are also transmitted through sexual contact and perinatally. HDV is unique in that it is a defective virus that can replicate only in the presence of HBV. HDV coinfection (HDV and HBV) significantly increases the severity of disease. Acute HCV infection may be asymptomatic, but most infections are chronic; chronic infection may lead to cirrhosis and hepatocellular carcinoma. In the United States, viral hepatitis is generally caused by HAV, HBV, or HCV. Other causative viruses include cytomegalovirus (CMV), Epstein-Barr virus (EBV), and human immunodeficiency virus (HIV). Hepatitis may also be due to other diseases or medications. A variety of immunologic and molecular assays are available for diagnosing viral hepatitis and monitoring treatment response. This guide provides
259
Gastroenterology Reference Guide
an overview of available tests and indications for their use. Individuals Suitable for Testing include (1) individuals with clinical symptoms or abnormal liver enzyme levels; (2) children born to infected women, especially those who are HBV e antigen (HBeAg)positive; (3) household or sexual contacts of infected persons or carriers; (4) individuals participating in high-risk sexual activities (multiple sexual partners, same-sex intercourse); (5) intravenous drug users; (6) recipients of organ transplants or multiple blood transfusions; (7) hemodialysis patients; (8) recent visitors or immigrants from endemic areas; and (9) health care workers. Available Tests: Tests for antibodies and antigens are available for hepatitis A-E, including those specific for hepatitis B core, surface, and e proteins. Techniques for antibody detection include enzyme immunoassay (EIA) and recombinant immunoblot assay (RIBA'). EIA technology is also used for antigen testing. Branched DNA (bDNA), solution hybridization-hybrid capture (Digene), transcription-mediated amplification (TMA), and polymerase chain reaction (PCR) are used for DNA and RNA testing to determine the presence of viremia and measure the viral load. HCV and HBV genotypes can also be determined with hybridization or sequencing-based assays. Test Selection Diagnose Acute Infection Four initial tests are generally recommended to diagnose acute hepatitis (Figure 3): HAV immunoglobulin M (IgM) antibody, HBV core IgM antibody (HBcAb, IgM), HBV surface antigen (HBsAg), and HCV antibody by EIA. HAV IgM
260
Gastroenterology Reference Guide
Symptomatic or high-risk individual
Part 3: Test Application and Interpretation
HAV IgM Ab HAV IgM Ab+
HAV infection unlikely HAV infection
Test for:
HAV IgM Ab HBc IgM Ab HBs Ag HCV Ab (EIA)
HBc IgM Ab HBsAg HBc IgM Ab+ or HBsAg+
HBV infection unlikely Consider test for HDV Ab
HDV Ab HBc IgM Ab+ HDV Ab+ HBc IgM Ab HDV Ab+
HDV infection unlikely HBV with HDV coinfection HBV with HDV superinfection
HBV infection
HCV Ab (EIA) HCV Ab (EIA)+, s/co >8* HCV Ab (EIA)+, s/co 1 but <8.0*
HCV infection unlikely Active or resolved HCV infection
Confirm with HCV RNA tes t or RIB A
HCV RNA+
HCV RNA
RIBA+
RIBA
RIBA indeterminate
HCV infection
Active HCV infection unlikely; rule out active or resolved infection with RIBA
Active or resolved HCV infection
HCV infection unlikely
Test for HCV RNA, or repeat RIBA 1 month later
Note: If infection is not diagnosed in a symptomatic individual, consider testing for HEV. *s/co (signal-to-cutoff ratio) is specific to the chemiluminescent EIA used by Quest Diagnostics.
Figure 3. Diagnosis of acute hepatitis. antibody is the preferred test for diagnosis of acute hepatitis A infection because it rises early and persists only 3 to 12 months. HBcAb IgM is detectable during acute but not chronic HBV infection. HBsAg, however, is detectable in both stages. Simultaneous use of these 2 tests therefore not only detects both acute and chronic HBV infection, but also helps to
261
Gastroenterology Reference Guide
differentiate between them. The EIA (antibody test) is used as the initial assay for diagnosing HCV infection because of its high sensitivity, wide availability, and low cost. However, antibody is not detected for many months after infection. RNA tests can detect virus prior to seroconversion and serve to differentiate between active and resolved infection. RIBA may be used in patients with positive EIA results and negative HCV RNA results, although a repeat HCV RNA assay may also be used in this setting. A negative RIBA result is required for re-entry into the blood donor pool. In cases of fulminant hepatitis, the possibility of coinfection or superinfection (HBV with HCV or HDV) should be explored (Figure 3). Diagnose Chronic Infection When screening for chronic hepatitis, 2 laboratory tests are recommended (Figure 4): HBsAg and HCV antibody by EIA. Positive HBsAg results obtained 6 months or more after the initial diagnosis indicate chronic infection. Either HBV DNA or the HBeAg assay can be used for confirmation. HCV RNA testing is used to confirm positive HCV antibody results, but when clinical suspicion is high and results from the 2 tests are discrepant, RIBA can be helpful. HDV infection should be considered in chronic HBV carriers who experience a further acute attack and/or rapidly progressive liver disease. The HDV antibody assay is recommended for the initial test; positive results may be followed by the HDV antigen test for confirmation. HDV antigen testing may also be useful in HBsAg-positive/HDVAb-negative individuals if coinfection or superinfection is strongly suspected.
262
Gastroenterology Reference Guide
HBsAg with no clinical symptoms HBsAg with clinical symptoms
HBV infection unlikely
Part 3: Test Application and Interpretation
Test for HB V DNA +
HBV infection unlikely HBV infection
Test for:
HBsAg HCV Ab
HBsAg+
HBV infection
Consider test for HDV Ab
HCV Ab (EIA) HCV Ab (EIA)+, s/co >8* HCV Ab (EIA)+, s/co 1 but <8*
HCV infection unlikely Active or resolved HCV infection
HDV Ab HDV Ab+
HDV infection unlikely HBV/HDV infection
Confi rm with HCV RNA test or RIBA
HCV RNA+
HCV RNA
RIBA+
RIBA
RIBA indeterminate
HCV infection
Active HCV infection unlikely; rule out active or resolved infection with RIBA
Active or resolved HCV infection
HCV infection unlikely
Test for HCV RNA, or repeat RIBA 1 month later
*s/co (signal-to-cutoff ratio) is specific to the chemiluminescent EIA used by Quest Diagnostics.
Figure 4. Diagnosis of chronic hepatitis. Demonstrate Carrier Status Following disappearance of clinical symptoms, carrier status can be demonstrated by testing for persistence of HBV antigen, HBV DNA, or HCV RNA. For HBV, the presence of the following conditions indicates inactive carrier state: HBsAg positive for 6 months, HBeAg-negative, HBeAb-positive, serum HBV DNA <105 copies/mL, and persistently normal ALT/AST
263
Gastroenterology Reference Guide
levels. For HCV, use a quantitative or qualitative RNA test. For HDV, use the HDV antigen test. Demonstrate Recovery or Differentiate Between Active and Resolved Infection Differentiating current vs past infection is possible using HBV DNA, HBsAg, and HBeAg testing for HBV; highly sensitive quantitative or qualitative HCV RNA testing for HCV; and antigen testing for HDV. Recovery from hepatitis B (in patients with known history of acute or chronic HBV or the presence of HBcAb and/or HBsAb) is signaled by the disappearance of HBsAg and HBV DNA along with persistently normal ALT levels. Some individuals have detectable DNA after disappearance of HBsAg. While this may not be associated with active disease in immunocompetent individuals, it may represent treatment failure or failure of natural immunity when HBsAb is absent. Additionally, HBV DNA-positive individuals may be at risk for recurrent HBV disease and HBV DNA-positive organ donors could potentially transmit the infection to organ transplant recipients. HCV recovery is indicated by repeatedly negative HCV RNA test results. HDVAg disappears within months after recovery. Assist with Treatment Decision-making and Therapeutic Monitoring (Figure 5) The alanine aminotransferase (ALT) assay is important when assessing liver function. In chronic HBV infection, the baseline ALT level is associated with the likelihood of treatment response; elevated ALT in the presence of a positive HBV DNA assay is an indication for treatment initiation. Quantitative HBV DNA assays can help assess the likelihood of response to treatment, monitor response to therapy, and predict the emergence of resistance to antiviral
264
Gastroenterology Reference Guide
3A
Part 3: Test Application and Interpretation
Diagnosed HAV infection
ALT levels every 1 to 2 weeks until normal
3B
Acute ALT levels every 1 to 2 weeks until normal HBsAg HBsAb after 6 months HBsAg HBsAb+ HBsAg+ HBsAb Resolved infection Chronic infection
Diagnosed HBV infection
Chronic Monitor therapy with HBV DNA
3C Diagnosed chronic HBV/ HDV infection 3D
Negative Acute Monitor ALT levels periodically for 6 months HCV RNA assay after 6 months Positive
Monitor therapy with HBV DNA and HDV Ag
Probable resolved infection Chronic infection
Diagnosed HCV infection
Chronic Perform HCV genotyping and measure viral load at baseline to guide duration of treatment Monitor therapy with HCV RNA assay*
*Refer to Molecular Testing in the Management of Hepatitis C Virus Infection, section 13.3.1, for more detailed information.
Figure 5. Laboratory management of patients with hepatitis. 3A, hepatitis A; 3B, hepatitis B; 3C, hepatitis B with D coinfection or superinfection; 3D, hepatitis C. agents. The HBV genotyping assay is used to determine the HBV genotype, which is important for epidemiologic studies and may be associated with the clinical course and response to therapy. The HBV genotype assay can also detect the emergence of
265
Gastroenterology Reference Guide
mutations associated with resistance to antiviral drugs. In HCV infection, elevated ALT in the presence of a positive HCV RNA assay is an indication for treatment initiation. Highly sensitive qualitative and quantitative HCV RNA tests are useful to monitor response to therapy and document resolved infection. Quantitative RNA tests can also help predict the likelihood of response and select the appropriate duration of therapy. The HCV genotype assay is important for selecting the appropriate duration of therapy and evaluating the likelihood of treatment response. Screen for Immunity or Successful Vaccination HAV total antibody, HBsAb, or HBc total antibody assays are generally recommended to determine immune status following infection, pre- or postvaccination or post-administration of immune globulin. Multiple tests may be required to completely characterize an individual patients infection. To further clarify the role of the available viral hepatitis tests, specific clinical applications for each are addressed in Table 17. Figures 35 provide algorithms for the use of diagnostic assays in the diagnosis and management of viral hepatitis. Test Interpretation: A negative antibody test result indicates lack of immunologic response to that type of hepatitis virus. False-negative results may occur in early-stage acute disease (prior to seroconversion) or in patients with a suppressed or non-functioning immune system. If clinical suspicion is high, negative results can be verified by testing for type-specific antigen, DNA, or RNA, as appropriate.
266
Gastroenterology Reference Guide
Table 17. Clinical Application of Laboratory Tests for Hepatitis
Test Alanine Aminotransferase (ALT) Clinical Application Indicate hepatic disease Monitor response to antiviral therapy Indicate resolution of HAV or HEV infection First-line diagnostic test for acute hepatitis A Screen for immunity prior to vaccination First-line diagnostic test for acute hepatitis B Indicate recent infection (within preceding 46 months) Indicate current or prior infection Determine need to treat chronic HBV infection Indicator of chronic hepatitis when still positive 6 months after diagnosis of acute HBV infection Monitor response to therapy Demonstrate viral replication in patients with mutant HBV (eg, HBeAg- and HBeAb+ individuals) All indications listed for qualitative HBV DNA assay above Predict likelihood of response to therapy Indicate emergence of resistant variants during antiviral therapy Indicate treatment response Indicate active viral replication and high infectivity Detect HBV mutations associated with resistance to antiviral agents Predict and monitor response to therapy Identify HBV genotype (AG) for epidemiologic and prognostic purposes Detect mutations in precore and basal core promoter regions, which may influence immune response and outcome Indicate immunity post-infection, vaccination, or HBIG Indicate immunity post-infection, vaccination, or HBIG; high levels are suggestive of a protective response First-line diagnostic test for acute hepatitis B Indicates chronic hepatitis when still positive 6 months after diagnosis of acute HBV infection
Part 3: Test Application and Interpretation
HAV Antibody (IgM) HAV Total Antibody HBV Core Antibody (IgM)
HBV Core Total Antibody (IgG + IgM) HBV DNA, Qualitative
HBV DNA, Quantitative
HBV e Antibody HBV e Antigen HBV Genotype
HBV Surface Antibody, Qualitative HBV Surface Antibody, Quantitative
HBV Surface Antigen
267
Gastroenterology Reference Guide
Table 17. Clinical Application of Laboratory Tests for Hepatitis (cont.)
Test HBV Surface Antigen Confirmation HCV Antibody, EIA HCV Antibody, RIBA Clinical Application Routinely used to confirm positive HBV surface antigen tests First-line screening test for detection of acute and chronic hepatitis C Confirm infection when the antibody and RNA tests are discrepant and clinical suspicion is high; negative result required for re-entry to blood donor pool Predict likelihood of therapeutic response Determine the duration of treatment Detect acute infection prior to seroconversion (ie, within 1-2 weeks post-exposure) Confirm EIA diagnosis of acute or chronic infection (LOD <50 IU/mL) Differentiate between resolved and active infection Demonstrate resolution of infection Highly sensitive quantitative assays (at least as sensitive as relevant qualitative assay) only: all indications listed for qualitative HCV RNA assay above Predict response to antiviral therapy Differentiate lack of therapeutic response from partial therapeutic response Diagnose HDV infection in patients with fulminant hepatic failure or known previous HBV infection Diagnose HDV infection in symptomatic, HBsAg-positive, HDV antibody-negative individuals Demonstrate recent or past hepatitis E infection Diagnose acute HEV infection
HCV Genotyping HCV RNA, Qualitative
HCV RNA, Quantitative
HDV Antibody
HDV Antigen
HEV Antibody (IgG) HEV Antibody (IgM)
HBIG, hepatitis B immune globulin; LOD, limit of detection.
If an antibody test is positive, the patient has generated an immune response to that type of hepatitis virus and should be evaluated further with type-specific supplemental testing (eg, antigen, DNA, or RNA testing). In an infant less than 18 months of age, a positive antibody test result may indicate
268
Gastroenterology Reference Guide
passive transfer of maternal antibody. Testing with a type-specific antigen or nucleic acid-based assay may reveal active infection. Additional antibody-specific interpretive information follows: Presence of total HAV antibody, in the absence of HAV IgM antibody, indicates immunity against HAV infection. HBc IgM antibody positivity usually indicates HBV infection within the preceding 4 to 6 months. HBc IgG antibody positivity indicates prior HBV infection and may be associated with chronic or resolved infection. HBeAb presence indicates resolving infection or response to therapy. HBsAb presence indicates immunity against HBV infection. A positive HDVAb test, coincident with the presence of HBsAg, indicates HBV/HDV coinfection. False-positive HCV antibody results may be generated by the EIA in cases of alcoholic liver disease, autoimmune chronic active hepatitis, or improper sample storage and testing conditions. A positive HCV RNA test result confirms a positive EIA result. In the presence of a positive EIA result, a negative HCV RNA result should be confirmed by repeat RNA assay or RIBA. A negative RIBA excludes HCV as the cause of a positive EIA result and is required for re-entry into the blood donor pool. A negative HBsAg, HBV DNA, or HCV RNA test result indicates lack of current infection. In rare cases, a negative result reflects a viral load below the assays limit of detection. Thus, a negative result does not exclude the possibility of infection. Repeatedly
269
Part 3: Test Application and Interpretation
Gastroenterology Reference Guide
positive antigen, DNA, or RNA test results, on the other hand, indicate active infection. A return to a negative test result following therapy indicates resolution of the infection. After resolution, reappearance of a marker may indicate a relapse. HBsAg presence does not reflect the level of active virus, nor does it differentiate between acute and chronic infection or between mild and severe disease. False-positive results are uncommon, but when they occur they are generally due to technical limitations of the test. In low-risk populations, the HBsAg confirmation test can help verify a repeatedly reactive result as a true positive. Relatively low levels of HBV DNA or HCV RNA are associated with acute or resolving infection and with the probability of a sustained therapeutic response; high levels predict lack of therapeutic response. In general, a stable or rising viral load is indicative of lack of therapeutic response, while falling levels indicate that the patient is responding to treatment. Persistent detection of HCV RNA after 3 months of interferon monotherapy or 6 months of interferon/ribavirin combination therapy indicates that sustained response to therapy is unlikely. Recent studies have shown, however, that a small subset of these patients may still benefit from further therapy. DNA and RNA levels need to be interpreted in combination with all available clinical, biochemical, and liver biopsy information. Even after apparent recovery from HBV infection, viable virus may remain in the liver where it can be detected in biopsy material, can infect a transplant recipient who is HBcAb negative, and may even cause recurrent HBV disease in individuals with profound immunosuppression.
270
Gastroenterology Reference Guide
Table 18. Diagnosis of Acute Hepatitis
Part 3: Test Application and Interpretation
Hepatitis Virus A B B with D coinfection B with D superinfection C E HAV IgM + HBsAg + + + HBV HBc HBc HCV HCV HDV HDV HEV HEV DNA IgM Total Ab RNA Ag Ab IgM IgG + + + + + + + + + + + + /+
Tables 18-20 detail test result patterns and their associated clinical significance. References
1. Buti M, Sanchez F, Cotrina M, et al. Quantitative hepatitis B virus DNA testing for the early prediction of the maintenance of response during lamivudine therapy in patients with chronic hepatitis B. J Infect Dis. 2001;183:1277-1280. 2. EASL International Consensus Conference on Hepatitis C. Paris, 26-28 February, 1999, Consensus Statement. European Association for the Study of the Liver. J Hepatol. 1999;30:956-961. 3. Hepatitis Resource Network. Hepatitis C treatment algorithm. Available at http://www.h-r-n.org. Accessed January 9, 2002. 4. Hoofnagle JH, di Bisceglie AM. Serologic diagnosis of acute and chronic viral hepatitis. Semin Liver Dis. 1991;11:73-83. 5. Hu KQ, Vierling JM. Molecular diagnostic techniques for viral hepatitis. Gastroenterol Clin North Am. 1994;23:479-498. 6. Kao JH, Chen PJ, Lai MY, et al. Genotypes and clinical phenotypes of hepatitis B virus in patients with chronic hepatitis B virus infection. J Clin Microbiol. 2002;40:1207-1209. 7. Kao JH, Wu NH, Chen PJ, et al. Hepatitis B genotypes and the response to interferon therapy. J Hepatol. 2000;33:998-1002. 8. Lindh M, Hannoun C, Dhillon AP, et al. Core promoter mutations and genotypes in relation to viral replication and liver damage in East Asian hepatitis B virus carriers. J Infect Dis. 1999;179:775-782.
Table 19. Diagnosis of Chronic Hepatitis
Hepatitis Virus B C HBsAg + HBsAb HBc IgM HBc Total + HBeAg + HBe Ab HBV DNA + HCV Ab - + HCV RNA +
271
Gastroenterology Reference Guide
Table 20. Interpretation of Hepatitis B Markers
Marker Acute (Early) Acute (Resolving) Chronic (Low Infectivity) ++ + Chronic (High Infectivity) ++ + + Inactive HBsAg Carrier State NA NA NA a b + Resolved Successful Vaccination
HBc IgM Ab HBc total Ab HBsAb HBsAg HBV DNA, quantitative HBeAb HBeAg
++ + + + +
+ + + c
+ c
NA, not applicable. a Present for at least 6 months; should be undetectable 1 year after acute infection. b < 105 copies/mL. c Very low levels may be detected with highly sensitive assays. Adapted from references 6, 7, and 9.
9. Lok AS, McMahon BJ; Practice Guidelines Committee, American Association for the Study of Liver Diseases. Chronic hepatitis B. Hepatology. 2001;34:1225-1241. 10. National Guideline for the Management of the Viral Hepatitides A, B, and C. Clinical Effectiveness Group (Association of Genitourinary Medicine and the Medical Society for the Study of Venereal Disease). Sex Transm Inf. 1999;75(Suppl 1):S57-S64. 11. National Institutes of Health Consensus Development Conference Statement: Management of Hepatitis C: 2002. Preliminary Draft Statement, June 12, 2002. Available at http://odp.od.nih.gov/ consensus/cons/116/116cdc_intro.htm. Accessed June 24, 2002. 12. Noskin GA with the AMA Advisory Group on Prevention, Diagnosis, and Management of Viral Hepatitis. Prevention, diagnosis, and management of viral hepatitis. Arch Fam Med. 1995;4:923-934. 13. Ohkubo K, Kato Y, Ichikawa T, et al. Viral load is a significant prognostic factor for hepatitis B virus-associated hepatocellular carcinoma. Cancer. 2002;94:2663-2668. 14. Puchhammer-Stokl E, Mandl C, Kletzmayr J, et al. Monitoring the virus load can predict the emergence of drug-resistant hepatitis B virus strains in renal transplantation patients during lamivudine therapy. J Infect Dis. 2000;181:2063-2066. 15. Recommendations for prevention and control of hepatitis C virus (HCV) infection and HCV-related chronic disease. Centers for Disease Control and Prevention. MMWR. 1998;47(RR-19):1-39. 16. San Francisco and Miami Centers of Excellence in Hepatitis C Research and Education and the Hepatitis C Technical Advisory Group, Department of Veterans Affairs. Treatment recommendations for patients with chronic hepatitis C: 2001 Version 1.0. Available at
272
Gastroenterology Reference Guide
http://www.va.gov/hepatitisc/pved/treatmntgdlnes_00.htm. Accessed December 6, 2001. 17. Sarrazin C, Teuber G, Kokka R, et al. Detection of residual hepatitis C virus RNA by transcription-mediated amplification in patients with complete virologic response according to polymerase chain reactionbased assays. Hepatology. 2000;32:818-823. 18. World Health Organization, Department of Communicable Disease Surveillance and Response. Hepatitis delta [WHO Web site, 2001]. Available at http://www.who.int/csr/disease/hepatitis/HepatitisD_ whocdscsrncs2001_1.pdf. Accessed June 24, 2002. 19. Yang G, Vyas GN. Immunodiagnosis of viral hepatitides A to E and nonA to -E. Clin Diagn Lab Immunol. 1996;3:247-256.
Part 3: Test Application and Interpretation
13.2 Hepatitis B 13.2.1 Hepatitis B Virus Genotype Clinical Use: This test is used to detect hepatitis B virus (HBV) mutations associated with resistance to antiviral agents; predict and monitor response to therapy; identify HBV genotype (AG) for epidemiologic and prognostic purposes; and detect mutations in precore and basal core promoter regions, which may influence immune response and outcome. Clinical Background: The goals of chronic hepatitis B (CHB) treatment are sustained suppression of HBV replication and remission of liver disease, defined as normalized ALT levels, undetectable HBV DNA in a non-amplification assay, loss of HBV e antigen (HBeAg), and improved liver histology.1 Until recently, interferon-alfa and lamivudine have been the only drugs FDA-approved for treatment of CHB, yielding response rates of about 20% to 35% overall and >50% in patients with ALT levels >5 times the upper limit of normal.2,3 Adefovir dipivoxil (ADV)4 and entecavir (ETV)5 are now also approved as treatment options for CHB.
273
Gastroenterology Reference Guide
Lamivudine provides sustained response in patients with loss of HBeAg, but those who do not become HBeAg-negative tend to relapse after therapy is withdrawn. Continued lamivudine treatment in patients without HBeAg loss after 1 year may still yield clinical benefit.1 In some cases, withdrawing lamivudine without initiating another antiviral agent can lead to acute exacerbation or fulminant hepatitis.6 However, long-term lamivudine therapy selects for resistance-associated mutations in the YMDD (tyrosine, methionine, aspartate, aspartate) motif of the HBV DNA polymerase; these mutations arise in about 16% to 32% of patients at 1 year of treatment7 and in about 57% by 3 years.8 ADV has clinical efficacy against lamivudine-resistant and wild-type strains of HBV. Although continued treatment for up to 60 weeks appeared not to select for clinically resistant variants,9 ADV resistance associated with the rtN236T or rtA181V mutations arises in about 2% of patients by year 2 and 3.9% by year 3.10,11 ADV-resistant strains appear to remain susceptible to lamivudine.10 ETV also shows clinical efficacy against lamivudineresistant and wild-type strains of HBV.5 However, reduced ETV susceptibility, associated with development of additional reverse-transcriptase mutations, can occur infrequently after more than 52 weeks of ETV therapy.12 Resistance should be assessed every 3 to 6 months in patients receiving lamivudine.13 Because of adefovirs lower rate of resistance, adefovir-treated patients should be monitored for resistance every 6 months after the first year of therapy. A similar schedule may be appropriate for ETV-treated patients as well. Resistance can be clinically detected by a 1-log10 increase in serum HBV DNA level from the patients
274
Gastroenterology Reference Guide
lowest on-treatment level, occurring on 2 sequential occasions, and can be confirmed by genotyping. In addition to detecting mutations associated with resistance to antiviral drugs (lamivudine, ADV, and famciclovir), this assay also assesses HBV genotype (AG) and mutations in the precore (pre-C) and basal core promoter (BCP) regions. HBV genotypes AG are classified according to sequence variations in the HBV S gene and have distinct geographic distributions. Mutation at nucleotide 1896 of the preC region abolishes production of the HBeAg, while mutations at nucleotide 1762 and 1764 of the BCP region may play a role in HBeAg clearance. The preC and BCP mutations may also influence response to interferon treatment in HBeAg-positive patients.14 Individuals Suitable for Testing include patients receiving lamivudine, ADV, or ETV for treatment of CHB and those being considered for antiviral therapy. Method: This assay uses polymerase chain reaction with HBV-specific primers to amplify relevant portions of the HBV genome. Sequence data are analyzed for mutations at codons rt180, 181, 184, 202, 204, 207, 236, and 250 of the polymerase gene, nucleotide 1896 of the pre-C region, and nucleotides 1762 and 1764 of the BCP region. The HBV genotype is determined by computer-aided alignment and phylogenetic analysis of the amplified portion of the S gene. The analytical sensitivity of this assay is 1,000 HBV copies/mL plasma (500 HBV copies/mL serum).
This test was developed and its performance characteristics determined by Quest Diagnostics Nichols Institute. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that
Part 3: Test Application and Interpretation
275
Gastroenterology Reference Guide
such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test.
Interpretive Information: The rtL180M, rtM204V/I and rtA181T mutations decrease sensitivity to lamivudine, whereas the rt236 and rtA181V mutations reduce sensitivity to ADV. The rtM250V, rtT184G, and rtS202I mutations appear to reduce sensitivity to ETV when combined with lamivudineassociated mutations. The rtL180M and rtV207I mutations appear to decrease sensitivity to famciclovir. The effect of these mutations on the clinical course in patients treated with lamivudine is variable. Some patients develop severe exacerbation of hepatitis or, rarely, decompensated hepatitis, suggesting the need for careful monitoring when these mutations are identified.7 However, many patients with resistant virus experience clinical benefit from continued therapy, including reduced ALT and HBV DNA levels, decreased hepatic damage, and HBeAg seroconversion.6 Individuals with lamivudine-resistant variants appear to respond well to ADV, and patients with an ADV resistanceassociated mutation have responded to lamivudine. The influence of HBV genotype on disease course and treatment response is not fully understood. Genotype C may be associated with more severe liver disease than genotype B,12,13 although contradictory findings have been reported.10 In addition, genotypes A and B may respond better than genotypes C and D to interferon treatment.14 Although their effects are not yet well established, mutations in the BCP and pre-C regions may influence disease course and response to interferon. BCP mutations at nucleotides 1762 and 1764 are associated with low levels of HBeAg and may predict a more favorable response to interferon treatment.
276
Gastroenterology Reference Guide
The G1896A pre-C variant, which abrogates HBeAg formation, has been associated with lower rates of interferon response. Patients with mutations in either region can return to high levels of HBV viremia after loss of HBeAg.10 References
1. Lok AS, McMahon BJ; Practice Guidelines Committee, American Association for the Study of Liver Diseases. Chronic hepatitis B. Hepatology. 2001;34:1225-1241. 2. Lok AS, Heathcote EJ, Hoofnagle JH. Management of hepatitis B: 2000summary of a workshop. Gastroenterology. 2001;120:1828-1853. 3. Malik A, Lee W. Chronic hepatitis B virus infection: treatment strategies for the next millennium. Ann Intern Med. 2000;132:723-731. 4. Lampertico P, Vigano M, Manenti E, et al. Adefovir rapidly suppresses hepatitis B in HBeAg-negative patients developing genotypic resistance to lamivudine. Hepatology. 2005;42:1414-1419. 5. Rivkin A. A review of entecavir in the treatment of chronic hepatitis B infection. Curr Med Res Opin. 2005;21:1845-1856. 6. Honkoop P, de Man RA, Niesters HG, et al. Acute exacerbation of chronic hepatitis B virus infection after withdrawal of lamivudine therapy. Hepatology. 2000;32:635-639. 7. GlaxoSmithKline. Epivir-HBV Product Information. August 2001. Available at http://us.gsk.com/products/assets/us_epivir_hbv.pdf. Accessed May 8, 2002. 8. Leung NW, Lai CL, Chang TT, et al; on behalf of the Asia Hepatitis Lamivudine Study Group. Extended lamivudine treatment in patients with chronic hepatitis B enhances hepatitis B e antigen seroconversion rates: results after 3 years of therapy. Hepatology. 2001;33:1527-1532. 9. Yang H, Westland CE, Delaney WE 4th, et al. Resistance surveillance in chronic hepatitis B patients treated with adefovir dipivoxil for up to 60 weeks. Hepatology. 2002;36:464-473. 10. Angus P, Vaughan R, Xiong S, et al. Resistance to adefovir dipivoxil therapy associated with the selection of a novel mutation in the HBV polymerase. Gastroenterology. 2003;125:292-297. 11. Xiong S, Qi X, Snow A, et al. Long-term incidence of adefovir dipivoxil resistance in chronic hepatitis B patients after 144 weeks of therapy. Abstract 57 (oral). Presented at the 39th Annual Meeting of the European Association for the Study of Liver Disease (EASL). April 1418, 2004. Berlin, Germany. 12. Tenney DJ, Levine SM, Rose RE, et al. Clinical emergence of entecavirresistant hepatitis B virus requires additional substitutions in virus already resistant to lamivudine. Antimicrob Agents Chemother. 2004;48:34983507. 13. Keeffe EB, Dieterich DT, Han SH, et al. A treatment algorithm for the management of chronic hepatitis B virus infection in the United States. Clin Gastroenterol Hepatol. 2004;2:87-106.
Part 3: Test Application and Interpretation
277
Gastroenterology Reference Guide
14. Conjeevaram HS, Lok AS. Management of chronic hepatitis. Br J Hepatol. 2003;38(Suppl):S90-S103. 15. Kao JH, Chen PJ, Lai MY, et al. Genotypes and clinical phenotypes of hepatitis B virus in patients with chronic hepatitis B virus infection. J Clin Microbiol. 2002;40:1207-1209. 16. Lindh M, Hannoun C, Dhillon AP, et al. Core promoter mutations and genotypes in relation to viral replication and liver damage in East Asian hepatitis B virus carriers. J Infect Dis. 1999;179:775-782. 17. Kao JH, Wu NH, Chen PJ, et al. Hepatitis B genotypes and the response to interferon therapy. J Hepatol. 2000;33:998-1002. 18. Stuyver LJ, Locarnini SA, Lok A, et al. Nomenclature for antiviralresistant human hepatitis B virus mutations in the polymerase region. Hepatology. 2001;33:751-757.
13.3 Hepatitis C 13.3.1 Molecular Testing in the Management of Hepatitis C Virus Infection Molecular assays are key components in the management of hepatitis C virus (HCV) infection, from diagnosis to documenting resolved infection. A suggested testing algorithm is provided in Figure 6. Tables 2123 detail quantitative and qualitative tests for HCV RNA and the HCV genotype test offered by Quest Diagnostics. References
1. San Francisco and Miami Centers of Excellence in Hepatitis C Research and Education and the Hepatitis C Technical Advisory Group, Department of Veterans Affairs. Treatment recommendations for patients with chronic hepatitis C: 2001 Version 1.0. Available at http://www.va.gov/hepatitisc/pved/treatmntgdlnes_00.htm. Accessed December 6, 2001. 2. EASL International Consensus Conference on Hepatitis C. Paris, 26-28 February, 1999, Consensus Statement. European Association for the Study of the Liver. J Hepatol. 1999;30:956-961. 3. Hepatitis Resource Network. Hepatitis C treatment algorithm. Available at http://www.h-r-n.org. Accessed January 9, 2002. 4. Sarrazin C, Teuber G, Kokka R, et al. Detection of residual hepatitis C virus RNA by transcription-mediated amplification in patients with complete virologic response according to polymerase chain reactionbased assays. Hepatology. 2000;32:818-823. 5. Fried MW, Shiffman ML, Reddy RK, et al. Pegylated (40 kDa) interferon alpha-2a (PEGASYS) in combination with ribavirin: efficacy and safety
278
Gastroenterology Reference Guide
Positive HCV Antibody (EIA)
Part 3: Test Application and Interpretation
HEPTIMAX to confirm diagnosis* and establish baseline viral load
HCV RNA <5 IU/mL Confirm with RIBA
HCV RNA
5 IU/mL and high ALT
HCV RNA
5 IU/mL and normal ALT
Repeat assays in 4-6 months
Consider liver biopsy to assess fibrosis stage
Decision to treat
HCV genotyping to guide duration of treatment
Begin combination therapy
HEPTIMAX at week 12 to assess treatment response
Genotype 1 <2 log decrease in HCV RNA Sustained virologic response not likely
Genotype 1 2 log decrease in HCV RNA
Genotype non-1
HEPTIMAX at week 24 to assess treatment response
HCV RNA
5 IU/mL
Genotype 1 HCV RNA <5 IU/mL Sustained virologic response likely with additional 24 weeks of treatment
Genotype non-1 HCV RNA <5 IU/mL Sustained virologic response likely without further treatment
Sustained virologic response not likely
HEPTIMAX at end of treatment and 24 weeks later to document sustained virologic response
*Other nucleic acid tests (NATs) may be substituted to confirm diagnosis. Recombinant immunoblot assay (RIBA) may also be used. A positive EIA result with a signal to cutoff ratio of 8.0 does not require confirmation, but baseline viral load should be established with a quantitative HCV RNA assay. Other nucleic acid tests (NATs) may be substituted to assess viral load. 5 IU/mL is the limit of quantitation for the HEPTIMAX assay.
Figure 6. HCV molecular testing algorithm. This algorithm is intended to assist in test selection and management of individuals infected with hepatitis C virus and is based in part on previous recommendations.1-7
Gastroenterology Reference Guide
Table 21. Quantitative HCV RNA Assays
Test Code Test Name (CPT Code*) 10565 (87522) HEPTIMAX Reportable Specimen Range, IU/mL Requirements 550,000,000 3 mL (min. 1.0 mL) plasma in PPTpotassium EDTA (white-top tube). Ship frozen. Clinical Applications
35645 (87522)
Hepatitis C Viral RNA, 50-50,000,000 Quantitative Real-Time PCR
10073 (87522)
Hepatitis C Viral RNA, Quantitative TMA
57,500
29271 (87522)
Hepatitis C Viral RNA, Quantitative bDNA
6157,700,000
11348 (87522)
Hepatitis C Viral RNA, Quantitative PCR with Reflex to Genotype, LiPA
50-50,000,000 (Reflex to genotype if >300 IU/mL)
Confirm infection; establish viral load at baseline; monitor viral load during therapy; determine duration of treatment; assess likelihood of non-response during treatment; assess likelihood of nonsustained response at end of treatment. 2 mL (min. 0.5 mL) Establish viral load at baseline; plasma in PPTmonitor viral load during potassium EDTA therapy; determine duration of (white-top tube). treatment; assess likelihood of Ship frozen. non-response during treatment. 2 mL (min. 0.6 mL) Confirm infection; assess plasma in PPTlikelihood of non-sustained potassium EDTA response at end of treatment. (white-top tube). Ship frozen. 1 mL (min. 0.2 mL) Establish viral load at baseline; plasma in potassium monitor viral load during EDTA (white-top therapy; determine duration of tube) or no-additive treatment; assess likelihood of serum-separator non-response during treatment. tube. Ship frozen. 3 mL (min. 1.1 mL) Establish viral load at baseline; plasma in PPTdetermine duration of potassium EDTA treatment and likelihood of (white-top tube). response. Ship frozen.
*The CPT codes provided are based on AMA guidelines and are for informational purposes only. CPT coding is the sole responsibility of the billing party. Please direct any questions regarding coding to the payor being billed. This test was developed and its performance characteristics determined by Quest Diagnostics Nichols Institute. It has not been cleared or approved by the US Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Reflex performed at additional charge. Polymerase chain reaction (PCR) is performed pursuant to a license agreement with Roche Molecular Systems, Inc.
results from a phase III randomized, controlled, actively controlled, multicenter study. Gastroenterology. 2001;120 (Suppl 1):A-55. Abstract 289. 6. National Institutes of Health. Consensus Development Conference Statement. Management of Hepatitis C: 2002. Available at http://
280
Gastroenterology Reference Guide
Table 22. Qualitative HCV RNA Assays
Part 3: Test Application and Interpretation
Test Code Test Name (CPT Code*) 37273 (87521) Hepatitis C Viral RNA, Qualitative TMA Limit of Detection, Specimen (LOD), IU/mL Requirements 10 2 mL (min. 0.6 mL) plasma in PPTpotassium EDTA (white-top tube). Ship frozen. 2 mL (min. 0.6 mL) plasma in PPTpotassium EDTA (white-top tube). Ship frozen. Clinical Applications Confirm presence of chronic HCV infection; differentiate between resolved and active infection. Confirm presence of chronic HCV infection; differentiate between resolved and active infection.
34024 (87521)
Hepatitis C Viral RNA, Qualitative PCR
50
*The CPT codes provided are based on AMA guidelines and are for informational purposes only. CPT coding is the sole responsibility of the billing party. Please direct any questions regarding coding to the payor being billed.
consensus.nih.gov/cons/116/116cdc_intro.htm. Accessed January 8, 2003. 7. Alter MJ, Kuhnert WL, Finelli L; Centers for Disease Control and Prevention. Guidelines for laboratory testing and result reporting of antibody to hepatitis C virus. Centers for Disease Control and Prevention. MMWR Recomm Rep. 2003;52(RR-3):1-16.
Table 23. HCV Genotype Assay
Test Code Test Name Limit of Detection (CPT Code*) 37811 Hepatitis C Viral RNA Minimum viral load: 300 IU/mL (87902) Genotype, LiPA Specimen Requirements 2 mL (min. 0.6 mL) plasma in PPT potassium EDTA (white -top tube). Ship frozen. Clinical Applications Assess length of treatment required and likelihood of response (used at baseline).
*The CPT codes provided are based on AMA guidelines and are for informational purposes only. CPT coding is the sole responsibility of the billing party. Please direct any questions regarding coding to the payor being billed. This test was developed and its performance characteristics determined by Quest Diagnostics Nichols Institute. It has not been cleared or approved by the US Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test.
281
Gastroenterology Reference Guide
13.3.2 Hepatitis C Viral RNA Genotype, LiPA' Clinical Use: This test is used to predict the likelihood of therapeutic response and to determine the duration of treatment. Clinical Background: Hepatitis C virus (HCV), one of 6 hepatitis viruses (AE and G), is a major cause of liver disease and the leading reason for liver transplantation in the United States. Although acute infection is usually asymptomatic, most patients (75%85%) develop chronic infection; about 60% to 70% of chronically infected individuals develop active liver disease, which can progress to cirrhosis or hepatocellular cancer. Current treatment recommendations for chronic HCV infection are either a 24- or 48-week course of interferon, which is used alone or in combination with ribavirin. Pegylated interferon alfa-2b is also approved for use with or without ribavirin. The combination therapies yield higher response rates, but are associated with more adverse effects. There are at least 6 major types and more than 50 subtypes of HCV (eg, 1a).1,2 Type 1, which accounts for about 70% of chronic HCV infections in the United States, is less responsive to current therapy than other genotypes.2-10 For example, patients with type 2 or 3 infection who are given combination therapy have cure rates about twice those of patients with type 1 infection (eg, 73% vs 30%5 and 69% vs 28%9). Moreover, individuals with type 2 or 3 infection are often cured after 24 weeks of combination therapy, whereas those with genotype 1 infection may benefit by extending therapy to 48 weeks.9 Thus, genotyping helps predict the likelihood of therapeutic response and helps determine optimal treatment duration.
282
Gastroenterology Reference Guide
Individuals Suitable for Testing include patients with detectable hepatitis C viral RNA (>1,000 copies/mL or >300 IU/mL) who are being evaluated for treatment. Method: This line probe assay (LiPA) is based on variations in the 5' untranslated region (UTR) of the HCV genome. Since it is quick and reproducible and correlates well with other methods,13 it is useful for predicting the likelihood of therapeutic response and determining optimal treatment duration. Unlike sequencing-based assays, LiPA does not detect novel sequence variations or provide sequence information from the coding region. However, it can provide a reportable genotype in samples with viral loads as low as 1,000 HCV RNA copies/mL. LiPA utilizes reverse transcription and polymerase chain reaction (RT-PCR) with genotype-specific probes from 7 regions of the HCV 5' UTR. It distinguishes among major types and most common subtypes of HCV: 1a, 1b, 1a/b; 1; 2a/c, 2b, 2; 3a, 3b, 3c, 3; 4a, 4b, 4c/d, 4e, 4f, 4h; 5a; 6a; and 10a (provisional classification). It does not distinguish between subtypes that have identical sequences in the 5' UTR (eg, subtype 2a cannot be distinguished from 2c and subtype 4c cannot be distinguished from 4d).
This test was developed and its performance characteristics determined by Quest Diagnostics Nichols Institute. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the tests.
Part 3: Test Application and Interpretation
Interpretive Information: Patients infected with HCV types other than 2 or 3 have a poor potential for response to treatment and require 48 weeks of therapy, even if the virus is undetectable at 24 weeks.11,13 Conversely, in patients with type 2 or 3
283
Gastroenterology Reference Guide
infection, treatment may be stopped at 24 weeks. Treatment decisions should also take into account other factors that may influence therapeutic response, such as pretreatment HCV viral load and cirrhosis status, sex and age of the patient, and other clinical and laboratory findings.13 Patients may be infected with multiple HCV subtypes. The frequency and geographic distribution of HCV types are listed in Tables 24 and 25. References
1. Simmonds P, Holmes EC, Cha T-A, et al. Classification of hepatitis C virus into six major genotypes and a series of subtypes by phylogenetic analysis of the NS-5 region. J Gen Virol. 1993;74:2391-2399. 2. Zein NN. Clinical significance of hepatitis C virus genotypes. Clin Microbiol Rev. 2000;13:223-235. 3. Amoroso P, Rapicetta M, Tosti ME, et al. Correlation between virus genotype and chronicity rate in acute hepatitis C. J Hepatol. 1998;28:939944. 4. Bellobuono A, Mondazzi L, Tempini S, et al. Prospective comparison of four lymphoblastoid interferon alpha schedules for chronic hepatitis C. A multivariate analysis of factors predictive of sustained response to treatment. Eur J Gastroenterol Hepatol. 1997;9:1169-1177. 5. Davis GL, Esteban-Mur R, Rustgi V, et al. Interferon alfa-2b alone or in combination with ribavirin for the treatment of relapse of chronic hepatitis C. N Engl J Med. 1998;339:1493-1499. 6. Gerken G, Knolle P, Jakobs S, Meyer zum Buschenfelde KH. Quantification and genotyping of serum HCV-RNA in patients with chronic hepatitis C undergoing interferon treatment. Arch Virol. 1997;142:459-464. 7. Management of hepatitis C. NIH Consensus Statement Online. 1997 Mar 24-26 [cited September 14, 2001];15(3):1-41. Available at http://odp.od.nih.gov/consensus/cons/105/105_statement.htm. 8. Martinot-Peignoux M, Boyer N, Pouteau M, et al. Predictors of sustained
Table 24. HCV Subtypes in the United States14
HCV Subtype 1a 1b 2b 3a Other Frequency (%) 58 21 13 5 3
284
Gastroenterology Reference Guide
Table 25. Worldwide HCV Genotype Distribution2
HCV Genotype 1 2 3 4 5 6 Predominant Geographic Location N America, Europe, East Asia N America, Europe, East Asia N America, Europe, East Asia Middle East, Central Africa South Africa, Southeast Asia South Africa, Southeast Asia
Part 3: Test Application and Interpretation
9.
10.
11. 12.
13.
14.
response to alpha interferon therapy in chronic hepatitis C. J Hepatol. 1998;29:214-223. McHutchison JG, Gordon SC, Schiff ER, et al. Interferon alfa-2b alone or in combination with ribavirin as initial treatment for chronic hepatitis C. Hepatitis Interventional Therapy Group. N Engl J Med. 1998;339:14851492. Poynard T, Marcellin P, Lee SS, et al. Randomized trial of interferon alpha2b plus ribavirin for 48 weeks or for 24 weeks versus interferon alpha2b plus placebo for 48 weeks for treatment of chronic infection with hepatitis C virus. International Hepatitis Interventional Therapy Group (IHIT). Lancet. 1998;352:1426-1432. Lauer GM, Walker BD. Hepatitis C virus infection. N Engl J Med. 2001;345:41-52. Lau JYN, Davis GL, Prescott LE, et al. Distribution of hepatitis C virus genotypes determined by line probe assay in patients with chronic hepatitis C seen at tertiary referral centers in the United States. Ann Intern Med. 1996;124:868-876. EASL International Consensus Conference on Hepatitis C. Paris, 26-28 February, 1999, Consensus Statement. European Association for the Study of the Liver. J Hepatol. 1999;30:956-961. Zein NN, Rakela J, Krawitt EL, et al. Hepatitis C virus genotypes in the United States: epidemiology, pathogenicity, and response to interferon therapy. Collaborative Study Group. Ann Intern Med. 1996;125:634-639.
13.3.3 Hepatitis C Viral RNA, Qualitative Clinical Use: These tests are used to confirm hepatitis C virus (HCV) infection and demonstrate resolution of infection. Clinical Background: These qualitative HCV RNA tests detect the presence of HCV circulating in the blood. They are used to confirm HCV diagnosis following a positive or indeterminate antibody test
285
Gastroenterology Reference Guide
result. These tests differentiate between resolved and active infection and may be useful for detecting acute infection prior to seroconversion. They are especially useful for confirming diagnosis in people with indeterminate HCV immunoblot (RIBA) results, as well as in immunosuppressed or immunoincompetent individuals. Methods PCR: In this polymerase chain reaction (PCR) method, viral RNA is reverse-transcribed to cDNA and amplified with biotin-labeled HCV-specific primers. Amplification products are then hybridized to HCV-specific capture probes and detected with an avidin-HRP conjugate in a colorimetric assay. This test detects HCV genotypes 1a and 1b; the ability to detect other genotypes is currently unknown. Analytical sensitivity is 50 IU/mL. TMA: In this transcription-mediated amplification (TMA) method, RNA is extracted from the patient sample and amplified by utilizing 2 enzymes (reverse transcriptase and T7 RNA polymerase) to cycle between RNA and DNA intermediates, resulting in several billion RNA amplicons. These amplicons are detected via hybridization protection assay (HPA) in which only hybridized probes remain chemiluminescent and are detected in a luminometer. Analytical sensitivity is 10 IU/mL. Interpretive Information: A detected result with either method indicates the presence of HCV RNA and is consistent with active infection (acute or chronic). A not detected result, on the other hand, is suggestive of the absence of detectable HCV RNA. False-negative results might occur due to heparin therapy or HCV RNA levels below the detectable limit of the assay. Because of the sensitivity of the
286
Gastroenterology Reference Guide
TMA method, some false-positive results may occur, particularly in specimens that have been contaminated through aliquotting or some other procedure. Six months following cessation of antiviral therapy, a repeatedly negative test suggests clearance of the virus and recovery from the infection. HCV RNA tests sensitive to 10 IU/mL or less are better indicators of resolved infection than are tests with lesser sensitivity. 13.3.4 Hepatitis C Viral RNA, Quantitative Clinical Use: These tests are used to predict response to antiviral therapy and to differentiate lack of therapeutic response from partial therapeutic response. Clinical Background: Quantitative HCV RNA tests measure the level of hepatitis C virus (HCV) circulating in blood. Although this level does not correlate with severity of disease, it does correlate with the likelihood of response to antiviral therapy. Patients with a low baseline HCV RNA level (<2 million copies/mL) are more likely to achieve eradication of the virus with treatment. During or after therapy, rising or sustained HCV RNA levels indicate a lack of therapeutic response. A partial response is indicated by a drop in viral level at least one-third of a log. In HCV type 1 infections, lack of a 2-log decrease after 12 weeks of treatment may predict treatment failure. At the end of treatment and afterward, an undetectable level suggests a favorable therapeutic response; however, an HCV RNA test that is sensitive to 10 IU/mL or less should be used before discontinuing therapy or concluding that the infection is resolved. Methods: Quest Diagnostics offers 3 technologies for
287
Part 3: Test Application and Interpretation
Gastroenterology Reference Guide
quantitative HCV RNA testing: real-time polymerase chain reaction (PCR), branched DNA (bDNA) signal amplification, and transcription-mediated amplification (TMA). Several combinations of these platforms are available, each with different sensitivities and linear ranges. HEPTIMAX offers the greatest sensitivity and broadest linear range of the available options (See Molecular Testing in the Management of Hepatitis C Virus Infection, section 13.3.1, for more information). bDNA: In this branched DNA (bDNA) signal amplification method, viral RNA is captured on the surface of a microtiter well by synthetic oligonucleotides coating the well. The solid phase bound viral RNA is hybridized to multiple branched DNA molecules. Alkaline phosphatase labeled probes are in turn hybridized to the branched DNA and reacted with a chemiluminescent substrate to produce a greatly amplified light signal. The amount of light emitted is directly proportional to the quantity of HCV RNA. This method demonstrates equal quantification of HCV genotypes 1-6. The linear range is 615 to 7,700,000 IU/mL (3,200 to 40,000,000 copies/mL). Real-time PCR: Viral RNA is reverse-transcribed to cDNA and amplified with HCV-specific primers and a fluorescent dye-labeled probe. Amplification products are detected by measuring fluorescent signals generated during the PCR. Viral copy numbers are quantified by comparing fluorescent signals generated in the specimen to those produced by calibration standards. The linear range of this assay is 50 to 50,000,000 IU/mL.
This test was developed and its performance characteristics determined by Quest Diagnostics Nichols Institute. It has not been cleared or approved by
288
Gastroenterology Reference Guide
the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Polymerase chain reaction (PCR) is performed pursuant to a license agreement with Roche Molecular Systems, Inc.
Part 3: Test Application and Interpretation
TMA: Viral RNA is extracted from the patient sample and amplified by utilizing 2 enzymes (reverse transcriptase and T7 RNA polymerase) to cycle between RNA and DNA intermediates, resulting in several billion RNA amplicons. These amplicons are detected via hybridization protection assay (HPA) in which only hybridized probes remain chemiluminescent and are detected in a luminometer. The linear range is 5 to 7500 IU/mL.
This test was developed and its performance characteristics determined by Quest Diagnostics Nichols Institute. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test.
HEPTIMAX: The HEPTIMAX test begins with the HCV RNA real-time polymerase chain reaction (PCR) method. If the HCV RNA level is below 50 IU/mL, then the sample is assayed again using the TMA method. The reportable range is 5 to 50,000,000 IU/mL.
This test was developed and its performance characteristics determined by Quest Diagnostics Nichols Institute. It has not been cleared or approved by the U.S. Food and Drug Administration. The FDA has determined that such clearance or approval is not necessary. Performance characteristics refer to the analytical performance of the test. Polymerase chain reaction (PCR) is performed pursuant to a license agreement with Roche Molecular Systems, Inc.
The following conversion factors are used when converting from copies/mL to IU/mL:
289
Gastroenterology Reference Guide
PCR: Copies/mL = IU/mL x 2.7 TMA: Copies/mL = IU/mL x 5.2 bDNA: Copies/mL = IU/mL x 5.2 Interpretive Information: The presence of detectable levels of RNA suggests continuing active HCV infection and may indicate insufficient therapeutic response. A rise in HCV RNA equal to or greater than 3 times the first result is significant for these assays and usually clinically significant. Decreasing levels are suggestive of therapeutic response when levels decrease by one-third of the first result or more. For more information, read Clinical Background, above. 13.4 Hepatitis E 13.4.1 Hepatitis E Antibody (IgG) Clinical Use: This assay is used in the diagnosis of acute hepatitis E virus (HEV) infection and in the differential diagnosis of enteric hepatitis. Clinical Background: Hepatitis E virus (HEV) is the major etiologic agent of enterically transmitted nonA, non-B hepatitis in developing countries. In the United States, it is usually diagnosed in recent travelers to endemic areas (India, Asia, Africa, and Central America). Like hepatitis A, HEV occurs in both sporadic and epidemic forms and causes an acute, moderately severe but not chronic hepatitis that is frequently cholestatic. Unlike hepatitis A virus, HEV progresses to fatal fulminant hepatitis in at least 15% to 30% of pregnant patients, especially in the third trimester. The infection may also manifest without jaundice or be present subclinically. Hepatitis E IgG antibodies have been detected in up to 93% of patients during the acute phase. In most
290
Gastroenterology Reference Guide
patients, IgG antibodies are short lived, often being undetectable 6 to 12 months after onset; however, duration up to 4.5 years has been observed. Method: In this enzyme immunoassay (EIA), antiHEV antibodies in patient serum bind to 2 recombinant HEV antigens coating the polystyrene well. Following a wash to remove unbound material, HRP-conjugated goat anti-human IgG is added to bind to the antigen-antibody complexes. After a second wash, o-phenylenediamine (OPD) substrate is added, producing a yellow-orange color. The amount of color produced is directly proportional to the amount of antibody present in the patient specimen. Results are reported as non-reactive or repeatedly reactive. Aliases include anti-HEV and HEV antibody.
This test is performed using a kit that has not been approved or cleared by the FDA. The analytical performance characteristics of this test have been determined by Quest Diagnostics Nichols Institute. This test should not be used for diagnosis without confirmation by other medically established means.
Part 3: Test Application and Interpretation
Interpretive Information: A reactive result is associated with HEV infection. Non-reactive results are associated with absence of HEV infection, early HEV infection (prior to seroconversion), and past, resolved HEV infection. References
1. Anonymous. Hepatitis E among US travelers, 1989-1992. Morbid Mortal Weekly Rep. 1992;42:1-4. 2. Bradley DW. Enterically-transmitted non-A, non-B hepatitis. Br Med Bull. 1990;46:442-461. 3. Choo QL, Kuo G, Weiner AJ, et al. Isolation of a cDNA clone derived from a blood-borne non-A, non-B hepatitis genome. Science. 1990;244:359-361. 4. Dawson G, Gutierrez PR, Pilot-Matias T, et al. Recombinant antigens and synthetic peptides for serodiagnosis of hepatitis E infection. In: Nishioka K, Suzuki H, Mishiro S, et al, eds. Viral Hepatitis and Liver Disease. Tokyo: Springer-Verlag; 1994:371-374.
291
Gastroenterology Reference Guide
5. Fields HA, Favorov MO, Margolis HS. The hepatitis E virus: a review. Journal of Clinical Immunoassays. 1993;16:215-222. 6. Purdy MA, Krawczynski K. Hepatitis E. Gastroenterol Clin North Am. 1994;23:537-546. 7. Reyes GR, Purdy MA, Kim JP, et al. Isolation of a cDNA from the virus responsible for enterically-transmitted non-A, non-B hepatitis. Science. 1990; 247:1335-1339. 8. Ticehurst J. Hepatits E virus. In: PR Murray, ed. Manual of Clinical Microbiology. 6th ed. Washington, DC: ASM Press;1995:1056-1067. 9. Yang G, Vyas GN. Immunodiagnosis of viral hepatitides A to E and nonA to -E. Clin Diagn Lab Immunol. 1996;3:247-256. 10. Yarbough PO, Tam AW, Fry KE, et al. Hepatitis E virus: identification of type-common epitopes. J Virol. 1991;65:5790.
14. IGA, SERUM Clinical Use: This test is used to diagnose IgA deficiencies and to determine the etiology of recurrent infections. Clinical Background: IgA is the first line of defense for the majority of infections at mucosal surfaces and consists of 2 subclasses. IgA1 is the dominant subclass, accounting for 80% to 90% of total serum IgA and greater than half of the IgA in secretions such as milk, saliva, and tears. IgA2, on the other hand, is more concentrated in secretions than in blood. IgA2 is more resistant to proteolytic cleavage and may be more functionally active than IgA1. IgA deficiency is the most prevalent isotype deficiency, occurring in 1/400 to 1/700 individuals. Many patients with IgA deficiency are asymptomatic, while others may develop allergic disease, repeated sinopulmonary or gastroenterologic infections, and/or autoimmune disease. Individuals with complete absence of IgA (<5 mg/dL) may develop autoantibodies to IgA after blood or intravenous immunoglobulin infusions and may experience anaphylaxis on repeat exposure. Method: In this nephelometry method, human anti-
292
Gastroenterology Reference Guide
IgA binds to IgA in the patient sample, forming an insoluble complex. The amount of light scattered by this insoluble complex is proportional to the concentration of IgA present in the sample. Interpretive Information: Age-related IgA reference ranges are listed in Table 26. 15. INFLAMMATORY BOWEL DISEASE (IBD) DIFFERENTIATION PANEL Clinical Use: This test is used to differentiate Crohns disease from ulcerative colitis, to stratify Crohns disease subtypes,1 and to assess need for further invasive testing in children with IBD symptoms.2 Clinical Background: Crohns disease (CD) and ulcerative colitis (UC) are the most common forms of IBD. Although UC and CD are typically differentiated on the basis of clinical, radiographic, and endoscopic findings, distinguishing between these conditions can be difficult in about 10% to 15% of patients, especially when disease is confined Table 26. IgA Reference Ranges in Children and Adults
Age, yr 611 months 1 2 3 47 811 1217 18 Reference Range, mg/dL 3101 6112 11134 16155 31214 43268 65356 81463
Part 3: Test Application and Interpretation
Pediatric ranges are from Schauer U, Stemberg F, Rieger CH, et al. Establishment of age-dependent reference values for IgA subclasses. Clin Chim Acta. 2003;328:129-133. Adult ranges is from Quest Diagnostics Nichols Institute Clinical Correlations Department.
293
Gastroenterology Reference Guide
to the colon. Because the treatment and prognosis of UC and CD differ, accurate diagnosis is critical for management. Numerous studies have investigated the utility of 2 serologic markers, perinuclear anti-neutrophil cytoplasmic antibody (pANCA) and anti-Saccharomyces cerevisiae antibody (ASCA), in differentiating between UC and CD. The pANCA associated with IBD differs from that found in the vasculitides, having an atypical perinuclear staining pattern that can be identified by differential staining patterns with ethanolformalin fixation. This atypical pANCA is found in about 50% to 80% of UC patients but only 10% to 30% of those with CD. ASCA, on the other hand, is more common in CD (46% to 70%) than in UC (6%-12%).3,4 The combination of these markers has high specificity for UC (94%-97%; pANCA+/ ASCA-) and CD (81%-98%; ASCA+/pANCA-).5 Serologic results can also assist in stratification of CD: pANCA-positive CD is associated with a clinical phenotype similar to that of UC (UC-like CD),4 while positivity for ASCA IgG and IgA is associated with non-UC-like disease.6 Several reports have noted the potential utility of serologic testing, combined with other clinical and laboratory information, to identify children with suspected IBD who may not require invasive testing.2,7 Method: This panel includes a pANCA screen, with reflex to titer at an additional charge, and an ASCA IgG and IgA test. References
1. Klebl FH, Bataille F, Bertea CR, et al. Association of perinuclear antineutrophil cytoplasmic antibodies and anti-Saccharomyces cerevisiae antibodies with Vienna classification subtypes of Crohns disease. Inflamm Bowel Dis. 2003;9:302-307. 2. Dubinsky MC, Ofman JJ, Urman M, et al. Clinical utility of
294
Gastroenterology Reference Guide
3.
4. 5.
6.
7.
serodiagnostic testing in suspected pediatric inflammatory bowel disease. Am J Gastroenterol. 2001;96:758-765. Savige J, Dimech W, Fritzler M, et al. Addendum to the International Consensus Statement on testing and reporting of antineutrophil cytoplasmic antibodies. Quality control guidelines, comments, and recommendations for testing in other autoimmune diseases. Am J Clin Pathol. 2003;120:312-318. Abreu MT, Vasiliauskas EA, Kam LY, et al. Use of serologic tests in Crohns disease. Clinical Perspectives in Gastroenterology. 2001;4:155-164. Reumaux D, Sendid B, Poulain D, et al. Serological markers in inflammatory bowel diseases. Best Pract Res Clin Gastroenterol. 2003;17:1935. Walker LJ, Aldhous MC, Drummond HE, et al. Anti-Saccharomyces cerevisiae antibodies (ASCA) in Crohns disease are associated with disease severity but not NOD2/CARD15 mutations. Clin Exp Immunol. 2004;135:490-496. .Bartunkova Kolarova I, Sediva A, et al. Antineutrophil cytoplasmic antibodies, anti-Saccharomyces cerevisiae antibodies, and specific IgE to food allergens in children with inflammatory bowel diseases. Clin Immunol. 2002;102:162-168.
Part 3: Test Application and Interpretation
16. LACTOFERRIN Clinical Use: This test is used to rule out irritable bowel syndrome (IBS) in patients presenting with IBD symptoms. Clinical Background: An estimated 30 million Americans suffer from irritable bowel syndrome (IBS), a disorder characterized by crampy abdominal pain, bloating, constipation, and/or diarrhea. The same clinical picture may be seen in individuals with ulcerative colitis (UC) and Crohns disease (CD). Collectively known as inflammatory bowel disease (IBD), UC and CD affect more than 1 million Americans. Although individuals with IBS may experience severe discomfort and require symptomatic treatment, patients with IBD may develop rectal bleeding and permanent intestinal damage. Furthermore, patients with IBD frequently require long-term steroid therapy and immunosuppressive agents. Consequently,
295
Gastroenterology Reference Guide
distinguishing IBS from IBD is critical for patient management. In patients with active IBD, lactoferrin, a proven marker of inflammation, is released from leukocytes infiltrating the intestinal mucosa. Whereas fecal lactoferrin tends to be elevated in patients with active IBD, it is minimally present in patients with IBS. In the stool of patients presenting with symptoms of IBD, lactoferrin is 86% sensitive and 100% specific in distinguishing IBD from IBS, thus making fecal lactoferrin an important diagnostic tool (Am J Gastroenterol. 2003;98:1309-1314). The evaluation of fecal lactoferrin offers a safe, noninvasive, accurate method to quickly differentiate IBD from IBS once infectious causes of intestinal inflammation and colorectal cancer are ruled out. A positive fecal lactoferrin result can be complemented by the Quest Diagnostics Inflammatory Bowel Disease Differentiation Panel (separate order code) to assist in distinguishing UC from CD.
296
S-ar putea să vă placă și
- Fit FormulaDocument264 paginiFit FormulaRyanÎncă nu există evaluări
- Ventriloquism For DummiesDocument4 paginiVentriloquism For DummiesAri Syuhada PutraÎncă nu există evaluări
- TomatoDocument40 paginiTomatosourie_66Încă nu există evaluări
- Eating Fruit On Empty StomachDocument5 paginiEating Fruit On Empty StomachCandice Dela Sierra GermataÎncă nu există evaluări
- A Simple Guide to Celiac Disease and Malabsorption DiseasesDe la EverandA Simple Guide to Celiac Disease and Malabsorption DiseasesÎncă nu există evaluări
- Partha Nandi 77 Snacks and Smoothies Cookbook LO RES PDFDocument76 paginiPartha Nandi 77 Snacks and Smoothies Cookbook LO RES PDFgoldieÎncă nu există evaluări
- Parvo Treatment 101 PET Version v3.0Document110 paginiParvo Treatment 101 PET Version v3.0Paito Moro MoroÎncă nu există evaluări
- Celiac DiseaseDocument37 paginiCeliac DiseaseTaj lamajed100% (1)
- Celiac Disease (Updated 4th Edition): A Hidden EpidemicDe la EverandCeliac Disease (Updated 4th Edition): A Hidden EpidemicÎncă nu există evaluări
- Celiac DiseaseDocument12 paginiCeliac DiseaseDasagrandhi Chakradhar100% (1)
- Chevron Safety Bulletin 2008Document12 paginiChevron Safety Bulletin 2008somayajÎncă nu există evaluări
- Nutritional Requirements of Asian SeabassDocument6 paginiNutritional Requirements of Asian SeabassGiuseppe AV0% (1)
- Celiac DiseaseDocument25 paginiCeliac DiseaseMateen ShukriÎncă nu există evaluări
- knh411 Celiac DiseaseDocument11 paginiknh411 Celiac Diseaseapi-301897220100% (1)
- Celiac DiseaseDocument42 paginiCeliac DiseaseTri P BukerÎncă nu există evaluări
- Enteral and Parenteral Nutrition SeminarDocument20 paginiEnteral and Parenteral Nutrition SeminarAmin AksherÎncă nu există evaluări
- Involuntary Weight Loss (GSH)Document30 paginiInvoluntary Weight Loss (GSH)Febriliana Mao-maoÎncă nu există evaluări
- 10 Wood For The TreesDocument129 pagini10 Wood For The Treessweeching_limÎncă nu există evaluări
- Celiac Desease: By: Leila Floresca Esteban BSNIII-BDocument38 paginiCeliac Desease: By: Leila Floresca Esteban BSNIII-BScarletÎncă nu există evaluări
- Celiac DiseaseDocument14 paginiCeliac Diseaseraed faisalÎncă nu există evaluări
- Celiac Disease: DR Ajeet Kumar Lohana Senior Registrar Gastroenterology AtmcDocument59 paginiCeliac Disease: DR Ajeet Kumar Lohana Senior Registrar Gastroenterology AtmcAjeet LohanaÎncă nu există evaluări
- Neonatal CholestasisDocument13 paginiNeonatal Cholestasisgts999Încă nu există evaluări
- Gastroenterolgy Reference Guide PDFDocument0 paginiGastroenterolgy Reference Guide PDFbibicul1958Încă nu există evaluări
- Celiac Disease: Mobin Ur RehmanDocument46 paginiCeliac Disease: Mobin Ur RehmanMobin Ur Rehman KhanÎncă nu există evaluări
- Celiac DiseaseDocument20 paginiCeliac DiseasezaydeeeeÎncă nu există evaluări
- Celiac Disease FinalDocument7 paginiCeliac Disease FinalacholineÎncă nu există evaluări
- Orphanet Journal of Rare Diseases: Celiac DiseaseDocument8 paginiOrphanet Journal of Rare Diseases: Celiac DiseaseFauzi NoviaÎncă nu există evaluări
- Celiac Disease in Women: Mohamed Kandeel, M.D. Professor of Obstetrics and Gynecology Menofyia University EgyptDocument19 paginiCeliac Disease in Women: Mohamed Kandeel, M.D. Professor of Obstetrics and Gynecology Menofyia University EgyptMohammad EklakhÎncă nu există evaluări
- Celiac Disease - 2024Document9 paginiCeliac Disease - 2024khaleelÎncă nu există evaluări
- Coeliac Disease: John S. Leeds, Andrew D. Hopper, and David S. SandersDocument14 paginiCoeliac Disease: John S. Leeds, Andrew D. Hopper, and David S. Sandersbdalcin5512Încă nu există evaluări
- Gluten-Free Diet in Celiac Disease-ForeverDocument14 paginiGluten-Free Diet in Celiac Disease-ForeverRadwan AjoÎncă nu există evaluări
- Non Celiac Enteropathy Level 2 - July 2016Document7 paginiNon Celiac Enteropathy Level 2 - July 2016احمد ليمونهÎncă nu există evaluări
- Celiac Disease (Gluten-Sensitive Enteropathy)Document6 paginiCeliac Disease (Gluten-Sensitive Enteropathy)Cricket Trick & FitnessÎncă nu există evaluări
- Diseases of The Gastrointestinal Tract: Dr. Gábor KökényDocument52 paginiDiseases of The Gastrointestinal Tract: Dr. Gábor Kökényאיתי עוזרÎncă nu există evaluări
- Celiac Disease: Clinical PracticeDocument8 paginiCeliac Disease: Clinical PracticeRo RojasÎncă nu există evaluări
- AJGP 2018 0102 Clinical CoeliacDocument6 paginiAJGP 2018 0102 Clinical CoeliacAngie Viquez BeitaÎncă nu există evaluări
- DC Mais Comum Do Que Se PensaDocument8 paginiDC Mais Comum Do Que Se PensaMary Jane NascimentoÎncă nu există evaluări
- Celiac Disease Celiac Sprue Gluten SensiDocument2 paginiCeliac Disease Celiac Sprue Gluten SensiNərmin ŞahverdiyevaÎncă nu există evaluări
- Chronic Diarrhea EvaluationDocument34 paginiChronic Diarrhea EvaluationarthoclaseÎncă nu există evaluări
- Group 2 Presentation DieteticsDocument30 paginiGroup 2 Presentation DieteticsEman ZahraÎncă nu există evaluări
- Involuntary Weight Loss (GSH)Document39 paginiInvoluntary Weight Loss (GSH)AchmadRizaÎncă nu există evaluări
- Celiac Disease - Case StudyDocument29 paginiCeliac Disease - Case StudyRye HanaÎncă nu există evaluări
- Immunology of Type 1 DiabetesDocument14 paginiImmunology of Type 1 DiabetesKPRI Bina WaluyaÎncă nu există evaluări
- KNH 413 Diet Instruction Celiac DiseaseDocument3 paginiKNH 413 Diet Instruction Celiac Diseaseapi-301897220Încă nu există evaluări
- Nursing Care of Children With Indian Childhood Cirrhosis, Wilsons Disesase, Reyes SyndromeDocument26 paginiNursing Care of Children With Indian Childhood Cirrhosis, Wilsons Disesase, Reyes SyndromeDivya Nair100% (2)
- Booklet On Coeliac DiseaseDocument12 paginiBooklet On Coeliac DiseaseQiliang Liu100% (1)
- Hepatic ProblemsDocument29 paginiHepatic ProblemsQing Liang OngÎncă nu există evaluări
- Review Article On Gluten AllergyDocument4 paginiReview Article On Gluten Allergyfelicsp2001Încă nu există evaluări
- Diarrhoea in TravellersDocument5 paginiDiarrhoea in TravellersMazo KhanÎncă nu există evaluări
- Celiac DiseaseDocument35 paginiCeliac DiseaseRye HanaÎncă nu există evaluări
- Future diagnosis and management of celiac diseaseDocument9 paginiFuture diagnosis and management of celiac diseaseمودة المنعميÎncă nu există evaluări
- Pharmaceutical Sciences: Celiac Disease: From Pathophysiology To TreatmentDocument4 paginiPharmaceutical Sciences: Celiac Disease: From Pathophysiology To TreatmentiajpsÎncă nu există evaluări
- Gluten IntoleranceDocument8 paginiGluten IntoleranceSanda Maria CretoiuÎncă nu există evaluări
- Report DISORDERS OF MALABSORPTIONDocument8 paginiReport DISORDERS OF MALABSORPTIONKathleen Anzhelika B. NemenzoÎncă nu există evaluări
- Case Study 1-1Document9 paginiCase Study 1-1api-242226130Încă nu există evaluări
- C D /G I: Case ReportDocument3 paginiC D /G I: Case ReportCatalina Mariana MargarintÎncă nu există evaluări
- Case Study 1Document10 paginiCase Study 1api-242123281Încă nu există evaluări
- Celiac Disease: The Right Clinical Information, Right Where It's NeededDocument42 paginiCeliac Disease: The Right Clinical Information, Right Where It's NeededDragomir SandaÎncă nu există evaluări
- Chronic Diarrhea in ChildrenDocument30 paginiChronic Diarrhea in ChildrenRyan KadavilÎncă nu există evaluări
- Celiac DiseaseDocument11 paginiCeliac DiseaseXela AviàÎncă nu există evaluări
- REVISADO Murch2016 - Article - RecentAdvancesInCeliacDiseaseDocument8 paginiREVISADO Murch2016 - Article - RecentAdvancesInCeliacDiseaseCamilo ReyesÎncă nu există evaluări
- IBD Final11Document41 paginiIBD Final11abraham debebeÎncă nu există evaluări
- The Spectrum of Autoimmune Enteropathy: Natalia Nedelkopoulou, Evangelia Farmaki, Maesha Deheragoda and Babu VadamalayanDocument11 paginiThe Spectrum of Autoimmune Enteropathy: Natalia Nedelkopoulou, Evangelia Farmaki, Maesha Deheragoda and Babu VadamalayanjessicaÎncă nu există evaluări
- NCGS or WIS - J Pediatr 2015Document7 paginiNCGS or WIS - J Pediatr 2015Fernando Clemente YagoÎncă nu există evaluări
- Clinical Biochemistry of The Gastrointestinal TractDocument4 paginiClinical Biochemistry of The Gastrointestinal TractReuben JosephÎncă nu există evaluări
- Salmonella, Campylobacter, Yersinia Enterocolitica and Shigella InfectionsDocument3 paginiSalmonella, Campylobacter, Yersinia Enterocolitica and Shigella InfectionsKelvin BolusanÎncă nu există evaluări
- Adil Abood: Lec. 7 Gastrointestinal and Liver Diseases Gluten-Sensitive EnteropathyDocument6 paginiAdil Abood: Lec. 7 Gastrointestinal and Liver Diseases Gluten-Sensitive Enteropathyrania rÎncă nu există evaluări
- Diagnosing Toxic Megacolon and Amoebic Colitis (38 charactersDocument3 paginiDiagnosing Toxic Megacolon and Amoebic Colitis (38 charactersElle ReyesÎncă nu există evaluări
- Reviews: The Spectrum of Celiac Disease: Epidemiology, Clinical Aspects and TreatmentDocument10 paginiReviews: The Spectrum of Celiac Disease: Epidemiology, Clinical Aspects and TreatmentsserggiosÎncă nu există evaluări
- Diabetic Ketoacidosis in Toddler With A Diaper RashDocument4 paginiDiabetic Ketoacidosis in Toddler With A Diaper RashKarl Angelo MontanoÎncă nu există evaluări
- Jurnal Antioksidant Kel 1 Kelas ADocument8 paginiJurnal Antioksidant Kel 1 Kelas ACahyadi AzanÎncă nu există evaluări
- Hematemesis PDFDocument7 paginiHematemesis PDFkevin_jawanÎncă nu există evaluări
- Infection, Genetics and EvolutionDocument9 paginiInfection, Genetics and EvolutionAri Syuhada PutraÎncă nu există evaluări
- Hematemesis PDFDocument7 paginiHematemesis PDFkevin_jawanÎncă nu există evaluări
- Sri WahdaningDocument8 paginiSri WahdaningAri Syuhada PutraÎncă nu există evaluări
- Independent watchdog for natural aromatic materialsDocument36 paginiIndependent watchdog for natural aromatic materialsmosnaz13100% (1)
- 1 1Document5 pagini1 1Ari Syuhada PutraÎncă nu există evaluări
- Sri WahdaningDocument8 paginiSri WahdaningAri Syuhada PutraÎncă nu există evaluări
- Alisi and Onyeze 2008Document6 paginiAlisi and Onyeze 2008Ari Syuhada Putra100% (1)
- Terminalia CatappaDocument4 paginiTerminalia CatappadrvenkataÎncă nu există evaluări
- Thesis Shabboo (Inclusion of Mentha Piperita.... )Document126 paginiThesis Shabboo (Inclusion of Mentha Piperita.... )Ari Syuhada PutraÎncă nu există evaluări
- 1 1Document5 pagini1 1Ari Syuhada PutraÎncă nu există evaluări
- DocDocument16 paginiDocAri Syuhada PutraÎncă nu există evaluări
- IJBPS 7 (1) 20-27oDocument8 paginiIJBPS 7 (1) 20-27oAri Syuhada PutraÎncă nu există evaluări
- Jsir 64 (12) 973-977Document5 paginiJsir 64 (12) 973-977Ari Syuhada PutraÎncă nu există evaluări
- Objective: Methods:: D A A o - S V - L S S G I MDocument2 paginiObjective: Methods:: D A A o - S V - L S S G I MAri Syuhada PutraÎncă nu există evaluări
- In Situ Gel-Forming Systems for Sustained Ocular Drug DeliveryDocument4 paginiIn Situ Gel-Forming Systems for Sustained Ocular Drug DeliveryAri Syuhada PutraÎncă nu există evaluări
- Medicinal Plants of the Zingiberaceae FamilyDocument32 paginiMedicinal Plants of the Zingiberaceae FamilyAPLAshokÎncă nu există evaluări
- 6 Ajps 3 1 2013Document6 pagini6 Ajps 3 1 2013Ari Syuhada PutraÎncă nu există evaluări
- (98252436) 1 2013Document24 pagini(98252436) 1 2013Ari Syuhada PutraÎncă nu există evaluări
- Antioxidant Properties of Ligustrum vulgare ExtractsDocument0 paginiAntioxidant Properties of Ligustrum vulgare ExtractsAri Syuhada PutraÎncă nu există evaluări
- OkeDocument9 paginiOkeAri Syuhada PutraÎncă nu există evaluări
- Comp RAPD-ERIC 4 SalmDocument6 paginiComp RAPD-ERIC 4 SalmAri Syuhada PutraÎncă nu există evaluări
- Ecoli 0157Document4 paginiEcoli 0157Ari Syuhada PutraÎncă nu există evaluări
- Salmonella EnteritidisDocument9 paginiSalmonella EnteritidisAri Syuhada PutraÎncă nu există evaluări
- ViewFreeArticle PDFDocument13 paginiViewFreeArticle PDFAri Syuhada PutraÎncă nu există evaluări
- Jung Et Al PDFDocument9 paginiJung Et Al PDFAri Syuhada PutraÎncă nu există evaluări
- 11 RJPT 5 12 2012 PDFDocument6 pagini11 RJPT 5 12 2012 PDFAri Syuhada PutraÎncă nu există evaluări
- Glositis PDFDocument1 paginăGlositis PDFNenny HariyantoÎncă nu există evaluări
- Sample Chapter 8.1Document25 paginiSample Chapter 8.1Adel Hassan100% (1)
- Application of Dorothea Orem-PRELIMSDocument6 paginiApplication of Dorothea Orem-PRELIMSJessica Ella Hernandez Agunday0% (1)
- Benefits of Sunflower OilDocument13 paginiBenefits of Sunflower OilMihaela StancescuÎncă nu există evaluări
- Popular Pet Snakes Available in South Africa EbookDocument15 paginiPopular Pet Snakes Available in South Africa EbookTimothy ZediÎncă nu există evaluări
- Adolescent Development ArticleDocument8 paginiAdolescent Development Articleapi-308979239Încă nu există evaluări
- Underutilised Greens in KarnatakaDocument3 paginiUnderutilised Greens in KarnatakashalÎncă nu există evaluări
- Aet 1 Fruit Crops (2010) PDFDocument311 paginiAet 1 Fruit Crops (2010) PDFIqbalFahreziÎncă nu există evaluări
- Feasibility Study On Production of RasaposhaDocument42 paginiFeasibility Study On Production of Rasaposhaesubalew sintieÎncă nu există evaluări
- Dr. Berg Has Devised A Unique Ketogenic Diet That Is Adaptable To Any LifestyleDocument3 paginiDr. Berg Has Devised A Unique Ketogenic Diet That Is Adaptable To Any LifestylePR.comÎncă nu există evaluări
- Understanding Consumer Preference For Coconut Sugar Using Conjoint Analysis Approach 121212Document5 paginiUnderstanding Consumer Preference For Coconut Sugar Using Conjoint Analysis Approach 121212Ralph Justin IIÎncă nu există evaluări
- OpdDocument341 paginiOpdzahrabokerÎncă nu există evaluări
- HPLC-ESI-MS Analysis of Vitamin B12 in Food Products and in Multivitamins-Multimineral Tablets PDFDocument5 paginiHPLC-ESI-MS Analysis of Vitamin B12 in Food Products and in Multivitamins-Multimineral Tablets PDFGiangÎncă nu există evaluări
- CALORIE CONTENT OF FOODSDocument2 paginiCALORIE CONTENT OF FOODSSusan MishraÎncă nu există evaluări
- SPM 4551 2006 Biology k2 BerjawapanDocument15 paginiSPM 4551 2006 Biology k2 Berjawapanpss smk selandarÎncă nu există evaluări
- 3 DayfullbodyplantfitnessworkoutDocument1 pagină3 DayfullbodyplantfitnessworkoutFelix ReveronÎncă nu există evaluări
- Dietabajaencarbohidratos Moreno Capponi 2020Document11 paginiDietabajaencarbohidratos Moreno Capponi 2020PerlaÎncă nu există evaluări
- LipidsDocument49 paginiLipidsAnumeha MittalÎncă nu există evaluări
- Chap44 PDFDocument4 paginiChap44 PDFHerry SasukeÎncă nu există evaluări
- Risk Factors of Diabetes in RawalpindiDocument29 paginiRisk Factors of Diabetes in RawalpindiFarrukh Ali BaigÎncă nu există evaluări
- Resume For AsanteDocument2 paginiResume For Asanteapi-239305061Încă nu există evaluări
- Application of High Hydrostatic Pressure To Meat andDocument16 paginiApplication of High Hydrostatic Pressure To Meat andJohanna VargasÎncă nu există evaluări