Documente Academic
Documente Profesional
Documente Cultură
Milroy Disease Pak Tomo
Încărcat de
Meta Sari0 evaluări0% au considerat acest document util (0 voturi)
220 vizualizări3 paginiMilroy Disease is an autosomal dominant inherited form of lymphedema. Inadequate lymphatic drainage may be attributed to congenital lymphatic hypoplasia or structural damage to lymphatic vessels. There is no specific therapy for Milroy disease.
Descriere originală:
Drepturi de autor
© © All Rights Reserved
Formate disponibile
DOCX, PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentMilroy Disease is an autosomal dominant inherited form of lymphedema. Inadequate lymphatic drainage may be attributed to congenital lymphatic hypoplasia or structural damage to lymphatic vessels. There is no specific therapy for Milroy disease.
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca DOCX, PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
220 vizualizări3 paginiMilroy Disease Pak Tomo
Încărcat de
Meta SariMilroy Disease is an autosomal dominant inherited form of lymphedema. Inadequate lymphatic drainage may be attributed to congenital lymphatic hypoplasia or structural damage to lymphatic vessels. There is no specific therapy for Milroy disease.
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca DOCX, PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 3
Milroy Disease
Wed, 02/20/13 - 13:29
Authors:
ALEXANDER K. C. LEUNG, MD
University of Calgary
HARDALLY R. HEGDE, MD
Alberta Childrens Hospital
Deepak M. Kamat, MD, PhDSeries Editor: Dr Kamat is professor of pediatrics at Wayne State University in
Detroit. He is also director of the Institute of Medical Education and vice chair of education at Childrens Hospital of
Michigan, both in Detroit.
A male infant was delivered at term to a 24-year-old woman (gravida 3, para 1). The pregnancy had been
uncomplicated; the vaginal delivery was normal. Apgar scores were 7 at 1 minute and 9 at 5 minutes. Birth weight
was 3020 g (6 lb 11 oz); length, 51 cm (20 in); and head circumference, 36 cm (14 in).
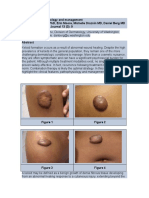
Nonpitting edema of both feet was noted at birth; all other physical examination findings were normal. A review of the
family history revealed that the childs father and paternal grandfather had lymphedema of both feet at birth.
Milroy disease was diagnosed. This is an autosomal dominant inherited form of lymphedema, with onset at or near
birth.
Inadequate lymphatic drainage that causes lymphedema may be attributed to congenital lymphatic hypoplasia or to
structural damage to lymphatic vessels. Congenital lymphatic hypoplasia is associated with Milroy disease, Turner
syndrome, Noonan syndrome, yellow nail syndrome, lymphedema praecox, and distichiasis. Damage to the
lymphatic vessels can occur from surgery, trauma, neoplasms, radiation therapy, and chronic lymphangitis caused by
filariasis or lymphogranuloma venereum.
There is no specific therapy for Milroy disease. Affected limbs should be elevated whenever possible. If skin sepsis
occurs, prompt treatment is necessary to prevent further lymphatic insufficiency. Over time, fibrosis develops in the
interstitial tissues and the skin may become thickened and pigmented. Skin ulcers can occur at sites of pressure.
FOR MORE INFORMATION:
Leung AK, Robson WL. Oedema in childhood. J R Soc Health. 2000;120:212-219.
Milroy Disease.
Authors
Brice GW, Mansour S, Ostergaard P, Connell F, Jeffery S, Mortimer P.
Editors
In: Pagon RA, Adam MP, Ardinger HH, Bird TD, Dolan CR, Fong CT, Smith RJH, Stephens K, editors.
Source
GeneReviews
[Internet]. Seattle (WA): University of Washington, Seattle; 1993-2014.
2006 Apr 27 [updated 2009 Jul 23].
Excerpt
DISEASE CHARACTERISTICS:
Milroy disease is characterized by lower-limb lymphedema, present at birth as pedal edema or developing
soon after. Occasionally it develops later in life. The severity of edema shows both inter- and intrafamilial
variability. Swelling is usually bilateral but can be asymmetric. The degree of edema can progress but in
some instances can improve, particularly in early years. Other features sometimes associated with Milroy
disease include hydrocele (37% of males), prominent veins (23%), upslanting toenails (14%),
papillomatosis (10%), and urethral abnormalities in males (4%). Cellulitis, which can damage the
lymphatic vessels, occurs in approximately 20% of affected individuals, with infection significantly more
likely in males than females.
DIAGNOSIS/TESTING:
Milroy disease is diagnosed by clinical findings and confirmed by molecular genetic testing.
Lymphoscintigraphy can be performed; the characteristic finding is lack of uptake of radioactive colloid in
the ilioinguinal lymph nodes caused by a paucity of lymphatic vessels or abnormal function of the vessels
in the lower limbs. FLT4 (VEGFR3) is the only gene known to be associated with Milroy disease.
MANAGEMENT:
Treatment of manifestations: A lymphedema therapist may utilize fitted stockings and massage to
improve the cosmetic appearance or decrease the size of the limb and reduce the risk of complications.
Improvement in swelling is usually possible with use of properly fitted compression hosiery and/or
bandaging. Prevention of secondary complications: Frequency of cellulitis can be reduced through good
skin hygiene, prompt treatment of infections with antibiotics, and prophylactic antibiotics for recurrent
episodes. Agents/circumstances to avoid: wounds to limbs; long periods of immobility with the legs in a
dependent position; and medications that can cause increased leg swelling. Evaluation of relatives at risk:
Evaluating relatives at risk ensures identification of those who will benefit from treatment early in the
disease course.
GENETIC COUNSELING:
Milroy disease is inherited in an autosomal dominant manner. Each child of an individual with Milroy
disease has a 50% chance of inheriting the mutation. The proportion of cases caused by de novo
mutations is not known. Ultrasonography in the third trimester of pregnancy may detect swelling of the
dorsum of the feet and more extensive edematous states in an affected fetus. Prenatal testing is possible
for pregnancies at increased risk if the disease-causing mutation in the family is known; however, it is
rarely requested.
Copyright 1993-2014, University of Washington, Seattle. All rights reserved.
S-ar putea să vă placă și
- Multiple Myeloma and Other Plasma Cell NeoplasmsDe la EverandMultiple Myeloma and Other Plasma Cell NeoplasmsMeletios A. DimopoulosÎncă nu există evaluări
- Sickle Cell DiseaseDocument10 paginiSickle Cell Diseasekarthikavvari2002Încă nu există evaluări
- CREOG OutlineDocument68 paginiCREOG OutlineadfsnkdfÎncă nu există evaluări
- Lipedema An Inherited Condition 2010Document7 paginiLipedema An Inherited Condition 2010cure lipedema100% (1)
- Why Are My Legs SwollenDocument5 paginiWhy Are My Legs SwollenekramsÎncă nu există evaluări
- Diagnosis and Clinical Features of Pemphigus VulgarisDocument1 paginăDiagnosis and Clinical Features of Pemphigus VulgarisDwiKamaswariÎncă nu există evaluări
- NCM 112 Guide to Caring for Patients with CancerDocument15 paginiNCM 112 Guide to Caring for Patients with CancerShiena Mae PelagioÎncă nu există evaluări
- Soroori-Motlagh Nastaran 200705 (SCID)Document29 paginiSoroori-Motlagh Nastaran 200705 (SCID)Charles IppolitoÎncă nu există evaluări
- Refmh 9Document10 paginiRefmh 9Anonymous S0MyRHÎncă nu există evaluări
- Multiple Dermatofibromas in An Adult FemaleDocument3 paginiMultiple Dermatofibromas in An Adult FemaleDeba P SarmaÎncă nu există evaluări
- Ecthyma Contagiosum (Human Orf)Document2 paginiEcthyma Contagiosum (Human Orf)Deba P SarmaÎncă nu există evaluări
- Seminar Presentation On GeneticsDocument60 paginiSeminar Presentation On GeneticsHardeep KaurÎncă nu există evaluări
- Seminar PresentatonDocument14 paginiSeminar PresentatonTemidayoÎncă nu există evaluări
- Lymphogranuloma Venereum (LGV) - Background, Pathophysiology, EpidemiologyDocument7 paginiLymphogranuloma Venereum (LGV) - Background, Pathophysiology, EpidemiologyARHÎncă nu există evaluări
- Literature Review On ElephantiasisDocument6 paginiLiterature Review On Elephantiasisdajev1budaz2100% (1)
- Literature Review CellulitisDocument6 paginiLiterature Review Cellulitisc5qe3qg3100% (1)
- CSS Uterine FibroidDocument20 paginiCSS Uterine FibroidDwiki Wahyu PratamaÎncă nu există evaluări
- Advanced Rhabdomyosarcoma During Pregnancy: Author InformationDocument4 paginiAdvanced Rhabdomyosarcoma During Pregnancy: Author InformationJonathan PabloÎncă nu există evaluări
- We Care House FixDocument24 paginiWe Care House FixRifa'atul MahmudahÎncă nu există evaluări
- Keloid (Ing)Document16 paginiKeloid (Ing)Daniel PremÎncă nu există evaluări
- Problem 4-Block 6 KamlaDocument10 paginiProblem 4-Block 6 KamlaKemo ElmughrabiÎncă nu există evaluări
- Hiperleucocitosis 2010Document3 paginiHiperleucocitosis 2010MAR�A FERNANDA MEDINA FUENTESÎncă nu există evaluări
- LeukemiaDocument7 paginiLeukemiaHilda HallÎncă nu există evaluări
- SLE (Vicky.R)Document5 paginiSLE (Vicky.R)Anggi TalumepaÎncă nu există evaluări
- Your Guide to Understanding Systemic SclerodermaDocument6 paginiYour Guide to Understanding Systemic SclerodermaNarendraswari Mendina KusumawardhaniÎncă nu există evaluări
- CELLULAR and CHROMOSOMAL ABERRATIONSDocument6 paginiCELLULAR and CHROMOSOMAL ABERRATIONSVIVIEN CONSIGNAÎncă nu există evaluări
- Genes and Human Disease: Monogenic DiseasesDocument8 paginiGenes and Human Disease: Monogenic DiseasesE.R.OÎncă nu există evaluări
- Genes and Human Disease: Monogenic DiseasesDocument8 paginiGenes and Human Disease: Monogenic DiseasesE.R.OÎncă nu există evaluări
- Vgygcc BHJJJJDocument4 paginiVgygcc BHJJJJVsbshÎncă nu există evaluări
- Complications of Ichthyosis in ChildrenDocument8 paginiComplications of Ichthyosis in ChildrenEnny AndrianiÎncă nu există evaluări
- Keloid SDocument33 paginiKeloid SnovieÎncă nu există evaluări
- Cancer: The Uncontrolled Growth of Abnormal CellsDocument10 paginiCancer: The Uncontrolled Growth of Abnormal CellsManik KapoorÎncă nu există evaluări
- PHD Thesis LeukemiaDocument6 paginiPHD Thesis Leukemiaafjryccau100% (2)
- RPB14150079015Document5 paginiRPB14150079015Ijupbs IjupbsÎncă nu există evaluări
- A Mutation On The 22 ChromosomeDocument16 paginiA Mutation On The 22 ChromosomeRose de DiosÎncă nu există evaluări
- Keloids: Clinica L Fea Tures A ND M A Na Gem Ent.: Review ArticleDocument8 paginiKeloids: Clinica L Fea Tures A ND M A Na Gem Ent.: Review ArticleAndri Feisal NasutionÎncă nu există evaluări
- University of Makati FinalDocument48 paginiUniversity of Makati FinalJosephus Vejano BlancoÎncă nu există evaluări
- Adult Lymphangioma Rare CasesDocument3 paginiAdult Lymphangioma Rare CasesRini RahmawulandariÎncă nu există evaluări
- Shankland NHL Lancet Review PDFDocument10 paginiShankland NHL Lancet Review PDFNadhila ByantÎncă nu există evaluări
- LEUKEMIADocument19 paginiLEUKEMIAjay dewanagnÎncă nu există evaluări
- Haematogenous OsteomyelitisDocument6 paginiHaematogenous OsteomyelitisbilafarÎncă nu există evaluări
- Genetic Basis of DiseaseDocument6 paginiGenetic Basis of Diseasedr saadia anjumÎncă nu există evaluări
- Diagnostics 11 00794 v2Document11 paginiDiagnostics 11 00794 v2Adn crnÎncă nu există evaluări
- Children - Acute Transvers MyelitisDocument6 paginiChildren - Acute Transvers MyelitisHAKIMOPÎncă nu există evaluări
- Monkey PoxDocument10 paginiMonkey PoxJohn AmazingÎncă nu există evaluări
- Scloderma JurnalDocument17 paginiScloderma JurnalImam Hakim SuryonoÎncă nu există evaluări
- Unilesional Self-Limited LangerhansDocument6 paginiUnilesional Self-Limited LangerhansumhuyÎncă nu există evaluări
- US Surgeons Remove Huge Tumor Off Haitian GirlDocument5 paginiUS Surgeons Remove Huge Tumor Off Haitian Girlapi-26570979Încă nu există evaluări
- Pityriasis Alba: A Condition With Possibly Multiple EtiologiesDocument2 paginiPityriasis Alba: A Condition With Possibly Multiple EtiologiesAndana Haris R.Încă nu există evaluări
- Hutter2010 LeucemiaDocument10 paginiHutter2010 LeucemiasarabisimonaÎncă nu există evaluări
- Fetal-Specific CD8+ Cytotoxic T Cell Responses Develop During Normal Human Pregnancy and Exhibit Broad Functional CapacityDocument10 paginiFetal-Specific CD8+ Cytotoxic T Cell Responses Develop During Normal Human Pregnancy and Exhibit Broad Functional Capacity石一Încă nu există evaluări
- Slifirczyk 1Document6 paginiSlifirczyk 1fatimamahmoud.20129Încă nu există evaluări
- 430141019 blood cancer محولDocument22 pagini430141019 blood cancer محولShaker MahmoodÎncă nu există evaluări
- CancerDocument14 paginiCancerNano AlmukasabyÎncă nu există evaluări
- Loa LoaDocument22 paginiLoa LoaphilmonÎncă nu există evaluări
- Dermatological Signs in Wilson's DiseaseDocument4 paginiDermatological Signs in Wilson's DiseaseGingerWiseÎncă nu există evaluări
- Infantile Hemangiomas: A Review: Pediatric Ophthalmology UpdateDocument9 paginiInfantile Hemangiomas: A Review: Pediatric Ophthalmology UpdateYipno Wanhar El MawardiÎncă nu există evaluări
- Phimosis in ChildrenDocument7 paginiPhimosis in ChildrenfeonajaparÎncă nu există evaluări
- Dialysis Power PointDocument20 paginiDialysis Power PointJor GarciaÎncă nu există evaluări
- AcetaminophenDocument2 paginiAcetaminophendrugcardref100% (1)
- Divine Intervention Episode 22 Obgyn Shelf Review PDFDocument167 paginiDivine Intervention Episode 22 Obgyn Shelf Review PDFSwisskelly1100% (1)
- PMVDocument28 paginiPMVRajesh VermaÎncă nu există evaluări
- Anti-Drug Campaign SpeechDocument2 paginiAnti-Drug Campaign SpeechGracel Gonzaga Eviota91% (11)
- Glutathione and Its Antiaging and Antimelanogenic EffectsDocument7 paginiGlutathione and Its Antiaging and Antimelanogenic EffectsG. I.Încă nu există evaluări
- Psychoanalysis Case Study of Gregory HouseDocument6 paginiPsychoanalysis Case Study of Gregory HouseTheodora Catalina100% (2)
- Gad-7 Questionnaire SpanishDocument86 paginiGad-7 Questionnaire Spanishrowanpurdy100% (1)
- Depression: A Global Public Health ConcernDocument3 paginiDepression: A Global Public Health ConcernanalailaÎncă nu există evaluări
- Lab Technician Resume TitleDocument1 paginăLab Technician Resume TitleSilvio DTÎncă nu există evaluări
- Daftar Pustaka: Farmakologi Terapi. Goodman & Gilman. Edisi 10. Jakarta. EGC. H. 433-464Document5 paginiDaftar Pustaka: Farmakologi Terapi. Goodman & Gilman. Edisi 10. Jakarta. EGC. H. 433-464Muhammad FadhlurrohmanÎncă nu există evaluări
- PublicationDocument5 paginiPublicationMahfuzur RÎncă nu există evaluări
- Ann BibDocument5 paginiAnn Bibapi-317311486Încă nu există evaluări
- Skin, Soft Tissue & BreastDocument10 paginiSkin, Soft Tissue & BreastFarhin100% (1)
- Preterm Labor ManagementDocument50 paginiPreterm Labor ManagementDr-Firas Nayf Al-ThawabiaÎncă nu există evaluări
- CKD CHCRTDocument28 paginiCKD CHCRTNurhidayati KeriyunÎncă nu există evaluări
- Taming The Id and Strengthening The Ego - Martha Stark MDDocument208 paginiTaming The Id and Strengthening The Ego - Martha Stark MDSasu NicoletaÎncă nu există evaluări
- Foreign Qualification Recognition GuideDocument2 paginiForeign Qualification Recognition Guidesatishg99Încă nu există evaluări
- Biology ProjectDocument12 paginiBiology Projectapi-380313126100% (2)
- NANDA DefinitionDocument5 paginiNANDA DefinitionAngel_Liboon_388Încă nu există evaluări
- RICE or MEAT Protocol For Acute Ligament Sprain Treatment - The Sports PhysiotherapistDocument4 paginiRICE or MEAT Protocol For Acute Ligament Sprain Treatment - The Sports PhysiotherapistZach FallonÎncă nu există evaluări
- Albert Ellis Reason and Emotion in PsychotherapyDocument456 paginiAlbert Ellis Reason and Emotion in PsychotherapyCristian Catalina100% (2)
- Couple Therapy QuestionsDocument2 paginiCouple Therapy QuestionsAnda OpreaÎncă nu există evaluări
- Proptosis UnilateralDocument5 paginiProptosis UnilateralCarlos NiveloÎncă nu există evaluări
- Tgwellness Massage g10pdfDocument71 paginiTgwellness Massage g10pdfStephenÎncă nu există evaluări
- Alzheimer's Research PaperDocument5 paginiAlzheimer's Research PaperJosh BarnutÎncă nu există evaluări
- Kasabach Merritt SyndromeDocument33 paginiKasabach Merritt SyndromeAndrew Arnold David VillanuevaÎncă nu există evaluări
- Oral Candidiasis: Dr. Ahmad Yusran, SPPDDocument87 paginiOral Candidiasis: Dr. Ahmad Yusran, SPPDM Nedi Sevtia BudiÎncă nu există evaluări
- Pfizer Et. Al. v. Intas Pharmaceuticals Et. Al.Document15 paginiPfizer Et. Al. v. Intas Pharmaceuticals Et. Al.PriorSmartÎncă nu există evaluări
- Reality TherapyDocument2 paginiReality TherapyAGLDÎncă nu există evaluări