Documente Academic
Documente Profesional
Documente Cultură
Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, And Endodontology Volume 93 Issue 1 2002 [Doi 10.1067_moe.2002.119519] Norbert Jakse; Vedat Bankaoglu; Gernot Wimmer; Antranik Eskici; -- Primary Woun
Încărcat de
Mr-Ton Drg0 evaluări0% au considerat acest document util (0 voturi)
99 vizualizări6 paginiEnvelope flap with a distal relieving incision to the mandibular ramus is the most common approach for lower third molar surgery. Wound dehiscences at the distofacial edge of the adjacent second molar are very frequent. Several different flap techniques were developed, compared, and discussed.
Descriere originală:
Drepturi de autor
© © All Rights Reserved
Formate disponibile
PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentEnvelope flap with a distal relieving incision to the mandibular ramus is the most common approach for lower third molar surgery. Wound dehiscences at the distofacial edge of the adjacent second molar are very frequent. Several different flap techniques were developed, compared, and discussed.
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
99 vizualizări6 paginiOral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, And Endodontology Volume 93 Issue 1 2002 [Doi 10.1067_moe.2002.119519] Norbert Jakse; Vedat Bankaoglu; Gernot Wimmer; Antranik Eskici; -- Primary Woun
Încărcat de
Mr-Ton DrgEnvelope flap with a distal relieving incision to the mandibular ramus is the most common approach for lower third molar surgery. Wound dehiscences at the distofacial edge of the adjacent second molar are very frequent. Several different flap techniques were developed, compared, and discussed.
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 6
The envelope flap with a distal relieving incision to the
mandibular ramus is the most common approach for
lower third molar surgery. This flap technique has often
been described extensively in the relevant literature and
is certainly favored by a majority of the oral surgery
centers.
1-7
Usually, a primary wound closure is
performed, both to diminish the patients discomfort
and to simplify postsurgical treatment.
There are no specific data available from the litera-
ture, but when using the envelope flap, it must be
remembered that wound dehiscences at the distofacial
edge of the adjacent second molar are very frequent in
the first phase of wound healing.
8
Such dehiscences
may heal secondarily without any additional discom-
fort or consequences. Nevertheless, they potentially
extend the time of postsurgical treatment. From the
patients point of view, they could cause a longer
period of discomfort and continuous pain. Furthermore,
they may favor the development of alveolar osteitis,
and, in consequence, they could be the reason for a loss
of attachment distal to the adjacent second molar (Fig
1, A and B).
With the aim of avoiding potential periodontal
complications to the adjacent second molar, several
different flap techniques were developed, compared,
and discussed.
3-5,9-15
Nevertheless, all published
studies are restricted to long-term results of the peri-
odontal tissue around the second and the first molar.
None of the studies evaluates primary wound healing
after third molar surgery.
It was the aim of this prospective study to evaluate
the influence of flap design on the course of primary
wound healing. We examined whether a modification
of a vestibular triangular flap, as first described by
Szmyd,
2
would reduce the incidence of dehiscences. In
addition, the importance of flap design for wound
healing was compared with factors such as nicotine
habits, the patients age, the duration of surgery, and
the level of impaction.
Primary wound healing after lower third molar surgery: Evaluation
of 2 different flap designs
Norbert Jakse, MD, DDS,
a
Vedat Bankaoglu, DDS,
a
Gernot Wimmer, MD,
b
Antranik Eskici, MD,
DDS,
a
and Christof Pertl, MD, DDS,
a
Graz, Austria
KARL-FRANZENS UNIVERSITY GRAZ
Objectives. Wound dehiscences after lower third molar surgery potentially extend the time of postsurgical treatment and may
cause long-lasting pain. It was the aim of this prospective study to evaluate the primary wound healing of 2 different flap
designs.
Methods. Sixty completely covered lower third molars were removed. In 30 cases, the classic envelope flap with a sulcular
incision from the first to the second molar and a distal relieving incision to the mandibular ramus was used, whereas the other
30 third molars were extracted after preparation of a modified triangular flap first similarly described by Szmyd. Wound
healing was controlled on the first postoperative day, as well as 1 and 2 weeks after surgery.
Results. The overall result was a total of 33% wound dehiscence. In the envelope-flap group, wound dehiscences developed
in 57% of the cases. This represents a relative risk ratio of 5.67, with a 95% CI from 1.852 to 12.336. With the modified trian-
gular-flap technique, only 10% of the wounds gaped during wound healing.
Conclusion. This study confirms evidence that the flap design in lower third molar surgery considerably influences primary
wound healing. The modified triangular flap is significantly less conducive to the development of wound dehiscence.
(Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2002;93:7-12)
a
The Department for Oral Surgery and Radiology, Dental School,
Karl-Franzens University Graz.
b
Department for Prosthetics and Periodontology, Dental School,
Karl-Franzens University Graz.
Received for publication Apr 12, 2001; returned for revision Jun 8,
2001; accepted for publication Aug 13, 2001.
Copyright 2002 by Mosby, Inc.
1079-2104/2002/$35.00 + 0 7/12/119519
doi:10.1067/moe.2002.119519
7
ORAL AND MAXILLOFACIAL SURGERY Editor: Larry J. Peterson
ORAL SURGERY
ORAL MEDICINE
ORAL PATHOLOGY
Vol. 93 No. 1 January 2002
MATERIAL AND METHODS
A total of 60 completely covered lower third molars
from 60 patients were removed by 3 experienced oral
surgeons. Patients were between 15 and 60 years old,
with the average age being 25 years. There were 32
female and 28 male patients.
The medical history revealed no sickness or medica-
tion that would influence the course of wound healing
after oral surgery. The number of smokers among those
60 patients was 9, with 5 of them smoking occasionally
(ie, up to 10 cigarettes a day), 3 patients smoking up to
20 cigarettes a day, and 1 patient more than 20 a day.
Among the relevant criteria for the study were a healthy
dental and periodontal state (CPITN 0-1). All patients
were referred for wisdom teeth removal. The referring
doctor gave the indication in each case, with all of the
cases being prophylactic or concerning orthodontics.
There was no case of local inflammation or pathology.
Before the procedure, all patients were informed
about the operation, the recommended postsurgical
behavior, and possible complications. All patients
agreed to the operation, indicated by their signature (in
case of minors, the parents gave the signed consent).
Out of 60 completely covered lower third molars, 38
were totally osseously impacted. There were 33 left
lower wisdom teeth and 27 right lower wisdom teeth.
The surgery was carried out with the patients under
local anesthesia. The anesthetic was Articaine in a 4%
solution with additional epinephrine in a concentration
of 1:100 000 (Ultracaine-Dental forte; Hchst Marion
Roussel, Frankfurt/Main, Germany).
In 30 cases, which were chosen at random, the enve-
lope flap with a sulcular incision from the first to the
second molar and a distal relieving incision to the
mandibular ramus were used (technique I), whereas the
other 30 wisdom teeth were extracted after a modified
triangular flap design first described by Szmyd
2
(tech-
nique II).
Flap designs
Technique I: envelope flap with a sulcular incision
from the first to the second molar and a distal
relieving incision to the mandibular ramus. The inci-
sion was done from the mandibular ramus to the disto-
buccal crown edge of the second molar, cutting in one
move through all layers of the soft tissue to the bone.
From there, a sulcular buccal incision was made to the
middle of the first molar (Fig 2). The mucoperiosteal
flap was elevated entirely down to the buccal surface of
the mandible. Distal to the second molar a periosteal
elevator was used to prepare subperiosteally to the
lingual area, to protect the lingual nerve.
Technique IImodified triangular flap. The first
part of the incision was similar to technique I. The inci-
sion was done from the mandibular ramus to the disto-
buccal crown edge of the second molar, continued by a
perpendicular incision line, obliquely into the
mandibular vestibulum, with a length of about 10 mm.
In contrast to the incision line originally described by
Szmyd,
2
the modified incision extends over the
mucogingival borderline. The periodontium of the
second molar was only touched at the distofacial edge
(Fig 3). By preparing the buccal mucoperiosteum, a
triangular flap was formed (vestibular triangular flap).
The lingual preparation was the same as for technique I.
After mobilizing the mucoperiosteal flap and uncov-
ering the surgical site, the proceedings were always the
8 Jakse et al ORAL SURGERY ORAL MEDICINE ORAL PATHOLOGY
January 2002
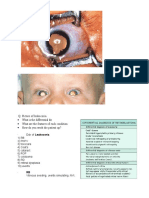
Fig 1. A, B, Illustration and clinical view of a dehiscence after
third molar surgery using the envelope flap technique.
A
B
same, regardless of the flap design. The crown, which
was partially or even completely osseously covered,
was uncovered from occlusal down to the equator with
rotating instruments of diminishing size. In case of
tilted teeth, a fissure bur was used to separate the tooth.
After extraction, potential rests of the dental follicle
were removed. The alveolus was filled with a gelatin
sponge (Spongostan; Johnson & Johnson Medical
Limited, Gargrave, Skipton, United Kingdom). In all
cases a primary wound closure was carried out with
atraumatic sutures (Supramid 3-0; B. Braun Surgical
GmbH, Melsungen, Germany).
The envelope flap was closed with 2 or 3 single-button
sutures distal to the second molar, paying special atten-
tion to an exact repositioning in the area of the gingival
margin. In addition, the flap was adapted with inter-
dental sutures between the first and the second molar.
For the triangular flap, the same suturing technique was
used distally, whereas the perpendicular incision was only
adapted with a single coronally placed suture. Again,
exact reposition of the gingival margin in the area of the
second molar was the aim. The loose adaption in the
apical portion allows easy relief of a hematoma (Fig 4).
After the operation, all patients were treated antibiot-
ically and antiphlogistically as follows: for 4 days with
cephalosporin (Ospexin, 1000 mg 3 1; Biochemie,
Vienna, Austria), and for 2 days with diclofenac
(Voltaren, 50 mg 3 1; Novartis Pharma, Vienna,
Austria).
All patients were seen on days 1, 7, and 14 after
surgery. On the first postoperative day, all wounds were
relieved distally by slight spreading and compression
in case of envelope flaps, whereas triangular flaps were
relieved in the area of the vestibular incision. Visual
control and cautious exploration with a periodontal
probe were used to evaluate a possible dehiscence. In
this study, every gaping along the entire incision line
was defined as a dehiscence. In this respect, particular
attention was paid to the gingival margin at the distal
rim of the second molar. This evaluation, as well as the
preoperative periodontal diagnosis, was performed by
one periodontist who was not involved in the surgical
procedure. Sutures were removed after 1 week.
Only patients with good oral hygiene and no signs of
plaque-induced inflammation before and after surgery
were included in the study.
The subsequent statistical evaluation was performed
with the relative risk ratio of cohort or prospective
studies.
16
It was composed of the factors that may
influence wound healing (ie, flap design, the patients
age, duration of the surgery, level of retention, and
nicotine habits). These aspects were defined in terms of
their relationship with the occurrence of dehiscences.
The relative risk of a disturbance in the healing process
(ie, wound dehiscences) was determined for each of the
aforementioned factors.
RESULTS
Out of the 60 surgical sites, 20 dehiscences (33%)
were found. Although on the first day after surgery, all
wounds were well closed without any sign of a begin-
ning rupture, after 1 week, 20 cases showed gaping
wound margins distobuccal to the second molar. No
additional dehiscence developed between day 7 and
ORAL SURGERY ORAL MEDICINE ORAL PATHOLOGY Jakse et al 9
Volume 93, Number 1
Fig 2. Illustration of the incision line used for the envelope
flap in lower third molar surgerydistal relieving incision to
the mandibular ramus and sulcular incision from the second
molar to the first molar.
Fig 3. Illustration of the incision line used for the triangular
flap in lower third molar surgerywith a distal relieving inci-
sion to the mandibular ramus and a perpendicular anterior
incision into the mandibular vestibulum.
day 14 postsurgery. Neither the size nor the shape of
the present dehiscences changed during this time.
The age of the patient did not influence the incidence
of dehiscences. In the group of patients up to the age of
25 years (n = 41), a dehiscence occurred in 34% of the
cases, whereas for those older than 25 years (n = 19),
the percentage was 32%. The relative risk ratio for a
dehiscence was 0.93 (95% CI from 0.421 to 2.031) in
the group of older patients.
The duration of the surgery was between 10 and 50
minutes. When the surgery lasted less than 25 minutes
(n = 42), dehiscences occurred in 29% of the cases
during wound healing. When the duration of the
surgery exceeded 25 minutes (n = 18), there was a
dehiscence percentage of 44%. This represents a rela-
tive risk ratio of 1.56 (95% confidence interval from
0.769 to 3.145) for a dehiscence in the group with the
longer surgery duration compared with the ratio of the
group with a surgery shorter than 25 minutes.
Among the 38 osseous impacted teeth, 10 cases
(26%) of postoperative dehiscences were found. The
22 molars that were only partially covered by bone in
10 cases (46%) showed dehiscences. The relative risk
ratio of a rupture of the primary wound closure for this
group was 1.73 (95% CI from 0.856 to 3.485).
Without considering the extent of the individual
nicotine habit, there was a 40% dehiscence rate found
in the group of smokers. The relative risk ratio for the
smoking patients to develop a dehiscence was 1.25
(95% CI from 0.529 to 2.954).
Duration of surgery, level of impaction, and smoking
habit did influence the primary wound healing, but
these factors did not attain statistical significance.
In 17 (57%) of the 30 surgeries performed with the
envelope-flap technique, a dehiscence was found. The
30 cases done with the triangular-flap technique, a
dehiscence developed in only 3 cases (10%). This
result represents a relative risk ratio of 5.67 (95%
confidence interval from 1.852 to 12.336) for the enve-
lope-flap design, which is of high statistical signifi-
cance (Fig 5).
DISCUSSION
An envelope flap with a sulcular incision from the
first to the second molar and a distal relieving incision
to the mandibular ramus is a widely used technique for
lower third molar surgery.
3-7
There are definite advan-
tages of this flap design. The surgical site is generously
uncovered, ensuring a good overview during surgery.
The sulcular incision can be prolonged mesially any
time, in case cystic lesions should extend mesially or if
additional endosurgery of the adjacent molars is
requested. As a consequence of the extensively
prepared mucoperiosteal flap, the osseous defect can
always be safely covered after the removal of the
molar. Moreover, a large flap with a broad base guar-
antees good vascularity up to the wound margins.
In the literature, possible disadvantages of this
method are discussed. Every preparation of a mucoper-
iosteal flap leads to a growing activity of osteoclasts in
the area of the alveolar process, inducing loss of alve-
olar bone.
17
Every sulcular incision is an intervention
to the periodontal ligament and may lead to periodontal
damage. Alternatively, paragingival
13
and vestibular
tongue-shaped
11
flap designs, which aim at sparing the
periodontal ligament of the adjacent molar, have been
described. Especially in cases of thin keratinized
gingiva in the area of the second molar, the conven-
tional flap design may lead to a total loss of the
attached gingiva in this area after the operation. This,
again, can cause pocket formation and loss of attach-
ment in the area of the second molar.
18
In addition, the frequent occurrence of dehiscences
distofacial to the second molar seems to be another
disadvantage of the envelope-flap design.
8
To our
knowledge, such primary wound healing disorders
have not been studiedparticularly in lower third
molar surgery.
These gapings are usually located at the distobuccal
gingival rim of the adjacent second molar, where the
distal relieving incision leads into the sulcular incision.
In this area, soft tissue tensions resulting from postop-
erative hematoma and masticatory movements may
induce a rupture of the wound margins during the first
few postoperative days. This is particularly true for the
envelope flap because it is fixed anteriorly with inter-
sulcular sutures. Such dehiscences can take place
inconspicuously and unnoticed by the patient and may
heal secondarily. Thus, secondary wound healing can
cause wedge-shaped defects of the gingiva distal to the
second molar, or it can favor a loss of attachment distal
10 Jakse et al ORAL SURGERY ORAL MEDICINE ORAL PATHOLOGY
January 2002
Fig 4. The triangular flap allows easy relief of the hematoma
during the first postoperative day.
to the second molar. This periodontal complication
after lower third molar surgery has been studied by
several authors.
1,3-5
A dehiscence does make hygiene more difficult and
requires intense follow-up treatment (ie, frequent irri-
gation and possible local medication). There is also a
chance for longer-lasting discomfort caused by hyper-
sensitivity in the area of the distally exposed root
surface of the second molar. Alveolar osteitis and soft
tissue abscess are more severe complications that are
possible.
The present study has clearly shown that the flap
design considerably influences primary wound healing
in lower third molar surgery. When the conventional
sulcular flap design is used, 56% of the patients
develop a disorder in primary wound healing, although
a primary wound closure was the aim. With the modi-
fication of a flap design, primary wound healing can be
significantly improved. With this flap design, dehis-
cences occurred in only 10% of our cases. We suggest
that this was because of a tension decrease in the area
of the distal wound closure compared with the situation
of the envelope flap technique. The vestibular trian-
gular flap can be easily moved to lingual, ensuring a
wound closure that is almost tension-free. The mesial
vestibular relieving incision, which is only adapted
coronally by a single suture, allows depletion of the
postoperative hematoma during masticatory move-
ments. On the first postoperative day, a present
hematoma is easy to relieve by spreading and compres-
sion. In this respect, we can see the advantage that the
release area has bone support.
This study has shown that the conventional sulcular flap
design has a nearly 6-times-higher risk of rupture of the
primary wound closure than the modified triangular flap.
The patients age has been described as one of the
factors influencing primary wound healing. Wound
healing up to age 25 years was supposed to be more
uncomplicated.
5
In our group of patients, primary
wound healing was not influenced by age.
Molars with complete bone coverage do not cause
bone loss distal to the adjacent molar, nor do they exert
a traumatic stimulus on the oral mucosain contrast
with impacted teeth, which lie directly underneath the
mucosa. In these cases, the covering mucosa often
displays chronic inflammation, with the impacted
molar having already caused loss of attachment of the
adjacent molar at the time of its removal. This seems to
explain the higher rate of dehiscences in the group of
not completely osseous impacted teeth.
It is obvious that longer-lasting and, thus, more
complicated surgery causes wound healing disorders,
but in our study the influence of the duration of the
surgery seemed to be less important than the flap design.
The group of smokers in this study is too small to
have statistical relevance. Nevertheless, it can be said
that the percentage of wound healing disorders was
higher in the smoking group, which corresponds to
results in the literature.
19
In conclusion, it can be said that the flap design
considerably influences primary wound healing after
lower third molar surgery. The modified triangular flap
design, when compared with the conventional sulcular
incision, definitely makes primary wound healing
easier. Factors such as the degree of impaction, the
duration of the surgery, and nicotine habits clearly have
less influence on primary wound healing.
REFERENCES
1. Ash MM, Costich ER, Hayward JR. A study of periodontal
hazards of third molars. Periodontol 1962;33:209-19.
2. Szmyd L. Impacted teeth. Dent Clin North Am 1971;15:299-
318.
3. Stephens RJ, App GR, Foreman DW. Periodontal evaluation of
two mucoperiosteal flaps used in removing impacted mandibular
third molars. J Oral Maxillofac Surg 1983;41:719-24.
4. Quee TA, Gosselin D, Millar EP, Stamm JW. Surgical removal
of the fully impacted mandibular third molar. The influence of
flap design and alveolar bone height on the periodontal status of
the second molar. J Periodontol 1985;56:625-30.
5. Kugelberg CF, Ahlstrm U, Ericson S, Hugoson A, Kvint S.
Periodontal healing after impacted lower third molar surgery in
adolescents and adults. A prospective study. Int J Oral
Maxillofac Surg 1991;20:18-24.
6. Sands T, Pynn BR, Nenniger S. Third molar surgery: current
concepts and controversies. Part 2. Oral Health 1993;83:19, 21-
2, 27-30.
ORAL SURGERY ORAL MEDICINE ORAL PATHOLOGY Jakse et al 11
Volume 93, Number 1
Fig 5. The relative risk ratio and 95% CI of dehiscences for
factors that might influence wound healing (ie, flap design,
level of retention, duration of the surgery, nicotine habits, and
patient age). Compared with the triangular flap, the envelope
flap has a relative risk of a dehiscence during primary wound
healing of 5.67, with a 95% CI from 1.852 to 12.336. This
result is highly statistically significant, whereas the factor
levels of retention, duration, and smoking habits seemed to
influence primary wound healingbut without statistical
significance.
7. Pajarola GF, Jaquiery C, Lambrecht JT, Sailer HF. Die
Entfernung unterer retinierter Weisheitszhne (II) Schweiz
Monatsschr Zahnmed 1994;104:1521-30.
8. Klatil L. Komplikationen bei der Entfernung von
Weisheitszhnen [doctoral thesis]. KF-University Graz; 1998.
9. Thoma KH. The management of malposed inferior third molars.
J Dent Res 1932;12:175-80.
10. Szmyd L, Hester WR. Crevicular depth of the second molar in
impacted third molar surgery. J Oral Surg Anesth Hosp Dent
Serv 1963;21:185-8.
11. Berwick WA. Alternative method of flap reflection. Br Dent J
1966;121:295-6.
12. Groves BJ, Moore JR. The periodontal implications of flap
design in lower third molar extractions. Dent Pract Dent Rec
1970;20:297-304.
13. Magnus WW, Castner DV, Hiatt WR. An alternative method of
flap reflection of mandibular third molars. Mil Med
1972;137:232-3.
14. Woolf RH, Malmquist JP, Wright WH. Third molar extractions:
periodontal implications of two flap designs. Gen Dent
1978;26:52-6.
15. Papassotiriou A. Parodontalbefunde nach Zahnfleischrandschnitt
zur Weisheitszahnentfernung. Zahnrztliche Praxis 1991;6:206-
11.
16. Norusis MJ. SPSS for Windows: Base system users guide,
Release 5.0. Chicago: SPSS Inc; 1992. p. 211.
17. Tavtigian R. The height of facial radicular alveolar crest
following apically positioned flap operations. J Periodontol
1970;41:412-8.
18. Motamedi MH. A technique to manage gingival complications
of third molar surgery. Oral Surg Oral Med Oral Pathol Oral
Radiol Endod 2000;90:140-3.
19. Silverstein P. Smoking and wound healing. Am J Med
1992;93(1A):S22-S24.
Reprint requests:
Norbert Jakse, MD, DDS
Department for Oral Surgery and Radiology
Dental School, Karl-Franzens University Graz
Auenbruggerplatz 12, 8036 Graz, Austria
norbert.jakse@uni-graz.at
12 Jakse et al ORAL SURGERY ORAL MEDICINE ORAL PATHOLOGY
January 2002
CALL FOR REVIEW ARTICLES
The January 1993 issue of Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology,
and Endodontics contained an Editorial by the Journals Editor in Chief, Larry J. Peterson, that
called for a Review Article to appear in each issue.
These Review Articles should be designed to review the current status of matters that are
important to the practitioner. These articles should contain current developments, changing
trends, as well as reaffirmation of current techniques and policies.
Please consider submitting your article to appear as a Review Article. Information for
authors appears in each issue of Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology,
and Endodontics.
We look forward to hearing from you.
S-ar putea să vă placă și
- WHO Vaccine Manual PDFDocument112 paginiWHO Vaccine Manual PDFRagel CorpsÎncă nu există evaluări
- Principles of The Alexander DisciplineDocument5 paginiPrinciples of The Alexander DisciplineSarah Fauzia SiregarÎncă nu există evaluări
- MARPE AbdAllah Bahaaa Ref NewDocument23 paginiMARPE AbdAllah Bahaaa Ref NewAya ElsayedÎncă nu există evaluări
- Rapid MaxillaryDocument24 paginiRapid MaxillaryDon George GeojanÎncă nu există evaluări
- Reffered PainDocument26 paginiReffered PainHappy Septianto SÎncă nu există evaluări
- Peat 1Document37 paginiPeat 1Denise Junio100% (4)
- Transverse Dimension Andlong-Term Stability Robert L Vanarsdall JRDocument10 paginiTransverse Dimension Andlong-Term Stability Robert L Vanarsdall JRMa Lyn GabayeronÎncă nu există evaluări
- Abo GradingDocument11 paginiAbo GradingSonu RajuÎncă nu există evaluări
- Tarrson Family Endowed Chair in PeriodonticsDocument54 paginiTarrson Family Endowed Chair in PeriodonticsAchyutSinhaÎncă nu există evaluări
- Space AnalysisDocument43 paginiSpace AnalysismarieÎncă nu există evaluări
- Case Study Severe Depression With Psychosis.: Submitted To:-Submitted ByDocument33 paginiCase Study Severe Depression With Psychosis.: Submitted To:-Submitted ByPallavi KharadeÎncă nu există evaluări
- The Orthodontics Effective RoleDocument31 paginiThe Orthodontics Effective RoleHamza BelhajÎncă nu există evaluări
- Indices / Orthodontic Courses by Indian Dental AcademyDocument77 paginiIndices / Orthodontic Courses by Indian Dental Academyindian dental academyÎncă nu există evaluări
- Arch ExpansionDocument32 paginiArch ExpansionMoola Bharath Reddy100% (5)
- Oxford GastroenterologyDocument673 paginiOxford Gastroenterologymymamym100% (1)
- Biomekanik Pergerakan Gigi Ortodonti: Dr. I.B.Narmada. DRG., SP - Ort (K)Document62 paginiBiomekanik Pergerakan Gigi Ortodonti: Dr. I.B.Narmada. DRG., SP - Ort (K)Aisah DirawidyaÎncă nu există evaluări
- Molares InclinadosDocument13 paginiMolares Inclinadosmaria jose peña rojas100% (1)
- Journal Club1 / Orthodontic Courses by Indian Dental AcademyDocument19 paginiJournal Club1 / Orthodontic Courses by Indian Dental Academyindian dental academyÎncă nu există evaluări
- Dental Management of the Pregnant PatientDe la EverandDental Management of the Pregnant PatientChristos A. SkouterisÎncă nu există evaluări
- Case Report Class III Orthodontic Camouflage: Is The "Ideal" Treatment Always The Best Option? A Documented Case ReportDocument7 paginiCase Report Class III Orthodontic Camouflage: Is The "Ideal" Treatment Always The Best Option? A Documented Case ReportDany PapuchoÎncă nu există evaluări
- Understanding Masticatory Function in Unilateral CrossbitesDe la EverandUnderstanding Masticatory Function in Unilateral CrossbitesÎncă nu există evaluări
- Healers Versus Stealers: How to Outsmart the Thief in Your Dental PracticeDe la EverandHealers Versus Stealers: How to Outsmart the Thief in Your Dental PracticeÎncă nu există evaluări
- Manual of Dental Practice 2014 Estonia: Council of European DentistsDocument10 paginiManual of Dental Practice 2014 Estonia: Council of European DentistsMohd GhausÎncă nu există evaluări
- N.DR - Gopal Maharjan BDS (Pakistan) PG Training (USA) Dental Department Shree Birendra HospitalDocument13 paginiN.DR - Gopal Maharjan BDS (Pakistan) PG Training (USA) Dental Department Shree Birendra HospitalAnil ShahÎncă nu există evaluări
- Iatrogenic Effects of Orthodontic TreatmentDocument29 paginiIatrogenic Effects of Orthodontic TreatmentKomal AsifÎncă nu există evaluări
- Indices PDFDocument10 paginiIndices PDFBhavikPatelÎncă nu există evaluări
- Early Treatment of Class III Malocclusion With Modified Tandem Traction Bow Appliance and A Brief Literature Review 2247 2452.1000644Document5 paginiEarly Treatment of Class III Malocclusion With Modified Tandem Traction Bow Appliance and A Brief Literature Review 2247 2452.1000644kinayungÎncă nu există evaluări
- Alveolar Distraction For ImplantsDocument17 paginiAlveolar Distraction For ImplantsPoornima SoujanyaÎncă nu există evaluări
- Miniscrew-Assisted Rapid Palatal Expansion: A Review of Recent ReportsDocument5 paginiMiniscrew-Assisted Rapid Palatal Expansion: A Review of Recent ReportsCynthia Alfaro100% (1)
- Review Article: Barry H. Grayson, Pradip R. ShetyeDocument7 paginiReview Article: Barry H. Grayson, Pradip R. ShetyeHARITHA H.PÎncă nu există evaluări
- Methods of Correction of Unilateral Posterior CrossbiteDocument36 paginiMethods of Correction of Unilateral Posterior CrossbiteSwathiLingannagariÎncă nu există evaluări
- Class III TTT OptionsDocument9 paginiClass III TTT OptionsMADAÎncă nu există evaluări
- Open Bite CaseDocument10 paginiOpen Bite CaseezfreshÎncă nu există evaluări
- PREPROSTHETIC SURGERY - RamonDocument49 paginiPREPROSTHETIC SURGERY - Ramonjamaica faith ramonÎncă nu există evaluări
- Comparisson Cephalometric PorionDocument5 paginiComparisson Cephalometric Porionmerc0581Încă nu există evaluări
- Moving The TeethDocument117 paginiMoving The TeethThirunavukkarasu Srinivasan100% (2)
- Three-Dimensional Evaluation of Dentofacial Transverse Widths in Adults With Different Sagittal Facial Patterns PDFDocument10 paginiThree-Dimensional Evaluation of Dentofacial Transverse Widths in Adults With Different Sagittal Facial Patterns PDFSoe San KyawÎncă nu există evaluări
- Pain ManagementDocument44 paginiPain ManagementSaherish FarhanÎncă nu există evaluări
- Goals of Orthodontic TreatmentDocument14 paginiGoals of Orthodontic TreatmentemanÎncă nu există evaluări
- Space AnalysisDocument8 paginiSpace AnalysisMohammed JaberÎncă nu există evaluări
- Critical Review of Cephalometric RadiographyDocument26 paginiCritical Review of Cephalometric RadiographyEki Ryan SetiowatiÎncă nu există evaluări
- Orthodontically Induced Inflammatory Root ResorptionDocument15 paginiOrthodontically Induced Inflammatory Root ResorptionmutansÎncă nu există evaluări
- Ghafari (1997) Emerging Paradigms in Orthodontics - An EssayDocument8 paginiGhafari (1997) Emerging Paradigms in Orthodontics - An EssayMaja Maja BułkaÎncă nu există evaluări
- Arch Expansion: Dr. Fatima Burney FCPS Part II ResidentDocument33 paginiArch Expansion: Dr. Fatima Burney FCPS Part II ResidentGareth BaleÎncă nu există evaluări
- 01 - Introduction To DentistryDocument18 pagini01 - Introduction To Dentistrymichal ben meronÎncă nu există evaluări
- Relapse of Anterior Crowding 3 and 2017 American Journal of Orthodontics AnDocument13 paginiRelapse of Anterior Crowding 3 and 2017 American Journal of Orthodontics Andruzair007Încă nu există evaluări
- MANAGEMENT OF VERTICAL MAXILLARY EXCESS WWWDocument24 paginiMANAGEMENT OF VERTICAL MAXILLARY EXCESS WWWsweetieÎncă nu există evaluări
- Early Alt-RAMEC and Facial Mask Protocol in Class III MalocclusionDocument9 paginiEarly Alt-RAMEC and Facial Mask Protocol in Class III MalocclusionNievecillaNeiraÎncă nu există evaluări
- CLP SeminarDocument125 paginiCLP SeminarNiyati VerulkarÎncă nu există evaluări
- Surgically Assisted Rapid Maxillary Expansion Combined With MaxillaryDocument21 paginiSurgically Assisted Rapid Maxillary Expansion Combined With MaxillaryKumar NiwalikarÎncă nu există evaluări
- The University Münster Model Surgery System For Orthognathic Surgery. Part I - The Idea BehindDocument6 paginiThe University Münster Model Surgery System For Orthognathic Surgery. Part I - The Idea BehindDr Mostafa FarahatÎncă nu există evaluări
- Royal London Space AnalysisDocument47 paginiRoyal London Space AnalysisYusra ShaukatÎncă nu există evaluări
- Practical Techniques For Achieving Improved Accuracy in Bracket PositioningDocument14 paginiPractical Techniques For Achieving Improved Accuracy in Bracket Positioninganon-976413Încă nu există evaluări
- Newer Orthodontic Archwires Imparting EfDocument244 paginiNewer Orthodontic Archwires Imparting EfSelvaArockiamÎncă nu există evaluări
- OPEN BITE 1 / Orthodontic Courses by Indian Dental AcademyDocument23 paginiOPEN BITE 1 / Orthodontic Courses by Indian Dental Academyindian dental academyÎncă nu există evaluări
- Pre-Natal and Post-Natal Development of Maxilla Part 4 / Orthodontic Courses by Indian Dental AcademyDocument76 paginiPre-Natal and Post-Natal Development of Maxilla Part 4 / Orthodontic Courses by Indian Dental Academyindian dental academyÎncă nu există evaluări
- Ceph HandoutDocument18 paginiCeph Handoutwaheguru13he13Încă nu există evaluări
- Orthognathic DR Shruthi PDFDocument54 paginiOrthognathic DR Shruthi PDFShruthee KÎncă nu există evaluări
- Comparison of Anterior Retraction and Anchorage Control BetweenDocument44 paginiComparison of Anterior Retraction and Anchorage Control BetweenAnushriya DuttaÎncă nu există evaluări
- AJODO-2013 Angelieri 144 5 759Document11 paginiAJODO-2013 Angelieri 144 5 759osama-alali100% (1)
- Fixed Orthodontic Appliances: A Practical GuideDe la EverandFixed Orthodontic Appliances: A Practical GuideEvaluare: 1 din 5 stele1/5 (1)
- Essential Tissue Healing of the Face and NeckDe la EverandEssential Tissue Healing of the Face and NeckEvaluare: 5 din 5 stele5/5 (2)
- Maxillary Acrylic Stabilization ApplianceDocument1 paginăMaxillary Acrylic Stabilization ApplianceMr-Ton DrgÎncă nu există evaluări
- 00f48d69 98Document1 pagină00f48d69 98Mr-Ton DrgÎncă nu există evaluări
- 2dbfa8b2 IIDocument1 pagină2dbfa8b2 IIMr-Ton DrgÎncă nu există evaluări
- 03cc8288 364Document1 pagină03cc8288 364Mr-Ton DrgÎncă nu există evaluări
- Platelet Rich Plasma Myth or RealityDocument3 paginiPlatelet Rich Plasma Myth or RealityKarol Yulissa0% (1)
- Fundamental Principles of The Comprehensive Approach: The Case For The Four - Part Comprehensive EvaluationDocument1 paginăFundamental Principles of The Comprehensive Approach: The Case For The Four - Part Comprehensive EvaluationMr-Ton DrgÎncă nu există evaluări
- Clinical Cases in Restorative & Reconstructive DentistryDocument1 paginăClinical Cases in Restorative & Reconstructive DentistryMr-Ton DrgÎncă nu există evaluări
- Price List Implant Biomet 3iDocument1 paginăPrice List Implant Biomet 3iMr-Ton DrgÎncă nu există evaluări
- BSSPD GuidelinesDocument46 paginiBSSPD GuidelinesMr-Ton DrgÎncă nu există evaluări
- Letters To The Editor: Int. J. Oral Maxillofac. Surg. 2012 41: 1030-1031 Available Online atDocument2 paginiLetters To The Editor: Int. J. Oral Maxillofac. Surg. 2012 41: 1030-1031 Available Online atMr-Ton DrgÎncă nu există evaluări
- 2f6480be 45Document1 pagină2f6480be 45Mr-Ton DrgÎncă nu există evaluări
- Compendium 1997 Sonick ECLMATDocument11 paginiCompendium 1997 Sonick ECLMATMr-Ton DrgÎncă nu există evaluări
- 1 s2.0 S0901502711013981 MainDocument9 pagini1 s2.0 S0901502711013981 MainMr-Ton DrgÎncă nu există evaluări
- Interventions For Replacing Missing Teeth: 1-Versus 2-Stage Implant Placement (Review)Document27 paginiInterventions For Replacing Missing Teeth: 1-Versus 2-Stage Implant Placement (Review)Mr-Ton DrgÎncă nu există evaluări
- CD 003878Document96 paginiCD 003878Mr-Ton DrgÎncă nu există evaluări
- Pharmacologic Considerations: CorticosteroidsDocument1 paginăPharmacologic Considerations: CorticosteroidsMr-Ton DrgÎncă nu există evaluări
- 4d293240-fd0a-4adb-a5d9-e7716a08924eDocument3 pagini4d293240-fd0a-4adb-a5d9-e7716a08924eMr-Ton DrgÎncă nu există evaluări
- The Effects On Inmediate Placement and Restoration of Dental ImplantsDocument7 paginiThe Effects On Inmediate Placement and Restoration of Dental ImplantsAkarantayr Curtis ObaldoÎncă nu există evaluări
- Interventions For Replacing Missing Teeth: Surgical Techniques For Placing Dental Implants (Review)Document4 paginiInterventions For Replacing Missing Teeth: Surgical Techniques For Placing Dental Implants (Review)Mr-Ton DrgÎncă nu există evaluări
- 1c27bb51 90Document1 pagină1c27bb51 90Mr-Ton DrgÎncă nu există evaluări
- BSSPD GuidelinesDocument46 paginiBSSPD GuidelinesMr-Ton DrgÎncă nu există evaluări
- Article Folder 1Document9 paginiArticle Folder 1Mr-Ton DrgÎncă nu există evaluări
- Advanced Drug Delivery Reviews: G. Pagni, D. Kaigler, G. Rasperini, G. Avila-Ortiz, R. Bartel, W.V. GiannobileDocument10 paginiAdvanced Drug Delivery Reviews: G. Pagni, D. Kaigler, G. Rasperini, G. Avila-Ortiz, R. Bartel, W.V. GiannobileMr-Ton DrgÎncă nu există evaluări
- Dental Implant ComplicationsDocument1 paginăDental Implant ComplicationsMr-Ton DrgÎncă nu există evaluări
- Take-Home Hints: Implant Complications Associated With Systemic Disorders and MedicationsDocument1 paginăTake-Home Hints: Implant Complications Associated With Systemic Disorders and MedicationsMr-Ton DrgÎncă nu există evaluări
- Dental Implant Complications: Alzheimer's DiseaseDocument1 paginăDental Implant Complications: Alzheimer's DiseaseMr-Ton DrgÎncă nu există evaluări
- Surgical KnotDocument99 paginiSurgical KnotmherbergÎncă nu există evaluări
- Mental Nerve Function After Inferior Alveolar Nerve Transposition For Placement of Dental ImplantsDocument5 paginiMental Nerve Function After Inferior Alveolar Nerve Transposition For Placement of Dental ImplantsMr-Ton DrgÎncă nu există evaluări
- DR Anton For AlDocument8 paginiDR Anton For AlMr-Ton DrgÎncă nu există evaluări
- Surgical Procedures in Partially EdentulousDocument18 paginiSurgical Procedures in Partially EdentulousEliza DNÎncă nu există evaluări
- Case Study Formate MSNDocument2 paginiCase Study Formate MSNLijoÎncă nu există evaluări
- RabdoDocument7 paginiRabdoErik Ulises Teolotitla RoslaesÎncă nu există evaluări
- Closing The Cancer Divide: A Blueprint For ActionDocument45 paginiClosing The Cancer Divide: A Blueprint For ActionPresentaciones_FKÎncă nu există evaluări
- Nursing DiagnosisDocument3 paginiNursing DiagnosislesternÎncă nu există evaluări
- Devoir de Synthèse N°2 2011 2012 (Lycée Ali Bourguiba Bembla)Document4 paginiDevoir de Synthèse N°2 2011 2012 (Lycée Ali Bourguiba Bembla)ferchichi halimaÎncă nu există evaluări
- Tetagam P: Human Tetanus Immunoglobulin IM 250 IUDocument25 paginiTetagam P: Human Tetanus Immunoglobulin IM 250 IUhamilton lowisÎncă nu există evaluări
- Seminar - Discussion 1Document3 paginiSeminar - Discussion 1api-373572658Încă nu există evaluări
- Neonatal HypotoniaDocument7 paginiNeonatal HypotoniaShirley KoehÎncă nu există evaluări
- Toxicity Review Natural ProductsDocument5 paginiToxicity Review Natural Productsamino12451Încă nu există evaluări
- Perioperative Nursing: Lecturer: Mr. Renato D. Lacanilao, RN, MANDocument27 paginiPerioperative Nursing: Lecturer: Mr. Renato D. Lacanilao, RN, MANJmarie Brillantes PopiocoÎncă nu există evaluări
- Consent To Surgery/Anaesthesia: Ilocos Sur Provincial Hospital-Gabriela SilangDocument1 paginăConsent To Surgery/Anaesthesia: Ilocos Sur Provincial Hospital-Gabriela SilangRyrey Abraham PacamanaÎncă nu există evaluări
- مختارات د.ومضة-1-1Document5 paginiمختارات د.ومضة-1-1Djdjjd SiisusÎncă nu există evaluări
- Failures in ImplantsDocument8 paginiFailures in ImplantsDr FarhatÎncă nu există evaluări
- International Journal of Surgery Open: Amir Forouzanfar, Jonathan Smith, Keith S. ChappleDocument3 paginiInternational Journal of Surgery Open: Amir Forouzanfar, Jonathan Smith, Keith S. ChappleSiti Fildzah NadhilahÎncă nu există evaluări
- Solution Manual For Fordneys Medical Insurance 15th Edition Linda SmithDocument24 paginiSolution Manual For Fordneys Medical Insurance 15th Edition Linda SmithSarahAlexanderrkcq100% (39)
- Laporan Persediaan 1sd30okt2023Document28 paginiLaporan Persediaan 1sd30okt2023ARIEF YUNIARDIÎncă nu există evaluări
- LeukocoriaDocument5 paginiLeukocoriabahaashakirÎncă nu există evaluări
- Fees and Charges - Summary From 1 July 2020 Version 1.0, June 2020Document51 paginiFees and Charges - Summary From 1 July 2020 Version 1.0, June 2020QualityMattersÎncă nu există evaluări
- Senior CapstoneDocument6 paginiSenior Capstoneapi-313278667Încă nu există evaluări
- HeartburnDocument76 paginiHeartburnRock ArtadiÎncă nu există evaluări
- Sitecore - Media Library - Files.3d Imaging - Shared.7701 3dbrochure UsDocument28 paginiSitecore - Media Library - Files.3d Imaging - Shared.7701 3dbrochure UsandiÎncă nu există evaluări
- Mechanical Therapy: by Nikola TeslaDocument2 paginiMechanical Therapy: by Nikola TeslaRommy RahmansyahÎncă nu există evaluări
- Danish Mask StudyDocument1 paginăDanish Mask StudyJuana AtkinsÎncă nu există evaluări
- Nursing Care Plan Guide: Subjective DataDocument1 paginăNursing Care Plan Guide: Subjective DataJan Oliver YaresÎncă nu există evaluări
- Guidance COVID-19Document5 paginiGuidance COVID-19hemkumar DahalÎncă nu există evaluări