Documente Academic
Documente Profesional
Documente Cultură
Gastrocnemius Soleus
Încărcat de
goldfishx0 evaluări0% au considerat acest document util (0 voturi)
127 vizualizări8 paginiThis document provides a review of equinus deformity, including the relevant anatomy and biomechanics. Equinus is defined as limited ankle dorsiflexion. The minimum dorsiflexion required for normal gait is 10 degrees, with 20 degrees of plantarflexion. The gastrocnemius and soleus muscles are identified as the primary cause of equinus deformity when shortened. Surgical techniques to correct equinus include gastrocnemius recession and tendo Achillis lengthening, with the appropriate procedure determined by the anatomical level of involvement.
Descriere originală:
Article
Drepturi de autor
© © All Rights Reserved
Formate disponibile
PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentThis document provides a review of equinus deformity, including the relevant anatomy and biomechanics. Equinus is defined as limited ankle dorsiflexion. The minimum dorsiflexion required for normal gait is 10 degrees, with 20 degrees of plantarflexion. The gastrocnemius and soleus muscles are identified as the primary cause of equinus deformity when shortened. Surgical techniques to correct equinus include gastrocnemius recession and tendo Achillis lengthening, with the appropriate procedure determined by the anatomical level of involvement.
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
127 vizualizări8 paginiGastrocnemius Soleus
Încărcat de
goldfishxThis document provides a review of equinus deformity, including the relevant anatomy and biomechanics. Equinus is defined as limited ankle dorsiflexion. The minimum dorsiflexion required for normal gait is 10 degrees, with 20 degrees of plantarflexion. The gastrocnemius and soleus muscles are identified as the primary cause of equinus deformity when shortened. Surgical techniques to correct equinus include gastrocnemius recession and tendo Achillis lengthening, with the appropriate procedure determined by the anatomical level of involvement.
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 8
18 January/February 2005 Vol 95 No 1 Journal of the American Podiatric Medical Association
Equinus deformity is defined as a limitation of dorsi-
flexion motion of the ankle joint. Although many au-
thors have attempted to specify the necessary degrees
of ankle dorsiflexion, normative values have been lim-
ited.
1, 2
Biomechanically, the maximum amount of
dorsiflexion in the stance phase of normal gait oc-
curs just before heel lift with the knee extended.
1
The minimum amount of ankle range of motion nec-
essary for normal gait is 10 of dorsiflexion and 20
of plantarflexion.
1-3
DiGiovanni et al
2
differentiated
gastrocnemius equinus from gastrocnemius soleus
equinus. Gastrocnemius equinus is defined as 5 or
less of ankle dorsiflexion with the knee in full exten-
sion, and gastrocnemius soleus equinus is defined as
10 or less of ankle dorsiflexion with the knee in full
extension or in 90 of flexion.
Equinus imparts a major deforming force on the
foot and is a causative factor in many foot and ankle
pathologic entities, including plantar fasciitis, pes
planus, hallux abducto valgus, Achilles tendinosis,
Charcots midfoot collapse, and diabetic ulcerations.
3
DiGiovanni et al
2
found either gastrocnemius or gas-
trocnemius soleus equinus in patients with a symp-
tomatic foot and ankle. In asymptomatic patients,
gastrocnemius and gastrocnemius soleus equinus are
not uncommon (33% and 17%, respectively).
4
Many types of equinus have been described: os-
seous equinus, pseudoequinus (plantarflexed fore-
foot without ankle equinus), gastrocnemius equinus,
gastrocnemius soleus equinus, and a combination of
types.
3
In addition, an ankle joint capsule contracture
can produce or contribute to any type of equinus.
5
We present a review of the anatomy, biomechan-
ics, and clinical assessment of equinus. A detailed
surgical technique for gastrocnemius soleus reces-
sion is outlined, and an anatomical guide for surgical
treatment is presented.
Anatomy
The gastrocnemius muscle has two heads (medial
and lateral) that originate from the posterior aspect
of the medial and lateral femoral condyles, the supra-
condylar ridge, and the posterior capsule of the knee
joint. The gastrocnemius heads expand to reach their
greatest size just proximal to the middle of the leg.
The medial head is typically larger and extends more
distally than the lateral head. The gastrocnemius
muscle fibers insert into an aponeurotic tendon that
forms along the anterior surface of the muscle. This
aponeurotic junction marks the division between the
proximal and middle thirds of the posterior leg.
6
The soleus muscle arises from the posterior sur-
face of the fibular shaft and head, from the posterior
proximal tibia at the soleal line, and from the middle
third of the medial border of the tibial shaft. In addi-
tion, a fibrous arch forms proximally between the
tibia and the fibula and gives rise to the soleus mus-
cle. This fibrous arch is the upper end of a central
aponeurotic tendon of origin that descends on the
Gastrocnemius Soleus Recession
A Simpler, More Limited Approach
Bradley M. Lamm, DPM*
Dror Paley, MD*
John E. Herzenberg, MD*
Multiple surgical procedures have been described for the correction of
equinus deformity. We present a review of the anatomy, biomechanics,
and clinical assessment of equinus. In addition, we provide a detailed
surgical technique for gastrocnemius soleus recession and introduce
an anatomical guide for surgical treatment. (J Am Podiatr Med Assoc
95(1): 18-25, 2005)
*Rubin Institute for Advanced Orthopedics, Sinai Hospi-
tal of Baltimore, Baltimore, MD.
Corresponding author: Bradley M. Lamm, DPM, Rubin
Institute for Advanced Orthopedics, Sinai Hospital of Balti-
more, 2401 W Belvedere Ave, Baltimore, MD 21215.
Journal of the American Podiatric Medical Association Vol 95 No 1 January/February 2005 19
anterior surface of the soleus muscle, protecting the
deep neurovascular bundle and giving rise to the
bulk of the muscle fibers. The soleus muscle is bi-
pennate, with the fibers directed in an inferior and
posterior direction, making the soleus muscle thicker
distally. The most distal soleus muscle fibers mark
the division between the middle and distal thirds of
the posterior leg.
6
In the distal third of the posterior leg, the gastroc-
nemius aponeurosis and the soleus tendon merge
and form the Achilles tendon, which inserts into the
posterior upper third of the posterior calcaneus. The
Achilles tendon is the largest and strongest tendon in
the body, measuring up to 2.5 cm in diameter.
6, 7
The
Achilles tendon fibers, from origin to insertion, spiral
from medial to lateral such that the gastrocnemius
fibers insert on the lateral aspect of the calcaneus
and the soleus fibers insert on the medial aspect of
the calcaneus.
6-8
The plantaris is a small muscle that arises from the
distal lateral femur and posterior knee joint capsule.
This small, flat muscle runs inferomedially between
the gastrocnemius and soleus muscles to the medial
edge of the Achilles tendon. The plantaris muscle in-
serts on the posteromedial calcaneus adjacent to the
Achilles tendon insertion. As in the gastrocnemius
muscle, the plantaris muscle flexes the knee and plan-
tarflexes the ankle. Compared with the gastrocne-
mius and soleus muscles, the plantaris muscle is
much weaker and smaller.
6
We defined anatomical levels that are simple to
identify topographically and proposed a surgical
treatment guide for each level. The posterior leg and
the triceps surae muscle (the gastrocnemius and so-
leus muscles) can be divided into five anatomical lev-
els. A surgical guide is presented for each specific
type of equinus correction in conjunction with these
anatomical levels. The proximal fifth of the leg is
level 5, which consists of the origin and the tendons
or the medial and lateral heads of the gastrocnemius
muscle. At level 5, a proximal gastrocnemius tenoto-
my can be performed. Level 4 begins with the gas-
trocnemius muscle and includes the medial and later-
al heads of the gastrocnemius muscle. At level 4, a
deep gastrocnemius or soleus recession (intermuscu-
lar lengthening) can be performed. Level 3 begins as
the gastrocnemius muscle becomes tendon and com-
prises the soleus muscle and the distal gastrocne-
mius tendon. The distal extent of level 3 is defined by
the aponeurotic tendon (combined gastrocnemius
and soleus tendon). At level 3, a distal gastrocnemius
tenotomy can be performed. Level 2 begins at the
gastrocnemius soleus aponeurotic tendon and ends
at the most distal extent of the soleus muscle. At
level 2, a gastrocnemius soleus recession can be per-
formed. The distal fifth of the leg is defined as level 1,
at which a tendo Achillis lengthening can be per-
formed. Level 1 consists of the rotating tendon fibers
of the triceps surae muscle that constitute the Achilles
tendon (Fig. 1).
Biomechanics
Ankle equinus is most noticeable during the mid-
stance phase of gait. By inducing a more rapid en-
trance and exit into and out of the midstance phase
of gait, equinus produces a reduced step length and
thus a slower walking velocity. Compensatory mech-
anisms for equinus deformity include forward torso
lean, pelvic rotation, hip flexion, knee hyperexten-
sion, and external rotation of the leg.
9
Equinus of the
ankle results in compensatory subtalar pronation,
thereby unlocking the midtarsal joint and producing
midtarsal joint pronation. This motion results in dor-
siflexion of the forefoot on the rearfoot. Pronation of
the subtalar and midtarsal joints then produces a hy-
Figure 1. The posterior leg can be divided into five
anatomical levels. Based on anatomical level and
clinical assessment, specific surgical procedures are
indicated. The location for superficial gastrocnemius
soleus recession is highlighted. GT, gastrocnemius
tenotomy; GSR, gastrocnemius soleus recession; TAL,
tendo Achillis lengthening.
Surgical
Procedure Eponym
Anatomical
Level
20 January/February 2005 Vol 95 No 1 Journal of the American Podiatric Medical Association
permobile first ray and a subsequent forefoot patho-
logic abnormality.
3
In static stance, the soleus and gastrocnemius
muscles are active postural stabilizers that help main-
tain balance. The gastrocnemius muscle is active in-
termittently when the knees flex but shows no activi-
ty when the knees are fully extended. The lateral
portion of the soleus muscle is the only muscle in the
leg that is active during bipedal postural stance.
5
The gastrocnemius, soleus, and plantaris muscles
are located in the superficial posterior compartment
of the leg, and they all cross the subtalar and ankle
joints. The soleus and plantaris muscles have been
described as two-joint muscles. Because the gastroc-
nemius muscle spans the knee, ankle, and subtalar
joints, it has been described as a three-joint muscle.
3
During the midstance and propulsive phases of
gait, the soleus and gastrocnemius muscles are active.
The gastrocnemius and soleus muscles plantarflex
the ankle joint and, because of the ankle joints
oblique axis, act to invert the rearfoot during plan-
tarflexion.
3
The gastrocnemius muscle acts on the
ankle joint only when the knee is flexed. During the
propulsive phase of gait, the knee is slightly flexed;
therefore, the gastrocnemius and soleus muscles act
on the ankle joint during propulsion. Gait analysis
has shown the importance of a minimum of 10 of
ankle dorsiflexion in the propulsive phase of gait to
allow for foot clearance.
1, 5
The soleus muscle acts in-
dependently of the knee position but serves as a sta-
bilizer of the tibia by preventing anterior translation
of the tibia at the knee joint when the foot is planted.
This is important in the anterior cruciate ligament
deficient knee.
10
Clinical Assessment
Equinus should be measured with the knee extended
and with the knee flexed. The amount of ankle dorsi-
flexion is measured using a goniometer. Measure-
ments can be obtained by determining the angle be-
tween the plantar aspect of the heel (medially or
laterally) and the tibia. When clinically assessing for
equinus, care must be taken to maintain the subtalar
joint in a neutral position and to measure ankle dor-
siflexion and not midfoot dorsiflexion (rocker-bot-
tom) or midfoot equinus (pseudoequinus). Osseous
and muscular equinus can be differentiated radio-
graphically in standing mortise lateral radiographs of
the foot and ankle in maximum dorsiflexion.
11
Os-
seous equinus may result from bony procurvatum of
the distal tibia or from osteophytes on the anterior lip
of the distal tibia or neck of the talus.
9
Once osseous equinus is ruled out, the Silfverskild
test is performed to differentiate gastrocnemius
equinus from other types of equinus.
12
The medial
and lateral heads of the gastrocnemius and plantaris
muscles originate from the femoral condyles proxi-
mal to the knee joint. Therefore, when the knee is
flexed, the gastrocnemius and plantaris muscles
relax. The generally accepted amount of normal
ankle dorsiflexion is approximately 10 with the knee
extended and 20 with the knee flexed (Fig. 2).
1-3, 13
Gastrocnemius equinus is indicated by the inability
of the ankle to dorsiflex normally with the knee ex-
tended but the ability of the ankle to dorsiflex more
than 10 with the knee flexed (Fig. 3). Gastrocnemius
soleus equinus is defined by the inability of the ankle
to dorsiflex beyond a neutral position with the knee
extended (it remains <0) or with the knee flexed (it
remains <0) (Fig. 4).
2, 3, 12
None of these tests would
differentiate a situation in which the soleus was tight
but the gastrocnemius was lax. However, it is diffi-
cult to imagine such a clinical situation.
Surgical Treatments
Surgical strategies to correct ankle equinus are based
on clinical evaluation. The Silfverskild test has been
the gold standard for determining whether a patient
has gastrocnemius or gastrocnemius soleus equinus.
Many techniques, therefore, have been developed to
treat positive (gastrocnemius recession) and nega-
tive (tendo Achillis lengthening) Silfverskild test re-
sults. The surgical procedure that is most appropri-
ate for the specific pathologic abnormality should be
selected. For example, lengthening of the Achilles
tendon should be avoided if the problem is limited to
a tight gastrocnemius muscle. In such a case, recess-
ing the gastrocnemius muscle will preserve soleus
muscle strength.
The techniques presented by Vulpius and Stoffel
in 1924
14
and by Strayer
15, 16
in the 1950s for triceps
surae muscle lengthening were described as being
performed in levels 2 and 3, respectively. These two
procedures are often confused. The Vulpius proce-
dure is a gastrocnemius soleus recession performed
at level 2. Vulpius made one or more chevron-shaped
cuts through the gastrocnemius tendon and incised
the deep tendon raphe of the soleus muscle. Baker
17
modified the Vulpius procedure by making a tongue-
shaped recession of the gastrocnemius soleus tendon.
Strayer
15, 16
described a gastrocnemius tenotomy at
level 3, just proximal to the gastrocnemius soleus
aponeurotic tendon. He separated these two muscles
to allow the gastrocnemius muscle to retract proximal-
ly and then sutured it in its new, more proximal loca-
Journal of the American Podiatric Medical Association Vol 95 No 1 January/February 2005 21
A B
Figure 2. Silfverskild test results show normal ankle dorsiflexion with the knee extended (A) and with the knee
flexed to 90 (B).
A B
Figure 3. Silfverskild test results show limited ankle dorsiflexion with knee extension (A) and improved ankle dor-
siflexion with knee flexion (90) (B). This is an example of pure gastrocnemius equinus, which would benefit from
isolated gastrocnemius recession or gastrocnemius soleus recession.
A B
Figure 4. Silfverskild test results show that ankle dorsiflexion greater than neutral (0) is not present with the
knee extended (A) or with the knee flexed to 90 (B). This is an example of gastrocnemius soleus equinus, which
would benefit from tendo Achillis lengthening or gastrocnemius soleus recession.
10 Dorsiflexion
20 Dorsiflexion
10 Dorsiflexion
20
Plantarflexion
20 Plantarflexion
20 Plantarflexion
20 Plantarflexion
Straight knee tightens
gastrocnemius muscle
Bent knee relaxes
gastrocnemius muscle,
allowing further dorsiflexion
Dorsiflexion
achieved with a
relaxed gastrocnemius
muscle
No improvement
in dorsiflexion despite
relaxing the
gastrocnemius muscle
Soleus muscle
limits dorsiflexion
Tight soleus muscle,
gastrocnemius muscle, or both?
Tight soleus muscle,
gastrocnemius muscle, or both?
Normal
dorsiflexion
Interpretation:
Soleus, normal
Gastrocnemius, normal
Diagnosis:
No equinus
Interpretation:
Soleus, normal
Gastrocnemius, tight
Diagnosis:
Gastrocnemius equinus
Recommendation:
Gastrocnemius recession
Gastrocnemius soleus
recession
Interpretation:
Soleus, tight
Gastrocnemius, tight
Diagnosis:
Gastrocnemius soleus
equinus
Recommendation:
Tendo Achillis
lengthening
Gastrocnemius soleus
recession
Limited
dorsiflexion
Limited
dorsiflexion
tion, calling this technique a gastrocnemius recession.
The advantage of the Vulpius technique over that
presented by Strayer is that the gastrocnemius soleus
recession includes intramuscular lengthening of the
soleus muscle. The Baumann procedure, which has
been described for cases of cerebral palsy, is a gas-
trocnemius and/or soleus recession performed at
level 4.
18, 19
At level 5, Silfverskild described a proxi-
mal gastrocnemius tenotomy. A tendo Achillis length-
ening at level 1 can be performed by percutaneous Z-
lengthening,
9
percutaneous triple hemisectioning,
20
or
open Z-lengthening.
21
22 January/February 2005 Vol 95 No 1 Journal of the American Podiatric Medical Association
Gastrocnemius Soleus Recession
Technique
We found that most children and adults present with
combined gastrocnemius soleus equinus. As an alter-
native to tendo Achillis lengthening, which weakens
the entire triceps surae muscle, we prefer gastrocne-
mius soleus recession, except in cases of very severe
contracture, for which maximal lengthening is need-
ed. Since 1996, the senior author (D.P.) has used this
modified Vulpius technique when performing gas-
trocnemius soleus recession.
The patient, under general anesthesia, is posi-
tioned supine, with a thigh tourniquet in place. After
exsanguination with elevation of the lower extremity
and inflation of the tourniquet, an assistant holds the
leg up at an angle of 45 from the table, with the ankle
placed in a neutral position. A 3-cm longitudinal mid-
line incision is made at the distal end of level 2 (Fig.
1). Careful dissection is then performed at that inter-
val to identify the sural nerve and lesser saphenous
vein (Fig. 5). These structures are retracted to either
side. The tendon sheath is identified, and a longitudi-
nal incision is made through it. The plantaris muscle
is identified and completely released. With the ankle
maintained in a neutral position, the gastrocnemius
tendon is transversely incised. The underlying soleus
tendon is then cut, stopping when the soleus muscle
fibers are seen. The soleus tendon extends farther
medially than laterally, covering the soleus muscle
fibers. It is important to retract one side at a time so
that the tendon can be cut under direct visualization
(Figs. 6 and 7). The ankle should then be maximally
dorsiflexed with the knee in full extension to separate
the cut tendons (recession). The Silfverskild test is
again performed to assess the remaining equinus de-
formity. If the equinus deformity is not completely
corrected, the soleus tendon median raphe is identi-
fied and cut. To cut this safely, the median raphe, or
central tendon portion of the soleus muscle, is dis-
sected from the muscle medially and laterally (Fig. 8).
Direct visualization of the median raphe is recom-
mended to avoid injury to the posterior tibial nerve
bundle. Using a Beaver blade (BD Ophthalmic Sys-
tems, Waltham, Massachusetts), the thick longitudi-
nal soleus raphe is released. The wound is then irri-
gated with normal saline. The sheath covering the
outer border of the tendon is closed if possible. The
skin incision is closed in two layers. A small gauze
pad and a transparent dressing (Tegaderm; 3M Health
Care, St Paul, Minnesota) are then applied.
Rehabilitation typically depends on the concomi-
tant procedures. In general, after undergoing this
type of recession, patients are protected in a weight-
bearing, removable, short-leg cast or boot for 3 weeks
and undergo early range-of-motion exercises. The pa-
tient should be encouraged to keep the knee extend-
ed with a knee immobilizer to maintain the maxi-
mum recession effect of the gastrocnemius muscle
obtained at surgery. Active physical therapy is start-
ed 3 weeks after surgery.
Discussion
We present a new technique of gastrocnemius soleus
recession. A surgical guide for each specific type of
equinus correction has been introduced in conjunc-
tion with the respective anatomical levels (Fig. 1).
When a positive Silfverskild test result is elicited, a
proximal gastrocnemius tenotomy (level 5, Silfver-
skild), a deep gastrocnemius recession (level 4,
Baumann), or a distal gastrocnemius tenotomy (level
3, Strayer) is recommended. When the Silfverskild
test result is negative, the recommended treatment is
either tendo Achillis lengthening (level 1)
9, 20, 21
or su-
perficial gastrocnemius soleus recession (level 2).
Our approach, like the Vulpius approach, is gas-
trocnemius soleus recession. Our technique differs,
however, in that the incision through the tendons is a
single transverse cut, not a single or multiple chevron-
Figure 5. Cross-sectional view of level 2. The broken
line represents the tendon portion of the gastrocne-
mius and soleus muscles and the median raphe of
the soleus muscle. Steps in performing gastrocne-
mius soleus recession are numbered sequentially.
Soleus
Posterior
tibial
nerve
Soleus
Sural nerve
Lesser
saphenous vein
1.
Vertical midline
skin incision
2.
Divide superficial
fascial sheath
3. Divide
gastrocnemius tendon
4. Divide
soleus tendon
5. Divide
median raphe
of soleus muscle
6. Divide
plantaris tendon
Journal of the American Podiatric Medical Association Vol 95 No 1 January/February 2005 23
type cuts. In addition, we use a minimally invasive
approach that is performed exclusively in level 2.
Differentiation between the need for tendo Achillis
lengthening and the need for gastrocnemius soleus
recession is based on the degree of the deformity and
the cause of the equinus. Large equinus contractures
typically require open tendo Achillis lengthening to
gain the needed amount of length and to determine
the appropriate length-tension ratio for the tendon.
Smaller amounts of equinus can be corrected through
percutaneous slide-type procedures, such as the
triple hemisection technique; however, slide-type
techniques render an unpredictable final length. Gas-
trocnemius soleus recession leaves some of the soleus
muscle strength undisturbed compared with tendo
Achillis lengthening, which weakens the entire soleus
muscle. Gastrocnemius soleus recession allows for
sequential lengthening and obviates the need for re-
suturing the cut tendons. After transverse release of
the gastrocnemius soleus tendon, the Silfverskild
test is conducted to reassess the deformity before re-
lease of the median raphe of the soleus muscle. This
clinical reassessment of equinus during the proce-
dure allows for more accurate correction. It is impor-
tant to remember that restriction of ankle motion can
be attributed to contracture of one muscle or a group
of muscles. A recession of the soleus muscle main-
tains muscle strength and is preferred to a tendo
Figure 6. After the midline vertical incision, vertical
division of the superficial fascia, and horizontal re-
lease of the gastrocnemius tendon, the soleus tendon
is released. Deep retraction allows for full release at
the more anterior edge of the tendon laterally.
Figure 8. Locate the median raphe (central tendon)
of the soleus muscle. Release of this tendon using a
blade or dissecting scissors achieves additional length-
ening.
Figure 7. The soleus tendon is also released hori-
zontally to the opposite edge (medially) of the tendon
using deep retraction.
Achillis lengthening, which causes maximum loss of
strength, especially if the tendon is overlengthened.
The advantage of performing gastrocnemius or
gastrocnemius soleus recession is that these proce-
dures preserve the magnitude of muscle strength be-
24 January/February 2005 Vol 95 No 1 Journal of the American Podiatric Medical Association
cause they are intramuscular lengthenings.
3, 22
Tendo
Achillis tendon lengthening has been shown to mark-
edly decrease the strength of the triceps surae mus-
cle because of partial or complete division of the ten-
don.
22
Delp and Zajac
22
found that lengthening the
soleus tendon by 1.2 cm or lengthening the gastroc-
nemius tendon by 1.5 cm reduces the respective
muscle force by 50%. Their results confirm the im-
portance of conservative lengthening of the tendo
Achillis to avoid plantarflexion weakness.
In static bipedal stance, the soleus is active and
thus important for balance. Patients who undergo
tendo Achillis lengthening may have decreased strength
in the soleus muscle during static stance, thereby im-
pairing imbalance. Therefore, the gastrocnemius so-
leus recession may be advantageous for patients with
diabetes mellitus with peripheral neuropathy, who
typically have diminished proprioception and lack of
balance after lengthening of the tendo Achillis. Patients
with diabetes often undergo tendo Achillis lengthen-
ing to reduce excessive pressure on the forefoot. Com-
plete disruption of a tendon will inhibit the stretch re-
flex, whereby sufficient impulses cannot be released
from the Golgi tendon organs and the spindle fibers
of the muscle to excite the motor neuron.
23
Theoreti-
cally, this muscular deficiency could create a static
and dynamic postural imbalance, especially in the al-
ready insensate patient with diabetes. Simmons et
al
24
studied patients with diabetic neuropathy and
loss of protective sensation as confirmed by a 10-g
monofilament. They found significantly reduced ac-
tive and passive ankle joint mobility compared with
control participants. These authors also theorized
that limited ankle joint mobility might contribute to a
decrease in postural stability.
Surgical decisions should be made systemically to
obtain optimal results. Osseous equinus should be
treated initially with a bone procedure and then
retested intraoperatively to assess the soft tissues.
After completion of each step of a procedure, the sur-
geon should repeat the Silfverskild test to reassess
the deformity. Long-standing deformities can also re-
sult in ankle joint capsule contracture, which may re-
quire capsulotomy or gradual distraction with exter-
nal fixation.
Conclusion
This article presents a new technique for gastrocne-
mius soleus recession and introduces an anatomical
guide for surgical treatment of equinus deformity. An
accurate clinical assessment and Silfverskild test,
coupled with an understanding of the anatomical lev-
els of the posterior leg, provide a specific guide for
the surgeon. Our gastrocnemius soleus recession, a
modified Vulpius procedure, is performed in level 2
as a simpler and more limited approach. Moreover,
our technique is an intermuscular lengthening of the
soleus, which limits the amount of triceps surae mus-
cle weakening.
References
1. ROOT ML, ORIEN WP, WEED JH: Normal and Abnormal
Function of the Foot, Clinical Biomechanics Corp, Los
Angeles, 1977.
2. DIGIOVANNI CW, KUO R, TEJWANI N, ET AL: Isolated gas-
trocnemius tightness. J Bone Joint Surg Am 84: 962,
2002.
3. DOWNEY MS, BANKS AS: Gastrocnemius recession in the
treatment of nonspastic ankle equinus: a retrospective
study. JAPMA 79: 159, 1989.
4. BRODERSEN A, PEDERSEN B, REIMERS J: Foot deformities
and relation to the length of leg muscles in Danish chil-
dren aged 3-17 years. Ugeskr Laeger 155: 3914, 1993.
5. PALEY D: Gait Considerations, in Principles of Defor-
mity Correction, 2nd Ed, p 717, Springer-Verlag, Berlin,
2003.
6. GRAY H: Grays Anatomy, 37th Ed, p 647, Churchill Liv-
ingstone, London, 1989.
7. CUMMINS EJ, ANSON BJ, CARR BW, ET AL: The structure
of the calcaneal tendon (of Achilles) in relation to or-
thopedic surgery: with additional observations on the
plantaris muscle. Surg Gynecol Obstet 83: 107, 1946.
8. VAN GILS CC, STEED RH, PAGE JC: Torsion of the human
Achilles tendon. J Foot Ankle Surg 35: 41, 1996.
9. PALEY D: Principles of Deformity Correction, 2nd Ed,
Springer-Verlag, Berlin, 2003.
10. SHERBONDY PS, QUEALE WS, MCFARLAND EG, ET AL: So-
leus and gastrocnemius muscle loading decreases an-
terior tibial translation in anterior cruciate ligament
intact and deficient knees. J Knee Surg 16: 152, 2003.
11. LAMM BM, PALEY D: Deformity correction planning for
foot, ankle, and lower limb. Clin Podiatr Med Surg 21:
305, 2004.
12. SILFVERSKILD N: Reduction of the uncrossed two-joint
muscles of the leg to one-joint muscles in spastic con-
ditions. Acta Chir Scand 56: 315, 1924.
13. DOWNEY MS: Ankle Equinus, in Comprehensive Textbook
of Foot Surgery, 2nd Ed, Vol 1, ed by ED McGlamry, AS
Banks, MS Downey, p 687, Williams & Wilkins, Balti-
more, 1992.
14. VULPIUS O, STOFFEL A: Orthopdische Operationslehre,
Verlag von Ferdinand Enke, Stuttgart, Germany, 1924.
15. STRAYER LM JR: Recession of the gastrocnemius: an op-
eration to relieve spastic contracture of the calf mus-
cles. J Bone Joint Surg Am 32: 671, 1950.
16. STRAYER LM JR: Gastrocnemius recession: five-year re-
port of cases. J Bone Joint Surg Am 40: 1019, 1958.
17. BAKER LD: A rational approach to the surgical needs of
the cerebral palsy patient. J Bone Joint Surg Am 38:
313, 1956.
18. BAUMANN JU, KOCH HG: Lengthening of the anterior
aponeurosis of the gastrocnemius muscle [in German].
Operat Orthop Traumatol 1: 254, 1989.
Journal of the American Podiatric Medical Association Vol 95 No 1 January/February 2005 25
19. SARAPH V, ZWICK EB, UITZ C, ET AL: The Baumann pro-
cedure for fixed contracture of the gastrosoleus in cere-
bral palsy: evaluation of function of the ankle after
multilevel surgery. J Bone Joint Surg Br 82: 535, 2000.
20. HOKE M: An operation for the correction of extremely
relaxed flat feet. J Bone Joint Surg 13: 773, 1931.
21. WHITE JW: Torsion of the Achilles tendon: its surgical
significance. Arch Surg 46: 784, 1943.
22. DELP SL, ZAJAC FE: Force- and moment-generating ca-
pacity of lower-extremity muscles before and after ten-
don lengthening. Clin Orthop 284: 247, 1995.
23. GANONG WF: Excitable Tissue: Muscle, in Review of
Medical Physiology, 16th Ed, p 56, Appleton & Lange,
East Norwalk, CT, 1993.
24. SIMMONS RW, RICHARDSON C, DEUTSCH K: Limited joint
mobility of the ankle in diabetic patients with cuta-
neous sensory deficit. Diabetes Res Clin Pract 37: 137,
1997.
S-ar putea să vă placă și
- Improving Ankle and Knee Joint Stability: Proprioceptive Balancefit Discs DrillsDe la EverandImproving Ankle and Knee Joint Stability: Proprioceptive Balancefit Discs DrillsÎncă nu există evaluări
- Anatomia Clinica KneeDocument17 paginiAnatomia Clinica KneeMauricio OjedaÎncă nu există evaluări
- Healthy Hips Handbook: Exercises for Treating and Preventing Common Hip Joint InjuriesDe la EverandHealthy Hips Handbook: Exercises for Treating and Preventing Common Hip Joint InjuriesÎncă nu există evaluări
- Anatomi AnkleDocument15 paginiAnatomi AnkleZera DirgantaraÎncă nu există evaluări
- Practices of Anorectal SurgeryDe la EverandPractices of Anorectal SurgeryDong Keun LeeÎncă nu există evaluări
- Ankle JointDocument6 paginiAnkle JointIfeanyichukwu OgbonnayaÎncă nu există evaluări
- Hamstring 12-23 2Document10 paginiHamstring 12-23 2Pótha JohannaÎncă nu există evaluări
- Chapter 24 - MSKDocument3 paginiChapter 24 - MSKannoja selvaÎncă nu există evaluări
- Genu Recurvatum SyndromDocument7 paginiGenu Recurvatum SyndromRoxana RascaÎncă nu există evaluări
- Anatomy of Hip JointDocument5 paginiAnatomy of Hip JointSneha ParveenÎncă nu există evaluări
- Joint of Lower LimbDocument8 paginiJoint of Lower LimbZaid AbdulqadirÎncă nu există evaluări
- Adjustable Hip OrthosisDocument33 paginiAdjustable Hip Orthosismanoremo88Încă nu există evaluări
- A Systematic Approach To Adult Hip PainDocument12 paginiA Systematic Approach To Adult Hip Pain69016Încă nu există evaluări
- Anatomy, Back, Scapula: Paul T. Cowan Matthew VaracalloDocument6 paginiAnatomy, Back, Scapula: Paul T. Cowan Matthew Varacalloaccounts 3 lifeÎncă nu există evaluări
- Biomechanics and Pathophysiology of Flat FootDocument12 paginiBiomechanics and Pathophysiology of Flat FootGeorge FernandoÎncă nu există evaluări
- DEN 015L - General Anatomy 1 Student'S Activity Sheet Dentistry / First YearDocument20 paginiDEN 015L - General Anatomy 1 Student'S Activity Sheet Dentistry / First YearMhdv Ndn McmÎncă nu există evaluări
- Anatomy of The Ankle and FootDocument13 paginiAnatomy of The Ankle and FootRichard MillerÎncă nu există evaluări
- Soleus - PhysiopediaDocument6 paginiSoleus - PhysiopediaVahid AtaeiÎncă nu există evaluări
- Ospe-Ll 16Document35 paginiOspe-Ll 16Muthu GuhaanÎncă nu există evaluări
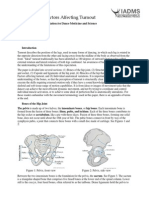
- Turnout For Dancers: Hip Anatomy and Factors Affecting TurnoutDocument7 paginiTurnout For Dancers: Hip Anatomy and Factors Affecting TurnoutsstavrosÎncă nu există evaluări
- Structures of The Hip Joint: Articulating SurfacesDocument7 paginiStructures of The Hip Joint: Articulating SurfacesChethan K NarayanÎncă nu există evaluări
- CASE JadiDocument32 paginiCASE JadiDian RasitawatiÎncă nu există evaluări
- Case Report OA HipDocument38 paginiCase Report OA HipDian RasitawatiÎncă nu există evaluări
- Pes Cavus and Pes PlanusDocument7 paginiPes Cavus and Pes PlanuspetcudanielÎncă nu există evaluări
- Sport Traumatology-III Knee Complex-7Document24 paginiSport Traumatology-III Knee Complex-7kamran aliÎncă nu există evaluări
- GRDA Intro Bony PelvisDocument5 paginiGRDA Intro Bony PelvisKingÎncă nu există evaluări
- Anatomy and PhysiologyDocument4 paginiAnatomy and PhysiologySarah CabalquintoÎncă nu există evaluări
- VSAQS Imp - Biom.Document8 paginiVSAQS Imp - Biom.Meenakshiputraeashwarprasad MacherlaÎncă nu există evaluări
- Anatomy, Shoulder and Upper Limb, Shoulder MusclesDocument12 paginiAnatomy, Shoulder and Upper Limb, Shoulder MusclesluizamgoÎncă nu există evaluări
- College of Human Sciences & Psychology Department: ClavicleDocument17 paginiCollege of Human Sciences & Psychology Department: ClavicleJohn Patrick LagmayÎncă nu există evaluări
- Naik, S. - Biomechanics of Knee ComplexDocument25 paginiNaik, S. - Biomechanics of Knee ComplexKyle Bois100% (4)
- Papers - Tibial PosteriorDocument10 paginiPapers - Tibial PosteriorGiancarlo Gardella MartínezÎncă nu există evaluări
- Anatomy, Bony Pelvis and Lower Limb, Hip - StatPearls - NCBI BookshelfDocument7 paginiAnatomy, Bony Pelvis and Lower Limb, Hip - StatPearls - NCBI BookshelfBBD BBDÎncă nu există evaluări
- Coxa SaltansDocument6 paginiCoxa SaltansignashyaÎncă nu există evaluări
- RCT PROJECT WORK FullDocument94 paginiRCT PROJECT WORK FulliquramasiddiqueÎncă nu există evaluări
- B1fe PDFDocument13 paginiB1fe PDFKiki Apdillah FeriÎncă nu există evaluări
- Any PDFDocument252 paginiAny PDFRaja VeerappanÎncă nu există evaluări
- Anatomy, Bony Pelvis and Lower Limb, Thigh Adductor Magnus Muscles - StatPearls - NCBI BookshelfDocument6 paginiAnatomy, Bony Pelvis and Lower Limb, Thigh Adductor Magnus Muscles - StatPearls - NCBI BookshelfDavid LorencÎncă nu există evaluări
- Presented By: DR Venkatesh V Moderator: DR Harish KDocument81 paginiPresented By: DR Venkatesh V Moderator: DR Harish KPankaj VatsaÎncă nu există evaluări
- Hip JointDocument40 paginiHip Jointafeefa.gbgÎncă nu există evaluări
- Joints of The Lower Limb DiagramsDocument39 paginiJoints of The Lower Limb Diagramssanullah123khan.13Încă nu există evaluări
- Bow Leg (Final) 3.9.20Document23 paginiBow Leg (Final) 3.9.20Gerald EthelieÎncă nu există evaluări
- CASE REPORT Hip DislocationDocument42 paginiCASE REPORT Hip DislocationvereriÎncă nu există evaluări
- Ultrasound Guided Interventional Procedures In.4Document13 paginiUltrasound Guided Interventional Procedures In.4andrew herringÎncă nu există evaluări
- Knee ExaminationDocument17 paginiKnee ExaminationHaider GhazanfarÎncă nu există evaluări
- Scapular Dyskinesia, The Forgotten Culprit of Shoulder Pain and How To RehabilitateDocument6 paginiScapular Dyskinesia, The Forgotten Culprit of Shoulder Pain and How To RehabilitateQuiroprácticaParaTodosÎncă nu există evaluări
- Rehabilitation Medicine Assistant - Range of Motion of Hip JointDocument3 paginiRehabilitation Medicine Assistant - Range of Motion of Hip Jointsnehapsra1Încă nu există evaluări
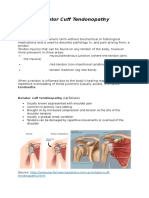
- PBL 1 - Rotator CuffDocument11 paginiPBL 1 - Rotator CuffEmmanuel Saka100% (1)
- Knee MechanicsDocument107 paginiKnee MechanicsAhmed El goharyÎncă nu există evaluări
- Anatomy of A Human BeingDocument6 paginiAnatomy of A Human BeingIshimaru ThorÎncă nu există evaluări
- Biomechanics of The Shoulder: Dennis L. Hart, Mpa, PT, Stephen W. Carmichael, PHDTDocument6 paginiBiomechanics of The Shoulder: Dennis L. Hart, Mpa, PT, Stephen W. Carmichael, PHDTPrem KumarÎncă nu există evaluări
- Anatomy and Bio Mechanics of The KneeDocument15 paginiAnatomy and Bio Mechanics of The KneeaimanshalpyÎncă nu există evaluări
- Foot and Ankle ArthrokinematicsDocument6 paginiFoot and Ankle ArthrokinematicsCraig StewartÎncă nu există evaluări
- Clinical Anatomy of The Knee PDFDocument7 paginiClinical Anatomy of The Knee PDFJuan Victor Briceno OrtizÎncă nu există evaluări
- Skeletal and Muscular SystemDocument18 paginiSkeletal and Muscular SystemkimberlynÎncă nu există evaluări
- Gadline PrsentationDocument12 paginiGadline PrsentationsumardiÎncă nu există evaluări
- Equinus ContracturesDocument7 paginiEquinus Contracturesa013bsy2496Încă nu există evaluări
- Anatomia de La RodillaDocument11 paginiAnatomia de La RodillaMilena Cardona RuizÎncă nu există evaluări
- DaSilva 2021Document12 paginiDaSilva 2021goldfishxÎncă nu există evaluări
- Appi Ajp 2017 16091037 ds001Document6 paginiAppi Ajp 2017 16091037 ds001goldfishxÎncă nu există evaluări
- ICCR Prostate Core Needle Biopsy Part 2 Specimen Level 1st Ed V1 1 BookmarkedDocument12 paginiICCR Prostate Core Needle Biopsy Part 2 Specimen Level 1st Ed V1 1 BookmarkedgoldfishxÎncă nu există evaluări
- Future Treatment Strategies For Menopausal Symptom ManagementDocument26 paginiFuture Treatment Strategies For Menopausal Symptom ManagementgoldfishxÎncă nu există evaluări
- ANC CalculationDocument2 paginiANC CalculationgoldfishxÎncă nu există evaluări
- My Man JeevesDocument112 paginiMy Man JeevesgoldfishxÎncă nu există evaluări
- Chapter 3: Ethical and Legal Issues: Multiple ChoiceDocument7 paginiChapter 3: Ethical and Legal Issues: Multiple ChoicegoldfishxÎncă nu există evaluări
- Enlightenment Art and MusicDocument9 paginiEnlightenment Art and MusicgoldfishxÎncă nu există evaluări
- Chapter 003 Geriatric Pharmacology: Multiple Choice QuestionsDocument15 paginiChapter 003 Geriatric Pharmacology: Multiple Choice QuestionsgoldfishxÎncă nu există evaluări
- Photogrammetric Facial Analysis of Attractive Korean EntertainersDocument8 paginiPhotogrammetric Facial Analysis of Attractive Korean EntertainersgoldfishxÎncă nu există evaluări
- Understanding Equinus: This Profound Causal Agent Is Commonly Overlooked and Under-TreatedDocument12 paginiUnderstanding Equinus: This Profound Causal Agent Is Commonly Overlooked and Under-TreatedCarl AzzopardiÎncă nu există evaluări
- Connective Tissue Injury in Calf Muscle Tears and Return To Play: MRI CorrelationDocument7 paginiConnective Tissue Injury in Calf Muscle Tears and Return To Play: MRI CorrelationMosiah Araújo SilvaÎncă nu există evaluări
- Muscle Manual From Active IQDocument81 paginiMuscle Manual From Active IQRicardoMontenegroMartinezÎncă nu există evaluări
- محاضرة تمزق عضلات الفخذ والكالف PDFDocument16 paginiمحاضرة تمزق عضلات الفخذ والكالف PDFAZOZ 19Încă nu există evaluări
- Muscle Manual: WWW - Premierglobal.Co - UkDocument94 paginiMuscle Manual: WWW - Premierglobal.Co - UkMilena RohenkohlÎncă nu există evaluări
- GastrocnemiusDocument3 paginiGastrocnemiustuhinsinghÎncă nu există evaluări
- 12 Weeks To Ticc and Joocy Legs PDFDocument32 pagini12 Weeks To Ticc and Joocy Legs PDFomar cepeda patiño100% (7)
- Lower Extremity KinesiologyDocument530 paginiLower Extremity KinesiologyDennis Nabor Muñoz, RN,RM89% (9)
- Gastrocnemius SoleusDocument8 paginiGastrocnemius SoleusgoldfishxÎncă nu există evaluări
- Repair of Neglected Achilles Tendon Ruptures JFAS 1994Document8 paginiRepair of Neglected Achilles Tendon Ruptures JFAS 1994Evan BowlesÎncă nu există evaluări
- ABFAS - Trauma Section Flashcards - QuizletDocument21 paginiABFAS - Trauma Section Flashcards - Quizletpjanu86Încă nu există evaluări
- Peak: The New Science of Athletic Performance That is Revolutionizing SportsDe la EverandPeak: The New Science of Athletic Performance That is Revolutionizing SportsEvaluare: 5 din 5 stele5/5 (97)
- The Yogi Code: Seven Universal Laws of Infinite SuccessDe la EverandThe Yogi Code: Seven Universal Laws of Infinite SuccessEvaluare: 4.5 din 5 stele4.5/5 (104)
- Relentless: From Good to Great to UnstoppableDe la EverandRelentless: From Good to Great to UnstoppableEvaluare: 5 din 5 stele5/5 (788)
- Aging Backwards: Reverse the Aging Process and Look 10 Years Younger in 30 Minutes a DayDe la EverandAging Backwards: Reverse the Aging Process and Look 10 Years Younger in 30 Minutes a DayÎncă nu există evaluări
- Chair Yoga: Sit, Stretch, and Strengthen Your Way to a Happier, Healthier YouDe la EverandChair Yoga: Sit, Stretch, and Strengthen Your Way to a Happier, Healthier YouEvaluare: 3.5 din 5 stele3.5/5 (5)
- Strong Is the New Beautiful: Embrace Your Natural Beauty, Eat Clean, and Harness Your PowerDe la EverandStrong Is the New Beautiful: Embrace Your Natural Beauty, Eat Clean, and Harness Your PowerEvaluare: 4 din 5 stele4/5 (5)
- Boundless: Upgrade Your Brain, Optimize Your Body & Defy AgingDe la EverandBoundless: Upgrade Your Brain, Optimize Your Body & Defy AgingEvaluare: 4.5 din 5 stele4.5/5 (67)
- Power of 10: The Once-A-Week Slow Motion Fitness RevolutionDe la EverandPower of 10: The Once-A-Week Slow Motion Fitness RevolutionEvaluare: 3.5 din 5 stele3.5/5 (11)
- Functional Training and Beyond: Building the Ultimate Superfunctional Body and MindDe la EverandFunctional Training and Beyond: Building the Ultimate Superfunctional Body and MindEvaluare: 4.5 din 5 stele4.5/5 (1)
- Yin Yoga: How to Enhance Your Modern Yoga Practice With Yin Yoga to Achieve an Optimal Mind-Body Connection: Yoga Mastery SeriesDe la EverandYin Yoga: How to Enhance Your Modern Yoga Practice With Yin Yoga to Achieve an Optimal Mind-Body Connection: Yoga Mastery SeriesÎncă nu există evaluări
- Pranayama: The Yoga Science of BreathingDe la EverandPranayama: The Yoga Science of BreathingEvaluare: 4.5 din 5 stele4.5/5 (8)
- Muscle for Life: Get Lean, Strong, and Healthy at Any Age!De la EverandMuscle for Life: Get Lean, Strong, and Healthy at Any Age!Evaluare: 4.5 din 5 stele4.5/5 (22)
- True Yoga: Practicing With the Yoga Sutras for Happiness & Spiritual FulfillmentDe la EverandTrue Yoga: Practicing With the Yoga Sutras for Happiness & Spiritual FulfillmentEvaluare: 4.5 din 5 stele4.5/5 (22)
- Not a Diet Book: Take Control. Gain Confidence. Change Your Life.De la EverandNot a Diet Book: Take Control. Gain Confidence. Change Your Life.Evaluare: 4.5 din 5 stele4.5/5 (124)
- Strength Training Over 40: The Only Weight Training Workout Book You Will Need to Maintain or Build Your Strength, Muscle Mass, Energy, Overall Fitness and Stay Healthy Without Living in the GymDe la EverandStrength Training Over 40: The Only Weight Training Workout Book You Will Need to Maintain or Build Your Strength, Muscle Mass, Energy, Overall Fitness and Stay Healthy Without Living in the GymEvaluare: 4 din 5 stele4/5 (6)
- Tibetan Yoga: Magical Movements of Body, Breath, and MindDe la EverandTibetan Yoga: Magical Movements of Body, Breath, and MindEvaluare: 5 din 5 stele5/5 (1)
- Roxane Gay & Everand Originals: Built for This: The Quiet Strength of PowerliftingDe la EverandRoxane Gay & Everand Originals: Built for This: The Quiet Strength of PowerliftingEvaluare: 4.5 din 5 stele4.5/5 (133)
- Fascial Training: With Easy Exercises To More Mobility And Less Pain (10 Minutes Fascia Workout For Home)De la EverandFascial Training: With Easy Exercises To More Mobility And Less Pain (10 Minutes Fascia Workout For Home)Evaluare: 5 din 5 stele5/5 (3)
- Which Comes First, Cardio or Weights?: Fitness Myths, Training Truths, and Other Surprising Discoveries from the Science of ExerciseDe la EverandWhich Comes First, Cardio or Weights?: Fitness Myths, Training Truths, and Other Surprising Discoveries from the Science of ExerciseEvaluare: 4 din 5 stele4/5 (47)
- Easy Strength: How to Get a Lot Stronger Than Your Competition-And Dominate in Your SportDe la EverandEasy Strength: How to Get a Lot Stronger Than Your Competition-And Dominate in Your SportEvaluare: 4.5 din 5 stele4.5/5 (17)
- Not a Diet Book: Take Control. Gain Confidence. Change Your Life.De la EverandNot a Diet Book: Take Control. Gain Confidence. Change Your Life.Evaluare: 3.5 din 5 stele3.5/5 (7)
- Wheels of Life: A User's Guide to the Chakra SystemDe la EverandWheels of Life: A User's Guide to the Chakra SystemEvaluare: 4.5 din 5 stele4.5/5 (34)
- Music For Healing: With Nature Sounds For Natural Healing Powers: Sounds Of Nature, Deep Sleep Music, Meditation, Relaxation, Healing MusicDe la EverandMusic For Healing: With Nature Sounds For Natural Healing Powers: Sounds Of Nature, Deep Sleep Music, Meditation, Relaxation, Healing MusicEvaluare: 5 din 5 stele5/5 (1)
- 5-Minute Yoga: A More Energetic, Focused, and Balanced You in Just 5 Minutes a DayDe la Everand5-Minute Yoga: A More Energetic, Focused, and Balanced You in Just 5 Minutes a DayEvaluare: 5 din 5 stele5/5 (2)
- Endure: Mind, Body, and the Curiously Elastic Limits of Human PerformanceDe la EverandEndure: Mind, Body, and the Curiously Elastic Limits of Human PerformanceEvaluare: 4.5 din 5 stele4.5/5 (237)
- Mind Your Body: 4 Weeks to a Leaner, Healthier LifeDe la EverandMind Your Body: 4 Weeks to a Leaner, Healthier LifeEvaluare: 4.5 din 5 stele4.5/5 (5)
- Calisthenics: Guide for Bodyweight Exercise, Build your Dream Body in 30 MinutesDe la EverandCalisthenics: Guide for Bodyweight Exercise, Build your Dream Body in 30 MinutesEvaluare: 3 din 5 stele3/5 (5)
- Somatic Exercises for Beginners: Transform Your Life in 30 Days with Personalized Exercises for Body and MindDe la EverandSomatic Exercises for Beginners: Transform Your Life in 30 Days with Personalized Exercises for Body and MindÎncă nu există evaluări