Documente Academic
Documente Profesional
Documente Cultură
Management of Neck in ORAL CANCER
Încărcat de
nandhinisankaran0 evaluări0% au considerat acest document util (0 voturi)
113 vizualizări8 paginimanagement of neck in oral cancer
Titlu original
management of neck in ORAL CANCER
Drepturi de autor
© © All Rights Reserved
Formate disponibile
PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentmanagement of neck in oral cancer
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
113 vizualizări8 paginiManagement of Neck in ORAL CANCER
Încărcat de
nandhinisankaranmanagement of neck in oral cancer
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 8
1
Surgical Neck Management in Head
and Neck Carcinoma
Chul-Ho Kim, MD. Ph.D
Level I : submental
submandibular(6)
Level II : upper jugular
Level III : Mid jugular
Level IV : lower jugular
Level V : posterior
Level VI : central neck
Level VII : upper mediastinal
IIb IIa
Levels of the Neck (1998, T. Robbins)
VI
Ib
Ia
III
IVb IVa
Va
Vb
VII
SAN
IJV
SCM
Radical Neck Dissection
( RND )
1. Spinal accessory nerve
2. Internal jugular vein
3. Sternocleidomastoid m.
Modified RND ( mRND )
Type I SAN
II SAN + IJV
III SAN + IJV + SCM
( = FND )
Classification of Neck Dissection
AAO-HNS(1991) Medinas modification(1989)
Radical ND Comprehensive neck dissection
Modifed RND(I, II, III) Radical ND
Selective ND Modified RND
Supraomohyoid Type I(CN XI)
Lateral Type II( + IJV)
Posterolateral Type III(+ SCM)
Anterior compartment Selective ND
Extended RND
Definition
All lymph nodes in Levels I-V
including spinal accessory nerve (SAN), SCM, and IJV
Indications
Extensive cervical involvement or matted lymph nodes
with gross extracapsular spread and invasion
into the SAN, IJV, or SCM
Radical Neck Dissection Modified Radical Neck Dissection (MRND)
Definition
Excision of same lymph node bearing regions as RND
with preservation of one or more non-lymphatic structures
(SAN, SCM, IJV)
Spared structure specifically named
MRND is analogous to the functional neck dissection
described by Bocca
2
Modified Radical Neck Dissection
Three types (Medina 1989) commonly referred to not
specifically named by committee.
Type I: Preservation of SAN
Type II: Preservation of SAN and IJV
Type III: Preservation of SAN, IJV, and SCM
( Functional neck dissection)
Modified Radical Neck Dissection
Rationale
Reduce postsurgical shoulder pain and shoulder dysfunction
Improve cosmetic outcome
Reduce likelihood of bilateral IJV resection
Contralateral neck involvement
MRND Type I
Indications
Clinically obvious lymph node metastases
SAN not involved by tumor
Intraoperative decision
Rationale
RND vs MRND Type I:
Actuarial 5-year survival and neck failure rates for RND (63%
and 12%) not statistically different compared to MRND I
(71% and 12%) (Andersen)
No difference in pattern of neck failure
MRND Type II
Indications
Rarely planned
Intraoperative tumor found adherent to the SCM, but
not IJV and SAN
MRND TYPE III
Rationale
Suarez (1963) necropsy and surgery specimens of larynx
and hypopharynx lymph nodes do not share the same
adventitia as adjacent BVs
Nodes not within muscular aponeurosis or glandular capsule
(submandibular gland)
Sharpe (1981) showed ) 0% involvement of the SCM in 98
RND specimens despite 73 have nodal metastases
Survival approximates MRND Type I assuming IJV, and
SCM not involved
CND : Anterior Compartment
Definition
En bloc removal of lymph structures in Level VI
Perithyroidal nodes
Pretracheal nodes
Precricoid nodes (Delphian)
Paratracheal nodes along recurrent nerves
Limits of the dissection are the hyoid bone, suprasternal
notch and carotid sheaths
CommandB
3
Boundaries
- hyoid
- suprasternal notch
- medial border of carotid sheath
Indications
Selected cases of thyroid
carcinoma
Parathyroid carcinoma
Subglottic carcinoma
Laryngeal carcinoma with
subglottic extension
CA of the cervical esophagus
CND: Anterior Compartment
Extended Neck Dissection
Definition
Any previous dissection which includes removal of one
or more additional lymph node groups and/or non-
lymphatic structures.
Usually performed with N+ necks in MRND or RND
when metastases invade structures usually preserved
Extended Neck Dissection
Indications
Carotid artery invasion
Other examples:
Resection of the hypoglossal nerve resection or digastric
muscle,
dissection of mediastinal nodes and central compartment
for subglottic involvement, and
removal of retropharyngeal lymph nodes for tumors
originating in the pharyngeal walls.
A. Preoperative considerations
1. Planning of operation
1) Thorough knowledge of patients history
2) Understanding of the extent of disease
3) Awareness of relevant laboratory and
radiologic data
4) Discussion with the patient about what to
expect and possible contingencies
; essential to a smooth course through the
operative and postoperative periods
2. Airway
1) Awake tracheotomy under local anesthesia in
compromised airway
2) Awake intubation in less tenuous airway
3) Tracheotomy
C Routine unilateral RND or bilateral MND
: not always necessary
C Bilateral RND
: protective tracheotomy should be
performed
3. Skin injection
- Best to inject the proposed skin incision with
epinephrine
- Most conveniently done with a mixture of
local anesthetics (Xylocaine)
- 10-15 minutes should be allowed to attain
maximum benefits
4. Skin marking
- methylene blue
- Gentian violet
- Tip of 23G needle punctures the skin edges
opposite one another
4
5. Location of tracheotomy or other incisions
- Incorporation or not
- entirely depends on the incision types used
- Any neck incisions used for previous biopsy
should be incorporated
6. Perioperative antibiotics
- If RND is included as part of an operation in
which upper aerodigestive tract is open
- Appropriate antibiotic coverage for G(+),
anaerobic and possibly G(-) bacteria
- In case of RND alone, no evidence that
antibiotics prophylaxis is advantageous
- Broad-spectrum antibiotics at least until the
drains are removed
B. Considerations in selection of incision
1.Provide appropriate exposure to underlying
compartment
- L/N groups targeted for removal
- the possibility of performing a bilateral neck
dissection
- Surgical exposure for removing cancer of the
primary site
B. Considerations in selection of incision
2. Minimize wound complication
- Protect the carotid artery
CNo long vertical segments directly over the
carotid
CNo trifurcation directly over the carotid
- Avoid devascularizing portions of any skin flaps
3.Optimize aesthetic results
- natual skin crease, curvilinear incision,
minimizing the use of T-shaped and/or Y-shaped
incision
C. Skin flap elevation
- Subplatysmal layer
- Traction and counter-traction
- Hemostasis
- Care to be in the proper surgical plane
superoposteriorly and at the midline where
platysma is absent
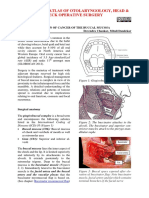
1. Superiorly up to inferior border of the mandible
* Preservation of marginal mandibular nerve
C Upward dissection of superficial layer of deep
cervical fascia off the capsule of submandibular gland
C Careful dissection and suspension by ligatures
placed on anterior facial vein
: best, especially in oral cavity primary, to remove
pre- and post-vascular facial lymph nodes
C Postero-superiorly, raise the flap superficial to the
aponeurosis over the parotid as in parotidectomy
5
2. Anteriorly to strap muscles and midline
3. Inferiorly to the level of clavicle
4. Posteriorly to the anterior border of trapezius
muscle
- best by dissection quite superficial to avoid the
vertical branch of transverse cervical vein
5. Secure the skin flaps by suturing either to the drapes
or to the skin
Exposure of Surgical Field
1. Superior dissection
1) Level Ia
C Fibrofatty tissues are
incised along the anterior belly
of contralateral digastric muscle
and swept inferoposteriorly
from central portion of
mylohyoid muscle
C Remove pre- & post-vascular facial lymph nodes
C Anterior belly of ipsilateral digastric muscle is cleaned,
leaving submental contents (Level Ia) attached to
submandibular triangle (Level Ib)
2) Level Ib
C SMG is elevated from floor of submandibular triangle,
facilitating identification of hypoglossal nerve
C On inferior traction, soft tissue separation from
inferior border of mandible
C Anterior traction of posterior border of mylohyoid muscle
C Identification of lingual nerve, submandibular ganglion, and
postganglionic parasympathetic fibers to the gland
2) Level Ib (contd)
C Ganglion is divided between clamps
Submandibular duct is divided and tied
C Identification, clamping, and division of facial artery by
posterior and downward traction of the tissues
Level II
Tail of parotid gland
C Posterior belly of digastric muscle is identified
C Division of parotid tail and control of posterior
facial vein
6
Level II
C Delineation of inferior
border of digastric m.
C Upward retraction of the
belly with Army-Navy
C Identification of upper
stump of IJV
C Cut the proximal end of
spinal accessory nerve
1) Division of SCM m.
CDelineation of anterior
border of trapezius muscle
from clavicle upward to its
junction with mastoid tip
CSCM muscle is divided
along the anterior border of
trapezius and is freed from
its mastoid insertion
Division of SCM muscle
1) Dissection of tissue (Level V)
2. Posterior dissection
C Four clamps placed on the posterior margin of neck contents
anterior to the border of trapezius for traction
C Sharp dissection of the tissue from the deep layer of deep
cervical fascia : allows preservation of posterior (motor)
branch of cervical plexus, thereby preserving innervation to
the levator scapulae, splenius capitis, and scalene muscles
Trapezius
Innervation
CN XI : 5 cmfrom clavicle
Surgical considerations
Posterior limit
of Level V neck dissection
Denervation results in
shoulder drop and winged
scapula
*
*
*
*
3. Inferior dissection: Level IV
1) Division of SCM muscle
C Sternal and clavicular heads divided while
placing upward traction on the belly
C Cautious incision by layers
- paying great attention to the carotid sheath
and its contents lying immediately deep to
the muscle
C Alternately, the muscle can be separated from
the underlying carotid sheath by gentle
dissection with a blunt Kelly clamp
2) Identification and opening of carotid sheath
C Soft tissue overlying sternothyroid muscle is
separated from posterior border of the muscle
C Medial traction of sternothyroid muscle
identification of carotid sheath
C Open the sheath with Metzenbaum scissors
7
C Four clamps to the lower aspect of IJV
(or 2 inferiorly and 1 superiorly)
Cut between middle two clamps
C Double ligation with 2-0 silk ties and 3-0 silk
suture ligatures or four 2-0 silk ties
Care must be taken not to saw through the
vein with these ties
4) Dissection of supraclavicular tissue (Levels IV & V)
CRetraction with sponge
and incision in sequential
layers after incision of
fascia superficial to
clavicle
CControl of EJV
CDivision of omohyoid m.
CExtend from IJV to
anterior border of
trapezius muscle
3) Internal jugular vein (IJV)
C Blunt dissection with blunt Kelly clamps
C Avoiding undue forces on IJV preventing
severe hemorrhage or air embolism
C Exposure of adequate length of IJV to allow
easy passage of the clamps
C Visual identification of vagus nerve and CCA
* Fascial carpet
CDissection down to deep
layer of deep cervical
fascia overlying phrenic
nerve, brachial plexus &
posterior branches of
cervical plexus
Continued cephalad
traction
CPreservation of this
fascia prevents injury to
the above structures
* Thoracic duct on
the left neck
If injured, clear
identification and ligation
needed to prevent
chylous fistula
1 Tissue pedicle in IJV
stump area between
phrenic and vagus nerves
should always be divided
between clamps and tied
Thoracic duct
8
C Upward and medially to the level of cervical plexus
C Division & ligation of anterior (sensory) branches of
cervical plexus : transition from level V to levels II, III, IV
C Posterior approach to the carotid sheath
- Separating IJV from vagus and carotid
- Care not to dissect deep to carotid
(cervical sympathetic trunk)
Completion of Levels II~V
Level II
-Roll the specimen forward, clear separation of
vagus nerve and carotids
(together with Levels III & IV)
-Identification of hypoglossal nerve above carotid
bifurcation - Control of veins
Venae commitantes nervi hypoglossi
Lingual vein
Veins draining pharyngeal plexus
-Division of ansa hypoglossi
3. Anterior dissection
- along the undersurface
of omohyoid
- Up to the level of hyoid
bone, at which point
anterior belly of
omohyoid is divided
F. Closure
C Meticulous hemostasis
C Wound irrigation with sterile saline
C Place suction drains through separate stab
incisions in the lower flap below clavicle,
considering last functioning hole of the catheter
C Secure the drains away from the carotid, cranial
nerves, and mucosal suture lines
C Closure of skin incisions in layers
Airtight closure of platysma with absorbable sutures
Placement of Suction Drain
S-ar putea să vă placă și
- Lyme Disease in Dogs-TestingDocument3 paginiLyme Disease in Dogs-TestingnandhinisankaranÎncă nu există evaluări
- 37 - Asterix and The Chariot Race PDFDocument48 pagini37 - Asterix and The Chariot Race PDFnandhinisankaranÎncă nu există evaluări
- Yamada2014 PDFDocument1 paginăYamada2014 PDFnandhinisankaranÎncă nu există evaluări
- Transfusion Guidelines HemDocument4 paginiTransfusion Guidelines HemnandhinisankaranÎncă nu există evaluări
- Submandibular Gland Excision PDFDocument7 paginiSubmandibular Gland Excision PDFnandhinisankaranÎncă nu există evaluări
- Submandibular Gland Excision PDFDocument7 paginiSubmandibular Gland Excision PDFnandhinisankaranÎncă nu există evaluări
- Advances in Dental Local Anesthesia Techniques and Devices - An UpdateDocument9 paginiAdvances in Dental Local Anesthesia Techniques and Devices - An UpdatenandhinisankaranÎncă nu există evaluări
- ZygofractDocument2 paginiZygofractnandhinisankaranÎncă nu există evaluări
- Cary - Blair MediumDocument2 paginiCary - Blair MediumnandhinisankaranÎncă nu există evaluări
- Natural History and Clinical Staging of HIV: Training For Medical Officers Day 2 Session 7Document25 paginiNatural History and Clinical Staging of HIV: Training For Medical Officers Day 2 Session 7nandhinisankaranÎncă nu există evaluări
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5795)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (588)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (400)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2259)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (74)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (121)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- Cancer of Oral CavityDocument27 paginiCancer of Oral CavityMihai AlexandruÎncă nu există evaluări
- Examination Methods in Plastic Surgery PDFDocument69 paginiExamination Methods in Plastic Surgery PDFSanÎncă nu există evaluări
- Parotid MassDocument9 paginiParotid MassAndre Eka Putra PrakosaÎncă nu există evaluări
- Surgical Resection of Cancer of The Buccal MucosaDocument21 paginiSurgical Resection of Cancer of The Buccal MucosapradeepÎncă nu există evaluări
- Icd 9 10 THTDocument34 paginiIcd 9 10 THTlistianiayuÎncă nu există evaluări
- Neck Dissection PPs PresentationDocument139 paginiNeck Dissection PPs PresentationDrMohmd ZidaanÎncă nu există evaluări
- Pearls and Pitfalls in Head and Neck Surgery - Claudio CerneaDocument225 paginiPearls and Pitfalls in Head and Neck Surgery - Claudio CerneaAlvaro rivero calleÎncă nu există evaluări
- Parotid Gland NeoplasmDocument107 paginiParotid Gland NeoplasmigorÎncă nu există evaluări
- M Sandamela Salivary Gland SandamelaDocument45 paginiM Sandamela Salivary Gland SandamelaRockson SamuelÎncă nu există evaluări
- Head and Neck Cancer GuidelinesDocument96 paginiHead and Neck Cancer GuidelinesTri KurniawanÎncă nu există evaluări
- Radical Neck DissectionDocument11 paginiRadical Neck DissectionHendry Johannes100% (1)
- Oncology CasesDocument96 paginiOncology CasesPrutha Vaidya100% (1)
- Tumors of The Head and NeckDocument5 paginiTumors of The Head and NeckMiguel CuevasÎncă nu există evaluări
- Ooi 150050Document7 paginiOoi 150050MelaNia Elonk ZamroniÎncă nu există evaluări
- List of Surgeries: AbdomenDocument35 paginiList of Surgeries: AbdomenSaurav SaikiaÎncă nu există evaluări
- Neck DissectionsDocument9 paginiNeck DissectionsMax FaxÎncă nu există evaluări
- Definition of Lymph Node Groups Neck DissectonDocument22 paginiDefinition of Lymph Node Groups Neck DissectonSundeep Sharma100% (3)
- Metastasis in Head and Neck Jochen A.werner, R. Kim DavisDocument237 paginiMetastasis in Head and Neck Jochen A.werner, R. Kim DavisChandramohan SettyÎncă nu există evaluări
- COSTAR Outlining GuidelinesDocument33 paginiCOSTAR Outlining GuidelinesYizhouZhaoÎncă nu există evaluări
- Bailey Reading Ch7 21-50 ArpanDocument61 paginiBailey Reading Ch7 21-50 ArpandeniadillaÎncă nu există evaluări
- Carcinoma Buccal Mucosa: Dr. Abhilash G JR-3Document47 paginiCarcinoma Buccal Mucosa: Dr. Abhilash G JR-3LingeshÎncă nu există evaluări
- Papillary Thyroid CancerDocument7 paginiPapillary Thyroid CancerLalaine RomeroÎncă nu există evaluări
- Lymph Node DissectionDocument17 paginiLymph Node Dissectionperdhana kusumaÎncă nu există evaluări
- SEER Lymph Node FieldsDocument9 paginiSEER Lymph Node FieldsNetradeep Narayansa DagduÎncă nu există evaluări
- Neck DissectionDocument43 paginiNeck DissectionMeilina Elin WardhaniÎncă nu există evaluări
- Neck DissectionDocument51 paginiNeck DissectionRakshith12Încă nu există evaluări
- Elective Neck Dissection in Tongue CancerDocument6 paginiElective Neck Dissection in Tongue CancerDiah HayustiningsihÎncă nu există evaluări
- Head and NeckDocument21 paginiHead and NeckUday PrabhuÎncă nu există evaluări
- Neckdissections 130421031843 Phpapp02Document62 paginiNeckdissections 130421031843 Phpapp02azizÎncă nu există evaluări
- CAP Protocol-2016 Thyroid - HighlightedDocument8 paginiCAP Protocol-2016 Thyroid - Highlightedpath2016Încă nu există evaluări