Documente Academic
Documente Profesional
Documente Cultură
The Cardiovascular System
Încărcat de
SarahSalvan0 evaluări0% au considerat acest document util (0 voturi)
81 vizualizări7 paginiThe Cardiovascular System
Drepturi de autor
© © All Rights Reserved
Formate disponibile
DOCX, PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentThe Cardiovascular System
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca DOCX, PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
81 vizualizări7 paginiThe Cardiovascular System
Încărcat de
SarahSalvanThe Cardiovascular System
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca DOCX, PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 7
The Cardiovascular System
The Cardiovascular System
This system is composed of the heart and the blood vessels
The main functions of this system are:
to transport oxygen, hormones and nutrients to the tissues
and to transport waste products to the lungs and kidneys for excretion
The Gross Anatomy of the Heart
The heart is located within the thorax behind the sternum in the compartment called MEDIASTINUM
The heart is commonly described as the size of a clenched fist
The shape is conical, with a base and an apex
The base is directed upward
The apex is directed downward to the left at the level of the 5
th
ICS LMCL
Heart Surface
ANTERIOR SURFACE
Right ventricle
POSTERIOR SURFACE
Left ventricle
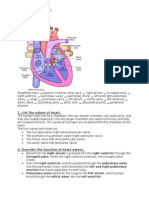
The Heart: Anatomy
The heart has four chambers
The Right Atrium
The Right Ventricle
The Left Atrium
The Left Ventricle
The Valves of the Heart
Valve Type Name Location
Atrioventricular Tricuspid
Mitral (Bicuspid)
Separates right atrium and right
ventricle
Separates left atrium and left
ventricle
Semilunar Pulmonic
Aortic
Between right ventricle and
pulmonary artery
Between left ventricle and aorta
The blood supply of the heart:
The coronary arteries are the blood supply
There are two main coronary arteries- the right coronary artery and the left coronary artery
The venous drainage of the heart is the coronary sinus; the anterior cardiac vein and the
smallest cardiac vein
Venous Drainage
Coronary sinus will collect all the venous blood from the heart into the RIGHT atrium
The anterior cardiac vein drains NOT into the coronary sinus but DIRECTLY into the right atrium
Cardiovascular Assessment
Cardiac History
Interview
Focused assessment
Health History
During the health history, the nurse should assess for significant past diseases and recent
illness
Family history may highlight risk factors
Obtain description of present illness and the chief complaint
Chest pain, edema, etc.
Assess risk factors
Physical Examination
Vital signs- BP, PP
Inspection of the skin
Inspection of the thorax
Palpation of the PMI, pulses
Auscultation of the heart sounds
Inspection
Palpation of the apical pulse and PMI at the 5
th
intercostal space, left midclavicular line
Auscultation
o For the heart sounds (S1, S2, S3, and S4)
S1 is due to the closure of the atrioventricular valves lub
S2 is due to the closure of the semilunar valves dub
S3 is due to the rushing of blood through the atrioventricular opening
S4 is due to contraction of the atrium
o For the heart valves
Tricuspid Valve
Mitral Valve
Pulmonic Valve
Aortic Valve
Surface Anatomy Auscultation
Tricuspid Valve
lies behind right half of the
sternum; opposite the 4
th
ICS
LEFT half of the lower end of the
body of the sternum (4
th
ICS)
Mitral Valve
lies behind the left half of the
sternum; opposite the 4
th
costal
cartilage
Apex beat (5
th
ICS LMCL)
Pulmonary Valve
Lies behind the medial end of the
3
rd
left costal cartilage & the
adjoining part of the sternum
Medial end of the 2
nd
left ICS
Aortic Valve
Behind left half of sternum;
opposite 3
rd
ICS
Medial end of the 2
nd
right ICS
Laboratory and diagnostic studies
CBC
Lipid profile
arteriography
Cardiac enzymes
CXR
ECG
Holter monitoring
Exercise ECG
The Normal Cardiovascular Pattern
Factors that identify the normal function of the heart
The heart rate - the normal heart rate varies on the average of 60 to 100 beats per minute
This is reflected by the pulses determined by palpating them in areas of the body.
The heart rate is highest in the newborn and decreases with age.
Blood pressure - the force with which the blood is pushed through the arterial system
Normal BP also varies with age. The adult average is 120/80 mmHg
It varies during the day, being highest during late afternoon.
Skin temperature and skin color
A person with good circulatory status is warm, with fairly uniform skin temperature.
Skin color can reflect the level of blood oxygenation and adequacy of blood flow.
Urine output
Sensorium or Level of consciousness
Other indicators:
Absence of pain in the chest
Normal urine output of more than 30 ml/hour
Normal cognitive function
Age - the rapid metabolic rate of the newborns demands tremendous blood flow to the developing
tissues.
Heart rate is considerably faster in the young.
In old age, the vascular system has naturally narrowed and stiffened, thus BP somewhat
increases.
Activity and Exercise
Increased metabolic demands from the exercising muscles will force the heart to beat faster.
The increased temperature causes vasodilatation increasing local blood flow.
Gender heart rate and BP vary slightly among men and women
Menopause women however have comparable increase in BP
Body Position
Blood tends to pool in the lower gravity-dependent extremities.
Temperature
When body temperature begins to rise, the autonomic system signals the peripheral arterioles
to open wide (vasodilatation) to allow heat loss.
When the body is exposed to cold, the opposite happens peripheral arterioles become
narrow (vasoconstriction)
Lifestyle and Habits
Smoking increases heart rate and BP
Common Altered Cardiac Functions
Decreased Pumping ability of the heart (decreased cardiac output) - a healthy heart is able to create
tremendous pressure and eject blood through the arteries to the lungs and body tissues.
Decreased pumping action can be the result of conduction problems termed as cardiac
arrhythmias.
Another cause of pump failure is valvular dysfunction. The valves which guard the chambers
may be damaged by infection, trauma or inflammation.
Muscle damage such as in myocardial infarction can weaken the pump action of the heart.
Altered blood flow (Impaired tissue perfusion) - blood vessels control the amount of blood entering
the heart and tissues.
Obstruction and narrowing can greatly affect tissue oxygenation.
Capillary dysfunction (when subjected to inflammatory mediators)
Venous pooling (collection of blood in the venous system caused commonly be venous valve
incompetence).
Signs of impaired peripheral circulation can be: decreased peripheral pulses, pale skin color,
cool extremities and decreased hair distribution.
Altered blood composition (Blood alterations) - alteration in RBC, plasma or circulating volume can
affect the tissue oxygenation.
Anemia can lead to inadequate oxygenation of body tissues leading to hypoxia.
Signs of anemia may include chronic fatigue, pallor, shortness of breath and hypotension.
Bleeding, burns, dehydration can all lead to deficit in blood volume
The Nursing Process Applied in Oxygenation: Cardiac Function
Assessment
To formulate accurate nursing care plan, the nurse must conduct an assessment of the CVS status.
This may include gathering of subjective data, objective data (through physical examination) and
laboratory data.
Nursing History
o Information obtained by the nurse often provides the basis for interventions.
o The nurse must elicit from the history the risk factors present, the functional pattern of
the patient before consultation, the events that lead to the occurrence of the
manifestations and the abnormal pattern of cardiovascular functions.
Physical Examination
o During inspection, the nurse observes the general behavior, sensorium, and appearance.
o The nurse must inspect the skin for color changes, edema, abnormal pulsations,
varicosities and nail clubbing
o Palpation involves checking for skin temperature, capillary refill time (normally is less than
3 seconds), pulses (either apical or peripheral).
o Auscultation involves the use of a stethoscope to hear for the different heart sounds.
Blood pressure is also taken with the aid of the apparatus and stethoscope.
Diagnostic Tests
o CBC can determine the information about the blood components. The hemoglobin
reflects the oxygen carrying capacity of the blood
o Cardiac Enzymes are released by DAMAGED cardiac cells and may indicate tissue damage
as in myocardial infarction.
o Serum electrolytes can directly affect the heart functions. Imbalances may cause
arrhythmias.
o ECG records the electrical impulse conduction of the heart in the resting patient. The
treadmill test involves checking the ECG of a patient subjected to exercise.
o Echocardiogram is simply the ultrasound of the heart
o The Nursing Process in Cardiac Care
Nursing Diagnosis
Altered tissue perfusion (Renal, Cerebral,
Cardiopulmonary, GI and Peripheral)
Decreased Cardiac Output
Activity Intolerance
Fluid volume excess
Fluid volume deficit
Planning (Goals)
Patient will demonstrate adequate knowledge concerning cardiovascular dysfunction
Patient will maintain adequate cardiac output
Patient will demonstrate adequate tissue perfusion with adequate oxygenation of body tissues
Patient will cope effectively with resulting changes in self-concept and lifestyle.
Implementation
1. Assess the cardio-pulmonary status
VS, BP, Cardiac assessment
2. Enhance cardiac output
Establish IV line to administer fluids
3. Promote CARDIOVASCULAR health and function
The nurse can employ health teaching strategies by presenting information concerning risk
factors, availability of healthy lifestyle programs like fitness clubs.
The nurse can employ various therapeutic interventions that will address specific problems
Examples of Nursing Measures
Nursing
Diagnosis
Interventions
Activity
intolerance
Monitor TPR and BP
Space activities in the day
Permit rest period before activity
Limit activity 1 hour before meals
Teach energy conservation measures like bed rest
Edema
Instruct patient to avoid constricting garments
Instruct to elevate edematous areas
Instruct patient to avoid dependent positions
Teach patient to prepare low sodium meals
Apply anti-embolic stockings
Pain
Instruct patient to stop activity when pain occurs
Administer nitroglycerin for angina
Pace activities within patients limits
Instruct patient to avoid cold temperatures and smoking
Instruct to report unrelieved pain immediately
4. Energy Conservation
The patient should be warned against Valsalva maneuver which can cause sudden increase in
blood pressure but simultaneously preventing venous return.
The most important energy conserving activity is REST
Regular rest periods should be provided. Activities should be spaced to avoid fatigue.
5. Administer medications as ordered
Administration of meds is an important nursing function
The nurse is also responsible for assessing the effects of medications and for potential
complications
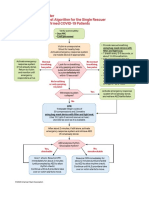
6. Perform CPR as needed.
CPR is a combination of oral resuscitation which supplies oxygen to the lungs and external
cardiac massage which is intended to re-establish cardiac functions.
The three cardinal signs of cardiac arrest that the nurse must assess are Apnea, Absence of
carotid or femoral pulses and dilated pupils.
Respiratory Arrest is the cessation of breathing. It often occurs because of blocked airway.
7. Promote gas exchange
Administer O2
Position client in SEMI-Fowlers
Encourage coughing and deep breathing exercises
8. Promote client comfort
Assess the clients description of pain and chest discomfort
Administer medication as prescribed
Morphine for MI
Nitroglycerine for Angina
Diuretics to relieve congestion (CHF)
9. Prevent infection
Monitor skin integrity of lower extremities
Assess skin site for edema, redness and warmth
Monitor for fever
Change position frequently
10. Minimize patient anxiety
Encourage verbalization of feelings, fears and concerns
Answer client questions. Provide information about procedures and medications
Evaluation
Patients with cardiovascular dysfunction show widely variable rates of progress.
Specific goals for these patients must be individualized.
In Summary:
The cardiovascular system transports gases in the blood to and from the tissues and facilitates the
diffusion of gases between the capillaries and body tissues
The heart and blood vessels make up the cardiovascular system that together with blood is the major
system for transporting oxygen and nutrients to the tissues and wastes products away from the tissues
for elimination
The right side of the heart receives the unoxygenated blood while the left side of the heart receives
oxygenated blood
The coronary arteries supply the oxygen and nutrients to the heart muscles
The cardiac cycle is made up of systole / contraction and diastole/ relaxation
Cardiac output depends on the stroke volume or the amount of blood ejected per heart beat
The systemic vessels carry blood to the tissues through the system of arteries, and return it to the
heart via a system of veins
The blood pressure is determined by the cardiac output and the peripheral vascular resistance. It rises
gradually from birth to adult range in the adolescent period
There are many factors that affect cardiovascular functions; atherosclerosis causes fatty deposition
within the arterioles/arteries
Decreased cardiac output, impaired tissue perfusion, and disorders affecting the blood are the major
cardiovascular problems that may affect oxygenation.
The most common cause of impaired blood flow is atherosclerosis.
Nursing interventions to promote circulation include using anti-embolic stockings, sequential
compression devices and administration of cardiac medications
Cardiopulmonary resuscitation (CPR) is used during cardiopulmonary arrest.
The Heart
Microscopic Anatomy
The heart has three layers (The epicardium, myocardium, and endocardium)
The heart is covered by the pericardium with a parietal and visceral layers
The pericardial sac is a potential space in between the two pericardial layers with a minimal (15 cc)
fluid
The Layers of the Heart Wall
Epicardium
(Visceral Pericardium)
Essential layer of the heart
Coronary arteries are found in this layer
Myocardium
Middle and thickest layer of the heart
Responsible for contraction of the heart
Endocardium
Innermost layer of the heart
Lines the inside of the myocardium
Covers the heart valves
Myocardial Cell Types
Kind of Cardiac Cells Where Found Primary Function Primary Property
Myocardial cells Myocardium Contraction and relaxation Contractility
Specialized cells of the
electrical conduction system
Electrical conduction
system
Generation and conduction of
electrical impulses
Automaticity and
conductivity
Characteristics of cardiac cells: Physiology
Automaticity
Excitability
Ability to INITIATE an electrical impulse
Ability to RESPOND to the electric impulse
Conductivity
Contractility
Ability of the cardiac cells to TRANSMIT the impulse to other cells
Ability of the cardiac cells to CONTRACT or shorten in response to
electric stimulus
Physiology
The Conducting System
The conducting system of the heart is a group of specialized heart cells that functions to
conduct electrical impulses independent of any nerve supply
The parts of the conducting system of the heart are:
o The SA (sino-atrial) node
o The AV (atrio-ventricular) node
o The Bundle of His with its right and left bundle
o The Purkinje fibers
The Cardiac Cycle
Refers to the repetitive pumping process that begins with the onset of cardiac muscle
contractions and ends with the beginning of the next contractions.
The cardiac cycle consists of the contraction phase and the relaxation phase in each heartbeat
The SYSTOLE is the contraction phase
The DIASTOLE is the relaxation phase
The Cardiac Output and Blood Pressure (Regulation of Heart Function)
The amount of blood the heart pumps out in each beat is called the STROKE VOLUME
CARDIAC OUTPUT(CO) Vol. of blood pumped by either ventricle of the heart each minute
CO = SV x HR (the number of times contracts each minute
CO at rest = 70ml/beat x 72bpm
= 5040 ml/min or 5L/min
(Intrinsic Regulation) *the force of contraction produced by cardiac muscle is related to the
degree of stretch of cardiac muscle fibers
Venous Return - is the amount of blood that returns to the heart
The Preload and Afterload
The PRELOAD is the degree of stretching of the ventricular walls when it is filled-up with blood
The AFTERLOAD is the resistance to which the heart must pump to eject the blood
The Starlings law of the heart - relationship between preload and stroke volume
Increased Venous Return - heart fills to a greater volume and stretch = increased preload
Cardiac muscle fibers contract with greater force = increased volume of blood to be ejected
from the heart = increased stroke volume
Increased venous return increased preload increased CO
Extrinsic (Blood Pressure) Regulation
Nervous Control
Central (Pons and Medulla)
Sympathetic nervous system - increases heart rate
Parasympathetic nervous system (Vagus) - decreases heart rate
Reflex Control
Baroreceptors - receptors sensitive to stretch located in the carotid sinuses and aortic arch
stretch reflex increase in heart rate BP
stretch reflex decrease in heart rate BP
Hormonal Control
Epinephrine vasoconstriction(skin and viscera) increased resistance increased BP
- epinephrine causes vasodilation of blood vessels in skeletal muscles & cardiac muscles
ADH water reabsorption Blood volume increased BP
Angiotensinogen
blood
A1
lung
Angiotensin 2
ANF increase sodium excretion increased urine decreased blood volume
decreased BP
Vascular System
Anatomy
This consists of the artery, vein and capillary together with the lymphatic vessels
The ARTERY has thicker wall, deeply located, pulsating, reddish, with abundant smooth
muscles and elastic tissues that carries oxygenated blood away from the heart towards the
body tissues
The VEIN is thin-walled, superficially located, non-pulsating, bluish vessel that carries
unoxygenated/deoxygenated blood towards the heart
Arterioles are small arteries
Venules are small veins
CAPILLARIES are diffuse network of thin- walled tubules that connect arterioles and venules
together
Physiology
The diameter of the arterioles is the main contributor of the peripheral resistance
In the presence of epinephrine, cold temperature and irritation, the smooth muscles of the
blood vessels will contract making the lumen smaller resistance
In the presence of histamine, warm temperature, the vessels will dilate resistance
Terminology
Chronotropic
Effect
Refers to a change in heart rate
A positive chronotropic effect refers to an increase in heart rate
A negative chronotropic effect refers to a decrease in heart rate
Dromotropic
Effect
Refers to a change in the speed of conduction through the AV junction
A positive dromotropic effect results in an increase in AV conduction velocity
A negative dromotropic effect results in a decrease in AV conduction velocity
Inotropic Effect
Refers to a change in myocardial contractility
A postive inotropic effect results in an increase in myocardial contractility
A negative inotropic effect results in a decrease in myocardial contractility
Systemic circulation
The aorta- leaves the left ventricle to form the ascending aorta, aortic arch, descending aorta,
thoracic aorta and abdominal aorta
The Vena cava ( superior and inferior) drains the whole body and returns the blood to the right
atrium
Physiology of circulation
Blood pressure is the measure of force exerted by blood against the blood vessel wall
Measured by sphygmomanometer
Normally BP is measured as systolic pressure and diastolic pressure
PULSE PRESSURE = SP-DP
S-ar putea să vă placă și
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (588)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5795)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (74)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1091)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (121)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- Evi Anus ChaniagoDocument11 paginiEvi Anus Chaniagorode sihombingÎncă nu există evaluări
- Mobile Coronary Care UnitDocument16 paginiMobile Coronary Care UnitArcha100% (2)
- UGEO H60 Reference Manual PDocument182 paginiUGEO H60 Reference Manual PRafael AndriaÎncă nu există evaluări
- ArrhythmiaDocument2 paginiArrhythmiaChris Pritchard93% (30)
- Heart PathophysiologyDocument20 paginiHeart PathophysiologyDoctorDrapion100% (2)
- 8 Coronary CirculationDocument31 pagini8 Coronary CirculationAhmed AliÎncă nu există evaluări
- Gagal JantungDocument101 paginiGagal JantungAde Fitriyani LubisÎncă nu există evaluări
- Assignment CVSDocument6 paginiAssignment CVSBSN 2-2 Espiritu Melody Mae DÎncă nu există evaluări
- Electrocardiography: Dr. Arun Goel Associate Professor Department of PhysiologyDocument29 paginiElectrocardiography: Dr. Arun Goel Associate Professor Department of PhysiologyAnkarao IttadiÎncă nu există evaluări
- European Journal of Internal MedicineDocument4 paginiEuropean Journal of Internal Medicinesamer battatÎncă nu există evaluări
- Physiology Practical 2: Toad HeartDocument10 paginiPhysiology Practical 2: Toad HeartAdams OdanjiÎncă nu există evaluări
- Electrolyte ImbalanceDocument4 paginiElectrolyte ImbalanceBharathbushan V MandiriÎncă nu există evaluări
- Myocardial Ischemia: Dr. Wael H. Mansy, MDDocument37 paginiMyocardial Ischemia: Dr. Wael H. Mansy, MDHaleema SultanÎncă nu există evaluări
- Cardiac Pacing Learning Package 2013Document34 paginiCardiac Pacing Learning Package 2013Chetan Amberkar100% (1)
- Erc - Sva 2021Document37 paginiErc - Sva 2021Vinícius MenegatÎncă nu există evaluări
- AlgorithmBLS Ped CA Single RescuerCOVID 200406Document1 paginăAlgorithmBLS Ped CA Single RescuerCOVID 200406Karla HernandezÎncă nu există evaluări
- Acls Drug OverviewDocument2 paginiAcls Drug OverviewShannon Davis100% (1)
- Full Report Holter Lorena M 1-23-13Document36 paginiFull Report Holter Lorena M 1-23-13traja_vlrÎncă nu există evaluări
- Eurheartj 40 3 237Document33 paginiEurheartj 40 3 237Maxim BadanÎncă nu există evaluări
- CardiacDocument32 paginiCardiacAlli OmerÎncă nu există evaluări
- Electrocardiography: ECG StandardizationDocument4 paginiElectrocardiography: ECG StandardizationRayan OlivaÎncă nu există evaluări
- 38.17 Cardiac Pacing: Basic Concepts: Renato Pietro RicciDocument16 pagini38.17 Cardiac Pacing: Basic Concepts: Renato Pietro RicciurtikikeÎncă nu există evaluări
- PiCCO Technology Brochure PDFDocument32 paginiPiCCO Technology Brochure PDFHue PhamÎncă nu există evaluări
- Sphygmomanometer Calibration: Why, How and How Often?Document4 paginiSphygmomanometer Calibration: Why, How and How Often?roydityanaziÎncă nu există evaluări
- Qrs Complexes: Fast & Easy Ecgs - A Self-Paced Learning ProgramDocument49 paginiQrs Complexes: Fast & Easy Ecgs - A Self-Paced Learning ProgramMuhammad Hatta HamzahÎncă nu există evaluări
- Cardiomyopathy and MyocarditisDocument69 paginiCardiomyopathy and MyocarditisImmanuel100% (1)
- Technical Publication: H48651FE Direction KTI106019-100 Revision 4Document316 paginiTechnical Publication: H48651FE Direction KTI106019-100 Revision 4Tatiana Dayana BautistaÎncă nu există evaluări
- AclsDocument11 paginiAclsdyah rahayu hutamiÎncă nu există evaluări
- SilverCrest Blood PressureDocument178 paginiSilverCrest Blood PressureFaisal AwadÎncă nu există evaluări
- Hotel Dpalma, Bandung 16 Maret 2018: Dr. Benny Prasetya PDocument145 paginiHotel Dpalma, Bandung 16 Maret 2018: Dr. Benny Prasetya PkangheriÎncă nu există evaluări