Documente Academic
Documente Profesional
Documente Cultură
Guía para Diagnostico Con Oftalmoscopio y Otoscopio Welch Allyn
Încărcat de
guero3261Titlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Guía para Diagnostico Con Oftalmoscopio y Otoscopio Welch Allyn
Încărcat de
guero3261Drepturi de autor:
Formate disponibile
A Guide to the Use of
Diagnostic Instruments in Eye and Ear Examinations
Contents
The Eye 4
The PanOptic Ophthalmoscope 6
The Coaxial Ophthalmoscope 7
How to Conduct a PanOptic Ophthalmologic Exam 8
How to Conduct a Coaxial Ophthalmologic Exam 10
Common Pathologies of the Eye 12
The Ear 18
The Otoscope 20
How to Conduct an Otoscopic Examination 22
Pneumatic Otoscopy 24
Common Pathologies of the Ear 25
Other Ear Care Products 31
3 2
About Welch Allyn: Welch Allyn, Inc. was founded in 1915 and is today a leading manufacturer of innovative
medical diagnostic and therapeutic devices, cardiac defibrillators, patient monitoring systems, and miniature
precision lamps. Headquartered in Skaneateles Falls, New York, USA, Welch Allyn employs more than 2,300
people and has numerous manufacturing, sales, and distribution facilities located throughout the world.
Additional information on Welch Allyn and its products may be found at www.welchallyn.com.
Sponsored by
The Eye
Transparency of the cornea, lens and vitreous humor permits
the practitioner to directly view arteries, veins, the optic nerve
and the retina.
Direct observation of the structures of the fundus through an
effective ophthalmoscope may show disease of the eye itself or
may reveal abnormalities indicative of disease elsewhere in the
body. Among the most important of these are vascular changes
due to diabetes or hypertension and swelling of the optic nerve
head due to papilledema or optic neuritis. In this sense, the eye
serves as a window through which many valuable clinical
evaluations may be made.
When a preliminary diagnosis of an imminently dangerous eye
condition, such as acute glaucoma or retinal detachment, is made
by the examiner, prompt referral to an ophthalmologist may
prevent irreversible damage. Or, when distressing but less urgent
conditions, such as visual impairment due to cataract or vitreous
floaters are recognized, the patient can be reassured and referred.
Welch Allyn ophthalmoscopes, with their bright, white halogen
illumination coupled with their patented optical systems, allow
the examiner to clearly see these important structures of the eye
to aid in making the correct diagnosis.
Little has been written giving the practitioner detailed instructions
on the use of the ophthalmoscope. Because the examination can
give so much information about a patients well being, correct use
of the ophthalmoscope makes it one of the most valuable tools
available for diagnostic use. The following pages in this section
contain information on ophthalmoscopes, how to conduct an
ophthalmic exam, and what to look for while examining the eye.
NORMAL FUNDUS
Optic Disc
Physiological Cup
Macula
Vein
Artery
5 4
A- Macula
B- Vitreous Humor
C- Sclera
D- Choroid
E- Retina
F - Ora Serrata
G- Canal of Schlemm
H- Anterior Chamber
I - Iris
J - Cornea
K - Ciliary Body
L - Zonule (Suspensory Ligament)
M- Conjuctiva
N - Lens
O - Hyaloid Canal
P - Central Retinal Vein
Q - Optic Nerve
R - Central Retinal Artery
PanOptic
TM
Ophthalmoscope Coaxial Ophthalmoscope
7 6
The Welch Allyn PanOptic Ophthalmoscope incorporates a patented*
Axial PointSource optical system. The optics system converges
the light to a point at the cornea, which allows the practitioner easy
entry into small pupils. The illumination pathway then diverges to
the retina, illuminating a very wide area of the fundus. The viewing
system enables the operator to view the illuminated area on virtually
the same axis, thus creating the widest field of view attainable in
undilated ophthalmoscopy.
The PanOptic has a focusing range from -20 to +20 diopters. The
Dynamic Focusing Wheel adjusts the focus in a continuous, smooth
action for more precise control and optimum view. This helps com-
pensate for patient or examiner refractive error, the position of the
ophthalmoscope and the changes in viewing requirements necessitated
by focusing on different points within the eye.
The patient side eyecup helps the practitioner establish and maintain the
proper viewing distance and provides stabilization for the view during the
exam. It also serves as the pivoting point for leverage in panning around the
retina. While in contact with the patient, the eyecup occludes ambient light,
eliminating interference from other light sources.
ADDITIONAL USES FOR THE PANOPTIC OPHTHALMOSCOPE
In addition to examination of the fundus, the ophthalmoscope is a useful
diagnostic aid in studying other ocular structures. The light beam can be
used to illuminate the cornea and the iris for detecting foreign bodies in
the cornea and irregularities of the pupil.
The PanOptic Ophthalmoscope features a Cobalt Blue Filter and add-on
Corneal Viewing Lens (model 11820 only), which together can be used
along with fluorescein dye applied to the cornea to look for abrasions
and foreign bodies on the cornea.
To attach the Corneal Viewing Lens:
1. Remove the patient eyecup.
2. Push and twist on the lens in place of the eyecup, until the
bottoms ribs catch.
Refer to pages 8 and 9 to learn how to conduct an ophthalmic
exam with the PanOptic ophthalmoscope.
*U.S. PATENT NOS. 6,637,882; 6,527,390
Welch Allyn Coaxial ophthalmoscopes incorporate a patented* coaxial
optical system, allowing the axis of illumination to be coincidental
with the axis of vision into the retina, thereby eliminating annoying
shadows and facilitating examination through virtually any size pupil
or vitreous disorder. The fundus and interior anatomy of the eye are
viewed with precision and clarity.
Welch Allyn scopes offer a wide choice of 28 viewing lenses, ranging
from 25 to +40 diopters, with fast, accurate one-hand selection.
This helps compensate for patient or examiner refractive error, the
position of the ophthalmoscope and the changes in viewing require-
ments necessitated by focusing on different points within the eye.
Some coaxial models offer an additional crossed linear polarizing
filter/red-free filter switch that increases the versatility of this instru-
ment. When used in conjunction with available apertures, the coaxial
ophthalmoscope yields 15 possible apertures.
The illuminated lens dial enables the practitioner to check the lens being
used for a particular examination even in a darkened examination room.
The brow rest allows the practitioner to use his/her own eyeglasses
comfortably and safely. It also steadies the instrument while in use.
ADDITIONAL USES FOR THE COAXIAL OPHTHALMOSCOPE
In addition to examination of the fundus, the ophthalmoscope is a useful
diagnostic aid in studying other ocular structures. The light beam can
be used to illuminate the cornea and the iris for detecting foreign bodies
in the cornea and irregularities of the pupil.
Refer to pages 10 and 11 to learn how to conduct an ophthalmic
examination with the Coaxial ophthalmoscope.
When used correctly and regularly, the Welch Allyn ophthalmoscope is
one of the most effective diagnostic instruments available.
*U.S. PATENT NOS. 4,998,818; 4,526,449
APERTURES AND FILTERS
There is a wide range of practical apertures and filters to select from on
both the PanOptic and Coaxial ophthalmoscopes: small spot, large spot,
micro spot, slit aperture, red-free filter, cobalt blue filter, half-moon, and
fixation aperture. This selection of apertures covers all the practitioners
basic needs in an ophthalmoscope.
Micro Spot Aperture: Allows easy
entry into very small, undilated pupils.
Slit Aperture: Helpful in determining
various elevations of lesions, particu-
larly tumors and edematous discs.
Aperture Dial
PanOptic Soft Grip
Front
surface
mirror
Crossed
linear
polarizing
filter/red-free
filter switch
Aperture
selection dial
Dynamic
Focusing Wheel
Patented* Glare
Extinguishment
Patient Eyecup
Rubber
brow rest
Lens
selection
disc
Illuminated
lens indicator
On/Off switch
and rheostat
control
Practitioner Side Patient Side
Small Aperture: Provides easy view of the fundus
through an undilated pupil. Always start the examina-
tion with this aperture and proceed to micro aperture
if pupil is particularly small and/or sensitive to light.
Large Aperture: Standard aperture for dilated pupil
and general examination of the eye.
Half-Moon Aperture (PanOptic Model
11810 only): Provides a combination of
depth perception and field of view.
Fixation Aperture (Coaxial Model only):
The pattern of an open center and thin
lines permits easy observation of eccen-
tric fixation without masking the macula.
Cobalt Blue Filter: Blue filter used
with fluorescein dye permits easy
viewing of small lesions, abrasions,
and foreign objects.
Red-Free Filter: Excludes red
rays from examination field for
easy identification of veins,
arteries, and nerve fibers.
basic needs in an ophthalmoscope.
How to Conduct an Ophthalmologic Examination
with the PanOptic
TM
Ophthalmoscope
1. Take the PanOptic ophthalmoscope in your right hand with the
Practitioner's Side facing you and place your thumb on the Focusing
Wheel. Hold the instrument up to your right eye and look through
the eyepiece. By rotating the Focusing Wheel with your thumb,
focus the instrument on an object approximately 20 feet away.
2. Set the Aperture/Filter Dial to the small spot (green line).
3. Dim the room lights. Instruct the patient to look straight ahead
at a distant object.
4. Hold the PanOptic up to your eye and position the ophthalmo-
scope about 6 inches (15 cm) in front and at a slight angle (15 to
20 degrees) on the temporal side of the patient. Direct the light
beam into the pupil. A red reflex should appear as you look
through the pupil.
5. Rest your left hand on the patients forehead and hold the upper
lid of the eye near the eyelashes with your thumb. While the patient
is fixating on the specified object, keep the red reflex in view and
slowly move toward the patient. Follow the red reflex into the pupil
until the PanOptic eyecup rests on the orbit of the patients eye. The
trip from 6 inches away to making contact must be one that is slow,
deliberate, and steady.
9 8
The optic disc should come into view when you are about 1 to 2 inches (3-5 cm)
from the patient. Gentle compression of the eyecup will maximize the field of view.
If the optic disc is not focused clearly, rotate the Dynamic Focusing Wheel with
your thumb until the optic disc is as clearly visible as possible. The hyperopic,
or far-sighted, eye requires more plus (rotation towards green) focus for
clear focus of the fundus; the myopic, or near-sighted, eye requires minus
(rotation towards red) focus for clear focus.
If you lose the view of the optic disc while approaching the patients eye, pull
back slowly, relocate the red reflex, and try again.
6. Now examine the disc for clarity of outline, color, elevation and condition
of the vessels. Follow each vessel as far to the periphery as you can.
7. To view the macula, instruct your patient to look directly into the light of
the ophthalmoscope. This will automatically place the macula in full view. An
alternative technique is to have your patient fixate straight ahead. Attain the
red reflex from a 15 angle at 6 inches away from the patients eye. When the
PanOptic is 3 inches from contact, instruct the patient to look into the light
while the patient is still facing straight ahead. Continue moving towards the
patient until the eyecup reaches the orbit of the patient.
Look for abnormalities in the macula area. The red-free filter facilitates
viewing of the center of the macula.
8. To examine the extreme periphery, instruct the patient to fixate straight
ahead while performing the examination. Pivot around the eye by leveraging
the eyecup against the orbit of the patients eye to achieve the desired view. It
is important to compress the eyecup to maximize this technique. Without full
compression, the chances of losing your view increase significantly.
This routine will reveal almost any abnormality that occurs in the fundus.
9. To examine the left eye, repeat the procedure outlined above.
ADDITIONAL EXAMS
WITH THE PANOPTIC
OPHTHALMOSCOPE
To look for abrasions and foreign bodies
on the cornea with the corneal viewing
lens, no contact is made between the
ophthalmoscope and the patient.
Begin the exam about 6 inches from the
patient with the focus wheel in the neu-
tral position.
Look through the scope at the patients
cornea to direct the light at the target area.
Adjust the focus wheel into the green
(plus) diopters while moving slightly in
(closer) or out (further) until a comfort-
able working distance and magnification
of the cornea are achieved.
The following steps will help the practitioner obtain satisfactory results with the PanOptic Ophthalmoscope:
8. To examine the extreme periphery, instruct the patient to:
Look up for examination of the superior retina
Look down for examination of the inferior retina
Look temporally for examination of the temporal retina
Look nasally for examination of the nasal retina.
This routine will reveal almost any abnormality that occurs in
the fundus.
9. To examine the left eye, repeat the procedure outlined above but
hold the ophthalmoscope in your left hand, stand at the patients left
side and use your left eye.
OVERCOMING CORNEAL REFLECTION
One of the most troublesome barriers to a good view of the retina
is the light reflected back into the examiners eye from the patients
corneaa condition known as corneal reflection. There are three
ways to minimize this nuisance:
The Coaxial ophthalmoscope features a crossed linear polarizing filter
that may be used. The filter reduces corneal reflection by 99%. It is recom-
mended that the polarizing filter be used when corneal reflection is present.
Use the small aperture. However, this reduces the area of the
retina illuminated.
Direct the light beam toward the edge of the pupil rather than directly
through its center. This technique can be perfected with practice.
USE OF FIXATION TARGET
Direct the patient to focus on the center of the fixation target projected
within the light beam. Simultaneously check the location of the pattern
on the fundus. If the center of the pattern does not coincide with the
macula, eccentric fixation is indicated. In this procedure, the crossed
linear polarizing filter is especially useful since it dramatically reduces
reflections caused by the direct corneal light path.
ADDITIONAL EXAMS WITH COAXIAL OPHTHALMOSCOPE
By selecting the +15 lens in the scope and looking at the pupil as in
a fundus examination [2 inches (5 cm) distance from the patient],
the examiner may verify doubtful pupillary action.
One can also easily detect lens opacities by looking at the pupil
through the +6 lens setting at a distance of 6 inches (15 cm) from
the patient. In the same manner, vitreous opacities can be detected
by having the patient look up and down, to the right and to the left.
Any vitreous opacities will be seen moving across the pupillary area
as the eye changes position or comes back to the primary position.
11 10
How to Conduct an Ophthalmologic Examination
with a Coaxial Ophthalmoscope
In order to conduct a successful examination of the fundus, the examining
room should be either semidarkened or completely darkened. It is
preferable to dilate the pupil when there is no pathologic contraindication,
but much information can be obtained through the undilated pupil.
The following steps will help the practitioner obtain satisfactory results:
1. For examination of the right eye, sit or stand at the patients right side.
2. Select 0 on the illuminated lens disc of the ophthalmoscope and
start with the small aperture.
3. Take the ophthalmoscope in the right hand and hold it vertically in
front of your own right eye with the light beam directed toward the
patient and place your right index finger on the edge of the lens dial
so that you will be able to change lenses easily if necessary.
4. Dim room lights. Instruct the patient to look straight ahead at a
distant object.
5. Position the ophthalmoscope about 6 inches (15 cm) in front and
slightly to the right (25) of the patient and direct the light beam into
the pupil. A red reflex should appear as you look through the pupil.
6. Rest your left hand on the patients forehead and hold the upper lid of
the eye near the eyelashes with the thumb. While the patient is fixating on
the specified object, keep the reflex in view and slowly move toward
the patient. The optic disc should come into view when you are about
1 to 2 inches (3-5 cm) from the patient. If it is not focused clearly, rotate
lenses with your index finger until the optic disc is as clearly visible as
possible. The hyperopic, or far-sighted, eye requires more plus (green
numbers) lenses for clear focus of the fundus; the myopic, or near-
sighted, eye requires minus (red numbers) lenses for clear focus.
7. Now examine the disc for clarity of outline, color, elevation and
condition of the vessels. Follow each vessel as far to the periphery as
you can. To locate the macula, focus on the disc, then move the light
approximately 2 disc diameters temporally. You may also have the
patient look at the light of the ophthalmoscope, which will automatically
place the macula in full view. Look for abnormalities in the macula
area. The red-free filter facilitates viewing of the center of the macula.
Position the ophthalmoscope about 6 inches (15 cm)
in front and 25 to the right side of the patient.
Examine the disc for clarity of outline, color,
elevation and condition of the vessels (Step 7).
13 12
Common Pathologies of the Eye
NORMAL FUNDUS
Disc: Outline clear; central physiological cup is pale
Retina: Normal red/orange color, macula is dark; avascular
area temporally
Vessels: Arterial/venous ratio 2 to 3; the arteries appear a bright
red, the veins a slightly purplish color
HYPERTENSIVE RETINOPATHY
Disc: Outline clear
Retina: Exudates and flame hemorrhages
Vessels: Attenuated arterial reflex
HYPERTENSIVE RETINOPATHY
(ADVANCED MALIGNANT)
Disc: Elevated, edematous disc; blurred disc margins
Retina: Prominent flame hemorrhages surrounding vessels
near disc border
Vessels: Attenuated retinal arterioles
CENTRAL RETINAL VEIN OCCLUSION
Disc: Virtually obscured by edema and hemorrhages
Retina: Extensive blot retinal hemorrhages in all quadrants
to periphery
Vessels: Dilated tortuous veins; vessels partially obscured
by hemorrhages
INFERIOR BRANCH RETINAL ARTERY
OCCLUSION DUE TO EMBOLUS
Disc: Prominent embolus at retinal artery bifurcation
Retina: Inferior retina shows pale, milky edema; superior
retina is normal
Vessels: Inferior arteriole tree greatly attenuated and irregular;
superior vessel is normal
NONPROLIFERATIVE DIABETIC RETINOPATHY
Disc: Normal
Retina: Numerous scattered exudates and hemorrhages
Vessels: Mild dilation of retinal veins
15 14
Common Pathologies of the Eye
PROLIFERATIVE DIABETIC RETINOPATHY
Disc: Net of new vessels growing on disc surface
Retina: Numerous hemorrhages, new vessels at superior
disc margin
Vessels: Dilated retinal veins
END STAGE DIABETIC RETINOPATHY
Disc: Partially obscured by fibrovascular proliferation
Retina: Obscured by proliferating tissue; small area of
retina with hemorrhage seen through window of
fibrovascular membrane
Vessels: Abnormal new vessels in fibrous tissue
Vitreous: Prominent fibrovascular tissue
ADVANCED HEMORRHAGIC
MACULAR DEGENERATION
Disc: Normal
Retina: Large macular scar with drusen; prominent
macular hemorrhage
Vessels: Normal
MACULAR DRUSEN (COLLOID BODIES)
Disc: Normal
Retina: Extensive white drusen of the retina
Vessels: Normal
INACTIVE CHORIORETINITIS (TOXOPLASMAS)
Disc: Normal
Retina: Well-circumscribed lesion with areas of hyperpigmentation
and atrophy of retina, white sclera showing through
Vessels: Normal
ADVANCED RETINITIS PIGMENTOSA
Disc: Normal
Retina: Scattered retinal pigmentation in classic bone
spicule pattern
Vessels: Greatly attenuated
17 16
Common Pathologies of the Eye
RETINAL DETACHMENT
Disc: Normal
Retina: Gray elevation in temporal area with folds in
detached section
Vessels: Tortuous and elevated over detached retina
BENIGN CHOROIDAL NEVUS
Disc: Normal
Retina: Slate gray, flat lesion under retina; several drusen
overlying nevus
Vessels: Normal
PAPILLEDEMA
Disc: Elevated, edematous disc; blurred disc margins;
vessels engorged
Retina: Flame retinal hemorrhage close to disc
Vessels: Engorged tortuous veins
OPTIC NEURITIS
Disc: Elevated with blurred margins
Retina: Mild peripapillary edema
Vessels: Mild dilation of vessels on disc
OPTIC ATROPHY
Disc: Margins sharp and clear; pale white color
Retina: Normal
Vessels: Arteries attenuated; veins normal
GLAUCOMATOUS CUPPING OF DISC
Disc: Large cup, disc vessels displaced peripherally;
pale white color; pigment ring surrounding disc
Retina: Normal
Vessels: Normal
The Ear
Since symptoms of ear disease are relatively few in number
and frequently nonspecific, a clinical examination of the ear
is important in the management of ear disorders.
When a patient complains of ear pain, examination of the ear is
indicated to differentiate whether the patients disorder is an ear
infection or a disorder originating in adjacent structures, such as
the tempomandibular joint, the teeth or the tonsils. As the only
window into the middle ear, the appearance and behavior of the
tympanic membrane offer valuable information about possible
disease within the middle ear.
Fortunately, the ear provides easy access for examining and
diagnosing disorders of the complex and interrelated ear, nose
and throat system. The Welch Allyn otoscope, when used
correctly, is the single most important diagnostic tool available
to the practitioner for determining whether the ear is the source
of the patients complaint.
Otoscopy is one of the primary methods a practitioner uses
for diagnosing patient complaints for the entire ear-nose-throat
complex. Use of a well-designed otoscope which provides illumi-
nation, magnification and air pressure capability for checking
tympanic membrane mobility is, therefore, essential, allowing
the practitioner to view the ear canal and, in particular, the
tympanic membrane with clarity.
The examination instructions that follow this section use the
Welch Allyn otoscope, which incorporates many features that aid
in achieving an accurate, thorough examination.
19 18
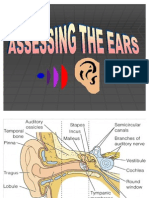
Outer
Ear
Epitympanic
Recess
Tympanic Cavity
Stapes
Tympanic Membrane
Malleus
Incus
Semicircular Canals Vestibule
Endolymphatic
Duct and Sac
Cochlea
Eustachian
Tube
External Ear
Canal
21 20
2.5 mm 3 mm 4 mm 5 mm
3 mm 5 mm 7 mm
2.75 mm 4.25 mm
MacroView
TM
Otoscope
The Welch Allyn MacroView otoscope features a patented
optical system that provides the practitioner with an increased
field of view and magnification to get a large, clear image of
the tympanic membrane. Welch Allyns traditional diagnostic
otoscopes feature a wide-angle magnified viewing lens.
Fiber optics and halogen light
produce optimum illumination
The Welch Allyn otoscope uses both fiber optic
technology and Halogen HPX
illumination. Fiberoptic
light transmission provides a 360 ring of light without visual
obstruction or specular reflection. This distal light results in
glare-free viewing and an easier examination.
Focusing capability (MacroView Otoscope Only)
The Welch Allyn MacroView otoscope has the capability to zoom
in or out on the area in view, resulting in a clearer image to aid
in diagnosis. A focusing wheel, conveniently located on each
side of the otoscope and the back eyepiece, is available to the
practitioner for adjusting the focal length. The adjustable focal
length can compensate for both the practitioners vision and
the length of the patients ear canal, thus creating the clearest
view of the tympanic membrane possible.
Pneumatic otoscopy capability
When examining tympanic membrane mobility, the
ability to perform pneumatic otoscopy is extremely
valuable. The Welch Allyn otoscope incorporates
a closed system and an airtight seal.
Specula attachment and removal
The Welch Allyn MacroView otoscope features
a unique specula attachment and removal design,
the TipGrip, which provides the practitioner with a
secure attachment between the specula and the otoscope during the exam.
After the examination is complete, the tip can be released from the otoscope
by turning the TipGrip counterclockwise or by simply twisting off the tip
with one hand, as is the technique with traditional otoscope models.
SPECULUM OPTIONS
In order to obtain the maximum field of view, the examiner should
always select the largest size speculum which fits comfortably into the
patients ear canal.
The following guidelines may be helpful:
The examiner can choose from several types of specula and
specula accessories:
The first type of speculum is reusable and made of lightweight, durable
polypropylene. Reusable specula are available in four sizes: 2.5 mm,
3 mm, 4 mm and 5 mm.
The second type of speculum is the Universal KleenSpec
, a disposable,
economical and convenient tip. KleenSpec tips are made of nontoxic
plastic and are available in two sizes: 2.75 mm (pediatric) and
4.25 mm (adult).
The third type of speculum, available for traditional Welch Allyn
otoscopes, is SofSpec.,
a reusable specula with a rigid plastic base and
a special soft material at the distal end. SofSpec fits snugly into the
external ear canal. These specula are available in three sizes: 3 mm, 5 mm,
and 7 mm and may be cleaned or sterilized by conventional methods.
For improved seal and comfort during pneumatic otoscopy, the
SofSeal can be placed on the end of either a disposable or reusable
ear speculum. Available in two sizes, the various combinations of
the SofSeal and ear specula allow you to optimize the fit for each
individual patients ear canal.
To perform instrumentation under visualization, the slotted instrumentation
tip (compatible with 23810 and 23820 MacroView) is recommended.
Default Focus: Optimal setting for
most ear examinations
Throat illuminator: Provides light in
a handy built-in penlight
MacroView Otoscope
with Throat Illuminator
Patient Size
Adults 4 mm or 5 mm
Children 3 mm or 4 mm
Infants 2.5 mm or 3 mm Adjustable Focus: Ability to zoom in
or out to fine tune view
TipGrip: Ensures ear speculum
is fastened securely and
easily disposed
Insufflation Port: Creates closed
system for pneumatic otoscopy to
assess middle ear disorders. Apply
positive and negative air pressure
and view tympanic membrane Traditional
Otoscope
Two sizes fit ear specula
ranging from 2 to 5 mm
SOFSEAL
TM
SLOTTED SPECULA
SOFSPEC
KLEENSPEC
REUSABLE
23 22
How to Conduct an Otoscopic Examination
1. Carefully inspect the pinna and postauricular skin. Gently palpate the pinna to
determine if any tenderness exists.
2. Inspect the entrance to the ear canal for debris or pus, which might interfere
with further examination.
3. Choose the largest speculum that can comfortably be inserted into the ear
canal. Straightening the outer ear canal makes insertion of the speculum easier.
For adults, this is accomplished by retracting the pinna upwards and backwards.
For children, this is accomplished by retracting the pinna horizontally backwards.
4. When using the MacroView
TM
otoscope, set the focusing wheel of the otoscope
to the default position by aligning the green line on the focusing wheel with the
corresponding green dot on the side of the instrument. You will feel the focusing
wheel settle into the default setting. The majority of the exams can be completed
at the default focusing position.
5. There are two common ways to hold the otoscope. The first way is
to hold the otoscope like a hammer by gripping the top of the power
handle between your thumb and forefinger, close to the light source. You
can conveniently hold the bulb of the pneumatic attachment between the
palm of the same hand and the power handle. It is recommended that
you extend the middle and ring finger outward so they come into contact
with the persons cheek. This way, any sudden flinch by the patient will
not cause the otoscope to be jammed into the ear canal.
The otoscope can also be held like a pencil, between the thumb and the
forefinger, with the ulnar aspect of the hand resting firmly but gently
against the patients cheek. You can hold the bulb of the pneumatic
attachment in the palm of the same hand. If the patient turns or moves,
the otoscope will move in unison with the patients head. This will avoid
possible injury to the ear canal or even the tympanic membrane.
It is very important that the otoscope be held correctly, particularly
when examining children. A sudden movement by the patient could
cause the skin on the inside of the ear canal to be pierced by the end
of the speculum.
6. It may be necessary to adjust the line of sight and the position of the
speculum to get a complete view of the entire ear canal and all areas of
the tympanic membrane. This yields a composite view of the external
canal and the tympanic membrane.
7. If the tympanic membrane or desired area in view is not in focus, the
practitioner has the option to adjust the focal length of the optics system
of the MacroView otoscope. To adjust the focal length, place a finger on
either side of the focusing wheel or on the back eyepiece of the otoscope.
To shorten the focal length or zoom in, rotate the focusing wheel towards
the smaller dashes on the side of the otoscope. To increase the focal length
or zoom out, rotate the focusing wheel towards the longer dashes.
8. After the examination is complete, the used specula should be
removed from the otoscope. Simply twist the specula off or use the
TipGrip feature (MacroView only) by rotating the TipGrip counter-
clockwise to disengage the specula.
25 24
Pneumatic Otoscopy
Pneumatic otoscopy provides practitioners with a simple method for
determining tympanic mobility and helps then recognize many middle
ear disorders.
It is the pneumatic capability and insufflator attach-
ment of the otoscope which enable the examiner to
assess the mobility of the intact tympanic membrane.
This first requires that you use a speculum sufficiently
large to fit snugly into the ear canal in order to
establish an airtight chamber between the canal
and the interior of the otoscope head.
Gently squeezing the insufflator attachment produces small changes
in the air pressure of the canal. By observing the relative movements
of the tympanic membrane in response to the induced changes in
pressure, the practitioner can obtain valuable diagnostic information
about the mobility of the tympanic membrane. When fluid is present
in the middle ear, for example, movement of the tympanic membrane
is generally diminished or absent. The pneumatic otoscope may
also be useful in distinguishing between a thin atrophic intact
tympanic membrane adherent to the medial wall of the middle
ear, which can be made to move, and a large perforation, which
will not move. This procedure provides a simple method for
determining tympanic membrane mobility and is of value in
the recognition of many middle ear disorders.
Common Pathologies of the Ear
NORMAL TYMPANIC MEMBRANE (LEFT EAR)
The normal tympanic membrane (TM) is a pale, gray, ovoid
semitransparent membrane situated obliquely at the end of the
bony external auditory canal. The handle of the malleus is seen
extending downwards and backwards, ending at the apex of the
triangular cone of reflected light. The long process of the incus
and its articulation with the head of the stapes may frequently be
seen through the postero-superior quadrant of a thin tympanic
membrane. The mobility of an intact TM can readily be assessed
by using the pneumatic attachment to the otoscope.
RED REFLEX (RIGHT EAR)
The introduction of a speculum into the external auditory canal
may cause a reflex dilatation of the circumferential and manubrial
blood vessels supplying the tympanic membrane.
Following a prolonged examination of the ear or in a crying child,
this vasodilatation may produce an appearance mimicking that of
an early acute otitis media.
EXOSTOSIS (LEFT EAR)
Exostoses appear as discreet, hard, round or oval outcroppings
which are sometimes pedunculated. Exostoses in the ear canal are
more often multiple than single and are usually bilateral. They are
usually asymptomatic, extremely slow growing and seldom enlarge
sufficiently to occlude the meatus. Multiple exostoses appear to
result from the prolonged stimulation of the bony external canal
with cold water and are consequently seen more commonly in
persons who swim frequently.
27 26
Common Pathologies of the Ear
FOREIGN BODY
A varied selection of foreign bodies has been discovered in the ear
canals of children. In this case, a large piece of sponge rubber was
removed. In adults, a forgotten piece of cotton wool is frequently
found. The foreign body or an unsuccessful attempt to remove
it can both product secondary otitis externa or damage to the
tympanic membrane and ossicles. In young children, it is sometimes
safer to administer a short, general anesthetic.
ACUTE OTITIS EXTERNA (LEFT EAR)
Trauma (fingernails, bobby pins, cotton tipped swabs) and moisture
(after showering or swimming) are the most common factors
responsible for the development of acute diffuse otitis externa.
The skin of the ear canal is painful, infected and swollen, and it
may be impossible to visualize the tympanic membrane. There is
often a considerable amount of keratin debris in the canal which
must be removed if local treatment is to be effective. Gramnegative
and anaerobic bacteria are the most common pathogens; however,
a culture of material should be a clinical consideration.
KERATOSIS OBTURANS
In this condition of unknown etiology, the bony meatus is
totally occluded by a stony, hard plug of whitish keratin debris.
Keratosis obturans is more frequently seen in patients with
bronchiectasis and chronic sinusitis. Removal of this material is
extremely difficult because of its consistency and its frequent
adherence to the underlying canal skin; a general anesthetic
may be required in some patients.
OTOMYCOSIS
Otoscopic examination in cases of otomycosis reveals a white or
cream colored, thickish debris which may have a fluffy appear-
ance due to the presence of tiny mycelia. When the infection is
caused by Aspergillus niger, it may be possible to identify the tiny
grayish-black conidiophores. The underlying external canal skin
is often inflamed and granular from invasion by fungal mycelia.
Otomycosis may follow the use of topical antibiotic ear drops.
ACUTE OTITIS MEDIA
This acute infection of the middle ear cleft frequently intensifies
upper respiratory tract infections and occurs more commonly
in children. In the early stages of acute otitis media, the tympanic
membrane varies according to the stage of the disease. The
tympanic membrane is retracted and pink with dilatation of the
manubrial and circumferential vessels. Later, as the disease pro-
gresses, the tympanic membrane bulges, becoming fiery red
in color and may eventually perforate, releasing pus into the
external auditory canal.
SEROUS OTITIS MEDIA (RIGHT EAR)
In serous otitis media the tympanic membrane is retracted and
shows decreased mobility with pneumatic otoscopy. The handle
of the malleus is usually foreshortened, chalky-white in color, and
the lateral process is prominent. The presence of a thin, serous
effusion within the middle ear gives the tympanic membrane a
yellowish or even bluish appearance, and in cases of incomplete
eustachian tube obstruction, air bubbles or an air fluid level may
be seen.
29 28
Common Pathologies of the Ear
TYMPANOSTOMY TUBE (RIGHT EAR)
A tympanostomy tube is often inserted into the tympanic
membrane to ventilate the middle ear in cases of chronic serous
otitis media. These tubes come in a variety of sizes, shapes and
materials. The tympanostomy tube should be seen to be in place
in the tympanic membrane with its lumen patent and free of any
exudate or debris.
CENTRAL PERFORATION OF THE
TYMPANIC MEMBRANE (LEFT EAR)
Perforations of the pars tensa of the tympanic membrane can
result from infection or trauma. In this case the large central
perforation resulted from repeated middle ear infections.
HEALED CENTRAL PERFORATION
(RIGHT EAR)
When a large perforation heals, the middle fibrous layer of
the tympanic membrane remains deficient so that a thin semi-
transparent pseudomembrane resembling an open perforation
may be seen. Gentle use of the pneumatic otoscope will, however,
demonstrate that the drum is intact. This thinned segment of a
healed tympanic membrane lacks the strength of a normal drum
and forceful syringing may result in reperforation.
CHRONIC SUPPURATIVE OTITIS MEDIA
(LEFT EAR)
Chronic suppurative otitis media is characterized by recurrent
painless otorrhea. The discharge may vary from mucoid to
frankly purulent. Pseudomonas, Proteus, and Coliforms are
the three most commonly isolated bacteria; however, fungal
organisms can also coexist.
TYMPANOSCLEROSIS (RIGHT EAR)
Tympanosclerotic plaques of varying sizes are seen as chalky
white deposits in the tympanic membrane. They occur as a
result of a postinflammatory deposition of thickened hyalinized
collagen fibrils in the middle fibrous layer of the tympanic
membrane and indicate that the patient has had a previous
significant ear infection.
TYMPANOSCLEROSIS INVOLVING
THE OSSICLES (LEFT EAR)
Tympanosclerotic plaques may also occur within the middle
ear cavity. This photograph shows tympanosclerotic deposits
enveloping the incudostapedial joint. A few plaques are also
present on the promontory. Partial or total fixation of the
ossicular chain by tympanosclerosis is responsible for some
cases of acquired conductive hearing loss.
31 30
Common Pathologies of the Ear
ADHESIVE (ATROPHIC) OTITIS MEDIA
(LEFT EAR)
Following long-standing eustachian tube obstruction, the tympanic
membrane may become atrophic and retracted onto the medial
wall of the middle ear and ossicles, thereby obliterating the middle
ear space. In this case, a thin atrophic tympanic membrane
is draped over the head of the stapes and the tip of the long
process of the incus has been eroded. It can sometimes be
difficult to differentiate an atrophic, immobile, retracted tympanic
membrane from a large central perforation. In this circumstance,
pneumatic otoscopy is often of value.
TRAUMATIC PERFORATION (LEFT EAR)
These perforations result from a variety of causes, including
a blow to the ear, blast injury, or the insertion of a cotton tipped
swab or bobby pin, but rarely follow forceful syringing. Traumatic
perforations generally involve the posterior part of the pars
tensa. While traumatic perforations may be of any shape or
size, they are usually small with clean-cut edges. Fresh blood
may be seen in the deep meatus. Most traumatic perforations
heal spontaneously, provided the ear canal is kept clean and
dry to prevent secondary infection.
CHOLESTEATOMA (RIGHT EAR)
A cholesteatoma is a slowly expanding and eroding cyst lined
with stratified squamous keratinizing epithelium which invades
the middle ear cleft. The presence of whitish keratin debris
within a postero-superior perforation indicates the presence of
an underlying epidermoid cholesteatoma. Serious intracranial
complications may result from the expansion and erosion of the
cholesteatoma sac.
Other Ear Care Products
EXTERNAL EAR: EAR CANAL
Ear Wash System
Some patients suffer from a build-up of cerumen in the ear canal, which can result in
reduced hearing and prevent the examiner from viewing the tympanic membrane. Ear
washing is a proven method to remove cerumen, and is one of the most commonly
performed procedures in the primary care office. The Welch Allyn Ear Wash System
provides an effective device using suction and irrigation to remove cerumen from
patients of all ages. This easy-to-use system allows for cleaner and safer irrigation
compared to other methods.
MIDDLE EAR: TYMPANOMETRY
A tympanometer provides the most accurate, objective means of determining
middle ear status. Tympanometric results can indicate otitis media with effusion,
perforated tympanic membrane, patent tympanostomy tube, ossicular disruption,
tympanosclerosis, cholesteatoma, as well as other middle ear disorders.
Welch Allyn MicroTymp
2: A portable and compact tympanometric instrument that
provides accurate, objective results and printed documentation in seconds.
Welch Allyn TM262
TM
AutoTymp
: A three-in-one instrument that offers tympanometry
and ipsilateral acoustic reflex testing, with optional manual audiometry in one convenient,
compact design.
INNER EAR: AUDIOMETRY OR OTOACOUSTIC EMISSIONS (OAE)
An audiometer is an electronic instrument for generating sounds that can be used
to measure an individuals hearing sensitivity. Audiometric measurement of auditory
function can determine the degree of hearing loss, estimate the location of the lesion
within the auditory system that is producing the problem, and help establish the
cause of the hearing problem.
Welch Allyn AudioScope
3: A portable audiometer to quickly and accurately screen
patients at three different levels: 20, 25, and 40 dB, allowing all patients to be
screened with a single instrument.
Welch Allyn AM232
TM
: A manual audiometer that has the ability to test hearing in
ranges beyond speech frequencies. With this instrument, the practitioner can obtain the
precise threshold of patients hearing to better identify specific patterns of hearing loss.
Otoacoustic emissions is a response generated by structures (outer hair cells) in the
healthy cochlea to sounds presented into the ear canal. The Welch Allyn OAE Hearing
Screener will detect hearing loss, prevent language disabilities and improve patient
outcomes. The child-friendly hearing screener is objective, accurate and easy to use. outcomes. The child-friendly hearing screener is objective, accurate and easy to use.
4341 State Street Road, P.O. Box 220, Skaneateles Falls, NY 13153-0220 USA
(p) 800.535.6663 (f) 315.685.3361 www.welchallyn.com
2006 Welch Allyn, Inc. Printed in USA SM2815 Rev C
S-ar putea să vă placă și
- A Guide To The Use of Ophthalmoscopes in The Eye ExaminationDocument48 paginiA Guide To The Use of Ophthalmoscopes in The Eye ExaminationSaul Olmeda FregosoÎncă nu există evaluări
- 23466fundamentals of OphthalmosDocument6 pagini23466fundamentals of OphthalmosCarla Saab AñezÎncă nu există evaluări
- Manual PanopticDocument28 paginiManual PanopticMauricio RodriguezÎncă nu există evaluări
- Fundamentals of Ophthalmoscopy For Medical StudentsDocument4 paginiFundamentals of Ophthalmoscopy For Medical StudentsAboDilanÎncă nu există evaluări
- Ocular Emergencies 2017Document18 paginiOcular Emergencies 2017Sebastian BarreraÎncă nu există evaluări
- Practicalophthalmology Web 2Document104 paginiPracticalophthalmology Web 2mohalbhm9Încă nu există evaluări
- EquipmentDocument3 paginiEquipmentapi-394275021Încă nu există evaluări
- Examination of EyeDocument33 paginiExamination of EyeSumit YadavÎncă nu există evaluări
- Indirect OphthalmosDocument3 paginiIndirect Ophthalmosbijujc100% (1)
- Ophthalmolog Y: Instruments & InvestigationDocument15 paginiOphthalmolog Y: Instruments & Investigationhenry cazeÎncă nu există evaluări
- Aio Vol 1 Issue 1 Sep 2013Document56 paginiAio Vol 1 Issue 1 Sep 2013aiojournalÎncă nu există evaluări
- Ocular Examination and Imaging TechniqueDocument33 paginiOcular Examination and Imaging TechniqueluckyÎncă nu există evaluări
- Visual Fields Guide for OphthalmologistsDocument23 paginiVisual Fields Guide for OphthalmologistsPRANEET MISHRAÎncă nu există evaluări
- Bo 405 (32301721022)Document8 paginiBo 405 (32301721022)AvinabaÎncă nu există evaluări
- STD Subj Refract MinusCyl CliniciansDocument8 paginiSTD Subj Refract MinusCyl CliniciansawaisÎncă nu există evaluări
- STD Subj Refract Plus MinusCyl ClinicansDocument12 paginiSTD Subj Refract Plus MinusCyl ClinicansawaisÎncă nu există evaluări
- Basic Eye ExamDocument8 paginiBasic Eye ExamLisa AguilarÎncă nu există evaluări
- Examination of The RetinaDocument3 paginiExamination of The RetinaGus LionsÎncă nu există evaluări
- Manual RefractionDocument36 paginiManual Refractionjzaib1154Încă nu există evaluări
- Binocular Indirect Ophthalmoscopy GuideDocument5 paginiBinocular Indirect Ophthalmoscopy GuideMario JohanÎncă nu există evaluări
- This Site Is Intended For Healthcare ProfessionalsDocument10 paginiThis Site Is Intended For Healthcare ProfessionalssudheervermaÎncă nu există evaluări
- Intoduction and MethodologyDocument11 paginiIntoduction and MethodologyKarthikÎncă nu există evaluări
- Ophthalmic Emergencies in The 2021 Veterinary Clinics of North America EquiDocument20 paginiOphthalmic Emergencies in The 2021 Veterinary Clinics of North America EquiJuan Pardo CarrascoÎncă nu există evaluări
- Fundoscopy GuideDocument10 paginiFundoscopy Guidedrjanggeum0% (1)
- Clinical Study: Aspheric Intraocular Lenses Implantation For Cataract Patients With Extreme MyopiaDocument6 paginiClinical Study: Aspheric Intraocular Lenses Implantation For Cataract Patients With Extreme MyopiaKevin ArdiansyahÎncă nu există evaluări
- Cataract SurgeryDocument14 paginiCataract SurgeryRenato AbellaÎncă nu există evaluări
- 21 Visual TestDocument22 pagini21 Visual TestPatricia Zabala Animas100% (3)
- Ophthalmoscopy SlideDocument19 paginiOphthalmoscopy SlidemhixgoodieÎncă nu există evaluări
- Optometry Department OPTO 374 The Synoptophore Dr. Safiah Mulla Name: Fatima Ahmad Abo-Qoaied ID: 426200452Document25 paginiOptometry Department OPTO 374 The Synoptophore Dr. Safiah Mulla Name: Fatima Ahmad Abo-Qoaied ID: 426200452zecemariÎncă nu există evaluări
- AvanseePreset Review Article Miyake Et Al EuroTimes - Sept 2014Document12 paginiAvanseePreset Review Article Miyake Et Al EuroTimes - Sept 2014Hombre69Încă nu există evaluări
- Indirect OphthalmosDocument8 paginiIndirect OphthalmosAnumeha JindalÎncă nu există evaluări
- Fundoscopy Made Easy Ming 2009Document34 paginiFundoscopy Made Easy Ming 2009Laura100% (1)
- Ophthalmology OSCE GuideDocument86 paginiOphthalmology OSCE GuideChefera Aga100% (1)
- Mentahan PPT Lapsus DR BasDocument20 paginiMentahan PPT Lapsus DR BasArlinda Silva PrameswariÎncă nu există evaluări
- Tinted Lens in Low VisionDocument10 paginiTinted Lens in Low VisionAmrit PokharelÎncă nu există evaluări
- Accurate Optical Biometry Using IOL MasterDocument5 paginiAccurate Optical Biometry Using IOL Mastermuzicka9Încă nu există evaluări
- Nursing Assessment: Presented byDocument42 paginiNursing Assessment: Presented byBrent Balusdan SongabenÎncă nu există evaluări
- The Scrub's Bible: How to Assist at Cataract and Corneal Surgery with a Primer on the Anatomy of the Human Eye and Self AssessmentDe la EverandThe Scrub's Bible: How to Assist at Cataract and Corneal Surgery with a Primer on the Anatomy of the Human Eye and Self AssessmentÎncă nu există evaluări
- What Is Retinoscopy?: Myopia HyperopiaDocument4 paginiWhat Is Retinoscopy?: Myopia HyperopiababyswitÎncă nu există evaluări
- Literature Review of Cataract SurgeryDocument5 paginiLiterature Review of Cataract Surgeryafmacfadbdwpmc100% (1)
- How To Use OphthalmoscopeDocument2 paginiHow To Use Ophthalmoscopeaashish_39Încă nu există evaluări
- Extracapsular Cataract Extraction (OR)Document4 paginiExtracapsular Cataract Extraction (OR)Jet-Jet GuillerganÎncă nu există evaluări
- Fundus Camera Project ReportDocument37 paginiFundus Camera Project ReportbhonslechetankumarÎncă nu există evaluări
- OrthopticDocument9 paginiOrthopticSobiafarooqÎncă nu există evaluări
- Understanding RetinoscopyDocument14 paginiUnderstanding RetinoscopyŠadïįaQasimÎncă nu există evaluări
- Comprehensive Eye Exams - What To Expect - AllAboutVisionDocument8 paginiComprehensive Eye Exams - What To Expect - AllAboutVisionIsniÎncă nu există evaluări
- Mri MachineDocument16 paginiMri Machineمحمد المدنيÎncă nu există evaluări
- Dr. Mamta Dept of Ophthalmology RNT Medical College, UdaipurDocument56 paginiDr. Mamta Dept of Ophthalmology RNT Medical College, UdaipurGideon IrwandaÎncă nu există evaluări
- Phacoemulsification & Extra Capsular Cataract ExtractionDocument7 paginiPhacoemulsification & Extra Capsular Cataract ExtractionJo-anne CorderoÎncă nu există evaluări
- Effectiveness and Safety of The Clareon Monofocal Intraocular Lens: Outcomes From A 12-Month Single-Arm Clinical Study in A Large SampleDocument11 paginiEffectiveness and Safety of The Clareon Monofocal Intraocular Lens: Outcomes From A 12-Month Single-Arm Clinical Study in A Large SampleHariom ShuklaÎncă nu există evaluări
- Manual of Eye Emergencies Diagnosis and ManagementDocument221 paginiManual of Eye Emergencies Diagnosis and ManagementPhilip McNelson100% (2)
- Opth 14 815Document8 paginiOpth 14 815Andrés QueupumilÎncă nu există evaluări
- MX of Patients With Senile CataractDocument6 paginiMX of Patients With Senile CataractzusehenÎncă nu există evaluări
- Dispensing NotesDocument103 paginiDispensing Notesjancok100% (1)
- Examination of The Eye in The Emergency Room: Christopher Calandrella D.O - Pgy2Document104 paginiExamination of The Eye in The Emergency Room: Christopher Calandrella D.O - Pgy2Alexandra Mendoza100% (1)
- Eye Assessment: OptometristsDocument8 paginiEye Assessment: OptometristsLiam MaghanoyÎncă nu există evaluări
- Current Examination Methods of The Canine Eye: J. Beránek, P.J. VítDocument6 paginiCurrent Examination Methods of The Canine Eye: J. Beránek, P.J. VítOktavia firnandaÎncă nu există evaluări
- Current Advances in Ophthalmic TechnologyDe la EverandCurrent Advances in Ophthalmic TechnologyParul IchhpujaniÎncă nu există evaluări
- Multifocal Intraocular Lenses: The Art and the PracticeDe la EverandMultifocal Intraocular Lenses: The Art and the PracticeJorge L. AlióÎncă nu există evaluări
- Heine XHL Xenon Halogen Bulbs: For Optimum Performance and Cost-EffectivenessDocument7 paginiHeine XHL Xenon Halogen Bulbs: For Optimum Performance and Cost-EffectivenessGunwant SinghÎncă nu există evaluări
- 18C Medical3 (PDF Library)Document28 pagini18C Medical3 (PDF Library)Michael KnightsÎncă nu există evaluări
- Medical Instruments Pictures & Thier UsesDocument74 paginiMedical Instruments Pictures & Thier UsesMohsan Raza100% (1)
- Cerumen Impaction FinalDocument8 paginiCerumen Impaction FinalRose Ann Del MundoÎncă nu există evaluări
- Otomicroscopy (Adult, Peds)Document4 paginiOtomicroscopy (Adult, Peds)Carmen EneaÎncă nu există evaluări
- Otoscopy and Hearing Protection Practicum GuideDocument29 paginiOtoscopy and Hearing Protection Practicum GuideSarah EddiahÎncă nu există evaluări
- HargaDocument1.176 paginiHargaRSUD SOLOKÎncă nu există evaluări
- Ent enDocument868 paginiEnt enmmt amerikanÎncă nu există evaluări
- Earsi Otoscope BrochureDocument12 paginiEarsi Otoscope BrochureHaag-Streit UK (HS-UK)Încă nu există evaluări
- 1Document472 pagini1official0% (1)
- Ear Examination GuideDocument12 paginiEar Examination GuideAmit SinghÎncă nu există evaluări
- Atlas Instruments Ent Head NeckDocument317 paginiAtlas Instruments Ent Head NeckDr-Firas Nayf Al-Thawabia100% (1)
- Celebrating 25 Years: CatalogueDocument76 paginiCelebrating 25 Years: CatalogueTiago DiasÎncă nu există evaluări
- Accesorios Welch AllynDocument17 paginiAccesorios Welch AllynJuan MoralesÎncă nu există evaluări
- Assessing The EarsDocument56 paginiAssessing The EarsRosela Ponio100% (1)
- CA Eye and Ear DisorderDocument20 paginiCA Eye and Ear DisorderEsmareldah Henry Sirue100% (1)
- Notes For The New Exam.: DR Swamy PLAB CoursesDocument44 paginiNotes For The New Exam.: DR Swamy PLAB CoursesBeaulah100% (1)
- Welch Allyn Diagnostic SetsDocument2 paginiWelch Allyn Diagnostic SetsDappa DatuboÎncă nu există evaluări
- 9 Ear ExaminationDocument25 pagini9 Ear ExaminationMariam QaisÎncă nu există evaluări
- ENT Ear Examination ScriptDocument2 paginiENT Ear Examination ScriptVanessa HermioneÎncă nu există evaluări
- Otosim (Watermark)Document3 paginiOtosim (Watermark)mat koolÎncă nu există evaluări
- CMOS Technology in Otorhinolaryngology: Maximum Compatibility For State-Of-The-Art DiagnosisDocument12 paginiCMOS Technology in Otorhinolaryngology: Maximum Compatibility For State-Of-The-Art DiagnosisPeter SalimÎncă nu există evaluări
- Health Assessment 4Document13 paginiHealth Assessment 4shannon c. lewisÎncă nu există evaluări
- American Ent Oxford PDFDocument461 paginiAmerican Ent Oxford PDFanna100% (3)
- Assessment of The Ears Rev 4-2013Document8 paginiAssessment of The Ears Rev 4-2013alphabennydelta4468Încă nu există evaluări
- Assess Ear Exam ProceduresDocument2 paginiAssess Ear Exam ProceduresAnonymous Ez2YZIsZÎncă nu există evaluări
- EP59-11234 Issue 8 - EnglishDocument37 paginiEP59-11234 Issue 8 - EnglishFahcrezaÎncă nu există evaluări
- Diagnostic Tests For ENTDocument32 paginiDiagnostic Tests For ENTNalafÎncă nu există evaluări
- Health Assessment For Nursing Practice 5th Edition Wilson Test BankDocument16 paginiHealth Assessment For Nursing Practice 5th Edition Wilson Test BankJordanGibsonopaxj100% (13)
- otoRhinoLaRynGoLogic Exam ChecklistDocument5 paginiotoRhinoLaRynGoLogic Exam ChecklistSulabh ShresthaÎncă nu există evaluări