Documente Academic
Documente Profesional
Documente Cultură
Guias para Administrar en Forma Segura Altas Dosis de Interleukina 2007
Încărcat de
api-26302710Descriere originală:
Titlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Guias para Administrar en Forma Segura Altas Dosis de Interleukina 2007
Încărcat de
api-26302710Drepturi de autor:
Formate disponibile
PROLEUKIN (aldesleukin) for Injection:
High-Dose Guidelines
Pretherapy interventions Target systolic blood pressure during therapy When to delay or discontinue IL-2
Observation Category* Action
• Discontinue antihypertensive medications. Normal Blood Target Blood
Pressure Pressure Any relative criterion • Initiate corrective measure
• Start acetaminophen, indomethacin, and an H2 and/or delay IL-2.
for the Patient on Therapy
blocker 8-12 hours before administering IL-2. ≥ 3 relative criteria • Initiate corrective measures
and delay IL-2.
• Start maintenance intravenous fluids (ie, lactated <100 mm Hg >80 mm Hg
• Stop IL-2 if adverse events
Ringer’s solution) at 50-100 mL/h immediately are not easily reversed.
before administering IL-2. 100-120 mm Hg >85 mm Hg
Any absolute criterion • Initiate corrective measure
and delay IL-2.
• Premedicate the patient for nausea before
>120 mm Hg >90 mm Hg • Stop IL-2 if adverse event
administering IL-2. is not easily reversed.
Adapted from Schwartzentruber.1 Adapted from Schwartzentruber.1 Adapted from Schwartzentruber.1
*See table below for relative and absolute criteria.
Relative or absolute criteria to be considered when deciding whether to delay or discontinue high-dose IL-2 administration (see table above for decision points)
System Relative Criteria Absolute Criteria
Cardiac • Sinus tachycardia (120-130 bpm) • Sustained sinus tachycardia (if heart rate >130 bpm persists after stopping dopamine and
taking action to correct hypotension, fever, and tachycardia)
• Atrial fibrillation
• Supraventricular tachycardia
• Ventricular arrhythmias (frequent premature ventricular contractions, bigeminy, tachycardia)
• Elevated creatine kinase isoenzymes or troponin
• Electrocardiogram changes indicative of ischemia
Dermatologic – • Moist desquamation
Gastrointestinal • Diarrhea ≥1000 mL/shift • Diarrhea ≥1000 mL/shift on 2 consecutive shifts
• Ileus and/or abdominal distention • Vomiting not responsive to medication
• Bilirubin >7 mg/dL • Severe abdominal distention affecting breathing
• Severe, unrelenting abdominal pain
Hemodynamic • Maximum phenylephrine hydrochloride 1-1.5 µg/kg/min • Maximum phenylephrine hydrochloride 1.5-2 µg/kg/min
• Minimum phenylephrine hydrochloride >0.5 µg/kg/min • Minimum phenylephrine hydrochloride >0.8 µg/kg/min
Hemorrhagic • Frank blood in sputum, emesis, or stool • Guiac-positive sputum, emesis, and/or stool
• Platelet count of 30,000-50,000/mm3 • Platelet count <30,000/mm3
Infection – • Documented or strongly suspected
Musculoskeletal • Extremity tightness • Extremity paresthesias
Neurologic/Psychiatric • Vivid dreams • Hallucinations
• Emotional lability • Persistent crying
• Mental status changes not reversible within 2 hours
• Inability to subtract serial 7s or spell “WORLD” backward (“DLROW”)
• Disorientation
Pulmonary • 3-4 L O2 by nasal cannula to achieve O2 saturation ≥95% • >4 L O2 by nasal cannula to achieve O2 saturation ≥95% or 40% O2 mask to achieve
• Shortness of breath while resting O2 saturation ≥95%
• Rales 1/3 up chest • Endotracheal intubation
• Moist rales 1/2 up chest
• Pleural effusion requiring tap or chest tube while on therapy
Renal • Urine output of 80-160 mL/shift • Urine output <80 mL/shift
• Urine output rate of 10-20 mL/h • Urine output rate <10 mL/h
• Creatinine level of 2.5-2.9 mg/dL • Creatinine level ≥3 mg/dL
Systemic • Weight gain of >15% –
Adapted from Schwartzentruber. 1
Please see accompanying full prescribing information, including boxed warning.
PROLEUKIN (aldesleukin) for Injection:
®
High-Dose Guidelines (continued)
ICU transfer criteria related to the development Requirements for managing capillary leak
Management of capillary leak syndrome
of capillary leak syndrome (CLS) syndrome in the ICU
Oliguria • Monitor blood pressure before and after IL-2 doses.
• Central venous catheter to monitor central • Assess clinical symptoms of hypotension, dizziness, light-headedness,
• Inability to maintain urine output >20 mL/h with 2 L venous pressure and fainting.
normal saline solution (0.9%) IV boluses • Report persistent hypotension (SBP <90 mm Hg) that does not
respond to 2 L normal saline solution (0.9%) IV boluses, begin
Hypotension • Foley catheter to monitor urine output dopamine and transfer to ICU.
• Auscultate for breath sounds.
• Persistent SBP <90 mm Hg
• Monitor O2 saturation.
• O2 saturation monitor for hypoxia; O2 at • Monitor heart rate; assess with ECG; report significant tachycardia
Cardiac arrhythmias 2-5 L to prevent hypoxemia or arrhythmias.
• ST wave changes • Monitor urine output (strict intake and output recording); Foley
catheter may be needed to monitor hourly output.
• Increasing creatinine phosphokinase
• Dopamine 2-5 µg/kg/min to maintain urine • Monitor daily weight.
• Need to constantly monitor cardiac arrhythmias
output at ≥20 mL/h • Monitor electrolytes, blood urea nitrogen, creatinine, liver enzymes;
• Tachycardia >120 bpm initiate treatment to correct abnormally low levels of magnesium,
phosphorus, and/or potassium.
Somnolence • Dopamine and phenylephrine to maintain • Initiate diuretics when hypotension is controlled and creatinine is stable.
SBP at ≥90 mm Hg • Assist patient in adjusting physical activity to conserve energy.
• Mechanism not understood; may be related to CLS
• Report significant changes to physician.
Adapted from White et al.2 Adapted from White et al.2 Adapted from Seipp.3
Symptom management
Symptom Corrective Measure(s)
Arrhythmia (other than sinus tachycardia) Stop IL-2 (most arrhythmias); correct electrolytes, minerals, anemia, hypoxia
Anemia Transfuse packed red blood cells to achieve hematocrit >28% during IL-2 dosing
Acidosis CO2 <20 mmol/L, give 50 mEq sodium bicarbonate IV; CO2 <18 mmol/L, give 100 mEq sodium bicarbonate IV
Chills Warm blankets at first instance; meperidine IV if chills persist
Creatine kinase elevation Order lab tests for isoenzymes or troponin; administer electrocardiogram; if evidence of myocarditis, stop IL-2 (exercise echocardiogram
required before next cycle of IL-2 to rule out myocardial dysfunction; future IL-2 may be considered if echocardiogram is normal)
Dermatitis Oatmeal baths; nonsteroidal, nonalcoholic lotions
Diarrhea Antidiarrheals (alternate medications); avoid overuse because of complicating ileus and distention
Edema Elevate symptomatic extremity; use fluids judiciously
Epigastric pain Evaluate cause; give indomethacin rectally; consider antacids
Fever breakthrough Increase frequency of indomethacin to every 6 hours; consider septic workup if fever happens after first 24 hours of therapy
(ie, high spike above rising baseline during therapy)
Hypoalbuminemia Observe
Hypocalcemia Maintain above lowest normal value
Hypokalemia Maintain potassium above 3.6 mmol/L
Hypomagnesemia Maintain above lowest normal value
Hypotension Initially fluids; add phenylephrine hydrochloride after 1-1.5 L of fluid boluses
Infection Stop IL-2; treat infection as indicated
Mucositis/stomatitis Frequent oral care; mouthwashes; topical anesthetics; room humidifier
Nausea/vomiting Antiemetics (alternate medications and routes if any one not effective)
Nasal congestion Room humidifier; decongestant (no inhalational steroids)
Oliguria Initially fluids; add dopamine after 1-1.5 L of fluid boluses
Poor venous access Peripherally inserted central catheter (PICC) or central line; antibiotic prophylaxis started when PICC/central line is inserted and continued
until line is removed (remove line as soon as not needed for fluids, vasopressors, replacements, diuretics)
Pruritus Oatmeal baths; nonsteroidal, nonalcoholic lotions; antipruritics
Shortness of breath Check transcutaneous O2 saturation and use O2 if <95%; use fluids judiciously; do not use inhalational steroids
Tachycardia (sinus) Correct fever, hypotension, hypoxia, anemia; consider discontinuation of dopamine if used
Thrombocytopenia Consider transfusion if count <20,000/mm3
Troponin elevation Must stop IL-2; will need exercise echocardiogram before the next cycle of IL-2 to rule out myocardial dysfunction; future IL-2 may be
considered if echocardiogram is normal
Adapted from Schwartzentruber.1
Please see accompanying full prescribing information, including boxed warning.
REFERENCES 1. Schwartzentruber DJ. Guidelines for the safe administration of high-dose interleukin-2. J Immunother. 2001;24:287-293. 2. White RL, Jr, Schwartzentruber DJ, Guleria A, et al. Cardiopulmonary toxicity of treatment with
high dose interleukin-2 in 199 consecutive patients with metastatic melanoma or renal cell carcinoma. Cancer. 1994;74:3212-3222. 3. Seipp CA. Guidelines for the safe administration of high-dose interleukin-2: nursing considerations.
Biotherapy: Considerations for Oncology Nurses. 2003;6:11-15.
©September, 2004 Chiron Corporation PR068
S-ar putea să vă placă și
- CEG Formulary: Cardiac Medications For Dogs: ... Bringing Cardiology Into PracticeDocument6 paginiCEG Formulary: Cardiac Medications For Dogs: ... Bringing Cardiology Into PracticeAngeles MerinoÎncă nu există evaluări
- NCP 1Document9 paginiNCP 1Princess Rodginia Mae MagayonÎncă nu există evaluări
- Drug in EmergencyDocument8 paginiDrug in EmergencySuzana YusofÎncă nu există evaluări
- Anaesthesia Revision E6.5Document33 paginiAnaesthesia Revision E6.5Riya SharmaÎncă nu există evaluări
- Drug Action Indication Contraindicati ON Adverse Effects Nursing ConsiderationsDocument3 paginiDrug Action Indication Contraindicati ON Adverse Effects Nursing ConsiderationsRaphael PalomataÎncă nu există evaluări
- Anti Hypertensive DrugsDocument113 paginiAnti Hypertensive DrugsRobert DowneyÎncă nu există evaluări
- TablesDocument21 paginiTablesMélissa BlancÎncă nu există evaluări
- Generic Name:: ElectrolytesDocument9 paginiGeneric Name:: ElectrolytesEleazar Desillarico GonzalesÎncă nu există evaluări
- MedicationsDocument63 paginiMedicationssaraÎncă nu există evaluări
- ACLS ACS Algorithm NewDocument3 paginiACLS ACS Algorithm Newsambo100% (1)
- Management Strategy in Hypertensive Crisis The Role of NicardipineDocument38 paginiManagement Strategy in Hypertensive Crisis The Role of Nicardipinezulfikar adiÎncă nu există evaluări
- Drug StudyDocument3 paginiDrug StudyTrixia ArcegonoÎncă nu există evaluări
- 6 Alterations On Tissue Perfusion Poleno Serrano TajalaDocument18 pagini6 Alterations On Tissue Perfusion Poleno Serrano TajalaSophia A. GoÎncă nu există evaluări
- Adult Cardiac Arrest Circular Algorithm: Monitor CPR QualityDocument1 paginăAdult Cardiac Arrest Circular Algorithm: Monitor CPR QualityAlexis HospitalÎncă nu există evaluări
- Adult Cardiac Arrest Circular Algorithm: Monitor CPR QualityDocument1 paginăAdult Cardiac Arrest Circular Algorithm: Monitor CPR QualityChris LeeÎncă nu există evaluări
- Commonly Used IV Cardiac Medications For Adults Pocket Reference Card PDFDocument12 paginiCommonly Used IV Cardiac Medications For Adults Pocket Reference Card PDFYannis Zoldenberg100% (1)
- Microsoft Word Cardiac Medications 1231855169882073 2Document1 paginăMicrosoft Word Cardiac Medications 1231855169882073 2api-19824701Încă nu există evaluări
- Drugs Used in Cardiovascular SystemDocument57 paginiDrugs Used in Cardiovascular SystemSandeep ChaudharyÎncă nu există evaluări
- Ventura County Medical Center: Mi Thrombolysis, Management ofDocument3 paginiVentura County Medical Center: Mi Thrombolysis, Management ofblackcat657Încă nu există evaluări
- Prehospital MedicationsDocument123 paginiPrehospital Medicationshilwaalfi100% (1)
- Cardiovascular DrugsDocument7 paginiCardiovascular Drugsacademic purposesÎncă nu există evaluări
- High AlertDocument61 paginiHigh Alertdrsidra.mustafaÎncă nu există evaluări
- Test 2 OutlineDocument7 paginiTest 2 Outlinemara5140Încă nu există evaluări
- AdenosineDocument2 paginiAdenosinejdmedicÎncă nu există evaluări
- CPR PosterDocument1 paginăCPR PosterHemantÎncă nu există evaluări
- Acute Coronary Syndrome / Acute Myocardial Infarction AlgorithmDocument37 paginiAcute Coronary Syndrome / Acute Myocardial Infarction Algorithmjitendra magarÎncă nu există evaluări
- Obat Obat EmergencyDocument34 paginiObat Obat EmergencymatkwokÎncă nu există evaluări
- Rawabi Saleh Bakrman Fatima Mohammed Dawood Supervision: Dr. Hassan BayashootDocument21 paginiRawabi Saleh Bakrman Fatima Mohammed Dawood Supervision: Dr. Hassan BayashootRawabi SalehÎncă nu există evaluări
- ICU 2 - Management For DICDocument20 paginiICU 2 - Management For DICNur Aziemah Mohd ZamriÎncă nu există evaluări
- QRH 3-10 Local Anaesthetic Toxicity v2 June 2023Document1 paginăQRH 3-10 Local Anaesthetic Toxicity v2 June 2023ReddyÎncă nu există evaluări
- Algorithms of AHA 2020Document23 paginiAlgorithms of AHA 2020Emirhan llkhanÎncă nu există evaluări
- Pharmacology 1Document33 paginiPharmacology 1Sultan SalmanÎncă nu există evaluări
- Eremblen Toroljuuleliitn ZaawarDocument2 paginiEremblen Toroljuuleliitn ZaawarОюунгэрэл Бархас-ОдÎncă nu există evaluări
- Electrolyte Prescribe Gline AdultDocument2 paginiElectrolyte Prescribe Gline AdultMirelaÎncă nu există evaluări
- TRANSF Sangre MapaDocument1 paginăTRANSF Sangre MapaSiu Lin WongÎncă nu există evaluări
- AmlodipineDocument2 paginiAmlodipineCj LowryÎncă nu există evaluări
- AmlodipineDocument2 paginiAmlodipineVina Jane P Laurel92% (12)
- Pharmacological Tools: Doses, Routes, and Uses of Common DrugDocument1 paginăPharmacological Tools: Doses, Routes, and Uses of Common DrugApuntesdemedicinaa blogÎncă nu există evaluări
- MENDOZA, Francis Luigi C. - DRUG STUDYDocument11 paginiMENDOZA, Francis Luigi C. - DRUG STUDYbaka esh toÎncă nu există evaluări
- Access Pathways To Queensland Health Adult Inpatient Beds For Patients With Eating DisordersDocument10 paginiAccess Pathways To Queensland Health Adult Inpatient Beds For Patients With Eating DisordersGrace McConnochieÎncă nu există evaluări
- Anesthesia Revision E6.5 (Medicalstudyzone - Com)Document34 paginiAnesthesia Revision E6.5 (Medicalstudyzone - Com)Rohan RathoreÎncă nu există evaluări
- Acute Coronary Syndrome / Acute Myocardial Infarction AlgorithmDocument37 paginiAcute Coronary Syndrome / Acute Myocardial Infarction AlgorithmHan OWÎncă nu există evaluări
- Amlodipine Drug StudyDocument2 paginiAmlodipine Drug StudyAbigail Basco100% (3)
- ACLS DrugsDocument16 paginiACLS Drugstostc100% (2)
- Atrial Fibrillation TDDocument6 paginiAtrial Fibrillation TDapi-594366475Încă nu există evaluări
- Ecart MedsDocument5 paginiEcart Medsしゃいな ふかみÎncă nu există evaluări
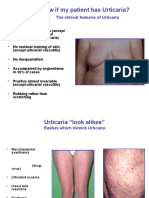
- How Do I Know If My Patient Has Urticaria?: The Clinical Features of UrticariaDocument13 paginiHow Do I Know If My Patient Has Urticaria?: The Clinical Features of UrticariaRajesh MevawalaÎncă nu există evaluări
- Agent For Treating Heart FailureDocument26 paginiAgent For Treating Heart FailureClarisse SuanÎncă nu există evaluări
- Isoflurane ThiopentalDocument13 paginiIsoflurane ThiopentalMr rawr100% (1)
- Anti ArrhythmicsDocument46 paginiAnti Arrhythmicsmunim1192Încă nu există evaluări
- Emergecy DrugsDocument6 paginiEmergecy DrugsChristopher EsguerraÎncă nu există evaluări
- HPN Drug StudyDocument4 paginiHPN Drug StudyJohn Haider Colorado GamolÎncă nu există evaluări
- Farmakologi 1 Antihypertension: NURUL HASANAH (1800085)Document31 paginiFarmakologi 1 Antihypertension: NURUL HASANAH (1800085)MutiaraBintangÎncă nu există evaluări
- Drug Study On Emergency Drugs Final - )Document12 paginiDrug Study On Emergency Drugs Final - )wen_pil100% (3)
- Tatalaksana Krisis HipertensiDocument38 paginiTatalaksana Krisis HipertensiDr Edi HidayatÎncă nu există evaluări
- NCP AccDocument19 paginiNCP AccAthyrah KadirÎncă nu există evaluări
- Ischaemic Heart DiseaseDocument30 paginiIschaemic Heart DiseaseEBÎncă nu există evaluări
- Terapia Sistémica en Carcinoma Metastásico de Colon Y Recto: Mauricio Lema Medina MDDocument14 paginiTerapia Sistémica en Carcinoma Metastásico de Colon Y Recto: Mauricio Lema Medina MDapi-26302710Încă nu există evaluări
- Post ASCO2009Document51 paginiPost ASCO2009api-26302710Încă nu există evaluări
- GCis in Bladder Cancer 2006Document5 paginiGCis in Bladder Cancer 2006api-26302710Încă nu există evaluări
- PACCE01Document9 paginiPACCE01api-26302710Încă nu există evaluări
- Everolimus RCCDocument8 paginiEverolimus RCCapi-26302710Încă nu există evaluări
- CLAGDocument8 paginiCLAGapi-26302710Încă nu există evaluări
- Ncologist: R I FDADocument7 paginiNcologist: R I FDAapi-26302710Încă nu există evaluări
- Adjuvant Imatinib GISTDocument8 paginiAdjuvant Imatinib GISTapi-26302710Încă nu există evaluări
- Terapia Sistémica en Carcinoma Metastásico de Colon Y Recto: Mauricio Lema Medina MDDocument14 paginiTerapia Sistémica en Carcinoma Metastásico de Colon Y Recto: Mauricio Lema Medina MDapi-26302710Încă nu există evaluări
- Vorinostat CTCLLandmark Study 02Document7 paginiVorinostat CTCLLandmark Study 02api-26302710Încă nu există evaluări
- Mycosis Fungoides and Sézary Syndrome: SeminarDocument13 paginiMycosis Fungoides and Sézary Syndrome: Seminarapi-26302710Încă nu există evaluări
- IL2 in MRCCDocument9 paginiIL2 in MRCCapi-26302710Încă nu există evaluări
- Beethoven Piano Sonata Op. 57 N. 23Document29 paginiBeethoven Piano Sonata Op. 57 N. 23GiancarloÎncă nu există evaluări
- For Refractory Cutaneous T-Cell Lymphoma (CTCL) Phase 2 Trial of Oral Vorinostat (Suberoylanilide Hydroxamic Acid, SAHA)Document10 paginiFor Refractory Cutaneous T-Cell Lymphoma (CTCL) Phase 2 Trial of Oral Vorinostat (Suberoylanilide Hydroxamic Acid, SAHA)api-26302710Încă nu există evaluări
- Letters: Epigenetic Silencing of Tumour Suppressor Gene p15 by Its Antisense RNADocument6 paginiLetters: Epigenetic Silencing of Tumour Suppressor Gene p15 by Its Antisense RNAapi-26302710Încă nu există evaluări
- Letters: Carcinoma-Produced Factors Activate Myeloid Cells Through TLR2 To Stimulate MetastasisDocument6 paginiLetters: Carcinoma-Produced Factors Activate Myeloid Cells Through TLR2 To Stimulate Metastasisapi-26302710Încă nu există evaluări
- Nature 07762Document6 paginiNature 07762api-26302710Încă nu există evaluări
- Nature 07423Document7 paginiNature 07423api-26302710Încă nu există evaluări
- Letters: Regulation of ERBB2 by Oestrogen receptor-PAX2 Determines Response To TamoxifenDocument6 paginiLetters: Regulation of ERBB2 by Oestrogen receptor-PAX2 Determines Response To Tamoxifenapi-26302710Încă nu există evaluări
- Nature 07485Document7 paginiNature 07485api-26302710Încă nu există evaluări
- EditorialDocument1 paginăEditorialapi-26302710Încă nu există evaluări
- Aldesleukin For Injection RX Only: DescriptionDocument16 paginiAldesleukin For Injection RX Only: Descriptionapi-26302710Încă nu există evaluări
- Nature 07385Document8 paginiNature 07385api-26302710Încă nu există evaluări
- Nature 07567Document7 paginiNature 07567api-26302710Încă nu există evaluări
- Ncologist: T C O D O F SDocument12 paginiNcologist: T C O D O F Sapi-26302710Încă nu există evaluări
- Proleukin Melanoma Evidencia en 270 Pacientes Con Dosis AltasDocument12 paginiProleukin Melanoma Evidencia en 270 Pacientes Con Dosis Altasapi-26302710Încă nu există evaluări
- Guidelines Interleukin-2 For Safe AdministrationDocument7 paginiGuidelines Interleukin-2 For Safe Administrationapi-26302710Încă nu există evaluări
- CaScreening2009 01Document16 paginiCaScreening2009 01api-26302710Încă nu există evaluări
- Neo Adjuvant CTin LACervical CancerDocument10 paginiNeo Adjuvant CTin LACervical Cancerapi-26302710Încă nu există evaluări
- ASYNCHRONOUS-ACTIVITY-Module 1Document7 paginiASYNCHRONOUS-ACTIVITY-Module 1Grant Wynn ArnucoÎncă nu există evaluări
- Points To Be DiscussedDocument4 paginiPoints To Be DiscussedShalini ShekharÎncă nu există evaluări
- High PlateletsDocument9 paginiHigh PlateletsHemal VyasÎncă nu există evaluări
- Predictive Models Receiver-Operating Characteristic Analysis For Evaluating Diagnostic Tests andDocument5 paginiPredictive Models Receiver-Operating Characteristic Analysis For Evaluating Diagnostic Tests andLucila Figueroa GalloÎncă nu există evaluări
- StoryDocument6 paginiStoryGerard NicholasÎncă nu există evaluări
- The Dandenong Dossier 2010Document243 paginiThe Dandenong Dossier 2010reshminÎncă nu există evaluări
- MfA Leadership ExperienceDocument49 paginiMfA Leadership ExperienceAlex MoralesÎncă nu există evaluări
- Catalogo Baby MarketDocument53 paginiCatalogo Baby Marketmiguel quispeÎncă nu există evaluări
- M Fajar Alwi Muchsin - D3TGDocument7 paginiM Fajar Alwi Muchsin - D3TGNugi AshterÎncă nu există evaluări
- PDF 20221013 211252 0000Document1 paginăPDF 20221013 211252 0000Meann جرابيللوÎncă nu există evaluări
- Mira Nepali CV OnlyDocument3 paginiMira Nepali CV OnlydistanceindistanceÎncă nu există evaluări
- Govindarajan Reverse Innovation Chapter1Document10 paginiGovindarajan Reverse Innovation Chapter1hvactrg1Încă nu există evaluări
- Therapy Is For Everybody: Black Mental HealthDocument22 paginiTherapy Is For Everybody: Black Mental HealthIresha Picot100% (2)
- Unit 1 - Task 3 - Comprehension Quiz - Evaluation QuestionnaireDocument9 paginiUnit 1 - Task 3 - Comprehension Quiz - Evaluation QuestionnaireAleja OrozcoÎncă nu există evaluări
- WONCA2013 - Book of Abstracts PDFDocument830 paginiWONCA2013 - Book of Abstracts PDFBruno ZanchettaÎncă nu există evaluări
- Mastertile A 200 Msds PDFDocument11 paginiMastertile A 200 Msds PDFyaswanth reddy mummadiÎncă nu există evaluări
- DMF 40 199 PDFDocument14 paginiDMF 40 199 PDFsiraj_khan_13Încă nu există evaluări
- STEVENS DRRR Module 6 Opon Christian Joy ADocument7 paginiSTEVENS DRRR Module 6 Opon Christian Joy AAnthony Bryan Cartujano100% (1)
- Sacrococcygeal TeratomaDocument21 paginiSacrococcygeal TeratomaEm VelascoÎncă nu există evaluări
- Philippine Science and Technology InnovationDocument7 paginiPhilippine Science and Technology Innovationgabosara298Încă nu există evaluări
- Nexus Magazine AprilMay 2019Document100 paginiNexus Magazine AprilMay 2019Izzy100% (2)
- Good Knight 420 GPatien ManualDocument30 paginiGood Knight 420 GPatien ManualJose Antonio AlcazarÎncă nu există evaluări
- Book StickerDocument4 paginiBook Stickerilanabiela90Încă nu există evaluări
- Bakery Business PlanDocument31 paginiBakery Business PlanRohit Gupta93% (14)
- P1 Cri 089Document2 paginiP1 Cri 089Joshua De Vera RoyupaÎncă nu există evaluări
- Iriga Zone Ibd List: Nabua ADocument20 paginiIriga Zone Ibd List: Nabua AAnonymous dPCnM2a1Încă nu există evaluări
- Vince Gironda 8x8 RoutineDocument10 paginiVince Gironda 8x8 RoutineCLAVDIVS0% (2)
- Amy L. Lansky - Impossible Cure - The Promise of HomeopathyDocument295 paginiAmy L. Lansky - Impossible Cure - The Promise of Homeopathybjjman88% (17)
- Chevron Phillips Chemical Company Issued Sales SpecificationDocument1 paginăChevron Phillips Chemical Company Issued Sales SpecificationSarmiento HerminioÎncă nu există evaluări
- UNSAFE aCTS & UNSAFECONDITIONDocument48 paginiUNSAFE aCTS & UNSAFECONDITIONSn CarbonelÎncă nu există evaluări