Documente Academic
Documente Profesional
Documente Cultură
Copd /pulmonary Board Review
Încărcat de
AzmachamberAzmacare0 evaluări0% au considerat acest document util (0 voturi)
66 vizualizări68 paginiPulmonary
Titlu original
Copd /Pulmonary Board review
Drepturi de autor
© © All Rights Reserved
Formate disponibile
PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentPulmonary
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
66 vizualizări68 paginiCopd /pulmonary Board Review
Încărcat de
AzmachamberAzmacarePulmonary
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 68
ACC
8oard kev|ew 2011
CCD art II
S|dney S. 8raman MD ICC
rov|dence, kI
D|sc|osures
ConsulLanL Sunovlon, 8l, loresL
non-promouonal Speaker CSk, CenenLech
uesnon 1
A 4S year o|d man |s smok|ng 1 pack of c|gareues a day. ne adm|ts
to chron|c da||y cough and sputum producnon. ne |s GCLD stage II
CCD
Wh|ch of the fo||ow|ng statements about h|m |s true?
a) Pe ls more suscepuble Lo exacerbauons because of hls
chronlc bronchlus sympLoms
b) Pls sympLoms predlcL emphysemaLous changes on hls
chesL radlograph
c) Pls sympLoms (cough and phlegm) do noL predlcL fuLure
dlsease progresslon
d) unreporLed exacerbauons of chronlc bronchlus are
common buL Lhey do noL have a slgnlcanL lmpacL on a
pauenLs quallLy of llfe
Iactors Assoc|ated W|th Increased k|sk
for Lxacerbanons
lncreased age
SeverlLy of alrway obsLrucuon
(lLv
1
lmpalrmenL)
Chronlc bronchlal mucous
hypersecreuon
Longer durauon of CCu
roducuve cough and wheeze
LlevaLed cough and spuLum
Anublouc or sysLemlc corucosLerold use
ln Lhe pasL year
rlor use of medlcauons for CCu
8acLerlal colonlzauon
Comorbld condluons
(e.g., cardlovascular dlsease)
oor healLh-relaLed quallLy of llfe
.
LCLISL: Iactors Assoc|ated W|th Increased
Lxacerbanon Irequency
5.72
1.11
1.07
2.07
1.08
0
1
2
3
4
5
6
7
Exacerbation During
Previous Year
FEV (per 100 mL
decrease)
SGRQ Score (per 4 point
increase)
Positive History for
Reflux/Heartburn
White Cell Count (per
increase of 1000/mL)
1
O
d
d
s
R
a
t
i
o
f
o
r
!
2
v
e
r
s
u
s
0
E
x
a
c
e
r
b
a
t
i
o
n
s
P<0.001
P<0.001
P<0.001
P<0.001
P=0.002
N=2138
Hurst JR, et al. N Engl J Med. 2010;363:1128-1138.
L|evated Lxacerbanon k|sk Assoc|ated W|th
Cough and Sputum roducnon
*
* P<0.0001
P
e
r
c
e
n
t
w
i
t
h
!
2
E
x
a
c
e
r
b
a
t
i
o
n
s
p
e
r
Y
e
a
r
Burgel P-R, et al. Chest. 2009;135:975-982.
Lar|y Chron|c 8ronch|ns Symptoms Are
red|cnve of D|sease rogress|on
Guerra S, et al. Thorax. 2009;64:894-900. Permission requested.
Years of Follow-up
0 5 10 15 20 25 30
C
u
m
u
l
a
t
i
v
e
S
u
r
v
i
v
a
l
C
u
r
v
e
s
f
o
r
A
l
l
-
C
a
u
s
e
M
o
r
t
a
l
i
t
y
0.0
0.2
0.4
0.6
0.8
1.0
Age < 50 years
No C. Bronchitis
(N = 653)
Age < 50 years
C. Bronchitis
(N = 46)
Age ! 50 years
No C. Bronchitis
(N = 661)
Age ! 50 years
C. Bronchitis
(N = 51)
Anthonisen NR, et al. Am Rev Respir Dis. 1986;133:14-20.
ke|anonsh|p 8etween Lung Iuncnon
and Morta||ty
1
2
Years
100
90
80
70
60
0
3
FEV
1
Normals
!50%
40-49%
30-39%
<30%
%
s
u
r
v
i
v
i
n
g
Surv|va| by Lung Iuncnon Impa|rment
GOLD 3/4
GOLD 2
GOLD 1
No Lung Disease
Restrictive Disease
GOLD 0
Mannino et al, Thorax 2003;58:388-393
Follow up in Years
20 10 0
P
r
o
p
o
r
t
i
o
n
S
u
r
v
i
v
i
n
g
1.0
.8
.6
.4
.2
0.0
CCD Sever|ty C|ass|hcanon
u|monary and System|c Lects
8CDL
8ody-Mass Index
Degree of A|row Cbstrucnon
Dyspnea
Lxerc|se Capac|ty Index
Celli et al NEJM 2004350:1005-12
FEV
1
Stage BODE
Months
1.0
0.8
0.6
0.4
0.2
0.0
0 4 8 12 16 20 24 28 32 36 40 44 48 52 0 4 8 12 16 20 24 28 32 36 40 44 48 52
Stage I (> 50%) predicted
Stage II (36-50%) predicted
Stage III (! 35%) predicted
Quartile 1 (BODE 0-2)
Quartile 2 (BODE 3-4)
Quartile 3 (BODE 5-6)
Quartile 4 (BODE 7-10)
P
r
o
b
a
b
i
l
i
t
y
o
f
s
u
r
v
i
v
a
l
P<0.001 P<0.001
Celli BR, et al. N Engl J Med. 2004;350:1005-1012.
Surv|va| |n CCD
uesnon 2
A 63 year old man, smoker of 1-2 packs of clgareues a day,
has CCLu SLage lll CCu. Pe complalns of chronlc cough
and dyspnea and has 2-3 exacerbauons of hls sympLoms
each year LreaLed aL home wlLh oral anubloucs and
corucosLerolds. Whlch sLaLemenL ls Lrue abouL Lhls man?
uesnon 2
Wh|ch statement |s correct?
a) unllke asLhma, bacLerlal lnfecuons and noL vlral lnfecuons
are Lhe cause of hls exacerbauons
b) 1he frequency of hls exacerbauons ls llkely Lo worsen as hls
lung funcuon deLerloraLes
c) 8ecovery of lung funcuon buL noL sympLoms occurs wlLhln
Lhe rsL week followlng an exacerbauon
d) 8CuL lndex wlll predlcL severlLy and noL frequency of
exacerbauons
Lp|dem|o|ogy of Lxacerbanons:
Irequency Increases w|th Dec||n|ng ILV
1
Donaldson GC, Wedzicha JA. Thorax. 2006;61:164-168.
FEV
1
(1)
2.5
2.0
0.5
0
< 1.25 1.25 1.54 > 1.54 2.40
3.0
1.5
E
x
a
c
e
r
b
a
t
i
o
n
s
p
e
r
Y
e
a
r
2.50
1.0
Irequent Lxacerbanons Are Assoc|ated W|th
More kap|d Dec||ne |n u|monary Iuncnon
*
-40.1
-2.94
-32.1
-0.72
-45
-40
-35
-30
-25
-20
-15
-10
-5
0
Frequent Exacerbators
Infrequent
Exacerbators
FEV
1
(mL) PEF (L/minute)
A
n
n
u
a
l
C
h
a
n
g
e
**
* P<0.05 versus infrequent exacerbators; ** P<0.001 versus infrequent exacerbators
Donaldson GC, et al. Thorax. 2002;57:847-852.
Lno|ogy of ALCCD
Papi A, et al. Am J Respir Crit Care Med. 2006;173:1114-21.
Causes of exacerbations requiring hospitalization in patients (N=64)
23.4%
21.8%
25.0%
29.7%
Bacteria
Bacteria
and Virus
Virus
Non-infectious
Inc|dence of V|rus Detecnon W|th Ck
|n Adu|t opu|anons
Population
Virus General Adult High Risk COPD Inpatient COPD ICU COPD
RSV 4.5-11.6% 4.3-12.0% 2.6-15.3% 6.5%
Influenza A 18.4% 3.4% 15.6-17.6% 13.1%
Influenza B 1.9% NR 4.7% 5.6%
Rhinovirus 10.5% 25.6% 11.7-24.7% 6.5%
Coronavirus 0.8% 8.5% 7.8% 2.8%
Parainfluenza 1.1% 5.1% 3.9% 10.3%
Metapneumovirus 1.5-3.4% 0% 0% 2.8%
Adenovirus 0.8% 0% 1.3% NR
NR = not reported
Adapted from Ramaswamy M, et al. COPD. 2009;Feb:64-75.
V|ra| Infecnon and the CCD Lxacerbanon
lnvesugaLed Lhe role of vlral lnfecuon ln Lhe exacerbauon of
CCu uslng C8 Lechnology
39 were assoclaLed wlLh vlral lnfecuon
lnammaLory markers hlgh (lL-6, brlnogen)
vlral lnfecuons assoclaLed wlLh more severe sympLoms and
longer durauon of lllness (13 d)
8hlnovlrus was predomlnanL vlrus (38)
Seemungal et al AJRCCM 2001; 164:1618-1623
kecovery Irom Lxacerbanons:
V|ra| Versus Non-v|ra|
Non-Viral Exacerbation
Viral Exacerbation
80
0
0
100
40
20
10 20 30 40
Days from Onset of Exacerbation
50 60
%
E
x
a
c
e
r
b
a
t
i
o
n
s
R
e
c
o
v
e
r
e
d
60
P=0.006 for viral versus non-viral infections
. Seemungal T, et al. 2001. . American Journal of Respiratory and Critical Care Medicine. 164:1618-1623.
kesp|ratory Syncyna| V|rus (kSV) I||ness |n the
L|der|y
rospecuve sLudy of healLhy and hlgh-rlsk elderly (chronlc hearL and
lung dlsease)
8Sv developed annually ln 3-7 percenL of healLhy & 4-10 percenL of
hlgh-rlsk adulLs
8Sv was ldenued ln 142 and lnuenza A ln134 hosplLallzed pauenLs.
(n=1388)
8Sv and lnuenza A resulLed ln slmllar LCS, lCu use and morLallLy (8
vs 7)
8Sv lnfecuon accounLed for 10.6 of hosplLallzauons for pneumonla
& 11.4 CCu
Falsey AR et al NEJM 2005;352:1749-1759
In Stab|e CCD n|gh resence of kSV Is Assoc|ated
W|th More kap|d Dec||ne |n ILV
1
A
n
n
u
a
l
D
e
c
l
i
n
e
i
n
F
E
V
1
(
m
L
/
y
e
a
r
)
*
* P=0.01 versus lower RSV
Wilkinson TM, et al. Am J Respir Crit Care Med. 2006;173:871-876.
D
a
i
l
y
M
e
d
i
a
n
P
E
F
R
a
s
%
B
a
s
e
l
i
n
e
u|monary Iuncnon kecovers S|ow|y
Aher an Lxacerbanon
Seemungal TA, et al. Am J Respir Crit Care Med. 2000;161:16081613.
Days
100
99
96
95
-14
101
98
97
-9 -4 1 6 11 16 21 26 31
Exacerbation
1|me Course and kecovery of anents W|th
CCD Lxacerbanon
Medlan recovery of Ll8 paralleled sympLom recovery 6-7
days
AL day 33, Ll8 reLurned Lo normal ln 73 of pauenLs, 86
aualned sympLomauc recovery
AL 90 days, 7 had noL reLurned Lo Ll8 basellne
CreaLer dyspnea and falls ln l1s as well as colds aL onseL
of exacerbauon are assoclaLed wlLh longer recovery umes.
Seemungal et.al. Am J Resp Crit Care Med 2000;161:1608-1613
1he 8ody Mass Index, Cbstrucnon, Dyspnea,
Lxerc|se Capac|ty (8CDL) Index red|cts
Lxacerbanon Irequency
Hodgev VA, et al. Folia Med . 2006;48:18-22.
M
e
a
n
B
O
D
E
I
n
d
e
x
S
c
o
r
e
P=0.002
_
_
0
1
2
3
4
5
6
7
8
9
Frequent Exacerbators Infrequent Exacerbators
0.0
0.2
0.4
0.6
0.8
1.0
0 10 20 30 40 50 60
Time (months)
P
r
o
b
a
b
i
l
i
t
y
o
f
s
u
r
v
i
v
i
n
g
p<0.0001
p<0.001
p=0.07
34 exacerbations
12 exacerbations
No exacerbation
CCD Lxacerbanons: Impact Surv|va|
Soler-Catalua JJ et al. Thorax. 2005;64:925-31
uesnon 3
Wh|ch of the fo||ow|ng therapeunc measures has no
|mprovement on year|y exacerbanon rate?
a) lnhaled corucosLerold
b) Cral corucosLerold
c) Long Lerm anublouc prophylaxls
d) neumococcal vacclne
e) 8oumllasL
Inuenza Vacc|nanon: k|sk for Any
Lxacerbanon
Lvaluauon of resulLs from randomlzed cllnlcal Lrlals lndlcaLes LhaL
lnacuvaLed lnuenza vacclne reduces exacerbauons ln CCu
pauenLs
1he magnlLude of Lhls beneL ls slmllar Lo LhaL seen ln large
observauonal sLudles, and was due Lo a reducuon ln
exacerbauons occurrlng Lhree or more weeks aer vacclnauon,
and due Lo lnuenza
1here ls a mlld lncrease ln LranslenL local adverse eecLs wlLh
vacclnauon, no evldence of lncrease ln early exacerbauons
Poole PJ, et al. Cochrane Database Syst Rev. 2006;CD002733.
Relative Risk (95% CI)
COPD hospitalization
All-cause mortality
COPD hospitalization
All-cause mortality
Pneumococcal vaccination
Pneumococcal + influenza
vaccination
0 0.2 0.4 0.6 0.8 1 1.2 1.4 1.6 1.8 2.0
neumococca| and Inuenza Vacc|nanons
keduce CCD Lxacerbanons
Nichol et al. Arch Intern Med. 1999;159:2437-2442
neumococca| Vacc|nanon |n CCD
neumon|a kates Improved |f <6S yrs and ILV1 <40
Alfageme I, et al. Thorax. 2006;61:189-195.
C
u
m
m
u
l
a
t
i
v
e
P
r
o
p
o
r
t
i
o
n
o
f
P
a
t
i
e
n
t
s
W
i
t
h
o
u
t
P
n
e
u
m
o
n
i
a
Log rank = 6.68
P=0.0097
Time (days)
1.00
0.90
0 250 750 1250
0.95
0.80
0.85
0.75
0.70
500 1000
Vaccinated = 91
Control = 116
C
u
m
m
u
l
a
t
i
v
e
P
r
o
p
o
r
t
i
o
n
o
f
P
a
t
i
e
n
t
s
W
i
t
h
o
u
t
P
n
e
u
m
o
n
i
a
Log rank = 3.85
P=0.0498
Time (days)
1.00
0.90
0 300 900 1500
0.95
0.80
0.85
0.75
0.70
600 1200
Vaccinated = 132
Control = 114
Age <65
FEV1 <40%
ICS Decreases Lxacerbanon k|sk
Burge PS, et al. BMJ. 2000;320:1297-1303.
A
n
n
u
a
l
E
x
a
c
e
r
b
a
t
i
o
n
R
a
t
e
* P=0.026 versus placebo
*
0.99
1.32
1.4
1.2
1.0
0.8
0.6
0.4
0.2
0
Fluticasone Placebo
1CkCn: Lower Lxacerbanon kate W|th
LA8A |us ICS
Calverley PM, et al. N Engl J Med. 2007;356:775-789.
* P<0.05 versus placebo
*
*
*
*
*
*
*
*
1.13
0.8
0.19
0.97
0.64
0.16
0.93
0.52
0.17
0.85
0.46
0.16
0
0.2
0.4
0.6
0.8
1
1.2
Moderate or Severe Requiring Systemic
Steroids
Requiring
Hospitalization
A
n
n
u
a
l
R
a
t
e
Placebo (N=1524)
Salmeterol (N=1521)
Fluticasone (N=1534)
Combination Therapy
(N=1533)
1|otrop|um Decreases k|sk for
Lxacerbanons
Casaburi R, et al. Eur Respir J. 2002;19:217-224.
* P=0.045 versus placebo
*
0.76
0.95
1.0
0.9
0.8
0.7
0.6
0.5
0.4
0.3
0.2
0.1
0
E
x
a
c
e
r
b
a
t
i
o
n
s
p
e
r
P
a
t
i
e
n
t
-
Y
e
a
r
Tiotropium Placebo
Hazard ratio = 0.86,
(95% CI = 0.81, 0.91)
P<0.0001 (log-rank test)
Months
Tiotropium
Control
0
20
40
60
80
0 6 12 18 24 30 36 42 48
P
r
o
b
a
b
i
l
i
t
y
o
f
e
x
a
c
e
r
b
a
t
i
o
n
(
%
)
0.85/yr
0.73/yr; P<0.001
(14% reduction)
ULII1 Study - Lects on Lxacerbanons
Tashkin DP, et al. N Engl J Med. 2008;359:1543-1554.
37
Annb|onc rophy|ax|s keduces
Lxacerbanons
Suzuki T, et al. Chest. 2001;120:730-733.
60
P
e
r
c
e
n
t
o
f
P
a
t
i
e
n
t
s
w
i
t
h
E
x
a
c
e
r
b
a
t
i
o
n
*
* P<0.007 versus control
11
56
40
30
20
10
0
Erythromycin Control
50
Macro||des revents CCD Lxacerbanons
Seemungal TAR, et al. AJRCCM 2008
Median time to 1
st
exacerbation
271 days Macrolide; 89 days Placebo
Proportion of Participants Free from
Acute Exacerbations of
COPD for 1 Year
Albert RK et al NEJM 2011
Median time to exacerbation
266 Azithro 174 Placebo
-21%
(CI -31;-9)
P=0.0011
Mean rate
exacerbations
(moderate or
severe)
per patient
per year
*Hanania et al. Am J Respir Crit Care Med 2010;181:A4435
Fabbri et al Lancet 2009;374:695-703.
koum||ast S|gn|hcant|y keduces
Lxacerbanons When Added to LA8A*
CCD 1herapy 8y Stage
0 1-Mild 2-Mod 3-Severe 4-Very Sev
At risk FEV
1
! 80% FEV
1
! 50% FEV
1
! 30% FEV
1
< 30%
Avoid risk factors; yearly flu shot
PRN /
SABD
PRN / Reg
SABD
PRN / Reg
SABD
PRN / Reg
SABD
Albuterol
Ipratropium
Combination
+ LABD
(TIO / LABA) +
REHAB
+ LABD
(TIO / LABA) +
REHAB
+ LABD
(TIO / LABA)
+ REHAB
+ ICS + ICS +PDE-4
+ O
2
/LVRS?
GOLD 20013
uesnon 4
A 6S year o|d panent w|th GCLD Stag III CCD has [ust been entered
|nto a pu|monary rehab|||tanon program. Wh|ch of the fo||ow|ng |s
an un||ke|y outcome of th|s program?
a. 8educed rlsk of unplanned admlsslon
b. 8educed hosplLallzauon readmlsslon raLes
c. lmprovemenL ln lvC and lLv1
d. lmprovemenL ln walklng ume
Lects of u|monary kehab|||tanon aher
nosp|ta| Adm|ss|on for an Lxacerbanon
7
20
33
23
0
5
10
15
20
25
30
35
Hospital Admission for Exacerbation ED Visit for Exacerbation
PEPR (n=30)
Usual Care (n=30)
P
e
r
c
e
n
t
o
f
P
a
t
i
e
n
t
s
P=0.02
PEPR = post-exacerbation pulmonary rehabilitation Seymour JM, et al. Thorax. 2010;65:423-428.
u|monary kehab|||tanon
Overall (47/46)
Risk ratio (95% CI)
0.17 (0.04 to 0.69)
0.40 (0.09 to 1.70)
1.5
Risk of unplanned
hospital admission
.5 1 .25
Favours usual care Favours rehabilitation
.75
Study
(rehabilitation/
usual care group)
Man (20/21)
Murphy (13/13)
Length of
follow-up
3 months
6 months
Weight in %
44%
19%
0.29 (0.10 to 0.82) Behnke (14/12) 18 months 37%
0.26 (0.12 to 0.54)
Chi-Squared 0.70, p=0.71
Puhan MA, et al. Respir Res. 2005;6:54.
u|monary kehab|||tanon:
Lects on anent Acnv|ty
Pitta F, et al. Chest. 2008 ;134:273-280.
7%
20%
0%
10%
20%
30%
40%
50%
3 Months 6 Months
I
m
p
o
r
v
e
m
e
n
t
f
r
o
m
B
a
s
e
l
i
n
e
i
n
D
a
i
l
y
W
a
l
k
i
n
g
T
i
m
e
*
* P=0.008 versus baseline
u|monary kehab|||tanon
8eneLs all levels of dlsease severlLy
8educes resplraLory sympLoms
8educes anxleLy and depresslon
8educes medlcal and hosplLal usage
lmproves exerclse performance
lmproves quallLy of llfe
ls Lyplcally provlded as ouLpauenL
Can be lnluaLed as an lnpauenL unul funcuonal ablllLy has lmproved
uesnon S
Wh|ch of the fo||ow|ng statements about system|c |nammanon and
CCD |s correct?
a) SysLemlc markers of lnammauon are elevaLed only ln
CCLu lll and lv CCu (severe and very severe)
b) MeLabollc syndrome ls rare ln CCu pauenLs because mosL
pauenLs have conslderable welghL loss
c) Smokers wlLh and wlLhouL CCu have slmllarly elevaLed
levels of C8
d) CsLeoporosls ln pauenLs wlLh CCu correlaLes wlLh Lhe
degree of sysLemlc lnammauon
System|c Inammanon and |ts Consequences |n
CCD
SysLemlc lnammauon rlses wlLh CCu severlLy
LlevaLed levels of C8, lL-6 llbrlnogen, 1nl" W8Cs
Comorbldlues ln CCu
MeLabollc Abnormallues ln CCu
Cardlovascular ulsease
CsLeoporosls
CasLrolnLesunal ulsease
SkeleLal Muscle uysfuncuon
Anemla of Chronlc ulsease
Angina
Cataracts
Respiratory Infection
Myocardial Infarction
Fractures
Osteoporosis
Glaucoma
Skin Bruises
Soriano et al. Chest. 2005;128:2099-2107.
!
!
!
!
!
!
!
!
RR in COPD versus non-COPD
R
a
t
e
p
e
r
1
0
,
0
0
0
4 3 2 0 1
0
100
200
300
400
Pneumonia !
CCD Increases k|sk for Med|ca| Lvents
37
25
22.5
19
13
12
11
5
22
14
10
12
8.5
6.5
10
3
0
5
10
15
20
25
30
35
40
RF Pneumonia Heart Failure IHD Hypertension TM Diabetes PVD
I
n
H
o
s
p
i
t
a
l
M
o
r
t
a
l
i
t
y
(
a
s
%
o
f
d
i
s
c
h
a
r
g
e
s
)
COPD
No COPD
Holguin et al. Chest. 2005;128:2005-2011.
IHD = ischaemic heart disease, CHF =
congestive heart failure, RF = respiratory
failure, PVD = pulmonary vascular disease,
TM = thoracic malignancy
Death Due to Co-Morb|d|nes |s More
Common |n CCD
System|c Inammanon k|ses
w|th CCD Sever|ty
Franciosi et al. Pulm Pharmacol Ther. 2006;19:189-199.
CRP TNF-!
Severe
COPD
Moderate
COPD
Mild
COPD
Healthy
0
Serum C-Reactive Protein (mg/L)
20 30 40 50 60 70 10
Severe
COPD
Moderate
COPD
Mild
COPD
Healthy
0 40 100 60 80 20
Serum TNF-Alpha (pg/mL)
*
* P<.05 versus other groups
Pinto-Plata et al. Thorax. 2006;61:23-8.
Ck |s L|evated |n anents w|th CCD
versus Smokers and Nonsmokers
Sin et al. Am J Med. 2003;114:10-14.
A|row Cbstrucnon and Csteoporos|s |n
CCD
Kim B-J, et al. Clin Endocrinol. 2007;67:152-158.
NTx=N-terminal telopeptide of type I collagen, BCE=bone collagen equivalent
0-50 0-00 0-50 1-00
150-50
100-50
50-50
0-50
Log
10
hsCRP (mg1)
U
r
i
n
a
r
y
N
T
x
(
n
M
B
C
E
/
u
)
*"=0-288, P<0-001
Premenopausal
Women
0-10
0-00
0-10
0-20
Normal
(N = 30)
Osteoporia
(N = 109)
Osteoporosis
(N = 50)
P for trend = 0-282
L
o
g
1
0
h
s
C
R
P
(
m
g
1
)
8one 1urnover and Csteoporos|s
are Corre|ated w|th Inammanon
Severe COPD Use of ICS
Adjusted Odds Ratio
for Osteoporotic
Fracture
No No 1.06
No Yes 1.08
Yes No 1.47*
Yes Yes 1.48*
* P<.05
De Vries et al. Eur Respir J. 2005;25:879-884.
CCD, ICS, and Csteoporonc Iracture
Systemic
*
*
McEvoy et al. Am J Resp Crit Care Med. 1998;157:704-709.
* P<.05 versus no corticosteroid
Inha|ed versus Cra| Corncostero|d Use
and Iracture k|sk |n CCD
49
50
51
52
53
54
55
COPD (N=40) No COPD (N=46)
F
a
t
-
f
r
e
e
M
a
s
s
(
k
g
)
Iat-free Mass |s keduced |n CCD
Sergi et al. Respir Med. 2006;100:1918-1924.
*
* P<0.05
50.7
53.9
CHI = creatine height index, a measure of skeletal muscle mass, Normal CHI #80% predicted, Low CHI <80% predicted
* P<.05 for between-group difference
"
*
*
Eid et al. Am J Respir Crit Care Med. 2001;164:1414-1418.
ke|anonsh|p between Ske|eta| Musc|e Mass
and Inammatory Markers |n CCD
*
* P<.05 vs no COPD
Rana et al. Diabetes Care. 2004;27:2478-2484.
reva|ence of D|abetes n|gher |n anents
w|th CCD
*
* P=0.032 vs no COPD
Bolton CE, et al. COPD. 2007;4:121-126.
1.68
1.13
0
0.2
0.4
0.6
0.8
1
1.2
1.4
1.6
1.8
COPD (n=56) No COPD (n=29)
H
O
M
A
I
n
s
u
l
i
n
R
e
s
i
s
t
a
n
c
e
Insulin resistance was significantly correlated with
circulating TNF-" and IL-6
Insu||n kes|stance |s L|evated |n CCD anents and
Corre|ated w|th Inammatory Markers
* MeLabollc syndrome #3 of Lhe followlng: abdomlnal obeslLy, elevaLed
Lrlglycerldes, reduced PuL-C, hyperLenslon, hyperglycaemla
Marquis et al. J Cardiopulm Rehabil. 2005;25:226-232.
reva|ence of Metabo||c Syndrome n|gher
|n CCD
System|c Inammanon and Increased k|sk of
Card|ovascu|ar D|sease
0
1
2
3
4
5
6
7
Sin DD & Man SF. Circulation 2003; 107: 15141519.
C
a
r
d
i
a
c
I
n
f
a
r
c
t
i
o
n
I
n
j
u
r
y
S
c
o
r
e
High CRP
No Obstruction
Low CRP
Moderate
Obstruction
High CRP
Moderate
Obstruction
Low CRP
Severe
Obstruction
High CRP
Severe
Obstruction
P for Trend = 0.001
CRP = C-Reactive Protein
uesnon 6
A SS year o|d obese man presents w|th |ncreas|ng dyspnea and ank|e
swe|||ng (k greater than L). u|monary funcnon tests show that he
|s GCLD Stage II w|th an ILV1 of 2.2 ||ters. Arter|a| b|ood gases show
a pn of 7.37 aCC2 of SS and a aC2 of 68. What |s the most ||ke|y
cause of h|s worsen|ng dyspnea?
a) CCu
b) CbsLrucuve Sleep Apnea
c) ulmonary embollc dlsease
d) Comblned ulmonary llbrosls and Lmphysema Syndrome
our patient
ke|anonsh|p between ILV
1
and aCC
2
|eve|
|n CCD
S|eep-d|sordered breath|ng and CCD: 1he over|ap
syndrome
More severe nocLurnal hypoxemla Lhan elLher dlsease
alone.
auenLs wlLh CCu and CSA have a subsLanually greaLer
rlsk of morbldlLy and morLallLy, compared Lo Lhose wlLh
elLher CCu or CSA alone.
lmproved survlval and reduced exacerbauons ln pauenLs
wlLh Lhe over|ap syndrome who are LreaLed wlLh
conunuous posluve alrway pressure
Marin JM et alAm J Respir Crit Care Med. 2010;182:325-31.
Todd N et al Fibrogenesis Tissue Repair. 2011; 4: 6
Comb|ned u|monary I|bros|s and Lmphysema
Syndrome-beuer prognos|s than II?
CenLrllobular and/or parasepLal
emphysemas ln upper lung zones
coexlsL wlLh pulmonary brosls
lnlower lobes ln lndlvlduals
Men >40 pack years, exposure Lo
agrochemlcal compounds
Assoclauons: C1 dlsease (8A, sysLemlc
sclerosls, mlxed C1 dlsease) pulmonary
hyperLenslon, lung cancer,
Lung volumes may be nl., uLCC very
low, exerclse hypoxemla
u|monary nypertens|on |n CCD
rlmarlly due Lo hypoxlc vasoconsLrlcuon of small pulmonary arLerles
LhaL evenLually resulLs ln sLrucLural changes lncludlng lnumal
hyperplasla and smooLh muscle hyperLrophy and hyperplasla
non-hypoxemlc facLors may also conLrlbuLe
elevaLed pulmonary caplllary wedge pressure (from dlasLollc le venLrlcular
dysfuncuon
gas Lrapplng wlLh lncreased lnLra-Lhoraclc pressure
sysLemlc lnammauon wlLh vascular remodellng
emphysema-assoclaLed caplllary loss.
small vessel vascular abnormallues occur very early ln Lhe course of Lhe dlsease
and may lead Lo large vessel remodellng
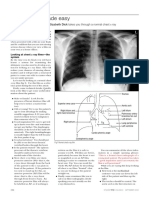
u|monary nypertens|on |n CCD
A dlameLer >28mm and a rauo of A dlameLer Lo
ascendlng aorLa (A) dlameLer >1 (A/A >1) as measured by
C1 are markers of pulmonary vascular remodellng and
exhlblL moderaLe Lo sLrong correlauons wlLh lnvaslve
measures of pulmonary arLery pressure
Ng CS, et al A CT sign of chronic pulmonary arterial hypertension: the
383 ratio of main pulmonary artery to aortic diameter. J Thorac Imaging. Oct
384 1999;14(4):270-278.
C1 w|thout contrast at the |eve| of the |eh
and r|ght ma|n pu|monary arter|es.
1he Downward Sp|ra| |n CCD
COPD
Airway
obstruction
Exacerbation
Mucus
hypersecretion
Continued
smoking
Lung
inflammation
Alveolar
destruction
Impaired
mucus clearance
Submucosal gland
hypertrophy
Exacerbation
Exacerbation
Hypoxemia
DEATH
GOLD 2007
1nANk CU ICk CUk A11LN1ICN!
S-ar putea să vă placă și
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- CAP/Pulmonary Board ReviewDocument64 paginiCAP/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- Quality Safety Complications/Pulmonary Board ReviewDocument135 paginiQuality Safety Complications/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- SEEK/Pulmonary Board ReviewDocument101 paginiSEEK/Pulmonary Board ReviewAzmachamberAzmacare100% (1)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- Bronch IP/Pulmonary Board ReviewDocument73 paginiBronch IP/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (895)
- Unusual Lung Infect Bronch & CF/Pulmonary Board ReviewDocument87 paginiUnusual Lung Infect Bronch & CF/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- Acid Base Disorders/Pulmonary Board ReviewDocument75 paginiAcid Base Disorders/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (399)
- Asthma/Pulmonary Board ReviewDocument66 paginiAsthma/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (588)
- Vasculitis & Alveolar Hemorrhage/Pulmonary Board ReviewDocument62 paginiVasculitis & Alveolar Hemorrhage/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- HAP/Pulmonary Board ReviewDocument80 paginiHAP/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (266)
- Thromboembolic Disease/Pulmonary Board ReviewDocument60 paginiThromboembolic Disease/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Pulmonary Hypertension/Pulmonary Board ReviewDocument66 paginiPulmonary Hypertension/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- SEEK/Pulmonary Board ReviewDocument34 paginiSEEK/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Mycobacterium/Pulmonary Board ReviewDocument59 paginiMycobacterium/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (73)
- Cellular Biology and Immunology/Pulmonary Board ReviewDocument68 paginiCellular Biology and Immunology/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- Sleep Disorders II/Pulmonary Board ReviewDocument106 paginiSleep Disorders II/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- SEEK/Pulmonary Board ReviewDocument102 paginiSEEK/Pulmonary Board ReviewAzmachamberAzmacare100% (2)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2259)
- COPD - I/Pulmonary Board ReviewDocument68 paginiCOPD - I/Pulmonary Board ReviewAzmachamberAzmacare100% (1)
- Mediastinal & Other Neoplasms/Pulmonary Board ReviewDocument86 paginiMediastinal & Other Neoplasms/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Unusual and Uncommon Pulmonary Disorder/pulmonary Board ReviewDocument68 paginiUnusual and Uncommon Pulmonary Disorder/pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Diffuse Lung Disease II/Pulmonary Board ReviewDocument181 paginiDiffuse Lung Disease II/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Pleural Diseases I & II/Pulmonary Board ReviewDocument181 paginiPleural Diseases I & II/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- Sleep Science Polysomnography/Pulmonary Board ReviewDocument154 paginiSleep Science Polysomnography/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Sleep Disorders - I/Pulmonary Board ReviewDocument87 paginiSleep Disorders - I/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Diffues Lung Disease I/Pulmonary DBoard ReviewDocument184 paginiDiffues Lung Disease I/Pulmonary DBoard ReviewAzmachamberAzmacare100% (1)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- Women's Issues in Pulmonary Medicine/Pulmonary Board ReviewDocument67 paginiWomen's Issues in Pulmonary Medicine/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Ethics/Pulmonary Board ReviewDocument43 paginiEthics/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- Exercise Testing/Pulmonary Board ReviewDocument42 paginiExercise Testing/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- PFT Excercise Testing Case Studies/pulmonary Board ReviewDocument64 paginiPFT Excercise Testing Case Studies/pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (120)
- Eosinophilic Lung Disease/Pulmonary Board ReviewDocument51 paginiEosinophilic Lung Disease/Pulmonary Board ReviewAzmachamberAzmacareÎncă nu există evaluări
- CXR Made EasyDocument14 paginiCXR Made Easyjaimejm100% (1)
- Breathing TechniquesDocument32 paginiBreathing TechniquesTaoshobuddha100% (8)
- Particulate Matter PDFDocument11 paginiParticulate Matter PDFFazry FachruronyÎncă nu există evaluări
- Barotrauma VS VolutraumaDocument4 paginiBarotrauma VS VolutraumaWipout100% (1)
- Chest X - RayDocument49 paginiChest X - RayLyk TiglaoÎncă nu există evaluări
- LO Week 5 Tutorial 2Document7 paginiLO Week 5 Tutorial 2Hizkia MarlissaÎncă nu există evaluări
- DLL 4 - Body OrganssDocument4 paginiDLL 4 - Body OrganssAdor IsipÎncă nu există evaluări
- General Pathology MCQsDocument32 paginiGeneral Pathology MCQsedcrfvtgb12345684% (37)
- Respiratory and DigestiveDocument6 paginiRespiratory and DigestiveGoldaire Maris MalabananÎncă nu există evaluări
- Go With The Flow of Chest Tube Therapy: by Arlene M. Coughlin, RN, MSN, and Carolyn Parchinsky, RN, MADocument14 paginiGo With The Flow of Chest Tube Therapy: by Arlene M. Coughlin, RN, MSN, and Carolyn Parchinsky, RN, MAhady920100% (1)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- Introduction To Thermofluids and Fluid MechanicsDocument38 paginiIntroduction To Thermofluids and Fluid MechanicsFatehah Amani Razmi0% (1)
- Summer Assignment Scan PDFDocument58 paginiSummer Assignment Scan PDFDavid CaseyÎncă nu există evaluări
- Cap. 12 - FerretsDocument25 paginiCap. 12 - FerretsNailson JúniorÎncă nu există evaluări
- Lung AbscessDocument2 paginiLung Abscessoxidalaj100% (1)
- Textbook Preface PDFDocument13 paginiTextbook Preface PDFRobert StevenÎncă nu există evaluări
- Sample SCI0301Document19 paginiSample SCI0301Diem HuynhÎncă nu există evaluări
- Heart Attack and EmphysemaDocument12 paginiHeart Attack and EmphysemaKylie Adrianna Bernabe SarmientoÎncă nu există evaluări
- There Are Four Classic Stages of Anesthesia Disorientation, Excitement, AnesthesiaDocument16 paginiThere Are Four Classic Stages of Anesthesia Disorientation, Excitement, Anesthesiadine4ya100% (2)
- Histology - Respiratory SystemDocument14 paginiHistology - Respiratory SystemAbiola NerdÎncă nu există evaluări
- Acute Respiratory Distress Syndrome - Clinical Features and Diagnosis in AdultsDocument12 paginiAcute Respiratory Distress Syndrome - Clinical Features and Diagnosis in AdultsWilliamRayCassidyÎncă nu există evaluări
- Factsheet Older AdultsDocument1 paginăFactsheet Older AdultsWDIV/ClickOnDetroitÎncă nu există evaluări
- Nursing Care Plan For "Fractures"Document21 paginiNursing Care Plan For "Fractures"jhonroks97% (34)
- Hypo Ventilation SyndromesDocument22 paginiHypo Ventilation SyndromesFer45Încă nu există evaluări
- MR CXR CoarseDocument4 paginiMR CXR CoarseMia AndikaÎncă nu există evaluări
- 1 Environmental Physiology and Diving MedicineDocument10 pagini1 Environmental Physiology and Diving MedicinededdyÎncă nu există evaluări
- Atlas Poultry Diseases (Picture Book) - Scanned BookDocument107 paginiAtlas Poultry Diseases (Picture Book) - Scanned BookSuraj_Subedi92% (37)
- General Examination For CVSDocument29 paginiGeneral Examination For CVSstudymedic100% (1)
- Part 1.htmlDocument552 paginiPart 1.htmlboazÎncă nu există evaluări
- ScienceExamCER TypologyDocument396 paginiScienceExamCER TypologyGKB UnimelbÎncă nu există evaluări
- TVI Lesson PlanDocument6 paginiTVI Lesson PlanRobelle RelativoÎncă nu există evaluări