Documente Academic
Documente Profesional
Documente Cultură
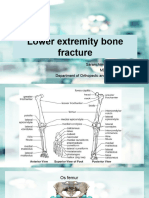
Musculoskeletal Trauma
Încărcat de
Rivani Kurniawan0 evaluări0% au considerat acest document util (0 voturi)
57 vizualizări12 paginitrauma
Drepturi de autor
© © All Rights Reserved
Formate disponibile
DOC, PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documenttrauma
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca DOC, PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
57 vizualizări12 paginiMusculoskeletal Trauma
Încărcat de
Rivani Kurniawantrauma
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca DOC, PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 12
MUSCULOSKELETAL TRAUMA OBJECTIVES
Upon completion of this chapter/lecture, the learner should be able to:
1. Identify the common mechanisms of injury associated with musculoskeletal trauma.
2. Describe the path physioloic chanes as a basis for sins and symptoms.
!. Discuss the nursin assessment of the patient with musculoskeletal trauma.
". #ased on the assessment data, identify appropriate nursin dianoses and e$pected
outcomes associated with patients with musculoskeletal trauma.
%. &lan appropriate inter'entions for patients with musculoskeletal trauma.
(. )'aluate the effecti'eness of nursin inter'entions for patients with specific types of
musculoskeletal trauma.
INTRODUCTION
)pidemioloy
*ore than half of all hospital admissions because of trauma are patients with some type
of fracture, usually of the lower limb+.,he elderly are at a particularly hih risk of bein
hospitali-ed for an e$tremity injury. .f those injuries sustained by passeners in'ol'ed in
nonfatal motor 'ehicle crashes, "(/ sustain pel'ic fractures and "1/ sustain femur
fractures. Dri'ers sustain femur fractures 0(%/1, pel'ic fractures 0"(/1, and ankle
fractures 0!2/1.3
,he 4merican 4ssociation of .rthopedic 5ureons reported an annual estimate of !2.6
million musculoskeletal injuries, which included (.1 million fractures, 1".( million
dislocations and sprains, 2." million open wounds, and 2.( million other injuries.
*usculoskeletal injuries account for 7,333 deaths per year.
Mechanisms of Injur an! Biomechanics
*usculoskeletal trauma can be sustained as a sinle system injury or in combination with
other systems. Injuries to the e$tremities are not usually considered the first priority.
*echanisms of injury include motor 'ehicle crashes, assaults, falls, sports, leisure, or
home acti'ities.
Differentiatin between unintentional and intentional injury can be difficult. 4buse
should be considered as a possible cause of the injury. 5uspicion of abuse should be
raised if the type or deree of injury does not correspond8to the history.
*usculoskeletal injuries can result from the application of both acceleration and
deceleration forces.
Injuries to the bone result from tension, compression, bendin, and torsion type forces9
:hen there is enouh force to fracture the shaft of a bone, this force may be transmitted
to the joints; for e$ample, fractures of the shaft of the radius and ulna may be associated
with fractures to the wrist, elbow, and shoulder.
<alls are a fre=uent mechanism of injury, especially for the elderly. )lderly patients who
fall often sustain pel'ic or lower e$tremity injuries. ,hese injuries, e'en if not life
threatenin, can seriously alter the elderly person9s lifestyle and reduce his or her
functional independence. Underlyin bone disease, such as osteoporosis or cancer
metastases, may predispose the patient to an e$tremity injury.
1
T"es of Injuries
*usculoskeletal injuries may be blunt or penetratin. ,hey may in'ol'e bone, soft tissue,
muscles, ner'es, and/or blood 'essels. Injuries include fractures and/or dislocations of the
bone or joint, sprains, strains, liamentous tears, tendon lacerations, and neuro'ascular
compromises.
Usua# Concurren$ Injuries
#ony e$tremity injuries may be associated with concurrent injury to ner'es, arteries,
'eins, or soft tissue. 5uspect neuro'ascular injury with any injury to the bones of an
e$tremity. 5e'ere pel'ic fractures can be associated with injuries to pel'ic orans and
lare blood loss. >enitourinary injuries, especially to the bladder or the urethra in males,
can result from pel'ic fractures. Dependin on the mechanism of injury, bony injury of
the e$tremities may be associated with 'ertebral column injuries.
%AT&O%&'SIOLO(' AS A BASIS )OR SI(NS AND S'M%TOMS
B#oo! Loss
*usculoskeletal trauma can be associated with lare blood loss because of disruption of
arteries or 'eins in close pro$imity to bones. Up to 1,%33 ml of blood can be lost from an
isolated femur fracture. 4 tibia or humeral fracture can lead to a blood loss up to 6%3 ml.
*ultiple fractures may result in sinificant blood loss, which can potentiate shock from
other injuries. #lood loss from pel'ic fractures 'aries sinificantly based on the
mechanism of injury, type of fracture, the particular 'essels injured, and whether there are
other intra8abdominal injuries.
?apillaries and cellular membranes can be disrupted or torn with all types of
musculoskeletal injuries. #lood from 'ascular disruption and intracellular fluid are
released into the area surroundin the injury.
)dema from fluid and blood accumulation can cause compression of surroundin
structures. @ormal physioloical mechanisms are acti'ated to minimi-e damae caused
by these structural disruptions:
A Initiation of the clottin system to decrease bleedin
A Bestoration of cellular membrane interity to enhance fluid reabsorption
A Increased collateral blood flow to promote healin
#one or joint displacement can compress surroundin 'essels and ner'es, causin
pathophysioloical chanes distal to the injury. 4s arterial blood flow is obstructed, tissue
o$yenation decreases resultin in tissue ischemia and cellular death. Durin this
process, pain increases, pulses become more difficult to palpate, the limb becomes pale,
cyanotic and cool, and capillary refill time increases.
Neuro#o*ic Defici$s
If ner'es are compressed or lacerated, conduction pathways are interrupted and the relay
of ner'e impulses are blocked or diminished. @er'e injury can result in diminished pain
sensation. Injury distal to a ner'e may result in partial or complete loss of motor and
sensory function.
2
)rac$ures
<ractures in'ol'e a disruption of bony continuity
Sof$ $issue injur
Disruption in the skin can result in a disturbance in fluid, electrolyte le'els, or
temperature control. 4ny skin surface wound with loss of skin interity pro'ides an entry
for microoranisms. ,his can lead to infection, especially if necrotic tissue is present.
,he followin terms used to describe soft tissue injuries:
Abrasion
4n epidermal and dermal injury caused by a friction, rubbin, or scrapin motion
Avulsion
4 full thickness skin loss or resultant flap in which the wound edes cannot be
appro$imated
Degloving
4 serious type of a'ulsion injury resultin from hih8enery shearin forces that tear
lare areas of skin and subcutaneous tissue away from the underlyin 'ascular supply
+ Contusion
Disruption of small blood 'essels and e$tra'asation of blood into the skin and/or mucous
membranes that does not interrupt the skin interity
Laceration
.pen wound from e$ternal forces causin a tearin or splittin of the skin, in'ol'in the
dermis, epidermis, or underlyin structures
Puncture
:ound with a narrow openin that can penetrate deeply into the skin. &uncture wounds
bleed minimally and tend to trap forein material that can lead to infection. 4nimal and
human bites can be considered puncture wounds and should be treated as contaminated
wounds.C
!
SELECTED MUSCULOSKELETAL INJURIES
Join$ Injuries
4 joint may become dislocated when the normal rane of motion is e$ceeded. Doint
dislocations may be complicated by neuro'ascular compromise and associated fractures.
Delayed reduction of a hip dislocation can lead to a 'ascular necrosis 04E@1 of the
femoral head and permanent disability.
.C Dislocation of the knee re=uires immediate inter'ention since peroneal ner'e injury
and compromises to the popliteal artery and 'ein may de'elop. 4nioraphy is necessary
to dianose 'ascular trauma.
5I>@5 4@D 5F*&,.*5
A&ain
A Doint deformity
A )dema
A Inability to mo'e the affected joint
A 4bnormal rane of motion
A @euro'ascular compromise: distal pulses may be diminished or absent; sensory function
may be affected
)emur )rac$ures
<emur fractures are a result of major trauma, such as falls, motor 'ehicle crashes,.
<ractures of the femoral neck are common after a fall in the elderly population.
?losed femur fractures can result in a collection of 1,333 to 1,%33 ml of blood in the
thih.
5I>@5 4@D 5F*&,.*5
A &ain and inability to bear weiht
A 5hortenin of the affected le
A Botation internally or e$ternally dependin on the location of the fracture site in the hip
A )dema of the thih
A Deformity of the thih
A )'idence of hypo'olemic shock
%e#,ic )rac$ures
&el'ic fractures are classified as either stable or unstable. 4 stable fracture is defined as
Cone that can withstand normal physioloic forces without abnormal deformation.CC 4n
unstable fracture occurs when the pel'ic rin is fractured in more than one place resultin
in two displacements on the rin; rotational
"
5I>@5 4@D 5F*&,.*5
A&ain
A)'idence of hypo'olemic shock
A5hortenin or abnormal rotation of the affected le
A >enitourinary or intra8abdominal injury
O"en )rac$ures
4ll open fractures are considered contaminated because of the forein materials and
bacteria that can be introduced into the wound. 4ny open fracture may result in an
infection. ,he risk of serious infection is reater with se'ere fractures. Infections can be
manifested by poor tissue healin, osteomyelitis, or sepsis.
.pen fractures are raded from I to 111 accordin to the deree of skin and soft tissue
injury surroundin the fracture site. >rade III open fractures are further described by the
amount of non'iable tissue, injury to the periosteum, and 'ascular trauma.
5I>@5 4@D 5F*&,.*5
A )'idence of skin disruption 0e.., laceration or puncture1 near or o'er the fracture
A &rotrusion of bone throuh open wounds
A&ain
A @euro'ascular compromise
A #leedin may be minimal to se'ere
Am"u$a$ions
4mputations may be partial or complete and usually in'ol'e the diits, distal half of the
foot, the lower le, the hand, or the forearm. ,he a$iom of sa'in Clife o'er limbC is a
reminder to the trauma team to fully resuscitate the patient before manain the
amputation.
,he followin ha'e been cited as indications for replantationl
A *ultiple diits
A ,humb
A :rist
A <orearm
A &ediatric patient 0children typically, ha'e a more positi'e outcome from replantation
procedures1
4mputations that are uillotine8type amputations ha'e a better chance of bein
successfully replanted as opposed to a'ulsi'e/tearin types of injuries. ,he decision to
replant should be made by a sureon or replantation team, if a'ailable.
5I>@5 4@D 5F*&,.*5
A .b'ious tissue loss
A &ain
A #leedin 0may be minimal to se'ere1 .
?omplete amputations will ha'e less acti'e bleedin than partial amputations because of
retraction of the se'ered arteries. 4n e$ception is an a'ulsi'e type of complete
amputation, which can result in e$tensi'e bleedin.
%
A )'idence of hypo'olemic shock
Crush Injuries
?ertain crush injuries, dependin on the location of the injury, may be life8threatenin
0e.., pel'is and both lower e$tremities1. ?ellular destruction and damae to 'essels and
ner'es make crush injuries difficult to treat. Gemorrhae from the damaed tissue,
destruction of muscle and bone tissue, fluid loss resultin in hypo'olemic shock,
compartment syndrome, and infection are se=uelae associated with crush injuries. ,he
destruction of muscle tissue associated with release of myolobin can result in renal
dysfunction.
5I>@5 4@D 5F*&,.*5
A *assi'ely crushed pel'is or e$tremity 0ies1 with soft tissue swellin
A&ain
A )'idence of hypo'olemic shock
A 5ins of compartment syndrome
A Hoss of neuro'ascular function distal to the injury
Com"ar$men$ Sn!rome
?ompartment syndrome occurs as pressure increases inside a fascial compartment. ,his
results in impaired capillary blood flow and cellular ischemia. ,his occurs more
fre=uently in the muscles of the lower le or forearm, but can in'ol'e any fascial
compartment. ,he increased pressure may be because of an internal source, such as
hemorrhae or edema, caused by open or closed fractures, or crush injuries. It
can also result from an e$ternal source, such as a cast, e$cessi'e traction, air splint, or
&45>. @er'es, blood 'essels, and muscles can be compressed. If compartment syndrome
results in CprolonedC ischemia of the muscles and ner'es, the patient may be left with a
limb that is painful and without function
5I>@5 4@D 5F*&,.*5
A &ain disproportionate to the injury because of increased tissue pressures and ischemia
A 5ensory deficit 0e.., numbness, tinlin, total loss of sensation1
A&roressi'e muscle weakness
A ,ense, swollen area
(
%&'SICAL ASSESSMENT
Befer to Initial 4ssessment, for a description of assessment of the patient9s airway,
breathin, circulation, and disability
Ins"ec$ion
A .bser'e eneral appearance of e$tremities
@ote color, position, and ob'ious differences of injured e$tremity as compared to
uninjured e$tremity
A4ssess interity of the injured area
A @ote protrusion of bone or any break in the skin
A 4ssess for bleedin
A Identify soft tissue damae, includin edema, ecchymosis, contusions, abrasions,
a'ulsions, or lacerations
A 4ssess for deformity and/or anulation of e$tremity
%a#"a$ion
)$tremity assessment is described by the fi'e &s: pain, pallor, pulses, paresthesia, and
paralysis. ,his assessment relates to the neuro'ascular status of the injured e$tremity.
4ssess the injured e$tremity and compare with an assessment of the opposite, uninjured
e$tremity.
A 4ssess the fi'e &s
A &ain
?arefully palpate the entire lenth of each e$tremity for pain. Determine location and
=uality of pain. Ischemic pain is often described as burnin or throbbin.
A &allor
@ote color and temperature of injured e$tremity. &allor, delayed capillary refill 0I two
seconds1, and a cool e$tremity indicate 'ascular compromise.
A &ulses
&alpate pulses pro$imal and distal to the injury for comparison. ,hen compare =uality of
pulses with the opposite, uninjured e$tremity.
A &aresthesia
Determine presence of abnormal sensations 0e.., burnin, tinlin, numbness1
A &aralysis
4ssess motor function. ,he ability to mo'e can be related to neuroloic function.
A &alpate the pel'is for pain or bony instability. 4pply entle pressure on the iliac crests
towards midline, notin any instability or increased pain. >ently press downward on the
symphysis pubis a fracture is suspected, carefully palpates the pel'is. Do not rock the
pel'is.
A @ote bony crepitus durin palpation, which is a cracklin sound produced by the
ratin of the end of fractured bones.
DIA(NOSTIC %ROCEDURES
Refer to Initial Assessment, for frequently ordered radiographic and laboratory studies
Additional studies for patients ith musculos!eletal trauma are listed belo"
Radiographic #tudies
A 4nterior8posterior and lateral of injured e$tremity
5ome fractures can 9only be seen from one radioraphic anle; therefore, an obli=ue
6
'iew may be indicated. ,he film should include the joints immediately abo'e and
below the injury.
+ 4nioraphy
4nioraphy may be indicated to identify tears or compressions in the arterial or
'enous network the injured e$tremity.
ANAL'SIS- NURSIN( DIA(NOSES- INTERVENTIONS- AND E.%ECTED
OUTCOMES
In addition to the nursing diagnoses outlined in Initial Assessment, the folloing nursing
diagnoses are potential problems for the patient ith musculos!eletal in$uries" %nce a
patient has been assesses diagnoses can be defined as either actual or ris!" An actual
nursing diagnosis is derived from a decision based on the patient&s presenting signs and
symptoms" A ris! nursing diagnosis is a $udgment the nurse ma!e based on a particular
patient&s ris! and potential for developing certain problems"
NURSIN( DIA(NOSIS INTERVENTION E.%ECTED OUTCOME
'luid volume deficit,
related to
(emorrhage
?ontrol any uncontrolled
bleedin by: applyin direct
pressure
o'er bleedin site;
ele'atin e$tremity;
applyin pressure
o'er arterial pressure
sites
A ?annulate two 'eins with
lare bore catheters and
initiate infusion of lactated
Biner9s solution or normal
saline
A 4dminister blood, as
indicated
A splint injured e$tremity
,he patient will ha'e an
effecti'e circulatin
'olume, as e'idenced by:
A 5table 'ital sins
appropriate for ae
A Urine output of 1ml/k/hr
A 5tron, palpable
peripheral pulses
A He'el of consciousness,
awake and alert,
ae appropriate
A 5kin normal color, warm,
and dry
A *aintains hematocrit of
!3 ml/dl or hemolobin of
12 to 1" /dl or reater
A ?apillary refill time of /0
seconds
Physical mobility, impaired,
related to)
A #one, soft tissue and/or
ner'e injury of e$tremity
+ &ain
+ )dema
A )$ternal immobili-ation
de'ices
A Himited rane of motion
5plint and immobili-e
affected e$tremity
Immobili-e joints abo'e
and below the deformity
4dminister analesia
medications, as prescribed
Use touch, positionin, or
rela$ation techni=ues to
i'e comfort
,he patient will e$perience
increased
mobility, as e'idenced by:
A 4bility to tolerate
mo'ement and increased
acti'ity
A :illinness to mo'e
affected part to deree
allowed
7
of affected bone A *aintenance of proper
body alinment
Infection, risk, related to:
A Impaired skin interity
A ?ontamination of wound
from
initial injury or
instrumentation
A In'asi'e fi$ation de'ices
A Interruption in perfusion
A 5uppressed inflammatory
response
.btain blood/wound
cultures
*onitor 'ital sins
4dminister antibiotics, as
prescribed
Jeep wound clean and
apply
dressin usin aseptic
techni=ue
*aintain aseptic techni=ue
?o'er open wounds with a
sterile dressin
Do not reposition
protrudin
bone framents
&repare for definiti'e care
5tabili-e impaled objects
,he patient will be free
from infection, as
e'idenced by:
A ?ore temperature
measurement of !(
!6.%K? 027 8 22.%K<1
A :hite blood cell count
within normal
limits
A 4bsence of sins of
infection: redness,
swellin, purulent
drainae, odor, and
tenderness
Impaired skin interity, risk,
related to:
A *o'ement of fractured
bones
A &ressure, shear, friction
on skin
and tissue
A *echanical irritants:
<i$ation de8
'ices, splints, and castin
material
A Impaired mobility
A )ffects of trauma/injury
aents
4ssess skin interity
fre=uently
Jeep skin dry
*aintain aseptic/clean
techni=ue, as appropriate
5plintin, as indicated
,he patient will e$perience
absence or
resolution of impaired skin
interity, as
e'idenced by:
A *aintenance of intact skin
o'erlyin
fracture
A 4bsence of sins of
irritation: redness,
blanchin, and itchin
2
&lannin and Implementation
Befer to Initial 4ssessment, for a description of the specific nursin inter'entions for
patients with compromises to airway, breathin, circulation, and disability.
A ?ontrol bleedin
A 5plint and immobili-e the affected e$tremity
A 5plintin is indicated when there is e'idence of the followin:
A Deformity
A &ain
A #ony crepitus
A )dema
A )cchymosis
A ?irculatory compromise
A .pen soft tissue injury
A Impaled object
A &aresthesia or paralysis
A 5elect an appropriate splint. ,hree types of splints are a'ailable:
A Biid splints, such as cardboard, plastic de'ices or metal splints
A 5oft splints, such as pillows, slins, or air splints
A ,raction splintsLapplied for actual or suspected femur or pro$imal tibial fractures
A Bemo'e jewelry or constrictin items of clothin prior to immobili-ation
A Do not reposition protrudin bone ends
A 4'oid e$cessi'e mo'ement of the fractured bone framents. 4ny manipulation can
increase bleedin into the tissues, increase the risk of fat emboli, or con'ert a closed
fracture to an open fracture.
A Immobili-e the joints abo'e and below the deformity
A *odify the splint to fit the fracture, if necessary
A Beassess neuro'ascular status before and after immobili-ation. If neuro'ascular status is
compromised, reassess, remo'e, adjust, or reapply the splint.
A 4pply ice to reduce swellin and pain
A )le'ate the e$tremity abo'e the le'el of the heart to reduce swellin and pain. If
compartment
A )le'ate the e$tremity abo'e the le'el of the heart to reduce swellin and pain. If
compartment syndrome is suspected, then ele'ate to the le'el of the heart.
A 4dminister analesic medications, as prescribed
A ?onsider reional analesia. 4 femoral ner'e block is fre=uently performed on patients
in many emerency departments in the United Jindom and 4ustralia.
A &repare for definiti'e stabili-ation. ,raction, castin, internal or e$ternal fi$ation may
be indicated.
A &repare for conscious sedation, as prescribed 05ee 4ppendi$ %1
A &repare for closed reduction, as indicated
A &ro'ide psychosocial support
13
A &repare patient for operati'e inter'ention, hospital admission or transfer, as indicated
@UB5I@> I@,)BE)@,I.@5 <.B ,G) &4,I)@, :I,G 4 &)HEI?
<B4?,UB)
A 5tabili-e pel'ic fractures
A 4pply &45> to splint pel'ic fractures, as indicated
A :rap the pel'is in a folded sheet which is clamped or knotted at the front, as indicated
A &repare for application of e$ternal fi$ator. Unstable pel'ic fractures with se'ere blood
loss may re=uire immediate stabili-ation with an e$ternal fi$ator.l!
A 4ssist with additional dianostic radioraphs, includin cystoram, anioram, or ?,
scan of the pel'is, as ordered. &atients must be carefully monitored durin anioraphy
and related therapeutic
emboli-ation.
@UB5I@> I@,)BE)@,I.@5 <.B ,G) &4,I)@, :I,G 4@ .&)@
:.U@D
A .btain a wound culture from an open fracture site
A Irriate any wound, as indicated
A ?o'er open wounds with dry, sterile dressins. 4'oid fre=uent dressin chanes to
minimi-e the risk
of bacterial contamination.
A 4dminister antibiotics, as prescribed
A Inspect dressins fre=uently for continued bleedin
A 4dminister tetanus prophyla$is, as indicated
@UB5I@> I@,)BE)@,I.@5 <.B ,G) &4,I)@, :I,G
4@4*&U,4,I.@
A ?ontrol any acti'e bleedin with pressure dressins and ele'ation. 4'oid tourni=uets or
clamps.
A )le'ate the stump
A 5plint the stump as needed
A Bemo'e ross dirt or debris
A Jeep the amputated part cool and wrap the part in a saline8moistened au-e, then place
in a sealed plastic ba, and finally place the ba in crushed ice and water. Do not allow
the part to free-e.
A &repare for radioraphs of both the stump and the amputated part M N 9
A &repare patient for hospital admission, operati'e inter'ention, or transfer to a facility
with a replantation team, as indicated
A 4dminister antibiotics, as prescribed
A 4dminister tetanus prophyla$is, as indicated
@UB5I@> I@,)BE)@,I.@5 <.B ,G) &4,I)@, :I,G 4 ?BU5G
I@DUBF
A 4dminister an intra'enous crystalloid solution to increase urinary output and facilitate
e$cretion of myolobin
A )le'ate the injured e$tremity abo'e the le'el of the heart to reduce swellin and pain
A >ently clean open wounds
A Beassess
A Urinary output
11
A &resence of myolobin in the urine
A *otor and sensory function 9 A
A &repare patient for surical debridement, fasciotomy, and/or amputation
@UB5I@> I@,)BE)@,I.@5 <.B ,G) &4,I)@, :I,G &.55I#H)
?.*&4B,*)@, 5F@DB.*)
A )le'ate the limb to the le'el of the heart to promote 'enous outflow and pre'ent further
swellin. Do not ele'ate the limb abo'e the heart as this may decrease perfusion to
compromised e$tremity.
A 4ssist with measurement of fascial compartment pressure, as indicated. @ormal
pressure is I 13 mm G 01.! J&a1.23 4 readin of I !% to "% mm G 0".68( J&a1 is
suesti'e of possible ano$ia to muscles and ner'es. 21
A &repare for fasciotomy, as indicated. 4 fasciotomy may pre'ent muscle and/or
neuro'ascular damae and loss of the limb.
ABeassess and document neuro'ascular status on an onoin basis. ?ommunicate chanes
to the physician immediately.
)'aluation and .noin 4ssessment
Befer to ?hapter !, Initial 4ssessment, for a description of the onoin e'aluation of the
patient9s airway, breathin, circulation, and disability. 4dditional e'aluations include:
A *onitorin breathin effecti'eness and rate of respiration
,achpynea, rales, and whee-es may be indicators of fat embolus syndrome.
A Beassess and document the fi'e &s
5U**4BF
Injuries of the e$tremities are usually not the first priority of care for the multiple trauma
patients. Gowe'er, there is a hih incidence of injuries to upper and lower e$tremities
that, althouh usually not life8threatenin, can result in functional disability and/or loss,
and lon8term rehabilitation.
,he pro$imity of 'essels and ner'es to musculoskeletal structures increases the risk of
neuro'ascular damae ranin from motor, sensory, or 'ascular deficits to paralysis
and/or hemorrhae, and shock.
Disruptions and fractures of the pel'is may result in sinificant blood loss because of
concurrent injury to the blood 'essels in the pel'ic ca'ity. ?ollaborate with members of
the trauma team to correct any life8threatenin compromises to circulation.
Durin the secondary assessment, assess the e$tremities for indications of a fracture or
dislocation.
Inter'ene early to splint the suspected fracture and reassess neuro'ascular function both
before and after the application of any splintin de'ice.
,imely identification and manaement of suspected musculoskeletal injuries, includin
the use of pain control, splints, traction, and/or e$ternal fi$ation, contribute o impro'ed
functional patient outcomes.
12
S-ar putea să vă placă și
- Neck Trauma, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDe la EverandNeck Trauma, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsÎncă nu există evaluări
- Hip Neck Fracture, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDe la EverandHip Neck Fracture, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsÎncă nu există evaluări
- Musculoskeletal TraumaDocument12 paginiMusculoskeletal Traumahatem alsrour100% (1)
- PEMBAHASAN EnglishDocument12 paginiPEMBAHASAN EnglishEinz Nur Amalyah IdrusÎncă nu există evaluări
- FracturesDocument4 paginiFracturesJoerich Montesclaros100% (1)
- Orthopaedic EssaysDocument139 paginiOrthopaedic EssaysDuncan Jackson100% (1)
- AMPUTATIONDocument73 paginiAMPUTATIONmohammad farhanÎncă nu există evaluări
- Orthopedic InjuriesDocument27 paginiOrthopedic InjuriesvikramÎncă nu există evaluări
- Percutaneous Osteosynthesis of The Distal Fractures of The Femur. Eladio Saura Mendoza e Eladio Saura SanchezDocument12 paginiPercutaneous Osteosynthesis of The Distal Fractures of The Femur. Eladio Saura Mendoza e Eladio Saura SanchezNuno Craveiro LopesÎncă nu există evaluări
- Diaphyseal Femur FracturesDocument9 paginiDiaphyseal Femur FracturesSoulmates1Încă nu există evaluări
- Maxillofacial TraumaDocument7 paginiMaxillofacial TraumaRegina Desi GresianaÎncă nu există evaluări
- Ortho LMRP 2019Document44 paginiOrtho LMRP 2019skÎncă nu există evaluări
- Clavicle FractureDocument15 paginiClavicle Fracturesalsabil aurellÎncă nu există evaluări
- Frienchzel Joy A. Asis Group 3 BSN 3-ADocument14 paginiFrienchzel Joy A. Asis Group 3 BSN 3-AKenneth Louis GalizaÎncă nu există evaluări
- Litrev SCHDocument7 paginiLitrev SCHdedyalkarni08Încă nu există evaluări
- Anatomy of Spinal CordDocument43 paginiAnatomy of Spinal CordGargi MPÎncă nu există evaluări
- Clavicle Fractures - StatPearls - NCBI BookshelfDocument9 paginiClavicle Fractures - StatPearls - NCBI BookshelfRizqan Fahlevvi AkbarÎncă nu există evaluări
- Selected Instructional Course LecturesDocument27 paginiSelected Instructional Course LecturesAhmad ShakirÎncă nu există evaluări
- Chapter 3Document2 paginiChapter 3ahmadreyhaanÎncă nu există evaluări
- Orthopedic InjuriesDocument24 paginiOrthopedic InjuriesvikramÎncă nu există evaluări
- Spinal Cord InjuryDocument9 paginiSpinal Cord InjurytasneemÎncă nu există evaluări
- Case Report Juli 2013Document21 paginiCase Report Juli 2013NahdiaÎncă nu există evaluări
- Sidhant ThesisDocument109 paginiSidhant ThesisSomeshwar GuptÎncă nu există evaluări
- Actures & DislocationsDocument16 paginiActures & Dislocationssabina_grapiniÎncă nu există evaluări
- College of Nursing Adult Nursing Academic Year Lec. Waleed IbrahimDocument6 paginiCollege of Nursing Adult Nursing Academic Year Lec. Waleed Ibrahimمحمد سعد طه احمدÎncă nu există evaluări
- 1spinal Cord InjuryDocument8 pagini1spinal Cord Injurysunny_jr_Încă nu există evaluări
- Principles of Spine Trauma and Spinal Deformities PDFDocument34 paginiPrinciples of Spine Trauma and Spinal Deformities PDFVirlan Vasile CatalinÎncă nu există evaluări
- Fracture Case AbstractDocument27 paginiFracture Case AbstractMaribel Briones JuanÎncă nu există evaluări
- Proximal Humeral Fracture Repair and RehabilitationDocument8 paginiProximal Humeral Fracture Repair and RehabilitationAnonymous UClts4nYÎncă nu există evaluări
- Fracture and Joint Injuries-General FeaturesDocument19 paginiFracture and Joint Injuries-General Featuresngurah123456789Încă nu există evaluări
- Li LBM 4 Blok 18 AnggunDocument8 paginiLi LBM 4 Blok 18 AnggunAnggun Amanda SaveriiaÎncă nu există evaluări
- Nonunion of FracturesDocument43 paginiNonunion of FracturessharenÎncă nu există evaluări
- Hip FractureDocument4 paginiHip FractureJoel Vertt C. Balboa100% (1)
- Orthopaedic Surgery Fractures and Dislocations: Tomas Kurakovas MF LL Group 29Document13 paginiOrthopaedic Surgery Fractures and Dislocations: Tomas Kurakovas MF LL Group 29Tomas Kurakovas100% (1)
- Fracture ComplicationsDocument11 paginiFracture ComplicationsVALIANT PERMATAPUTRAÎncă nu există evaluări
- Clavicle Fracture - TeachMeSurgeryDocument3 paginiClavicle Fracture - TeachMeSurgeryTeshanKoralageÎncă nu există evaluări
- La Consolacion College Manila: Femoral Neck FractureDocument3 paginiLa Consolacion College Manila: Femoral Neck FractureIvan Liquiran AvenadoÎncă nu există evaluări
- Essay On Fracture ComplicationsDocument9 paginiEssay On Fracture ComplicationsadibahÎncă nu există evaluări
- Femoral Neck FractureDocument19 paginiFemoral Neck FractureTabita P SÎncă nu există evaluări
- 2.supracondylar Humerus FracturesDocument26 pagini2.supracondylar Humerus FracturesDabessa MosissaÎncă nu există evaluări
- Sot 1 2011 6Document4 paginiSot 1 2011 6Erwin CandraÎncă nu există evaluări
- Tibia and Fibula Shaft Fracture in Pediatric Case (Ola)Document20 paginiTibia and Fibula Shaft Fracture in Pediatric Case (Ola)Junarto Putra Tandiarrang100% (1)
- Fracture in Leg Tibia and FibulaDocument27 paginiFracture in Leg Tibia and Fibulachilsya shajiÎncă nu există evaluări
- 116 Muscoskeletal 3NCGroup1Document16 pagini116 Muscoskeletal 3NCGroup1Dud AccÎncă nu există evaluări
- Lower Extremity Bone Fracture Lecture 3Document88 paginiLower Extremity Bone Fracture Lecture 3Tselmeg TselmegÎncă nu există evaluări
- Ortho Questions 1Document10 paginiOrtho Questions 1Kay BristolÎncă nu există evaluări
- CBD FixDocument17 paginiCBD FixAziir 'arÎncă nu există evaluări
- Pediatric Supracondylar Fractures of The Distal Humerus: Provided by Springer - Publisher ConnectorDocument7 paginiPediatric Supracondylar Fractures of The Distal Humerus: Provided by Springer - Publisher ConnectorBison_sonÎncă nu există evaluări
- 2 - Local Complications of Fractures - D3Document26 pagini2 - Local Complications of Fractures - D3Zainul FatimahÎncă nu există evaluări
- Facial Trauma: Dr. Azher A. Auda Oral and Maxillofacial Surgeon Bds CabsDocument56 paginiFacial Trauma: Dr. Azher A. Auda Oral and Maxillofacial Surgeon Bds CabsHaider F YehyaÎncă nu există evaluări
- 978-0-7817-5096-7 - Chapter 5Document5 pagini978-0-7817-5096-7 - Chapter 5VelventinÎncă nu există evaluări
- Treatment Options of Pelvic and Acetabular Fractures in Patients With Osteoporotic BoneDocument12 paginiTreatment Options of Pelvic and Acetabular Fractures in Patients With Osteoporotic Bonefajri_amienÎncă nu există evaluări
- Mandibular FracturesDocument171 paginiMandibular FracturesBalen ShalawÎncă nu există evaluări
- Clinical Features and Diagnosis of FracturesDocument43 paginiClinical Features and Diagnosis of FracturesChenna Kesava100% (2)
- Hip Fracture: Navigation SearchDocument8 paginiHip Fracture: Navigation SearchjobinbionicÎncă nu există evaluări
- 76040138-Referat-Fraktur-Pelvis EditDocument34 pagini76040138-Referat-Fraktur-Pelvis Editsri wulanÎncă nu există evaluări
- Lowe Limb AmputationDocument11 paginiLowe Limb AmputationNadya ZahraÎncă nu există evaluări
- Anestheticconsiderations Fororal, Maxillofacial, and NecktraumaDocument17 paginiAnestheticconsiderations Fororal, Maxillofacial, and NecktraumaDasubabu GantiÎncă nu există evaluări
- Orthopaedic Essays: Faculty of Medical Sciences Mona CampusDocument185 paginiOrthopaedic Essays: Faculty of Medical Sciences Mona CampusHiruzaminÎncă nu există evaluări
- Treatment of The Fracture of Femur in ChildrenDocument35 paginiTreatment of The Fracture of Femur in Childrenmoaz.zaiter.transporteÎncă nu există evaluări
- 2002 Vol.40 Issues 4 Vascular Imaging PDFDocument278 pagini2002 Vol.40 Issues 4 Vascular Imaging PDFRivani KurniawanÎncă nu există evaluări
- Imaging Acute Abdomen DR - Rivani Kurniawan FixDocument86 paginiImaging Acute Abdomen DR - Rivani Kurniawan FixRivani KurniawanÎncă nu există evaluări
- Intervensi Pulmo Konas Perpari-1Document32 paginiIntervensi Pulmo Konas Perpari-1Rivani KurniawanÎncă nu există evaluări
- Latent TB Infection Provider GuideDocument17 paginiLatent TB Infection Provider GuideRivani KurniawanÎncă nu există evaluări
- Identification and Management of Latent Tuberculosis InfectionDocument8 paginiIdentification and Management of Latent Tuberculosis InfectionRivani KurniawanÎncă nu există evaluări
- Daftar Pustaka 7689Document20 paginiDaftar Pustaka 7689Rivani KurniawanÎncă nu există evaluări
- HI Local Nov07Document15 paginiHI Local Nov07Rivani KurniawanÎncă nu există evaluări
- Bcgletter1 09Document1 paginăBcgletter1 09Rivani KurniawanÎncă nu există evaluări
- Daftar Pustaka bcg098Document6 paginiDaftar Pustaka bcg098Rivani KurniawanÎncă nu există evaluări
- The Epidemiology of Childhood Tuberculosis in The Netherlands: Still Room For PreventionDocument9 paginiThe Epidemiology of Childhood Tuberculosis in The Netherlands: Still Room For PreventionRivani KurniawanÎncă nu există evaluări
- Rhabdomyosarcoma in PediatricDocument2 paginiRhabdomyosarcoma in PediatricRivani KurniawanÎncă nu există evaluări
- TendinitisDocument6 paginiTendinitisRivani KurniawanÎncă nu există evaluări
- Imaging Vesika Seminalis Dan Vas DeferenDocument68 paginiImaging Vesika Seminalis Dan Vas DeferenRivani KurniawanÎncă nu există evaluări
- PP Jurnal Thorak NewDocument93 paginiPP Jurnal Thorak NewRivani KurniawanÎncă nu există evaluări
- Chest Wall TumorDocument27 paginiChest Wall TumorRivani KurniawanÎncă nu există evaluări
- Chest 2003 Jun 123 (6) 2019-27, Figure 3Document1 paginăChest 2003 Jun 123 (6) 2019-27, Figure 3Rivani KurniawanÎncă nu există evaluări
- Skeletal Radiology LengkapDocument89 paginiSkeletal Radiology LengkapRivani KurniawanÎncă nu există evaluări
- GastrointestinalDocument29 paginiGastrointestinalRivani KurniawanÎncă nu există evaluări
- Xiaxi Gb-43: Gall Bladder Channel 1Document2 paginiXiaxi Gb-43: Gall Bladder Channel 1ray72roÎncă nu există evaluări
- U.S. Patent 9,301,519, Entitled, Systems and Methods For Ex Vivo Organ Care, To Hassanein Et Al., Issued Apr. 5, 2016.Document106 paginiU.S. Patent 9,301,519, Entitled, Systems and Methods For Ex Vivo Organ Care, To Hassanein Et Al., Issued Apr. 5, 2016.Anonymous a7S1qyXÎncă nu există evaluări
- HbA1c OdtDocument2 paginiHbA1c OdtAhmed AssafÎncă nu există evaluări
- Deyo 1992Document6 paginiDeyo 1992Wwwanand111Încă nu există evaluări
- Ramatu Kamara ResumeDocument1 paginăRamatu Kamara Resumeapi-707616686Încă nu există evaluări
- General Surgery ConceptsDocument4 paginiGeneral Surgery ConceptsPau De GuzmanÎncă nu există evaluări
- Foundations in Microbiology: TalaroDocument76 paginiFoundations in Microbiology: Talaromertx013Încă nu există evaluări
- Corticosteroids and Associated DiseasesDocument76 paginiCorticosteroids and Associated DiseasesALNAKIÎncă nu există evaluări
- Borax - The Inexpensive Detox, Arthritis, Osteoporosis and Mycoplasma CureDocument14 paginiBorax - The Inexpensive Detox, Arthritis, Osteoporosis and Mycoplasma Curebammer189% (9)
- KDIGO Clinical Practice Guideline On The.9Document93 paginiKDIGO Clinical Practice Guideline On The.9PD18Încă nu există evaluări
- EDiR Notebook (For European Diploma in Radiology)Document250 paginiEDiR Notebook (For European Diploma in Radiology)Parthiban Bala100% (4)
- 26 - Nonsurgical Treatment of Peyronies DiseaseDocument4 pagini26 - Nonsurgical Treatment of Peyronies DiseaseNunuh SulaemanÎncă nu există evaluări
- Sample Nursing Care PlanDocument3 paginiSample Nursing Care Planhyunbin18100% (4)
- Zygomatic Arch and Orbital FracturesDocument6 paginiZygomatic Arch and Orbital FractureszacrouchyÎncă nu există evaluări
- Approach To The Patient With Facial Erythema PDFDocument38 paginiApproach To The Patient With Facial Erythema PDFFilipa FigueiredoÎncă nu există evaluări
- Elc501 - Group Portfolio ForumDocument11 paginiElc501 - Group Portfolio ForumAhmad SyamiÎncă nu există evaluări
- MR - Kuldeep Pandya PDFDocument1 paginăMR - Kuldeep Pandya PDFabhishek mayekarÎncă nu există evaluări
- First Aid For Snake BiteDocument11 paginiFirst Aid For Snake BiteHenryVanDerSchyffÎncă nu există evaluări
- Department of Education: School Contingency PlanDocument14 paginiDepartment of Education: School Contingency PlanClerica RealingoÎncă nu există evaluări
- Fecal Elimination and Urinary EliminationDocument6 paginiFecal Elimination and Urinary Eliminationincent100% (1)
- Group 7 (GIT & Hepatobiliary Case Simulation)Document41 paginiGroup 7 (GIT & Hepatobiliary Case Simulation)Zil Kamleshkumar PanchalÎncă nu există evaluări
- د. هالة Dermatitis-1 (Muhadharaty)Document7 paginiد. هالة Dermatitis-1 (Muhadharaty)adwÎncă nu există evaluări
- 10 Commandments of ConsultationDocument4 pagini10 Commandments of ConsultationZlatan KurjakovicÎncă nu există evaluări
- Dry Fasting The AMAZING Health Benefits Everyone Should Know AboutDocument4 paginiDry Fasting The AMAZING Health Benefits Everyone Should Know AboutMariaÎncă nu există evaluări
- Kshudra Roga Critical Understanding: Dr. Gaurav DesaiDocument39 paginiKshudra Roga Critical Understanding: Dr. Gaurav DesaiDrVikas100% (3)
- Laryngopharyngeal Reflux and Functional Laryngeal Disorder: Perspective and Common Practice of The General GastroenterologistDocument9 paginiLaryngopharyngeal Reflux and Functional Laryngeal Disorder: Perspective and Common Practice of The General GastroenterologistKenzi A HasyaputraÎncă nu există evaluări
- PathogenesisDocument14 paginiPathogenesisIdreesÎncă nu există evaluări
- Modified Ashworth ScaleDocument3 paginiModified Ashworth ScaleSundarajan ManiÎncă nu există evaluări
- v20 n4Document223 paginiv20 n4Sivanantham KrishnamoorthiÎncă nu există evaluări
- K10 - Materi 10 - Tugas CA EBMDocument14 paginiK10 - Materi 10 - Tugas CA EBMputri vivianeÎncă nu există evaluări