Documente Academic
Documente Profesional
Documente Cultură
Neonatal Extra-Renal Wilm's Tumour: Division of Paediatric Surgery, Aga Khan University Hospital, Karachi
Încărcat de
dydy_71930 evaluări0% au considerat acest document util (0 voturi)
7 vizualizări2 paginiWT
Titlu original
329
Drepturi de autor
© © All Rights Reserved
Formate disponibile
PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentWT
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
7 vizualizări2 paginiNeonatal Extra-Renal Wilm's Tumour: Division of Paediatric Surgery, Aga Khan University Hospital, Karachi
Încărcat de
dydy_7193WT
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 2
Introduction
Wilms tumour is one of the most common solid
neoplasia of the childhood and the most common tumour of
genito-urinary tract in that age group.
1
Its origin in location
other than kidney is rare. Only 57 such cases could be found
in international literature mostly in infants and older
children.
2
Willms tumours are the malignancies with a
characteristic histology seen typically during childhood and
almost exclusively arising from the Kidney.
3
In United
States the incidence remained constant at 7.8 per million
populations per year.
4
Extra renal sites for origin of Wilms tumour are
extremely rare. The diagnosis of extra renal Wilms tumour
is made only after a primary tumour of the kidneys has been
ruled out with a secondary extra renal metastasis.
5
Below we report a case of extra-renal Wilm's tumour
in a neonate with intra spinal extension through vertebral
column.
Case Report
An eight days old male neonate presented with three
days history of Jaundice, Abdominal distension and one
episode of haematemesis. Clinical examination revealed a
3.0 kg lethargic and icteric neonate.His abdomen was
distended with visible veins.Awell defined abdominal mass
was palpable in right Iliac fossa.Haematological and
biochemical examination were normal except, total
bilirubin 13 mg/dl alfa-fetoprotein 6138 IU/ml; LDH 1463.
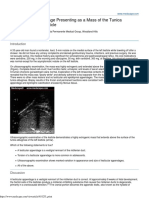
Ultrasound scan and CT abdomen (Figure 1) revealed a
8x9cm heterogeneous mass in lower abdomen which was
extending across the midline and also entering into spinal
canal. Right kidney was hydronephrotic but both kidneys
were free of any tumour and were well away from the mass.
On exploratory laparotomy a lobulated mass was
present in lower abdomen retroperitoneally. It was
extending from bifurcation of aorta up to coccyx and
extending in both the flanks. On the right side mass was
over ileo-psoas and on the left side it was extending behind
the ileopsoas and was tethered to the vertebral column. The
right iliac vessel and ureter was stretched over the tumour.
Mass was excised completely but spinal canal was not
opened. Histology showed mass to be well encapsulated,
yellow and soft in consistency. Microscopically features
were those of Willms tumour (Figure 2). In view of
possible stage 3 disease with residual tumour chemotherapy
was commenced. The follow up MRI, eight months after
surgery, revealed persistence of soft tissue mass in spinal
canal which was explored, mass removed but did not show
any viable tumour. Two years following surgery, the child is
doing well with no clinical or radiological recurrence.
Discussion
There are two types of extra renal Wilms tumour.
6
One arises in the line from the renal bed to the scrotum,
supposedly from residual embryonic renal tissue.
7
The
second consists of teratome with nephroblastic tissue.
8
The
exact embryological origin is not clear. Multiple hypotheses
have been proposed including a more primitive
mesonephric or pronephric origin. Normally the
mesonephros degenerates after fourth month of gestation.
However, juxta-gonadal mesonephric glomeruli have been
identified as late as 21st week of gestation.
9
Thus the Wilm's
tumour that is adjacent to the gonads may have a
mesonephric origin. Likewise the pronephros, first and
embryologically most primitive of the excretory organs,
Neonatal Extra-Renal Wilm's Tumour
S. Hussain, S. Nizami, F. Tareen
Division of Paediatric Surgery, Aga Khan University Hospital, Karachi.
Vol. 54, No. 1, January 2004 37
arise in a cranial position, adjacent to the somites 9 to 12,
which are lower thoracic in position.
1
Malignant
transformation of aberrantly located cells derived from this
tissue may account for chest wall tumours. The
transformation of primitive embryological tissue into
nephroblastome tissue is unknown. One theory is that the
mesonephric conversion to Wilm's tumour requires two
cellular events.
10
The first results in the development of an
aberrant rest of mesonephric remnant tissue. The second is
malignant transformation of the mesonephric rest into
Wilms tumour. Twenty five percent of extra-renal Wilm's
show the Wilm's tumour gene.
3
Thus mutation of this gene
may be the aetiology of extra-renal Wilm's tumour.
Most reported cases of extra renal Wilm's are in first
four years of life. Only one has been reported in a neonate
and oldest was a forty one year old.
11
The retro peritoneum
being the most frequent location followed by
inguinoscrotal area, sacrococcygeal teratoma, the
mediastinum, and the lower chest wall.
11
The intra spinal extension has rarely been reported
in literature. There is one case report of a four year old
child, presenting with sudden onset of paraplegia and sacral
tumour, in association with spina bifida. Imaging studies
confirmed a sacral tumour with extradural extension up to
T10 and spinal dysraphism.The histological features of
sacral and intraspinal components of the mass was
consistent with Wilm's tumour.
12
Presently there is no staging for extra-renal Wilms
tumour. Coppe's series and the cases reported since show
that the prognosis and clinical course of extra renal Wilm's
tumour is parallel to those of intra renal Wilm's tumour.
13
Extra renal Wilms tumour should be treated according to
NWTS protocol.
The unique features in our patient were a neonate
with the origin of Wilms tumour at extrarenal sites from
embryological elements and having an intraspinal
component.
References
1. Broeker BH, Calamone AA. Primary extrarenal Wilm's tumour in children. J
Paediatr Surg 1989;12:24.
2. Oner U, Toker B, Wilm's tumour of ovary: a case report. J Paediatr Surg
2002;1;37.
3. Roberts DJ, Haber D, Sklar J, et al. Extrarenal Wilm's tumour: a study of their
relationship with classical renal Wilms tumor using expression of WT1 as a
moleculer marker. Lab.Invest 1993;68:528-36.
4. Cutler SJ,Young JL. Third National Cancer Survey. Incidence data. National
Cancer Institute. Monograph 41, March 1975.
5. Andrews PE, Kelalid PP. Extra renal Wilm's tumour; result of national Wilm's
tumour study. J Paediatr Surg 1992;9;27.
6. Mang LL, Jagadessan K. Extra renal Wilm's tumour. Med J Malaysia
1983;28:134-36.
7. Bhajekar AB, Joseph M, Bhat HS. Unattached nephroblastoma,
Br. J. Urol 1964;36:187-90.
8. Malik TA, Malik GB, Diesh G. Retroperitoneal teratoma with nephroblastoma
tissue as the main component. Int Surg 1967;47:246-9.
9. D'angio GJ, Breslow N, Beckwith JB, et al. Treatment of Wilm's tumor: result
of the Third National Wilm's tumour study. Cancer 1989;64;349-60.
10. Knudson AG, Strong LC. Mutation and cancer; a model for Wilm's tumour of
the Kidney. J Natl Cancer Inst 1972;48:313-24.
11. Narashimarao KI, Marhawa RK. Extra renal Wilm's tumour. J Paediatr Surg
1989;2:24.
12. Govender D, Hadley GP, Nadvi SS, et al. Primary Lumbosacral Wilm's
tumour associated with spinal dysraphism. Virchows Arch 2000;436:502-5.
13. Coppes MJ, Wilson PCG, Wenaeitzman S. Extra renal Wilm's tumour staging,
treatment and prognosis. J Clin Oncol 1991;9:167-74.
J Pak Med Assoc
38
S-ar putea să vă placă și
- Wilms Tumor: Imaging of Pediatric Renal MassesDocument35 paginiWilms Tumor: Imaging of Pediatric Renal MassesEnny AndrianiÎncă nu există evaluări
- 21 PDFDocument4 pagini21 PDFMatteo ChinaskiÎncă nu există evaluări
- Testicular AppendagesDocument4 paginiTesticular AppendagesJohn stamosÎncă nu există evaluări
- Krukenberg Tumour Simulating Uterine Fibroids and Pelvic Inflammatory DiseaseDocument3 paginiKrukenberg Tumour Simulating Uterine Fibroids and Pelvic Inflammatory DiseaseradianrendratukanÎncă nu există evaluări
- Nephroblastoma: Radiological and Pathological Diagnosis of A Case With Liver MetastasesDocument5 paginiNephroblastoma: Radiological and Pathological Diagnosis of A Case With Liver MetastasesfifahcantikÎncă nu există evaluări
- Sacrococcygeal TeratomaDocument21 paginiSacrococcygeal TeratomaEm VelascoÎncă nu există evaluări
- Superior Vesical Fissure: Variant Classical Bladder ExstrophyDocument3 paginiSuperior Vesical Fissure: Variant Classical Bladder ExstrophyChindia BungaÎncă nu există evaluări
- Unusual Variants of Fibroadenoma Breast Diagnosed on CytologyDocument5 paginiUnusual Variants of Fibroadenoma Breast Diagnosed on CytologyEnvhy WinaÎncă nu există evaluări
- Dec24 16 PDFDocument8 paginiDec24 16 PDFijasrjournalÎncă nu există evaluări
- Congenital Ovarian CystDocument4 paginiCongenital Ovarian CystSastra SinagaÎncă nu există evaluări
- Giant Uterine Leiomyoma - Case Report and Review of LiteratureDocument3 paginiGiant Uterine Leiomyoma - Case Report and Review of LiteratureMan ManuelÎncă nu există evaluări
- Nasopharyngeal Carcinoma in Children and Young AdultsDocument9 paginiNasopharyngeal Carcinoma in Children and Young AdultsSunardiasihÎncă nu există evaluări
- Rare Uterine Leiomyoma in Adolescent FemaleDocument3 paginiRare Uterine Leiomyoma in Adolescent Femaledr.putra888Încă nu există evaluări
- Umbilical Cord Hernias: Prenatal Diagnosis and Natural HistoryDocument4 paginiUmbilical Cord Hernias: Prenatal Diagnosis and Natural HistoryFriska GriffinÎncă nu există evaluări
- Duktus ThyroglosusDocument13 paginiDuktus ThyroglosusOscar BrooksÎncă nu există evaluări
- The Paediatric Thymus: Recognising Normal and Ectopic Thymic TissueDocument11 paginiThe Paediatric Thymus: Recognising Normal and Ectopic Thymic TissueFifi FathiraÎncă nu există evaluări
- Hirose 2003Document5 paginiHirose 2003lakshay raoÎncă nu există evaluări
- Fetal Axillary Cystic Hygroma Detected by Prenatal UltrasonographyDocument3 paginiFetal Axillary Cystic Hygroma Detected by Prenatal UltrasonographywitaÎncă nu există evaluări
- Finger Clubbing and A Lung MassDocument5 paginiFinger Clubbing and A Lung MassSeptinaAyuSamsiatiÎncă nu există evaluări
- Discussion: Meigs' Syndrome and Pseudo-Meigs' SyndromeDocument3 paginiDiscussion: Meigs' Syndrome and Pseudo-Meigs' SyndromeFlapianne SimenceriauÎncă nu există evaluări
- Meigs' Syndrome and Pseudo-Meigs' Syndrome: Report of Four Cases and Literature ReviewsDocument6 paginiMeigs' Syndrome and Pseudo-Meigs' Syndrome: Report of Four Cases and Literature ReviewsAlfa FebriandaÎncă nu există evaluări
- Pe09055 PDFDocument5 paginiPe09055 PDFMed MedÎncă nu există evaluări
- Low Peh Hueh International Medical University, MalaysiaDocument19 paginiLow Peh Hueh International Medical University, MalaysiaChaitanya Venkata SattiÎncă nu există evaluări
- Wilms Tumour: Shiraz Deen University of ManchesterDocument14 paginiWilms Tumour: Shiraz Deen University of ManchesterJomalyn FloresÎncă nu există evaluări
- Testicular TestisDocument16 paginiTesticular TestisGede Mei PutraÎncă nu există evaluări
- Dematos 1997Document6 paginiDematos 1997Ali AmokraneÎncă nu există evaluări
- Uterine Fibroid Mimicking Ovarian TumorDocument3 paginiUterine Fibroid Mimicking Ovarian Tumorasshagab04Încă nu există evaluări
- Adult Nephroblastoma Wilms Tumor A Case Report 2168 9857 1000150Document3 paginiAdult Nephroblastoma Wilms Tumor A Case Report 2168 9857 1000150Mi KaÎncă nu există evaluări
- Abdominal Inflammatory Myofibroblastic Tumor: Report On Four Cases and Review of LiteratureDocument6 paginiAbdominal Inflammatory Myofibroblastic Tumor: Report On Four Cases and Review of LiteratureLisma EkayantiÎncă nu există evaluări
- Askin TumorDocument6 paginiAskin TumorGaluh Kresna BayuÎncă nu există evaluări
- MCQ Jeddah - Doc (FINAL) 2Document9 paginiMCQ Jeddah - Doc (FINAL) 2Indrajit Barua100% (1)
- Fetirorm TeratomaDocument4 paginiFetirorm Teratomaasshagab04Încă nu există evaluări
- HemangiomaDocument1 paginăHemangiomaLeon Suárez AcuarioÎncă nu există evaluări
- Giant Malignant Phyllodes Tumor of the Breast Case ReportDocument5 paginiGiant Malignant Phyllodes Tumor of the Breast Case Reportsiti qomaria usuÎncă nu există evaluări
- 262 A Rare Case of Anterior VaginalDocument3 pagini262 A Rare Case of Anterior VaginalVibhor Kumar JainÎncă nu există evaluări
- Neoplasia ExamDocument9 paginiNeoplasia ExamYheng Gaosaii100% (1)
- Ca Gla BartholinDocument3 paginiCa Gla BartholinMaria Alejandra SolisÎncă nu există evaluări
- Gyne - Torsion of Dermoid CystDocument4 paginiGyne - Torsion of Dermoid CystroshmaeÎncă nu există evaluări
- Jurnal Kista Ovarium2Document5 paginiJurnal Kista Ovarium2Isara Nur LatifahÎncă nu există evaluări
- Eyelid TattoingDocument15 paginiEyelid Tattoing小島隆司Încă nu există evaluări
- Rare Clear Cell Adenocarcinoma of the Colon Case ReportDocument2 paginiRare Clear Cell Adenocarcinoma of the Colon Case ReportOscar HalumÎncă nu există evaluări
- AMasculine PresentingFemaleAdolescentaRareCaseofPoorly DifferentiatedSertoli LeydigCellTumorDocument15 paginiAMasculine PresentingFemaleAdolescentaRareCaseofPoorly DifferentiatedSertoli LeydigCellTumorDaniella Ashley BaltesÎncă nu există evaluări
- Fibrolamellar Variant of Hepatocellular Carcinoma in A Young FemaleDocument3 paginiFibrolamellar Variant of Hepatocellular Carcinoma in A Young FemaleIKIKIKIKIKI999999Încă nu există evaluări
- Stein1935 PDFDocument11 paginiStein1935 PDFXime RdzÎncă nu există evaluări
- Rare Peritoneal Tumour Presenting As Uterine Fibroid: Janu Mangala Kanthi, Sarala Sreedhar, Indu R. NairDocument3 paginiRare Peritoneal Tumour Presenting As Uterine Fibroid: Janu Mangala Kanthi, Sarala Sreedhar, Indu R. NairRezki WidiansyahÎncă nu există evaluări
- 1 s2.0 S1930043321006816 MainDocument5 pagini1 s2.0 S1930043321006816 MainFatimah AssagafÎncă nu există evaluări
- Unusual Presentation of Choriocarcinoma: Case ReportDocument2 paginiUnusual Presentation of Choriocarcinoma: Case ReportcuyÎncă nu există evaluări
- Objectives:: Ahmed H. Al-SalemDocument4 paginiObjectives:: Ahmed H. Al-SalemHarun NasutionÎncă nu există evaluări
- Pielonefritis Kronis: Tujuan PraktikumDocument12 paginiPielonefritis Kronis: Tujuan PraktikumFp Cyninthia KennedyÎncă nu există evaluări
- A Case of Body Stalk Anomaly Arising After Invitro Fertilization at 26 Week' GestationDocument3 paginiA Case of Body Stalk Anomaly Arising After Invitro Fertilization at 26 Week' GestationasclepiuspdfsÎncă nu există evaluări
- RPB14150079015Document5 paginiRPB14150079015Ijupbs IjupbsÎncă nu există evaluări
- A Case of Ovarian Fibroma Masquerading As A Uterine FibroidDocument5 paginiA Case of Ovarian Fibroma Masquerading As A Uterine FibroidAnonymous UHnQSkxLBDÎncă nu există evaluări
- 2 5 21 861 PDFDocument3 pagini2 5 21 861 PDFAhmed ZidanÎncă nu există evaluări
- 1 s2.0 S1028455911001823 MainDocument6 pagini1 s2.0 S1028455911001823 MainFatimah AssagafÎncă nu există evaluări
- An Unusual Cause of "Appendicular Pain" in A Young Girl: Mesenteric Cystic LymphangiomaDocument3 paginiAn Unusual Cause of "Appendicular Pain" in A Young Girl: Mesenteric Cystic LymphangiomaSherif Abou BakrÎncă nu există evaluări
- Jurnal 3 Pa Wilms Tumor BismillahDocument16 paginiJurnal 3 Pa Wilms Tumor Bismillahkiki tuanaya1Încă nu există evaluări
- Uterine Fibroid EmbolizationDocument8 paginiUterine Fibroid EmbolizationAlexandre Campos Moraes AmatoÎncă nu există evaluări
- Solving the riddle of cancer: new genetic approaches to treatmentDe la EverandSolving the riddle of cancer: new genetic approaches to treatmentÎncă nu există evaluări
- DHF Menurut WHO 2011Document212 paginiDHF Menurut WHO 2011Jamal SutrisnaÎncă nu există evaluări
- PCH 32 s1 033Document6 paginiPCH 32 s1 033dydy_7193Încă nu există evaluări
- FMB 15 105 PDFDocument15 paginiFMB 15 105 PDFdydy_7193Încă nu există evaluări
- F1000research 5 6687 PDFDocument10 paginiF1000research 5 6687 PDFdydy_7193Încă nu există evaluări
- 2016 Cha Dengue Guide Patient Care AmericasDocument136 pagini2016 Cha Dengue Guide Patient Care Americasdydy_7193Încă nu există evaluări
- 2 Indian Guidelines DENGUEDocument39 pagini2 Indian Guidelines DENGUEAmanda WrightÎncă nu există evaluări
- Ajid411 9Document9 paginiAjid411 9Jenaro Helí Ardila CortésÎncă nu există evaluări
- DOH Revised Clinical Guidelines - DENGUE PDFDocument27 paginiDOH Revised Clinical Guidelines - DENGUE PDFRey San Luis III0% (1)
- JurnalDocument12 paginiJurnalIrara RaÎncă nu există evaluări
- 2016 Article 1849 PDFDocument8 pagini2016 Article 1849 PDFdydy_7193Încă nu există evaluări
- FMB 15 105Document15 paginiFMB 15 105dydy_7193Încă nu există evaluări
- DHF Menurut WHO 2011Document212 paginiDHF Menurut WHO 2011Jamal SutrisnaÎncă nu există evaluări
- 5502 PDFDocument68 pagini5502 PDFdydy_7193Încă nu există evaluări
- 3.3. Fluid Treatment dengue-Trisakti-OK PDFDocument38 pagini3.3. Fluid Treatment dengue-Trisakti-OK PDFdydy_7193Încă nu există evaluări
- Childhood Cervical Lymphadenopathy: Original ArticleDocument5 paginiChildhood Cervical Lymphadenopathy: Original Articledydy_7193Încă nu există evaluări
- 00 B 4953 B 560 Ccca 872000000Document9 pagini00 B 4953 B 560 Ccca 872000000dydy_7193Încă nu există evaluări
- PGH 106 02 094 PDFDocument8 paginiPGH 106 02 094 PDFdydy_7193Încă nu există evaluări
- Ja2014 983635Document7 paginiJa2014 983635Jinan Fairuz Anindika RÎncă nu există evaluări
- Nihms 437493Document15 paginiNihms 437493dydy_7193Încă nu există evaluări
- 2016 Article 1849Document8 pagini2016 Article 1849dydy_7193Încă nu există evaluări
- F1000research 5 6687Document10 paginiF1000research 5 6687dydy_7193Încă nu există evaluări
- 00 B 4953 B 560 Ccca 872000000Document9 pagini00 B 4953 B 560 Ccca 872000000dydy_7193Încă nu există evaluări
- Gonorrhea Infection in Women: Prevalence, Effects, Screening, and ManagementDocument10 paginiGonorrhea Infection in Women: Prevalence, Effects, Screening, and ManagementAfria Beny SafitriÎncă nu există evaluări
- 15 - 1 - 31 (1) - 1Document6 pagini15 - 1 - 31 (1) - 1dydy_7193Încă nu există evaluări
- Stress Aging Role of GlucocorticoidDocument14 paginiStress Aging Role of Glucocorticoiddydy_7193Încă nu există evaluări
- 181089Document7 pagini181089dydy_7193Încă nu există evaluări
- Ccid 7 059Document6 paginiCcid 7 059dydy_7193Încă nu există evaluări
- Characteristics of Leprosy Patients in Jakarta: Artikel PenelitianDocument5 paginiCharacteristics of Leprosy Patients in Jakarta: Artikel Penelitiandydy_7193Încă nu există evaluări
- Characteristics of Leprosy Patients in Jakarta: Artikel PenelitianDocument5 paginiCharacteristics of Leprosy Patients in Jakarta: Artikel Penelitiandydy_7193Încă nu există evaluări