Documente Academic
Documente Profesional
Documente Cultură
Ameloblastoma in The Mandible
Încărcat de
bangunazhariyusufTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Ameloblastoma in The Mandible
Încărcat de
bangunazhariyusufDrepturi de autor:
Formate disponibile
Rev Bras Otorrinolaringol
2008;74(3):478.
CASE REPORT
Ameloblastoma in the
mandible
Marcelo Medeiros1, Gabriela Granja Porto2, Jose
Rodrigues Laureano Filho3, Lus Portela4, Ricardo
Holanda Vasconcellos5
INTRODUCTION
The ameloblastoma is an enamel
tissue tumor, which does not differentiate to
form the enamel. It is benign and of ectodermic origin. Although considered a benign
tumor, its clinical behavior can be considered of middle ground, between benign and
malignant. The tumor is characterized by
slow but persistent growth and infiltration in
adjacent tissue1,2.
CASE PRESENTATION
R.T.B., male, 30 years old, came to
the Department of Maxillo-Facial Surgery
complaining of a bulging in his left-side mandible, which had been enlarging for the past
ten years. An incisional biopsy was carried
out through the oral cavity. The pathology
finding was ameloblastoma. In order to better plan access to the lesion and mandible
reconstruction after tumor exeresis, we made
a model through the prototyping technique.
Treatment chose was hemimandibulectomy,
with mandibular condyle loosening on the
ipsilateral side, since the tumor had already
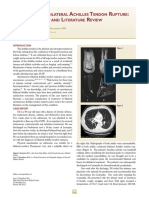
Figure 1. Postoperative clinical and radiographic aspects, prototyping model and postoperative radiographic aspect.
Keywords: ameloblastoma, surgery, mandible patology.
invaded the cortical bone, with immediate
reconstruction with reconstruction plate and
condyle coupled to it. Currently the patient
has been under observation for four years,
without signs of recurrence (Figure 1).
DISCUSSION
Ameloblastomas are classified in
unicystic, solid or multicystic, peripheral and
malignant subtypes in conventional or multicystic solid (86% of the cases), unicystic (13%
of the cases) and peripheral or extra-osseous
(about 1% of the cases)3. Such distinction is
important because the treatment of a unicystic
lesion can be more conservative, for it has a
less aggressive behavior and smaller size than
its solid or multicystic counterpart4.
Typical ameloblastoma starts insidiously as a central bony lesion which is
slowly destructive; however tends to expand
the bone instead of punching a hole through it. The tumor is rarely painful, unless
infected and usually does not cause signs
and symptoms of nerve involvement, even
when large3.
Radiographically, the most common
aspect of multicystic ameloblastomas is a
multilocular lesion; often times described
as having the appearance of soap bubbles
when large, and are described as honeycomb
when small. There is frequently a lingual
cortical and oral expansion, and usually the
teeth roots adjacent to the tumor are resorbed.
Unicystic ameloblastomas present a radiolucent image that surrounds the crown of an
unerupted tooth or, they simply appear as a
well defined radiotransparent areas3.
Gender distribution as far as ameloblastomas are concerned is 1:14,5. The
age of most frequent onset is the 3rd and
4th decades of life6. The mandible is about
four times more affected than the maxilla6.
About of mandible tumors are located in
the mandible ramus and molar teeth. When
it involves the maxilla, the posterior region is
also the one most affected, and as it develops,
the tumor may involve the maxillary sinus
and the orbit5.
There is a trend to treat unicystic
ameloblastomas by curettage with 10%-15%
of recurrence; however, avoiding patient
mutilation. In the solid or multicystic tumor, it
is necessary to have radical surgical excision,
with resection of the affected bone with at least 15 mm of healthy tissue as safety margin6.
The mucosa in contact with the tumor must
be entirely removed, because it may contain
ameloblastic cells that can contaminate the
graft during reconstruction1.
It is important to stress the capacity
the tumor has to develop late recurrences.
Because of its slow growth, these recurrences
may take years, and even decades to happen
after the first surgery1.
FINAL COMMENTS
Thus, we conclude that radical
surgery is the treatment of choice most of
the times. We must stress that radiographic
methods are not able to determine the exact
disease extension and the recurrence rate is
close to 100% when not treated properly.
REFERENCES
1. Ferretti C, Polakow C, Coleman H. Recurrent
Ameloblastoma: Report of 2 Cases. J Oral
Maxillofac Surg 2000;58:800-4.
2. AlKhateeb T, Ababneh KT. Ameloblastoma in
Young Jordanians: A Review of the Clinicopathologic Features and Treatment of 10
Cases. J Oral Maxillofac Surg 2003;61:13-8.
3. Neville BW, Damm DD, Allen CM, et al. Patologia Oral & Maxilofacial. Rio de Janeiro:
Guanabara Koogan; 1998.
4. Ord RA, Blanchaert Jr RH, Nikitakis NG, Sauk
JJ. Ameloblastoma in Children. J Oral Maxillofac Surg 2002;60:762-70.
5. Zwahlen RA, Vogt P, Fischer FS, Gratz KW.
Case Report: Myocardial Metastasis of a
Maxillary Malignant Ameloblastoma. J Oral
Maxillofac Surg 2003;61:731-4.
6. Pizer ME, Page DG, Svirsky JA. ThirteenYear
Follow-Up of Large Recurrent Unicystic Ameloblastoma of the Mandible in a 15 Year Old
Boy. J Oral Maxillofac Surg 2002;60:211-5.
Specialist in maxillo-facial surgery and traumatology, Masters program in maxillo-facial surgery and traumatology student
2
Specialist in maxillo-facial surgery and traumatology, MSc student - MFS FOP-UPE.
3
PhD in maxillo-facial surgery and traumatology, adjunct professor of maxillo-facial surgery and traumatology University of Pernambuco.
4
MSc in Biomedical Engineering, Assistant Professor of Tooth Implants at the University of Pernambuco.
5
PhD in Maxillo-facial Surgery and Traumatology, Adjunct Professor of Maxillo-facial Surgery and traumatology University of Pernambuco.
This paper was submitted to the RBORL-SGP (Publishing Manager System) on 24 October 2006. code 3470.
The article was accepted on 5 November 2006.
1
Brazilian Journal of Otorhinolaryngology 74 (3) May/June 2008
http://www.rborl.org.br / e-mail: revista@aborlccf.org.br
478
S-ar putea să vă placă și
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (587)
- Food Challenge TestDocument2 paginiFood Challenge TestbangunazhariyusufÎncă nu există evaluări
- Achilles Tendon RuptureDocument11 paginiAchilles Tendon RupturebangunazhariyusufÎncă nu există evaluări
- Anaemia of Chronic Kidney Diseas8 PDFDocument49 paginiAnaemia of Chronic Kidney Diseas8 PDFDevi Resmi SariÎncă nu există evaluări
- Anaemia of Chronic Kidney Diseas8 PDFDocument49 paginiAnaemia of Chronic Kidney Diseas8 PDFDevi Resmi SariÎncă nu există evaluări
- Spontaneous Bilateral Achilles Tendon RuptureDocument5 paginiSpontaneous Bilateral Achilles Tendon RupturebangunazhariyusufÎncă nu există evaluări
- Ruptured Foot Tendon: Background & Etiology (Cause)Document4 paginiRuptured Foot Tendon: Background & Etiology (Cause)bangunazhariyusufÎncă nu există evaluări
- Biology of Tendon Injury: Healing, Modeling and Remodeling: P. Sharma and N. MaffulliDocument10 paginiBiology of Tendon Injury: Healing, Modeling and Remodeling: P. Sharma and N. MaffulliBrianna RyanÎncă nu există evaluări
- Puskesmas Rawat InapDocument1 paginăPuskesmas Rawat InapbangunazhariyusufÎncă nu există evaluări
- Complicated Periorbital Cellulitis Case ReportDocument4 paginiComplicated Periorbital Cellulitis Case ReportbangunazhariyusufÎncă nu există evaluări
- Achilles Tendon RuptureDocument11 paginiAchilles Tendon RupturebangunazhariyusufÎncă nu există evaluări
- Management of Extensor Tendon InjuriesDocument7 paginiManagement of Extensor Tendon InjurieskenthepaÎncă nu există evaluări
- Thyroid-Stimulating Hormone, White MatterDocument8 paginiThyroid-Stimulating Hormone, White MatterbangunazhariyusufÎncă nu există evaluări
- Extensor Tendon Injury ProtocolDocument11 paginiExtensor Tendon Injury ProtocoltasneempichoriÎncă nu există evaluări
- Achilles Tendon RuptureDocument6 paginiAchilles Tendon RupturechloramphenicolÎncă nu există evaluări
- Ruptur Tendon AchillesDocument18 paginiRuptur Tendon AchillesAulya Novaldy PratomoÎncă nu există evaluări
- Non Surgical Repair Achilles Tendon2Document4 paginiNon Surgical Repair Achilles Tendon2bangunazhariyusufÎncă nu există evaluări
- Facial Nerve Decompression For Idiopathic Bell's PalsyDocument8 paginiFacial Nerve Decompression For Idiopathic Bell's PalsybangunazhariyusufÎncă nu există evaluări
- The Effect of Early Neuromuscular ElectricalDocument7 paginiThe Effect of Early Neuromuscular ElectricalhasÎncă nu există evaluări
- Lateralization in Cluster Headache A Nordic Multicenter StudyDocument6 paginiLateralization in Cluster Headache A Nordic Multicenter StudybangunazhariyusufÎncă nu există evaluări
- Lateralization in Cluster Headache A Nordic Multicenter StudyDocument6 paginiLateralization in Cluster Headache A Nordic Multicenter StudybangunazhariyusufÎncă nu există evaluări
- Does Prolonged Length of Stay in The Emergency DepartmentDocument9 paginiDoes Prolonged Length of Stay in The Emergency DepartmentbangunazhariyusufÎncă nu există evaluări
- Brainstem Infarcts Predict REM Sleep BehaviorDocument5 paginiBrainstem Infarcts Predict REM Sleep BehaviorbangunazhariyusufÎncă nu există evaluări
- Classification and Clinical Features of Headache PatientsDocument8 paginiClassification and Clinical Features of Headache PatientsbangunazhariyusufÎncă nu există evaluări
- Facial Nerve Decompression For Idiopathic Bell's PalsyDocument8 paginiFacial Nerve Decompression For Idiopathic Bell's PalsybangunazhariyusufÎncă nu există evaluări
- Antibacterial and Antifungal Properties of Human CerumenDocument1 paginăAntibacterial and Antifungal Properties of Human CerumenbangunazhariyusufÎncă nu există evaluări
- Cover Proposal BayuDocument7 paginiCover Proposal BayubangunazhariyusufÎncă nu există evaluări
- SkrofulodermaDocument4 paginiSkrofulodermabangunazhariyusufÎncă nu există evaluări
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (894)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (399)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (73)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2219)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (265)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (119)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- Long-Term Results of the Kumamoto Study on Optimal Diabetes Control in Type 2 Diabetic PatientsDocument19 paginiLong-Term Results of the Kumamoto Study on Optimal Diabetes Control in Type 2 Diabetic PatientsCarlosZamÎncă nu există evaluări
- Mod 3 Guidelines in Giving Emergency CAreDocument5 paginiMod 3 Guidelines in Giving Emergency CArerez1987100% (2)
- Empagliflozin Metformin HCL: Jardiance Duo®Document2 paginiEmpagliflozin Metformin HCL: Jardiance Duo®Lord Carlo CabangalÎncă nu există evaluări
- DigoxinDocument4 paginiDigoxinapi-379794167% (3)
- Europass Curriculum Vitae: Personal InformationDocument7 paginiEuropass Curriculum Vitae: Personal InformationAndrei TudoracheÎncă nu există evaluări
- ATI Comprehensive Predictor STUDY THIS ONE Questions and AnswersDocument2 paginiATI Comprehensive Predictor STUDY THIS ONE Questions and Answersianshirow834Încă nu există evaluări
- Pedia CaseDocument65 paginiPedia CaseJason MirasolÎncă nu există evaluări
- Continuum CareDocument24 paginiContinuum CareJovelyn EspanolaÎncă nu există evaluări
- Drug Study (Newborn Screening)Document2 paginiDrug Study (Newborn Screening)Aaron Christian AlmoiteÎncă nu există evaluări
- RLE Manual EditedDocument68 paginiRLE Manual EditedReymondÎncă nu există evaluări
- Test Bank For Comprehensive Perinatal and Pediatric Respiratory Care 4th Edition by WhitakerDocument7 paginiTest Bank For Comprehensive Perinatal and Pediatric Respiratory Care 4th Edition by Whitakerdonnamcbride10021996wqk100% (21)
- Genetic CounsellingDocument52 paginiGenetic CounsellingVijetha RaiÎncă nu există evaluări
- WLP - Q4 - Health 9 - Week 8Document8 paginiWLP - Q4 - Health 9 - Week 8Gladys GutierrezÎncă nu există evaluări
- Excerpt From "Diabetes: A Lifetime of Being Too Sweet"Document9 paginiExcerpt From "Diabetes: A Lifetime of Being Too Sweet"waltcrockerÎncă nu există evaluări
- Body temperature, vital signs, anthropometric measurementsDocument23 paginiBody temperature, vital signs, anthropometric measurementsWYNE BRENT M CORPUZÎncă nu există evaluări
- Assessment Diagnosis Planning Implementatio N Rationale Evaluation Short Term: Indipendent Short TermDocument2 paginiAssessment Diagnosis Planning Implementatio N Rationale Evaluation Short Term: Indipendent Short TermKenneth PoncialÎncă nu există evaluări
- Pre-Eclampsia and EclampsiaDocument21 paginiPre-Eclampsia and EclampsiaTamratKelelegn100% (1)
- Manajemen Pre-Operatif Pasien Dengan DMDocument12 paginiManajemen Pre-Operatif Pasien Dengan DMyanayas28Încă nu există evaluări
- Heart Failure: Definition, Classification, Epidemiology & PathophysiologyDocument10 paginiHeart Failure: Definition, Classification, Epidemiology & PathophysiologyAlbert ShantoÎncă nu există evaluări
- CHED Memorandum Order No. 13 Series of 2017 Medical Technology Laws and Bioethics (MTLB211Document51 paginiCHED Memorandum Order No. 13 Series of 2017 Medical Technology Laws and Bioethics (MTLB211REYMAR VICU BRAVOÎncă nu există evaluări
- RSVDocument8 paginiRSVilyas9558Încă nu există evaluări
- Vertigo and Dizziness Guide for Healthcare ProvidersDocument50 paginiVertigo and Dizziness Guide for Healthcare ProvidersAu Ah Gelap100% (1)
- Lesson PlanDocument5 paginiLesson Planapi-458907281100% (1)
- Covid 19 Brochure enDocument23 paginiCovid 19 Brochure enFerdinand FajardoÎncă nu există evaluări
- Dizziness - Vertigo and HomoeopathyDocument38 paginiDizziness - Vertigo and HomoeopathyDr. Rajneesh Kumar Sharma MD HomÎncă nu există evaluări
- Comorbidities of Hearing Loss and The Implications of Multimorbidity For Audiological Care. Hearing Research - 10.1016:j.heares.2018.06.008Document12 paginiComorbidities of Hearing Loss and The Implications of Multimorbidity For Audiological Care. Hearing Research - 10.1016:j.heares.2018.06.008ALEIRAMGONZALEZÎncă nu există evaluări
- Worksheet Chapter 6Document42 paginiWorksheet Chapter 6kevin fajardoÎncă nu există evaluări
- Some Applications of Genetic EngineeringDocument9 paginiSome Applications of Genetic Engineeringshibi sharmaÎncă nu există evaluări
- DSHS Letter To Bowie County Judge GA-32 50 Percent Occupancy For BusinessesDocument2 paginiDSHS Letter To Bowie County Judge GA-32 50 Percent Occupancy For BusinessesField WalshÎncă nu există evaluări
- Workplace Violence in HealthcareDocument5 paginiWorkplace Violence in HealthcareÁngela María GuevaraÎncă nu există evaluări