Documente Academic
Documente Profesional
Documente Cultură
Acute Hydrops in The Donor Cornea Graft in Non-Keratoconus Patients
Încărcat de
April FoleyTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Acute Hydrops in The Donor Cornea Graft in Non-Keratoconus Patients
Încărcat de
April FoleyDrepturi de autor:
Formate disponibile
[Downloadedfreefromhttp://www.meajo.orgonWednesday,May07,2014,IP:112.215.66.
75]||ClickheretodownloadfreeAndroidapplicationforthisjournal
Case Report
Acute Hydrops in the Donor Cornea Graft in
Non-Keratoconus Patients
John B. Cason, Samuel C. Yiu1
Access this article online
ABSTRACT
A 44-year-old Hispanic male and 91-year-old Caucasian male presented to the clinic with acute
vision loss and pain years after penetrating keratoplasty (PKP). Neither patient had a history
of keratoconus. Both patients had a history of eye rubbing and intraocular device present in
the anterior chamber. The first patient had a history of a glaucoma drainage tube and the
second patient had an anterior chamber intraocular lens implanted. Anterior segment ocular
coherence tomography showed deep stromal cystic cavities. Both patients exhibited breaks
in the endothelium by ultrasound biomicroscopy and the histopathologic examination after
repeat PKP. Those findings were most consistent with acute corneal hydrops in the donor graft.
Website:
www.meajo.org
DOI:
10.4103/0974-9233.114808
Quick Response Code:
Key words: Corneal transplant, Descemets membrane, Hydrops
INTRODUCTION
orneal hydrops is a condition of acute stromal edema that
occurs after a rupture in Descemets membrane. This is
not an uncommon sequelae of late keratoconus and is a frequent
indication for penetrating keratoplasty (PKP). Approximately,
3% of keratoconus patients experience one or more episodes
of corneal hydrops.1 Rarely, it can occur in a corneal graft and
is frequently an extension of a break in Descemets membrane
from the host cornea to the donor graft. This has been reported
in two separate case reports.2,3
To the authors knowledge, hydrops in a donor corneal graft
has not been described outside of the context of keratoconus.
We present two patients with no history of keratoconus that
developed acute hydrops in the donor corneal graft.
CASE REPORTS
Case 1
A 44-year-old human immunodeficiency virus positive Hispanic
male with undetectable viral load presented to the clinic with
a 5-week history of decreased vision, 1 year after undergoing
PKP in the left eye. The patient had a history of herpes keratitis
complicated by severe glaucoma in that eye. He had received a
corneal transplant 2 years before for corneal decompensation.
On the day of presentation, his best-corrected vision was 20/20
in the right eye and hand-motion at 6 feet in the left eye. His
manifest refraction in the right eye was 3.00 + 0.50 148. The
intraocular pressure was 15 mm Hg in the right eye. His corneal
graft was very edematous, opaque, and protuberant making it
impossible to measure the intraocular pressure in the left eye.
The glaucoma drainage valve in the superotemporal quadrant
was well-covered. There was no evidence of keratoconus in the
fellow eye. Ocular coherence tomography (OCT) of the anterior
segment showed a deep stromal cystic cavity consistent with
hydrops in the left eye [Figure 1a]. Ultrasound biomicroscopy
(UBM) of the anterior segment revealed a Descemets membrane
detachment and severe corneal edema with stromal cystic cavities
[Figure 1b]. The patient received a repeat PKP of the left eye.
During surgery, the glaucoma drainage tube was noted to be
positioned close to the cornea and was trimmed under the host
cornea rim. Pathology examination revealed a rupture and recoil
of Descemets membrane centrally and a near perforation with
a substantial amount of corneal stromal edema, consistent with
hydrops [Figure 2].
Department of Ophthalmology, Naval Medical Center San Diego, San Diego, California, 1Department of Ophthalmology,
Johns Hopkins University, Wilmer Eye Institute, Baltimore, Maryland, USA
Corresponding Author: Dr. Samuel Yiu, Department of Ophthalmology, The Johns Hopkins University, The Wilmer Eye Institute, 400 N
Broadway/Smith Bldg 6001-R, Baltimore, Maryland 21231, USA. E-mail: syiu2@jhmi.edu
Middle East African Journal of Ophthalmology, Volume 20, Number 3, July - September 2013
265
[Downloadedfreefromhttp://www.meajo.orgonWednesday,May07,2014,IP:112.215.66.75]||ClickheretodownloadfreeAndroidapplicationforthisjournal
Cason and Yiu: Acute hydrops in the donor cornea graft in non-keratoconus patients
Figure 1: (a) High-definition anterior segment optical coherence tomographic image
of corneal hydrops. There is marked fluid within the corneal stroma (b) Ultrasound
biomicroscopy of acute corneal hydrops. Note the apparent break in Descemets
membrane
frequent eye rubbing. On examination, he had light perception
with projection in the right eye and 20/25 best-corrected
vision in the left eye. The manifest refraction in the left eye was
1.50 + 1.50 141. Intraocular pressure was not measurable
in the right eye and was 14 mm Hg in the left eye. A very large
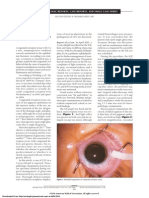
pedunculated cyst was seen within the corneal graft in the
right eye [Figure 3]. There was no evidence of keratoconus
in the fellow eye. OCT of the anterior segment revealed
a deep stromal cystic cavity consistent with the hydrops.
UBM of the anterior segment showed the presence of an
anterior chamber intraocular lens and a large cystic cavity
with a suspected break in the superior region of Descemets
membrane. The patient subsequently received a PKP of the
right eye. The anterior chamber intraocular lens was an openloop Kelman-style and was left in place. The corneal graft
was oversized by 0.5 mm. Pathology examination revealed
marked central corneal edema consistent with the hydrops.
Descemets membrane was absent except for fragments on
both sides of the button.
DISCUSSION
Figure 2: Pathology slide showing a focal break in Descemets membrane and large
amounts of stromal edema
Corneal edema after corneal transplant can also be secondary
to corneal graft failure from endothelial dysfunction or corneal
transplant rejection. In those occasions, the edema is not quite so
dramatic. The large fluid clefts in this case series demonstrated
by anterior segment OCT and UBM show focal collections of
fluid rather than a diffuse distribution consistent with corneal
edema secondary to rejection or endothelial failure. Those cases
highlight the importance of clinical suspicion and thorough
diagnostic evaluation to rule out these other causes since the
treatment would be markedly different.
We could not find other reports of patients without a history of
keratoconus who developed hydrops in the donor corneal graft.
An anterior chamber intraocular lens and a glaucoma drainage
tube were the suspected culprits in the two patients who were
surgically treated.
Figure 3: Acute corneal hydrops within a corneal donor graft
Case 2
A 91-year-old Caucasian male with a history of PKP in the right
eye was referred to the clinic for descemetocele evaluation.
He had a corneal transplant of the right eye originally for
pseudophakic bullous keratopathy. The patient reported
266
Hydrops within a corneal donor graft is a rare complication after
corneal transplant for patients with a history of keratoconus. In
prior reports, it was believed to occur in patients who developed
a tear in Descemets membrane within the host corneal rim.
This break would then extend into the donor cornea and allow
the cornea to imbibe the fluid.
The common feature in these patients was eye rubbing,
which might be implicated in the unexpected dislocation of
intraocular devices and damage of the Descemets membrane.
If this important structure is violated, hydrops could ensue.
Corneal transplant patients should be advised not to rub
their eyes.
Middle East African Journal of Ophthalmology, Volume 20, Number 3, July - September 2013
[Downloadedfreefromhttp://www.meajo.orgonWednesday,May07,2014,IP:112.215.66.75]||ClickheretodownloadfreeAndroidapplicationforthisjournal
Cason and Yiu: Acute hydrops in the donor cornea graft in non-keratoconus patients
REFERENCES
1.
2.
Tuft SJ, Gregory WM, Buckley RJ. Acute corneal hydrops in
keratoconus. Ophthalmology 1994;101:1738-44.
Wickremasinghe SS, Smith GT, Pullum KW, Buckley RJ.
Acute hydrops in keratoconus masquerading as acute corneal
transplant rejection. Cornea 2006;25:739-41.
3.
Ezra DG, Mehta JS, Allan BD. Late corneal hydrops after
penetrating keratoplasty for keratoconus. Cornea 2007;26:639-40.
Cite this article as: Cason JB, Yiu SC. Acute Hydrops in the Donor Cornea
Graft in Non-Keratoconus Patients. Middle East Afr J Ophthalmol 2013;20:265-7.
S ource of S upport: Thi s w ork w as supported i n part by an
unrestricted grant from Research to Prevent Blindness, New York, NY,
Conflict of Interest: None declared.
Middle East African Journal of Ophthalmology, Volume 20, Number 3, July - September 2013
267
S-ar putea să vă placă și
- Case Review - EndophthalmitisDocument4 paginiCase Review - EndophthalmitisDr Shawgat Ul Karim KhanÎncă nu există evaluări
- Macular Hole Development After Vitrectomy For Floaters A Case ReportDocument5 paginiMacular Hole Development After Vitrectomy For Floaters A Case Reportmistic0Încă nu există evaluări
- Management of Double-Penetrating Ocular Injury With Retained Intraorbital Metallic Foreign BodyDocument4 paginiManagement of Double-Penetrating Ocular Injury With Retained Intraorbital Metallic Foreign BodyShirakawa AlmiraÎncă nu există evaluări
- Staphylococcus Epidermidis End PDFDocument4 paginiStaphylococcus Epidermidis End PDFNisaÎncă nu există evaluări
- Clinical StudyDocument6 paginiClinical StudyKarina Mega WÎncă nu există evaluări
- Rare Case of A Conjunctival Cyst Formation in An Anophthalmic Socket of A 10 Years Old PatientDocument2 paginiRare Case of A Conjunctival Cyst Formation in An Anophthalmic Socket of A 10 Years Old PatientPeertechz Publications Inc.Încă nu există evaluări
- Posted at The Institutional Resources For Unique Collection and Academic Archives at Tokyo Dental College, Available From Http://ir - Tdc.ac - JPDocument20 paginiPosted at The Institutional Resources For Unique Collection and Academic Archives at Tokyo Dental College, Available From Http://ir - Tdc.ac - JPwhiezardÎncă nu există evaluări
- Aplikasi Lenticule Patch Graft Sebagai Penatalaksaan Perforasi KorneaDocument14 paginiAplikasi Lenticule Patch Graft Sebagai Penatalaksaan Perforasi KorneaAtika AndiantiÎncă nu există evaluări
- Conjunctivitis As A Manifestation of Wegener 'S GranulomatosisDocument5 paginiConjunctivitis As A Manifestation of Wegener 'S GranulomatosisAsd DsaÎncă nu există evaluări
- Endoftalmitis 3Document4 paginiEndoftalmitis 3andisibaÎncă nu există evaluări
- Msor 000504Document3 paginiMsor 000504MudrikahHaniyahÎncă nu există evaluări
- Anterior Vitrectomy and Partial Capsulectomy Anterior Approach To Treat Chronic Postoperative EndophthalmitisDocument3 paginiAnterior Vitrectomy and Partial Capsulectomy Anterior Approach To Treat Chronic Postoperative EndophthalmitisSurendar KesavanÎncă nu există evaluări
- AAO Position Paper Keratoconus 042008Document13 paginiAAO Position Paper Keratoconus 042008Philip McNelsonÎncă nu există evaluări
- Brown DepositsDocument5 paginiBrown DepositsAnkit RaizadaÎncă nu există evaluări
- Abstract Book PVSM2021 FinalDocument374 paginiAbstract Book PVSM2021 FinalnitaÎncă nu există evaluări
- Indications Vitrectomy Retinoschisis: For CongenitalDocument5 paginiIndications Vitrectomy Retinoschisis: For CongenitalRohamonangan TheresiaÎncă nu există evaluări
- Panophthalmitis After Aurolab Aqueous Drainage Implant (AADI) in Refractory Glaucoma With Vogt-Koyanagi-Harada Syndrome (VKH) : A Case ReportDocument4 paginiPanophthalmitis After Aurolab Aqueous Drainage Implant (AADI) in Refractory Glaucoma With Vogt-Koyanagi-Harada Syndrome (VKH) : A Case ReportBOHR International Journal of Current Research in Optometry and Ophthalmology (BIJCROO)Încă nu există evaluări
- IJGMP - Medicine - Clinical Study of DALK in Heterogeneous Corneal Diseases - Srinivas K.HDocument6 paginiIJGMP - Medicine - Clinical Study of DALK in Heterogeneous Corneal Diseases - Srinivas K.Hiaset123Încă nu există evaluări
- Bilateral Proptosis in Acute Leukemia: Irawadi Putra, Ardizal RahmanDocument1 paginăBilateral Proptosis in Acute Leukemia: Irawadi Putra, Ardizal RahmanirawadiputraÎncă nu există evaluări
- Jurnal KoreaDocument7 paginiJurnal KoreachindiaÎncă nu există evaluări
- DjkfhjadsbfjabsDocument31 paginiDjkfhjadsbfjabsRadit FauzieÎncă nu există evaluări
- Herpes Zoster & KatarakDocument6 paginiHerpes Zoster & KatarakSteve aokiÎncă nu există evaluări
- A Clinical Study On Visual Outcome and Complications of Penetrating KeratoplastyDocument12 paginiA Clinical Study On Visual Outcome and Complications of Penetrating KeratoplastyIOSRjournalÎncă nu există evaluări
- Soal RetinaDocument2 paginiSoal RetinaAnggisari Danastri DharmaÎncă nu există evaluări
- External Dacryocystorhinostomy Outcomes in Patients With A History of DacryocystitisDocument9 paginiExternal Dacryocystorhinostomy Outcomes in Patients With A History of DacryocystitisRegina HershaaÎncă nu există evaluări
- Advanced Ophthalmic Diagnostic Procedures and InbstrumentationDocument5 paginiAdvanced Ophthalmic Diagnostic Procedures and InbstrumentationSayoki GhoshÎncă nu există evaluări
- Jurnal Mata 5Document6 paginiJurnal Mata 5Dahru KinanggaÎncă nu există evaluări
- Penetrating Keratoplasty in Active Acanthamoeba KeratitisDocument5 paginiPenetrating Keratoplasty in Active Acanthamoeba Keratitisdrvishalkulkarni2007Încă nu există evaluări
- Uveitis 2Document9 paginiUveitis 2srihandayaniakbarÎncă nu există evaluări
- Posterior Uveitis: Advances in Imaging and TreatmentDe la EverandPosterior Uveitis: Advances in Imaging and TreatmentNarsing A. RaoÎncă nu există evaluări
- Jurding Mata EndophthalamitisDocument24 paginiJurding Mata EndophthalamitisBenk Setsuna F. SeieiÎncă nu există evaluări
- As Oct 3Document5 paginiAs Oct 3Rasha Mounir Abdel-Kader El-TanamlyÎncă nu există evaluări
- A Case of Bilateral Corneal Perforation in A Patient With Severe Dry Eye in IndiaDocument2 paginiA Case of Bilateral Corneal Perforation in A Patient With Severe Dry Eye in IndiaIqbal Farid MunggaranÎncă nu există evaluări
- Epithelial DowngrowthDocument5 paginiEpithelial Downgrowthaghnia jolandaÎncă nu există evaluări
- Clinicopathologic Reports, Case Reports, and Small Case SeriesDocument3 paginiClinicopathologic Reports, Case Reports, and Small Case SeriesDiaz RandanilÎncă nu există evaluări
- Bosch ErDocument8 paginiBosch ErPhilip McNelsonÎncă nu există evaluări
- OpthalmologiDocument7 paginiOpthalmologirais123Încă nu există evaluări
- The Pathogenesis and Prevention of Corneal Graft Melting After KeratoplastyDocument9 paginiThe Pathogenesis and Prevention of Corneal Graft Melting After KeratoplastywahyuÎncă nu există evaluări
- An Incident of Subcutaneous Emphysema Following Laser Tooth ExposureDocument4 paginiAn Incident of Subcutaneous Emphysema Following Laser Tooth ExposureVeronica ChinÎncă nu există evaluări
- Objective Assessment of Symptomatic Vitreous Floaters Using Optical Coherence Tomography A Case ReportDocument3 paginiObjective Assessment of Symptomatic Vitreous Floaters Using Optical Coherence Tomography A Case Reportmistic0Încă nu există evaluări
- Therapeutic Effectiveness of Toric Implantable Collamer Lens in Treating Ultrahigh Myopic AstigmatismDocument7 paginiTherapeutic Effectiveness of Toric Implantable Collamer Lens in Treating Ultrahigh Myopic AstigmatismStephanie PfengÎncă nu există evaluări
- Clinical Characteristics and Surgical Safety in Congenital Cataract Eyes With Three Pathological Types of Posterior Capsule AbnormalitiesDocument9 paginiClinical Characteristics and Surgical Safety in Congenital Cataract Eyes With Three Pathological Types of Posterior Capsule Abnormalitiesaristo callenÎncă nu există evaluări
- Ijo 07 02 264Document9 paginiIjo 07 02 264Imade Candra PÎncă nu există evaluări
- Safety and Efficacy of Colored Iris Reconstruction Lens ImplantationDocument12 paginiSafety and Efficacy of Colored Iris Reconstruction Lens ImplantationDanty IndriastutyÎncă nu există evaluări
- Elevated White Blood Cell Count May Predict Risk of Orbital Implant ExposureDocument5 paginiElevated White Blood Cell Count May Predict Risk of Orbital Implant ExposureSiti AlfianaÎncă nu există evaluări
- 69 EdDocument10 pagini69 EdAnna ListianaÎncă nu există evaluări
- PanAmJOphthalmol211-3727391 102113Document3 paginiPanAmJOphthalmol211-3727391 102113Karina BudijantoÎncă nu există evaluări
- Matching The Patient To The Intraocular Lens Preoperative Considerations To Optimize Surgical OutcomesDocument10 paginiMatching The Patient To The Intraocular Lens Preoperative Considerations To Optimize Surgical Outcomesakun kd876Încă nu există evaluări
- Selamat Dicoba 2009Document38 paginiSelamat Dicoba 2009Rizky AgustriaÎncă nu există evaluări
- Abstractbook2020 2Document50 paginiAbstractbook2020 2alpaslan alkanÎncă nu există evaluări
- Achromobacter Xylosoxidans Keratitis After Contact Lens UsageDocument5 paginiAchromobacter Xylosoxidans Keratitis After Contact Lens UsageDenata PrabhasiwiÎncă nu există evaluări
- 2015 Article 36Document8 pagini2015 Article 36SUSPAÎncă nu există evaluări
- 135 139 PDFDocument5 pagini135 139 PDFBramantya WuÎncă nu există evaluări
- Sutureless and Glue Free Conjunctivo-Limbal Autograft in Primary Pterygium Surgery - Outcome S and Recurrence RateDocument8 paginiSutureless and Glue Free Conjunctivo-Limbal Autograft in Primary Pterygium Surgery - Outcome S and Recurrence RateThomas KweeÎncă nu există evaluări
- Persistent Corneal Edema After Collagen Cross-Linking For KeratoconusDocument6 paginiPersistent Corneal Edema After Collagen Cross-Linking For KeratoconusRestu MegantaraÎncă nu există evaluări
- Basak 2012Document3 paginiBasak 2012funtyms4uÎncă nu există evaluări
- Sulcus Implantation of A Single-Piece Foldable Acrylic Intraocular Lens After Posterior Capsular Rupture in Cataract SurgeryDocument6 paginiSulcus Implantation of A Single-Piece Foldable Acrylic Intraocular Lens After Posterior Capsular Rupture in Cataract SurgeryPrizilia SaimimaÎncă nu există evaluări
- Keratoconus: Picture 1Document6 paginiKeratoconus: Picture 1BuiyiWongÎncă nu există evaluări
- Keratoconus: Picture 1Document6 paginiKeratoconus: Picture 1BuiyiWongÎncă nu există evaluări
- Surgical Management of Childhood Glaucoma: Clinical Considerations and TechniquesDe la EverandSurgical Management of Childhood Glaucoma: Clinical Considerations and TechniquesAlana L. GrajewskiÎncă nu există evaluări
- Herpes Blood TestsDocument1 paginăHerpes Blood TestsApril FoleyÎncă nu există evaluări
- Herpes, Genital: Basic Information Description Possible ComplicationsDocument1 paginăHerpes, Genital: Basic Information Description Possible ComplicationsApril FoleyÎncă nu există evaluări
- Jurnal Zinc AsliDocument10 paginiJurnal Zinc AsliApril FoleyÎncă nu există evaluări
- LicenseDocument2 paginiLicenseDidit AgusÎncă nu există evaluări
- Gambar EarDocument11 paginiGambar EarApril FoleyÎncă nu există evaluări
- 3a. OMADocument15 pagini3a. OMAApril FoleyÎncă nu există evaluări
- GLP BmsDocument18 paginiGLP BmsDr.Subhashish TripathyÎncă nu există evaluări
- 3.1 - Sequences and SeriesxbxhhdDocument92 pagini3.1 - Sequences and SeriesxbxhhdHelloÎncă nu există evaluări
- Intumescent Paint For Steel NZ - Coating - Co.nzDocument8 paginiIntumescent Paint For Steel NZ - Coating - Co.nzPeter ThomsonÎncă nu există evaluări
- Abnormalities of Placenta, Amniotic Fluid and Cord: Prepared By, B. Ezhilarasi, Nursing TutorDocument21 paginiAbnormalities of Placenta, Amniotic Fluid and Cord: Prepared By, B. Ezhilarasi, Nursing TutorGopala KrishnanÎncă nu există evaluări
- Abdominal Examination OSCE GuideDocument30 paginiAbdominal Examination OSCE Guideزياد سعيدÎncă nu există evaluări
- Natural Disasters Vocabulary Exercises Fun Activities Games Icebreakers Oneonone Activiti 42747Document2 paginiNatural Disasters Vocabulary Exercises Fun Activities Games Icebreakers Oneonone Activiti 42747Andrea Tercero VillarroelÎncă nu există evaluări
- Chapter 5 AGVDocument76 paginiChapter 5 AGVQuỳnh NguyễnÎncă nu există evaluări
- YellowstoneDocument1 paginăYellowstoneOana GalbenuÎncă nu există evaluări
- (G. Lakshmi Narasaiah) Finite Element Analysis PDFDocument349 pagini(G. Lakshmi Narasaiah) Finite Element Analysis PDFmoljaime1326Încă nu există evaluări
- Basses: Pricelist March 2019Document3 paginiBasses: Pricelist March 2019zhaihaijunÎncă nu există evaluări
- Single Door Feeder Pillar 200A MCCBDocument1 paginăSingle Door Feeder Pillar 200A MCCBMiqdad AliÎncă nu există evaluări
- Siprotec 7ut82 ProfileDocument2 paginiSiprotec 7ut82 ProfileOliver Atahuichi TorrezÎncă nu există evaluări
- (Eng) Zx890lch 5a Ks En316Document13 pagini(Eng) Zx890lch 5a Ks En316MC TAK LEEÎncă nu există evaluări
- Mathematical Modeling of Mechanical Systems and Electrical SystemsDocument49 paginiMathematical Modeling of Mechanical Systems and Electrical SystemsMary DunhamÎncă nu există evaluări
- 10th Aug. 2011 Structural Calculation (For Sub.) - 03Document29 pagini10th Aug. 2011 Structural Calculation (For Sub.) - 03Nguyễn Tiến Việt100% (1)
- Course Structure and Content For Mechatronics, Systems and CDocument32 paginiCourse Structure and Content For Mechatronics, Systems and CAnimonga HajimeÎncă nu există evaluări
- Nutrient DeficiencyDocument8 paginiNutrient Deficiencyfeiserl100% (1)
- Drug Study LidocaineDocument15 paginiDrug Study LidocaineFrancym R. BatengaÎncă nu există evaluări
- CE Review GEOMETRY 2Document6 paginiCE Review GEOMETRY 2Paul Gerard AguilarÎncă nu există evaluări
- Dizziness - Vertigo and HomoeopathyDocument38 paginiDizziness - Vertigo and HomoeopathyDr. Rajneesh Kumar Sharma MD HomÎncă nu există evaluări
- THE WEATHER LISTENING - Stalin GuañunaDocument1 paginăTHE WEATHER LISTENING - Stalin GuañunaSTALIN JESUS GUA�UNA CHICAIZAÎncă nu există evaluări
- Army Aviation Digest - Nov 1978Document52 paginiArmy Aviation Digest - Nov 1978Aviation/Space History Library100% (1)
- Product Lifecycle Management and Sustainable Development in The Context of Industry 4.0: A Systematic Literature ReviewDocument10 paginiProduct Lifecycle Management and Sustainable Development in The Context of Industry 4.0: A Systematic Literature ReviewJosip StjepandicÎncă nu există evaluări
- YogaDocument116 paginiYogawefWE100% (2)
- Relationships, 365 Day Devotional Mylesunroe 377pgDocument377 paginiRelationships, 365 Day Devotional Mylesunroe 377pgEla100% (7)
- Fret Position Calculator - StewmacDocument1 paginăFret Position Calculator - StewmacJuan Pablo Sepulveda SierraÎncă nu există evaluări
- Resumen C37 010 Aplicacion de Breaker Disenados IC Simetrica PDFDocument9 paginiResumen C37 010 Aplicacion de Breaker Disenados IC Simetrica PDFglendathais100% (1)
- PEDocument12 paginiPEMae Ann Base RicafortÎncă nu există evaluări
- Michelle LeBaron, Venashri - Pillay) Conflict AcrosDocument241 paginiMichelle LeBaron, Venashri - Pillay) Conflict AcrosBader100% (2)
- Chapter 04 Product and ServDocument43 paginiChapter 04 Product and ServAlireza AlborziÎncă nu există evaluări