Documente Academic
Documente Profesional
Documente Cultură
Primary Peritonitis
Încărcat de
dietho666Titlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Primary Peritonitis
Încărcat de
dietho666Drepturi de autor:
Formate disponibile
ACTA FAC MED NAISS
UDC 616.381-002
Professional article
ACTA FAC MED NAISS 2008; 25 (3): 133-138
Milan Radojkovic,Miroslav Stojanovic
Aleksandar Zlatic, Ljiljana Jeremic-Savic
Danijela Radojkovic
Mirjana Radisavljevic
Surgical Clinic, Clinical Center Nis
Clinic for endocrinology,
diabetes and metabolic diseases,
Clinical Center Nis
Clinic for gastroenterology
and hepatology, Clinical Center Nis
PRIMARY PERITONITIS
SUMMARY
Due to its relatively low incidence, unspecific etiopathogenesis, often
vague simptomatology and complex multidisciplinary treatment primary
peritonitis remains a diagnostic and therapeutic challenge for a physician,
especially for the general surgeons who most commonly deal with
intraabdominal infections that are the result of a hollow viscus perforation
(secondary peritonitis). Primary peritonitis as challenging multidisciplinary
clinical entity and possible surgical problem is under review in presenting paper.
The definition, incidence, pathogenesis, microbiological etiology, clinical
presentation, diagnosis, treatment and prevention are analyzed in order to
provide with updated information most valuable for adequate management of
this serious clinical condition.
Key words: primary peritonitis, cirrhosis, ascites
INTRODUCTION
Peritonitis implies an inflammatory
response of the abdominal cavity peritoneal layer in
terms of an activation of local mediator cascades by
different stimuli (1). Viral, bacterial and chemical
agents and trauma may be involved in the
etiopathogenesis of peritoneal inflammation. In
surgical practice, trauma, bacterial and sometimes
chemical agents are the most frequent causes of
peritonitis (1,2). The terms intraabdominal infection
and abdominal sepsis are often used to describe
peritonitis of an infectious etiology. Peritonitis is
classified into three specific types, depending on the
clinical scenario: primary, secondary or tertiary,
each representing a distinct clinical entity. In most of
the different forms of peritonitis there is the main,
surgically relevant underlying problem associated
with abdominal sepsis. However, peritonitis is
inhomogenous in regard to the cause, pathophysiology and severity. Considering that these aspects
influence the choice of therapy and prognosis, each
individual case of peritonitis needs profound consideration. Due to its relatively low incidence, unspecific etiopathogenesis, often vague simptomatology and complex multidisciplinary treatment, primary peritonitis remains a diagnostic and therapeutic
challenge for a physician, especially for the general
surgeons who most commonly deal with
intraabdominal infections that are the result of a
hollow viscus perforation (secondary peritonitis).
Primary peritonitis as challenging multidisciplinary
clinical entity and possible surgical problem is under
review in presenting paper.
DEFINITION AND INCIDENCE
Primary peritonitis is an infection of the
peritoneal cavity not directly related to other
intraabdominal abnormalities. This term describes a
peritoneal infection without an evident source. Since
the vast majority of cases are due to bacterial
Corresponding author. Milan Radojkovic Phone: +38118238563, +381637165677 E-mail: mida@bankerinter.net
133
Milan Radojkovic, Miroslav Stojanovic, Aleksandar Zlatic, Ljiljana Jeremic-Savic, Danijela Radojkovic, Mirjana Radisavljevic
infection, this condition is also commonly known as
spontaneous bacterial peritonitis. In primary
peritonitis, bacteria invade the peritoneal cavity from
a suspected extraperitoneal source via a hematogeneous, lymphogeneous or luminal route.
Although a rare condition, in adults primary
peritonitis develops in up to 25% of patients with
alcoholic cirrhosis. Also, it has been reported to
occur in patients with postnecrotic cirrhosis, chronic
active hepatitis, acute viral hepatitis, congestive
heart failure, metastatic malignant (especially liver)
disease, systemic lupus erythematosus, lymphedema
and rarely in adults with no underlying disease (3).
The presence of ascites appears to be a common link
among these various conditions (Table 1).
Table 1. Risk factors for ascitic fluid infection
- Severe liver disease (cirrhosis Child-Pugh C)
- Low total protein concentration in ascitic fluid
(<1,5gm/dL, especially if <1,0gm/dL)
- Esophageal variceal or gastrointestinal bleeding
- Urinary tract infection
- Intestinal bacterial overgrowth
- Previous spontaneous bacterial peritonitis
- Iatrogenic factors
(urinary bladder and intravascular catheters etc.)
Today, spontaneous peritonitis in adults due
to liver cirrhosis is considered to be an episode of
liver failure indicating the necessity of liver
transplantation (4). Primary bacterial peritonitis is
also the most common complication in patients with
chronic renal failure undergoing continuous
ambulatory peritoneal dialysis (CAPD) and is
considered to be a distinct entity. Overall, the
average incidence of this infection is 1,3-1,4
episodes per CAPD patient per year (5). More than
half of these episodes are experienced by only 25%
of patients. In children, in the preantibiotic era
primary peritonitis accounted for about 10% of all
pediatric abdominal emergencies. It now accounts
for less than 1-2% (6). The decline has been
attributed to widespread use of antibiotics for minor
upper respiratory tract illness. Although primary
peritonitis may occur in children without
predisposing disease, it is especially associated with
postnecrotic cirrhosis and nephrotic syndrome.
PATHOGENESIS
Although the route of infection in primary
peritonitis is usually not apparent, it is thought to be
hematogenous, lymphogenous, via transmural
migration through an intact gut wall from the
intestinal lumen or, in women, from the vagina via
the fallopian tubes (Table 2).
134
Table 2. Pathogenesis of primary peritonitis
Primary peritonitis
Bacterial invasion
- Hematogenous
- Lymphatic
-Intraluminal (transmural)
In cirrhotic patients the hematogenous route
is most likely: microorganisms removed from
circulation by the liver may contaminate hepatic
lymph and pass through the permeable lymphatic
walls into the ascitic fluid. In addition, portosystemic
shunting greatly diminishes hepatic clearance of
bacteremia, which would tend to perpetuate
bacteremia and increase the opportunity to cause
metastatic infection at susceptible sites, such as the
ascitic collection. The infrequency of primary
peritonitis in forms of ascites other than that due to
liver disease emphasizes the importance of
intrahepatic shunting in the pathogenesis of this
disease. The hepatic reticuloendothelial system is
known to be a major site for removal of bacteria from
blood and destruction of blood-borne bacteria by the
reticuloendothelial system is impaired in animal
experimental cirrhosis and in alcoholic liver disease.
The decrease in phagocytic activity seen in alcoholic
cirrhosis is proportional to the severity of the liver
disease.
Enteric bacteria may also gain access to the
peritoneal cavity by directly traversing the intact
intestinal wall. The infrequent occurrence of
bacteremia and the multiplicity of species in
peritoneal fluid when anaerobic bacteria are
involved suggest that transmural migration of
bacteria is the probable route of infection of ascitic
fluid in most of these patients.
In prepubertal girls, the pathogenesis of
primary peritonitis is likely related to an ascending
infection of genital origin, as suggested by the
simultaneous presence of pneumococci in vaginal
secretions and peritoneal fluid. Alkaline vaginal
secretions that occur in this age group may be less
inhibitory to bacterial growth than the acidic
secretions of postpubertal females. Transfallopian
spread is also suggested by the development of
primary peritonitis in women with intrauterine
devices. The route of spread in women with
gonococcal or chlamydial perihepatitis (Fitz-HughCurtis syndrome) is presumably via the fallopian
tubes and paracolic gutters to the subphrenic space,
but it may also be hematogenous.
Tuberculous patients are considered to be a
distinct category of patients exposed to the risk of
primary peritonitis development. Although tuberculous peritonitis may result from direct entry into the
peritoneal cavity of tubercle bacilli (from the lymph
nodes, intestine or genital tract in patient with active
Primary peritonitis
disease of these organs), it is more likely to be
disseminated hematogenously from remote foci of
tuberculosis, most commonly in the lung.
Tuberculous peritonitis may become clinically
evident after the initial focus has completely healed.
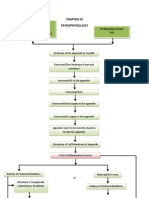
Pathophysiology of peritonitis includes complex
interactions between various triggers of the mediator
cascade, endogenous mediators and host responses
(Figure 1).
Bacteria
peritonitis may also be caused by Neisseria
gonorrhoeae, Chlamydia trachomatis, Mycobacterium tuberculosis or Coccidioides immitis.
Patients who have positive cultures of ascitic
fluid with few leukocytes and no clinical signs of
peritonitis are considered to have bacterascites. This
may represent early colonization of ascites before a
host response. Mortality among patients with a low
leukocyte response is the same as among those with a
Endotoxin
Superantigen
Activation of PMN, monocytes, complement
system, endothelial cells and others
Complex interactions between exogenous and
endogenous mediators and host responses
Defense prevails
attack
Local infection
Local infection is
overwhelmed
Systemic illness up to
septic shock and MOF
PMN polymorphonuclear leucocytes; MOF multiorgan failure;
Figure 1. Pathophysiology of peritonitis (endotoxin: trigger of the mediator cascade)
MICROBIOLOGY
Primary peritonitis represent an infection
that is microbiologically distinct from other
peritoneal infections because it is usually monomicrobial. In nephrotic children the most frequent
primary peritonitis are due to gram-negative enteric
bacilli and staphylococci, while streptococcal
peritonitis has declined. In cirrhotic patients,
microorganisms of enteric origin account for
approximately 70% of the causative pathogens.
E.coli is the most frequently discovered pathogen,
followed by Klebsiella pneumoniae, S.pneumoniae
and other streptococcal species, including enterococci. Staphylococcus aureus is an unusual cause of
primary peritonitis, accounting for only 2-4% of
cases, but has been noted especially in patients with
erosion of an umbilical hernia. Anaerobes and
microaerophilic organisms are infrequently reported
(7). Possible explanations include the intrinsic
bacteriostatic activity of ascites against Bacteroides
species, the relatively high pO2 of ascitic fluid and
the lack of optimal anaerobic bacteriologic
techniques used to study patients in the past. The
presence of anaerobes correlates strongly with
polymicrobial infection. Occasionally, primary
greater response. Conversely, several series have
identified cases of primary peritonitis with negative
ascitic fluid cultures, termed culture-negative
neutrocytic ascites (8). Blood-cultures are positive in
1/3 of these patients. The frequency of negative
results of ascitic fluid cultures may be decreased by
inoculating blood culture bottles with ascitic fluid at
the bedside.
CLINICAL PRESENTATION
AND DIAGNOSIS
In children, primary peritonitis is an acute
febrile illness often confused with acute appendicitis. Fever, abdominal pain, nausea, vomiting and
diarrhea usually occur, with palpatory diffuse
abdominal tenderness, rebound tenderness and
hypoactive or absent bowel sounds. In cirrhotic
patients the clinical manifestation of primary
peritonitis may be atypical. Onset may be insidious,
without findings of peritoneal irritation. Fever
(>38,5) is the most common presenting sign,
occuring in 50-80% of cases and even in the absence
of abdominal signs or symptoms. Primary peritonitis
should always be considered in the differential
diagnosis of decompensation of previously stable
135
Milan Radojkovic, Miroslav Stojanovic, Aleksandar Zlatic, Ljiljana Jeremic-Savic, Danijela Radojkovic, Mirjana Radisavljevic
chronic liver disease, especially hepatic encephalopathy. Primary tuberculous peritonitis is usually
gradual in onset, with fever, weight loss, malaise,
night sweats and abdominal distension. The
abdomen may not be rigid and is often characterized
as being doughy on palpation. The findings at
diagnostic surgery or laparoscopy consist of multiple
nodules scattered over the peritoneal surface and
omentum. Adhesiones and a variable amount of
peritoneal fluid are usually present. Similarly,
Coccidioides immitis can cause a granulomatous
peritonitis with variable clinical manifestations.
Although the diagnosis of primary peritonitis can be established with certainty only after
thorough laparotomy to exclude a primary intraabdominal site of infection, it can usually be surmised
from examination of the peritoneal fluid (Table 3).
Table 3. Indications for diagnostic paracenthesis
- New onset of ascites
- Hospital admission in a patient with
known ascites
- Clinical deterioration (onset of abdominal
symptoms) in a patient with cirrhosis
and ascites
- Azotemia
- Hepatic encephalopathy
- Gastrointestinal bleeding
- Deterioration in laboratory test values
(leucocytosis etc.)
Fluid obtained at paracentesis should be
analyzed for cell count, differential count and protein
concentration and a gram-staining and culture should
be performed (Table 4). Specimens for culture
should be sent in an airless, capped syringe or
injected directly into aerobic and anaerobic broth
culture media. Volumes of >10ml will increase the
yield of cultures (6). A gram-stain of the sediment is
diagnostic when positive, but is more commonly
negative. Bacteremia occurs in up to 75% of patients
with primary peritonitis due to aerobic bacteria, but it
is rare in those with peritonitis due to anaerobes.
Usually the same organisms isolated from the
peritoneal fluid are discovered in the blood. The
ascitic fluid protein concentration may be low
(<3,5g/L) because of hypoalbuminemia and dilution
with transudate from the portal system. The
leukocyte count in peritoneal fluid usually is
>300/mm (>1000/mm in 85%), with granulocytes
predominating in >80% of cases. However, the total
leukocyte count of some patients with ascites
uncomplicated by infection may be similarly
elevated. Indeed, an increase in ascitic leukocyte
counts has been noted during diuresis in patients with
chronic liver disease. Other parameters of ascitic
136
fluid that may help in diagnosing primary bacterial
peritonitis are pH and lactate concentration. An
ascitic fluid pH of <7.35 and a lactate concentration
of >25mg/dL are more specific but less sensitive than
a leukocyte count of >500/mm for diagnostic
purposes. Still, using all three parameters together
increases the diagnostic accuracy.
Table 4. Analysis of ascitic fluid
Routine
-Total protein
-Albumin
Optional
Unusual
- Gram stain - Cytology
- Amylase - Acid-fast
bacillus smear
and culture
-Cell count with WBC - LDH
- Triglycerides
differential
-Culture in bllood
- Glucose
culture bottles
In patients with negative ascitic fluid
cultures, laparoscopic peritoneal examination and
biopsy may be necessary. Peritonitis secondary to
other intraabdominal causes should be excluded and
specimens for fungal and mycobacteriologic
cultures should be obtained. In children, if gramnegative organisms, a mixed flora or no organisms
are obtained from peritoneal fluid, full exploratory
laparotomy is generally indicated to rule out possible
intraabdominal sources of continuing peritoneal
contamination. However, in end-stage cirrhotic
patients exploratory laparotomy may be lifethreatening and the likelihood of finding a primary
intraabdominal focus may be small. Surgery for
these patients can be deferred while the response to
antimicrobial therapy is awaited. Patients with
primary peritonitis usually respond within 48 hours
to appropriate antimicrobial therapy. The rapid
decrease of the number of ascitic fluid leukocytes
that can be observed after initiation of antimicrobial
therapy for primary peritonitis has been found to help
differentiate primary from secondary bacterial
peritonitis (9).
In patients with a subacute or chronic course
of primary peritonitis, other pathogens must be
considered, including M.tuberculosis or C.immitis.
The diagnosis of tuberculous peritonitis can usually
be made at operation or laparoscopy and confirmed
by the histologic characteristics and bacteriologic
examination of the peritoneal biopsy specimen and
fluid. The diagnosis of C.immitis peritonitis can be
made with a wet mount of ascitic fluid, by finding the
organism in culture or on histologic examination.
MANAGEMENTAND PREVENTION
Traditional therapy for peritonitis is
presented in Table 5. Because the gram stain is
Primary peritonitis
frequently negative in primary bacterial peritonitis,
the initial choice of antimicrobial drug is often
empirical, based on the most likely pathogens. Some
of the third-generation cephalosporin antibiotics
have been demonstrated to be as efficacious as the
combination of ampicillin plus an aminoglycoside in
primary bacterial peritonitis. They also eliminate the
risk of nephrotoxicity, which is sufficiently frequent
in this group of patients to warrant avoidance of
aminoglycosides if an equally effective alternative
antimicrobial regimen can be used. Other
antimicrobial agents such as the broad-spectrum
penicillins (e.g., mezlocillin, ticarcillin, and
piperacillin), carbapenems (e.g., imipenem) and lactam antibiotic/-lactamase inhibitor combinations (e.g., ticarcillin-clavulanate and ampicillinsulbactam) are potential alternatives. If peritonitis
develops during hospitalization, the therapeutic
regimen such as administration of an aminoglycoside antibiotic and an antipseudomonal penicillin
or cephalosporin in combination, should also be
active against Pseudomonas aeruginosa. For those
situations in which the gram stain is suggestive of a
Bacteroides species or polymicrobial peritonitis is
evident, antimicrobials with activity against the
Bacteroides fragilis group and other anaerobic
organisms should be added (e.g., metronidazole,
clindamycin). The antimicrobial regimen can be modified once the results of the culture and susceptibility tests are available (Table 6).
In cases where there is a strong clinical
suspicion of primary bacterial peritonitis, but all
cultures are sterile, antimicrobial therapy should be
continued. Clinical improvement, together with a
significant decline in the ascitic fluid leukocyte
count, should occur after 24-48 hours of
antimicrobial therapy if the diagnosis is correct.
Failure to respond should prompt an examination for
additional pathological conditions. Antimicrobial
therapy is usually continued for 10-14 days if
improvement is noted, but short-course therapy for 5
days has been shown to be as efficacious as the
longer course in some patients. Administration of
intraperitoneal antimicrobials is not necessary.
Table 5. Traditional therapy for peritonitis
- Alimentary decompression
- Fluid resuscitation
- Systemic antibiotics
- Contamination source control
Treatment of primary peritonitis is successful in more than one-half of cirrhotic patients, but
because of the underlying liver condition the overall
mortality has been reported as high as 95% in some
series. Those patients with the poorest prognosis
were found to have renal insufficiency, hypothermia,
hyperbilirubinemia and hypoalbuminemia (10).
Treatment of peritonitis caused by gram-positive
organisms, as well as of early infections, has been
more frequently successful than treatment of gramnegative or late infections. In nephrotic patients with
gram-positive infections or in patients who do not
have a preterminal underlying illness, the survival
rate is >90%.
Table 6. Surgical Infection Society guidelines
for antibiotic treatment of established peritonitis
Single agents:
- ampicillin-sulbactam
- cephalosporins (according to antibiogram)
- imipenem-cilastatin
- meropenem
- piperacillin-tazobactam
- ticarcillin-clavulanic acid
Combination regimens:
- aminoglycoside plus antianaerobe
- aztreonam plus clindamycin
- cefuroxime plus metronidazole
- ciprofloxacin plus metronidazole
- III and IV generation cephalosporins
plus antianaerobe
Considering the common occurrence and
high mortality of primary peritonitis in the setting of
cirrhosis with ascites, prevention is a desirable
strategy. This is particularly true for patients who are
awaiting liver transplantation. Selective decontamination of the gut with oral norfloxacin (400mg daily)
has been shown to reduce the incidence of spontaneous bacterial peritonitis. Norfloxacin has the disadvantage of selecting for gram-positive organisms,
including S.aureus and quinolone-resistant gramnegative organisms. More recently, trimethoprimsulfamethoxazole (double-strenght, given once daily
for 5 days each week) has been shown to be welltolerated and reduce the incidence of peritonitis (11).
A survival-rate advantage has not been demonstrated
for any of these preventive regimens.
137
Milan Radojkovic, Miroslav Stojanovic, Aleksandar Zlatic, Ljiljana Jeremic-Savic, Danijela Radojkovic, Mirjana Radisavljevic
REFERENCES
1. Hau T. Bacteria, toxins and the peritoneum. World J
Surg 1990; 14: 167-175.
2. McClean KL, Sheehan GJ, Harding GK.
Intraabdominal infection: a review. Clin Infect Dis 1994; 19:
100-116.
3. Conn HO, Fessel JM. Spontaneous bacterial
peritonitis in cirrhosis: variations on a theme. Medicine
(Baltimore) 1971; 50: 161-197.
4. Bac DJ. Spontaneous bacterial peritonitis: an
indication for liver transplantation? Scand J Gastroenterol 1996;
(Suppl) 218: 38-42.
5. Linblad AS, Novak JW, Nolph KD, Stablein DM,
Cutler SJ. The 1987 USA National CAPD Registry report. Trans
Am SocArtif Intern Organs 1988; 34: 150-156.
6. Runyon BA, Umland ET, Merlin T. Inoculation of
blood culture bottles with ascitic fluid: improved detection of
spontaneous bacterial peritonitis. Arch Intern Med 1987; 147:
73-75.
7. Sheckman P, Onderdonk AB, Bartlett JG.
Anaerobes in spontaneous peritonitis (letter). Lancet 1977; 2:
1223.
8. Runyon BA, Hoefs JC. Culture-negative
neutrocytic ascites: a variant of spontaneous bacterial peritonitis.
Hepatology 1984; 4: 1209-11.
9. Runyon BA, Hoefs JC. Ascitic fluid analysis in the
differentiation of spontaneous bacterial peritonitis from
gastrointestinal tract perforation into ascitic fluid. Hepatology
1984; 4: 447-50.
10. Weinstein MP, Iannini PB, Stratton CW, Eickhoff
TC. Spontanous bacterial peritonitis: a review of 28 cases with
emphasis on improved survival and factors influencing
prognosisAm J Med 1978; 64: 592-8.
11. Singh N, Gayowski T, Yu VL, Wagener MM.
Trimethoprim-sulfamethoxazole for the prevention of
spontaneous bacterial peritonitis in cirrhosis: a randomized trial.
Ann Intern Med 1995; 122: 595-8.
PRIMARNI PERITONITIS
Milan Radojkovi1, Danijela Radojkovi2, Miroslav Stojanovi1, Aleksandar Zlati1,
Ljiljana Jeremi-Savi1, Mirjana Radisavljevi3
1
Hirurka klinika, Kliniki centar Ni
Klinika za endokrinologiju, dijabetes i bolesti metabolizma, Kliniki centar Ni
3
Klinika za gastroenterologiju i hepatologiju, Kliniki centar Ni
SAETAK
Zahvaljujui relativno niskoj incidenci, nespecifinoj etiopatogenezi, esto
neodreenoj simptomatologiji i kompleksnom multidisciplinarnom leenju, primarni
peritonitis i dalje predstavlja dijagnostiki i terapijski izazov za kliniara, a posebno za opte
hirurge koji najee lee intraabdominalne infekcije, koje nastaju kao rezultat perforacije
upljih trbunih organa (sekundarni peritonitis). Prezentovani rad predstavlja pregled
literaturnih podataka o primarnom peritonitisu kao izazovnom multidisciplinarnom
klinikom entitetu i moguem hirurkom problemu. Data je definicija i analizirani su podaci i
dileme o incidenci, patogenezi, mikrobiolokim uzronicima, klinikoj prezentaciji, dijagnozi,
leenju i prevenciji primarnog peritonitisa u cilju pruanja savremenih informacija i stavova
najznaajnijih za adekvatan tretman ovog ozbiljnog klinikog stanja.
Kljune rei: primarni peritonitis, ciroza, ascites
138
S-ar putea să vă placă și
- Peritonitis Update On Pathophysiology, Clinical Manifestations, and PDFDocument11 paginiPeritonitis Update On Pathophysiology, Clinical Manifestations, and PDFAnonymous InJS6aYZ100% (1)
- Placino HIRSCHPRUNG DX PDFDocument15 paginiPlacino HIRSCHPRUNG DX PDFSiena PlacinoÎncă nu există evaluări
- Burn Ctu 312 - 2Document1 paginăBurn Ctu 312 - 2Shaira Ann CalambaÎncă nu există evaluări
- Drug StudyDocument5 paginiDrug StudyJanine Erika Julom BrillantesÎncă nu există evaluări
- SucralfateDocument3 paginiSucralfateViziteu AlexandraÎncă nu există evaluări
- Epidemiology and Pathophysiology of Colonic Diverticular DiseaseDocument8 paginiEpidemiology and Pathophysiology of Colonic Diverticular DiseaseAnonymous Hz5w55Încă nu există evaluări
- Subjective Cues:: IndependentDocument4 paginiSubjective Cues:: IndependentitsmeayaÎncă nu există evaluări
- Intestinal ObstructionDocument27 paginiIntestinal ObstructionAna AvilaÎncă nu există evaluări
- Bioethical, Legal IssuesDocument6 paginiBioethical, Legal IssuesAlyxen PelingenÎncă nu există evaluări
- Pathophysiology of Hypovolemic ShockDocument5 paginiPathophysiology of Hypovolemic ShockIan Rama100% (1)
- Colon Cancer Introduction Case StudyDocument1 paginăColon Cancer Introduction Case StudyHaru ZenkonsteinÎncă nu există evaluări
- NCP AgnDocument2 paginiNCP Agnj3nann3Încă nu există evaluări
- Assessment Nursing Diagnosis Planning Nursing Interventions Rationale EvaluationDocument5 paginiAssessment Nursing Diagnosis Planning Nursing Interventions Rationale EvaluationMeena KoushalÎncă nu există evaluări
- Pa Tho Physiology of RaDocument7 paginiPa Tho Physiology of Ralisalmar2008Încă nu există evaluări
- Drug StudyDocument13 paginiDrug StudyClarkEstacioÎncă nu există evaluări
- Upper Gastrointestinal Bleeding Case StudyDocument5 paginiUpper Gastrointestinal Bleeding Case StudyClaudine Lacaden0% (1)
- What Is PeritonitisDocument9 paginiWhat Is PeritonitisArsitoÎncă nu există evaluări
- Background of The Study ExampleDocument2 paginiBackground of The Study ExampleJohn Paulo RodriguezÎncă nu există evaluări
- Case Scenario (Lung Cancer)Document12 paginiCase Scenario (Lung Cancer)Mitzi CastuloÎncă nu există evaluări
- Case Scenario Dengue FeverDocument2 paginiCase Scenario Dengue FeverJaslir MendozaÎncă nu există evaluări
- AzithromycinDocument4 paginiAzithromycinBrittany ClontzÎncă nu există evaluări
- Case Study 2Document13 paginiCase Study 2api-271069101Încă nu există evaluări
- Course in The WardDocument7 paginiCourse in The WardKevin CalaraÎncă nu există evaluări
- Lymphangitis LymphadenitisDocument5 paginiLymphangitis LymphadenitisGabriela Cocieru MotelicaÎncă nu există evaluări
- Case Study Ugib Lower MBDocument65 paginiCase Study Ugib Lower MBQuolette Constante100% (1)
- DiverticulitisDocument15 paginiDiverticulitisElisabeth MelisaÎncă nu există evaluări
- Appendectomy: NCP For CholecystectomyDocument16 paginiAppendectomy: NCP For CholecystectomyBenjie ArelÎncă nu există evaluări
- Acute AppendicitisDocument23 paginiAcute AppendicitisSandie Daniel GabalunosÎncă nu există evaluări
- Acute PancreatitisDocument10 paginiAcute PancreatitisAndrés Menéndez RojasÎncă nu există evaluări
- GlomerulonephritisDocument4 paginiGlomerulonephritisMary Cris BasayaÎncă nu există evaluări
- Or RRLDocument4 paginiOr RRLAlponce Edal AdagÎncă nu există evaluări
- Case Pres A1-RhdDocument11 paginiCase Pres A1-RhdCharm TanyaÎncă nu există evaluări
- Abdominal Aortic AneurysmDocument44 paginiAbdominal Aortic Aneurysmalebelucci69Încă nu există evaluări
- Pathophysiology Precipitsting Factors: Predisposing FactorsDocument2 paginiPathophysiology Precipitsting Factors: Predisposing FactorsGeofrey MaglalangÎncă nu există evaluări
- Sample Case Study SLE ExacerbationDocument4 paginiSample Case Study SLE ExacerbationNicole BrassingtonÎncă nu există evaluări
- Risk For Bleeding - Cirrhosis NCPDocument2 paginiRisk For Bleeding - Cirrhosis NCPPaula AbadÎncă nu există evaluări
- Crizotinib Improves ProgressionDocument3 paginiCrizotinib Improves ProgressionIsabella RoselliniÎncă nu există evaluări
- Diabetic Nephropathy - Practice Essentials, Pathophysiology, EtiologyDocument6 paginiDiabetic Nephropathy - Practice Essentials, Pathophysiology, EtiologyIrma KurniawatiÎncă nu există evaluări
- Penicillin GDocument2 paginiPenicillin Gapi-295691235Încă nu există evaluări
- Bleeding Peptic Ulcer Disease Case StudyDocument17 paginiBleeding Peptic Ulcer Disease Case StudyChino Dela Cruz100% (2)
- Febrile SeizureDocument6 paginiFebrile SeizurepipimseptianaÎncă nu există evaluări
- Ulcerative ColitisDocument18 paginiUlcerative ColitisHoussein EL HajjÎncă nu există evaluări
- Case Study 3D FinaaaalDocument34 paginiCase Study 3D FinaaaalPaul AnteÎncă nu există evaluări
- The Pathophysiology of Peptic UlcerDocument15 paginiThe Pathophysiology of Peptic UlcerKike Meneses100% (1)
- Case Study PneumoniaDocument10 paginiCase Study PneumoniaGrace Ann67% (3)
- Part 1Document37 paginiPart 1anon_154149519Încă nu există evaluări
- NCP Ko BabyDocument3 paginiNCP Ko BabyDaniel ApostolÎncă nu există evaluări
- RRS at RRLDocument19 paginiRRS at RRLNicole MangosanÎncă nu există evaluări
- CASE STUDY PheumoniaDocument5 paginiCASE STUDY PheumoniaEdelweiss Marie CayetanoÎncă nu există evaluări
- Effectiveness of Milieu Therapy To Patients As Perceived by The Nursing Students Assigned at The Cavite Center For Mental HealthDocument68 paginiEffectiveness of Milieu Therapy To Patients As Perceived by The Nursing Students Assigned at The Cavite Center For Mental Healthjeko23Încă nu există evaluări
- Drug StudyDocument40 paginiDrug StudyLyka Milo AvilaÎncă nu există evaluări
- Pathophysiology of HyperthyroidismDocument4 paginiPathophysiology of HyperthyroidismKitty YuffieÎncă nu există evaluări
- Unit 1 5ADocument7 paginiUnit 1 5AArvin O-CaféÎncă nu există evaluări
- Duodenal UlcerDocument4 paginiDuodenal UlcerLourenz BontiaÎncă nu există evaluări
- Patofisiologi, Manifestasi Klinik, Dan Manajemen PeritonitisDocument11 paginiPatofisiologi, Manifestasi Klinik, Dan Manajemen Peritonitistika tikaÎncă nu există evaluări
- Peritonitis: Update On Pathophysiology, Clinical Manifestations, and ManagementDocument11 paginiPeritonitis: Update On Pathophysiology, Clinical Manifestations, and ManagementerikafebriyanarÎncă nu există evaluări
- PeritonitisDocument5 paginiPeritonitisdnllkzaÎncă nu există evaluări
- Peritonitis: Update On Pathophysiology, Clinical Manifestations, and ManagementDocument11 paginiPeritonitis: Update On Pathophysiology, Clinical Manifestations, and ManagementMuhamad Chairul SyahÎncă nu există evaluări
- PeritonitissDocument46 paginiPeritonitissNinaÎncă nu există evaluări
- Intra-Abdominal and Pelvic EmergenciesDocument21 paginiIntra-Abdominal and Pelvic Emergenciesqhrn48psvwÎncă nu există evaluări
- Notes by Dr. Khurram PDFDocument22 paginiNotes by Dr. Khurram PDFAdnan AsgharÎncă nu există evaluări
- Cardiogenic SyokDocument51 paginiCardiogenic SyokRamadhyanÎncă nu există evaluări
- Writers Cramp - A Major Conundrum: Review Article44Document7 paginiWriters Cramp - A Major Conundrum: Review Article44IJAR JOURNALÎncă nu există evaluări
- Blood Bank PDFDocument178 paginiBlood Bank PDFamit ingaleÎncă nu există evaluări
- Neck Pain ManagementDocument35 paginiNeck Pain ManagementNur Elisaa100% (1)
- CH 084 Oral ThrushDocument7 paginiCH 084 Oral ThrushSavir GuptaÎncă nu există evaluări
- Capgras' Delusion: A Systematic Review of 255 Published CasesDocument13 paginiCapgras' Delusion: A Systematic Review of 255 Published CasesKaren RosasÎncă nu există evaluări
- Specimen Rejection Criteria - The Doctors LaboratoryDocument2 paginiSpecimen Rejection Criteria - The Doctors LaboratoryRevathyÎncă nu există evaluări
- CPG DyslipidemiaDocument26 paginiCPG DyslipidemiaRenzy SalumbreÎncă nu există evaluări
- UCDocument6 paginiUCapiv2010_808955526Încă nu există evaluări
- Toc PDFDocument24 paginiToc PDFFacebook HackerÎncă nu există evaluări
- Health Status of Sanitary Workers of Municipal Corporation of Aurangabad CityDocument7 paginiHealth Status of Sanitary Workers of Municipal Corporation of Aurangabad CityIheti SamÎncă nu există evaluări
- Healing-Chakras (GLB)Document21 paginiHealing-Chakras (GLB)GetaLuciaÎncă nu există evaluări
- Knowledge, Attitude and Practice Toward Cervical Cancer and Cervical Cancer Screening and Its Associated Factors Among Women in The City of Bamenda, CameroonDocument17 paginiKnowledge, Attitude and Practice Toward Cervical Cancer and Cervical Cancer Screening and Its Associated Factors Among Women in The City of Bamenda, CameroonEditor IJTSRDÎncă nu există evaluări
- Hand Washing Lesson PlanDocument9 paginiHand Washing Lesson PlanLisa GurreaÎncă nu există evaluări
- A Psychosomatic Perspective On Endometriosis - A MDocument18 paginiA Psychosomatic Perspective On Endometriosis - A MsilsilviasilÎncă nu există evaluări
- 3 ACC Prevention Blood PressureDocument69 pagini3 ACC Prevention Blood PressureMelissa Delgado100% (1)
- Joshis External Stabilisation System Jess For Recurrent Ctev Due To Irregular Follow Up PDFDocument5 paginiJoshis External Stabilisation System Jess For Recurrent Ctev Due To Irregular Follow Up PDFshankarÎncă nu există evaluări
- Hospital Teams: Bahasa InggrisDocument6 paginiHospital Teams: Bahasa InggrisIlhamÎncă nu există evaluări
- Late Pregnancy Bleeding (LPB) : Antepartum Hemorrhage (Aph) Dr. A. MutungiDocument3 paginiLate Pregnancy Bleeding (LPB) : Antepartum Hemorrhage (Aph) Dr. A. Mutungikhadzx100% (2)
- Leech TherapyDocument30 paginiLeech TherapyMohamed ShiffaÎncă nu există evaluări
- What Are Early Indicators of Mesothelioma. Realizing The Early Signs ofDocument2 paginiWhat Are Early Indicators of Mesothelioma. Realizing The Early Signs ofthasyaÎncă nu există evaluări
- KSC WSSforKSCCQIDocument34 paginiKSC WSSforKSCCQILệnhHồXungÎncă nu există evaluări
- Dr. Tans Acupuncture 1 2 3Document23 paginiDr. Tans Acupuncture 1 2 3Diana Pires96% (47)
- 06 Clinical Pathology MCQs With Answers 1Document29 pagini06 Clinical Pathology MCQs With Answers 1Habib Ullah100% (1)
- Should Covid Vaccination Really Needs To Be Mandatory?Document2 paginiShould Covid Vaccination Really Needs To Be Mandatory?ElenizelÎncă nu există evaluări
- ParkinsonDocument24 paginiParkinsonSandy AgustianÎncă nu există evaluări
- Chapter 4 of 10 - Kelsey HillDocument3 paginiChapter 4 of 10 - Kelsey HillspiritualbeingÎncă nu există evaluări
- How To Diagnose LBP RevisiDocument65 paginiHow To Diagnose LBP RevisiDedy SavradinataÎncă nu există evaluări
- Result Analysis Date: November 22, 2017 Conclusion: V. Laboratories and Diagnostic ExamsDocument7 paginiResult Analysis Date: November 22, 2017 Conclusion: V. Laboratories and Diagnostic ExamsEllaine Joy Mesina PadizÎncă nu există evaluări
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)De la EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Evaluare: 3 din 5 stele3/5 (1)
- The Age of Magical Overthinking: Notes on Modern IrrationalityDe la EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityEvaluare: 4 din 5 stele4/5 (30)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsDe la EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsÎncă nu există evaluări
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionDe la EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionEvaluare: 4 din 5 stele4/5 (404)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisDe la EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisEvaluare: 4.5 din 5 stele4.5/5 (42)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDDe la EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDEvaluare: 5 din 5 stele5/5 (3)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeDe la EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeEvaluare: 2 din 5 stele2/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedDe la EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedEvaluare: 5 din 5 stele5/5 (81)
- The Marshmallow Test: Mastering Self-ControlDe la EverandThe Marshmallow Test: Mastering Self-ControlEvaluare: 4.5 din 5 stele4.5/5 (60)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsDe la EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsEvaluare: 5 din 5 stele5/5 (1)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsDe la EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsEvaluare: 4 din 5 stele4/5 (4)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaDe la EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaEvaluare: 4.5 din 5 stele4.5/5 (266)
- The Obesity Code: Unlocking the Secrets of Weight LossDe la EverandThe Obesity Code: Unlocking the Secrets of Weight LossEvaluare: 4 din 5 stele4/5 (6)
- Why We Die: The New Science of Aging and the Quest for ImmortalityDe la EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityEvaluare: 4 din 5 stele4/5 (5)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsDe la EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsEvaluare: 4.5 din 5 stele4.5/5 (170)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeDe la EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeEvaluare: 4.5 din 5 stele4.5/5 (253)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisDe la EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisEvaluare: 3.5 din 5 stele3.5/5 (2)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.De la EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Evaluare: 4.5 din 5 stele4.5/5 (110)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryDe la EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryEvaluare: 4 din 5 stele4/5 (46)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessDe la EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessEvaluare: 4.5 din 5 stele4.5/5 (328)
- Empath: The Survival Guide For Highly Sensitive People: Protect Yourself From Narcissists & Toxic Relationships. Discover How to Stop Absorbing Other People's PainDe la EverandEmpath: The Survival Guide For Highly Sensitive People: Protect Yourself From Narcissists & Toxic Relationships. Discover How to Stop Absorbing Other People's PainEvaluare: 4 din 5 stele4/5 (95)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesDe la EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesEvaluare: 4.5 din 5 stele4.5/5 (1412)