Documente Academic
Documente Profesional
Documente Cultură
Crid2014 741402
Încărcat de
karenafiafiTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Crid2014 741402
Încărcat de
karenafiafiDrepturi de autor:
Formate disponibile
Hindawi Publishing Corporation
Case Reports in Dentistry
Volume 2014, Article ID 741402, 4 pages
http://dx.doi.org/10.1155/2014/741402
Case Report
Nonsurgical Management of Nifedipine Induced
Gingival Overgrowth
George Sam1 and Staly Chakkalakkal Sebastian2
1
2
Department of Periodontics, Government Dental College, Kottayam, Kerala, India
Obstetrics and Gynaecology, Kerala Institute of Medical Sciences, Trivandrum, Kerala, India
Correspondence should be addressed to George Sam; 007georgy@gmail.com
Received 11 May 2014; Revised 8 July 2014; Accepted 16 July 2014; Published 3 August 2014
Academic Editor: Pablo I. Varela-Centelles
Copyright 2014 G. Sam and S. C. Sebastian. This is an open access article distributed under the Creative Commons Attribution
License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly
cited.
Drug-induced gingival overgrowth is frequently associated with three particular drugs: phenytoin, cyclosporin, and nifedipine.
As gingival enlargement develops, it affects the normal oral hygiene practice and may interfere with masticatory functions. The
awareness in the medical community about this possible side effect of nifedipine is less when compared to the effects of phenytoin
and cyclosporin. The frequency of gingival enlargement associated with chronic nifedipine therapy remains controversial. Within
the group of patients that develop this unwanted effect, there appears to be variability in the extent and severity of the gingival
changes. Although gingival inflammation is considered a primary requisite in their development, few cases with minimal or no
plaque induced gingival inflammation have also been reported. A case report of gingival overgrowth induced by nifedipine in a
patient with good oral hygiene and its nonsurgical management with drug substitution is discussed in this case report.
1. Introduction
Gingival enlargement is a well-known consequence of the
administration of some anticonvulsants, immunosuppressants, and calcium channel blockers and may create speech,
mastication, tooth eruption, and aesthetic problems.
Not all the patients using these agents are affected by
gingival overgrowth, and the extent and severity are variable
in such patients. Phenytoin-induced overgrowth may be
present in 50 to 100% of patients treated with such drug,
whereas cyclosporin and calcium channel blocker-induced
overgrowths seem to be less common, with a prevalence of
30% and 20%, respectively [13]. Although there are previous
reports of nifedipine induced gingival enlargement managed with nonsurgical therapy, there are no comprehensive
description of cases managed effectively with drug substitution. This may partly be explained due to the enlargement in
most cases having a predominant inflammatory component
that often requires only an improvement in plaque control.
In other cases, the present medical condition may prevent
the offending drug from being discontinued. In the present
case, the patient presented with minimal plaque and calculus
suggesting a minor role of inflammation in the overall
development of the enlargement. Since scaling and root
planning did not show improvement in the condition, drug
substitution was done with losartan potassium and the two
months followup showed significant reduction in gingival
enlargement.
2. Case Report
A 53-year-old male patient reported to the Department of
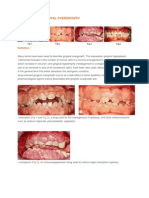
Periodontology, with a complaint of swollen gums. On examination, generalized gingival enlargement was noticed in the
lower arch, whereas an isolated nodular growth was observed
in the right side of upper arch. The enlarged gingiva was
firm, pale pink, and resilient with a minutely lobulated surface
and displayed no tendency to bleed (Figure 1). The teeth
displayed generalized cervical abrasion, probably attributed
to the vigorous tooth brushing habit of the patient. There were
little amounts of calculus present, and no deep periodontal
pockets were detected. The medical history of the patient
revealed that the patient was hypertensive and that he was
under medication for a period of 4 years for the same.
Case Reports in Dentistry
(a)
(b)
Figure 1: (a) Preoperative view. (b) Preoperative view.
He was consuming nifedipine 20 mg a day for the past 4
years. Based on the clinical presentation of the gingival
enlargement and a history of nifedipine intake, the case
was diagnosed as Nifedipine induced gingival overgrowth.
Periodontal management consisted of performing thorough
oral prophylaxis followed by careful instructions on oral
hygiene procedures. The case was reviewed for any signs of
improvement after a period of 2 weeks. Since there were no
changes noticed, a referral was made to the patients physician
to consider drug substitution with respect to nifedipine.
Nifedipine was substituted with losartan potassium 25 mg by
the physician and the patient was reevaluated after 2 months.
The bulk of the gingival enlargement had subsided in the
lower arch and the isolated nodular growth in the upper arch
had also reduced in size (Figure 2).
3. Discussion
The pathogenesis of drug-induced gingival overgrowths is
still not completely understood. It has been demonstrated
that gingival enlargement has a multifactorial nature and
is affected by factors such as age, demographic variables,
genetic predisposition, oral hygiene status, pharmacokinetic
variables, and molecular and cellular changes in gingival
tissues [4].
Despite their pharmacological diversity, the three major
drugs causing gingival overgrowth, namely, anticonvulsants,
calcium channel blockers, and immunosuppressants, have
similar mechanism of action at the cellular level, where they
inhibit intracellular calcium ion influx. The action of these
drugs on calcium and sodium ion flux may prove to be the key
in understanding why three dissimilar drugs have a common
side effect upon a secondary target tissue, such as gingival
connective tissue.
Calcium channel blockers are drugs developed for the
treatment of cardiovascular conditions such as hypertension, angina pectoris, coronary artery spasms, and cardiac
arrhythmias. Gingival enlargement associated with nifedipine was first reported in the early 1980s and was soon also
described with diltiazem and verapamil and in cases with
amlodipine and felodipine [46]. The possible hypothesis to
explain this overgrowth is that the fibroblasts contain strongly
sulfated mucopolysaccharides that are precursors of ground
substance. After an interaction between nifedipine and gingival fibroblasts, overproduction of collagen and extracellular
ground substance occurs and leads to an increase in the size of
the gingiva. The drug interferes with the calcium metabolism
of fibroblast cells and hence reduces the production of the
degrading enzyme collagenase [7].
Some investigators believe that inflammation is a prerequisite for development of the enlargement, which therefore
could be prevented by plaque removal and fastidious oral
hygiene [8, 9]. The severity of gingival enlargement in patients
taking medications correlates well with poor plaque control
and is commensurate with the degree of plaque induced
inflammation. This is supported by the fact that edentulous
areas did not show signs of enlargement in most reported
cases [10, 11]. A synergistic enhancement of collagenous
protein synthesis by human gingival fibroblasts was found
when these cells were simultaneously exposed to nifedipine
and interleukin-1 (IL-1), a proinflammatory cytokine that
is elevated in inflamed gingival tissues [4]. But in our
case there was little inflammation which is attributed to
minimal amounts of plaque and calculus and good oral
hygiene displayed by the patient. The enlargement had little
relationship with inflammation, and other factors might have
played a major role in their development.
It has also been proposed that susceptibility or resistance
to pharmacologically induced gingival overgrowth may be
governed by the existence of specific genetically predetermined subpopulations of fibroblasts in each individual which
exhibit a fibrogenic response to these medications [4]. It
has been suggested that there may be subpopulations of
fibroblasts which are sensitive to nifedipine and cause an
increase in the production of collagen [12].
Mast cells have been found to participate in many
inflammatory oral diseases, particularly those associated
with fibrosis. They possess very diverse roles ranging from
proinflammatory to immunomodulatory. Upon their activation, they promote the local renin angiotensin system
generation consequently able to stimulate endothelin and
other profibrotic mediators [13].
The presence of the enlargement makes plaque control
difficult, often resulting in a secondary inflammatory process
that complicates the gingival overgrowth caused by the drug.
The primary aim of nonsurgical approaches is to reduce
Case Reports in Dentistry
(a)
(b)
Figure 2: (a) Postoperative view (2 months after drug substitution). (b) Postoperative view (2 months after drug substitution).
the inflammatory component in the gingival tissues and
thereby avoid the need for surgery. Patients at risk from or
who have developed drug-induced gingival overgrowth will
benefit from effective oral hygiene measures, professional
tooth cleaning, scaling, and root surface instrumentation.
For some patients these measures alone could reduce the
gingival overgrowth to acceptable levels, and for others, it
could make surgical correction easier [1416]. However, in
our case there was no resolution in the size of the enlargement
following scaling and root planning because there was little
inflammation to begin with. Nevertheless, the importance
of strict plaque control in the management of drug-induced
enlargement should not be underestimated.
The dose of the drug also has an impact on gingival
oral growth. It is reported that nifedipine was found 15
316 times more in the gingival crevicular fluid compared
to plasma [17]. The higher concentration of nifedipine in
the gingival crevicular fluid could increase the severity of
gingival enlargement [10]. Consideration should be given
to the possibility of discontinuing the drug or of changing
medication. These possibilities should be consulted with the
patients physician. Simple discontinuation of the offending
agent is usually not a practical option but replacing it with
another medication might be. Reduction in the size of the
gingival overgrowth has been reported within a week of drug
withdrawal and may lead to full resolution [18]. If any drug
substitution is attempted, it is important to allow for 612
months to elapse between discontinuation of the offending
drug and the possible resolution of gingival enlargement
before a decision to implement surgical treatment is made
[19].
The number of prescriptions for calcium channel blockers
has been increasing in recent years. There is infinitesimal
awareness about this effect of drugs on gingival tissues in
medical community. There is a need for physicians and
dentists to make a coordinated treatment plan for the patients
indicated for these drug therapies. Our case showed that not
every case of drug-induced gingival enlargement requires
plaque induced gingival inflammation for their development.
In such cases drug substitution should be considered a valid
treatment option especially when the gingival enlargement is
present in spite of good oral hygiene.
Conflict of Interests
The authors declare that there is no conflict of interests
regarding the publication of this paper.
References
[1] R. A. Seymour, The pathogenesis of drug-induced gingival
overgrowth, Journal of Clinical Periodontology, vol. 23, no. 3,
part 1, pp. 165175, 1996.
[2] I. Cebeci, A. Kantarci, E. Firatli, S. Aygun, H. Tanyeri, and A.
E. Aydin, Evaluation of the frequency of HLA determinants in
patients with gingival overgrowth induced by cyclosporine-A,
Journal of Clinical Periodontology, vol. 23, no. 8, pp. 737742,
1996.
[3] S. Barclay, J. M. Thomason, J. R. Idle, and R. A. Seymour,
The incidence and severity of nifedipine-induced gingival
overgrowth, Journal of Clinical Periodontology, vol. 19, no. 5, pp.
311314, 1992.
[4] A. Dongari-Bagtzoglou, Drug-associated gingival enlargement, Journal of Periodontology, vol. 75, no. 10, pp. 14241431,
2004.
[5] Y. Ramon, S. Behar, Y. Kishon, and I. S. Engelberg, Gingival
hyperplasia caused by nifedipinea preliminary report, International Journal of Cardiology, vol. 5, no. 2, pp. 195206, 1984.
[6] R. I. Marshall and P. M. Bartold, A clinical review of druginduced gingival overgrowths, Australian Dental Journal, vol.
44, no. 4, pp. 219232, 1999.
[7] M. Mishra, Z. Khan, and S. Mishra, Gingival overgrowth and
drug association: a review, Indian Journal of Medical Sciences,
vol. 65, no. 2, pp. 7382, 2011.
[8] L. A. Klar, Gingival hyperplasia during dilantin-therapy; a
survey of 312 patients, Journal of Public Health Dentistry, vol.
33, no. 3, pp. 180185, 1973.
[9] J. Slavin and J. Taylor, Cyclosporin, nifedipine, and gingival
hyperplasia, The Lancet, vol. 2, article 739, no. 8561, 1987.
[10] P. M. Sunil, J. S. Nalluswami, S. J. Sanghar, and I. Joseph,
Nifedipine-induced gingival enlargement: correlation with
dose and oral hygiene, Journal of Pharmacy and Bioallied
Sciences, vol. 4, no. 6, pp. 191193, 2012.
[11] V. Margiotta, I. Pizzo, G. Pizzo, and A. Barbaro, Cyclosporinand nifedipine-induced gingival overgrowth in renal transplant
patients: correlations with periodontal and pharmacological
[12]
[13]
[14]
[15]
[16]
[17]
[18]
[19]
Case Reports in Dentistry
parameters, and HLA-antigens, Journal of Oral Pathology &
Medicine, vol. 25, no. 3, pp. 128134, 1996.
S. Barak, I. S. Engelberg, and J. Hiss, Gingival hyperplasia
caused by nifedipine. Histopathologic findings, Journal of
Periodontology, vol. 58, no. 9, pp. 639642, 1987.
T. Subramani, V. Rathnavelu, S. K. Yeap, and N. B. Alitheen,
Influence of mast cells in drug-induced gingival overgrowth,
Mediators of Inflammation, vol. 2013, Article ID 275172, 8 pages,
2013.
M. Mavrogiannis, J. S. Ellis, J. M. Thomason, and R. A. Seymour,
The management of drug-induced gingival overgrowth, Journal of Clinical Periodontology, vol. 33, no. 6, pp. 434439, 2006.
R. P. Dhale and M. B. Phadnaik, Conservative management of
amlodipine influenced gingival enlargement, Journal of Indian
Society of Periodontology, vol. 13, no. 1, pp. 4143, 2009.
A. K. Srivastava, D. Kundu, P. Bandyopadhyay, and A. K. Pal,
Management of amlodipine-induced gingival enlargement:
series of three cases, Journal of Indian Society of Periodontology,
vol. 14, no. 4, pp. 279281, 2010.
T. D. Rees and R. A. Levine, Systematic drugs as a risk factor for
periodontal disease initiation and progression, Compendium,
vol. 16, no. 1, pp. 2042, 1995.
P. G. Raman, V. N. Mishra, and D. Singh, Nifedipine induced
gingival hyperplasia, The Journal of the Association of Physicians
of India, vol. 36, no. 3, pp. 231233, 1988.
P. M. Camargo, P. R. Melnick, F. Q. M. Pirih, R. Lagos, and
H. H. Takei, Treatment of drug-induced gingival enlargement:
aesthetic and functional considerations, Periodontology 2000,
vol. 27, no. 1, pp. 131138, 2001.
S-ar putea să vă placă și
- Cholesterol Does Not Cause Heart Disease PDFDocument20 paginiCholesterol Does Not Cause Heart Disease PDFRani Oktaviani Sidauruk100% (2)
- Cholesterol GuideDocument26 paginiCholesterol GuideRavi DesaiÎncă nu există evaluări
- Journal of Clinical Dentistry Pro-Argin Special Issue 2009Document36 paginiJournal of Clinical Dentistry Pro-Argin Special Issue 2009IntelligentiaÎncă nu există evaluări
- General Pathology NotesDocument29 paginiGeneral Pathology NotesMohd Syaiful Mohd ArisÎncă nu există evaluări
- Intermittent ExotropiaDocument15 paginiIntermittent ExotropiakarenafiafiÎncă nu există evaluări
- 1.1 Systemic and Clinical Treatment of Gingival HyperplasiaDocument3 pagini1.1 Systemic and Clinical Treatment of Gingival HyperplasiaRaluca ElenaÎncă nu există evaluări
- Pharm Cvs McqsDocument30 paginiPharm Cvs McqsSoodn Kang Soodn100% (3)
- Ischemic Heart DiseaseDocument8 paginiIschemic Heart DiseaseNina Natalia Bautista100% (1)
- Risk Factors For Periodontal Diseases 2022Document13 paginiRisk Factors For Periodontal Diseases 2022SnowÎncă nu există evaluări
- Peripheral Vascular InterventionsDocument1.225 paginiPeripheral Vascular InterventionsAvinash6614Încă nu există evaluări
- The Effect of Injectable Platelet-Rich Fibrin Use in TheDocument6 paginiThe Effect of Injectable Platelet-Rich Fibrin Use in TheNurul Fajriah YunitaÎncă nu există evaluări
- Rotablation TipsDocument60 paginiRotablation TipsSabyasachi MukhopadhyayÎncă nu există evaluări
- NURSING CARE PLAN For Myocardial InfarctionDocument16 paginiNURSING CARE PLAN For Myocardial InfarctionFreisanChenMandumotan100% (1)
- Understanding Periodontitis: A Comprehensive Guide to Periodontal Disease for Dentists, Dental Hygienists and Dental PatientsDe la EverandUnderstanding Periodontitis: A Comprehensive Guide to Periodontal Disease for Dentists, Dental Hygienists and Dental PatientsÎncă nu există evaluări
- Conservative Management of Nifedipine Influenced Gingival Enlargement - A Case ReportDocument9 paginiConservative Management of Nifedipine Influenced Gingival Enlargement - A Case ReportAgathaPutriÎncă nu există evaluări
- Drug Induced Gingival OvergrowthDocument4 paginiDrug Induced Gingival OvergrowthAdit VekariaÎncă nu există evaluări
- Fibrous Hyperplasia A Case ReportDocument4 paginiFibrous Hyperplasia A Case ReportBramita Beta ArnandaÎncă nu există evaluări
- Conservative Management of Amlodipine Induced Gingival Enlargement: A ClinicalDocument3 paginiConservative Management of Amlodipine Induced Gingival Enlargement: A ClinicalachmadsyobriÎncă nu există evaluări
- Case Report Necrotizing Ulcerative Gingivitis, A Rare Manifestation As A Sequel of Drug-Induced Gingival Overgrowth: A Case ReportDocument7 paginiCase Report Necrotizing Ulcerative Gingivitis, A Rare Manifestation As A Sequel of Drug-Induced Gingival Overgrowth: A Case ReportPutri Dwi AnggrainiÎncă nu există evaluări
- Amlodipine-Induced Gingival Overgrowth: Case ReportDocument4 paginiAmlodipine-Induced Gingival Overgrowth: Case ReportjulietÎncă nu există evaluări
- Gingival HyperplasiaDocument12 paginiGingival HyperplasiaMaliha TahirÎncă nu există evaluări
- 19 FullDocument5 pagini19 FullBramita Beta ArnandaÎncă nu există evaluări
- 2.2 Valproate-Induced Gingival Overgrowth - A Case ReportDocument5 pagini2.2 Valproate-Induced Gingival Overgrowth - A Case ReportRaluca ElenaÎncă nu există evaluări
- Interdisciplnary Approach in The Management of Medically Compromised Patient With Drug Induced Gingival EnlargemnetDocument4 paginiInterdisciplnary Approach in The Management of Medically Compromised Patient With Drug Induced Gingival EnlargemnetPriska AngeliaÎncă nu există evaluări
- Gingival EnlargementDocument6 paginiGingival EnlargementLutfiah HafizahÎncă nu există evaluări
- Artículo de Periodoncia 2Document7 paginiArtículo de Periodoncia 2Margareth Roxanna Mendieta GirónÎncă nu există evaluări
- Gingival EnlargementDocument56 paginiGingival Enlargementaichayehdih booksÎncă nu există evaluări
- Recurrent Localized Chronic Gingival Enlargement in Fixed Orthodontic Treatment-A Novel Case ReportDocument3 paginiRecurrent Localized Chronic Gingival Enlargement in Fixed Orthodontic Treatment-A Novel Case ReportBramita Beta ArnandaÎncă nu există evaluări
- Eksperimental 2021Document8 paginiEksperimental 2021Putri NurhadizahÎncă nu există evaluări
- Chronic Inflammatory Gingival Enlargement: A CaseDocument3 paginiChronic Inflammatory Gingival Enlargement: A CaseArida Khoiruza Asy'ariÎncă nu există evaluări
- Case Report Periodontal Management of Cyclosporin A-Induced Gingival Overgrowth: A Nonsurgical ApproachDocument9 paginiCase Report Periodontal Management of Cyclosporin A-Induced Gingival Overgrowth: A Nonsurgical ApproachdellaÎncă nu există evaluări
- Lit Review-PharmDocument5 paginiLit Review-Pharmapi-669282924Încă nu există evaluări
- Case Report: Untypical Amlodipine-Induced Gingival HyperplasiaDocument4 paginiCase Report: Untypical Amlodipine-Induced Gingival HyperplasiakarenafiafiÎncă nu există evaluări
- InflammatoryGingivalEnlargement ACaseReport PDFDocument5 paginiInflammatoryGingivalEnlargement ACaseReport PDFMardianiPutriPutriÎncă nu există evaluări
- Ijpi 3 2 75 79Document5 paginiIjpi 3 2 75 79Rabiatul AdawiyahÎncă nu există evaluări
- Gingival Enlargement 2Document39 paginiGingival Enlargement 2Aicha Sid AhmedÎncă nu există evaluări
- Effectiveness of Non-Surgical Periodontal Therapy On Amlodipine Induced Gingival Enlargement: A Case ReportDocument3 paginiEffectiveness of Non-Surgical Periodontal Therapy On Amlodipine Induced Gingival Enlargement: A Case ReportAliyah SaraswatiÎncă nu există evaluări
- 1752 1947 3 98Document4 pagini1752 1947 3 98Rini RiantiÎncă nu există evaluări
- JOHCD PregnancyAssociatedGingivalEnlargementDocument5 paginiJOHCD PregnancyAssociatedGingivalEnlargementAZWAN RAHMADHAN PUTRAÎncă nu există evaluări
- Systemic Medication-It's Effects On Oral HealthDocument6 paginiSystemic Medication-It's Effects On Oral Healthkevin1678Încă nu există evaluări
- Gingival Overgrowth and Altered Passive Eruption in Adolescents Literature Review and Case ReportDocument8 paginiGingival Overgrowth and Altered Passive Eruption in Adolescents Literature Review and Case ReportAulia ElnisaÎncă nu există evaluări
- Gingivitis - WikipediaDocument35 paginiGingivitis - Wikipediamuhamad Fadilah hardiansyahÎncă nu există evaluări
- Perio Research PaperDocument10 paginiPerio Research Paperapi-738832489Încă nu există evaluări
- Effect of Morinda Citrifolia L. Fruit Juice On Gingivitis/periodontitisDocument7 paginiEffect of Morinda Citrifolia L. Fruit Juice On Gingivitis/periodontitisMuhamad Vicki SyahrialÎncă nu există evaluări
- Calcium Channel Blocker-Induced Gingival EnlargementDocument5 paginiCalcium Channel Blocker-Induced Gingival EnlargementMichelleLeeÎncă nu există evaluări
- Research Article: Morphological Changes of Gingiva in Streptozotocin Diabetic RatsDocument5 paginiResearch Article: Morphological Changes of Gingiva in Streptozotocin Diabetic RatsAdrian BoerÎncă nu există evaluări
- Maintainence Phase of Periodontal CareDocument4 paginiMaintainence Phase of Periodontal CareDeen MohdÎncă nu există evaluări
- Open Drainage or NotDocument6 paginiOpen Drainage or Notjesuscomingsoon2005_Încă nu există evaluări
- Articulo Aumento Gingival Por MedicamentosDocument6 paginiArticulo Aumento Gingival Por MedicamentosNatalia Celis MejiaÎncă nu există evaluări
- Periodontal Maintenance - A ReviewDocument7 paginiPeriodontal Maintenance - A ReviewVanessa MordiÎncă nu există evaluări
- Perio PaperDocument7 paginiPerio Paperapi-663488649Încă nu există evaluări
- Effectiveness of An Essential Oil Mouthrinse in Improving Oral Health in Orthodontic PatientsDocument5 paginiEffectiveness of An Essential Oil Mouthrinse in Improving Oral Health in Orthodontic PatientsHamza GaaloulÎncă nu există evaluări
- Pastagia2006 PDFDocument8 paginiPastagia2006 PDFRENATO SUDATIÎncă nu există evaluări
- Oral Findings in Chronic Kidney Disease: Implications For Management in Developing CountriesDocument8 paginiOral Findings in Chronic Kidney Disease: Implications For Management in Developing CountriesEstherÎncă nu există evaluări
- Drug Induced Gingival Overgrowth: Corresponding AuthorDocument5 paginiDrug Induced Gingival Overgrowth: Corresponding Authorjorge villamizarÎncă nu există evaluări
- Oral Health in Children With Leukemia: Review ArticleDocument8 paginiOral Health in Children With Leukemia: Review ArticleNindy TweelingenÎncă nu există evaluări
- Periodontal Disease and Control of Diabetes Mellitus: Clinical PracticeDocument6 paginiPeriodontal Disease and Control of Diabetes Mellitus: Clinical PracticeOsama HandrÎncă nu există evaluări
- Jurnal Porio 1Document3 paginiJurnal Porio 1Neo YustindraÎncă nu există evaluări
- Treatment of Plaque-Induced Gingivitis, Chronic Periodontitis, and Other Clinical ConditionsDocument10 paginiTreatment of Plaque-Induced Gingivitis, Chronic Periodontitis, and Other Clinical ConditionsLeony RicciÎncă nu există evaluări
- Case Report: Idiopathic Gingival Hyperplasia: A Case Report With A 17-Year FollowupDocument6 paginiCase Report: Idiopathic Gingival Hyperplasia: A Case Report With A 17-Year Followupade ismailÎncă nu există evaluări
- Risk Factors in Bone Augmentation Procedures: Peter K. Moy - Tara AghalooDocument15 paginiRisk Factors in Bone Augmentation Procedures: Peter K. Moy - Tara Aghalooxiaoxin zhangÎncă nu există evaluări
- Maxillary Ulceration Resulting From Using A Rapid Maxillary Expander in A Diabetic PatientDocument5 paginiMaxillary Ulceration Resulting From Using A Rapid Maxillary Expander in A Diabetic PatientPrabowo BomazdicahyoÎncă nu există evaluări
- Nonsurgical Periodontal TherapyDocument2 paginiNonsurgical Periodontal TherapyMohammed NabeelÎncă nu există evaluări
- Oral and Maxillofacial Surgery Cases: Janina Golob Deeb, Denver J. Lyons, Daniel M. Laskin, George R. DeebDocument6 paginiOral and Maxillofacial Surgery Cases: Janina Golob Deeb, Denver J. Lyons, Daniel M. Laskin, George R. DeebAgum Nila Sari IIÎncă nu există evaluări
- SummaryDocument5 paginiSummarygabrielkhmÎncă nu există evaluări
- Perio PBLKasvuGingivalOvergrowthDocument32 paginiPerio PBLKasvuGingivalOvergrowthDraspiÎncă nu există evaluări
- The Effect of Listerine Mouthwash On Dental Plaque Gingival Inflammation and C Reactive Protein CRP 2161 1122.1000191Document5 paginiThe Effect of Listerine Mouthwash On Dental Plaque Gingival Inflammation and C Reactive Protein CRP 2161 1122.1000191Bagus RahmawanÎncă nu există evaluări
- Management of Deep Carious LesionsDe la EverandManagement of Deep Carious LesionsFalk SchwendickeÎncă nu există evaluări
- Presentation 05-06-15 EnglishDocument20 paginiPresentation 05-06-15 EnglishkarenafiafiÎncă nu există evaluări
- Name: Ronal Afan Home Address Office Address ID Card PositionDocument1 paginăName: Ronal Afan Home Address Office Address ID Card PositionkarenafiafiÎncă nu există evaluări
- Results of Surgery For Congenital Esotropia: Original ResearchDocument6 paginiResults of Surgery For Congenital Esotropia: Original ResearchkarenafiafiÎncă nu există evaluări
- 129 Accommodative EsotropiaDocument6 pagini129 Accommodative EsotropiakarenafiafiÎncă nu există evaluări
- Infantile Esotropia Diagnosis and ManagementDocument10 paginiInfantile Esotropia Diagnosis and ManagementkarenafiafiÎncă nu există evaluări
- S64 FullDocument3 paginiS64 FullkarenafiafiÎncă nu există evaluări
- Calcium Channel Blocker Use and Mortality Among Patients With End-Stage Renal DiseaseDocument8 paginiCalcium Channel Blocker Use and Mortality Among Patients With End-Stage Renal DiseasekarenafiafiÎncă nu există evaluări
- Case Report: Untypical Amlodipine-Induced Gingival HyperplasiaDocument4 paginiCase Report: Untypical Amlodipine-Induced Gingival HyperplasiakarenafiafiÎncă nu există evaluări
- Afhs1204 0576Document3 paginiAfhs1204 0576karenafiafiÎncă nu există evaluări
- Oral Test PracticeDocument12 paginiOral Test PracticekarenafiafiÎncă nu există evaluări
- Non-Hodgkin Lymphoma Affecting The Tongue: Unusual Intra-Oral LocationDocument5 paginiNon-Hodgkin Lymphoma Affecting The Tongue: Unusual Intra-Oral LocationkarenafiafiÎncă nu există evaluări
- Update On Otitis MediaDocument28 paginiUpdate On Otitis MediakarenafiafiÎncă nu există evaluări
- Defense Against Infectious Disease: Skin As A Barrier To InfectionDocument8 paginiDefense Against Infectious Disease: Skin As A Barrier To InfectionFranchesca Rosabel BudimanÎncă nu există evaluări
- Practice Paper 1: AnswersDocument9 paginiPractice Paper 1: AnswersOHÎncă nu există evaluări
- Ischemic Heart DiseaseDocument4 paginiIschemic Heart DiseaseBanana CakeÎncă nu există evaluări
- Good Thesis Statement For Heart DiseaseDocument5 paginiGood Thesis Statement For Heart Diseasemarilynmarieboston100% (2)
- Upper Limb Post Stroke Rehabilitation Performance Monitoring Tools Using Optical MouseDocument12 paginiUpper Limb Post Stroke Rehabilitation Performance Monitoring Tools Using Optical MouseAbdul Shokor Abd TalibÎncă nu există evaluări
- Thesis On Coronary Heart DiseaseDocument7 paginiThesis On Coronary Heart Diseasetracyclarkwarren100% (1)
- Insight To The Pathophysiology of Stable Angina PectorisDocument8 paginiInsight To The Pathophysiology of Stable Angina PectorisZaid AlSaadyÎncă nu există evaluări
- Heart Attacks and There Effects On LifeDocument11 paginiHeart Attacks and There Effects On Lifeapi-291565665Încă nu există evaluări
- Imagem PlacaDocument23 paginiImagem PlacaMatheus Nucci RiccettoÎncă nu există evaluări
- Cardiovascular SyllabusDocument13 paginiCardiovascular SyllabusBrandonGilbertÎncă nu există evaluări
- Gender Differences in Coronary Heart Disease 06 February 2016Document16 paginiGender Differences in Coronary Heart Disease 06 February 2016Mohamad ZulmiÎncă nu există evaluări
- Vessel Wall 1Document12 paginiVessel Wall 1Matheus Nucci RiccettoÎncă nu există evaluări
- Coronary Artery Bypass Surgery: UnderstandingDocument24 paginiCoronary Artery Bypass Surgery: UnderstandingNurArsitaPebruatiÎncă nu există evaluări
- Case Studies: Duplex Evaluation of The Postoperative CarotidDocument7 paginiCase Studies: Duplex Evaluation of The Postoperative CarotidJoseph GlaserÎncă nu există evaluări
- كتاب التمريض الجديد2022Document206 paginiكتاب التمريض الجديد2022mohamed mohamedÎncă nu există evaluări
- Health and Wellness 2 - Mpu3313 - V2Document19 paginiHealth and Wellness 2 - Mpu3313 - V2SHANU NAIR A/P SASEEDHAARAN student100% (1)
- Jurding DR SaugiDocument44 paginiJurding DR SaugiDian FitriÎncă nu există evaluări
- Astaxanthin 2.5HNDocument32 paginiAstaxanthin 2.5HNRaziel Alvarez RebolloÎncă nu există evaluări
- Luminair PDFDocument229 paginiLuminair PDFMohammed Shahin40% (5)
- Treating Cardiac Diseas 2Document20 paginiTreating Cardiac Diseas 2Muhammed Luthufi EÎncă nu există evaluări
- Esc Cardiomed (3 Edn) : Epidemiology and Risk FactorsDocument12 paginiEsc Cardiomed (3 Edn) : Epidemiology and Risk FactorsNadhila IchwanÎncă nu există evaluări
- (Rath & Pauling) - Heart Disease Part Two by Jeffrey Dach MDDocument22 pagini(Rath & Pauling) - Heart Disease Part Two by Jeffrey Dach MDpedpixÎncă nu există evaluări