Documente Academic
Documente Profesional
Documente Cultură
WHC
Încărcat de
Ahmed MagdyTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
WHC
Încărcat de
Ahmed MagdyDrepturi de autor:
Formate disponibile
Womens Health Care
Maternal Serum Screening:
What Do The
Results Mean?
MSS can be a valuable screening test for fetal neural tube defects
or chromosomal anomalies. As part of this, physicians should
counsel their patients about the potential for false-positive or
false-negative results.
By Bernard N. Chodirker, MD
lthough this article is being written in
The Canadian Journal of Diagnosis,
it must be emphasized that maternal serum
screening (MSS) in not a diagnostic test. It
is a screening test. The purpose of a screening test is not to determine if a person has a
particular condition, but rather to identify
individuals who are at high risk for developing that condition.
In the case of MSS, the test is designed to
identify women at increased risk for carrying a fetus with a neural tube defect, including spina bifida and anencephaly, or a chromosomal anomaly (i.e., Down syndrome or
Trisomy 18). Although other maternal or
fetal conditions may cause abnormal maternal serum screen results, these former conditions are the primary focus of MSS.
Maternal serum alpha-fetoprotein
(MSAFP) testing began in the 1970s as a
means of screening for fetal neural tube
defects. MSAFP is a protein of fetal origin
that rises in the maternal serum with
advancing gestation from 13 weeks to 32
weeks. MSAFP levels are first determined
in biochemical units (e.g., g/L). These are
converted to multiples of the median
(MOMs) by dividing this value by the
The Canadian Journal of Diagnosis / July 2001
57
Maternal Serum Screening
Unaffected
Spina Bifida
0.7
2.3
Anencephaly
5.0
MSAFP levels in MOMs
Figure 1. Distribution of MSAFP levels with fetal neural tube defects.
median for the gestational age at which
the test was done.
A positive screen test for neural tube
defects occurs when the MSAFP is greater
than a certain cut-off value. Most programs use cut-offs between 2.0 and 2.5
Dr. Chodirker is medical
geneticist and associate
professor, department of
pediatrics and child health,
biochemistry and human
genetics, University of
Manitoba, and clinical
director, Manitoba Maternal
Serum Screening Program,
Winnipeg, Manitoba.
58
MOMs. This cut-off is chosen as a compromise to get the best detection rate relative to the false-positive rate. As Figure 1
demonstrates, if the only concern was a
high detection rate, then a cut-off value of
0.7 MOMs could be used. Although
almost all cases of fetal spina bifida and
anencephaly would be detected, over 50%
of pregnant women would have a positive
test. Conversely, if the major concern was
the false-positive rate, a cut-off of 5.O
MOMs could be used. There would be
very few false-positives, but the detection
rate would be very poor. With a cut-off
between 2.0 and 2.5 MOMs, a detection
rate of 80% for spina bifida and 90% for
anencephaly is expected, with a false-positive rate of 2.5% to 4%.1
The Canadian Journal of Diagnosis / July 2001
Maternal Serum Screening
In 1984, one study showed that MSAFP
levels in mothers whose babies had Down
syndrome were lower than the levels of
those in control groups.2 This led to the use
of MSAFP (combined with maternal age)
as a screening test for fetal Down syndrome. Since it was known that advanced
maternal age was a major risk factor for
having a child with Down syndrome, the
original screening test for fetal Down syndrome was to simply ask a woman how old
she would be on her due date. If the answer
was 35 years or greater, she was considered
screen-positive. Using this approach, about
5% of women would be screen-positive
(i.e., a 5% false-positive rate) and 20% of
babies with Down syndrome would be born
to women who were screen-positive (i.e., a
20% detection rate).3 Combining a risk
based on the MSAFP level with maternal
age improved the screening performance to
a 35% detection rate, with a similar falsepositive rate.3
The most common form of MSS is triple
testing, which is based on MSAFP, human
chorionic gonadotropin (HCG) and estriol
(E3). HCG is a placental hormone, the levels of which drop between 10 and 20 weeks
gestation. E3 is made by the placenta from
precursors from the fetal adrenal and liver.
The levels of E3 continue to rise after nine
weeks gestation.
Since MSAFP levels are lower in mothers carrying fetuses with Down syndrome, a
low MSAFP level will statistically increase
a womans risk of having a baby with Down
syndrome. The chance of this happening is
calculated by comparing the heights of the
Down syndrome curve to the unaffected
curve for a given MOM. A MSAFP level of
about O.5 MOMs will double the chance of
fetal Down syndrome (likelihood ratio =
2.0) while a level of about 1.4 MOMs will
decrease the risk by one-half (Figure 2).
Maternal HCG levels tend to be higher
and maternal E3 levels tend to be lower in
mothers of Down syndrome fetuses.
Likelihood
ratios,
therefore, are calcuThe most
lated for HCG and E3
in a similar fashion to common form of
MSAFP. The risk for
MSS is triple
fetal Down syndrome
testing, which is
then is calculated by
multiplying
the based on MSAFP,
womans risk, based
on her age, by the human chorionic
three
likelihood
gonadotropin
ratios. A computer
and estriol.
program is required
for proper interpretation. With triple testing, the detection rate
for fetal Down syndrome is about 60%,
with a false-positive rate of 5%.4 Other
first- and second-trimester markers, including biochemical and ultrasound parameters,
have been added by various groups to standard triple testing. This has resulted in even
better screening performance.5
Fetal trisomy 18 is associated with low
levels of all three biochemical parameters,
and a similar calculation is made to determine the fetal trisomy 18 risk.
The first step in MSS is to counsel the
woman patient. This test should be considered strictly voluntary. She should be
informed that the test is associated with significant false-positive and false-negative
The Canadian Journal of Diagnosis / July 2001
59
Maternal Serum Screening
LR 1.0
LR 0.5
LR 2.0
Down
syndrome
Unaffected
0.5
0.8
1.4
MSAFP levels in MOMs
Figure 2. Distribution of MSAFP levels with fetal Down syndrome.
rates. She should be made aware that an
abnormal test result does not mean that the
fetus is affected, while a normal test result
does not guarantee an
unaffected fetus.
Small errors in
Currently, the policy
assignment of
in Canada is that all
women who will be
gestational age
over 35 years of age on
can cause major their due date should
be offered an invasive
errors in risk
test for fetal chromosodetermination.
mal abnormalities (i.e.,
an amniocentesis or
chorionic villus sampling). This policy
may change in the future. If a woman
chooses to have MSS, care must be taken
to send the sample at the appropriate gesta-
62
tion point. Some programs will require
ultrasound dating before a sample is tested. Most Canadian centers prefer ultrasound-derived dates, but will use gestation calculations based on the patients
last period, provided these dates are reliable. The ideal time to send the blood
sample is between 15 and 18 weeks. The
author would not recommend sending a
sample at exactly 15 weeks, as the computer used by the MSS program may
determine the gestation to be 14.9 weeks,
and recommend repeat samples. Samples
could be drawn laterat up to 22
weeksbut this can cause unnecessary
delays.
It is important that requisitions for
MSS be filled in as completely and accu-
The Canadian Journal of Diagnosis / July 2001
Maternal Serum Screening
rately as possible. Small errors in assignment of gestational age can cause major
errors in risk determination. The interpretation also should take into consideration
the maternal age, maternal weight, diabetic status and the patients ethnic origin, all
of which can influence the interpretation.
A series of six case presentations are
provided here to illustrate the possible
outcomes after MSS. The reader is invited
to try and predict the outcome before
reading the actual outcome. All risks quoted are term risks, i.e., the chance of having a live child born with a specific condition.
Comment
This case illustrates the importance of an
accurate determination of gestation. Since
AFP and E3 levels rise and HCG levels
fall with advancing gestation, overestimation of the gestational age will show an
MSS pattern identical to that expected
with fetal Down syndrome. Conversely,
the underestimation of dates will result in
elevated MSAFP levels. Inaccurate estimation of the gestation is one of the
Elevated MSAFP
most common explalevels can be a
nations for false-positive test results.
sign of placental
Case 1
Case 2
A 26-year-old gravida 2 (G2) para 1 (P1)
woman has an MSS drawn at 16.2 weeks
gestation. The MSAFP is 0.5 MOMs, the
HCG is 2.0 MOMs and the E3 is 0.4
MOMs. The gestational age is based on
her last menstrual period (LMP). The risk
for fetal Down syndrome went from an
age-related risk of 1/1,300 to 1/80.
A
24-year-old
woman has an MSS
drawn at 15.5 weeks,
according to her
LMP. Her periods
have been regular,
occurring every 28 days, and the last period was normal. Her MSAFP level was 2.5
MOMs, the HCG was 1.2 MOMs and the
E3 level was 0.9 MOMs. The Down syndrome risk was 1/14,000. The MSS was
done as part of her routine pregnancy
blood work without any explanation or
consent. She is extremely anxious, as she
believes her baby has spina bifida.
Outcome
Further review determined that she has
had only one period since her last pregnancy due to breast feeding. An ultrasound examination showed that she was
only 12.5 weeks pregnant when the blood
was drawn. The original blood test was,
therefore, drawn too early. A repeat blood
sample was drawn at 15.5 weeks by ultrasound dates, and was screen-negative. No
amniocentesis was done and the mother
gave birth to a healthy baby.
compromise, and
may indicate
later problems,
such as maternal
hypertension.
Outcome
The woman was told that, although an elevated MSAFP level is a risk factor for various problems, including fetal spina bifida, this MSAFP level is associated most
The Canadian Journal of Diagnosis / July 2001
63
Maternal Serum Screening
all these conditions, most
women with elevated MSAFP
levelsespecially those with
minimal elevationsgo on to
have normal pregnancies and
healthy babies.
Case 3
An 18-year-old woman from
Northern Manitoba had an
MSAFP drawn at 16 weeks by
sure dates. The MSAFP levels
was 7.8 MOM, the HCG was
1.1 MOM and the E3 was 0.1
MOM.
often with a normal outcome. A fetal
assessment showed no abnormality and
confirmed the gestational age. She was
seen again at 31 weeks gestation and the
assessment was again normal. Her baby
was born healthy.
Comment
This case illustrates the worst aspects of
MSS. The patient was not properly counseled in advance of testing or about the
meaning of a positive result. Only about
one in 50 women with an elevated
MSAFP level will have a baby with spina
bifida.6 Elevated MSAFP can be seen with
other fetal anomalies, including ventral
wall defects. Elevated MSAFP levels also
can be a sign of placental compromise,
and can be indicators of later problems,
such as maternal hypertension, intrauterine growth retardation, oligohydramnious
and subsequent fetal demise. Although an
elevated MSAFP level is a risk factor for
64
Outcome
Extremely high MSAFP levels in association with very low E3 levels strongly suggest fetal anencephaly. The E3 levels are
low because the fetal adrenals are underdeveloped. The primary-care physician
was notified about this and an ultrasound
examination was arranged in Northern
Manitoba, rather than in Winnipeg. The
ultrasound confirmed fetal anencephaly.
The woman chose to have a pregnancy
termination in her hometown. She was
subsequently seen for genetic counseling
in Winnipeg.
Comment
Extremely high MSAFP levels (i.e., > 5.0
MOM) are usually associated with poor
outcomes. In this case, the low E3 level
suggested anencephaly. One cause of an
extremely elevated MSAFP level that has
a good prognosis is gastroschisis, which
can be corrected post-natally.
The Canadian Journal of Diagnosis / July 2001
Maternal Serum Screening
Case 4
A 36-year-old woman had an MSS at 16.5
weeks gestation, as determined by an
early ultrasound examination. The MSAFP
is 0.8 MOM, the HCG is 1.3 MOM and the
E3 is 0.9 MOM. The risks for fetal Down
syndrome went from 1/340 to 1/370. The
fetal assessment confirms the gestation, and
no abnormalities suggestive of Down syndrome are seen.
Outcome
After appropriate counseling, the woman
decided to have an amniocentesis. The
fetal karyotype was 47,XY, +21, confirming Down syndrome. After much deliberation, the woman decided to terminate the
pregnancy.
Comment
This is an example of a true-positive
screen. Although the risks of fetal Down
syndrome were lowered by the MSS, the
results were considered screen-positive
since the risks were greater than the cut-off
used by the MSS program. The Manitoba
MSS program uses a risk of 1/384 as a cutoff. This is the risk of an average 35-yearold having a live-born child with Down
syndrome. Some programs base their risk
cut-off on the risk of diagnosing fetal
Down syndrome at amniocentesis. A midtrimester risk of 1/270 is equivalent to a
term risk of 1/384, since about one-third of
fetuses with Down syndrome will die
before term. This case also illustrates that
applying a second screening test, such as
ultrasound, to a positive test is inappropriate. Since less than 70% of fetuses with
Down syndrome have any detectable signs
on a second-trimester ultrasound,7 relying
on the ultrasound as a second layer screen
would decrease the overall detection rate to
60% times 0.7, or
42%.
The detection rate MSAFP and HCG
for Down syndrome levels tend be be
increases
with
about twice as
advancing maternal
age, but so does the
high in twin
false-positive rate.
pregnancies.
The detection rate for
20-year-olds is about
40%, with a false-positive rate of 2.4%, as
compared to the detection rate of 75% and
a false-positive of 16% for 36-year-olds.8
Case 5
A 22-year-old has an MSS at 16.0 weeks
by sure dates. The MSAFP is 2.5 MOM,
the HCG is 2.1 MOM and the E3 is 1.7
MOM. The Down syndrome risk is
1/26,400.
Outcome
A fetal assessment shows that this is a
twin pregnancy. The results are considered normal for twins.
Comment
MSAFP and HCG levels tend be be about
twice as high in twin pregnancies. E3 levels are about 1.67 times higher. This MSS
pattern should strongly suggest a twin
pregnancy. Physicians should be careful
not to rely on MSS as a screening test for
twins, as only about 50% to 60% of cases
The Canadian Journal of Diagnosis / July 2001
65
Maternal Serum Screening
of twins are associated with elevated
MSAFP levels.9 Occasionally, the elevated HCG levels in twin pregnancies will
cause the test to be screen-positive for
Down syndrome. The MSS should not be
considered reliable in predicting the
chances of fetal Down syndrome when
twins are present. Some programs will
calculate a pseudo-risk estimate in this
situation.
Case 6
A 31-year-old has an MSS at 16 weeks by
certain dates. The MSAFP is 0.3 MOM,
the HCG is 0.2 MOM and the E3 is 0.3
MOM. The Down syndrome risk is 1/736
by age and 1/1,011 by MSS. The risk for
fetal trisomy 18 is quoted as 1/11.
Outcome
The women is counseled about the possibility of trisomy 18, and consents to an
amniocentesis. The ultrasound, however,
shows a fetal demise. The fetus appears to
be about 13 weeks size.
Comments
The pattern of low levels of all three parameters is suggestive of trisomy 18, but
also can be seen with a fetal demise as
levels return to the non-pregnant state.
Since fetal demise is much more common, it may be wise to suggest an ultrasound examination be done locally before
the woman travels long distances to the
tertiary center for an amniocentesis. Low
levels of E3 can be seen in a variety of
other conditions, including a relatively
66
benign skin disorder known as X-linked
ichthyosis. A recent fetal demise will
often cause elevated MSAFP levels
before the levels begin to drop.
Conclusion
MSS can be a valuable screening test for
fetal neural tube defects or chromosomal
anomalies. Physicians should counsel
their patients about the potential for falsepositive or false-negative results. There
are many causes for positive MSS results.
The pattern of the MSS levels may suggest an underlying cause and may be useful in providing post-test counseling. Dx
References
1. Rose NC, Mennuti MT: Maternal serum screening for
neural tube defects and fetal chromosome abnormalities. West J Med 1993; 159:312-7.
2. Merkatz IR, Nitowsky HM, Macri JN, et al: An association
between low maternal serum alpha-fetoprotein and
fetal chromosomal abnormalities. Am J Obstet
Gynecol 1984; 148:886-94.
3. Knight GJ, Palomaki GE, Haddow JE: Use of maternal
serum alpha-fetoprotein measurements to screen for
Downs syndrome. Clin Obstet Gynecol 1988; 31:30627.
4. Canick J, Knight GJ: Multiple marker screening for fetal
Down syndrome. Contemporary Ob/Gyn 1992; 36:2542.
5. Wald NJ, Watt HC, Hackshaw AK: Integrated screening
for Downs syndrome based on tests performed during the first and second trimester. N Engl J Med 1999;
341:461-7.
6. Haddow JE, Palomaki G, Knight GJ, et al: The Foundation
for Blood Research Handbook. Volume 1. The
Foundation for Blood Research, Maine, 1990, pp. 5-8.
7. Smith-Bindman R, Homer W, Feldstein VA, et al: Secondtrimester ultrasound to detect fetuses with Down syndrome. JAMA 2001; 285:1044-55.
8. Haddow JE, Palomaki GE: Prenatal screening for Down
syndrome. In: Simpson JL, Elias S (eds.): Essentials of
Prenatal Diagnosis. Churchill Livingstone, New York,
1993, p. 209.
9. Johnson JM, Harman CR, Evans JA, et al: Maternal
serum a-fetoprotein in twin pregnancy. Am J Obstet
Gynecol 1990; 162:1020-5.
The Canadian Journal of Diagnosis / July 2001
S-ar putea să vă placă și
- Quality Control Measurement Report Subject: Propeller Push Up. Rudder & Propeller Section Nord HoustonDocument2 paginiQuality Control Measurement Report Subject: Propeller Push Up. Rudder & Propeller Section Nord HoustonAhmed Magdy100% (1)
- Cracks in Propeller HubDocument2 paginiCracks in Propeller Hublitos_92Încă nu există evaluări
- Paper Torsional Vibration Calculation Issues With Propulsion SystemsDocument38 paginiPaper Torsional Vibration Calculation Issues With Propulsion Systemsgatheringforgardner9550Încă nu există evaluări
- Validation of Analysis Methods For Pad EyeDocument49 paginiValidation of Analysis Methods For Pad Eyegeorgekc77Încă nu există evaluări
- Bujes DuramaxDocument31 paginiBujes DuramaxAhmed Magdy0% (1)
- Paper Torsional Vibration Calculation Issues With Propulsion SystemsDocument38 paginiPaper Torsional Vibration Calculation Issues With Propulsion Systemsgatheringforgardner9550Încă nu există evaluări
- Design, Machining and Installation Manual for FEROFORM Marine BearingsDocument49 paginiDesign, Machining and Installation Manual for FEROFORM Marine BearingsWalter JosephÎncă nu există evaluări
- About Lip SealsDocument2 paginiAbout Lip SealsAhmed MagdyÎncă nu există evaluări
- PT-MT Kurs NotuDocument300 paginiPT-MT Kurs NotuBahadir TekinÎncă nu există evaluări
- D0401.02.01 - Calculation of Shaft Alignment FM-10Document20 paginiD0401.02.01 - Calculation of Shaft Alignment FM-10Ahmed MagdyÎncă nu există evaluări
- Validation of Analysis Methods For Pad EyeDocument49 paginiValidation of Analysis Methods For Pad Eyegeorgekc77Încă nu există evaluări
- Fast 50 Pips ProfitDocument19 paginiFast 50 Pips ProfitAhmed Magdy100% (1)
- CouplingDocument133 paginiCouplingAhmed Magdy100% (2)
- D0401.02.01 - Calculation of Shaft Alignment FM-10Document20 paginiD0401.02.01 - Calculation of Shaft Alignment FM-10Ahmed MagdyÎncă nu există evaluări
- Publications BroDocument2 paginiPublications BroAhmed MagdyÎncă nu există evaluări
- GEIT 40007EN NDT Film BrochureDocument56 paginiGEIT 40007EN NDT Film BrochurevrapciudorianÎncă nu există evaluări
- Ur A2 Rev3 Cor1 pdf2425Document6 paginiUr A2 Rev3 Cor1 pdf2425Ahmed MagdyÎncă nu există evaluări
- HiMSEN Global Academy CurriculumDocument1 paginăHiMSEN Global Academy CurriculumAhmed MagdyÎncă nu există evaluări
- Scienfdgfdce Seawater SgfdgdfcientistDocument8 paginiScienfdgfdce Seawater SgfdgdfcientistAhmed MagdyÎncă nu există evaluări
- Mastering Chart Analysis SkillsDocument47 paginiMastering Chart Analysis SkillsAhmed Magdy100% (6)
- COMPAC ConversionDocument12 paginiCOMPAC ConversionAhmed MagdyÎncă nu există evaluări
- Careers Advert NigerdockDocument1 paginăCareers Advert NigerdockAhmed MagdyÎncă nu există evaluări
- Apexior No1 pc900Document2 paginiApexior No1 pc900Ahmed MagdyÎncă nu există evaluări
- Damage To Stern Tube Bearing and SealsDocument4 paginiDamage To Stern Tube Bearing and SealsJoão Henrique Volpini MattosÎncă nu există evaluări
- Pub1466 WebDocument128 paginiPub1466 WebALE X RAY100% (1)
- SKF Bearing Installation and MaintenanceDocument146 paginiSKF Bearing Installation and MaintenanceDefinal ChaniagoÎncă nu există evaluări
- Impa Marine Stores Guide 3RD EdDocument0 paginiImpa Marine Stores Guide 3RD EdAhmed Magdy88% (41)
- Inert Gas Generator Systems (Iggs) - Cold Harbour MarineDocument1 paginăInert Gas Generator Systems (Iggs) - Cold Harbour MarineAhmed MagdyÎncă nu există evaluări
- 692D Guidelines Marine DesignersDocument9 pagini692D Guidelines Marine Designerspapaki2Încă nu există evaluări
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (890)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (587)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (73)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (265)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2219)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (119)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- Smoking Cessation: Prepared by Dr. Ahmed El MasryDocument77 paginiSmoking Cessation: Prepared by Dr. Ahmed El Masryاحمد المصرىÎncă nu există evaluări
- Sepsis: Symptoms, Causes and TreatmentDocument6 paginiSepsis: Symptoms, Causes and Treatmentapalah_niÎncă nu există evaluări
- Athero 2 Dr. Raquid 2021Document93 paginiAthero 2 Dr. Raquid 2021oreaÎncă nu există evaluări
- CDC guidelines for treating syphilisDocument27 paginiCDC guidelines for treating syphilisGabrielaGushikenÎncă nu există evaluări
- Surgical Pathology I: Mrs. Ngouah Odile Master in Public HealthDocument92 paginiSurgical Pathology I: Mrs. Ngouah Odile Master in Public Healthbomo floreÎncă nu există evaluări
- Luminaire - ENTDocument50 paginiLuminaire - ENTNikhil DeleepÎncă nu există evaluări
- Queratoglobo Expo 2012Document42 paginiQueratoglobo Expo 2012Oscar Alberto Rojas CabanillasÎncă nu există evaluări
- History History History: CounsellingDocument2 paginiHistory History History: CounsellingMahad IbrahemÎncă nu există evaluări
- DSM V Clinical Cases - Chapter 12 Sleep Wake DisordersDocument13 paginiDSM V Clinical Cases - Chapter 12 Sleep Wake DisordersIzzyinOzzieÎncă nu există evaluări
- Diabetic Striatopathy PosterDocument6 paginiDiabetic Striatopathy Posteradityamurugan1154Încă nu există evaluări
- Differential Diagnosis of Gastric CarcinomaDocument3 paginiDifferential Diagnosis of Gastric CarcinomaNantini GopalÎncă nu există evaluări
- Post Operative Emergency Management in Periodontics PeioDocument40 paginiPost Operative Emergency Management in Periodontics PeioFourthMolar.comÎncă nu există evaluări
- The Ai/Rheum Knowledge-Based Computer Consultant System in RheumatologyDocument8 paginiThe Ai/Rheum Knowledge-Based Computer Consultant System in RheumatologyMugundhan RamamoorthyÎncă nu există evaluări
- The Pediatrics HO GuideDocument44 paginiThe Pediatrics HO GuideAlex MatthewÎncă nu există evaluări
- GP Data InterpretationDocument2 paginiGP Data Interpretationareejk_94Încă nu există evaluări
- Assignment AnsDocument2 paginiAssignment AnsGurvirÎncă nu există evaluări
- Pearson Vue 1000 File (Corrected 11-2017)Document245 paginiPearson Vue 1000 File (Corrected 11-2017)adamÎncă nu există evaluări
- Bpac Antibiotics Booklet PDFDocument20 paginiBpac Antibiotics Booklet PDFVenny Tri Pahlevi IIÎncă nu există evaluări
- Practical 2 - Health - Assessment - Prac - 2023Document5 paginiPractical 2 - Health - Assessment - Prac - 2023Sreya PÎncă nu există evaluări
- Standard Operating Procedure (Haematology) : R. K. Life Services Private LimitedDocument61 paginiStandard Operating Procedure (Haematology) : R. K. Life Services Private LimitedAniruddha ChatterjeeÎncă nu există evaluări
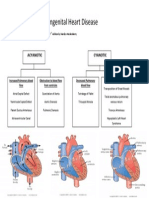
- Classification of Congenital Heart DiseaseDocument1 paginăClassification of Congenital Heart DiseaseClaudia SanchezÎncă nu există evaluări
- Problem Prioritization 1Document9 paginiProblem Prioritization 1Bernard A. EstoÎncă nu există evaluări
- PycnodysostosisDocument19 paginiPycnodysostosiscorneliusÎncă nu există evaluări
- Clostridia and Bacillus Lecture NotesDocument37 paginiClostridia and Bacillus Lecture NotesPrincewill SeiyefaÎncă nu există evaluări
- Differentiating Familial and Guillain-Barré NeuropathiesDocument22 paginiDifferentiating Familial and Guillain-Barré NeuropathiesKartika IwangÎncă nu există evaluări
- Thrombin Time - GRP 5Document14 paginiThrombin Time - GRP 5Joyce LeeÎncă nu există evaluări
- Filename-0 VNSG 1304 Pain Case Study Student Version Fall 2016Document2 paginiFilename-0 VNSG 1304 Pain Case Study Student Version Fall 2016thecheekymomÎncă nu există evaluări
- Natural Hygiene What Is ItDocument5 paginiNatural Hygiene What Is ItJonas Sunshine Callewaert100% (1)
- To Compare The Clinical Effectiveness of Azithromycin Vs Doxycycline On The First Follow-Up Visit of Acne Vulgaris PatientsDocument5 paginiTo Compare The Clinical Effectiveness of Azithromycin Vs Doxycycline On The First Follow-Up Visit of Acne Vulgaris PatientsI Made AryanaÎncă nu există evaluări
- English-Burmese Avian Flu GlossaryDocument30 paginiEnglish-Burmese Avian Flu GlossarywhitemaleandproudÎncă nu există evaluări