Documente Academic
Documente Profesional
Documente Cultură
Ethics
Încărcat de
Terence Shane AcodDrepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Ethics
Încărcat de
Terence Shane AcodDrepturi de autor:
Formate disponibile
Stem cell technology
Paulo A Fontes, Angus W Thomson
Thomas E Starzl Transplantation Institute, Department of Surgery, University of Pittsburgh Medical Center,
4C Falk Clinic, Pittsburgh, PA 15213, USA
Paulo A Fontes
assistant professor of surgery. Angus W Thomson
professor of surgery and molecular genetics and biochemistry
Correspondence to: P Fontes fontesp@msx.upmc.edu
BMJ 1999;319:1308
Stem cell technology is a rapidly developing field that combines the efforts of cell biologists, geneticists, and clinicians and
offers hope of effective treatment for a variety of malignant and non-malignant diseases. Stem cells are defined as
totipotent progenitor cells capable of self renewal and multilineage differentiation.1 Stem cells survive well and show stable
division in culture, making them ideal targets for in vitro manipulation. Although early research has focused on
haematopoietic stem cells, stem cells have also been recognised in other sites. Research into solid tissue stem cells has not
made the same progress as that on haematopoietic stem cells. This is due to the difficulty of reproducing the necessary and
precise three dimensional arrangements and tight cell-cell and cell-extracellular matrix interactions that exist in solid
organs. However, the ability of tissue stem cells to integrate into the tissue cytoarchitecture under the control of the host
microenvironment and developmental cues, makes them ideal for cell replacement therapy. In this overview, we briefly
discuss the current research and the clinical status of treatments based on haematopoietic and tissue stem cells.
Summary points
Stem cells are progenitor cells that are capable of self
renewal and differentiation into many different cell lineages
Stem cells have potential for treatment of many malignant
and non-malignant diseases
Peripheral blood stem cells are used routinely in
autologous and allogeneic bone marrow transplantation
Gene transfer into haematopoetic stem cells may allow
treatment of genetic or acquired diseases
Embryonic stem cells may eventually be grown in vitro to
produce complex organs
Neuronal stem cells are being used for neurone
replacement in neurovegetative disorders such as Parkinsons
and Huntingdons diseases
Haematopoietic stem cells
Applications of cultured haematopoietic stem cells
Haematopoietic stem cells are a somatic cell population
with highly specific homing properties and are capable of self
renewal and differentiation into multiple cell lineages.2 Human
haematopoietic progenitor cells, like stromal cell precursors in
bone marrow, express the CD34 antigen, a transmembrane cell
surface glycoprotein identified by the My10 monoclonal
antibody.3 However, pluripotent stem cells constitute only a small
fraction of the whole CD34+ population, which is by itself rather
heterogeneous regarding phenotype and function. The best way
to define haematopoietic stem cells is from their functional biology. They are known to restore multilineage, long term haematopoietic cell differentiation, and maturation in lethally
cytoablated hosts.4 Haematopoietic stem cells can be obtained
from bone marrow, peripheral blood,5 umbilical cord blood,6 and
fetal liver.7
The use of peripheral blood stem cells in both autologous
and allogeneic transplantation has become routine as they can
BMJ VOLUME 319
13 NOVEMBER 1999
www.bmj.com
be collected on an outpatient basis and also promote a consistent acceleration in haematopoietic reconstitution after
engraftment.8 Umbilical cord blood stem cells have been used
progressively in paediatric patients, from both related and unrelated HLA-matched donors. In recipients with severe T cell
immunodeficiency disorders, fast engraftment is required
together with a low risk of graft versus host disease and a low
viral transmission rate.9 Since umbilical cord blood stem cells
can be expanded in vitro or frozen for storage in cell banks10 they
have been used in clinical trials for both autologous and allogeneic haematopoietic stem cell transplantation.11
The bone marrow is a mesenchyme derived tissue consisting of a complex haematopoietic cellular component supported
by a microenvironment composed of stromal cells embedded in
a complex extracellular matrix.12 This extracellular matrix has an
important role in the facilitation of cell-to-cell interaction, in
addition to a more complex role in the binding and presentation
of cytokines to the haematopoietic progenitor cells.13 The
cytokine milieu and extracellular matrix interaction provides the
road map for maturation and differentiation of stem cells,14
which should be instrumental for their in vitro manipulation
before therapeutic use. For example, haematopoietic stem cells
can be manipulated in vitro to generate dendritic cells, the most
potent antigen presenting cells.
Dendritic cells have a pivotal role in the elicitation and regulation of antigen specific, major histocompatibility complexrestricted T cell responses and are thought to be the only antigen
presenting cells able to prime naive T cells. Dendritic cells can be
derived from CD34+ precursors in response to granulocyte
macrophage colony stimulating factor and tumour necrosis factor and from monocytes cultured with granulocyte macrophage
colony stimulating factor and interleukin-4.15 In vitro generated
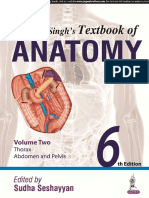
dendritic cells (fig) that have been transduced with genes coding
for tumour specific antigens or pulsed with tumour specific antigen or peptide could be useful for induction of cytotoxic T cell
responses.16 Dendritic cell tumour vaccines could be important
1
Characteristic dendritic cells derived from CD34+ haematopoietic stem
cells and propagated in granulocyte macrophage colony stimulating factor
future therapeutic tools; phase II clinical trials are under way and
show limited efficacy.17 On the other hand, the migration and
function of dendritic cells derived from liver in an allogeneic environment may be seminal in the development of donor specific
tolerance.1820 Genetic engineering of dendritic cells to express
immunosuppressive or immunoregulatory molecules may
provide a novel method to promote graft tolerance, reducing
dependence on systemic immunosuppression.21
Haematopoietic stem cells and gene therapy
Haematopoietic stem cells themselves are also a promising
target for gene therapy. Haematopoietic stem cells have been
made resistant to one or more cytotoxic drugs22 with retroviral
transfection of the multidrug resistance gene (MDR1). This
should help circumvent the myelosuppressive effects of standard
regimens of chemotherapy.23 Haematopoietic stem cells can also
be genetically marked to allow assessment of patterns of cell
survival, localisation, and function after bone marrow transplantation.24 This strategy has already been used with retroviral vectors.25 Double genetic marking is also being used to determine
the long term effects of different protocols of cytokines given to
promote bone marrow regeneration after cytoablative treatment.26 Gene transfer into haematopoietic stem cells represents
a novel approach for treating some genetic or acquired diseases.
So far, transduction of genes into humans using haematopoietic
stem cells has shown low efficiency, especially in the quiescent
stem cell population.27
Recent advances in reproductive biology and gene therapy
have used ex vivo transduced autologous umbilical cord blood
cells or direct targeting in utero as a potential means to correct
haematopoietic, immunological, and metabolic single gene disorders.28 This technique has the advantage of using normal haematological development, which induces the fetus to allow
space for a new cell population and promotes tolerance in the
developing immune system. Unfortunately, infection and graft
versus host disease are still potential risks for both the mother
and the fetus. However, advances in the understanding of dose
requirements and manipulation of peripheral blood sources to
enrich for stem cells may provide strategies to overcome these
problems.
Non-haematopoietic stem cells
The adult bone marrow also contains mesenchymal stem
cells29 which are involved in the regeneration of mesenchymal
tissues such as bone, cartilage, muscle, ligament, tendon, adipose tissue, and stroma. Although human mesenchymal stem
cells have been isolated, it remains unclear how basal nutrients,
cell density, spatial organisation, mechanical forces, growth factors, and cytokines control their differentiation.30 Isolated human
mesenchymal stem cells constitute a single, phenotypically distinct population and are uniformly positive for SH2, SH3, CD44,
CD71, CD90, CD106, CD120a, and CD124. They are also
2
negative for CD14 and CD34 and can be induced to differentiate
into adipocytes, chondrocytes, tenocytes, and osteocytes.
Transplantation of mesenchymal stem cells into tendon defects
in rabbits can significantly improve biomechanical properties of
the damaged area.31
Embryonic stem cells were first isolated in 1981 through
studies focusing primarily on murine blastocysts.32 Embryonic
stem cells are derived from totipotent cells of the early mammalian embryo and are capable of unlimited, undifferentiated proliferation in vitro.33 Human embryonic stem cells can express high
levels of telomerase activity, comparable with that expressed by
cells isolated from germ lines and embryonic tissues.34 They can
also form several cell types and simple tissue. Further
understanding of cell tissue interactions and their relation with
the extracellular matrix may eventually enable in vitro production
of complex organs.35 In vitro manipulation of embryonic stem
cells can be enhanced by nuclear transfer and cloning.36
Advances in stem cell technology have stimulated rapid
growth in the understanding of embryonic and postnatal neural
development. A population of neuronal stem cells capable of
extended self renewal in addition to subsequent differentiation
into both neurones and glia has already been identified.37 These
common neurohaematopoietic stem cells can be isolated from
the subventricular zone in the wall of the lateral ventricle of the
brain. They divide in response to epidermal growth factor and
fibroblast growth factor-2.38 Transplanted neuronal stem cells
can integrate into an intact brain and differentiate into neuronal
and glial cells. They may also function as haematopoietic stem
cells when infused into irradiated mice.39 This last finding is controversial and may represent an artefact of the experimental
technique, since only one contaminating haematopoietic stem
cell would be needed to repopulate a mouse haematopoietic
system. However, the reverse has also been shown, with stem
cells derived from bone marrow entering through the brain-blood
barrier, becoming fully differentiated, and displaying
macrophage-like function (microglia).40
Initial clinical trials have shown that neurone replacement
for neurovegetative diseases such as Parkinsons and
Huntingtons diseases is now feasible. Reports of transplantation
of fetal striatal tissue in patients with mild to severe Huntingtons
disease suggest that transplantation of neuronal stem cells may
improve some of the cognitive symptoms associated with the
condition, as well as potentially modifying its clinical course.41
Neuronal stem cells can also be manipulated before grafting;
they have been shown to respond to stimulation with fibroblast
growth factor-2, and immortalised neural stem-like cells infected
with viral vectors have been found to express factors that are
related to neural repair.42
The existence of prostate stem cells is still a matter of
debate.43 Nevertheless, the concept is interesting, mainly
because of the possible analogy between effects of androgens
on the prostate stem cells and that of cytokines on haematopoietic stem cells. Prostate stem cells could have important
implications in the development of prostatic carcinoma.44
Understanding of liver regeneration has improved greatly
since the initial description of oval cells as progeny of facultative
stem cells.45 Hepatic stem cells, which are found in the
interlobular bile ducts and possibly also in the canals of Hering,
could have a large impact on the pathophysiology of hepatocellular carcinomas and cholangiocarcinomas.46 47
Limbal stem cells have been described at the junction
between the cornea and sclerae.48 These cells are known to be
progenitors of corneal epithelium. Keratolimbal allografts are a
promising treatment for bilateral blindness,49 and limbal stem
cells can now be safely obtained from living related donors.50
Conclusions
Stem cell technology is progressing as the result of
multidisciplinary effort, with clinical applications of manipulated
BMJ VOLUME 319
13 NOVEMBER 1999
www.bmj.com
stem cells combining developments in transplantation and gene
therapy. There are rather complex ethical issues related to the
applications of cloning and nuclear transfer in human stem cells.
Successful ex vivo manipulation of stem cells will depend on
improved understanding of the interactions between cytokines
and the extracellular matrix. Cytokines may decrease binding
forces between stem cells and components of the stromal
microenvironment, thus facilitating the migration of stem cells
into the peripheral blood. Improvements in mobilisation
schedules using growth factors, stem cell isolation, and purification procedures and techniques for both positive and negative
purging (to reduce tumour cell contamination or to deplete T
lymphocytes) are emerging. The possibility of ex vivo multiplication of stem cells to accelerate haematopoietic recovery or to
provide sufficient stem cells from one extraction to support
several cycles of high dose chemotherapy is under investigation.
The applications for autologous stem cell transplantation should
increase as it avoids the use of non-specific immunosuppressive
therapy. Peripheral blood stem cells have advantages over bone
marrow cells for autologous transplantation in that they show
consistently faster haematopoietic reconstitution and can be
collected on an outpatient basis.
Stem cells originating from solid tissue can potentially be
applied in tissue repair. Techniques by which new genetic material is introduced into stem cells are being developed, and may
lead to the cure of various inherited diseases by somatic gene
therapy.
We thank David Kramer, Dana Faratian, and Dona Kocan for
scentific help with preparing the manuscript.
Funding: NIH grants DK49745 and AI41011.
Competing interests: None declared.
1
2
7
8
9
10
11
12
13
14
15
Till J, McMulloch E. A direct measurement of the radiation sensitivity of normal mouse
bone marrow cells. Rad Res 1961;14:1419-30.
Wu A, Till J, Simminovitch L, McCulloh E. Cytological evidence for a relationship between
normal hematopoietic colony-forming cells and cells from the lymphoid system. J Exp
Med 1968;127:455-67.
Civin CI, Strauss LC, Brovall C, Fackler MJ, Schwartz JF, Shaper JH. Antigenic analysis of
hematopoiesis III. A hematopoietic progenitor cell surface antigen defined by a
monoclonal antibody raised against KG-1a cells. J Immunol 1984;133:157-65.
Fraser C, Szilvassy S, Eaves C, Humphries R. Proliferation of totipotent hemopoietic stem
cells in vitro with retention of long term competitive in vivo reconstituting ability. Proc Natl
Acad Sci USA 1992;89:1968-72.
Kessinger HH, Armitage JO, Smither DM, Landmark JD, Bierman PJ, Weisenburger DD.
High dose chemotherapy and autologous peripheral blood stem cell transplantation for
patients with lymphoma. Blood 1989; 74:1260-5.
Broxmeyer HE, Douglas GW, Hangoc G, Cooper S, Bard J, English D, et al. Human
umbilical cord blood as a potential source of transplantable hemopoietic stem/progenitor
cells. Proc Natl Acad Sci USA 1989; 86:3828.
Morrison SJ, Hemmati HD, Wandycz AM, Weissman IL. The purification and characterization of fetal liver hematopoietic stem cells. Proc Natl Acad Sci USA 1995;92:10302-06.
Byrne JL, Russel NH. Peripheral blood stem cell transplants. J Clin Pathol 1998;51:35155.
Knusten AP, Wall D. Kinetics of T-cell development of umbilical cord blood transplantation
in severe T-cell immunodeficiency disorders. J Allergy Clin Immunol 1999;103:823-32.
Broxmeyer HE, Hangoc G, Cooper S, Ribeiro RC, Graves V, Yoder M, et al. Growth characteristics and expansion of human umbilical cord blood and estimation of its potential
for transplantation in adults. Proc Natl Acad Sci USA 1992;89:4109.
Rubinstein P, Adamson JW, Stevens C. The placental/umbilical cord blood program of the
New York Blood Center. A progress report. Ann NY Acad Sci 1999;872:328-34.
Rafii S, Shapiro F, Rimarachin J, Nachan RL, Ferris B, Weksler B, et al. Isolation and
characterization of human bone marrow microvascular endothelial cells: hematopoietic
progenitor cell adhesion. Blood 1994;84:10-9.
Sutherland HJ, Lansdorp PM, Henkelman DH, Eaves AC, Eaves CJ. Functional
characterization of individual human hematopoietic stem cells cultured at limiting dilution
on supportive marrow stromal layers. Proc Natl Acad Sci USA 1990;87:3584-88.
Petzer AL, Zandstra PW, Piret JM, Eaves CJ. Differential cytokine effects on primitive
(CD34+ CD38-) human hematopoietic cells: novel response to flt-3-ligand and thrombopoietin. J Exp Med 1996;183:2551-58.
Caux C,Massacrier C, Vanbervliet B, Dubois B, De Saint-Vis B, Dezotter-Dambuyant C, et
al. CD34+ hematopoietic progenitors from human cord blood differentiate along two
BMJ VOLUME 319
13 NOVEMBER 1999
www.bmj.com
independent dendritic cell pathways in response to GM-CSF+TNFa. J Exp Med
1996;184:695-706.
16 Timmerman JM, Levy R. Dendritic cell vaccines for cancer immunotherapy. Ann Rev Med
1999;50:507-29.
17 Tjoa BA, Simmons SJ, Elgamal A, Rogers M, Ragde H, Kenny GM, et al. Follow-up evaluation of a phase II prostate cancer vaccine trial. Prostate 1999;40:125-9.
18 Starzl TE, Demetris AJ, Murase N, Ildstad S, Ricordi C Trucco M. Cell migration, chimerism and graft acceptance. Lancet 1992;339:1579-82.
19 Thomson AW, Lu L, Murase N, Demetris AJ, Rao AS, Starzl TE. Microchimerism, dendritic
cell progenitors and transplantation tolerance. Stem Cells 1995;13:622-39.
20 Thomson AW, Lu L. Are dendritic cells the key to liver transplantation tolerance? Immunol Today 1999;20:27-32.
21 Lu L, Lee WC, Takayama T, Qian S, Gambotto A, Robbins PD. Genetic engineering of
dendritic cells to express immunosuppressive molecules. J Leukocyte Biol
1999;66:293-6.
22 Cowan KH, Moscow JA, Huang H, Zujewski JA, OShaughnessy J, Sorretino B, et al.
Paclitaxel chemotherapy after autologous stem-cell transplantation and engraftment of
hematopoietic cells transduced with a retrovirus containing the multidrug resistance
complementary DNA (MDR1) in metastatic breast cancer patients. Clin Cancer Res
1999;5:1619-28.
23 Rafferty JA, Hickson I, Chinnasamy N, Lashford LS, Margison GP, Dexter TM, et al. Chemoprotection of normal tissues by transfer of drug resistance genes. Cancer Metastasis
Rev 1996;15:365-83.
24 Capel B, Hawley RG, Mintz B. Long and short-lived murine hematopoietic stem cell
clones individually identified with retroviral integration markers. Blood 1990;75:226770.
25 Bachier CR, Giles RE, Ellerson D, Hanania EG, Garcia-Sanchez F, Andreeff M, et al.
Hematopoietic retroviral gene marking in patients with follicular non-Hodgkins
lymphoma. Leukemia Lymphoma 1999;32:279-88.
26 Heslop HE, Brenner MK, Krance RA, Bowman L, Cunningham JM, Richardson S, et al.
Use of double marking with retroviral vectors to determine rate of reconstitution of
untreated and cytokine expanded CD34+ selected marrow cells in patients undergoing
autologous bone marrow transplantation. Hum Gene Ther 1996;7:655-7.
27 Podsakoff G, Wong KK, Chatterjee S. Efficient gene transfer into non-dividing cells by
adeno-associated virus-based vectors. J Virol 1994;68:5656-66.
28 Flake A, Zanjani ED. In utero hematopoietic stem cell transplantation: a status report.
JAMA 1997;278:932-7.
29 Pittenger MF, Mackay AM, Beck SC, Jaiswal RK, Douglas R, Mosca JD, et al. Multilineage
potential of adult human mesenchymal stem cells. Science 1999;284:143-7.
30 Bruder SP, Ricalton NS, Boynton RE, Connolly TJ, Jaiswal N, Zaia J, et al. Mesenchymal
stem cell surface antigen SB-10 corresponds to activated leukocyte cell adhesion molecule and is involved in osteogenic differentiation. J Bone Min Res 1998;13:655-63.
31 Awad HA, Butler DL, Boivin GP, Smith FN, Malaviya P, Huibregtse B, et al. Autologous
mesenchymal stem cell-mediated repair of tendon. Tissue Eng 1999;5:267-77.
32 Magnuson T, Epstein CJ, Silver LM, Martin GR. Pluripotent embryonic stem cell lines can
be derived from tw5/tw5 blastocysts. Nature 1982;298:750-3.
33 Thomson JA, Marshall VS. Primate embryonic stem cells. Curr Top Devel Biol
1998;38:133-65.
34 Martin GR. Isolation of pluripotent cell line from early mouse embryos cultured in medium
conditioned by teratocarcinoma stem cells. Proc Natl Acad Sci USA 1981;78:7634-8.
35 Solter D, Gearhart J. Putting stem cells to work. Science 1999;283:1468-70.
36 Nagy A, Rossant J, Nagy R, Abramow-Newerly W, Roder JC. Derivation of completely cell
culture-derived mice from early-passage embryonic stem cells. Proc Natl Acad Sci USA
1993;90:8424-8.
37 Fisher LJ. Neural precursor cells: applications for the study and repair of the central nervous system. Neurobiol Dis 1997;4:1-22.
38 Shihabuddin LS, Ray J, Gage F. Stem cell technology for basic science and clinical applications. Arch Neurol 1999;56:29-32.
39 Bjorklund A, Svendsen C. Stem cells: breaking the brain-blood barrier. Nature
1999;397:569-7.
40 Dunnett SB, Bjorklund A. Prospects for new restorative and neuroprotective treatments
in Parkinsons disease. Nature 1999;399:32-9.
41 Philpott LM, Kopyov OV, Lee AJ, Jacques S, Duma CM, Caine S, et al. Neuropsychological functioning following fetal striatal transplantation in Huntingtons chorea: three case
presentations. Cell Transplant 1997;6:203-12.
42 Frisen J, Johansson CB, Lothian C, Lendahl U. Central nervous system stem cells in the
embryo and adult. Cellular Molecular Life Sci 1998;54:933-45.
43 Foster CS, Ke Y. Stem cells in prostatic epithelia. Int J Exp Path 1997;78:311.
44 Bonkhoff H, Remberger K. Differentiation pathways and histogenetic aspects of normal
and abnormal prostatic growth: a stem cell model. Prostate 1996;28:98.
45 Alison MR, Golding MHC, Sarraf CE. Pluripotential liver stem cells: facultative stem cells
located in the biliary tree. Cell Proliferation 1996;29:373-402.
46 Ruck P, Xiao JC, Kaiserling E. Small epithelial cells and the histogenesis of hepatoblastoma: electron microscopic, immunoelectron microscopic and immunohistochemical
findings. Am J Pathol 1996;148:321-9.
47 Hsia CC, Evarts RP, Nakatsukasa H, Marsden ER, Thorgeirsson SS. Occurrence of ovaltype cells in hepatitis B virus-associated human hepatocarcinogenesis. Hepatology
1992;16:1327-33.
48 Pellegrini G, Golisano O, Paterna P, Lambiase A, Bonini S, Rama P, et al. Location and
clonal analysis of stem cells and their differentiated progeny in the human ocular surface.
J Cell Biol 1999;145:769-82.
49 Holland EJ, Schwartz GS. Epithelial stem-cell transplantation for severe ocular-surface
disease. N Engl J Med 1999;340:1752-3.
50 Akpek EK, Foster CS. Limbal stem-cell transplantation. Int Ophthalmol Clinics
1999;39:71-82.
S-ar putea să vă placă și
- Strategies To Optimize Adult Stem Cell Therapy For Tissue RegenerationDocument16 paginiStrategies To Optimize Adult Stem Cell Therapy For Tissue RegenerationIhsan AnasÎncă nu există evaluări
- Stem Cell Therapy: A Novel & Futuristic Treatment Modality For Disaster InjuriesDocument17 paginiStem Cell Therapy: A Novel & Futuristic Treatment Modality For Disaster InjuriesChiboyKrenzÎncă nu există evaluări
- Strategies To Capitalize On Cell Spheroid Therapeutic Potential For Tissue Repair and Disease ModelingDocument13 paginiStrategies To Capitalize On Cell Spheroid Therapeutic Potential For Tissue Repair and Disease ModelingShai FuchsÎncă nu există evaluări
- Stem Cell Therapy: Jessica M. QuimbyDocument9 paginiStem Cell Therapy: Jessica M. QuimbySJ JungÎncă nu există evaluări
- HomingDocument14 paginiHomingMaría P SÎncă nu există evaluări
- მეზენქიმური ღეროვანი უჯრედებიDocument1 paginăმეზენქიმური ღეროვანი უჯრედებიEMD GROUPÎncă nu există evaluări
- Immunobiology of Human Mesenchymal Stem Cells and Future Use in Hematopoietic Stem Cell TransplantationDocument14 paginiImmunobiology of Human Mesenchymal Stem Cells and Future Use in Hematopoietic Stem Cell TransplantationTharissa SyabaniaÎncă nu există evaluări
- Mesenchymal Stem Cells Literature ReviewDocument9 paginiMesenchymal Stem Cells Literature ReviewafdtygyhkÎncă nu există evaluări
- JR 043 - Mesenchymal Stem Cell and Clinical Application in Chronic Lung Disease.210921-RevisionDocument10 paginiJR 043 - Mesenchymal Stem Cell and Clinical Application in Chronic Lung Disease.210921-RevisionLaila MaulidÎncă nu există evaluări
- Stem Cells Past, Present and FutureDocument3 paginiStem Cells Past, Present and FutureAndrés ChávezÎncă nu există evaluări
- Cell Biology:: Extracellular Supportive and Unsupportive Comparative Proteomic Analysis ofDocument17 paginiCell Biology:: Extracellular Supportive and Unsupportive Comparative Proteomic Analysis ofGeasle DerremenÎncă nu există evaluări
- 2010 Reumaticas N Nat Rev Rheumatol 2009 Jul 57 392-9Document8 pagini2010 Reumaticas N Nat Rev Rheumatol 2009 Jul 57 392-9Rafael Martinez FigueroaÎncă nu există evaluări
- Stem Cells and Cancer Stem Cells, Volume 3 - Stem Cells and Cancer Stem Cells, Therapeutic Applications in Disease and Injury - Volume 3Document426 paginiStem Cells and Cancer Stem Cells, Volume 3 - Stem Cells and Cancer Stem Cells, Therapeutic Applications in Disease and Injury - Volume 3Artan100% (1)
- 1 s2.0 S018844092030638X MainDocument9 pagini1 s2.0 S018844092030638X MainDarshan GandhiÎncă nu există evaluări
- Cancer 1Document8 paginiCancer 1JoseRodrigoSuarezCamposÎncă nu există evaluări
- Characterisation of Thrombocytes in Osteichthyes: Michał Stosik, Beata Tokarz-Deptuła, Wiesław DeptułaDocument9 paginiCharacterisation of Thrombocytes in Osteichthyes: Michał Stosik, Beata Tokarz-Deptuła, Wiesław DeptułaNovi AndrianiÎncă nu există evaluări
- Comparison of Migration PotentialDocument14 paginiComparison of Migration PotentialsmilecluodÎncă nu există evaluări
- Monocytes in Tumorigenesis and Tumor ImmunotherapyDocument19 paginiMonocytes in Tumorigenesis and Tumor ImmunotherapyIvan PerezÎncă nu există evaluări
- Mesenchymal Stem CellsDocument13 paginiMesenchymal Stem CellsArya NugrahaÎncă nu există evaluări
- Storti Foundation: Mesenchymal Stem Cells: The Fibroblasts' New Clothes?Document6 paginiStorti Foundation: Mesenchymal Stem Cells: The Fibroblasts' New Clothes?Irma GultomÎncă nu există evaluări
- The Future Role of Mesenchymal Stem Cells inDocument5 paginiThe Future Role of Mesenchymal Stem Cells inAthenaeum Scientific PublishersÎncă nu există evaluări
- Mekanisme Stem CellDocument17 paginiMekanisme Stem CellKEBIDANAN 16 UNHAS UNHASÎncă nu există evaluări
- OpTechSportsMed - 2017 - Friel - Amniotic Fluid - Cells - and Membrane ApplicationDocument5 paginiOpTechSportsMed - 2017 - Friel - Amniotic Fluid - Cells - and Membrane ApplicationJacob DoughertyÎncă nu există evaluări
- HepatocytesDocument2 paginiHepatocytesSandeep MandibeleÎncă nu există evaluări
- Stem Cell TherapyDocument4 paginiStem Cell TherapycharlottefongersÎncă nu există evaluări
- Comparing The Therapeutic Potential of Stem CellsDocument30 paginiComparing The Therapeutic Potential of Stem CellsAnaaya SinghaniaÎncă nu există evaluări
- Stem Cells and Cancer Stem Cells, Volume 2 - Stem Cells and Cancer Stem Cells, Therapeutic Applications in Disease and Injury - Volume 2Document409 paginiStem Cells and Cancer Stem Cells, Volume 2 - Stem Cells and Cancer Stem Cells, Therapeutic Applications in Disease and Injury - Volume 2ArtanÎncă nu există evaluări
- Cardiac Stem Cell Therapy: An Overview: AKM M Islam, AAS Majumder, F Doza, MM Rahman, H JesminDocument15 paginiCardiac Stem Cell Therapy: An Overview: AKM M Islam, AAS Majumder, F Doza, MM Rahman, H JesminNavojit ChowdhuryÎncă nu există evaluări
- Extracellular Matrix ScafoldDocument16 paginiExtracellular Matrix ScafoldmanishÎncă nu există evaluări
- Tissue EngineeringDocument8 paginiTissue EngineeringJimsÎncă nu există evaluări
- Broekman 2018Document14 paginiBroekman 2018NicoÎncă nu există evaluări
- The Tissue Engineering Triad - Combining Cells, Biomaterials and Signaling Mechanisms ToDocument23 paginiThe Tissue Engineering Triad - Combining Cells, Biomaterials and Signaling Mechanisms ToVeronica VianaÎncă nu există evaluări
- Immunobiology of Mesenchymal Stem Cells: ReviewDocument10 paginiImmunobiology of Mesenchymal Stem Cells: ReviewjoshuaÎncă nu există evaluări
- The Potencial of Mesenchymal Stem CellsDocument14 paginiThe Potencial of Mesenchymal Stem CellsBruno SouzaÎncă nu există evaluări
- Immunomodulatory Properties of Dental Tissue-Derived Mesenchymal Stem CellsDocument25 paginiImmunomodulatory Properties of Dental Tissue-Derived Mesenchymal Stem CellsFernando CruzÎncă nu există evaluări
- Mesenchymal Stem Cells: From Biology To Clinical UseDocument10 paginiMesenchymal Stem Cells: From Biology To Clinical UseroyÎncă nu există evaluări
- Mesenchymal Stem Cell Derived-Exosomes: A Modern Approach in Translational MedicineDocument21 paginiMesenchymal Stem Cell Derived-Exosomes: A Modern Approach in Translational MedicineMuhammad Javed GabaÎncă nu există evaluări
- Donor Selection Is A Critical Component Using Naive Endogenous Adult Stem CellsDocument28 paginiDonor Selection Is A Critical Component Using Naive Endogenous Adult Stem CellsAthenaeum Scientific PublishersÎncă nu există evaluări
- 17d Stem Cells ScieMedPoliticalDocument4 pagini17d Stem Cells ScieMedPoliticalbbdddÎncă nu există evaluări
- Ijms 21 04521Document19 paginiIjms 21 04521Farah BdrÎncă nu există evaluări
- Ex Vivo Culture of Human Bone Marrow Mesenchymal Stem CellsDocument10 paginiEx Vivo Culture of Human Bone Marrow Mesenchymal Stem CellsVillarreal FarelÎncă nu există evaluări
- Cap 5Document14 paginiCap 5NatsumiTakamoriÎncă nu există evaluări
- J Cellular Molecular Medi - 2014 - Liu - The Multiple Functional Roles of Mesenchymal Stem Cells in Participating inDocument10 paginiJ Cellular Molecular Medi - 2014 - Liu - The Multiple Functional Roles of Mesenchymal Stem Cells in Participating indr. RiyanÎncă nu există evaluări
- Stem Cells and Cancer Stem Cells (2015) PDFDocument159 paginiStem Cells and Cancer Stem Cells (2015) PDFdr.yogaÎncă nu există evaluări
- Changes in The Cell Surface Markers During NormalDocument10 paginiChanges in The Cell Surface Markers During NormalMaw BerryÎncă nu există evaluări
- tmpDBD5 TMPDocument6 paginitmpDBD5 TMPFrontiersÎncă nu există evaluări
- In Vitro Mesenchymal Stem Cell Differentiation After Mechanical StimulationDocument10 paginiIn Vitro Mesenchymal Stem Cell Differentiation After Mechanical StimulationBastion ReinhartÎncă nu există evaluări
- Chapter 8Document12 paginiChapter 8lala_0Încă nu există evaluări
- Jurnal KJH-Derivation of Mesenchymal Stem Cells From HumanDocument9 paginiJurnal KJH-Derivation of Mesenchymal Stem Cells From HumanClarion 642Încă nu există evaluări
- Cancer Stem Cell Niche The Place To BeDocument7 paginiCancer Stem Cell Niche The Place To BeAlejandra Isabel Juarez JimenezÎncă nu există evaluări
- Stemcells 2007-0416Document12 paginiStemcells 2007-0416Ikke OppgaveÎncă nu există evaluări
- Embryonic Stem Cell Properties and UseDocument6 paginiEmbryonic Stem Cell Properties and UseRaj Kumar SoniÎncă nu există evaluări
- Review: Multipotential Differentiation of Adipose Tissue-Derived Stem CellsDocument10 paginiReview: Multipotential Differentiation of Adipose Tissue-Derived Stem CellsHanayuki VizureiÎncă nu există evaluări
- Jurnal NeoplasmaDocument10 paginiJurnal NeoplasmaFadhilah Asyifa DewantiÎncă nu există evaluări
- Extracellular Matrix Scaffolds For Cartilage and Bone RegenerationDocument8 paginiExtracellular Matrix Scaffolds For Cartilage and Bone Regenerationduverney.gaviriaÎncă nu există evaluări
- Identification of New Genes Associated To Senescent and Tumorigenic Phenotypes in Mesenchymal Stem CellsDocument13 paginiIdentification of New Genes Associated To Senescent and Tumorigenic Phenotypes in Mesenchymal Stem CellsirmaÎncă nu există evaluări
- 1247 FTPDocument10 pagini1247 FTPMeow WeddingÎncă nu există evaluări
- Cutaneous MSCDocument11 paginiCutaneous MSCargolo_napoleaoÎncă nu există evaluări
- 03 TovarDocument8 pagini03 TovarSujith KuttanÎncă nu există evaluări
- Floyd17 TB Ch12Document5 paginiFloyd17 TB Ch12sdjuknicÎncă nu există evaluări
- Human Body Temperature and New Approaches To ConstDocument21 paginiHuman Body Temperature and New Approaches To ConstCarlos Apodman BellaÎncă nu există evaluări
- CDU ZOOLOGY Anatomical Terminologies in Chordates and Vertebrates WorksheetDocument4 paginiCDU ZOOLOGY Anatomical Terminologies in Chordates and Vertebrates WorksheetKrisha Mae VillanuevaÎncă nu există evaluări
- Skeletal System4Document1 paginăSkeletal System4Elisha DienteÎncă nu există evaluări
- Normocytic Normochromic AnemiaDocument18 paginiNormocytic Normochromic AnemiaElaizha PagulayanÎncă nu există evaluări
- Anatomy Chapters 6&7Document17 paginiAnatomy Chapters 6&7Tamara IdalyÎncă nu există evaluări
- Blood Group & RHDocument27 paginiBlood Group & RHfamtaluÎncă nu există evaluări
- HLTAAP002 Student Assessment Task 1 - QuestioningDocument18 paginiHLTAAP002 Student Assessment Task 1 - QuestioningMuskan Sohal0% (1)
- Hemangiopericytoma of Palate A Rare Case ReportDocument4 paginiHemangiopericytoma of Palate A Rare Case ReportIJAR JOURNALÎncă nu există evaluări
- Module 13 Answersheet Anatomy 21Document3 paginiModule 13 Answersheet Anatomy 21Cherold RoldanÎncă nu există evaluări
- Ai Chi - Meridians2Document4 paginiAi Chi - Meridians2sale18100% (1)
- Immunology Exam Q's With AnswersDocument26 paginiImmunology Exam Q's With AnswersHavardKrovel87% (55)
- AIIMS - Nov - 2012 - Paper @mmedicalbooksDocument289 paginiAIIMS - Nov - 2012 - Paper @mmedicalbooksbetsyÎncă nu există evaluări
- Science ReviewerDocument13 paginiScience ReviewerLenie MatanguihanÎncă nu există evaluări
- Effects of Myofascial Release and Stretching Technique On ROM and Reaction Time PDFDocument3 paginiEffects of Myofascial Release and Stretching Technique On ROM and Reaction Time PDFfisionovaisÎncă nu există evaluări
- Unit 1 Anatomy, Physiology and The Human Body: Learning OutcomesDocument91 paginiUnit 1 Anatomy, Physiology and The Human Body: Learning OutcomesDeolita BadiangÎncă nu există evaluări
- Large Intestine CA 2Document21 paginiLarge Intestine CA 2Worku KifleÎncă nu există evaluări
- KP 2. Pengaruh Agen Biologi Dan Mekanisme Perubahan Sel Serta Penyakit Yang DitimbulkannyaDocument28 paginiKP 2. Pengaruh Agen Biologi Dan Mekanisme Perubahan Sel Serta Penyakit Yang DitimbulkannyaShintia Surya PutriÎncă nu există evaluări
- Liver Function TestsDocument28 paginiLiver Function TestsDr. Ashish Jawarkar100% (2)
- ThyroidDocument7 paginiThyroidverawoÎncă nu există evaluări
- Immunity and Vaccination RecordedDocument49 paginiImmunity and Vaccination RecordedMOMINAH AbbasiÎncă nu există evaluări
- Physiology of Reproduction in Women IDocument34 paginiPhysiology of Reproduction in Women Iapi-196413370% (1)
- IB Biology HL: 11.1 Antibody Production and VaccinationDocument7 paginiIB Biology HL: 11.1 Antibody Production and VaccinationpetraÎncă nu există evaluări
- IB Singh Vol-2Document387 paginiIB Singh Vol-2dannyÎncă nu există evaluări
- Nervous System - Anatomy & PhysiologyDocument2 paginiNervous System - Anatomy & PhysiologykathzheinÎncă nu există evaluări
- Making Sense of TasteDocument10 paginiMaking Sense of TastetufekciosmanÎncă nu există evaluări
- Multiple MyelomaDocument28 paginiMultiple Myelomamedical notes100% (1)
- Gram Staining Protocol or ProcedureDocument4 paginiGram Staining Protocol or Procedurearavindbt2523Încă nu există evaluări
- Grade 9 QDocument4 paginiGrade 9 Qhanatabbal19Încă nu există evaluări
- End Feel: K.SoundararajanDocument33 paginiEnd Feel: K.Soundararajanjack sparrowÎncă nu există evaluări