Documente Academic
Documente Profesional
Documente Cultură
Hiv and Folliculitis
Încărcat de
Giorgos Doukas KaranasiosTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Hiv and Folliculitis
Încărcat de
Giorgos Doukas KaranasiosDrepturi de autor:
Formate disponibile
Sex Transm Inf 1999;75:291293
Clinical
knots
291
HIV associated eosinophilic folliculitis
diVerential diagnosis and management
Sara L Simpson-Dent, Louise A Fearfield, Richard C D Staughton
Eosinophilic folliculitis (EF) is a chronic, intensely pruritic condition of unknown pathogenesis
that causes marked morbidity in those HIV patients whom it aVects. There is a wide diVerential
diagnosis of itchy skin conditions in HIV which are amenable to diVerent treatments. It is therefore essential to take a biopsy of each suspected case and examine multiple sections of the biopsy
to confirm or refute a diagnosis of EF. Treatment of EF can be diYcult but we hope that by suggesting a rational approach to this and considering possible therapeutic options more patients
may be helped with this troublesome dermatosis.
(Sex Transm Inf 1999;75:291293)
Keywords: eosinophilic folliculitis; HIV
Introduction
Eosinophilic pustular folliculitis was originally
described by Ofuji et al.1 It was not until 1986
that it was first recognised to occur in the
human immunodeficiency virus (HIV) infected population.2 In this group it is now
referred to as HIV associated eosinophilic
folliculitis (EF) as it shows diVerences from the
original Japanese description in its distribution,
appearance of lesions, disease course, and
symptoms. EF is not unique to HIV as it has
rarely been described in association with
haematological malignancies.3
Department of
Dermatology, Chelsea
and Westminster
Hospital, London
SW10 9NH
S Simpson-Dent
L Fearfield
R Staughton
Correspondence to:
Dr Simpson-Dent.
Accepted for publication
7 September 1999
Clinical picture
Patients aVected by EF classically complain of
a persistent pruritic rash. The intensity of the
itch is akin to that of scabies and patients excoriate deeply. Clinically, one can see 23 mm
erythematous papules or pustules, most frequently aVecting the shoulders, trunk, upper
arms, neck and forehead, where it can be
disfiguring (fig 1). Less commonly, other areas
of the body are aVected but EF is only rarely
generalised. Lesions are follicular and are often
markedly excoriated, making it diYcult to
determine their nature. It is therefore important to look for fresh unexcoriated lesions.
There are no associated systemic features but
patients are often tired and irritable.
EF is quite common, occurring in HIV
infected individuals with a CD4 count of less
than 250 106/l with an incidence, in one series,
of 9%.4 Up to 50% of suVerers will have a
peripheral eosinophilia, up to 4109/l in our
series and their IgE is often also elevated.
DiVerential diagnosis
Clinically the diVerential diagnosis of EF is
between the infective folliculitides or other
dermatoses that may or may not be HIV
relatedfor example, scabies, urticaria, drug
rashes, and eczema. Clues in the history and
the examination can help refine the diagnosis
(table 1). Of note we feel that it is inappropriate to make a diagnosis of papular eruption of
Figure 1 (A) Back of patient suVering from EF. Note the
multiple excoriation marks. (B) Close up of a patients
forehead demonstrating the characteristic erythematous
follicular papules of EF.
HIV as most cases will turn out to be EF if
investigated appropriately.
Investigation of EF
Owing to the wide diVerential diagnosis of EF
we always recommend that a skin biopsy is
taken and sent for histology for routine haematoxylin and eosin stain as well as for special
stains for fungi, bacteria, and viruses, as
cutaneous infections can present with atypical
clinical features. The biopsy should, if possible,
be taken from an unexcoriated fresh lesion and
serially sectioned. Sellotape strippings for
demodex mites and scrapings for scabies
should also be performed if there is any clinical
suspicion of these.
Simpson-Dent, Fearfield, Staughton
292
Table 1
Ways of obtaining diagnosis of eosinophilic folliculitis
DiVerential diagnosis
Infestations:
Scabies
Papular urticaria
(insect bite reactions)
Atopy:
Urticaria
Eczema
Clues in history and examination
Nightime itching
Partner itching
Genital and web space lesions present
No facial lesions
Crops of linearly arranged papules
Pets at home, hostel accommodation, or of no fixed abode
?Lice on seams of patients clothes
Individual weals lasting 612 hours
?Family or personal history of atopy
Flexural rash
Iatrogenic:
Drug rash
New drug within past 1014 days
Generalised rash
Other:
Nodular prurigo
Lichen planus/nitidis
Nodular rather than papular lesions lasting months/years
Flat topped purple papules with Wickhams striae
?Any buccal or genital lesions
proposed although no one organism has
consistently been isolated in biopsy specimens.
Fungi, yeasts, demodex, and bacteria have all at
times been seen and implicated. Other theories
are of a follicular hypersensitivity reaction or an
autoimmune reaction to sebum (L A Fearfield,
in preparation).
Treatment of EF
Treatment of EF is diYcult and varied because
the underlying pathogenic mechanism of EF still
remains to be elucidated. Treatments tried have
included topical steroids, topical ascaridesfor
example, permethrin, phototherapy (ultraviolet
A and B light), itraconazole, isotretinoin, and
metronidazole. All have had reported successes
but the series reported have tended to be of
small size and anecdotal rather than controlled
or randomised. We discuss the diVerent modalities below and our recommendations for treatment are shown in table 2.
TOPICAL STEROIDS
These can give partial temporary symptomatic
relief but new lesions continue to crop up. For
example, 0.1% betamethasone valerate (Betnovate, Glaxo), can be useful as a temporary measure when awaiting the results of the biopsy.
ANTIHISTAMINES
Figure 2 Medium power of haematoxylin and eosin stained
section showing an infiltrate of eosinophils and lymphocytes
centred on the follicle with marked sebaceous lysis.
Histology of EF
The histology of EF5 shows an inflammatory
infiltrate, predominantly of eosinophils and
lymphocytes which is folliculocentric with
marked sebaceous lysis (fig 2). This is distinct
from infective causes of folliculitisfor example, Gram positive cocci, demodex, and pityrosporum when micro-organisms are seen within
the inflammatory infiltrate (macrophages and
neutrophils). The aVected follicle is frequently
ruptured in a bacterial folliculitis. The histopathologist should be asked to take multiple
serial sections of the EF biopsy as otherwise the
aVected follicle may be missed and the
incorrect diagnosis made.
Pathogenesis of EF
The pathogenesis of EF is unknown but, owing
to the folliculocentric nature of the inflammation, an opportunistic infection has been
Table 2
Management of eosinophilic folliculitis
Short term management
(1) Biopsy, then while awaiting result:
(2) Topical steroidfor example, 0.1% betamethasone valerate ointment
(3) Antihistaminefor example, cetirizine 2040 mg daily
Long term management
4 week trial of itraconazole 200 mg once daily
or
metronidazole 250 mg three times daily
or
referral to a dermatologist for ultraviolet B 23 times/week to clearance
+/ maintenance
or
isotretinoin 2040 mg daily for 46 weeks
The anti-eosinophilic cetirizine (Zirtek,
Schering-Plough) gives modest symptomatic
relief especially if higher than usual dosages are
usedfor example, 2040 mg daily in divided
doses.
ULTRAVIOLET B PHOTOTHERAPY
Patients often report an improvement in symptoms after sunny holidays abroad and
ultraviolet B is established as an eVective
treatment.6 Patients mostly respond to thrice
weekly broad band ultraviolet B within 36
weeks. Relapse is frequent and weekly maintenance ultraviolet B may be needed. Ultraviolet
B exerts an immunosuppressive eVect on the
skin and herpes simplex virus is reactivated in
some. Earlier fears of accelerating progression
of HIV disease have not been borne out.
ITRACONAZOLE
It has been suggested, by some authors, that
fungi or yeastsfor example, Pityrosporum
ovale may be involved in the pathogenesis of
EF. This is certainly supported by the response
of EF to oral itraconazole. In one study, by
Berger et al, of 28 patients 74% showed initial
complete or partial response to oral itraconazole. At 3 months five remained clear oV treatment, two required topical steroids only, and
12 were controlled (n=8) or partly controlled
with oral itraconazole.7 It is suggested that itraconazole is started at a dose of 200 mg daily. A
response is normally seen within the first 2
weeks but if this has not occurred or the
response is incomplete then the dose may be
increased to 300 mg or 400 mg daily although
the incidence of side eVects is then increased.
Maintenance therapy may be necessary. Fluconazole is not a substitute for itraconazole as
patients changed to this drug relapsed.7
HIV associated eosinophilic folliculitis
METRONIDAZOLE
Metronidazole 250 mg three times daily for 4
weeks was reported to be eVective in clearing
EF in five out of five patients initially8 and following any subsequent relapse. This followed
the finding of a Gram negative organism on
one of the patients biopsies.
293
introduction of highly active antiretroviral
therapy (HAART), although there have not
been any reports of this in the literature. This is
probably because patients CD4 counts usually
rise above 250 106/l on HAART.
OTHERS
ISOTRETINOIN
In an initial study in 19959 all of the seven
patients treated demonstrated complete response within 14 weeks of starting isotretinoin
treatment at a dose of 4080 mg/day (higher
doses were given for those patients who were
more severely aVected). Any relapses responded
to repeat courses of isotretinoin. (It must be
remembered that isotretinoin is teratogenic and
therefore should be used only with extreme caution in women of childbearing age.)
In our experience it is a very eVective and
well tolerated treatment using a lower dose of
20 mg daily for 68 weeks. The usual side effect
of drying of the skin can be counteracted by the
liberal use of moisturisers. The mechanism of
action may be to reduce perifollicular cellular
infiltration but the drug greatly curtails sebum
production, which Fearfield has proposed as
the putative autoantigen in EF.
PERMETHRIN
The commensal follicle mite, demodex, is a
possible trigger antigen. A small series of
patients have responded to topical 5% permethrin cream used daily on lesions and were
able to control the disease eventually with one
or two applications per week but upon
cessation of treatment lesions recurred,10 but
we have been unable repeat such success.
ANTIRETROVIRAL THERAPY
We have seen a marked decrease in the number
of patients with EF in our clinics since the
Topical sodium cromoglycate, topical antibiotics, prednisolone, and dapsone have also been
successfully used in some patients.
Contributors: SLS-D wrote the paper; LAF performed the
research project and provided references and clinical and
histopathological pictures; RCDS supervised the research
project and the paper.
1 Ofuji S, Ogino A, Horio T, et al. Eosinophilic pustular
folliculitis. Acta Derm Venereol (Stockh) 1970;50:195203.
2 Soeprono FF, Schinella RA. Eosinophilic pustular folliculitis in patients with acquired immunodeficiency syndrome.
J Am Acad Dermatol 1986;14:10202.
3 Bull RH, Harland CA, Fallowfield ME, et al. Eosinophilic
folliculitis: a self-limiting illness in patients being treated for
haematological malignancy. Br J Dermatol 1993;129:178
82.
4 Uthayakumar S, Nandwani R, Drinkwater T, et al. The
prevalence of skin disease in HIV infection and its relationship to the degree of immunosuppression. Br J Dermatol
1997;137:5958.
5 McCalmont TH, Altemus D, Maurer T, et al. Eosinophilic
folliculitis. The histologic spectrum. Am J Dermatopathol
1995;17:43946.
6 Buchness MR, Lim HW, Hatcher VA, et al. Eosinophilic
pustular folliculitis in the acquired immunodeficiency syndrome. Treatment with ultraviolet B phototherapy. N Engl
J Med 1988;318:11836.
7 Berger TG , Heon V, King C, et al. Itraconazole therapy for
human immunodeficiency virus-associated eosinophilic
folliculitis. Arch Dermatol 1995;131:35860.
8 Smith KJ, Skelton HG, Yeager J, et al. Metronidazole for
eosinophilic pustular folliculitis in human immunodeficiency virus type 1-positive patients. Arch Dermatol
1995;131:108991.
9 Otley CC, Avram MR, Johnson RA. Isotretinoin treatment
of human immunodeficiency virus-associated eosinophilic
folliculitis. Arch Dermatol 1995;131:104750.
10 Blauvelt A, Plott RT, Spooner K, et al. Eosinophilic folliculitis associated with the acquired immunodeficiency
syndrome responds well to permethrin. Arch Dermatol
1995;131:3601.
S-ar putea să vă placă și
- Lecture 01 - Introduction To ParasitologyDocument38 paginiLecture 01 - Introduction To ParasitologyGiorgos Doukas KaranasiosÎncă nu există evaluări
- Parasitology NotesDocument59 paginiParasitology NotesGiorgos Doukas KaranasiosÎncă nu există evaluări
- Carol Davila Pathophysiology NotesDocument10 paginiCarol Davila Pathophysiology NotesGiorgos Doukas KaranasiosÎncă nu există evaluări
- Pulmonary Consolidation SyndromesDocument141 paginiPulmonary Consolidation SyndromesGiorgos Doukas KaranasiosÎncă nu există evaluări
- LP2 enDocument4 paginiLP2 enGiorgos Doukas KaranasiosÎncă nu există evaluări
- Credit & Subjects An 2 (Highlighted Is Sem 1)Document1 paginăCredit & Subjects An 2 (Highlighted Is Sem 1)Giorgos Doukas KaranasiosÎncă nu există evaluări
- Kidney 2 AdelinaVladDocument65 paginiKidney 2 AdelinaVladGiorgos Doukas KaranasiosÎncă nu există evaluări
- Subjects For The Physiology Practical Exam - Sem 2 - 2015Document1 paginăSubjects For The Physiology Practical Exam - Sem 2 - 2015Giorgos Doukas KaranasiosÎncă nu există evaluări
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (588)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (345)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (74)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2259)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (121)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- Movie Piracy in Ethiopian CinemaDocument22 paginiMovie Piracy in Ethiopian CinemaBehailu Shiferaw MihireteÎncă nu există evaluări
- AIA1800 Operator ManualDocument184 paginiAIA1800 Operator ManualZain Sa'adehÎncă nu există evaluări
- Technology Management 1Document38 paginiTechnology Management 1Anu NileshÎncă nu există evaluări
- Environmental Economics Pollution Control: Mrinal Kanti DuttaDocument253 paginiEnvironmental Economics Pollution Control: Mrinal Kanti DuttashubhamÎncă nu există evaluări
- B122 - Tma03Document7 paginiB122 - Tma03Martin SantambrogioÎncă nu există evaluări
- DPSD ProjectDocument30 paginiDPSD ProjectSri NidhiÎncă nu există evaluări
- UTP Student Industrial ReportDocument50 paginiUTP Student Industrial ReportAnwar HalimÎncă nu există evaluări
- UC 20 - Produce Cement Concrete CastingDocument69 paginiUC 20 - Produce Cement Concrete Castingtariku kiros100% (2)
- Elements of ArtDocument1 paginăElements of Artsamson8cindy8louÎncă nu există evaluări
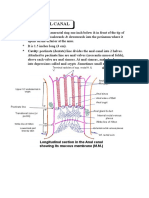
- Anatomy Anal CanalDocument14 paginiAnatomy Anal CanalBela Ronaldoe100% (1)
- Lec 33 - Householder MethodDocument11 paginiLec 33 - Householder MethodMudit SinhaÎncă nu există evaluări
- 2021-03 Trophy LagerDocument11 pagini2021-03 Trophy LagerAderayo OnipedeÎncă nu există evaluări
- All You Need To Know About Egg YolkDocument7 paginiAll You Need To Know About Egg YolkGolden Era BookwormÎncă nu există evaluări
- Obesity - The Health Time Bomb: ©LTPHN 2008Document36 paginiObesity - The Health Time Bomb: ©LTPHN 2008EVA PUTRANTO100% (2)
- Origami Oso HormigueroDocument9 paginiOrigami Oso HormigueroRogelio CerdaÎncă nu există evaluări
- Technical Bulletin LXL: No. Subject Release DateDocument8 paginiTechnical Bulletin LXL: No. Subject Release DateTrunggana AbdulÎncă nu există evaluări
- Read While Being Blind.. Braille's Alphabet: Be Aware and Active !Document3 paginiRead While Being Blind.. Braille's Alphabet: Be Aware and Active !bitermanÎncă nu există evaluări
- Shostack ModSec08 Experiences Threat Modeling at MicrosoftDocument11 paginiShostack ModSec08 Experiences Threat Modeling at MicrosoftwolfenicÎncă nu există evaluări
- Corrosion Fatigue Phenomena Learned From Failure AnalysisDocument10 paginiCorrosion Fatigue Phenomena Learned From Failure AnalysisDavid Jose Velandia MunozÎncă nu există evaluări
- 1.technical Specifications (Piling)Document15 pagini1.technical Specifications (Piling)Kunal Panchal100% (2)
- Assembler Pass 2Document5 paginiAssembler Pass 2AnuÎncă nu există evaluări
- GT-N7100-Full Schematic PDFDocument67 paginiGT-N7100-Full Schematic PDFprncha86% (7)
- 70 Valves SolenoidDocument105 pagini70 Valves SolenoidrizalÎncă nu există evaluări
- DP 2 Human IngenuityDocument8 paginiDP 2 Human Ingenuityamacodoudiouf02Încă nu există evaluări
- II 2022 06 Baena-Rojas CanoDocument11 paginiII 2022 06 Baena-Rojas CanoSebastian GaonaÎncă nu există evaluări
- Report Card Grade 1 2Document3 paginiReport Card Grade 1 2Mely DelacruzÎncă nu există evaluări
- 2009 2011 DS Manual - Club Car (001-061)Document61 pagini2009 2011 DS Manual - Club Car (001-061)misaÎncă nu există evaluări
- Introduction-: Microprocessor 68000Document13 paginiIntroduction-: Microprocessor 68000margyaÎncă nu există evaluări
- Online Extra: "Economists Suffer From Physics Envy"Document2 paginiOnline Extra: "Economists Suffer From Physics Envy"Bisto MasiloÎncă nu există evaluări
- Analizador de Combustion Kigaz 310 Manual EngDocument60 paginiAnalizador de Combustion Kigaz 310 Manual EngJully Milagros Rodriguez LaicheÎncă nu există evaluări