Documente Academic
Documente Profesional
Documente Cultură
Cambios de Paradigmas en Tratamiento Del Fallo Cardíaco
Încărcat de
Sander San MartínDrepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Cambios de Paradigmas en Tratamiento Del Fallo Cardíaco
Încărcat de
Sander San MartínDrepturi de autor:
Formate disponibile
PE R S PE C T IV E
Paradigm Shifts in Heart-Failure Therapy
Paradigm Shifts in Heart-Failure Therapy A Timeline
Chana A. Sacks, M.D., John A. Jarcho, M.D., and Gregory D. Curfman, M.D.
Related article, p. 993
ith the publication of the
PARADIGM-HF trial in the
Journal (pages 9931004) we may
be entering a new era of treatment
for heart failure with reduced
ejection fraction. To provide a historical perspective on the beginning of this new epoch, we constructed an interactive
An interactive
timeline (available with
timeline is
available
the full text of this arat NEJM.org
ticle at NEJM.org) of
26 randomized, controlled trials
in heart-failure treatment that have
been published in the Journal since
1986. Each of these articles
some demonstrating successes
and others documenting disappointments represents a critical step in the effort to reduce
mortality from heart failure with
reduced ejection fraction. The
timeline includes important milestones, some of which mark
paradigm shifts in the treatment
of this debilitating disorder.
The timeline makes clear that
highly productive research in heart
failure has been an international
effort. This pattern of international collaboration was continued in
PARADIGM-HF, a trial conducted in 47 countries, with principal investigators from Scotland
and the United States.
The modern history of therapy
for heart failure with reduced
ejection fraction began with the
introduction of vasodilatation as
a treatment for heart failure. The
V-HeFT I study (1986; see box for
cited Journal articles) demonstrated that treatment with hydralazine plus isosorbide dinitrate, as
compared with either placebo or
prazosin, reduced mortality. Soon
thereafter, the CONSENSUS (1987)
and SOLVD-Treatment (1991a) trials established that angiotensinconvertingenzyme (ACE) inhibition with enalapril reduced overall
mortality by 16 to 40%. V-HeFT II
(1991b) showed that enalapril was
superior to the combination of
hydralazine and isosorbide dinitrate. The SOLVD-Prevention trial
(1992) showed that enalaprils benefit in reducing the rate of hospitalizations for heart failure extended to asymptomatic patients with
reduced ejection fraction. These
landmark trials ushered in the era
of ACE inhibition, which has been
the centerpiece of heart-failure
therapy for 25 years.
Angiotensin-receptor blockers
(ARBs) interfere with the action
of angiotensin II at its type 1 receptor, resulting in vasodilatation.
These agents interrupt the angiotensin pathway by a different
mechanism than ACE inhibitors,
which block the conversion of angiotensin I to angiotensin II and
also interfere with the breakdown
of kinins. The Val-HeFT trial
(2001c) introduced the concept of
ARB therapy for heart failure, but
because treatment with ARBs is
not superior to treatment with
ACE inhibitors, ARBs have generally been reserved for patients who
cannot take ACE inhibitors because of cough or angioedema.
The use of beta-blocker therapy, now a cornerstone of heartfailure treatment, was once considered counterintuitive, because
of concern that patients with reduced ejection fraction either
would not benefit or would have
unacceptable side effects from
adrenergic blockade. However,
evidence of a mortality benefit
emerged for three beta-blockers,
bisoprolol, carvedilol, and sustained-release metoprolol. In the
timeline, we include two studies
on the alpha- and beta-adrenergic blocker carvedilol (the U.S.
Carvedilol Heart Failure Study,
1996, and COPERNICUS, 2001a).
Both studies demonstrated that
carvedilol led to a substantial reduction in mortality and contributed to our understanding of the
role of adrenergic activation in
the pathophysiology of heart failure. These studies underscored a
novel, transformative approach
to therapy.
Another paradigm shift in
heart-failure therapy occurred
with the RALES trial (1999) of
spironolactone, a mineralocorticoid-receptor antagonist (MRA).
The investigators reported a 30%
reduction in mortality among patients already receiving an ACE
inhibitor and a loop diuretic. The
EMPHASIS-HF trial (2011a), in
which investigators studied the
MRA eplerenone in patients with
systolic heart failure and mild
symptoms, confirmed and extended this finding. Together,
these trials added another important drug class to the heartfailure armamentarium.
Not all therapies listed on the
timeline proved successful. Drugs
with positive inotropic effects,
such as the phosphodiesterase
inhibitor milrinone, provide a
striking example. In a large clinical trial (PROMISE, 1991c), oral
milrinone, as compared with placebo, increased mortality among
patients with heart failure by 28%.
Novel inotropic agents generally
proved disappointing.
n engl j med 371;11nejm.orgseptember 11, 2014
The New England Journal of Medicine
Downloaded from nejm.org on September 10, 2014. For personal use only. No other uses without permission.
Copyright 2014 Massachusetts Medical Society. All rights reserved.
989
PERS PE C T IV E
Paradigm Shifts in Heart-Failure Therapy
Heart-Failure Therapy Articles in the New England Journal of Medicine
1986. V-HeFT I. Cohn JN, Archibald DG, Ziesche S, et al. Effect of vasodilator therapy on mortality in chronic congestive heart failure. 314:1547-52.
1987. CONSENSUS. The Consensus Trial Study Group. Effects of enalapril on
mortality in severe congestive heart failure. 316:1429-35.
1991a. SOLVD-Treatment. The SOLVD Investigators. Effect of enalapril on survival
in patients with reduced left ventricular ejection fractions and congestive heart
failure. 325:293-302.
1991b. V-HeFT II. Cohn JN, Johnson G, Ziesche S, et al. A comparison of enalapril
with hydralazineisosorbide dinitrate in the treatment of chronic congestive
heart failure. 325:303-10.
1991c. PROMISE. Packer M, Carver JR, Rodeheffer RJ, et al. Effect of oral milrinone
on mortality in severe chronic heart failure. 325:1468-75.
1992. SOLVD-Prevention. The SOLVD Investigators. Effect of enalapril on mortality
and the development of heart failure in asymptomatic patients with reduced
left ventricular ejection fractions. 327:685-91.
1996. U.S. Carvedilol Heart Failure Study Group. Packer M, Bristow MR, Cohn JN,
et al. The effect of carvedilol on morbidity and mortality in patients with chronic heart failure. 334:1349-55.
1997. DIG. The Digitalis Investigation Group. The effect of digoxin on mortality
and morbidity in patients with heart failure. 336:525-33.
1999. RALES. Pitt B, Zannad F, Remme WJ, et al. The effect of spironolactone on
morbidity and mortality in patients with severe heart failure. 341:709-17.
2001a. COPERNICUS. Packer M, Coats AJS, Fowler MB, et al. Effect of carvedilol
on survival in severe chronic heart failure. 344:1651-8.
2001b. REMATCH. Rose EA, Gelijns AC, Moskowitz AJ, et al. Long-term use of a
left ventricular assist device for end-stage heart failure. 345:1435-43.
2001c. Val-HeFT. Cohn JN, Tognoni G. A randomized trial of the angiotensinreceptor blocker valsartan in chronic heart failure. 345:1667-75.
2004. COMPANION. Bristow MR, Saxon LA, Boehmer J, et al. Cardiacresynchronization therapy with or without an implantable defibrillator in advanced chronic heart failure. 350:2140-50.
2005a. SCD-HeFT. Bardy GH, Lee KL, Mark DB, et al. Amiodarone or an implantable cardioverterdefibrillator for congestive heart failure. 352:225-37.
2005b. CARE-HF. Cleland JGF, Daubert J-C, Erdmann E, et al. The effect of cardiac
resynchronization on morbidity and mortality in heart failure. 352:1539-49.
2009. MADIT-CRT. Moss AJ, Hall WJ, Cannom DS, et al. Cardiac-resynchronization
therapy for the prevention of heart-failure events. 361:1329-38.
2010. RAFT. Tang ASL, Wells GA, Talajic M, et al. Cardiac-resynchronization therapy for mild-to-moderate heart failure. 363:2385-95.
2011a. EMPHASIS-HF. Zannad F, McMurray JJV, Krum H, et al. Eplerenone in patients with systolic heart failure and mild symptoms. 364:11-21.
2011b. ASCEND-HF. OConnor CM, Starling RC, Hernandez AF, et al. Effect of nesiritide in patients with acute decompensated heart failure. 365:32-43.
2014a. MADIT-CRT follow-up. Goldenberg I, Kutyifa V, Klein HU, et al. Survival
with cardiac-resynchronization therapy in mild heart failure. 370:1694-701.
2014b. PARADIGM-HF. McMurray JJV, Packer M, Desai AS, et al. Angiotensin
neprilysin inhibition versus enalapril in heart failure. DOI: 10.1056/
NEJMoa1409077.
An older class of inotropic
agents, the cardiac glycosides,
also met with disappointment.
Since the classic observations of
990
William Withering, recorded 230
years ago in his extraordinary document, An Account of the Foxglove, and
Some of Its Medical Uses: With Practical
Remarks on Dropsy, and Other Diseases,
digitalis glycosides were a mainstay of therapy for heart failure.
However, a trial published in the
Journal (Digitalis Investigation
Group, DIG, 1997) showed unequivocally that digoxin had no
beneficial effect on mortality in
heart failure, though it did reduce overall hospitalizations and
specifically reduced hospitalizations for heart failure by 28%.
Despite their long history, cardiac glycosides are no longer firstline therapy for heart failure,
though they may be used to mitigate symptoms and prevent hospitalizations for heart failure.
The story of nesiritide, a recombinant B-type natriuretic peptide with vasodilator properties,
reinforces the fundamental importance of evidence-based practice. Nesiritide was approved for
use in acute heart failure in 2001
to improve dyspnea. Given by infusion, the drug was administered
at many outpatient centers established specifically for this purpose. However, the ASCEND-HF
trial (2011b) demonstrated no benefit of nesiritide on the coprimary end point of death or rehospitalization for heart failure and no
significant improvement in dyspnea. Thus, an interesting and
widely used biologic agent proved
to be ineffective when subjected
to a rigorous clinical trial.
The introduction of cardiac
devices represents perhaps the
most fundamental paradigm
shift exhibited on the timeline.
Not appearing on the timeline
until 2001, device trials nevertheless appear more frequently than
trials of any single class of medical therapy. The timeline includes
three types of cardiac devices:
the left ventricular assist device
(LVAD) in REMATCH (2001b), the
implantable cardioverter-defibril-
n engl j med 371;11nejm.orgseptember 11, 2014
The New England Journal of Medicine
Downloaded from nejm.org on September 10, 2014. For personal use only. No other uses without permission.
Copyright 2014 Massachusetts Medical Society. All rights reserved.
PE R S PE C T IV E
Paradigm Shifts in Heart-Failure Therapy
lator (ICD) in SCD-HeFT (2005a),
and cardiac resynchronization
therapy (biventricular pacemakers, CRT) in COMPANION (2004),
CARE-HF (2005b), MADIT-CRT
(2009), and RAFT (2010). All
three types of devices have been
shown to reduce mortality in
heart failure. LVADs may be used
as a bridge to cardiac transplantation or, in some patients, as
destination therapy. ICDs may be
used alone or together with CRT
(CRT-D). A recent follow-up study
of the MADIT-CRT trial (2014a)
demonstrated that as compared
with ICD alone, CRT-D reduced
mortality among patients with
heart failure and mild symptoms,
but only when the QRS complex
was greater than 130 msec with a
left bundle-branch block pattern.
The final entry in the timeline
is the PARADIGM-HF trial (2014b),
now published in the Journal. The
study showed that a novel approach to heart-failure therapy,
A video is
available at
NEJM.org
angiotensin-receptor and neprilysin inhibition with LCZ696, a
combination of sacubitril and valsartan, reduced cardiovascular
mortality by 20% and overall mortality by 16%, as compared with
enalapril. Neprilysin is a neutral
endopeptidase involved in the metabolism of a number of vasoactive peptides. The inhibitor blocks
the action of neprilysin, resulting
in higher levels of peptides such
as natriuretic peptides, which have
vasodilator properties, facilitate
sodium excretion, and most likely have effects on remodeling.
The timeline reveals steady
progress, punctuated by paradigm
shifts, in the treatment of heart
failure over the past 28 years. At
the timelines beginning, two
drugs with no mortality benefit
digoxin and diuretics represented first-line treatment for
heart failure. By the timelines
last entry, ACE inhibitors, betablockers, aldosterone antagonists,
cardiac devices, and now angiotensin-receptorneprilysin inhibitors have strong evidence bases
demonstrating a reduction in mortality. Still, in the intervention arm
of PARADIGM-HF, the mortality
rate among patients with heart
failure remains about 20% over
2 years, highlighting the reality
that this newest entry hardly
concludes the compelling story of
heart-failure treatment. We anticipate that progress will continue,
and we hope that a timeline
crafted three decades from now
will reveal novel therapies and
new paradigms that push our understanding of heart failure to a
level unimaginable today.
Disclosure forms provided by the authors are available with the full text of this
article at NEJM.org.
This article was published on September 3,
2014, at NEJM.org.
DOI: 10.1056/NEJMp1410241
Copyright 2014 Massachusetts Medical Society.
Perspective Roundtable:
PARADIGM-HF The Experts
Discussion
Leading cardiologists discuss PARADIGM-HF, a trial of angiotensin
neprilysin inhibition versus enalapril in advanced heart failure.
n engl j med 371;11nejm.orgseptember 11, 2014
The New England Journal of Medicine
Downloaded from nejm.org on September 10, 2014. For personal use only. No other uses without permission.
Copyright 2014 Massachusetts Medical Society. All rights reserved.
991
S-ar putea să vă placă și
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
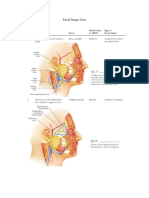
- Facial Danger ZoneDocument4 paginiFacial Danger ZoneMizanMaulanaÎncă nu există evaluări
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- Asidosis Laktat 2Document10 paginiAsidosis Laktat 2MizanMaulanaÎncă nu există evaluări
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- Sub LO Sken 2Document1 paginăSub LO Sken 2MizanMaulanaÎncă nu există evaluări
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (895)
- Facial Danger ZoneDocument4 paginiFacial Danger ZoneMizanMaulanaÎncă nu există evaluări
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (400)
- Ryan2018 Prevention of Otic Barotrauma of AviationDocument11 paginiRyan2018 Prevention of Otic Barotrauma of AviationMizanMaulanaÎncă nu există evaluări
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- MDG 2015 Rev (July 1)Document75 paginiMDG 2015 Rev (July 1)yensyÎncă nu există evaluări
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Humphrey 2017Document22 paginiHumphrey 2017MizanMaulanaÎncă nu există evaluări
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- Malaria OsteoclastDocument22 paginiMalaria OsteoclastMizanMaulanaÎncă nu există evaluări
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (588)
- Amblyomma Testudinarium A Rare Foreign Bodies in The Ear That Needs To Be Alerted in Agricultural CountriesDocument3 paginiAmblyomma Testudinarium A Rare Foreign Bodies in The Ear That Needs To Be Alerted in Agricultural CountriesMizanMaulanaÎncă nu există evaluări
- Sanchez2016 Clear Cell CA PenisDocument6 paginiSanchez2016 Clear Cell CA PenisMizanMaulanaÎncă nu există evaluări
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- Ca PenisDocument9 paginiCa PenisMizanMaulanaÎncă nu există evaluări
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (74)
- Facial Danger ZoneDocument4 paginiFacial Danger ZoneMizanMaulana100% (1)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- Duchenne CareConsiderations 2018 Part1Document17 paginiDuchenne CareConsiderations 2018 Part1MizanMaulanaÎncă nu există evaluări
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (266)
- Child Tick ParalysisDocument4 paginiChild Tick ParalysisMizanMaulanaÎncă nu există evaluări
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- AsmaDocument12 paginiAsmasiska_marsiskaÎncă nu există evaluări
- Jurnal Skripsi Anestesi 4Document8 paginiJurnal Skripsi Anestesi 4Tiara Anggun NurartoÎncă nu există evaluări
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (121)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)