Documente Academic
Documente Profesional
Documente Cultură
ACLS Pocket Card
Încărcat de
no_spam_mangDescriere originală:
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
ACLS Pocket Card
Încărcat de
no_spam_mangDrepturi de autor:
Formate disponibile
i
AMERICAN
ASSOCIATION
OJ CRITICAL-CARE
NURSES
American
Doses/Details for the Cardiac Arrest Algorithms
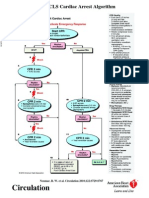
l Cardiac Arrest Algorithm
.r
Heart
Association..
ACLS
Cardia c Arrest,
A rrhythmias, and
T heir Treatment
ardiac Arrest Circular Algorithm
Shout for Help/Activate Emergency Response
Start CPR
Give oxygen
o Attach monitor/ defibrillator
o
2 minutes
CPR Quality
Push hard (;;,2 inches [5 em]) and
fast (;;,100/min) and allow complete
chest recoil
Minimize interruptions in
compressions
Avoid excessive ventilation
Rotate compressor every
2 minutes
If no advanced airway, 30:2
compression-ventilation ratio
Quantitative waveform
capnography
- If PETC02 <10 mm Hg, attempt
to improve CPR quality
Intra-arterial pressure
- If relaxation phase (diastolic)
pressure <20 mm Hg, attempt
to improve CPR quality
Return of Spontaneous
Circulation (ROSC)
Pulse and blood pressure
Abrupt sustained increase
in PETC0 2 (typically ;;,40 mm Hg)
Spontaneous arterial pressure
waves with intra-arterial
monitoring
Drug Therapy
IV/10 access
Epinephrine every 3-5 minutes
A miodarone for refractory VFNT
Shock Energy
Biphasic: Manufacturer
recommendation (eg, initial
dose of 120-200 J); if unknown ,
use maximum avai lable.
Second and subsequent doses
should be eqUiva en_, and higher
doses may be considered .
Monopl!_asic: 3.9 J
Consider Advanced Airway
Quantit ative waveform capno grap hy
Shout for Help/ Activate Emergency Response
Drug Therapy
Epinephrine IV/10 Dose:
1 mg every 3-5 minutes
Vasopressin IV/10 Dose:
40 units can replace first or
second dose of epinephrine
Rhythm shockable?
Amiodarone IV/10 Dose:
First dose: 300 mg bolus.
Second dose: 150 mg .
Advanced Airway
Supraglottic advanced airway
or endotracheal intubation
Waveform capnography to confirm
and monitor ET tube placement
8-1 0 breaths per minute with
continuous chest compressions
Reversible Causes
- Hypovolemia
- Hypoxia
- Hydrogen ion (acidosis)
- Hypo-/ hyperkalemia
- Hypot hermia
- Tension pneumothorax
- Tamponade, cardiac
- Toxins
- Thrombosis, pu lmonary
- Th rombosis, coronary
No
No
11
C PR 2 min
Treat reversible causes
12 r-_________ L_ _ _ _ _ __
If no signs of return of
spontaneous circulation
90-1012 (1 of 2)
ISBN 978-1-61669-01 3-7
5/11
C 2011 American Heart Association
Printed In the USA
(ROSC), go to 10 or 11
If ROSC , go t o
Post-Cardiac Arrest Care
Go to 5 or 7
mmediate Post-Cardiac Arrest Care Algorithm
Bradycardia With a Pulse Algorithm
Assess appropriateness for c linical condition.
Heart rate typically <50/min if bradyarrhythmia.
Return of Spontaneous Circulation (ROSC)
Tachycardia With a Pulse Algorithm
Assess appropriateness for clinical condition.
Heart rate typically ~ 150/min if tachyarrhythmia.
Optim ize ventilation and oxygenation
Maintain patent airway; assist breathing as necessary
Oxygen {if hypoxemic)
Cardiac monitor to identify rhythm ; monitor blood
pressure and oximetry
IV access
12-Lead EGG if available; don 't delay therapy
Doses/Details
Ventilation/ Oxygenation
Avoid excessive ventilation .
Start at 10-12 breaths/min
and titrate to target PETC02
of 35-40 mm Hg.
When feasible, titrate F102
to minimum necessary to
achieve Spe, ~94%.
Treat hypotension
(SBP <90 mm Hg)
IV/10 bolus
Vasopressor infusion
Consider treatable
causes
12-Lead EGG
IV Bolus
1-2 L normal saline
or lactated Ringer's.
If inducing hypothermia,
may use 4c fluid .
Epinephrine IV Infusion:
0.1-0.5 meg/kg per minute
(in 70-kg adult: 7-35 meg
per minute)
Norepinephrine
IV Infusion:
0.1-0.5 meg/kg per minute
On 70-kg adult: 7-35 meg
per minute)
STEM I
OR
high suspicion
of AMI
No
Reversible Causes
- Hypovolemia
- Hypoxia
- Hydrogen ion (acidosis)
- Hypo-/hyperkalemia
- Hypothermia
- Tension pneumothorax
- Tamponade, cardiac
- Toxins
- Thrombosis, pulmonary
- Thrombosis, coronary
Maintain patent airway; assist breathing
as necessary
Oxygen (if hypoxemic)
Cardiac monitor to identify rhythm;
monitor blood pressure and oximetry
Persistent
tachyarrhythmia
causing:
Persistent bradyarrhythmia
causing:
Monitor
and
observe
Hypotension?
Acutely altered
mental status?
Signs of shock?
Ischemic chest
discomfort?
Acute heart
failure?
Hypotension?
Acutely altered mental status?
Signs of shock?
Ischemic chest discomfort?
Acute heart failure?
Yes
;---+
Synchronized
cardioversion
Consider sedation
If regular narrow
complex, consider
adenosine
No
Dopamine IV Infusion:
5-1 0 meg/kg per minute
Advanced critical care
Identify and treat underlying cause
Identify and treat underlying cause
Maintain oxygen saturation ~94 %
Consider advanced airway and
waveform capnography
Do not hyperventilate
Doses/Details
Atropine
If atropine ineffective:
Transcutaneous pacing
OR
Dopamine infusion
OR
Epinephrine infusion
Consider:
Expert consultation
Transvenous pacing
Atropine IV Dose:
First dose:
0.5 mg bolus
Repeat every
3-5 minutes
Maximum: 3 mg
Dopamine
IV Infusion:
2-1 0 meg/kg per
minute
Epinephrine
IV Infusion:
2-1 0 m9 pe
mm te
WideQRS?
:?:0.12 second
)
J
Yes
No
IV access and 12-lead EGG
if available
Vagal maneuvers
Adenosine (if regular)
~ - Blocker or calcium
channel blocker
Consider expert consultation
IV access and
12-lead EGG
if available
Consider
adenosine only
if regular and
monomorphic
Consider
antiarrhythmic
infusion
Consider expert
consultation
Doses/Details
Synchronized
Cardioversion
Initial recommended doses:
Narrow regular: 50-1 00 J
Narrow irregular:
120-200 J biphasic or
200 J monophasic
Wide regular: 100 J
Wide irregular:
defibrillation dose
(NOT synchronized)
Adenosine IV Dose:
First dose: 6 mg rapid IV push;
follow with NS flush.
Second dose: 12 mg
if required.
Antiarrhythmic Infusions
for Stable Wide-QRS
Tachycardia
Procainamide IV Dose:
20-50 mg/min until
arrhythmia suppressed,
hypotension ensues, ORS
duration increases >50%, or
maximum dose 17 mglkg
given. Maintenance infusion:
1-4 mg/min. Avoid ~ prolonged
QTorCHF.
Amiodarone IV Dose:
First dose: 150 mg over
10 minutes. Repeat as
needed if VT recurs. Follow
by maintenance infusion of
1 mg/min tor first 6 hours.
Sotalol IV Dose:
100 mg (1.5 mglkg)
over 5 minutes. Avoid if
prolonged QT.
A m erican
Heart
Asso ciat ion.
Acute Coronary Syndromes Algorithm (continued)
AMERICAN
..r
ASSOCIATION
~ CRmCAL-CARE
NURSES
ACLS
Acute Coronary
Syndromes and Stroke
ST elevation or new or
presumably new LBBB;
strongly suspicious
for injury
ST-elevation Ml (STEMI)
Normal or
nondiagnostic changes
in ST segment
orTwave
low-/intermediate-nsk
ACS
ST depression or dynamic
T-wave inversion; strongly
suspicious for ischemia
H1gh-risk unstable ang1na/
non-ST-elevation Ml
(UAINSTEMI)
Acute Coronary Syndromes Algorithm
Symptoms suggestive of ischemia or infarction
Start adjunctive
therapies as 1nd1cated
Do not delay
reperfusion
EMS assessment and care and hospital preparation
Monttor, support ABCs. Be prepared to provtde CPR and defibrillation
Administer asptnn and consider oxygen, nitroglycerin, and morphine tf needed
Obtatn 12-lead ECG; tf ST elevation:
- Nottfy recetvtng hospital wtth transmtssion or Interpretation; note time of
onset and first medical contact
Nottfied hospttal should mobilize hospital resources to respond to STEMI
If considenng prehospttal fibnnolys1s, use fibrinolytic checklist
Concurrent ED assessment (<10 minutes)
Check vttal signs; evaluate oxygen
saturation
Establish IV access
Perform brief, targeted history,
physical exam
Rev1ew/complete fibrinolytiC checklist;
check contratndications
Obtain 1n1t1al card1ac marker levels,
inttial electrolyte and coagulation studies
Obtain portable chest x-ray (<30 min)
Immediate ED general treatment
If 0 sat <94%, start oxygen at
4 Um1n, titrate
Aspirin 160 to 325 mg
(if not given by EMS)
Nitroglycerin sublingual or spray
Morphine IV 1f discomfort not
relieved by nitroglycenn
ECG interpretation
90-1012 (2 of 2)
ISBN 978-1-61669-013-7
5/11
C 2011 American Heart Association
Printed In the USA
Time from
onset of
symptoms
S12 hours?
>1 2
hours
Troponin elevated or
high-risk patient
Cons1der early 1nvas1ve
strategy if:
Refractory ischemic
chest dtscomfort
RecurrenVpersistent
ST deviation
Ventricular
tachycardia
Hemodynamic
Instability
Signs of heart failure
Consider admission
to ED chest pain unit
or to appropriate bed
and follow:
Serial cardiac markers
(including tropon1n)
Repeat EGG/continuous
ST-segment monitoring
Cons1der noninvasive
diagnostic test
S12 hours
Start adjunctive
treatments as indicated
Nitroglycenn
Heparin (UFH or LMWH)
Cons1der: PO 13-blockers
Consider: Clopidogrel
Cons1der: Glycoprotetn
lib/lila inhibitor
Reperfusion goals:
Therapy defined by
patient and center
cnteria
Door-to-balloon
inflation (PCI) goal
of 90 minutes
Door-to-needle
(fibrinolysis) goal
of 30 minutes
....___
Yes
Develops 1 or more:
Clinical high-risk
features
Dynamic ECG
changes
consistent with
ischemia
Troponin elevated
No
Abnormal
Admit to monitored bed
Assess risk status
Continue ASA, heparin,
and other therapies as
indicated
ACE inhibitor/ARB
HMG CoA reductase
inhibitor (stalin therapy)
Not at high risk:
cardiology to nsk strat1fy
Yes
diagnostic
noninvasive
imaging or
physiologic
testing?
No
If no evidence
of ischemia or
infarction by
testing, can
discharge with
follow-up
Step 1
Has patient experienced chest discomfort for
greater than 15 minutes and less than 12 hours?
Contraindications for fibrinolytic use in STEMI consistent with ACCIAHA
2007 Focused Update
Absolute Contraindication&
Any prior intracranial hemorrhage
Does ECG show STEMI or new or
presumably new LBBB?
Known structural cerebral vascular lesion (eg, arteriovenous
malformation)
Known malignant intracranial neoplasm (primary or metastatic)
Ischemic stroke within 3 months EXCEPT acute ischemic stroke
within 3 hours
Are there contraindications to fibrinolysis?
Step2
Suspected aortic dissection
If ANY one of the following is checked YES,
fibrinolysis MAY be contraindicated.
Systolic BP > 180 to 200 mm Hg or diastolic BP > 100 to
110mm Hg
Right vs left arm systolic BP difference > 15 mm Hg
History of structural central nervous system disease
Significant closed head/facial trauma within the
previous 3 weeks
Stroke >3 hours or <3 months
Rebent (within 2-4 weeks) major trauma, surgery
(including laser eye surgery), GI/GU bleed
Any history of intracranial hemorrhage
Bleeding, clotting problem, or blood thinners
Pregnant female
Serious systemic disease (eg, advanced cancer,
severe liver or kidney disease)
Active bleeding or bleeding diathesis (excluding menses)
Significant closed head trauma or facial trauma within 3 months
) YES
) YES
) YES
) NO
) NO
) NO
) YES
) YES
) NO
) NO
)
)
)
)
)
)
"J
:>
YES
YES
YES
YES
) YES
NO
NO
NO
NO
) NO
Severe uncontrolled hypertension on presentation
(SSP > 180 mm Hg or DBP > 11 0 mm Hg)t
History of prior ischemic stroke >3 months, dementia, or known
intracranial pathology not covered in contraindications
Traumatic or prolonged (> 10 minutes) CPR or major surgery
(<3 weeks)
Recent (within 2 to 4 weeks) internal bleeding
For streptokinase/anistreplase: prior exposure (>5 days ago) or
prior allergic reaction to these agents
If ANY one of the following is checked YES,
consider transfer to PCI facility.
Heart rate ~ 1 00/min AND systolic BP <1 00 mm Hg
Pulmonary edema (rales)
Signs of shock (cool, clammy)
Contraindications to fibrinolytic therapy
Required CPR
History of chronic, severe, poorly controlled hypertension
Noncompressible vascular punctures
Is patient at high risk?
Step3
Relative Contraindication&
.) YES
) YES
) YES
J vest
) YES
Pregnancy
)
.)
)
)
)
NO
NO
NO
NO
NO
'Contra1ndications for fibrinolytiC use 1n STEM I cons1stent w1th "ThrombolytiC Therapy and Balloon
Angioplasty 1n Acute ST Elevation Myocard1allnfarction (STEMI)" at Agency for Healthcare Research
and Quality National Gu1dehne Clearinghouse (www.Guidel1nes.gov).
tCons1der transport to pnmary PCI fac1hty as destination hosprtal.
Active peptic ulcer
Current use of anticoagulants: the higher the INA, the higher the
risk of bleeding
'Viewed as advisory for clinical decision making and may not be all-inclusive or definitive.
tCould be an absolute contraindication in low-risk patients with myocardial infarction.
I Stroke Assessment
Suspected Stroke Algorithm:
Goals for Management of Stroke
Identify signs and symptoms of possible stroke
Activate Emergency Response
The Cincinnati Prehospital Stroke Scale
Facial Droop (have patient show teeth or smile):
Critical EMS assessments and actions
NINDS
TIME
GOALS
ED
Arrival
10
mm
ED
Support ABCs; g1ve oxygen If needed
Perform prehospltal stroke assessment
Establish t1me of symptom onset (last normaQ
Tnage to stroke center
Alert hospital
Check glucose if possible
Normal- both sides of
face move equally
Abnormal-one side of
face does not move
as well as the other side
Immediate general assessment and stabilization
Assess ABCs, v1tal stgns
Prov1de oxygen 1f hypoxemic
Obtam IV access and perform
laboratory assessments
Check glucose: treat if indiCated
Perform neurologic screenirtg
assessment
Activate stroke team
Order emergent CT or MAl of bram
Obtaln 12-lead ECG
Left: Normal. Right: Stroke patient
with facial droop (right side of face).
t
Immediate neurologic assessment by stroke team or designee
Review patient history
Establish time of symptom onset or last known normal
Perform neurologic examination (NIH Stroke Scale or
Canadian Neurological Scale)
25 mm
ED
Arrival
(Does CT
t
8CM1 show
t
Probable acute ischemic stroke;
c onsider fibrinolytic therapy
Arm Drift (patient closes eyes and extends both arms straight out,
with palms up, for 10 seconds):
r-------------~
hemontlage?}
No HemorTh1111e
t
(
Patient retnlllnS CMKI#dafe
for flbrlnolytJc tltwapy?
Candidate
Review risks/benefits with patient
and family. If acceptable:
Stroke
Admission
3 hours
G1ve rtPA
No anticoagulants or anllpiatelet
treatment for 24 hours
t
Beg1n post-rtPA stroke pathway
Aggressively mon1tor.
- BP per protocol
- For neurologiC detenoration
Emergent admission to stroke un1t
or Intensive care un1t
Normal- both arms move
the same or both arms do
not move at all (other findings,
such as pronator drift, may
be helpful)
Abnormal-one arm does
not move or one arm drifts
down compared with the
other
HemorTh1111e
t
Consult neurolog1st or neurosurgeon:
conSider transfer if not available
Check for fibnnolytic exclusions
Repeat neurolog1c exam: are defic1ts
rapidly improving to normal?
ED
Arrival
60 min
Not a
Candidate
Left: Normal. Right: One-sided
motor weakness (right arm).
: Administer aspirin
Beg1n stroke or
hemorTtlage pathway
Admit to stroke un1t or
lntens1ve care un1t
Abnormal Speech (have the patient say "you can't teach an old dog
new tricks"):
e
Normal-patient uses correct words with no slurring
Abnormal-patient slurs words, uses the wrong words, or is unable
to speak
Interpretation: If any 1 of these 3 signs is abnormal, the probability of a
stroke is 72%.
Modrfoed from Kothari AU. PanciOir A, Uu T, Brott T, Broderick J. Crncinnati Prehosprtal Stroke Scale: reproducobthty and
vahdoty. Ann Emerg Mad. 1999;33:373-378. W~h permission from 8sevrer.
Patients Who Could Be Treated With rtPA Within 3 Hours
From Symptom Onset*
Inclusion Criteria
Diagnosis of ischemic stroke causing measurable neurologic deficit
Onset of symptoms <3 hours before beginning treatment
Age ~18 years
Exclusion Criteria
Head trauma or prior stroke in previous 3 months
Symptoms suggest subarachnoid hemorrhage
Arterial puncture at noncompressible site in previous 7 days
History of previous intracranial hemorrhage
Elevated blood pressure (systolic >185 mm Hg or diastolic >11 0 mm Hg)
Evidence of active bleeding on examination
Acute bleeding diathesis, including but not limited to
- Platelet count <100 OOO/mm3
- Heparin received within 48 hours, resulting in aPTT >upper limit of normal
- Current use of anticoagulant with INA >1.7 or PT > 15 seconds
Blood glucose concentration <50 mg/dl (2. 7 mmoVL)
CT demonstrates multilobar infarction (hypodensity > 1/3 cerebral hemisphere)
Relative Exclusion Criteria
Recent experience suggests that under some circumstances-with careful
consideration and weighing of risk to benefit-patients may receive fibrinolytic
therapy despite 1 or more relative contraindications. Consider risk to benefit of rtPA
administration carefully if any one of these relative contraindications is present:
Only minor or rapidly improving stroke symptoms (clearing spontaneously)
Seizure at onset with postictal residual neurologic impairments
Major surgery or serious trauma within previous 14 days
Recent gastrointestinal or urinary tract hemorrhage (within previous 21 days)
Recent acute myocardial infarction (within previous 3 months)
Patients Who Could Be Treated With rtPA From 3 to 4.5 Hours
From Symptom Onsett
Potential Approaches to Arterial Hypertension in
Acute Ischemic Stroke Patients Who Are Potential Candidates
for Acute Reperfusion Therapy*
Patient otherwise eligible for acute reperfusion therapy except that blood pressure
is >185/ 110 mm Hg:
Labetalol 10-20 mg IV over 1-2 minutes, may repeat x 1, or
Nicardipine IV 5 mg per hour, titrate up by 2.5 mg per hour every 5-15 minutes,
maximum 15 mg per hour; when desired blood pressure is reached, lower to
3 mg per hour, or
Other agents (hydralazine, enalaprilat, etc) may be considered when appropriate
If blood pressure is not maintained at or below 185/11 0 mm Hg, do not administer rtPA.
Management of blood pressure during and after rtPA or other acute reperfusion
therapy:
Monitor blood pressure every 15 minutes for 2 hours from the start of rtPA
therapy, then every 30 minutes for 6 hours, and then every hour for 16 hours.
If systolic blood pressure 180-230 mm Hg or diastolic blood pressure
105- 120 mm Hg:
Labetalol 10 mg IV followed by continuous IV infusion 2-8 mg per minute, or
Nicardipine IV 5 mg per hour, titrate up to desired effect by 2.5 mg per hour
every 5-15 minutes, maximum 15 mg per hour
If blood pressure not controlled or diastolic blood pressure > 140 mm Hg, consider
sodium nitroprusside.
Approach to Arterial Hypertension In Acute Ischemic Stroke
Patients Who Are Not Potential Candidates for Acute
Reperfusion Therapy*
Inclusion Criteria
Diagnosis of ischemic stroke causing measurable neurologic deficit
Onset of symptoms 3 to 4.5 hours before beginning treatment
Exclusion Criteria
Age >80 years
Severe stroke (NIHSS >25)
Taking an oral anticoagulant regardless of INA
History of both diabetes and prior ischemic stroke
Notes
Consider blood pressure reduction as indicated for other concomitant organ
system injury:
The checklist includes some US FDA-approved indications and contraindications for administratiOO
A reasonable target is to lower blood pressure by 15% to 25% within the first day.
of rtPA for acute ischemic stroke. Recent AHNASA guideline revisions may differ slightly from
FDA criteria. A physician with expertise in acute stroke care may modify this list.
Onset t ime is either witnessed or last known normal.
In patients without recent use of oral anticoagulants or heparin, treatment with rtPA can be
initiated before availability of coagulation study results but should be discontinued if INA 1s
> 1.7 or PT is elevated by local laboratory standards.
In patients without history of thrombocytopenia, treatment with rtPA can be init iated before
availability of platelet count but should be discontinued if platelet count is <100 000/mm.
Abbreviations: aPTT, activated partial thromboplastin time; FDA, Food and Drug Administration;
INA, international normalized ratio; NIHSS, Nat1onal Institutes of Health Stroke Scale; PT,
prothrombin time; rtPA, recombinant tissue plasminogen activator.
Consider lowering blood pressure in patients with acute ischemic stroke if systolic
blood pressure >220 mm Hg or diastolic blood pressure > 120 mm Hg.
Acute myocardial infarction
Congestive heart failure
Acute aortic dissection
'Adams HP Jr, del Zoppo G, Alberts MJ, Bhatt DL, Brass L, Fur1an A, Grubb RL, H1gashlda AT, Jauch EC,
Kidwell C, Lyden PO, Morgenstern LB, Qureshi AI, Rosenwasser RH. Scott PA, W1J(i1Cks EFM. Gu1delines
for the ear1y management of adults w1th ischermc stroke: a guldel1ne from the Amencan Heart Association/
Amencan Stroke Association Stroke Council, Clinical Cardiology Council, Cardiovascular Radiology and
Intervention Council, and the Atherosclerotic Peripheral Vascular Disease and Quality of Care Outcomes in
Research Interdisciplinary Working Groups. Stroke. 2007;38:1655-1711 .
tdel Zoppo GJ, Saver JL, Jauch EC, Adams HP Jr; on behalf of the AmeriCan Heart Association Stroke
Council. Expansion of the t1me w1rldow for treatment of acute 1schemic stroke w1th Intravenous t1ssue
plasm~nogen actiVator: a science advisory from the Amencan Heart Associat10n/Amencan Stroke Associat1011
Sttoke. 2009;40:2945-2948.
S-ar putea să vă placă și
- Advance Cardiac Life Support: Short, Sweet and to the PointDe la EverandAdvance Cardiac Life Support: Short, Sweet and to the PointEvaluare: 3 din 5 stele3/5 (2)
- Acls Cheat Sheet PDFDocument3 paginiAcls Cheat Sheet PDFDarren Dawkins100% (4)
- ACLS Advanced Cardiovascular Life Support Provider Manual 2023De la EverandACLS Advanced Cardiovascular Life Support Provider Manual 2023Încă nu există evaluări
- Basic Life Support (BLS) and Advanced Cardiovascular Life Support (ACLS)Document35 paginiBasic Life Support (BLS) and Advanced Cardiovascular Life Support (ACLS)rajÎncă nu există evaluări
- ACLS Cheat SheetDocument8 paginiACLS Cheat SheetLenTheRN85% (27)
- ACLS PharmacologyDocument6 paginiACLS PharmacologyEunice Angela Fulgueras80% (5)
- ACLS Rhythms Practice Test 2020 Recognition Rhythm Strips (PDF)Document11 paginiACLS Rhythms Practice Test 2020 Recognition Rhythm Strips (PDF)김민길100% (2)
- Advanced Cardiac Life Support Quick Study Guide 2015 Updated GuidelinesDe la EverandAdvanced Cardiac Life Support Quick Study Guide 2015 Updated GuidelinesEvaluare: 4 din 5 stele4/5 (6)
- ACLS Rhythms Cheat SheetDocument21 paginiACLS Rhythms Cheat SheetShannon Hagan Wilson100% (8)
- EKG and ECG Interpretation: Learn EKG Interpretation, Rhythms, and Arrhythmia Fast!De la EverandEKG and ECG Interpretation: Learn EKG Interpretation, Rhythms, and Arrhythmia Fast!Încă nu există evaluări
- Study Guide: MandatoryDocument24 paginiStudy Guide: Mandatorybooksir86% (7)
- Acls Pre Course Self Assessment Study GuideDocument7 paginiAcls Pre Course Self Assessment Study Guidenova939100% (5)
- Pediatric Advanced Life Support Quick Study Guide 2015 Updated GuidelinesDe la EverandPediatric Advanced Life Support Quick Study Guide 2015 Updated GuidelinesEvaluare: 5 din 5 stele5/5 (2)
- AHA ACLS Megacode ScenariosDocument6 paginiAHA ACLS Megacode ScenariosChad Sanford78% (18)
- Cardiac Arrhythmia Recognition: an easy learning guideDe la EverandCardiac Arrhythmia Recognition: an easy learning guideÎncă nu există evaluări
- PALS Pamphlet Edited PDFDocument4 paginiPALS Pamphlet Edited PDFsaleem50% (4)
- Haemodynamic Monitoring & Manipulation: an easy learning guideDe la EverandHaemodynamic Monitoring & Manipulation: an easy learning guideÎncă nu există evaluări
- 2021 ACLS Study GuideDocument20 pagini2021 ACLS Study GuideShane Brown83% (12)
- ACLS PrecourseAssessmentDocument19 paginiACLS PrecourseAssessmentBrigitte Elaine81% (21)
- The Art of the Iv Start: Common Techniques and Tricks of the Trade for Establishing Successful Peripheral Intravenous LinesDe la EverandThe Art of the Iv Start: Common Techniques and Tricks of the Trade for Establishing Successful Peripheral Intravenous LinesÎncă nu există evaluări
- ACLS Rhythms Cheat SheetDocument21 paginiACLS Rhythms Cheat SheetSisca MetasariÎncă nu există evaluări
- The 12-Lead Electrocardiogram for Nurses and Allied ProfessionalsDe la EverandThe 12-Lead Electrocardiogram for Nurses and Allied ProfessionalsÎncă nu există evaluări
- ACLS DrugsDocument16 paginiACLS Drugstostc100% (2)
- ACLS Pretest Questions and Answers 2020 (Full Practice Test)Document23 paginiACLS Pretest Questions and Answers 2020 (Full Practice Test)김민길50% (4)
- Bonehead Electrocardiography: The Easiest and Best Way to Learn How to Read Electrocardiograms—No Bones About It!De la EverandBonehead Electrocardiography: The Easiest and Best Way to Learn How to Read Electrocardiograms—No Bones About It!Evaluare: 5 din 5 stele5/5 (2)
- Acls - Megacode - UpdatedDocument4 paginiAcls - Megacode - UpdatedDivine Dela Pena100% (1)
- Ccrn Certification Examination Practice Questions and Answers with Rationale: First EditionDe la EverandCcrn Certification Examination Practice Questions and Answers with Rationale: First EditionEvaluare: 5 din 5 stele5/5 (1)
- BLS Acls Aha 2020Document103 paginiBLS Acls Aha 2020Nicholas PetrovskiÎncă nu există evaluări
- American Heart Association: Precourse Written Examination May 2001Document10 paginiAmerican Heart Association: Precourse Written Examination May 2001Ericka SwordÎncă nu există evaluări
- ECG TipsDocument7 paginiECG TipsMar Kristian Vero Lumen100% (1)
- ACLS Review TestDocument5 paginiACLS Review Testtostc60% (5)
- ACLS Precourse Test AnswersDocument60 paginiACLS Precourse Test AnswersTip Piraya60% (5)
- ACLS Test BankDocument13 paginiACLS Test BankSofiaSheikh94% (51)
- 2016 Updated ACLS HandoutsDocument24 pagini2016 Updated ACLS Handoutskarenjlazarus86% (14)
- ACLS Exam ADocument8 paginiACLS Exam AAgil Rumboko Sumitro100% (3)
- ACLS Answer KeyDocument23 paginiACLS Answer KeyKirana Budhiarta94% (17)
- ACLS Pretest Exam AnnotatedDocument21 paginiACLS Pretest Exam AnnotatedMOLLYÎncă nu există evaluări
- ACLS Provider Manual 2015 NotesDocument5 paginiACLS Provider Manual 2015 Notescrystalshe93% (14)
- ACLS Algorithms 2020 (Advanced Cardiac Life Support)Document1 paginăACLS Algorithms 2020 (Advanced Cardiac Life Support)evelyn k100% (2)
- ACLS Exam ADocument8 paginiACLS Exam ASean Johnson83% (30)
- FREE 2022 ACLS Study Guide - ACLS Made Easy! PDFDocument18 paginiFREE 2022 ACLS Study Guide - ACLS Made Easy! PDFkumar23Încă nu există evaluări
- ACLS2Document7 paginiACLS2Jennifer Kaye L. DucaoÎncă nu există evaluări
- ACLS Study Guide NewDocument35 paginiACLS Study Guide NewNIRANJANA SHALINIÎncă nu există evaluări
- ACLS Memory AidsDocument2 paginiACLS Memory Aidsmaur_jmp78% (9)
- ACLSDocument17 paginiACLSms_lezah100% (4)
- ACLS AlgorithmsDocument4 paginiACLS Algorithmsmonickams100% (1)
- TestDocument11 paginiTestzenagit123456100% (1)
- ACLS Class Packet 2015Document9 paginiACLS Class Packet 2015Chi Wiin100% (3)
- ACLS Student GuideDocument28 paginiACLS Student GuideSamuel de Lima71% (7)
- AclsDocument20 paginiAclsqueennita69100% (4)
- Acls Algorithms 2021 ChecklistDocument1 paginăAcls Algorithms 2021 ChecklistpepÎncă nu există evaluări
- ACLS Manual Provider 2016Document207 paginiACLS Manual Provider 2016AhmedShareef100% (9)
- 2011 ACLS Pretest Annotated Answer KeyDocument19 pagini2011 ACLS Pretest Annotated Answer KeyMohammed Abdou92% (13)
- Congestive Heart Failure (PH 2 Bemdiji)Document1 paginăCongestive Heart Failure (PH 2 Bemdiji)api-285694335Încă nu există evaluări
- Endodontics in Systemically Compromised PatientsDocument30 paginiEndodontics in Systemically Compromised Patientscarolina pavezÎncă nu există evaluări
- Non Invasive VentilationDocument442 paginiNon Invasive Ventilationagnese valentiniÎncă nu există evaluări
- Bermton Academy: Ischemic Heart DiseaseDocument2 paginiBermton Academy: Ischemic Heart DiseaseGERARD NIÑO JUSAYANÎncă nu există evaluări
- Measurement of M Mode Echocardiographic Parameters in Healthy Adult Persian CatsDocument7 paginiMeasurement of M Mode Echocardiographic Parameters in Healthy Adult Persian CatsAna AldazÎncă nu există evaluări
- Drug Study 2Document8 paginiDrug Study 2rey_tengÎncă nu există evaluări
- Trismed - Cardiapia 400 406N 406P 406R 406RS 406NH 406PH 406RH 406RSH PDFDocument65 paginiTrismed - Cardiapia 400 406N 406P 406R 406RS 406NH 406PH 406RH 406RSH PDFDireccion Tecnica100% (2)
- 500 QuestionsDocument54 pagini500 QuestionsdprincebuchikoyÎncă nu există evaluări
- Acsms Resources For The Exercise Physiologist 2nd Edition Ebook PDFDocument61 paginiAcsms Resources For The Exercise Physiologist 2nd Edition Ebook PDFjames.keeter432100% (41)
- Shannon Hanchett Autopsy ReportDocument1 paginăShannon Hanchett Autopsy ReportOKCFOXÎncă nu există evaluări
- Test Bank For Ekg Plain and Simple 3rd Edition EllisDocument8 paginiTest Bank For Ekg Plain and Simple 3rd Edition Elliscanebrutalfniy66Încă nu există evaluări
- Kounis Syndrome A Pediatric PerspectiveDocument10 paginiKounis Syndrome A Pediatric PerspectiveAna Belén Artero CastañoÎncă nu există evaluări
- NST1501 Exam Ndou LDocument7 paginiNST1501 Exam Ndou Llufunondou12Încă nu există evaluări
- Oxygen Insufficiency.Document54 paginiOxygen Insufficiency.Josephine George JojoÎncă nu există evaluări
- Muscular TissueDocument6 paginiMuscular TissueChezkaMayC.OliverosÎncă nu există evaluări
- 1012 Vital SignsDocument46 pagini1012 Vital SignsZainescu DanÎncă nu există evaluări
- Declaration Good Health Form PDFDocument2 paginiDeclaration Good Health Form PDFMurali SiddarthÎncă nu există evaluări
- Physical Assessment of Preeclamptic PatientDocument3 paginiPhysical Assessment of Preeclamptic PatientAndreiÎncă nu există evaluări
- Combined Science PDFDocument57 paginiCombined Science PDFRadhika Meher58% (33)
- Aortic Regurgitation (Ar)Document18 paginiAortic Regurgitation (Ar)rameshbmc100% (1)
- Vagus NerveDocument7 paginiVagus NervePeter100% (1)
- Start CPR Shout For Help/Activate Emergency Response: Give Oxygen Attach Monitor/DefibrillatorDocument2 paginiStart CPR Shout For Help/Activate Emergency Response: Give Oxygen Attach Monitor/DefibrillatorFelicia ErikaÎncă nu există evaluări
- How The Body WorksDocument34 paginiHow The Body Worksapi-135186943Încă nu există evaluări
- DR - Tahir Mahmood (PT) IIIRS, SialkotDocument40 paginiDR - Tahir Mahmood (PT) IIIRS, SialkotRabia RaufÎncă nu există evaluări
- Acute Coronary SyndromeDocument1 paginăAcute Coronary SyndromeMike GÎncă nu există evaluări
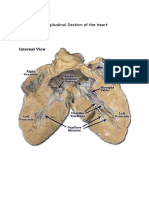
- Longitudinal Section of The HeartDocument2 paginiLongitudinal Section of The HeartkayannaÎncă nu există evaluări
- Physiological Indicators: Heart Rate Rate of Perceived Exertion PacingDocument29 paginiPhysiological Indicators: Heart Rate Rate of Perceived Exertion PacingAlyssa AlejandroÎncă nu există evaluări
- CABG x4Document2 paginiCABG x4Indranil SinhaÎncă nu există evaluări
- A Practical Handbook of Macroscopic Examination in PathologyDocument63 paginiA Practical Handbook of Macroscopic Examination in PathologyMariaÎncă nu există evaluări
- Paida Lajin Self-Healing EnglishDocument69 paginiPaida Lajin Self-Healing EnglishKarma Arnab100% (2)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)De la EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Evaluare: 3 din 5 stele3/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedDe la EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedEvaluare: 4.5 din 5 stele4.5/5 (82)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDDe la EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDEvaluare: 5 din 5 stele5/5 (3)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionDe la EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionEvaluare: 4 din 5 stele4/5 (404)
- The Age of Magical Overthinking: Notes on Modern IrrationalityDe la EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityEvaluare: 4 din 5 stele4/5 (32)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeDe la EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeEvaluare: 2 din 5 stele2/5 (1)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesDe la EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesEvaluare: 4.5 din 5 stele4.5/5 (1412)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsDe la EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsÎncă nu există evaluări
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsDe la EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsEvaluare: 4 din 5 stele4/5 (4)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsDe la EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsEvaluare: 5 din 5 stele5/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisDe la EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisEvaluare: 4.5 din 5 stele4.5/5 (42)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaDe la EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaEvaluare: 4.5 din 5 stele4.5/5 (266)
- The Obesity Code: Unlocking the Secrets of Weight LossDe la EverandThe Obesity Code: Unlocking the Secrets of Weight LossEvaluare: 4 din 5 stele4/5 (6)
- Why We Die: The New Science of Aging and the Quest for ImmortalityDe la EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityEvaluare: 4.5 din 5 stele4.5/5 (6)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisDe la EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisEvaluare: 3.5 din 5 stele3.5/5 (2)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeDe la EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeEvaluare: 4.5 din 5 stele4.5/5 (254)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.De la EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Evaluare: 4.5 din 5 stele4.5/5 (110)
- To Explain the World: The Discovery of Modern ScienceDe la EverandTo Explain the World: The Discovery of Modern ScienceEvaluare: 3.5 din 5 stele3.5/5 (51)
- Critical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsDe la EverandCritical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsEvaluare: 4.5 din 5 stele4.5/5 (39)