Documente Academic
Documente Profesional
Documente Cultură
ROOT COVERAGE WITH PERIOSTEUM PEDICLE GRAFT - A NOVEL APPROACH DR Vineet Vinayak
Încărcat de
Dr Vineet Vinayak0 evaluări0% au considerat acest document util (0 voturi)
109 vizualizări3 paginiABSTRACT : Aim : To cover root surface with periosteum pedicle graft. Methods : A patient with miller class I recession i.r.t 31, 32 and 33, with probing depth of 2.5mm and clinical attachment loss of 4mm i.r.t 31, 32 and 33 and class III gingival recession i.r.t 41 and 43 was treated using periosteum pedicle graft. 42 was missing. Periosteum was dissected and increased in length coronaly to cover the root surface. After stabilizing the periosteal graft with sutures, the epithelium was positioned over it and sutured. Result : Uneventful healing of the operated site was observed after 1 month. There was full coverage of the gingival recession with satisfactory results. There was an increase in morphologic and chromatic resemblance with the adjacent area. Conclusion : Periosteum can be successfully used for the treatment of multiple gingival recession defects. Key words : gingival recession, osteogenic properties, periosteum.
Dr VINEET VINAYAK | dr VINEET VINAYAK |
Titlu original
ROOT COVERAGE WITH PERIOSTEUM PEDICLE GRAFT – A NOVEL APPROACH ; Dr vineet vinayak
Drepturi de autor
© © All Rights Reserved
Formate disponibile
PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentABSTRACT : Aim : To cover root surface with periosteum pedicle graft. Methods : A patient with miller class I recession i.r.t 31, 32 and 33, with probing depth of 2.5mm and clinical attachment loss of 4mm i.r.t 31, 32 and 33 and class III gingival recession i.r.t 41 and 43 was treated using periosteum pedicle graft. 42 was missing. Periosteum was dissected and increased in length coronaly to cover the root surface. After stabilizing the periosteal graft with sutures, the epithelium was positioned over it and sutured. Result : Uneventful healing of the operated site was observed after 1 month. There was full coverage of the gingival recession with satisfactory results. There was an increase in morphologic and chromatic resemblance with the adjacent area. Conclusion : Periosteum can be successfully used for the treatment of multiple gingival recession defects. Key words : gingival recession, osteogenic properties, periosteum.
Dr VINEET VINAYAK | dr VINEET VINAYAK |
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
109 vizualizări3 paginiROOT COVERAGE WITH PERIOSTEUM PEDICLE GRAFT - A NOVEL APPROACH DR Vineet Vinayak
Încărcat de
Dr Vineet VinayakABSTRACT : Aim : To cover root surface with periosteum pedicle graft. Methods : A patient with miller class I recession i.r.t 31, 32 and 33, with probing depth of 2.5mm and clinical attachment loss of 4mm i.r.t 31, 32 and 33 and class III gingival recession i.r.t 41 and 43 was treated using periosteum pedicle graft. 42 was missing. Periosteum was dissected and increased in length coronaly to cover the root surface. After stabilizing the periosteal graft with sutures, the epithelium was positioned over it and sutured. Result : Uneventful healing of the operated site was observed after 1 month. There was full coverage of the gingival recession with satisfactory results. There was an increase in morphologic and chromatic resemblance with the adjacent area. Conclusion : Periosteum can be successfully used for the treatment of multiple gingival recession defects. Key words : gingival recession, osteogenic properties, periosteum.
Dr VINEET VINAYAK | dr VINEET VINAYAK |
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 3
CASE REPORT
ROOT COVERAGE WITH PERIOSTEUM PEDICLE GRAFT A NOVEL APPROACH
Authors : (1) H.S Grover, (2) Anil Yadav, (3) Vineet Vinayak, (4) Meenu Jain, (5) Sunil Goyal, (6) Sagrika Shukla
(1) Head Of Department, Department of Periodontics, SGTDC, Gurgoan,( Haryana)
(2) Reader, Department of Periodontics SGTDC, Gurgoan, (Haryana)
(3) Professor, Department of Conservative Dentistry & Endodontics, Institute of Dental Sciences, Bareilly (U.P)
(4) Professor, Department of Prosthodontics and Crown & Bridge, Institute of Dental Sciences, Bareilly (U.P)
(5) Post Graduate Student SGTDC, Gurgoan, (Haryana)
Correspondence : Dr. Vineet Vinayak, Professor, Department of Conservative Dentistry & Endodontics, Institute of Dental Sciences, Bareilly (U.P)
Email - vineet2th@rediffmail.com
ABSTRACT :
Aim : To cover root surface with periosteum pedicle graft.
Methods : A patient with miller class I recession i.r.t 31, 32 and 33, with probing depth of 2.5mm and clinical attachment loss of 4mm i.r.t 31, 32 and 33 and
class III gingival recession i.r.t 41 and 43 was treated using periosteum pedicle graft. 42 was missing. Periosteum was dissected and increased in length
coronaly to cover the root surface. After stabilizing the periosteal graft with sutures, the epithelium was positioned over it and sutured.
Result : Uneventful healing of the operated site was observed after 1 month. There was full coverage of the gingival recession with satisfactory results.
There was an increase in morphologic and chromatic resemblance with the adjacent area.
Conclusion : Periosteum can be successfully used for the treatment of multiple gingival recession defects.
Key words : gingival recession, osteogenic properties, periosteum.
14
Introduction:
devascularised. Skoog raised periosteal flaps from the palatal
Gingival recession is a common problem affecting 40-90% of
surface of maxilla to obtain bony closure of palatal defects in
population1 leading to poor esthetics, root caries, erosion and
children. These flaps were raised by sharp dissection and
dental hypersensitivity and to address these problems various
published results strongly supported osteogenic properties of
techniques have been developed to achieve root coverage.
well vascularised periosteum within 36 months following
There is always a need of developing newer procedures for root
surgery. `Since then many investigators have utilized
coverage and the use of various grafts and tissue engineering
osteogenic property of periosteum for cell culture and root
techniques including stem cell research are testimony to the
coverage procedures.
ever increasing need for most suitable treatment option to
Case description:
3
replace/repair lost tissues to various pathologic processes . One
A 30 years old male patient, reported with unesthetic problems
such successful root coverage procedure is the periosteum
in lower anteriors. On presurgical intraoral examination,
pedicle graft.
gingival status was normal except i.r.t 31,33. There was miller
Periosteum is a highly vascular connective tissue
class I recession i.r.t 31, 32 and 33, with probing depth of
sheath covering the external surface of all the bones except for
4
2.5mm and clinical attachment loss of 4mm i.r.t 31, 32 and 33.
sites of articulation and muscle attachment . The periosteum
comprises of at least two layers, an inner cellular or cambium
There was class III gingival recession i.r.t 41 and 43. 42 was
5
layer and an outer fibrous layer . The inner layer contains
missing. Patient was willing for the treatment of the defect and
numerous osteoblasts and osteoprogenitor cells, and the outer
an informed consent was taken for the same.
layer is composed of dense collagen fiber, fibroblasts and their
6
At the start of surgical procedure patients was given
progenitor cells .
local
anesthesia
with a solution of 2% lignocaine with
Periosteum-derived progenitor cells have the ability
to proliferate rapidly and capability to differentiate into
1:200000 adrenaline. An intra- crevicular incision was given
multiple mesenchymal lineages3. Cells residing within
from 33-43 and vertical incision was given beyond the
periosteum may be excised from any surgically accessible bone
mucogingival junction to release the flap. A Full-thickness flap
surfaces. When properly stimulated, these acts as a bioreactor
was
raised, double the amount of recession to be covered. This
supporting a dramatic increase in the progenitor cell population
3
full-thickness flap was then pulled buccally to create tension
over the course of a few days .
Duhame was the first investigator to study the
on the periosteum. An incision was made at the base of the
osteogenic potential of periosteum8. Ollier9 proved that
periosteum, it was dissected and lifted slowly in a coronal
periosteum produces bone and his study was reinforced by
direction and was brought till the CEJ. The exposed root
10
11
Axhausen . Hey groves in his detailed study concluded that
surface was covered with periosteum and sutured with 4-0
periosteum is osteogenic, but only if elevated by sharp
vicryl sutures using sling suture technique. After stabilizing
dissection, with preservation of a middle or cambium layer
lying between bone and periosteum. Trueta and Cavadias12
the periosteal graft, the flap was coronally positioned and
observed that proliferation of the periosteal blood vessels was
sutured. The releasing incisions were closed with interrupted
followed by new bone formation in the subperiosteal region.
sutures after which the operated site was covered with non13
According to Zucman, Maurer and Berbesson periosteal cells
eugenol periodontal dressing for protection.
retain osteogenic potential even though temporarily
Journal of Dental Sciences & Oral Rehabilitation, July-September 2012
45
Post-operatively the patient was prescribed
amoxicillin 500 mg TDS for 5 days, Ibuprofen 400 mg thrice
daily for 3 days and 0.2% chlorhexidine mouthwash for 2
weeks. Postoperative instruction and oral hygiene
instructions were given to the patient. After 1 week, the
periodontal dressing and sutures were removed and patient
was asked to maintain strict oral hygiene with periodic checkups every month.
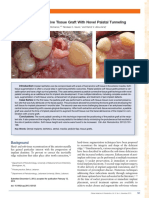
Pre-operative picture
Partial-thickness flap raised. Incisal view: Full-thickness
flap raised
Dissected Periosteum
Periosteum being sutured at the level of CEJ.
Incisal view:
Periosteum stabilized
Partial thickness
flap sutured
Post-operative 1 month
Periodontal
dressing given
Result: Patient reported after 1 week, intraoral post-operative
checkup revealed uneventful healing of the operated site, full
coverage of the gingival recession and satisfactory results. At 1
month postoperative check up there was satisfactory root
coverage and an increase in morphologic and chromatic
resemblance with the adjacent area.
Discussion:
The regeneration of the tooth supporting structures which have
been lost as a consequence of periodontal disease has become
an elusive goal in periodontics. Although periodontal
regeneration, i.e. the formation of new bone and new
cementum with supportive periodontal ligament, is a possible
objective of several periodontal therapeutic modalities,
15
outcomes of such modalities are not always predictable .
Inherent problems of a limited quantity of available graft, the
need for two surgical sites, compromised patient esthetics,
postoperative discomfort and complications, and increased
costs of treatment have limited the success of one single
universal technique that can be used with high predictability,
effectiveness, and efficiency without compromising patient
centered criteria like pain, postoperative esthetic outcomes,
and costs of treatment16. Research has shown that periosteum is
17
18
rich in osteogenic cells. According to Simon and Bhaskar ,
the inner layer of periosteum contains numerous osteoblasts
and osteoprogenitor cells and the outer layer contains dense
collagen fiber and fibroblasts and their progenitor cells making
periosteum a highly regenerative tissue. According to
Bouchard et al19 tissues produced by these cells include
cementum with periodontal ligament fibers and bone20, making
it an ideal graft material in cases of recession and bone loss. In a
recent in-vitro study by Kawase et al21, cultured periosteum
cells on HA (hydroxyapatite) block demonstrated that an
osteogenic tissue engineered bone substitute could be prepared
by periosteal cells, which have regenerative capacity.
16
According to Mahajan results were highly encouraging
when periosteum pedicle graft was used to cover recession
defects which showed reduction to 0.3 0.57 mm from 3.75
1.55, also there was a gain in widths of keratinized and
attached gingiva, however he used partial thickness flap which
has the disadvantage of loss of radicular bone, which is
amplified in thin gingival
biotype, also if partial dissection of this biotype is done it
leads to compromised blood supply and eventual flap death or
recession22. Claffey and Shanley23 reported that subjects
with gingiva <1.5 mm thick at a mid-buccal location lost
attachment after supra- and sub-gingival debridement. No sites
with mucosa >2mm receded. A study on pedicle flaps in pigs
demonstrated that subjectively thick flaps survived twice as
often as thin flaps (55.7% versus 26.5%) and that thin flaps
relied mostly on collateral circulation from the recipient bed
for oxygen and nutrients24. In our technique we have raised a
full thickness flap which eliminates these disadvantages in
cases with thin gingival biotype.
The wound healing after surgery requires rich blood
supply, revascularization and maintenance of blood supply for
reattachment to take place. Also, a vascular graft has more
chances of surviving on an avascular root surface16.
According to a study by Bourke25 periosteal cells release
vascular endothelial growth factors; such properties make the
periosteum suitable graft over an avascular root surface. Also
as it is a pedicle graft, it retains the blood supply maintaining
vascularity. The advantage of using peristeum graft is that its
patient's own tissue and there is no chance of infection or
reaction. It is affordable and second surgical site is not
required, also a larger area can be grafted using patient's own
tissue. This technique has minimal intraoperative time and
minimum postoperative complications.
This technique is better as compared to other
Journal of Dental Sciences & Oral Rehabilitation, July-September 2012
46
techniques used for root coverage such as the use of alloderm,
bone in the repair of defects caused by injury or disease.
as it has chances of reaction and is an expensive treatment.
British Journal of Surgery, 5, 185-242.
Palatal connective tissue grafting technique is sensitive and
12. Trueta J., Cavadias A. X. Vascular changes caused by the
gives the patient two surgical sites in the mouth, making eating,
Kuntscher type of nailing. Journal of Bone and Joint
swallowing and speaking difficult. Also, a small amount of
Surgery, 37-B, 492-505.
tissue can be harvested which sometimes is not enough with
13. Zucman J, Maurer P, Berbesson C. The effect of autografts of
huge defects.
bone and periosteum in recent diaphysial fractures. J Bone
The only disadvantage of this technique is that it requires a
Joint Surg 1968;50:409-422.
skilled operator, also long-term results of this technique are yet
14. Skoog T. The use of periosteal flaps in the repair of clefts of
to be assessed, however, healing in case of periosteal graft
the primary palate. Cleft Palate J 1965; 2:332-339.
gives satisfactory results.
15. Position Paper. Periodontal Regeneration. J Periodontol
Conclusion
2005;76:1601-1622.
Periosteum can be successfully used for the treatment of
16. Mahajan A. Treatment of Multiple Gingival Recession
multiple gingival recession defects. However, further research
Defects Using Periosteal Pedicle Graft: A Case Series. J
and clinical assessment is needed with respect to this
Periodontol 2010;81:1426-1431.
technique. Also, long term results of periosteum graft
17. Simon TM, Van Sickle DC, Kunishima DH, Jackson DW.
are lacking, which also need further research.
Cambium cell stimulation from surgical release of
References
theperiosteum. JOrthopRes 2003;21:470-480
1. Lang NP, Loe H. The relationship between the width of
18. BhaskarSN. In:BhaskarSN,ed.Orban'sOralHistology and
keratinized gingival health. J Periodontal 1972;43:623-27.
Embryology, 11th ed. New Delhi: Harcourt India Private
2. Kumar ABT, Mehta DS. Comparative evaluation of
Ltd.; 1991:209.
subepithelial connective tissue graft (SCTG) and acellular
19. Bouchard P, Malet J, Borghetti A. Decision-making in
dermal matrix allograft (ADMA) in the treatment of
aesthetics: Root coverage revisited. Periodontol 2000
localized gingival recession-a clinical study. j Int Clin Dent
2001;27:97-120.
Res Org 2009;1:8-16.
20. De Bari C, Dell'Accio F, Vanlauwe J, et al. Mesenchymal
3 Mahajan A. Periosteum: A Highly Underrated Tool in
multipotency of adult human periosteal cells demonstrated
Dentistry. Int J Dent, 2011;2012:1-6.
by single-cell lineage analysis. Arthritis Rheum
4. Provenza DV, Seibel W. Basic Tissues, Oral Histology
2006;54:1209-1221.
Inheritance and Development, Lea and Feibger, 2nd edition,
21. Kawase T, Okuda K, Kogami H, Nakayama H, Nagata M,
1986.
Sato T, Wolff LF, Yoshie H. human Periosteum-derived cells
5. Finley JM, Acland RD, Wood MB. Revascularized periosteal
combined with superporous hydroxyapatite block used as an
grafts. A new method to produce functional new bone
osteogenic bone substitute for periodontal regenerative
without bone grafting, Plastic and Reconstructive Surgery,
therapy: an animal implantation study using nude mice. J
vol. 61, no. 1, pp. 16, 1978.
periodontal 2010;81:420-427.
6. Orban B J, Bhaskar SN. Orbans Oral Histology and
22. Hwang D, Wang HL. Flap Thickness as a Predictor of Root
Embryology, 11th edition, 2002.
Coverage:A Systematic Review. J Periodontol
7. Arnsdorf EJ, Jones LM, Carter DR, Jacobs CR. The
2006;77:1625-1634.
periosteum as a cellular source for functional tissue
23. Claffey N, Shanley D. Relationship of gingival thickness and
engineering. Tissue Engineering 2009;15:26372642.
bleeding to loss of probing attachment in shallow sites
8. Hutmacher DW. Sittinger M. Periosteal cells in bone tissue
following nonsurgical periodontal therapy. J Clin
engineering, Tissue Engineering, 2003; 9 (supp):S45S64.
Periodontol 1986;13:654-657.
9. Oilier L. Traite experimental et clinique de la regeneration des
24. Clodius L, Smahel J. Thin and thick pedicle flap. Acta Chir
os et de la production artificielle do tissu osseu.v. 2 vols.
Plast 1972;14:30-35.
Paris : Victor Masson et Fils
25. Bourke HE, Sandison A, Hughes SP, Reichert IL. Vascular
10. Axhausen G. Die histologischen und klinischen Gesetze der
endothelial growth factor (VEGF) in human periosteum
freien Osteoplastik aufGrund von Thierversuchen. Archiv
Normal expression and response to fracture. J Bone Joint
fur klinische Chirurgie, 88, 23-145.
Surg Br 2003;85-B(Suppl):4.
11. Groves E. W. H. Methods and results of transplantation of
Journal of Dental Sciences & Oral Rehabilitation, July-September 2012
47
S-ar putea să vă placă și
- Peri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentDe la EverandPeri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentÎncă nu există evaluări
- Case SeriesDocument7 paginiCase Seriesemi_alaÎncă nu există evaluări
- Evaluacion Histologica de Los Diversos Estadios de Curacion en El Paladar Luego de Un Procedimiento de Injerto de Tej Conevtivo Subepitelial PDFDocument7 paginiEvaluacion Histologica de Los Diversos Estadios de Curacion en El Paladar Luego de Un Procedimiento de Injerto de Tej Conevtivo Subepitelial PDFpyrockerÎncă nu există evaluări
- Surgical Reconstruction of Interdental PDocument11 paginiSurgical Reconstruction of Interdental PMaria Jose GodoyÎncă nu există evaluări
- Free Gingival Grafting To Increase The Zone of Keratinized Tissue Around ImplantsDocument5 paginiFree Gingival Grafting To Increase The Zone of Keratinized Tissue Around ImplantsWinfield LiongÎncă nu există evaluări
- Theevolutionofsurgical Techniquesandbiomaterials ForperiodontalregenerationDocument11 paginiTheevolutionofsurgical Techniquesandbiomaterials ForperiodontalregenerationYasuAAA AanzaiÎncă nu există evaluări
- Alogénico Vs AutoóogoDocument4 paginiAlogénico Vs AutoóogoMaximiliano Jara ContrerasÎncă nu există evaluări
- Autologus Fibroblast InjectionsDocument14 paginiAutologus Fibroblast InjectionsDr. DeeptiÎncă nu există evaluări
- Management of Infected Radicular Cyst by Surgical Approach: Case ReportDocument2 paginiManagement of Infected Radicular Cyst by Surgical Approach: Case ReportEzza RiezaÎncă nu există evaluări
- Modified TwoDocument20 paginiModified TwoElmer Rubén Laura JoveÎncă nu există evaluări
- One Step Solution For Multiple Marginal Tissue Recession in Thin Gingival BiotypeDocument6 paginiOne Step Solution For Multiple Marginal Tissue Recession in Thin Gingival BiotypeIJAR JOURNALÎncă nu există evaluări
- Esthetic and Functional Reconstruction of Large Mandibular Defects Using Free Fibula Flap and Implant-Retained Prosthetics - A Case Series With Long-Term Follow-UpDocument7 paginiEsthetic and Functional Reconstruction of Large Mandibular Defects Using Free Fibula Flap and Implant-Retained Prosthetics - A Case Series With Long-Term Follow-UppankajÎncă nu există evaluări
- Tent-Pole in Regeneration TechniqueDocument4 paginiTent-Pole in Regeneration TechniqueangelicapgarciacastilloÎncă nu există evaluări
- Aumento de Reborde Con Tejido BlandoDocument8 paginiAumento de Reborde Con Tejido BlandoSilvia SolisÎncă nu există evaluări
- Ijomi 15 415Document4 paginiIjomi 15 415Bagis Emre GulÎncă nu există evaluări
- Direct Maxillary Sinus Lift For Single Tooth Implant A Clinical StudyDocument4 paginiDirect Maxillary Sinus Lift For Single Tooth Implant A Clinical StudyRadita Dwihaning PutriÎncă nu există evaluări
- Case Report On Maxillary Labial FrenectomyDocument9 paginiCase Report On Maxillary Labial Frenectomyviolita chresnaÎncă nu există evaluări
- 20 DR Arvind UDDocument7 pagini20 DR Arvind UDJohn SmithÎncă nu există evaluări
- A Novel Modified Vista Technique With Connective Tissue Graft in The Treatment of Gingival Recession - Chowdary 2020Document19 paginiA Novel Modified Vista Technique With Connective Tissue Graft in The Treatment of Gingival Recession - Chowdary 2020Natalia AcevedoÎncă nu există evaluări
- GINGIVEKTOMIDocument6 paginiGINGIVEKTOMIAstrid ChrisanditaÎncă nu există evaluări
- Whale's Tail TechniqueDocument32 paginiWhale's Tail Techniquevijeta vyasÎncă nu există evaluări
- Evaluation of The Effectiveness of Collagen Membrane in The Management of Oro Antral FistulaCommunication A Clinical StudyDocument8 paginiEvaluation of The Effectiveness of Collagen Membrane in The Management of Oro Antral FistulaCommunication A Clinical StudyAthenaeum Scientific PublishersÎncă nu există evaluări
- Kassab2010 PDFDocument12 paginiKassab2010 PDFdhwanit31Încă nu există evaluări
- Tre Atm Ent of Gingiva L Re Cession: Moawia M. Kassab,, Hala Badawi,, Andrew R. DentinoDocument12 paginiTre Atm Ent of Gingiva L Re Cession: Moawia M. Kassab,, Hala Badawi,, Andrew R. Dentinodhwanit31100% (1)
- Prosthetic Management of Hemimandibulectomy Patient - A Case ReportDocument3 paginiProsthetic Management of Hemimandibulectomy Patient - A Case ReportIOSRjournalÎncă nu există evaluări
- 1 s2.0 S0022391321000056 MainDocument6 pagini1 s2.0 S0022391321000056 MainAlex OprisanÎncă nu există evaluări
- 2000 J C. H S W A: Udson Ickey Cientific Riting WardDocument6 pagini2000 J C. H S W A: Udson Ickey Cientific Riting WardPremshith CpÎncă nu există evaluări
- Roll Man 2013Document6 paginiRoll Man 2013SergioÎncă nu există evaluări
- Journal ProstoDocument6 paginiJournal ProstoAvila Aita Harun RasyidÎncă nu există evaluări
- Recovery of Pulp Sensibility After The Surgical Management of A Large Radicular CystDocument5 paginiRecovery of Pulp Sensibility After The Surgical Management of A Large Radicular CystmeryemeÎncă nu există evaluări
- Esthetic Zone Root Coverage With Lateral Pedicle Flap - A CaseDocument5 paginiEsthetic Zone Root Coverage With Lateral Pedicle Flap - A CaseHiroj BagdeÎncă nu există evaluări
- Materials: A Modified Ridge Splitting Technique Using Autogenous Bone Blocks-A Case SeriesDocument10 paginiMaterials: A Modified Ridge Splitting Technique Using Autogenous Bone Blocks-A Case SeriesLouis HutahaeanÎncă nu există evaluări
- Vestibuloplasty New TechniqueDocument4 paginiVestibuloplasty New TechniqueFerdinan Pasaribu0% (1)
- Significance of The Width of KeratinizedDocument6 paginiSignificance of The Width of KeratinizedRahma Hesham Ahmed HusseinÎncă nu există evaluări
- A Case Report On Combination of Vista With Connective Tissue Graft As A Predictable Surgical Approach in Management of Multiple Gingival RecessionDocument5 paginiA Case Report On Combination of Vista With Connective Tissue Graft As A Predictable Surgical Approach in Management of Multiple Gingival RecessionInternational Journal of Innovative Science and Research TechnologyÎncă nu există evaluări
- Clinical Study: A Liquid Membrane As A Barrier Membrane For Guided Bone RegenerationDocument6 paginiClinical Study: A Liquid Membrane As A Barrier Membrane For Guided Bone RegenerationStanislav ȘuiuÎncă nu există evaluări
- Dens Evaginatus and Type V Canal Configuration: A Case ReportDocument4 paginiDens Evaginatus and Type V Canal Configuration: A Case ReportAmee PatelÎncă nu există evaluări
- HFM Free Flap Versus Fat GraftingDocument10 paginiHFM Free Flap Versus Fat GraftingNelson LowÎncă nu există evaluări
- Three-Dimensional Vertical Alveolar Ridge Augmentation in The Posterior Maxilla: A 10-Year Clinical StudyDocument10 paginiThree-Dimensional Vertical Alveolar Ridge Augmentation in The Posterior Maxilla: A 10-Year Clinical StudyFabian Sanabria100% (1)
- Preservation and Augmentation of Molar Extraction Sites Affected by Severe Bone Defect Due To Advanced Periodontitis A Prospective Clinical TrialDocument12 paginiPreservation and Augmentation of Molar Extraction Sites Affected by Severe Bone Defect Due To Advanced Periodontitis A Prospective Clinical TrialBagis Emre GulÎncă nu există evaluări
- 10 1111@scd 12546Document7 pagini10 1111@scd 12546Maisely Fabiluz Galindo GomezÎncă nu există evaluări
- Dr. Neeraj AgrawalDocument4 paginiDr. Neeraj AgrawalYulinda PrimilisaÎncă nu există evaluări
- 软组织相关的并发症风险Document15 pagini软组织相关的并发症风险xiaoxin zhangÎncă nu există evaluări
- Vestibular Deepening To Improve Periodontal Pre-ProstheticDocument5 paginiVestibular Deepening To Improve Periodontal Pre-ProstheticRAKERNAS PDGI XIÎncă nu există evaluări
- Harris1992 The Connective Tissue and Partial Thickness Double Pedicle GraftDocument10 paginiHarris1992 The Connective Tissue and Partial Thickness Double Pedicle GraftAna Maria Montoya GomezÎncă nu există evaluări
- Periodontology 2000 - 2023 - Roccuzzo - The Importance of Soft Tissue Condition in Bone Regenerative Procedures To EnsureDocument10 paginiPeriodontology 2000 - 2023 - Roccuzzo - The Importance of Soft Tissue Condition in Bone Regenerative Procedures To Ensuremạnh nguyễn xuânÎncă nu există evaluări
- Fotos OclusalesDocument6 paginiFotos OclusalesMarco Antonio García LunaÎncă nu există evaluări
- Artículo Khoury2018Document10 paginiArtículo Khoury2018Basma Derdabi100% (1)
- Implante Articulo 4Document8 paginiImplante Articulo 4alessandrachumbimuneÎncă nu există evaluări
- Free Flaps MaxillaDocument7 paginiFree Flaps MaxillaFahad QiamÎncă nu există evaluări
- Coronally Advanced Flap With and Without VerticalDocument13 paginiCoronally Advanced Flap With and Without VerticalLEONARDO ALBERTO CRESPIN ZEPEDAÎncă nu există evaluări
- 5500-Article Text-10024-1-10-20210515Document5 pagini5500-Article Text-10024-1-10-20210515DrRobin SabharwalÎncă nu există evaluări
- Drughelp - Care 6.22Document10 paginiDrughelp - Care 6.22Joko RifaiÎncă nu există evaluări
- Jurnal PPGDocument8 paginiJurnal PPGsari elyÎncă nu există evaluări
- Free Gingival Grafting To Increase The Zone of Keratinized Tissue Around ImplantsDocument4 paginiFree Gingival Grafting To Increase The Zone of Keratinized Tissue Around ImplantsVikas AggarwalÎncă nu există evaluări
- Reconstruction of Mandible by Free Fibular Flap: Original ArticleDocument5 paginiReconstruction of Mandible by Free Fibular Flap: Original ArticleSani Solihatul FitriÎncă nu există evaluări
- DR Bhaumik Nanavati Proof ApprovedDocument6 paginiDR Bhaumik Nanavati Proof ApprovedFahmi FirmansyahÎncă nu există evaluări
- Continuing Education 1: Horizontal Alveolar Ridge Augmentation: The Importance of Space MaintenanceDocument11 paginiContinuing Education 1: Horizontal Alveolar Ridge Augmentation: The Importance of Space MaintenanceJuan Jose Sosa BerganzaÎncă nu există evaluări
- Types of Gingival GraftsDocument34 paginiTypes of Gingival GraftsAhmad KurukchiÎncă nu există evaluări
- Influence of Ultrasonic Irrigation and Chloroform On Cleanliness of Dentinal Tubules During Endodontic Retreatment-An Invitro SEM StudyDocument5 paginiInfluence of Ultrasonic Irrigation and Chloroform On Cleanliness of Dentinal Tubules During Endodontic Retreatment-An Invitro SEM StudyDr Vineet VinayakÎncă nu există evaluări
- BELLS PALSY - A REVIEW OF IDIOPATHIC FACIAL PARALYSIS DR Vineet VinayakDocument2 paginiBELLS PALSY - A REVIEW OF IDIOPATHIC FACIAL PARALYSIS DR Vineet VinayakDr Vineet VinayakÎncă nu există evaluări
- MONOCHROMATIC INTENSE PULSED LIGHT FOR TREATMENT OF LIP VITILIGO DR Vineet VinayakDocument2 paginiMONOCHROMATIC INTENSE PULSED LIGHT FOR TREATMENT OF LIP VITILIGO DR Vineet VinayakDr Vineet VinayakÎncă nu există evaluări
- Naturopathy and Endodontics in Succesful Root Canal Treatment DR Vineet VinayakDocument3 paginiNaturopathy and Endodontics in Succesful Root Canal Treatment DR Vineet VinayakDr Vineet VinayakÎncă nu există evaluări
- Flare Up in Root Canal Treatments DR Vineet VinayakDocument3 paginiFlare Up in Root Canal Treatments DR Vineet VinayakDr Vineet VinayakÎncă nu există evaluări
- Hemisection Divide A Tooth To Save A Tooth - DR Vineet VinayakDocument3 paginiHemisection Divide A Tooth To Save A Tooth - DR Vineet VinayakDr Vineet VinayakÎncă nu există evaluări
- Post Endodontic Restoration Using Glass Fiber Non Metallic Posts - DR Vineet VinayakDocument3 paginiPost Endodontic Restoration Using Glass Fiber Non Metallic Posts - DR Vineet VinayakDr Vineet VinayakÎncă nu există evaluări
- DR Vineet VinayakDocument2 paginiDR Vineet VinayakDr Vineet VinayakÎncă nu există evaluări
- Final Year Clinical OSCE For Medical UndergraduatesDocument97 paginiFinal Year Clinical OSCE For Medical UndergraduatesSiam Weng LoongÎncă nu există evaluări
- For Wastewater Systems: BioaugmentationDocument3 paginiFor Wastewater Systems: BioaugmentationPalak AgarwalÎncă nu există evaluări
- Peka SainsDocument26 paginiPeka SainsPuvaan RaajÎncă nu există evaluări
- Boarding SchoolDocument24 paginiBoarding Schooledwardoplunkett100% (1)
- Mandibular Expansion AppliancesDocument9 paginiMandibular Expansion AppliancesGeorgiana BlagociÎncă nu există evaluări
- Blindness Control ProgramsDocument66 paginiBlindness Control ProgramsAravind KumarÎncă nu există evaluări
- Solomon Ankle Injury PDFDocument9 paginiSolomon Ankle Injury PDFHikmah Wahid AkbarÎncă nu există evaluări
- Monmeet Instrumentation MMDTDocument18 paginiMonmeet Instrumentation MMDTMonmeet MallickÎncă nu există evaluări
- STRONG Fitness Training Guide - Fall 2014 USA PDFDocument44 paginiSTRONG Fitness Training Guide - Fall 2014 USA PDFPeter AsanÎncă nu există evaluări
- POAG, GlaukomaDocument19 paginiPOAG, GlaukomaAffan ZulkarnainÎncă nu există evaluări
- Uterine motilityMD20.8.55 Sheet PDFDocument45 paginiUterine motilityMD20.8.55 Sheet PDFNirut SrimakamÎncă nu există evaluări
- Efficacy of Surfactant at Different Gestational Ages For Infants With Respiratory Distress Syndrome PDFDocument7 paginiEfficacy of Surfactant at Different Gestational Ages For Infants With Respiratory Distress Syndrome PDFnisaÎncă nu există evaluări
- Postmodern Counseling ApproachesDocument20 paginiPostmodern Counseling ApproachesJangHendi75% (4)
- CM Health Insurance - Tender - Tamil NaduDocument116 paginiCM Health Insurance - Tender - Tamil NadukayalonthewebÎncă nu există evaluări
- MetaanalysisDocument12 paginiMetaanalysisAhmed BadrÎncă nu există evaluări
- Intro To Psychology UnitsDocument38 paginiIntro To Psychology Unitsapi-325580763Încă nu există evaluări
- Management of Perioperative ArrhythmiasDocument51 paginiManagement of Perioperative ArrhythmiasAbhishek LonikarÎncă nu există evaluări
- Ulcerative ColitisDocument5 paginiUlcerative ColitisVenice Jame SanchezÎncă nu există evaluări
- Coreg (Carvedilol) 6.25mgDocument3 paginiCoreg (Carvedilol) 6.25mgE100% (2)
- Hormone Cure Instructor Manual PDFDocument26 paginiHormone Cure Instructor Manual PDFGabriel Camarena83% (6)
- Kala Azar EthiopiaDocument11 paginiKala Azar EthiopiaPrabir Kumar ChatterjeeÎncă nu există evaluări
- Mona CVDocument97 paginiMona CVarushikhandelwalÎncă nu există evaluări
- Lanoxin: (Digoxin) InjectionDocument35 paginiLanoxin: (Digoxin) InjectionZainÎncă nu există evaluări
- Cardio OrientationDocument6 paginiCardio OrientationBandana RajpootÎncă nu există evaluări
- Although Shock Has Been Recognised For Over 100 YearsDocument4 paginiAlthough Shock Has Been Recognised For Over 100 YearsRusty HoganÎncă nu există evaluări
- Questionnaire - 11Document3 paginiQuestionnaire - 11S.Abyisheik ReddyÎncă nu există evaluări
- Management of The Urologic Sepsis SyndromeDocument10 paginiManagement of The Urologic Sepsis SyndromeNur Syamsiah MÎncă nu există evaluări
- CBD Dr. SaugiDocument37 paginiCBD Dr. SaugiKikyÎncă nu există evaluări
- Aroonika S. Bedre, Dr. Ganesh JeevanandhamDocument5 paginiAroonika S. Bedre, Dr. Ganesh JeevanandhamMalavika BedreÎncă nu există evaluări
- Nso ErcpDocument3 paginiNso Ercptry dokkÎncă nu există evaluări