Documente Academic
Documente Profesional
Documente Cultură
Neurosurgery TechChir 2006 PDF
Încărcat de
karahmanDescriere originală:
Titlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Neurosurgery TechChir 2006 PDF
Încărcat de
karahmanDrepturi de autor:
Formate disponibile
OPERATIVE TECHNIQUES
OLFACTORY GROOVE MENINGIOMAS FROM
NEUROSURGICAL AND EAR, NOSE, AND
THROAT PERSPECTIVES: APPROACHES,
TECHNIQUES, AND OUTCOMES
Sergey Spektor, M.D.,
Ph.D.
Department of Neurosurgery,
Hadassah University Hospital,
Jerusalem, Israel
Javier Valarezo, M.D.
Department of Neurosurgery,
Hadassah University Hospital,
Jerusalem, Israel
Dan M. Fliss, M.D.
Department of Otolaryngology,
Head and Neck Surgery,
Tel Aviv Sourasky Medical Center,
Tel Aviv, Israel
Ziv Gil, M.D., Ph.D.
Department of Otolaryngology,
Head and Neck Surgery,
Tel Aviv Sourasky Medical Center,
Tel Aviv, Israel
Jose Cohen, M.D.
Department of Neurosurgery,
Hadassah University Hospital,
Jerusalem, Israel
Jose Goldman, M.D.
Department of Neurosurgery,
Hadassah University Hospital,
Jerusalem, Israel
Felix Umansky, M.D.
Department of Neurosurgery,
Hadassah University Hospital,
Jerusalem, Israel
Reprint requests:
Sergey Spektor, M.D., Ph.D.,
Department of Neurosurgery,
P.O. Box 12000,
Hadassah University Hospital,
Jerusalem, Israel 91120.
Email: spektor@hadassah.org.il
Received, September 1, 2004.
Accepted, March 8, 2005.
OBJECTIVE: To review the surgical approaches, techniques, outcomes, and recurrence
rates in a series of 80 olfactory groove meningioma (OGM) patients operated on
between 1990 and 2003.
METHODS: Eighty patients underwent 81 OGM surgeries. Tumor diameter varied
from 2 to 9 cm (average, 4.6 cm). In 35 surgeries (43.2%), the tumor was removed
through bifrontal craniotomy; nine operations (11.1%) were performed through a
unilateral subfrontal approach; 18 surgeries (22.2%) were performed through a pterional approach; seven surgeries (8.6%) were carried out using a fronto-orbital craniotomy; and 12 procedures (14.8%) were accomplished via a subcranial approach.
Nine patients (11.3%) had undergone surgery previously and had recurrent tumor.
RESULTS: Total removal was obtained in 72 patients (90.0%); subtotal removal was
achieved in 8 patients (10.0%). Two patients, one with total and one with subtotal
removal, had atypical (World Health Organization Grade II) meningiomas, whereas 78
patients had World Health Organization Grade I tumors. There was no operative
mortality and no new permanent focal neurological deficit besides anosmia. Twentyfive patients (31.3%) experienced surgery-related complications. There were no recurrences in 75 patients (93.8%) 6 to 164 months (mean, 70.8 mo) after surgery. Three
patients (3.8%) were lost to follow-up. In two patients (2.5%) with subtotal removal,
the residual evidenced growth on computed tomography and/or magnetic resonance
imaging 1 year after surgery. One of them had an atypical meningioma. The second,
a multiple meningiomata patient, was operated on twice in this series.
CONCLUSION: A variety of surgical approaches are used for OGM resection. An
approach tailored to the tumors size, location, and extension, combined with modern
microsurgical cranial base techniques, allows full OGM removal with minimal permanent morbidity, excellent neurological outcome, and very low recurrence rates.
KEY WORDS: Cranial base, Olfactory groove meningioma, Radical resection, Recurrence, Surgical
approach, Tumor extension
Neurosurgery 57[ONS Suppl 3]:ONS-268ONS-280, 2005
lfactory groove meningiomas (OGMs)
arise in the midline over the cribriform
plate and frontosphenoidal suture (18,
31). It is well known that most of these tumors
occupy the floor of the anterior cranial fossa,
extending all the way from the crista galli to the
tuberculum sellae (4). There are some similarities between posteriorly extending OGMs and
tuberculum sellae meningiomas. The main distinguishing feature is the location of the optic
ONS-268 | VOLUME 57 | OPERATIVE NEUROSURGERY 4 | OCTOBER 2005
DOI: 10.1227/01.NEU.0000176409.70668.EB
apparatus in relation to the tumor (18). OGMs
push the optic nerves and the chiasm downward and posteriorly as they grow (31, 45).
Tuberculum sellae meningiomas elevate the chiasm and displace the optic nerve superolaterally; thus, the tumor occupies a subchiasmal
position (2, 18, 19). These benign, slow-growing
tumors frequently achieve large size before detection. Surgical removal of small to mid-size
OGMs usually is not difficult. However in a
www.neurosurgery-online.com
OLFACTORY GROOVE MENINGIOMA SURGERY
significant proportion of patients, the tumor is very large and/or
infiltrates or involves surrounding structures, making its removal challenging.
Several surgical approaches can be applied for tumor removal. Traditionally, frontal or bifrontal craniotomy has been
used with subfrontal approach to the tumor (4, 6, 10, 29, 31, 35,
4345). More recently, some surgeons have used a pterional
approach (17, 33, 38, 46, 47). More aggressive approaches have
been proposed for resection of OGMs expanding into the
paranasal sinuses and orbits, including transbasal (9), subcranial (13, 36), and fronto-orbital approaches (41), frontal or
bifrontal craniotomy combined with orbital or nasal osteotomies (3, 18), and craniofacial resection (15).
This article presents results from the surgical treatment of 80
patients with OGMs via bifrontal, unilateral subfrontal, pterional, fronto-orbital, and subcranial approaches from 1990
through 2003, the largest patient series and the longest postoperative follow-up reported in the recent neurosurgical
literature.
PATIENTS AND METHODS
Patient Population
From September 1990 through October 2003, our neurosurgical team operated on 68 patients with OGM tumors in
Hadassah University Hospital, Jerusalem, and 12 patients
jointly with an ear, nose, and throat (ENT) team at the IchilovSourasky Medical Center, Tel Aviv. One multiple meningioma
patient who underwent surgery at Hadassah was operated on
a second time when his meningioma recurred within the first
year.
Demographic data are presented in Table 1. There was a
significant female predominance (58 patients; 72.5%). Patient
age ranged from 16 to 85 years (average, 55 yr). Headache in
41 patients (51.3%) and anosmia in 39 patients (48.8%) were
the most common presenting symptoms. At admission, 21
patients (26.3%) had both mental and personality changes.
Twenty-two patients (27.5%) demonstrated visual impairment, including 11 (13.8%) with papilledema. Nine patients
(11.3%) had epilepsy at presentation (Table 2). All patients
underwent preoperative and postoperative neuroimaging
TABLE 1. Demographic data of 80 patients operated for
olfactory groove meningioma
Characteristic
No. of patients (%)
Sex
Male
Female
22 (27.5%)
58 (72.5%)
Age (yr)
Median
Range
55
16 85
NEUROSURGERY
TABLE 2. Presenting signs and symptoms in olfactory groove
meningioma patients
Signs and symptoms
No. of patients (%)
Olfactory impairment
47 (58.8%)
Headache
41 (51.3%)
Visual impairment
22 (27.5%)
Mental change
21 (26.3%)
Papilledema
11 (13.8%)
Epilepsy
9 (11.3%)
Nasal obstruction
8 (10.0%)
Motor deficit
4 (5.0%)
Incontinence
3 (3.8%)
Optic atrophy
3 (3.8%)
Foster Kennedy
3 (3.8%)
Sinusitis
2 (2.5%)
Exophthalmos
1 (1.3%)
Telecanthus
1 (1.3%)
Facial deformity
1 (1.3%)
studies, including computed tomography and/or magnetic
resonance imaging (MRI), and an ophthalmic examination.
Fifty-eight patients (72.5%) had tumors 4 cm or more in
diameter. Tumors were centered on the midline in 73 patients
(91.3%). Seven tumors extended laterally (six right [7.5%]; one
left [1.3%]). Thirty-eight patients (47.5%) had purely intracranial tumors with no optic nerve involvement; 21 patients
(26.3%) had intracranial tumors including optic nerve involvement; 15 (18.8%) patients had intracranial tumors with extension to the ethmoidal sinus, frontal sinus, nasal cavity, and/or
orbital area; and 6 patients (7.5%) had both optic nerve involvement and paranasal sinus extension (Table 3).
Nine patients (11.3%) referred for recurrent tumor had been
operated on previously via regular craniotomy (using a bifrontal,
frontal, or pterional approach) from 1 to 16 years earlier (average,
5.8 yr). Among the nine patients, five patients had intracranial
tumors with no optic nerve involvement, two patients had intracranial tumors with optic nerve involvement, one had both paranasal extension and optic nerve involvement, and one had paranasal extension but no optic nerve involvement. MRI studies
depicting OGM extension patterns characteristic of tumors in our
series are shown in Figure 1.
Surgical Techniques
The surgical goal was radical tumor resection unless safe
removal was precluded by significant invasion of the anterior
VOLUME 57 | OPERATIVE NEUROSURGERY 4 | OCTOBER 2005 | ONS-269
SPEKTOR
ET AL.
TABLE 3. Tumor location and invasion patterns
Tumor location and invasion
No. of patients (%)
Intracranial tumor, no optic nerve
involvement
38 (47.5%)
Intracranial tumor, optic nerve
involvement
21 (26.2%)
Intracranial tumors with paranasal
extension
Ethmoidal, optic nerve
Ethmoidal, nasal, orbital
Ethmoidal, frontal, nasal, orbital
Ethmoidal
Ethmoidal, nasal, optic nerve
Ethmoidal, nasal
Ethmoidal, nasal, orbital, sphenoidal
Ethmoidal, frontal, orbital, sphenoidal
Ethmoidal, frontal
Ethmoidal, nasal, orbital, optic nerve
Frontal
Orbital, maxillar, infratemporal
21 (26.3%)
Total patients
80 (100.0%)
4
4
3
2
1
1
1
1
1
1
1
1
communicating artery complex or optic nerves. After tumor
removal, the dural attachment was coagulated and the dura
was stripped. Underlying hyperostosis was drilled away.
Thirty-five surgeries (43.2%) in patients with large tumors
were performed through a bifrontal craniotomy, and nine
surgeries (11.1%) were performed through a unilateral subfrontal approach. Twelve patients (14.8%) with tumors extending far into the paranasal sinus, nasal cavity, and/or
orbits were operated on via a subcranial approach. We used
the pterional approach in 18 surgeries (22.2%) and the frontoorbital approach in 7 surgeries (8.6%). Figure 2 illustrates each
of the approaches, Table 4 summarizes data on tumor extension and surgical approach, and Table 5 summarizes data on
tumor size and surgical approach.
Bifrontal, unilateral-subfrontal, and pterional approaches
were performed as described previously (17, 31, 35, 46). The
fronto-orbital approach was made through a frontotemporal
craniotomy with a single-piece bone flap containing the frontal bone, frontozygomatic process, supraorbital rim, and anterior part of the orbital roof, as proposed by Delashaw et al. (7).
The subcranial approach was performed using the technique of Raveh et al. (36), with modifications as described
elsewhere (12, 13). With the patient in the supine position, a
very low bicoronal skin flap beneath the orbital rims and
nasion is elevated, preserving the pericranium. The periorbit
beneath both orbital roofs is separated. Orbital and frontal
osteotomies are made, and the bone flap, containing both
orbital rims, orbital roofs, nasion, frontal sinuses, and a part of
the ethmoidal air cells, is elevated. This approach provides an
ONS-270 | VOLUME 57 | OPERATIVE NEUROSURGERY 4 | OCTOBER 2005
immediate and direct route to the cribriform plate and olfactory grooves, ethmoidal and sphenoid sinuses, nasal cavities,
and both orbits. The optic canals may be opened if necessary,
exposing the optic nerves.
An autologous pericranial flap, fat, temporal muscle and
temporal fascia, autologous fascia lata, and fibrin glue were
used for reconstruction and prophylaxis of rhinorrhea, regardless of the surgical approach, whenever the frontal and/or
ethmoidal sinuses were opened. Naturally, the subcranial approach created the most significant intracranial and nasopharyngeal anterior cranial base defect. Meticulous multilayer
reconstruction was performed for these patients, as previously
described (11), and they were managed with continuous lumbar drain for a minimum of 5 days.
RESULTS
The most frequent postoperative complication was cerebrospinal fluid (CSF) leak, which occurred in 10 patients (12.5%)
and resulted in meningitis in 4 patients (5%). CSF leak stopped
after several days of lumbar draining in eight patients. Two
patients with persistent rhinorrhea underwent reoperation
and their sinuses were obliterated. Rhinorrhea recurred in one
of these patients and led to meningitis and death 6 months
after surgery. Four patients (5%) experienced intracranial hematoma with resulting surgical evacuation in two cases. Three
hemorrhages occurred in the tumor bed; the fourth was a
remote contralateral, frontoparietal, epidural hematoma.
Three patients (3.8%) experienced seizures immediately after
surgery. Five patients (6.3%) had deep vein thrombosis and
two patients (2.5%) experienced pulmonary embolism. There
was no new permanent neurological deficit besides anosmia.
Table 6 summarizes postoperative complications according to
surgical approach.
Total removal was obtained in 72 patients (90%). Subtotal
removal was achieved in eight patients (10%) with tumors 4
cm or larger and capsule adherent to the optic nerve and/or
vascular structures, precluding safe, complete removal (Table
7). Two patients, one with total and one with subtotal removal,
had atypical (World Health Organization [WHO] Grade II)
meningiomas, whereas 78 patients had WHO Grade I tumors
(meningothelial, transitional, psammomatous, or secretory).
Postoperative Karnofsky score was 100 in 37 patients (46.3%),
90 in 28 patients (35.0%), 80 in 11 patients (13.8%), 70 in 3
patients (3.8%), and 50 in 1 patient who had a Karnofsky score
of 30 before surgery.
We examined retrospectively the postoperative history of
the 80 patients in this study, who are now 6 to 164 months
(average, 70.8 mo) from surgery, with telephone contact
and/or medical examination, as well as file review. Seventytwo patients (90.0%) are alive, 1 patient died 6 months after
OGM surgery of meningitis resulting from persistent rhinorrhea, 4 patients died of causes unrelated to surgery, and 3
patients (3.8%) who had total removal of their WHO I meningiomas were lost to follow-up.
www.neurosurgery-online.com
OLFACTORY GROOVE MENINGIOMA SURGERY
FIGURE 1. MRI scans showing common growth patterns of olfactory groove meningiomas in patients from this study.
There has been no clinical or radiographic (MRI) olfactory
groove recurrence documented to date in any of the 72 patients with total removal. Eight patients had subtotal removal.
Six of these patients are alive and have had no regrowth from
17 to 90 months after surgery (average, 63.5 mo). Residual
tumor showed growth on MRI images within 1 year of surgery
in two of these eight patients. One patient had multiple meningiomas at presentation, including a 6-cm OGM. Residual
tumor evidenced growth within 1 year after subtotal resection
via a bifrontal approach. He underwent surgery a second time
in this series with a subfrontal approach, and residual tumor
again showed growth on MRI within 1 year. He is alive 112
months after the second surgery, but his multiple meningiomata and his overall clinical state preclude further surgery.
The second patient underwent surgery at age 85 years via the
pterional approach for a 7-cm atypical meningioma. He demonstrated residual regrowth 1 year after surgery but did not
undergo reoperation. He died of a massive stroke 2 years after
surgery.
NEUROSURGERY
DISCUSSION
Surgical techniques have evolved a great deal since Cushings pioneering 1938 publication describing OGM removal in
22 patients through a unilateral subfrontal approach with
partial frontal lobe resection (6). Although OGM is the subject
of many publications, optimal surgical policy is still to be
defined. Today, the range of approaches varies from a very
wide bifrontal craniotomy (10) to minimally invasive endoscopic techniques (20) and craniofacial approaches (15, 23, 26,
34). For many years, unilateral or bifrontal craniotomy followed by subfrontal access to the tumor have been considered
standard approaches for OGM resection (4, 27, 29, 31, 35, 43,
45).
Mortality rates in the literature vary from 0% (18, 29, 32, 37,
46) to 17% (43) and even 22.7% (6) in the older literature.
Complications include postoperative epilepsy, postoperative
hematoma, hemiparesis, visual and mental deterioration, bone
flap infection, and CSF leak. Surgical approaches have contin-
VOLUME 57 | OPERATIVE NEUROSURGERY 4 | OCTOBER 2005 | ONS-271
SPEKTOR
ET AL.
ued to evolve over time. The pterional approach (17, 33, 46)
and approaches complemented with fronto-orbital osteotomies (1, 3, 40, 41) are now well described. There are also a few
reports describing removal of OGM through craniofacial (15,
23, 34) and subcranial approaches (13, 14, 21, 26).
In our experience, the procedure evolved from surgery
through a standard unilateral or bilateral subfrontal approach
to resection through a pterional approach, and later to pterional approach extended by fronto-orbital osteotomy and subcranial approach. Tables 6 to 10 describe the outcomes, advantages, and disadvantages of these surgical approaches.
Bifrontal Craniotomy with Subfrontal Approach
The advantage of the bilateral subfrontal approach, wide
symmetrical anterior cranial fossa exposure, is described in
many papers (10, 24, 29, 31, 35). This approach provides
excellent opportunity for radical tumor resection, drilling of
hyperostosis in the cribriform plate area of the planum sphe-
FIGURE 2. Diagrams
showing surgical approaches used for OGM resection in this study. A, bifrontal craniotomy with
subfrontal approach. B,
unilateral-frontal craniotomy with subfrontal approach. C, pterional approach. D, fronto-orbital approach. E, subcranial approach.
noidale and tuberculum sellae, and unroofing of optic nerves
when necessary.
Disadvantages are also well known. The frontal sinuses are
usually opened; nevertheless, the anterior inferior border of
the craniotomy is not low enough to prevent significant brain
retraction. In patients with large tumors, swollen brain often
herniates into the craniotomy window, frequently demanding
partial resection of a frontal lobe. The most important structuresthe optic apparatus, carotids, and the anterior communicating complexcome into view late, after a major part of
the tumor has been removed. The superior sagittal sinus
should be divided, compromising venous drainage from the
frontal lobes and thus contributing to brain edema. Preservation of olfaction is problematic.
In our series, 35 surgeries (43.8%) were performed with this
approach. Total resection was achieved in 31 surgeries, and
subtotal resection was achieved in 4 surgeries. There were no
recurrences in 32 patients during the observation period; 2
patients with total removal were lost to follow-up. One multiple meningiomata patient evidenced growth of his residual
tumor within the first year after surgery. Five patients had
CSF leak through the frontal sinuses, complicated with meningitis in three patients. Two patients had frontal contusion as
a result of retraction against swollen brain during the early
steps of surgery. Two patients experienced intraparenchymatous frontal hemorrhage; one hemorrhage required surgical
evacuation. Three patients experienced deep vein thrombosis,
one had a pulmonary embolism, and one experienced
convulsions.
Unilateral Frontal Craniotomy with
Subfrontal Approach
This approach has the advantage of sparing the contralateral
frontal lobe and the superior sagittal sinus. The disadvantages
include those described above. In addition, this approach provides only a small opening with a very narrow view.
Nine surgeries (11.1%) were
performed through a unilatTABLE 4. Tumor extension patterns according to surgical approach
eral subfrontal approach. We
achieved total resection in
Intracranial,
Intracranial and
Intracranial and
paranasal sinus,
seven patients and subtotal reIntracranial
optic nerve
paranasal sinus
Total
and optic nerve
section in two patients. One
involvement
extension
involvement
patient underwent surgery
twice in our series, first via a
Bifrontal
19
8
4
4
35
bifrontal approach and 1 year
Unilateral subfrontal
5
3
1
9
later via a subfrontal approach
after the tumor recurred. This
Pterional
13
4
1
18
same patient underwent reoperation for a persistent CSF
Fronto-orbital
1
6
7
leak after the subfrontal resecSubcranial
11
1
12
tion, and again experienced
tumor regrowth. No other paTotal surgeries
38
21
15
7
81a
tient experienced recurrence
a
Eighty-one surgeries were performed on 80 patients.
after subfrontal resection. One
patient experienced pulmo-
ONS-272 | VOLUME 57 | OPERATIVE NEUROSURGERY 4 | OCTOBER 2005
www.neurosurgery-online.com
OLFACTORY GROOVE MENINGIOMA SURGERY
shorter distance to the tumor
compared with the subfrontal route. The pterional apUnilateral
FrontoSize (cm)
Bifrontal
Pterional
Subcranial
Total (%)
proach also spares venous
subfrontal
orbital
structures (33) and provides
2
1
2
3 (3.7%)
the possibility of early tumor
detachment from the cranial
3 4
17
5
11
1
3
37 (45.7%)
base and debulking.
5 6
18
2
5
4
3
32 (39.5%)
The major disadvantage is
a narrow working angle. In
6
2
1
2
4
9 (11.1%)
patients with high-riding tumors, the upper part of the
Total surgeries
35
9
18
7
12
81 (100%)
tumor is in a blind area, and
significant brain retraction
may be demanded to visualize it. The working distance
TABLE 6. Complications according to surgical approacha
to the opposite side of meninNo. of CSF
gioma is very long. Orbital
Approach
Meningitis Bleeding Convulsion DVT PE Reoperation Death
patients leak
roof bulging obscures the olb
c
d
factory groove, and so signifBifrontal
35
5
3
2
1
3
1
2
1
icant frontal lobe retraction
Unilateral
9
1
1
1e
may be necessary to improve
subfrontal
the working angle.
Initially, we chose this apPterional
18
1
2
proach only for resection of
Fronto-orbital
7
1
2f
1g
relatively small tumors, but
with experience we also used
Subcranial
12
3
1
1
it for larger tumors, with the
Total
81
10
4
4
3
5
2
4
1
limitations mentioned above.
surgeries
We applied this approach for
a
removal of OGM in 18 surCSF, cerebrospinal fluid; DVT, deep vein thrombosis; PE, pulmonary embolus.
b
geries (22.2%), with total reTwo patients experienced hemorrhage in the surgical site.
c
One patient was reoperated for hemorrhage in the surgical site, one for persistent rhinorrhea.
section in 15 surgeries. Residd
In one patient, persistent rhinorrhea led to meningitis and death 6 months after surgery.
ual tumor increased in size
e
One patient reoperated for persistent rhinorrhea.
within the first year after surf
One patient developed a remote, contralateral, fontal parietal, epidural hematoma, and one experienced hemorrhage
gery in one patient operated
in the surgical site. The second patient experienced coagulopathy secondary to hepatic cirrhosis.
g
The contralateral epidermal hematoma was evacuated.
on at age 85 years who had
subtotal resection of his atypical 7-cm meningioma. He
experienced no complications, but died following a massive stroke 2 years after OGM
nary embolism. One patient with total removal of his WHO
surgery. Two other patients who had subtotal resection, a
Grade I meningioma was lost to follow-up.
72-year-old man and an 83-year-old woman, both with de
novo intracranial WHO Grade I meningiomas, as well as all
Pterional Approach
patients with total resection, are alive and have experienced
no tumor regrowth. One patient had convulsions, and two had
This relatively new approach to OGM (17, 46) provides
deep vein thrombosis. No patient operated on with the pteriseveral significant advantages, clearly described by Bricolo (5),
onal approach was lost to follow-up.
compared with the subfrontal approaches. It is less time consuming than bifrontal craniotomy and avoids CSF leak, because the frontal sinus is not transected. The basal cisterns may
Fronto-orbital Approach
be opened before the tumor is even touched, releasing the CSF
and providing fair brain relaxation. The optic nerve may be
Adding basal osteotomy to frontal, bifrontal, or pterional
localized and secured before the tumor is manipulated. The
craniotomy provides a lower angle of attack and eliminates
ipsilateral internal carotid artery comes into view early, and
the need for brain retraction. Al-Mefty (1) proposed widening
the anterior cerebral arteries may be followed into the tumor
bifrontal craniotomy with unilateral orbital rim osteotomy.
(Fig. 3). Turazzi et al. (46) proved that this approach provides
Sekhar et al. (40) perform frontotemporal craniotomy and
TABLE 5. Tumor size and surgical approach
NEUROSURGERY
VOLUME 57 | OPERATIVE NEUROSURGERY 4 | OCTOBER 2005 | ONS-273
SPEKTOR
ET AL.
We found this approach to
be the most suitable for resection of large, high-riding meMedian
Total
Subtotal
Residual
ningiomas. It has many adApproach
Recurrence
postoperative
resection
resection
regrowth
vantages, including benefits of
Karnofsky score
both the subfrontal and pteriBifrontal
31
4
1a
90
onal approaches. Orbital osa
teotomy brings the operator
Unilateral
7
2
1
90
immediately to the tumor insubfrontal
sertion, and the pterional comPterional
15
3
1
100
ponent of the approach enables early identification of the
Fronto-orbital
7
90
ipsilateral optic nerve and conSubcranial
12
100
trol over the internal carotid
artery. Orbital roof removal
Total
72
9b
0
3c
90
and frontozygomatic osteota
Olfactory groove meningioma regrew twice in this multiple meningiomata patient: once after initial bifrontal removal,
omy provide a direct angle of
and again after a second attempt at removal via a subfrontal approach.
attack and improved tumor
b
Includes two subtotal resections in two surgeries for one multiple meningiomata patient.
c
exposure, as proven quantitaIncludes residual regrowth twice after two surgeries in one multiple meningiomata patient.
tively by Schwartz et al. (39).
This approach offers the shortest working distance to the tumor, even in comparison with the pterional approach, and eliminates the need for brain retraction. As with pterional
TABLE 8. Surgical mortality in published olfactory groove
meningioma series
craniotomy, the basal cisterns are opened and the brain is relaxed
before tumor manipulation (Fig. 4). After tumor detachment and
No. of Operative
Series (ref. no.)
debulking, the upper posterior aspect of the tumor, usually inpatients mortality
volving the anterior communicating artery complex and hypoCushing and Eisenhardt, 1938 (6)
22
5 (22.7%)
thalamus, is easily accessed, as demonstrated by Schwartz et al.
The anterior cerebral arteries can be manipulated without brain
Solero et al., 1983 (43)
98
17 (17.3%)
retraction because of the lower attack angle.
Ojemann, 1991 (31)
17
1 (5.9%)
This approach provides the best conditions for brain preservation
without retraction and meticulous dissection. If necRansohoff and Nockels, 1993 (35)
33
2 (6.1%)
essary, the planum sphenoidale and tuberculum sellae may be
Schaller et al., 1994 (38)
28
1 (3.6%)
drilled and the optic nerves unroofed. After tumor resection,
there is much room for treatment of the anterior cranial base
Tsikoudas and Martin-Hirsch, 1999 (45)
13
2 (15%)
tumor insertion area. Reconstruction and closure are easy and
Turazzi et al., 1999 (46)
37
1 (2.7%)
not time consuming. This is now our approach of choice for
surgery of large OGMs.
Hentschel and DeMonte, 2003 (18)
13
0
The approach has disadvantages. It is more time consuming. The frontal sinus is frequently opened wide, necessitating
Obeid and Al-Mefty, 2003 (29)
15
0
its obliteration with a pericranial flap. However, when these
Present study
80
0a
sinuses are small, fronto-orbital osteotomy lateral to the sua
In one patient, persistent rhinorrhea led to meningitis and death 6 months
praorbital notch may obviate frontal sinus penetration.
after surgery.
We performed seven surgeries (8.6%) in patients with large
tumors using this approach. Six patients had optic nerve involvement and five had visual impairment before surgery. We
achieved total resection in all seven patients. Six of seven
half-frontal craniotomy, and then add an orbital osteotomy
patients are alive and have had no recurrence. One woman
just across the midline. Babu et al. (3) combine frontal cranioperated on at age 73 years died later with no evidence of
otomy with orbital osteotomy.
recurrence. In one patient, CSF leak developed through the
We perform fronto-orbital craniotomy as described by
ethmoidal sinus, which was opened during extensive cranial
Delashaw et al. (7), removing a bone flap that includes the
base drilling. A pericranial flap laid over the defect did not
orbital rim and frontozygomatic process of the frontal bone in
prevent this complication. The CSF leak was cured by several
a single piece. We modify this approach by placing the posdays of spinal drainage. Two patients experienced hemorterior border of the craniotomy further back, as in frontotemrhage. One of them had a contralateral epidural hematoma
poral (pterional) craniotomy.
TABLE 7. Outcome according to surgical approach
ONS-274 | VOLUME 57 | OPERATIVE NEUROSURGERY 4 | OCTOBER 2005
www.neurosurgery-online.com
OLFACTORY GROOVE MENINGIOMA SURGERY
This approach is not our
first choice. We use it only for
patients with primary or reNo. of
% total
%
Series (ref. no.)
Follow-up, yr (range)
current tumors invading the
patients resection
recurrence
paranasal sinuses and/or the
Mirimanoff et al., 1985 (25)a
22
77.3
5
30
orbits. In this series, 12 operations were performed with
10
41
the subcranial approach. Six
Tsikoudas and Martin-Hirsch, 1999 (45)
13
100
Approximately 10 (122)
30.8
patients had been operated
on elsewhere through subTurazzi et al., 1999 (46)
37
100
Average, 4 (1 8)
0
frontal, frontal, or pterional
approaches from 1 to 6 years
Hentschel and DeMonte, 2003 (18)
13
84.6
Average, 2 (0 5)
0
earlier (average, 3.5 yr). All
Obeid and Al-Mefty, 2003 (29)
15
93.3
Average, 3.7 (17.3)
0
12 patients had meningiomas
penetrating into ethmoidal
Present study
80
90
Average, 5.9 (0.513.7)
2.5
and/or frontal sinuses. In
a
Mirimanoff et al. reported recurrance rates separately for patients who were followed for 5 and 10 years after surgery.
one patient, the tumor involved orbits and optic canals, necessitating extensive
that was evacuated surgically. The second patient, who had
drilling. Total resection was achieved in all 12 procedures. All
cirrhosis and coagulopathy, experienced a hemorrhage in the
patients initially were managed with postoperative spinal
tumor bed that dissolved without surgical intervention. No
drain. Three had significant CSF leak during the first days
patient operated on with this approach was lost to follow-up.
after surgery that demanded some extra period of spinal
drain. One patient experienced meningitis, and one had convulsions. All patients operated on with this approach are alive
Subcranial Approach
with no clinical or imaging evidence of OGM recurrence.
This approach, described elsewhere (13, 36), was developed for
removal of invasive cranial base tumors, mainly by ENT surgeons.
Choosing the Optimal Approach and
We applied the subcranial approach for resection of 12 OGMs.
Recurrence Prevention
The advantage to this approach is wide exposure of the intracranial anterior cranial base compartment in continuity with
Technical developments and improved microsurgical techneighboring structures, including the frontal, sphenoid, and ethniques have significantly reduced mortality rates after OGM
moidal sinuses, the orbits, and the nasal cavity. The optic canal
resection from 17.3 to 22.7% (6, 43), to nearly 0% (46) (Table 8).
may be drilled, exposing the optic nerves and removing the
Current debate regarding surgical strategy and tactics focuses
tumor from the optic canals. This access provides optimum conon the extent of tumor resection and the optimal approach.
ditions for radical tumor removal (Figs. 5 and 6). The disadvanThe ideal, most radical resection is Simpson Grade I, which
tage of the approach is its greater technical difficulty, including
demands bone drilling beneath the tumor insertion (42). Hiscomplex reconstruction. Both the approach and reconstruction
torically, some authors (22, 31, 32, 35) weighed the high risk of
are time consuming. A spinal drain is obligatory to avoid perCSF leak, potentially complicated with meningitis, against the
manent postoperative CSF leak.
potential for recurrence after radical anterior cranial base drilTABLE 9. Resection and rates of recurrence in published olfactory groove meningioma series
TABLE 10. Comparison of surgical approachesa
Paranasal
sinus
transection
Brain retraction
SSS
ligation
CSF leak
Surgical field
exposure
Complexity
Time
consuming
Approach
Yes
Significant
Yes
High risk
Good
Moderate
Yes
Very significant
No
Moderate risk
Poor
Low
Unilateral subfrontal
No
Moderate
No
Low risk
Good
Low
Pterional
Yes
Slight
No
Moderate risk
Very good
Moderate
Yes
Slight
No
High risk
Very good
High
Bifrontal
Fronto-orbital
Subcranial
SSS, superior sagittal sinus; CSF, cerebrospinal fluid; , relative amount of time.
NEUROSURGERY
VOLUME 57 | OPERATIVE NEUROSURGERY 4 | OCTOBER 2005 | ONS-275
SPEKTOR
ET AL.
FIGURE 3. Illustrations of the pterional approach. A, T1-weighted
gadolinium-enhanced axial MRI scan demonstrating a large OGM. B, a
retractor (R) has been introduced beneath the frontal lobe and the parachiasmatic cistern has been opened, providing excellent visualization of the
caudal part of the tumor (T), the right olfactory tract (OT), the optic
nerve (ON), and internal carotid artery (ICA).
ling and recommended only prudent drilling of the cranial
base. Indeed, the rate of OGM recurrence is relatively low in
some reports (31, 35, 43). However, other studies demonstrated OGM recurrence rates of up to 30% over 10 years in
patients whose tumor is not radically removed (45). Mirimanoff et al. (25) reported 30% recurrence rates for OGM
meningiomas at 5 years and 41% at 10 years after surgery
(Table 9).
In recent publications, there is an obvious trend toward
more aggressive tumor resection. Obeid and Al-Mefty (29)
and Hentschel and DeMonte (18) advocate radical tumor resection, including drilling of hyperostotic bone and pursuing
tumor extending into the paranasal sinuses, with consequent
meticulous cranial base reconstruction. We strongly support
this concept.
DeMonte (8) notes that at least 15% of OGMs grow into the
ethmoidal sinuses. In our series, 21 patients (26.3%) demonstrated extension to the paranasal sinuses, including 6 patients
with both paranasal sinus and optic nerve involvement. Morris et al. (28) stress that extracranial spread of OGM should not
be underappreciated, because managing regrowth of residual
disease is difficult, and suggest radical resection in the first
instance. All four of their patients sought treatment at the ENT
service.
Nine patients in our series were operated on elsewhere and
had recurrent tumors at presentation. We observed similar
regrowth patterns. Recurrent tumor originating from the periphery of the original tumor typically involved the falx and
anterior cranial basethe cribriform plate, planum sphenoidal, and tuberculum sellae, expanding downward into the
ethmoidal sinusesand sometimes invaded the dura of the
optic nerves (Figs. 5 and 6).
Some patients who develop recurrent tumor expanding into
the paranasal sinuses or orbits may be referred to ENT surgeons and be lost to neurosurgical follow-up. In our series,
ENT surgeons diagnosed six patients with recurrent tumor
involving the ethmoidal, sphenoidal, and frontal sinuses, nasal cavity, orbits, and even the optic canals. All had been
ONS-276 | VOLUME 57 | OPERATIVE NEUROSURGERY 4 | OCTOBER 2005
FIGURE 4. Illustrations of the fronto-orbital approach. A and B,
T1-weighted gadolinium-enhanced coronal (A) and sagittal (B) MRI scans
demonstrating a large OGM. C, intraoperative photograph of right-sided,
fronto-orbital osteotomy. D, macroscopic view after a right-sided, frontoorbital approach has been performed and the dura mater opened. Note perfect brain relaxation. With the naked eye, and without retraction, the right
optic nerve is visualized perfectly at the posterior end of the tumor
(arrow). FL, frontal lobe; T, tumor; BD, basal dura mater. E and F, postoperative T1-weighted gadolinium-enhanced (E) coronal and (F) sagittal
MRI scans demonstrating radical tumor removal.
operated on elsewhere by neurosurgeons. Several of these
patients were definitely informed by their surgeons that their
tumors had been totally removed. The cases of these patients
demanded a subcranial approach with extensive anterior cranial base drilling, which was not performed during primary
removal. Reoperation was definitely more challenging because of scars and adhesions from the earlier procedures, as
well as the need to unroof and manipulate the optic nerves
and to perform extensive cranial base reconstruction. We cannot accept that prudent drilling of the anterior cranial base
is sufficient to prevent tumor recurrence.
Several approaches with different levels of complexity have
been proposed for the surgical treatment of meningiomas with
extensive anterior cranial base involvement. Persky and Som
(34) suggested a combination frontal craniotomy and lateral
www.neurosurgery-online.com
OLFACTORY GROOVE MENINGIOMA SURGERY
FIGURE 6. Images from a patient who had
undergone surgery for OGM via a rightsided pterional craniotomy 5 years earlier. A,
intraoperative macroscopic picture at an early
step of a subcranial approach. B and C, T1-weighted gadolinium-enhanced
coronal MRI scans. Note tumor spread along the falx and ethmoidal sinus
invasion.
FIGURE 5. Illustrations of the subcranial approach. AD, T1-weighted
gadolinium-enhanced sagittal (A), coronal (B), and axial (C and D) MRI scans
demonstrating recurrent OGM invading the ethmoidal sinus and right orbit. EG,
intraoperative macroscopic pictures of the subcranial approach. HK, T1-weighted
gadolinium-enhanced sagittal (H), coronal (I), and axial (J and K) MRI scans
demonstrating absence of the tumor and anterior cranial base reconstruction with the
fascia lata (H, arrow).
NEUROSURGERY
rhinotomy. Maiuri et al. (23) used combined subfrontal and
nasal approaches. Goffin et al. (15) selected craniofacial resection. A telecanthal approach was proposed by Fujitsu et al.
(14), and Hallacq et al. (16) operated using a frontal sinus
approach. Ohata et al. (30) suggested a bi-orbitofrontobasal
interhemispheric approach.
We applied the subcranial approach in 12 patients and
consistently achieved excellent tumor exposure. All 12 had
extensive paranasal sinus and/or orbital involvement. Six had
local recurrence secondary to the lack of meticulous tumor
removal from all surrounding structures. Tumor has not recurred in these patients after their second surgery. These
patients have been followed for 11 to 105 months (average,
62.3 mo) after surgery. Moore et al. (26) also concluded that
the subcranial approach is preferable to traditional frontal
craniotomy combined with lateral rhinotomy. We did not find
more extensive approaches necessary.
The choice of approach is clearly important and probably
contributes to the near zero mortality and reduced morbidity
rates reported in some recent papers describing experience
with the pterional approach (17, 46). However, we do not
believe that the pterional approach is entirely responsible for
improved outcomes with these patients compared with earlier
reports. Certainly widespread improvements in surgical techniques and instrumentation also contributed significantly to
these excellent results.
We present here the largest OGM series with the longest
follow-up published in modern neurosurgical literature based
on an integrated, multidisciplinary approach to OGM patient
management and using a variety of surgical techniques. We
have achieved good clinical resultszero operative mortality,
low morbidity, and very low recurrence rates. Based on our
VOLUME 57 | OPERATIVE NEUROSURGERY 4 | OCTOBER 2005 | ONS-277
SPEKTOR
ET AL.
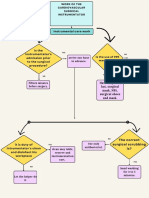
experience with multiple surgical approaches, we tried to
introduce an algorithm facilitating the choice of an optimal
approach for OGM removal in each situation (Table 10).
We find that the pterional, fronto-orbital, and subcranial
approaches generally are the most effective. For small tumors
that are purely intracranial and do not involve the anterior
cranial base, a regular pterional approach is sufficient. Large
and very large high-riding OGMs are better removed via the
fronto-orbital approach, because swollen brain pushes such
tumors downward as soon as part of the anterior cranial base
is removed. The fronto-orbital approach also enables sufficient
resection of meningiomas with moderate anterior cranial base
invasion. Tumors that have significantly infiltrated the anterior cranial base, invaded ethmoidal and sphenoid sinuses,
and extended into the nasal cavity and orbits are best removed
through the subcranial approach. The goal of OGM surgery
should be radical resection. Hyperostotic bone and sinus invasion are not limitations.
CONCLUSION
OGMs should be approached with the techniques and attitudes applied to cranial base tumors. Modern microsurgical
techniques and careful choice of surgical approach help to
achieve excellent results in the surgical treatment of OGMs.
REFERENCES
1. Al-Mefty O: Tuberculum sellae and olfactory groove meningioma, in Sekhar
LN, Janecka IP (eds): Surgery of Cranial Base Tumors. New York, Raven Press,
1993, pp 507519.
2. Al-Mefty O, Smith R: Tuberculum sellae meningiomas, in Al-Mefty O (ed):
Meningiomas. New York, Raven Press, 1991, pp xix, 395411, 630.
3. Babu R, Barton A, Kasoff SS: Resection of olfactory groove meningiomas:
Technical note revisited. Surg Neurol 44:567572, 1995.
4. Bakay L, Cares HL: Olfactory meningiomas: Report on a series of twentyfive cases. Acta Neurochir (Wien) 26:112, 1972.
5. Bricolo A: Commentary on Babu R, Barton A, Kasoff SS. Resection of
olfactory groove meningiomas: Technical note revisited. Surg Neurol 44:
567572, 1995.
6. Cushing H, Eisenhardt L: The olfactory meningiomas with primary anosmia, in Cushing H, Eisenhardt L (eds): Meningiomas: Their Classification,
Regional Behavior, Life History, and Surgical Results. Springfield, Charles C
Thomas, 1938, pp 250282.
7. Delashaw JB Jr, Jane JA, Kassell NF, Luce C: Supraorbital craniotomy by
fracture of the anterior orbital roof: Technical note. J Neurosurg 79:615618,
1993.
8. DeMonte F: Surgical treatment of anterior basal meningiomas. J Neurooncol
29:239248, 1996.
9. Derome PJ, Guiot G: Bone problems in meningiomas invading the base of
the skull. Clin Neurosurg 25:435451, 1978.
10. El Gindi S: Olfactory groove meningioma: Surgical techniques and pitfalls.
Surg Neurol 54:415417, 2000.
11. Fliss DM: Skull base reconstruction after anterior subcranial tumor resection. Neurosurg Focus 12(5):Article 10, 2002.
12. Fliss D, Zucker G, Amir A, Gatot A, Cohen M, Spektor S: The subcranial
approach for anterior skull base tumors. Otolaryngol Head Neck Surg
11:238253, 2000.
13. Fliss DM, Zucker G, Cohen A, Amir A, Sagi A, Rosenberg L, Leiberman A,
Gatot A, Reichenthal E: Early outcome and complications of the extended
subcranial approach to the anterior skull base. Laryngoscope 109:153160,
1999.
ONS-278 | VOLUME 57 | OPERATIVE NEUROSURGERY 4 | OCTOBER 2005
14. Fujitsu K, Saijoh M, Aoki F, Sakata K, Fujii S, Mochimatsu Y, Kuwabara T:
Telecanthal approach for meningiomas in the ethmoid and sphenoid sinuses. Neurosurgery 28:714720, 1991.
15. Goffin J, Fossion E, Plets C, Mommaerts M, Vrielinck L: Craniofacial resection for anterior skull base tumours. Acta Neurochir (Wien) 110:3337, 1991.
16. Hallacq P, Moreau JJ, Fischer G, Beziat JL: Frontal sinus approach to olfactory groove meningiomas [in French]. Neurochirurgie 45:329337, 1999.
17. Hassler W, Zentner J: Pterional approach for surgical treatment of olfactory
groove meningiomas. Neurosurgery 25:942947, 1989.
18. Hentschel S, DeMonte F: Olfactory groove meningiomas. Neurosurg Focus
14(6):Article 4, 2003.
19. Jallo GI, Benjamin V: Tuberculum sellae meningiomas: Microsurgical anatomy and surgical technique. Neurosurgery 51:14321440, 2002.
20. Jho HD, Alfieri A: Endoscopic glabellar approach to the anterior skull base:
A technical note. Minim Invasive Neurosurg 45:185188, 2002.
21. Kawakami K, Yamanouchi Y, Kawamura Y, Matsumura H: Operative approach to the frontal skull base: Extensive transbasal approach. Neurosurgery 28:720725, 1991.
22. Lagares A, Lobato RD, Castro S, Alday R, De la Lama A, Alen JF, Gonzalez
P: Meningioma of the olfactory groove: review of a series of 27 cases [in
Spanish]. Neurocirugia (Astur) 12:1722, 2001.
23. Maiuri F, Salzano FA, Motta S, Colella G, Sardo L: Olfactory groove meningioma with paranasal sinus and nasal cavity extension: removal by combined subfrontal and nasal approach. J Craniomaxillofac Surg 26:314317,
1998.
24. Mayfrank L, Gilsbach JM: Interhemispheric approach for microsurgical
removal of olfactory groove meningiomas. Br J Neurosurg 10:541545, 1996.
25. Mirimanoff RO, Dosoretz DE, Linggood RM, Ojemann RG, Martuza RL:
Meningioma: Analysis of recurrence and progression following neurosurgical resection. J Neurosurg 62:1824, 1985.
26. Moore CE, Ross DA, Marentette LJ: Subcranial approach to tumors of the
anterior cranial base: Analysis of current and traditional surgical techniques.
Otolaryngol Head Neck Surg 120:387390, 1999.
27. Morley T: Tumors of the cranial meninges, in Youmans J (ed): Neurological
Surgery. Philadelphia, W.B. Saunders, 1973, pp 13881411.
28. Morris KM, Campbell D, Stell PM, MacKenzie I, Miles JB: Meningiomas
presenting with paranasal sinus involvement. Br J Neurosurg 4:511515,
1990.
29. Obeid F, Al-Mefty O: Recurrence of olfactory groove meningiomas. Neurosurgery 53:534543, 2003.
30. Ohata K, Hakuba A, Nagai K, Morino M, Iwa Y: A biorbitofrontobasal
interhemispheric approach for suprasellar lesions. Mt Sinai J Med 64:217
221, 1997.
31. Ojemann RG: Olfactory groove meningiomas, in Al-Mefty O (ed): Meningiomas. New York, Raven Press, 1991, pp 383392.
32. Ojemann RG, Swan K: Surgical management of olfactory groove, suprasellar
and medial sphenoid ridge meningiomas, in Schmidek HH, Sweet WH
(eds): Operative Neurosurgical Techniques. Orlando, Grune & Stratton, 1988,
pp 531545.
33. Paterniti S, Fiore P, Levita A, La Camera A, Cambria S: Venous saving in
olfactory meningiomas surgery. Clin Neurol Neurosurg 101:235237, 1999.
34. Persky MS, Som ML: Olfactory groove meningioma with paranasal sinus
and nasal cavity extension: A combined approach. Otolaryngology 86:ORL714ORL-720, 1978.
35. Ransohoff J, Nockels R: Olfactory groove and planum meningiomas, in
Apuzzo M (ed): Brain Surgery: Complication Avoidance and Management. New
York, Churchill Livingstone, 1993, pp 177185.
36. Raveh J, Laedrach K, Speiser M, Chen J, Vuillemin T, Seiler R, Ebeling U,
Leibinger K: The subcranial approach for fronto-orbital and anteroposterior
skull-base tumors. Arch Otolaryngol Head Neck Surg 119:385393, 1993.
37. Samii M, Ammirati M: Olfactory groove meningiomas, in Samii M (ed):
Surgery of the Skull Base: Meningiomas. Berlin, Springer-Verlag, 1992, pp
1525.
38. Schaller C, Veit R, Hassler W: Microsurgical removal of olfactory groove
meningiomas via the pterional approach. Skull Base Surg 4:189192, 1994.
www.neurosurgery-online.com
OLFACTORY GROOVE MENINGIOMA SURGERY
39. Schwartz MS, Anderson GJ, Horgan MA, Kellogg JX, McMenomey SO,
Delashaw JB Jr: Quantification of increased exposure resulting from orbital
rim and orbitozygomatic osteotomy via the frontotemporal transsylvian
approach. J Neurosurg 91:10201026, 1999.
40. Sekhar LN, Nanda A, Sen CN, Snyderman CN, Janecka IP: The extended
frontal approach to tumors of the anterior, middle, and posterior skull base.
J Neurosurg 76:198206, 1992.
41. Sekhar LN, Tzortzidis F: Resection of tumors by the fronto-orbital approach,
in Sekhar LN, de Oliveira EP (eds): Cranial Microsurgery: Approaches and
Techniques. New York, Thieme, 1999, pp 6175.
42. Simpson D: The recurrence of intracranial meningioma after surgical treatment. J Neurol Neurosurg 20:2239, 1957.
43. Solero CL, Giombini S, Morello G: Suprasellar and olfactory meningiomas: Report
on a series of 153 personal cases. Acta Neurochir (Wien) 67:181194, 1983.
44. Symon L: Olfactory groove and suprasellar meningioma, in Krayenbhl H
(ed): Advances and Technical Standards in Neurosurgery. New York, SpringerVerlag, 1983, p 67.
45. Tsikoudas A, Martin-Hirsch DP: Olfactory groove meningiomas. Clin
Otolaryngol 24:507509, 1999.
46. Turazzi S, Cristofori L, Gambin R, Bricolo A: The pterional approach for the
microsurgical removal of olfactory groove meningiomas. Neurosurgery
45:821826, 1999.
47. Yasargil MG: Microneurosurgery. New York, Thieme Stratton, 1984.
Acknowledgment
We thank Shifra Fraifeld for her help in preparing this manuscript.
rhinorrhea, and seizure prophylaxis that is usually begun
intraoperatively.
Smaller tumors can be removed using the pterional approach. In
larger tumors, we prefer to have an additional midline access as well.
This makes it possible to divide the anterior falx if necessary. The
reason we like to have midline access for larger tumors is that the
ipsilateral optic nerve may conceal part of the tumor behind it, requiring perhaps undue surgical manipulation of the optic nerve to visualize and free this tumor portion. In addition, in larger tumors, the
craniotomy is augmented with a fronto-orbital-clinoidal extradural
cranial base dissection. Such a dissection that includes removal of the
supraorbital rim brings the surgeon even closer to the tumor and
affords additional maneuvering space without the need for brain
retraction. Our technique of sinus closure includes either exenteration
of the frontal sinus mucosa or stripping away and collapsing it toward
the frontonasal canal, packing the sinus with an autologous fat graft
and using a vascularized pericranial flap to seal off the frontal sinuses
from the operative site by tacking the pericranial flap to the underlying dura with a surface- to- surface suture technique.
As far as accomplishing a complete tumor removal (Simpson 1) we
tend to strike a balance between the degree of cranial base removal
and the potential for postoperative complications, especially a CSF
rhinorrhea. Our recurrence rate after the removal of OGMs has been
lower compared with meningiomas in other locations.
Ivan S. Ciric
Evanston, Illinois
COMMENTS
his is a retrospective review of 80 olfactory groove meningiomas
(OGM) operated on over a period of approximately 13 years. The
authors describe their surgical technique and outcomes. Close to
one-half of the operations were performed using a bifrontal craniotomy approach. The other surgical approaches included a unilateral
frontal craniotomy, a parietal craniotomy, a fronto-orbital-zygomatic
craniotomy, and a subcranial cranial base approach. The authors
discuss advantages and disadvantages of each approach.
Although most of the operations were performed using the bifrontal
craniotomy approach, the authors do not seem to advocate this approach.
Instead, they favor the pterional approach, with or without the addition
of the fronto-orbital-zygomatic cranial base dissection. They base their
recommendation on several factors, including avoidance of brain retraction, access to the basal cisterns, the potential for a cerebrospinal fluid
(CSF) leak, and the complexity of cranial base reconstruction. The authors
claim no neurological morbidity other than anosmia in any of their 80
cases. On the other hand, they report an approximately 30% operative
morbidity (mostly consisting of CSF leakage, and a few cases of meningitis, seizures, deep vein thrombosis, etc.).
I fully agree with the authors that the choice of the operative
approach should be tailored to the tumor location, size (high riding or
not), relationship to the carotid arteries and its branches, presence or
absence of significant preoperative frontal lobe vasogenic edema
and/or visual deficits, and many other factors.
The principles for removal of OGMs in our practice have been very
similar to those of other cranial base operations: an exposure that
would bring the surgeon close to the tumor, early release of CSF so as
to allow for brain relaxation, avoidance of brain retraction, meticulous
preservation of all arterial and venous channels not belonging to the
tumor capsule, adequate internal decompression of the tumor before
the tumor capsule is separated from the surrounding neuro-vascular
structures along the tumor capsule-arachnoid interface, meticulous
closure of the open sinus cavities so as to prevent a postoperative CSF
NEUROSURGERY
he authors present what could be one of the largest series of OGMs
treated using different surgical approaches chosen on the basis of
the characteristics of the tumors. The criteria they use in their decisions are acceptable and are in line with what is found in the literature. The results achieved are good, and one may have the impression
of an accurate and competent management of this pathology. In the
article, the authors show their preference toward the bilateral subfrontal approach in agreement with a consolidated tendency; and the
majority of their patients are operated on with this approach. The
same authors emphasize some limits of the pterional approach, which
in our hands (1) we do not encounter, such as the difficulty in drilling
the osteoma at the olfactory groove and in controlling the controlateral
tumor expansion. The pterional approach allows a safer dissection of
the optic nerves and of the anterior arteries of the Willis Circle as well
as the frontobasal ones, with little or no damage to the basal frontal
lobe as stated by Yasargils comment on our above-mentioned article
(1). The problem of recurrences from the ethmoidal plane, which is
managed in cooperation with ear, nose, and throat surgeons, is commented on exhaustively, whereas posterior recurrences in the parasellar area, which are often difficult to treat, are never mentioned. Nor
is the possibility of preserving the olfaction mentioned, which may
give great satisfaction using the pterional approach. In conclusion, the
article presents a large caseload that is well treated and managed,
following present trends.
Sergio Turazzi
Albino Bricolo
Verona, Italy
1. Turazzi A, Cristofori L, Gambin R, Bricolo A: The pterional approach for the
microsurgical removal of olfactory groove meningiomas. Neurosurgery 45:
821826, 1999.
VOLUME 57 | OPERATIVE NEUROSURGERY 4 | OCTOBER 2005 | ONS-279
SPEKTOR
ET AL.
he authors report their experience during a 13-year period with 80
patients who underwent a surgical treatment (81 OGM surgeries).
This well-written article describes the different techniques for access to
meningiomas in the olfactory grove. The authors review the potential
advantages and disadvantages associated with the use of determined
surgical approach to OGMs, as well as outcomes and recurrence rates. In
this series, the main approaches were through bifrontal craniotomy,
unilateral subfrontal approach, pterional approach with fronto-orbital
craniotomy, and subcranial approach. Total removal was obtained in
90% of the patients, subtotal in 10%. No operative mortality and no new
permanent focal neurological deficit other than anosmia were identified
in this series. However, 31.3% developed surgery-related complications.
These patients outcomes prove that proper use of modern microsurgical
techniques leads to excellent results.
Given the increasing number of operations on the anterior fossa in
patients with OGMs, the selection of the most appropriate approach is
especially important. Previous publications have described many surgical managements of these tumors. For patients with large and small
OGMs, we prefer the extended frontopterional approach. This approach
may accomplish complete removal and the preservation of vascular
structures surrounding the tumor. During the craniotomy, care is taken
at the frontobasal anterior extension to reach the midline (falx and crista).The dissection of the Sylvian fissure is very important and is followed
by opening the carotid and interpeduncular cisterns. These procedures
allow the release of CSF and relaxation of the brain. The pterional
approach also allows early visualization of the neurovascular structures
and their dissection. Control of the posterior part of the tumor in relation
to the most important structures (optic nerves and internal carotid artery)
may be obtained by this approach. Dissection of the anterior cerebral
arteries from the capsule may prove difficult because of adherence or
encasement. The artery recurrent of Heubner should always be preserved during the dissection. A bifrontal approach is more direct to the
tumors. However, in our opinion the late visualization of the optic nerves
and the anterior cerebral complex are disadvantageous points to be
considered in the choice of this approach.
Evandro P. de Oliveira
So Paulo, Brazil
pector et al. have reported a large series of OGMs operated on over
a 13-year period with excellent results. They used a variety of
approaches to these tumors. The patients were not selected for theapproaches in any prospective fashion. However, their comments regarding the operative approaches are useful.
ONS-280 | VOLUME 57 | OPERATIVE NEUROSURGERY 4 | OCTOBER 2005
I agree that for small tumors, a small pterional craniotomy, with an
orbitotomy is adequate. For larger tumors, I use an unilateral frontotempororal craniotomy, with unilateral orbitotomy. For giant-sized
tumors, I prefer a frontotemporal craniotomy which extends just
across the midline, with an orbitotomy which also extends across the
midline. In smaller tumors, preservation of olfaction, at least on the
contralateral side, is possible, and preferable. For the larger tumors,
layered cranial base reconstruction is very important to avoid CSF
leakage. The surgeon should be aware of where these tumors tend to
recur, especially near the optic canal, in the anterior fossa bones, and
in the ethmoid sinus. Particularly in younger patients, these areas
should receive careful attention during the resection.
More recently, some surgeons have been using an endoscopic approach to the resection of these tumors. While it has the advantage of
no brain retraction, the various critical structures are seen at the end
of the operation, or not very well, and if there is a vascular injury, it
would be very difficult to manage by the endoscopic approach. CSF
leakage has been a problem for the endoscopic approaches. These
surgeons seem to be performing mostly partial tumor resection and
radiosurgery for the larger tumors, and have not published any surgical series of resection and follow-up. For the present, such endoscopic approaches may remain primarily in the hands of selected
surgeons, because of safety and efficacy issues.
Laligam N. Sekhar
Seattle, Washington
his is a pretty large series of OGMs (N80) treated by different
surgical approaches. The results are excellent with no mortality
after complete removal in 90% of the cases. Certainly, the best treatment is radical resection which is better achieved through a subfrontal
approach with deposition of the medial part of the fronto-orbital
ridge. This approach is useful in resecting completely the zone of
insertion including the bone and, when it exists, the ethmoidonasal
extension of the meningioma. This is not possible with the pterional
approach and is difficult with a single standard of subfrontal approach. This article nicely reviews the advantages and disadvantages
of each technique and the complications (mostly CSF leak) related to
them. A better assessment of the benefits of each approach could have
been done with cognitive and psychometric tests.
Bernard George
Paris, France
www.neurosurgery-online.com
S-ar putea să vă placă și
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- Ielts Writing Task 1Document123 paginiIelts Writing Task 1Adalat Adel97% (72)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (587)
- Neil McDonald - Master Class - Typical MistakesDocument16 paginiNeil McDonald - Master Class - Typical MistakeskarahmanÎncă nu există evaluări
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (890)
- Water&Environmental EngDocument33 paginiWater&Environmental EngMd Jony AhmedÎncă nu există evaluări
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- 15 Days Practice For IELTS WritingDocument174 pagini15 Days Practice For IELTS WritingnguyenbatiepÎncă nu există evaluări
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (399)
- Edmar Mednis, Colin Crouch - Rate - Your - EndgameDocument252 paginiEdmar Mednis, Colin Crouch - Rate - Your - Endgamekarahman100% (6)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (73)
- MigraineDocument106 paginiMigrainekarahmanÎncă nu există evaluări
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- The Brain and The Nervous System (The Human Body)Document281 paginiThe Brain and The Nervous System (The Human Body)Hameleo1000100% (1)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- 15 Days Practice For IELTS ReadingDocument281 pagini15 Days Practice For IELTS ReadingHampson Malekano100% (1)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- ICP Waveform Analysis J Ball 2004Document16 paginiICP Waveform Analysis J Ball 2004karahmanÎncă nu există evaluări
- Mastering Tactical Ideas-Im Nikolay MinevDocument237 paginiMastering Tactical Ideas-Im Nikolay Minevkarahman100% (3)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- Modification of VP Shunt IntroducerDocument2 paginiModification of VP Shunt IntroducerkarahmanÎncă nu există evaluări
- Angus Dunnington-Understanding The SacrificeDocument140 paginiAngus Dunnington-Understanding The Sacrificekarahman100% (6)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- Neil McDonald - Master Class - Typical MistakesDocument16 paginiNeil McDonald - Master Class - Typical MistakeskarahmanÎncă nu există evaluări
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- Dan Heisman-Everyones 2nd ChessbookDocument129 paginiDan Heisman-Everyones 2nd Chessbookkarahman90% (10)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2219)
- Angus Dunnington-Understanding The SacrificeDocument140 paginiAngus Dunnington-Understanding The Sacrificekarahman100% (6)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- Chess Middlegame PlanningDocument229 paginiChess Middlegame Planningfokionas100% (33)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- Injury: Clinically Its Defined As Solution or Disruption of The Anatomical Continuity of Any Tissues of The BodyDocument83 paginiInjury: Clinically Its Defined As Solution or Disruption of The Anatomical Continuity of Any Tissues of The BodykarahmanÎncă nu există evaluări
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (265)
- Head Injury - the silent epidemicDocument52 paginiHead Injury - the silent epidemickarahmanÎncă nu există evaluări
- FPG 007 CriticalCareinNeurology 2012Document119 paginiFPG 007 CriticalCareinNeurology 2012Pintu Mahligai100% (2)
- Traumatic Subarachnoid Hemorrhage - Demographic ... (Neurosurgery. 2002) - PubMed - NCBIDocument2 paginiTraumatic Subarachnoid Hemorrhage - Demographic ... (Neurosurgery. 2002) - PubMed - NCBIkarahmanÎncă nu există evaluări
- Andrew Soltis - Grandmaster Secrets, EndingsDocument224 paginiAndrew Soltis - Grandmaster Secrets, Endingskarahman100% (5)
- Brachial Plexus InjuriesDocument345 paginiBrachial Plexus Injuriesmohamedwhatever100% (2)
- Rural MEdical Camps - PDF FinalDocument32 paginiRural MEdical Camps - PDF FinalKashish KhuranaÎncă nu există evaluări
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- OsteomyelitisDocument7 paginiOsteomyelitis4kscribd100% (1)
- Going Under General Anesthesia With A ColdDocument3 paginiGoing Under General Anesthesia With A ColdColtonÎncă nu există evaluări
- Basmajian 2019Document21 paginiBasmajian 2019Santiago MartinezÎncă nu există evaluări
- OPD Schedule of Specialists at Venkateshwar HospitalDocument2 paginiOPD Schedule of Specialists at Venkateshwar HospitalVenkateshwar HospitalÎncă nu există evaluări
- Colonial Adaptations in Tropical Asia: Spanish Medicine in The Philippines in The Seventeenth and Eighteenth CenturiesDocument16 paginiColonial Adaptations in Tropical Asia: Spanish Medicine in The Philippines in The Seventeenth and Eighteenth CenturiesKeshaÎncă nu există evaluări
- Perception and Coordination Concepts in Orthopedic, Neurology and ENT NursingDocument15 paginiPerception and Coordination Concepts in Orthopedic, Neurology and ENT NursingKakaiÎncă nu există evaluări
- Scrubbing Up Policy for Dorset Primary Care TrustDocument9 paginiScrubbing Up Policy for Dorset Primary Care TrustAzwar ArigaÎncă nu există evaluări
- Journal Abdominal SurgeryDocument4 paginiJournal Abdominal SurgeryrizkaÎncă nu există evaluări
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (119)
- Pravilnik o Vigilanci Engleski FinalDocument58 paginiPravilnik o Vigilanci Engleski FinalSlaviša ŠimetićÎncă nu există evaluări
- Abdul Malik PresenttionDocument18 paginiAbdul Malik PresenttionAfzalDaadÎncă nu există evaluări
- Spinal Injection TechniquesDocument310 paginiSpinal Injection TechniquesКарим МухамедяновÎncă nu există evaluări
- Dental Suturing Materials and Techniques: OtolaryngologyDocument11 paginiDental Suturing Materials and Techniques: OtolaryngologyorizaÎncă nu există evaluări
- Mobile C Arm PortfolioDocument6 paginiMobile C Arm PortfolioAri ReviantoÎncă nu există evaluări
- Strategies To Prevent Surgical Site Infections in Acute Care Hospitals 2022 UpdateDocument26 paginiStrategies To Prevent Surgical Site Infections in Acute Care Hospitals 2022 UpdatePaola Cristini Gama SilvaÎncă nu există evaluări
- The Effects of Nurse Staffing On The Medical Surgical Unit Involving Patient Safety and Quality of CareDocument13 paginiThe Effects of Nurse Staffing On The Medical Surgical Unit Involving Patient Safety and Quality of Careapi-402644703Încă nu există evaluări
- 11 B - All On Four Group 01 PDFDocument3 pagini11 B - All On Four Group 01 PDFLuis Humberto BorgesÎncă nu există evaluări
- Fall 2020 NRP Poster Acp FinalDocument1 paginăFall 2020 NRP Poster Acp Finalapi-579593882Încă nu există evaluări
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- Gil Intra Moot Court Competition For The Academic Year 2022-2023Document16 paginiGil Intra Moot Court Competition For The Academic Year 2022-2023Kriti sharmaÎncă nu există evaluări
- Long Term Effects of Surgically Assisted Rapid Maxillary Expansion Without Performing Osteotomy of The Pterygoid PlatesDocument4 paginiLong Term Effects of Surgically Assisted Rapid Maxillary Expansion Without Performing Osteotomy of The Pterygoid PlatesAngélica Valenzuela AndrighiÎncă nu există evaluări
- Abdominal Aortic Aneurysm Case Study: by Lisa ErwertDocument21 paginiAbdominal Aortic Aneurysm Case Study: by Lisa ErwertShashidhar Venkatesh MurthyÎncă nu există evaluări
- Throughput Accounting-AccaDocument25 paginiThroughput Accounting-AccaDamalai YansanehÎncă nu există evaluări
- Colloidal SilverDocument11 paginiColloidal SilverAmit ChaudharyÎncă nu există evaluări
- No Nama Obat Kemasan Isi Per Kemas Jan-Jun 2021 MerkDocument3 paginiNo Nama Obat Kemasan Isi Per Kemas Jan-Jun 2021 MerkPercetakan Panji JayaÎncă nu există evaluări
- Volume 15, Number 4 April 2011Document162 paginiVolume 15, Number 4 April 2011Nicolai BabaliciÎncă nu există evaluări
- Complete Product Catalog With LineDocument29 paginiComplete Product Catalog With LineAarsol AdvanceÎncă nu există evaluări
- Cardiovascular Surgical InstrumentatorDocument3 paginiCardiovascular Surgical Instrumentatorapi-626421480Încă nu există evaluări
- Assael 2003Document7 paginiAssael 2003Varun bharathiÎncă nu există evaluări
- Basic Surgical Skills Indonesia 2016Document17 paginiBasic Surgical Skills Indonesia 2016'putu' AcaaRyaaÎncă nu există evaluări
- Settlement DemandDocument4 paginiSettlement Demandapi-291819279Încă nu există evaluări
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionDe la EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionEvaluare: 4 din 5 stele4/5 (402)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingDe la EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingEvaluare: 5 din 5 stele5/5 (4)
- The Age of Magical Overthinking: Notes on Modern IrrationalityDe la EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityEvaluare: 4 din 5 stele4/5 (13)
- The Happiness Trap: How to Stop Struggling and Start LivingDe la EverandThe Happiness Trap: How to Stop Struggling and Start LivingEvaluare: 4 din 5 stele4/5 (1)