Documente Academic
Documente Profesional
Documente Cultură
Indication For Red Cell Transfusion
Încărcat de
Risma Rachmawati FatimahTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Indication For Red Cell Transfusion
Încărcat de
Risma Rachmawati FatimahDrepturi de autor:
Formate disponibile
Ref: CG070
Authorised by: Dr H Eden/Clinical Guidelines
Committee
Issue: 4
Revalidated/Revised by: Dr P Cervi
Date: July 07
Revalidated: December 08
Revalidated/revised: February 2011
Date: 06.04.05
SOUTHEND HOSPITAL
GUIDELINES
INDICATION FOR RED CELL TRANSFUSION
January 2005
Prepared by Dr H Eden, Consultant Haematologist and
Lesley Hough, Hospital Transfusion Practitioner
and
Approved by the Hospital Transfusion Committee
09/03/2011
CONTENTS
Page 3
Summary chart of indications for red cell transfusion
Page 4
Introduction
Page 6
Indications for red cell transfusion.
Page 10
Alternatives to red cell transfusion
Page 11
References
indications for red cell transfusion
09/03/2011
INDICATION CODES FOR RED CELL TRANSFUSION
SUMMARY
R1 Acute blood loss
Objective: to maintain circulating blood volume and haemoglobin (Hb) concentration > 7
g/dl in otherwise fit patients, and 8 - 9g/dl in older patients and those with known
cardiovascular disease.
15-30% loss of blood volume (800-1500 in an adult) red cell transfusion is unlikely to
be necessary, transfuse crystalloids or synthetic colloids. In obstetrics transfusion should
commence when blood loss approaches 1000ml and is continuing.
30 -40% loss of blood volume (1500-2000 in an adult) Rapid volume replacement is
required with crystalloids or synthetic colloids and red cell transfusion probably required to
maintain Hb levels.
>40% loss of blood volume (>2000ml in an adult) Rapid volume replacement is
required including red cell transfusion.
R2
Hb concentration < 7g/dl
R3
Hb concentration < 8 or 9g/dl in patients with known cardiovascular
disease or those with significant risk factors of such disease ( e.g. elderly patients, those
with hypotension, diabetes mellitus PVD.
For Chronic renal failure transfuse to maintain Hb > 10g/dl )
R4
In critical care transfuse to maintain Hb > 7 g/dl. or >9 g/dl if cardiac
or respiratory disease present.
R5 Post-chemotherapy / radiotherapy: There is no evidence based
guide to practice
Most hospitals use a threshold of Hb 8 or 9 g/dl for chemotherapy and 11 12 for
radiotherapy
R6 Chronic anaemia; Transfuse to maintain the Hb concentration just above the
lowest concentration which is not associated with symptoms of anaemia. Many patients
may be asymptomatic with an Hb >8g/dl. Do not transfuse when effective alternatives
exist.
indications for red cell transfusion
09/03/2011
INTRODUCTION
Red cell transfusions are required to increase the oxygen carrying capacity of the blood by
raising the haemoglobin concentration of patients with acute or chronic anaemia and avoid
tissue hypoxia.
Transfusion medicine is changing rapidly in response to a number of different
developments. There are renewed concerns about the safety of transfusion, in relation to
both infectious and non-infectious complications, as highlighted in the Serious Hazards of
Transfusion (SHOT) initiative. Hence appropriate use of donor blood is becoming an
increasingly important clinical governance and public health issue.
There are no reliable parameters to guide the need for red cell transfusion. The decision
to transfuse red cells is a complex one and depends on factors such as the cause of the
anaemia, its severity and chronicity, the patients ability to compensate for anaemia, the
likelihood of further blood loss and the need to provide some reserve before the onset of
tissue hypoxia. The risk of a transfusion should be taken seriously on balance against the
perceived benefits. Although in these guidelines we will try to specify a given
concentration of haemoglobin to trigger transfusion, consideration of the patients clinical
condition is an essential part of the decision to transfuse red cells or not.
Associated documentation:
CG-260: Guideline for the Management of Adult massive Haemorrhage
CG 060 indications for the Use of Fresh Frozen Plasma and Cryoprecipitate
CG 071 Indications for the Use of Platelet Transfusion
CG 242 Guideline for the Management of Patients who Refuse Blood Product
Transfusion
BT-11: Policy for the Administration of Blood and Blood Components
CG-051: Guidelines for the use of ORhD Negative Red Cells (including major
incident planning)
indications for red cell transfusion
09/03/2011
General Principles
Clinician prescribing red cell (RBC) transfusion should be aware of indications and
the risks and benefits of transfusion.
Patients should be given information about the risks and benefits of RBC
transfusion in advance of transfusion whenever possible, together with possible
alternatives (National Blood Transfusion information leaflets available). Patients
have the right to refuse transfusion but this must be documented in the medical
notes.
The cause of anaemia should be established.
There is no universal trigger for RBC transfusion (a haemoglobin concentration at
which transfusion of red cells is appropriate for all patients). Clinical judgement
plays a vital role in the decision to transfuse red cells or not.
In acute blood loss, crystalloids or synthetic colloids should be used for rapid
volume replacement.
The reason for administration of RBC transfusion and the record of each unit of
blood must be documented in the patients medical records.
Normally patients should not be transfused if haemoglobin concentration is above
10g/dl.
A strong indication for transfusion is haemoglobin concentration below 7g/dl.
Transfusion will become essential when haemoglobin concentration decreases to
5g/dl.
Haemoglobin concentration between 8g/dl and 10g/dl is a safe level even for those
patients with significant cardio respiratory disease.
Symptomatic patients should be transfused.
indications for red cell transfusion
09/03/2011
Indications for the use of red cell transfusion
R1. Acute blood loss
Objective : to maintain circulating the blood volume and haemoglobin
concentration > 7g/dl in otherwise fit patients and > 8 or 9g/dl in older
patients and those with known cardiovascular and respiratory disease.
It may be difficult to assess the amount of blood loss, but consideration of lost circulatory
volume may be useful in guiding the transfusion management. The following is a general
guide for the need for transfusion based on acute blood loss in an adult.
15% loss of blood volume (750 ml) : no need for transfusion unless blood loss is
superimposed on pre-existing anaemia or unable to compensate due to severe
cardiac or respiratory disease.
15-30% loss of blood volume (800-1500 ml) : need to transfuse crystalloid or
synthetic colloids. The need for red cell transfusion is unlikely unless the patient
has pre-existing anaemia, reduced cardio-respiratory reserve or blood loss
continues.
30-40% loss of blood volume (1500-2000 ml) : rapid volume replacement is
required with crystalloid or synthetic colloids, and red cell transfusion will probably
be required.
40% loss of blood volume (> 2000 ml) : rapid volume replacement, including red cell
transfusion, is required.
To start with, 2 units of red cells should be transfused and then the clinical situation
and haemoglobin concentration should be re-assessed.
R2
Clinical evidence suggests that transfusion of patients with haemoglobin
concentration between 7 10g/dl is not always justifiable.
R3
However, in elderly patients and patients with cardiovascular and respiratory
disease, you may need to consider transfusion when haemoglobin is < 8 or 9 g/dl.
Renal patients maintain Hb > 10g/dl
NOTE: Blood volume 70ml/kg body weight in adult
indications for red cell transfusion
09/03/2011
Consideration of abnormal haemostasis resulting in increased risk of
bleeding
Thrombocytopenia
Platelets dysfunction, either inherited or acquired due to Aspirin or non-steroidal
anti-inflammatory drugs.
The above two causes should be treated with platelets transfusion according to our
current guideline.
R4
Abnormal clotting screen needs to be treated according to our current guideline.
Anaemia in critically ill patients
Transfuse blood to maintain the haemoglobin > 7 g/dl or >9 if patient has cardio
respiratory disease
Over transfusion may increase mortality in this group.
The importance of adequate volume replacement.
Maintenance of blood pressure and the use of inotropic drugs to maintain normal
cardiac output.
Using crystalloids may be preferred to colloids for fluid resuscitation of patients with
acute hypovolaemia. Colloids have the potential disadvantage of hypersensitivity,
including occasional severe anaphylactoid reactions, and exacerbation of any
haemostatic problems and hypotension.
indications for red cell transfusion
09/03/2011
R5
Post -chemotherapy / radiotherapy
R6
There is no evidence based guide to practice. Most hospitals use a threshold
of Hb 8 or 9 g/dl for chemotherapy and 11 12 g/dl for radiotherapy
Chronic anaemia
The cause of anaemia should be established and treatment with red cell
transfusions should not be given where effective alternatives exist, e.g. iron
deficiency, megaloblastic and auto-immune haemolytic anaemia, unless the
anaemia is life threatening.
An alternative treatment with erythropoietin can be used for chronic anaemia e.g.
cancer patients, myelodysplasia, renal failure etc.
Red cell transfusion in patients with haemoglobinopathy
a) The aim of hypertransfusion programme in beta thalassaemia major is to
suppress erythropoiesis and correction of the anaemia. In order to minimise
iron overload, trigger haemoglobin concentration is < 9.5 g/dl.
b) Long term transfusion programmes used in sickle cell disease to reduce risk
of vaso-occlusive events in patients with previous stroke and during
pregnancy. Transfusion is not routinely indicated for patients with sickle-cell
disease, unless the haemoglobin is low or pre-operatively please refer to
special guidelines for further details.
indications for red cell transfusion
09/03/2011
Transfusion in surgical patients
Surgical patients receive more than 1,000,000 units annually, half of transfused
allogeneic blood in the U.K. Several factors need to be taken into account before
considering transfusion in the surgical patient.
Ensure all patients should have pre-operative assessment.
The decision to transfuse should always be made on an individual patient
basis.
Patients should not be transfused to achieve a normal haemoglobin
concentration.
The reason for pre and post-operative transfusions must be recorded in the
clinic notes.
Record of the administration of each unit of blood must be kept permanently
in the clinical notes.
Surgical blood ordering schedule should be followed and audited regularly.
Up to 30% of blood loss can be treated with crystalloid or colloid solutions.
There is no increase in mortality providing the haemoglobin concentration
was kept above 8 g/dl even in an elderly population.
Haemoglobin concentration above 8 g/dl is sufficient for patients with severe
cardio-respiratory disease.
Post-operative patients who are limited in their activity are unlikely to have
oxygen demands that exceed supply.
Wound healing is not affected, only when haematocrit is less than 18%.
Iron deficiency anaemia should be investigated and corrected during preoperative period.
indications for red cell transfusion
09/03/2011
Alternative to Allogeneic Blood Transfusion
Autologous transfusion:
The use of red cell salvage.
Pre-deposit programs reduce the need for allogeneic blood. However risk of
clerical errors and chances of transfusing the wrong blood is still possible
and is now only recommended for exceptional clinical circumstances
Acute normovolaemic haemodilution.
10
indications for red cell transfusion
09/03/2011
References
1.
Guidelines for the clinical use of red cell transfusion.
Haematologists, 2001, 113, 24-31.
2.
Blood Transfusion and the Anaesthetist. Red cell Transfusion June 2008
issued by the Association of Anaesthetists of Great Britain & Ireland.
3.
Handbook of Transfusion Medicine. Blood Transfusion Services of the
United Kingdom. Fourth edition 2007. Editor: DBL McClelland.
4.
Guideline for Policies for Alternatives to Allogenic Blood Transfusion
December 2006 BCSH Guidelines.
11
British Journal of
indications for red cell transfusion
S-ar putea să vă placă și
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (895)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (73)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- Quick Guide To ProscriptDocument20 paginiQuick Guide To ProscriptAmit Raj100% (2)
- BONUS - 7 Day Ab Targeted Cardio and Intervals PDFDocument42 paginiBONUS - 7 Day Ab Targeted Cardio and Intervals PDFScott Levine100% (6)
- Phonetics in Complete Denture-3670Document5 paginiPhonetics in Complete Denture-3670Najeeb UllahÎncă nu există evaluări
- Snakebite Envenoming: A Strategy For Prevention and ControlDocument70 paginiSnakebite Envenoming: A Strategy For Prevention and ControlApotik ApotekÎncă nu există evaluări
- LPL - Pasricha Diagnostics & Ultrasound Clinic: Patientreportscsuperpanel - SP - General - Template01 - SC (Version: 7)Document3 paginiLPL - Pasricha Diagnostics & Ultrasound Clinic: Patientreportscsuperpanel - SP - General - Template01 - SC (Version: 7)isw1707Încă nu există evaluări
- Cognitive DistortionsDocument7 paginiCognitive Distortionsoana liminala100% (1)
- Sun Salutations Yoga Lesson PlanDocument8 paginiSun Salutations Yoga Lesson PlanErica Harris100% (1)
- TX 5005002Document9 paginiTX 5005002Rio Van Der SarÎncă nu există evaluări
- Invisible Fluorescent Skin Stamp Ink, GreenDocument4 paginiInvisible Fluorescent Skin Stamp Ink, GreenHasanzubyreÎncă nu există evaluări
- The Human Brain Project 2014Document2 paginiThe Human Brain Project 2014api-165776946Încă nu există evaluări
- Krok 2 Paper 4Document6 paginiKrok 2 Paper 4berdaderagaÎncă nu există evaluări
- Fracture Management in of Ulna Fractures in The Avian PatientDocument6 paginiFracture Management in of Ulna Fractures in The Avian PatientChau BuiÎncă nu există evaluări
- OB PACU Severe PreeclampsiaDocument65 paginiOB PACU Severe Preeclampsiasurbakti_christineÎncă nu există evaluări
- NG Comprehension PassagesDocument7 paginiNG Comprehension Passagessalbina arabiÎncă nu există evaluări
- NY Physician Survey Report FINALDocument10 paginiNY Physician Survey Report FINALBethanyÎncă nu există evaluări
- TgaDocument33 paginiTgavarun rajÎncă nu există evaluări
- Role Play Discharge PlanningDocument3 paginiRole Play Discharge PlanningChoirunnisa Putri100% (1)
- 4 671945747968557164Document67 pagini4 671945747968557164McMillanÎncă nu există evaluări
- Raheem Khan - WikipediaDocument10 paginiRaheem Khan - WikipediaRaheem MahirÎncă nu există evaluări
- FEB Brickclean Safety DatasheetDocument10 paginiFEB Brickclean Safety DatasheetMhd ThrÎncă nu există evaluări
- Emergency Rescue and Transfer HardDocument5 paginiEmergency Rescue and Transfer HardJorhally B Edzraphil100% (1)
- RRL FinalDocument19 paginiRRL FinalGerald John PazÎncă nu există evaluări
- The Effect of Physical Activity On Primary Dysmenorrhea of Female University StudentsDocument8 paginiThe Effect of Physical Activity On Primary Dysmenorrhea of Female University Studentssekar ayuÎncă nu există evaluări
- Pediatric HeadachesDocument34 paginiPediatric HeadachesVirda Maharani100% (2)
- Sandeep MedicalDocument2 paginiSandeep MedicalSandeep GAMING YTÎncă nu există evaluări
- Laporan Stock Opname Desember 2019 Pelaksanaan 2 Januari 2020Document17 paginiLaporan Stock Opname Desember 2019 Pelaksanaan 2 Januari 2020RS PKU MUHAMMADIYAH WONOSARIÎncă nu există evaluări
- Dermocosmetic Care For RosaceaDocument16 paginiDermocosmetic Care For Rosaceariki fazar rahmaditaÎncă nu există evaluări
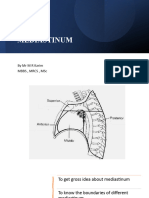
- MediastinumDocument27 paginiMediastinumRezaul KarimÎncă nu există evaluări
- Overview of Selected Family Therapy ModelsDocument5 paginiOverview of Selected Family Therapy ModelsErin Richardson100% (1)
- Andrew Austin - IEMT & Long Term Anxiety - DVD Cover PDFDocument2 paginiAndrew Austin - IEMT & Long Term Anxiety - DVD Cover PDFMichael CliftonÎncă nu există evaluări