Documente Academic
Documente Profesional
Documente Cultură
IV Fluids
Încărcat de
cbac1990Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
IV Fluids
Încărcat de
cbac1990Drepturi de autor:
Formate disponibile
8/12/2016
Calculating Maintenance Fluid Rates
[http://twitter.com/#!/SickKidsNews]
[http://instagram.com/sickkidstoronto/]
[https://www.youtube.com/user/SickKidsInteractive]
[http://www.linkedin.com/company/the-hospital-for-sick-children?trk=tyah]
[https://www.facebook.com/sickkidsfoundation]
Nursing
Calculating Maintenance Fluid Rates
Although it is the physicians responsibility to calculate and order daily uid requirements for
patients, Registered Nurses are responsible for double checking the order for accuracy. Below are
two different methods used in calculating paediatric maintenance uid rates.
Formula Method
(100 ml for each of the rst 10kg) + ( 50ml for each kg 11-20) + (20 ml for each additional kg) /
24hour
Example:
Calculate the hourly maintenance uid rate for a child
who weighs 25kg
(100mL x 10kg) + (50mL x 10kg) + (20mL x 5kg) / 24hrs
(1000mL) + (500mL) + (100mL) = 1600mL / 24hrs =
66.7ml/hr
Using this formula the hourly uid maintenance for this
child is 67mL/hr
4 / 2 / 1 Method
(4ml/kg for the rst 10kg) + (2ml/kg for kg 11-20) + (1ml/kg for every kg above 20) = hourly rate
Example:
Calculate the hourly maintenance uid rate for a child
who weighs 25kg
(4ml x 10kg) + (2ml x 10kg) + (1ml x 5kg) = hourly rate
40ml + 20ml + 5ml = 65ml/hr
Using the 4/2/1 method, this child's hourly maintenance
uid rate is 65mL/hr
Copyright 1999-2014 The Hospital for Sick Children (SickKids). All rights reserved.
The Hospital for Sick Children (SickKids) is a health-care, teaching and research centre dedicated exclusively to children; afliated with the University of Toronto
[http://www.utoronto.ca/] . For general inquires please call: 416-813-1500.
Please note: Some of the content photography on this website is being used for illustrative purposes only and any person depicted in the content is a model.
http://www.sickkids.ca/Nursing/Education-and-learning/Nursing-Student-Orientation/module-two-clinical-care/paediatric-iv-therapy/Calculating-Maintenance-Fl 1/1
8/12/2016
Clinical Practice Guidelines : Intravenous uids
Intravenous uids
This guideline has been adapted for statewide use with the support of the Victorian Paediatric Clinical Network
IV Fluids - for children beyond the newborn period
See also:
Guideline on Neonatal Fluid Requirements
Checklist of commonly used uids
Dehydration
Hyponatraemia Guideline
Hypernatraemia Guideline
Background:
Whenever possible the enteral route should be used for uids. These guidelines only apply to children who
cannot receive enteral uids.
The safe use of IV uid therapy in children requires accurate prescribing of uid and careful monitoring
Always check orders that you have written, and ensure that you double check on orders written by other staff
when you take over the child's care
Incorrectly prescribed or administered uids are potentially very dangerous. More adverse events are
described from uid administration than for any other individual drug. If you have any doubt about a child's uid
orders - ask a senior doctor.
Remember to check compatibility of intravenous uid with any intravenous drugs that are being coadministered.
Assessment of uid requirements: Unwell children (+/- abnormal hydration)
How much Fluid?
If required, administer an initial bolus(es) of uid to correct intravascular depletion then:
Hypovolaemia
Give boluses of 10-20ml/kg of 0.9% sodium chloride (normal saline), which may be repeated.
Do not include this uid volume in any subsequent calculations
Maintenanceplus
Decit(dehydration guidelines), plus
Ongoing losses(dehydration guidelines)
Maintenance
This guideline should be used as a starting point and will need to be adjusted in ALL unwell children.
http://www.rch.org.au/clinicalguide/guideline_index/Intravenous_Fluids/
1/4
8/12/2016
Clinical Practice Guidelines : Intravenous uids
Generally 2/3 of maintenance rate should be used in unwell children unless they are dehydrated. This is because they
are likely to be secreting anti-diuretic hormone (ADH), so will need less uid. Children with meningitis or other acute
CNS conditions will likely require additional uid restriction seek senior advice.
For uid options in the dehydrated child see dehydration guidelines.
Weight (kg)
Full Maintenance (mL/hour)
Well child eg fasting for theatre
2/3 maintenance (mL/hour)
Most unwell children eg pneumonia, meningitis
20
13
10
40
27
15
50
33
20
60
40
25
65
43
30
70
47
35
75
50
40
80
53
45
85
57
50
90
60
55
95
63
60
100
67
REMEMBER to consider decit and ongoing losses - especially in severe gastroenteritis, if there are drain losses,
ileostomies etc.
Which Fluid?
Some good uid solutions for sick children include:
Fluid
Alternative
names
Uses
0.9% sodium chloride
Normal
saline
Initial boluses
Replacement of decit
Replacement of losses
Plasma-Lyte148 and 5% Glucose
Maintenance hydration
(contains 5mmol/L of potassium)
(this should be the standard maintenance
uid prescribed at RCH)
Replacement of decit
Replacement of losses
Plasma-Lyte148 and 5% Glucose with 20mmol/L
potassium
http://www.rch.org.au/clinicalguide/guideline_index/Intravenous_Fluids/
Maintenance hydration - should only be
used for children with hypokalaemia
2/4
8/12/2016
Clinical Practice Guidelines : Intravenous uids
(15mmol/L of KCl will need to be added to a
standard bag to bring the concentration to
20mmol/L)
0.9% sodium chloride and 5% Glucose +/20mmol/L KCl
Replacement of decit
Replacement of losses
Normal
saline with
glucose
Maintenance
Replacement of decit
Replacement of losses
Consider whether potassium is required in the uid. This should be avoided, if possible, unless premade uid
bags containing potassium are available. Adding potassium to bags of uid on the ward is a safety risk.
Hypotonic uid (containing a sodium concentration less than plasma) is no longer recommended in children. These
uids have been associated with morbidity/mortality secondary to hyponatraemia. Fluids that should NOT be given
include:
0.18% NaCl with 4% glucose +/- KCl 20mmol/L (or 4% and 1/5 NS) should NOT be given
Monitoring
All children on IV uids should be weighed prior to the commencement of therapy, and daily afterwards. Ensure
you request this on the treatment orders.
Children with ongoing dehydration/ongoing losses may need 6 hourly weights to assess hydration status
All children on IV uids should have serum electrolytes and glucose checked before commencing the infusion
(typically when the IV is placed) and again within 24 hours if IV therapy is to continue.
For more unwell children, check the electrolytes and glucose 4-6 hours after commencing, and then according
to results and the clinical situation but at least daily.
Pay particular attention to the serum sodium on measures of electrolytes. If <135mmol/L (or falling signicantly
on repeat measures) see Hyponatraemia Guideline. If >145mmol/L (or rising signicantly on repeat measures)
see Hypernatraemia guideline.
Children on iv uids should have a uid balance chart documenting input, ongoing losses and urine output.
Special uids
Outside the newborn period, do not use these uids apart from exceptional circumstances and check the
serum sodium regularly
10% Dextrose
Used in neonates (sometimes with additional NaCl). Used in ICU for patients under 12 months (with 0.45% saline).
Sometimes used by infusion in neonates and children with metabolic disorders. Check blood glucose regularly.
15-20% Dextrose
Very occasionally used by infusion in children with metabolic disorders. Check blood glucose regularly.
25% and 50% Dextrose
Rarely required in children, misuse can cause severe adverse events.Only used in discussion with senior staff as
bolus or low volume infusions (1-2 ml/hr) to correct refractory hypoglycaemia.
Consider consultation with local paediatric team when:
-Unsure of which uid/how much uid to use
-Electrolyte abnormalities
-Using a non-standard 'special' uid
Consider transfer when:
http://www.rch.org.au/clinicalguide/guideline_index/Intravenous_Fluids/
3/4
8/12/2016
Clinical Practice Guidelines : Intravenous uids
-Children requiring care above the level of comfort of the local hospital.
-Severe electrolyte or glucose abnormalities
For emergency advice and paediatric or neonatal ICU transfers, call the Paediatric Infant Perinatal Emergency
Retrieval (PIPER) Service: 1300 137 650.
Information Specic to RCH
From February 2016, Plasma-Lyte148 and 5% Glucose will be the standard maintenance uid prescribed.
0.45% sodium chloride and 5% glucose +/- KCl (or 5% and NS) should NOT be given.
Children on intravenous uids need daily electrolyte monitoring.
20-50% dextrose should not be given outside the ICU or NNU setting without discussion with a consultant.
Calculating maintenance uid:
Calculating Maintenance uid rate:
Most unwell children should have a restriced (2/3) maintenance rate prescribed. The basis from which calculations
are made are detailed below
daily uid intake which replaces the insensible losses (from breathing, through the skin, and in the stool)
allows excretion of the daily production of excess solute load (urea, creatinine, electrolytes, etc) in a volume of
urine that is of an osmolarity similar to plasma.
volume calculated per kilo.
Patients weight
Full Maintenance mls/day
mls/hour
3 to 10kg
100 x wt
4 x wt
10 - 20kg
1000 plus 50 x (wt-10)
40 plus 2 x (wt-10)
>20kg
1500 plus 20 x (wt-20)
60 plus 1 x (wt-20) [S1]
100mls/hour (2400mls/day) is the normal maximum amount.
Additional notes
There is often confusion about the difference between oral and iv uid requirements for young infants. The water
requirement is identical for both routes of administration. The relatively low energy density of milk means that infants
need 150-200mls/kg/day to obtain adequate nutrition. That is why they pass more dilute urine than older children.
Contentauthorisedby:Webmaster.Enquiries:Webmaster.
http://www.rch.org.au/clinicalguide/guideline_index/Intravenous_Fluids/
4/4
8/12/2016
How to calculate IV ow rates
HowtocalculateIVflowrates:
Intravenousfluidmustbegivenataspecificrate,neithertoofastnortooslow.Thespecificratemaybe
measuredasml/hour,L/hourordrops/min.Tocontroloradjusttheflowrateonlydropsperminuteareused.
Theburettecontainsaneedleorplasticdropperwhichgivesthenumberofdropsperml(thedropfactor).A
numberofdifferentdropfactorsareavailable(determinedbythelengthanddiameteroftheneedle).
Commondropfactorsare:
10drops/ml(bloodset),15drops/ml(regularset),60drops/ml(microdrop).
Tomeasuretheratewemustknow:
(a)thenumberofdrops
(b)timeinminutes.
Theformulaforworkingoutflowratesis:
volume(ml)Xdropfactor(gtts/ml)
=gtts/min
(flowrate)
time(min)
Example:
1500mlIVSalineisorderedover12hours.Usingadropfactorof15drops/ml,howmanydropsper
minuteneedtobedelivered?
1500(ml)X15(gttss/ml)
=31gtts/minute
12x60(givesustotalminutes)
http://www.unc.edu/~bangel/quiz/testivh.htm
1/1
S-ar putea să vă placă și
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5795)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1091)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (895)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (121)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2259)
- Case Analysis - Rosemont Hill Health Center - V3Document8 paginiCase Analysis - Rosemont Hill Health Center - V3thearpan100% (2)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (74)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- Gyne - Lec 03 CytologyDocument3 paginiGyne - Lec 03 Cytologycbac1990Încă nu există evaluări
- Gyne - Case 11 Lower Genital UTI PDFDocument2 paginiGyne - Case 11 Lower Genital UTI PDFcbac1990Încă nu există evaluări
- Gyne - Case 16 Neoplastic Lesions of The CevixDocument1 paginăGyne - Case 16 Neoplastic Lesions of The Cevixcbac1990Încă nu există evaluări
- Gyne - Case 15 Benign Lesions of The Vulva & VaginaDocument2 paginiGyne - Case 15 Benign Lesions of The Vulva & Vaginacbac1990Încă nu există evaluări
- Gyne - Case 13 Benign Lesions of The UterusDocument2 paginiGyne - Case 13 Benign Lesions of The Uteruscbac1990Încă nu există evaluări
- Gyne - Case 05 Abnormal Uterine BleedingDocument3 paginiGyne - Case 05 Abnormal Uterine Bleedingcbac1990Încă nu există evaluări
- Gyne - Case 07 Secondary Amenorrhea (Hyperprolactinemia)Document1 paginăGyne - Case 07 Secondary Amenorrhea (Hyperprolactinemia)cbac1990Încă nu există evaluări
- Gyne - Case 10 MenopauseDocument2 paginiGyne - Case 10 Menopausecbac1990Încă nu există evaluări
- Case 3 Congenital Anomalies, Primary AmenorrheaDocument3 paginiCase 3 Congenital Anomalies, Primary Amenorrheacbac1990Încă nu există evaluări
- Case 2 Pre-Op & Post-Op CareDocument1 paginăCase 2 Pre-Op & Post-Op Carecbac1990Încă nu există evaluări
- Specific Antibiotics Lecture NotesDocument28 paginiSpecific Antibiotics Lecture Notescbac1990100% (5)
- Pedia Revalida ReviewDocument83 paginiPedia Revalida Reviewcbac1990Încă nu există evaluări
- Case 1 History & PEDocument3 paginiCase 1 History & PEcbac1990Încă nu există evaluări
- A Proposal For A'new Method of Evaluation - of The Newborn Infant PDFDocument8 paginiA Proposal For A'new Method of Evaluation - of The Newborn Infant PDFcbac1990Încă nu există evaluări
- Comparative Evaluation of Two Techniques in AchievingDocument5 paginiComparative Evaluation of Two Techniques in AchievingNoland NaidooÎncă nu există evaluări
- FCPS Pulmonogy CPSP Course BookletDocument32 paginiFCPS Pulmonogy CPSP Course BookletQiblaHazoor100% (1)
- MINI MARKETING PLAN - Individualized PDFDocument3 paginiMINI MARKETING PLAN - Individualized PDFMichelle Dalton NettleÎncă nu există evaluări
- Evolution of NeonatologyDocument17 paginiEvolution of NeonatologyClaudia KosztelnikÎncă nu există evaluări
- Curriculum Vitae Nata (English)Document3 paginiCurriculum Vitae Nata (English)Nata SanjayaÎncă nu există evaluări
- Adjuvant AnalgesicsDocument44 paginiAdjuvant AnalgesicsZulfan EfendiÎncă nu există evaluări
- CTEVDocument17 paginiCTEVamal.fathullah100% (1)
- ChapterDocument26 paginiChapterKlarence MendozaÎncă nu există evaluări
- HDN Alias Eritroblastosis FetalisDocument6 paginiHDN Alias Eritroblastosis FetalisOlivia RamadhaniÎncă nu există evaluări
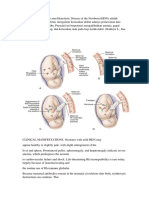
- Moyamoya DiseaseDocument14 paginiMoyamoya Diseasethomsoon01Încă nu există evaluări
- Clubfoot Written ReportDocument7 paginiClubfoot Written ReportAira Madel ArabaÎncă nu există evaluări
- Kaplan All SubjectsDocument8 paginiKaplan All Subjectssarmad_bayatliÎncă nu există evaluări
- The Common ColdDocument240 paginiThe Common ColdvorezÎncă nu există evaluări
- Shelby FurubayashiDocument1 paginăShelby Furubayashiapi-403090420Încă nu există evaluări
- Prof DR Ali Ghufron MuktiDocument3 paginiProf DR Ali Ghufron MuktiKhalid Bin Tatang HarmaenÎncă nu există evaluări
- Peran - Fungsi Perawat Safe SurgeryDocument69 paginiPeran - Fungsi Perawat Safe Surgeryerwin salehÎncă nu există evaluări
- Comprehensive Study Guide. 7Th Ed. New York: Mcgraw-Hill 2011Document3 paginiComprehensive Study Guide. 7Th Ed. New York: Mcgraw-Hill 2011Jefri EfendiÎncă nu există evaluări
- InterviewerDocument4 paginiInterviewerBianca DanciÎncă nu există evaluări
- Thalidomide GrunenthalDocument8 paginiThalidomide GrunenthalTiffany_Strang_6184Încă nu există evaluări
- MMSE Vs MocaDocument3 paginiMMSE Vs MocaIrene Olivia SalimÎncă nu există evaluări
- Lifecare PLV 100 PDFDocument13 paginiLifecare PLV 100 PDFGregorio NavarreteÎncă nu există evaluări
- MetablocDocument20 paginiMetablocDragos Lunca100% (1)
- De Quervain Tenosynovitis of The WristDocument8 paginiDe Quervain Tenosynovitis of The Wristrani_zÎncă nu există evaluări
- Body PlathyDocument13 paginiBody PlathyWayanWahyuSemaraPutraÎncă nu există evaluări
- Aace - Ace - 2016 - Comprehensive Clinical Practice Guidelines For Medical Care of Patients With ObesityDocument203 paginiAace - Ace - 2016 - Comprehensive Clinical Practice Guidelines For Medical Care of Patients With ObesityLintang AdhiÎncă nu există evaluări
- Guideline Molar ExtractionDocument3 paginiGuideline Molar Extractionmentacity10Încă nu există evaluări
- Effects of Lantana CamaraDocument8 paginiEffects of Lantana CamaraRogênio MendesÎncă nu există evaluări
- Lac RhesusDocument4 paginiLac RhesusmiadelfiorÎncă nu există evaluări
- Amabala Ayushman 20240110484466Document5 paginiAmabala Ayushman 20240110484466OFC accountÎncă nu există evaluări