Documente Academic
Documente Profesional
Documente Cultură
Schwartz Chapter 33 Spleen
Încărcat de
Gay Solas EpalanDescriere originală:
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Schwartz Chapter 33 Spleen
Încărcat de
Gay Solas EpalanDrepturi de autor:
Formate disponibile
Chapter 34 Spleen Surgery II
Reference: Scwartz Principles in Surgery
EMBRYOLOGY
5th AOG, the spleen is evident
Accessory spleen
Most common anomaly of splenic embryology
20% of the population
30% with hematologic disease
80% found in the splenic hilum and vascular pedicle region
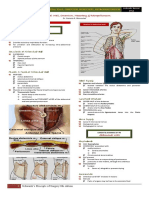
ANATOMY
Largest reticuloendothelial organ in the body
Capsule 1-2 mm thick, contains:
Collagen and elastin fibers
Average size 7-11 cm in lenght
Average weight 150g (70-250g)
If >500g and > 15 cm= Splenomegaly
In cadaveric anatomic series: Tail of pancreas
75% lies within 1 cm of the splenic hilum
30% abuts the spleen
Suspended in position by several ligaments and peritoneal folds
Colon
Splenocolic ligament
Avascular
Stomach
Gastrosplenic
ligament
Short gastric vessels
Diaphragm
Phrenosplenic
ligament
Avascular
Kidney, adrenal
gland, and tail of the
pancreas
Splenorenal ligament
Avascular
Blood Supply
Splenic artery (Main)
Short Gastric artery
Branches of the left gastroepiploic artery
Types of Splenic arteries
I Distributed type
70% Most common
Short trunk
Long branches
Entering over 75% of the medial surface
II Magistral type
30% Less common
Long main trunk
Short terminal branches
Entering over 2530% of the medial surface
Venous Supply
Splenic vein major venous drainage
Two elements of splenic parenchyma
I Red pulp
~ 75 % of total splenic volume
Comprised of large numbers of venous sinuses
Lined by long, narrow endothelial cells
Drain into tributaries of the splenic vein
Reticulum
Fibrocellular network
Consisting of collagen fibers and fibroblasts.
Within this network or mesh lie splenic macrophages.
Surrounded and separated the venous sinuses
Splenic cord
Intersinusoidal regions
Function
Dynamic filtration system
Enabling macrophages to remove microorganisms, cellular debris, antigen/antibody complexes, and senescent
erythrocytes from circulation.
II White pulp
Periarticular lymphatic sheath
Replaces the adventitia of the vessel splenic arterioles
Comprised of T lymphocytes and intermittent aggregations of B lymphocytes or lymphoid follicles.
Lymphoid follicles
Centers of lymphocyte proliferation,
Develop germinal centers
Regress as the stimulus or infection subsides
Normally consisting of nodules 1 mm in size
Can increase to several centimeters in size when nodules coalesce.
Marginal zone
Interface between the white and red pulp
Lymphocytes are more loosely aggregated
Blood is delivered to the red pulp
Lymphocytes and locally produced immunoglobulins ultimately enter the systemic circulation.
PHYSIOLOGY
Major organ clearing damaged or aged red blood cells; abnormal white blood cells and platelets.
Splenic function has historically been summarized as:
Filtration
Host Defense
Storage
Cytopoiesis.
Total splenic inflow of blood
~ 250300 mL/min.
Filtration function of the spleen occurs primarily via the slower circulation
Further evidence of selective slowing of blood cell flow versus plasma flow is indicated by a concentration of erythrocytes
(hematocrit) twice that of the general circulation within the spleen.
Erythrocytes 120-day life cycle
2-day minimum is spent sequestered in the spleen
20 mL of aged red blood cells are removed daily.
Act as a host defense
Significant, not indispensable role
Contributing to both humoral and cell-mediated immunity
The splenic RE system is better able to clear bacteria poorly or inadequately opsonized from the circulation than is the
hepatic RE system
Produces proteins such as:
Tuftsin
Stimulant to general phagocytic function in the host, facilitate clearance of bacteria.
Circulating monocytes converted into fixed macrophages with the red pulp account for the spleens remarkable
phagocytic activity.
Properdin
Important in the initiation of the alternate pathway of complement activation.
Physiologic capacity within the complement cascade to withstand the loss of tuftsin and properdin production
without increasing patient vulnerability postsplenectomy
Opsonins
PATHOPHYSIOLOGY
Splenectomy
Splenomegaly alone is an uncommon indication for splenectomy.
Most common indications
Hypersplenism
Presence of cytopenia (of one or more blood cell lines)
Disorders causing hypersplenism in an intrinsically normal spleen can be categorized as:
Increased destruction of abnormal blood cells
Increased sequestration and destruction of normal blood cells
Hypersplenism
May result in neutropenia or thrombocytopenia, and Alteration of splenic immune function
I Neutropenia
May result from sequestration of normal white blood cells or the removal of abnormal ones.
IIThrombocytopenia
May result from excessive sequestration of platelets and accelerated platelet destruction in the spleen.
Immunologic alteration of platelets
(-) splenomegaly
Platelet
Generally survive in the circulation for 10 days.
Under normal circumstances
33% or one third of the total platelet pool is sequestered in the spleen.
Up to 80% splenomegaly
III Alteration of splenic immune function
Alteration immune function often gives rise to antibody production,resulting in blood cell destruction.
EVALUATION OF SIZE AND FUNCTION
Before elective splenectomy, imaging of the spleen is frequently indicated to assess size and to determine
degree, if any, of splenomegaly
I Ultrasound
~98% sensitivity for detecting textural lesions of the spleen
II Computed tomography (CT) scanning
Affords a high degree of resolution and detail of the spleen
Useful for:
Assessment of splenomegaly
Identification of splenic lesions
Guidance for percutaneous procedures.
III Iodinated contrast material
Adds diagnostic clarity to CT imaging.
IV Plain radiography
Rarely used alone for splenic imaging
Can provide an outline of the spleen in the left upper quadrant, suggest splenomegaly
Demonstrate calcifications.
V Magnetic resonance imaging (MRI)
Offers no advantages in depicting anatomic spleen abnormalities.
VI Radioscintigraphy with 99mTc sulfur colloid
Demonstrates splenic location and size
Little benefit to its use as a preoperative scan.
The splenic index (SI)
Expresses spleen size as a volume in milliliters (mL)
Obtained by multiplying the spleens length, width, and height as determined by a reliable imaging modality.
Normal values for SI range = 120480 mL.
The normal ex vivo weight = 150 g.
INDICATIONS FOR SPLENECTOMY
The conditions for which splenectomy is therapeutic include:
Disorders of red blood cells
Myeloproliferative disorders (Early cell lines)
Disorders of white blood cells
Disorders of platelets
Miscellaneous disorders and lesions
Trauma to the spleen
The most common indication for splenectomy
Red Blood Cell Disorders
Acquired
Autoimmune hemolytic anemia
Warm-antibody AIHA
Congenital
Hereditary spherocytosis
Hemoglobinopathies
Sickle cell disease
Thalassemia
Autoimmune hemolytic anemia.
Set of disorders characterized by autoantibodies against antigens on red blood cells
Decrease the erythrocyte life span
Classified based on the temperature
Warm
Autoantibodies (IgG)
Bind erythrocytes at 37 C (98.6 F)
Best treated by splenectomy.
Cold
Ttypically IgM)
Cause erythrocytes to clump at cold temperatures.
Warm-antibody AIHA
Incidence
Approximately 1:100,000
More common among women
Principally seen in mid-life
50% cases are idiopathic
Clinical findings include:
Mild jaundice
Symptoms and signs of anemia
Splenomegaly 33-50%
occurs in one third to one half of patients, sometimes enough
Presentation
Acutely, with severe symptoms and signs
Gradually, with a relatively asymptomatic
In acute disease:
Signs of congestive heart failure may be observed.
Confirmation Diagnosis Direct Coombs test
Demonstrating hemolysis
Intravascular hemolysis
Extravascular hemolysis
Intravascular hemolysis
Red blood cells are opsonized by autoantibodies and are destroyed, directly within the circulation
Extravascular hemolysis
Removed from the circulation by tissue macrophages located primarily in the spleen and to a lesser extent in
the liver
Teatment of AIHA
Red blood cell transfusion.
For severe anemia (<4 g/dL), causing:
Pulmonary edema, tachycardia, postural hypotension, dyspnea, and angina
Corticosteroids
Act as the mainstay of treatment for both primary and secondary forms of symptomatic, unstable AIHA.
Splenectomy
Indicated for failure to respond to steroids, intolerance of steroid side effects, requirement for excessive steroid
doses to maintain remission, or inability to receive steroids for other reasons.
Favorable response up to 80 percent of patients with warm-antibody AIHA.
Hereditary spherocytosis
Prevalence: Western populations of 1 in 5000
Most common hemolytic anemia for which splenectomy is indicated.
Disorder of the red blood cell membrane resulting in hemolytic anemic
Underlying abnormality
Inherited dysfunction or deficiency in one of the erythrocyte membrane proteins:
Spectrin, ankyrin, band 3 protein, or protein 4.2
Rare fatal crises occur, usually in the setting of infection (e.g., parvovirus).
Clinical findings:
Relatively asymptomatic
Mild jaundice
Splenomegaly
Diagnosis:
Spherocytes are readily apparent on peripheral blood film.
Treatment: Splenectomy
Curative for typical forms of HS and serves as the sole mode of therapy.
Timing is important to reduce the very small possibility of overwhelming postsplenectomy sepsis.
At least age 4 but before age 7 unless the anemia and hemolysis accelerate
Early splenectomy
Indication for intractable leg ulcers
Heal only after removal
Sickle cell disease
Prevalence of sickle cell carriers
African Americans in the United States
Western Africa,
Inherited chronic hemolytic anemia
Due to mutant sickle cell hemoglobin (HbS) within the red blood cell.
Underlying abnormality
Substitution of valine for glutamic acid as the sixth amino acid of the beta-globin chain.
Results in microvascular congestion, which may lead to thrombosis, ischemia, and tissue necrosis.
Clinical Findings
Intermittent painful episodes
Treatment:
Palliative
Splenectomy
Blood transfusion
Splenectomy
Most frequent indications for splenectomy:
Hypersplenism
Acute sequestration crises
Splenic abscess
Does not affect the sickling process
Preoperative preparation includes:
Special attention to adequate hydration
Avoidance of hypothermia.
Transfusions
Indicated for anemia especially before splenectomy
For moderately severe episodes of the acute chest syndrome associated with new symptoms, such as fever,
cough, sputum production, or hypoxia.
Thalassemia
Group of inherited disorders of hemoglobin synthesis
Prevalent among people of Mediterranean extraction
As a group they are the most common genetic diseases defect.
The primary defect in all forms of thalassemia is reduced or absent production of hemoglobin chains
Two significant abnormalities:
Underproduction of hemoglobin
Excess production of unpaired hemoglobin subunits
Both factors contribute to the morbidity and mortality
The clinical spectrum of the thalassemias
Heterozygous carriers
Asymptomatic
Homozygous carriers
Present before 2 years of age
Pallor, growth retardation, jaundice, and abdominal swelling (Hepatosplenomegaly)
Other characteristic of thalassemia major include:
Intractable leg ulcers
Head enlargement
Frequent infections
Requirement for chronic blood transfusions.
Treatment for thalassemia consists:
Red blood cell transfusions
To keep the hemoglobin count > 9 mg/dL
Intensive parenteral chelation therapy
Deferoxamine.
Splenectomy
For patients with excessive transfusion requirements (> 200 mL/kg per year)
Discomfort because of splenomegaly
Painful splenic infarction.
Careful assessment:
Infectious morbidity following splenectomy is greater than in other patients undergoing splenectomy for
hematologic indications
BONE MARROW DISORDERS (MYELOPROLIFERATIVE DISORDERS)
Characterized by an abnormal growth of cell lines in the bone marrow.
The common underlying problem leading to splenectomy
Symptomatic splenomegaly.
Symptoms consist
Early satiety
Poor gastric emptying
Heaviness or pain in the left upper quadrant
Diarrhea.
Hypersplenism usually associated with splenomegaly
Chronic Myeloid Leukemia (CML)
Disorder of the primitive pluripotent stem cell in the bone marrow
Genetic hallmark
Transposition between the bcr gene on chromosome 9 and the abl gene on chromosome 22.
Clinical Findings
Frequently asymptomatic
Present with the gradual onset of fatigue, anorexia, sweating, and left upper quadrant pain and early satiety
secondary to splenomegaly.
Diagnosis
Significant increase in erythroid, megakaryotic, and pluripotent progenitors in the peripheral blood smear.
Treatment
Splenectomy
To ease pain and early satiety.
Acute Myeloid Leukemia (AML)
Characterized by a more rapid and dramatic clinical presentation than CML.
Increased risk for leukemic transformation to AML.
Polycythemia vera
Primary thrombocytosis
Myeloid metaplasia
Clinical Findings:
Viral-like illness with fever, malaise
Bone pain because of the expansion of the medullary space.
Splenomegaly is modest but palpable ~ 50%
Treatment
Splenectomy
If left upper quadrant pain and early satiety become unbearable.
Adds further risk of infection to immunocompromised by neutropenia and chemotherapy.
If untreated Death usually results within weeks to months
Chronic Myelomonocytic Leukemia
Associated with monocytosis in the peripheral smear (> 1 103/mm3) and in the bone marrow.
Splenomegaly occurs in one-half of these patients
Treatment:
Splenectomy can result in symptomatic relief.
Essential Thrombocythemia
Represents abnormal growth of the megakaryocyte cell line, resulting in increased levels of platelets in the
bloodstream.
Clinical manifestations of ET include:
Vasomotor symptoms
Thrombohemorrhagic events
Recurrent fetal loss
Transformation to myelofibrosis with myeloid metaplasia or acute myeloid leukemia
Splenomegaly 33%-50%
Treatment: Splenectomy
Not felt to be helpful in the early stages
Best reserved for the later stages of disease
Complication to surgery
Significant bleeding
Polycythemia Vera
Rare, chronic, progressive myeloproliferative disorder
Increase in red blood cell mass, frequently accompanied by leukocytosis, thrombocytosis, and splenomegaly.
Number of nonspecific complaints, including:
Headache, dizziness, weakness, pruritus, visual disturbances, excessive sweating, joint symptoms, and weight
loss.
Physical findings include
Ruddy cyanosis, conjunctival plethora, hepatomegaly, splenomegaly, and hypertension.
Treatment:
Phlebotomy
Aspirin
Chemotherapeutic agents.
Spelenctomy
Not helpful in the early stages
Best reserved for late-stage patients
Prognosis
Typically enjoy prolonged survival compared to others affected by hematologic malignancies.
Myelofibrosis (Agnogenic Myeloid Metaplasia)
Generic condition of fibrosis of the bone marrow
Specific, chronic, malignant hematologic disease
Associated with splenomegaly, red blood cell and white blood cell progenitors in the bloodstream, marrow
fibrosis, and extramedullary hematopoiesis
Underlying abnormality
Response to a clonal proliferation of hematopoietic stem cells.
Marrow failure often ensues, either:
Secondary to the fibrosis itself
Unknown malignant proliferation of cells
Clinical manifestations:
Asymptomatic ~ 20%
Most frequently related to ANEMIA
Including fatigue, weakness, dyspnea on exertion, and palpitations.
Others: Bleeding, fever, weight loss, gout/renal stones, night sweats, and symptoms because of an enlarged
spleen.
Nearly all patients with AMM
Nearly all have splenomegaly
35 % massive splenomegaly
67% hepatomegaly.
Diagnosis:
~ 96 cases = Nucleated red blood cells and immature myeloid elements in the blood are
Care must be taken, however, to exclude a history of a primary neoplasm or tuberculosis,
These conditions may develop secondary myelofibrosis.
Treatment
Asymptomatic patients
Closely followed and monitor
Symptomatic patients
Undergo therapeutic intervention targeted toward their symptoms.
Sprenectomy
Best treated with splenomegaly related symptoms
Effective palliation for nearly all patients with AMM
Preoperative workup:
Candidate must possess acceptable cardiac, pulmonary, hepatic, and renal reserve for the operation.
The coagulation system should be examined, including tests of coagulation factors V and VIII, fibrin split
products, platelet count, and bleeding time.
Low platelet counts may require adrenal steroids and/or platelet transfusion at the time of surgery.
Prognosis
Postoperative complications are more common in patients with AMM than in those with other hematologic
indications.
White Blood Cell Disorders
Leukemias
Chronic lymphocytic leukemia
Hairy cell leukemia
Both are amenable to treatment by splenectomy
Lymphoma
Non Hodgkin Disease
Hodgkin Disease
Chronic lymphocytic leukemia (CLL)
Symptoms of are nonspecific and include:
Weakness, fatigue, fever without illness, night sweats, and frequent bacterial and viral infections.
Splenomegaly
May be massive or barely palpable below the costal margin
Treatment:
Splenectomy
To improve cytopenias
May thus facilitate chemotherapy in patients whose cell counts were prohibitively low prior to spleen removal.
Palliative splenectomy also is indicated for symptomatic splenomegaly.
Hairy cell leukemia
Characterized by splenomegaly, pancytopenia, and large numbers of abnormal lymphocytes in the bone
marrow.
Number of complaints, including:
Anemia
Neutropenia
Thrombocytopenia,
Splenomegaly most common physical finding ~80%
Diagnosis
Lymphocytes contain irregular hair-like cytoplasmic projections identifiable on the peripheral smear
Treatment is indicated for:
Those with moderate to severe symptoms related to cytopenias, such as:
Repeated infections
Bleeding episodes
Splenomegaly.
Newer chemotherapeutic agents
Able to induce durable complete remission in most patients.
2-deoxycoformycin
2-chlorodeoxyadenosine
NonHodgkin lymphoma (NHL)
Encompasses all malignancies derived from the lymphoid system except classic Hodgkin disease.
Surgical staging is no longer indicated for NHL
History and physical examination, chest radiograph and abdominal/pelvic CT scan, biopsy of involved lymph
nodes and bone marrow biopsy is sufficient.
Splenomegaly
Exists in various, but not all, forms of NHL
Splenectomy
Indicated for symptoms related to an enlarged spleen
To improve cytopenias
Hodgkin disease (HD)
Disorder of the lymphoid systemcharacterized by the presence of Reed-Sternberg cells form the minority of the
Hodgkins tumor.
The spleen is often an occult site of spread
Massive splenomegaly is not common.
The staging procedure for HD begins:
Wedge biopsy of the liver
Splenectomy
Removal of representative nodes in the retroperitoneum,mesentery, and hepatoduodenal ligament.
Laparoscopic core biopsy of the liver
Performed under direct visualization, either using:
Tru-cut needle percutaneously or by
Wedge resection with shears and cautery.
Current indications for surgical staging include:
Clinical stage I
Stage II with nodular sclerosing histology
No symptoms referable to HD
Staging information affects treatment:
Radiotherapy
Early stage patients who have no splenic involvement
Chemotherapy or multimodality therapy
Splenic involvement
PLATELET DISORDERS
Idiopathic Thrombocytopenic Purpura (ITP)
Also called immune thrombocytopenic purpura
Autoimmune disorder characterized by a low platelet count and mucocutaneous and petechial bleeding.
Underlying abnormality:
Low platelet count stems from premature removal of platelets opsonized by antiplatelet IgG autoantibodies
produced in the spleen.
Patients with ITP typically present:
Petechiae
Ecchymosis
Some will experience major bleeding
Bleeding may occur from mucosal surfaces in the form:
Gingival bleeding
Epistaxis
Menorrhagia
Hematuria
Melena.
Risk for internal bleeding
Platelet counts < 10,000/mm3
The estimated incidence of ITP
~50% are children.
~ 1% major intracranial hemorrhage.
Children often present at a young age
Peak age approximately 5 years
Sudden onset several days to weeks after an infectious illness
Adults experience a more chronic form of disease with an insidious onset.
Splenomegaly with ITP is uncommon in both adults and children
Diagnosing ITP
Based on exclusion of other possibilities in the presence of a low platelet count and mucocutaneous bleeding:
Systemic lupus erythematosus,
Certain antimicrobials or other drugs
Laboratory findings:
Large, immature platelets (megathrombocytes) on peripheral blood smear.
Treatment
Oral Prednison
The usual first line of therapy
Dose of 1.01.5 mg/kg per day
Responses occur within the first 3 weeks, rates range from 5075%
Relapses are common.
Intravenous immunoglobulin
Dose of 1.0 g/kg per day for 23 days
Indicated for internal bleeding if below 5000/mm3 or when extensive purpura exists.
Immediate response is common, but a sustained remission is not
Splenectomy
Indicated for failure of medical therapy, or for most cases of first relapse
Provides a permanent response without subsequent need for steroids in 7585%
Management
Platelet replacement/transfusion
For lowplatelet counts (< 10,000/mm3)
Should not receive them preoperatively.
Given to those who continue to bleed after the splenic pedicle is ligated
Prognosis
In children with ITP, the course is self-limited, with durable and complete remission ~70%
Managed principally by observation, with shortterm therapy in select cases.
Splenectomy
Reserved for failure of medical therapy in children who have
Immune thrombocytopenic purpura for at least 1 year with symptomatic
Severe thrombocytopenia.
Urgent splenectomy may play a role in the rare circumstance of severe, life-threatening bleeding, in conjunction
with aggressive medical therapy.
Thrombotic thrombocytopenic purpura (TTP)
Serious, rare disorder characterized by thrombocytopenia, microangiopathic hemolytic anemia, and neurologic
complications.
Underlying abnormality:
Abnormal platelet clumping occurs in arterioles and capillaries
predisposing the patient to microvascular thrombotic episodes.
Clinical features of the disorder include:
Petechiae in lower extremities
Most common sign
Fever
Neurologic symptoms
Headaches to altered mental status, seizures, and even coma
Renal failure
Infrequently cardiac symptoms
Heart failure or arrhythmias
Differential Diagnosis by a negative Coombs test.
Evans syndrome (ITP and autoimmune hemolytic anemia)
Systemic lupus erythematosus
Treatment
Plasma exchange
The first line of therapy
Splenectomy
Plays a key role for patients who relapse or require multiple plasma exchanges to control symptoms
Generally well-tolerated without significant morbidity
Typically do not relapse.
Platelet transfusions are not recommended
MISCELLANEOUS DISORDERS AND LESIONS
Infections and abscess
Storage Diseases
Gauchers disease
Niemanns Pick Disease
Amyloidosis
Infiltrative Disorders
Felty Syndrome
Sarcoidosis
Cysts and Tumor
Portal Hypertension
Splenic Artery Aneurysm
Infections and Abscesses
Abscesses are uncommon, with incidence of 0.140.7 %,
Five distinct mechanisms of splenic abscess formation:
Hematogenous infection
Contiguous infection
Hemoglobinopathy
Immunosuppression, including hiv and chemotherapy
Trauma.
The most common origins for hematogenous spread are:
Infective endocarditis
Typhoid fever
Malaria
Urinary tract infection
Osteomyelitis
Clinical manifestations Presentation is frequently delayed
Fever
Left upper quadrant pain
Leukocytosis
Splenomegaly about 33%
Diagnosis
Confirmed by ultrasound or CT scan
95% sensitivity and specificity
Treatment
Broad-spectrum antibiotics for 14 days.
Splenectomy is the operation of choice
Percutaneous drainage
Optional
successful for patients with unilocular disease.
Open drainage
Options for patients who cannot tolerate splenectomy.
Gauchers disease.
Inherited lipid storage disease
Deposition of glucocerebroside in cells of the macrophage-monocyte system.
Clinical features
Early satiety
Abdominal discomfort
Hypersplenism
Includethrombocytopenia, normocytic anemia, and mild leukopenia.
Treatment
Splenectomy
Alleviates hematologic abnormalities in patients with hypersplenism
Does not correct the underlying disease process.
Niemann-Pick disease.
Inherited disease of abnormal lysosomal storage of sphingomyelin and cholesterol in cells of the macrophagemonocyte system.
Types A and B forms
Most likely to demonstrate splenomegaly with its concomitant symptoms.
Treatment
Splenectomy
Successfully treat symptoms of splenomegaly
Amyloidosis
Disorder of abnormal extracellular protein deposition.
Treatment
Splenectomy
Relieved symptoms of splenomegaly
To cure patients of factor X deficiency associated with primary amyloidosis
Felty Syndrome
The triad of:
Rheumatoid arthritis (RA)
Splenomegaly
Neutropenia
Spleen is 4x heavier than normal
Neutropenia
Causing frequent infections
Driving force behind the decision for splenectomy
Treatment of neutropenia
Hematopoeitic growth factors
Methothrexate
Splenectomy
Sarcoidosis
Inflammatory disease of young adults
Characterized by noncaseating granulomas in affected tissues.
Any organ system may be involved:
Lung most common
Spleen 2nd common
25% have Splenomegaly
Massive splenomegaly (>1 kg) is rare.
Treatment: Splenectomy
Indicated for symptomatic splenomegaly and hypersplenism
Relieves symptoms and corrects hematologic abnormalities such as anemia and thrombocytopenia.
Cysts
Splenic cysts are rare lesions
Most common etiology for splenic cysts
Parasitic infestation, particularly echinococcal.
Treatment for Symptomatic parasitic cysts are:
Splenectomy choice treatment
Also amenable to percutaneous aspiration, instillation of protoscolicidal agent, and reaspiration.
Nonparasitic cysts
Also called Pseudocyst
Most commonly result from trauma
Treatment and Management of Nonparasitic cysts
Asyptomatic patients
Observed with close ultrasound follow up to exclude significant expansion
Advised of the risk of cyst rupture with even minor abdominal trauma
Small symptomatic nonparasitic cysts
May be excised with splenic preservation
May be performed laparoscopically.
Large symptomatic nonparasitic cysts
May be unroofed. Both of these operations
May be performed laparoscopically.
Tumors
Sarcomatous
Most common primary tumor of the spleen
NonHodgkin lymphoma of the spleen
Rare, but splenectomy imparts an excellent prognosis.
Lung cancer
Most common tumor to spread to the spleen.
Portal Hypertension
Result from numerous causes
Usually is because of cirrhosis.
Often accompanied by splenomegaly and splenic congestion
Splenectomy
Not indicated for hypersplenism
No correlation exists between the degree of pancytopenia and long-term survival
Curable if Portal hypertension secondary to splenic vein thrombosis
Splenic vein thrombosis
Should be examined if with bleeding from isolated gastric varices in the presence of normal liver function tests
Especially with a history of pancreaticdisease,
Splenic Artery Aneurysm
Rare but most common visceral artery aneurysm
Usually arises in the middle to distal portion of the splenic artery.
The risk of rupture
Between 3 and 9 %
If rupture occurs, mortality is substantial 3550%.
If rupture during pregnancy, mortality:
Mother (70 %)
Fetus (95 %).
Indications for treatment include:
Presence of symptoms
Pregnancy
Intention to become pregnant, and
Pseudoaneurysms associated with inflammatory processes.
Indication for surgery:
For asymptomatic patients, size > 2 cm
Treatment:
Aneurysm resection or ligation alone
Acceptable for amenable lesions in the mid-splenic artery,
Splenectomy
For distal lesions in close proximity to the splenic hilum
PREOPERATIVE CONSIDERATIONS
Splenic Artery Embolization
Became available with advances in angiographic technology.
Theoretical advantages of SAE include:
Reduced operative blood loss from a devascularized spleen
Reduced spleen size for easier dissection and removal.
Potential disadvantages of the procedure include
Acute left-sided pain (although usually of limited duration)
Pancreatitis
Other embolization-related complications.
There is currently no consensus on the role of preoperative SAE for elective splenectomy.
Vaccination
Splenectomy imparts a small (<15%) but definite life-time risk of fulminant, potentially life-threatening infection.
Therefore, when elective splenectomy is planned,
Vaccinations against encapsulated bacteria
Should be given at least 2 weeks before surgery:
Streptococcus pneumonia
Haemophilus influenzae type B
Meningococcus
If the spleen is removed emergently (e.g., for trauma),
Should be given as soon as possible following surgery, allowing at least 12 days for recovery.
Booster injections of pneumococcal vaccine
Should be considered every 56 years
Annual influenza immunization is advisable.
Deep Venous Thrombosis Prophylaxis
For patients undergoing splenectomy
Deep venous thrombosis (DVT) is common following splenectomy, especially in cases involving:
Splenomegaly
Myeloproliferative disorders (MPD).
The risk of portal vein thrombosis (PVT) may ~ 40%
For patients with both splenomegaly and MPD.
Postsplenectomy PVT typically presents with:
Anorexia
Abdominal pain
Leukocytosis
Thrombocytosis
Keys to successful treatment for PVT: High index of suspicion
Early diagnosis with contrast-enhanced CT
Immediate anticoagulation
DVT prophylaxis
Compression devices with subcutaneous heparin (5000 U).
Patients risk factors for DVT
Obesity
History of prior VTE
Known hypercoagulable state
Age > 60
More Aggressive antithrombotic regimen, including low-molecular-weight heparin (LMWH)
SPLENECTOMY TECHNIQUES
Patient Preparation
Vaccination for elective splenectomy at least 1 week preoperatively with:
Polyvalent pneumococcal
Meningococcal
Haemophilus.
Blood product transfusion
Anemic patients
Transfused to a hemoglobin of 10 g/dL.
For more complex patients, including those with splenomegaly
Type and cross is recommended for at least 24 units of blood.
Platelet transfusions
May transiently correct thrombocytopenia
Preferably not preoperatively
Ideally not before intraoperative ligation of the splenic artery.
Perioperatively parenteral corticosteroid therapy
Patients who have been maintained on corticosteroid therapy preoperatively:
Deep vein thrombosis (DVT) prophylaxis
Intravenous administration of a first-gen. cephalosporin.
Nasogastric (NG) tube
To decompress the stomach.
Open Splenectomy (OS)
Widely practiced due to the standard approach of laparoscopic surgery (LS) for normosplenic patients
Indication for:
Traumatic rupture of the spleen Most indication
Massive splenomegaly
Ascites
Portal hypertension
Multiple prior operations
Extensive splenic radiation
Possible splenic abscess.
Open Splenectomy Technique
Incision
Left subcostal incision
Preferred for most elective splenectomies
Midline incision
If exposure of a ruptured
If massively enlarged spleen
If abdominal access is needed for a staging laparotomy.
Dividing ligamentous attachment to mobilizes the spleen
Splenocolic ligament
First to divide
Splenophrenic ligament
Spleens lateral peritoneal attachments
Further medial mobilization
Role of early ligation of the splenic artery
Safer manipulation of the spleen and dissection of the splenic hilum,
Spleen shrinkage
Autotransfusion of erythrocytes and platelets.
Pointers:
Early ligation of splenic artery for patients with significant splenomegaly
Avoid injuring the tail of the pancreas.
Splenic bed is not routinely drained.
Laparoscopic Splenectomy
Supplanted OS as the elective splenectomy approach of
Laparoscopic Splenectomy Tachnique/Procedure
Vital anatomy
Allowing for an intuitive dissection sequence.
Short gastric vessels and splenic hilum are divided by:
Individual clip applications
Endovascular staples
Hemostatic energy sources
Pointers
Lower spleen pole can be elevated
For accessible dissection of splenic hilum
Retract to spleen
For easily visualizes the tail of the pancreas and can avoid its injury. .
Surgeons hand
Introduced completely into the peritoneal cavity for palpation of appropriate tissues
Allows for identification, retraction, and dissection.
Partial Splenectomy
Amenable for certain lipid storage disorders and some forms of traumatic splenic injury
Indicated in children to minimize postsplenectomy sepsis risk
SPLENECTOMY OUTCOMES
Changes to blood composition
Appearance of Howell-Jolly bodies
Siderocytes.
Leukocytosis
Increased platelet counts commonly
Classification of Complications:
Pulmonary
Left lower lobe atelectasis,
~ 16%, most complication
Pleural effusion
Pneumonia
Hemorrhagic ~ 3%
Intraoperative hemorrhage
Postoperative hemorrhage
Infectious
Subphrenic abscess
Wound infection
Pancreatic
Pancreatitis
Pseudocyst
Pancreatic fistula
Thromboemboli ~ 5-10%
Hematologic Outcomes
Thrombocytopenia
Long-term response
Platelet count > 150,000/mL, > 2 months after surgery without medications.
Laparoscopic splenectomy provide a long-term platelet response in 85% with ITP.
Chronic hemolytic anemias
Rise in hemoglobin levels to >10 g/dL
Without the need for transfusion signifies a successful response to splenectomy.
Success rate 60-80% of splenectomy
Patients with spherocytosis
Success rate 90100% of splenectomy.
Laparoscopic approach typically results:
Longer operative times
Shorter hospital stays
Lower morbidity rates
Similar blood loss
Similar mortality rates.
Overwhelming Postsplenectomy Infection (OPSI)
OPSI usually develops within the first 2 years after splenectomy due the loss of spleens ability
More likely to occur:
Children > Adults
With hematologic disorders > splenic trauma.
Loss of the spleens ability:
To filter and phagocytose bacteria
Parasitized blood cells
Loss of a significant source of antibody production.
The most common source of infection:
Streptococcus pneumonia ~5090%
H. influenzae type
B, meningococcus
Group A streptococci
Clinical findings:
Mild-appearing prodrome:
Fever, malaise, myalgias, headache, vomiting, diarrhea, and abdominal pain.
May progress rapidly to fulminant bacteremic septic shock, with accompanying hypotension, anuria, and DIC
Risk factors for the development of OPSI:
Patients undergoing splenectomy for hematologic indications
Hodgkin disease
Those taking chemotherapy or radiation therapy
Prophylaxis and vaccination
Immunoprophylaxis consists of pneumococcal, meningococcal, and H. influenzae type B vaccination
Pneumococcal vaccine booster injections
Annual influenza immunization
Antibiotic prophylaxis
Penicillin or amoxicillin
Single Daily Dose for asplenic children for the first 2 years after splenectomy.
S-ar putea să vă placă și
- NEET SS January 2022 MCh GI Surgery RecallDocument58 paginiNEET SS January 2022 MCh GI Surgery RecallRajhan 410Încă nu există evaluări
- MOST IMPORATANT ONE LINERS Compiled by Medicinosis Magnus 2Document18 paginiMOST IMPORATANT ONE LINERS Compiled by Medicinosis Magnus 2VAIBHAV SHARMA- 122Încă nu există evaluări
- Schwartz Cpap 16 Skin and Subcutaneous TissueDocument16 paginiSchwartz Cpap 16 Skin and Subcutaneous TissueRem AlfelorÎncă nu există evaluări
- Absite High Yield 2008Document50 paginiAbsite High Yield 2008Shawn Robinson100% (4)
- Essential Notes in General SurgeryDe la EverandEssential Notes in General SurgeryEvaluare: 4.5 din 5 stele4.5/5 (6)
- 1-4 Hemostasis, Surgical Bleeding and TransfusionDocument17 pagini1-4 Hemostasis, Surgical Bleeding and TransfusionRobin Tolentino100% (3)
- SURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Document13 paginiSURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Medisina101Încă nu există evaluări
- Hemolytic Anemia - Evaluation and Differential DiagnosisDocument8 paginiHemolytic Anemia - Evaluation and Differential Diagnosiscarolinapolotorres100% (1)
- Surgery 1Document73 paginiSurgery 1Ong Kie80% (5)
- 5B Surgery 1st-2nd SE #28-32 #17-18Document3 pagini5B Surgery 1st-2nd SE #28-32 #17-18Liza SoberkaayoÎncă nu există evaluări
- Internal Hernias Diagnosis and TypesDocument26 paginiInternal Hernias Diagnosis and TypesIslam MagdyÎncă nu există evaluări
- Swarthz TRAUMADocument26 paginiSwarthz TRAUMAAlexandra Niken Larasati75% (4)
- 5 6057345046456304562Document490 pagini5 6057345046456304562DK DeepakÎncă nu există evaluări
- Physiologic Monitoring of The Surgical PatientDocument56 paginiPhysiologic Monitoring of The Surgical PatientSeid Adem100% (2)
- General and Vascular Surgery Princess Margaret Hospital: Dr. D. FarquharsonDocument16 paginiGeneral and Vascular Surgery Princess Margaret Hospital: Dr. D. FarquharsonacklinsdocÎncă nu există evaluări
- A Disease Study On: AppendectomyDocument8 paginiA Disease Study On: Appendectomybryan leguiabÎncă nu există evaluări
- My Notes For USMLEDocument1 paginăMy Notes For USMLEmonica ortizÎncă nu există evaluări
- Neurogenic Shock: Understanding the Hemodynamic ResponseDocument7 paginiNeurogenic Shock: Understanding the Hemodynamic Responseyayayaniza100% (1)
- Surgery TacticsDocument154 paginiSurgery TacticsAiman Arifin0% (1)
- NEET-SS GI SurgeryDocument72 paginiNEET-SS GI SurgeryadiÎncă nu există evaluări
- Long Cases in General Surgery: 2nd EditionDocument259 paginiLong Cases in General Surgery: 2nd EditionDiornald Mogi100% (1)
- Schwartz UrologyDocument10 paginiSchwartz UrologyRem Alfelor100% (1)
- Metabolic Response To InjuryDocument55 paginiMetabolic Response To InjuryMuhammad NaveedÎncă nu există evaluări
- Chapter Summary - PANCREAS Final (Schwartz) PDFDocument19 paginiChapter Summary - PANCREAS Final (Schwartz) PDFMiguel Cuevas DolotÎncă nu există evaluări
- Absite January2014 ReviewDocument1.226 paginiAbsite January2014 ReviewAnnTran100% (12)
- Surgical Oncology and Breast BiopsyDocument12 paginiSurgical Oncology and Breast Biopsybo gum parkÎncă nu există evaluări
- SCHWARTZ Surgical InfectionDocument25 paginiSCHWARTZ Surgical InfectionAlexandra Niken Larasati78% (9)
- Benign Gynecologic LesionsDocument103 paginiBenign Gynecologic Lesions201286% (7)
- Wound Healing SchwartzDocument37 paginiWound Healing SchwartzCarla Putri Chandra100% (1)
- Surgical InfectionDocument9 paginiSurgical InfectionJL DeomampoÎncă nu există evaluări
- Schwartz Hour - BurnDocument62 paginiSchwartz Hour - BurnM3 SURGERY100% (1)
- A System of Operative Surgery, Volume IV (of 4)De la EverandA System of Operative Surgery, Volume IV (of 4)Evaluare: 4 din 5 stele4/5 (1)
- 0.6 Surgery Trans PDFDocument17 pagini0.6 Surgery Trans PDFJoy ManzanoÎncă nu există evaluări
- Absite CH 32 BilliaryDocument14 paginiAbsite CH 32 BilliaryJames JosephÎncă nu există evaluări
- Breast Schwartz 2015 10th EditionDocument141 paginiBreast Schwartz 2015 10th EditionKlaire LodroñoÎncă nu există evaluări
- History Taking for Gallstones (CholelithiasisDocument6 paginiHistory Taking for Gallstones (CholelithiasisToria053Încă nu există evaluări
- Bowel AnastomosisDocument30 paginiBowel AnastomosismrashaiedehÎncă nu există evaluări
- Schwarts - BurnDocument43 paginiSchwarts - BurnAlexandra Niken Larasati100% (4)
- BURNS INITIAL EVALUATION GUIDEDocument80 paginiBURNS INITIAL EVALUATION GUIDEmarÎncă nu există evaluări
- Therapeutic Apheresis (Plasma Exchange or Cytapheresis) - Indications and TechnologyDocument16 paginiTherapeutic Apheresis (Plasma Exchange or Cytapheresis) - Indications and TechnologyBS3091Încă nu există evaluări
- Cystic LesionsDocument101 paginiCystic LesionsKartik GuptaÎncă nu există evaluări
- The Spleen - A Surgical Perspective: by Col. Abrar Hussain ZaidiDocument43 paginiThe Spleen - A Surgical Perspective: by Col. Abrar Hussain Zaidiabrar_zaidiÎncă nu există evaluări
- Pediatric Surgery Conditions of the Respiratory and Gastrointestinal SystemsDocument12 paginiPediatric Surgery Conditions of the Respiratory and Gastrointestinal SystemsRenatoCosmeGalvanJunior100% (1)
- C 10 + 11 GALLBLADDER AND BILIARY TRACT Part1Document45 paginiC 10 + 11 GALLBLADDER AND BILIARY TRACT Part1mikaaa0000% (1)
- Pediatric Surgery Dr. A. IgamaDocument6 paginiPediatric Surgery Dr. A. IgamaMarco Paulo Reyes NaoeÎncă nu există evaluări
- The Surgical Oncology Review: For the Absite and BoardsDe la EverandThe Surgical Oncology Review: For the Absite and BoardsÎncă nu există evaluări
- University of Perpetual Help Rizal Jonelta Foundation School of Medicine Department of Surgery - ConsortiumDocument17 paginiUniversity of Perpetual Help Rizal Jonelta Foundation School of Medicine Department of Surgery - Consortiummefav7778520Încă nu există evaluări
- Gastrectomy 1Document86 paginiGastrectomy 1Mysnow OpalÎncă nu există evaluări
- Pancreatic Cancer: Early Detection Offers Best Chance of CureDocument18 paginiPancreatic Cancer: Early Detection Offers Best Chance of Curemywifenoor1983Încă nu există evaluări
- Benign Anorectal Conditions: Ahmed Badrek-AmoudiDocument20 paginiBenign Anorectal Conditions: Ahmed Badrek-AmoudiAna De La RosaÎncă nu există evaluări
- Schwartz 9th Ed: Chapter Outline: The SpleenDocument22 paginiSchwartz 9th Ed: Chapter Outline: The SpleenKathryn Reunilla100% (1)
- Penetrating Abdominal Injury DiagnosisDocument3 paginiPenetrating Abdominal Injury DiagnosisRaquel ReyesÎncă nu există evaluări
- Bile Duct InjuryDocument62 paginiBile Duct InjuryShashidhara Puttaraj100% (1)
- Schwartz's Hemostasis, Surgical BleedingDocument33 paginiSchwartz's Hemostasis, Surgical BleedingArifHidayat100% (4)
- Dr. E. J. Arteen F.R.C.S General & Colorectal Consultant Surgeon European-Gaza HospitalDocument83 paginiDr. E. J. Arteen F.R.C.S General & Colorectal Consultant Surgeon European-Gaza Hospitalpt.mahmoudÎncă nu există evaluări
- Upper Gastrointestinal Bleeding (Ugib) : First Shift: August 13, 2018Document10 paginiUpper Gastrointestinal Bleeding (Ugib) : First Shift: August 13, 2018Angelo Dela Cruz VillaromanÎncă nu există evaluări
- On PurpuraDocument22 paginiOn Purpurakiran kumari yadav100% (1)
- Approach To Patients With Inguinoscrotal Masses: Section of Urology Department of Surgery The Medical CityDocument43 paginiApproach To Patients With Inguinoscrotal Masses: Section of Urology Department of Surgery The Medical CityKevin Eric SantosÎncă nu există evaluări
- 1.40 (Surgery) GIT Surgical Diseases - Diagnostics - Obesity ManagementDocument10 pagini1.40 (Surgery) GIT Surgical Diseases - Diagnostics - Obesity ManagementLeo Mari Go LimÎncă nu există evaluări
- Surgery II - Pancreas 2014Document20 paginiSurgery II - Pancreas 2014Medisina101Încă nu există evaluări
- Surgery 1.1 Fluid and Electrolyte Balance - Azares PDFDocument7 paginiSurgery 1.1 Fluid and Electrolyte Balance - Azares PDFAceking MarquezÎncă nu există evaluări
- Surgical Anatomy of The Chest Wall, Pleura, and MediastinumDocument8 paginiSurgical Anatomy of The Chest Wall, Pleura, and MediastinumNooneÎncă nu există evaluări
- Abdominal Pain Content PDFDocument71 paginiAbdominal Pain Content PDFyanÎncă nu există evaluări
- 1 LiverDocument10 pagini1 LiverAlbino Fulgencio Santos III100% (1)
- 4 PEDIA 8 - Bleeding DisordersDocument5 pagini4 PEDIA 8 - Bleeding DisordersRainy Liony DuhÎncă nu există evaluări
- Preparing Severely Jaundiced Patient For SurgeryDocument2 paginiPreparing Severely Jaundiced Patient For Surgerylentini@maltanet.netÎncă nu există evaluări
- Thrombotic Microangiopathies: T. Matthew Eison, MD Lebonheur Children'S Hospital Pediatric NephrologyDocument83 paginiThrombotic Microangiopathies: T. Matthew Eison, MD Lebonheur Children'S Hospital Pediatric NephrologyMarcelliaÎncă nu există evaluări
- Platelets - The Lancet 2000Document9 paginiPlatelets - The Lancet 2000bluemleinÎncă nu există evaluări
- Protocol TPEDocument19 paginiProtocol TPEPatricia TamasÎncă nu există evaluări
- Thrombotic Thrombocytopenic Purpura PDFDocument6 paginiThrombotic Thrombocytopenic Purpura PDFDany EdyÎncă nu există evaluări
- Ash TTP RefractoryDocument8 paginiAsh TTP RefractoryJulius Dominique L. AnjaoÎncă nu există evaluări
- Guidelines For The Rational Use of Blood Blood ProductsDocument120 paginiGuidelines For The Rational Use of Blood Blood ProductsHafiz Hamidi100% (1)
- Platelet Disorders: Autoimmune ThrombocytopeniasDocument6 paginiPlatelet Disorders: Autoimmune ThrombocytopeniasShī Fu KoÎncă nu există evaluări
- HemaDocument17 paginiHemakamaluÎncă nu există evaluări
- Managing Coagulopathy ICUDocument38 paginiManaging Coagulopathy ICUMirabela Colac100% (1)
- Icsh Hemostasis Critical ValuesDocument12 paginiIcsh Hemostasis Critical Valuescitometria prolabÎncă nu există evaluări
- Atypical Thrombotic Thrombocytopenic PurpuraDocument5 paginiAtypical Thrombotic Thrombocytopenic PurpuraOrxan HumbetovÎncă nu există evaluări
- Oxford McqsDocument15 paginiOxford McqsaliaaÎncă nu există evaluări
- Eferesis 2008Document17 paginiEferesis 2008xander trujilloÎncă nu există evaluări
- Quiz - Red Blood Cell and Bleeding Disorder - Attempt ReviewDocument83 paginiQuiz - Red Blood Cell and Bleeding Disorder - Attempt ReviewAdrian CaballesÎncă nu există evaluări
- Evans Syndrome - StatPearls - NCBI BookshelfDocument4 paginiEvans Syndrome - StatPearls - NCBI BookshelfJunbek nov23Încă nu există evaluări
- Comparative Study of Serum and Biliary Lipid Profile in Libyan Gallstone PatientsDocument54 paginiComparative Study of Serum and Biliary Lipid Profile in Libyan Gallstone PatientsJagannadha Rao PeelaÎncă nu există evaluări
- Management of Stroke in PregnancyDocument10 paginiManagement of Stroke in PregnancyIwi DancelÎncă nu există evaluări
- PracticeExam1 & 2Document160 paginiPracticeExam1 & 2Arash SamieiÎncă nu există evaluări
- Hypertensive Disorders in PregnancyDocument10 paginiHypertensive Disorders in PregnancyRwabugili ChrisÎncă nu există evaluări
- Causes and Types of Low Platelet Count (ThrombocytopeniaDocument4 paginiCauses and Types of Low Platelet Count (Thrombocytopeniavenni dimitriÎncă nu există evaluări
- Part 1 Examination: Candidates Must Answer All Questions. Each Question Is Worth A Total of 25 MarksDocument15 paginiPart 1 Examination: Candidates Must Answer All Questions. Each Question Is Worth A Total of 25 MarksSyed Danish AliÎncă nu există evaluări
- Plasmaflux Psu Filters PDFDocument4 paginiPlasmaflux Psu Filters PDFMauricio Martinez ReyesÎncă nu există evaluări
- Haemostasis TutorialDocument5 paginiHaemostasis TutorialRonaldoÎncă nu există evaluări
- Managing bleeding disorders during pregnancyDocument7 paginiManaging bleeding disorders during pregnancyKharismaNisaÎncă nu există evaluări