Documente Academic
Documente Profesional
Documente Cultură
A. Demographic: Patient's Profile
Încărcat de
Steffi MurielDescriere originală:
Titlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
A. Demographic: Patient's Profile
Încărcat de
Steffi MurielDrepturi de autor:
Formate disponibile
Patients Profile
A. Demographic
Name:
Address:
Age: 20 year old
Gender: Male
Civil Status: Single
Occupation:
Nationality:
Religion:
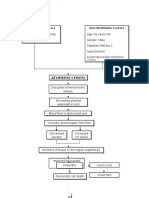
Admitting diagnosis:
Date of Admission:
Time of Admission:
B. Chief Complaint
Gynecomastia.
C. History of the Present Illness
The patient came in for a routine annual examination to establish adult
care and was evaluated because of gynecomastia.
D. History of the Past Illness
When patient was between 6 to 13 years old, patient had:
o Generalized nocturnal tonic-clonic seizures;
o Focal seizures involving the right leg, approximately twice a
o
year, for a total of 10-13 generalized seizure; and
Had taken carbamazepine until 14 years old after which the
seizure did not recur.
When patient was 7 years old, patient had:
o MRI of the head which revealed no abnormalities.
6 months PTA, patient had:
o Extracted his wisdome tooth;
o Constipation; and
o Chronic pilonidal cyst.
3 year history of:
o Bilateral chest enlargement with no nipple discharges;
o Occasional morning erections;
o Has never been sexually active, did not masturbate.
4 years before this evaluation, patient had:
o Increased thirst; (thirst was normal months before this
o
o
evaluation);
Fluid consumption;
Frequent urination, 4 to 5 times during the day and up to 3 times
each night; (months before evaluation frequency of urination
has decreased)
Patient had a several-year history of:
o Blurred vision which was correctedwith glasses; and
o Has occasional headaches after exertion
8 months PTA:
o Frequency of shaving decreased from weekly to every 2 weeks
E. Social History
Patient was a college student;
Lived with his parents;
Rarely drank alcohol; and
Had never smoked or used illicit drugs
F. Family History
His father had basal cell carcinoma;
maternal uncle had had colon cancer at 36 years of age;
his paternal grandfather died of colon cancer; and
his maternal grandfather had had renal cancer.
G. Allergies
No known allergies noted.
H. ASSESSMENT
Blood Pressure: 98/62 mm Hg, other vital signs were normal
Height= 179cm
Weight= 85kg
BMI= 26.5
1. Physical Assessment
1. General
The patient appeared young for his age
2. Chest
and had minimal facial hair.
Both breasts were enlarged, with no
3. Reproductive system
nipple retraction, masses, or discharge.
The testicles were small (approximately
2.5 cm in length; has small posterior
anal fissure and a small lump over the
coccyx with a central punctum and no
discharge.
S-ar putea să vă placă și
- Incomplete Abortion PanggoDocument20 paginiIncomplete Abortion PanggoRoselle Joy D. RosalejosÎncă nu există evaluări
- Tugas Penilaian Status GiziDocument12 paginiTugas Penilaian Status GiziZahra ZahiraÎncă nu există evaluări
- Gynecology Case PresentationDocument10 paginiGynecology Case PresentationAmrin TankÎncă nu există evaluări
- Soap NotesDocument4 paginiSoap NotesLatora Gardner Boswell100% (3)
- Case DonyDocument17 paginiCase Donymuhamad donyÎncă nu există evaluări
- Buergers Power PointDocument16 paginiBuergers Power PointYan VencerÎncă nu există evaluări
- Complete Nursing Health HistoryDocument23 paginiComplete Nursing Health Historyrbulibol100% (5)
- Rectal AdenocarcinomaDocument93 paginiRectal AdenocarcinomaLara MenÎncă nu există evaluări
- Bell113016nursfallsoapnote4 WomenshealthDocument21 paginiBell113016nursfallsoapnote4 Womenshealthapi-350882100Încă nu există evaluări
- Long Case Rama FixDocument13 paginiLong Case Rama FixRamaÎncă nu există evaluări
- HistoryDocument7 paginiHistoryMaryamÎncă nu există evaluări
- StephanieDocument35 paginiStephaniepermatamoÎncă nu există evaluări
- Case History: Personal DataDocument5 paginiCase History: Personal DataMohammed AhmedÎncă nu există evaluări
- PEDIA Case - Pneumonia 2 VSDDocument17 paginiPEDIA Case - Pneumonia 2 VSDGrace Antonette PatiÎncă nu există evaluări
- Case Study AnemiaaaaDocument40 paginiCase Study Anemiaaaageniziz rafaelÎncă nu există evaluări
- History: O Identifying DataDocument10 paginiHistory: O Identifying DataJofen Ann Hisoler TangpuzÎncă nu există evaluări
- Child With Respiratory DisorderDocument4 paginiChild With Respiratory Disorderleih jsÎncă nu există evaluări
- Gynecologic Neoplasia Topic 1: Gestational Trophoblastic Neoplasia (GTD)Document4 paginiGynecologic Neoplasia Topic 1: Gestational Trophoblastic Neoplasia (GTD)Elaine Marie Rendon PalmejarÎncă nu există evaluări
- Health HistoryDocument7 paginiHealth Historyapi-545001894Încă nu există evaluări
- Peds Case 3Document5 paginiPeds Case 3Mohammed AhmedÎncă nu există evaluări
- Pneumonia: - "The Forgotten Killer"Document38 paginiPneumonia: - "The Forgotten Killer"MishaDehalÎncă nu există evaluări
- Araullo University FinalDocument19 paginiAraullo University FinalManzano JenecaÎncă nu există evaluări
- Abortion, Myoma, H Mole, EctopicDocument93 paginiAbortion, Myoma, H Mole, Ectopicdhainey100% (4)
- Ward Work 1Document6 paginiWard Work 1Jermaine SerranoÎncă nu există evaluări
- Obstructive Uropathy Secondary To Benign Prostatic HyperplasiaDocument74 paginiObstructive Uropathy Secondary To Benign Prostatic HyperplasiaGregory Litang100% (1)
- (WR) Group 2 - Ward Work 4Document9 pagini(WR) Group 2 - Ward Work 4Rodrigo Joseph PaysonÎncă nu există evaluări
- Antenatal ExaminationDocument8 paginiAntenatal ExaminationAli 13Încă nu există evaluări
- Case Protocol OB - H MOLEDocument3 paginiCase Protocol OB - H MOLEKim Adarem Joy ManimtimÎncă nu există evaluări
- Case Scenario Peptic UlcerDocument2 paginiCase Scenario Peptic Ulcerchetankumarbhumireddy0% (1)
- CPC CaseDocument8 paginiCPC CasePingky khingthongÎncă nu există evaluări
- Pedia 1Document8 paginiPedia 1Jani MisterioÎncă nu există evaluări
- Case Press Ob WardDocument9 paginiCase Press Ob Wardjohn castroÎncă nu există evaluări
- Case 5 Gastric Carcinoma: Divided Into A Number of Subtypes IncludingDocument18 paginiCase 5 Gastric Carcinoma: Divided Into A Number of Subtypes IncludingGaurav UpretiÎncă nu există evaluări
- Pediatrics Preceptorial JuanitasMDDocument5 paginiPediatrics Preceptorial JuanitasMDCharles Jebb Belonio JuanitasÎncă nu există evaluări
- Health History Documentation Form ChristinaDocument6 paginiHealth History Documentation Form Christinaapi-545542584Încă nu există evaluări
- Case Presentation: Group 9Document141 paginiCase Presentation: Group 9marialourdes2489Încă nu există evaluări
- Dengue Case Presentation Pedia (PCMC)Document59 paginiDengue Case Presentation Pedia (PCMC)Michael Valderrama100% (4)
- Case 22-2007: A Woman With A Family History of Gastric and Breast CancerDocument9 paginiCase 22-2007: A Woman With A Family History of Gastric and Breast CancerBulborea MihaelaÎncă nu există evaluări
- Surg Week 4Document75 paginiSurg Week 4Casey YanoÎncă nu există evaluări
- A Case Study On Colon MassDocument29 paginiA Case Study On Colon MassDahlia D. SuelloÎncă nu există evaluări
- Case-Protocol-Hodgkins FinalDocument14 paginiCase-Protocol-Hodgkins FinalbabbettemdÎncă nu există evaluări
- CR HematoDocument89 paginiCR HematoEsther BoasÎncă nu există evaluări
- Cryptic Cachexia: Clinical Problem-SolvingDocument7 paginiCryptic Cachexia: Clinical Problem-SolvingrestiÎncă nu există evaluări
- Hirschsprung'S Disease in A Child: Case ReportDocument57 paginiHirschsprung'S Disease in A Child: Case ReportHans NatanaelÎncă nu există evaluări
- Exposure To Toxic SubstancesDocument21 paginiExposure To Toxic SubstancesDavid VillanuevaÎncă nu există evaluări
- Geri SOAPsampleDocument8 paginiGeri SOAPsampleJacquelineÎncă nu există evaluări
- Benign Gynecologic Lesions 2 Dr. Castro July 13, 2022Document26 paginiBenign Gynecologic Lesions 2 Dr. Castro July 13, 2022JohnJoelArzagaÎncă nu există evaluări
- Case AGNDocument66 paginiCase AGNMohaima PanditaÎncă nu există evaluări
- SamplesDocument4 paginiSamplesRalph Lawrence Ruiz Tagorda0% (1)
- Single Best Answer (SBA) QuestionsDocument16 paginiSingle Best Answer (SBA) QuestionsKrairat Komdee50% (2)
- Severe Malaria With HaemoglobulinuriaDocument9 paginiSevere Malaria With HaemoglobulinuriaNAMANYA ASA MUHOOZIÎncă nu există evaluări
- Short StatureDocument14 paginiShort StatureEmily EresumaÎncă nu există evaluări
- Case Study QossayDocument10 paginiCase Study QossayAngel Joy CatalanÎncă nu există evaluări
- Integration Activity 3 PDFDocument18 paginiIntegration Activity 3 PDFCzarinaÎncă nu există evaluări
- Emergency Services Admission ReportDocument2 paginiEmergency Services Admission ReportJaslynn White100% (3)
- Gyn Uterine Myoma EkarinaDocument21 paginiGyn Uterine Myoma EkarinaarifsandroÎncă nu există evaluări
- Long Case Presentation: Saadia Rehman (1502-mbbs-038)Document42 paginiLong Case Presentation: Saadia Rehman (1502-mbbs-038)Radial ArteryÎncă nu există evaluări
- Grand Rounds Case PresentationDocument13 paginiGrand Rounds Case PresentationMaurice OballoÎncă nu există evaluări
- Esller History and PEDocument4 paginiEsller History and PEKUNWAR BRIKSHAÎncă nu există evaluări
- Nurselabs PEDIA QuestionsDocument13 paginiNurselabs PEDIA QuestionsSteffi MurielÎncă nu există evaluări
- CellulitisDocument1 paginăCellulitisSteffi MurielÎncă nu există evaluări
- Ca2 HW1Document1 paginăCa2 HW1Steffi MurielÎncă nu există evaluări
- Ccu Patho AcsDocument2 paginiCcu Patho AcsSteffi MurielÎncă nu există evaluări
- Modifiable Risk Factors: Non-Modifiable Risk Factors:: IV. Pathophysiology of Chronic Kidney DiseaseDocument5 paginiModifiable Risk Factors: Non-Modifiable Risk Factors:: IV. Pathophysiology of Chronic Kidney DiseaseSteffi MurielÎncă nu există evaluări
- Imaging Studies of The ChestDocument2 paginiImaging Studies of The ChestSteffi MurielÎncă nu există evaluări
- DRUGsssDocument2 paginiDRUGsssSteffi MurielÎncă nu există evaluări
- Ccu Patho AcsDocument2 paginiCcu Patho AcsSteffi MurielÎncă nu există evaluări
- NCPDocument3 paginiNCPSteffi MurielÎncă nu există evaluări
- Ccu Patho AcsDocument2 paginiCcu Patho AcsSteffi MurielÎncă nu există evaluări
- Case 21: A 32 Year Old Man in An Unresponsive State: Patient's Profile A Demographic DataDocument2 paginiCase 21: A 32 Year Old Man in An Unresponsive State: Patient's Profile A Demographic DataSteffi MurielÎncă nu există evaluări
- 3 NCP Ineffective Tissue PerfusionDocument2 pagini3 NCP Ineffective Tissue PerfusionSteffi MurielÎncă nu există evaluări
- Case 20-2016Document20 paginiCase 20-2016Steffi MurielÎncă nu există evaluări
- Drugs MOA I & Ci Se & Ar Nursing Considerations Generic: Indications:-CnsDocument7 paginiDrugs MOA I & Ci Se & Ar Nursing Considerations Generic: Indications:-CnsSteffi MurielÎncă nu există evaluări
- 20 NCP Impaired Skin IntegrityDocument4 pagini20 NCP Impaired Skin IntegritySteffi MurielÎncă nu există evaluări
- Referencess: Wenson Pajaron College Graduate - Accountancy Cebu, City 09331389968Document1 paginăReferencess: Wenson Pajaron College Graduate - Accountancy Cebu, City 09331389968Steffi MurielÎncă nu există evaluări
- End-Stage Renal Disease: Secondary To Hypertension NephrosclerosisDocument2 paginiEnd-Stage Renal Disease: Secondary To Hypertension NephrosclerosisSteffi MurielÎncă nu există evaluări
- Assessment Nursing Diagnosis Nursing InterventionDocument2 paginiAssessment Nursing Diagnosis Nursing InterventionSteffi MurielÎncă nu există evaluări
- A&E - Urinary / DM/ Toxicology-Mergencies Traumatized UtsDocument22 paginiA&E - Urinary / DM/ Toxicology-Mergencies Traumatized UtsSteffi MurielÎncă nu există evaluări
- Complications of IV TherapyDocument10 paginiComplications of IV TherapySteffi MurielÎncă nu există evaluări
- Patient's Profile A Demographic DataDocument2 paginiPatient's Profile A Demographic DataSteffi MurielÎncă nu există evaluări
- O o o O: Emergency Management Status AsthmaticusDocument8 paginiO o o O: Emergency Management Status AsthmaticusSteffi MurielÎncă nu există evaluări
- Objective 4 Graphs AgeDocument81 paginiObjective 4 Graphs AgeSteffi MurielÎncă nu există evaluări
- Decision Tree For Continuum of Care SchizoprheniaDocument1 paginăDecision Tree For Continuum of Care SchizoprheniaSteffi MurielÎncă nu există evaluări
- Objective 4 Graph Hours Working Per DayDocument9 paginiObjective 4 Graph Hours Working Per DaySteffi MurielÎncă nu există evaluări
- Objective 4 Graphs GenderDocument9 paginiObjective 4 Graphs GenderSteffi MurielÎncă nu există evaluări
- Objective 4 Graph AlcoholDocument9 paginiObjective 4 Graph AlcoholSteffi MurielÎncă nu există evaluări
- Drug Name Mechanism of Action Indication Side Effects GN: Dopamine BN: Classification: AdrenergicDocument14 paginiDrug Name Mechanism of Action Indication Side Effects GN: Dopamine BN: Classification: AdrenergicSteffi MurielÎncă nu există evaluări
- Objective 4 Graph EmploymentDocument9 paginiObjective 4 Graph EmploymentSteffi MurielÎncă nu există evaluări
- Objective 4 Graph EducationDocument9 paginiObjective 4 Graph EducationSteffi MurielÎncă nu există evaluări