Documente Academic
Documente Profesional
Documente Cultură
1752 1947 3 9288 PDF
Încărcat de
EndahD'LamdaTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
1752 1947 3 9288 PDF
Încărcat de
EndahD'LamdaDrepturi de autor:
Formate disponibile
Journal of Medical Case Reports
BioMed Central
Open Access
Case report
Laryngeal tuberculosis presenting as a supraglottic carcinoma: a
case report and review of the literature
Yvette E Smulders1, Bert-Jan De Bondt2, Martin Lacko1, Janice AL Hodge3 and
Kenneth W Kross*1
Address: 1Department of Otolaryngology/Head and Neck Surgery, Maastricht University Medical Centre, the Netherlands, 2Department of
Radiology, Isala Klinieken, Zwolle, the Netherlands and 3Department of Pathology, Maastricht University Medical Centre, the Netherlands
Email: Yvette E Smulders - Yvette.Smulders@gmail.com; Bert-Jan De Bondt - r.b.j.de.bondt@isala.nl; Martin Lacko - martin.lacko@mumc.nl;
Janice AL Hodge - Janice.hodge@mumc.nl; Kenneth W Kross* - kenneth.kross@mumc.nl
* Corresponding author
Published: 20 November 2009
Journal of Medical Case Reports 2009, 3:9288
doi:10.1186/1752-1947-3-9288
Received: 22 August 2008
Accepted: 20 November 2009
This article is available from: http://www.jmedicalcasereports.com/content/3/1/9288
2009 Smulders et al; licensee BioMed Central Ltd.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/2.0),
which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Introduction: Laryngeal tuberculosis used to be a common complication in advanced pulmonary
tuberculosis. However, it has become a rare occurrence in developed countries since the
introduction of antituberculous agents. Moreover, the pattern of the disease has changed over the
years. Nowadays, it more closely resembles a laryngeal carcinoma than any other laryngeal illness.
Case presentation: We describe the case of a 50-year-old Caucasian man who presented with
the clinical picture of laryngeal cancer, but which turned out to be tuberculosis. We illustrate the
difficulty of recognizing laryngeal tuberculosis both clinically and even with radiological examination.
Conclusion: Although laryngeal tuberculosis is uncommon, especially in developed countries, it
still occurs and should be considered as a differential diagnosis in any laryngeal disease, in particular
in the case of a laryngeal carcinoma.
Introduction
Tuberculosis (TB) was a highly prevalent disease in
humans for many decades until the early 1900s and is still
the main cause of death in some parts of the world. In
2007, approximately 13.7 million people contracted TB
and 1.8 million died as a result of the disease. A total of
68% of newly infected people were of Asian or African origin, whereas ethnic Europeans only made up 5% of global
TB cases [1].
After the introduction of antituberculous agents, preventive programs and better socioeconomic conditions, TB
incidence decreased dramatically up until the 1980s [1-4].
In subsequent years, however, the epidemic spread of
HIV, illicit drug use and the emergence of multi-drugresistant mycobacteria have resulted in a resurgence of TB.
In 1993, it became the leading cause of death from a single infectious agent. Increased numbers of migration and
travelling to and from less-developed countries also contributed to the worldwide spread of TB [3-7]. The incidence of TB continues to increase (122 per 100,000 in
1997 versus 142 per 100,000 in 2007), despite the fact
that it has stabilized or decreased in over 70% of countries. A minority of underdeveloped, mainly African,
countries has been the major contributor to the global
incidence growth [1]. The change in TB incidence over
time for underdeveloped, developing and developed
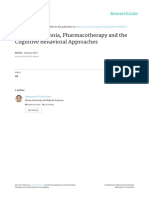
countries is shown in Figure 1.
Page 1 of 4
(page number not for citation purposes)
Journal of Medical Case Reports 2009, 3:9288
http://www.jmedicalcasereports.com/content/3/1/9288
Tuberculosis Incidence vs Human Development Index (HDI)
TB Incidence per 100
0,000 people
400
tions. The purpose of this case report and review of the literature is to raise awareness of this rare but prevailing
disease.
350
Case presentation
300
250
Hi h HDI
High
200
Medium HDI
Low HDI
150
Average
100
50
0
Figure
TB
ing
incidence
and underdeveloped
1
per 100,000countries
inhabitants
in the
for developed,
past decadedevelopTB incidence per 100,000 inhabitants for developed,
developing and underdeveloped countries in the past
decade. Based on the Human Development Index (HDI) and
tuberculosis (TB) incidence per country between 1997 and
2007 [1]. The graph summarizes data of 172 countries: 73
developed countries (HDI >0.8), 73 developing countries
(HDI 0.5-0.8) and 26 underdeveloped countries (HDI <0.5).
Laryngeal TB used to be a common complication of pulmonary TB. At the start of the 20th century it affected 2530% of all infected patients. Today, laryngeal TB occurs in
only 1% of cases [4,8-10]. The pattern and clinical symptoms of laryngeal TB have also changed. Currently, it has
many similarities to laryngeal carcinoma [4,5,7,11].
We present a case of laryngeal TB in a Caucasian man who
had characteristic symptoms of a supraglottic laryngeal
carcinoma without any clinical pulmonary manifesta-
A 50-year-old Caucasian man was referred to our
otolaryngology outpatient clinic with a two-month history of persistent dysphonia, dysphagia and odynophagia
with radiating pain to the right ear. In addition, he had
experienced recurrent aspiration of liquids and had lost 3
kg in weight. His prior medical history was unremarkable.
He had been a tobacco smoker for 40 years, but there was
no history of alcohol abuse. Laryngoscopy revealed an
ulcer on the right false vocal cord with an extension to the
epiglottis. Oedema and decreased mobility of the right
true vocal cord were observed as well as the diffused swelling of both arytenoids. There was no lymphadenopathy as
confirmed by an ultrasound sonography of the neck. The
initial anteroposterior chest X-ray, being part of the routine diagnostic work-up, showed miliary nodules that
were predominantly bilaterally distributed in the upper
parts of the lung parenchyma (Figure 2A). The axial contrast-enhanced computed tomography (CT) scan of the
neck demonstrated an enhanced mass in the right false
vocal cord with an obliteration of the paraglottic fat,
extending into the anterior commissure and cranially,
obliterating the right piriform sinus (Figure 2B). A full
blood count and electrolytes were within normal limits.
Direct laryngoscopy performed under general anaesthesia
revealed a tumour covering the entire right, false vocal
cord with an extension to the laryngeal side of the epiglottis without affecting the glottis. The tumour was clinically
staged as a T3N0 supraglottic laryngeal carcinoma.
Radiography
Figure
2
Radiography. (A) Initial antero-posterior chest X-ray. Miliary nodules predominantly bilaterally distributed in the upper parts
of the lung parenchyma. (B) Axial contrast-enhanced computed tomography image of the neck: enhanced mass (arrows) in the
false vocal cord which extends into the anterior commissure and obliteration of the paraglottic fat (arrowhead). (C) Axial high
resolution computed tomography image of the chest: diffusely distributed interstitial nodular alterations with formation of central cavities (arrows).
Page 2 of 4
(page number not for citation purposes)
Journal of Medical Case Reports 2009, 3:9288
Histopathological examination, however, revealed a necrotising granulomatous inflammation without signs of
malignancy (Figure 3A, C, D). Ziehl-Neelsen staining of
the tissue biopsies and sputum revealed acid-fast bacilli
(Figure 3B). Sputum culture turned out to be positive for
Mycobacterium tuberculosis. An additional axial high resolution CT scan of the chest demonstrated diffuse interstitial nodular alterations with the formation of central
cavities, indicative of pulmonary TB (Figure 2C).
Treatment commenced with isoniazid 300 mg/day,
rifampicin 600 mg/day, pyrizinamide 1500 mg/day and
ethambutol 1400 mg/day for a period of 2 months. Sputum cultures became negative after a 3-month follow up.
Because of cavity formations, as revealed by the chest CT,
treatment with isoniazid and rifampicin was prolonged
for another 3 months.
Because the patient was discharged from hospital a day
after a direct laryngoscopy, there was ample opportunity
for the patient to infect his healthcare providers. Contact
surveys revealed that the resident and nurse, who both
assisted in performing the laryngoscopy, two of the
patient's relatives and two of his friends all tested positive
in their purified protein derivative tests (PPD). They were
all preventively treated with tuberculostatics.
Discussion
Extra pulmonary TB in the head and neck region most frequently occurs in the cervical lymph nodes (>90%), fol-
Figurehistology
Biopsy
3
Biopsy histology. (A) Necrotising granulomatous inflammation: granuloma on the left and necrosis on the right side
of the image. (B) Red stained Mycobacterium tuberculosis in
Ziehl-Neelsen acid fast stain. (C) Granuloma with a multinucleated giant cell in the center (left side of image). (D) Overview of a necrotising granulomatous inflammation:
granulomas on the left side and necrosis on the right.
http://www.jmedicalcasereports.com/content/3/1/9288
lowed by the larynx (2% to 6%) [8,9]. Involvement of the
temporal bone, sinonasal cavity, eye, pharynx, thyroid
and skull base are even less frequently observed [4,8,9].
The characteristics of laryngeal TB have changed over the
years and it has become a challenge for otolaryngologists
to distinguish this disease from others. In the past, laryngeal TB typically affected young people in the second or
third decade of life with advanced pulmonary TB. Symptoms were cough, haemoptysis, fever, weight loss and
night sweats. An ulcerative, granulomatous lesion was
generally positioned on the posterior part of the larynx
due to accumulation of sputum in the arytenoid region in
bed-bound patients. Today, laryngeal TB mainly involves
people in their 50 s or 60 s presenting first and foremost
with hoarseness (80% to 100%). Other symptoms are
odynophagia (50% to 67%) and to a lesser extent, dysphagia, dyspnoea, stridor, cough and haemoptysis.
Systemic symptoms have become rare [2,4-7,9,11]. Laryngeal TB can involve all parts of the larynx and there is no
longer an unmistakable association with pulmonary TB.
The larynx becomes infected either by a direct spread from
the lungs, or by a haematogenous spread from sites other
than the lungs [5,11,12]. The former mechanism is most
common and probably relevant for the patient in our case.
In the case of a haematogenous spread, there is no evidence of pulmonary disease [3,7,9]. The distinction
between laryngeal TB and chronic laryngitis or laryngeal
carcinoma in particular has become difficult.
Odynophagia is described as an important discriminating
symptom, since it is considered rare in laryngeal cancer
[2,5-7,11]. Yet, from experience we know that painful dysphagia is a well-known symptom reported among
patients suffering from a supraglottic laryngeal carcinoma. In a physical examination, the true vocal cords are
most frequently affected by laryngeal TB, followed by the
epiglottis, false vocal cords and ventricles, arytenoids, posterior commissure and the subglottic area [4,7,12]. Laryngeal TB can manifest as oedema, hyperaemia or ulcerative
lesions, but can also present as a nodule, an exophytic
mass or obliteration of an anatomical structure [12]. Aside
from chronic laryngitis and laryngeal carcinoma, these
various presentations give rise to a comprehensive differential diagnosis including cat-scratch disease, syphilis,
sarcoidosis, Wegener's granulomatosis and fungal infections [8]. Since pathognomonic characteristics indicative
of laryngeal TB do not exist and the fact that it is an
uncommon disease in industrialised countries, the infection is easily mistaken for the more frequently occurring
laryngeal carcinoma [3,6,8]. Our patient had a longstanding history of heavy smoking, and had symptoms of
hoarseness and odynophagia. Laryngoscopy revealed an
oedematous tumour with decreased mobility of the vocal
cord. The clinical signs, supported by the findings on the
initial CT scan of the larynx, led us to the diagnosis of a
Page 3 of 4
(page number not for citation purposes)
Journal of Medical Case Reports 2009, 3:9288
laryngeal carcinoma. Laryngeal TB, however, can have the
exact same symptoms. In the majority of cases, there is an
association with pulmonary TB [2,4]. Therefore, an anomalous chest X-ray, if not compatible with pulmonary
metastasis, should alert the radiologist and otolaryngologist to the possibility of TB, especially when former chest
X-rays were normal.
http://www.jmedicalcasereports.com/content/3/1/9288
Consent
Written informed consent was obtained from the patient
for publication of this case report and any accompanying
images. A copy of the written consent is available for
review by the Editor-in-Chief of this journal.
References
1.
Laboratory techniques for detecting TB infections include
histopathological tissue examinations with Ziehl-Neelsen
histochemical staining for acid-fast bacilli and identification of M. tuberculosis by polymerase chain reaction or
bacterial culture. The latter method, although time-consuming, is considered the reference standard [13]. A CT of
the neck cannot definitively identify laryngeal TB since, as
in a chest X-ray, it can imitate many other diseases. Antituberculous agents are the primary treatment for laryngeal
TB. The improvement of dysphagia and resolving of cavernous lung lesions are expected to occur within several
weeks [6,12,14,15]. If not treated early, laryngeal TB can
result in (sub)glottic stenosis, muscular involvement and
vocal cord paralysis when the cricoarytenoid joint or
recurrent laryngeal nerve are invaded [5,12].
Conclusion
Laryngeal TB is uncommon, particularly in developed
countries, but it still occurs. There are no pathognomonic
features indicative of this disease and it can mimic many
others. If misdiagnosed, laryngeal TB can have severe consequences for the patient and anyone he comes into contact with. Therefore, it is important for otolaryngologists
to recognise the altered pattern of laryngeal TB and to be
familiar with its resemblance to malignancy. This is not
only in view of clinical symptoms, but also from a radiological point of view. Laryngeal TB should be considered
as a differential diagnosis in any laryngeal disease and in
particular in the case of a laryngeal carcinoma.
Abbreviations
CT: computed tomography; PPD: purified protein derivative tests; TB: tuberculosis.
2.
3.
4.
5.
6.
7.
8.
9.
10.
11.
12.
13.
14.
15.
World Health Organization (WHO): Global Tuberculosis
Database
2009
[http://www.who.int/tb/country/
global_tb_database/en/index.html]
Harney M, Hone S, Timon C, Donnelly M: Laryngeal tuberculosis:
an important diagnosis. J Laryngol Otol 2000, 114:878-880.
Rizzo PB, Da Mosto MC, Clari M, Scotton PG, Vaglia A, Marchiori C:
Laryngeal tuberculosis: an often forgotten diagnosis. Int J
Infect Dis 2003, 7:129-131.
Williams RG, Douglas-Jones T: Mycobacterium marches back. J
Laryngol Otol 1995, 109:5-13.
Lim JY, Kim KM, Choi EC, Kim YH, Kim HS, Choi HS: Current clinical propensity of laryngeal tuberculosis: review of 60 cases.
Eur Arch Otorhinolaryngol 2006, 263:838-842.
Lin CJ, Kang BH, Wang HW: Laryngeal tuberculosis masquerading as carcinoma. Eur Arch Otorhinolaryngol 2002, 259:521-523.
Shin JE, Nam SY, Yoo SJ, Kim SY: Changing trends in clinical manifestations of laryngeal tuberculosis.
Laryngoscope 2000,
110:1950-1953.
Moon WK, Han MH, Chang KH, Im JG, Kim HJ, Sung KJ, Lee HK: CT
and MR imaging of head and neck tuberculosis. Radiographics
1997, 17:391-402.
Nalini B, Vinayak S: Tuberculosis in ear, nose, and throat practice: its presentation and diagnosis. Am J Otolaryngol 2006,
27:39-45.
Topak M, Oysu C, Yelken K, Sahin-Yilmaz A, Kulekci M: Laryngeal
involvement in patients with active pulmonary tuberculosis.
Eur Arch Otorhinolaryngol 2008, 265:327-330.
Hunter AM, Millar JW, Wightman AJ, Horne NW: The changing
pattern of laryngeal tuberculosis.
J Laryngol Otol 1981,
95:393-398.
Yencha MW, Linfesty R, Blackmon A: Laryngeal tuberculosis. Am
J Otolaryngol 2000, 21:122-126.
Al Serhani AM: Mycobacterial infection of the head and neck:
presentation and diagnosis. Laryngoscope 2001, 111:2012-2016.
Nederlandse Vereniging van Artsen voor Longziekten en Tuberculose
(NVALT): Richtlijn Medicamenteuze behandeling van tuberculose 2005.
2005 [http://www.nvalt.nl/uploads/48/2917/
4933_nvalt-richtlijntuberculosebinnenwerkdef_pp_10.pdf]. Alphen
aan den Rijn: Van Zuiden Communications B.V
Blumberg HM, Burman WJ, Chaisson RE, Daley CL, Etkind SC, Friedman LN, Fujiwara P, Grzemska M, Hopewell PC, Iseman MD, Jasmer
RM, Koppaka V, Menzies RI, O'Brien RJ, Reves RR, Reichman LB,
Simone PM, Starke JR, Vernon AA: American Thoracic Society/
Centers for Disease Control and Prevention/Infectious Diseases Society of America: Treatment of Tuberculosis. Am J
Respir Crit Care Med 2003, 167:603-662.
Competing interests
The authors declare that they have no competing interests.
Authors' contributions
KK, YS and ML were in charge of the medical care of the
patient. RB was responsible for the interpretation of the
radiological findings and JH for the interpretation of the
histopathological findings. They cooperated with each
other to find the correct diagnosis and treatment. YS wrote
the manuscript and studied the literature. KK, JH and RB
reviewed the draft critically and provided helpful comments. All authors read and approved the final manuscript.
Publish with Bio Med Central and every
scientist can read your work free of charge
"BioMed Central will be the most significant development for
disseminating the results of biomedical researc h in our lifetime."
Sir Paul Nurse, Cancer Research UK
Your research papers will be:
available free of charge to the entire biomedical community
peer reviewed and published immediately upon acceptance
cited in PubMed and archived on PubMed Central
yours you keep the copyright
BioMedcentral
Submit your manuscript here:
http://www.biomedcentral.com/info/publishing_adv.asp
Page 4 of 4
(page number not for citation purposes)
S-ar putea să vă placă și
- Estimating The Time After Death On The Basis of Corneal Opacity 2157 7145.1000269Document5 paginiEstimating The Time After Death On The Basis of Corneal Opacity 2157 7145.1000269Herik Okta JonandaÎncă nu există evaluări
- Thali - Virtopsy, A New Imaging Horizon in Forensic Pathology, Virtual Autopsy by Postmortem MSCT and MRI, A Feasibility Study - 2003 - J Forensic Sci PDFDocument18 paginiThali - Virtopsy, A New Imaging Horizon in Forensic Pathology, Virtual Autopsy by Postmortem MSCT and MRI, A Feasibility Study - 2003 - J Forensic Sci PDFChristianWicaksonoÎncă nu există evaluări
- GINA Pocket 2015Document32 paginiGINA Pocket 2015Ramzi AkramÎncă nu există evaluări
- 5469e9760cf2f5eb1806310d PDFDocument9 pagini5469e9760cf2f5eb1806310d PDFEndahD'LamdaÎncă nu există evaluări
- 2016 Article 253Document9 pagini2016 Article 253EndahD'LamdaÎncă nu există evaluări
- Diretrizes Européias para DislipidemiaDocument50 paginiDiretrizes Européias para DislipidemiaEno FilhoÎncă nu există evaluări
- Common Genetic Disease Related Hormonal and Metabolism: DR Erna Mirani, M.Si - MedDocument63 paginiCommon Genetic Disease Related Hormonal and Metabolism: DR Erna Mirani, M.Si - MedFahmi Nur ZamanÎncă nu există evaluări
- Researcharticle Open AccessDocument7 paginiResearcharticle Open Accesswicak_spÎncă nu există evaluări
- 5469e9760cf2f5eb1806310d PDFDocument9 pagini5469e9760cf2f5eb1806310d PDFEndahD'LamdaÎncă nu există evaluări
- Insomnia PDFDocument5 paginiInsomnia PDFEndahD'LamdaÎncă nu există evaluări
- Piis1040842816300257 PDFDocument11 paginiPiis1040842816300257 PDFEndahD'LamdaÎncă nu există evaluări
- 2016 Article 291 PDFDocument9 pagini2016 Article 291 PDFEndahD'LamdaÎncă nu există evaluări
- Acne Vulgaris Treatment and Causes ExplainedDocument13 paginiAcne Vulgaris Treatment and Causes ExplainedRachmansyah RizalÎncă nu există evaluări
- POLIOMYELITISDocument15 paginiPOLIOMYELITISEndahD'LamdaÎncă nu există evaluări
- Guillain Barre SyndromeDocument22 paginiGuillain Barre SyndromeEndahD'LamdaÎncă nu există evaluări
- Essential Neurology 4Th Ed PDFDocument290 paginiEssential Neurology 4Th Ed PDFPutu 'yayuk' Widyani WiradiraniÎncă nu există evaluări
- Paratiroid (PTH)Document29 paginiParatiroid (PTH)EndahD'LamdaÎncă nu există evaluări
- Guillain-Barré SyndromeDocument21 paginiGuillain-Barré SyndromeReza AkbarÎncă nu există evaluări
- Neurologic Clinics Pediatric Neurology Part IDocument296 paginiNeurologic Clinics Pediatric Neurology Part IPirokunÎncă nu există evaluări
- Post Herpetic Neuralgia andDocument63 paginiPost Herpetic Neuralgia andEndahD'LamdaÎncă nu există evaluări
- Jonathan Edlow, Magdy Selim Neurology Emergencies 2010Document251 paginiJonathan Edlow, Magdy Selim Neurology Emergencies 2010Alina AndreiÎncă nu există evaluări
- Faktor Resiko Stroke Post HerpesDocument7 paginiFaktor Resiko Stroke Post HerpesEndahD'LamdaÎncă nu există evaluări
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5783)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (890)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (399)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (72)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (119)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- PERSONAL PROFILE: Gender: Marital Status Date ofDocument3 paginiPERSONAL PROFILE: Gender: Marital Status Date ofetienoetokÎncă nu există evaluări
- 245 Q4 AR Extra PracticeDocument9 pagini245 Q4 AR Extra PracticeKausarAtiqueÎncă nu există evaluări
- Bài Tập Ngữ Pháp Lý Thuyết (Tiếng Anh) Có Đáp ÁnDocument28 paginiBài Tập Ngữ Pháp Lý Thuyết (Tiếng Anh) Có Đáp ÁnMan EbookÎncă nu există evaluări
- Black Asclepius, White ImhotepDocument7 paginiBlack Asclepius, White Imhoteptahuti696Încă nu există evaluări
- Timken Ball Bearings CatalogDocument126 paginiTimken Ball Bearings Catalogmohananc67Încă nu există evaluări
- RPH Module 3Document37 paginiRPH Module 3Ninia Crishelle A. ManzanoÎncă nu există evaluări
- Pressure Loss Experiment Gunt Hamburg HM 150.29Document2 paginiPressure Loss Experiment Gunt Hamburg HM 150.29eldwin_dj7216Încă nu există evaluări
- Cambridge Primary ProgressionTests - Past Papers PDFDocument3 paginiCambridge Primary ProgressionTests - Past Papers PDFPinky Dey8% (13)
- OPERA Credit Card Encryption Key Utility 50Document18 paginiOPERA Credit Card Encryption Key Utility 50eltoroÎncă nu există evaluări
- BgpmsDocument16 paginiBgpmsKrystal Mae Quibol-PaciosÎncă nu există evaluări
- Project Grant Chart Al AmalDocument3 paginiProject Grant Chart Al AmalBalaji SelvarajÎncă nu există evaluări
- Chapter 18 Theoretical Bases For Promoting Family HealthDocument43 paginiChapter 18 Theoretical Bases For Promoting Family Healthbaashe100% (2)
- Analisis Tingkat Keterampilan Berpikir Kritis Siswa SMA: Jurnal Pendidikan Fisika Dan Teknologi February 2020Document7 paginiAnalisis Tingkat Keterampilan Berpikir Kritis Siswa SMA: Jurnal Pendidikan Fisika Dan Teknologi February 2020Nurkholifatul MaulaÎncă nu există evaluări
- HR307 - Configuration of HR System Controls PDFDocument227 paginiHR307 - Configuration of HR System Controls PDFRajesh Reghu Nadh NadhÎncă nu există evaluări
- Corps 2e - Apv2701 Corps Rules ExpansionDocument226 paginiCorps 2e - Apv2701 Corps Rules ExpansionAnonymous Bi6HNNhFÎncă nu există evaluări
- Complete CV (CCIU)Document8 paginiComplete CV (CCIU)Yinda Godwin SendzeÎncă nu există evaluări
- Mathematics 8 - Module 1Document4 paginiMathematics 8 - Module 1Robert ClavoÎncă nu există evaluări
- PT - Mathematics 4 - Q2Document6 paginiPT - Mathematics 4 - Q2MAY ANNE SITJARÎncă nu există evaluări
- Reactive Distillation For Producing N-Butyl Acetate: Experiment and SimulationDocument8 paginiReactive Distillation For Producing N-Butyl Acetate: Experiment and SimulationHemant RathvaÎncă nu există evaluări
- PANASONIC MD2 and E3D Chassis Technical GuideDocument108 paginiPANASONIC MD2 and E3D Chassis Technical GuideavrelecÎncă nu există evaluări
- Primer - UP Open UniversityDocument14 paginiPrimer - UP Open UniversityLin Coloma Viernes WagayenÎncă nu există evaluări
- Vonnegut Images and RepresentationsDocument211 paginiVonnegut Images and RepresentationsAnonymous XTXCntXXH100% (1)
- Achieving Personal and Professional Excellence Through Goal SettingDocument4 paginiAchieving Personal and Professional Excellence Through Goal SettingRidhima LuthraÎncă nu există evaluări
- U-Type CrossarmDocument9 paginiU-Type CrossarmMosa Elnaid ElnaidÎncă nu există evaluări
- Propositional LogicDocument26 paginiPropositional LogicSeham123123Încă nu există evaluări
- Missing The Point(s) : The Declining Fortunes of Canada's Economic Immigration ProgramDocument26 paginiMissing The Point(s) : The Declining Fortunes of Canada's Economic Immigration ProgramGerman Marshall Fund of the United StatesÎncă nu există evaluări
- Meth Confronting The ProblemDocument1 paginăMeth Confronting The ProblemamychowÎncă nu există evaluări
- Vocabulary - Active and Passive Vocabulary - Various Techniques of Teaching Vocabulary - The Criterion - An International Journal in English PDFDocument4 paginiVocabulary - Active and Passive Vocabulary - Various Techniques of Teaching Vocabulary - The Criterion - An International Journal in English PDFaknithyanathan100% (1)
- Como Criar Micromarcas PDFDocument28 paginiComo Criar Micromarcas PDFJoséÎncă nu există evaluări
- A Credit Risk Model For AlbaniaDocument37 paginiA Credit Risk Model For AlbaniarunawayyyÎncă nu există evaluări