Documente Academic
Documente Profesional
Documente Cultură
17-1 Tung
Încărcat de
Pierre A. Rodulfo0 evaluări0% au considerat acest document util (0 voturi)
51 vizualizări6 pagini17-1 Tung
Drepturi de autor
© © All Rights Reserved
Formate disponibile
PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest document17-1 Tung
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
51 vizualizări6 pagini17-1 Tung
Încărcat de
Pierre A. Rodulfo17-1 Tung
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 6
ORTHOKERATOLOGY
and
VISION THERAPY
to
MANAGE ACCOMMODATIVE ESOTROPIA
A Case Study
E
n Tung Hsiao-Ching, M.D. INTRODUCTION
sotropia (ET) is the most thereby decreasing the associated conver-
common type of strabismus, gence and the eyes tend to straighten so
Abstract occurring in approximately that less esophoria or esotropia results.4-7
This case describes a six-year-old girl with 1-2% of the population. It can be further The effect of correcting the hyperopia
a comitant, constant, alternating, accom- divided into various groups, e.g., infantile, and the binocular imbalance may have
modative esotropia with hyperopia. The refractive, and accommodative, requiring further benefits to the child. There is evi-
esotropia was intermittent and evident different prognoses and approaches to dence that there is relationship between
since infancy and became increasingly con- treatment. One of these groups, accom- hyperopia and reading.8,9 These findings
stant with age. Management of accommo- modative ET, develops between the ages also suggest a relationship between hyper-
dative esotropia involves the application of of six months and seven years, most often opia and reading-disabled students.10-15
plus to reduce accommodative effort. While in two- to three-year-olds, and is related to
TREATMENTS
other options had been tried or considered, an abnormal accommodation-conver-
Spectacle Correction
I used orthokeratology to correct the hy- gence relationship.1
The conventional approach to man-
peropia and vision therapy to manage the Accommodative ET occurring in
agement of accommodative ET is to pro-
binocular function and sensory anomalies young children is an excellent illustration
vide the patient with single vision plus
associated with the esotropia. of abnormal binocular visual function
(convex) lenses and/or bifocal specta-
caused by an uncorrected or undercor-
cles.3,4 However, compliance with wear-
rected refractive condition. While accom-
ing the spectacle lenses, often in a bifocal
Key Words modative ET is usually associated with
or progressive lens design, can lead to
accommodative esotropia, contact lenses, moderate hyperopia, it also may occur in
non-compliance with children for reasons
orthokeratology, hyperopia, vision therapy. lower amounts of hyperopia, emmetropia
that include: appearance (cosmesis), so-
AC/A ratio, spectacle plus lenses or even myopia due to unusually high
cial and peer pressure effects, and simply
AC/A ratios.2,3
not understanding the need to wear the
Accommodative ET arises because of
lenses.
an abnormal relationship between accom-
modation and convergence. Normally Contact Lenses
there is a linear relationship between the These devices have the property of re-
two, but in accommodative ET this rela- ducing prismatic effect during near work,
tionship is higher than normal, resulting in and they do not produce spectacle magni-
an over convergence response to accom- fication. Further there is no cosmesis com-
modation.3 ponent as with spectacles. In this regard
The primary treatment for accommo- they can provide a viable option to treat
dative ET typically involves full-time accommodative ET. However, in young
wearing of ophthalmic lenses or contact children, insertion, removal, and daily
lenses to correct the refractive condition, care can be a significant obstacle to com-
which is most usually hyperopia. The pliance.
lenses reduce the accommodative effort
Journal of Behavioral Optometry Volume 17/2006/Number 1/Page 3
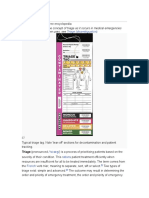
Refractive Surgery An ortho-K contact lens comprising:
Another option for treatment of ac-
A. An optical zone (1) having a curvature
commodative ET is hyperopic laser in 2 defined by a base curve (2), the base curve
situ keratomileusis (LASIK). Several 5 being steeper than a measured curvature (3)
studies have shown the efficacy of this 7
of a central portion of said cornea;
procedure in adults.16-18 Though there 9 B. A plateau zone (4) coupled to the optical
11
was some success in adults, there is zone and extending radially there from the
still no evidence of the use of LASIK in plateau zone having a curvature defined by
children for hyperopia and esotropia. 3 a plateau curve (5), the plateau curve being
flatter than the base curve (2).
Orthokeratology
I propose that a fourth option is the C. A fitting zone (6) coupled to the plateau
zone and extending radially there from, the
use of orthokeratology (Ortho-K) to fitting zone having a curvature defined by a
correct the hyperopia. Just as providing fitting curve (7), the fitting curve being
an appropriate lens correction, steeper that the plateau curve.
Ortho-K may be effective in managing 10
D. A alignment zone (8) coupled to the
horizontal vergence problems e.g., ac- fitting zone and extending radially there
8
commodative esophoria or ET. from the alignment zone having a curvature
Ortho-K is a clinical contact lens tech- defined by an alignment curve (9), the
4 1 alignment curve being flatter than the
nique that can be defined as the reduc- fitting curve.
tion, modification, or elimination of
refractive error by the application of E. A peripheral zone (10) coupled to the
contact lenses.19 It had lost favor in alignment zone and extending radially
6
there from the peripheral zone having a
the late 1970s and early 1980s, due to curvature defined by a peripheral curve
the unpredictability reported in several (11), the peripheral zone forming an edge
controlled studies.20,21 However, the lift to act as tear reservoir.
use of Ortho-K for myopia and astig-
matism reduction has more recently Figure 1. Dual geometric lens for hyperopic presbyopia or multi-focal ortho-K. There are one or more optical
zones used to redistribute corneal tissue to cause the cornea to have a steepened central portion surrounded by
been shown to be effective.22-25 In view a flat mid-peripheral ring.31
of the high incidence of myopia in Chi-
nese children, overnight Ortho-K has
verse design to the traditional Ortho-K the BOZR is the plateau zone which is ap-
become a popular treatment for myopia
26,27 lens for myopia. (Figure1) proximately 5 to 20 diopters flatter than
control in Hong Kong.
The contact lens has a plurality of the central BOZR and blends into the fit-
LENS DESIGN FOR HYPEROPIC zones that includes one or two optical ting zone. The fitting zone is 10 to 30 di-
ORTHO-K zones, a plateau zone, a fitting zone, an opters steeper than the plateau zone and
The use of Ortho-K for hyperopia re- alignment zone and a peripheral zone. The brings the lens back into alignment with
duction has not been generally investi- one or more optical zones are utilized to the peripheral cornea. The balance of the
gated clinically or, if so, it is only on a redistribute corneal tissue to cause the lens is the alignment curve, which is
minimal and subjective basis. Contact cornea to have a steepened central portion aspheric and provides centration and ap-
lens designs for the correction of hyper- surrounded by a flat mid-peripheral ring proximately 100 of edge lift to facilitate
opia through Ortho-K are being devel- The plateau zone helps steepen the central tear circulation and prevent lens binding.
oped in Australia and in the USA. In cornea in two ways: a positive molding ef- The anterior surface of the lens consists of
principle, these lenses aim to gently fect of pushing the cornea tissue inward to a central power curve to correct the dis-
steepen the cornea, increase corneal opti- pile up, and a negative molding effect to tance vision. Generally speaking, the lens
cal power, and thus correct the hyperopia. enhance flattening of the mid-peripheral has a central optical zone steeper than the
The traditional method of managing cornea. central cornea. This is followed by a flat
hyperopia by Ortho-K is to apply a series The optical zone of the lens is de- plateau zone to prevent tissue pile up at the
of progressively steeper GP (oxygen per- signed steeper than the measured curva- mid peripheral area when trying to push
meable) contact lenses in order to move ture of a central portion of the cornea. This the tissue all the way into the central por-
the corneal tissue toward its central por- is intended to provide a steep central space tion of the cornea.
tion.28-30 However, anecdotal reports have for cornea tissue to pile up during vision The dual geometric designs may also
found that often the tissue piles up at the correction. This is accomplished by using be used for correcting hyperopic presby-
mid-peripheral portion instead of at the the mean keratometry measurements in opia (HP lens). This lens provides a steep
central portion of the cornea; this can flat- diopters and the spherical equivalent of central button for reading and a sloping
ten the central cornea curvature and in- the refractive condition to determine the pericentral zone for correcting hyperopia.
crease the hyperopia. Base Curve or Back Optic Zone Radius The BOZR of a HP lens is determined in a
To address this, I designed the dual (BOZR). The BOZR targets the total cor- similar way to target hyperopia plus the
geometric lens,31 intended for the reduc- rection plus an additional +0.75 diopters add required for correction. This
tion of hyperopia by Ortho-K. It is a re- to ensure a full reduction. In concert with multi-focal ortho-K design can also be
Volume 17/2006/Number 1/Page 4 Journal of Behavioral Optometry
used to eliminate or to relieve the exces- for all eye structures including: cornea, fitting rationale was to overcorrect the
sive convergence, triggered by near-work crystalline lens and retina. manifest hyperopia by +0.75D; conse-
accommodation in cases with high AC/A quently, I used the base curve of 6.94mm
Initial Diagnosis and Management
ratios. radius for the OD, 6.87 mm for the OS. I
The diagnosis was comitant, constant,
The dual geometric lens is matched to instructed the patients mother in lens in-
alternating basic accommodative ET with
the individual cornea by the same princi- sertion and removal and that the devices
a preference for the right eye for fixation,
ple of sagittal depth calculation in myopia were to be worn overnight. I further in-
without amblyopia. A new prescription of
Ortho-K correction.32 structed that the spectacle lenses were to
OD: +2.75, OS: +3.00 was issued with in-
be worn during all other hours until MB
CASE REPORT structions for constant wear.
experienced blurred vision with them; at
This case report describes the use of a
Follow Up Visit this time, the glasses should not be worn.
unique contact lens design that provides
We scheduled another visit to evaluate My examination on the first morning
Ortho-K treatment of hyperopia and vi-
her binocular vision status one month showed a mild cornea superficial punctate
sion therapy (VT) for a six-year old fe-
later. MBs mother reported poor compli- keratitis (SPK) at the nasal lower portion
male patient with accommodative ET.
ance with the spectacle wearing instruc- of the left eye. This did not occur on subse-
History tions. The Keystone Vision Testera and quent nights and the initial SPK was likely
Acolleague referred a six-year-old girl Random Dot Stereogram in the Vision due to her mother not being adept with the
(MB) to me requesting an evaluation of an Therapy Assessment (VTA)b were used. insertion and removal of the lenses. The
ET. She appeared shy but cooperative. With the new prescription MB demon- central portion of the cornea gradually
The ET was apparently evident even with strated only simultaneous perception, and steepened following two weeks of night
her spectacles. Her parents reported they the binocular alignment test indicated eso wear and her manifest refraction became
noted MB to have intermittent ET, more in posture (uncrossed diplopia). The useable OD: plano and OS: +0.50
her left eye during infancy. The intermit- vision, Random Dot Stereogram and After two weeks on this protocol, her
tent ET became constant gradually with Worth 4-Dot Tests established that there eyes appeared better aligned, but MB was
age. After visiting a pediatric ophthalmol- was a constant suppression of the left eye. still intermittently esotropic at near. Bin-
ogist, she was confirmed to have moderate Based on her history and early onset of the ocular sensory testing still showed un-
hyperopia and accommodative ET at ET, the lack of stereopsis and suppression crossed diplopia without stereopsis. An
about two years of age. Plus lens and par- in the left eye may be associated with a addition of +2.00 D. OU changed the re-
tial time right eye occlusion were initiated monofixational esophoria-tropia.33,34 sidual ET at 40cm to slight esophoria. We
as treatment. She was willing to wear the Considering her age, personality, and continued to monitor her refractive status
glasses only for close work because of the poor compliance with the lenses as well as and binocular status. After approximately
heaviness and unpleasant appearance of good vision with each eye, I considered al- four weeks of wearing these lenses, I insti-
her glasses. ternative treatments. Contact lenses were tuted a program of vision VT. The imme-
There was no reported family history a possibility, but I decided to offer my new diate goal was to eliminate the residual
of strabismus. The birth history was also hyperopic Ortho-K protocol. My goals ET. See the discussion of VT below.
uneventful and normal. There was no re- were to reduce the hyperopia and conse-
Step 2: Multifocal Ortho-K Contact
ported febrile events, trauma or acquired quently reduce the esotropia with the pos-
Lenses
head injury during her infancy. She was in sibility of enhancing her overall binocular
I now proceeded to the next step of
good health and was not taking any medi- status. The girl and her mother were
multifocal molding. I designed these
cations. pleased to have an alternative to the
lenses so that the base curves were much
glasses.
Diagnostic Data steeper than the central portion of the cor-
Her entering prescription was: OD: Treatment Rationale nea and overcorrected her hyperopia by
+1.75 DS, OS: +2.00 DS. Her corrected Step 1: Fitting TRIAL hyperopia 2.00 diopters. The base curves of the con-
visual acuities were: OD: 20/25 and OS: Ortho-K contact lenses tact lenses now became OD: 6.67 mm and
20/25. Without correction the ET was I fit all Ortho-K patients, including OS: 6.60 mm. The aspheric base curves
comitant, and cover testing revealed 35 those with myopia, with my standardized were carefully calculated to ensure shap-
prism diopters of constant alternating ET. trial fitting system.c The system utilizes ing a new corneal curvature that provided
With correction, the strabismic angle subjective spherical equivalent and mean good far visual acuity, while relieving the
decreased to approximately 8-10 prism di- corneal curvature measurements for lens near stress of accommodation after mold-
opters of constant alternating ET at far and selection, which then are verified by ing.
near. Dry and wet (2% cyclopentolate and fluorescein stain before ordering lenses The Ortho-K lenses were manufac-
1% tropicamide) retinoscopies and sub- from specific contact lens laboratories in tured using Boston XO lens material
jective refractions indicated: OD: +2.75 the United States. In this case I ordered (Bausch and Lomb, Rochester, New
DS, OS: +3.00 DS. The best correctable from E &E Optics.d The original corneal York). This is a tough, stable, high Dk ma-
visual acuity was 20/20 in each eye. curvatures were: 44.50/ 44.75 @90 with a terial that can be made into a wide variety
Pupillary responses were present with mean K of 44.62 D, in each eye. The mani- of special designs for special visual re-
no afferent defect. External and internal fest refraction, as aforementioned, was, quirements. This material has an ISO/Fatt
ocular examinations were unremarkable OD: +2.75D and OS: +3.00D. My initial Dk of 100 with a established record as a
Journal of Behavioral Optometry Volume 17/2006/Number 1/Page 5
tially less spherical aberration. At this
writing, MB has worn the second pair,
nearly everyday, for 18 months. There
have been no corneal problems, her hyper-
opia has been fully corrected and there is
no evidence of strabismus or significant
phoria at distance and near.
Step 3: Vision Therapy
My overall strategy was to reduce the
ET primarily with application of plus lens
power through Ortho-K and VT, and then
to continue VT to ameliorate any residual
binocular vision dysfunctions. Even
though there was orthophoria after the fi-
nal Ortho-K treatment and MB now at-
tained second degree fusion, she still
could not appreciate clinical stereopis. I
considered this absence was possibly re-
lated to the early onset of her ET that re-
Figure 2. Corneal Topography illustrates the central corneal steepening sulted in a microesotropia with mono-
fixation. If the eyes are straightened be-
fore or shortly after the esodeviation be-
comes constant, then there is a much
better chance of bifixation and binoculari-
ty.34
VT for esophoria/ET is thought more
difficult than that of exotropia/exophoria
especially if no fusion or stereopsis is de-
tectable.25-29 Although we were unsuc-
cessful in obtaining third degree fusion
and stereopsis after corneal molding, she
did show flat fusion. We scheduled her for
Figure 3. This illustrates the fluorescent stain oculomotor, anti-suppression, and
pattern with central pooling and Bulls eye pattern. vergence therapy. Techniques such as a
swinging ball and computerized saccadic,
pursuit, anti suppression, and vergence
premium extra oxygen exceptional stabil- eye) as before at distance and near. Her training were applied. In addition, we uti-
ity GP material for overnight wear. In this eyes appeared aligned and were cosmetic- lized the Red-Green anaglyphic fusion
case, I recommended a wearing schedule ally straighter at both far and near though targetsd and the computerized HTS pro-
of 8-10 hours per night for the initial pe- there were variable and small amounts of gram.b Office based VT was conducted
riod of several days until the cornea dem- an eso deviation at distance. She devel- twice a week with home therapy at least
onstrated a steepened central button. This oped a mild post-fitting problem, not due three times per week.
then could be reduced to a maintenance to the molding or lens, but rather to an al- At the cessation of 20 VT office ses-
wear of 6-8 hours per night. The pair of lergic reaction. The ocular condition re- sions, MB was still orthophoric at distance
multifocal Ortho-K lenses effectively turned to normal after replacing the and near, and demonstrated stable second
straightened her eyes to ortho at near and soaking solution. I propose that the resid- degree fusion. This is consistent with
far without glasses. The corneal topogra- ual soaking solution may have affected other reports in the literature that a good
phy showed much steeper central buttons the eyes more during overnight wear. Her number of the patients with accommoda-
as evidence of the additional plus lens ef- hyperopia reduced to nearly plano within tive ET developed good fusion but poor
fect for relieving her accommodation and two weeks. With Ortho-K, there is a po- stereopsis at the end of treatment. 35 The
excessive convergence during near-work. tential for residual glare or similar distur- last evaluation indicated that MBs ocular
(Figures 2 and 3) bances. In her case, there were no such health status was unremarkable, notably
The second pair of lenses were dis- complaints of glare for several possible that there were no corneal problems. The
pensed five weeks after the initiation of reasons. First, she was virtually never sub- Ortho-K findings and the patients binoc-
VT. The distance refractive status became jected to bright night lights. Further, a hy- ular status were now stable for about 15
slightly myopic ( 0.50 D OU ) without peropia molding is prolate in shape, i.e., months. As she grows older and matures,
much interference to her daily life. Her vi- watermelon shaped (central steepest and continual monitoring of the binocular sta-
sual acuity remained stable (20/20 in each flattens to the periphery) creating poten- tus will be maintained as well as consider-
Volume 17/2006/Number 1/Page 6 Journal of Behavioral Optometry
ation of incorporating contact lenses and ible and that reversibility has been demon- 12. Sherman A. Relating vision disorders to learn-
ing disability. J Am Optom Assoc
spectacle lenses as an alternative treat- strated after short to medium term 1973;44:140-1.
ment. lens-wearing periods,41 although no data 13. Eames TH. A comparison of the ocular charac-
are currently available with regard to teristics of unselected and reading disability
DISCUSSION groups. J Ed Res 1932; 25:211.
hyperopic Ortho-K.
Modern Ortho-K has been shown to be 14. Eames TH: Comparison of eye conditions
an effective procedure for the reduction of among 1,000 reading failures, 500 ophthalmic
Dr. Tung holds the US patents for, and
certain myopias and astigmatism.36-38 patients and 150 unselected children. Am J
is the owner of the System and Method for Ophthalmo 1948; 31:713.
Because of reports of corneal infections 15. Scheiman M M. Treatment of visual efficiency
Orthokeratology and the Dual Geometric
with the overnight component of Ortho-K, problems. In: Optometric management of
Contact Lenses for Hyperopia and Pres-
the safety of the procedure is under active learning-related vision problems. St. Louis:
byopia Orthokeratology. He has no finan- Mosby-year book, 1994: 406-11.
investigation. It is clear that minimal clini-
cial interest in the other products 16. Hoyos JE, Cigales M, Hoyos-Chacon J, Ferrer
cal standards must be promulgated inter- J, Maldonado-Bas A. Hyperopic laser in situ
discussed in the article.
nationally to ensure a future for this keratomileusis for refractive accommodative
approach to refractive correction.39-40 The Sources esotropia.J Cataract Refract Surg
use of an overnight lens-wearing protocol a. Keystone Vision Tester; Keystone View Co 2002;28:1522-9.
Div Mast/Keystone Inc 17. Stidham DB, Borissova O, Borissov V, Prager
provides an alternative to refractive sur- 340 Western Rd Suite 1, Reno, NV 89506 TC. Effect of hyperopic laser in situ
gery for many patients. My experience is (702) 827-8110) keratomileusis on ocular alignment and
that the onset of the refractive effect is rel- b. Vision Therapy Assessment (VTA ) available stereopsis in patients with accommodative
atively quick, with observable changes from HTS Inc. 5301 S. Superstition Mtn. Dr., esotropia. Ophthalmol 2002;109:1148-53.
PMB 483 Suite 104, Gold Canyon, AZ 85216, 18. Bilgihan K, Akata F, Or M, Hasanreisoglu B.
within days, and the procedure appears to c. System and Method for Orthokeratology. US Photorefractive keratectomy in refractive ac-
be fully reversible on cessation of lens patent # 6;361,169 granted March, 2002. Tung commodative esotropia (Pt 3). Eye
wear. Hsiao-Ching, 2F, 164 Lin-Jiang St., Taipei 1997;11:409-10.
106, Taiwan. 19. Mountford, J. Orthokeratology. In: Phillips,
CONCLUSION d. E &E Optics, 14640 Victory Blvd Van Nuys, AJ Speedwell, L eds. Contact Lenses 4th ed.
This case of a six-year old girl with ac- CA 91411, Distributor: VIPOK Inc.:1234 S. Oxford: Butterworth-Heinemann
commodative ET is an example of the Garfield Ave.,#105 Alhambra, CA 91801. 1997:653-692.
e. Bernell VTP Corp ; 4016 N Home St. 20. Kerns RL. Research in orthokeratology. Part
benefit and potential use of applying this Mishawaka, IN 46545 VIII: results, conclusions and discussion of
innovative method of multifocal Ortho-K techniques. J Am Optom
to young children. Since there was poor References Assoc1978;49:308-14.
1. Donnelly UM, Stewart NM, Hollinger M. 21. Polse KA,Brand RJ,Schwable JS, Vastine
compliance with the traditional method of Prevalence and outcomes of childhood visual DW,Keeler RJ. The Berkeley Orthokeratology
spectacles, this alternative method was disorders. Ophthalmol Epidemiol study, Part II: efficacy and duration. Am J
applied. She was shy and self demeaned 2005;12:243-50. Optom Physiol Opt 1983;60:187-98.
with the heavy glasses and the clearly visi- 2. Rouse MW: Optometric assessment of visual 22. Coon LJ. Orthokeratology. Part II: evaluating
efficiency problems. In: Optometric manage- the Tabb method. I Am Optom Assoc
ble ET. She rejected the spectacles and ment of learning-related vision problems. St. 1984;55:409-18.
wore them only occasionally for reading. Louis: Mosby-year book, 1994: 270-1. 23. Swarbrick HA, Wong G, Oleary DJ. Corneal
She was unhappy and unwilling to face 3. Lambert SR. Accommodative esotropia. response to orthokeratology. Optom Vision Sci
people and the camera. When I asked her Ophthalmol Clin North Am 2001 1998;75:791-9.
Sep;14(3):425-32. 24. Lui W-O, Edwards MH. Orthokeratology in
mother for previous pictures as demon- 4. Rutstein RP, Marsh-Tootle W. Clinical course low myopia. Part 1: efficacy and predictability.
stration, only a few were available. of accommodative esotropia. Optom Vis Sci. Contact Lens Ant Eye 2000;23:77-89.
The use of Ortho-K is not new; how- 1998 ;75:97-102. 25. Rah MJ, Jackson JM, Jones LA, Marsden HJ,
ever, it has been mainly used in the treat- 5. Coats DK, Avilla CW, Paysse EA, Sprunger Bailey MD, Barr JT. Overnight orthoker-
DT, Steinkuller PG, Somaiya M. Early-onset atology: preliminary results of the Lenses and
ment of myopia in the adult population. In refractive accommodative esotropia.J AAPOS Overnight Orthokerartology(LOOK) study.
this case, I employed similar methods of 1998 Oct;2(5):275-8. Optom Vis Sci 2002;79:598-605.
tissue molding, but applied different lens 6. Hutcheson KA. Childhood esotropia. Curr 26. Cho P, Cheung SW, Edwards M. The longitu-
designs of dual geometry for hyperopia Opin Ophthalmol 2004 Oct;15(5):444-8. dinal orthokeratology research in children
7. Mulvihill A, MacCann A, Flitcroft I, OKeefe (LORIC) in Hong Kong: a pilot study on re-
molding. This new and unique applica- M. Outcome in refractive accommodative fractive changes and myopic control. Curr Eye
tion of Ortho-K and the use of VT to en- esotropia.Br J Ophthalmol 2000;84:746-9. Res 2005;30:71-80.
hance binocular functioning resulted in 8. Solan HA. Learning disabilities. In: 27. Lam SY, Goh SH. The incidence of refractive
several behavioral changes in this Rosenbloom Morgan. Principles and practice errors among school children in Hong Kong
of pediatric optometry. Philadelphia: J.B. and its relations with the optical components.
hyperopic six-year old. Her mother re- Lippincott, 1990:500-1. Clin Exp Optom 1991;74:97-103.
ports she is more at ease and confident in 9. Garzia R. The relationship between visual effi- 28. Mountford J, Pseudovs K. An analysis of the
school. She faces the camera naturally ciency problems and learning. In: Optometric astigmatic changes induced by accelerated
and smilingly with her cosmetically management of learning-related vision prob- orhtokeratology. Clin Exp Optm
lems. St. Louis: Mosby-year book, 1994: 2002;85:284-93.
straightened eyes. In spite of an inability 156-7. 29. Jessen GN. Orthofocus techniques. Contacto
to attain stereopsis, her level of 10. Hoffman LG. Incidence of vision difficulties in 1962;6:200-4.
binocularity has been significantly en- children with learning disabilities. J Am 30. Jessen GN. Contact lenses as a therapeutic de-
hanced. Optom Assoc 1980;51:447-51. vice. Am J Optom Arch Am Acad Optom
11. Wold RM, ed. Vision, Its Impact on Learning. 1964;41:429-35.
Current clinical evidence strongly Seattle: Special Child Publications,
suggests that myopic Ortho-K is revers- 1978;96-110.
Journal of Behavioral Optometry Volume 17/2006/Number 1/Page 7
31. U.S. Patent office; Patent Number 6,652,095.
Dual Geometric Contact Lenses for Hyperopia OEP PUBLICATIONS - PATIENT LIBRARY
and Presbyopia Orthokeratology. Approved
September, 2003. Tung; Hsiao-Ching (2F, No.
164, Ling Jiang Street, Taipei, TW)
32. Mountford J. An analysis of the Changes in
Corneal Shape and Refractive Errors Induced
by Accelerated Orthokeratology. ICLC
1997;24:128-43.
33. Parks. M . The monofixation syndrome.Trans
Am Ophthalmol Soc 1969;67:609-57
34. Wilson ME, Bluestein EC, Parks MM Binocu-
larity in accommodative esotropia. J Pediatr
Ophthalmol Strabismus 1993;4:233-6.
35. Berk AT, Kocak N, Ellidokuz H. Treatment
outcomes in refractive accommodative
esotropia. JAAPOS 2004;4:384-8.
36. Nichols JJ, Marsich MM, Nguyen M, Barr JT,
Bullimore MA. Overnight orthokeratology.
Optom Vis Sci 2000;77:252-9. The more informed your patients are, the better choices theyll make in
37. Walline JJ, Rah MJ, Jones LA. The Childrens
vision care. If all 47 titles listed were purchased individually, the total
Overnight Orthokeratology Investigation
(COOKI) pilot study.Optom Vis Sci
cost would be over $750.00 - a savings of $200.00! Full descriptions of
2004;81:407-13. all titles
38. Cheung SW, Cho P. Subjective and objective
assessments of the effect of ! A Practical Guide for Remedial ! Overcoming Left/Right
orthokeratologya cross-sectional study. Curr Approaches to Left/Right Confusion & Reversals: A
Eye Res 2004;28:121-7. Confusion & Reversals Classroom Approach
39. Young AL, Leung AT, Cheng LL, Law RW, ! Buzzards To Bluebirds ! Reflexes, Learning &
Wong AK, Lam DS. Orthokeratology ! Childhood Learning - Journey Behavior: A Window Into the
Lens-Related Corneal Ulcers In Children: A or Race? Childs Mind
Case Series. Ophthalmol 2004;111:590-5. ! Reversal Errors: Theories &
40. Wu CC, Lee SM, Hsu WM, Lau LI. Pseudo-
! Classroom Visual Activities
! Creating Your Personal Vision Therapy Procedures
monas corneal ulcer related to overnight
orthokeratology. Cornea 2003 ;22:262-4 ! Dancing in the Rain ! Seeing is Achieving
41. Bar JT., Rah, MJ; Meyers W. Science & Clin- ! Dear Teacher: Eyes & Their ! Seeing Without Glasses
ical Practice. Corneal Refractive Therapy: Signals ! Smart Medicine For Your
Challenges, Controversies, and New Opportu- ! Developing Your Child For Eyes
nities. Eye & Contact Lens 2004;30:247-251. Success ! Stress & Vision
! Effects of Vision on Learning & ! Suddenly Successful
Corresponding author: School Performance ! Suddenly Successful Student
Tung Hsiao-Ching, M.D ! Electromagnetic Pollution ! Take Off Your Glasses and
2F,164 Lin-Jiang St. Solutions See
Tapei 106, Taiwan ! Enhance Your Infants ! The Power Behind Your Eyes
tung.hsiao.ching@vipok.com Development ! The Rage
! Eye Q and the Efficient Learner ! The Myth of the A.D.D. Child
Date accepted for publication:
! Eyes On Track: A Missing Link ! The Pros Edge: Visual
December 28,2005 To Successful Learning Training For Golf
! Focus Your Minds Eye ! The Coordinated Classroom
! Help Your Child to Learn ! The Turtle Who Needed
! Helping Your Child to Learn Glasses
! How to Develop Your Childs ! Thinking Goes to School
Intelligence ! Tomorrows Children for
! How to Use Your Power of Parents
Visualization ! Total Health at the Computer
! Integrating Mind, Brain & Body ! Total Vision
Through Movement ! Vision & School Success
! Light: Medicine of the Future ! Visual Imagery
! Little Kims Left & Right Book ! Without Ritalin: A Natural
! Magic Eye - Beyond 3D Approach To ADD
! Natural Eye Care: An ! Your Childs Vision
Encyclopedia
Patient Library - 47 titles listed above
PATLIB-1 $550.00
Order 5 or more titles and take a 10% discount. Use code
PATLIB-DISC
To place order, contact OEP at (949) 250-8070
Volume 17/2006/Number 1/Page 8 Journal of Behavioral Optometry
S-ar putea să vă placă și
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (399)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (587)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (890)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- Ashley Jones RN ResumeDocument1 paginăAshley Jones RN Resumeapi-299649525100% (1)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (73)
- RISK Analysis Example For Medical Devices According To EN ISO 14971:2012Document6 paginiRISK Analysis Example For Medical Devices According To EN ISO 14971:2012patricia colinÎncă nu există evaluări
- Medical Prioritization ProcessDocument20 paginiMedical Prioritization ProcessIGDÎncă nu există evaluări
- Patient care and discharge planDocument2 paginiPatient care and discharge planBryan Carmona100% (1)
- Ambu BagDocument29 paginiAmbu BagJessa Borre100% (2)
- The Quest for Conservative and Predictable Esthetic Posterior RestorationsDocument31 paginiThe Quest for Conservative and Predictable Esthetic Posterior RestorationsJitender Reddy50% (2)
- JCI Reference Guide WRDocument55 paginiJCI Reference Guide WRSanjeev Chougule100% (1)
- IDS Inmediate Dentin Sealing For Tooth Preparations... Magne 2014Document2 paginiIDS Inmediate Dentin Sealing For Tooth Preparations... Magne 2014Angie HernándezÎncă nu există evaluări
- Use of Machine Learning To Identify Children With Autism and Their Motor AbnormalitiesDocument12 paginiUse of Machine Learning To Identify Children With Autism and Their Motor AbnormalitiesPierre A. RodulfoÎncă nu există evaluări
- Accommodative Insufficiency A Literature and Record ReviewDocument6 paginiAccommodative Insufficiency A Literature and Record ReviewPierre A. RodulfoÎncă nu există evaluări
- Changing Paradigms Optometric Vision Therapy Is Neuro-ScienceDocument4 paginiChanging Paradigms Optometric Vision Therapy Is Neuro-SciencePierre A. RodulfoÎncă nu există evaluări
- Maintaining CompetitivenessDocument1 paginăMaintaining CompetitivenessPierre A. RodulfoÎncă nu există evaluări
- 3D Technology Increasing The Need For Optometric Vision TherapyDocument2 pagini3D Technology Increasing The Need For Optometric Vision TherapyPierre A. RodulfoÎncă nu există evaluări
- Accommodative Response in ChildrenDocument7 paginiAccommodative Response in ChildrenPierre A. RodulfoÎncă nu există evaluări
- A Consideration of Binocular Parameters in The Spectacle PDFDocument5 paginiA Consideration of Binocular Parameters in The Spectacle PDFPierre A. RodulfoÎncă nu există evaluări
- Demographic and Clinical Profile of Patients Who Underwent Refractive Surgery ScreeningDocument8 paginiDemographic and Clinical Profile of Patients Who Underwent Refractive Surgery ScreeningPierre A. RodulfoÎncă nu există evaluări
- 23 3 HowellDocument5 pagini23 3 HowellPierre A. RodulfoÎncă nu există evaluări
- A Five-Year Review of Refractive Procedures, Outcomes and ComplicationsDocument9 paginiA Five-Year Review of Refractive Procedures, Outcomes and ComplicationsPierre A. RodulfoÎncă nu există evaluări
- Is Femtosecond Technology The Future of Our Cataract SurgeryDocument4 paginiIs Femtosecond Technology The Future of Our Cataract SurgeryPierre A. RodulfoÎncă nu există evaluări
- 23 4 Viewpoint LaudonDocument2 pagini23 4 Viewpoint LaudonPierre A. RodulfoÎncă nu există evaluări
- 2014 Updated Recommendations For Preschool Vision Screening Guidelines For Filipino Children Entering The Philippine Public School SystemDocument5 pagini2014 Updated Recommendations For Preschool Vision Screening Guidelines For Filipino Children Entering The Philippine Public School SystemPierre A. RodulfoÎncă nu există evaluări
- Profile of Glaucoma Patients in a Philippine HospitalDocument7 paginiProfile of Glaucoma Patients in a Philippine HospitalPierre A. RodulfoÎncă nu există evaluări
- 23 Final WeigelDocument5 pagini23 Final WeigelPierre A. RodulfoÎncă nu există evaluări
- 22 5 Fox PDFDocument4 pagini22 5 Fox PDFPierre A. RodulfoÎncă nu există evaluări
- 23 Final NewmanDocument4 pagini23 Final NewmanPierre A. RodulfoÎncă nu există evaluări
- 23 3 GodtlandDocument4 pagini23 3 GodtlandPierre A. RodulfoÎncă nu există evaluări
- The Golf Putting Stroke: Psychological Pressure Eye, Head, Heart & Breathing ResponsesDocument7 paginiThe Golf Putting Stroke: Psychological Pressure Eye, Head, Heart & Breathing ResponsesPierre A. RodulfoÎncă nu există evaluări
- Intermittent Exotropia: Management Options and Surgical OutcomesDocument4 paginiIntermittent Exotropia: Management Options and Surgical OutcomesPierre A. RodulfoÎncă nu există evaluări
- 22-6 Harris ReviewDocument2 pagini22-6 Harris ReviewPierre A. RodulfoÎncă nu există evaluări
- 20-2 Editorial MaplesDocument2 pagini20-2 Editorial MaplesPierre A. RodulfoÎncă nu există evaluări
- 21-2 DudleyDocument7 pagini21-2 DudleyPierre A. RodulfoÎncă nu există evaluări
- 22-6 Gallop ViewpointDocument3 pagini22-6 Gallop ViewpointPierre A. RodulfoÎncă nu există evaluări
- Literature Review: Contact Lenses Slow Myopia in ChildrenDocument3 paginiLiterature Review: Contact Lenses Slow Myopia in ChildrenPierre A. RodulfoÎncă nu există evaluări
- 21-2 Fortenbacher EditorialDocument3 pagini21-2 Fortenbacher EditorialPierre A. RodulfoÎncă nu există evaluări
- 20 4 MassucciDocument5 pagini20 4 MassucciPierre A. RodulfoÎncă nu există evaluări
- 20-1 BartuccioDocument5 pagini20-1 BartuccioPierre A. RodulfoÎncă nu există evaluări
- The Golf Putting Stroke: Psychological Pressure Eye, Head, Heart & Breathing ResponsesDocument7 paginiThe Golf Putting Stroke: Psychological Pressure Eye, Head, Heart & Breathing ResponsesPierre A. RodulfoÎncă nu există evaluări
- 19-5 CloptonDocument3 pagini19-5 CloptonPierre A. RodulfoÎncă nu există evaluări
- Salwa Maghrabi Teacher Assistant Nursing Department: Prepared byDocument30 paginiSalwa Maghrabi Teacher Assistant Nursing Department: Prepared byPearl DiBerardino100% (1)
- Nurse Case Manager Care Coordinator in Philadelphia PA Resume Kimberly BolenDocument2 paginiNurse Case Manager Care Coordinator in Philadelphia PA Resume Kimberly BolenKimberlyBolenÎncă nu există evaluări
- Complaints Data Collection LetterDocument4 paginiComplaints Data Collection LetterthrinathÎncă nu există evaluări
- Rhopalurus Junceus: and The Treatment of CancerDocument17 paginiRhopalurus Junceus: and The Treatment of CancerAmalia Tri UtamiÎncă nu există evaluări
- Beltran, Justin KyleDocument4 paginiBeltran, Justin KyleKYLEÎncă nu există evaluări
- Rift Valley FeverDocument9 paginiRift Valley Feverapi-390015550Încă nu există evaluări
- New Fixed Acrylic Bite Plane for Deep Bite CorrectionDocument6 paginiNew Fixed Acrylic Bite Plane for Deep Bite CorrectionFisaÎncă nu există evaluări
- 0315 DVTDocument28 pagini0315 DVTEloisa TardioÎncă nu există evaluări
- CLASSIFYING GASTRITISDocument40 paginiCLASSIFYING GASTRITISmadalinamihaiÎncă nu există evaluări
- Socolov Et. Al., 2018 Cognitive Impairment in MEDocument19 paginiSocolov Et. Al., 2018 Cognitive Impairment in MERicardo Jose De LeonÎncă nu există evaluări
- Vincent Mosca - Clubfoot Guide For ParentsDocument3 paginiVincent Mosca - Clubfoot Guide For ParentsCatalin FloreaÎncă nu există evaluări
- Case Study SLDocument5 paginiCase Study SLCharmie Mei Paredes-RoqueÎncă nu există evaluări
- Andre Hannah NursingresumeDocument1 paginăAndre Hannah Nursingresumeapi-450112281Încă nu există evaluări
- 2015 Sigmoid DiverticulitisDocument11 pagini2015 Sigmoid DiverticulitisDinÎncă nu există evaluări
- Challenges in Hospital IT & Networking Design - Niranjan - Invest2Care PDFDocument15 paginiChallenges in Hospital IT & Networking Design - Niranjan - Invest2Care PDFVelram ShanmugamÎncă nu există evaluări
- NIH Public Access: Author ManuscriptDocument24 paginiNIH Public Access: Author ManuscriptireneaureliaÎncă nu există evaluări
- SAFERamp - Whe-2314-09Document3 paginiSAFERamp - Whe-2314-09608943Încă nu există evaluări
- MCQDocument6 paginiMCQalirbidiÎncă nu există evaluări
- Jurnal Studi Kasus AskepDocument8 paginiJurnal Studi Kasus Askepaji bayuÎncă nu există evaluări
- Dental and Craniomaxillofacial Implant SurgeryDocument35 paginiDental and Craniomaxillofacial Implant SurgeryJean Carlos Barbosa FerreiraÎncă nu există evaluări
- Improving Patient Safety in Radiotherapy by Learning From Near Misses, Incidents and ErrorsDocument5 paginiImproving Patient Safety in Radiotherapy by Learning From Near Misses, Incidents and ErrorsrosanaÎncă nu există evaluări
- Anemia of Prematurity UpToDate PDFDocument13 paginiAnemia of Prematurity UpToDate PDFАлександар ТасићÎncă nu există evaluări