Documente Academic
Documente Profesional
Documente Cultură
Chest: The Role of CT Scanning in Multidimensional Phenotyping of COPD
Încărcat de
Atika Indah SariTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Chest: The Role of CT Scanning in Multidimensional Phenotyping of COPD
Încărcat de
Atika Indah SariDrepturi de autor:
Formate disponibile
CHEST Original Research
COPD
The Role of CT Scanning in
Multidimensional Phenotyping of COPD
Mona Bafadhel, MBChB; Imran Umar, BSc; Sumit Gupta, MBBS; J. Vimal Raj, MBBS;
Dhiraj D. Vara, BSc; James J. Entwisle, MBBS; Ian D. Pavord, DM;
Christopher E. Brightling, PhD, FCCP; and Salman Siddiqui, PhD
Background: COPD is a heterogeneous disease characterized by airow obstruction and diag-
nosed by lung function. CT imaging is emerging as an important, noninvasive tool in phenotyping
COPD. However, the use of CT imaging in dening the disease heterogeneity above lung func-
tion is not fully known.
Methods: Seventy-ve patients with COPD (58 men, 17 women) were studied with CT imaging and
with measures of airway inammation. Airway physiology and health status were also determined.
Results: The presence of emphysema (EM), bronchiectasis (BE), and bronchial wall thickening
(BWT) was found in 67%, 27%, and 27% of subjects, respectively. The presence of EM was associ-
ated with lower lung function (mean difference % FEV1, 220%; 95% CI, 228 to 211; P , .001).
There was no difference in airway inammation, exacerbation frequency, or bacterial load in
patients with EM alone or with BE and/or BWT EM. The diffusing capacity of the lung for car-
bon monoxide/alveolar volume ratio was the most sensitive and specic parameter in identifying
EM (area under the receiver operator characteristic curve, 0.87; 95% CI, 0.79-0.96). Physiologic
cluster analysis identied three clusters, two of which were EM predominant and the third char-
acterized by a heterogeneous combination of EM and BE.
Conclusions: The application of CT imaging can be useful as a tool in the multidimensional
approach to phenotyping patients with COPD. CHEST 2011; 140(3):634642
Abbreviations: BE 5 bronchiectasis; BWT 5 bronchial wall thickening; Dlco 5 diffusing capacity of the lung for carbon
monoxide; EM 5 emphysema; RV 5 residual volume; Va 5 alveolar volume
COPD is a heterogeneous disease characterized by
airow obstruction that is not fully reversible and
lung parenchyma and changes within the large and
small airways.8 This evident disease heterogeneity
is associated with a progressive decline in lung func- cannot be dened by the FEV1 alone, and alternative
tion.1 Airway inammation in COPD is usually neu- methods need to be sought to develop mechanistic,
trophilic,2,3 but eosinophilic airway inammation has prognostic, and therapeutic applications in the man-
been found at stable state4,5 and during exacerbations.6,7 agement of COPD.9 CT imaging has emerged as a
Pathologic processes in COPD include destruction of noninvasive tool in the phenotyping of COPD, with
measures investigating changes in the airway wall and
Manuscript received November 22, 2010; revision accepted
February 19, 2011.
Afliations: From the Department of Infection, Immunity and Correspondence to: Salman Siddiqui, PhD, Institute for Lung
Inammation (Drs Bafadhel, Pavord, Brightling, and Siddiqui and Health, University of Leicester, Department of Infection, Immunity
Mr Umar), University of Leicester; the Department of Radiology and Inammation, Clinical Sciences Wing, Gleneld Hospital,
(Drs Gupta, Raj, and Entwisle); and the Department of Respira- Groby Road, Leicester, LE3 9QP, England; e-mail: salman95@
tory Physiology (Mr Vara), University Hospitals of Leicester NHS yahoo.com
Trust, Leicester, England. 2011 American College of Chest Physicians. This is an
Drs Brightling and Siddiqui were joint senior authors of this article. Open Access article distributed under the terms of the Creative
Funding/Support: Dr Bafadhel is funded by a grant from the Commons Attribution-Noncommercial License (http://creative
Medical Research Council, and Dr Brightling is funded by a commons.org/licenses/by-nc/3.0/), which permits unrestricted
Wellcome Senior Clinical Fellowship [03/91/68] that requires use, distribution, and reproduction in any medium, provided the
Open Access placement. The research was performed in labo- original work is properly cited. Information for commercial entities
ratories partly funded by the European Regional Development is available online (http://www.chestpubs.org/site/misc/reprints.xhtml).
Fund [ERDF 05567]. DOI: 10.1378/chest.10-3007
634 Original Research
Downloaded from chestjournal.chestpubs.org by Kimberly Henricks on September 7, 2011
2011 AmericanatCollege
Downloaded for dr. Avit Suchitra 100 (avitsuchitra@fk.unand.ac.id) ClinicalKeyofGlobal
Chest Physicians
Guest Users from ClinicalKey.com by Elsevier on July 22, 2017.
For personal use only. No other uses without permission. Copyright 2017. Elsevier Inc. All rights reserved.
lumen and within the lung parenchyma,10-12 as well overall impairment, with zero indicating best possible health sta-
as assessments of the degree of emphysema (EM) tus and 100 indicating worst possible health status; the Chronic
Respiratory Disease Interviewer-Administered Questionnaire
and burden of small airways disease. CT imaging (McMaster University; Hamilton, Ontario, Canada),28 which mea-
quantitative assessments have shown, inter alia, asso- sures disease-specic quality of life with scores ranging from 1 to 7,
ciations with parameters of airway physiology,13-15 with a higher score indicating a better quality of life for the
important COPD outcome measures,15-18 and sys- domains of emotion, mastery, dyspnea, and fatigue; and the
temic inammatory mediators.19 visual analog scale (VAS) for the domains of cough, breathless-
ness, sputum production, and sputum purulence, which consists of
However, the role of CT imaging in dening COPD a 100-mm line for each measured domain, with no symptoms at one
phenotypes above and beyond conventional charac- end and the worst symptoms ever at the other.29 Body composi-
terization with full lung function (spirometry, static tion was calculated using BMI.30 Spontaneous or induced sputum
lung volumes, and gas transfer) remains to be fully was collected and analyzed for bacteria,31 including colony-forming
determined. Furthermore, the validity of CT imag- units.32 Quantitative real-time polymerase chain reaction was used
to estimate the total bacterial load based on the abundance of
ing as a biomarker of airways disease has yet to be 16S ribosomal subunit encoding genes. In brief, bacterial DNA
established.20,21 was extracted from homogenized sputum according to the
We hypothesized that CT imaging provides addi- manufacturers instructions, using the QIAmp DNA Mini Kit
tional value to clinical and physiologic parameters assay (QIAGEN, Ltd; Hilden, Germany). Quantication of the
in the multidimensional phenotyping of COPD. We total bacterial load was performed using the SYBR green assay
(PE Applied Biosystems; Warrington, England). Sputum samples
tested our hypothesis by evaluating whether pheno- were then processed to produce cytospins for cell differential.33,34
typing of COPD using factor and cluster analysis Venous blood was collected for assessment of peripheral blood
with lung function parameters (physiologic clustering) differential cell counts and serum C-reactive protein.
would generate the radiologic COPD disease groups
seen in clinical practice (EM, bronchial wall thick- CT Imaging
ening [BWT], and bronchiectasis [BE]).
CT imaging was performed using a Sensation 16-slice scanner
(Siemens Healthcare; Knoxville, Tennessee). Sequential scanning
Materials and Methods was performed at maximal inspiration from the apex to the dia-
phragm at 10-mm increments, with 1-mm collimation, while patients
were in the supine position. Image reconstruction was per-
Patients formed by using a high-spatial-frequency algorithm through a
Patients with a physician diagnosis of COPD as per GOLD 512 3 512 matrix with a small eld of view. Scanning time ranged
(Global Initiative for Chronic Obstructive Lung Disease) criteria1 from 30 to 45 s with a 120-kV peak and an effective tube current
were recruited consecutively from general respiratory clinics and of 140 mA. Images were reported at a window width and level of
through local advertising to enter the longitudinal Biomarkers in 1,600 and 2500 Hounseld units, respectively. CT scan qualita-
COPD Exacerbation study. Patients with a diagnosis of asthma, tive radiologic reporting for EM, BE, and BWT was performed in
current active pulmonary TB, or any other clinically relevant accordance with published guidelines.35 BE was present when
lung disease were excluded. All patients had obstructive spirom- one or more of the following criteria were fullled: (1) an internal
etry with a postbronchodilator FEV1/FVC ratio of , 0.7, whereas diameter of the bronchus greater than that of the adjacent pul-
severity was classied according to the GOLD criteria.1 Patients monary artery, (2) a lack of tapering of the bronchial lumen toward
with COPD who demonstrated bronchodilator reversibility were the periphery, or (3) visualization of the bronchus within 10 mm
not excluded. All patients gave written informed consent, and of the pleural space. EM was present when focal areas of low
the study was approved by the Leicestershire, Northamptonshire, attenuation without visible walls were detected, and included the
and Rutland ethics committee (REC 07/H0406/157). presence of centrilobular, panlobular, and paraseptal EM. BWT
was assessed subjectively as described previously.36 Previous stud-
Study Design ies at our institution have shown that the qualitative description
method of EM, BWT, and BE has good interobserver agreement
Seventy-ve patients enrolled in the Biomarkers in COPD and image reconstruction; scanning and reporting was optimized
Exacerbation study, who had previously undergone a CT scan as for analysis of BWT, EM, and BE as previously described.36
part of their clinical management, were studied. The median
(interquartile range) interval time between patient characteriza- Statistical Analysis
tion and CT scanning was 15 (25) months.
Statistical analysis was performed using PRISM, version 4
Measurements (GraphPad Software; San Diego, California) and SPSS, version 16
(SPSS Inc; Chicago, Illinois). Parametric and nonparametric data
All patients had complete demographic data recorded, includ- are presented as mean (SEM) and median (interquartile range)
ing age, duration of symptoms, and full smoking and medical unless stated otherwise. Log-transformed data are presented as
history. Full lung function, including reversibility testing with geometric mean (95% CI). For comparison of unpaired or paired,
400 mg inhaled albuterol, was also performed according to the parametric or nonparametric groups, the Student t test, paired
American Thoracic Society/European Respiratory Society con- t test, Mann-Whitney test, and Wilcoxon matched pairs test
sensus guidelines.22-26 Health status and symptom scores were mea- were used, respectively. For comparison of three groups or more
sured using the St. George Respiratory Questionnaire (University for parametric and nonparametric variables, the one-way analysis
of London; London, England),27 a two-part questionnaire measur- of variance or Kruskal-Wallis test was used and the x2 test was
ing recollection of symptoms and assessment of current activity used for proportions. Logistic regression analysis was used37 to
and impact, in which scores are expressed as a percentage of assess the relationship of the dependant variables of (1) presence
www.chestpubs.org CHEST / 140 / 3 / SEPTEMBER, 2011 635
Downloaded from chestjournal.chestpubs.org by Kimberly Henricks on September 7, 2011
2011 AmericanatCollege
Downloaded for dr. Avit Suchitra 100 (avitsuchitra@fk.unand.ac.id) ClinicalKeyofGlobal
Chest Physicians
Guest Users from ClinicalKey.com by Elsevier on July 22, 2017.
For personal use only. No other uses without permission. Copyright 2017. Elsevier Inc. All rights reserved.
of EM, (2) presence of BE, and (3) presence of BWT with explan- Table 1Clinical Characteristics of Patients With
atory (independent) variables, using the block entry method. Vari- COPD With Corresponding CT Scan
ables entered into the logistic regression model, chosen for clinical
relevance, were the following continuous variables: FEV1 % pre- Patients With COPD With
dicted, diffusing capacity of the lung for carbon monoxide (Dlco)/ Characteristic CT scan Data (n 5 75)
alveolar volume (Va), residual volume (RV) % predicted, total
Male, No. (%) 58 (77)
sputum neutrophil count, and percentage sputum eosinophils (both
Age, y, mean (range) 67 (43-88)
log transformed). Model inspection showed no multicollinearity,
Current smoker, No. (%) 24 (32)
goodness of t was performed using the Hosmer-Lemeshow
Ex-smoker, No. (%) 50 (67)
x2 test, and the NagelKerke R2 was used to estimate the variance
Pack-y smoked, mean (range) 48 (10-153)
explained by the model. The Wald test was used to assess the
Exacerbation history in previous y 4.3 (0.3)
signicance of the individual dependant variables to the model.
BMI, kg/m2 26.1 (0.6)
Unsupervised multivariate modeling using principal component
ICS usage, No. (%) 68 (91)
factor reduction analysis (orthogonal varimax rotation method)
ICS dosage, mg 1424 (92)
was used to explore airway physiologic pattern expression in the
FEV1,a L 1.22 (0.06)
patients. Hierarchic cluster analysis was then applied from the
FEV1 % predicteda 46 (2)
identied factors to determine physiologic clusters of COPD.
Reversibility, % 3 (1)
Clinical characteristics for the physiologic clusters were tabulated.
FEV1/FVC,a % 47 (2)
One-way analysis of variance, Kruskal Wallis, and the x2 test were
SGRQ total, units 55.2 (2.0)
used to compare parametric, nonparametric, and proportions of
CRQ total, units 4.00 (0.13)
clinical characteristics between physiologic cluster groups. A P value
VAS total, mm 147 (9)
of , .05 was deemed to be statistically signicant.
Sputum total cell count 3 106 cells/g, 3.8 (2.8-5.3)
geometric mean (95% CI)
Sputum neutrophils, % 69 (3)
Sputum eosinophils, %, geometric 1.3 (0.9-1.9)
Results
mean (95% CI)
CT data were available in 75 patients (58 men, Data are presented as mean (SEM) unless otherwise indicated.
17 women). The most common clinical indication for CRQ 5 Chronic Respiratory Disease Interviewer-Administered Ques-
tionnaire; ICS 5 inhaled corticosteroid; SGRQ 5 St. George Respiratory
CT scanning was investigation or exclusion of malig-
Questionnaire; VAS 5 visual analog scale.
nancy (40%), followed by assessment for radiographic aPostbronchodilator.
evidence of BE (30%) and suitability for lung volume
reduction surgery (20%). The clinical characteristics
of patients are shown in Table 1. identify the presence of EM was 0.87 (95% CI,
0.79-0.96) (Fig 2). All of the conventional measures
EM, BE, and BWT Are Common Radiologic of lung function (FEV1, Dlco/Va, RV, and FEV1/FVC)
Observations in COPD, With Signicant Overlap were reliable in distinguishing between EM only
and EM plus BE and/or BWT (EM 1 BE/BWT),
The CT scan description of EM, BE, and BWT with receiver operator characteristic curves of , 0.6
was present in 67%, 27%, and 27%, respectively. (Fig 3).
The number of patients with EM, BE, and BWT, and In contrast to this, patients with radiologic EM in
the associated overlap, are shown in Figure 1. No evi- the presence or absence of BE and/or BWT did not
dence of EM, BE, or BWT on CT scanning was have any signicant difference in markers of proximal
found in 13 patients in the COPD cohort. Subjects airway inammation (sputum total cell count and cel-
with CT scan evidence of disease had worse lung lular differential count) or bacterial load (measured
function, but there was no difference in demo-
graphic distribution, health status, or symptom scores
(Table 2).
Conventional Lung Function Reliably Identies
Patients With Radiologic EM and COPD
CT scan evidence of EM compared with no evi-
dence of EM was associated with lower lung func-
tion (39 vs 61; mean difference, 222%; 95% CI, 230
to 213; P , .001), impaired Dlco (3.8 vs 5.6; mean
difference, 21.8; 95% CI, 22.7 to 20.9; P , .001), and
increased airway obstruction (FEV1/FVC) (0.43 vs 0.57;
mean difference, 20.14; 95% CI, 20.20 to 20.08;
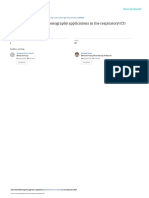
Figure 1. Nonproportional Venn diagram representing patients
P , .001). The receiver operator characteristic curve with EM, BE, and BWT on CT scanning. BE 5 bronchiectasis;
(area under the curve) for the Dlco/Va to correctly BWT 5 bronchial wall thickening; EM 5 emphysema.
636 Original Research
Downloaded from chestjournal.chestpubs.org by Kimberly Henricks on September 7, 2011
2011 AmericanatCollege
Downloaded for dr. Avit Suchitra 100 (avitsuchitra@fk.unand.ac.id) ClinicalKeyofGlobal
Chest Physicians
Guest Users from ClinicalKey.com by Elsevier on July 22, 2017.
For personal use only. No other uses without permission. Copyright 2017. Elsevier Inc. All rights reserved.
Table 2Clinical Comparisons in Patients With Demonstrable Absence or Presence of CT Scan Evidence
of EM, BE, or BWT
Characteristic Absence of EM/BE/BWT (n 5 13) Presence of EM/BE/BWT (n 5 62) P Value
Male, No. (%) 8 (62) 50 (81) 0.63
Age, y, mean (range) 68 (49-88) 67 (43-85) .90
Pack-y smoked mean (range) 35 (10-68) 50 (10-153) .10
Exacerbation history in previous y 3.7 (0.9) 4.4 (0.3) .43
ICS dosage, mg 831 (213) 1548 (95) , .001
FEV1 % predicteda 62 (5) 43 (2) , .001
FEV1/FVC,a % 59 (3) 45 (2) , .001
SGRQ total, units 50.3 (5.9) 56.4 (2.0) .23
CRQ total, units 4.21 (0.35) 3.95 (0.14) .45
VAS total, mm 149 (16) 146 (10) .92
Sputum total cell count 3 106 cells/g, 3.5 (1.9 -6.6) 3.9 (2.7-5.6) .82
geometric mean (95% CI)
Sputum neutrophils, % 66 (5) 70 (3) .64
Sputum eosinophils, %, 1.2 (0.5-2.8) 1.3 (0.9-2.0) .83
geometric mean (95% CI)
Data are presented as mean (SEM) unless otherwise indicated. BE 5 bronchiectasis; BWT 5 bronchial wall thickening; EM 5 emphysema.
See Table 1 legend for expansion of other abbreviations.
aPostbronchodilator.
by colony-forming units and abundance of 16S ribo- Conventional Lung Function Fails to Identify
somal subunit encoding genes) (Table 3). Patients With BE and BWT in COPD
Having conrmed that static lung volumes and
Static Lung Volume and Transfer Factor
transfer factor were predictive of radiologic EM, we
Are Independent Predictors of EM in
sought to identify whether these markers could inde-
COPD, But Not of BE or BWT
pendently group patients with EM-predominant
The Dlco/Va and RV were conrmed by logistic disease (EM1) or disease without EM (EM2) in the
regression analysis to be independent predictors of presence or absence of BWT/BE, using unsupervised
EM on CT scanning in patients with COPD. In con- statistical techniques. Principal component analysis
trast, the variables entered into the model were not using airway physiologic parameters in all patients with
independent predictors of BE or BWT (Table 4). full physiologic testing and CT scan (n 5 64) identi-
ed three factors with eigen values . 1 (Table 5),
highlighting the following dominant physiologic com-
ponents: (1) RV, (2) Dlco/Va, and (3) lung capacity.
Hierarchic cluster analysis determined three cluster
groups. Two were EM predominant, discrete only
in their degree of air trapping and gas transfer. The
third cluster was characterized by a heterogeneous
combination of EM and BE, with preservation of gas
transfer and lung volumes (Table 6).
Repeatability of Airway Physiologic Phenotypes
Forty-seven patients had spirometry performed
12 months after the initial characterization visit. In
these patients, the repeatability of the measures of
FEV1 and FVC was good, with intraclass coefcients of
0.91 and 0.82, respectively (P , .001). There was no dif-
ference in the mean change in lung function for each
of the physiologic clusters identied after 12 months
(cluster 1 [EM-predominant, moderate lung func-
tion], 0.03; 95% CI, 20.11 to 0.17; cluster 2 [heteroge-
neous, lung function preserved], 20.13; 95% CI, 20.23
Figure 2. Receiver operator characteristic curve (sensitivity and
1-specicity) of diffusing capacity of the lung for carbon monox- to 20.03; and cluster 3 [EM-predominant, severe lung
ide corrected for alveolar volume for identifying emphysema. function], 0.00; 95% CI, 20.12 to 0.12; P 5 .17).
www.chestpubs.org CHEST / 140 / 3 / SEPTEMBER, 2011 637
Downloaded from chestjournal.chestpubs.org by Kimberly Henricks on September 7, 2011
2011 AmericanatCollege
Downloaded for dr. Avit Suchitra 100 (avitsuchitra@fk.unand.ac.id) ClinicalKeyofGlobal
Chest Physicians
Guest Users from ClinicalKey.com by Elsevier on July 22, 2017.
For personal use only. No other uses without permission. Copyright 2017. Elsevier Inc. All rights reserved.
with COPD, whereas the presence of BWT alone is
sparse. Current guidelines use bedside spirometry and
FEV1 to diagnose and guide the severity of COPD.1
Although this tool can be widely applied, it has less
accuracy when used to measure small airways dys-
function (airways with internal diameter , 2 mm).9
Using CT imaging, we have shown that, in patients
with COPD, there are variation and overlap in the
associated pathologic ndings. Thus, the use of FEV1
alone to diagnose and guide management in COPD
highlights that spirometry cannot dene these patho-
logic processes with clarity. Our nding of BE in those
with spirometric classication of COPD is compara-
ble to those observed previously38 and highlights
the heterogeneity that exists, which can, in turn, be
partly delineated by radiologic characterization.38-40
Figure 3. Receiver operator characteristic curves for distin- In patients with EM on CT scan, we found wors-
guishing the presence of emphysema alone vs emphysema plus ened lung function, airow obstruction, and larger
bronchiectasis and/or bronchial wall thickening. Dlco/Va 5 increases in residual lung volume, compared with
diffusing capacity of the lung for carbon monoxide/alveolar volume;
RV 5 residual volume. patients with radiologic evidence of BE or BWT,
although the clinical parameters of airway inam-
Discussion mation, health status, and microbiologic qualitative
or quantitative inammation are indistinguishable
In this study, we have shown that there is overlap between these radiologic phenotypes. This is in keep-
in radiologic evidence of EM, BE, and BWT in patients ing with previous physiologic observations15 and
Table 3Airway Inammometry, Physiology, and Health Status in Patients With EM Alone,
BE and/or BWT Without EM, and EM With BWT and/or BE
Characteristic EM (n 5 29) BE/BWT 2 EM (n 5 12) EM 1 BWT/BE (n 5 21) P Value
Male, No. (%) 22 (76) 9 (75) 19 (91) .37
Age, y, mean (range) 64 (43-83) 71 (60-84) 69 (47-85) .07
Ex-smoker, No. (%) 17 (59) 11 (92) 12 (57) .09
Pack-y smoked, mean (range) 48 (18-120) 47 (10-153) 55 (10-134) .68
Exacerbation history in previous y 4.0 (0.5) 3.9 (0.9) 5.1 (0.5) .32
BMI, kg/m2 25.2 (0.9) 28.2 (1.4) 24.7 (0.4) .10
Sputum total cell count 3 106 cells/g, 3.2 (2.0-5.2) 8.4 (4.3-16.5) 3.6 (1.7-7.7) .18
geometric mean (95% CI)
Sputum neutrophils, % 70 (4) 77 (6) 65 (6) .44
Sputum eosinophil, %, geometric mean (95% CI) 1.6 (0.9-2.8) 0.8 (0.4-1.7) 1.3 (0.6-2.7) .55
Potential pathogenic organism, % 14 25 38 .08
Sputum neutrophil count 3 106 cells/g, 2.3 (1.3-4.0) 6.3 (2.8-14.1) 1.9 (0.8-4.8) .18
geometric mean (95% CI)
Total bacterial load (16S), geometric mean (95% CI) 1.58 (6.67-3.28) 1.78 (3.57-8.18) 1.58 (3.27-6.78) .99
Colony forming units per mL of sputum, 1.46 (6.35-3.06) 1.26 (1.56-9.16) 7.85 (3.05-2.06) .71
geometric mean (95% CI)
FEV1 % predicteda 41 (3) 59 (5) 37 (4) , .01
FEV1/FVC,a % 42 (2) 56 (4) 44 (2) .01
Reversibility, % 4.0 (1.9) 3.0 (2.9) 20.4 (3.3) .44
RV, % 162 (10) 115 (10) 139 (10) .02
Total lung capacity, % 124 (10) 99 (5) 103 (7) .13
Dlco, mL CO/min/mm Hg 4.0 (0.3) 5.8 (0.6) 3.6 (0.3) , .01
Dlco % predicted 46 (4) 73 (7) 32 (4) ,.01
Dlco/Va, mL CO/min/mm Hg/L 0.8 (0.1) 1.0 (0.1) 1.3 (0.4) .37
Dlco/Va % predicted 56 (5) 89 (10) 49 (4) , .01
SGRQ total, units 57.9 (3.1) 52.3 (3.5) 56.4 (3.6) .61
CRQ total, units 3.79 (0.21) 4.07 (0.31) 4.11 (0.26) .57
VAS total, mm 163 (13) 143 (25) 126 (18) .24
Data are presented as mean (SEM) unless otherwise indicated. Dlco 5 diffusing capacity of the lung for carbon monoxide; Va 5 alveolar volume;
RV 5 residual volume. See Table 1 and 2 legends for expansion of other abbreviations.
aPostbronchodilator.
638 Original Research
Downloaded from chestjournal.chestpubs.org by Kimberly Henricks on September 7, 2011
2011 AmericanatCollege
Downloaded for dr. Avit Suchitra 100 (avitsuchitra@fk.unand.ac.id) ClinicalKeyofGlobal
Chest Physicians
Guest Users from ClinicalKey.com by Elsevier on July 22, 2017.
For personal use only. No other uses without permission. Copyright 2017. Elsevier Inc. All rights reserved.
Table 5Extracted Factors With Eigenvalues . 1 Using
1.00 (0.96-1.04)
0.72 (0.23-2.25)
0.97 (0.93-1.01)
1.00 (0.98-1.02)
0.60 (0.23-1.61)
OR (95% CI)
Unsupervised Principal Component Analysis for Airway
Physiologic Parameters
Factors
Correlation Matrix 1 2 3
P Value
BWT (R2 5 0.14)
.97
.57
.10
.91
.32
FEV1/FVC, % 20.49 0.60
Table 4Logistic Regression for the Presence of EM, BE, and BWT (Dependent Variables) and the Listed Independent Variables
FEV1 % predicted 20.35 0.44 0.74
VC, % 0.94
Wald Test FRC, % 0.89 20.40
, 0.01
0.32
2.67
0.01
0.99
RV, % 0.85
TLC, % 0.90
Dlco, % 0.93
, 0.01 (0.02)
20.33 (0.58)
20.03 (0.02)
, 0.01 (0.01)
20.49 (0.49)
Dlco/Va, % 0.95
B (SE)
FRC 5 functional residual capacity; TLC 5 total lung capacity;
VC 5 vital capacity. See Table 3 for expansion of other abbreviations.
evidence of a lack of correlation between sputum
0.97 (0.93-1.02)
0.39 (0.11-1.42)
1.02 (0.99-1.05)
1.00 (0.98-1.02)
1.63 (0.55-4.84)
OR (95% CI)
neutrophils and EM score in patients with COPD,15,41
and outlines the radiologic complement to pheno-
typing COPD. The evidence of eosinophilic airway
inammation and CT imaging in patients with COPD
has been conicting.40,42 However, these differences
B 5 unstandardized coefcients; R 5 NagelKerke R squared. See Table 2 and 3 legends for expansion of other abbreviations.
P Value
BE (R2 5 0.14)
could be accounted for by differences in study design.
.21
.15
.26
.70
.38
Interestingly, Miller and colleagues42 found close
correlations between eosinophil degradation prod-
Wald Test
ucts and EM score in a group of well-characterized
1.62
0.79
2.04
1.76
0.15
patients with COPD, suggesting that these may con-
tribute to the progression of EM.
In this study, we have shown that FEV1 using
20.03 (0.02)
20.95 (0.66)
0.02 (0.02)
20.01 (0.01)
0.49 (0.56)
B (SE)
regression model analysis was not predictive for the
identication of EM, BE, or BWT on CT scan. This
further illustrates the reduced accuracy of FEV1 in
identifying the key pathologic processes of COPD.
0.98 (0.93-1.03)
0.72 (0.14-3.77)
0.94 (0.89-0.99)
1.04 (1.00-1.08)
0.18 (0.03-1.00)
OR (95% CI)
On the other hand, CT scan COPD phenotype
identication has been associated with key clinical
outcomes, including bronchodilator reversibility,39,43
effect of airow obstruction,11 and severity of COPD
exacerbations.44 We also concluded that the use of
P Value
EM (R2 5 0.68)
conventional lung function testing alone was unable
.41
.70
.02
.04
.05
to delineate between patients with EM alone and
those with EM plus phenotypes.
Wald Test
Using cluster analysis, an unbiased statistical
0.69
0.15
5.63
4.46
3.57
approach investigating airway physiologic pattern
expression, we identied three clusters that were
largely clinically indistinguishable in the expression
20.22 (0.03)
20.33 (0.84)
20.06 (0.03)
0.04 (0.02)
21.71 (0.87)
B (SE)
of airway inammation, bacterial load, and quality-
of-life scores. These clusters identied two emphyse-
2
matous groups discrete by the degree and severity of
hyperination and gas exchange, and a third group that
Multivariate Modeling for
Total sputum neutrophils
was heterogeneous. Although largely useful, physiology
Detection of Radiologic
3 106 cells/g sputum
Sputum eosinophils, %
Dlco/Va % predicted
alone could not clearly and robustly identify the patho-
FEV1 % predicted
logic processes seen in COPD. The application of
RV % predicted
CT imaging provided additional clinically important
Phenotypes
information as a noninvasive biomarker in COPD.20
One limitation of this study is that we used qualita-
tive and not quantitative classication of EM, BE, and
www.chestpubs.org CHEST / 140 / 3 / SEPTEMBER, 2011 639
Downloaded from chestjournal.chestpubs.org by Kimberly Henricks on September 7, 2011
2011 AmericanatCollege
Downloaded for dr. Avit Suchitra 100 (avitsuchitra@fk.unand.ac.id) ClinicalKeyofGlobal
Chest Physicians
Guest Users from ClinicalKey.com by Elsevier on July 22, 2017.
For personal use only. No other uses without permission. Copyright 2017. Elsevier Inc. All rights reserved.
Table 6Demographic and Clinical Characteristics of Physiologic Clusters in COPD
Cluster 1 (EM-Predominant, Cluster 2 (Heterogeneous, Cluster 3 (EM-Predominant,
Moderate Lung Function Lung Function Preserved Severe Lung Function
Characteristic [n 5 30]) [n 5 20]) [n 5 14]) P Value
Male, No. (%) 23 (77) 17 (85) 12 (86) .68
Age, y, mean (range) 68 70 64 .23
Pack-y smoked, mean (range) 63 32 44 , .01
Exacerbation history in previous y 4.3 (0.5) 3.3 (0.6) 4.6 (0.6) .25
BMI, kg/m2 24.6 (0.8) 28.8 (1.2) 24.9 (1.3) .01
Sputum total cell count 3 106 cells/g, 4.2 (3.3-6.8) 4.7 (3.6-8.0) 3.4 (2.1-8.6) .79
geometric mean (95% CI)
Sputum neutrophils, % 68 (5) 68 (5) 73 (6) .77
Sputum eosinophils, %, 1.6 (1.2-2.9) 0.8 (0.6-1.4) 2.0 (1.3-4.5) .17
geometric mean (95% CI)
Potential pathogenic organism, % (95% CI) 41 (23-61) 11 (2-34) 20 (5-52) .09
Absolute neutrophil count 3 106 cells/g, 2.8 (2.0-5.0) 3.0 (2.2-5.8) 2.3 (1.4-6.6) .91
geometric mean (95% CI)
Total bacterial load (16S), 2.68 (1.68-6.68) 1.48 (7.97-4.28) 6.87 (3.67-2.48) .30
geometric mean (95% CI)
Colony-forming units, 7.25 (4.55-1.88) 1.56 (9.45-3.66) 2.96 (1.76-8.26) .17
geometric mean (95% CI)
FEV1 % predicteda 45 (4) 62 (3) 27 (3) , .01
FEV1/FVC,a % 45 (2) 58 (3) 35 (2) , .01
Reversibility, % 4 (2) 5 (3) 23 (4) .12
RV, % 143 (3) 88 (6) 194 (11) , .01
TLC, % 110 (4) 85 (5) 124 (4) , .01
Dlco/Va % predicted 63 (4) 90 (6) 42 (4) , .01
SGRQ total, units 54 (3) 53 (5) 57 (4) .79
CRQ total, units 3.8 (0.2) 4.3 (0.3) 4.3 (0.3) .30
VAS total, units 154 (13) 164 (16) 102 (18) .03
VAS dyspnea, mm 53 (4) 44 (6) 38 (8) .13
VAS cough, mm 41 (5) 45 (6) 25 (8) .12
VAS sputum production, mm 35 (4) 38 (7) 28 (8) .53
VAS sputum purulence, mm 25 (4) 39 (6) 11 (3) , .01
EM, % (95% CI) 80 (62-91) 25 (11-47) 93 (66-100) , .01
BE, % (95% CI) 23 (12-41) 35 (18-57) 21 (7-48) .58
BWT, % (95% CI) 37 (22-55) 5 (0-25) 29 (11-55) .04
Data are presented as mean (SEM) unless otherwise indicated. See Table 1, 2, 3, and 5 legends for expansion of abbreviations.
aPostbronchodilator.
BWT. Although this qualitative description of EM, BE, val between characterization and CT scanning had
and BWT introduces bias into a study such as this a median of 15 months and may have affected the
one, we aimed to reduce this by showing substantial stability of the physiologic phenotype. We found in a
agreement between two observers in using this form large cohort of subjects with COPD that parameters of
of radiologic description.36 Future studies that use spirometry (namely, FEV1 and FVC) were unchanged
similar unbiased statistical approaches combining mul- 12 months after characterization, and that measures
tiple dimensions of airway inammation, physiology, of detailed lung function were also repeatable in this
and structure determined by quantitative densitom- cohort. This further conrms our nding that the
etry and geometry are required. The study investigated use of physiology that is repeatable can identify an
patients who were concurrently enrolled in a longitu- EM phenotype, whereas imaging is required to iden-
dinal biomarkers in COPD exacerbation study. This tify BE and BWT in COPD. Whether the presence of
may have introduced selection bias in the physiologic radiologic BE and BWT in COPD alters the clini-
analysis because the indication for CT scan was pri- cal prognosis, management, and therapeutic response
marily for clinical purposes, namely malignancy, BE, needs to be examined further in larger clinical stud-
and lung volume reduction surgery. However, as com- ies with specic phenotypic strategies of trial design.
monly found in clinical practice, the group with COPD
was likely to have measures of lung function with Conclusions
imaging in a selected group only; our study thus
highlights that lung function tools alone do not In conclusion, COPD is a heterogeneous disease
clearly identify important pathologic processes that currently diagnosed and classied according to spirom-
may subsequently alter management. The time inter- etry. The application of radiologic imaging can be a
640 Original Research
Downloaded from chestjournal.chestpubs.org by Kimberly Henricks on September 7, 2011
2011 AmericanatCollege
Downloaded for dr. Avit Suchitra 100 (avitsuchitra@fk.unand.ac.id) ClinicalKeyofGlobal
Chest Physicians
Guest Users from ClinicalKey.com by Elsevier on July 22, 2017.
For personal use only. No other uses without permission. Copyright 2017. Elsevier Inc. All rights reserved.
useful tool in further phenotyping patients with chronic obstructive bronchitis. Am J Respir Crit Care Med.
COPD where clinical markers of airway inamma- 1998;158(5 Pt 1):1511-1517.
5. Brightling CE, McKenna S, Hargadon B, et al. Sputum
tion and health status are indistinguishable, and where eosinophilia and the short term response to inhaled mometa-
static or dynamic lung function tests provide some, sone in chronic obstructive pulmonary disease. Thorax. 2005;
but not all, clarication. 60(3):193-198.
6. Papi A, Luppi F, Franco F, Fabbri LM. Pathophysiology
of exacerbations of chronic obstructive pulmonary disease.
Acknowledgments Proc Am Thorac Soc. 2006;3(3):245-251.
7. Bathoorn E, Kerstjens H, Postma D, Timens W, MacNee W.
Author contributions: All authors approved the nal version of
the manuscript. Airways inammation and treatment during acute exacer-
Dr Bafadhel: contributed to the design of the study, data collec- bations of COPD. Int J Chron Obstruct Pulmon Dis. 2008;
tion, data analysis, and writing of the manuscript, and can vouch 3(2):217-229.
for the integrity of the data analysis. 8. Jeffery PK. Structural and inammatory changes in COPD:
Mr Umar: contributed to the data collection and writing of the a comparison with asthma. Thorax. 1998;53(2):129-136.
manuscript. 9. Han MK, Agusti A, Calverley PM, et al. Chronic obstructive
Dr Gupta: contributed to the data collection and writing of the lung disease phenotypes: the future of COPD. Am J Respir
manuscript.
Crit Care Med. 2010;182(5):598-604.
Dr Raj: contributed to the data collection and writing of the
manuscript. 10. Nakano Y, Muro S, Sakai H, et al. Computed tomographic
Mr Vara: contributed to the data collection and writing of the measurements of airway dimensions and emphysema in
manuscript. smokers. Correlation with lung function. Am J Respir Crit
Dr Entwisle: contributed to the data collection and writing of the Care Med. 2000;162(3 Pt 1):1102-1108.
manuscript. 11. Patel BD, Coxson HO, Pillai SG, et al; International COPD
Dr Pavord: contributed to the design of the study, data analysis, Genetics Network. Airway wall thickening and emphysema
and writing of the manuscript. show independent familial aggregation in chronic obstructive
Dr Brightling: contributed to the design of the study, data collec-
tion, data analysis, and writing of the manuscript, and can vouch pulmonary disease. Am J Respir Crit Care Med. 2008;178(5):
for the integrity of the data analysis. 500-505.
Dr Siddiqui: contributed to the design of the study, data analysis, 12. Hasegawa M, Nasuhara Y, Onodera Y, et al. Airow limi-
and writing of the manuscript. tation and airway dimensions in chronic obstructive pul-
Financial/nonnancial disclosures: The authors have reported monary disease. Am J Respir Crit Care Med. 2006;173(12):
to CHEST the following conicts of interest: Dr Pavord has 1309-1315.
received consultancy fees from AstraZeneca, GlaxoSmithKline, 13. Kinsella M, Mller NL, Abboud RT, Morrison NJ, DyBuncio A.
and Novartis. Dr Brightling has received consultancy fees from Quantitation of emphysema by computed tomography using
Medimmune, AstraZeneca, GlaxoSmithKline, and Roche, and has
received research grants from AstraZeneca, Medimmune, and a density mask program and correlation with pulmonary
GlaxoSmithKline. Dr Siddiqui has received pharmaceutic grant function tests. Chest. 1990;97(2):315-321.
monies and has participated in speaking activities for Merck, Sharp, 14. Yuan R, Hogg JC, Par PD, et al. Prediction of the rate of
and Dome. Drs Bafadhel, Gupta, Raj, Entwisle and Messrs Umar decline in FEV(1) in smokers using quantitative computed
and Vara have reported that no potential conicts of interest tomography. Thorax. 2009;64(11):944-949.
exist with any companies/organizations whose products or ser- 15. ODonnell RA, Peebles C, Ward JA, et al. Relationship
vices may be discussed in this article. between peripheral airway dysfunction, airway obstruction,
Role of sponsors: The sponsors had no role in the writing or
and neutrophilic inammation in COPD. Thorax. 2004;
analysis of the manuscript.
Other contributions: The authors thank all the patients who 59(10):837-842.
took part in the study and acknowledge the following persons 16. Han MK, Bartholmai B, Liu LX, et al. Clinical signicance
for their assistance in patient characterization, laboratory support, of radiologic characterizations in COPD. COPD. 2009;6(6):
and microbiology facilitation: S. Terry, BSc; S. McKenna, RGN; 459-467.
V. Mistry, BSc; M. Pancholi, BSc; C. Reid, BSc; A. Singapuri, BSc; 17. Ogawa E, Nakano Y, Ohara T, et al. Body mass index in male
K. Haldar, MSc; H. Patel, BSc; B. Hargadon, RGN; M. Shelley, RGN; patients with COPD: correlation with low attenuation areas
M. Bourne, RGN; and M. R. Barer, PhD. on CT. Thorax. 2009;64(1):20-25.
18. Camp PG, Coxson HO, Levy RD, et al. Sex differences in
emphysema and airway disease in smokers. Chest. 2009;
References 136(6):1480-1488.
1. Rabe KF, Hurd S, Anzueto A, et al; Global Initiative for 19. Bon JM, Leader JK, Weissfeld JL, et al. The inuence of
Chronic Obstructive Lung Disease. Global strategy for the radiographic phenotype and smoking status on peripheral
diagnosis, management, and prevention of chronic obstructive blood biomarker patterns in chronic obstructive pulmonary
pulmonary disease: GOLD executive summary. Am J Respir disease. PLoS ONE. 2009;4(8):e6865.
Crit Care Med. 2007;176(6):532-555. 20. Coxson HO. Quantitative computed tomography assess-
2. Keatings VM, Collins PD, Scott DM, Barnes PJ. Differences in ment of airway wall dimensions: current status and potential
interleukin-8 and tumor necrosis factor-alpha in induced spu- applications for phenotyping chronic obstructive pulmonary
tum from patients with chronic obstructive pulmonary disease disease. Proc Am Thorac Soc. 2008;5(9):940-945.
or asthma. Am J Respir Crit Care Med. 1996;153(2):530-534. 21. Coxson HO, Lam S. Quantitative assessment of the airway wall
3. Ronchi MC, Piragino C, Rosi E, Amendola M, Duranti R, using computed tomography and optical coherence tomogra-
Scano G. Role of sputum differential cell count in detect- phy. Proc Am Thorac Soc. 2009;6(5):439-443.
ing airway inammation in patients with chronic bronchial 22. Brusasco V, Crapo R, Viegi G; American Thoracic Society;
asthma or COPD. Thorax. 1996;51(10):1000-1004. European Respiratory Society. Coming together: the ATS/ERS
4. Pizzichini E, Pizzichini MM, Gibson P, et al. Sputum eosino- consensus on clinical pulmonary function testing. Eur Respir J.
philia predicts benet from prednisone in smokers with 2005;26(1):1-2.
www.chestpubs.org CHEST / 140 / 3 / SEPTEMBER, 2011 641
Downloaded from chestjournal.chestpubs.org by Kimberly Henricks on September 7, 2011
2011 AmericanatCollege
Downloaded for dr. Avit Suchitra 100 (avitsuchitra@fk.unand.ac.id) ClinicalKeyofGlobal
Chest Physicians
Guest Users from ClinicalKey.com by Elsevier on July 22, 2017.
For personal use only. No other uses without permission. Copyright 2017. Elsevier Inc. All rights reserved.
23. Miller MR, Crapo R, Hankinson J, et al; ATS/ERS Task 35. Hansell DM, Bankier AA, MacMahon H, McLoud TC,
Force. General considerations for lung function testing. Mller NL, Remy J. Fleischner Society: glossary of terms
Eur Respir J. 2005;26(1):153-161. for thoracic imaging. Radiology. 2008;246(3):697-722.
24. Miller MR, Hankinson J, Brusasco V, et al; ATS/ERS Task 36. Gupta S, Siddiqui S, Haldar P, et al. Qualitative analysis
Force. Standardisation of spirometry. Eur Respir J. 2005; of high-resolution CT scans in severe asthma. Chest. 2009;
26(2):319-338. 136(6):1521-1528.
25. Pellegrino R, Viegi G, Brusasco V, et al. Interpretative strategies 37. Moss M, Wellman DA, Cotsonis GA. An appraisal of mul-
for lung function tests. Eur Respir J. 2005;26(5):948-968. tivariable logistic models in the pulmonary and critical care
26. Wanger J, Clausen JL, Coates A, et al. Standardisation of the literature. Chest. 2003;123(3):923-928.
measurement of lung volumes. Eur Respir J. 2005;26(3):511-522. 38. OBrien C, Guest PJ, Hill SL, Stockley RA. Physiological
27. Jones PW, Quirk FH, Baveystock CM, Littlejohns P. A self- and radiological characterisation of patients diagnosed with
complete measure of health status for chronic airow limi- chronic obstructive pulmonary disease in primary care. Thorax.
tation. The St. Georges Respiratory Questionnaire. Am Rev 2000;55(8):635-642.
Respir Dis. 1992;145(6):1321-1327. 39. Fujimoto K, Kitaguchi Y, Kubo K, Honda T. Clinical analysis
28. Guyatt G. Measuring health status in chronic airow limita- of chronic obstructive pulmonary disease phenotypes classi-
tion. Eur Respir J. 1988;1(6):560-564. ed using high-resolution computed tomography. Respirology.
29. Brightling CE, Monterio W, Green RH, et al. Induced 2006;11(6):731-740.
sputum and other outcome measures in chronic obstructive 40. Kitaguchi Y, Fujimoto K, Kubo K, Honda T. Characteristics
pulmonary disease: safety and repeatability. Respir Med. of COPD phenotypes classied according to the ndings of
2001;95(12):999-1002. HRCT. Respir Med. 2006;100(10):1742-1752.
30. Bailey KV, Ferro-Luzzi A. Use of body mass index of adults 41. Simpson JL, Milne DG, Gibson PG. Neutrophilic asthma
in assessing individual and community nutritional status. has different radiographic features to COPD and smokers.
Bull World Health Organ. 1995;73(5):673-680. Respir Med. 2009;103(6):881-887.
31. Health Protection Agency. Investigation of bronchoalveolar 42. Miller M, Ramsdell J, Friedman PJ, Cho JY, Renvall M,
lavage, sputum and associated specimens. BSOP 57. 2009:3. Broide DH. Computed tomographic scan-diagnosed chronic
32. Pye A, Stockley RA, Hill SL. Simple method for quantify- obstructive pulmonary disease-emphysema: eotaxin-1 is associ-
ing viable bacterial numbers in sputum. J Clin Pathol. 1995; ated with bronchodilator response and extent of emphysema.
48(8):719-724. J Allergy Clin Immunol. 2007;120(5):1118-1125.
33. Pizzichini E, Pizzichini MM, Efthimiadis A, et al. Indices of 43. Kurashima K, Takayanagi N, Sato N, et al. High resolution
airway inammation in induced sputum: reproducibility and CT and bronchial reversibility test for diagnosing COPD.
validity of cell and uid-phase measurements. Am J Respir Respirology. 2005;10(3):316-322.
Crit Care Med. 1996;154(2 Pt 1):308-317. 44. Patel IS, Vlahos I, Wilkinson TM, et al. Bronchiectasis,
34. Pizzichini MM, Popov TA, Efthimiadis A, et al. Spontaneous and exacerbation indices, and inammation in chronic obstruc-
induced sputum to measure indices of airway inammation in tive pulmonary disease. Am J Respir Crit Care Med. 2004;
asthma. Am J Respir Crit Care Med. 1996;154(4 Pt 1):866-869. 170(4):400-407.
642 Original Research
Downloaded from chestjournal.chestpubs.org by Kimberly Henricks on September 7, 2011
2011 AmericanatCollege
Downloaded for dr. Avit Suchitra 100 (avitsuchitra@fk.unand.ac.id) ClinicalKeyofGlobal
Chest Physicians
Guest Users from ClinicalKey.com by Elsevier on July 22, 2017.
For personal use only. No other uses without permission. Copyright 2017. Elsevier Inc. All rights reserved.
S-ar putea să vă placă și
- A Study of Prolonged FastingDocument438 paginiA Study of Prolonged FastingjuanojedamenaÎncă nu există evaluări
- Cat Anatomy and PhysiologyDocument44 paginiCat Anatomy and PhysiologyJovana Stankovic Popovic100% (3)
- Assessment of The Critically Ill Patients and Their FamiliesDocument48 paginiAssessment of The Critically Ill Patients and Their Familiesjhing_apdan100% (1)
- Drugs Acting On Respiratory SystemDocument52 paginiDrugs Acting On Respiratory SystemIrwan M. Iskober100% (4)
- Chapter 27 Acute Lung Injury, Pulmonary Edema and Multi Organ System FailureDocument10 paginiChapter 27 Acute Lung Injury, Pulmonary Edema and Multi Organ System FailureShanin SalapuddinÎncă nu există evaluări
- Oxygen Therapy For HODocument55 paginiOxygen Therapy For HOansuh22Încă nu există evaluări
- Experiment 4 Rat RespiratoryDocument5 paginiExperiment 4 Rat RespiratoryMuhammad Safwan100% (3)
- Administration of OxygenDocument52 paginiAdministration of OxygenSivabarathy50% (2)
- ERS Handbook-Self-Assessment in Respiratory Medicine, 2e (Sep 1, 2015) - (1849840784) - (European Respiratory Society) .PDF (Konrad E. Bloch, Thomas Brack, Anita K. Simonds)Document560 paginiERS Handbook-Self-Assessment in Respiratory Medicine, 2e (Sep 1, 2015) - (1849840784) - (European Respiratory Society) .PDF (Konrad E. Bloch, Thomas Brack, Anita K. Simonds)Shop Upmed100% (1)
- RPH Biologi TG4Document28 paginiRPH Biologi TG4lilyraj100% (1)
- Acute Respiratory Failure For StudentDocument41 paginiAcute Respiratory Failure For Studentapi-379952350% (4)
- The Accuracy of Ultrasound-Guided Lung Biopsy Pathology andDocument8 paginiThe Accuracy of Ultrasound-Guided Lung Biopsy Pathology andHeru SigitÎncă nu există evaluări
- Exhaled Breath Analysis For Lung CancerDocument12 paginiExhaled Breath Analysis For Lung CancerIkaPKÎncă nu există evaluări
- Diffusing Capacity of Carbon Monoxide in Assessment of COPD: Original ResearchDocument9 paginiDiffusing Capacity of Carbon Monoxide in Assessment of COPD: Original ResearchKlinikdr RIDHAÎncă nu există evaluări
- Case Report Displasia BronkopulmonerDocument5 paginiCase Report Displasia BronkopulmonerVivi DeviyanaÎncă nu există evaluări
- Proteome Profiling of Lung Tissues in ChronicDocument8 paginiProteome Profiling of Lung Tissues in ChronicAndreea MoalesÎncă nu există evaluări
- Aspergillus Fumigatus During COPD Exacerbation: A Pair-Matched Retrospective StudyDocument8 paginiAspergillus Fumigatus During COPD Exacerbation: A Pair-Matched Retrospective StudyJames 'jps' SimanjuntakÎncă nu există evaluări
- Qin 2010Document8 paginiQin 2010jajajaneinÎncă nu există evaluări
- Chest X Ray in CAPDocument7 paginiChest X Ray in CAPsahatmanurungÎncă nu există evaluări
- The Value of Chest Ultrasonography Applications in The Respiratory ICUDocument6 paginiThe Value of Chest Ultrasonography Applications in The Respiratory ICUHeru SigitÎncă nu există evaluări
- Predicting Lung Nodules MalignancyDocument7 paginiPredicting Lung Nodules MalignancyhajajÎncă nu există evaluări
- Lood Eosinophil Percentage As A Predictor of Response Toinhaled Corticosteroid in BronchiectasisDocument8 paginiLood Eosinophil Percentage As A Predictor of Response Toinhaled Corticosteroid in BronchiectasiskarlosÎncă nu există evaluări
- ENG JCOPDF-2019-0128-StringerDocument11 paginiENG JCOPDF-2019-0128-Stringerulfiandi rizkiÎncă nu există evaluări
- Cigarette Smoke Promotes Dendritic Cell Accumulation in COPD A Lung Tissue Research Consortium StudyDocument13 paginiCigarette Smoke Promotes Dendritic Cell Accumulation in COPD A Lung Tissue Research Consortium StudyArry SetyowatiÎncă nu există evaluări
- Emphysema Versus Chronic Bronchitis in COPD: Clinical and Radiologic CharacteristicsDocument8 paginiEmphysema Versus Chronic Bronchitis in COPD: Clinical and Radiologic CharacteristicsChairul Nurdin AzaliÎncă nu există evaluări
- Thoracic Imaging: Think Tank ReviewDocument8 paginiThoracic Imaging: Think Tank ReviewmenafabÎncă nu există evaluări
- Low 2018Document9 paginiLow 2018Hendri WahyudiÎncă nu există evaluări
- Tuberculosis Mimicking Lung CancerDocument3 paginiTuberculosis Mimicking Lung CancerdyahÎncă nu există evaluări
- Kuo2017 Article DiagnosisOfBronchiectasisAndAiDocument10 paginiKuo2017 Article DiagnosisOfBronchiectasisAndAipunct_org3256Încă nu există evaluări
- Identification and Characterization of Human Pulmonary Dendritic CellsDocument8 paginiIdentification and Characterization of Human Pulmonary Dendritic CellsMostafa MagarÎncă nu există evaluări
- Evaluation of Retrieval Accuracy and Visual Similarity in Contentbased Image Retrieval of Chest CT For Obstructive Lung Diseasescientific ReportsDocument11 paginiEvaluation of Retrieval Accuracy and Visual Similarity in Contentbased Image Retrieval of Chest CT For Obstructive Lung Diseasescientific ReportsAshwini AminÎncă nu există evaluări
- CopdDocument7 paginiCopdMelinda Anzani PutriÎncă nu există evaluări
- Vol Pulmon Art AcDocument7 paginiVol Pulmon Art AcdanielÎncă nu există evaluări
- Bronchiectasis in nonCF in ChildrenDocument9 paginiBronchiectasis in nonCF in ChildrenathaÎncă nu există evaluări
- 2015 Article 91Document7 pagini2015 Article 91Karel ZertucheÎncă nu există evaluări
- AMJ-Volume 50-Issue 2 - Page 1489-1496Document8 paginiAMJ-Volume 50-Issue 2 - Page 1489-1496Pandu Putra Wijaya RestaÎncă nu există evaluări
- Lust StudyDocument7 paginiLust Studyadrianoneto60Încă nu există evaluări
- From Pre-COPD To COPD - A Simple, Low Cost and Easy To IMplement (SLIM) Risk CalculatorDocument12 paginiFrom Pre-COPD To COPD - A Simple, Low Cost and Easy To IMplement (SLIM) Risk CalculatorLorena ZirondiÎncă nu există evaluări
- Tanimura Et Al 2016 Quantitative Assessment of Erector Spinae Muscles in Patients With Chronic Obstructive PulmonaryDocument8 paginiTanimura Et Al 2016 Quantitative Assessment of Erector Spinae Muscles in Patients With Chronic Obstructive Pulmonarysasan.zamani.sasanÎncă nu există evaluări
- CT Scanning-Based Phenotypes Vary With ADRB2 Polymorphisms in Chronic Obstructive Pulmonary DiseaseDocument6 paginiCT Scanning-Based Phenotypes Vary With ADRB2 Polymorphisms in Chronic Obstructive Pulmonary DiseaseAtika Indah SariÎncă nu există evaluări
- Reversed Halo Sign in Active Pulmonary Tuberculosis: Criteria For Differentiation From Cryptogenic Organizing PneumoniaDocument4 paginiReversed Halo Sign in Active Pulmonary Tuberculosis: Criteria For Differentiation From Cryptogenic Organizing PneumoniaElza Astri SafitriÎncă nu există evaluări
- HRCT Computed Score in Usual InterstitiaDocument8 paginiHRCT Computed Score in Usual InterstitiaClaudio Rafael Salazar MÎncă nu există evaluări
- Global Burden of COPD: Systematic Review and Meta-AnalysisDocument10 paginiGlobal Burden of COPD: Systematic Review and Meta-AnalysisastreedewiÎncă nu există evaluări
- Central Airway TumorDocument9 paginiCentral Airway TumorYanuar AbdulhayÎncă nu există evaluări
- Clinical, Radiological, and Pathological Investigation of AsbestosisDocument14 paginiClinical, Radiological, and Pathological Investigation of Asbestosisintan danayantiÎncă nu există evaluări
- Clinical Features of TAC Phenotypes of COPD. Int J of COPD 2019Document10 paginiClinical Features of TAC Phenotypes of COPD. Int J of COPD 2019Claudio Rafael Salazar MÎncă nu există evaluări
- Asthma: Further ReadingDocument13 paginiAsthma: Further ReadingcarlosÎncă nu există evaluări
- 360 713 1 SMDocument8 pagini360 713 1 SMadityachupezÎncă nu există evaluări
- Neuhaus Et Al. 2017 - PCLS Cultivados Por Longos PeríodosDocument8 paginiNeuhaus Et Al. 2017 - PCLS Cultivados Por Longos PeríodosIgor OliveiraÎncă nu există evaluări
- MakananDocument8 paginiMakananAnonymous VXZymiÎncă nu există evaluări
- Pul InfectionsDocument5 paginiPul InfectionsSameer VermaÎncă nu există evaluări
- Adenosquamous Carcinomaof The Lung: Two Cases ReportDocument5 paginiAdenosquamous Carcinomaof The Lung: Two Cases ReportIJAR JOURNALÎncă nu există evaluări
- State of The Art IPDocument13 paginiState of The Art IPSam SamiÎncă nu există evaluări
- Radiol 2018172688Document10 paginiRadiol 2018172688Nurul Rahmadiani UkfahÎncă nu există evaluări
- Teknik Acbt Untuk Kasus BronkhiektasisDocument9 paginiTeknik Acbt Untuk Kasus Bronkhiektasisfister19 rifaudinÎncă nu există evaluări
- Radiologic Manifestations of Pulmonary Tuberculosis in Patients of Intensive Care UnitsDocument6 paginiRadiologic Manifestations of Pulmonary Tuberculosis in Patients of Intensive Care UnitsAnonymous qwH3D0KrpÎncă nu există evaluări
- Lung Ultrasound Vs CTDocument9 paginiLung Ultrasound Vs CTValentinaNiñoÎncă nu există evaluări
- Cytological Analysis of Bronchial Washings in RSUD Pasar MingguDocument8 paginiCytological Analysis of Bronchial Washings in RSUD Pasar MingguReza DigambiroÎncă nu există evaluări
- A 56 Year Old Woman With Multiple Pulmonary CystsDocument8 paginiA 56 Year Old Woman With Multiple Pulmonary CystsAchmad Dodi MeidiantoÎncă nu există evaluări
- THT JURNALDocument6 paginiTHT JURNALNia IfrianaÎncă nu există evaluări
- Impact of InflamationDocument9 paginiImpact of InflamationMilutin MelkaÎncă nu există evaluări
- The Positive Result of Cytology Brushing at Flexible Fiberoptic Bronchoscopy Compared With Transthoracic Needle Aspiration in Central Lung TumorDocument10 paginiThe Positive Result of Cytology Brushing at Flexible Fiberoptic Bronchoscopy Compared With Transthoracic Needle Aspiration in Central Lung TumorKezzia Putri WazaneÎncă nu există evaluări
- 1 s2.0 S0010865013001276 MainDocument5 pagini1 s2.0 S0010865013001276 MainliyaÎncă nu există evaluări
- Role of Chest Computed Tomography in Evaluation and Management of Chronic Obstructive Pulmonary DiseaseDocument10 paginiRole of Chest Computed Tomography in Evaluation and Management of Chronic Obstructive Pulmonary DiseaseIJAR JOURNALÎncă nu există evaluări
- Actinomyces Pulmonar 2013Document8 paginiActinomyces Pulmonar 2013Elizabeth SantillanÎncă nu există evaluări
- Stem Cell-Based Therapy for Lung DiseaseDe la EverandStem Cell-Based Therapy for Lung DiseaseJanette K. BurgessÎncă nu există evaluări
- Uso de Ultrassonografia Nos Probelmas Respiratórios de BovinosDocument17 paginiUso de Ultrassonografia Nos Probelmas Respiratórios de BovinosVitor BarbosaÎncă nu există evaluări
- Case 1: Recurrent Pneumonia in A 15-Year-Old Girl: Article Figures & Data Info & Metrics CommentsDocument7 paginiCase 1: Recurrent Pneumonia in A 15-Year-Old Girl: Article Figures & Data Info & Metrics CommentsJoshua MendozaÎncă nu există evaluări
- BJR 85 897 PDFDocument8 paginiBJR 85 897 PDFRila NurulÎncă nu există evaluări
- Jurnal BiomedikDocument10 paginiJurnal BiomedikneaÎncă nu există evaluări
- Pulmonary Functional Imaging: Basics and Clinical ApplicationsDe la EverandPulmonary Functional Imaging: Basics and Clinical ApplicationsYoshiharu OhnoÎncă nu există evaluări
- Etg MeningitisDocument1 paginăEtg MeningitisAtika Indah SariÎncă nu există evaluări
- Primary Care of The Patient With Chronic Obstructive Pulmonary Disease in ItalyDocument7 paginiPrimary Care of The Patient With Chronic Obstructive Pulmonary Disease in ItalyAtika Indah SariÎncă nu există evaluări
- DM Dan GD PDFDocument9 paginiDM Dan GD PDFrizky ananda prawira marpaungÎncă nu există evaluări
- Form Data KosongDocument1 paginăForm Data KosongRizky Bagus PÎncă nu există evaluări
- Primary Care of The Patient With Chronic Obstructive Pulmonary Disease in ItalyDocument7 paginiPrimary Care of The Patient With Chronic Obstructive Pulmonary Disease in ItalyAtika Indah SariÎncă nu există evaluări
- CT Scanning-Based Phenotypes Vary With ADRB2 Polymorphisms in Chronic Obstructive Pulmonary DiseaseDocument6 paginiCT Scanning-Based Phenotypes Vary With ADRB2 Polymorphisms in Chronic Obstructive Pulmonary DiseaseAtika Indah SariÎncă nu există evaluări
- Chronic Obstructive Pulmonary Disease-Radiology-Pathology Correlation PDFDocument10 paginiChronic Obstructive Pulmonary Disease-Radiology-Pathology Correlation PDFAtika Indah SariÎncă nu există evaluări
- Chronic Obstructive Pulmonary Disease-Radiology-Pathology CorrelationDocument4 paginiChronic Obstructive Pulmonary Disease-Radiology-Pathology CorrelationAtika Indah SariÎncă nu există evaluări
- DownloadDocument26 paginiDownloadAtika Indah SariÎncă nu există evaluări
- Jurnal NeuroDocument8 paginiJurnal NeuroAtika Indah SariÎncă nu există evaluări
- GINA Pocket 2015Document32 paginiGINA Pocket 2015Ramzi AkramÎncă nu există evaluări
- Nelson 2016Document8 paginiNelson 2016Atika Indah SariÎncă nu există evaluări
- Pre Peri Neonatal ASD Risk Factors 2012 PDFDocument14 paginiPre Peri Neonatal ASD Risk Factors 2012 PDFAtika Indah SariÎncă nu există evaluări
- Blanco 2016Document7 paginiBlanco 2016Atika Indah SariÎncă nu există evaluări
- Jurnal Disfungsi Kognitif Pada Depresi MayorDocument6 paginiJurnal Disfungsi Kognitif Pada Depresi MayorAtika Indah SariÎncă nu există evaluări
- Jurnal PDFDocument6 paginiJurnal PDFAtika Indah SariÎncă nu există evaluări
- Creamer Et Al-2016-British Journal of DermatologyDocument34 paginiCreamer Et Al-2016-British Journal of DermatologyAtika Indah SariÎncă nu există evaluări
- Science 9 W AnswerDocument62 paginiScience 9 W AnswerAstrande KevinÎncă nu există evaluări
- 3rd Summative Test For Grade 6 Set BDocument20 pagini3rd Summative Test For Grade 6 Set BRhea Mae Saquibal GalleneroÎncă nu există evaluări
- Bronchiectasis PathophysiologyDocument1 paginăBronchiectasis PathophysiologyRayne Dunstan Pascual VergaraÎncă nu există evaluări
- Applied Technologies in Pulmonary Medicine (PDFDrive)Document271 paginiApplied Technologies in Pulmonary Medicine (PDFDrive)Богдана ВацебаÎncă nu există evaluări
- Intra-Operative PEEP Vs ZEEPDocument37 paginiIntra-Operative PEEP Vs ZEEPMohamed RifanÎncă nu există evaluări
- Anatomy of Nose: Dr. Ra. Shivaraman Postgraduate in Plastic Surgery Govt. Kilpauk Medical CollegeDocument48 paginiAnatomy of Nose: Dr. Ra. Shivaraman Postgraduate in Plastic Surgery Govt. Kilpauk Medical CollegeShivaramanRamachandranÎncă nu există evaluări
- Craven & Hirnle's Nursing Procedures and Fundamentals OnlineDocument4 paginiCraven & Hirnle's Nursing Procedures and Fundamentals Onlineisapatrick8126Încă nu există evaluări
- Material Safety Data Sheet: Saf-Sol Section I - General InformationDocument6 paginiMaterial Safety Data Sheet: Saf-Sol Section I - General InformationmathpowerguidoÎncă nu există evaluări
- DiBlasi Webinar2Document88 paginiDiBlasi Webinar2zomweÎncă nu există evaluări
- Anatomi Dan Fisiologi RespirasiDocument22 paginiAnatomi Dan Fisiologi RespirasinortonaingÎncă nu există evaluări
- PathophysiologyDocument3 paginiPathophysiologycpccoderÎncă nu există evaluări
- Ojsadmin, 279Document5 paginiOjsadmin, 279Muhammad FaizanÎncă nu există evaluări
- 2.0 Respiration: 2.1 Respiratory System 2.5 Gaseous Exchange in PlantsDocument1 pagină2.0 Respiration: 2.1 Respiratory System 2.5 Gaseous Exchange in PlantsaslendabasarÎncă nu există evaluări
- Foreign Body AspirationsDocument7 paginiForeign Body AspirationsEzzati Aiza100% (1)
- Gas ExchangeDocument3 paginiGas ExchangeDemi Ruth ElenÎncă nu există evaluări
- Living With A Tracheostomy: Patient EducationDocument2 paginiLiving With A Tracheostomy: Patient EducationJack Supramaniam100% (1)
- Acetone MSDSDocument8 paginiAcetone MSDSSiti MusabikhaÎncă nu există evaluări
- Alveolar Stress How To Measure 2161 105X 1000273Document3 paginiAlveolar Stress How To Measure 2161 105X 1000273Ade Satria ElismanÎncă nu există evaluări