Documente Academic
Documente Profesional
Documente Cultură
Lorenzo Franchi 2011
Încărcat de
Cris CavaliDrepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Lorenzo Franchi 2011
Încărcat de
Cris CavaliDrepturi de autor:
Formate disponibile
Original Article
Effectiveness of comprehensive fixed appliance treatment used with the
Forsus Fatigue Resistant Device in Class II patients
Lorenzo Franchia; Lisa Alvetrob; Veronica Giuntinic; Caterina Masuccid; Efisio Defraiae;
Tiziano Baccettia
ABSTRACT
Objective: To assess the dental, skeletal, and soft tissue effects of comprehensive fixed appliance
treatment combined with the Forsus Fatigue Resistant Device (FRD) in Class II patients.
Materials and Methods: Thirty-two Class II patients (mean age 12.7 6 1.2 years) were treated
consecutively with the FRD protocol and compared with a matched sample of 27 untreated Class II
subjects (mean age 12.8 6 1.3 years). Lateral cephalograms were taken before therapy and at the
completion of comprehensive therapy. The mean duration of comprehensive treatment was 2.4 6
0.4 years. Statistical comparisons were carried out with the Students t-test (P , .05).
Results: The success rate was 87.5%. The FRD group showed a significant restraint in the sagittal
skeletal position of the maxilla (also at the soft tissue level), a significant increase in mandibular
length, and a significant improvement in maxillo-mandibular sagittal skeletal relationships. The
treated group exhibited a significant reduction in overjet and a significant increase in molar
relationship. The lower incisors were significantly proclined and intruded, while the lower first
molars moved significantly in a mesial and vertical direction.
Conclusions: The FRD protocol is effective in correcting Class II malocclusion with a combination
of skeletal (mainly maxillary) and dentoalveolar (mainly mandibular) modifications. (Angle Orthod.
2011;81:678683.)
KEY WORDS: Class II malocclusion; Fixed functional appliances; Cephalometrics
INTRODUCTION Fixed devices for sagittal advancement of the
mandible that do not require the patients collaboration
Class II malocclusion is the most frequent sagittal
and that can be worn in association with fixed
problem in orthodontics, as it affects one third of the
appliances have been introduced to the orthodontic
population.1 One of the recommended therapeutic
community in order to overcome two major limitations
approaches to Class II malocclusion in growing
of removable functional appliances: the need for
patients is functional jaw orthopedics through the
patient collaboration and the lack of the possibility of
primary mechanism of mandibular advancement.2 combining the use of the functional appliance with
a
Assistant Professor, Department of Orthodontics, University
multibracket therapy in order to shorten treatment
of Florence, Florence, Italy; Thomas M. Graber Visiting Scholar, duration.3
Department of Orthodontics and Pediatric Dentistry, School of The effects of several compliance-free appliances
Dentistry, The University of Michigan, Ann Arbor, Mich. for mandibular anterior repositioning in association
b
Private Practice, Sidney, Ohio. with fixed appliances have been investigated in the
c
Research Assistant, Department of Orthodontics, University
of Florence, Florence, Italy.
literature. The Eureka Spring proved to be efficient in
d
PhD student, Department of Orthodontics, University of correcting Class II malocclusions without increasing
Florence, Florence, Italy. the vertical dimension.4 The Jasper Jumper appliance
e
Associate Professor, Department of Orthodontics, University produced very similar outcomes by improving both the
of Florence, Florence, Italy. skeletal imbalance and the profile in growing Class II
Corresponding author: Dr Lorenzo Franchi, Via del Ponte di
Mezzo 46-48 Firenze, Italy 50127 Italy
patients.5 Very recently, Jena and Duggal6 reported a
(e-mail: lorenzo.franchi@unifi.it) combination of favorable maxillary and mandibular
dentoskeletal effects leading to correction of Class II
Accepted: December 2010. Submitted: October 2010.
Published Online: February 7, 2011 malocclusion induced by the Mandibular Protraction
G 2011 by The EH Angle Education and Research Foundation, Appliance-IV. An increasingly popular fixed functional
Inc. appliance is the Forsus device. The Forsus (also
Angle Orthodontist, Vol 81, No 4, 2011 678 DOI: 10.2319/102710-629.1
EFFECTS OF FRD 679
archwire was consistently cinched distal to the molars.
In addition, brackets on the lower incisors presented
with a torque of 26u to limit the buccal inclination of the
lower incisors. The management of the maxillary
archwire varied according to the individual need in
terms of upper molar distalization. The rods of the FRD
were placed on the mandibular archwire distal to the
first bicuspids.
The phase with the FRD was undertaken until Class
II occlusion was overcorrected to an edge-to-edge
incisor relationship. The mean duration of the FRD
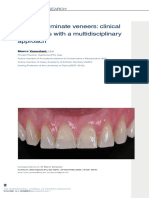
Figure 1. Forsus Fatigue Resistant Device (FRD) in association with active phase was 5.2 6 1.3 months. Thereafter, fixed
complete fixed orthodontic appliances. appliances were maintained in order to finalize the
occlusion. Comprehensive treatment of Class II
known as the Forsus Fatigue Resistant Device [FRD]) malocclusion was performed during the circumpubertal
is a semirigid telescoping system incorporating a phases of skeletal development, as assessed with the
superelastic nickel-titanium coil spring that can be cervical vertebral maturation method.9 Lateral cepha-
assembled chair-side, and it can be used in conjunc- lograms taken before (T1) and after (T2) treatment
tion with complete fixed orthodontic appliances (Fig- were analyzed, with T1 corresponding to the initiation
ure 1). The FRD attaches at the maxillary first molar of therapy with the fixed appliances and T2 corre-
and onto the mandibular archwire, distal to either the sponding to the completion of the comprehensive
canine or first premolar bracket (the latter option treatment.
making the appliance less visible and more comfort- A sample of 27 subjects was selected from the files
able). The clinical application of the FRD was of the University of Michigan Growth Study (12
described by Vogt7 in 2006 and was evaluated in a subjects) and of the Denver Child Growth Study (15
sample of 34 Class II patients (in comparison with a subjects); subjects presented with the same dento-
group treated with fixed appliances and Class II skeletal characteristics and skeletal maturational lev-
elastics) by Jones et al.8 in 2008. No previous study els at T1 as did the FRD sample subjects. The duration
assessed the effectiveness of FRD when compared of T1-T2 observation interval in the control group
with untreated Class II controls. matched the T1-T2 interval of the treatment group.
The aim of the present controlled clinical trial was to Differences in the male:female ratios in treatment vs
evaluate the dentoskeletal outcomes of FRD in control groups were not significant (chi-square 5
combination with fixed appliances in a group of 0.744; P 5 .388) in order to avoid the effects of sexual
consecutively treated Class II growing patients. Main dimorphism on craniofacial size and changes. Mean
features of the study include the comparison with ages at T1 and T2, mean duration of T1-T2 intervals,
matched untreated Class II controls; the use of FRD gender distribution, and skeletal maturation during
during the circumpubertal ages; and the appraisal of treatment or observation intervals for both treatment
dental, skeletal, and soft tissue profile changes at the and control groups are shown in Table 1.
end of comprehensive treatment.
The examiners who analyzed lateral cephalograms
of treated and control patients before and after
SUBJECTS AND METHODS treatment were blind with regard to the origin of the
Study Design films and the group to which individual subjects
belonged. The T2 observations were collected and
A sample of 32 subjects with Class II division 1 analyzed, regardless of the treatment outcomes, in
malocclusion (overjet larger than 5 mm, full Class II or terms of correction of Class II malocclusion in the
Class II tendency molar relationship, and ANB larger individual patients. This allowed for a further reduction
than 3u) was treated consecutively at a single private in potential selection biases in the study.
practice by one of the authors. All treated patients
were in the permanent dentition at the start of
Cephalometric Analysis
treatment, and they underwent a specific treatment
protocol with preadjusted fixed appliances in combi- Evaluation of dentoskeletal relationships. A custom-
nation with the FRD. The FRD was applied at the end ized digitization regimen and analysis provided by
of the aligning and leveling phase of orthodontic cephalometric software (Viewbox, ver 3.0, dHAL
treatment, when a 0.019 3 0.025inch stainless-steel Software, Kifissia, Greece) were utilized for all of the
archwire was inserted at both arches. The mandibular cephalograms that were examined in this study. The
Angle Orthodontist, Vol 81, No 4, 2011
680 FRANCHI, ALVETRO, GIUNTINI, MASUCCI, DEFRAIA, BACCETTI
Table 1. Demographics for the Treated and Untreated Class II Groupsa
Age at T1, y Age at T2, y T1-T2 Interval, y
n Female Male Prepubertal Pubertal Postpubertal Mean SD Mean SD Mean SD
FRD group 32 13 19 2 14 16 12.7 1.2 15.1 1.0 2.4 0.4
Control group 27 14 13 12 15 12.8 1.3 15.3 1.4 2.6 0.9
a
T1 indicates before treatment; T2, after treatment; SD, standard deviation; and FRD, Forsus Fatigue Resistant Device.
customized cephalometric analysis containing mea- The power of the study was calculated on the basis
surements from the analyses of Steiner,10 Jacobson,11 of the sample size of the two groups and of an effect
Ricketts,12 and McNamara13 was used and generated size equal to 1.17 The power exceeded 0.90 at an alpha
33 variables, 11 angular and 22 linear, for each tracing. level of .05.
For the analysis of the soft tissue profile changes the
method of Arnett et al.14 was used, with modifications RESULTS
(Figure 1).15
The statistical comparison on starting forms for hard
Error of the method. A total of 40 lateral cephalo-
tissue measurements between the two groups did not
grams randomly chosen from all observations were re-
reveal any significant differences, with the exception of
traced in random order and re-digitized to calculate
the FH to palatal plane measurement, which yielded a
method error by means of the Dahlbergs formula.16 The
greater value in the controls (3.2u).
operator who re-traced and re-digitized the cephalo-
Results for statistical comparisons on the T2-T1
grams was blinded with regard to time period and group.
changes for the FRD group and the Class II untreated
The error for linear measurements ranged from 0.25 mm controls are shown in Table 2. The statistical compar-
(overjet) to 0.75 mm (Pg to Nasion perpendicular), while ison showed a significant restraint in the sagittal
the error for angular measurements varied from 0.35u skeletal position of the maxilla (SNA, Pt A to Nasion
(ANB) to 1.40u (interincisal angle). perp, and Co-A). The increase in effective mandibular
The assessment of the stages in cervical vertebral length (Co-Gn) was significantly greater in the FRD
maturation9 on lateral cephalograms for each subject group when compared to natural growth changes in
was performed by one investigator and then verified by Class II controls. Comparison of changes in intermax-
a second. Any disagreements were resolved to the illary relationships revealed a significantly greater
satisfaction of both observers. decrease in ANB angle and Wits appraisal as well as
The magnification values of the data sets with a significant increase in the maxillo-mandibular differ-
regard to the treated Class II patients and the ential in the treatment group. With regard to changes in
untreated Class II subjects were different, with the vertical skeletal relationships, the increase in lower
lateral cephalograms of treated subjects showing 0% anterior facial height (ANS to Me) was significantly
enlargement and those from the control group showing greater in the treatment group compared to the
a magnification of either 12.1% (UMGS) or 4% untreated controls.
(DCGS). The lateral cephalograms of all treated and With regard to the interdental changes, the treat-
untreated subjects were corrected to match an 8% ment group exhibited a significant reduction in overjet,
enlargement factor. overbite, and interincisal angle, as well as a significant
improvement in molar relationship. A significantly more
Statistical Analysis retruded position of the upper incisors (U1 to Pt A
Descriptive statistics of craniofacial measurements vertical and U1 horizontal) was assessed in the treated
in all treated and untreated Class II samples at T1 and group, as was a greater vertical eruption of the upper
T2 were calculated, as were the between-stage incisors (U1 vertical). All of the changes in the
changes. Kolmogorov-Smirnov test revealed normality mandibular dentoalveolar parameters were statistically
of distribution for the measurements used in the study. significant in the FRD group when compared with the
Therefore, parametric statistics (Students t-test for untreated control group. As a result of therapy the
independent samples) were utilized (SPSS Version lower incisors were significantly proclined and intrud-
12.0, SPSS Inc, Chicago, Ill). The following compar- ed, while the lower first molars extruded significantly
and moved significantly in a mesial direction.
isons were carried out for the dentoskeletal variables:
The analysis of the changes in the soft tissue
N Treated group vs untreated group at T1 (comparison measurements between treated Class II patients and
on starting forms); and untreated controls showed significantly greater back-
N T2-T1 changes in treated group vs untreated group ward movement of the soft tissue A point in the FRD
(dentoskeletal and soft tissue profile variables). group.
Angle Orthodontist, Vol 81, No 4, 2011
EFFECTS OF FRD 681
Table 2. Descriptive Statistics and Statistical Comparisons of the Pretreatment (T1)Posttreatment (T2) Changes Between Class II Patients
Treated With Forsus Fatigue Resistant Device (FRD)/Fixed Appliances and Untreated Class II Controlsa
FRD Group (N 5 32) Control Group (N 5 27)
Cephalometric Measures Mean SD Mean SD Difference P Significance
Cranial base
NSBa, u 0.8 2.0 20.2 1.8 1.0 0.052 NS
Maxillary skeletal
SNA, u 21.6 1.4 0.5 1.3 22.1 0.000 ***
Pt A to Nasion perp, mm 20.7 1.8 0.5 1.1 21.2 0.005 **
Co-Pt A, mm 2.2 2.4 3.6 2.2 21.4 0.032 *
Mandibular skeletal
SNB, u 0.3 1.4 0.7 0.9 20.4 0.151 NS
Pg to Nasion perp, mm 2.2 3.7 1.8 2.2 0.4 0.603 NS
Co-Gn, mm 7.5 3.4 5.7 1.7 1.8 0.014 *
Co-Go, mm 5.8 3.6 4.3 2.8 1.5 0.071 NS
Maxillary/mandibular
ANB, u 21.9 1.2 20.2 0.8 21.7 0.000 ***
WITS, mm 22.0 3.0 0.5 1.5 22.5 0.000 ***
Maxillary/mandibular
difference, mm 5.1 2.5 2.7 1.7 2.4 0.000 ***
Vertical skeletal
FH to palatal plane, u 20.1 1.2 20.2 1.4 0.1 0.922 NS
FH to mandibular plane, u 21.1 2.2 21.2 1.5 0.1 0.922 NS
Palatal plane to mandibular
plane, u 21.0 2.2 21.0 2.3 0.0 0.994 NS
ArGoMe, u 21.4 2.6 21.6 2.2 0.2 0.807 NS
CoGoMe, u 20.4 2.2 20.6 2.0 0.2 0.690 NS
N to ANS, mm 2.8 2.2 2.1 1.4 0.7 0.114 NS
ANS to Me, mm 4.0 2.6 2.7 1.4 1.3 0.012 *
Interdental
Overjet, mm 25.4 2.0 0.1 1.1 25.5 0.000 ***
Overbite, mm 22.5 2.0 20.1 1.0 22.4 0.000 ***
Interincisal angle, u 23.8 12.6 2.3 5.1 26.1 0.016 *
Molar relationship, mm 3.4 1.3 0.0 1.4 3.4 0.000 ***
Maxillary dentoalveolar
U1 to Pt A vertical, mm 21.2 2.3 0.2 0.9 21.4 0.003 **
U1 to FH, u 21.2 8.9 20.9 2.6 20.3 0.865 NS
U1 horizontal, mm 21.1 2.3 0.4 1.0 21.5 0.002 **
U1 vertical, mm 1.6 1.7 0.6 0.9 1.0 0.011 *
U6 horizontal, mm 1.0 1.5 1.4 1.1 20.4 0.234 NS
U6 vertical, mm 1.6 1.5 1.6 0.8 0.0 0.989 NS
Mandibular dentoalveolar
L1 to Pt A-pogonion, mm 3.4 2.0 20.2 1.1 3.6 0.000 ***
L1 to mandibular plane, u 6.1 6.3 0.9 4.1 5.2 0.001 **
L1 horizontal, mm 2.3 2.0 20.2 1.6 2.5 0.000 ***
L1 vertical, mm 20.5 1.4 1.5 1.1 22.0 0.000 ***
L6 horizontal, mm 2.4 1.6 0.9 1.5 1.5 0.000 ***
L6 vertical, mm 3.6 1.5 1.4 1.1 2.2 0.000 ***
Soft tissue
A9-VL, mm 20.8 1.1 0.3 1.2 21.1 0.000 ***
B9-VL, mm 1.8 2.3 0.5 2.7 1.3 0.051 NS
Pg9-VL, mm 0.9 2.6 0.4 2.9 0.5 0.488 NS
a
SD indicates standard deviation; NS, not significant.
* P , .05; ** P , .01; *** P , .001.
Angle Orthodontist, Vol 81, No 4, 2011
682 FRANCHI, ALVETRO, GIUNTINI, MASUCCI, DEFRAIA, BACCETTI
DISCUSSION The FRD protocol also induced a significantly
(1.8 mm) greater increase in total mandibular length
The aim of the present study was to assess the
(Co-Gn) with respect to untreated controls. However,
dental, skeletal, and soft tissue changes produced by a
this favorable skeletal change was not associated with
fixed interarch appliance for Class II treatment, the
a significant improvement in the sagittal position of the
FRD, within a comprehensive orthodontic treatment
bony and soft tissue chin.
with preadjusted fixed appliances. Significant features
The dentoalveolar changes were highly significant
of this study were the analysis of patients treated
both at the maxillary and mandibular arches. The
consecutively by a single operator and the blind
upper incisors demonstrated a significant, though
methodology employed in the analysis of the data, in
modest, amount of retrusion and extrusion
conjunction with the use of an historical sample of
(#1.5 mm). On the other hand, the lower incisors
untreated Class II controls at the same skeletal exhibited a large amount of proclination (5.2u), forward
maturation phases as the treated subjects, for the movement (2.5 mm), and intrusion (2.0 mm). The
evaluation of treatment effectiveness vs physiological mandibular first molars also showed a significant
growth in Class II malocclusion. The methodology amount of mesial movement (1.5 mm) and extrusion
used reduced the potential selection and proficiency (2.2 mm). These outcomes are similar to those
biases of the study. Furthermore, the treated and reported by Jones et al.8 for both the FRD and Class
control groups exhibited very similar characteristics in II elastics.
terms of responsiveness to mandibular growth stimu- A general overview of the effects of Class II
lation, as assessed by the pretreatment Co-Go-Me treatment with fixed appliances and FRD leads to the
angle.18 Both groups showed a prevalence rate of consideration that skeletally one of the main outcomes
good responders (Co-Go-Me smaller than 125.5u) of of this protocol consists of a significant restraint in the
about 81%. This similarity controlled for a potential sagittal position of the maxilla. This effect has been
susceptibility bias on the basis of pretreatment reported previously for the Herbst appliance in
morphological characteristics. combination with fixed appliances at puberty,22 for
While not ideal, the use of historical controls with the FRD without controls,8 and for the Jasper Jumper
untreated Class II malocclusions was due mainly to the appliance.5 The skeletal maxillary effect was reflected
ethical issue involved in leaving subjects with full-cusp also by a modest, though significant, improvement in
Class II malocclusions without orthodontic treatment the sagittal position of the maxillary soft tissues. On the
during the pubertal and postpubertal stages of other hand, the skeletal outcomes of the FRD protocol
development, a biological period that has been with regard to the mandible appeared to be rather
demonstrated1921 to be associated with the most limited. Although an enhancement in total mandibular
favorable treatment effects in Class II patients. length of about 2 mm was found in the treated group vs
The treatment regimens proved to be effective on the untreated controls, this growth modification did not
occlusal parameters. A net reduction of 5.5 mm was significantly affect the sagittal position of either the
recorded for the overjet, while a net improvement of bony or soft tissue chin. The lack of a significant effect
3.4 mm was obtained for the molar relationship. In of the FRD on the sagittal position of the chin might be
terms of overall correction of Class II division 1 correlated with the short duration of active treatment
malocclusion, the success rate (87.5%) was very high (on average less than 6 months).23
in the treated group; this value is very similar to those The changes at the dentoalveolar level showed a
reported22 for other comprehensive Class II treatment reverse pattern with respect to the skeletal changes. In
modalities incorporating either the Herbst appliance or fact, the upper incisor exhibited modest changes, while
headgear and Class II elastics. the mandibular dentition displayed highly significant
The most relevant skeletal changes occurred in the modifications. The FRD protocol produced a large
maxillary region, and they were confirmed by all the amount of mesial movement of the lower arch, with
angular and linear measurements used in the present proclination of the lower incisors. This effect occurred
study. These changes revealed a significant effect of in spite of the cinching back of the mandibular archwire
the FRD protocol in restraining sagittal growth of the distal to the molars and despite the torque of 26u
maxilla, ranging from 1.2 mm for Pt A to Nasion perp to embedded in the brackets on the lower incisors. It is
22.1u for SNA. A significant improvement in the sagittal therefore recommended that practitioners implement
position of the maxillary soft tissues was recorded in the all those procedures that can prevent the proclination
treated group as well. The maxillary changes accounted and protrusion of the lower incisors during treatment
for significant improvements in maxillo-mandibular (the use of mandibular rectangular archwires of greater
sagittal relationships that ranged from 21.7u for the size, the addition of a negative torque also to the
ANB angle to 22.5 mm for the Wits appraisal. archwire in the lower incisor region, etc).
Angle Orthodontist, Vol 81, No 4, 2011
EFFECTS OF FRD 683
The outcomes reported in the current study refer to Device versus intermaxillary elastics. Angle Orthod. 2008;
the end of comprehensive Class II treatment, without 78:332338.
9. Baccetti T, Franchi L, McNamara JA Jr. The cervical
follow-up observation. However, it should be noted that vertebral maturation (CVM) method for the assessment of
more than half of the patients in the FRD group optimal treatment timing in dentofacial orthopedics. Semin
completed their treatment protocols at very advanced Orthod. 2005;11:119129.
postpubertal stages in skeletal maturation (CS5 or 10. Steiner CC. Cephalometrics for you and me. Am J Orthod.
CS6). The amount of craniofacial growth occurring 1953;39:729755.
11. Jacobson A. The Wits appraisal of jaw disharmony.
after those stages is very limited in Class II subjects, Am J Orthod. 1975;67:125138.
and, more importantly, growth differences between 12. Ricketts RM. Perspectives in the clinical application of
Class II and normal occlusion subjects after late cephalometrics. The first fifty years. Angle Orthod. 1981;51:
puberty are insignificant.24 When orthodontic therapy 115150.
of Class II malocclusion is completed at late puberty, 13. McNamara JA Jr. A method of cephalometric evaluation.
Am J Orthod. 1984;86:449469.
close to completion of active craniofacial growth, 14. Arnett GW, Jelic JS, Kim J, Cummings DR, Beress A,
relapse tendency due to a reestablishment of Class II Worley CM Jr, Chung B, Bergman R. Soft tissue cephalo-
growth characteristics is expected to occur less metric analysis: diagnosis and treatment planning of
often.24,25 dentofacial deformity. Am J Orthod Dentofacial Orthop.
1999;116:239253.
15. Baccetti T, Franchi L, Kim LH. Effect of timing on the
CONCLUSIONS outcomes of 1-phase nonextraction therapy of Class II
malocclusion. Am J Orthod Dentofacial Orthop. 2009;136:
N The FRD protocol led to a successful correction of
501509.
Class II malocclusion in 87.5% of the patients. 16. Dahlberg G. Statistical Methods for Medical and Biological
N The protocol had a greater skeletal effect on the Students. London, UK: G Allen & Unwin Ltd; 1940.
maxillary structures by restraining the sagittal ad- 17. Cohen J. A power primer. Psychol Bull. 1992;112:155159.
vancement of the maxilla. 18. Franchi L, Baccetti T. Prediction of individual mandibular
changes induced by functional jaw orthopedics followed by
N The effects on the mandible were mainly at the fixed appliances in Class II patients. Angle Orthod. 2006;76:
dentoalveolar level, with a large amount of mesial 950954.
movement of the lower incisors and first molars. 19. Malmgren O, Omblus J, Hagg U, Pancherz H. Treatment
with an appliance system in relation to treatment intensity
and growth periods. Am J Orthod Dentofacial Orthop. 1987;
ACKNOWLEDGMENT 91:143151.
20. Hagg U, Pancherz H. Dentofacial orthopaedics in relation to
The authors wish to thank Dr Fredrik Bergstrand for his chronological age, growth period and skeletal development:
valuable advice in the critical review of this article. an analysis of 72 male patients with Class II division 1
malocclusion treated with the Herbst appliance. Eur J Orthod.
REFERENCES 1988;10:169176.
21. Petrovic A, Stutzmann J, Lavergne J. Mechanism of
1. Proffit WR, Fields HW, Moray LJ. Prevalence of malocclu- craniofacial growth and modus operandi of functional
sion and orthodontic treatment need in the United States: appliances: a cell-level and cybernetic approach to ortho-
estimates from the NHANES-III survey. Int J Adult Orthod dontic decision making. In: Carlson DS, ed. Craniofacial
Orthognath Surg. 1998;13:97106. Growth Theory and Orthodontic Treatment. Craniofacial
2. McNamara JA Jr, Brudon WL. Orthodontics and Dentofacial Growth Series, Vol 23. Ann Arbor, Mich: Center for Human
Orthopedics. Ann Arbor, Mich: Needham Press, Inc; Growth and Development, University of Michigan;
2001:73. 1990:1374.
3. Tulloch JF, Proffit WR, Phillips C. Outcomes in a 2-phase 22. Baccetti T, Franchi L, Stahl F. Comparison of 2 compre-
randomized clinical trial of early Class II treatment. hensive Class II treatment protocols including the bonded
Am J Orthod Dentofacial Orthop. 2004;125:657667. Herbst and headgear appliances: a double-blind study of
4. Stromeyer EL, Caruso JM, DeVincenzo JP. A cephalometric consecutively treated patients at puberty. Am J Orthod
study of the Class II correction effects of the Eureka Spring. Dentofacial Orthop. 2009;135:698.e1698.e10.
Angle Orthod. 2002;72:203210. 23. Phan KL, Bendeus M, Hagg U, Hansen K, Rabie AB.
5. Kucukkeles N, Ilhan I, Orgun IA. Treatment efficiency in Comparison of the headgear activator and Herbst appli-
skeletal Class II patients treated with the Jasper Jumper. ance-effects and post-treatment changes. Eur J Orthod.
Angle Orthod. 2007;77:449456. 2006;28:594604.
6. Jena AK, Duggal R. Treatment effects of twin-block and 24. Baccetti T, Stahl F, McNamara JA Jr. Dentofacial growth
mandibular protraction appliance-IV in the correction of changes in subjects with untreated Class II malocclusion
class II malocclusion. Angle Orthod. 2010;80:485491. from late puberty through young adulthood. Am J Orthod
7. Vogt W. The Forsus Fatigue Resistant Device. J Clin Dentofacial Orthop. 2009;135:148154.
Orthod. 2006;40:368377. 25. von Bremen J, Pancherz H. Efficiency of early and late
8. Jones G, Buschang PH, Kim KB, Oliver DR. Class II non- Class II division 1 treatment. Am J Orthod Dentofacial
extraction patients treated with the Forsus Fatigue Resistant Orthop. 2002;121:3137.
Angle Orthodontist, Vol 81, No 4, 2011
S-ar putea să vă placă și
- Angle, Forsus Com MIDocument12 paginiAngle, Forsus Com MIMariana SantosÎncă nu există evaluări
- Evaluation of Soft-Tissue Changes in Young Adults Treated With The Forsus Fatigue-Resistant DeviceDocument11 paginiEvaluation of Soft-Tissue Changes in Young Adults Treated With The Forsus Fatigue-Resistant DeviceDominikaSkórkaÎncă nu există evaluări
- Class II Correction in Orthodontic Patients Utilizing The Mandibular Anterior Repositioning Appliance (MARA)Document7 paginiClass II Correction in Orthodontic Patients Utilizing The Mandibular Anterior Repositioning Appliance (MARA)rÎncă nu există evaluări
- Treatment and Posttreatment Effects Induced by The Forsus Appliance A Controlled Clinical StudyDocument8 paginiTreatment and Posttreatment Effects Induced by The Forsus Appliance A Controlled Clinical Studyorthodonticlit orthodonticlitÎncă nu există evaluări
- Secretos de La Mordida ProfundaDocument11 paginiSecretos de La Mordida Profundaaldair villazoÎncă nu există evaluări
- Class II Subdivision Treatment With The Forsus Fatigue Resistant Device Vs Intermaxillary ElasticsDocument6 paginiClass II Subdivision Treatment With The Forsus Fatigue Resistant Device Vs Intermaxillary ElasticsClarissa KnebelÎncă nu există evaluări
- Effect of Timing On The Outcomes of 1-Phase Nonextraction Therapy of Class II MalocclusionDocument9 paginiEffect of Timing On The Outcomes of 1-Phase Nonextraction Therapy of Class II MalocclusionLudy Jiménez ValdiviaÎncă nu există evaluări
- Cji078 2Document9 paginiCji078 2nevier chanÎncă nu există evaluări
- Longterm Treatment Effects of The FR2Document6 paginiLongterm Treatment Effects of The FR2Fabian BarretoÎncă nu există evaluări
- 13Document10 pagini13Mohammed ijasÎncă nu există evaluări
- Maxillary Molar Distalization With The Dual-ForceDocument5 paginiMaxillary Molar Distalization With The Dual-ForceMaria SilvaÎncă nu există evaluări
- Tanpa Judul PDFDocument7 paginiTanpa Judul PDFnadyashintakasihÎncă nu există evaluări
- Andresen InnovationDocument1 paginăAndresen Innovationelvin peraltaÎncă nu există evaluări
- Am Journal 2008, Papadopoulos, Correção CL II Com MIDocument16 paginiAm Journal 2008, Papadopoulos, Correção CL II Com MIMariana SantosÎncă nu există evaluări
- Franchi 2006Document5 paginiFranchi 2006Goutam NookalaÎncă nu există evaluări
- 1 s2.0 S2212443814000186 Main 2Document6 pagini1 s2.0 S2212443814000186 Main 2Pau ContrerasÎncă nu există evaluări
- Treatment Timing of MARA and Fixed Appliance Therapy of Class II MalocclusionDocument7 paginiTreatment Timing of MARA and Fixed Appliance Therapy of Class II MalocclusionOmar DSÎncă nu există evaluări
- Ocr 12416Document7 paginiOcr 12416khaled mohammadÎncă nu există evaluări
- Space Closure by Miniscrew-Assisted Mesialization of An Upper Third Molar and Partial Vestibular Fixed Appliance: A Case ReportDocument15 paginiSpace Closure by Miniscrew-Assisted Mesialization of An Upper Third Molar and Partial Vestibular Fixed Appliance: A Case ReportCarol Gissel FloresÎncă nu există evaluări
- 132 53shahid 2Document5 pagini132 53shahid 2melissa.etienne0311Încă nu există evaluări
- MARA Vs AdvansyncDocument8 paginiMARA Vs AdvansyncrohitÎncă nu există evaluări
- Class II Subdivision Treatment With The Forsus Fatigue ResistantDocument6 paginiClass II Subdivision Treatment With The Forsus Fatigue Resistantjcesar8745Încă nu există evaluări
- Jurnal 1 (Klas II Skeletal - Headgear)Document7 paginiJurnal 1 (Klas II Skeletal - Headgear)rif'atir rizqiyahÎncă nu există evaluări
- Clinical Assessment of Short Implants Retsining Removsble Partial DenturesDocument7 paginiClinical Assessment of Short Implants Retsining Removsble Partial DenturesLouis HutahaeanÎncă nu există evaluări
- Treatment Timing For Functional Jaw Orthopaedics Followed by Fixed Appliances: A Controlled Long-Term StudyDocument7 paginiTreatment Timing For Functional Jaw Orthopaedics Followed by Fixed Appliances: A Controlled Long-Term StudyEggula AnushaÎncă nu există evaluări
- AW - Sys Revw - 2017Document11 paginiAW - Sys Revw - 2017plsssssÎncă nu există evaluări
- Dentofacial Effects of Two Facemask Therapies For Maxillary Protraction Miniscrew Implants Versus Rapid Maxillary ExpandersDocument9 paginiDentofacial Effects of Two Facemask Therapies For Maxillary Protraction Miniscrew Implants Versus Rapid Maxillary ExpandersMariana SantosÎncă nu există evaluări
- 1 s2.0 S1073874623000476 MainDocument6 pagini1 s2.0 S1073874623000476 MainDANTE DELEGUERYÎncă nu există evaluări
- Jced 9 E1029Document6 paginiJced 9 E1029Ana Gabriela AlbuquerqueÎncă nu există evaluări
- Twin SupportDocument11 paginiTwin SupportArwa Said Shokri KhalilÎncă nu există evaluări
- Effectiveness of Maxillary Protraction Using A Hybrid Hyrax-Facemask Combination: A Controlled Clinical StudyDocument7 paginiEffectiveness of Maxillary Protraction Using A Hybrid Hyrax-Facemask Combination: A Controlled Clinical StudyKarin UchimaÎncă nu există evaluări
- Growing The Mandible? Impossible, Right?: SpecialDocument4 paginiGrowing The Mandible? Impossible, Right?: SpecialAriana Moreno ZavalaÎncă nu există evaluări
- Stability of Class II Malocclusion Treatment With The Distal Jet Followed by Fixed AppliancesDocument8 paginiStability of Class II Malocclusion Treatment With The Distal Jet Followed by Fixed AppliancesFabian BarretoÎncă nu există evaluări
- 1985 Australian Orthodontic Journal, MelbourneDocument19 pagini1985 Australian Orthodontic Journal, MelbourneMariyamÎncă nu există evaluări
- Book Reviews and Article Abstracts: Treatment Timing: Orthodontics in Four DimensionsDocument2 paginiBook Reviews and Article Abstracts: Treatment Timing: Orthodontics in Four DimensionsmeghaÎncă nu există evaluări
- Gao 2021Document8 paginiGao 2021KATERIN TTITO MAMANIÎncă nu există evaluări
- Long-Term Stability of Anterior Open-Bite Treatment by Intrusion of Maxillary Posterior TeethDocument9 paginiLong-Term Stability of Anterior Open-Bite Treatment by Intrusion of Maxillary Posterior TeethNg Chun HownÎncă nu există evaluări
- MicroscopeDocument8 paginiMicroscopeapi-3769525100% (2)
- Ojo 2013112116194629 PDFDocument5 paginiOjo 2013112116194629 PDFYash SharmaÎncă nu există evaluări
- Complica C I OnesDocument7 paginiComplica C I OnesDiana Carvajal ManriqueÎncă nu există evaluări
- Dental and Skeletal Effects of Herbst Appliance, Forsus Fatigue Resistance Device, and Class II Elastics-A Systematic Review and Meta-AnalysisDocument30 paginiDental and Skeletal Effects of Herbst Appliance, Forsus Fatigue Resistance Device, and Class II Elastics-A Systematic Review and Meta-Analysisjcesar8745Încă nu există evaluări
- Frenectomy - Different TechniquesDocument7 paginiFrenectomy - Different TechniquesIJAR JOURNALÎncă nu există evaluări
- Relevance Of: Step-B in The Treatment of M Ular Ion The Frbkel ApplianceDocument9 paginiRelevance Of: Step-B in The Treatment of M Ular Ion The Frbkel AppliancericardoÎncă nu există evaluări
- CrossbowDocument11 paginiCrossbowm.malekiÎncă nu există evaluări
- Maxillary "En Masse" High-Pull Traction in Class II Division 1 Subjects: Which Kind of Skeletal Outcomes Does It Produce?Document6 paginiMaxillary "En Masse" High-Pull Traction in Class II Division 1 Subjects: Which Kind of Skeletal Outcomes Does It Produce?Werlin Torres ZÎncă nu există evaluări
- Chin Cup Therapy An Effective Tool For The Correction of Class III Malocclusion in Mixed and Late Deciduous DentitionsDocument6 paginiChin Cup Therapy An Effective Tool For The Correction of Class III Malocclusion in Mixed and Late Deciduous Dentitionschic organizerÎncă nu există evaluări
- RK Ibm 1Document4 paginiRK Ibm 1Yassie ShaillaÎncă nu există evaluări
- Delir 2013Document7 paginiDelir 2013Karam EidÎncă nu există evaluări
- Comparison of Facemask Therapy Effects Using Skeletal and Tooth-Borne AnchorageDocument8 paginiComparison of Facemask Therapy Effects Using Skeletal and Tooth-Borne AnchorageMariana SantosÎncă nu există evaluări
- Ojsadmin, 388Document10 paginiOjsadmin, 388Srishti Jain MalooÎncă nu există evaluări
- 2003-09 Magnification (Endod. Practice)Document8 pagini2003-09 Magnification (Endod. Practice)Puscas IulianaÎncă nu există evaluări
- MARS Appliance - Clements1982Document11 paginiMARS Appliance - Clements1982rohitÎncă nu există evaluări
- FixedfunctionalAppliance AnoverviewDocument8 paginiFixedfunctionalAppliance Anoverviewmanuel marinÎncă nu există evaluări
- Mallet Finger Suturing TechniqueDocument5 paginiMallet Finger Suturing TechniqueSivaprasath JaganathanÎncă nu există evaluări
- FFA Flexible and Rigid Summary PDFDocument17 paginiFFA Flexible and Rigid Summary PDFrohit100% (1)
- Bionator RetrospectivoDocument7 paginiBionator RetrospectivoCATALINA VASQUEZ LOPEZÎncă nu există evaluări
- 2013 Laser FrenectomyDocument9 pagini2013 Laser FrenectomyCristina FernándezÎncă nu există evaluări
- Dentoskeletal Effects of Twin Block Appliance inDocument6 paginiDentoskeletal Effects of Twin Block Appliance inNORMA EDITH JIMENEZ LUNAÎncă nu există evaluări
- Adult Class LLL Treatment Using A J-Hook Headgear To The Mandibular ArchDocument8 paginiAdult Class LLL Treatment Using A J-Hook Headgear To The Mandibular ArchRocioÎncă nu există evaluări
- Peri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentDe la EverandPeri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentÎncă nu există evaluări
- StdoutDocument1 paginăStdoutCris CavaliÎncă nu există evaluări
- FAQ For Windows PortDocument3 paginiFAQ For Windows PortDerek Souza E SouzaÎncă nu există evaluări
- Readme WindowsDocument15 paginiReadme WindowsJonathan Soto CanoÎncă nu există evaluări
- Remotedassensing 04 01392Document19 paginiRemotedassensing 04 01392Cris CavaliÎncă nu există evaluări
- Remotedassensing 04 01392Document19 paginiRemotedassensing 04 01392Cris CavaliÎncă nu există evaluări
- Literatura Amazônica Seus Mitos e Suas LendasDocument48 paginiLiteratura Amazônica Seus Mitos e Suas LendasAbenisÎncă nu există evaluări
- Eula 1036Document4 paginiEula 1036Erik Yoel T RÎncă nu există evaluări
- Quick Start Guide for SanDisk SecureAccessDocument21 paginiQuick Start Guide for SanDisk SecureAccessbijan034567Încă nu există evaluări
- And The Tooth CrackedDocument20 paginiAnd The Tooth Crackedpablogdv956Încă nu există evaluări
- RELINING COMPLETE DENTURES WITH TISSUE CONDITIONER AND FUNCTIONAL IMPRESSIONDocument4 paginiRELINING COMPLETE DENTURES WITH TISSUE CONDITIONER AND FUNCTIONAL IMPRESSIONsasanÎncă nu există evaluări
- Rubber DamDocument78 paginiRubber DamDevanshi Sharma100% (1)
- Sem 15 Occ Eq FinalDocument64 paginiSem 15 Occ Eq FinalpriyaÎncă nu există evaluări
- Health Problems: Dealing With Problems: 1. Read The Situations and Circle The Odd One OutDocument2 paginiHealth Problems: Dealing With Problems: 1. Read The Situations and Circle The Odd One Outsonia martinsÎncă nu există evaluări
- Current Concepts On Caries RemovalDocument16 paginiCurrent Concepts On Caries RemovalgarciadeluisaÎncă nu există evaluări
- 490.062-En - Low - Variobase Technical InformationDocument40 pagini490.062-En - Low - Variobase Technical InformationansdkalsÎncă nu există evaluări
- Different Types of Tooth PreparationDocument56 paginiDifferent Types of Tooth PreparationSahana Rangarajan100% (1)
- American College of Prosthodontist 2013 Mock Exam With ReferencesDocument32 paginiAmerican College of Prosthodontist 2013 Mock Exam With ReferencesAwaisÎncă nu există evaluări
- Ergonomics in DentistryDocument55 paginiErgonomics in DentistryheycoolalexÎncă nu există evaluări
- IntJForensicOdontol2118-3910049 105140Document4 paginiIntJForensicOdontol2118-3910049 105140Javeria KhanÎncă nu există evaluări
- Răng trẻ emDocument39 paginiRăng trẻ emHoàng Đức NghĩaÎncă nu există evaluări
- KimDocument12 paginiKimIvanna H. A.Încă nu există evaluări
- Dental Implantology and Biomaterial (PDFDrive)Document191 paginiDental Implantology and Biomaterial (PDFDrive)Maier OlimpiuÎncă nu există evaluări
- Altering Gingival Levels: The Restorative Connection Biologic VariablesDocument7 paginiAltering Gingival Levels: The Restorative Connection Biologic Variablespooja100% (1)
- Dental diagnosis and treatment codesDocument2 paginiDental diagnosis and treatment codesReza Ma'lufiana ZuhriÎncă nu există evaluări
- Orthodontic Tooth Movement: A Historic ProspectiveDocument10 paginiOrthodontic Tooth Movement: A Historic ProspectivelauÎncă nu există evaluări
- Picasso OperatingInstructions Manual 211018 WEBDocument27 paginiPicasso OperatingInstructions Manual 211018 WEBBill McFarlandÎncă nu există evaluări
- Tangsripongkul2020 PDFDocument5 paginiTangsripongkul2020 PDFdrpriyanka patelÎncă nu există evaluări
- IMPLANTOLOGÍA. Tarnow When To Save or Extract A Tooth in The Esthetic Zone A CommentaryDocument12 paginiIMPLANTOLOGÍA. Tarnow When To Save or Extract A Tooth in The Esthetic Zone A CommentaryKenigal14Încă nu există evaluări
- Three-Dimensional Assessment of Virtual Bracket Removal For Orthodontic Retainers: A Prospective Clinical StudyDocument10 paginiThree-Dimensional Assessment of Virtual Bracket Removal For Orthodontic Retainers: A Prospective Clinical StudyAndré DrumondÎncă nu există evaluări
- A Clinical Approach Strategy For The Diagnosis Treatment and Evaluation of ExternalDocument27 paginiA Clinical Approach Strategy For The Diagnosis Treatment and Evaluation of Externaltrain.with.asadhamoodÎncă nu există evaluări
- Science Investigatory Project TankDocument6 paginiScience Investigatory Project TankLei Andrew BalmacedaÎncă nu există evaluări
- UNITEKDocument301 paginiUNITEKManpowerTMÎncă nu există evaluări
- Ceramic Laminate Veneers: Clinical Procedures With A Multidisciplinary ApproachDocument23 paginiCeramic Laminate Veneers: Clinical Procedures With A Multidisciplinary ApproachBenjiÎncă nu există evaluări
- The Straight-Wire Appliance 17 Years Later: Roth Prescription OvercorrectionDocument11 paginiThe Straight-Wire Appliance 17 Years Later: Roth Prescription OvercorrectionMarcela Sandoval100% (2)
- Replacing Damaged Crowns with Modified Crowns and PonticsDocument5 paginiReplacing Damaged Crowns with Modified Crowns and PonticsNgatimahÎncă nu există evaluări
- Restorations in Primary Teeth: A Systematic Review On Survival and Reasons For FailuresDocument18 paginiRestorations in Primary Teeth: A Systematic Review On Survival and Reasons For FailuresRayhan DaneoÎncă nu există evaluări
- E-Catalogue 16 Agustus 22Document100 paginiE-Catalogue 16 Agustus 22Danang K T KusumoÎncă nu există evaluări
- Anxiety Disorders EssayDocument7 paginiAnxiety Disorders Essayvdyvfjnbf100% (2)