Documente Academic
Documente Profesional
Documente Cultură
Exercise Training Program in Children and Adolescents With Cerebral Palsy
Încărcat de
Valentina SiegmundDrepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Exercise Training Program in Children and Adolescents With Cerebral Palsy
Încărcat de
Valentina SiegmundDrepturi de autor:
Formate disponibile
ARTICLE
Exercise Training Program in Children
and Adolescents With Cerebral Palsy
A Randomized Controlled Trial
Olaf Verschuren, BSc, PT; Marjolijn Ketelaar, PhD; Jan Willem Gorter, MD, PhD;
Paul J. M. Helders, MSc, PhD, PCS; Cuno S. P. M. Uiterwaal, MD, PhD; Tim Takken, MSc, PhD
Objective: To evaluate the effects of an 8-month training ondary outcome measures included agility, muscle
program with standardized exercises on aerobic and anaero- strength, self-competence, gross motor function, partici-
bic capacity in children and adolescents with cerebral palsy. pation level, and health-related quality of life.
Design: Pragmatic randomized controlled clinical trial Results: A significant training effect was found for aero-
with blinded outcome evaluation between July 2005 and bic (P .001) and anaerobic capacity (P =.004). A sig-
October 2006. nificant effect was also found for agility (P.001), muscle
strength (P .001), and athletic competence (P=.005).
Setting: Participants were recruited from 4 schools for The intensity of participation showed a similar effect for
special education in the Netherlands. formal (P .001), overall (P =.002), physical (P=.005),
and skilled-based activities (P .001). On the health-
Participants: A total of 86 children with cerebral palsy
related quality of life measure, a significant improve-
(aged 7-18 years) classified at Gross Motor Function Clas-
ment was found for the motor (P = .001), autonomy
sification System level I or II.
(P =.02), and cognition (P=.04) domains.
Intervention: Participants were randomly assigned to
Conclusions: An exercise training program improves
either the training group (n = 32) or the control group
(n=33). The training group met twice per week for 45 physical fitness, participation level, and quality of life in
minutes to circuit train in a group format that focused children with cerebral palsy when added to standard care.
on aerobic and anaerobic exercises.
Trial Registration: isrctn.org Identifier:
Main Outcome Measures: Aerobic capacity was as- ISRCTN77274716
sessed by the 10-m shuttle run test, and anaerobic ca-
pacity was assessed by the Muscle Power Sprint Test. Sec- Arch Pediatr Adolesc Med. 2007;161(11):1075-1081
C
Author Affiliations: EREBRAL PALSY (CP) DE- distinctly subnormal aerobic and anaero-
Rehabilitation Centre De bic capacity in comparison with typically
scribes a group of disor-
Hoogstraat (Mr Verschuren
ders that affect the devel- developing peers.4-6 Also, muscle mass is
and Drs Ketelaar and Gorter),
Department of Pediatric opment of movement and low,4 and muscle strength is reduced.7-9
Physical Therapy and Exercise posture, causing activity Low levels on these fitness components
Physiology, University Hospital limitation, and are attributed to nonpro- may contribute to the difficulties in mo-
for Children and gressive disturbances that occurred in the tor activities most children with CP en-
Youth Het Wilhelmina developing fetal or infant brain.1 The mo- counter in daily life. Moreover, evidence
Kinderziekenhuis tor disorders of CP are often accompa- suggests that hypoactive children are more
(Mr Verschuren and likely to become physically sedentary
Drs Helders and Takken), and
nied by disturbances of sensation, cogni-
tion, communication, perception, and/or adults and that encouraging the develop-
Rudolf Magnus Institute of ment of physical activity habits in chil-
Neuroscience (Drs Ketelaar and behavior and/or by a seizure disorder.1 Im-
proving the ability to walk or perform other dren will help establish activity patterns
Gorter), University Medical
Center Utrecht, Partner of functional activities are often the pri- that continue into adulthood.10
Netchild, Network for mary therapeutic goals for children with
Childhood Disability Research CP.2 Because of existing impairments, For editorial comment
(Mr Verschuren and
Drs Ketelaar and Gorter), and
many children and adolescents with CP see page 1104
Julius Centre for Health have difficulty with activities such as walk-
Sciences and Primary Care ing independently, negotiating stairs, run- In general, aerobic capacity, anaero-
(Dr Uiterwaal), Utrecht, ning, or navigating safely over uneven ter- bic capacity, and muscle strength can be
the Netherlands. rain.3 Additionally, children with CP have trained in typically developing children of
(REPRINTED) ARCH PEDIATR ADOLESC MED/ VOL 161 (NO. 11), NOV 2007 WWW.ARCHPEDIATRICS.COM
1075
2007 American Medical Association. All rights reserved.
Downloaded From: http://archpedi.jamanetwork.com/ by a Purdue University User on 05/26/2015
all ages.11-13 Studies of the effects of lower limb exercises cated to the training group or the control group. An indepen-
in children with CP have demonstrated an increase in dent off-site researcher not involved in the assessments used a
muscle strength and function,7,14-16 as well as in aerobic concealed method for allocation. The children in the control
capacity,17,18 while no negative effects on spasticity or ab- group received their usual rehabilitation care. Because this might
affect functional gains among participants, provided care was
normal movements have been reported.14,15,19,20 To date,
tracked from the medical progress records. Usual care ranged
none of the training programs in children with CP have from no treatment to various therapeutic approaches. There was
focused on anaerobic capacity, which is important be- no difference in usual care between both groups.
cause almost all daily childhood activities are more short-
term (15 seconds) and high intensity than long- TRAINING PROGRAM
term.21,22
Activities of daily childhood life consist of well- We developed a functionally based exercise program that was
balanced aerobic, anaerobic, and muscle strength com- easily implemented in clinical practice. This program consisted
ponents. The principle of specificity of learning states that of 8 standardized aerobic exercises that lasted 3 to 6 minutes and
learning is optimized by practice that approximates the 8 standardized anaerobic exercises that lasted 20 to 30 seconds.
target skill.23 To date, we know of no study that trained All children, regardless of their age or GMFCS level, performed
the aerobic and anaerobic fitness components as well as the same exercises during the program. The task-specific exer-
muscle strength in task-specific, functional activities in cises, such as running and changing direction of the body abruptly,
children with CP. Therefore, we conducted a pragmatic step-ups, and negotiating stairs, were repeated throughout the
program and aimed to improve daily functioning. Each session
randomized controlled clinical trial to determine the ef- lasted 45 minutes. The total program consisted of a 5-minute
fects of a standardized 8-month exercise program with warm-up period; 25 to 35 minutes of functional aerobic, anaero-
an extra 4 months of follow-up after the training. bic, and muscle-strengthening exercises in circuit format; and a
Accordingly, the primary objective of this study was 5-minute cooldown. During the first 4 months, the main focus
to determine the specific (ie, aerobic and anaerobic ca- of the program was to improve aerobic capacity. After 4 months
pacity) effects of an exercise program in addition to usual (after the second measurement), when the participants were ex-
care at the end of the training period. Moreover, we in- pected to have improved their aerobic capacity, the focus shifted
vestigated the effects of this program on all International toward anaerobic capacity.
Classification of Functioning, Disability, and Health24 lev- The children in the training group received the exercise pro-
els and health-related quality of life (HRQOL) at the end gram in addition to their usual care. The participants in the train-
ing group trained in age-related groups (7-12 and 13-18 years
of the training period and at 4 months follow-up. of age) that were formed after the randomization and con-
sisted of 4 to 6 children. Consequently, each school had 2 dif-
METHODS ferent age-related groups that participated in the training ses-
sions. Standardized training sessions were led by 2 local pediatric
physiotherapists during school hours at school. All therapists
PARTICIPANTS
received the standardized fitness program training prior to the
start of the fitness program. The training group trained 2 days
Children and adolescents with CP were recruited from 4 schools
per week for 8 months.
for special education in the Netherlands. To be included, par-
ticipants had to be 7 to 20 years of age, diagnosed with spastic
CP, and classified at level I or II on the Gross Motor Function OUTCOME MEASURES ACCORDING
Classification System (GMFCS).25 Children older than 12 years TO THE INTERNATIONAL CLASSIFICATION
were classified using the same criteria as those used for 6- to OF FUNCTIONING, DISABILITY, AND HEALTH
12-year-olds. All children in the study were able to follow simple
verbal commands. They were all receiving rehabilitation ser- Primary outcome measures were aerobic and anaerobic capac-
vices at the time of the study. Participants were excluded if they ity measured at the end of the training period. Additional mea-
had had orthopedic surgery or neurosurgery and/or botuli- surements included agility, muscle strength, body mass index,
num toxin injection(s) within 6 months prior to study entry self-perception, gross motor function, participation, and HRQOL.
or cardiac or respiratory conditions that could negatively be
affected by exercise. Body Function
STUDY DESIGN Aerobic capacity was reflected by the achieved level on the 10-m
shuttle run test.26 This test requires children to walk or run be-
A pragmatic randomized controlled clinical trial was con- tween 2 markers delineating the respective course of 10 m at a
ducted between June 2005 and October 2006. The Institu- set incremental speed determined by a signal (every minute). The
tional Ethics Committee of the University Medical Center achieved level was recorded and used for analysis. Anaerobic ca-
Utrecht approved the study. Participating schools for special pacity was measured using mean power (measured in watts) de-
education were informed about the study and the inclusion and rived from the Muscle Power Sprint Test.27 For the Muscle Power
exclusion criteria. Based on clinical examination, pediatric phys- Sprint Test, the subjects were instructed to complete six 15-m
iatrists working in these schools referred suitable participants. runs at a maximum pace. Between each run, the subject was al-
The Dutch translation of the GMFCS25 was used to classify lowed a timed 10-second rest. Power output (measured in watts)
the children with CP into 2 groups based on their functional for each sprint was calculated. Agility was assessed by the 105-m
ability. Participants were randomly assigned to 2 groups using Sprint Test.27 Muscle strength of the lower extremities was mea-
a 4-block randomization protocol. Each block represented all sured with the 30-second repetition maximum.28
participants from 1 school. The groups within each block con- The body mass index was calculated as weight in kilo-
sisted of children classified at level I or II on the GMFCS.25 From grams divided by height in meters squared. Participants weight
each block and group, every participant was randomly allo- and height were measured using a standard protocol. Each child
(REPRINTED) ARCH PEDIATR ADOLESC MED/ VOL 161 (NO. 11), NOV 2007 WWW.ARCHPEDIATRICS.COM
1076
2007 American Medical Association. All rights reserved.
Downloaded From: http://archpedi.jamanetwork.com/ by a Purdue University User on 05/26/2015
was weighed to the nearest 100 g on electronic scales (Seca,
Hamburg, Germany). Height measurements were taken to the
nearest 0.5 cm while the child was standing with his or her back 86 Assessed for eligibility
against a wall.
We used the Self-Perception Profile for Children29 to evalu-
ate the self-concept of the children. This scale is designed to 1 Did not meet
assess childrens perceptions of themselves. We assessed the inclusion criteria
17 Declined to participate
domains of athletic competence, physical appearance, and global
perception of their worth or esteem as a person.
68 Randomized
Activity
In this study, gross motor function was assessed using dimen- 34 Assigned to receive 34 Assigned to receive
sions D and E of the Gross Motor Function Measure (GMFM),30 functional fitness usual care
training (training group) (control group)
which measures activities in a standing position and walking, run-
ning, and jumping, respectively. These dimensions were chosen
because they represent areas that many young people with CP 2 Discontinued study 1 Discontinued study
who are able to walk have difficulty with.7 (personal reasons) (personal reasons)
during baseline during baseline
measurements measurements
Participation
32 Completed treatment 33 Completed
The Childrens Assessment of Participation and Enjoyment and measurements at measurements at
T0, T1, and T2 T0, T1, and T2
(CAPE)31 was used to document change in how children and
youth participate in everyday activities outside mandated school
activities. The CAPE provides 3 levels of scoring: (1) overall 32 Completed 4-month 33 Completed 4-month
participation scores; (2) domain scores reflecting participa- follow-up follow-up
tion in formal and informal activities; and (3) scores reflecting
participation in 5 types of activity (recreational, active physi-
cal, social, skill-based, and self-improvement activities). The 32 Included in primary 33 Included in primary
intensity scores reflect the average amount of time that a child analysis analysis
spends participating in different activities. The intensity scores
of all types of activity were measured.
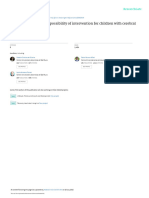
Figure 1. Flow of participants through the trial. T0 indicates baseline;
Health-Related Quality of Life T1, after 4 months; T2, after 8 months.
The TNO-AZL Questionnaire for Childrens Health-Related
Quality of Life (TACQOL) is a generic, multidimensional in- All data analyses were carried out according to a preestab-
strument.32 It asks about health problems in the past few weeks lished analysis plan and were performed according to the in-
using a 3-point Likert scale and about the emotional response tention-to-treat principle. To assess the effects of training as
to these problems on a 4-point scale. This instrument con- compared with standard care, we used repeated-measures analy-
tains 7 scales: (1) pain and symptoms, (2) basic motor func- sis of variance (group [2]time [3]) with repeated aerobic and
tioning, (3) autonomy, (4) cognitive functioning, (5) social func- anaerobic capacity measures as dependent variables and treat-
tioning, (6) global positive emotional functioning, and (7) global ment group as an independent variable. We used the same analy-
negative emotional functioning. We used the TACQOL Par- sis to assess our secondary objective. In case of violation of the
ent Form (TACQOL-PF) because we expected that a part of sphericity assumption, we used the Greenhouse-Geisser cor-
the participants were too young or too low functioning to com- rection.
plete the TACQOL themselves. To assess the effects during and after the fitness program as
To reduce bias, 8 assessors who were not the treating thera- compared with control treatment effects, repeated-measures
pist and who were blinded for the treatment modality under- analysis of variance (group [2]time [4]) with repeated con-
took the testing without review of previous scores. Prior to data trasts was used. Violations of assumptions were checked in all
collection, the assessors had formal training and were given writ- cases.
ten instructions in the application and scoring of all tests and The level was set at .05. Data were analyzed using SPSS,
measurements. version 13.0 (SPSS Inc, Chicago, Illinois).
Assessments were performed at baseline, after 4 months, and
directly after the 8 months of the intervention period in both
groups. There was a follow-up assessment with the same mea- RESULTS
sures in both groups at 12 months after baseline.
PARTICIPANT FLOW
STATISTICAL ANALYSIS
Age-eligible participants were recruited from July 2005
The sample size for the trial was determined by the most de-
manding hypothesis to detect effects of treatment on aerobic
to September 2005. Figure 1 shows the participant flow
capacity. The sample size was calculated from data for the 10-m from initial recruitment to assessment after training and
shuttle run test,26 with a significance level of .05, a d of 0.65, follow-up (October 2006). A total of 86 participants were
and a power of 80%. Therefore, 30 participants were required assessed for eligibility for the study. One of the children
for each group. To compensate for dropouts, we planned to en- did not meet the inclusion criteria, 9 of the eligible par-
roll 35 patients per group. ticipants did not take part for logistical reasons (year of
(REPRINTED) ARCH PEDIATR ADOLESC MED/ VOL 161 (NO. 11), NOV 2007 WWW.ARCHPEDIATRICS.COM
1077
2007 American Medical Association. All rights reserved.
Downloaded From: http://archpedi.jamanetwork.com/ by a Purdue University User on 05/26/2015
Table 1. Baseline Characteristics of the Participants 9.0
A
Achieved Level on the 10-m Shuttle Run Test, min
8.5
Training Group Control Group
(n = 34) (n = 34) 8.0
Demography 7.5
Age, y, mean (SD) 11.6 (2.5) 12.7 (2.7) 7.0
Male/female, No. 20/14 24/10
6.5
Anthropometry, mean (SD)
Body height, cm 148.0 (17.5) 154.6 (18.4) 6.0
Body weight, kg 44.7 (16.5) 48.4 (17.8)
5.5
BMI 19.8 (4.1) 19.6 (4.1)
Cerebral palsy, classification and 5.0
distribution, No. (%) Training group
4.5 Control group
GMFCS25 level I 24 (71) 23 (68)
GMFCS level II 10 (29) 11 (32) 4.0
Unilateral 23 (68) 22 (65) T0 T1 T2
Bilateral 11 (32) 12 (35)
Aerobic capacity, mean (SD)
Level on shuttle run test, min 6.2 (3.1) 7.6 (4.8) 140
B
Anaerobic capacity, mean (SD)
130
Mean power, W 84.6 (78.6) 121.2 (88.1)
120
Abbreviations: BMI, body mass index (calculated as weight in kilograms
divided by height in meters squared); GMFCS, Gross Motor Function 110
Mean Power, W
Classification System.
100
90
their graduation), and 8 children and adolescents re-
fused to participate for unknown reasons. Sixty-eight pa- 80
tients and their parents gave written informed consent Training group
70
before entering the study and were randomized to either Control group
the control group or the training group. Baseline demo- 60
graphic and clinical characteristics of each group are listed T0 T1 T2
in Table 1. At baseline, there were no significant dif- Measurement
ferences between study groups. During baseline mea-
surements, 3 children (boys aged 11.3, 15.1, and 16.1 Figure 2. Profile plots for aerobic capacity (A) (P .001) and anaerobic
years) discontinued the study because of personal rea- capacity (B) (P = .004). P values are for the repeated-measures analysis of
sons, such as lack of motivation, and were lost to follow- variance (group [2] time [3]). T0 indicates baseline; T1, after 4 months;
T2, after 8 months.
up. These children completed the fitness measures but
did not complete most of the other measures. Sixty-five
participants completed the entire study. The median at- the overall, formal, physical, and skill-based activities of
tendance in exercise training was 56 of 60 sessions (93%), the CAPE.
with all children attending at least 85% of the training
sessions. During a training session, 1 child fell and frac- Health-Related Quality of Life
tured her radius; she missed 4 training sessions because
she was wearing a cast. For HRQOL, significant changes over time that differed
by group were found for the motor, autonomy, and cog-
EFFECTS OF TRAINING nition domains of the TACQOL-PF (Table 2). The con-
trasts between all measurements (at baseline, 4 months,
Body Function and 8 months) show that during the first 4 months of
the training period (focused on aerobic capacity) there
As shown in Figure 2, improvements on aerobic (38%) was a significant change in favor of the training group
and anaerobic capacity (25%) were found for the train- for aerobic capacity, agility, athletic competence, and
ing group. Moreover, as shown in Table 2, improve- GMFM dimension D (standing). Moreover, a similar
ments were found on agility (15%), muscle strength change was also found for overall, formal, physical, skill-
of the lower extremities (left and right side, 20% and based, and self-improvement activities as measured with
23%, respectively), and athletic competence on the Self- the CAPE. On the TACQOL-PF, significant changes in
Perception Profile for Children (11%). favor of the training group were found for the motor, au-
tonomy, cognition, and social domains during the first
Activity and Participation 4 months. No significant effects were observed for muscle
power.
A positive training effect was present for dimension D During the last 4 months of the training period (fo-
(standing) of the GMFM. For participation, there were cused on anaerobic capacity), we found an improve-
significant differences in favor of the training group on ment in the training group for aerobic capacity, anaero-
(REPRINTED) ARCH PEDIATR ADOLESC MED/ VOL 161 (NO. 11), NOV 2007 WWW.ARCHPEDIATRICS.COM
1078
2007 American Medical Association. All rights reserved.
Downloaded From: http://archpedi.jamanetwork.com/ by a Purdue University User on 05/26/2015
bic capacity, agility, muscle strength, and GMFM
dimension E (walking, running, and jumping). There was Table 2. Differences Between T0 and T2 Outcome Measures
no improvement on the CAPE. On the TACQOL-PF, the for the Training Group and Control Group
only significant change in favor of the training group was
Difference T0-T2,
for the autonomy domain. Mean (SD)
FOLLOW-UP EFFECTS AT 12 MONTHS Training Control P
Group Group Value a
Body function and structure
At follow-up (4 months after the training period), we
BMI 0.7 (2.1) 0.3 (1.1) .51
noted a significant difference in outcome measures, as Aerobic capacity: level on 10-m 2.4 (1.9) 0.4 (1.6) .001
measured with repeated contrasts between groups. The shuttle run test, min
training group reached levels that were similar to the lev- Anaerobic capacity: mean 20.4 (38.0) 4.8 (28.2) .004
els after 4 months of training; there was a decrease in aero- power, W
bic capacity (8.4%), anaerobic capacity (8.5%), agil- Agility: 10 5-m Sprint Test 4.5 (4.1) 0.2 (4.4) .001
Muscle strength left 6.9 (7.2) 1.9 (8.7) .001
ity (4.3%), muscle strength (left side, 4.4%; right side,
Muscle strength right 7.7 (9.0) 1.9 (10.0) .001
8.3%), and athletic competence (9.8%). The control Self-concept (SPPC29)
group remained stable on these measures. Significant dif- Athletic competence 2.0 (4.2) 1.3 (3.7) .005
ferences between groups were found at follow-up on di- Physical appearance 0.03 (4.4) 0.2 (4.4) .90
mension D (1.1% for the training group) of the GMFM Global perception of worth 0.5 (3.3) 1.0 (4.0) .20
and on the skill-based activities of the CAPE (20% for Gross motor function (GMFM30)
Dimension D (standing) 2.6 (5.4) 0.7 (5.1) .03
the training group). These measures remained stable in
Dimension E (walking, running, 1.5 (6.4) 0.9 (3.5) .27
the control group. For HRQOL, there were no signifi- and jumping)
cant differences between groups at follow-up. Participation (CAPE31)
Overall activities 0.0 (0.5) 0.4 (0.6) .002
Formal activities 0.2 (0.4) 0.4 (0.8) .001
COMMENT Informal activities 0.0 (0.7) 0.4 (0.7) .07
Recreational activities 0.2 (1.0) 0.4 (1.1) .69
To our knowledge, this is the first randomized multi- Physical activities 0.3 (0.8) 0.3 (0.7) .005
Social activities 0.1 (0.8) 0.4 (1.1) .12
center clinical trial studying the effects of an exercise pro-
Skill-based activities 0.2 (0.5) 0.6 (0.9) .001
gram with emphasis on movements of daily childhood Self-improvement activities 0.1 (0.9) 0.5 (0.8) .10
life, nowadays called functional exercises, combining Health-related quality of life
3 fitness elements (aerobic and anaerobic capacity and (TACQOL-PF32)
muscle strength) in a large number of participants with Pain and symptoms 0.4 (3.6) 1.0 (2.3) .30
CP. This study provides evidence that a group circuit- Basic motor functioning 2.1 (4.3) 1.7 (4.3) .001
Autonomy 0.5 (4.3) 0.2 (3.1) .02
training program can be an effective and feasible strat-
Cognitive functioning 0.9 (4.7) 0.2 (4.0) .04
egy for increasing both aerobic capacity and anaerobic Social functioning 0.7 (4.0) 0.0 (3.9) .13
capacity in young people with CP. Global positive emotions 0.3 (3.9) 0.1 (1.9) .25
To date, only 1 randomized controlled study investi- Global negative emotions 0.7 (2.9) 0.0 (1.7) .15
gating the efficacy of aerobic training in children with
CP has been published.18 After an aerobic training pro- Abbreviations: BMI, body mass index (calculated as weight in kilograms
gram of 9 months, observed improvements were 35% divided by height in meters squared); CAPE, Childrens Assessment of
Participation and Enjoyment; GMFM, Gross Motor Function Measure;
(4 sessions a week) and 21% (2 sessions a week) in aero- SPPC, Self-Perception Profile for Children; T0, baseline; T2, after 8 months;
bic capacity and there were no training-related improve- TACQOL-PF, TNO-AZL Questionnaire for Childrens Health-Related Quality of
ments in anaerobic capacity. Our study showed improve- Life Parent Form.
a P values are for the repeated-measures analysis of variance (group
ments of 38% in aerobic capacity and significant [2] time [3]).
improvements of 11% in anaerobic capacity in the sec-
ond 4 months of the exercise program when anaerobic
exercises were incorporated.
The main focus during the last 4 months of the fit- bic and anaerobic), there was a significant interaction
ness program was anaerobic capacity. The significant in- between groups in favor of the training group for agility.
teraction in favor of the training group during the last 4 The finding that training focus is not specifically related
months of training shows that a fitness training pro- to improvement of agility could be explained by the fact
gram with a predominantly anaerobic nature can im- that the children in the training group had more exercise
prove the anaerobic capacity of children with CP. These and were training at higher velocities than in general.
improvements also led to significant changes in muscle Our study also showed a significant increase in per-
strength (22%). Other studies focusing specifically on im- ceived athletic competence but no significant changes over
proving muscle strength have reported similar results af- time for physical appearance or global perception of worth.
ter training in children with CP.7,14-16 One randomized controlled trial that studied the effects
Children with CP often have difficulties changing of an exercise program on the self-concept of children
direction of the body abruptly or quickly shifting the di- with CP found a change in self-concept.33 The training
rection of movement without losing balance (agility). Dur- group did not increase to the same extent in some as-
ing both training periods, with different main foci (aero- pects of self-concept as the children in the control group.33
(REPRINTED) ARCH PEDIATR ADOLESC MED/ VOL 161 (NO. 11), NOV 2007 WWW.ARCHPEDIATRICS.COM
1079
2007 American Medical Association. All rights reserved.
Downloaded From: http://archpedi.jamanetwork.com/ by a Purdue University User on 05/26/2015
Another randomized study demonstrated an increase in CONCLUSIONS
self-concept of the children after training.34 Possible ex-
planations for these differences might be explained by An 8-month, standardized, functionally based exercise
differences in settings, the illness severity of the chil- program significantly improved physical fitness, the in-
dren included in either study, the length of the exercise tensity of activities, and HRQOL in children with CP when
program, and the type of exercises. These and other pos- added to standard care.
sible factors need to be studied.
Participation in everyday childhood activities plays an
important role in the development of a childs social rela- Accepted for Publication: May 24, 2007.
tionships and skills and also influences long-term mental Correspondence: Olaf Verschuren, BSc, PT, Rehabilita-
and physical health.31,35,36 Participation enables children to tion Centre De Hoogstraat, Rembrandtkade 10, 3583TM
explore their social, intellectual, emotional, communica- Utrecht, the Netherlands (o.verschuren@dehoogstraat
tive, and physical potential and is an important predictor .nl).
of future life satisfaction.37 Margalit38 and Stevenson et al39 Author Contributions: Study concept and design: Ver-
looked at children with CP and found significant limita- schuren, Ketelaar, Gorter, Helders, and Takken. Acquisi-
tions in participation. Law et al40 identified several child tion of data: Verschuren. Analysis and interpretation of data:
factors that affect participation, including that higher lev- Verschuren, Ketelaar, Gorter, Uiterwaal, and Takken. Draft-
els of physical function are associated with increased in- ing of the manuscript: Verschuren. Critical revision of the
tensity of participation. Therefore, it could be expected that manuscript for important intellectual content: Ketelaar,
involvement in an exercise program might lead to more per- Gorter, Helders, Uiterwaal, and Takken. Statistical analy-
manent changes in everyday physical activities that in turn sis: Verschuren, Ketelaar, Uiterwaal, and Takken. Ob-
might lead to maintenance of the fitness benefits. Based on tained funding: Verschuren, Ketelaar, and Gorter. Admin-
the findings of this study, we conclude that having a higher istrative, technical, and material support: Ketelaar and Gorter.
physical function does lead to an increased intensity of par- Study supervision: Ketelaar, Gorter, Helders, and Takken.
ticipation. Overall, formal, physical, and skill-based activi- Financial Disclosure: None reported.
ties were improved at the end of the training period. Un- Funding/Support: This research was supported by the
fortunately, most of these improvements were not Dr W. M. Phelps Foundation.
maintained at follow-up. In future studies, factors that may Disclaimer: The funding body did not participate in the
contribute to a positive long-term change in lifestyle hab- design and execution of the study; collection, manage-
its should be taken into account. ment, analysis, and interpretation of the data; or prepa-
Health-related quality of life is an important outcome ration, review, or approval of the manuscript.
of treatment for chronic conditions such as CP.41 This is, Additional Contributions: We gratefully acknowledge all
to our knowledge, the first study that assessed the effects children and their parents for participation. We thank the
of an exercise intervention program on the quality of life physical therapists and pediatric phsysiatrists in the re-
in children with CP. Improvements in HRQOL in favor habilitation centers in Breda, Goes, Utrecht, and Zwolle
of the training group were seen for 3 domains. The par- (all in the Netherlands) for treating the children and thank
ents of the children with CP noticed improvements for the research assistants Ilse Oosterom, BSc, Chantal Hiddink,
motor, autonomy, and cognition domains. BSc, Radmer Schalkx, BSc, Jose Ermers, BSc, Anneleen de
The amount of time spent in physical activity has de- Pagter, BSc, Heidi Vogels, BSc, Annelies Polman, BSc, and
creased markedly over the past decades.42 Our study shows Joep Janssen, BSc, for their time and help.
aerobic and anaerobic capacity, agility, and muscle
strength decreased during the intervention period in the REFERENCES
control group. Given this decline in fitness levels, chil-
dren and adolescents with CP are at risk of a sedentary 1. Bax M, Goldstein M, Rosenbaum P, et al. Proposed definition and classification
lifestyle that will continue throughout their lives.43 The of cerebral palsy, April 2005. Dev Med Child Neurol. 2005;47(8):571-576.
2. Shepherd R. Cerebral palsy. In: Shepherd R, ed. Physiotherapy in Paediatrics.
adverse effects of this decreased fitness may be reduced Oxford, England: Butterworth-Heinemann; 1995:110-144.
with involvement in a fitness program. 3. Styer-Acevedo J. Physical therapy for the child with cerebral palsy. In: Tecklin
The findings of this study suggest that the benefits that JS, ed. Pediatric Physical Therapy. 3rd ed. Philadelphia, PA: Lippincott Williams
children gained during training were only partially main- & Wilkins; 1999.
tained at follow-up. A decrease in fitness after an exer- 4. Lundberg A. Maximal aerobic capacity of young people with spastic cerebral palsy.
Dev Med Child Neurol. 1978;20(2):205-210.
cise training program in children with CP was previ- 5. Lundberg A. Longitudinal study of physical working capacity of young people
ously reported.18 It seems very difficult for children with with spastic cerebral palsy. Dev Med Child Neurol. 1984;26(3):328-334.
CP to maintain the gains of an exercise program. Con- 6. Parker DF, Carriere L, Hebestreit H, Bar-Or O. Anaerobic endurance and peak muscle
sequently, it can be concluded that children with CP must power in children with spastic cerebral palsy. Am J Dis Child. 1992;146(9):
1069-1073.
continue their training to maintain their fitness levels. 7. Damiano DL, Vaughan CL, Abel MF. Muscle response to heavy resistance exer-
Limited exercise and sport opportunities in their neigh- cise in children with spastic cerebral palsy. Dev Med Child Neurol. 1995;37
borhoods might impede transfer of the gains in fitness (8):731-739.
into extra participation in regular physical activities. Su- 8. Wiley ME, Damiano DL. Lower-extremity strength profiles in spastic cerebral palsy.
pervised training programs at schools or in the commu- Dev Med Child Neurol. 1998;40(2):100-107.
9. van den Berg-Emons RJ, van Baak MA, de Barbanson DC, Speth L, Saris WH.
nity might provide fitness training for children and ado- Reliability of tests to determine peak aerobic power, anaerobic power and iso-
lescents with CP. These possibilities need to be studied kinetic muscle strength in children with cerebral palsy. Dev Med Child Neurol.
in future research. 1996;38(12):1117-1125.
(REPRINTED) ARCH PEDIATR ADOLESC MED/ VOL 161 (NO. 11), NOV 2007 WWW.ARCHPEDIATRICS.COM
1080
2007 American Medical Association. All rights reserved.
Downloaded From: http://archpedi.jamanetwork.com/ by a Purdue University User on 05/26/2015
10. Powell KE, Dysinger W. Childhood participation in organized school sports and validity of data for 2 newly developed shuttle run tests in children with cerebral
physical education as precursors of adult physical activity. Am J Prev Med. 1987; palsy. Phys Ther. 2006;86(8):1107-1117.
3(5):276-281. 27. Verschuren O, Takken T, Ketelaar M, Gorter JW, Helders PJM. Reliability of run-
11. Mahon AD. Exercise training. In: Armstrong N, van Mechelen W, eds. Paediatric ning tests for measuring agility and anaerobic muscle power in children with ce-
Exercise Science and Medicine. New York, NY: Oxford University Press, Inc; 2000: rebral palsy. Pediatr Phys Ther. 2007;19(2):108-115.
201-211. 28. Verschuren O, Takken T, Ketelaar M, Gorter JW, Helders PJM. Functional strength
12. McManus AM, Armstrong N, Williams CA. Effect of training on the aerobic and assessment of the lower extremity in children with cerebral palsy [abstract]. Dev
anaerobic performance of prepubertal girls. Acta Paediatr. 1997;86(5):456- Med Child Neurol. 2006;48(suppl 106):31.
459. 29. Harter S. The Self-Perception Profile for Children. Denver, CO: University of Den-
13. Rotstein A, Dotan R, Bar-Or O, Tennenbaum G. Effect of training on anaerobic ver; 1985.
threshold, maximal aerobic power and anaerobic performance of preadolescent 30. Russell D, Rosenbaum P, Gowland C, et al. Gross Motor Function Manual. Hamil-
boys. Int J Sports Med. 1986;7(5):281-286. ton, ON, Canada: McMaster University; 1993.
14. MacPhail HEA, Kramer JF. Effect of isokinetic strength-training on functional abil- 31. King G, Law M, King S, et al. Childrens Assessment of Participation and Enjoy-
ity and walking efficiency in adolescents with cerebral palsy. Dev Med Child Neurol. ment (CAPE) and Preferences for Activities of Children (PAC). San Antonio, TX:
1995;37(9):763-775. Harcourt Assessment, Inc; 2004.
15. Damiano DL, Kelly LE, Vaughn CL. Effects of quadriceps femoris muscle strength- 32. Vogels T, Verrips GHW, Koopman HM, Theunissen NCM, Fekkes M, Kamphuis
ening on crouch gait in children with spastic diplegia. Phys Ther. 1995;75(8): RP. TACQOL Manual. Parent Form and Child Form . Leiden, the Netherlands:
658-667. Leiden Center for Child Health and Pediatrics; 2000.
16. Dodd KJ, Taylor NF, Graham HK. A randomized clinical trial of strength training 33. Dodd KJ, Taylor NF, Graham HK. Strength training can have unexpected effects
in young people with cerebral palsy. Dev Med Child Neurol. 2003;45(10):652- on the self-concept of children with cerebral palsy. Pediatr Phys Ther. 2004;
657. 16(2):99-105.
17. Parker DF, Carriere L, Hebestreit H, Salsberg A, Bar-Or O. Muscle performance 34. Darrah J, Wessel J, Nearinburg P, OConnor M. Evaluation of a community fit-
and gross motor function of children with spastic cerebral palsy. Dev Med Child ness program for adolescents with cerebral palsy. Pediatr Phys Ther. 1999;
Neurol. 1993;35(1):17-23. 11(1):18-23.
18. Van den Berg-Emons RJ, van Baak MA, Speth L, Saris WH. Physical training of 35. Simeonsson RJ, Carlson D, Huntington GS, McMillen JS, Brent JL. Students with
school children with spastic cerebral palsy: effects on daily activity, fat mass and disabilities: a national survey of participation in school activities. Disabil Rehabil.
fitness. Int J Rehabil Res. 1998;21(2):179-194. 2001;23(2):49-63.
19. Darrah J, Fan JS, Chen LC, Nunweiler J, Watkins B. Review of the effects of pro- 36. Larson RW, Verma S. How children and adolescents spend time across the world:
gressive resisted muscle strengthening in children with cerebral palsy: a clinical work, play, and developmental opportunities. Psychol Bull. 1999;125(6):701-
consensus exercise. Pediatr Phys Ther. 1997;9(1):12-17. 736.
20. Fowler EG, Ho TW, Nwigwe AI, Dorey FJ. The effect of quadriceps femoris muscle 37. Kinney WB, Coyle CP. Predicting life satisfaction among adults with physical
strengthening exercises on spasticity in children with cerebral palsy. Phys Ther. disabilities. Arch Phys Med Rehabil. 1992;73(9):863-869.
2001;81(6):1215-1223. 38. Margalit M. Leisure activities of cerebral palsied children. Isr J Psychiatry Relat
21. Bailey RC, Olsen J, Pepper SL, Porszasz J, Bartsow TJ, Cooper DM. The level Sci. 1981;18(3):209-214.
and tempo of childrens physical activities: an observational study. Med Sci Sports 39. Stevenson CJ, Pharoah POD, Stevenson R. Cerebral palsythe transition from
Exerc. 1995;27(7):1033-1041. youth to adulthood. Dev Med Child Neurol. 1997;39(5):336-342.
22. Rowland TW. The biological basis of physical activity. Med Sci Sports Exerc. 1998; 40. Law M, King G, King S, et al. Patterns of participation in recreational and leisure
30(3):392-399. activities among children with complex physical disabilities. Dev Med Child Neurol.
23. Schmidt RA, Wrisberg CA. Motor Learning and Performance. 3rd ed. Cham- 2006;48(5):337-342.
paign, IL: Human Kinetics Publishers; 2004. 41. Bjornson KF, McLaughlin JF. The measurement of health-related quality of life (HRQL)
24. Organization WH. ICF: International Classification of Functioning, Disability and in children with cerebral palsy. Eur J Neurol. 2001;8(suppl 5):183-193.
Health. Geneva, Switzerland: WHO; 2001. 42. Heath GW, Pratt M, Warren C, Kann L. Physical activity patterns in American high
25. Palisano R, Rosenbaum P, Walter S. The development and reliability of a sys- school students: results from the 1990 Youth Risk Behavior Survey. Arch Pedi-
tem to classify gross motor function in children with cerebral palsy. Dev Med atr Adolesc Med. 1994;148(11):1131-1136.
Child Neurol. 1997;39(4):214-223. 43. Longmuir P, Bar-Or O. Factors influencing the physical activity levels of youths
26. Verschuren O, Takken T, Ketelaar M, Gorter JW, Helders PJM. Reliability and with physical and sensory disabilities. Adapt Phys Educ Q. 2000;17(1):40-53.
Announcement
Trial Registration Required. In concert with the Inter-
national Committee of Medical Journal Editors (ICMJE),
Archives of Pediatrics and Adolescent Medicine will re-
quire, as a condition of consideration for publication, reg-
istration of all trials in a public trials registry (such as http://
ClinicalTrials.gov). Trials must be registered at or before
the onset of patient enrollment. This policy applies to any
clinical trial starting enrollment after July 1, 2005. For trials
that began enrollment before this date, registration will
be required by September 13, 2005, before considering the
trial for publication. The trial registration number should
be supplied at the time of submission.
For details about this new policy, and for information
on how the ICMJE defines a clinical trial, see the edito-
rials by DeAngelis et al in the September 8, 2004 (2004;
292:1363-1364) and June 15, 2005 (2005;293:2927-
2929) issues of JAMA. Also see the Instructions to Authors
on our Web site: www.archpediatrics.com.
(REPRINTED) ARCH PEDIATR ADOLESC MED/ VOL 161 (NO. 11), NOV 2007 WWW.ARCHPEDIATRICS.COM
1081
2007 American Medical Association. All rights reserved.
Downloaded From: http://archpedi.jamanetwork.com/ by a Purdue University User on 05/26/2015
S-ar putea să vă placă și
- (129 136) V9N5PTDocument8 pagini(129 136) V9N5PTAqila NurÎncă nu există evaluări
- Cureus 0014 00000030571Document11 paginiCureus 0014 00000030571zizee61Încă nu există evaluări
- Strength Training Adolescent Learners With Cerebral Palsy: Randomized ControlledDocument9 paginiStrength Training Adolescent Learners With Cerebral Palsy: Randomized ControlledtiaraaaindahÎncă nu există evaluări
- Research in Developmental DisabilitiesDocument12 paginiResearch in Developmental DisabilitiesRun CapÎncă nu există evaluări
- sergii,+Journal+editor,+03Hamed Articulo 2Document8 paginisergii,+Journal+editor,+03Hamed Articulo 2anye daniela gilÎncă nu există evaluări
- Exercise Interventions Improve Postural Control in Children With Cerebral Palsy: A Systematic ReviewDocument17 paginiExercise Interventions Improve Postural Control in Children With Cerebral Palsy: A Systematic ReviewEmad Eldin Mohamed AbdelatiefÎncă nu există evaluări
- Pa Tikas 2006Document8 paginiPa Tikas 2006tiaraaaindahÎncă nu există evaluări
- Develop Med Child Neuro - 2014 - Dewar - Exercise Interventions Improve Postural Control in Children With Cerebral Palsy ADocument17 paginiDevelop Med Child Neuro - 2014 - Dewar - Exercise Interventions Improve Postural Control in Children With Cerebral Palsy AEvelyn_D_az_Ha_8434Încă nu există evaluări
- TFM 4Document8 paginiTFM 4Miguel de VivarÎncă nu există evaluări
- Comparing The Effects of Aquatic and Land-Based Exercises On Balance and Walking in Spastic Diplegic Cerebral Palsy ChildrenDocument8 paginiComparing The Effects of Aquatic and Land-Based Exercises On Balance and Walking in Spastic Diplegic Cerebral Palsy ChildrenJorgeAdalbertoCabralPerezÎncă nu există evaluări
- SUMBER Eom2014Document6 paginiSUMBER Eom2014Felix Valerian HalimÎncă nu există evaluări
- Journal Pone 0208792Document12 paginiJournal Pone 0208792mariskaÎncă nu există evaluări
- Effects of Hippotherapy and Therapeutic Horseback Riding On Postural Control or Balance in Children With Cerebral Palsy: A Meta-AnalysisDocument8 paginiEffects of Hippotherapy and Therapeutic Horseback Riding On Postural Control or Balance in Children With Cerebral Palsy: A Meta-AnalysisEduardo EstevamÎncă nu există evaluări
- Papn MS Id 000156Document7 paginiPapn MS Id 000156niekoÎncă nu există evaluări
- Physiotherapy: J o U R N A L o FDocument10 paginiPhysiotherapy: J o U R N A L o FImran TarmiziÎncă nu există evaluări
- 2.effect of Core Stability Exercises OnDocument8 pagini2.effect of Core Stability Exercises OnDaniela NevesÎncă nu există evaluări
- Tdcs Inglês 1Document8 paginiTdcs Inglês 1Augusto ManoelÎncă nu există evaluări
- TFM 1Document10 paginiTFM 1Miguel de VivarÎncă nu există evaluări
- Comparison of Different Therapy Approaches in Children With Down SyndromeDocument6 paginiComparison of Different Therapy Approaches in Children With Down SyndromeRosy OktaridaÎncă nu există evaluări
- Fragala Pinkham2013Document10 paginiFragala Pinkham2013Beatriz Garcia-PoggioÎncă nu există evaluări
- Aricol IMC Si EscaladaDocument5 paginiAricol IMC Si EscaladacristinaelenazahariaÎncă nu există evaluări
- The Effects of Kinesio Taping On Body Functions and Activity in Unilateral Spastic Cerebral Palsy: A Single-Blind Randomized Controlled TrialDocument8 paginiThe Effects of Kinesio Taping On Body Functions and Activity in Unilateral Spastic Cerebral Palsy: A Single-Blind Randomized Controlled TrialEddy Lanang'e JagadÎncă nu există evaluări
- Effectiveness of Proprioceptive Training Over Strength Training in Improving The Balance of Cerebral Palsy Children With Impaired BalanceDocument14 paginiEffectiveness of Proprioceptive Training Over Strength Training in Improving The Balance of Cerebral Palsy Children With Impaired BalanceDr. Krishna N. SharmaÎncă nu există evaluări
- Original Article: Effects of Neurodevelopmental Therapy On Gross Motor Function in Children With Cerebral PalsyDocument6 paginiOriginal Article: Effects of Neurodevelopmental Therapy On Gross Motor Function in Children With Cerebral PalsyIkhwatul FitriÎncă nu există evaluări
- A Community-Based Strength Training Programme IncreasesDocument10 paginiA Community-Based Strength Training Programme IncreasesMaryuri PortillaÎncă nu există evaluări
- TFM 3Document9 paginiTFM 3Miguel de VivarÎncă nu există evaluări
- Schenkman: Exercise To Improve Spinal Flexibility and Function For People With Parkinson's Disease: A Randomized, Controlled TrialDocument10 paginiSchenkman: Exercise To Improve Spinal Flexibility and Function For People With Parkinson's Disease: A Randomized, Controlled TrialGerman BuyattiÎncă nu există evaluări
- Jurnal Propriosepsi GeriatriDocument9 paginiJurnal Propriosepsi GeriatriIra AdventiaÎncă nu există evaluări
- Effect of Core Stability Exercises and Treadmill Training On Balance in Children With Down Syndrome - Randomized Controlled TrialDocument10 paginiEffect of Core Stability Exercises and Treadmill Training On Balance in Children With Down Syndrome - Randomized Controlled TrialGayuh Candra BuanaÎncă nu există evaluări
- 51 55Document5 pagini51 55SuniÎncă nu există evaluări
- 2013-Haugen-Valores Normativos Sit and ReachDocument7 pagini2013-Haugen-Valores Normativos Sit and ReachChuleÎncă nu există evaluări
- Reduced CooperDocument9 paginiReduced CooperticsneyplusÎncă nu există evaluări
- Water-Versus Land-Based Exercise Effects On Physical Fitness in Older WomenDocument8 paginiWater-Versus Land-Based Exercise Effects On Physical Fitness in Older WomenHONGJY100% (1)
- J Jsams 2018 11 029Document5 paginiJ Jsams 2018 11 029nidhi wahiÎncă nu există evaluări
- Renang 1 PDFDocument13 paginiRenang 1 PDFD KaÎncă nu există evaluări
- Active Play Exercise Intervention in Children With Asthma: A PILOT STUDYDocument9 paginiActive Play Exercise Intervention in Children With Asthma: A PILOT STUDYKrisna ajiÎncă nu există evaluări
- Investigeting The Effects of Standing Training On Body Functions and Activity For Nonambulatory Children With MyelomeningoceleDocument6 paginiInvestigeting The Effects of Standing Training On Body Functions and Activity For Nonambulatory Children With MyelomeningoceleMutiarahmiÎncă nu există evaluări
- Effectiveness of Sensory Integration Therapy (Vestibular & Proprioception Input) On Gross Motor Functioning in Developmental Delayed and Spastic Diplegic CP ChildrenDocument6 paginiEffectiveness of Sensory Integration Therapy (Vestibular & Proprioception Input) On Gross Motor Functioning in Developmental Delayed and Spastic Diplegic CP ChildrenYanuar Adi SanjayaÎncă nu există evaluări
- Cia 11 749Document6 paginiCia 11 749Edward KenwayÎncă nu există evaluări
- Artritis Idiopatica JuvenilDocument12 paginiArtritis Idiopatica JuvenilJhos_Leon15Încă nu există evaluări
- Canadian Society For Exercise Physiology Position Paper - Resistance Training in Children and AdolescentsDocument15 paginiCanadian Society For Exercise Physiology Position Paper - Resistance Training in Children and AdolescentsDian Permata PutraÎncă nu există evaluări
- Lowe 2015Document9 paginiLowe 2015ﻱﺪﺢ ﺁﻏﻦﻎÎncă nu există evaluări
- Rehabilitacion en NiñosDocument6 paginiRehabilitacion en NiñosYasser SaraviaÎncă nu există evaluări
- An Aquatic Physical Therapy Program at A Pediatric.12Document11 paginiAn Aquatic Physical Therapy Program at A Pediatric.12Ruxandra NicaÎncă nu există evaluări
- Content ServerDocument9 paginiContent ServerKennie RamirezÎncă nu există evaluări
- HTTPS-::WWW Nature Com:articles:pr2003504Document8 paginiHTTPS-::WWW Nature Com:articles:pr2003504LucyFloresÎncă nu există evaluări
- Experimental Gerontology: Contents Lists Available atDocument9 paginiExperimental Gerontology: Contents Lists Available atGorkaBuesaÎncă nu există evaluări
- Updated Chap 1 and 2Document38 paginiUpdated Chap 1 and 2Jemie JaleaÎncă nu există evaluări
- Impact of Aquatic Exercise Program On Muscle Tone in Spastic Hemiplegic Children With Cerebral PalsyDocument7 paginiImpact of Aquatic Exercise Program On Muscle Tone in Spastic Hemiplegic Children With Cerebral Palsyilona ilincaÎncă nu există evaluări
- Sensorimotor Training For BalanceDocument7 paginiSensorimotor Training For BalanceAgatha SharmaÎncă nu există evaluări
- Postural Orientation During Standing in Children With Bilateral Cerebral PalsyDocument7 paginiPostural Orientation During Standing in Children With Bilateral Cerebral PalsyRaul Vieira VillarroelÎncă nu există evaluări
- Therapeutic Interventions in Cerebral Palsy: Dilip R. PatelDocument5 paginiTherapeutic Interventions in Cerebral Palsy: Dilip R. PatelclikgoÎncă nu există evaluări
- Evidencias VojtaDocument9 paginiEvidencias VojtaRommel AndresÎncă nu există evaluări
- Basso Etal++2015Document11 paginiBasso Etal++2015Violeta Aguayo MüllerÎncă nu există evaluări
- The Carry-Over Effect of An Aquatic-Based Intervention in Children With Cerebral PalsyDocument8 paginiThe Carry-Over Effect of An Aquatic-Based Intervention in Children With Cerebral PalsyFabrício MarquesÎncă nu există evaluări
- Pediatrik Denge Olcegi ToadDocument7 paginiPediatrik Denge Olcegi ToadFarzaneh CadirciÎncă nu există evaluări
- Pedia TriDocument6 paginiPedia TriRIZHAN ATHAYAÎncă nu există evaluări
- Efficacy of Botulinum Toxin A in Children With Cerebral Palsy in Gross MotorDocument10 paginiEfficacy of Botulinum Toxin A in Children With Cerebral Palsy in Gross MotorShawna ChiewÎncă nu există evaluări
- Stretch PDFDocument14 paginiStretch PDFCarolina B. SánchezÎncă nu există evaluări
- Exercise Physiology for the Pediatric and Congenital CardiologistDe la EverandExercise Physiology for the Pediatric and Congenital CardiologistÎncă nu există evaluări
- Terapia de Habla y Lenguaje para Mejorar La Comunicación de Niños y Adolescentes Con Parálisis CerebralDocument50 paginiTerapia de Habla y Lenguaje para Mejorar La Comunicación de Niños y Adolescentes Con Parálisis CerebralValentina SiegmundÎncă nu există evaluări
- Exercise Training Program in Children and Adolescents With Cerebral PalsyDocument7 paginiExercise Training Program in Children and Adolescents With Cerebral PalsyValentina SiegmundÎncă nu există evaluări
- Investigation of Practices To Support The Complex Communication Needs of Children With Hearing Impairment and Cerebral Palsy in A Rural District of Kenya: A Case SeriesDocument14 paginiInvestigation of Practices To Support The Complex Communication Needs of Children With Hearing Impairment and Cerebral Palsy in A Rural District of Kenya: A Case SeriesValentina SiegmundÎncă nu există evaluări
- Series Causa EfectoDocument9 paginiSeries Causa EfectoCamilofonoÎncă nu există evaluări
- Investigation of Practices To Support The Complex Communication Needs of Children With Hearing Impairment and Cerebral Palsy in A Rural District of Kenya: A Case SeriesDocument14 paginiInvestigation of Practices To Support The Complex Communication Needs of Children With Hearing Impairment and Cerebral Palsy in A Rural District of Kenya: A Case SeriesValentina SiegmundÎncă nu există evaluări
- Preschoolers Can Recognize Violations of The Gricean MaximsDocument9 paginiPreschoolers Can Recognize Violations of The Gricean MaximsValentina SiegmundÎncă nu există evaluări
- Advances in Psychedelic TherapyDocument22 paginiAdvances in Psychedelic TherapylgessaÎncă nu există evaluări
- Yolanda Paramitha ProceedingDocument6 paginiYolanda Paramitha Proceedingyolanda paramithaÎncă nu există evaluări
- Assignment Model: Suraj MaratheDocument20 paginiAssignment Model: Suraj Maratheutpal364Încă nu există evaluări
- Salmonella SPP.: Version of RecordDocument36 paginiSalmonella SPP.: Version of RecordkupcovalilaÎncă nu există evaluări
- The Relationship Between Customer Satisfaction and Customer Loyalty Among Customers of Luxury ProductsDocument15 paginiThe Relationship Between Customer Satisfaction and Customer Loyalty Among Customers of Luxury ProductsKris Lopez0% (1)
- PP-Selection-Guide Hyujdi PDFDocument20 paginiPP-Selection-Guide Hyujdi PDFparijat patelÎncă nu există evaluări
- Regression ExampleDocument7 paginiRegression ExamplerasnimÎncă nu există evaluări
- Role of 360-Degree Feedback From An Employee Perspective at British Petroleum, Cranford.Document38 paginiRole of 360-Degree Feedback From An Employee Perspective at British Petroleum, Cranford.Anthony GeorgeÎncă nu există evaluări
- Sociolinguistics Help Us To Develop A Better Understanding of Society and Language 1Document6 paginiSociolinguistics Help Us To Develop A Better Understanding of Society and Language 1Ikram KhanÎncă nu există evaluări
- Professional Goals Strengths and Areas For Further ImprovementDocument2 paginiProfessional Goals Strengths and Areas For Further Improvementapi-317272307100% (1)
- Easa 145 Safety PDFDocument53 paginiEasa 145 Safety PDFZain HasanÎncă nu există evaluări
- Experimental and Quasi Experimental Designs For Research PDFDocument2 paginiExperimental and Quasi Experimental Designs For Research PDFAmy100% (1)
- Reviewer in Practical Research 2Document3 paginiReviewer in Practical Research 2Elmo Vincent Bernardo MurosÎncă nu există evaluări
- Swati Tripathi: Jayoti Vidyapeeth Womens University, JaipurDocument18 paginiSwati Tripathi: Jayoti Vidyapeeth Womens University, JaipurdrsurendrakumarÎncă nu există evaluări
- Hris Practice in BangladeshDocument7 paginiHris Practice in BangladeshnaimÎncă nu există evaluări
- Harvey (2021) Reliability Analysis Guide PreprintDocument13 paginiHarvey (2021) Reliability Analysis Guide Preprintjim alexÎncă nu există evaluări
- Web Analytics 20 SEMJDocument5 paginiWeb Analytics 20 SEMJThk WaitsÎncă nu există evaluări
- Field Study 2Document72 paginiField Study 2Janella DasaÎncă nu există evaluări
- Doctoral Writing and Inquiry Into Research Assignment 1Document16 paginiDoctoral Writing and Inquiry Into Research Assignment 1General L. JohnstonÎncă nu există evaluări
- For Teachers Only: Comprehensive Examination in LatinDocument4 paginiFor Teachers Only: Comprehensive Examination in LatinJasonWestbrookÎncă nu există evaluări
- Sampling Distribution of Sample Means (Gorospe)Document21 paginiSampling Distribution of Sample Means (Gorospe)Margie YbañezÎncă nu există evaluări
- 2 - 23 - A Survey of Vision-Language Pre-Training From The Lens of Multimodal Machine TranslationDocument10 pagini2 - 23 - A Survey of Vision-Language Pre-Training From The Lens of Multimodal Machine TranslationPhạm Thanh TrườngÎncă nu există evaluări
- Scientific Inquiry Vs Engineering DesignDocument1 paginăScientific Inquiry Vs Engineering DesignMahfud AfandiÎncă nu există evaluări
- PresedexDocument1 paginăPresedexapi-439573239Încă nu există evaluări
- Organisational Behaviour: Faculty: Dr. Vinit Singh ChauhanDocument5 paginiOrganisational Behaviour: Faculty: Dr. Vinit Singh ChauhanSagar PanchalÎncă nu există evaluări
- Part 1 - Unit 7 of 7 Procedures, Analysis, Conclusions, and DocumentationDocument14 paginiPart 1 - Unit 7 of 7 Procedures, Analysis, Conclusions, and DocumentationMuhammad Shahzad KhanÎncă nu există evaluări
- Classroom Assessment in The K To 12 Basic Education ProgramDocument50 paginiClassroom Assessment in The K To 12 Basic Education ProgramMaria Luisa Gentoleo QuipitÎncă nu există evaluări
- How To Write A Research IntroductionDocument29 paginiHow To Write A Research IntroductionFerdinand VillanuevaÎncă nu există evaluări
- Fisheries Situation Report, April To June 2021 - 0Document27 paginiFisheries Situation Report, April To June 2021 - 0Jack Robert LabradorÎncă nu există evaluări