Documente Academic
Documente Profesional
Documente Cultură
Urinary Incontinence in The Older Adult: by Kristen Cook, Pharm.D., BCPS and Linda M. Sobeski, Pharm.D., BCPS
Încărcat de
Nurul HafizaTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Urinary Incontinence in The Older Adult: by Kristen Cook, Pharm.D., BCPS and Linda M. Sobeski, Pharm.D., BCPS
Încărcat de
Nurul HafizaDrepturi de autor:
Formate disponibile
Urinary Incontinence
in the Older Adult
By Kristen Cook, Pharm.D., BCPS; and
Linda M. Sobeski, Pharm.D., BCPS
Reviewed by Gregory J. Hughes, Pharm.D., BCPS, CGP; and Helen M. LoSasso, Pharm.D., BCPS
Learning Objectives than in men until 80 years of age, after which UI rates are
similar. Despite its high prevalence, up to one-half of cases
1. Evaluate symptoms to accurately classify a patient
with urinary incontinence (UI). may not be reported because individuals with UI may not
2. Apply an understanding of the pathophysiology and seek medical intervention. Embarrassment and the per-
risk factors for UI to patient care. ception that UI is an expected consequence of aging are
3. Evaluate the most recent clinical evidence for pharma- common factors in lack of treatment.
cologic and nonpharmacologic treatment of UI. Urinary incontinence is categorized according to
4. Design a patient-specific treatment plan to achieve pathophysiology and clinical presentation. The four main
optimal outcomes in an elderly patient with UI. categories are (1) stress urinary incontinence (SUI), (2)
5. Assess for reversible causes in the patient with UI. urge urinary incontinence (UUI), (3) overflow inconti-
6. Analyze the risks and benefits of using UI medica- nence, and (4) functional incontinence. Mixed types of
tions in patients with dementia. incontinence are common and may complicate diagnosis
and treatment because of overlapping symptoms.
Studies have found that UI significantly affects psy-
Introduction chological well-being and health carerelated quality of
The International Continence Society defines urinary life. Urinary incontinence may impair sexual function,
incontinence (UI) as the involuntary loss of urine. In both restrict activities, interfere with interpersonal relationships,
men and women, age is a consistently reported risk factor decrease self-esteem, increase caregiver burden, increase
for UI; however, it is not considered a normal consequence financial burden, and cause anxiety or depression. It is a
of aging. Overall, UI affects up to 30% of community- common precipitant of institutionalization in older adults.
dwelling older adults and more than 50% of nursing home Because of current demographic trends, UI is an increas-
residents. It is about 23 times more common in women ingly common medical and socioeconomic problem.
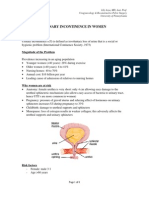
Baseline Knowledge Statements
Readers of this chapter are presumed to be familiar with the following:
Urinary tract anatomy and physiology
Mechanism of action and basic pharmacology of drugs used to treat UI
Effect of UI on quality of life
Basic pathophysiology of the different types of UI
Treatment of benign prostatic hyperplasia
Additional Readings
The following free resources are available for readers wishing additional background information on this topic.
Lucas MG, Bedretdinova D, Bosch JLHR, et al.; for the European Association of Urology. Guidelines on Urinary
Incontinence, 2013.
Lucas MG, Bosch RJL, Burkhard FC, et al.; for the European Association of Urology. EAU Guidelines on Assessment
and Nonsurgical Management of Urinary Incontinence, 2012.
PSAP 2013 Special Populations 3 Urinary Incontinence in the Older Adult
fills without leakage while the parasympathetic nervous
Abbreviations in This Chapter system is inhibited. As the bladder fills and pressure rises,
BPH Benign prostatic hyperplasia increased parasympathetic tone causes the detrusor mus-
CVA Cerebrovascular accident cle to contract and the bladder to empty. The primary
LUTS Lower urinary tract symptoms neurotransmitter involved in bladder contraction is ace-
OAB Overactive bladder tylcholine, which acts at muscarinic receptors. Muscarinic
PMR Pelvic muscle rehabilitation 2 receptors are usually found in the lower urinary tract;
PVR Post void residual however, most UI drug therapy targets the muscarinic 3
RCT Randomized controlled trial receptors, which are thought to have a larger role in blad-
SNS Sacral nerve stimulation der emptying. -Adrenergic receptors are involved in
SUI Stress urinary incontinence urethral smooth muscle control.
UI Urinary incontinence Several classifications of incontinence are based on the
UTI Urinary tract infection underlying problem in the lower urinary tract. Although
UUI Urge urinary incontinence the terms overactive bladder (OAB) and urge incontinence
are used interchangeably, they describe two different con-
ditions. Overactive bladder is a symptom syndrome that
includes frequency, urgency, and nocturia. These can all
Pathophysiology occur with or without urge incontinence. Although the
Continence requires both an appropriately functioning definitions are distinct, these two conditions are treated
lower urinary tract and the physical and cognitive ability in the same manner. Table 1-1 outlines the main classifica-
to use a toilet. Function of the lower urinary tract is com- tions of UI.
plicated and not completely understood. In individuals Age-related changes within the urinary tract contribute
with normal physiology, activation of the sympathetic ner- to the increased prevalence of UI in the older population.
vous system aids in closing the bladder neck; the bladder These changes include decreases in bladder compliance,
Table 1-1. Types of Urinary Incontinence
Type Definition Common Causes
Stress Involuntary loss of urine (small amounts) with Weak pelvic floor muscles (childbirth, pregnancy,
increasing intraabdominal pressure (e.g., coughing, menopause)
laughing, exercise) Bladder outlet or urethral sphincter weakness
Post-urologic surgery
Urge Leakage of urine (can be large volumes) because of Detrusor overactivity, either isolated or associated with
inability to delay voiding after sensation of bladder one or more of the following:
fullness is perceived Local genitourinary conditions (e.g., tumors, stones,
diverticula, outflow obstruction)
CNS disorder (e.g., stroke, parkinsonism, dementia,
spinal cord injury)
Overflow Leakage of urine (small amounts) caused by either Anatomic obstruction by prostate, stricture, cystocele
mechanical forces on an overdistended bladder Acontractile bladder associated with diabetes or spinal
(resulting in stress leakage) or other effects of cord injury
urinary retention on bladder and sphincter function
Neurogenic associated with multiple sclerosis or other
(contributing to urge leakage)
spinal cord lesions
Medication effect (see Table 1-2)
Functional Urinary accidents associated with the inability to Severe dementia or other neurologic disorder
toilet because of impairment of cognitive and or Psychological factors such as depression and hostility
physical functioning, psychological unwillingness,
or environmental barriers
CNS = central nervous system.
Adapted with permission from Halter JB, Ouslander JG, Tinetti ME, et al. Hazzards Geriatric Medicine and Gerontology, 6th ed. New York:
McGraw-Hill, 2009:720.
PSAP 2013 Special Populations 4 Urinary Incontinence in the Older Adult
bladder capacity, urethral closing pressure, and ability patients continue to have UI at 12 months after a CVA.
to postpone voiding; increases in involuntary detrusor A case-control analysis noted a higher incidence of UI in
contractions, post void residual (PVR), and frequency community-dwelling individuals with CVA (28%) than in
of voiding; and weakened pelvic floor musculature (in those without stroke (20%) (Divani 2011). Risk factors for
women) and prostatic enlargement (in men). In addition UI after stroke include hemiparesis, depression, impaired
to age-associated factors, chronic disease burden can con- cognition, age older than 75 years, dysphagia, visual field
tribute to UI. defect, and motor weakness.
Other conditions resulting in impaired mobility and/
Epidemiology/Functional Impact or cognition (e.g., Parkinson disease, osteoarthritis,
Prevalence estimates of UI vary significantly by type of dementia) are also associated with UI. Urinary frequency
incontinence, definition of UI, and target populations, as and nocturia associated with congestive heart failure or
well as with variations in study design. Urinary inconti- peripheral venous insufficiency can contribute to UI.
nence is reported to affect 30%60% of women who are Diabetes is an independent risk factor for developing UI
middle-aged and older. The NOBLE (National Overactive because of polyneuropathy, changes in fluid intake, and
Bladder Evaluation) Program estimated that one-third of diabetes-related functional impairment.
women older than 65 suffer from OAB, with about two- Urinary incontinence has a significant socioeco-
thirds of these cases associated with incontinence. Stress nomic impact. Individuals with UI may suffer medical
urinary incontinence affects about 13% of women 1944 and quality-of-life consequences that compromise over-
years of age and 22% of women 4564 years of age. In all well-being. Urinary incontinence has been associated
older women, mixed incontinence is most common and with an increased risk of urinary tract infections (UTIs),
accounts for about 50% of all cases. pressure ulcers, falls, fractures, and sleep disturbance,
Risk factors for UI in women include age, race/eth- all of which may lead to functional impairment and
nicity, childbirth, hysterectomy, oral hormone therapy, decline in overall health status. Urinary incontinence
obesity, cognitive impairment, mobility impairment, and is a well-recognized risk factor for nursing home place-
diabetes. Control of the lower urinary tract system in
ment. Incontinence after a stroke adversely affects 2-year
women is directly affected by loss of pelvic organ support
survival, disability, and functional outcome; it is also asso-
and loss of estrogen at menopause. Up to 70% of women
ciated with a 4-fold increased risk of institutionalization
with UI relate the onset of symptoms with menopause.
at 1 year (Kolominsky-Rabas 2003). Psychological and
Both qualitative and quantitative changes in the connec-
tive tissue of the urogenital tract are believed to contribute social complications of UI include isolation, depression,
to SUI. Recent investigations suggest a higher prevalence anxiety, impaired sexual function, decreased work pro-
of SUI in postmenopausal women who possess a collagen ductivity, increased functional dependency, and increased
type I 1 Sp1 polymorphism (Sioutis 2011). Type 1 col- caregiver burden.
lagen is the main structural protein in connective tissue. According to the National Institutes of Health, the
Polymorphism may be associated with alterations in the annual direct cost of UI in the United States was about
quality and quantity of pelvic floor collagen. $19.5 billion in 2000. Up to 70% of the cost is attributed
Because UI is more common in women, there are to routine care such as incontinence pads and diapers,
fewer studies evaluating the prevalence and epidemiol- protective items, laundry, odor control, and skin care
ogy of UI in men. In men, UI has a later and more sudden products. A major contributor to this figure is the cost of
onset than in women. The National Health and Nutrition institutional care.
Examination Study reported an overall UI prevalence in
men of 4.5%; this prevalence increased to 16% in men 75 Clinical Evaluation and Diagnosis
years or older. Factors associated with UI in men of this
study were age, major depression, benign prostatic hyper- In a large Medicare study, only 56% of patients who
plasia (BPH), and hypertension (Markland 2010). In self-reported UI symptoms had them discussed at their
other studies, associated risk factors included lower uri- most recent health care visit (Mardon 2006). Screening
nary tract symptoms (LUTS), impaired mobility, and is necessary to identify patients because many patients do
urethral surgery or irradiation. Despite surgical advances, not report symptoms. Screening questions such as Do
UI remains a common complication for 12%16% of men you ever leak urine when you do not want to? and Do
after surgery for prostate cancer. you ever leak urine when you cough, sneeze, or laugh?
Several comorbid conditions are associated with UI in are now part of health care quality assessments through
both men and women. Urinary incontinence is common Medicare.
after a cerebrovascular accident (CVA), with 40%60% Women in the Medicare population reported inconti-
of patients experiencing UI during hospitalization nence symptoms at a rate of 43.6% and men at a rate of
immediately after a CVA. The incidence significantly 27.9% (Mardon 2006). The reporting of bothersome
declines over several months; however, up to one-third of symptoms increased with age for both men and women.
PSAP 2013 Special Populations 5 Urinary Incontinence in the Older Adult
The Agency for Healthcare Research and Quality retention, including those who have diabetes, are taking
recommends a basic diagnostic evaluation for UI. A thor- anticholinergic drugs, have a neurologic disorder, or have
ough history should focus on specific symptoms, as well symptoms of voiding difficulty or retention. A PVR of less
as quality of life and impact on the patient and caregiv- than 100 mL is normal; greater than 200 mL is consid-
ers. A bladder diary can be used to identify patterns and ered abnormal. Between those two values, the PVR must
measure treatment efficacy. Bladder diaries keep track of be interpreted with other information about the patient.
things such as liquid intake, number of trips to the bath- Specialty testing (e.g., urodynamics) is not necessary dur-
room, activities during leakage, strength of urge to void, ing initial evaluation and treatment.
and accidental leaks. A freely accessible bladder diary can Another important part of the initial evaluation of
be found online courtesy of the National Institutes of UI is to identify any reversible causes or contributors.
Health. An abdominal, rectal, and genital physical exam- Several chronic diseases and conditions can contribute to
ination should be performed, and a urinalysis should be UI. These include UTIs, atrophic vaginitis, urinary tract
used to rule out infection or glucosuria. There is no need surgeries (prostatectomy), constipation, uncontrolled
to treat asymptomatic bacteriuria in the institutional- diabetes, chronic venous insufficiency, delirium, and
ized patient; treatment has not been shown to decrease mobility restraint. Appropriate treatment for each of these
UI (Lucas 2012; Johnson 2009). In noninstitutionalized conditions should be implemented and incontinence reas-
patients, this is less clear. Treatment may be attempted sessed. Several drugs can also cause or exacerbate UI
first to see whether incontinence improves (Johnson (Table 1-2).
2009). Some groups recommend that PVRs be mea-
sured for all patients; however, this is controversial. The
American Urological Association recommends a PVR Management of UI
if, after a history and urinalysis, the diagnosis of OAB Nonpharmacologic Treatment
is unclear. The European Association of Urology cites a Nonpharmacologic and behavioral strategies are
lack of evidence for routine PVR measurement. Post void important in the comprehensive management of UI.
residuals help determine the amount of urinary retention Noninvasive lifestyle and behavioral interventions are
and should be performed in patients at high risk of urinary the first-line treatment of choice in the elderly population.
Table 1-2. Drugs That Can Affect Continence
Drug Effects on Continence
Alcohol Increased frequency, urgency, sedation, immobility
-Adrenergic agonists Outlet obstruction (men)
-Adrenergic blockers Stress leakage (women)
ACE inhibitors Cough worsens stress incontinence
Anticholinergics Impaired emptying, retention, delirium, sedation, constipation, fecal impaction
Antipsychotics Anticholinergic effects plus rigidity and immobility
Calcium channel blockers Impaired detrusor contractility and retention; dihydropyridine agents can cause pedal
edema, leading to nocturnal polyuria
Cholinesterase inhibitors Urinary incontinence, interactions with antimuscarinics
Estrogen Worsens stress and mixed leakage in women
GABAnergic agents Edema causing nocturia and nighttime incontinence
(gabapentin and pregabalin)
Loop diuretics Polyuria, frequency, urgency
Narcotic analgesics Urinary retention, fecal impaction, sedation, delirium
NSAIDs Pedal edema causing nocturnal polyuria
Sedative hypnotics Sedation, delirium, immobility
Thiazolidinediones Pedal edema causing nocturnal polyuria
ACE = angiotensin-converting enzyme; GABA = -aminobutyric acid; NSAID = nonsteroidal anti-inflammatory drug; TCA = tricyclic antidepressant.
Adapted with permission from: Reuben DB, Herr KA, Pacala JT, et al. Geriatrics at Your Fingertips, 14th ed. New York: American Geriatrics Society, 2012.
PSAP 2013 Special Populations 6 Urinary Incontinence in the Older Adult
Advantages of behavioral interventions include low cost, goal interval is initially based on the patients individual
absence of adverse effects, and ease of implementation. voiding habits. Intervals are increased by 15- to 30-min-
These interventions should be individually tailored; their ute increments per week until a voiding interval of 34
effectiveness largely depends on patient motivation, func- hours is achieved. Bladder diaries can be a useful adjunct
tional capacity, and cognitive function. to bladder training. The efficacy of bladder training has
been shown in several studies, with a reduction in incon-
Lifestyle Modification tinence episodes and a decrease in volume of urine lost
Lifestyle modifications for UI include smoking ces- (Subak 2002; Fantl 1991). Regular voiding at timed inter-
sation, caffeine and alcohol reduction, weight loss, and vals to avoid a full bladder or prevent involuntary bladder
modified fluid intake. The relationship between caf- contractions is a useful behavioral strategy for all types of
feine intake and OAB appears to be dose-dependent. incontinence.
Patients consuming greater than 400 mg/day of caffeine Pelvic muscle rehabilitation (PMR), also referred to as
are 2.4 times more likely to experience detrusor instabil- Kegel exercises, is commonly used as a treatment strategy
ity. Reductions in caffeine intake should be undertaken for SUI and UUI. Repetitive contraction and relaxation of
gradually to avoid withdrawal symptoms. Data exist to the pelvic floor muscles is used to improve the reflex inhi-
suggest obesity and type 2 diabetes mellitus as indepen- bition of involuntary detrusor contractions and enhance
dent risk factors for UI in women. In the Action for Health the ability to voluntarily contract the external sphincter.
in Diabetes (Look AHEAD) trial, moderate weight loss In randomized clinical trials, PMR reduced episodes of
was reported to reduce the incidence but not improve UI by 54%75% compared with reductions of 6%16%
the resolution rate of UI among overweight women with without treatment (Goode 2010). A systematic review of
type 2 diabetes mellitus (Phelan 2012). Another recent PMR for UI in men after prostatectomy found that PMR,
study of UI in overweight women reported that weight with or without biofeedback, improved continence com-
loss decreased the cost of incontinence management by pared to no PMR (MacDonald 2007). Some patients have
81% and was independently associated with decreased difficulty identifying and isolating pelvic floor muscles.
frequency of incontinence (Subak 2012). Modified fluid Biofeedback and vaginal weights are tools that are some-
intake encourages reductions in fluid intake during the times used to help patients correctly perform the exercises.
evening hours. Many patients will restrict fluid on their Studies have failed to show a benefit of PMR combined
own in an attempt to manage incontinence. Patient educa- with biofeedback or vaginal weights over PMR alone.
tion regarding the timing of fluid intake is critical; overall, Referral to a nurse specialist or physical therapist may
fluid restriction is not recommended because it may lead be of benefit for the patient who is cognitively intact but
to dehydration and increased risk of UTIs. who has difficulty effectively performing the exercises. In
Additional supportive measures include education summary, PMR is a safe but labor-intensive approach that
about bladder health, use of absorbent products, and requires a motivated and cooperative patient.
appropriate skin care. Environmental interventions such
as toilet proximity, safe path to bathroom, raised toilet Devices
seats, grab bars, and toilet substitutes (e.g., urinals, com- Sacral nerve stimulation (SNS) has U.S. Food and
modes) are particularly useful for patients with functional Drug Administration (FDA) approval for use in the
incontinence. treatment of patients with severe refractory UUI when
behavioral management and medications fail or are not
Behavioral Therapy tolerated. In SNS, a generator device is inserted subcuta-
The goal of behavioral interventions is to achieve a sat- neously in the lower back or buttocks. A lead is attached
isfactory voiding pattern. Patient-dependent behavioral to the S3 sacral nerve, and electrical stimulation results
therapies require functional capacity, learning ability, in decreased contraction of the detrusor muscle. Studies
and patient motivation. Patients with functional disabil- of SNS have shown significant decreases in the number of
ity or cognitive impairment require systematic toileting incontinence episodes as well as incontinence pads used
assistance, and they are often dependent on caregivers for in patients with OAB. Efficacy data from randomized con-
successful implementation of behavioral interventions. trolled trials (RCTs) show that complete continence or
Bladder training is an urge suppression technique that significant improvement was achieved in about 80% of
is effective in patients with intact cognition, adequate patients who received SNS compared with 3% in control
functional ability to toilet, and motivation to cooper- groups (Brazzelli 2006). Patients with a higher number
ate. The patient gradually increases toileting intervals by of daily incontinence episodes (greater than 10) are most
resisting or inhibiting the sensation of urgency. Patients likely to benefit. Surgical revision rates range from 3% to
learn to urinate according to a scheduled timetable, rather 33% and are attributed to lack of efficacy or infection.
than with the symptoms of urge. Distraction and relax- The extracorporeal magnetic innervation chair has FDA
ation techniques are employed to help delay voiding and approval for use in the treatment of uncomplicated mild
allow the development of increased bladder capacity. The SUI. A low-intensity magnetic field is used to strengthen
PSAP 2013 Special Populations 7 Urinary Incontinence in the Older Adult
pelvic floor muscles. Treatments are generally given for 20 Although not a first-line therapy, artificial urinary
minutes twice weekly for 8 weeks total. sphincters are the most effective treatment for intracta-
Women with good manual dexterity are candidates for ble postprostatectomy SUI in men. Subjective satisfaction
intravaginal support devices or urethral occlusion inserts. rates reach 85%95%; however, the risk of infection is
These devices offer the option of temporary or occasional high (1.8%10%). Other potential complications include
use and are suitable for patients with exercise-induced tissue atrophy resulting in worsening incontinence, ure-
SUI. Pessaries are often employed in older women who thral erosion, and device defects. These complications
have not responded to behavioral therapies. Insertion is often necessitate reoperation or removal of the system,
performed by a health care provider, and the pessary can with device defects accounting for about one-half of all
be removed for cleaning and reinserted every 46 weeks. revision procedures.
Pessaries are suitable for temporary or long-term use.
Monitoring for vaginal infection and ulceration is criti- Pharmacologic Treatment
cal to the safe use of these devices. A study conducted in Nonpharmacologic or behavioral therapy should
patients with SUI compared pessaries alone, behavioral always be implemented for patients with UI, but
treatment alone, or a combination of pessary and behav- pharmacotherapy is often added to help alleviate symp-
ioral treatment. The reported patient satisfaction rate was toms. Pharmacotherapy does not cure UI. Drugs should
greater than 50% for all treatment groups at 12 months not be implemented without the failure or addition of
(Richter 2010). behavioral therapies because of potential adverse effects.
Urinary catheters are reserved for patients with chronic Currently, data are limited to support the combination of
bladder-emptying difficulty and elevated PVR. Catheters drugs and behavioral therapy over each separately (Burgio
may also be useful as a temporary measure in patients 2010; Burgio 2008). Figure 1-1 describes the management
with open skin wounds that must be protected from urine. of the patient with UI.
Severely or terminally ill patients with chronic UI who are
bedbound may also be appropriate candidates for a uri- Antimuscarinics
nary catheter. The most commonly prescribed UI drug class is mus-
carinic receptor blockers. These drugs are primarily used
Invasive Treatments for UUI. During the past 10 years, there have been several
Surgical management of SUI is common in the United additions to this class, with the hope that these new drugs
States, with more than 200,000 procedures performed would be more selective for muscarinic receptors in the
annually. Surgery is considered the most effective treat- bladder. This specificity was aimed at reducing the com-
ment when SUI is accompanied by uterine prolapse. The mon anticholinergic adverse effects of these medications.
Burch colposuspension procedure involves supporting
the anterior vaginal wall to the Cooper ligament through Comparative Efficacy and Tolerability
a laparoscopic incision. In recent years, the midurethral Oxybutynin remains the gold standard by which other
mesh sling has replaced the Burch procedure as the new agents are measured. It was the first approved antimus-
gold standard. The midurethral sling procedure employs carinic agent for UI. The immediate-release formulation
transvaginal placement of a synthetic mesh below the has significant anticholinergic effects, however, and it is
midurethral area. The Burch procedure and the midurethral thought that the longer-acting formulations, as well as the
sling have comparable rates for cure and complications; topical and transdermal formulations, have fewer adverse
however, the midurethral sling procedure offers the advan- effects. The oxybutynin extended-release formulation may
tage of a less-invasive approach, shorter operative times, reduce first-pass metabolism, decreasing the active metab-
technical ease, and ability to be performed in the outpatient olite N-desethyloxybutynin. This metabolite is thought
setting. Reported cure rates are 77%96%. Recent data sug- to cause many of the anticholinergic adverse effects. The
gest that the overall reoperation rate after SUI surgery is oxybutynin transdermal patch and gel also bypass first-
higher for the midurethral sling (13.0%) than for the Burch pass metabolism.
procedure (10.8%) ( Jonsson Funk 2012). The oxybutynin transdermal patch must be applied
Periurethral injection of bulking agents (e.g., collagen) every 3 or 4 days, whereas the gel must be applied daily. In
improves urethral closure in SUI and may be beneficial a comparison of anticholinergic adverse effects, the rates
in mild cases of postprostatectomy SUI. High short-term of xerostomia with oxybutynin were 71% with immediate
cure rates are achieved; however, effectiveness is lost release, 29%61% with extended release, 4%10% with
over time, and repeated interventions are often neces- the transdermal patch, and 2%12% with gel. The reported
sary. Reinjection may be associated with inflammatory adverse event rates for other anticholinergic effects in the
reactions and scarring, which makes further treatment package inserts are listed in Table 1-3.
difficult. The use of bulking agents may be appropriate for In general, dry mouth occurs less often with
patients with refractory SUI who have shown sphincter extended-release formulations, and many of the anticho-
incompetence based on urodynamic studies. linergic adverse effects appear to be dose related. The risk
PSAP 2013 Special Populations 8 Urinary Incontinence in the Older Adult
Initial evaluation of UI Rule out reversible causes of UI
Screening questions, bladder diary, symptom Uncontrolled diabetes and heart failure, chronic venous
history, physical examination (genital, abdominal, insufficiency, constipation, delirium, atrophic vaginitis,
rectal), urinalysis, PVR urinary tract infection
Medications (see Table 1-2)
Lifestyle Interventions
Decreased caffeine and alcohol intake
Modified fluid intake
Weight loss/smoking cessation
Bladder training/timed voiding
Absorbent products/modified environment
Pelvic floor muscle rehabilitation
Stress Urge Functional Overflow
incontinence incontinence incontinence incontinence
Pessaries Antimuscarinics Implement lifestyle -Blockers
Minor surgical Mirabegron interventions 5- reductase inhibitors
procedures BPH
Duloxetine (may be Severe UUI Persistent UUI with
used first line) Sacral nerve neurologic condition
Antimuscarinics stimulators Onabotulinum toxin A
Topical estrogens
-Agonists (third line)
Figure 1-1. Decision tree for the patient with urinary incontinence.
BPH = benign prostatic hyperplasia; PVR = postvoiding residual; UUI = urge urinary incontinence.
of constipation appears to be slightly greater in the higher- with respect to better efficacy or tolerability. This is mainly
dosage forms of some of the newer agents (i.e., solifenacin because of the lack of head-to-head trials. Solifenacin and
and darifenacin). There is no evidence that QT prolonga- darifenacin were believed to be uroselective agents when
tion is a major adverse effect of the antimuscarinics when they were developed. However, the available data do not
used at usual dosages. Some evidence exists that these show that these agents are any better with respect to anti-
agents prolong QT intervals in higher dosages or overdose cholinergic adverse effects, and they should not be chosen
(Hesch 2007). Clinically, it is important to note whether a on the basis of being uroselective.
patient is taking other QT-prolonging agents when initiat- A recent systematic review evaluated the efficacy and
ing antimuscarinics because there may be a small additive tolerability of several antimuscarinic agents for UUI in
effect (Hesch 2007). women. This review included literature from 1966 to
Evidence is insufficient to support other agents (e.g., 2011, and only RCTs were eligible. In the 94 trials ana-
tolterodine, fesoterodine, trospium) over oxybutynin lyzed, antimuscarinics had only a small benefit over
PSAP 2013 Special Populations 9 Urinary Incontinence in the Older Adult
Table 1-3. Adverse Effect Profiles of Antimuscarinic Agents Used for UI
Blurred/
Urinary Dry Abnormal
Dry Mouth Constipation Nausea Headache Somnolence Dizziness Confusion Tachycardia Retention Eyes Vision
Adverse Effect (%) (%) (%) (%) (%) (%) (%) (%) (%) (%) (%)
Oxybutynin IR 71.4 15.1 11.6 7.5 14.6 16.6 25 25 6.0 9.6
Oxybutynin ER 29.0 7.0 2.0 6.0 2.0 4.0 3.0 1.0
Oxybutynin 9.6 3.3 12 12 2.5
transdermal
Tolterodine IR 35.0 7.0 7.0 3.0 5.0 3.0 2.0
Tolterodine ER 23.0 6.0 6.0 3.0 1.2 3.0 1.0
Trospium IR 20.1 9.6 4.2 1.2
Trospium XR 10.7 8.5 1.4 1.6
Solifenacin 5 mg 10.9 5.4 1.7 1.9 1.8 0 0.3 3.8
Solifenacin 10 mg 27.6 13.4 3.3 1.8 1.9 1.4 1.6 4.8
Darifenacin 7.5 mg 20.2 14.8 2.7 0.9 1.5
Darifenacin 15 mg 35.3 21.3 1.5 2.1 2.1
Fesoterodine 4 mg 18.8 4.0 0.7 <1 0.2 1.4 <1
Fesoterodine 8 mg 34.6 6.0 1.9 1.1 3.7
ER = extended release; IR = immediate release; UI = urinary incontinence; XR = extended release.
Information from manufacturers package inserts.
placebo in achieving continence and improving UI immediate release costs significantly less than most of the
symptoms. When all drugs were analyzed together, the other agents. Solifenacin and the extended-release and
absolute risk difference in continence was less than 20% transdermal formulations of other agents may have fewer
(Shamliyan 2012). The drug class also had a significantly anticholinergic adverse effects. These alternatives may be
higher discontinuation rate than placebo because of preferred when the patient has comorbidities that make
adverse effects. The lowest rates of discontinuation were these adverse effects particularly problematic.
with solifenacin 5 mg daily. More than 50% of patients Discontinuation rates do not typically differ with these
had discontinued treatment with their antimuscarinic at formulations. Skin reactions may limit the use of trans-
1 year (Shamliyan 2012). Dry mouth was the most com- dermal products because rates of pruritus and rash can be
mon adverse event reported in the analysis. The review as high as 15% (Dmochowski 2002). The 2012 American
also evaluated the trials that compared antimuscarinics Geriatrics Society Beers Criteria lists the oral antimus-
with each other. Fesoterodine was more effective than carinics as a class that exacerbates constipation and that
tolterodine, producing greater rates of continence, but it should be avoided unless no alternative is available (AGS
also had a higher discontinuation rate because of adverse 2012).
effects. There was no difference in UI improvement Drug interactions may also influence the choice of anti-
between oxybutynin and tolterodine, although treatment muscarinic. Tolterodine is metabolized by cytochrome
discontinuation rates for oxybutynin were greater. P450 (CYP) 2D6 in most patients. Some patients have a
Overall, a small benefit in UI symptoms was seen with genetic polymorphism that hampers metabolism through
antimuscarinic drugs compared with placebo. None of the the 2D6 pathway. These poor metabolizers rely more on
agents showed superiority on the basis of current evidence. the CYP3A4 pathway for metabolism. In patients who
Solifenacin 5 mg had the lowest discontinuation rate because are taking potent CYP 2D6 or 3A4 inhibitors, the dosage
of adverse effects and could be an option if other urge incon- of tolterodine should be reduced by 50%. Darifenacin is
tinence treatments have failed the patient. One of the main metabolized by CYP 2D6 and 3A4, but no formal dosage
limitations of this analysis is that more than 80% of the reductions are recommended for this drug. Fesoterodine
patients included were women, reducing the generalizability and solifenacin are metabolized by CYP3A4, and their
of the conclusions to men (Shamliyan 2012). maximal daily dosages with potent CYP3A4 inhibitors
Because efficacy is similar across the antimuscarinic are 4 mg and 5 mg, respectively.
class, the choice of a first-line agent is often influ- Antimuscarinics should exert their effect within the
enced by cost, drug interactions, patient comorbidities, first month a patient takes them. Follow-up should then
adverse effects, and route of administration. Oxybutynin be done to assess adverse effects and efficacy.
PSAP 2013 Special Populations 10 Urinary Incontinence in the Older Adult
Over-the-counter Oxybutynin Transdermal inserts for donepezil (1%3%), rivastigmine (not listed),
In January 2013, the FDA approved the switch of oxy- and galantamine (less than 1%2%); however, clinically,
butynin transdermal from prescription-only status to this is an important issue to consider. One retrospective
over the counter (OTC) (FDA Briefing Document 2012). study looked at the possible cascade of being prescribed
This was despite the Nonprescription Drugs Advisory an antimuscarinic agent in response to an adverse effect
Committee vote in November 2012 against the switch to from a cholinesterase inhibitor. The study looked at 44,884
OTC status. Oxytrol (oxybutynin transdermal) is cur- older adults, of whom 20,491 were prescribed a cholines-
rently projected to come to the OTC market in September terase inhibitor (95% donepezil). The results showed that
2013. Three types of studies were done to present evidence 4.5% of those prescribed a cholinesterase inhibitor were
to the FDA to approve this switch: a label comprehen- also prescribed an antimuscarinic agent. Another 3.1% of
sion study, which was aimed at assessing whether patients those not taking a cholinesterase inhibitor were prescribed
could understand the directions/labeling; a self-selection one by the studys conclusion (Gill 2005). This increase
study, which was aimed at assessing whether the appro- was statistically significant. An important consideration in
priate patients chose to use the product; and an actual patients taking both a cholinesterase inhibitor and an anti-
use study, which determined whether patients who were muscarinic agent is taking a detailed history of when UI
using the product discontinued use appropriately and fol- symptoms started or worsened in relation to the addition of
lowed labeling instructions. In these studies, 90% of men these drugs. A dose reduction or risk-benefit analysis of the
appropriately did not select the product for themselves, cholinesterase inhibitor may be needed to improve UI.
and 92% of pregnant patients appropriately did not select Dementia itself can worsen UI; this places an even
the product. In the actual use study, 3.4% of patients con- larger burden on caregivers. Up to one-third of patients
tinued using the oxybutynin transdermal product when with dementia are taking both cholinesterase inhibi-
they should have discontinued. All cases were reviewed tors and antimuscarinics. There is conflicting evidence
by physicians to determine whether patients should have on the extent to which antimuscarinics affect cogni-
discontinued. Originally, 14.4% should have discontin- tion or potentially reduce the efficacy of cholinesterase
ued according to labeling, but that number was reduced inhibitors. A prospective cohort study of 3536 nursing
to 3.4% after physician reviews. In those with UTIs, 98% home patients who were taking a cholinesterase inhibitor
discontinued appropriately. found that 10.6% were prescribed oxybutynin or toltero-
The OTC oxybutynin transdermal product will be mar- dine in the 2-year study period. The authors found that
keted only to women older than 18 years. This is because using these two agents together created an additional
men were not as able to effectively differentiate urinary 0.54 decrease in ADL (activities of daily living) points
symptoms caused by OAB from other causes of UI such as (028 scale) (p=0.01). The MDS-COGS (Minimum Data
BPH. The packaging will have a pink box and will state in Set Cognition Scale) score was used to assess cognitive
large letters that this product is for women so that men are decline, which did not differ between groups (Sink 2008).
discouraged from using it. The labeling for the new OTC Similarly, another RCT of 50 female nursing home patients
product will state that the product is to be used only for found no change in cognition when oxybutynin extended
symptoms that have been present for at least 3 months. This release was administered for 4 weeks (Lackner 2008).
will help women who have UTIs or are in early pregnancy These two trials cannot be generalized to the community-
avoid use of the product. The labeling also is meant to prom- dwelling elderly adult because they were performed in the
inently show symptoms that are cause for discontinuation. nursing home population. The smaller changes may have a
The OTC oxybutynin transdermal labeling states the med- greater effect on the highly functional community-dwell-
ication should also result in improvement in 2 weeks. If ing elderly adult. Several case reports also show cognitive
symptoms persist or worsen during or after this period, the decline with antimuscarinics (Donnellan 1997).
patient should seek medical advice. There is no definitive evidence of whether antimuscarin-
ics should be used in patients with cognitive impairment
Use with Cholinesterase Inhibitors and or in patients taking a cholinesterase inhibitor. Clinicians
in Patients with Dementia should consider the possible interactions carefully. If an
Urinary incontinence is often seen in elderly patients antimuscarinic is believed necessary in these patients,
with dementia. The antimuscarinic agents used to treat cognitive function should be monitored when initiating
UUI directly oppose many drugs that treat dementia by the drug and on a regular basis thereafter.
increasing cholinergic transmission. Whether antimusca- Use with -Blockers
rinics should be prescribed with cholinesterase inhibitors Men are underrepresented in trials of UI drugs, consti-
is controversial, as is whether they should be prescribed in tuting only 10%25% of study subjects. Drugs used for UI
general to patients with baseline cognitive impairment. are thought to have similar efficacy and tolerability in the
One overlooked issue is that cholinesterase inhibitors male population. Although the LUTS of UUI and bladder
have the ability to increase or possibly even precipitate UI outlet obstruction or BPH are similar, a distinction must
episodes. Only minimal rates of UI are cited in the package be made because the use of antimuscarinic agents in BPH
PSAP 2013 Special Populations 11 Urinary Incontinence in the Older Adult
can cause significant urinary retention. Using -blockers Estrogens
concomitantly with antimuscarinics has become a sub- Oral and topical estrogen therapy was thought to
ject of interest. In a few trials, this combination has shown improve the symptoms of SUI by increasing -receptors
improvement in LUTS (Chapple 2010). For a detailed and local circulation. Both the Heart and Estrogen/
discussion on using -blockers concomitantly with anti- Progestin Replacement Study (HERS) and the Womens
muscarinics, see the chapter on BPH in this book. Health Initiative study showed increased UI with the
use of oral estrogens. In the HERS study, 39% of patients
Duloxetine had worsening of incontinence, whereas only 27% in the
Although duloxetine is approved in Europe for use in placebo group had similar outcomes (Grady 2001). Oral
SUI, this remains an off-label use in the United States. estrogen also carries a risk of cardiovascular adverse
The 2012 European Association of Urology Guidelines events, possible worsening cognition, and increased
suggest offering duloxetine to both men and women who breast cancer risk. Oral estrogen should not be routinely
would like symptom relief from SUI, giving this recom- used for SUI. Topical estrogens can be used, and doses for
mendation a grade A evidence level. Trials in the United vaginal atrophy are recommended in this case. The 2012
States for this indication are ongoing. Several trials have European Association of Urology guidelines also endorse
looked at duloxetine versus placebo, usually at a dose of topical estrogen as an option for SUI, with a grade A level
40 mg twice daily. These studies have evaluated UI fre- recommendation. The 2012 Beers Criteria recommend
quency episodes and found significant median decreases against the use of oral or transdermal patch estrogen in
in these episodes with duloxetine to be 50%54% versus women.
placebo at 27%40% (Millard 2004; Van Kerrebroeck
2004; Dmochowski 2003). Botulinum Toxin
A 2009 Cochrane review of studies comparing dulox- In 2011, the FDA approved the labeling of
etine with placebo included 10 RCTs with 3944 adults Onabotulinum toxin A for use in patients with detrusor
having SUI. Trial duration was only 312 weeks, but the overactivity associated with a neurologic condition (e.g.,
frequency of incontinence episodes was reduced by up to spinal cord injury, multiple sclerosis) and inadequate
response to anticholinergic therapy. The injections are
50% with duloxetine compared with placebo (Mariappan
intradetrusor by cystoscopy. According to the package
2005). It was not known whether this benefit could be sus-
insert, in preapproval studies, the frequency of incon-
tained, but the available evidence suggested it was a good
tinence episodes at week 12 was decreased by 19.6% in
option for the treatment of SUI.
the Onabotulinum toxin A group compared with 8.9%
Duloxetine has shown improvement in quality of life in
in the placebo group. One of the primary risks of using
several trials, with some patients seeing benefit within 2 Onabotulinum toxin A is acute urinary retention. Patients
weeks of initiation. The typical dose is 40 mg twice daily, must be willing to undergo catheterization as part of this
and the most common adverse effect reported in most therapy. In the preapproval trials, catheterization at any
trials was nausea (4%24%), possibly related to rapid time was required by 30.6% of patients in the treatment
dose escalation (Millard 2004; Van Kerrebroeck 2004; group versus 6.7% in the placebo group. Prophylactic
Dmochowski 2003). Duloxetine is metabolized by CYP antibiotics should be given 13 days before the injec-
2D6 and 1A2, and caution must be used with inhibitors tion, again on the day of the injection, and 13 days after
of these two enzymes. In the 2012 American Geriatrics the injection. Aminoglycosides cannot be used because
Society Beers Criteria, duloxetine is listed with other of their interference with neuromuscular transmission,
serotonin-norepinephrine reuptake inhibitors for use with which can potentiate the effects of Onabotulinum toxin
caution in elderly patients because of the risk of syndrome A. Antiplatelet drugs also must be discontinued 3 days
of inappropriate antidiuretic hormone or hyponatremia before injection. The per-treatment dose is 200 units, and
(AGS 2012). Duloxetine is not recommended when the treatments should not be repeated any sooner than 12
CrCl is less than 30 mL/minute. weeks. According to the package insert, the mean effect of
the injection in the initial trials lasted 4248 weeks.
-Agonists In early 2013, Onabotulinum toxin A was also approved
The use of -agonists for SUI is not as common now that for use in OAB in those who cannot use or do not respond
duloxetine is considered a first-line agent. Some guidelines adequately to antimuscarinic medications. The injections
do not even list -agonists as an option for treatment any- are administered as described previously with cystoscopy.
more. Contraindications to the use of these agents (i.e., The dosing for this indication is 100 units. This is admin-
hypertension, arrhythmia, coronary artery disease, myo- istered by giving 20 injections of 5 units each about 1 cm
cardial infarction, hyperthyroidism, kidney failure, and apart in the detrusor muscle. The dose can be repeated if
narrow angle glaucoma) make them difficult to use. The the effect wears off, but it must have been at least 12 weeks
adverse effects of hypertension, headache, anxiety, and since the previous dose. The median time to requiring a
insomnia make these agents even less attractive. second dose was 24 weeks in approval studies.
PSAP 2013 Special Populations 12 Urinary Incontinence in the Older Adult
In the clinical trials for this indication, 1105 patients be determined but will likely significantly exceed that
were followed for 12 weeks (median time to repeat 24 of other antimuscarinic agents. Those with cognitive
weeks) after injection with Onabotulinum toxin A or pla- impairment may be a target patient population for this
cebo. The episodes of incontinence were 1.61.8 times agent if it is not cost-prohibitive.
less likely to occur in the treatment group. The main
adverse urologic events in the studies were UTIs (19%
vs. 6%), urinary retention (6% vs. 0%), and dysuria (9% Conclusion
vs. 7%). Providing prophylactic antibiotic therapy and Urinary incontinence has a large economic and func-
withholding antiplatelets is the same as previously rec- tional impact and will become an even larger issue in the
ommended for Onabotulinum toxin A. It should not be health care system as the population continues to age.
used in patients with a PVR greater than 200 mL unless Pharmacists can have a large effect on reducing this burden
they are performing self-catheterization. This informa- by reviewing the medication profiles of all patients with
tion and more extensive administration information can UI to identify potential reversible causes as well as evalu-
be found in the manufacturers package insert. ate for concurrent anticholinergic drugs. Pharmacists are
in a prime position to help guide the choice of antimus-
Mirabegron carinic with respect to cost, adverse effect profile, patient
Mirabegron, a new 3 -adrenergic receptor agonist, comorbidities, and administration. Discontinuation
was approved in mid-2012 for the treatment of OAB with rates of antimuscarinics are high because of intolerable
urgency symptoms. Stimulation of the 3 -receptor causes adverse effects. It is important for the pharmacist to coun-
bladder relaxation during filling. At very high doses (i.e., sel patients on what to expect from these agents and when
200 mg), there was some stimulation of the 1-adrenergic they should see results. For patients seeing benefit, adjunc-
receptors, but overall, mirabegron has low intrinsic activ-
tive treatment can be recommended to help with adverse
ity for 1- or 2-receptors. The starting daily dose is 25
effects such as constipation and dry mouth.
mg; if there is inadequate response at 8 weeks, it can be
titrated up to 50 mg. Patients with a CrCl of 1529 mL/
minute/1.73m 2 or moderate liver disease should receive
only the 25-mg dose.
Practice Points
According to the package insert, in preapproval tri-
als, mirabegron at 25 mg and 50 mg daily significantly There is no single antimuscarinic agent with sig-
decreased the number of incontinence episodes in 24 nificant data to show that it is the first-line choice
hours and the number of micturitions in 24 hours over
for urinary incontinence. Cost and comorbidities
placebo. Decreases were only in the 12 micturition range
but were statistically significant. Mirabegron should should be determining factors when selecting a
be used with caution in patients taking antimuscarinic drug.
therapy or in those who have bladder outlet obstruction Oxybutynin immediate release is sometimes cited
because it can cause urinary retention. The most common as the medication to try first line because no over-
adverse effect in initial trials was hypertension; healthy whelming evidence exists that it is tolerated any
volunteers had a mean increase in blood pressure in of 3.5 worse than other drugs, and it is known to be as
mm Hg systolic and 1.5 mm Hg diastolic. Patients with efficacious as other agents.
uncontrolled hypertension (i.e., greater than 180 mm Hg
systolic or 110 mm Hg diastolic) should not take mirabe- Topical preparations of antimuscarinic drugs
gron. Adverse event rates for the 25-mg daily dose were as have not been shown superior to other agents and
follows: hypertension (11.3%), nasopharyngitis (3.5%), therefore cannot be recommended as first-line
UTIs (4.2%), and headache (2.1%). treatment.
Mirabegron inhibits CYP2D6 metabolism, and The use of antimuscarinic agents in those with
caution should be used with other drugs that are 2D6 sub-
cognitive impairment is not contraindicated; how-
strates or inhibitors. Mirabegron increases the area under
the curve of digoxin by 27% when these are coadmin- ever, these drugs must be used at the lowest dose
istered. The lowest dose of digoxin should be used, and possible and for the fewest daily doses. Patients
monitoring should be continued regularly. When used and caregivers must be counseled on watching
concurrently, mirabegron increases warfarin concentra- for worsening cognition. Urinary incontinence is
tions as much as 9%, and warfarin dose adjustments may a leading cause of institutionalization, and use of
be needed. these drugs in patients with cognitive impairment
Mirabegrons place in therapy is yet to be determined. may delay this. These two factors must be weighed
Patients with significant cardiovascular issues may not in each individual patient.
be good candidates for this agent. Cost is also yet to
PSAP 2013 Special Populations 13 Urinary Incontinence in the Older Adult
References Grady D, Brown JS, Vittinghoff E, et al. Postmenopausal hor-
mones and incontinence: the Heart and Estrogen/Progestin
The American Geriatrics Society 2012 Beers Criteria Update Replacement Study. Obstet Gynecol 2001;97:116-20.
Expert Panel. American Geriatrics Society updated Beers PubMed Link
Criteria for potentially inappropriate medication use in older
adults. J Am Geriatr Soc 2012;60:616-31. Hesch K. Agents for treatment of overactive bladder:
PubMed Link a therapeutic class review. Proc (Bayl Univ Med Cent)
2007;20:307-14.
Brazzelli M, Murray A, Fraser C. Efficacy and safety of sacral PubMed Link
nerve stimulation for urinary urge incontinence: a systematic
review. J Urol 2006;175:835-41. Johnson TM II, Ouslander JG. Incontinence. In: Halter JB,
PubMed Link Ouslander JG, Tinetti ME, et al., eds. Hazzards Geriatric
Medicine and Gerontology, 6th ed. New York: McGraw-Hill,
Burgio KL, Goode PS, Richter HE, et al. Combined behav- 2009.
ioral and individualized drug therapy versus individualized
drug therapy alone for urge incontinence in women. J Urol Jonsson Funk M, Siddiqui NY, Kawasaki A, et al. Long-term
2010;184:598-603. outcomes after stress urinary incontinence surgery. Obstet
PubMed Link Gynecol 2012;120:83-90.
PubMed Link
Burgio KL, Kraus SR, Menefee S, et al. Behavioral ther-
apy to enable women with urge incontinence to discontinue Kolominsky-Rabas PL, Hilz MJ, Neundoerfer B, et al. Impact
drug treatment: a randomized trial. Ann Intern Med of urinary incontinence after stroke: results from a prospec-
2008;149:161-9. tive population-based stroke register. Neurourol Urodyn
PubMed Link 2003;22:322-7.
PubMed Link
Chapple C. Antimuscarinics in men with lower urinary tract
symptoms suggestive of bladder outlet obstruction due to Lackner TE, Wyman JF, McCarthy TC, et al. Randomized,
benign prostatic hyperplasia. Curr Opin Urol 2010;20:43-8. placebo-controlled trial of the cognitive effect, safety, and tol-
PubMed Link erability of oral extended-release oxybutynin in cognitively
Divani AA, Majidi S, Barrett S, et al. Consequences of stroke in impaired nursing home residents with urge urinary inconti-
community-dwelling elderly: the health and retirement study, nence. J Am Geriatr Soc 2008;56:862-70.
1998 to 2008. Stroke 2011;42:1821-5. PubMed Link
PubMed Link
Lucas MG, Bosch RJ, Burkhard FC, et al. EAU guidelines on
Dmochowski RR, Davila GW, Zinner NR, et al. Efficacy and assessment and nonsurgical management of urinary inconti-
safety of transdermal oxybutynin in patients with urge and nence. Eur Urol 2012;62:1130-42.
mixed urinary incontinence. J Urol 2002;168:580. PubMed Link
PubMed Link
Mardon RE, Halim S, Pawlson LG, et al. Management of uri-
Dmochowski RR, Miklos JR, Norton PA, et al. Duloxetine ver- nary incontinence in Medicare-managed beneficiaries: results
sus placebo for the treatment of North American women with from the 2004 Medicare Health Outcomes Survey. Arch
stress urinary incontinence. J Urol 2003;170(4 pt 1):1259-63. Intern Med 2006;166:1128-33.
PubMed Link PubMed Link
Donnellan CA, Fook L, McDonald P, et al. Lesson of the week: Markland AD, Goode PS, Redden DT, et al. Prevalence of uri-
oxybutynin and cognitive dysfunction. BMJ 1997;315:1363. nary incontinence in men: results from the National Health
PubMed Link and Nutrition Examination Survey. J Urol 2010;184:1022-7.
PubMed Link
Fantl JA, Wyman JF, McClish DK, et al. Efficacy of bladder
training in older women with urinary incontinence. JAMA Mariappan P, Ballantyne Z, NDow JM, et al. Serotonin and
1991;265:609-13. noradrenaline reuptake inhibitors (SNRI) for stress uri-
nary incontinence in adults. Cochrane Database Syst Rev
Gill SS, Mamdani M, Nagile G, et al. A prescribing cascade 2005;3:CD004742.
involving cholinesterase inhibitors and anticholinergic drugs. PubMed Link
Arch Intern Med 2005;165:808-13.
PubMed Link MacDonald R, Fink HA, Huckabay C, et al. Pelvic floor mus-
cle training to improve urinary incontinence after radical
Goode PS, Burgio KL, Richter HE, et al. Incontinence in older prostatectomy: a systematic review of effectiveness. Br J Urol
women. JAMA 2010;303:2172-81. 2007;100:76-81.
PubMed Link PubMed Link
PSAP 2013 Special Populations 14 Urinary Incontinence in the Older Adult
Millard RJ, Moore K, Rencken R, et al. Duloxetine vs placebo
in the treatment of stress urinary incontinence: a four conti-
nent randomized clinical trial. BJU Int 2004;93:311-8.
PubMed Link
Partial Rx to OTC Switch for Oxybutynin Transdermal
System. FDA Briefing Document for Nonprescription Drugs
Advisory Committee Briefing Document. NDA 202-211, Nov.
9, 2012. Accessed March 21, 2013.
Internet Link
Phelan S, Kanaya AM, Subak LL, et al. Weight loss prevents
urinary incontinence in women with type 2 diabetes: results
from the Look AHEAD trial. J Urol 2012;187:939-44.
PubMed Link
Richter HE, Burgio KL, Brubaker L, et al. Continence pes-
sary compared with behavioral therapy or combined therapy
for stress incontinence: a randomized controlled trial. Obstet
Gynecol 2010;115:609-17.
PubMed Link
Shamliyan T, Wyman JF, Ramakrishnan R, et al. Benefits
and harms of pharmacologic treatment for urinary incon-
tinence in women: a systematic review. Ann Intern Med
2012;156:861-74.
PubMed Link
Sink KM, Thomas J II, Xu H, et al. Dual use of bladder anticho-
linergics and cholinesterase inhibitors: long term functional
and cognitive outcomes. J Am Geriatr Soc 2008;56:847-53.
PubMed Link
Sioutis D, Economus E, Lambrinoudaki I, et al. Sp1 collagen I
A1 polymorphism in women with stress urinary incontinence.
Int Urogynecol J 2011;22:835-9.
PubMed Link
Subak LL, Marinilli Pinto A, Wing R, et al. Decrease in uri-
nary incontinence management costs in women enrolled in
a clinical trial of weight loss to treat urinary incontinence.
Obstet Gynecol 2012;120:227-83.
PubMed Link
Subak LL, Quesenberry CP, Posner SF, et al. The effect of
behavioral therapy on urinary incontinence: a randomized
controlled trial. Obstet Gynecol 2002;100:72-8.
PubMed Link
Van Kerrebroeck P, Abrams P, Lange R, et al. Duloxetine
versus placebo in the treatment of European and
Canadian women with stress urinary incontinence. BJOG
2004;111:249-57.
PubMed Link
PSAP 2013 Special Populations 15 Urinary Incontinence in the Older Adult
Self-Assessment Questions
Questions 1 and 2 pertain to the following case. 4. In which one of the following patients would a post
R.Z. is a 70-year-old woman who presents with increased void residual (PVR) be most important as part of an
urinary frequency and a few episodes of urinary inconti- initial evaluation for lower urinary tract symptoms
nence (UI) during the past few weeks. These episodes do and UI?
not occur during periods of coughing, sneezing, or laugh- A. A 36-year-old woman who has urine leakage
ing. R.Z. recently lost her job and has no prescription drug with coughing.
coverage. She was seen 4 weeks ago as a new patient in B. A 51-year-old man with type 2 diabetes
your family medicine clinic, and the following drugs were mellitus who has urine dribbling and increased
initiated: amlodipine 5 mg, calcium carbonate 500 mg/ frequency.
vitamin D 200 international units daily, alendronate 70 C. A 50-year-old woman with epilepsy who has UI
mg weekly, metformin 500 mg twice daily, and citalopram with seizures.
10 mg daily. The only drug she was taking 4 weeks ago D. A 45-year-old woman with burning on urination
was hydrochlorothiazide 25 mg daily, which she has taken and increased frequency.
for the past 3 years. Her medical history is significant for
osteoporosis, diastolic heart failure, hypertension, type 2
Questions 5 and 6 pertain to the following case.
diabetes mellitus, and depression. Laboratory test results
T.R. is a 67-year-old woman who has been initiated on
from 4 weeks ago include hemoglobin A1C (A1C) 7.3%,
mirabegron 25 mg daily for UUI. She has tried nothing
SCr 1.1 mg/dL, and potassium 4.0 mEq/L.
else in the past for UI. Her medical history includes heart
failure, deep venous thrombosis (three episodes), hyper-
1. Which one of the following is the best intervention for
tension, hyperlipidemia, and generalized anxiety disorder.
R.Z.?
Her current home drugs are as follows: carvedilol 6.25 mg
A. Initiate duloxetine 40 mg twice daily. twice daily, lisinopril 10 mg daily, warfarin 3 mg daily,
B. Initiate furosemide 20 mg daily. digoxin 0.125 mg daily, pravastatin 40 mg daily, and
C. Discontinue amlodipine 5 mg daily. escitalopram 10 mg daily. T.R.s calculated CrCl is 60
D. Discontinue hydrochlorothiazide 25 mg daily. mL/minute/1.73m2 . Her sitting blood pressure today is
132/80 mm Hg, and her heart rate is 76 beats/minute.
2. Four weeks later, R.Z. returns, and her UI symptoms
have not resolved. The symptoms have been particu- 5. Which one of the following option groups would be
larly bothersome when she has been out searching for best to counsel T.R. to monitor for upon initiation of
a job. This has also worsened her depression. Which mirabegron?
one of the following would be best to initiate in R.Z.? A. Cough, shortness of breath.
A. Oxybutynin immediate release 2.5 mg twice B. Nausea, vomiting, and diarrhea.
daily. C. Swelling, warmth, redness in legs.
B. Solifenacin 5 mg daily. D. Significant muscle weakness.
C. Vaginal estrogen.
D. Duloxetine 40 mg twice daily 6. T.R. does well on mirabegron. Two months later, she
has been titrated to 50 mg daily and returns to the
3. A 62-year-old woman with urge urinary incontinence clinic for follow-up. She reports a significant decrease
(UUI) comes to your clinic. She is taking mirtazap- in incontinence symptoms. There have been no
ine 30 mg for depression, but her depression is not changes in her medications or medical history. T.R.s
improving. Her primary care physician wants to CrCl today is 45 mL/minute/1.73m2 . Blood pressure
switch her to fluoxetine 10 mg daily. Which one of the and heart rate today are 182/88 mm Hg and 86 beats/
following would be the best choice for this patients minute. Which one of the following is best to recom-
UUI to avoid drug interactions? mend regarding T.R.s mirabegron dosage?
A. Tolterodine. A. Continue at 50 mg daily.
B. Oxybutynin. B. Reduce to 25 mg daily.
C. Trospium. C. Change to solifenacin 5 mg daily.
D. Darifenacin. D. Change to duloxetine 40 mg twice daily.
PSAP 2013 Special Populations 16 Urinary Incontinence in the Older Adult
7. An 80-year-old community-dwelling woman describes 10. An 83-year-old man with Alzheimer disease is being
increased frequency and urgency with urination for the cared for at home. During the past 2 months, his wife
past 2 months. She denies pain with urination and does has noticed that it is increasingly difficult for him to
not have a fever today. Her medical history includes make it to the restroom in time to urinate. He has
hypertension and constipation with two episodes of stopped telling her when he needs to use the rest-
bowel obstruction. Her home drugs include senno- room, and she is unable to direct him to the restroom
sides 8.6 mg three times daily, docusate 100 mg twice in the house quick enough. This is causing significant
daily, lisinopril 5 mg daily, and aspirin 81 mg daily. She caregiver stress. His wife believes his cognition has
gets a rash with sulfa drugs. Her urinalysis is positive begun to worsen during the past 6 months, and she is
for bacteriuria. Which one of the following is best to considering placing him in a nursing home. His home
initiate in this patient? drugs include terazosin 2 mg at bedtime, aspirin 81
A. Ciprofloxacin 500 mg twice daily for 7 days. mg daily, donepezil 10 mg at bedtime, lisinopril 5 mg
B. Oxybutynin extended release 5 mg daily. daily, and venlafaxine extended release 75 mg daily.
C. Sulfamethoxazole 800 mg/trimethoprim 160 His Mini-Mental State Examination score is 15/30,
mg twice daily for 10 days. and his Geriatric Depression Scale is 3/15. Standing
D. Darifenacin 7.5 mg daily. blood pressure is 110/70 mm Hg. Which one of the
following is best to recommend for this patient?
Questions 8 and 9 pertain to the following case. A. Change terazosin to tamsulosin 0.4 mg daily.
P.Q. is a 62-year-old woman (height 60 inches, weight B. Start finasteride 5 mg daily.
56 kg) who has been using vaginal estrogen for 1 year C. Change venlafaxine to duloxetine 20 mg twice
for symptoms of stress urinary incontinence (SUI). This daily.
was effective until a couple of months ago, when her D. Discontinue donepezil 10 mg daily.
symptoms began to return. Her medical history includes
coronary artery bypass graft (times 1), hypertension, 11. Three weeks ago, a 69-year-old man began tak-
hyperlipidemia, osteoporosis, peripheral neuropathy, ing oxybutynin immediate release 5 mg three times
osteoarthritis, and depression. Her other medications daily for UUI. His medical history is significant for
include aspirin 81 mg daily, metoprolol 25 mg twice severe psoriasis, bipolar disorder, and osteoarthri-
daily, lisinopril 10 mg daily, rosuvastatin 10 mg daily, tis. He noticed about 2 weeks ago that he is having
alendronate 70 mg weekly, calcium carbonate 500 mg/ significant dry mouth. The patient has tried several
vitamin D 200 units twice daily, gabapentin 300 mg twice nonpharmacologic options recommended by his
daily, zolpidem 10 mg daily, ibuprofen 200 mg twice daily, local pharmacist, but none has worked. Oxybutynin
and bupropion SR 150 mg twice daily. Blood pressure is has been effective, and he is happy with the results on
158/76 mm Hg, heart rate 72 beats/minute, and SCr 1.1 his UUI symptoms. Before taking it, he was using the
mg/dL. P.Q. would like to try other drug therapy for her bathroom 20 times during the day; he feels this num-
UI because she and her husband travel a lot, and it is both- ber has been cut in half. However, he does not feel
ersome on these trips. Her symptoms occur throughout he will be able to take this medication much longer
the day, usually with coughing or sneezing. because of the dry mouth. Which one of the following
is best to recommend for this patient?
8. Which one of the following would be best to recom- A. Oxybutynin extended release.
mend for P.Q.? B. Oxybutynin transdermal patch.
A. Duloxetine 20 mg twice daily. C. Oxybutynin 10% gel.
B. Oral conjugated estrogens 0.3 mg/ D. Oxybutynin immediate release 5 mg at bedtime.
medroxyprogesterone 1.5 mg daily.
C. Pseudoephedrine 30 mg three times daily. 12. A 45-year-old man with multiple sclerosis has prob-
D. Solifenacin 5 mg daily. lems with increased urinary frequency and urgency
on a daily basis. He is currently taking no drugs for
9. Which one of the following drugs is most likely exac- this problem. In the past, he has tried oxybutynin
erbating P.Q.s incontinence? transdermal patch 3.9 mg/day and tolterodine imme-
A. Gabapentin. diate release 2 mg twice daily; neither resulted in
B. Ibuprofen. significant improvement. The patients PVR is 50 cc.
C. Lisinopril. Which one of the following is best to recommend for
D. Zolpidem. this patient?
A. Darifenacin 7.5 mg daily.
PSAP 2013 Special Populations 17 Urinary Incontinence in the Older Adult
B. Onabotulinum toxin A 200 units of A. Pedal edema caused by ibuprofen.
intradetrusor injection. B. Functional disability because of osteoarthritis.
C. Mirabegron 25 mg daily. C. Decreased parasympathetic tone because of the
D. Duloxetine 20 mg twice daily. aging process.
D. Weakening of the pelvic floor musculature
13. An 86-year-old man presents to the geriatrics clinic caused by loss of estrogen.
with new-onset dribbling and urinary urgency. His
medical history includes osteoporosis, insomnia, 16. Which one of the following is the best intervention to
depression, and type 2 diabetes mellitus. His home recommend for B.K.?
drugs include glipizide 5 mg twice daily, citalopram
A. Absorbent pads.
20 mg daily, diphenhydramine 50 mg at bedtime,
B. Decaffeinated coffee.
alendronate 70 mg weekly, cholecalciferol 1000 units
daily, simvastatin 10 mg daily, aspirin 81 mg daily, and C. Weight loss.
loratadine 10 mg daily. His PVR in the clinic today D. Fluid restriction.
is 310 cc. Recent laboratory test results include A1C
7.5% and SCr 1.2 mg/dL. Which one of the following 17. A 72-year-old woman (height 66 inches, weight 54 kg)
is best to recommend for this patient? receives a diagnosis of UUI. She lives with her spouse,
who is retired. She is mildly cognitively impaired and
A. Start tamsulosin 0.4 mg daily. has mild limitations in performing activities of daily
B. Start tolterodine extended release 2 mg daily. living. Her home drugs include donepezil 10 mg at
C. Increase glipizide to 10 mg twice daily. bedtime and memantine 10 mg twice daily for mod-
D. Discontinue diphenhydramine 50 mg daily. erate Alzheimer disease, pravastatin 40 mg in the
evening for hyperlipidemia, levothyroxine 75 mcg
14. A 69-year-old woman experiences urine loss when she daily for hypothyroidism, sertraline 50 mg daily for
coughs, sneezes, or lifts something heavy. She uses an depression, and metoprolol 25 mg twice daily for
incontinence pad for protection. She was started on hypertension. She does not smoke or drink alcohol.
estrogen 0.625 mg daily at menopause, but this was She drinks only decaffeinated coffee. Which one of
discontinued 5 years ago. Her medical history is sig- the following is best to recommend for this patients
nificant for six vaginal deliveries, osteoarthritis, UUI?
hypertension, and severe Alzheimer dementia. Her
home drugs include acetaminophen 1000 mg twice A. Discontinue donepezil 10 mg daily.
daily and lisinopril 10 mg daily. Which one of the fol- B. Begin trospium 20 mg daily.
lowing is best to recommend for this patients UI? C. Begin pelvic floor rehabilitation.
D. Begin prompted toileting on a regular schedule.
A. Pelvic muscle rehabilitation.
B. Periurethral injection of a bulking agent.
C. Duloxetine 40 mg twice daily. 18. A 76-year-old woman (height 62 inches, weight 59 kg)
D. Conjugated estrogen 0.625 mg daily. with a diagnosis of SUI continues to have frequent epi-
sodes, despite attempts at pelvic floor rehabilitation
with Kegel exercises. A pelvic examination reveals
Questions 15 and 16 pertain to the following case. normal genitourinary anatomy. Her medical his-
B.K. is a 57-year-old woman (height 65 inches, weight tory is significant for hypertension, hyperlipidemia,
64 kg) who has progressive difficulty with bladder con- insomnia, and chronic kidney insufficiency. Her
trol during the daytime. When she feels like she needs to home drugs include atorvastatin 40 mg daily, amlo-
use the toilet, she is sometimes unable to get to the bath- dipine 10 mg daily, enteric-coated aspirin 81 mg daily,
room on time. She has experienced a few accidents and and calcium 600 mg/vitamin D 400 international
is deeply embarrassed. When she exercises or coughs, she
units twice daily. Her blood pressure is 152/88 mm
loses small amounts of urine. Her home drugs include
Hg, and her heart rate is 68 beats/minute. Her most
alendronate 70 mg weekly for osteoporosis, loratadine 10
recent laboratory results are as follows: TC 182 mg/
mg daily for allergies, calcium carbonate 600 mg twice
dL, LDL cholesterol 111 mg/dL, sodium 135 mEq/L,
daily, vitamin D 1000 units daily, and ibuprofen 200 mg
chloride 101 mEq/L, potassium 3.8 mEq/L, serum
once daily for osteoarthritis. She is a lifelong smoker and
does not drink alcohol. She consumes 1 cup of regular cof- glucose 88 mg/dL, and SCr 1.5 mg/dL. Which one of
fee with each meal. She complains of some osteoarthritis the following is best to recommend for this patient?
pain and her pain scale rating is 2/10. A. Duloxetine 40 mg twice daily.
B. Pessary placement.
15. Which one of the following best explains B.K.s symp- C. Sacral nerve stimulation.
toms of UI? D. Midurethral sling.
PSAP 2013 Special Populations 18 Urinary Incontinence in the Older Adult
19. Two months ago, a 67-year-old man presented to
the clinic with symptoms of urinary urgency, noc-
turia, and incontinence. His incontinence episodes
are characterized by the loss of large amounts of
urine. His PVR was 45 mL, and his prostate exami-
nation was normal. He was initiated on oxybutynin
5 mg three times daily. Today, he returns to the clinic
for follow-up. He now reports that the symptoms of
urgency are improved, but he continues to be incon-
tinent of small amounts of urine both day and night.
His PVR today is 315 mL. His medical history is sig-
nificant for diabetes and congestive heart failure. His
other current drugs include glipizide extended release
10 mg daily, furosemide 20 mg every morning, potas-
sium chloride 20 mEq daily, lisinopril 40 mg daily,
metoprolol extended release 50 mg daily, and enteric-
coated aspirin 81 mg daily. His laboratory results are
as follows: A1C 7.6%, sodium 140 mEq/L, potassium
4.1 mEq/L, and SCr 0.9 mg/dL. Which one of the fol-
lowing best explains this patients current symptoms?
A. Increased urine volume secondary to
furosemide.
B. Increased intraabdominal pressure secondary to
angiotensin-converting enzyme inhibitor cough.
C. Detrusor underactivity secondary to
oxybutynin.
D. Urethral relaxation secondary to -blocker.
20. A 70-year-old man has difficulty with bladder control
since undergoing radical prostatectomy for pros-
tatic carcinoma 6 months ago. He reports excessive
dribbling and must wear a pad to prevent soiling his
clothing. He loses small amounts of urine during
physical exertion. Cystoscopy shows normal sphinc-
ter morphology. His medical history is significant
for hypertension, constipation, glaucoma, gastro-
esophageal reflux disease, and insomnia. His current
drugs include losartan 100 mg daily, senna 8.6 mg
daily, timolol 0.5% one drop in both eyes twice daily,
and pantoprazole 40 mg daily. His blood pressure is
153/82 mm Hg, and his SCr is 1.1 mg/dL. Which one
of the following is the best initial treatment for this
patient?
A. Duloxetine 40 mg twice daily.
B. Pseudoephedrine 30 mg twice daily.
C. Pelvic floor rehabilitation.
D. Artificial urethral sphincter.
PSAP 2013 Special Populations 19 Urinary Incontinence in the Older Adult
Learner Chapter Evaluation: Urinary Incontinence in the Older Adult.
As you take the posttest for this chapter, also evaluate the Use the 5-point scale to indicate whether this chap-
materials quality and usefulness, as well as the achieve- ter prepared you to accomplish the following learning
ment of learning objectives. Rate each item using this objectives:
5-point scale:
12. Evaluate symptoms to accurately classify a patient
Strongly agree with urinary incontinence.
Agree 13. Apply an understanding of the pathophysiology and
Neutral risk factors for urinary incontinence to patient care.
Disagree 14. Evaluate the most recent clinical evidence for
Strongly disagree pharmacologic and nonpharmacologic treatment of
urinary incontinence.
1. The content of the chapter met my educational 15. Design a patient-specific treatment plan to achieve
needs. optimal outcomes in an elderly patient with urinary
2. The content of the chapter satisfied my expectations. incontinence.
3. The author presented the chapter content effectively. 16. Assess for reversible causes in the patient with uri-
4. The content of the chapter was relevant to my prac- nary incontinence.
tice and presented at the appropriate depth and 17. Analyze the risks and benefits of using urinary
scope. incontinence medications in patients with dementia.
5. The content of the chapter was objective and 18. Please provide any specific comments relating to any
balanced. perceptions of bias, promotion, or advertisement of
6. The content of the chapter is free of bias, promotion, commercial products.
or advertisement of commercial products. 19. Please expand on any of your above responses, and/
7. The content of the chapter was useful to me. or provide any additional comments regarding this
8. The teaching and learning methods used in the chap- chapter:
ter were effective.
9. The active learning methods used in the chapter
were effective.
10. The learning assessment activities used in the chap-
ter were effective.
11. The chapter was effective overall.
PSAP 2013 Special Populations 20 Urinary Incontinence in the Older Adult
S-ar putea să vă placă și
- Pathomechanisms - Doc Bali 2010.doc RevisiDocument14 paginiPathomechanisms - Doc Bali 2010.doc RevisiApriliaÎncă nu există evaluări
- كوزرملا حاضو .د .م.أ لباب ةعماج/ بطلا ةيلك 2019 Urinary Incontinence. Involuntary loss of urine in sufficient amount or frequency to constituteDocument8 paginiكوزرملا حاضو .د .م.أ لباب ةعماج/ بطلا ةيلك 2019 Urinary Incontinence. Involuntary loss of urine in sufficient amount or frequency to constitutewzeer mohammedÎncă nu există evaluări
- Developing Geriatric Services For Incontinence in The ElderlyDocument5 paginiDeveloping Geriatric Services For Incontinence in The ElderlyrnrmmanphdÎncă nu există evaluări
- Urinary IncontinenceDocument7 paginiUrinary IncontinenceasuratosÎncă nu există evaluări
- 3028 Manuscript 19093 1 10 20210629Document13 pagini3028 Manuscript 19093 1 10 20210629stella.gillesania.chenÎncă nu există evaluări
- Diagnosis & Management of Urinary Incontinence: G. M. Punarbawa RSUD Prov NTB/FK UNRAMDocument39 paginiDiagnosis & Management of Urinary Incontinence: G. M. Punarbawa RSUD Prov NTB/FK UNRAMfarlamayanti100% (1)
- Urinary Incontinence in Individuals With Diabetes MellitusDocument1 paginăUrinary Incontinence in Individuals With Diabetes MellitusBulan GhafirahÎncă nu există evaluări
- Pathophysiology of Urinary Incontinence: Basic ScienceDocument6 paginiPathophysiology of Urinary Incontinence: Basic ScienceLauris TrujilloÎncă nu există evaluări
- Urogynecology and Pelvic ReconstructionDocument28 paginiUrogynecology and Pelvic ReconstructionIKM FKUNSOEDÎncă nu există evaluări
- Overview On The Management of Adult Urinary IncontinenceDocument7 paginiOverview On The Management of Adult Urinary IncontinenceMUHAMMMAD FAKHRIÎncă nu există evaluări
- Ariel Pemicu 5Document37 paginiAriel Pemicu 5yuliÎncă nu există evaluări
- A Case Study of Urinary Incontinence Treated With AcupunctureDocument5 paginiA Case Study of Urinary Incontinence Treated With AcupunctureHerald Scholarly Open AccessÎncă nu există evaluări
- Pharma-URO-U IncontinenceDocument27 paginiPharma-URO-U IncontinenceHussein AlhaddadÎncă nu există evaluări
- Presentation 3Document34 paginiPresentation 3Chidube UkachukwuÎncă nu există evaluări
- Management of Urinary Incontinence in Frail Elderly Women: PrevalenceDocument7 paginiManagement of Urinary Incontinence in Frail Elderly Women: PrevalenceKaren MoctezumaÎncă nu există evaluări
- Overview of Urinary Incontinence (UI) in The Long Term Care FacilityDocument81 paginiOverview of Urinary Incontinence (UI) in The Long Term Care Facilityالغزال الذهبيÎncă nu există evaluări
- Lower Urinary Tract Symptoms (LUTS) in Middle-Aged and Elderly MenDocument6 paginiLower Urinary Tract Symptoms (LUTS) in Middle-Aged and Elderly MenIrfanArifZulfikarÎncă nu există evaluări
- Urinary Incontinence From Harrison's IMDocument2 paginiUrinary Incontinence From Harrison's IMnashey08Încă nu există evaluări
- Urinary Incontinence in Elderly: DefinitionDocument13 paginiUrinary Incontinence in Elderly: DefinitionTarek AhmedÎncă nu există evaluări
- Evaluación de La Incontinencia Urinaria de Esfuerzo No Complicada en Mujeres Antes Del Tratamiento QuirúrgicoDocument4 paginiEvaluación de La Incontinencia Urinaria de Esfuerzo No Complicada en Mujeres Antes Del Tratamiento QuirúrgicoJosue Manuel Torres CalcinaÎncă nu există evaluări
- Urinary Incontinence in Men - UpToDateDocument31 paginiUrinary Incontinence in Men - UpToDatehochanh199xÎncă nu există evaluări
- Park 2019 PrescriberDocument7 paginiPark 2019 PrescriberElysabet aristaÎncă nu există evaluări
- Basic Gastroenterology: Including Diseases of the LiverDe la EverandBasic Gastroenterology: Including Diseases of the LiverÎncă nu există evaluări
- Pathophysiology of Female LUTS: 1 Storage DysfunctionDocument10 paginiPathophysiology of Female LUTS: 1 Storage DysfunctionJaneva SihombingÎncă nu există evaluări
- Overaktifitas Kandung KemihDocument4 paginiOveraktifitas Kandung KemihSarah PerezÎncă nu există evaluări
- GBHLN5 PR QHNP 5 Sy 5 CJDJ DFSDocument8 paginiGBHLN5 PR QHNP 5 Sy 5 CJDJ DFSyasmim16catarinaÎncă nu există evaluări
- Urinary IncontinenceDocument14 paginiUrinary Incontinencehussain AltaherÎncă nu există evaluări
- Committee Opinion: Evaluation of Uncomplicated Stress Urinary Incontinence in Women Before Surgical TreatmentDocument5 paginiCommittee Opinion: Evaluation of Uncomplicated Stress Urinary Incontinence in Women Before Surgical Treatmentw yÎncă nu există evaluări
- Urinary Incontinence: Diagnostic Evaluation and First-Line TreatmentDocument11 paginiUrinary Incontinence: Diagnostic Evaluation and First-Line Treatmentstalker2222Încă nu există evaluări
- Urinary Incontinence - DiagnosisDocument2 paginiUrinary Incontinence - DiagnosisHoney Roselle MorenoÎncă nu există evaluări
- Pathophysiology 1. Urinary Incontinence PathophysiologyDocument6 paginiPathophysiology 1. Urinary Incontinence PathophysiologyDenny BunÎncă nu există evaluări
- Path o Physiology o AbDocument8 paginiPath o Physiology o Ab0395Încă nu există evaluări
- CDN JU28 I4S2 10 DrDenisenkoSDocument6 paginiCDN JU28 I4S2 10 DrDenisenkoSCATHERIN JULIANA LIZANA BERRUÎncă nu există evaluări
- Managing Urinary Tract Problem: FOCUS On The FollowingDocument11 paginiManaging Urinary Tract Problem: FOCUS On The FollowingLovely DaroleÎncă nu există evaluări
- Enuresis FinalDocument21 paginiEnuresis FinalNac OsceÎncă nu există evaluări
- Voiding DysfunctionsDocument50 paginiVoiding DysfunctionsHemantÎncă nu există evaluări
- Tsakiris 2008Document9 paginiTsakiris 2008Mitchel Cordova LoaizaÎncă nu există evaluări
- Pelvic Congestion Syndrome - Beyond Menstrual CrampsDe la EverandPelvic Congestion Syndrome - Beyond Menstrual CrampsÎncă nu există evaluări
- Urinary Incontinence HandoutDocument6 paginiUrinary Incontinence HandoutGautam ReddyÎncă nu există evaluări
- Managing Urinary Incontinence in Older PeopleDocument5 paginiManaging Urinary Incontinence in Older PeopleSarah Naura IrbahÎncă nu există evaluări
- Clothier-Wright2018 Article DysfunctionalVoidingTheImportaDocument14 paginiClothier-Wright2018 Article DysfunctionalVoidingTheImportaMarcello PinheiroÎncă nu există evaluări
- 1 s2.0 S183695532100014X MainDocument8 pagini1 s2.0 S183695532100014X MainMetin HakkanÎncă nu există evaluări
- EtiologyDocument15 paginiEtiologyrendyjiwonoÎncă nu există evaluări
- Clinical Review: The Management of Lower Urinary Tract Symptoms in MenDocument4 paginiClinical Review: The Management of Lower Urinary Tract Symptoms in MenSan Phạm ĐìnhÎncă nu există evaluări
- Alexander, L., Shakespeare, K., Barradell, V., & Orme, S. (2015) - Management of Urinary Incontinence in Frail Elderly Women.Document8 paginiAlexander, L., Shakespeare, K., Barradell, V., & Orme, S. (2015) - Management of Urinary Incontinence in Frail Elderly Women.NurRahMatÎncă nu există evaluări
- Neurogenic BowlDocument21 paginiNeurogenic BowlFaridatul IsniyahÎncă nu există evaluări
- Geriatric Urinary Incontinence & UTI CaseDocument9 paginiGeriatric Urinary Incontinence & UTI CaseStarr NewmanÎncă nu există evaluări
- BPH - TextDocument7 paginiBPH - TextSomesh GuptaÎncă nu există evaluări
- Fecal Impaction A Cause For ConcernDocument7 paginiFecal Impaction A Cause For Concernadkhiatul muslihatinÎncă nu există evaluări
- Geriatric Urologic Disorder: Assignment 1 Name:moubark Saad Alsubaie Id:201713512 To Dr:kashifDocument7 paginiGeriatric Urologic Disorder: Assignment 1 Name:moubark Saad Alsubaie Id:201713512 To Dr:kashifmoubarkÎncă nu există evaluări
- Urinary IncontinenceDocument16 paginiUrinary IncontinenceOana BalintÎncă nu există evaluări
- Types of Urinary IncontinenceDocument1 paginăTypes of Urinary Incontinencehrg79qzwc2Încă nu există evaluări
- Denys 2021Document5 paginiDenys 2021Anabella ScottiÎncă nu există evaluări
- Sacral Neuromodulation For Bowel Dysfunction: Weledji EP and Marti LDocument11 paginiSacral Neuromodulation For Bowel Dysfunction: Weledji EP and Marti LPetrina Theda PhilothraÎncă nu există evaluări
- MOrelandDocument8 paginiMOrelandWalter GrismeyerÎncă nu există evaluări
- Urinary Incontinence in Dementia SendDocument25 paginiUrinary Incontinence in Dementia SendpahalaboassimanjuntakÎncă nu există evaluări
- Sci Bladder ProtocolDocument45 paginiSci Bladder ProtocolAbbas JafarzadehabbasÎncă nu există evaluări
- Causes and Treatment of Nausea and Vomiting: Aaron Bhakta and Rishi GoelDocument7 paginiCauses and Treatment of Nausea and Vomiting: Aaron Bhakta and Rishi GoelVini SasmitaÎncă nu există evaluări
- Urinary TractDocument3 paginiUrinary TractRifki MuhamadÎncă nu există evaluări
- BPH - TextDocument7 paginiBPH - TextSomesh GuptaÎncă nu există evaluări
- Jurnal 3Document10 paginiJurnal 3Nurul HafizaÎncă nu există evaluări
- Riu017003 0129Document11 paginiRiu017003 0129Nurul HafizaÎncă nu există evaluări
- Research Project Plan RP10-03 Urinary Incontinence Among Dependent Women and Men Over 80 Years in Relation To Staff Attitudes and KnowledgeDocument5 paginiResearch Project Plan RP10-03 Urinary Incontinence Among Dependent Women and Men Over 80 Years in Relation To Staff Attitudes and KnowledgeNurul HafizaÎncă nu există evaluări
- P TJ 3706345Document24 paginiP TJ 3706345Nurul HafizaÎncă nu există evaluări
- Research Project Plan RP10-03 Urinary Incontinence Among Dependent Women and Men Over 80 Years in Relation To Staff Attitudes and KnowledgeDocument5 paginiResearch Project Plan RP10-03 Urinary Incontinence Among Dependent Women and Men Over 80 Years in Relation To Staff Attitudes and KnowledgeNurul HafizaÎncă nu există evaluări
- AmiDocument26 paginiAmiNurul HafizaÎncă nu există evaluări
- Dinamika Psikologi Kekerasan SexualDocument18 paginiDinamika Psikologi Kekerasan SexualVasmi ArielÎncă nu există evaluări
- Research Project Plan RP10-03 Urinary Incontinence Among Dependent Women and Men Over 80 Years in Relation To Staff Attitudes and KnowledgeDocument5 paginiResearch Project Plan RP10-03 Urinary Incontinence Among Dependent Women and Men Over 80 Years in Relation To Staff Attitudes and KnowledgeNurul HafizaÎncă nu există evaluări
- Patients' Experience of Living With Glaucoma: A Phenomenological StudyDocument11 paginiPatients' Experience of Living With Glaucoma: A Phenomenological StudyNurul HafizaÎncă nu există evaluări
- Aop047 12-Sci1219 PDFDocument6 paginiAop047 12-Sci1219 PDFNurul HafizaÎncă nu există evaluări
- P TJ 3706345Document24 paginiP TJ 3706345Nurul HafizaÎncă nu există evaluări
- Research Project Plan RP10-03 Urinary Incontinence Among Dependent Women and Men Over 80 Years in Relation To Staff Attitudes and KnowledgeDocument5 paginiResearch Project Plan RP10-03 Urinary Incontinence Among Dependent Women and Men Over 80 Years in Relation To Staff Attitudes and KnowledgeNurul HafizaÎncă nu există evaluări
- 18 Bicer Original 10 1Document8 pagini18 Bicer Original 10 1Nurul HafizaÎncă nu există evaluări
- Daftar PustakaDocument5 paginiDaftar PustakaNurul HafizaÎncă nu există evaluări
- Andropause: Kemungkinan Terapi Sulih Testosteron Pada Pria LansiaDocument7 paginiAndropause: Kemungkinan Terapi Sulih Testosteron Pada Pria LansiaAchmad Ageng SeloÎncă nu există evaluări
- 2 1 1 SMDocument6 pagini2 1 1 SMNurul HafizaÎncă nu există evaluări
- 6 CFP Dies 2016 WidiyonoDocument13 pagini6 CFP Dies 2016 WidiyonoNurul HafizaÎncă nu există evaluări
- 18 Bicer Original 10 1Document8 pagini18 Bicer Original 10 1Nurul HafizaÎncă nu există evaluări
- A Case of Colloidal Nodular GoiterDocument7 paginiA Case of Colloidal Nodular GoiterboalapsihicaÎncă nu există evaluări
- Andropause: Kemungkinan Terapi Sulih Testosteron Pada Pria LansiaDocument7 paginiAndropause: Kemungkinan Terapi Sulih Testosteron Pada Pria LansiaAchmad Ageng SeloÎncă nu există evaluări
- S2 2016 353892 BibliographyDocument14 paginiS2 2016 353892 BibliographyNurul HafizaÎncă nu există evaluări
- 1 s2.0 S1347861316300251 MainDocument107 pagini1 s2.0 S1347861316300251 MainNurul HafizaÎncă nu există evaluări
- 1 s2.0 S0085253815334748 Main - 2Document7 pagini1 s2.0 S0085253815334748 Main - 2Nurul HafizaÎncă nu există evaluări
- J.S.S College of Nursing 1 Main Saraswathipuram, MysoreDocument18 paginiJ.S.S College of Nursing 1 Main Saraswathipuram, MysoreNurul HafizaÎncă nu există evaluări
- J.S.S College of Nursing 1 Main Saraswathipuram, MysoreDocument18 paginiJ.S.S College of Nursing 1 Main Saraswathipuram, MysoreNurul HafizaÎncă nu există evaluări
- 9789 1 17895 1 10 20140908Document6 pagini9789 1 17895 1 10 20140908Nurul HafizaÎncă nu există evaluări
- J.S.S College of Nursing 1 Main Saraswathipuram, MysoreDocument18 paginiJ.S.S College of Nursing 1 Main Saraswathipuram, MysoreNurul HafizaÎncă nu există evaluări
- J.S.S College of Nursing 1 Main Saraswathipuram, MysoreDocument18 paginiJ.S.S College of Nursing 1 Main Saraswathipuram, MysoreNurul HafizaÎncă nu există evaluări
- Iaat14i2p879 PDFDocument5 paginiIaat14i2p879 PDFNurul HafizaÎncă nu există evaluări
- Nursing Positions GuideDocument3 paginiNursing Positions Guidepianoman95Încă nu există evaluări
- Cabg 130102113345 Phpapp01Document29 paginiCabg 130102113345 Phpapp01md.dascalescu2486Încă nu există evaluări
- HyperthyroidismDocument54 paginiHyperthyroidismAsiah JelitaÎncă nu există evaluări
- Chapter 14:: Skin Barrier:: Akiharu Kubo & Masayuki AmagaiDocument21 paginiChapter 14:: Skin Barrier:: Akiharu Kubo & Masayuki Amagaililis nur faridaÎncă nu există evaluări
- Chapter 2 - Bone Structure and Directional Terminology - ShilandDocument20 paginiChapter 2 - Bone Structure and Directional Terminology - ShilandAdityaÎncă nu există evaluări
- SASE Reviewer (Science)Document5 paginiSASE Reviewer (Science)Cyrel Sudaria92% (37)
- Semester Iv Pharmacology I (BP404 TP) Multiple Choice Questions Chapter 1 & 2Document34 paginiSemester Iv Pharmacology I (BP404 TP) Multiple Choice Questions Chapter 1 & 2Aman Gurjar100% (1)
- Chapter 6-Additional Suffixes & Digestive System Term.Document7 paginiChapter 6-Additional Suffixes & Digestive System Term.api-19824406Încă nu există evaluări
- Co-Ordination-Questions (Sec3)Document2 paginiCo-Ordination-Questions (Sec3)Tiurma Simanjuntak MSiÎncă nu există evaluări
- Diffusion Effects in Enzymes Immobilized in A Porous MatrixDocument18 paginiDiffusion Effects in Enzymes Immobilized in A Porous MatrixAegee0% (1)
- Final PPT of GauravDocument24 paginiFinal PPT of Gauravkirti pawar100% (1)
- Connective Tissue NotesDocument6 paginiConnective Tissue Notesferdinand padillaÎncă nu există evaluări
- 4-Blood (Hematopoiesis-Leukopoiesis) PDFDocument9 pagini4-Blood (Hematopoiesis-Leukopoiesis) PDFUmair IkhlaqÎncă nu există evaluări
- Assignment 1 Class 9 Bio Cell Unit of LifeDocument3 paginiAssignment 1 Class 9 Bio Cell Unit of LifeL Sri MadhiÎncă nu există evaluări
- Medicinal Chemistry/ CHEM 458/658 Chapter 8-Receptors and MessengersDocument41 paginiMedicinal Chemistry/ CHEM 458/658 Chapter 8-Receptors and MessengersMehak SarfrazÎncă nu există evaluări
- Stewart and Buffer Base.Document69 paginiStewart and Buffer Base.Yohanes George100% (1)
- Physiological JaundiceDocument11 paginiPhysiological Jaundiceapi-3859062Încă nu există evaluări
- Modulo EminicDocument13 paginiModulo EminicAndreaÎncă nu există evaluări
- Anatomy ProstateDocument2 paginiAnatomy ProstateCarl Julienne MasangcayÎncă nu există evaluări
- notice-EVS Class 5 U1 T1 WSDocument23 pagininotice-EVS Class 5 U1 T1 WSGovind RajÎncă nu există evaluări
- ResumeDocument2 paginiResumeVisaal PradhanÎncă nu există evaluări
- Phlebotomy in A NutshellDocument131 paginiPhlebotomy in A Nutshellgreen_archerÎncă nu există evaluări
- 0610 s12 QP 11Document16 pagini0610 s12 QP 11Choudhry WalidÎncă nu există evaluări
- Surgery Final ExamDocument21 paginiSurgery Final ExamAhmad AbusalahÎncă nu există evaluări
- CompendioacupunturajaponesaDocument53 paginiCompendioacupunturajaponesaCarplast Ecuador100% (2)
- Ucsc TranscriptDocument8 paginiUcsc Transcriptapi-463075447Încă nu există evaluări
- Roleplay OxigenationDocument3 paginiRoleplay Oxigenationnia martsianiÎncă nu există evaluări
- Picturing MedicineDocument20 paginiPicturing MedicineGermain Rider FigueroaÎncă nu există evaluări
- Digestive System Choice Board #1 Jan 2-4, 2012Document3 paginiDigestive System Choice Board #1 Jan 2-4, 2012abisantiago6131Încă nu există evaluări
- Resume WeeblyDocument2 paginiResume Weeblyapi-458045374Încă nu există evaluări