Documente Academic
Documente Profesional
Documente Cultură
Tissue Procurement, Processing, and Staining Techniques
Încărcat de
Muhammad JameelTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Tissue Procurement, Processing, and Staining Techniques
Încărcat de
Muhammad JameelDrepturi de autor:
Formate disponibile
Cambridge University Press
978-0-521-87410-6 - Diagnostic Histochemistry
Edited by Mark R. Wick
Excerpt
More information
CHAPTER 1
CHAPTER 1
Tissue Procurement, Processing, and
Staining Techniques
Mark R. Wick, M.D.,
Nancy C. Mills, H.T., QIHC (ASCP), and
William K. Brix, M.D.
It is an unfortunate reality that many pathologists have sizes; partial or complete excisions done with a scalpel;
only a rudimentary knowledge of the effects of surgical electrosurgical excisions; and laser-mediated biopsies. In
technique and tissue processing on the final results that choosing one of these options, the operator should be cog-
will be obtained in stained microscopic sections. All too nizant of the two opposing ‘‘forces’’ that affect his or her
often, one is faced with a sample that has been obtained final decision on this matter. On the one hand, the patient
crudely, fixed badly, or mishandled in the histology labo- is often preoccupied with the cosmetic effects of a biopsy,
ratory, making morphologic interpretation of it needlessly and this typically induces the surgeon to limit the size of
complex. These faults typically occur not through willful the sample as much as possible. The opposing consideration
neglect of proper methodology but rather because of is represented by the degree of difficulty with which the
ignorance of the sequence of steps that constitute the science microscopic diagnosis is made by the pathologist—a factor
of histotechnology. Most trainees in pathology are not well that is often predictable by the amount of material that will
versed in the details of this laboratory discipline, making be required to study the disease process adequately.
them totally dependent on the expertise of their techni- The cardinal rule to be remembered on this topic is that
cians, or the lack of it. a properly done biopsy is virtually never cosmetically
Accordingly, this chapter will provide an outline of rec- deforming, if it can be accomplished in an outpatient set-
ommendations for the procurement and subsequent han- ting by a competent operator. In contrast, specimen inad-
dling of histopathologic specimens. Potential reasons for equacy and artifactual changes in tissue are problems that
poor results are also included. relate to faulty procedure, and these account for the great
majority of diagnostic obstacles that pathologists encoun-
ter. There is nothing quite so aggravating for the clinician
BIOPSY TECHNIQUES (and the patient) as to be informed that a second biopsy will
The specific procedures that are used in performing biop- be necessary because of these deficiencies, causing addi-
sies of clinical lesions are usually left to the discretion of the tional expense and anxiety.
attending clinician. This provision is not a problem if the As an example of these contentions, it is well known
operator has been adequately educated on the specific that malignant hematolymphoid proliferations and certain
advantages and disadvantages of various techniques, as ap- metastatic carcinomas are composed of extremely fragile
plied to specific diseases. However, it may prove to be a di- cells that are exquisitely susceptible to the compressive or
saster if the surgeon is inexperienced in such matters. shearing effects of some biopsies (Figure 1.1) (2). More-
Conventional or enzyme histochemistry, immunohistol- over, it is probable that several cubic millimeters of tissue
ogy, or electron microscopy—all of which are greatly af- will be necessary for the complete pathologic characteriza-
fected by nuances in tissue preservation—may be necessary tion of such lesions. Hence, a small biopsy specimen would
in some instances to obtain a firm diagnosis. Because the be predictably unsuitable in these circumstances. When in
clinician may not be able to anticipate these possibilities doubt, the clinician should contact the pathologist before
before obtaining the tissue sample, a predetermined rou- the procedure is done and inquire about recommended
tine should be followed in doing so (1). handling of the tissue sample and its minimally acceptable
There are basically four generic categories of proce- size based on the likely diagnostic possibilities.
dures that may be used in any given case. These include Other procedures causing reproducibly detrimental
punch biopsies, using circular cutting devices of several physical effects on tissue specimens are represented by
page 1
© Cambridge University Press www.cambridge.org
Cambridge University Press
978-0-521-87410-6 - Diagnostic Histochemistry
Edited by Mark R. Wick
Excerpt
More information
2 D IAGNOSTIC H ISTOCHEMISTRY
IDENTIFICATION AND ORIENTATION OF THE
BIOPSY SPECIMEN
There is nothing quite so exasperating for the pathologist
as to receive a specimen that is unoriented and for which no
anatomic location is given on the request form for patho-
logic examination. A lack of meaningful clinical history
or a failure to list potential clinical diagnoses often com-
pounds such omissions. These problems usually cannot be
solved by the pathologist and typically require a laboratory
visit by, or a telephone conversation with, the responsible
physician. In many instances, it would be medicolegally
dangerous to attempt a morphologic interpretation in the
absence of such information. On occasion, a specimen may
be received that is so poorly labeled that the identity of the
patient is even in question. Such a submission should
never be accepted by the laboratory unless the clinician is
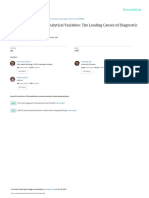
FIGURE 1.1: Smudging or ‘‘crush’’ artifact results from the mis- willing to provide written documentation verifying its or-
handling of tissue from fragile neoplasms such as lymphoma or igin and accepting exclusive legal responsibility for its
small cell carcinoma (shown here). interpretation.
If a lesion is a suspected malignancy for which a diag-
nostic biopsy is also intended to be a complete excision, the
electrocautery and laser excision. These methods enjoy clinician should provide some means of identifying the
wide clinical usage at present because of their ease of per- superior, inferior, medial, and lateral borders of the tissue
formance and the limitation of surrounding tissue damage sample. This can be accomplished by attaching sutures of
that they afford. Nonetheless, lesional cells in the specimen differing lengths or types to the specimen, and sending
are often rendered unrecognizable because of widespread a corresponding ‘‘map’’ of the tissue to the laboratory
thermal coagulation, precluding histologic interpretation along with the pathology request form (3). Alternatively,
altogether. It should therefore be obvious that cauterizing indelible (e.g., tattoo) ink of various colors can be affixed to
techniques must be avoided for diagnostic purposes. Sev- the borders of the specimen and identified accordingly
eral adjunctive pathologic studies require the availability of (Figure 1.2). As a minimal requirement—for example, in
specimens that have been handled in a special manner very small excisional biopsies—at least one pole of an el-
(Table 1.1). Again, these can be obtained prospectively liptical or circular tissue fragment should be labeled by
following preprocedural consultation with the laboratory. such means.
TABLE 1.1: Specimen Processing
Pathologic Technique Recommended Fixative Processing Time Comments
Conventional histology NBF or FA* 1 day Tissue should be sectioned at 2–3 mm for
good fixation
Immunohistology NBF or FA** 2–3 days Technique can be applied to frozen or fixed
sections
Electron microscopy 2% phosphate-buffered 3–4 days Tissue must be minced into 1- or 2-mm cubes
glutaraldehyde
Immunofluorescence None, if tissue is flash frozen; 1–2 days Tissue can be held in Michel’s medium for up
95% ethanol or acetone to 48 hours. Frozen tissue must be kept at
for touch preparations; 70°C until use
Michel’s medium for transportation
In situ hybridization NBF or FA for DNA studies; frozen 1 week DNA studies can be done on frozen or fixed
tissue preferred for RNA studies tissue
NBF = neutral-buffered 10% formalin, FA = NBF-ethanol (50%:50%).
* Tissue for routine histology can be fixed in B5 or Bouin’s solutions to improve nuclear morphology, but these preservatives require special processing
and compromise immunohistology.
** Certain tissue antigens (e.g., light chain immunoglobulins) are detectable only by frozen section immunohistochemistry.
© Cambridge University Press www.cambridge.org
Cambridge University Press
978-0-521-87410-6 - Diagnostic Histochemistry
Edited by Mark R. Wick
Excerpt
More information
Chapter 1 l Tissue Procurement, Processing, and Staining Techniques 3
FIGURE 1.2: Gross room inking stations (A) contain indelible inks of several colors, which can be applied to specimens with cotton-
tipped swabs and fixed in place with Bouin’s solution. The ink can then be seen in an FS (B) or permanent section.
The clinician should be discouraged from attempting to
prosect the specimen further before it is examined by the
pathologist, except in very well-defined settings. When
they are improperly performed, transections of small bi-
opsy samples often confound subsequent orientation steps
and may mechanically damage the lesion that is intended
for study. The only acceptable reason for undertaking fur-
ther clinical manipulation of the tissue sample is that of
preparing cellular ‘‘touch’’ preparations in examples of
suspected hematolymphoid disease. The latter can be
obtained if the operator bisects a lesion at its bulkiest point
and touches the cut surface of the tissue gently to glass
slides in a serial fashion (Figure 1.3) (2). When this is done,
special care should be taken subsequently to orient both
halves of the resulting two-part specimen for the patholo-
gist. Moreover, all air-dried or fixed touch preparations
must be labeled with the patient’s name, his or her date
of birth or medical record number, and the date on which
the procedure was performed.
PREPARATION OF FROZEN SECTIONS
Intraoperative consultations, generically termed ‘‘frozen
sections’’ (FSs) by many surgeons, are often requested in
treating presumed or proven malignancies (3,4). Proce-
dural aspects of the FS method are familiar to all anatomic
pathologists, but these will be reviewed briefly in this
section.
The purposes of obtaining FS examination are twofold;
it may be used to secure a rapid diagnosis for a lesion with
unknown histologic attributes, or the technique may be
employed to confirm that margins of excision are unin-
volved by the pathologic process in question. Because of
the potential distortion of morphologic detail that this pro-
FIGURE 1.3: Touch preparations can be made from fresh tissue
cedure may induce, the first of the cited applications is not
by serially touching a cut surface from it to adhesive-coated glass
one that should be used frequently. With respect to the slides (A). The touch imprint sections can then be air dried and
analysis of excisional margins, the operator must be certain stained with Romanowsky dyes, or briefly fixed in alcohol and
to supervise the orientation and labeling of all specimens, stained with H&E (B).
© Cambridge University Press www.cambridge.org
Cambridge University Press
978-0-521-87410-6 - Diagnostic Histochemistry
Edited by Mark R. Wick
Excerpt
More information
4 D IAGNOSTIC H ISTOCHEMISTRY
as outlined above. This makes the availability of indelible are then apposed to acid-cleaned glass slides that have been
ink an absolute requirement. kept at ambient temperature, causing the tissue to adhere
Following such steps, one must be certain that the tissue to them quickly. To eliminate concerns about the subse-
sample is small enough to assure rapid and uniform freez- quent loosening of this bond, slides that have been pre-
ing, and ease of sectioning with the cryomicrotome (cryo- coated with albumin, poly-L-lysine, or a chrome-alum gel
stat). The specimen is usually placed in a small pool of may be utilized (5).
gelatinous, water-soluble mounting medium (e.g., ‘‘opti- Most FS laboratories employ a brief (30–60 second)
mum cutting temperature’’ medium; CryogelR) that has fixation step immediately after mounted sections are pre-
been applied to a precooled Teflon or metal ‘‘chuck.’’ After pared, in Copland jars containing absolute acetone or 95%
making sure that the tissue is properly oriented on the flat ethanol. The slides may then be stained with hematoxylin
surface of this implement, it is then totally covered with and eosin (H&E), a ‘‘polychromatic’’ or metachromatic
additional mounting medium, fashioned into a circular reagent such as methylene blue, or other reagents. Follow-
pledget. Immediately thereafter, best results are obtained ing dehydration in graded alcohols and xylene, a synthetic
if the chuck is immersed in a bath of isopentane suspended mounting medium is placed over the tissue, and a glass
in an outer container of liquid nitrogen. These devices are coverslip is applied. Addition of a few drops of xylene to
available commercially, and they allow for virtually instan- the mounting medium will slightly lessen its viscosity and
taneous freezing of the mounting medium with minimal- help to prevent the entrapment of air bubbles under the
ization of ice crystal formation. The latter eventuality is coverslip.
undesirable because entrapment of ice in the specimen Alternatively, one may wish to keep some unstained FSs
(caused by slowly decreasing temperature) will cause sig- for future studies. This aim is best served by removing
nificant distortion (Figure 1.4) and may interfere with mi- slides from the acetone or alcohol fixative and placing them
croscopic interpretation. For this reason, the utilization of promptly in a freezer at 20 or 70°C. These can be kept in
metal cooling ‘‘plates,’’ which are incorporated into many such devices indefinitely for further analysis at a later date.
cryostats by their manufacturers, is not recommended as Specific problems connected with poor microtomy
a means whereby initial freezing is accomplished. How- technique will be considered subsequently in this discus-
ever, these plates are acceptable for maintaining the chucks sion. However, the most common difficulty that is seen in
in a frozen state while sections are being cut. the FS area can be ascribed to improper calibration of the
The microtome in any cryostat must be set in such cutting interval between successive sections. Overly thick
a manner that uniform sections of reproducible thickness sections may result in consumption of the tissue before
(approximately 5 lm) can be prepared. Regular mainte- a suitable slide is obtained for microscopic examination;
nance regarding the sharpness and integrity of microtomy in contrast, it is extremely hard to obtain very thin sections
blades is essential to this process. After ‘‘facing’’ the frozen without causing them to fold on themselves or shred.
block with the blade—to obtain a smooth, flat tissue Thus, it is essential for the cryostat to be checked fre-
surface—the operator cuts a ‘‘ribbon’’ of several individual quently to make certain that it is set up properly from
sections that can be kept flat by manipulation with a technical viewpoint. Also, there is no substitute for prac-
a camel-hair brush or with a Teflon-coated panel. These tice and experience on the part of the operator, in regard to
preparation of optimal FS slides. The labeling of speci-
mens used for FS examination should be no different than
that used for other samples. The remnant tissue should be
placed in a plastic cassette that is suitably inscribed with the
accession number of the case (preferably using a Cas-
MarkR-type labeler) and kept together with corresponding
paperwork for transmittal to the histology laboratory. Un-
der no circumstances should unlabeled frozen tissue be
allowed to accrue in the FS laboratory, lest disastrous
errors in identification occur.
FIXATION OF SPECIMENS
Questions that are often asked of the pathologist concern
the choice of one fixative solution over another for the
preservation of various cutaneous specimens. There is no
FIGURE 1.4: If ice crystals are allowed to form in tissue during
‘‘universal’’ fixative in pathology because tissue samples
the freezing process in a cryostat, linear defects will appear in the may be used for an ever-growing number of investigative
final FS. analyses, many of which demand that special processing
© Cambridge University Press www.cambridge.org
Cambridge University Press
978-0-521-87410-6 - Diagnostic Histochemistry
Edited by Mark R. Wick
Excerpt
More information
Chapter 1 l Tissue Procurement, Processing, and Staining Techniques 5
measures be applied in order to procure optimal results. Noncoagulative fixatives are the most widely used, and
Selected immunohistologic studies, electron microscopy, these include formaldehyde (called formalin when prepared
and genotypic assessment represent three advanced modal- in aqueous dilution and paraformaldehyde when employed
ities of pathologic evaluation that are associated with spe- in polymeric form), glutaraldehyde, acetic acid, potassium
cific fixation requirements. Laboratory specialists are dichromate, and osmium tetroxide. In contrast, acetone,
continuing to develop procedural modifications to lessen alcohols, chromium trioxide, mercuric chloride, and picric
the need for such provisions, but they still do exist. acid exemplify the coagulative preservatives. In the process
In the most optimistic of scenarios, it would be best to of denaturation and coagulation, a network of altered
submit all biopsies in their fresh state in physiologic saline protein is formed in tissue; in contrast, noncoagulative
solution, and for the pathologist to subdivide these speci- agents act to produce a stable intracellular ‘‘gel.’’ Acetone
mens into several parts for future diagnostic eventualities. and alcohol are the major nonaqueous reagents, with most
Nevertheless, this is often not practical for two main rea- others being soluble in water. Additive fixatives react
sons. First, outpatient specimens are commonly submitted with tissues by combining with them chemically, whereas
over long distances from the pathology laboratory, increas- nonadditive reagents (primarily alcohols and acetone) do not.
ing the likelihood that unfixed tissue will undergo autolysis Various combinations of these chemicals [e.g., formalin-
before it is received. Second, many biopsies are limited in alcohol or Carnoy’s solution (a mixture of ethanol, chloro-
size, making judiciousness in the selection of special studies form, and acetic acid)] are sometimes utilized as fixatives
an important point. The latter issue again emphasizes the that are intended to augment the stainability of predefined
wisdom of preprocedural consultation with the patholo- tissue components. Moreover, metal salts—such as those
gist, if unconventional evaluations are desired. containing zinc and mercury—may be added to aqueous
solutions, as in zinc-formalin or ‘‘B5’’ fixative (a mixture of
mercuric chloride, sodium acetate, and formalin). The ap-
Fixatives Used for ‘‘Routine’’ Histopathologic Examination parent effect of the latter agents is to stabilize complexes
In the great majority of cases, the clinician requesting his- that are formed by nucleic acid and protein, yielding im-
tologic examination of a biopsy is interested in a ‘‘tradi- proved preservation of nuclear detail. By convention, many
tional’’ interpretation based on microscopic findings as fixatives are named for the laboratory investigators who
seen with the H&E stains. With this stipulation in mind, devised them. Thus, one may encounter such designations
most laboratories have advocated the use of formalin as the as Bouin’s, Hollande’s, Zenker’s, Helly’s, Zamboni’s,
fixative of choice. Nonetheless, the following sections will Orth’s, and Carnoy’s solutions. Most of these are mixtures
briefly review the chemical characteristics of preservative of chemicals in different classes or showing differing effects
solutions in a broader sense, so that exceptions to the on proteins, with or without metal salts. Selected reagents
above-cited situation may be addressed. in this list will be alluded to later in this discussion.
One important concept to be borne in mind is that all
fixatives induce chemical artifacts in tissue sections. This
General Considerations effect has two potential ramifications for pathologists.
The preservative effects of certain chemicals have been First, we all become inured to the artifacts that we are
recognized for thousands of years, dating back to the an- accustomed to seeing with routine use of a particular pre-
cient Egyptians. On an empiric basis, therefore, various servative solution; indeed, we may even rely on such
fixatives have been employed to preclude bacterially medi- changes as diagnostic features. Changing the fixative one
ated putrefaction of human tissues since the inception of uses will also alter the tissue artifacts, often leading to in-
pathology as a discipline. terpretative confusion with any given staining method.
In the past century, detailed studies of these agents have Second, one artifact produced by a preservative may be
elucidated the probable mechanisms responsible for these desirable, whereas others are detrimental. For example,
beneficial effects (6–10). In addition to antibacterial ef- B5 solution yields excellent nuclear detail on H&E stains,
fects, fixatives also enhance the differences in refractive but it virtually destroys the integrity of some cellular pro-
indices between dissimilar tissue constituents, allowing teins that may be the targets of immunohistochemical
for greater resolution upon light microscopy. Moreover, studies (12). Lastly, the optimal period of fixation varies
they augment the affinity that chemical dyes have for par- greatly from one solution to another; tissue placed in for-
ticular cellular elements. It is now known that chemical malin may be allowed to remain in it for days with no
fixatives may be divided into two broad categories— compromise of morphologic features, whereas specimens
coagulating and noncoagulating—with respect to their in B5, Zenker’s, and Bouin’s fixatives must be transferred to
effects on proteins, which form the framework of virtually other chemical solutions after predefined periods of time
all cells. Further subdivision into aqueous and nonaqueous to avoid a serious loss of cellular definition (7,8). Thus, the
agents, as well as additive or nonadditive preservatives, is ultimate choice of a preservative solution is not one to be
also possible (11). made indiscriminately.
© Cambridge University Press www.cambridge.org
Cambridge University Press
978-0-521-87410-6 - Diagnostic Histochemistry
Edited by Mark R. Wick
Excerpt
More information
6 D IAGNOSTIC H ISTOCHEMISTRY
Specific Fixatives NBF ethanol (mixed in equal volumes) because it affords
Formalin: Formalin represents a 37–40% aqueous solu- a greater degree of tissue penetration than formalin alone.
tion of formaldehyde, the latter of which is marketed com-
mercially in the United States. Because the former reagent B5/Zenker’s/Helly’s Solutions: B5, Zenker’s, and Helly’s
is characteristically used at a 10% dilution, the final form- solutions were introduced because of their superiority over
aldehyde concentration is 3.7–4%. Various other chemi- NBF in the preservation of nuclear detail (7,8). They are
cals have been added to formalin to alter its stability and fixatives based on the inclusion of mercuric chloride, with
preservative capabilities, including calcium chloride, cal- or without sodium acetate, potassium dichromate, sodium
cium carbonate, ammonium bromide, sodium chloride, sulfate, acetic acid, and formaldehyde as additional constit-
sodium phosphate, sodium hydroxide, and absolute ethyl uents. Because of the excellent morphologic detail that is
alcohol. Among these mixtures, that consisting of forma- achievable with these solutions, many laboratories prefer
lin, distilled water, and monobasic/dibasic sodium phos- them for the routine preparation of H&E-stained sections.
phate is the most widely employed and is known as ‘‘10% Nevertheless, there are three distinct disadvantages of B5,
neutral-buffered formalin’’ (NBF). Paraformaldehyde is Zenker’s, or Helly’s reagent, as compared with NBF. Tis-
a polymerized form of formaldehyde admixed with meth- sue sections must be removed from the former three fix-
anol; it is generally employed as a fixative for specialized atives after no more than 8 hours and placed into 70%
immunohistologic procedures, particularly when com- ethanol; if this is not done, specimens will become ex-
bined with periodate and lysine (‘‘PLP’’ solution) (12,13). tremely brittle and virtually impossible to section (11).
Although it is a general-purpose fixative and yields good Also, the presence of mercuric chloride will cause deposi-
morphologic detail when prepared properly, NBF does tion of pigment in microscopic preparations, which must
have some disadvantages in tissue pathology. First, any be removed with iodine before final staining procedures
solution containing formaldehyde is potentially carcino- are done. Lastly, mercury-based solutions are powerful co-
genic, and levels of formalin vapor in the ambient air of agulating agents and therefore damage many cytoplasmic
the laboratory must be measured regularly by governmen- proteins. This effect commonly renders tissue sections un-
tal mandate. The maximum permissible exposure limit for suitable for a variety of immunohistochemical studies (12).
any individual employee is 1 part per million over an
8-hour period, as established by the Occupational Safety Bouin’s Solution: Bouin’s fixative is again based on form-
and Health Administration (14). Second, poorly prepared aldehyde as a major component, together with picric and
NBF, which has been buffered erroneously and has a pH acetic acids in aqueous solution. Like B5, this reagent
outside of the physiologic range, may cause unwanted pre- affords excellent preservation of nuclear morphology but
cipitates of ‘‘black acid hematin pigment’’ in tissue sec- suffers from failings pertaining to brittleness of tissue, pig-
tions. The latter has a dark particulate appearance, and ment deposition, and adverse effects on cytoplasmic poly-
may simulate microorganisms on a histologic slide. These peptides. In addition, Bouin’s-fixed specimens acquire
two possibilities can be distinguished through the use of a yellow color (because of the effects of picric acid) that
polarization microscopy because hematin pigment is bire- must be removed by postfixation washing in alcohol and
fringent, whereas microbes are not (11). Third, NBF that is lithium carbonate. Bouin’s fixative is preferred for visual-
allowed exposure to ambient air for prolonged periods of ization of delicate mesenchymal tissues because of its su-
time (as with large ‘‘batches’’ that are diluted for use in the perior differentiating abilities in regard to these elements
gross laboratory) will develop high levels of formic acid. (11). Accordingly, some ‘‘stromal’’ special stains (such as
The latter is detrimental to protein substructure and may the Masson trichrome method) are best performed on
accentuate the formation of methylol bonds between poly- specimens preserved in this solution.
peptides. This effect can ‘‘mask’’ proteinaceous epitopes
that correspond to the targets of immunohistologic anti- Acetone and Alcohols: Acetone and alcohols are rapidly
body reagents (15). Lastly, formalin has a limited capacity acting fixatives with good penetration of tissue. They also
for penetration of bulky pieces of tissue, and specimens afford better preservation of some cytoplasmic enzymes
fixed in it must be no thicker than 4–5 mm. than formaldehyde-based solutions do, in paraffin sections.
Despite these drawbacks, formalin is inexpensive and However, two major disadvantages attend the use of these
widely available, and is therefore ubiquitously employed organic reagents. They cause striking shrinkage of tissue
as the fixative of choice for clinical specimens. The because of their dehydrating effects, thereby altering mor-
above-cited failings of this preservative can be prevented phologic details appreciably. Also, acetone and methyl or
by careful technique in its preparation, adherence to envi- ethyl alcohol are relatively expensive, and they require spe-
ronmental monitoring requirements, and application of cial storage and inventory procedures because of possible
proper prosection and fixation techniques for the submis- use by laboratory workers as inebriants. In current prac-
sion of tissue sections. Some laboratories prefer to use tice, these agents are usually applied only in the fixation of
© Cambridge University Press www.cambridge.org
Cambridge University Press
978-0-521-87410-6 - Diagnostic Histochemistry
Edited by Mark R. Wick
Excerpt
More information
Chapter 1 l Tissue Procurement, Processing, and Staining Techniques 7
touch preparations and are not commonly utilized in the Specimen size is, in contrast, a potentially crucial factor
processing of biopsy specimens. Similar comments apply affecting quality of fixation, and this determinant goes
to Carnoy’s solution, which is constituted by ethyl alcohol, hand in hand with the volumetric relationship between
chloroform, and acetic acid. a tissue sample and the solution in which it is immersed.
Large, extremely thick specimens will be inadequately pen-
Decalcifying Solutions: Some biopsy samples may contain
etrated by most fixatives, allowing autolysis to proceed
obvious foci of calcium salts, as suggested by anatomic
unchecked in their central areas. This problem results in
location, clinical findings, or difficulty in performing the
eventual loss of the unfixed foci during microtomy, yield-
biopsy procedure. In these circumstances, two main meth-
ing microscopic sections that resemble doughnuts (Figure
ods exist for the removal of such minerals from the speci-
1.5). Because penetration is facilitated by minor thermal or
men. One employs simple acids (hydrochloric or nitric),
mechanical currents in the fixative solution, large speci-
which rapidly solubilize calcium deposits. The other tech-
mens that are covered with an inadequate volume of pre-
nique is based on the ability of certain chelating agents—
servative will predictably be underfixed. An experienced
such as ethylenediaminetetraacetic acid (EDTA)—to ac-
histotechnologist typically detects this problem upon
complish this task. The second of these methods is much
attempting microtomy of the tissue and will ‘‘run the spec-
gentler and does not cause the loss of microscopic detail
imen back’’ for more prolonged fixation and reprocessing.
that acid decalcification may incur. Fixation is allowed to
However, this consumes additional time and should be
progress in concert with decalcification with both acidic
unnecessary.
and EDTA reagents because they are commercially mar-
As noted at several points in the foregoing discussion,
keted as mixed solutions containing formaldehyde.
there is a maximum recommended period of fixation with
Glutaraldehyde: Glutaraldehyde is similar in chemical several preservatives, over which unwanted changes repro-
activity to formaldehyde; both cause cross-linkage of ducibly occur in tissue biochemistry. Overfixed specimens
proteins in tissue (7). However, glutaraldehyde penetrates are difficult to cut and often demonstrate alterations in
specimens very slowly, making the size of the tissue sample morphologic definition or antigenic integrity. In contrast,
a critical determinant of fixation with this reagent. More- underfixation allows bacterial putrefaction to proceed,
over, 2–4% glutaraldehyde (representing the usual work- similarly damaging the tissue sample. Specimens that are
ing concentration) has a propensity to cause brittleness of immersed in the most commonly used preservative—
specimens that are immersed in it for more than 2–3 hours; NBF—should ideally be processed further within 8–12
transfer to a buffer solution is absolutely necessary after hours.
this point. For these reasons, among others, glutaralde- The pH of fixatives is not critical for light microscopy,
hyde is not used often for the preservation of biopsy sam- except that certain unwanted pigmentary deposits may
ples that are intended for light microscopy. However, it is be seen with unduly acidic preservatives. Nonetheless, hy-
the preferred fixative for electron microscopy, wherein peracidity is extremely detrimental to cellular ultrastruc-
specimens are very small and limited ‘‘hardening’’ of tissue ture and also to the maintenance of tissue antigenicity
may actually be morphologically advantageous.
Other Factors Influencing Fixation
As outlined by Carson (11), there are several other consid-
erations in the fixation of tissue besides one’s choice of
preservative solution. These include temperature, size of
the sample, the volume ratio of tissue to fixative solution,
the duration of fixation, and the pH of the solution.
Recently, the rapid but controlled elevation of temper-
ature with microwave ovens has been utilized as an in-
dependent means of fixation, by coagulation of tissue
proteins (16). Surprisingly, this process appears to have
little if any adverse effect on staining characteristics, even
with immunohistologic methods. However, it must be em-
phasized that careful control is the key to thermal fixation;
overheating may completely destroy the specimen if it is
allowed to reach an extreme level (e.g., over 65°C). In
FIGURE 1.5: Inadequate fixation of tissues—especially fatty
a more conventional context, there are really no compel- ones—will often result in loss of the central areas of tissue blocks
ling reasons to employ fixative solutions at one tempera- in final microscopic sections because they ‘‘fall out’’ during
ture versus another. processing.
© Cambridge University Press www.cambridge.org
Cambridge University Press
978-0-521-87410-6 - Diagnostic Histochemistry
Edited by Mark R. Wick
Excerpt
More information
8 D IAGNOSTIC H ISTOCHEMISTRY
(11,12). For these reasons, it would be wise to control pH latter drawback, but they are subject to chemical carryover
within the physiologic range during fixation, in the event from one reagent pumping step to another. This poten-
that electron microscopy or immunohistology is necessary tially compromises the dehydration-clearing sequence. On
diagnostically. balance, individual experience on the part of technologists
and pathologists ultimately determines which type of pro-
Tissue Processing and Preparation of cessor will be chosen.
Microscopic Sections
Because most commonly employed fixatives are aqueous in
nature, the next step in tissue processing is usually that of EMBEDDING AND SECTIONING OF
dehydration and ‘‘clearing’’ (removal of all water from the BIOPSY SPECIMENS
specimen). Graded solutions of ethanol are used for this The final stations in any tissue processor infiltrate all speci-
purpose, and these must be changed frequently to maintain mens with paraffin or another wax-based embedding me-
their desiccating properties. A variety of clearing agents are dium. Thereafter, the technologist removes each biopsy
available, but the most common are xylene and limonene (one at a time) from its metal or plastic cassette and pro-
derivatives. In likeness to the alcohols, such reagents may ceeds to embed it in a rectangle of additional liquid wax,
be contaminated by water with repeated use and should be with attention to the proper orientation of the tissue sam-
monitored closely for this problem. ple. The pathologist may direct this process by notching or
Xylene is inexpensive and does not leave a residue on inking one or several surfaces of the specimen (Figure 1.6)
glassware or other instrument parts in the histology labo- and providing a ‘‘map’’ in accompanying paperwork that
ratory. In light of these virtues, it is the most popular clear- indicates whether these should be placed facedown, faceup,
ing agent. However, xylene fumes are potentially toxic to or in parallel with the lateral aspects of the cassette. Such
technologists, making careful storage, controlled disposal, provisions are usually necessary only with large pieces of
and environmental monitoring mandatory. In addition, we tissue. For example, technologists accustomed to handling
have found that xylene may damage the protein substruc- skin biopsies will, as a matter of routine, orient the epider-
ture of certain fragile tissue antigens (12). Limonene-type mis perpendicularly to the bottom of the cassette mold and
clearing agents are derived from plants and are therefore facing one of its long sides. If several pieces of tissue are
biodegradable. They have a strong odor—like that of lem- included in the same block, these are best arranged
ons or oranges—which is alternatively perceived as pleas- diagonally.
ant or noxious by various people. Other disadvantages of The embedding step is a potential source of great irri-
limonenes are that they leave a residue on mechanical tis- tation (and medicolegal liability) for the pathologist if it is
sue processors and may sometimes interfere with the ad- done by an inexperienced or careless laboratory worker.
herence of tissue sections to glass slides. The microtomy of With few exceptions, small biopsy specimens that are ori-
specimens cleared in limonenes has been said to be easier ented improperly cannot be interpreted microscopically
than that encountered with xylene (11). (Figure 1.7), necessitating that the block be remelted and
In the relatively early days of histotechnology, all de-
hydration and clearing steps were done by hand. Over
the past 45 years, however, a variety of automatic tissue
processors have been engineered and marketed. These
are used widely at present and may be divided into two
main groups—‘‘open’’ and ‘‘closed.’’ Open processors
mechanically transfer baskets containing tissue cassettes
from one ‘‘station’’ (chemical bath) to another, on a com-
puter-driven schedule. The latter may be altered by the
operator to change the time of dehydration, clearing, or
other steps. Closed instruments vary the solutions to
which each specimen basket is exposed by pumping chem-
icals in and out of fixed chambers, again according to a pro-
grammed schedule. In other words, open processors move
specimens, whereas closed processors move chemical
solutions.
Each of these two types of instruments has advantages
and disadvantages. Open processors show a low incidence
FIGURE 1.6: This microscopic section of a breast biopsy shows
of reagent contamination from one station to another, but the intersection of two anatomic planes that were labeled by the
they are subject to the mechanical ‘‘hang-up’’ of specimen submitting surgeon, and inked with two different colors by the
baskets in transit. Closed processors do not suffer from the prosecting pathologist.
© Cambridge University Press www.cambridge.org
Cambridge University Press
978-0-521-87410-6 - Diagnostic Histochemistry
Edited by Mark R. Wick
Excerpt
More information
Chapter 1 l Tissue Procurement, Processing, and Staining Techniques 9
FIGURE 1.7: Malorientation of biopsy ‘‘tips’’ or bisected biopsy FIGURE 1.8: ‘‘Chatter’’ artifact in tissue sections is the result of
specimens at the embedding station, as shown here, will compro- loose microtome blades or poor microtomy technique.
mise the pathologists’ ability to evaluate the true specimen mar-
gins for tumor involvement. Reprocessing may or may not solve
this problem, and every effort should be made to avoid it in the temperature of paraffin or Carbowax stations in the tissue
first place. processor, and at the embedding center, must be monitored
closely. Overheating the wax will cause unwanted thermal
re-embedded. This takes time, and in the process of facing artifacts in the tissue and compromise its cellular detail.
the poorly oriented specimen for preparation of initial sec- Excessively cool wax fails to infiltrate the specimens
tions, valuable tissue may be lost (17). adequately.
In order to circumvent embedding difficulties, some Another class of embedding compounds that is pres-
pathologists have taken to pre-embedding small biopsies ently in vogue in some centers is represented by polymeric
in agar before they are put in cassettes for fixation. This plastic resins such as glycol methacrylate or epoxy. Disad-
does assure proper orientation, but agar will not ‘‘fix’’ in vantages of these compounds include the necessity of cut-
the same manner that tissue does, nor will it respond sim- ting corresponding tissue sections with a glass or diamond
ilarly to dehydration, clearing, and infiltration by wax. All knife microtome, and the requirement for a transitional
these factors may cause the tissue to ‘‘pop’’ free of the fluid, such as propylene oxide, to embed the tissue after
surrounding agar after embedding and during tissue sec- dehydration and clearing (11). Moreover, plastic sections
tioning, defeating the purpose of the agar impregnation are difficult to stain with the same intensity as that seen in
step altogether. Therefore, we do not advocate this pro- paraffin-embedded preparations. The main advantage of
cedure, rather preferring to educate technologists on the plastic media is that extremely thin, flat sections may be
details of orientation during wax embedding. Even a very prepared by experienced microtomists, providing exquisite
small biopsy can be appropriately configured in the wax cellular detail. In addition, some enzyme-histochemical
block, with the use of a magnifying lens or dissecting staining methods that otherwise require the use of FSs
microscope. are possible with specimens embedded in epoxy or glycol
Paraffin is still the most widely utilized embedding methacrylate.
medium, but some laboratories have opted to employ Histomicrotomy is a seemingly straightforward pro-
‘‘Carbowax’’ as a substitute. The latter compound is a water- cess, representing the cutting of serial paraffin-embedded
soluble wax, making dehydration and clearing of the tissue sections with a tissue microtome. Nevertheless, this tech-
unnecessary and allowing for direct infiltration of formalin- nique has many hidden traps that relate to the proper
fixed tissue with embedding medium in the tissue processor maintenance, calibration, and orientation of cutting
(11). This element of simplicity is attractive, but Carbowax blades; preparation of paraffin blocks; and dexterity of
has its drawbacks. One concerns the dissolution of the em- the technologist. Microtome blades that are dull loose or
bedding medium when microtomized tissue ribbons are nicked will produce ‘‘chatter’’ or ‘‘venetian blind’’ artifacts
placed in a water bath prior to mounting them on glass in tissue sections (Figure 1.8). In addition, the ‘‘clearance
slides. This unwanted eventuality makes it difficult for the angle’’ (between the tissue block and the microtome knife)
technologist to keep the tissue section flat, resulting in unde- is crucial to good technique. It should be approximately
sirable folds in the final stained slide. Second, we have noted 3–8°. If the angle is too narrow, alternately thick and thin
irregularities in antigen preservation when Carbowax- sections are cut, or they are folded on themselves (18–20).
embedded tissues are studied immunohistologically. The An excessive clearance angle causes chattered or otherwise
© Cambridge University Press www.cambridge.org
Cambridge University Press
978-0-521-87410-6 - Diagnostic Histochemistry
Edited by Mark R. Wick
Excerpt
More information
10 D IAGNOSTIC H ISTOCHEMISTRY
hideous sections and may preclude the ability of the tech- One of the most dangerous of all mistakes in the histol-
nologist to obtain a tissue ribbon. Even worse are the ogy laboratory can take place when mounting sections
effects of loose microtome blades or tissue blocks in the from flotation baths. Friable tissue may ‘‘shed’’ small frag-
microtome chuck. These deficiencies may shatter the par- ments that float free on the surface of the water, and these
affin block entirely or deeply groove the tissue specimen. A may be inadvertently picked up when mounting slides from
block that is mounted crookedly in the microtome chuck subsequently processed unrelated cases. Derisively known
will produce irregular ribbons or cause individual sections as ‘‘floaters,’’ these rogue pieces of tissue commonly cause
in the ribbon to break free from one another. agonizing interpretative problems for the pathologist (Fig-
Regardless of whether one uses paraffin or Carbowax as ure 1.9). For example, it is not difficult to envision a small
an embedding medium, there is still a need to refrigerate piece of a prostatic carcinoma that may find its way onto
tissue blocks before microtomy is attempted. This step slides of another prostate biopsy, a ribbon of which is
hardens the wax slightly and allows for crisp sections to mounted subsequently in the same water bath. Technolo-
be cut. Warm blocks will yield wrinkled ribbons or cause gists must be impressed with the tremendous medicolegal
successive sections to anneal to one another. In addition, liabilities that such a mistake incurs, and they must rou-
failure to moisten the surface of blocked tissue suitably tinely skim, or otherwise clear, the surface of the water bath
before cutting it yields an excessive number of knife marks between cases. An alternative source of floater-type arti-
or fragmented sections. The technologist can simply rub facts is the ‘‘tongue blade metastasis,’’ wherein tissue
a wet finger over the block several times prior to micro- adheres to a wooden applicator stick that is used to float
tomy, if the specimen is small. If it is large, and particularly successively prepared ribbons from two different cases
if the tissue is heavily cornified, a wet piece of cloth or (11). Needless to say, this practice is highly inadvisable.
cotton soaked in 5% ammonium hydroxide may be applied With respect to optimizing the cost of slide preparation,
for 2 or 3 minutes to rehydrate the tissue face (18). we recommend that as many individual sections as possible
Another problem that is sometime seen at this step is the should be mounted on one slide, from the same ribbon. It is
tendency for ribbons to ‘‘fly’’ onto the knife blade. This is not difficult for adept technologists to include three to five
the result of static electricity between the wax or tissue and cuts of a specimen on each slide, arranged in a serial fash-
the metal blade, and also may be avoided by slightly moist- ion. Also, in light of the limited size of many skin, bron-
ening the knife and the block surface before each ribbon is choscopic, and gut biopsies, it is advisable to save any
prepared. unmounted paraffin ribbons (with appropriate identifica-
tion) from such cases for 1 week after they are accessioned.
Remounts can be prepared from these directly, without the
MOUNTING OF TISSUE SECTIONS need for further microtomy of the tissue block.
The wax ribbon of serial tissue sections can be removed Finally, the identification of tissue sections must be
from the microtome knife as it is cut, by using a wooden scrupulously maintained throughout the remainder of
tongue depressor blade. In this process, the operator exerts their sojourn in the histology laboratory. Such a necessity
slight traction on the end of the ribbon, stretching it grad- is assured by having the technologist scratch the case and
ually over the wooden blade, and subsequently depositing
it on the surface of a warm water bath at the cutting station.
The temperature of such flotation devices should be kept at
5–10°C below the melting point of the embedding wax. If
it is too hot, desiccated-looking sections will result; in con-
trast, cool flotation baths produce excessive wrinkling of
the tissue.
To facilitate the process of obtaining a smooth,
unwrinkled, paraffinized ribbon of tissue, it can be
stretched by slight traction on its ends while floating in
the warm water bath. Also, we have found that adding
a few milliliters of ethyl alcohol to the water is beneficial
in this regard. The ribbon must not be left in the bath for
more than 1 or 2 minutes, or spurious overhydration of the
tissue will be produced. This effect simulates the appear-
ance of edema fluid microscopically (17). Because tissue
sections do not adhere well to untreated glass slides,
a bonding agent also must be a component of the water FIGURE 1.9: ‘‘Floaters’’ (lower left) in microscopic sections are
bath. Elmer’s-GlueR, albumin, and poly-L-lysine are all unwanted pieces of tissue from other cases. They may cause seri-
suitable additives of this type. ous diagnostic mistakes and again should be avoided at all costs.
© Cambridge University Press www.cambridge.org
S-ar putea să vă placă și
- SQL-Problems Solutions PDFDocument11 paginiSQL-Problems Solutions PDFManpreet Singh100% (1)
- Case Study FormatDocument5 paginiCase Study FormatMyra Lyn Olores100% (1)
- Surgical Pathology IntroductionDocument10 paginiSurgical Pathology IntroductionRenatoCosmeGalvanJuniorÎncă nu există evaluări
- An Overview of Clinical Molecular GeneticsDocument352 paginiAn Overview of Clinical Molecular GeneticsQapaq ApuÎncă nu există evaluări
- Tissue Pathways For Breast Pathology: September 2010Document9 paginiTissue Pathways For Breast Pathology: September 2010fadoÎncă nu există evaluări
- Percutaneous Needle BiopsyDocument13 paginiPercutaneous Needle BiopsyAngelina JojoÎncă nu există evaluări
- CHAPTER 20 Fine Needle Aspiration Biopsy Techniques 2008 Comprehensive Cytopathology Third EditionDocument19 paginiCHAPTER 20 Fine Needle Aspiration Biopsy Techniques 2008 Comprehensive Cytopathology Third EditionXochitl ZambranoÎncă nu există evaluări
- Importance of Biopsy ProceduresDocument6 paginiImportance of Biopsy Procedureskatherine.hernandez.celeÎncă nu există evaluări
- Uses of biochemical data in clinical diagnosis and managementDocument5 paginiUses of biochemical data in clinical diagnosis and managementnour achkarÎncă nu există evaluări
- Vulva Biopsias HistopatologiaDocument10 paginiVulva Biopsias HistopatologiamariajoseoyanederÎncă nu există evaluări
- Pi Is 2213219820312435Document3 paginiPi Is 2213219820312435BrilliantÎncă nu există evaluări
- Endoscopic Mucosal Tissue Sampling ASGE 2013Document9 paginiEndoscopic Mucosal Tissue Sampling ASGE 2013DannyÎncă nu există evaluări
- Diagnosis MikrobiologiDocument14 paginiDiagnosis Mikrobiologiarmelya aisyahÎncă nu există evaluări
- Favaloro 2010Document13 paginiFavaloro 2010Yohana SetiawanÎncă nu există evaluări
- My Approach To Interstitial Lung Disease Usingclinical, Radiological and Histopathological PatternsDocument15 paginiMy Approach To Interstitial Lung Disease Usingclinical, Radiological and Histopathological PatternsMarcelle FreireÎncă nu există evaluări
- Molecular Diagnostics: An OverviewDocument5 paginiMolecular Diagnostics: An OverviewDanielRbÎncă nu există evaluări
- Cytology of Bone Fine Needle Aspiration BiopsyDocument11 paginiCytology of Bone Fine Needle Aspiration BiopsyRavi MehrotraÎncă nu există evaluări
- how-to-read-pathology-report.pdf_college of american pathologist_HODocument2 paginihow-to-read-pathology-report.pdf_college of american pathologist_HOdr.davidsitinjakÎncă nu există evaluări
- Variables Pre Post AnaliticaDocument29 paginiVariables Pre Post AnaliticaRandy HuyhuaÎncă nu există evaluări
- Malpractice For OncologistsDocument7 paginiMalpractice For OncologistsMuhsin ChistiÎncă nu există evaluări
- IDSA GUIDELINES: Practice Guidelines for the Management of Bacterial MeningitisDocument18 paginiIDSA GUIDELINES: Practice Guidelines for the Management of Bacterial MeningitisLuis Diego López ManjarresÎncă nu există evaluări
- Introduction and Safety in the Histopathology LabDocument4 paginiIntroduction and Safety in the Histopathology LabDanielle CapangpanganÎncă nu există evaluări
- 45 Supplement - 2 S99Document13 pagini45 Supplement - 2 S99Mustaqeem DawarÎncă nu există evaluări
- Practice Guidelines For The Management of Bacterial MeningitisDocument18 paginiPractice Guidelines For The Management of Bacterial MeningitishomayoonÎncă nu există evaluări
- Diagnostic Procedures: R. C. B. SlackDocument8 paginiDiagnostic Procedures: R. C. B. Slacknour achkarÎncă nu există evaluări
- Cytometry Part B Clinical - 2007 - Wood - 2006 Bethesda International Consensus Recommendations On The ImmunophenotypicDocument10 paginiCytometry Part B Clinical - 2007 - Wood - 2006 Bethesda International Consensus Recommendations On The ImmunophenotypicAzaelBermudesTorresÎncă nu există evaluări
- Special Article: Guidance For Fluorescence in Situ Hybridization Testing in Hematologic DisordersDocument10 paginiSpecial Article: Guidance For Fluorescence in Situ Hybridization Testing in Hematologic DisordersMuneeb ArshadÎncă nu există evaluări
- Bacterial Meningitis Guidelines IDSADocument18 paginiBacterial Meningitis Guidelines IDSAAldito GlasgowÎncă nu există evaluări
- IDSA Meningitis GuidelinesDocument18 paginiIDSA Meningitis GuidelinesSahid López GarcíaÎncă nu există evaluări
- Stromberg Gross Path Text Handout AU DVP 2016Document29 paginiStromberg Gross Path Text Handout AU DVP 2016Rachel Autran100% (1)
- Necrotising Fasciitis: ReferencesDocument6 paginiNecrotising Fasciitis: ReferencesNatalia MoranÎncă nu există evaluări
- Theory and Application in Transfusion Medicine at A Tertiary-Care InstitutionDocument6 paginiTheory and Application in Transfusion Medicine at A Tertiary-Care InstitutionfegariasÎncă nu există evaluări
- Artificial Intelligence in Ovarian Cancer HistopatDocument14 paginiArtificial Intelligence in Ovarian Cancer Histopatbrolyssj088Încă nu există evaluări
- Analitical ErrorDocument15 paginiAnalitical Errorlabor baiturrahimÎncă nu există evaluări
- Molecular Methods Used in Clinical Laboratory: Prospects and PitfallsDocument8 paginiMolecular Methods Used in Clinical Laboratory: Prospects and PitfallsRon VitorÎncă nu există evaluări
- Jimaging 07 00111Document19 paginiJimaging 07 00111okuwobiÎncă nu există evaluări
- Benefits and Limitations of Maldi Tof Mass Spectrometry For The Identification of Microorganisms Journal of Infectiology 1 1142Document5 paginiBenefits and Limitations of Maldi Tof Mass Spectrometry For The Identification of Microorganisms Journal of Infectiology 1 1142ntnquynhproÎncă nu există evaluări
- 2 - Tunkel2004Document18 pagini2 - Tunkel2004Muhammad SyaifullahÎncă nu există evaluări
- Genetic Diagnostic Methods For Inherited Eye DiseaDocument6 paginiGenetic Diagnostic Methods For Inherited Eye Diseaputri dwi nofrianiÎncă nu există evaluări
- Dekker 2008Document6 paginiDekker 2008Charles CardosoÎncă nu există evaluări
- Necropsy ManualDocument46 paginiNecropsy ManualMUSIC VIDEOSÎncă nu există evaluări
- Enhancing Analytical Reasoning in Intensive Care UnitDocument17 paginiEnhancing Analytical Reasoning in Intensive Care UnitMahmoud AbouelsoudÎncă nu există evaluări
- Practice of Medical Technology ProfessionDocument3 paginiPractice of Medical Technology ProfessionMARY GLORY IGNACIOÎncă nu există evaluări
- AllisonDocument11 paginiAllisonNabila NatasyaÎncă nu există evaluări
- Role of Biomarkers in The Diagnosis of Anastomotic Leakage After Colorectal Surgery - JPMS-20231215Document4 paginiRole of Biomarkers in The Diagnosis of Anastomotic Leakage After Colorectal Surgery - JPMS-20231215Mohammed YunusÎncă nu există evaluări
- Nuclear Medicine AIDocument8 paginiNuclear Medicine AIdistruckÎncă nu există evaluări
- Nihms 541476Document19 paginiNihms 541476doni AfrianÎncă nu există evaluări
- Gui 210 TU0807Document5 paginiGui 210 TU0807Paja StojkovicÎncă nu există evaluări
- Raise Standards For Preclinical Cancer ResearchDocument3 paginiRaise Standards For Preclinical Cancer ResearchMiguel CastroÎncă nu există evaluări
- Lectura Patologia Prog Cirugia Oncologica Parte 1 PreanaliticaDocument17 paginiLectura Patologia Prog Cirugia Oncologica Parte 1 Preanaliticaandres restrepoÎncă nu există evaluări
- Challenges in Clinical Microbiology TestingDocument12 paginiChallenges in Clinical Microbiology TestingDi MonizÎncă nu există evaluări
- SAC Review: Omic' Technologies: Genomics, Transcriptomics, Proteomics and MetabolomicsDocument7 paginiSAC Review: Omic' Technologies: Genomics, Transcriptomics, Proteomics and MetabolomicsandreaÎncă nu există evaluări
- Texas Tech Microbiology and Immunology Residency GoalsDocument7 paginiTexas Tech Microbiology and Immunology Residency GoalsOsama BakheetÎncă nu există evaluări
- Application IHC NeoplasmDocument19 paginiApplication IHC NeoplasmiuventasÎncă nu există evaluări
- Metastatic CADocument58 paginiMetastatic CAbeosroÎncă nu există evaluări
- 1 Cancer HO Set1 (Intro) Zoom LecDocument2 pagini1 Cancer HO Set1 (Intro) Zoom Leckarl montanoÎncă nu există evaluări
- Onken2021. Critical Values in CytologyDocument8 paginiOnken2021. Critical Values in CytologyMD LarasatiÎncă nu există evaluări
- Hemepath 2895 ZhaoDocument5 paginiHemepath 2895 ZhaoleartaÎncă nu există evaluări
- How-To Guide On Biomarkers: Biomarker Definitions, Validation and Applications With Examples From Cardiovascular DiseaseDocument8 paginiHow-To Guide On Biomarkers: Biomarker Definitions, Validation and Applications With Examples From Cardiovascular DiseaseAnaÎncă nu există evaluări
- Cancer Biomarkers: Easier Said Than Done: Kenneth P.H. PritzkerDocument4 paginiCancer Biomarkers: Easier Said Than Done: Kenneth P.H. Pritzkerdumboo21Încă nu există evaluări
- Activity 1 - Histopathology (DOMINGO, JAME-ANN S.)Document14 paginiActivity 1 - Histopathology (DOMINGO, JAME-ANN S.)Kang DanielÎncă nu există evaluări
- Rapid On-site Evaluation (ROSE): A Practical GuideDe la EverandRapid On-site Evaluation (ROSE): A Practical GuideGuoping CaiÎncă nu există evaluări
- Baluchistan PDFDocument59 paginiBaluchistan PDFMuhammad JameelÎncă nu există evaluări
- Biomedicine & Pharmacotherapy: Renu Arora, Ritesh Kumar, Amit Agarwal, K.H. Reeta, Y.K. GuptaDocument9 paginiBiomedicine & Pharmacotherapy: Renu Arora, Ritesh Kumar, Amit Agarwal, K.H. Reeta, Y.K. GuptaMuhammad JameelÎncă nu există evaluări
- CHO20 19 New PDFDocument81 paginiCHO20 19 New PDFMuhammad JameelÎncă nu există evaluări
- University of Veterinary & Animal Sciences LahoreDocument18 paginiUniversity of Veterinary & Animal Sciences LahoreXher FaixalÎncă nu există evaluări
- Postpartum Uterine Infections: Department of Theriogenology University of Veterinary & Animal Sciences, LahoreDocument24 paginiPostpartum Uterine Infections: Department of Theriogenology University of Veterinary & Animal Sciences, LahoreMuhammad JameelÎncă nu există evaluări
- 13 Deworming PDFDocument14 pagini13 Deworming PDFMuhammad JameelÎncă nu există evaluări
- Suicidal Inhibition or Reaction Based Inhibition PDFDocument7 paginiSuicidal Inhibition or Reaction Based Inhibition PDFMuhammad JameelÎncă nu există evaluări
- 4385e3432 PDFDocument81 pagini4385e3432 PDFMuhammad JameelÎncă nu există evaluări
- Clostridial Diseases in Cattle PDFDocument4 paginiClostridial Diseases in Cattle PDFMuhammad JameelÎncă nu există evaluări
- Metritis and PyometraDocument7 paginiMetritis and PyometraGonzález Mendoza DamielÎncă nu există evaluări
- A Review On Dystocia in CowsDocument10 paginiA Review On Dystocia in CowsMuhammad JameelÎncă nu există evaluări
- MSD Wva Scolarship Prog 2018-Pr FinalDocument5 paginiMSD Wva Scolarship Prog 2018-Pr FinalMuhammad JameelÎncă nu există evaluări
- Fao'S Work On Agroecology: A Pathway To Achieving The SdgsDocument28 paginiFao'S Work On Agroecology: A Pathway To Achieving The SdgsMuhammad JameelÎncă nu există evaluări
- 1 s2.0 S0378432004002465 MainDocument20 pagini1 s2.0 S0378432004002465 MainMuhammad JameelÎncă nu există evaluări
- 1 s2.0 S0001706X15301479 MainDocument15 pagini1 s2.0 S0001706X15301479 MainMuhammad JameelÎncă nu există evaluări
- 1 s2.0 0378432086901053 MainDocument3 pagini1 s2.0 0378432086901053 MainMuhammad JameelÎncă nu există evaluări
- 1 s2.0 0378432086901053 MainDocument3 pagini1 s2.0 0378432086901053 MainMuhammad JameelÎncă nu există evaluări
- Acta Tropica: SciencedirectDocument7 paginiActa Tropica: SciencedirectMuhammad JameelÎncă nu există evaluări
- 1 s2.0 S0010440X1630339X MainDocument23 pagini1 s2.0 S0010440X1630339X MainMuhammad JameelÎncă nu există evaluări
- Choke in A Cow - A Case ReportDocument2 paginiChoke in A Cow - A Case ReportMuhammad JameelÎncă nu există evaluări
- DocumentDocument8 paginiDocumentMuhammad JameelÎncă nu există evaluări
- 131217-GRE Form Session 2017-2018Document1 pagină131217-GRE Form Session 2017-2018Muhammad JameelÎncă nu există evaluări
- 459 ANN509 Lecture Note ADocument10 pagini459 ANN509 Lecture Note AMuhammad JameelÎncă nu există evaluări
- Cobb Vaccination Procedure Guide EnglishDocument38 paginiCobb Vaccination Procedure Guide EnglishRed PhoenixÎncă nu există evaluări
- Ahbp - Oss - 2017 - Annex-IDocument6 paginiAhbp - Oss - 2017 - Annex-IMuhammad JameelÎncă nu există evaluări
- MSC (Hons) MPhilDocument1 paginăMSC (Hons) MPhilMuhammad JameelÎncă nu există evaluări
- 131217-GRE Form Session 2017-2018Document1 pagină131217-GRE Form Session 2017-2018Muhammad JameelÎncă nu există evaluări
- Concept Paper Outlining: A National Animal Health StrategyDocument31 paginiConcept Paper Outlining: A National Animal Health StrategyMuhammad JameelÎncă nu există evaluări
- Medical Officer AdvtNo. 09-2017Document1 paginăMedical Officer AdvtNo. 09-2017Muhammad JameelÎncă nu există evaluări
- December 2018: Russian Journal of Agricultural and Socio-Economic SciencesDocument339 paginiDecember 2018: Russian Journal of Agricultural and Socio-Economic Sciencesnahla saviraÎncă nu există evaluări
- Iqvia PDFDocument1 paginăIqvia PDFSaksham DabasÎncă nu există evaluări
- MSDS Metafuron 20 WPDocument10 paginiMSDS Metafuron 20 WPAndi DarmawanÎncă nu există evaluări
- Diagram of Thermal RunawayDocument9 paginiDiagram of Thermal RunawayVeera ManiÎncă nu există evaluări
- Coupled Mode TheoryDocument5 paginiCoupled Mode TheoryRahul RoyÎncă nu există evaluări
- 11 Dole Philippines vs. Maritime Co., G.R. No. L-61352 PDFDocument8 pagini11 Dole Philippines vs. Maritime Co., G.R. No. L-61352 PDFpa0l0sÎncă nu există evaluări
- Vydyne® R533H NAT: Ascend Performance Materials Operations LLCDocument4 paginiVydyne® R533H NAT: Ascend Performance Materials Operations LLCJames FaunceÎncă nu există evaluări
- Resona I9 Neuwa I9 FDADocument2 paginiResona I9 Neuwa I9 FDAMarcos CharmeloÎncă nu există evaluări
- Request For AffidavitDocument2 paginiRequest For AffidavitGhee MoralesÎncă nu există evaluări
- nrcs143 009445Document4 pagininrcs143 009445mdsaleemullaÎncă nu există evaluări
- "Corbel" - Concrete Corbel Analysis: Program DescriptionDocument4 pagini"Corbel" - Concrete Corbel Analysis: Program DescriptioniuliandurdureanuÎncă nu există evaluări
- Human Resource Management: Chapter One-An Overview of Advanced HRMDocument45 paginiHuman Resource Management: Chapter One-An Overview of Advanced HRMbaba lakeÎncă nu există evaluări
- ECED Lab ReportDocument18 paginiECED Lab ReportAvni GuptaÎncă nu există evaluări
- cp2021 Inf03p02Document242 paginicp2021 Inf03p02bahbaguruÎncă nu există evaluări
- Best Homeopathic Doctor in SydneyDocument8 paginiBest Homeopathic Doctor in SydneyRC homeopathyÎncă nu există evaluări
- 13 Daftar PustakaDocument2 pagini13 Daftar PustakaDjauhari NoorÎncă nu există evaluări
- Vitamin D3 5GDocument7 paginiVitamin D3 5GLuis SuescumÎncă nu există evaluări
- Verificare Bujii IncandescenteDocument1 paginăVerificare Bujii IncandescentemihaimartonÎncă nu există evaluări
- HandoverDocument2 paginiHandoverKumaresh Shanmuga Sundaram100% (1)
- Synopsis: A Study On Customer Satisfaction AT Nerolac Paints LTD., KadapaDocument5 paginiSynopsis: A Study On Customer Satisfaction AT Nerolac Paints LTD., KadapaAnu GraphicsÎncă nu există evaluări
- Characteristics: Wheels Alloy Aluminium Magnesium Heat ConductionDocument4 paginiCharacteristics: Wheels Alloy Aluminium Magnesium Heat ConductionJv CruzeÎncă nu există evaluări
- SEEPZ Special Economic ZoneDocument2 paginiSEEPZ Special Economic ZonetarachandmaraÎncă nu există evaluări
- EE3331C Feedback Control Systems L1: Overview: Arthur TAYDocument28 paginiEE3331C Feedback Control Systems L1: Overview: Arthur TAYpremsanjith subramani0% (1)
- NH School Employee Criminal Record Check FormDocument2 paginiNH School Employee Criminal Record Check FormEmily LescatreÎncă nu există evaluări
- Scenemaster3 ManualDocument79 paginiScenemaster3 ManualSeba Gomez LÎncă nu există evaluări
- CCTV8 PDFDocument2 paginiCCTV8 PDFFelix John NuevaÎncă nu există evaluări
- Schedule of Charges General Banking 2022Document18 paginiSchedule of Charges General Banking 2022Shohag MahmudÎncă nu există evaluări
- 【4DI+4DO】MA01+-AXCX4040 UserManual EN v1.1Document36 pagini【4DI+4DO】MA01+-AXCX4040 UserManual EN v1.1RioNorte LojaÎncă nu există evaluări
- Incident Report Form: RPSG-IMS-F-24 Accident and Investigation Form 5ADocument2 paginiIncident Report Form: RPSG-IMS-F-24 Accident and Investigation Form 5ARocky BisÎncă nu există evaluări