Documente Academic
Documente Profesional
Documente Cultură
Word Antes de Traducir Yo PDFFF
Încărcat de
Sonia Tacuri SolanoTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Word Antes de Traducir Yo PDFFF
Încărcat de
Sonia Tacuri SolanoDrepturi de autor:
Formate disponibile
Seminar
Acute pancreatitis
Jean-Louis Frossard, Michael L Steer, Catherine M Pastor
Acute pancreatitis is an inflammatory disease of the pancreas. Acute abdominal pain is the most common symptom, Lancet 2008; 371: 143–52
and increased concentrations of serum amylase and lipase confirm the diagnosis. Pancreatic injury is mild in 80% of Division de Gastroentérologie,
patients, who recover without complications. The remaining patients have a severe disease with local and systemic Hôpitaux Universitaires de
Genève, Geneva, Switzerland
complications. Gallstone migration into the common bile duct and alcohol abuse are the most frequent causes of
(J-L Frossard MD,
pancreatitis in adults. About 15–25% of pancreatitis episodes are of unknown origin. Treatment of mild disease is C M Pastor MD); and
supportive, but severe episodes need management by a multidisciplinary team including gastroenterologists, Department of Surgery,
interventional radiologists, intensivists, and surgeons. Improved understanding of pathophysiology and better Tufts-New England Medical
Center, Boston, MA, USA
assessments of disease severity should ameliorate the management and outcome of this complex disease.
(M L Steer MD)
Correspondence to:
Introduction arose from multiple organ dysfunction secondary to Dr Jean-Louis Frossard, Division
In 1856, Claude Bernard suggested that bile reflux into the infected pancreatic necrosis. Causation of acute de Gastroentérologie, Hôpitaux
common pancreatic duct was the trigger that caused acute pancreatitis defines its epidemiology. Biliary stone Universitaires de Genève,
Rue Micheli-du-Crest, 24,
pancreatitis. Several subsequent studies led to theories migration is more frequent and alcohol abuse is less
1205 Geneva, Switzerland
fuelling the debate until 1901, when Eugene Opie proposed frequent in women than in men. However, causes are jean-louis.frossard@hcuge.ch
that gallstone migration into the common bile duct was related to risk factors (such as alcohol abuse) that might
the main cause of acute pancreatitis. His conclusion was vary between countries and over time in every country. In
based on two autopsies of young patients in whom he children, the main triggers of acute pancreatitis are
found a gallstone occluding the orifice of the pancreatic trauma, systemic diseases, infections, and drugs, whereas
duct. Since then, many other causes of pancreatitis have genetic causes are rare.
been discovered, and here we aim to review the clinical
and therapeutic aspects of acute pancreatitis. Pathophysiology
Although controversial, most investigators believe that
Epidemiology acute pancreatitis is caused by the unregulated activation
The incidence of acute pancreatitis has increased in the of trypsin within pancreatic acinar cells (figure 1). Enzyme
past two decades. Between 1994 and 2001, the incidence activation within the pancreas leads to the autodigestion
of first-time attack in California increased from 33 to 44 of the gland and local inflammation. The main factors that
per 100 000 adults, and at present acute pancreatitis trigger acute disease are pancreatic hyperstimulation
accounts for more than 200 000 hospital admissions every (mainly seen in experimental models), gallstones, and
year in the USA. Such increase is also seen in European alcohol abuse. Acute pancreatitis arises when intracellular
countries. In 80% of patients, acute pancreatitis is mild protective mechanisms to prevent trypsinogen activation
and resolves without serious morbidity, but in up to 20%, or reduce trypsin activity are overwhelmed. These
acute pancreatitis is complicated by substantial morbidity protective mechanisms include the synthesis of trypsin as
and mortality. However, the frequency of severe inactive enzyme trypsinogen, autolysis of activated
pancreatitis remained stable over time in the USA and trypsin, enzyme compartmentalisation, synthesis of
European countries. In California, from 1994 to 2001, specific trypsin inhibitors such as serine protease
about 4% of patients died within 92 days after admission, inhibitor Kazal type 1 (SPINK1), and low intracellular
half of whom did so within 14 days. Most late deaths ionised Ca²+ concentrations.
After activation of trypsinogen into active trypsin within
acinar cells, several enzymes, such as elastase and
Search strategy and selection criteria phospholipase A2, and the complement and kinin
We used the PubMed database to search with the terms pathways are activated. Additionally, inflammation is
“acute pancreatitis” together with “complications”, “death”, initiated with local production of mediators such as
“treatment”, “sphincterotomy”, “antibiotic prophylaxis”, and interleukin 1, interleukin 6, and interleukin 8 from
“enteral nutrition”. We selected citations from articles in neutrophils, macrophages, and lymphocytes. Tumour
English, German, and French from the past 5 years, but did necrosis factor α is also released by local macrophages
not exclude commonly referenced and highly cited older within pancreatic tissue and its production correlates with
publications. We also searched relevant citation lists in severity of the experimental disease. Anti-inflammatory
selected papers. Several review articles or book chapters were
cytokines, such as interleukin 10, decrease the severity of
included because they provide comprehensive overviews that experimental pancreatitis.
are beyond the scope of this Seminar. For treatment and In addition to these events, activation of endothelial
antibiotic prophylaxis of the disease, we focused on cells enables the transendothelial migration of
randomised controlled trials whenever available. leucocytes, which release other harmful enzymes.
Decreased oxygen delivery to the organ and generation
www.thelancet.com Vol 371 January 12, 2008 143
Seminar
bile duct
CI– HC0 – CI– HC0 –
pressure
CFTR CFTR
channel channel
Oddi dysfunction
Low (Ca2+) Alcohol High (Ca2+)
receptor
Nucleus
Figure 1: Pathophysiology of acute pancreatitis
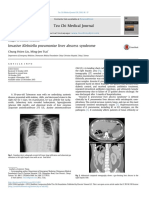
the periumbilical region (Cullen’s sign; figure 2) and the
flanks. Extension of inflammatory exudates from the
peripancreatic region to the diaphragm might lead to
shallow respiration.
Two enzymes (amylase and lipase) are released from
acinar cells during acute pancreatitis, and their
concentration in the serum is used to confirm diagnosis.
Serum amylase concentrations exceeding three times the
normal upper limit support the diagnosis of acute
pancreatitis. Amylase concentrations generally rise in the
serum within a few hours after the onset of symptoms and
return to normal values within 3–5 days. However,
amylase activity might remain within normal range on
admission in 19% of the patients. Also, serum amylase
Figure 2: Exudates (arrows) from pancreatic necrotic areas concentrations might be high in the absence of acute
pancreatitis in macroamylasaemia (a syndrome
of oxygen-derived free radicals also contribute to injury. characterised by the formation of large molecular
Thus, irrespective of the initial factor that triggers the complexes between amylase and abnormal
disease, severity of pancreatic damage is related to injury immunoglobulins), in patients with decreased glomerular
of acinar cells and to activation of inflammatory and filtration, in diseases of salivary glands, and in
endothelial cells. Then, local complications (acinar cell extrapancreatic abdominal diseases associated with
necrosis, pseudocyst formation, and abscess) might inflammation, including acute appendicitis, cholecystitis,
develop, and injury in remote organs (ie, lungs) might intestinal obstruction or ischaemia, peptic ulcer, and
follow the release of several mediators from the pancreas gynaecological diseases. Thus, when serum amylase
or from extrapancreatic organs such as the liver. concentration is high and clinical presentation is not
consistent with acute pancreatitis, the non-pancreatic
Diagnosis causes of hyperamylasaemia should be examined.
Acute pancreatitis is characterised by the presence of Follow-up, including CT scan examination and repeated
acute and constant pain in the epigastric area or the right amylase measurements, might help.
upper quadrant. Pain might last for several days, radiate Serum lipase concentrations remain high for a longer
to the back, and be associated with nausea and vomiting. period of time than do amylase concentrations, which is
Physical findings depend on severity of the disease. In an advantage over amylase measurement in patients with
mild disease, abdominal palpation reveals tenderness in a delayed presentation. Guidelines for the management
the upper abdomen. Exudates from pancreatic necrotic of acute pancreatitis emphasise this advantage. Assays of
areas tracking along the falciform ligament and into the many other pancreatic enzymes have been assessed
retroperitoneum can be seen in during the past 15 years, but none seems to offer better
diagnostic value than those of amylase and lipase.
144 www.thelancet.com Vol 371 January 12, 2008
Seminar
Diagnosis acute respiratory distress syndrome. Two peaks of
Abdominal radiography might show localised ileus in pulmonary complications have been seen during the early
severe pancreatitis. In a third of patients, chest phase of severe acute pancreatitis. The first peak arises
radiography shows abnormalities such as elevation of upon admission, and radiological abnormalities have been
one hemidiaphragm, and pleural effusions, pulmonary found in 15% of patients during that time. By day 5, new
infiltrates or both. When abdominal ultrasound is done, radiological abnormalities can be seen in an additional
bowel gases often mask focal hypoechoic areas within 71% of patients. Thereafter, pulmonary injury might result
the pancreas. from septic shock and complicate infection of the necrotic
Contrast-enhanced CT can be done after admission to pancreas. Other organs might also be affected during
confirm diagnosis of disease (87–90% sensitivity and 90– acute pancreatitis. By contrast with lung and renal injury,
92% specificity), or after 4 days to assess local hepatic injury is usually mild during acute pancreatitis but
complications such as fluid collections and necrosis, and contributes to the systemic inflammatory response.
to score the disease (see later section). MRI identifies Pancreatic necrosis is the most severe local complication
necrosis and fluid collections better than does CT scan. because it is frequently associated with pancreatic
infections. The diffuse or local area of non-viable
Course and severity parenchyma is initially sterile and can become infected
Most episodes of acute pancreatitis are mild and self- by bacteria of gut origin. Mortality in sterile and infected
limiting, needing only brief hospitalisation. However, necrosis is 10% and 25%, respectively. Pseudocyst is a
20% of patients develop a severe disease with local and collection of pancreatic juice enclosed by a wall of
extrapancreatic complications characterised by early granulation tissue that results from pancreatic duct
development and persistence of hypovolaemia, and leakage. Pancreatic abscess consists of a circumscribed
multiple organ dysfunction. Thus, close examination to collection of pus that arises around a restricted area of
assess early fluid losses, hypovolaemic shock, and pancreatic necrosis.
symptoms suggestive of organ dysfunction is crucial. The severity of acute pancreatitis is classified into five
Assessment methods such as the sequential organ failure grades (0–4) on unenhanced CT scan, whereas the degree
assessment (SOFA) score (table 1) help clinicians to of pancreatic necrosis is measured by contrast-enhanced
assess organ injury. Ascites, ileus, and, more importantly, CT scan. The sum of these two scores is used to calculate
increased capillary permeability, which conveys fluid the CT severity index for acute pancreatitis (table 2).
accumulation within the interstitium, contribute to the Patients with severe disease might recover but some die.
decreased intravascular volume. Renal dysfunction is also Half of the early deaths occur within 14 days, whereas
a severe complication that results from inadequate fluid late deaths happen within 3 months, with multiple organ
resuscitation, septic complications, or both. Incidence of dysfunction originating first from the systemic
pulmonary complications is high in severe pancreatitis, inflammatory response and then from infection within
ranging from 15% to 55%. Severity of pulmonary pancreatic necrosis.
complications can vary greatly from mild hypoxaemia Early diagnosis of severe disease is important because
without clinical or radiological abnormalities to severe it prompts an aggressive treatment, whereas mild
0 1 2 3 4
Respiration
PaO₂/FIO₂ (mm Hg) >400 ≤400 ≤300 ≤200 with respiratory ≤100 with respiratory
support support
Coagulation
Platelets (×10³ per µL) >150 ≤150 ≤100 ≤50 ≤20
Liver
Bilirubin (µmol/L) <20 20–32 33–101 102–204 >204
Cardiovascular
Hypotension No hypotension MAP <70 mm Hg Dopamine ≤5 or Dopamine >5 or epi ≤0·1* Dopamine >15 or epi
dobutamine (any dose)* or norepi ≤0·1* >0·1*or norepi >0·1*
Central nervous system
Glasgow coma score 15 13–14 10–12 6–9 <6
Kidney
Creatinine (µmol/L) <110 110–170 171–299 300–440 or <500 mL/day >440 or <200 mL/day
or urine output
MAP=mean arterial pressure. Epi=epinephrine. Norepi=norepinephrine. *Adrenergic agents administered for at least 1 h (doses given in µg/kg per min).
Table 1: Sequential organ failure assessment (SOFA) score in acute pancreatitis
www.thelancet.com Vol 371 January 12, 2008 145
Seminar
Points Panel: Causes of acute pancreatitis
Unenhanced CT Obstructive—biliary stone or sludge, pancreatic or ampullary
tumour, choledochal cyst and choledochocele, annular
Pancreatic enlargement pancreas, pancreas divisum (?), chronic pancreatitis, sphincter of
Oddi dysfunction, duodenal obstruction (duodenal
Single fluid collection diverticulum, Crohn’s disease).
Two or more fluid collections Toxic—alcohol, scorpion bite, organophosphate insecticide.
Contrast-enhanced CT
Class I drugs*—asparaginase, pentamidine, azathioprine,
Necrosis (proportion of cells) steroids,cytarabine, sulfamethoxazole-trimethoprim,
0% didanosine, furosemide, sulfasalazine, mesalazine, sulindac,
<30% mercaptopurine, tetracycline, opiates, valproic acid,
30–50% pentavalent antimonials, various oestrogens.
>50%
Class II drugs*—paracetamol, hydrochlorothiazide,
carbamazepine, interferon, cisplatin, lamivudine,
Table 2: CT severity index cyclopenthiazide, octreotide, enalapril, phenformin,
erythromycin, rifampicin.
Postsurgery—ERCP, abdominal or cardiac surgery.
attacks might be expected in the absence of severity.
Several scoring systems have been used to help to Genetic—PRSS1, SPINK1, CFTR.
identify patients at risk for adverse outcome, such as the Bacterial infection—Mycoplasma, legionella, leptospira, salmonella.
Ranson criteria, acute physiology and chronic health Viral infection—Mumps, coxsackie, hepatitis B,
evaluation (APACHE II), and SOFA scores (table 1). cytomegalovirus, varicella-zoster, herpes.
These scores assess injury in extrapancreatic organs; the
Parasitic infection—ascaris, cryptosporidium, toxoplasma.
greater the number of organs injured, the greater the
score. Large variation exists between these scores in the Metabolic—hypercalcaemia, hyperlipidaemia.
ability to predict severe diseases. Moreover, these scores Autoimmune—systemic lupus erythematosus, Sjögren’s syndrome.
should be repeated during hospitalisation, because their
modifications can predict the outcome. During the first Other—pregnancy, ischaemia, trauma.
week of admission, organ dysfunction usually resolves, Idiopathic
whereas worsening of organ dysfunction is associated
with high mortality rate. Absence of haemoconcentration *Drugs associated with pancreatitis in: 20 or more case
on admission excludes the occurrence of pancreatic reports and one positive re-exposure (class I); more than 10
necrosis in most patients. Another important factor that and less than 20 case reports with or without re-exposure
can contribute to severity is obesity. Early CT severity (class II); 10 or less case reports (class III).
score correlates well with the occurrence of
complications, sepsis, mortality rate, and need for
admission to intensive care units.
Besides markers included in severity scores, serum stones (38%) and alcohol abuse (36%) are the most
concentrations of additional mediators on admission, frequent causes of acute pancreatitis (figure 1 and panel).
such as C-reactiveprotein (CRP), cytokines, Gallstone-induced pancreatitis is caused by duct
phospholipase A2, antiproteases, and procalcitonin have obstruction of gallstone migration. Obstruction is
been correlated with disease development. Serum localised in the bile duct, the pancreatic duct, or both.
concentrations of the trypsinogen activation peptide Duct obstruction promotes pancreatitis by increasing
(TAP) and anionic trypsinogen 2 might also predict ductal pressure with subsequent unregulated activation of
severity. In healthy individuals, trypsinogen is cleaved by digestive enzymes. Gallstones that can migrate in the bile
a duodenal enterokinase into active trypsin and TAP, duct and trigger acute pancreatitis are those with a
whereas during acute pancreatitis inappropriate activation diameter up to 5 mm. Most gallstones that have a
of trypsinogen within acinar cells results in systemic diameter of 8 mm or more remain in the gallbladder.
release of TAP and trypsin. However, markers other than Gallstone migration as a cause of pancreatitis can be
CRP are not used in routine clinical practice. suspected when patients have a previous history of biliary
colic. Increase in serum hepatic enzyme concentrations
Causation (alanine aminotransferase concentration is three times or
Many causes for acute pancreatitis exist, and in 75–85% more the normal upper limit) on admission might help to
of patients the cause is easily identified. In developed predict biliary origin of pancreatitis (figure 3). However,
countries, obstruction of the common bile duct by almost 15–20% of patients with biliary acute
146 www.thelancet.com Vol 371 January 12, 2008
Seminar
pancreatitis have normal serum concentrations of hepatic include young age, female sex, number of cannulation
enzymes. Besides percutaneous ultrasound and CT, MRI attempts of papilla before success, and poor emptying of
is important for detection of gallstones. However, if pancreatic duct after opacification. Prevention of post-
suspicion of gallstone pancreatitis remains high despite a RCP pancreatitis in high-risk patients might be achieved
normal percutaneous ultrasonography or CT scan, by placing a temporary pancreatic stent. Serum
endoscopic ultrasonography should be done whenever triglyceride concentrations greater than 11 mmol/L
possible, because the bile duct is best imaged by this can worsen attacks of acute pancreatitis. However,
technique (figure 4). hypertriglyceridaemia is a rare (1–4%) cause of acute
Alcohol abuse is the second most frequent cause of pancreatitis, mostly seen in children with inherited
acute pancreatitis, but the correlation between alcohol disorders of lipoprotein metabolism (type I, II, and V
and pancreatitis is not completely understood. In hyperlipidaemia). Most adults with
experimental models, Gorelick showed that ethanol hypertriglyceridaemia-related pancreatitis have a mild
directly sensitises acinar cells to cholecystokinin form of genetically inherited type I or type V disease, in
stimulation (figure 1). Acute pancreatitis develops in 10% addition to conditions that raise triglyceride
of chronic alcohol abusers (>80 g daily intake). The
development of pancreatitis is affected by both genetic Acute pancreatitis of biliary origin?
and environmental factors. Thus, failure to inhibit trypsin
activity (gene mutation and absence of function of
jaundice
SPINK1) or failure to wash active trypsin into pancreatic
ducts (gene mutation with dysfunction of the cystic
fibrosis transmembrane conductance regulator gene,
Yes No
CFTR) might promote alcoholic pancreatitis.
Pancreas divisum is a common congenital anatomical
variant of the pancreatic duct in about 7% of autopsy series. ERCP
It results from the absence of fusion between the dorsal and Yes No
ventral ductal systems. The possible consequence of
pancreas divisum is a stenosed or inadequately patent minor EUS and MRCP No or low
papilla, preventing normal drainage of pancreatic secretions
and leading to increased intraductal pressure. However,
whether pancreas divisum is related to pancreatitis is highly
controversial. Whether dysfunction of sphincter of Oddi can
trigger acute pancreatitis by increasing intrapancreatic ductal
pressure is another controversial issue. Biliary sludge (figure ERCP
Sphincterectomy test within 12 h
4) refers to a viscous bile suspension that contains
cholesterol crystals and calcium bilirubinate granules Figure 3: Management of pancreatitis of biliary origin
embedded in strands of gallbladder mucus. Sludge is When patients have either jaundice or cholangitis, the biliary origin of disease is
associated with bile stasis, long-lasting fast, distal bile duct almost certain. Stones are preferentially removed by endoscopic retrograde
cholangiopancreatography (ERCP) or during sphincterotomy. When diagnosis is
obstruction, and total parenteral feeding. Most patients with unclear, endoscopic ultrasonography(EUS) and magnetic resonance
biliary sludge are asymptomatic. Biliary sludge is cholangiopancreatography (MRCP) might help identify stones. ALAT=alanine
commonly seen in patients with recurrent acute pancreatitis aminotransferase.
of unknown origin, and cholecystectomy might prevent the
recurrence of pancreatic disease. A
Intraductal papillary mucinous tumours might be
another cause of acute pancreatitis. The tumour or mucus
produced by the tumour obstruct the main pancreatic
duct, a side branch of the main duct, or both types of duct.
Freeman and colleagues showed that 5,4% of 2347
patients were at risk of developing acute pancreatitis
within 30 days after endoscopic retrograde
cholangiopancreatography (ERCP). Moreover,
Common bile duct
asymptomatic hyperamylasaemia arises in 35–70% of
patients after the procedure. The risk of acute pancreatitis
is higher when the procedure is done to treat Oddi
sphincter dysfunction than to remove gallstones in the
Figure 4: Stones detection by endoscopic ultrasonography
bile duct. Other risk factors for post-ERCP pancreatitis (A) A small stone undetectable by percutaneous ultrasonography is clearly seen by endoscopic ultrasonography
(note the postacoustic shadow of the stone). (B) Well delineated sludge that sticks to the gallbladder wall (no
postacoustic shadow).
www.thelancet.com Vol 371 January 12, 2008 147
Seminar
concentrations such as obesity, diabetes mellitus, PRSS1 gene are seen in most patients with hereditary
hypothyroidism, or pregnancy. Alcohol abuse and pancreatitis. In the most frequent mutations, the function
treatment by β blockers might also transiently increase of trypsinogen is increased, causing premature enzyme
serum triglyceride concentrations. The attacks of activation and autolysis of acinar cells.
pancreatitis are usually mild, and more severe attacks can The pancreas synthesises SPINK1, a specific trypsin
be successfully treated by plasmapheresis, especially in inhibitor, the function of which can be lost by mutation.
pregnant women. Mutations are rarely associated with pancreatitis, but in
Hypercalcaemia is another rare and inconsistent cause of association with other genetic traits, SPINK1 mutations
acute pancreatitis. Because the incidence of pancreatitis is might favour pancreatic attacks in the presence of
low in patients with chronic hypercalcaemia, additional environmental triggers. In pancreatic ductal cells, CFTR
factors are probably needed to induce pancreatitis attacks. controls chloride and bicarbonate fluxes (figure 1).
Drugs rarely induce acute pancreatitis (1,4–2%). Most Similar to SPINK1 mutation, CFTR mutations alone are
studies of drug-induced pancreatitis are case reports of rarely associated with pancreatitis. However, genetic
few patients. A review classified 80 or more drugs that can testing of SPINK1 and CFTR mutations for pancreatitis
induce pancreatitis into three categories, according to the might contribute to a better understanding of the
number of reports and the existence of studies with drug mechanisms linking these mutations to the disease, in
re-exposure (panel). Class I drugs are those associated association with the environmental context and triggers.
with 20 or more case reports with at least one drug re- Sarles and colleagues described a patient with acute
exposure. Class II drugs are those described in more than pancreatitis and hypergammmaglobulinaemia in 1965.
10 and less than 20 case reports with or without re- Since then, autoimmune pancreatitis has been associated
exposure. All other drugs associated with the disease with Sjögren’s syndrome, primary sclerosing cholangitis,
belong to class III. Diuretics, anti-inflammatory agents, and primary biliary cirrhosis. Autoimmune pancreatitis
antibiotics, AIDS therapeutics, immuno-suppressive might disappear with steroid therapy.
agents, and cardiovascular drugs such as statins (class III) In summary, the main causes of acute pancreatitis are
have all been implicated. Drug-induced acute pancreatitis gallstone migration and alcohol abuse. Other causes are
is either dose-dependent or dose-independent uncommon, situational, or subject to continuous
(hypersensitivity reaction), but most drug reactions are controversy, such as pancreas divisum or sphincter of
idiosyncratic. Oddi dysfunction. Personal and familial history, clinical
Many infectious agents are associated with acute symptoms, laboratory tests, and percutaneous and
pancreatitis, but no microorganism has ever been endoscopic ultrasonography identify most of the causes,
identified within the pancreas. However, acute but 15–25% of episodes remain of unknown origin. How
pancreatitis has been associated with viral or bacterial detailed the search for rare causes should be after the first
infections, and infestation with parasites (panel). The episode of acute pancreatitis is debated. With new
pancreatic tropism of HIV is also well documented, with imaging techniques and genetic testing, the number of
4,7% in 939 HIV-positive patients being affected in one patients diagnosed with idiopathic pancreatitis should
study. Genetic mutations such as those in CFTR and decrease. However, the complexity of the
SPINK1 genes are frequent in HIV-positive patients with pathophysiology of the disease, associated with genetic
acute pancreatitis. Pregnancy had long been regarded as and environmental risks and acute triggers, preclude the
a possible cause of acute pancreatitis, but recent studies identification of a unique cause for every episode of acute
emphasised the coexistence of additional factors such as pancreatitis. Finally, besides specific treatment (mostly
gallstones or hyperlipidaemia to explain the higher for gallstone-induced pancreatitis), the early therapeutic
frequency of the disease among pregnant women. Acute strategies are identical in all patients with acute
pancreatitis is frequent after pancreatic or biliary surgery. pancreatitis.
Extradigestive procedures such as cardiopulmonary
bypass for cardiac transplantation are also a risk factor; Treatment
the longer the cardiopulmonary bypass and crossclamp In mild forms of disease, besides the aetiological
times, the higher the risk. Pancreatic ischaemia probably treatment (mostly for gallstone-induced pancreatitis),
favours acute pancreatitis after surgery, shock, therapy is supportive and includes fluid resuscitation,
embolism, and systemic vasculitis. pain relievers, oxygen administration, and antiemetics,
In most patients, acute pancreatitis is caused by whereas oral feeding is stopped (figure 5). By contrast,
gallstone obstruction or alcohol, and no genetic testing is severe episodes (20% of patients) need management by a
needed. However, unexplained recurrent acute multidisciplinary team, including gastroenterologists,
pancreatitis might be associated with known genetic interventional radiologists, intensivists, and surgeons.
mutations in the cationic trypsinogen gene protease However, despite efforts to start an appropriate treatment,
serine 1 (PRSS1), SPINK1, or CFTR. Mutations in the mortality rate of severe attacks has not substantially
changed during the past two decades. For these patients,
resuscitation and close monitoring, nutritional support,
148 www.thelancet.com Vol 371 January 12, 2008
Seminar
and management of pancreatic necrosis are important.
However, treatment of severe pancreatitis seems to differ
considerably from centre to centre, according to local
experience and guidelines. Biological markers
An early medical treatment of acute pancreatitis is fluid Radiological signs
resuscitation to correct fluid losses in the third space and
maintain an adequate intravascular volume. Moreover,
close monitoring of respiratory, cardiovascular, and renal
Mild
function is needed to assess and treat complications
associated with hypovolaemia. Oral feeding is stopped,
whereas pain relievers, antiemetics, and oxygen
Fluid resuscitation
administration can be helpful. Most episodes of acute Oxygen Oxygen
pancreatitis are mild and self-limiting, needing only brief Pain relievers
Antiemetics Antiemetics
admission. Any patient with severe disease should be
admitted to the intensive care unit, the criteria for
admission being identical to those of other diseases.
Additionally, a stepdown unit must be considered in
patients at high risk of deterioration, such as elderly Yes No
patients, those who are obese, those needing a great
volume of resuscitation, and those with pancreatic ERCP Enteral
necrosis. nutrition to be discussed
To suppress the function of the exocrine pancreas, assessments
bowel rest by parenteral nutrition has been frequently
advocated. However, clinical and experimental studies Clinical improvement
showed that bowel rest is associated with intestinal
mucosal atrophy and increased infectious complications
due to bacterial translocation from the gut. Moreover, No Yes
total parenteral nutrition is also associated with enhanced
Repeated clinical
proinflammatory response. Thus, although mortality rate assessments
is not substantially different in patients treated with total
to be discussed
parenteral nutrition or enteral nutrition, infections,
surgical interventions, and non-infectious complications CT guided Clinical
are reduced by enteral nutrition. The type of enteral
nutrition (gastric or jejunal) is debated. Although two
studies showed that enteral nutrition can decrease the Sterile
number of infections when the feeding tube is positioned
in the jejunum, Eatock and colleagues showed no
significant clinical difference between early nasogastric Debridement or
and nasojejunal feeding. Early enteral feeding should be
provided, but the amount of calories and type of nutrient Figure 5: Severity assessment and proposed therapeutic management for
mixtures that should be given has yet to be established. acute pancreatitis
Infection of pancreatic necrosis is a very important
issue. This complication develops during the second or develop pancreatic necrosis might need debridement and
third week in 40–70% of patients. Because pancreatic percutaneous or endoscopic drainage of fluid collections,
infection is the leading cause of morbidity and mortality, pseudocysts, and abscesses. However, such interventions
early prevention of infected necrosis has been advocated. are needed only when the pancreatic or peripancreatic
However, the benefit of antibiotic prophylaxis is highly tissues are infected, because debridement or drainage
debated; some studies and a meta-analysis showed that increase the risk to infect sterile tissues. When necrosis
antibiotic prophylaxis reduced mortality and morbidity is sterile, mortality is low and necrosis is treated by a
of pancreatic necrosis, whereas another investigation conservative approach, although surgery might be needed
did not show any advantage. When infection is suspected for late complications or persistent severe pancreatitis.
and fine-needle aspiration of the pancreas for To discriminate between sterile and infected pancreatic
bacteriology done, the accepted treatment is to start necrosis when patients deteriorate, ultrasound- or CT-
antibiotics, intravenous imipenem or meropenem, for 14 guided fine-needle aspirations of pancreatic tissues are
days. Such treatment is rapidly stopped if infection is not repeatedly done. When infection is proven or in the
confirmed. Patients who presence of abscesses, besides antibiotherapy,
www.thelancet.com Vol 371 January 12, 2008 149
Seminar
removal of infected tissues is done either by serial Acknowledgments
laparotomies before final abdomen closure or by a single This Seminar has been supported in part by grant 320000-113225 from the
Swiss National Science Foundation to J-LF, 320000-109977 from the Swiss
laparotomy followed by subsequent closed drainages to
National Science Foundation to CMP, and grant RO1 DK31396 from the
remove residual necrosis. To keep the consequences of NHI to MLS.
serial laparotomies to a minimum in critically ill patients References
and to decrease the ensuing increased mortality, several 1 Bernard C. Leçons de physiologie expérimentale. Paris. Bailliere 1856;
minimally invasive techniques are done. These 2: 278.
procedures for debridement of infected necrosis include 2 Opie EL. The relation of cholelithiasis to disease of the pancreas and
to fat necrosis. Johns Hopkins Hosp Bull 1901; 12: 19–21.
CT-guided and ultrasonography-guided percutaneous 3 Imrie CW. Acute pancreatitis: overview. Eur J Gastroenterol Hepatol
drainages, transgastric or transdudodenal endoscopic 1997; 9: 103–05.
drainages, or minimally invasive laparoscopy with 4 Trapnell JE, Duncan EHL. Patterns of incidence in acute pancreatitis.
BMJ 1975; 2: 179–83.
retroperitoneal access. However, these techniques are still
5 Giggs JA, Bourke JB, Katschinski B. The epidemiology of primary
being developed and are indicated only in some patients. acute pancreatitis in Greater Nottingham: 1969–1983. Soc Sci Med
Finally, abdominal decompression through midline 1988; 26: 79–89.
laparotomy for abdominal compartment syndrome is 6 Jaakkola M, Nordback I. Pancreatitis in Finland between 1970 and
1989. Gut 1993; 34: 1255–60.
another surgical procedure for severe acute pancreatitis. 7 Frey CF, Zhou H, Harvey DJ, White RH. The incidence and
Pancreatic and retroperitoneal inflammation associated case-fatality rates of acute biliary, alcoholic, and idiopathic
with aggressive fluid administration increase the intra- pancreatitis in California, 1994–2001. Pancreas 2006; 33: 336–44.
abdominal pressure, decreasing abdominal organ perfusion 8 DeFrances CJ, Hall MJ, Podgornik MN. 2003 National Hospital
Discharge Survey. Advance data from vital and health statistics
with subsequent persistent organ dysfunction. The N° 359 Hyattsville, MD. National center for health statistics 2005.
consequences of surgical decompression on the outcome 9 Yadav D, Lowenfels AB. Trends in the epidemiology of the first attack
remain unclear. of acute pancreatitis: a systematic review. Pancreas 2006; 33: 323–30.
10 Lund H, Tonnesen H, Tonnesen MH, Olsen O. Long-term
To keep pancreatic injury to a minimum, broad- recurrence and death rates after acute pancreatitis.
spectrum antiprotease drugs such as aprotinin and Scand J Gastroenterol 2006; 41: 234–38.
gabexate mesilate have been advocated. Studies to test 11 Williams M, Simms HH. Prognostic usefulness of scoring systems
in critically ill patients with severe acute pancreatitis. Crit Care Med
the efficacy of blockers of specific biochemical pathways 1999; 27: 901–07.
that are activated during severe disease, including 12 Renner IG, Savage WT, Pantoja JL, Renner VJ. Death due to acute
antagonists of platelet activating factor or inhibitors of pancreatitis. A retrospective analysis of 405 autopsy cases. Dig Dis Sci
1985; 30: 1005–18.
basal and stimulated exocrine pancreatic secretion, have
13 Lankisch PG, Burchard-Reckert S, Petersen M, et al. Morbidity and
been disappointing and these treatments are not mortality in 602 patients with acute pancreatitis seen between the
recommended. years 1980–1994. Z Gastroenterol 1996; 34: 371–77.
Most patients with gallstone-induced pancreatitis 14 Benifla M, Weizman Z. Acute pancreatitis in childhood: analysis of
literature data. J Clin Gastroenterol 2003; 37: 100–02.
present with mild disease and quickly recover after early
15 Werlin SL, Kugathasan S, Frautschy BC. Pancreatitis in children.
resuscitation. In patients with severe biliary pancreatitis, J Pediatr Gastroenterol Nutr 2003; 37: 591–95.
early (within 72 h) endoscopic retrograde 16 Frossard JL, Hadengue A. Acute pancreatitis: new
cholangiopancreatography and endoscopic physiopatholological concepts. Gastro Clin Biol 2001; 25: 164–76.
17 Norman JG, Fink GW, Messina J, Carter G, Franz MG. Timing of
sphincterotomy have been recommended. Such early tumor necrosis factor antagonism is critical in determining outcome
procedures decrease the number of complications, such in murine lethal acute pancreatitis. Surgery 1996; 120: 515–21.
as biliary sepsis. However, Folsch and colleagues showed 18 Gloor B, Todd KE, Lane JS, Rigberg DA, Reber HA. Mechanism of
increased lung injury after acute pancreatitis in IL-10 knockout mice.
that early endoscopic retrograde J Surg Res 1998; 80: 110–14.
cholangiopancreatography and endoscopic 19 Frossard JL, Saluja A, Bhagat L, et al. The role of intracellular
sphincterotomy are not beneficial in patients with biliary adhesion molecule 1 and neutrophils in acute pancreatitis and
pancreatitis in the absence of biliary sepsis or pancreatitis-associated lung injury. Gastroenterology 1999;
116: 694–701.
obstruction. At present, the most accepted practice is to 20 Poch B, Gansauge F, Rau B, et al. The role of polymorphonuclear
do endoscopic sphincterotomy if biliary obstruction, leukocytes and oxygen-derived free radicals in experimental acute
biliary sepsis, and persistent organ dysfunction are pancreatitis: mediators of local destruction and activators of
inflammation. FEBS Lett 1999; 461: 268–72.
present. 21 Pastor CM, Matthay M, Frossard JL. Pancreatitis-associated lung
The need for follow-up cholecystectomy to prevent injury: new insights. Chest 2003; 124: 2341–51.
recurrent episodes is also an important question. When 22 Bradley EL. A clinically based classification system for acute
pancreatitis. Arch Surg 1993; 128: 586–90.
stones are present in the gallbladder, laparoscopic
23 Kemppainen E, Puolakkainen P, Leppaniemi A, et al. Diagnosis of
cholecystectomy is done either during the same acute pancreatitis. Ann Chir Gynaecol 1998; 87: 191–94.
admission, when acute pancreatitis is mild, or delayed 24 Fazar MH, Goldberg E. Acute abdominal pain. Med Clin North Am
until resolution of the inflammatory response and clinical 2006; 90: 481–503.
25 Matull WR, Pereira SP, O’Donohue JW. Biochemical markers of
improvement (within 6 weeks). Delayed cholecystectomy acute pancreatitis. J Clin Pathol 2006; 59: 340–44.
is also indicated after endoscopic sphincterotomy, except 26 Cotton PB, Lehman G, Vennes J, et al. Endoscopic sphincterotomy
when patients are too sick to undergo surgery. complications and their management: an attempt at consensus.
Gastrointest Endosc 1991; 37: 383–93
Conflict of interest statement
We declare that we have no conflict of interest.
150 www.thelancet.com Vol 371 January 12, 2008
Seminar
www.thelancet.com Vol 371 January 12, 2008 151
S-ar putea să vă placă și
- HypopituitarismDocument2 paginiHypopituitarismGerardLum100% (2)
- Body MeridianDocument65 paginiBody Meridiandcf67my100% (1)
- Psychiatric History and Mental Status Examination GuideDocument7 paginiPsychiatric History and Mental Status Examination GuideGabriel Gerardo N. Cortez100% (1)
- The Ayurveda Guide - Pitta Dosha - Healthy Ayurveda PDFDocument4 paginiThe Ayurveda Guide - Pitta Dosha - Healthy Ayurveda PDFChandra Sekhar Gajula100% (3)
- 3 ❤ Smart Sheet for History Taking in Pediatrics خلفية صفراءDocument14 pagini3 ❤ Smart Sheet for History Taking in Pediatrics خلفية صفراءsalah almozahemÎncă nu există evaluări
- Urinary Tract Infection in Childhood and Its Relevance to Disease in Adult LifeDe la EverandUrinary Tract Infection in Childhood and Its Relevance to Disease in Adult LifeEvaluare: 2 din 5 stele2/5 (2)
- Basic Gastroenterology: Including Diseases of the LiverDe la EverandBasic Gastroenterology: Including Diseases of the LiverÎncă nu există evaluări
- Psych Case StudyDocument14 paginiPsych Case Studyapi-604581864Încă nu există evaluări
- Bisoprolol PDFDocument69 paginiBisoprolol PDFDuwi Efasari100% (3)
- Neurological Exam Question on Sudden Behavior ChangeDocument107 paginiNeurological Exam Question on Sudden Behavior ChangekimÎncă nu există evaluări
- Medical-Surgical Nursing: (Prepared By: Prof. Rex B. Yangco)Document12 paginiMedical-Surgical Nursing: (Prepared By: Prof. Rex B. Yangco)Leilah Khan100% (1)
- Acute PancreatitisDocument10 paginiAcute PancreatitisAndrés Menéndez RojasÎncă nu există evaluări
- NCDD 04272009 ResearchPlan DiseasesofPancreasDocument10 paginiNCDD 04272009 ResearchPlan DiseasesofPancreasGmail JOÎncă nu există evaluări
- Braganza2011 PDFDocument14 paginiBraganza2011 PDFAmirullah AbdiÎncă nu există evaluări
- Pancreatitis Acute - StatPearls - NCBI BookshelfDocument6 paginiPancreatitis Acute - StatPearls - NCBI BookshelfJosé Jefferson Da SilvaÎncă nu există evaluări
- Acute Pancreatitis Review and Clinical UpdateDocument10 paginiAcute Pancreatitis Review and Clinical Updateemanuel santiago camargo parraÎncă nu există evaluări
- Acute Pancreatitis Causes and PathophysiologyDocument21 paginiAcute Pancreatitis Causes and PathophysiologyTapas Kumar SahooÎncă nu există evaluări
- Intestinal Tuberculosis: A Diagnostic Challenge: Open Access Case DOI: 10.7759/cureus.13058Document4 paginiIntestinal Tuberculosis: A Diagnostic Challenge: Open Access Case DOI: 10.7759/cureus.13058ATIKA INDAH SARIÎncă nu există evaluări
- Pancreatitis Aguda para Emergencia PDFDocument11 paginiPancreatitis Aguda para Emergencia PDFJudithzaloÎncă nu există evaluări
- Acute Pancreatitis: Current Perspectives On Diagnosis and ManagementDocument9 paginiAcute Pancreatitis: Current Perspectives On Diagnosis and ManagementGita Septiyani KusumaÎncă nu există evaluări
- Acute Pancreatitis: Review ArticleDocument4 paginiAcute Pancreatitis: Review ArticleFifin m saidÎncă nu există evaluări
- Acute PancreatitisDocument9 paginiAcute PancreatitispreetshardocÎncă nu există evaluări
- Acute Pancreatitis: SeminarDocument12 paginiAcute Pancreatitis: SeminarKaren JboÎncă nu există evaluări
- Pancretitis AgudaDocument12 paginiPancretitis Agudapruebaprueba321765Încă nu există evaluări
- Fluid Resuscitation in Acute PancreatitisDocument7 paginiFluid Resuscitation in Acute PancreatitisRicardo Isique SantillanÎncă nu există evaluări
- Acute CholangitisDocument11 paginiAcute CholangitisFrancisco EsparzaÎncă nu există evaluări
- Residents' Clinic: 22-Year-Old Man With Abdominal Pain and RashDocument4 paginiResidents' Clinic: 22-Year-Old Man With Abdominal Pain and RashAkhtar AliÎncă nu există evaluări
- Autoimmune PancreatitisDocument7 paginiAutoimmune PancreatitisWinstonÎncă nu există evaluări
- Wang 2009Document4 paginiWang 2009DANY ALEXIS SOBARZO SOTOÎncă nu există evaluări
- Emphysematous CystitiS IllustrativE Case ReportDocument7 paginiEmphysematous CystitiS IllustrativE Case ReportDetry Kala'lembangÎncă nu există evaluări
- Flgastro 2018 101102Document8 paginiFlgastro 2018 101102carolina pulidoÎncă nu există evaluări
- Pancreatite AgudaDocument8 paginiPancreatite AgudaGabriel MouraÎncă nu există evaluări
- Peritoneal Tuberculosis Mimicking Carcinomatous Ascites in A Child Living in A Low Prevalence Country: A Case ReportDocument7 paginiPeritoneal Tuberculosis Mimicking Carcinomatous Ascites in A Child Living in A Low Prevalence Country: A Case ReportyoshiangelÎncă nu există evaluări
- New Insights of Acute PancreatitisDocument18 paginiNew Insights of Acute Pancreatitispruebaprueba321765Încă nu există evaluări
- Acute PancreatitisDocument10 paginiAcute PancreatitisHarbin NicholsonÎncă nu există evaluări
- PatofisiologyDocument13 paginiPatofisiologyarinÎncă nu există evaluări
- pancreatitis-frontline-gastro-reviewDocument8 paginipancreatitis-frontline-gastro-reviewlaurentiu.ducuta12Încă nu există evaluări
- MRSAcolitisGastroenterol Report2015Document4 paginiMRSAcolitisGastroenterol Report2015selandia nisrinaÎncă nu există evaluări
- Dafpus LiverDocument2 paginiDafpus LiverMenda JangWooyoung SooyoungsterÎncă nu există evaluări
- International Journal of Infectious Diseases: Anshuman Pandey, Shakeel Masood, Namrata P. AwasthiDocument3 paginiInternational Journal of Infectious Diseases: Anshuman Pandey, Shakeel Masood, Namrata P. Awasthijohanna monsalveÎncă nu există evaluări
- New Insights Into Acute Pancreatitis: Peter J. Lee and Georgios I. PapachristouDocument18 paginiNew Insights Into Acute Pancreatitis: Peter J. Lee and Georgios I. PapachristouandreaÎncă nu există evaluări
- The Pathology of Acute AppendicitisDocument14 paginiThe Pathology of Acute Appendicitishokifoh169Încă nu există evaluări
- Pathophysiology of Pulmonary Complications of Acute PancreatitisDocument10 paginiPathophysiology of Pulmonary Complications of Acute PancreatitisAmri AdhyatmaÎncă nu există evaluări
- 28-Year-Old Man With Crohn Disease and Hematuria: Residents ' ClinicDocument5 pagini28-Year-Old Man With Crohn Disease and Hematuria: Residents ' ClinicDesi HutapeaÎncă nu există evaluări
- Septic Complications of Acute Pancreatitis: Bratislavske Lekarske Listy February 2006Document19 paginiSeptic Complications of Acute Pancreatitis: Bratislavske Lekarske Listy February 2006Stela HuzumÎncă nu există evaluări
- Pyelonephritis in Dogs Retrospective Study of 47 HDocument11 paginiPyelonephritis in Dogs Retrospective Study of 47 HI Nyoman Bagus Tri AribawaÎncă nu există evaluări
- 10.2215@Cjn.13191118 Aki y PancreatitisDocument10 pagini10.2215@Cjn.13191118 Aki y Pancreatitishemer hadyn calderon alvitesÎncă nu există evaluări
- Primary Peritonitis Due To Streptococcus Pyogenes: Eview RticleDocument5 paginiPrimary Peritonitis Due To Streptococcus Pyogenes: Eview RticleGabriÎncă nu există evaluări
- Pancreatitis RevDocument14 paginiPancreatitis Revbmoreno78Încă nu există evaluări
- The Diseases of The PancreasDocument40 paginiThe Diseases of The PancreasAroosha IbrahimÎncă nu există evaluări
- 2016 Article 1292 PDFDocument10 pagini2016 Article 1292 PDFPutriRahayuMoidadyÎncă nu există evaluări
- Acute Pancreatitis: Clinical PR ActiceDocument9 paginiAcute Pancreatitis: Clinical PR ActicesanthiagoschneiderÎncă nu există evaluări
- Acute Cholangitis - An Overview of Management and TreatmentDocument9 paginiAcute Cholangitis - An Overview of Management and TreatmentJohn DoeÎncă nu există evaluări
- Diagnosis and Management of Chronic PancreatitisDocument8 paginiDiagnosis and Management of Chronic PancreatitiscarmenÎncă nu există evaluări
- Seminar On Acute PancreatitisDocument20 paginiSeminar On Acute PancreatitisJoice DasÎncă nu există evaluări
- Global Epidemiology and Holistic Prevention of PancreatitisDocument24 paginiGlobal Epidemiology and Holistic Prevention of PancreatitisRoberto MaresÎncă nu există evaluări
- 8a Acute PancreatitisDocument12 pagini8a Acute PancreatitisTony SswwÎncă nu există evaluări
- Alcohol-Related Pancreatic Damage: Mechanisms and TreatmentDocument8 paginiAlcohol-Related Pancreatic Damage: Mechanisms and TreatmentRica Faye PorrasÎncă nu există evaluări
- Acute Suppurative Cholangitis: Edward Chock, M.D., Bruce Wolfe, M.D., and Nathaniel Matolo, M.DDocument8 paginiAcute Suppurative Cholangitis: Edward Chock, M.D., Bruce Wolfe, M.D., and Nathaniel Matolo, M.DAhmad Harissul IbadÎncă nu există evaluări
- Wa0093.Document27 paginiWa0093.EvaÎncă nu există evaluări
- Severe Peritonitis Case Report Highlights Diagnosis and Treatment of Acute PancreatitisDocument2 paginiSevere Peritonitis Case Report Highlights Diagnosis and Treatment of Acute PancreatitisJune Faith HacheroÎncă nu există evaluări
- Liver Fibrosis PDFDocument10 paginiLiver Fibrosis PDFPurwaning Nugroho WidiyatiÎncă nu există evaluări
- Pancreatitis AgudaDocument12 paginiPancreatitis AgudaWILLIAM RICARDO CASTAÑEDA VARGASÎncă nu există evaluări
- Lipase Vs AmylaseDocument6 paginiLipase Vs AmylaseLuis AcevedoÎncă nu există evaluări
- Role of Alcohol Metabolism in Chronic PancreatitisDocument7 paginiRole of Alcohol Metabolism in Chronic Pancreatitisnoam tiroshÎncă nu există evaluări
- Francisco G. La Rosa, M.D.: Pancreas Pathology and Diabetes Mellitus (Course Dsbs 5516)Document10 paginiFrancisco G. La Rosa, M.D.: Pancreas Pathology and Diabetes Mellitus (Course Dsbs 5516)madaniÎncă nu există evaluări
- Acute Pancreatitis-A Clinical Update: Review ArticleDocument6 paginiAcute Pancreatitis-A Clinical Update: Review ArticleDương Ngọc DiệpÎncă nu există evaluări
- Diseases of the Liver and Biliary TreeDe la EverandDiseases of the Liver and Biliary TreeAnnarosa FloreaniÎncă nu există evaluări
- Liver Disease: A Clinical CasebookDe la EverandLiver Disease: A Clinical CasebookStanley Martin CohenÎncă nu există evaluări
- Atypical Wounds: Causes, Examples & ManagementDocument13 paginiAtypical Wounds: Causes, Examples & Managementmian gÎncă nu există evaluări
- CHN Lec FinalsDocument14 paginiCHN Lec FinalsMay Chelle ErazoÎncă nu există evaluări
- An Approach To The Diagnostic Study On Annavaha Srotodusti in Urdwaga Amlapitta WSR To Oesophagogastroduodenoscopic ChangesDocument4 paginiAn Approach To The Diagnostic Study On Annavaha Srotodusti in Urdwaga Amlapitta WSR To Oesophagogastroduodenoscopic ChangesEditor IJTSRDÎncă nu există evaluări
- PCM ManualDocument230 paginiPCM ManualBostenLovelessÎncă nu există evaluări
- Antibiotic Guidelines (2020) - 0Document55 paginiAntibiotic Guidelines (2020) - 0yudhit bessieÎncă nu există evaluări
- Magnesium and Type 2 Diabetes: Mario Barbagallo, Ligia J DominguezDocument7 paginiMagnesium and Type 2 Diabetes: Mario Barbagallo, Ligia J DominguezbayuwinotoÎncă nu există evaluări
- The Over Training SyndromeDocument4 paginiThe Over Training SyndromeFilip ZalioÎncă nu există evaluări
- Best Practice Diagnostic Guidelines For Patients Presenting With Breast Symptoms PDFDocument60 paginiBest Practice Diagnostic Guidelines For Patients Presenting With Breast Symptoms PDFfauziafahmi95Încă nu există evaluări
- Diseases of The Newborn Part2Document6 paginiDiseases of The Newborn Part2sarguss14100% (1)
- Ezolvin Syrup Patient Information Leaflet PDFDocument1 paginăEzolvin Syrup Patient Information Leaflet PDFSameer SamouaÎncă nu există evaluări
- Epoch Elder Care Provides High Quality Assisted Living HomesDocument17 paginiEpoch Elder Care Provides High Quality Assisted Living HomesMahesh MahtoliaÎncă nu există evaluări
- Application Form of Adi-Kailash/ Aum Parvat Yatra - 2012: Kumaon Mandal Vikas Nigam LTDDocument4 paginiApplication Form of Adi-Kailash/ Aum Parvat Yatra - 2012: Kumaon Mandal Vikas Nigam LTDpsureshÎncă nu există evaluări
- Çikmiş Sorularinin Luk Kismi: E-Yds 2020-13Document5 paginiÇikmiş Sorularinin Luk Kismi: E-Yds 2020-13Mustafa AriÎncă nu există evaluări
- Cage HomesDocument8 paginiCage HomesstanhopekrisÎncă nu există evaluări
- Lemon Grass - Introduction FinalDocument13 paginiLemon Grass - Introduction FinalDiana Jane Lagundino100% (1)
- The Sketch of Indonesia Medicine: Sugma AP, MD, MARSDocument42 paginiThe Sketch of Indonesia Medicine: Sugma AP, MD, MARSRaja Friska YulandaÎncă nu există evaluări
- Dr. Jean Dodds Expert Report (Plaintiff)Document2 paginiDr. Jean Dodds Expert Report (Plaintiff)Osiris-KhentamentiuÎncă nu există evaluări
- Toxicological Materia MedicaDocument104 paginiToxicological Materia Medicakayes82Încă nu există evaluări
- GAGAL GINJAL KRONIS DAN INDIKASI DIALISISDocument34 paginiGAGAL GINJAL KRONIS DAN INDIKASI DIALISISDjumadi AkbarÎncă nu există evaluări
- Out 8Document10 paginiOut 8tofanÎncă nu există evaluări
- Soal Bahasa Inggris SNMPTN 2008 101Document5 paginiSoal Bahasa Inggris SNMPTN 2008 101DittoCendykiaIIÎncă nu există evaluări