Documente Academic
Documente Profesional
Documente Cultură
JInterdiscipDentistry6144-3926729 105427 PDF
Încărcat de
priyanka shelkeTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
JInterdiscipDentistry6144-3926729 105427 PDF
Încărcat de
priyanka shelkeDrepturi de autor:
Formate disponibile
[Downloaded free from http://www.jidonline.com on Wednesday, May 15, 2019, IP: 117.232.206.
232]
Review Article Periodontal biotype: Basics and clinical
considerations
Rucha Shah, N. K. Sowmya, Raison Thomas, Dhoom Singh Mehta
Department of Periodontics, Bapuji Dental College and Hospital, Davangere, Karnataka, India
Address for correspondence: Dr. Rucha Shah, E‑mail: srucha2k@yahoo.com
ABSTRACT
Gingival/periodontal biotype is now known to influence the indications and outcomes of various therapies routinely performed
in a dental clinic. The delicate thin biotype is more susceptible to injury and responds in a different way clinically as compared
to the sturdier thick biotype. Assessment, identification, and indicated treatment considerations are now becoming the key to
achieve predictable results, good esthetics, and stability of soft tissue margins. This review describes the various classifications,
methods of assessment and clinical considerations for both the thick and thin tissue biotypes.
CLINICAL RELEVANCE TO INTERDISCIPLINARY DENTISTRY
In the era of evidence‑based interdisciplinary dentistry, none of the dental disciplines are mutually exclusive. The treatment
plan, treatment response, and prognosis of dental procedures vary greatly between teeth with different biotypes. Hence, the
knowledge and assessment of gingival/periodontal biotype has become an important routine in clinical decision‑making.
Key words: Gingival biotype, periodontal biotype, periodontal therapy
INTRODUCTION morphology, namely the scalloped and thin or flat
and thick gingiva.[1] The term “periodontal biotype”
G ingiva is the part of the oral mucosa that
covers the alveolar processes of the jaws and
surrounds the necks of the teeth. A well‑scalloped
was later introduced by Seibert and Lindhe to
categorize the gingiva into “thick flat” and “thin
scalloped” biotypes.[2] In general, the term gingival
gingival line at the cemento‑enamel junction (CEJ) of biotype has been used to describe the thickness of
the teeth forms one of the pillars of a beautiful smile. the gingiva in the facio‑palatal dimension. Whereas
Clinicians handle gingiva in several dental procedures the term “periodontal biotype” encompasses not
and the resulting gingival architecture is not always only the thickness of gingiva, but also other features
ideal. In the era of esthetics‑driven dentistry, it is such as contour of gingiva, alveolar bone contour
of paramount importance that a clinician should be and thickness, amount of keratinized gingiva
well‑aware of all the factors that may influence the present, and crown shape. [3] With the increase
final esthetic outcome of a treatment. One such factor in the amount of literature on the topic, it is now
that clinicians should consider before starting any understood that dif ferent gingival/periodontal
restorative, prosthetic, and periodontal procedure is biotypes behave in a different manner under similar
the “tissue biotype.” clinical conditions. Furthermore, the treatment
considerations for individuals with dif fer ent
Ochsenbein and Ross in their pioneer study biotypes differ.
indicated that there were two main types of gingiva
This is an open access article distributed under the terms of the Creative Commons
Access this article online Attribution‑NonCommercial‑ShareAlike 3.0 License, which allows others to
remix, tweak, and build upon the work non‑commercially, as long as the author
Quick Response Code: is credited and the new creations are licensed under the identical terms.
Website:
www.jidonline.com For reprints contact: reprints@medknow.com
DOI: How to cite this article: Shah R, Sowmya NK, Thomas R, Mehta DS.
10.4103/2229-5194.188172 Periodontal biotype: Basics and clinical considerations. J Interdiscip
Dentistry 2016;6:44-9.
44 © 2016 Journal of Interdisciplinary Dentistry | Published by Wolters Kluwer - Medknow
[Downloaded free from http://www.jidonline.com on Wednesday, May 15, 2019, IP: 117.232.206.232]
Shah, et al.: Periodontal biotype
GINGIVAL/PERIODONTAL BIOTYPE contour, thick flat osseous gingival contour, broad apical
CLASSIFICATIONS contact areas in teeth, and square anatomic crowns. It
is mostly associated with periodontal health. The tissue
Several classifications have been pr oposed for is dense with a wide zone of attached gingiva. The
gingival/periodontal biotypes. Even while classifying underlying bony architecture is considered to be thick.
periodontal biotypes, gingival thickness is considered an Surgical exposures in such cases demonstrate thick
important factor as gingival and periodontal biotypes are underlying osseous forms [Figure 2].[3,10] The prevalence
considered to be closely related. Gingival/periodontal of thick biotype is around 56%.[11,12]
biotype may differ from tooth to tooth in a person; may differ
with age, gender, and dental arch location.[4] There is no
universally accepted classification for gingival/periodontal METHODS OF MEASUREMENT OF
biotypes. There is also a lack of agreement between GINGIVAL THICKNESS
authors as to what thickness of gingiva would be
considered thin or thick. Gingival biotypes were initially Many methods have been proposed till date to analyze the
classified by Oschenbein and Ross as thin or thick. gingival tissue thickness. These are described as follows:
However, several classifications of gingival biotypes
have been presented over time [Table 1].[5‑8] In a recent Direct measurements
systematic review, it was concluded that the available The gingiva is anesthetized by topical application of an
definitions of gingival/periodontal biotypes are unclear, anesthetic gel. An endodontic spreader with a rubber stop/
and the three biotypes: Thin scalloped, thick flat, and caliper is inserted at a point at the center of the gingival
thick scalloped seem a comprehensive categorization margin and mucogingival junction in a perpendicular
in defining periodontal biotypes in the population.[9] In direction and this measurement is recorded against a
spite of a lack of agreement for the classification method, digital caliper. It is an accurate method of measurement,
most of the studies attribute similar features to a thick and however it is an invasive technique.[8]
a thin biotype. Each biotype possesses its own unique
characteristics. Visual examination
The thin and scalloped biotype is said to have a delicate The gingival biotype is clinically evaluated based on the
and thin periodontium, highly scalloped gingival tissue, general appearance of the gingiva around the tooth. The
usually may present slight gingival recession, presents gingival biotype was considered thick if the gingiva was
highly scalloped osseous contour, small incisal contact
areas in the teeth, and triangular anatomic crowns. Thin Table 1: Different classifications for gingival/
gingival tissue tends to be delicate and almost translucent periodontal biotype
in appearance. The tissue appears friable with a minimal
Authors Classification
zone of attached gingiva, and the soft tissue is highly Ochsenbein and Ross[1] Scalloped Flat and thick
accentuated and often suggestive of thin or minimal bone and thin
over the labial roots. Surgical exposure in such cases Seibert and Lindhe[2] Thick ≥2 mm Thin <1.5 mm
generally demonstrates thin labial bone with an increased Becker et al.[5] (distance Flat: 2.1 mm Scalloped: Pronounced
between interproximal 2.8 mm scalloped: 4.1 mm
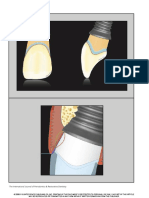
incidence of fenestration and dehiscence [Figure 1].[3,10] The and mid‑facial level of
prevalence of thin biotype is around 43%.[11,12] alveolar bone)
Kan et al.[6] Thick >1 mm Thin ≤1 mm
Claffey and Shanley[7] Thick ≥2 mm Thin <1.5 mm
The thick and flat biotype is characterized by thick heavy
Egreja et al.[8] Thick >1 mm Thin <1 mm
periodontium, gingival margin usually placed coronal
to CEJ, wide zones of keratinized gingiva, flat gingival
Figure 1: Clinical presentation of thin gingival biotype Figure 2: Clinical presentation of thick gingival biotype
Journal of Interdisciplinary Dentistry / Jan-Apr 2016 / Vol-6 / Issue-1 45
[Downloaded free from http://www.jidonline.com on Wednesday, May 15, 2019, IP: 117.232.206.232]
Shah, et al.: Periodontal biotype
dense and fibrotic and thin if the gingiva was delicate, in thin biotype, we see more inflammatory changes and
friable, and almost translucent. The advantage of this recession of gingiva.[10] This basic difference in the response
technique is that it is minimally invasive, however it has of thick biotype tissue as compared to thin biotype is the
been found to have a very low accuracy and a very high fundamental for the variation response and consideration
interexaminer variation.[13] for these under various clinical scenarios. Patients with a
thin biotype are more vulnerable to connective tissue loss
Probe transparency and epithelial damage, thus they need special atraumatic
treatment and oral hygiene techniques.[18]
Sulcus probing of the mid‑facial aspect of the tooth
is performed. The gingival biotype is categorized as
Crown lengthening procedure
either thin or thick according to the visibility of the
underlying periodontal probe through the gingival tissue In crown lengthening procedures, the amount of tissue
(visible = thin, not visible = thick). It is a minimally invasive exposure required for further rehabilitation of the
technique with a good accuracy.[14] tooth dictates the amount of bone removal during the
procedure. Significant postoperative tissue rebound has
Ultrasonic devices been observed in cases of thick biotype as compared to
thin biotype.[19] Thus, tissue biotype is an important feature
A sensitive, thin probe attached to an ultrasonic device to be assessed in such cases, and slight overcorrection or
measures the biotypes ultrasonically. It uses the pulse echo immediate rehabilitation may be advised in such cases.
principle for the determination of biotype thickness. This
technique gives accurate measurement ‑ digital display, Orthodontic therapy
avoids interexaminer variability, and noninvasive, but the
high cost of equipment and limited availability make it In the course of orthodontic therapy, teeth are moved
less feasible.[15] in various directions (buccally, lingually, coronally, and
apically). In an attempt to bring teeth in an ideal position,
Cone beam computed tomography it may sometimes lead to soft tissue recession or hard
tissue dehiscence and fenestration. It has been observed
It is used to visualize and measure the thickness of both that such tooth movement results in increased recession
hard and soft tissues. Highly accurate results can be and increased incidence of dehiscence and fenestration
achieved using cone beam computed tomography (CBCT), formation in cases with thin biotype.[20] Hence, such
and there is no interexaminer variation. However, there cases should be approached with more caution. Another
is some amount of radiation exposure and increased cost consideration could be placement of mini‑screws where
for the patients.[16,17] a thin biotype warrants more caution.
When the reliability of assessing gingival biotype of Prosthesis esthetics
maxillary anterior teeth with and without the use of a
periodontal probe in comparison with direct measurements The thin biotype is more prone to recession of gingiva. It has
was performed, the authors found that assessment been observed that in relation to metal ceramic prosthesis
with a periodontal probe is an adequately reliable and over a period of 5 years, significantly more gingival
objective method in evaluating gingival biotype, whereas recession is observed after prosthesis placement in thin
visual assessment of the gingival biotype by itself is not biotype as compared to thick biotype.[21] This underscores
sufficiently reliable compared to direct measurement.[6] the importance of assessment and management of thin
Keeping in mind all pros and cons of the various analytical biotype cases at the time of prosthesis placement. In areas
modalities, direct measurement and probe transparency of high esthetic requirement, biotype enhancement can
are good methods to detect gingival biotype clinically. prevent such unpleasant clinical scenario. On the basis
of these findings, it can be suggested that more caution
should be exercised while planning a subgingival margin
PERIODONTAL BIOTYPES: CLINICAL placement for patients with a thin biotype as minimal
tissue injury may result in adverse outcome in future.
APPLICATIONS
More controlled studies on these conditions are required.
Tissue biotypes are associated with the outcomes
Root coverage in thick versus thin biotypes
of a variety of dental clinical procedures. In several
dental procedures, the gingival tissue is subjected to It was proposed that thick gingival tissue eases
clinical/surgical insults and both the biotypes respond manipulation, maintains vascularity, and promotes wound
differently to them. In the event of inflammation or any healing during and after surgery. A critical threshold
other type of insult, soft tissue in a thick biotype responds thickness (>1.1 mm) for root coverage success may exist
by more fibrotic changes and pocket formation, however for predictable root coverage.[22] Hence, patients having a
46 Journal of Interdisciplinary Dentistry / Jan-Apr 2016 / Vol-6 / Issue-1
[Downloaded free from http://www.jidonline.com on Wednesday, May 15, 2019, IP: 117.232.206.232]
Shah, et al.: Periodontal biotype
thinner biotype can be treated preferably with techniques cases, preemptive biotype correction may be considered.
that create a pseudo‑thick biotype such as a connective The tissue biotype is considered a key factor in implant
tissue graft in conjunction with coronally advanced flap as esthetics, preventing future mucosal recession, and
compared to a coronally advanced flap alone.[10] In another improving immediate implant success.[28‑30]
study, it was mentioned that the thin gingival biotype may
impair the clinical outcome of root coverage procedures, Another emerging concept in patients with thin biotype
and to overcome this, the same coverage can be done is that of a flapless approach for implant placement. In
using sub‑epithelial connective tissue graft which provides the conventional method, a full‑thickness buccal and
better results.[23] lingual/palatal flap is raised, osteotomy is prepared, and
implant placement is done. In the minimally invasive
Supragingival tissue flapless approach, a surgical guide is prepared using the
CBCT image. Using the guide, a circular punch is made on
It has been observed that median supracrestal gingival
the ridge and implant placement is done. This prevents the
tissue is more in thick flat biotype as compared to thin
disruption of blood supply to alveolar bone which would
scalloped biotype.[24] Overhanging restorations can more
be occurring when we raise a full thickness flap. Studies
frequently and rapidly result in tissue destruction.
have shown that after the placement of implants using a
flapless approach, the papillary recession and bone loss
Flap handling were minimized in patients with thin gingival biotype.[31]
Owing to the delicate nature of gingival tissue in thin
biotype routine, procedures such as gingival curettage In addition, it has been shown in a study that laser
needs to be performed more carefully. In cases of flap micro‑textured implant collar may prevent proximal bone
surgery, careful handling of the flap is more significant in less in thin biotype cases.[27]
thin biotype cases.
Extraction of teeth in thick versus thin ENHANCING THE GINGIVAL BIOTYPE
biotypes
A preexisting thin gingival biotype can impede ideal
Although extractions should always be atraumatic, teeth esthetic result of many therapies. In such a scenario,
with thin gingival biotypes merit more attention due to gingival biotype can be enhanced. This concept is in its
their association with thin alveolar plates.[3,25] Atraumatic infancy and just emerging. A pseudo thick gingiva is
extraction and preservation of the alveolar plate are when an originally thin gingiva is converted to a thick
essential. Excessive force is more likely to fracture the gingiva.[10] This can be done to achieve more stable results
buccal alveolar plate in thin biotype and results in bone to avoid soft tissue relapse. It can also aid in achieving
resorption and unpredictable bone healing. more esthetic results. A study demonstrated that bone loss
can be controlled in thin biotype patients, if the biotype is
Ridge preservation in thick versus thin augmented prior to the placement of implant.[30]
biotypes
Few procedures can be performed to enhance the biotype of
Given the thin alveolar plate associated with thin
gingival tissue. One such procedure is the use of connective
periodontal biotypes, more extensive ridge remodeling
tissue grafts.[32] In this procedure, a connective tissue graft
is seen in thin biotype when compared to thick biotypes
harvested from palate/tuberosity is placed at the site of
leading to exaggerated loss in hard and soft tissue volume.
thin biotype subepithelially. For the same, either a full or
Hence, in a patient with thin biotype, augmentative
partial dissection can be done. Once the graft is in position,
procedures such as socket preservation/augmentation
it is sutured. Once healing is completed, a thin biotype is
may be performed to ensure an esthetic and functional
converted into a stable thick biotype. This can be attributed
result in future.[26]
to the primarily fibrous content of the graft and the bulk
that they provide at the recipient site. They have not only
Tissue biotype in implant treatment planning
been seen to improve gingival biotype, but also increase
In thick biotype, significantly, less bone loss is seen after the long‑term stability of the results. It is the most reliable
implant placement as compared to thin biotypes.[27] In a and frequently documented method of enhancing gingival
thick biotype environment, immediate placement of an biotype. However, donor site morbidity, limited availability,
implant can be completed with predictable results. In a and increased operating time are the disadvantages
thin biotype cases, the possibility of significant resorption, associated with connective tissue placement.
which may have an impact on esthetics, is high. A delayed
implant placement should be preferred when the thickness As an alternate to connective tissue, acellular dermal
of the periodontal tissues is not sufficient. In thin biotype matrix can also be used to enhance the biotype. The
Journal of Interdisciplinary Dentistry / Jan-Apr 2016 / Vol-6 / Issue-1 47
[Downloaded free from http://www.jidonline.com on Wednesday, May 15, 2019, IP: 117.232.206.232]
Shah, et al.: Periodontal biotype
procedure of placement and healing mechanism is similar Conflicts of interest
to that of the connective tissue graft. It has the advantage
There are no conflicts of interest.
of lowering the patient morbidity due to the absence of
a second donor site; however, the high cost and limited
availability are its drawbacks.
REFERENCES
Another mode of enhancing the gingival biotype is the 1. Ochsenbein C, Ross S. A reevaluation of osseous surgery. Dent Clin
placement of platelet‑rich fibrin (PRF) membrane. PRF is North Am 1969;13:87‑102.
a blood‑derived, autologous, second‑generation platelet 2. Seibert JL, Lindhe J. Esthetics and periodontal therapy. In: Lindhe J,
concentrate. It mainly consists of a three‑dimensional editor. Textbook of Clinical Periodontology. 2nd ed. Copenhangen,
fibrin matrix with platelets. These platelets then release Denmark: Munksgaard; 1989. p. 477‑514.
3. Cohen ES. Atlas of Cosmetic and Reconstructive Periodontal Surgery.
several growth factors including platelet‑derived growth
3rd ed. Hamilton: BC Decker Inc.; 2007. p. 247.
factor and vascular endothelial growth factor.[33] Shetty 4. Kolte R, Kolte A, Mahajan A. Assessment of gingival thickness with
et al. in their study demonstrated that placement of PRF regards to age, gender and arch location. J Indian Soc Periodontol
membrane over denuded root surface in conjunction with 2014;18:478‑81.
coronally advanced flap results in the improvement in the 5. Becker W, Ochsenbein C, Tibbetts L, Becker BE. Alveolar bone
thickness of gingiva.[34] anatomic profiles as measured from dry skulls. Clinical ramifications.
J Clin Periodontol 1997;24:727‑31.
6. Kan JY, Morimoto T, Rungcharassaeng K, Roe P, Smith DH. Gingival
Recently, use of fetal membranes such as amnion and biotype assessment in the esthetic zone: Visual versus direct
chorion membrane has demonstrated to enhance gingival measurement. Int J Periodontics Restorative Dent 2010;30:237‑43.
biotype.[35,36] These membranes are allografts derived 7. Claffey N, Shanley D. Relationship of gingival thickness and bleeding
from the human placenta. The membranes are then to loss of probing attachment in shallow sites following nonsurgical
periodontal therapy. J Clin Periodontol 1986;13:654‑7.
obtained, processed, and sterilized for human use. The
8. Egreja AM, Kahn S, Barceleiro M, Bittencourt S. Relationship
main advantage of their membranes is their excellent between the width of the zone of keratinized tissue and thickness of
revascularization, nil antigenicity, and easy availability. gingival tissue in the anterior maxilla. Int J Periodontics Restorative
They can be placed under a tunnel/pouch/coronally Dent 2012;32:573‑9.
advanced flap and sutured. This study demonstrated that 9. Zweers J, Thomas RZ, Slot DE, Weisgold AS, Van der Weijden FG.
Characteristics of periodontal biotype, its dimensions, associations and
after the placement of amnion membrane in conjunction
prevalence: A systematic review. lin Periodontol 2014;41:958‑71.
with coronally advanced flap, the gingival thickness was 10. Kao RT, Pasquinelli K. Thick vs. thin gingival tissue: A key determinant
improved.[34] in tissue response to disease and restorative treatment. J Calif Dent
Assoc 2002;30:521‑6.
However, such reports are few and more controlled 11. Shah R, Sowmya NK, Mehta DS. Prevalence of gingival biotype
studies are required to evaluate the efficacy of both PRF and its relationship to clinical parameters. Contemp Clin Dent
2015;6 Suppl 1:S167‑71.
membranes and fetal membranes. The most effective
12. Matarese G, Isola G, Ramaglia L, Dalessandri D, Lucchese A,
technique of biotype augmentation still remains connective Fabiano F, et al. Periodontal biotype: Characteristic, prevalence and
tissue grafting. dimensions related to dental malocclusion. Minerva Stomatol 2016.
[Epub ahead of print]. PubMed PMID: 27035270.
13. Cuny‑Houchmand M, Renaudin S, Ler oul M, Planche L,
CONCLUSION Guehennec LL, Soueidan A. Gingival biotype assessment: Visual
inspection relevance and maxillary versus mandibular comparison.
Open Dent J 2013;7:1‑6.
By understanding the nature of tissue biotype (thickness), 14. Kan JY, Rungcharassaeng K, Umezu K, Kois JC. Dimensions of
a practitioner can employ appropriate clinical procedures peri‑implant mucosa: An evaluation of maxillary anterior single
to minimize soft tissue loss and alveolar resorption and implants in humans. J Periodontol 2003;74:557‑62.
provide a more favorable tissue environment. Different 15. Müller HP, Heinecke A, Schaller N, Eger T. Masticatory mucosa in
subjects with different periodontal phenotypes. J Clin Periodontol
gingival biotype can influence the diagnosis and 2000;27:621‑6.
treatment planning for different patients. In addition, 16. Barriviera M, Duarte WR, Januário AL, Faber J, Bezerra AC. A new
these techniques when appropriately applied can save on method to assess and measure palatal masticatory mucosa
treatment time and cost for patients. Inclusion of biotype by cone‑beam computerized tomography. J Clin Periodontol
assessment in the diagnostic record of the patient can 2009;36:564‑8.
17. Memon S, Patel JR, Sethuraman R, Patel R, Arora H. A comparative
give the clinician an idea about the care to be taken in
evaluation of the reliability of three methods of assessing gingival
tissue handling, the type of procedure to be employed biotype in dentate subjects in different age groups: An in vivo study.
in a certain situation as well as the expected outcome. J Indian Prosthodont Soc 2015;15:313‑7.
18. Newman MG, Takei HH, Klokkevold PR, Carranza FA. Textbook of
Financial support and sponsorship Clinical Periodontology. 11th ed. Missouri: W.B. Saunders Company;
2012. p. 23.
Nil. 19. Arora R, Narula SC, Sharma RK, Tewari S. Evaluation of supracrestal
48 Journal of Interdisciplinary Dentistry / Jan-Apr 2016 / Vol-6 / Issue-1
[Downloaded free from http://www.jidonline.com on Wednesday, May 15, 2019, IP: 117.232.206.232]
Shah, et al.: Periodontal biotype
gingival tissue after surgical crown lengthening: A 6‑month clinical Implants Res 2015;26:599‑605.
study. J Periodontol 2013;84:934‑40. 28. Kois JC. Predictable single‑tooth peri‑implant esthetics: Five
20. Rasperini G, Acunzo R, Cannalire P, Farronato G. Influence of diagnostic keys. Compend Contin Educ Dent 2004;25:895‑6, 898,
periodontal biotype on root surface exposure during orthodontic 900.
treatment: A preliminary study. Int J Periodontics Restorative Dent 29. Lee A, Fu JH, Wang HL. Soft tissue biotype affects implant success.
2015;35:665‑75. Implant Dent 2011;20:e38‑47.
21. Tao J, Wu Y, Chen J, Su J. A follow‑up study of up to 5 years of 30. Puisys A, Linkevicius T. The influence of mucosal tissue thickening
metal‑ceramic crowns in maxillary central incisors for different on crestal bone stability around bone‑level implants. A prospective
gingival biotypes. Int J Periodontics Restorative Dent 2014;34:e85‑92. controlled clinical trial. Clin Oral Implants Res 2015;26:123‑9.
22. Hwang D, Wang HL. Flap thickness as a predictor of root coverage: 31. Cosyn J, Pollaris L, Van der Linden F, De Bruyn H. Minimally invasive
A systematic review. J Periodontol 2006;77:1625‑34. single implant treatment (M.I.S.I.T.) based on ridge preservation and
23. Kahn S, Almeida RA, Dias AT, Rodrigues WJ, Barceleiro MO, contour augmentation in patients with a high aesthetic risk profile:
Taba M Jr. Clinical considerations on the root coverage of gingival One‑year results. J Clin Periodontol 2015;42:398‑405.
recessions in thin or thick biotype. Int J Periodontics Restorative Dent 32. Grover HS, Yadav A, Yadav P, Nanda P. Optimizing gingival biotype
2016;36:409‑15. using subepithelial connective tissue graft: A case report and
24. Arora R, Narula SC, Sharma RK, Tewari S. Supracrestal gingival one‑year followup. Case Rep Dent 2011;2011:263813.
tissue: Assessing relation with periodontal biotypes in a healthy 33. Kothiwale S, Rathore A, Panjwani V. Enhancing gingival biotype
periodontium. Int J Periodontics Restorative Dent 2013;33:763‑71. through chorion membrane with innovative step in periodontal
25. Kao RT, Fagan MC, Conte GJ. Thick vs. thin gingival biotypes: A key pocket therapy. Cell Tissue Bank 2016;17:33‑8.
determinant in treatment planning for dental implants. J Calif Dent 34. Shetty SS, Chatterjee A, Bose S. Bilateral multiple recession coverage
Assoc 2008;36:193‑8. with platelet‑rich fibrin in comparison with amniotic membrane.
26. Maia LP, Reino DM, Novaes Junior AB, Muglia VA, Taba Junior M, J Indian Soc Periodontol 2014;18:102‑6.
Grisi MF, et al. Influence of periodontal biotype on buccal bone 35. Shah R, Sowmya NK, Mehta DS. Amnion membrane for coverage
remodeling after tooth extraction using the flapless approach with of gingival recession: A novel application. Contemp Clin Dent
a xenograft: A histomorphometric and fluorescence study in small 2014;5:293‑5.
dogs. Clin Implant Dent Relat Res 2015;17 Suppl 1:e221‑35. 36. Esteves J, Bhat KM, Thomas B, Jothi MV, Jadhav T. Efficacy of human
27. Linkevicius T, Puisys A, Svediene O, Linkevicius R, Linkeviciene L. chorion membrane allograft for recession coverage – A case series.
Radiological comparison of laser‑micr otextured and J Periodontol 2015:1-22. [Epub ahead of print] PubMed PMID:
platform‑switched implants in thin mucosal biotype. Clin Oral 25965119.
Journal of Interdisciplinary Dentistry / Jan-Apr 2016 / Vol-6 / Issue-1 49
S-ar putea să vă placă și
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (894)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (587)
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (119)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2219)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (73)
- 1000 Mcqs - Periodontics Plus September 2014 McqsDocument16 pagini1000 Mcqs - Periodontics Plus September 2014 McqsSelvaArockiam86% (7)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- Altered Cast TechniqueDocument7 paginiAltered Cast Techniquepriyanka shelkeÎncă nu există evaluări
- Nano DentistryDocument6 paginiNano Dentistrypriyanka shelkeÎncă nu există evaluări
- Dental JOURNAL: New Era in Denture Base Resins: A ReviewDocument8 paginiDental JOURNAL: New Era in Denture Base Resins: A Reviewpriyanka shelkeÎncă nu există evaluări
- Wear of EnamelDocument6 paginiWear of EnamelarrysanadianaÎncă nu există evaluări
- Imp Gingival Biotype To Be Read 1Document4 paginiImp Gingival Biotype To Be Read 1priyanka shelkeÎncă nu există evaluări
- Antiseptics and DisinfectantsDocument33 paginiAntiseptics and Disinfectantspriyanka shelkeÎncă nu există evaluări
- Chapter 3Document31 paginiChapter 3HugoMoralesTecnicoDental100% (1)
- 6 Prosthetic Driven ImplantologyDocument5 pagini6 Prosthetic Driven Implantologypriyanka shelkeÎncă nu există evaluări
- Smile ComponentDocument11 paginiSmile Componentpriyanka shelkeÎncă nu există evaluări
- Cad Cam PDFDocument4 paginiCad Cam PDFpriyanka shelkeÎncă nu există evaluări
- APRD - 2 (2) - 33-36 (B)Document4 paginiAPRD - 2 (2) - 33-36 (B)Nur Syfa MufidhahÎncă nu există evaluări
- A Telescopic Denture Is A Prosthesis Which Consists of A Primary Coping Which Is Cemented To The Abutments in A PatientDocument14 paginiA Telescopic Denture Is A Prosthesis Which Consists of A Primary Coping Which Is Cemented To The Abutments in A Patientpriyanka shelkeÎncă nu există evaluări
- IJCD RubberdamDocument13 paginiIJCD RubberdamAyik DarkerThan BlackÎncă nu există evaluări
- Long Case OmdrDocument22 paginiLong Case OmdrdhrÎncă nu există evaluări
- Restoration of Endodontically Treated TeethDocument84 paginiRestoration of Endodontically Treated TeethEazhil RajÎncă nu există evaluări
- Esej How Did Eqyptian Civilization Inventions Affect Modern World SocietyDocument5 paginiEsej How Did Eqyptian Civilization Inventions Affect Modern World SocietyEdin Cehic CehaÎncă nu există evaluări
- Molly Mcsweeney: 1653 San Marino Dr. Petaluma, Ca 94954Document4 paginiMolly Mcsweeney: 1653 San Marino Dr. Petaluma, Ca 94954api-305352923Încă nu există evaluări
- Operative 20 VeneersDocument21 paginiOperative 20 VeneersInneke SutantoÎncă nu există evaluări
- Muscle Deprogramming - An Orthodontist's Perspective: Batra Laxman Ra Angshuman B LlachDocument5 paginiMuscle Deprogramming - An Orthodontist's Perspective: Batra Laxman Ra Angshuman B LlachJulio Cesar AlvearÎncă nu există evaluări
- Lab 5 Cementum and Periodontal LigamentDocument13 paginiLab 5 Cementum and Periodontal Ligamentdr.naseer100% (1)
- Lec 4 (3rd) ClassDocument6 paginiLec 4 (3rd) ClassBrandon AviciiÎncă nu există evaluări
- Horizontal Jaw Relation, Method of Recording andDocument93 paginiHorizontal Jaw Relation, Method of Recording andHaroon Mohamed100% (1)
- Pediatric Oral MedicineDocument17 paginiPediatric Oral MedicinebanyubiruÎncă nu există evaluări
- Evaluation of Guided Bone Regeneration and or Bone Grafts in The Treatment of Ligature-Induced Peri-Implantitis DefectsDocument6 paginiEvaluation of Guided Bone Regeneration and or Bone Grafts in The Treatment of Ligature-Induced Peri-Implantitis Defectsmatias112Încă nu există evaluări
- Periodontal Care Plan TemplateDocument7 paginiPeriodontal Care Plan Templateapi-597791259Încă nu există evaluări
- A Clinical Guide To OrthodonticsDocument77 paginiA Clinical Guide To OrthodonticsSzenyes SzabolcsÎncă nu există evaluări
- Reducing The Risk of Failure Incomplete Denture PatientsDocument8 paginiReducing The Risk of Failure Incomplete Denture PatientsHisyam IshakÎncă nu există evaluări
- Dental Anthropology: September 2017Document9 paginiDental Anthropology: September 2017Amira IzzatusyuhadaÎncă nu există evaluări
- Canine Body LanguageDocument4 paginiCanine Body LanguageAB0% (1)
- Dental Caries SeminarDocument120 paginiDental Caries Seminarcoolprats_25Încă nu există evaluări
- Tooth Numbering System: Whydoweneed?Document3 paginiTooth Numbering System: Whydoweneed?najwan domaÎncă nu există evaluări
- Locator Overdenture Implant System Manual - INST1247Document28 paginiLocator Overdenture Implant System Manual - INST1247gildeipiraÎncă nu există evaluări
- Furcation Involvement Classification: A Comprehensive Review and A New System ProposalDocument13 paginiFurcation Involvement Classification: A Comprehensive Review and A New System ProposalBikram KarkiÎncă nu există evaluări
- Teeth: Miss Sandy TseDocument21 paginiTeeth: Miss Sandy Tseyin_sandy1129Încă nu există evaluări
- Anterior Open BiteDocument7 paginiAnterior Open BiteGowriÎncă nu există evaluări
- 8-Treatment of Deep Caries, Vital Pulp Exposure, Pulpless TeethDocument8 pagini8-Treatment of Deep Caries, Vital Pulp Exposure, Pulpless TeethAhmed AbdÎncă nu există evaluări
- Critical and Subcritical ContourDocument10 paginiCritical and Subcritical ContourAndrés LambarriÎncă nu există evaluări
- A Clinical and Histological Evaluation of Titanium Mini Implants As Anchors For Orthodontic Intrusion in The Beagle DogDocument9 paginiA Clinical and Histological Evaluation of Titanium Mini Implants As Anchors For Orthodontic Intrusion in The Beagle DogCansu ozguÎncă nu există evaluări
- Holistic Dental Approach For Visually Impaired Children: A Narrative ReviewDocument8 paginiHolistic Dental Approach For Visually Impaired Children: A Narrative ReviewIJAR JOURNAL100% (1)
- Literatur 2Document7 paginiLiteratur 2aninuraniyahÎncă nu există evaluări
- January 2018 1516198794 146 PDFDocument1 paginăJanuary 2018 1516198794 146 PDFGaby ZapataÎncă nu există evaluări