Documente Academic
Documente Profesional
Documente Cultură
Leukodystrophies 11
Încărcat de
Nathaly LapoTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Leukodystrophies 11
Încărcat de
Nathaly LapoDrepturi de autor:
Formate disponibile
REVIEW ARTICLE
Leukodystrophies
C O N T I N UU M A UD I O By Amy T. Waldman, MD, MSCE
I NT E R V I E W A V AI L A B L E
ONLINE
ABSTRACT
PURPOSE OF REVIEW: The leukodystrophies, typically considered incurable
neurodegenerative disorders, are often diagnosed after irreversible central
and peripheral nervous system injury has occurred. Early recognition of
CITE AS:
these disorders is imperative to enable potential therapeutic interventions.
CONTINUUM (MINNEAP MINN) This article provides a summary of the symptoms of and diagnostic
2018;24(1, CHILD NEUROLOGY): evaluation for leukodystrophies, along with the currently available
130–149.
therapies and recent advances in management.
Address correspondence to
Dr Amy T. Waldman, Children’s RECENT FINDINGS: The leukodystrophies are a rapidly expanding field because
Hospital of Philadelphia, CTRB
of advances in neuroimaging and genetics; however, recognition of the
10th Floor, Room 10012, 3501 Civic
Center Blvd, Philadelphia, PA clinical and biochemical features of a leukodystrophy is essential to
19104, waldman@email.chop. accurately interpret an abnormal MRI or genetic result. Moreover, the
edu.
initial symptoms of leukodystrophies may mimic other common pediatric
RELATIONSHIP DISCLOSURE: disorders, leading to a delay in the recognition of a degenerative disorder.
Dr Waldman serves on the
board of directors of the Child
Neurology Foundation and has SUMMARY: This article will aid the clinician in recognizing the clinical features
received personal compensation of leukodystrophies and providing accurate diagnosis and management.
for speaking engagements from
Johns Hopkins University, St.
Christopher’s Hospital for
Children, St. Peter’s University,
and SUNY Downstate Medical INTRODUCTION
T
Center. Dr Waldman receives he leukodystrophies are inherited disorders that predominantly affect
research/grant support from
Biogen, Elise’s Corner, the the white matter of the central nervous system (CNS). Leukodystrophy
National Institutes of Health is a unifying term for diseases that affect glial cells, resulting in
(K23NS069806, R01NS071463), myelin sheath and axonal damage; approximately 30 distinct
and the National Multiple
Sclerosis Society and receives disorders have been classified as leukodystrophies (TABLE 6-1). 1
publishing royalties from Leukodystrophies are distinguished from genetic leukoencephalopathies, which
UpToDate, Inc.
may also have significant white matter involvement but whose pathology does
UNLABELED USE OF not primarily affect glia. Such conditions include systemic inborn errors of
PRODUCTS/INVESTIGATIONAL metabolism and primary neuronal disorders (such as neuronal ceroid
USE DISCLOSURE:
Dr Waldman discusses published
lipofuscinoses, which are also lysosomal storage disorders). Altogether, more
clinical trial results presenting a than 91 leukodystrophies and genetic leukoencephalopathies have been
lentiviral vector in combination defined based on clinical, radiographic, and genetic data.
with hematopoietic stem cell
transplantation for Clinically, a leukodystrophy is generally suspected in a child with regression in
metachromatic leukodystrophy developmental skills or failure to acquire new skills. Peripheral nervous system
and X-linked
disease also occurs in some of the leukodystrophies and may be a presenting feature;
adrenoleukodystrophy. These
data are presented to therefore, a high index of suspicion is necessary to ensure a prompt diagnosis.
demonstrate advances in MRI is a key tool in differentiating leukodystrophies. On T2-weighted images,
potential treatments for this
disorder and also help to
symmetric hyperintensities occur in various regions depending upon the
understand the pathology and underlying disorder.2 Typically the affected white matter is significantly
need for newborn screening. hypointense on T1-weighted images; however, a distinct subgroup, the
© 2018 American Academy hypomyelinating leukodystrophies, are isointense or hyperintense (or sometimes
of Neurology. mildly hypointense) on T1-weighted images. The MRIs of patients with
130 FEBRUARY 2018
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
suspected leukodystrophies should be systematically reviewed to differentiate KEY POINTS
hypomyelinating from demyelinating disorders (using T1-weighted images),
● The leukodystrophies
determine the extent of white matter abnormality (confluent, isolated, comprise a heterogeneous
multifocal), categorize confluent disease by primary area of involvement group of disorders
(frontal, frontotemporal, parietooccipital, periventricular, subcortical, diffuse predominantly affecting
cerebral, or posterior fossa), and observe for the presence of MRI features unique the glial cell or myelin
sheath.
to certain disorders (eg, cysts, contrast enhancement, calcifications).2 Together,
these factors aid the clinician in narrowing the differential diagnosis. ● Genetic
Generally, the treatment of the leukodystrophies is supportive, with a leukoencephalopathies
multidisciplinary team to assist in managing the symptoms. Briefly, medications include metabolic
are used to treat seizures, spasticity, dystonia, autonomic dysfunction, and other disorders and primary
neuronal diseases that affect
symptoms, while equipment is used to optimize comfort, tone, and safety. Most the white matter through
children need further assistance with respect to nutrition and gastrointestinal mechanisms other than glial
function as well as pulmonary clearance and reserve. pathology.
The field of leukodystrophies is rapidly changing through gene discovery,
● X-linked
newborn screening, and novel therapy programs. This article focuses on a few adrenoleukodystrophy
of the leukodystrophies that highlight these advances, particularly those with should be considered in
recent clinical trials and treatment trials planned in the near future. Improved school-aged boys with the
neurologic outcomes occur with early treatment, which is predicated on prompt recent onset of attention
and behavioral difficulties,
recognition of the disorder.
especially for those who
demonstrate regression in
X-LINKED ADRENOLEUKODYSTROPHY cognition, fine motor skills,
X-linked adrenoleukodystrophy is a peroxisomal disorder caused by mutations or speech. While MRI may
be helpful in confirming
in ABCD1 on Xq28. ABCD1 encodes a peroxisomal membrane protein cerebral involvement, the
(ATP-binding cassette, subunit D) that is necessary for b-oxidation of saturated test of choice to confirm
unbranched very-long-chain fatty acids. As a result, very-long-chain fatty or exclude X-linked
acids accumulate in the brain, adrenal gland, and testes.3 adrenoleukodystrophy is
measurement of plasma
very-long-chain fatty acids.
Clinical Symptoms
Multiple phenotypes exist in X-linked adrenoleukodystrophy, with varying ● The adrenal function of
severity and clinical manifestations (TABLE 6-2 4 ). The earliest symptom in boys with X-linked
X-linked adrenoleukodystrophy is adrenal insufficiency, with affected boys adrenoleukodystrophy
should be monitored
coming to medical attention during an adrenal crisis. For approximately 10% of routinely by an
males, adrenal insufficiency is the only manifestation of disease (known as endocrinologist.
Addison only). The childhood cerebral form occurs in approximately 31% to 35%
of affected males and typically presents between 4 and 8 years of age with
attention difficulties, cognitive decline, and behavioral problems (CASE 6-1).
Changes in speech and handwriting occur, and school performance is affected.
Many children are initially thought to have attention deficit hyperactivity
disorder, and the delay in diagnosis precludes them from potential therapy. The
attention and behavioral problems may be present for several months, followed
by progressive loss of ambulation, speech, vision, and hearing over 6 months to
2 years. Adrenomyeloneuropathy (40% to 46% of affected males) occurs later in
life, manifesting as a distal axonopathy. Some females can develop symptoms in
adulthood, making the term carrier a misnomer.
Neuroimaging
Children with childhood cerebral X-linked adrenoleukodystrophy experience
inflammatory demyelination in the brain (confluent T2-hyperintense and
T1-hypointense lesions), typically beginning in the parietooccipital lobes (85% of
CONTINUUMJOURNAL.COM 131
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
LEUKODYSTROPHIES
cases) and posterior corpus callosum (FIGURE 6-1), although anterior
presentations can also occur. The Loes scoring system5,6 is universally applied to
quantify the extent of cerebral involvement. Regions of the brain (such as
parietooccipital white matter, anterior temporal white matter, visual pathway,
corpus callosum, auditory pathway, basal ganglia, projection fibers, and cerebellum)
are subdivided and scored based on the extent of disease (with a score of 0 if normal,
0.5 if unilateral involvement is present, and 1 if the lesion or atrophy is bilateral).
Global atrophy is also assessed. A normal MRI scan has a score of 0, and the
maximum severity score is 34. An enhancing rim is often seen at the border of the
T2-hyperintense area. Younger boys identified through newborn screening or
presentation with adrenal insufficiency have a normal brain MRI but require frequent
TABLE 6-1 The Leukodystrophiesa
Inborn Errors of Metabolism
u X-linked adrenoleukodystrophy
u Krabbe disease (globoid cell leukodystrophy)
u Metachromatic leukodystrophy
u Cerebrotendinous xanthomatosis
u Canavan disease
u Fucosidosis
u Peroxisomal biogenesis disorders (including Zellweger syndrome, neonatal
adrenoleukodystrophy, and infantile Refsum disease)
u Polyglucosan body disease
u Sialic acid storage disorders (Salla disease, infantile sialic acid storage disease, and
intermediate form)
u Single-bifunctional enzyme deficiencies of peroxisomal fatty acid b-oxidation (including
D-bifunctional protein deficiency, sterol carrier protein X [SCPx] deficiency, peroxisomal
acyl-coenzyme A [CoA] oxidase deficiency)
u Sjögren-Larsson syndrome
Disorders of RNA/DNA Transcription/Translation
u Aicardi-Goutières syndrome
u POL3-related disorders (hypomyelination, hypogonadotropic hypogonadism, and
hypodontia [4H syndrome])
u EIF2B-related disorder (vanishing white matter disease or childhood ataxia with central
nervous system hypomyelination [CACH])
u Hypomyelination with brainstem and spinal cord involvement and leg spasticity (HBSL)
u Leukoencephalopathy with brainstem and spinal cord involvement and lactate elevation (LBSL)
u Leukoencephalopathy with thalamus and brainstem involvement and high lactate (LTBL)
u RNAse T2–deficient leukoencephalopathy
CONTINUED ON PAGE 133
132 FEBRUARY 2018
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
MRI surveillance scans (every 6 months between 3 and 10 years of age) to promptly
recognize those who develop the cerebral form who may benefit from treatment.
Diagnosis
The diagnosis of X-linked adrenoleukodystrophy is confirmed by the presence of
elevated saturated unbranched very-long-chain fatty acids in plasma, red blood
cells, or cultured fibroblasts. The biochemical abnormalities among the
very-long-chain fatty acids include elevations in hexacosanoic acid (C26), the
hexacosanoic acid to docosanoic acid ratio (C26:C22), and the hexacosanoic
acid to tetracosanoic acid ratio (C26:C24). Variations in these three
measurements overlap with values for healthy controls; however, a
CONTINUED FROM PAGE 132
CONTINUED FROM PAGE 132
Genes Related to Proteins Critical for Myelin Development
u Pelizaeus Merzbacher disease (PMD)
u Pelizaeus Merzbacher–like disease (PMD)
u SOX10-associated peripheral demyelinating neuropathy, central dysmyelinating leukodystrophy,
Waardenburg syndrome, and Hirschsprung disease (PCWH)
Cytoskeletal
u Alexander disease
u Hypomyelination with atrophy of the basal ganglia and cerebellum (H-ABC)
u Autosomal dominant leukodystrophy with autonomic disease (ADLD)
Myelin Water Maintenance
u Chloride ion channel 2 (ClC2)–related leukoencephalopathy with intramyelinic edema
u Megalencephalic leukoencephalopathy with subcortical cysts (MLC)
Mechanism Not Yet Elucidated
u 18q deletion syndrome
u Adult-onset leukodystrophy with neuroaxonal spheroids and pigmented glia (including
hereditary diffuse leukoencephalopathy with spheroids [HDLS] and pigmentary type of
orthochromatic leukodystrophy with pigmented glia [POLD])
u Hypomyelination with congenital cataract (HCC)
u Oculodentodigital dysplasia
DNA = deoxyribonucleic acid; RNA = ribonucleic acid.
a
Data from Vanderver A, et al, Mol Genet Metab.1
CONTINUUMJOURNAL.COM 133
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
LEUKODYSTROPHIES
TABLE 6-2 X-linked Adrenoleukodystrophy Phenotypes and Frequenciesa
Phenotype Description Estimated Relative Frequency
Phenotypes in males with
X-linked adrenoleukodystrophy
Childhood cerebral Onset at 3–10 years of age; progressive behavioral, 31–35%
cognitive, and neurologic deficits, often leading to total
disability within 3 years; inflammatory brain
demyelination
Adolescent cerebral Like childhood cerebral; onset at 11–21 years of age; 4–7%
somewhat slower progression
Adrenomyeloneuropathy Onset 28 ± 9 years, progressive over decades; distal 40–46%
axonopathy that involves spinal cord mainly; inflammatory
response mild or absent; approximately 40% have or
develop cerebral involvement with varying degrees of
inflammatory response and more rapid progression
Adult cerebral Dementia, behavioral disturbances; sometimes focal 2–5%
deficits, without preceding adrenomyeloneuropathy;
white matter inflammatory response present;
progression parallels that of childhood cerebral form
Olivopontocerebellar Mainly cerebellar and brainstem involvement in 1–2%
adolescence or adulthood
“Addison-only” Primary adrenal insufficiency without apparent Varies with age; up to 50%
neurologic involvement; onset common before in childhood
7.5 years; most eventually develop
adrenomyeloneuropathy
Asymptomatic Biochemical and gene abnormality without Diminishes with age; common
demonstrable adrenal or neurologic deficit; detailed <4 years; very rare >40 years
studies often show adrenal hypofunction or subtle signs
of adrenomyeloneuropathy
Phenotypes in female X-linked
adrenoleukodystrophy carriers
Asymptomatic No evidence of adrenal or neurologic involvement Diminishes with age; most
women <30 years
neurologically uninvolved
Mild myelopathy Increased deep tendon reflexes and distal sensory Increases with age;
changes in lower extremities with absent or approximately 50% >40 years
mild disability
Moderate to severe Symptoms and pathology resemble Increases with age;
myeloneuropathy adrenomyeloneuropathy but milder and later onset approximately 15% >40 years
Cerebral involvement Rarely seen in childhood and slightly more common in Approximately 2%
middle age and later
Clinically evident adrenal Rare at any age Approximately 1%
insufficiency
a
Modified with permission from Kemp S, et al, Hum Mutat.4 © 2001 Wiley-Liss, Inc.
134 FEBRUARY 2018
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
discrimination function is applied that accurately distinguishes those with KEY POINT
X-linked adrenoleukodystrophy from healthy controls or those with
● Very-long-chain fatty
nonperoxisomal disorders.3 In a patient with elevated very-long-chain fatty acids, especially C26:0 and
acids, genetic sequencing of ABCD1 is performed. the ratios of C26:C22 and
Newborn screening for X-linked adrenoleukodystrophy has been implemented C26:C24, are elevated in
in some US states using various methodologies, such as the detection of all clinical phenotypes
of X-linked
1-hexacosanoyl-2-lyso-sn-3-glycero-phosphorylcholine (26:0-lyso-PC) in dried adrenoleukodystrophy,
blood spots using liquid chromatography–tandem mass spectrometry.7–9 The and these abnormalities
diagnosis of X-linked adrenoleukodystrophy through the newborn screening may be detected at birth,
program allows for proactive monitoring of adrenal function and neurologic facilitating a diagnosis prior
to symptom onset.
disease for affected boys and has further enabled the diagnosis of X-linked
adrenoleukodystrophy in family members (such as older siblings) who also
benefit from screening programs.
Disease-specific Therapy
The primary treatable manifestation of X-linked adrenoleukodystrophy is
adrenal insufficiency, which is the most common symptom of the disorder and
present in multiple phenotypes. Biochemical abnormalities in cortisol production
occur in 85% of all males with X-linked adrenoleukodystrophy; screening for
this should begin during infancy, with regular testing throughout the life of an
affected male. The need for cortisol supplementation and stress-dosed steroids or
both is determined in partnership with an endocrinologist.
A 6-year-old boy presented with attention and behavioral difficulties. CASE 6-1
According to his teachers, he had difficulty responding when his name
was called, following along during class activities, and following
directions, requiring reminders. His mother believed that he was often
lost in his thoughts and described him as a daydreamer. These symptoms
were first noted approximately 9 months before presentation.
Previously, he had no issues in preschool and was on target with his
peers. His brother died at 7 months of age “of an infection.”
On examination, he had difficulty with comprehension, often asking
for commands to be repeated, and abnormal expressive language. His
neurologic examination was also notable for difficulty with tandem gait,
brisk patellar reflexes, and extensor plantar responses. Brain MRI
revealed T2 hyperintensities in the parietooccipital lobes bilaterally with
an enhancing rim. Very-long-chain fatty acids revealed an elevation in
hexacosanoic acid (C26:0), an elevated hexacosanoic acid to docosanoic
acid ratio (C26:C22), and an elevated hexacosanoic acid to tetracosanoic
acid ratio (C26:C24).
This case illustrates the clinical variability of the presenting manifestations COMMENT
of X-linked adrenoleukodystrophy. This patient has childhood cerebral
adrenoleukodystrophy, whereas his brother likely died of an unrecognized
adrenal crisis in the setting of an illness.
CONTINUUMJOURNAL.COM 135
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
LEUKODYSTROPHIES
Hematopoietic stem cell
transplantation has been
successful in arresting or slowing
the progression of the cerebral
disease if initiated early in the
disease course (ie, Loes score less
than 10, no or minimal neurologic
symptoms, and preserved
cognition [Wechsler
Performance IQ higher than 80]).
In an experienced X-linked
adrenoleukodystrophy transplant
center, the 5-year survival rate
was 89% in those with a Loes
score of less than 10 (N = 30)
compared to 60% in boys with a
Loes score higher than 10
(N = 30). However, it is
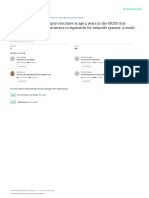
FIGURE 6-1
important to note that even after
Childhood cerebral X-linked adrenoleukodystrophy. successful engraftment, the
Axial fluid-attenuated inversion recovery (FLAIR) neurologic progression may
MRI demonstrates confluent white matter signal continue for 12 to 18 months
abnormality in the bilateral parietal white matter
posttransplant, with disability
with involvement of the splenium of the corpus
callosum, posterior aspect of the thalami, progression occurring during this
and posterior limbs of the internal capsules. time. Therefore, many boys with
minimal evidence of neurologic
disease prior to transplant
develop worsening symptoms, such as visual and cognitive impairment or
behavioral problems, after the transplant. In addition, the transplant itself
confers significant morbidity. Hematopoietic stem cell transplantation is only
performed for the cerebral form of the disease and is not indicated in males
without evidence of active cerebral disease (detected by MRI). Active research
programs are investigating biomarkers of neurologic dysfunction and other
strategies (including reduced-intensity conditioning) to improve
transplantation outcomes.10
Gene therapy using a lentiviral vector in combination with hematopoietic
stem cell transplantation was performed in 17 boys with early cerebral X-linked
adrenoleukodystrophy who did not have a suitable match for transplant.11
Although MRI disease progression was evident in some participants 12 to
18 months posttransplant, 14 out of 17 participants had no (or minimal) clinical
symptoms at a median of 29.4 months posttransplant. One participant had a
seizure; thus, he did not meet predefined criteria for minimal disease progression
but otherwise did well. Two participants demonstrated disease progression, one
within 2 weeks of transplant, indicating a rapidly progressive course. The other
participant withdrew from the study and underwent an allogeneic transplant,
later dying from complications related to a viral infection. In summary, males
with early cerebral disease should be referred for an urgent hematopoietic stem
cell transplant; gene therapy in combination with transplant may be an option in
the future for those individuals without a sibling match. Males diagnosed
through newborn screening undergo serial neurologic examinations and imaging
136 FEBRUARY 2018
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
protocols as toddlers to identify cerebral disease early, which enables prompt KEY POINT
treatment and improved outcomes.
● Infantile Krabbe disease
Aside from transplant, dietary therapy has been explored for X-linked should be considered in a
adrenoleukodystrophy, with a reduction in fat intake and the use of Lorenzo’s oil child 6 months of age or
(4:1 mix of glyceryl trioleate to glyceryl trierucate). While this combination may younger with irritability,
correct the measurement of very-long-chain fatty acids in the blood, reduction in sterile pyrexia, and
elevated CSF protein. Other
dietary fat and supplementation with Lorenzo’s oil have not been effective in symptoms in this age group
alleviating symptoms of cerebral X-linked adrenoleukodystrophy (or other include extremity stiffness,
symptoms) once present.12 fisted hands, and
decreased oral intake.
GLOBOID CELL LEUKODYSTROPHY (KRABBE DISEASE)
Globoid cell leukodystrophy, or Krabbe disease, is an autosomal recessive lysosomal
storage disorder caused by mutations in GALC on chromosome 14q31. GALC
encodes the enzyme galactosylceramidase, which is essential in the degradation
of lipids (galactosylceramide and psychosine) during myelin turnover.
Clinical Symptoms
Four classic phenotypes are associated with galactosylceramidase deficiency
(TABLE 6-3). The most common is the early-onset infantile phenotype (85% to
90%), which presents prior to 6 months of age, with irritability, stiffness, arrest
Krabbe Disease (Globoid Cell Leukodystrophy) Phenotypes and Frequencies TABLE 6-3
Phenotype Description Frequency
Early-onset infantile Onset prior to 6 months, regression occurs over several months 85–90%a
Stage 1: Irritability; failure to thrive (decreased intake, vomiting), developmental arrest
and regression (decreased head control, loss of smiling); hypersensitivity to auditory,
tactile, or visual stimuli; stiffness and clenched fists; episodes of sterile hyperpyrexia;
seizures
Stage 2: Rapid neurologic regression with arm flexion, leg extension, and scissoring;
opisthotonos; seizures; hyperreflexia; optic atrophy; and abnormal pupillary responses
Stage 3: The “burnt-out” stage, characterized by decerebrate posturing, blindness,
deafness, and the absence of voluntary movement
Late-onset infantile Onset between 6 months and 3 years of age; early milestones are achieved, followed by 10–15%
psychomotor regression, notably affecting gross motor skills; ataxia, stiffness, and visual
impairment; disease progression is slower than the early-onset infantile form
Juvenile onset Onset between 3 and 8 years of age; initial presentation is visual impairment, followed Unknown
by hemiparesis and ataxia; initial symptoms occur rapidly, followed by a plateau or slow
progression with improved survival over other forms
Adult onset Heterogeneous group combining those who are asymptomatic in childhood and Unknown
develop neurologic symptoms (such as spastic paraparesis) as adults (typically older
than 20 years of age) and those who are mildly symptomatic in childhood but for whom
the disease was not recognized
a
Newborn screening results and longitudinal data will impact our understanding of GALC mutations, galactosylceramidase enzyme activity, and
the frequency of these clinical phenotypes in the future.
CONTINUUMJOURNAL.COM 137
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
LEUKODYSTROPHIES
of development, and failure to
thrive.13 Older patients generally
present with spasticity,
paraparesis, visual impairment,
and ataxia (TABLE 6-3). A
peripheral neuropathy is also
present in Krabbe disease, and a
loss of reflexes may be the
presenting symptom.14 The
clinical course is not determined
by the genotype; however, a few
variants have some predictive
value. A 30-kb deletion of GALC
(either homozygous or in
combination with another severe
variant) causes early-onset
infantile disease.
FIGURE 6-2
Krabbe disease. Axial T2-weighted MRI Neuroimaging
demonstrates confluent diffuse T2 high signal Krabbe disease is a demyelinating
involving the central white matter and corpus disorder (T1 hypointense) with
callosum. The white matter has a striated
and speckled appearance. confluent T2 hyperintensities
with a periventricular or
parietooccipital predominance
(FIGURE 6-2). 2 Of note, MRI abnormalities in early-onset infantile disease are
not always appreciated because of the myelination pattern of a newborn. For
example, bilateral symmetric T2-weighted hyperintensity is present in the
dentate hilum, surrounded by hypointensity in the peridentate area and
hyperintensity in the cerebellar white matter.15 This pattern may not be
appreciated as it is similar to the normal variability of these structures present in
a newborn.
Diagnosis
The diagnosis of Krabbe disease is confirmed by low galactosylceramidase
(0% to 5% of normal values) in white blood cells or cultured fibroblasts,
followed by GALC sequencing for mutations. Of note, deletions (and
duplications) are not detected through sequencing; therefore, anyone
presenting with clinical features consistent with Krabbe disease for whom a
heterozygous mutation is detected should have further testing for a deletion.
For an irritable infant presenting to medical attention, a lumbar puncture may
be performed to exclude infection or other etiologies. While not specific for
Krabbe disease, CSF protein is frequently elevated in early-onset infantile
disease (with a normal CSF cell count).16
Newborn screening for Krabbe disease is under way in several US states
to identify early-onset infantile disease for possible treatment.
Galactosylceramidase activity, which is measured in dried blood spots using
various methodologies, is typically employed as an initial screen; however,
significant overlap exists between affected patients, carriers, and healthy
individuals. Moreover, the lack of genotype-phenotype correlations precludes
the ability to accurately predict the onset of neurologic symptoms in an affected
138 FEBRUARY 2018
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
individual; thus later-onset forms of the disease are identified through newborn KEY POINT
screening.17 As they may be asymptomatic for many years, these patients do
● The biochemical
not need an emergent transplant in the neonatal period. Some states use abnormality in Krabbe
psychosine as a second-tier test as elevated levels correlate with early-onset disease is an abnormal
infantile disease.18–20 Alternatively, some laboratories screen for the 30-kb galactosylceramidase level
deletion in GALC to identify early-onset infantile disease. In a child with a (typically 0% to 5% of
normal values) in white
positive newborn screen for Krabbe disease, the diagnosis is confirmed by low blood cells or cultured
galactosylceramidase followed by GALC sequencing/deletion analysis. fibroblasts.
Disease-specific Therapy
Hematopoietic stem cell transplantation may alter the neurologic progression in
asymptomatic early-onset infantile Krabbe disease, but the overall impact
on morbidity in this disorder remains in question. The outcomes of umbilical
cord blood transplantation for 11 children with asymptomatic disease (identified
prenatally or in the neonatal period through previously affected siblings) were
compared to 14 children diagnosed between 4 and 9 months of age.21 In the
asymptomatic group, the transplant occurred between 12 and 44 days of life,
compared to between 142 and 352 days in the symptomatic group. Survival was
100% in the asymptomatic group at a median of 36 months compared to 43%
of the symptomatic group (P=.01). In the asymptomatic group, brain MRIs
showed normal maturation of myelin, with decreased hyperintensity of affected
areas. In addition, transplant outcomes were significantly improved for the
asymptomatic children with respect to gross motor, fine motor, language, and
cognitive function. Many achieved developmental milestones; however, all
ultimately developed gross motor impairments of varying degrees (spasticity,
gait abnormalities, or needing assistance to stand or walk). In comparison, the
symptomatic children who survived lost all gross and fine motor skills. The
outcomes for many of these children were included in a subsequent publication
with longitudinal follow-up data (range 4 to 15 years). Of the 18 children with
Krabbe disease who were transplanted within 7 weeks of life, five ultimately
died (three died of transplant-related complications, one died of a surgical
complication unrelated to Krabbe disease, and one died of disease progression).
Surviving children had variable deficits in gross motor function, neurocognitive
skills, language, and adaptive behavior.22 These results, while encouraging for
early transplantation, suggest that additional modalities of therapy will likely be
necessary in Krabbe disease to achieve symptomatic control.
The state of New York has published its experience in screening over 2 million
infants for Krabbe disease and other disorders as part of its newborn screening
program since 2006.17 On the initial screen, approximately 10,200 infants were
identified with galactosylceramidase activity less than or equal to 20% of normal
activity. On repeat testing, 620 newborns who had galactosylceramidase activity
less than or equal to 12% of normal subsequently underwent genetic sequencing,
and 348 infants had at least one pathogenic GALC mutation. Ultimately, 14
children had very low galactosylceramidase activity (0 nmol/h/mg to
0.15 nmol/h/mg protein, considered high-risk), but only five were confirmed
through further evaluations (MRI, lumbar puncture, nerve conduction studies,
and brainstem auditory evoked response) to have early-onset infantile Krabbe
disease. One family declined treatment, and that child is deceased. Four of the
patients underwent umbilical cord blood transplantation: two died of
transplant-related complications, one is unable to walk independently and has
CONTINUUMJOURNAL.COM 139
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
LEUKODYSTROPHIES
KEY POINTS failure to thrive but receptive language appropriate for age, and one has severe
delays and failure to thrive.
● Metachromatic
leukodystrophy should be For older individuals, the assessment of transplantation outcomes is
considered in a toddler with challenged by differences in phenotypes, unpredictable disease onset, and
regression in gross motor variability in disease duration. Transplantation does not improve peripheral
skills, a peripheral nervous system disease for most patients.
neuropathy, or gall
bladder polyps.
METACHROMATIC LEUKODYSTROPHY
● Gall bladder disease Metachromatic leukodystrophy is also an autosomal recessive lysosomal storage
should be considered in disorder caused by an enzyme deficiency of arylsulfatase A, which is encoded on
patients with metachromatic
leukodystrophy who
the ARSA gene on chromosome 22q13.3-qter. Sulfatides accumulate in the central
experience feeding and peripheral nervous systems, kidneys, testes, and visceral organs (gall bladder).
intolerance.
Clinical Symptoms
●Arylsulfatase A
pseudodeficiency is The clinical phenotypes and frequencies of metachromatic leukodystrophy are
common; therefore, the presented in TABLE 6-4. Of note, the peripheral neuropathy may present prior
diagnosis of metachromatic to the onset of speech or other CNS abnormalities (CASE 6-2). In fact, several
leukodystrophy is confirmed patients with metachromatic leukodystrophy have been diagnosed with other
by low arylsulfatase A
activity along with an
disorders (eg, Guillain-Barré or spastic diplegia) because of the perceived
elevation in the urinary absence of CNS disease (clinically and radiographically).23,24 Any child with
excretion of sulfatides. normal early milestones followed by a decline in motor skills at any age should be
evaluated for metachromatic leukodystrophy through leukocytes and
urine sulfatides.
Unique to metachromatic leukodystrophy, the gall bladder is also involved,
likely due to sulfatide accumulation and irritation of the epithelium.25 Gall
bladder disease may be asymptomatic, detected through an ultrasound revealing
a polyp or thickening of the wall, or cause abdominal pain, vomiting, or biliary
colic. Asymptomatic gall bladder polyps were detected incidentally in two
patients (undergoing trauma evaluations) who later exhibited neurologic
symptoms 12 to 15 months after the polyps were detected.26,27 Neuroimaging was
available (as part of the trauma evaluation) for one of these patients, and the
TABLE 6-4 Metachromatic Leukodystrophy Phenotypes and Frequencies
Phenotype Description Frequency
Late infantile Onset <30 months; early milestones are often achieved, followed by regression in gross motor 50–60%
skills (especially gait) and speech; weakness and hypotonia evolve to spasticity, tonic spasms,
and decerebrate posturing; a peripheral neuropathy may be present prior to central nervous
system symptoms
Juvenile Onset between 30 months and puberty; early milestones are achieved, followed by 20–30%
psychomotor regression, mental status changes, and behavioral disturbances; declining
school performance, personality changes, or gait abnormalities may prompt medical attention
Adult Onset >12–14 years; psychiatric manifestations (such as behavioral changes and emotional 15–20%
lability or substance abuse) may lead to diagnoses of bipolar disorder and dementia prior
to the recognition of motor and cognitive symptoms; other adults may present with a
peripheral neuropathy
140 FEBRUARY 2018
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
brain MRI was normal at the time of the trauma. Fifteen months later, the MRI
was repeated because of regression in motor skills and was consistent with
metachromatic leukodystrophy.26
Neuroimaging
Metachromatic leukodystrophy is a demyelinating disorder (T1 hypointense)
with confluent T2 hyperintensities surrounding the frontal and parietal
periventricular white matter (FIGURE 6-3). 2 In patients with diffuse disease,
a striped (tigroid) appearance may be seen, in which normal white matter
alternates with hyperintense lesions (also seen in other leukodystrophies, such
as Pelizaeus-Merzbacher disease).28
Diagnosis
The diagnosis is suspected if a low arylsulfatase A level (less than 10% of normal
values) is detected in white blood cells or cultured fibroblasts; however,
arylsulfatase A pseudodeficiency is relatively common. Individuals with
arylsulfatase A pseudodeficiency have arylsulfatase A levels ranging from 5% to
20% of normal values without clinical or radiographic disease. Therefore, a
diagnosis of metachromatic leukodystrophy in individuals with low arylsulfatase A
must be confirmed by the detection of elevated sulfatides in the urine and ARSA
sequencing for mutations.29
A full-term infant boy was noted to have slow development of motor CASE 6-2
milestones. He walked around 18 months but continued to be unsteady.
He was referred for early intervention, and hypotonia was suspected. His
speech and cognition were normal for his age. At 2 years, he had
persistent gait unsteadiness and was referred to neurology. An EMG was
consistent with a demyelinating polyneuropathy. Subsequently, his gait
further regressed and a walker was needed. He could not push up into a
prone position or crawl. His speech regressed with decreased speech
production. His examination was notable for increased tone in the lower
extremities, decreased dorsiflexion, and absent patellar reflexes. He was
only able to walk with assistance. Brain MRI was performed at 2 years,
7 months, and diffuse T2 hyperintensities were seen throughout the white
matter. Arylsulfatase A level in leukocytes was low, and urine sulfatides
were elevated.
This case illustrates a delay in the diagnosis of metachromatic leukodystrophy. COMMENT
Late infantile metachromatic leukodystrophy typically presents between 1 and
3 years of age with gross motor delay or regression. In this patient, a peripheral
neuropathy, rather than symptoms localizing to the central nervous system,
was the initial manifestation of disease. Metachromatic leukodystrophy
should be considered in any child presenting with a peripheral neuropathy.
As the typical central nervous system involvement may develop later,
brain MRI findings may be subtle or unremarkable. Biochemical testing
(arylsulfatase A, urine sulfatides) is the diagnostic test of choice.
CONTINUUMJOURNAL.COM 141
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
LEUKODYSTROPHIES
A high index of suspicion for
metachromatic leukodystrophy
must exist for children presenting
with a peripheral neuropathy or
gall bladder abnormality in the
absence of other neurologic
features. The MRI may not reveal
pathology early in the disease
course; therefore, a normal MRI is
not sufficient to exclude
metachromatic leukodystrophy.
The diagnosis of metachromatic
leukodystrophy should be
excluded through a normal
arylsulfatase A level and the
absence of urinary sulfatides.
Legislation mandating newborn
screening for metachromatic
leukodystrophy has not been
FIGURE 6-3
Metachromatic leukodystrophy. Axial MRI in approved at the state or federal
metachromatic leukodystrophy demonstrates level. The required methodology
confluent diffuse T2 hyperintense signal involving for metachromatic leukodystrophy
the central white matter and corpus callosum, similar
newborn screening is still under
to Krabbe disease. The striped “tigroid” appearance
is not specific for metachromatic leukodystrophy development30 and is further
but characteristic of leukodystrophies. challenged by the frequency of
arylsulfatase A pseudodeficiency
in the population.
Disease-specific Therapy
Hematopoietic stem cell transplantation may be beneficial in asymptomatic
children with metachromatic leukodystrophy (diagnosed because of an affected
sibling) or early symptomatic juvenile-onset disease. Cohorts have included
those receiving bone marrow–derived cells,31 umbilical cord blood,32 or both.33
For late-infantile disease, four of ten in one cohort32 and two of four in a different
cohort died.33 Of the six children who died, five of the deaths occurred within the
first year posttransplant. One patient in each group was asymptomatic at the
time of transplant. In patients with juvenile disease, the 5-year survival
posttransplant is estimated to be 59% (N = 27),33 79% (N = 24),31 and 82.4%
(N = 17)32 across various studies. While disease stability may occur, many
patients experience decline posttransplant with respect to MRI involvement,
gross motor function, cognitive skills, nerve conduction velocities, and other
metrics, although outcomes are frequently better compared to affected siblings
or natural history cohorts.32,33
In a phase 1/2 clinical trial, gene therapy in combination with autologous
hematopoietic stem cell transplantation was performed in 20 children with
metachromatic leukodystrophy (asymptomatic late-onset infantile disease,
juvenile disease, and early-onset juvenile disease [less than 6 months from
symptom onset]).34,35 For this open-label study, hematopoietic stem cells were
removed from the patient, transduced with a lentiviral vector encoding ARSA
ex vivo, and returned to the patient after myeloablative conditioning. Two
142 FEBRUARY 2018
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
publications describe the outcomes of the first nine patients enrolled in the KEY POINTS
study.34,35 The onset of MRI abnormalities in asymptomatic individuals was
● Aicardi-Goutières
delayed compared to sibling controls, and many showed age-expected gains syndrome should be
in gross motor function and cognition. However, not all children remained considered in young
asymptomatic, and some disease progression occurred. The unique aspect of children with developmental
regression, acquired
this therapy is the ability of the transduced cells to make supranormal levels of
microcephaly, spasticity,
arylsulfatase A, which was detected as early as 1 month in blood and 6 months in and dystonia. Chilblains,
CSF. Data from the trial are still being analyzed to determine the future role of glaucoma, cardiomyopathy,
gene therapy for this disorder. stroke, and comorbid
autoimmune conditions are
present, with variability in
AICARDI-GOUTIÈRES SYNDROME the presence and frequency
of these symptoms by
Aicardi-Goutières syndrome is an inflammatory disorder caused by mutations genetic mutation.
in any one of seven genes (TREX1, RNASEH2A, RNASEH2B, RNASEH2C,
SAMHD1, ADAR, or IFIH1), all of which encode proteins involved in nucleic ● In Aicardi-Goutières
acid metabolism and signaling.36 The pathophysiology involves the accumulation syndrome, a CT scan may
be performed to
of nucleic acids (for all genes except ADAR and IFIH1) that activate the innate demonstrate calcium
immune response with increased expression of type I interferon–stimulated deposits in the basal
genes. The symptoms and imaging features of Aicardi-Goutières syndrome ganglia and other areas of
mimic TORCH (toxoplasmosis, other infections, rubella, cytomegalovirus the brain.
infection, and herpes simplex) and other in utero infections.
● Patients with
Aicardi-Goutières
Clinical Symptoms syndrome may have a CSF
lymphocytic pleocytosis,
In 1984, Jean Aicardi and Françoise Goutières described the syndrome that elevated interferon alfa, or
now bears their names.37 Among five families, eight infants had a progressive elevated neopterin or
encephalopathy presenting shortly after birth with feeding difficulties or biopterin.
manifesting as subacute neurologic deterioration after a period of normal
development, typically before 1 year of age. Ultimately, the affected children
developed appendicular spasticity and dystonia, truncal hypotonia, and acquired
microcephaly. These children were all found to have basal ganglia calcifications
on head CT and a persistently elevated CSF white blood cell count (lymphocytic
predominance) on serial measurements. Since the initial description, the clinical
phenotypes (TABLE 6-5) have evolved.
In addition to the neurologic manifestations, other symptoms provide clues to
the diagnosis of Aicardi-Goutières syndrome, and some trends in clinical
manifestations based on genetic mutations have been identified among 374
patients with Aicardi-Goutières syndrome.36 Chilblains, which are small purple-red
or white blistering lesions on the toes, fingers, helix, or pressure areas, occur in
approximately one-third of all patients with Aicardi-Goutières syndrome
(FIGURE 6-4 38 ). 39,40 They are most common after 1 year of age and increase in
cold weather.41 Chilblains have been reported with mutations of each of the seven
genes; however, they most frequently occur in children with SAMHD1 mutations
(approximately 54%, or 26 of 48 children) and rarely occur in ADAR mutations.
Glaucoma also occurs in approximately 20% of children (10 of 48) with SAMHD1
mutations, typically in the first 6 months of life, although it can occur at an older
age. Stroke due to large vessel disease has also been reported in SAMHD1
mutations (9 of 9 children). While infrequent, infantile-onset hypertrophic
cardiomyopathy may occur, especially in infants with a TREX1 mutation (9 of 12
infants with cardiomyopathy had mutations in the TREX1 gene). These
relationships may inform genetic testing of single genes but should not be used to
CONTINUUMJOURNAL.COM 143
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
LEUKODYSTROPHIES
exclude a diagnosis of Aicardi-Goutières syndrome, as overlap of genetic
syndromes does occur.
Although rare, other autoimmune diseases, including hypothyroidism,
diabetes mellitus, autoimmune gastritis, autoimmune hepatitis, panniculitis,
Crohn disease, systemic lupus erythematosus, and antiphospholipid antibody
syndrome, have been described in patients with Aicardi-Goutières syndrome.
Neuroimaging
The pathognomonic feature of Aicardi-Goutières syndrome on neuroimagingis
intracerebral calcifications, which are present in approximately 90% of
individuals (N = 121) using MRI (FIGURE 6-5) and CT.42 The calcium deposits
are frequently present in the basal ganglia, deep white matter, thalamus, and
dentate nuclei of the cerebellum. They can be visualized on MRI using
T1-weighted, gradient recalled echo (GRE), or susceptibility-weighted images;
however, a head CT may be necessary to confirm their presence. The cerebral
white matter is also affected (present in 120 of 121 children), with T2
hyperintensities or white matter rarefaction with a frontotemporal predominance or
diffuse involvement.42 In the same study, one patient had isolated bilateral striatal
necrosis, which has been reported in ADAR1 mutations.43 Other distinguishing MRI
features in infants with Aicardi-Goutières syndrome (median age 0.7 months)
include cerebral atrophy (with ventricular enlargement), temporal lobe swelling,
temporal horn dilation, and temporal cysts.44 A normal brain MRI and nonspecific
white matter changes have been reported in children with severe dystonia (but
preserved cognition) who have mutations in various Aicardi-Goutières syndrome
genes. As such, a normal or nondiagnostic brain MRI does not exclude the
diagnosis of Aicardi-Goutières syndrome.
Diagnosis
A diagnosis of Aicardi-Goutières syndrome should be considered in young
children with the clinical or radiographic features described. A lumbar puncture
TABLE 6-5 Aicardi-Goutières Syndrome Phenotypes and Frequenciesa
Phenotype Description Frequency
Prenatal Presents at birth with poor feeding, irritability, abnormal tone and movements, seizures; 11.4%
onset thrombocytopenia and hepatosplenomegaly at birth support the prenatal onset
Perinatal Presents at birth with similar features to the prenatal onset form but without the systemic 11.4%
involvement
Infancy Onset <1 year of age; may meet early milestones, followed by psychomotor regression, spasticity, 68.6%
dystonia, and acquired microcephaly; seizures and visual impairment may also occur
Childhood Variable symptoms and disease onset, although the oldest known age at symptom onset is 8.6%
5 years of age (subacute dystonia); glaucoma developed in a 6-year-old patient with
known disease
a
Data from Crow YJ, et al, Am J Med Genet.36
144 FEBRUARY 2018
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
may provide supportive evidence. The KEY POINT
CSF may reveal a lymphocytic pleocytosis.
● Infants with persistent
Elevated CSF neopterin and biopterin and jaundice or chronic diarrhea
reduced folate have been reported in and children with bilateral
patients with normal CSF profiles cataracts should be tested
(including cell counts, interferon, and for cerebrotendinous
xanthomatosis, even in the
interleukin levels).45 absence of neurologic
symptoms, through
Disease-specific Therapy measurement of serum
cholestanol and urine and
No therapies are currently approved for
serum bile alcohols.
Aicardi-Goutières syndrome; however,
active research studies and clinical trials
are investigating treatments that
target the interferon pathway and
autoantibody production in children with
Aicardi-Goutières syndrome.46
CEREBROTENDINOUS XANTHOMATOSIS
Cerebrotendinous xanthomatosis is an
autosomal recessive disorder caused by
mutations in the CYP27A1 gene, which
encodes sterol 27-hydroxylase. The
deficiency of this enzyme results in the
accumulation of cholesterol and cholestanol
and the formation of xanthomas in
tendons, CNS, skin, and other organs.
Clinical Symptoms
The earliest manifestation of
cerebrotendinous xanthomatosis is
neonatal cholestatic jaundice,47 which
persists beyond the first week of life with
chronic diarrhea and is associated with FIGURE 6-4
elevated transaminases and bilirubin. In Chilblains in Aicardi-Goutières
syndrome. Chilblains are vasculitis
childhood and adolescence, juvenile lesions (purple-red discolorations) of
bilateral cataracts occur, but they are often the skin typically located on the fingers,
thought to be “idiopathic,” and most toes, or other dependent areas (such
clinicians do not appreciate the possibility as elbows or earlobes); necrosis of these
lesions can occur.
of cerebrotendinous xanthomatosis. Reprinted with permission from Abe J, et al,
Xanthomas occur in the Achilles and other Rheumatology (Oxford).38 © 2013 The Authors.
tendons, especially over extensor surfaces,
in adolescence or adulthood. They can also
develop in the brain, lungs, and bones. The neurologic symptoms develop
predominantly in adulthood, with cognitive impairment, ataxia, and pyramidal
features (such as spasticity). Psychiatric symptoms can also occur.
Neuroimaging
The cerebellum is preferentially affected in cerebrotendinous xanthomatosis;
notably, T1 hypointense and T2 hyperintense lesions are seen in the bilateral
CONTINUUMJOURNAL.COM 145
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
LEUKODYSTROPHIES
dentate nuclei as well as T2
hyperintensities in the cerebellar
white matter.48 Cerebellar and
cerebral atrophy are also present.
The periventricular white matter,
globus pallidus, posterior limb of
the internal capsule, substantia
nigra, and cerebral peduncles
may also be affected.49
Diagnosis
A high index of suspicion is
needed for the diagnosis of
cerebrotendinous xanthomatosis
as serum cholesterol levels and
hepatic function testing are
normal. The diagnosis is
confirmed through elevated
FIGURE 6-5
Aicardi-Goutières syndrome. Axial T1-weighted
serum cholestanol, which
MRI demonstrates hyperintensity in the bilateral is 5 to 10 times normal values, and
basal ganglia, predominantly the putamen (arrows), the excretion of bile alcohols in
representing mineralization in a patient with the urine and serum.
Aicardi-Goutières syndrome.
Testing for cerebrotendinous
xanthomatosis has not been
incorporated into newborn
screening programs in the United States; however, a methodology
to detect a bile acid precursor in dried blood spots has successfully differentiated
infants with cerebrotendinous xanthomatosis from unaffected controls.50 In
Victoria, Australia, urine bile alcohols have been added to a urine metabolic
screening panel (including amino acids, organic acids, and others) and enabled
the diagnosis of four patients with cerebrotendinous xanthomatosis among
23,000 urine samples.51,52
Disease-specific Therapy
Chenodeoxycholic acid inhibits cholesterol and cholestanol synthesis by
downregulating CYP7A transcription.53 Treatment with chenodeoxycholic acid
does not improve neurologic deficits once present but, if started early, prevents
neurologic deterioration. For example, patients whose treatment with
chenodeoxycholic acid began before 25 years of age (N = 10) had improved
ambulation with significantly less pyramidal involvement and fewer cerebellar
deficits compared to those who started after 25 years of age (N = 6).54 Dysarthria
was not noted in any of the treated younger patients. Cholic acid is FDA approved
for children and adults with cerebrotendinous xanthomatosis and has fewer side
effects than chenodeoxycholic acid, especially in infants and children, whose
diarrhea worsens on chenodeoxycholic acid.55
TRENDS
Newborn screening programs for leukodystrophies are being implemented
for Krabbe disease and X-linked adrenoleukodystrophy, while testing for
146 FEBRUARY 2018
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
metachromatic leukodystrophy and cerebrotendinous xanthomatosis are under KEY POINT
development. Such programs are providing new challenges for disease prediction
● Cholic acid is a US Food
models. Genotype-phenotype correlations for many disorders do not predict age and Drug Administration–
of onset or functional decline; therefore, it is not clear when to introduce a approved treatment for
therapy, such as hematopoietic stem cell transplantation, or how to determine its cerebrotendinous
efficacy. Gene therapy trials in some of the leukodystrophies provide hope for xanthomatosis and, when
initiated early, delays the
families; however, more data are needed on their efficacy and safety profiles. onset of neurologic
Novel therapeutic strategies are needed for peripheral nervous system symptoms.
involvement of leukodystrophies such as Krabbe disease and metachromatic
leukodystrophy, as hematopoietic stem cell transplantation has a limited benefit
in the treatment of these symptoms.
CONCLUSION
The leukodystrophies are a group of complex disorders with variable
clinical features and presentations by age. Many of these disorders have
extra-CNS manifestations before the onset of neurologic symptoms
or MRI abnormalities, such as adrenal insufficiency in X-linked
adrenoleukodystrophy or chronic diarrhea and cataracts in cerebrotendinous
xanthomatosis. Both metachromatic leukodystrophy and Krabbe disease can
present with a peripheral neuropathy, and, in such cases, the brain MRI is
often normal or reveals subtle findings. Therefore, knowledge about the
typical disease presentations and a high index of suspicion are crucial to
confirming the diagnosis before the worsening of CNS symptoms and disease
progression on MRI. Biochemical testing, such as enzyme levels in Krabbe
disease and metachromatic leukodystrophy; very-long-chain fatty acids in
X-linked adrenoleukodystrophy; CSF cell counts, neopterin, and biopterin in
Aicardi-Goutières syndrome; and serum cholestanol in cerebrotendinous
xanthomatosis, are the tests of choice to screen suspected individuals for
these disorders.
ACKNOWLEDGMENT
This work was supported by a career training grant (K23NS069806) from the
National Institutes of Health.
REFERENCES
1 Vanderver A, Prust M, Tonduti D, et al. Case 4 Kemp S, Pujol A, Waterham HR, et al. ABCD1
definition and classification of leukodystrophies and mutations and the X-linked adrenoleukodystrophy
leukoencephalopathies. Mol Genet Metab 2015;114(4): mutation database: role in diagnosis and clinical
494–500. doi:10.1016/j.ymgme.2015.01.006. correlations. Hum Mutat 2001;18(6):499–515.
doi:10.1002/humu.1227.
2 Schiffmann R, van der Knaap MS. Invited article: an
MRI-based approach to the diagnosis of white 5 Loes D, Hite S, Moser H, et al. Adrenoleukodystrophy: a
matter disorders. Neurology 2009;72(8):750–759. scoring method for brain MR observations. AJNR
doi:10.1212/01.wnl.0000343049.00540.c8. Am J Neuroradiol 1994;15(9):1761–1766.
3 Moser HW. Adrenoleukodystrophy: phenotype, 6 Loes D, Fatemi A, Melhem E, et al. Analysis of MRI
genetics, pathogenesis and therapy. Brain patterns aids prediction of progression in X-linked
1997;120(8):1485–1508. doi:10.1093/ adrenoleukodystrophy. Neurology 2003;61(3):
brain/120.8.1485. 369–374. doi:10.1212/01.WNL.0000079050.91337.83.
CONTINUUMJOURNAL.COM 147
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
LEUKODYSTROPHIES
7 Hubbard WC, Moser AB, Tortorelli S, et al. Combined 21 Escolar ML, Poe MD, Provenzale JM, et al.
liquid chromatography-tandem mass spectrometry Transplantation of umbilical-cord blood in babies
as an analytical method for high throughput with Infantile Krabbe’s disease. N Engl J Med 2005;
screening for X-linked adrenoleukodystrophy and 352(20):2069–2081. doi:10.1056/NEJMoa042604.
other peroxisomal disorders: preliminary findings.
22 Wright MD, Poe MD, DeRenzo A, et al. Developmental
Mol Genet Metab 2006;89(1–2):185–187. doi:10.1016/
outcomes of cord blood transplantation for Krabbe
j.ymgme.2006.05.001.
disease. Neurology 2017;89(13):1–8. doi:10.1212/
8 Hubbard WC, Moser AB, Liu AC, et al. Newborn WNL.0000000000004418.
screening for X-linked adrenoleukodystrophy 23 Cruz Martinez A, Ferrer MT, Fueyo E, Galdos AL.
(X-ALD): validation of a combined liquid Peripheral neuropathy detected on electrophysiological
chromatography–tandem mass spectrometric study as first manifestation of metachromatic
(LC–MS/MS) method. Mol Genet Metab 2009; leucodystrophy in infancy. J Neurol Neurosurg
97(3):212–220. doi:10.1016/j.ymgme.2009.03.010. Psychiatry 1975;38(2): 169–174. doi:10.1136/jnnp.38.2.169.
9 Turgeon CT, Moser AB, Mørkrid L, et al. Streamlined 24 Haberlandt E, Scholl-Bürgi S, Neuberger J, et al.
determination of lysophosphatidylcholines in dried Peripheral neuropathy as the sole initial finding
blood spots for newborn screening of X-linked in three children with infantile metachromatic
adrenoleukodystrophy. Mol Genet Metab 2015;114(1): leukodystrophy. Eur J Paediatr Neurol 13(3):257–260.
46–50. doi:10.1016/j.ymgme.2014.11.013. doi:10.1016/j.ejpn.2008.04.011.
10 Tolar J, Orchard P, Bjoraker K, et al. N-acetyl-L-cysteine 25 van Rappard DF, Bugiani M, Boelens JJ, et al.
improves outcome of advanced cerebral Gallbladder and the risk of polyps and carcinoma in
adrenoleukodystrophy. Bone Marrow Transplant metachromatic leukodystrophy. Neurology 2016;
2007;39(4):211–215. doi:10.1038/sj.bmt.1705571. 87(1):103–111. doi:10.1212/WNL.0000000000002811.
11 Eichler F, Duncan C, Musolino PL, et al. 26 Agarwal A, Shipman PJ. Gallbladder polyposis in
Hematopoietic stem-cell gene therapy for cerebral metachromatic leukodystrophy. Pediatr Radiol 2013;
adrenoleukodystrophy. N Engl J Med 2017;377(17): 43(5):631–633. doi:10.1007/s00247-012-2523-y.
1630–1638. doi:10.1056/NEJMoa1700554.
27 Shah S, Ghosh S, Nagarajan L. Leukodystrophy:
12 Moser HW, Raymond G V, Lu S-E, et al. Follow-up of when gallbladder offers a clue to diagnosis. Pediatr
89 asymptomatic patients with adrenoleukodystrophy Neurol 2013;49(1):68–69. doi:10.1016/j.pediatrneurol.
treated with Lorenzo’s oil. Arch Neurol 2005;62(7): 2013.03.019.
1073–1080. doi:10.1001/archneur.62.7.1073.
28 Eichler F, Grodd W, Grant E, et al. Metachromatic
13 Wenger DA. Krabbe disease. In: Pagon RA, Adam MP, leukodystrophy: a scoring system for brain MR
Ardinger HH, et al, eds. GeneReviews. Seattle, WA: imaging observations. AJNR Am J Neuroradiol 2009;
University of Washington, Seattle, 2011: 30(10):1893–1897. doi:10.3174/ajnr.A1739.
1993–2017. ncbi.nlm.nih.gov/pubmed/20301416.
29 Fluharty AL. Arylsulfatase A deficiency. In: Pagon RA,
Accessed December 4, 2017.
Adam MP, Ardinger HH, et al, eds. GeneReviews.
14 Korn-Lubetzki I, Dor-Wollman T, Soffer D, et al. Seattle, WA: University of Washington, Seattle; 2014:
Early peripheral nervous system manifestations of 1993–2017. ncbi.nlm.nih.gov/pubmed/20301309.
infantile Krabbe disease. Pediatr Neurol 2003;28(2): Accessed December 4, 2017.
115–118. doi:10.1016/S0887-8994(02)00489-7.
30 Spacil Z, Babu Kumar A, Liao HC, et al. Sulfatide
15 Abdelhalim AN, Alberico RA, Barczykowski AL, analysis by mass spectrometry for screening of
Duffner PK. Patterns of magnetic resonance imaging metachromatic leukodystrophy in dried blood and
abnormalities in symptomatic patients with urine samples. Clin Chem 2016;62(1):279–286.
Krabbe disease correspond to phenotype. doi:10.1373/clinchem.2015.245159.
Pediatr Neurol 2014;50(2):127–134. doi:10.1016/
31 Groeschel S, Kühl J-S, Bley AE, et al. Long-term
j.pediatrneurol.2013.10.001.
outcome of allogeneic hematopoietic stem cell
16 Duffner PK, Barczykowski A, Kay DM, et al. Later onset transplantation in patients with juvenile metachromatic
phenotypes of Krabbe disease: results of the leukodystrophy compared with nontransplanted
world-wide registry. Pediatr Neurol 2012;46(5): control patients. JAMA Neurol 2016;73(9):1133–1140.
298–306. doi:10.1016/j.pediatrneurol.2012.02.023. doi:10.1001/jamaneurol.2016.2067.
17 Wasserstein MP, Andriola M, Arnold G, et al. Clinical 32 Martin HR, Poe MD, Provenzale JM, et al.
outcomes of children with abnormal newborn Neurodevelopmental outcomes of umbilical
screening results for Krabbe disease in New York cord blood transplantation in metachromatic
State. Genet Med 2016;18(12):1235–1243. doi:10.1038/ leukodystrophy. Biol Blood Marrow Transplant
gim.2016.35. 2013;19(4):616–624. doi:10.1016/j.bbmt.2013.01.010.
18 Chuang WL, Pacheco J, Zhang XK, et al. 33 Boucher AA, Miller W, Shanley R, et al. Long-term
Determination of psychosine concentration in dried outcomes after allogeneic hematopoietic
blood spots from newborns that were identified stem celltransplantation for metachromatic
via newborn screening to be at risk for Krabbe leukodystrophy: the largest single-institution cohort
disease. Clin Chim Acta 2013;419:73–76. doi:10.1016/ report. OrphanetJ Rare Dis 2015;10(1):94. doi:10.1186/
j.cca.2013.01.017. s13023-015-0313-y.
19 Turgeon CT, Orsini JJ, Sanders KA, et al. Measurement 34 Biffi A, Montini E, Lorioli L, et al. Lentiviral
of psychosine in dried blood spots–a possible hematopoietic stem cell gene therapy benefits
improvement to newborn screening programs for metachromatic leukodystrophy. Science 2013;
Krabbe disease. J Inherit Metab Dis 2015;38(5): 341(6148):1233158. doi:10.1126/science.1233158.
923–929. doi:10.1007/s10545-015-9822-z.
35 Sessa M, Lorioli L, Fumagalli F, et al. Lentiviral
20 Carter RL, Wrabetz L, Jalal K, et al. Can psychosine haemopoietic stem-cell gene therapy in
and galactocerebrosidase activity predict early-onset metachromatic leukodystrophy: an
early-infantile Krabbe’s disease ad-hoc analysis of a non-randomised, open-label,
presymptomatically? J Neurosci Res 2016;94(11): phase 1/2 trial. Lancet 2016;388(10043):476–487.
1084–1093. doi:10.1002/jnr.23793. doi:10.1016/S0140-6736(16)30374-9.
148 FEBRUARY 2018
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
36 Crow YJ, Chase DS, Lowenstein Schmidt J, et al. 46 Crow YJ, Vanderver A, Orcesi S, et al. Therapies in
Characterization of human disease phenotypes Aicardi-Goutieres syndrome. Clin Exp Immunol
associated with mutations in TREX1, RNASEH2A, 2014;175(1):1–8. doi:10.1111/cei.12115.
RNASEH2B, RNASEH2C, SAMHD1, ADAR, and IFIH1.
47 Clayton PT, Verrips A, Sistermans E, et al. Mutations
Am J Med Genet A 2015;167A(2):296–312.
in the sterol 27-hydroxylase gene (CYP27A) cause
doi:10.1002/ajmg.a.36887.
hepatitis of infancy as well as cerebrotendinous
37 Aicardi J, Goutières F. A progressive familial xanthomatosis. J Inherit Metab Dis 2002;25(6):
encephalopathy in infancy with calcifications of 501–513. doi:10.1023/A:1021211520034.
the basal ganglia and chronic cerebrospinal fluid
48 Barkhof F, Verrips A, Wesseling P, et al.
lymphocytosis. Ann Neurol. 1984;15(1): 49–54.
Cerebrotendinous xanthomatosis: the spectrum
doi:10.1002/ana.410150109.
of imaging findings and the correlation with
38 Abe J, Nakamura K, Nishikomori R, et al. A nationwide neuropathologic findings. Radiology 2000;217(3):
survey of Aicardi-Goutières syndrome patients 869–876. doi:10.1148/radiology.217.3.r00dc03869.
identifies a strong association between dominant
49 Pudhiavan A, Agrawal A, Chaudhari S, Shukla A.
TREX1 mutations and chilblain lesions: Japanese
Cerebrotendinous xanthomatosis-he spectrum of
cohort study. Rheumatology (Oxford) 2014;53(3):
imaging findings. J Radiol Case Rep 2013;7(4): 1–9.
448–458. doi:10.1093/rheumatology/ket372.
doi:10.3941/jrcr.v7i4.1338.
39 Tolmie JL, Shillito P, Hughes-Benzie R, Stephenson
JB. The Aicardi-Goutières syndrome (familial, early 50 Bleyle L, Huidekoper HH, Vaz FM, et al. Update
on newborn dried bloodspot testing for
onset encephalopathy with calcifications of the
basal ganglia and chronic cerebrospinal fluid cerebrotendinous xanthomatosis: an available
high-throughput liquid-chromatography tandem
lymphocytosis). J Med Genet 1995;32(11): 881–884.
mass spectrometry method. Mol Genet Metab
doi:10.1136/jmg.32.11.881.
Reports 2016;7:11–15. doi:10.1016/j.ymgmr.2016.
40 Kolivras A, Aeby A, Crow YJ, et al. Cutaneous 02.002.
histopathological findings of Aicardi-Goutieres
syndrome, overlap with chilblain lupus. J Cutan 51 Pitt JJ. High-throughput urine screening for
Smith-Lemli-Opitz syndrome and cerebrotendinous
Pathol 2008;35(8):774–778. doi:10.1111/j.1600-0560.
2007.00900.x. xanthomatosis using negative electrospray tandem
mass spectrometry. Clin Chim Acta 2007;380(1–2):
41 Abdel-Salam GMH, El-Kamah GY, Rice GI, et al. 81–88. doi:10.1016/j.cca.2007.01.016.
Chilblains as a diagnostic sign of Aicardi-Goutieres
52 Pitt JJ, Peters H. Screening for cerebrotendinous
syndrome. Neuropediatrics 2010;41(1):18–23.
xanthomatosis. J Inherit Metab Dis. 2015;38(2): 369.
doi:10.1055/s-0030-1255059.
doi:10.1007/s10545-014-9765-9.
42 La Piana R, Uggetti C, Roncarolo F, et al.
Neuroradiologic patterns and novel imaging findings 53 Batta AK, Salen G, Tint GS. Hydrophilic 7-hydroxy
in Aicardi-Goutières syndrome. Neurology 2016; bile acids, lovastatin, and cholestyramine are
86(1):28–35. doi:10.1212/WNL.0000000000002228. ineffective in the treatment of cerebrotendinous
xanthomatosis. Metabolism 2004;53(5): 556–562.
43 La Piana R, Uggetti C, Olivieri I, et al. Bilateral striatal doi:10.1016/j.metabol.2003.12.003.
necrosis in two subjects with Aicardi-Goutieres
syndrome due to mutations in ADAR1 (AGS6). Am J Med 54 Yahalom G, Tsabari R, Molshatzki N, et al.
Genet A 2014;164A(3):815–819. doi:10.1002/ajmg.a.36360. Neurological outcome in cerebrotendinous
xanthomatosis treated with chenodeoxycholic
44 Vanderver A, Prust M, Kadom N, et al. Early-onset acid: early versus late diagnosis. Clin
Aicardi-Goutieres syndrome: magnetic resonance Neuropharmacol 2013;36(3):78–83. doi:10.1097/
imaging (MRI) pattern recognition. J Child Neurol WNF.0b013e318288076a.
2015;30(10):1343–1348. doi:10.1177/0883073814562252.
45 Blau N, Bonafé L, Krägeloh-Mann I, et al. 55 Pierre G, Setchell K, Blyth J, et al. Prospective
treatment of cerebrotendinous xanthomatosis
Cerebrospinal fluid pterins and folates in
Aicardi-Goutières syndrome: a new phenotype. with cholic acid therapy. J Inherit Metab Dis 2008;
31(suppl 2):S241–S245. doi:10.1007/s10545-008-
Neurology 2003;61(5):642–647. doi:10.1212/
0815-z.
01.WNL.0000082726.08631.E7.
CONTINUUMJOURNAL.COM 149
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
S-ar putea să vă placă și
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (121)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (588)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (400)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2259)
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (895)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (74)
- Fluid & Electrolytes Cheat SheetDocument1 paginăFluid & Electrolytes Cheat SheetGelyn Gaylon0% (1)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- C 10 + 11 GALLBLADDER AND BILIARY TRACT Part1Document45 paginiC 10 + 11 GALLBLADDER AND BILIARY TRACT Part1mikaaa0000% (1)
- Anatomy Plable ClincherDocument6 paginiAnatomy Plable ClincherAkwu AkwuÎncă nu există evaluări
- The Teaching Files - Gastrointestinal PDFDocument854 paginiThe Teaching Files - Gastrointestinal PDFJave Mahsud100% (2)
- Approach To The Dysmorphic ChildDocument15 paginiApproach To The Dysmorphic ChildBashar KhalilÎncă nu există evaluări
- Npte Exam TablesDocument586 paginiNpte Exam TablesarbazÎncă nu există evaluări
- NBME Peds Form 2 AnswersDocument27 paginiNBME Peds Form 2 Answersjohndoe199580% (5)
- Risk Factors For Periodontal Diseases 2022Document13 paginiRisk Factors For Periodontal Diseases 2022SnowÎncă nu există evaluări
- Mitochondrial Cytopathies in Children and AdultsDocument28 paginiMitochondrial Cytopathies in Children and AdultsNathaly LapoÎncă nu există evaluări
- Hepatocellular Carcinoma: Manal Abdel Hamid Associate Prof. of Medical OncologyDocument24 paginiHepatocellular Carcinoma: Manal Abdel Hamid Associate Prof. of Medical OncologyfridaÎncă nu există evaluări
- XN - Clinical Case - ReportDocument83 paginiXN - Clinical Case - Report郑伟健Încă nu există evaluări
- Co AmoxiclavDocument1 paginăCo AmoxiclavGrace DonatoÎncă nu există evaluări
- Orofacial Complications of Non Surgical Cancer TherapyDocument59 paginiOrofacial Complications of Non Surgical Cancer TherapyKassim OboghenaÎncă nu există evaluări
- 1 s2.0 S1059131107000842 MainDocument12 pagini1 s2.0 S1059131107000842 MainNathaly LapoÎncă nu există evaluări
- Gonzalez Martinez 2014Document11 paginiGonzalez Martinez 2014Nathaly LapoÎncă nu există evaluări
- J Nucl Med 2010 Didelot 1732 9Document9 paginiJ Nucl Med 2010 Didelot 1732 9Nathaly LapoÎncă nu există evaluări
- 10 1006@nimg 2000 0606Document10 pagini10 1006@nimg 2000 0606Nathaly LapoÎncă nu există evaluări
- Behdad Et Al-2009-EpilepsiaDocument12 paginiBehdad Et Al-2009-EpilepsiaNathaly LapoÎncă nu există evaluări
- Pediatric Anti-NMDA-R Encephalitis - EstebanitoDocument4 paginiPediatric Anti-NMDA-R Encephalitis - EstebanitoNathaly LapoÎncă nu există evaluări
- Crocker 2016Document16 paginiCrocker 2016Nathaly LapoÎncă nu există evaluări
- Wjem12 1p0067 PDFDocument10 paginiWjem12 1p0067 PDFAkbal Nur KarimÎncă nu există evaluări
- 10 1111@epi 16469Document9 pagini10 1111@epi 16469Nathaly LapoÎncă nu există evaluări
- Mitochondrial Dna and DiseaseDocument16 paginiMitochondrial Dna and DiseaseNathaly LapoÎncă nu există evaluări
- Mitocondrial TratamientoDocument19 paginiMitocondrial TratamientoNathaly LapoÎncă nu există evaluări
- Narco TtoDocument59 paginiNarco TtoNathaly LapoÎncă nu există evaluări
- Yic AanDocument7 paginiYic AanNathaly LapoÎncă nu există evaluări
- Strokeduetovasculitisin Childrenandadults: David S. YoungerDocument24 paginiStrokeduetovasculitisin Childrenandadults: David S. YoungerNathaly LapoÎncă nu există evaluări
- West Tto 2Document10 paginiWest Tto 2Nathaly LapoÎncă nu există evaluări
- West TtoDocument3 paginiWest TtoNathaly LapoÎncă nu există evaluări
- Nonconvulsive Status Epilepticus: Validating The Salzburg Criteria Against An Expert EEG ExaminerDocument5 paginiNonconvulsive Status Epilepticus: Validating The Salzburg Criteria Against An Expert EEG ExaminerNathaly LapoÎncă nu există evaluări
- Clinical Review: The First Seizure and Its Management in Adults and ChildrenDocument4 paginiClinical Review: The First Seizure and Its Management in Adults and ChildrenNathaly LapoÎncă nu există evaluări
- Noninfectious Cerebral Vasculitis in Children: Indianapolis, IndianaDocument15 paginiNoninfectious Cerebral Vasculitis in Children: Indianapolis, IndianaNathaly LapoÎncă nu există evaluări
- Update On Antiepileptic - Drugs 2019 PDFDocument29 paginiUpdate On Antiepileptic - Drugs 2019 PDFRahul RaiÎncă nu există evaluări
- The EEG of Status Epilepticus: Peter W. KaplanDocument9 paginiThe EEG of Status Epilepticus: Peter W. KaplanNathaly LapoÎncă nu există evaluări
- 10 1111@epi 16469Document9 pagini10 1111@epi 16469Nathaly LapoÎncă nu există evaluări
- Hypoxic-Ischemic Encephalopathy and Other Neonatal EncephalopathiesDocument15 paginiHypoxic-Ischemic Encephalopathy and Other Neonatal EncephalopathiesNathaly LapoÎncă nu există evaluări
- ArchDisChild 2010 Darke 382 6Document7 paginiArchDisChild 2010 Darke 382 6Nathaly LapoÎncă nu există evaluări
- Encephalitis ChildDocument8 paginiEncephalitis ChildJeane SuyantoÎncă nu există evaluări
- Twilt-Benseler2015 Article TreatmentOfCNSVasculitisInChilDocument16 paginiTwilt-Benseler2015 Article TreatmentOfCNSVasculitisInChilNathaly LapoÎncă nu există evaluări
- Epileptic Spasms in Epilepsy With Myoclonic-Atonic Seizures (Doose Syndrome)Document8 paginiEpileptic Spasms in Epilepsy With Myoclonic-Atonic Seizures (Doose Syndrome)Nathaly LapoÎncă nu există evaluări
- Et DGDocument11 paginiEt DGNathaly LapoÎncă nu există evaluări
- Epileptic Encephalopathies.13Document15 paginiEpileptic Encephalopathies.13Nathaly LapoÎncă nu există evaluări
- Principles of Medical Laboratory Science PracticeDocument14 paginiPrinciples of Medical Laboratory Science PracticeJanna EchavezÎncă nu există evaluări
- Case ReviewDocument20 paginiCase ReviewEdwin OkonÎncă nu există evaluări
- Minerals Minerals Function S Food Sources RDA Deficiency ToxicityDocument7 paginiMinerals Minerals Function S Food Sources RDA Deficiency ToxicityPoinsithia OrlandaÎncă nu există evaluări
- CH 9 - Etiology of Heterophoria and Heterotropia, P. 134-152-EmailDocument19 paginiCH 9 - Etiology of Heterophoria and Heterotropia, P. 134-152-EmailAmi MisiciÎncă nu există evaluări
- Drug Study of Ron Steven AlvarezDocument2 paginiDrug Study of Ron Steven AlvarezAlvarez StevenÎncă nu există evaluări
- Transient Drug Induced Myopia PDFDocument5 paginiTransient Drug Induced Myopia PDFHamza BajwaÎncă nu există evaluări
- Hepatic ComaDocument4 paginiHepatic ComaAshraf Abu-ainÎncă nu există evaluări
- Posttest. Renal DisordersDocument3 paginiPosttest. Renal Disordersjbagacay100% (3)
- Congenital Heart Disease Surgery TransDocument9 paginiCongenital Heart Disease Surgery TransPuguinGamingÎncă nu există evaluări
- Diverticulosis!!Document10 paginiDiverticulosis!!Nahdah AidahÎncă nu există evaluări
- Cystic Fibrosis Late Diagnosis A Case ReportDocument3 paginiCystic Fibrosis Late Diagnosis A Case ReportVivi DeviyanaÎncă nu există evaluări
- 123Document10 pagini123Aryan SanezÎncă nu există evaluări
- Diphtheria SlideDocument11 paginiDiphtheria Slideandre andreÎncă nu există evaluări
- Medical-Surgical Nursing ArthritisDocument8 paginiMedical-Surgical Nursing ArthritisNoelyn BaluyanÎncă nu există evaluări
- Anaplastic Thyroid CancerDocument40 paginiAnaplastic Thyroid Cancershita febrianaÎncă nu există evaluări
- MS DiseaseDocument2 paginiMS Diseasesundareswar perumalÎncă nu există evaluări
- Managing Sclerotherapy Complications: ObjectivesDocument16 paginiManaging Sclerotherapy Complications: ObjectivesAnhÎncă nu există evaluări
- JaundiceDocument3 paginiJaundiceNyaoNyao MarcellanaÎncă nu există evaluări