Documente Academic
Documente Profesional
Documente Cultură
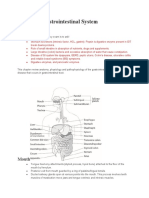
Gastrointestinal System
Încărcat de
Pinky CuaresmaDescriere originală:
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Gastrointestinal System
Încărcat de
Pinky CuaresmaDrepturi de autor:
Formate disponibile
Gastrointestinal System National University: College of Nursing
Gastrointestinal System :: Medical Surgical Nursing :: Review For Nursing Licensure Examination Slide
Transcript
Slide 1: Medical Surgical Nursing The GASTRO-INTESTINAL System Nurse Licensure Examination Review
Slide 2: The Gastro-Intestinal System Review of the GIT Anatomy and Physiology Review of Common
laboratory procedures Review of Common Symptoms and their nursing interventions Review of
common disorders of the: Esophagus -gallbladder Stomach -exocrine pancreas Small intestine -
liver Large Intestine
Slide 4: The GIT System: Anatomy and Physiology The GIT is composed of two general parts The main
GIT starts from the mouth EsophagusStomachSILI The accessory organs are the Salivary glands
Liver Gallbladder Pancreas
Slide 5: The GIT ANATOMY The Mouth Contains the lips, cheeks, palate, tongue, teeth, salivary glands,
masticatory/facial muscles and bones Anteriorly bounded by the lips Posteriorly bounded by the
oropharynx
Slide 6: The GIT Physiology The Mouth Important for the mechanical digestion of food The saliva
contains SALIVARY AMYLASE or PTYALIN that starts the INITIAL digestion of carbohydrates
Slide 7: The GIT ANATOMY The Esophagus A hollow collapsible tube Length- 10 inches Made up of
stratified squamos epithelium
Slide 8: The GIT ANATOMY The Esophagus The upper third contains skeletal muscles The middle
third contains mixed skeletal and smooth muscles The lower third contains smooth muscles and the
esophago-gastric/ cardiac sphincter is found here
Slide 9: The GIT PHYSIOLOGY The Esophagus Functions to carry or propel foods from the oropharynx
to the stomach Swallowing or deglutition is composed of three phases:
Slide 10: The GIT ANATOMY The stomach J-shaped organ in the epigastrium Contains four parts- the
fundus, the cardia, the body and the pylorus The cardiac sphincter prevents the reflux of the contents
into the esophagus The pyloric sphincter regulates the rate of gastric emptying into the duodenum
Capacity is 1,500 ml!
Slide 11: The GIT PHYSIOLOGY The functions of the stomach are generally to digest the food (proteins)
and to propel the digested materials into the SI for final digestion The Glands and cells in the stomach
secrete digestive enzymes:
Slide 12: The GIT PHYSIOLOGY Stomach: 1. Parietal cells- HCl acid and Intrinsic factor 2. Chief cells-
pepsin digestion of PROTEINS! 3. Antral G-cells- gastrin 4. Argentaffin cells- serotonin 5. Mucus
neck cells- mucus
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
Slide 13: The GIT ANATOMY The Small intestine Grossly divided into the Duodenum, Jejunum and
Ileum The duodenum contains the two openings for the bile and pancreatic ducts The ileum is the
longest part (about 12 feet)
Slide 14: The GIT physiology The intestinal glands secrete digestive enzymes that finalize the digestion
of all foodstuff Enzymes for carbohydrates disaccharidases Enzymes for proteins dipeptidases and
aminopeptidases Enzyme for lipids intestinal lipase
Slide 15: The GIT ANATOMY The Large intestine Approximately 5 feet long, with parts: 1. The cecum
widest diameter, prone to rupture 2. The appendix 3. The ascending colon 4. The transverse colon
5. The descending colon 6. The sigmoid most mobile, prone to twisting 7. The rectum
Slide 16: The GIT Physiology Absorbs water Eliminates wastes Bacteria in the colon synthesize
Vitamin K Appendix participates in the immune system
Slide 17: The GIT Physiology SYMPATHETIC PARASYMPATHETIC Generally INHIBITORY! Generally
EXCITATORY! Decreased gastric Increased gastric secretions secretions Decreased GIT motility
Increased gastric motility But: Increased sphincteric But: Decreased sphincteric tone and constriction
of tone and dilation of blood blood vessels vessels
Slide 18: The GIT ANATOMY The Liver The largest internal organ Located in the right upper quadrant
Contains two lobes- the right and the left The hepatic ducts join together with the cystic duct to
become the common bile duct
Slide 19: The GIT Physiology: LIVER Functions to store excess glucose, fats and amino acids Also stores
the fat soluble vitamins- A, D and the water soluble- Vitamin B12 Produces the BILE for normal fat
digestion The Von Kupffer cells remove bacteria in the portal blood Detoxifies ammonia into urea
Slide 20: The GIT anatomy The gallbladder Located below the liver The cystic duct joins the hepatic
duct to become the bile duct The common bile duct joins the pancreatic duct in the sphincter of Oddi
in the first part of the duodenum
Slide 21: The GIT Physiology Stores and concentrates bile Contracts during the digestion of fats to
deliver the bile Cholecystokinin is released by the duodenal cells, causing the contraction of the
gallbladder and relaxation of the sphincter of Oddi
Slide 22: The GIT anatomy The pancreas A retroperitoneal gland Functions as an endocrine and
exocrine gland The pancreatic duct (major) joins the common bile duct in the sphincter of Oddi
Slide 23: The GIT Physiology The exocrine function of the pancreas is the secretion of digestive
enzymes for carbohydrates, fats and proteins Pancreatic amylase carbohydrates Pancreatic lipase
(steapsin) fats Trypsin, Chymotrypsin and Peptidases proteins Bicarbonate to neutralize the acidic
chyme. Stimulated by SECRETIN!
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
Slide 24: Gastrointestinal Assessment Laboratory Procedures
Slide 25: COMMON LABORATORY PROCEDURES FECALYSIS Examination of stool consistency, color and
the presence of occult blood. Special tests for fat, nitrogen, parasites, ova, pathogens and others
Slide 26: COMMON LABORATORY PROCEDURES FECALYSIS: Occult Blood Testing Instruct the patient to
adhere to a 3-day meatless diet No intake of NSAIDS, aspirin and anti-coagulant Screening test for
colonic cancer
Slide 27: COMMON LABORATORY PROCEDURES Upper GIT study: barium swallow Examines the upper
GI tract Barium sulfate is usually used as contrast
Slide 28: COMMON LABORATORY PROCEDURES Upper GIT study: barium swallow Pre-test: NPO post-
midnight Post-test: Laxative is ordered, increase pt fluid intake, instruct that stools will turn white,
monitor for obstruction
Slide 31: COMMON LABORATORY PROCEDURES Lower GIT study: barium enema Examines the lower
GI tract Pre-test: Clear liquid diet and laxatives, NPO post-midnight, cleansing enema prior to the test
Slide 32: COMMON LABORATORY PROCEDURES Lower GIT study: barium enema Post-test: Laxative is
ordered, increase patient fluid intake, instruct that stools will turn white, monitor for obstruction
Slide 34: COMMON LABORATORY PROCEDURES Gastric analysis Aspiration of gastric juice to measure
pH, appearance, volume and contents Pre-test: NPO 8 hours, avoidance of stimulants, drugs and
smoking Post-test: resume normal activities
Slide 35: COMMON LABORATORY PROCEDURES EGD (esophagogastroduodenoscopy) Visualization of
the upper GIT by endoscope Pre-test: ensure consent, NPO 8 hours, pre-medications like atropine and
anxiolytics
Slide 37: COMMON LABORATORY PROCEDURES EGD esophagogastroduodenoscopy Intra-test:
position : LEFT lateral to facilitate salivary drainage and easy access
Slide 38: COMMON LABORATORY PROCEDURES EGD (esophagogastroduodenoscopy) Post-test: NPO
until gag reflex returns, place patient in SIMS position until he awakens, monitor for complications,
saline gargles for mild oral discomfort
Slide 39: COMMON LABORATORY PROCEDURES Lower GI- scopy Use of endoscope to visualize the
anus, rectum, sigmoid and colon Pre-test: consent, NPO 8 hours, cleansing enema until return is clear
Slide 41: COMMON LABORATORY PROCEDURES Lower GI- scopy Intra-test: position is LEFT lateral,
right leg is bent and placed anteriorly Post-test: bed rest, monitor for complications like bleeding and
perforation
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
Slide 43: COMMON LABORATORY PROCEDURES Cholecystography Examination of the gallbladder to
detect stones, its ability to concentrate, store and release the bile Pre-test: ensure consent, ask
allergies to iodine, seafood and dyes; contrast medium is administered the night prior, NPO after
contrast administration
Slide 44: COMMON LABORATORY PROCEDURES Cholecystography Post-test: Advise that dysuria is
common as the dye is excreted in the urine, resume normal activities
Slide 45: COMMON LABORATORY PROCEDURES Paracentesis Removal of peritoneal fluid for analysis
Slide 46: COMMON LABORATORY PROCEDURES Paracentesis Pre-test: ensure consent, instruct to
VOID and empty bladder, measure abdominal girth
Slide 47: COMMON LABORATORY PROCEDURES Paracentesis Intra-test: Upright on the edge of the bed,
back supported and feet resting on a foot stool
Slide 48: COMMON LABORATORY PROCEDURES Liver biopsy Pretest Consent NPO Check for the
bleeding parameters
Slide 49: COMMON LABORATORY PROCEDURES Liver biopsy Intratest Position: Semi fowler’s LEFT
lateral to expose right side of abdomen
Slide 50: COMMON LABORATORY PROCEDURES Liver biopsy Post-test: position on RIGHT lateral with
pillow underneath, monitor VS and complications like bleeding, perforation. Instruct to avoid lifting
objects for 1 week
Slide 51: The NURSING PROCESS in GIT Disorders Assessment Health history Nursing History PE
Laboratory procedures
Slide 52: The ABDOMINAL examination The sequence to follow is: Inspection Auscultation
Percussion Palpation
Slide 54: COMMON GIT SYMPTOMS AND MANAGEMENT CONSTIPATION DIARRHEA DUMPING
SYNDROME
Slide 55: COMMON GIT SYMPTOMS AND MANAGEMENT CONSTIPATION An abnormal infrequency and
irregularity of defecation Multiple causations
Slide 56: COMMON GIT SYMPTOMS AND MANAGEMENT CONSTIPATION: Pathophysiology
Interference with three functions of the colon 1. Mucosal transport 2. Myoelectric activity 3.
Process of defecation
Slide 57: COMMON GIT SYMPTOMS AND MANAGEMENT NURSING INTERVENTIONS 1. Assist physician
in treating the underlying cause of constipation 2. Encourage to eat HIGH fiber diet to increase the
bulk 3. Increase fluid intake 4. Administer prescribed laxatives, stool softeners 5. Assist in relieving
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
stress
Slide 58: COMMON GIT SYMPTOMS AND MANAGEMENT Diarrhea Abnormal fluidity of the stool
Multiple causes Gastrointestinal Diseases Hyperthyroidism Food poisoning
Slide 59: COMMON GIT SYMPTOMS AND MANAGEMENT Diarrhea Nursing Interventions 1. Increase fluid
intake- ORESOL is the most important treatment! 2. Determine and manage the cause 3. Anti-diarrheal
drugs
Slide 60: COMMON GIT SYMPTOMS AND MANAGEMENT DUMPING SYNDROME A condition of rapid
emptying of the gastric contents into the small intestine usually after a gastric surgery Symptoms
occur 30 minutes after eating
Slide 61: COMMON GIT SYMPTOMS AND MANAGEMENT PATHOPHYSIOLOGY Foods high in CHO and
electrolytes must be diluted in the jejunum before absorption takes place.
Slide 62: COMMON GIT SYMPTOMS AND MANAGEMENT PATHOPHYSIOLOGY The rapid influx of
stomach contents will cause distention of the jejunum early symptoms
Slide 63: COMMON GIT SYMPTOMS AND MANAGEMENT PATHOPHYSIOLOGY The hypertonic food bolus
will draw fluid from the blood vessels to dilute the high concentrations of CHO and electrolytes in the
food bolus
Slide 64: COMMON GIT SYMPTOMS AND MANAGEMENT Later, there is increased blood glucose
stimulating the increased secretion of insulin
Slide 65: COMMON GIT SYMPTOMS AND MANAGEMENT Then, blood glucose will fall causing reactive
hypoglycemia
Slide 66: COMMON GIT SYMPTOMS AND MANAGEMENT DUMPING SYNDROME ASSESSMENT FINDINGS:
early symptoms 1. Nausea and Vomiting 2. Abdominal fullness 3. Abdominal cramping 4.
Palpitation 5. Diaphoresis
Slide 67: COMMON GIT SYMPTOMS AND MANAGEMENT DUMPING SYNDROME ASSESSMENT FINDINGS:
LATE symptoms: 6. Drowsiness 7. Weakness and Dizziness 8. Hypoglycemia
Slide 68: COMMON GIT SYMPTOMS AND MANAGEMENT DS NURSING INTERVENTIONS 1. Advise
patient to eat LOW- carbohydrate HIGH-fat and HIGH- protein diet 2. Instruct to eat SMALL frequent
meals, include MORE dry items. 3. Instruct to AVOID consuming FLUIDS with meals
Slide 69: COMMON GIT SYMPTOMS AND MANAGEMENT DS NURSING INTERVENTIONS 4. Instruct to
LIE DOWN after meals 5. Administer anti-spasmodic medications to delay gastric emptying
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
Slide 70: GIT SYMPTOMS AND MANAGEMENT PERNICIOUS ANEMIA Results from Deficiency of vitamin
B12 due to autoimmune destruction of the parietal cells, lack of INTRINSIC FACTOR or total removal of
the stomach
Slide 71: GIT SYMPTOMS AND MANAGEMENT PERNICIOUS ANEMIA ASSESSMENT Severe pallor
Fatigue Weight loss SMOOTH BEEFY-RED TONGUE Mild jaundice Paresthesia of extremities
Balance disturbance
Slide 72: GIT SYMPTOMS AND MANAGEMENT NURSING INTERVENTION for Pernicious Anemia Lifetime
injection of Vitamin B 12 weekly initially, then MONTHLY
Slide 73: Conditions of the GIT UPPER GI system
Slide 74: CONDITION OF THE ESOPHAGUS HIATAL HERNIA Protrusion of the esophagus into the
diaphragm thru an opening Two types- Sliding hiatal hernia ( most common) and Axial hiatal hernia
Slide 75: CONDITION OF THE ESOPHAGUS ASSESSMENT Findings in Hiatal hernia 1. Heartburn 2.
Regurgitation 3. Dysphagia 4. 50%- without symptoms
Slide 76: CONDITION OF THE ESOPHAGUS DIAGNOSTIC TEST Barium swallow and fluoroscopy
Slide 77: CONDITION OF THE ESOPHAGUS NURSING INTERVENTIONS 1. Provide small frequent
feedings 2. AVOID supine position for 1 hour after eating 3. Elevate the head of the bed on 8- inch
block 4. Provide pre-op and post-op care
Slide 78: CONDITION OF THE ESOPHAGUS Esophageal Varices Dilation and tortuosity of the
submucosal veins in the distal esophagus ETIOLOGY: commonly caused by PORTAL hypertension
secondary to liver cirrhosis This is an Emergency condition!
Slide 79: CONDITION OF THE ESOPHAGUS ASSESSMENT findings for EV 1. Hematemesis 2. Melena
3. Ascites 4. jaundice 5. hepatomegaly/splenomegaly
Slide 80: CONDITION OF THE ESOPHAGUS ASSESSMENT findings for EV Signs of Shock- tachycardia,
hypotension, tachypnea, cold clammy skin, narrowed pulse pressure
Slide 81: CONDITION OF THE ESOPHAGUS DIAGNOSTIC PROCEDURE Esophagoscopy
Slide 82: CONDITION OF THE ESOPHAGUS NURSING INTERVENTIONS FOR EV 1. Monitor VS strictly.
Note for signs of shock 2. Monitor for LOC 3. Maintain NPO
Slide 83: CONDITION OF THE ESOPHAGUS NURSING INTERVENTIONS FOR EV 4. Monitor blood studies
5. Administer O2 6. prepare for blood transfusion
Slide 84: CONDITION OF THE ESOPHAGUS INTERVENTIONS FOR EV 7. prepare to administer
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
Vasopressin and Nitroglycerin 8. Assist in NGT and Sengstaken- Blakemore tube insertion for balloon
tamponade
Slide 85: CONDITION OF THE ESOPHAGUS NURSING INTERVENTIONS FOR EV 9. Prepare to assist in
surgical management: Endoscopic sclerotherapy Variceal ligation Shunt procedures
Slide 86: Conditions of the Stomach Gastro-esophageal reflux Backflow of gastric contents into the
esophagus Usually due to incompetent lower esophageal sphincter , pyloric stenosis or motility
disorder Symptoms may mimic ANGINA or MI
Slide 87: Conditions of the Stomach ASSESSMENT ( for GERD) Heartburn Dyspepsia Regurgitation
Epigastric pain Difficulty swallowing Ptyalism
Slide 88: Conditions of the Stomach Diagnostic test Endoscopy or barium swallow Gastric ambulatory
pH analysis Note for the pH of the esophagus, usually done for 24 hours The pH probe is located 5
inches above the lower esophageal sphincter The machine registers the different pH of the refluxed
material into the esophagus
Slide 89: Conditions of the Stomach NURSING INTERVENTIONS 1. Instruct the patient to AVOID
stimulus that increases stomach pressure and decreases GES pressure 2. Instruct to avoid spices,
coffee, tobacco and carbonated drinks 3. Instruct to eat LOW-FAT, HIGH- FIBER diet
Slide 90: Conditions of the Stomach NURSING INTERVENTIONS 4. Avoid foods and drinks TWO hours
before bedtime 5. Elevate the head of the bed with an approximately 8-inch block
Slide 91: Conditions of the Stomach NURSING INTERVENTIONS 6. Administer prescribed H2- blockers,
PPI and prokinetic meds like cisapride, metochlopromide 7. Advise proper weight reduction
Slide 92: Conditions of the Stomach GASTRITIS Inflammation of the gastric mucosa May be Acute or
Chronic Etiology: Acute- bacteria, irritating foods, NSAIDS, alcohol, bile and radiation Etiology:
Chronic- Ulceration, bacteria, Autoimmune disease, diet, alcohol, smoking
Slide 93: Conditions of the Stomach PATHOPHYSIOLOGY OF Gastritis Insults cause gastric mucosal
damage inflammation, hyperemia and edema superficial erosions decreased gastric secretions,
ulcerations and bleeding
Slide 94: Conditions of the Stomach ASSESSMENT ASSESSMENT (Chronic) (Acute) Pyrosis Dyspepsia
Singultus Headache Sour taste in the Anorexia mouth Dyspepsia Nausea/Vomiting
N/V/anorexia Pernicious anemia
Slide 95: Conditions of the Stomach DIAGNOSTIC PROCEDURE EGD- to visualize the gastric mucosa for
inflammation Low levels of HCl Biopsy to establish correct diagnosis whether acute or chronic
Slide 96: Conditions of the Stomach NURSING INTERVENTIONS 1. Give BLAND diet 2. Monitor for
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
signs of complications like bleeding, obstruction and pernicious anemia 3. Instruct to avoid spicy foods,
irritating foods, alcohol and caffeine
Slide 97: Conditions of the Stomach NURSING INTERVENTIONS 4. Administer prescribed medications-
H2 blockers, antibiotics, mucosal protectants 5. Inform the need for Vitamin B12 injection if deficiency
is present
Slide 98: Conditions of the Stomach PEPTIC ULCER DISEASE An ulceration of the gastric and duodenal
lining May be referred as to location as Gastric ulcer in the stomach, or Duodenal ulcer in the
duodenum Most common Peptic ulceration: anterior part of the upper duodenum
Slide 99: Conditions of the Stomach PATHOPHYSIOLOGY of PUD Disturbance in acid secretion and
mucosal protection Increased acidity or decreased mucosal resistance erosion and ulceration
Slide 100: Conditions of the Stomach GASTRIC ULCER Ulceration of the gastric mucosa, submucosa and
rarely the muscularis
Slide 101: Conditions of the Stomach GASTRIC ULCER Risk factors: Stress, smoking, NSAIDS abuse,
Alcohol, Helicobacter pylori infection, type A personality and History of gastritis Incidence is high in
older adults Acid secretion is NORMAL
Slide 102: Conditions of the Stomach ASSESSMENT (Gastric Ulcer) Epigastric pain Characteristic:
Gnawing, sharp pain in the mid-epigastrium 1-2 hours AFTER eating, often NOT RELIEVED by food intake,
sometimes AGGRAVATING the pain!
Slide 103: Conditions of the Stomach ASSESSMENT (Gastric Ulcer) Nausea Vomiting is more common
Hematemesis Weight loss
Slide 104: Conditions of the Stomach DIAGNOSTIC PROCEDURES 1. EGD to visualize the ulceration 2.
Urea breath test for H. pylori infection 3. Biopsy- to rule out gastric cancer
Slide 105: Conditions of the Stomach NURSING INTERVENTIONS 1. Give BLAND diet, small frequent
meals during the active phase of the disease 2. Administer prescribed medications- H2 blockers, PPI,
mucosal barrier protectants and antacids
Slide 106: Conditions of the Stomach NURSING INTERVENTIONS 3. Monitor for complications of
bleeding, perforation and intractable pain 4. provide teaching about stress reduction and relaxation
techniques
Slide 107: Conditions of the Stomach NURSING INTERVENTIONS FOR BLEEDING 1. Maintain on NPO
2. Administer IVF and medications 3. Monitor hydration status, hematocrit and hemoglobin
Slide 108: Conditions of the Stomach NURSING INTERVENTIONS FOR BLEEDING 4. Assist with SALINE
lavage 5. Insert NGT for decompression and lavage
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
Slide 109: Conditions of the Stomach NURSING INTERVENTIONS FOR BLEEDING 6. Prepare to
administer blood transfusion 7. Prepare to give VASOPRESSIN to induce vasoconstriction to reduce
bleeding 8. Prepare patient for SURGERY if warranted
Slide 110: Conditions of the Stomach SURGICAL PROCEDURES FOR PUD Total gastrectomy, vagotomy,
gastric resection, Billroth I and II, pyloroplasty
Slide 112: Conditions of the Stomach SURGICAL PROCEDURES FOR PUD Post-operative Nursing
management 1. Monitor VS 2. Post-op position: FOWLER’S 3. NPO until peristalsis returns 4.
Monitor for bowel sounds 5. Monitor for complications of surgery
Slide 113: Conditions of the Stomach Post-operative Nursing management 6. Monitor I and O, IVF 7.
Maintain NGT 8. Diet progress: clear liquid full liquid six bland meals 9. Manage DUMPING
SYNDROME
Slide 114: Condition of the Duodenum DUODENAL ULCER Ulceration of duodenal mucosa and
submucosa Usually due to increased gastric acidity
Slide 115: Condition of the Duodenum DUODENAL ULCER ASSESSMENT PAIN characteristic: Burning
pain in the mid- epigastrium 2-4 HOURS after eating or during the night, RELIEVED by food intake
Slide 117: Condition of the Duodenum DIAGNOSTIC TESTS EGD and Biopsy
Slide 120: Condition of the Duodenum NURSING INTERVENTIONS 1. Same as for gastric ulceration 2.
Patient teaching-avoid alcohol, smoking, caffeine and carbonated drinks Take NSAIDS with meals Adhere
to medication regimen
Slide 121: Ulcers GASTRIC DUODENAL Older Younger Normal Acidity INCREASED acidity Pain early after
eating Pain late after eating (2-4 hours) WORSENS by food, RELIEVES by food RELIEVED by VOMITING
Bleeding, weight loss and Less likely bleeding and vomiting vomiting (+) cancer (-) cancer
Slide 122: Conditions of the Lower Tract Small and Large Intestine
Slide 123: CONDITIONS OF THE SMALL INTESTINE CROHN’S DISEASE Also called Regional Enteritis An
inflammatory disease of the GIT affecting usually the small intestine
Slide 124: CONDITIONS OF THE SMALL INTESTINE CROHN’S DISEASE ETIOLOGY: unknown The
terminal ileum thickens, with scarring, ulcerations, abscess formation and narrowing of the lumen
Slide 125: CONDITIONS OF THE SMALL INTESTINE ASSESSMENT findings for CD 1. Fever 2. Abdominal
distention 3. Diarrhea 4. Colicky abdominal pain 5. Anorexia/N/V 6. Weight loss 7. Anemia
Slide 126: CONDITIONS OF THE LARGE INTESTINE ULCERATIVE COLITIS Ulcerative and inflammatory
condition of the GIT usually affecting the large intestine The colon becomes edematous and develops
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
bleeding ulcerations Scarring develops overtime with impaired water absorption and loss of elasticity
Slide 127: CONDITIONS OF THE LARGE INTESTINE ASSESSMENT findings for UC 1. Anorexia 2. Weight
loss 3. Fever 4. SEVERE diarrhea with Rectal bleeding 5. Anemia 6. Dehydration 7. Abdominal
pain and cramping
Slide 128: NURSING INTERVENTIONS for CD and UC 1. Maintain NPO during the active phase 2.
Monitor for complications like severe bleeding, dehydration, electrolyte imbalance 3. Monitor bowel
sounds, stool and blood studies 4. Restrict activities 5. Administer IVF, electrolytes and TPN if
prescribed
Slide 129: NURSING INTERVENTIONS for CD and UC 6. Instruct the patient to AVOID gas-forming foods,
MILK products and foods such as whole grains, nuts, RAW fruits and vegetables especially SPINACH,
pepper, alcohol and caffeine 7. Diet progression- clear liquid LOW residue, high protein diet 8.
Administer drugs- anti-inflammatory, antibiotics, steroids, bulk-forming agents and vitamin/iron
supplements
Slide 130: CONDITIONS OF THE LARGE INTESTINE APPENDICITIS Inflammation of the vermiform
appendix
Slide 132: CONDITIONS OF THE LARGE INTESTINE APPENDICITIS ETIOLOGY: usually fecalith, lymphoid
hyperplasia, foreign body and helminthic obstruction
Slide 133: CONDITIONS OF THE LARGE INTESTINE APPENDICITIS PATHOPHYSIOLOGY Obstruction of
lumen increased pressure decreased blood supply bacterial proliferation and mucosal
inflammation ischemia necrosis rupture
Slide 134: CONDITIONS OF THE LARGE INTESTINE ASSESSMENT FINDINGS for Appendicitis 1.
Abdominal pain: begins in the umbilicus then localizes in the RLQ (Mc Burney’s point) 2. Anorexia 3.
Nausea and Vomiting
Slide 135: CONDITIONS OF THE LARGE INTESTINE ASSESSMENT FINDINGS for Appendicitis 4. Fever 5.
Rebound tenderness and abdominal rigidity (if perforated) 6. Constipation or diarrhea
Slide 136: CONDITIONS OF THE LARGE INTESTINE DIAGNOSTIC TESTS 1. CBC- reveals increased WBC
count 2. Ultrasound 3. Abdominal X-ray
Slide 137: CONDITIONS OF THE LARGE INTESTINE NURSING INTERVENTIONS 1. Preoperative care NPO
Consent Monitor for perforation and signs of shock
Slide 138: CONDITIONS OF THE LARGE INTESTINE NURSING INTERVENTIONS 1. Preoperative care
Monitor bowel sounds, fever and hydration status POSITION of Comfort: RIGHT SIDELYING in a low
FOWLER’S Avoid Laxatives, enemas & HEAT APPLICATION
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
Slide 139: CONDITIONS OF THE LARGE INTESTINE 2. Post-operative care Monitor VS and signs of
surgical complications Maintain NPO until bowel function returns If rupture occurred, expect drains
and IV antibiotics
Slide 140: CONDITIONS OF THE LARGE INTESTINE 2. Post-operative care POSITION post-op: RIGHT side-
lying, semi- fowler’s to decrease tension on incision, and legs flexed to promote drainage Administer
prescribed pain medications
Slide 141: CONDITIONS OF THE LARGE INTESTINE Hemorrhoids Abnormal dilation and weakness of the
veins of the anal canal Variously classified as Internal or External, Prolapsed, Thrombosed and
Reducible
Slide 142: CONDITIONS OF THE LARGE INTESTINE Hemorrhoids PATHOPHYSIOLOGY Increased pressure
in the hemorrhoidal tissue due to straining, pregnancy, etc dilatation of veins
Slide 143: CONDITIONS OF THE LARGE INTESTINE Internal hemorrhoids These dilated veins lie above
the internal anal sphincter Usually, the condition is PAINLESS
Slide 144: CONDITIONS OF THE LARGE INTESTINE External hemorrhoids These dilated veins lie below
the internal anal sphincter Usually, the condition is PAINFUL
Slide 145: CONDITIONS OF THE LARGE INTESTINE ASSESSMENT findings for Hemorrhoids 1. Internal
hemorrhoids- cannot be seen on the peri-anal area 2. External hemorrhoids- can be seen 3. Bright
red bleeding with each defecation
Slide 146: CONDITIONS OF THE LARGE INTESTINE ASSESSMENT findings for Hemorrhoids 4. Rectal/
perianal pain 5. Rectal itching 6. Skin tags
Slide 147: CONDITIONS OF THE LARGE INTESTINE DIAGNOSTIC TEST 1. Anoscopy 2. Digital rectal
examination
Slide 148: CONDITIONS OF THE LARGE INTESTINE NURSING INTERVENTIONS 1. Advise patient to apply
cold packs to the anal/rectal area followed by a SITZ bath 2. Apply astringent like witch hazel soaks
Slide 149: CONDITIONS OF THE LARGE INTESTINE NURSING INTERVENTIONS 3. Encourage HIGH-fiber
diet and fluids 4. Administer stool softener as prescribed
Slide 150: CONDITIONS OF THE LARGE INTESTINE Post-operative care for hemorrhoidectomy 1.
Position: Prone or Side-lying 2. Maintain dressing over the surgical site
Slide 151: CONDITIONS OF THE LARGE INTESTINE Post-operative care for hemorrhoidectomy 3.
Monitor for bleeding 4. Administer analgesics and stool softeners 5. Advise the use of SITZ bath 3-4
times a day
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
Slide 152: CONDITIONS OF THE LARGE INTESTINE DIVERTICULOSIS AND DIVERTICULITIS Diverticulosis
Abnormal out-pouching of the intestinal mucosa occurring in any part of the LI most commonly in the
sigmoid Diverticulitis Inflammation of the diverticulosis
Slide 153: CONDITIONS OF THE LARGE INTESTINE PATHOPHYSIOLOGY Increased intraluminal pressure,
LOW volume in the lumen and Decreased muscle strength in the colon wall herniation of the colonic
mucosa
Slide 154: CONDITIONS OF THE LARGE INTESTINE ASSESSMENT findings for D/D 1. Left lower Quadrant
pain 2. Flatulence 3. Bleeding per rectum 4. nausea and vomiting 5. Fever 6. Palpable, tender
rectal mass
Slide 155: CONDITIONS OF THE LARGE INTESTINE DIAGNOSTIC STUDIES 1. If no active inflammation,
COLONOSCOPY and Barium Enema 2. CT scan is the procedure of choice! 3. Abdominal X-ray
Slide 156: CONDITIONS OF THE LARGE INTESTINE NURSING INTERVENTIONS 1. Maintain NPO during
acute phase 2. Provide bed rest 3. Administer antibiotics, analgesics like meperidine (morphine is not
used) and anti- spasmodics 4. Monitor for potential complications like perforation, hemorrhage and
fistula 5. Increase fluid intake
Slide 157: CONDITIONS OF THE LARGE INTESTINE NURSING INTERVENTIONS 6. Avoid gas-forming
foods or HIGH- roughage foods containing seeds, nuts to avoid trapping 7. introduce soft, high fiber
foods ONLY after the inflammation subsides 8. Instruct to avoid activities that increase intra-
abdominal pressure
Slide 158: Conditions of the GIT accessory organs The liver
Slide 159: CONDITION OF THE LIVER Liver Cirrhosis A chronic, progressive disease characterized by a
diffuse damage to the hepatic cells The liver heals with scarring, fibrosis and nodular regeneration
Slide 160: CONDITION OF THE LIVER Liver Cirrhosis ETIOLOGY: Post-infection, Alcohol, Cardiac diseases,
Schisostoma, Biliary obstruction
Slide 162: Liver physiology and Pathophysiology Normal Function Abnormality in function 1. Stores
glycogen = Hypoglycemia 2. Synthesizes proteins = Hypoproteinemia 3. Synthesizes globulins
=Decreased Antibody formation 4. Synthesizes Clotting factors = Bleeding tendencies 5. Secreting bile =
Jaundice and pruritus 6. Converts ammonia to urea =Hyperammonemia 7. Stores Vit and minerals
=Deficiencies of Vit and min 8. Metabolizes estrogen = Gynecomastia, testes atrophy
Slide 163: CONDITION OF THE LIVER ASSESSMENT FINDINGS 1. Anorexia and weight loss 2. Jaundice
3. Fatigue
Slide 164: CONDITION OF THE LIVER ASSESSMENT FINDINGS 4. Early morning nausea and vomiting 5.
RUQ abdominal pain 6. Ascites 7. Signs of Portal hypertension
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
Slide 166: CONDITION OF THE LIVER NURSING INTERVENTIONS 1. Monitor VS, I and O, Abdominal
girth, weight, LOC and Bleeding 2. Promote rest. Elevated the head of the bed to minimize dyspnea
Slide 167: CONDITION OF THE LIVER NURSING INTERVENTIONS 3. Provide Moderate to LOW-protein (1
g/kg/day) and LOW-sodium diet 4. Provide supplemental vitamins (especially K) and minerals
Slide 168: CONDITION OF THE LIVER NURSING INTERVENTIONS 5. Administer prescribed Diuretics= to
reduce ascites and edema Lactulose= to reduce NH4 in the bowel Antacids and Neomycin= to kill
bacterial flora that cause NH production
Slide 169: CONDITION OF THE LIVER NURSING INTERVENTIONS 6. Avoid hepatotoxic drugs
Paracetamol Anti-tubercular drugs
Slide 170: CONDITION OF THE LIVER NURSING INTERVENTIONS 7. Reduce the risk of injury Side rails
reorientation Assistance in ambulation Use of electric razor and soft- bristled toothbrush
Slide 171: CONDITION OF THE LIVER NURSING INTERVENTIONS 8. Keep equipments ready including
Sengstaken- Blakemore tube, IV fluids, Medications to treat hemorrhage
Slide 172: CONDITION OF THE LIVER Nursing Interventions Rationale 1. Low sodium Diet To reduce
edema 2. Low protein diet To reduce NH production 3. Benadryl and mild soap To relieve pruritus 4.
Pressure onto injection site To prevent bleeding Done to relieve abdominal pressure 5. Assist in
paracentesis 6. Administer Medications: Diuretics, Neomycin, Lactulose Albumin, Amino acid
Vitamin K (menadione)
Slide 173: Conditions of the Accessory organs The Gallbladder
Slide 174: CONDITION OF THE GALLBLADDER Cholecystitis Inflammation of the gallbladder Can be
acute or chronic
Slide 175: CONDITION OF THE GALLBLADDER Cholecystitis Acute cholecystitis usually is due to
gallbladder stones
Slide 176: CONDITION OF THE GALLBLADDER Cholecystitis Chronic cholecystitis is usually due to long
standing gall bladder inflammation
Slide 178: Cholelithiasis Formation of GALLSTONES in the biliary apparatus
Slide 179: Predisposing FACTORS “F” Female Fat Forty Fertile Fair
Slide 181: Pathophysiology Supersaturated bile, Biliary stasis Stone formation Blockage of Gallbladder
Inflammation, Mucosal Damage and WBC infiltration
Slide 182: Pathophysiology Less bile in the duodenum Impaired fat digestion and absorption Vitamin
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
ADEK mal-absorption, STEATORHEA with increased gas formation Jaundice ACHOLIC stools
Slide 183: CONDITION OF THE GALLBLADDER ASSESSMENT findings for cholecystitis 1. Indigestion,
belching and flatulence 2. Fatty food intolerance, steatorrhea
Slide 184: CONDITION OF THE GALLBLADDER ASSESSMENT findings for cholecystitis 3. Epigastric pain
that radiates to the scapula or localized at the RUQ 4. Mass at the RUQ
Slide 185: CONDITION OF THE GALLBLADDER ASSESSMENT findings for cholecystitis 5. Murphy’s sign
6. Jaundice 7. dark orange and foamy urine
Slide 186: CONDITION OF THE GALLBLADDER DIAGNOSTIC PROCEDURES 1. Ultrasonography- can
detect the stones 2. Abdominal X-ray 3. Cholecystography
Slide 187: CONDITION OF THE GALLBLADDER DIAGNOSTIC PROCEDURES 4. WBC count increased 5.
Oral cholecystography cannot visualize the gallbladder 6. ERCP: revels inflamed gallbladder with
gallstone
Slide 188: CONDITION OF THE GALLBLADDER NURSING INTERVENTIONS 1. Maintain NPO in the active
phase 2. Maintain NGT decompression
Slide 189: CONDITION OF THE GALLBLADDER NURSING INTERVENTIONS 3. Administer prescribed
medications to relieve pain. Usually Demerol (MEPERIDINE) Codeine and Morphine may cause spasm
of the Sphincter increased pain. Morphine cause MOREPAIN
Slide 190: CONDITION OF THE GALLBLADDER 4. Instruct patient to AVOID HIGH- fat diet and GAS-
forming foods 5. Assist in surgical and non- surgical measures 6. Surgical procedures-
Cholecystectomy, Choledochotomy, laparoscopy
Slide 191: CONDITION OF THE GALLBLADDER PHARMACOLOGIC THERAPY Analgesic- Meperidine 2.
Chenodeoxycholic acid= to 3. dissolve the gallstones Antacids 4. Anti-emetics 5.
Slide 194: CONDITION OF THE GALLBLADDER Post-operative nursing interventions 1. Monitor for
surgical complications 2. Post-operative position after recovery from anesthesia- LOW FOWLER’s
Slide 195: CONDITION OF THE GALLBLADDER Post-operative nursing interventions 3. Encourage early
ambulation 4. Administer medication before coughing and deep breathing exercises 5. Advise client
to splint the abdomen to prevent discomfort during coughing
Slide 196: CONDITION OF THE GALLBLADDER Post-operative nursing interventions 6. Administer
analgesics, antiemetics, antacids 7. Care of the biliary drainageor T-tube drainage 8. Fat restriction is
only limited to 4-6 weeks. Normal diet is resumed
Slide 197: Conditions of the accessory organs The pancreas: Exocrine function
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
Slide 198: CONDITION OF THE PANCREAS Pancreatitis Inflammation of the pancreas Can be acute or
chronic
Slide 199: CONDITION OF THE PANCREAS Pancreatitis Etiology and predisposing factors Alcoholism
Hypercalcemia Trauma Hyperlipidemia
Slide 200: CONDITION OF THE PANCREAS Pancreatitis Etiology and predisposing factors Biliary tract
disease - cholelithiasis Bacterial disease PUD Mumps
Slide 201: CONDITION OF THE PANCREAS PATHOPHYSIOLOGY of acute pancreatitis Self-digestion of
the pancreas by its own digestive enzymes principally TRYPSIN
Slide 202: CONDITION OF THE PANCREAS PATHOPHYSIOLOGY of acute pancreatitis Spasm, edema or
block in the Ampulla of Vater reflux of proteolytic enzymes auto digestion of the pancreas
inflammation
Slide 203: CONDITION OF THE PANCREAS PATHOPHYSIOLOGY of acute pancreatitis Autodigestion of
pancreatic tissue Hemorrhage, Necrosis and Inflammation KININ ACTIVATION will result to increased
permeability Loss of Protein-rich fluid into the peritoneum HYPOVOLEMIA
Slide 204: CONDITION OF THE PANCREAS ASSESSMENT findings 1. Abdominal pain- acute onset,
occurring after a heavy meal or alcohol intake 2. Abdominal guarding
Slide 205: CONDITION OF THE PANCREAS ASSESSMENT findings 3. Bruising on the flanks and umbilicus
4. N/V, jaundice 5. Hypotension and hypovolemia 6. HYPERGLYCEMIA, HYPOCALCEMIA 7. Signs
of shock
Slide 206: CONDITION OF THE PANCREAS DIAGNOSTIC TESTS 1. Serum amylase and serum lipase 2.
Ultrasound 3. WBC 4. Serum calcium 5. CT scan 6. Hemoglobin and hematocrit
Slide 207: CONDITION OF THE PANCREAS NURSING INTERVENTIONS 1. Assist in pain management.
Usually, Demerol is given. Morphine is AVOIDED 2. Assist in correction of Fluid and Blood loss
Slide 208: CONDITION OF THE PANCREAS NURSING INTERVENTIONS 3. Place patient on NPO to inhibit
pancreatic stimulation 4. NGT insertion to decompress distention and remove gastric secretions 5.
Maintain on bed rest
Slide 209: CONDITION OF THE PANCREAS NURSING INTERVENTIONS 7. Position patient in SEMI-
FOWLER’s to decrease pressure on the diaphragm 8. Deep breathing and coughing exercises 9.
Provide parenteral nutrition
Slide 210: CONDITION OF THE PANCREAS NURSING INTERVENTIONS 10. Introduce oral feedings
gradually- HIGH carbo, LOW FAT 11. Maintain skin integrity 12. Manage shock and other
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
Gastrointestinal System National University: College of Nursing
complications
Slide 211: Quick Summary Peptic Ulcer Ulceration of mucosa; In the stomach or duodenum
Outstanding Symptom: PAIN Nursing Goal: Allow ulcer to heal, prevent complication Rest: physical
and Mental Eliminate certain foods Medications: antacid, H2 blockers, Proton Pump inhibitors,
antibiotics, mucosal protectants Surgery: Vagotomy, Billroth 1 and 2
Slide 212: Quick Summary Liver Cirrhosis Destruction of liver with replacement by scars Common
causes: alcoholism, post-hepatitic Manifestations related to liver derangements Jaundice, Ascites,
splenomegaly, bleeding, enceph Nursing goal: Control manifestations and maximize liver function
Slide 213: Quick Summary Liver Cirrhosis Encourage rest Avoid hepatotoxic drugs Diet: HIGH
calorie, Restricted protein, LOW Na Weight client and measure abdominal girth daily Provide skin
care for jaundice and edema Assess for bleeding: esophageal, rectal, cutaneous DRUGS: Antacids,
Diuretics, Albumin, Neomycin and Lactulose
Slide 214: Quick Summary Cholecystitis Inflammation of the gallbladder commonly caused by
cholelithiasis (Female, Fat, Forty, Fertile, Fair) Manifestations: Fat intolerance, RUQ pain, Nausea and
vomiting, Jaundice, Murphy’s sign Nursing Goal: Relieve symptoms and assist in stone removal
Slide 215: Quick Summary Cholecystitis Administer MEPERIDINE, avoid morphine Maintain Fluid
and electrolyte balance Maintain a LOW fat diet Semi-fowler’s position Assist in surgery Care of
the T-tube
Slide 216: Quick Summary Pancreatitis Inflammation of the pancreas brought about by the digestion
of the organ by the enzyme it produces Common causes: Alcoholism, stone Manifestations: Extreme
upper abdominal pain radiating into the back, vomiting, nausea, Abdominal distention, Steatorrhea and
weight loss Laboratory: ELEVATED lipase and amylase
Slide 217: Quick Summary Pancreatitis Nursing Goal : relieve symptoms, maintain blood volume and
GIT rest NPO Provide IVF and Parenteral nutrition Drugs: MEPERIDINE, never morphine, Antacids,
anticholinergics After Acute phase: LOW fat diet, avoid alcohol, fat and vitamin replacements
Nurse Licensure Examination Dennis B. Brosola, RN, MSN
S-ar putea să vă placă și
- 2012 Metabolism Harley L. Dela Cruz RN Man InstructorDocument14 pagini2012 Metabolism Harley L. Dela Cruz RN Man InstructorHarley Justiniani Dela CruzÎncă nu există evaluări
- Gastrointestinal SystemDocument218 paginiGastrointestinal Systemnursereview92% (12)
- Endo and Git HandoutsDocument20 paginiEndo and Git HandoutsPhilip Simangan100% (1)
- Git DisturbancesDocument119 paginiGit DisturbancesPeterpan NguyenÎncă nu există evaluări
- Medical Surgical Nursing The Gastro-Intestinal System Nurse Licensure Examination Review By: John Mark B. Pocsidio, RN, Usrn, MSNDocument22 paginiMedical Surgical Nursing The Gastro-Intestinal System Nurse Licensure Examination Review By: John Mark B. Pocsidio, RN, Usrn, MSNjm_pocsidio8213Încă nu există evaluări
- Git NursingDocument245 paginiGit NursingWeng Maesa MontemayorÎncă nu există evaluări
- AnaPhy, IBD and Ulcerative ColitisDocument12 paginiAnaPhy, IBD and Ulcerative ColitisabdulhafezjamasariÎncă nu există evaluări
- Week 11 Gastrointestinal SystemDocument73 paginiWeek 11 Gastrointestinal Systemashwaaq9999Încă nu există evaluări
- Git HandoutsDocument49 paginiGit HandoutsCharlz Zipagan100% (1)
- Topic 1 MetaDocument68 paginiTopic 1 MetaArvin LazarteÎncă nu există evaluări
- What Is The Digestive System? The GI Tract: REMEMBER: Bacteria in Your GI Tract, Also Called Gut Flora orDocument10 paginiWhat Is The Digestive System? The GI Tract: REMEMBER: Bacteria in Your GI Tract, Also Called Gut Flora orTrương TríÎncă nu există evaluări
- ADN3-1 Digestive HP - 200 - Yang, Myung SookDocument37 paginiADN3-1 Digestive HP - 200 - Yang, Myung SookNorPhea - នភាÎncă nu există evaluări
- Peptic Ulcer Disease NCLEX ReviewDocument16 paginiPeptic Ulcer Disease NCLEX ReviewBianca Trish ManlangitÎncă nu există evaluări
- Case Study Report (Peptic Ulcer) Group 1Document9 paginiCase Study Report (Peptic Ulcer) Group 1Khrizlynne SoberanoÎncă nu există evaluări
- Medsurg Gi AnaphysioDocument13 paginiMedsurg Gi AnaphysioNermeen Mudsol100% (1)
- EBL Case 6Document4 paginiEBL Case 6T LolaÎncă nu există evaluări
- Lecture 15 Bowl EliminationDocument72 paginiLecture 15 Bowl EliminationIsbelÎncă nu există evaluări
- 16 Digestive SystemDocument4 pagini16 Digestive SystemOribello, Athenna Jae W.Încă nu există evaluări
- Metabolism (Ncm-216)Document10 paginiMetabolism (Ncm-216)Sofronio OmboyÎncă nu există evaluări
- Gastrointestinal System Review of Systems: (Image Taken From Medical-Surgical Nursing, M. Hogan & T. Madayag)Document26 paginiGastrointestinal System Review of Systems: (Image Taken From Medical-Surgical Nursing, M. Hogan & T. Madayag)pawnayÎncă nu există evaluări
- GROUP 11 Problem 1-2Document85 paginiGROUP 11 Problem 1-2Shitta InayahÎncă nu există evaluări
- Biopharmaceutics-01 AssignmentDocument14 paginiBiopharmaceutics-01 AssignmentRA TanvirÎncă nu există evaluări
- Case Study Ugib Lower MBDocument65 paginiCase Study Ugib Lower MBQuolette Constante100% (1)
- The Digestive System: G.R. Pitts, PH.D., J.R. Schiller, Ph.D. and James F. Thompson, PH.DDocument54 paginiThe Digestive System: G.R. Pitts, PH.D., J.R. Schiller, Ph.D. and James F. Thompson, PH.DAchmadPrihadianto100% (1)
- Digestive SystemDocument117 paginiDigestive SystemKBDÎncă nu există evaluări
- Ii. Diagnostic TestDocument93 paginiIi. Diagnostic TestFarisa Jane BanggoÎncă nu există evaluări
- Digestive System - MefloresDocument117 paginiDigestive System - MefloresJohnMichaelDominguezÎncă nu există evaluări
- Digestive SystemDocument55 paginiDigestive SystemPradeep KonduriÎncă nu există evaluări
- 9 Assessment of Gastrointestinal Function and Management of Gastrointestinal DisordersDocument61 pagini9 Assessment of Gastrointestinal Function and Management of Gastrointestinal DisordersNoor MajaliÎncă nu există evaluări
- Nursing Care Management of Clients With Gastrointestinal DisordersDocument50 paginiNursing Care Management of Clients With Gastrointestinal DisordersAriane-Gay Cristobal DuranÎncă nu există evaluări
- Obj, Intro, AnaDocument5 paginiObj, Intro, AnaarnieÎncă nu există evaluări
- All About GIT PhysiologyDocument79 paginiAll About GIT PhysiologyHarshavardhan AmancherlaÎncă nu există evaluări
- What Is Peptic Ulcer Disease?: Three Types of Peptic UlcersDocument56 paginiWhat Is Peptic Ulcer Disease?: Three Types of Peptic UlcersAsniah Hadjiadatu AbdullahÎncă nu există evaluări
- By124l Case Study 2Document2 paginiBy124l Case Study 2ashlyn granthamÎncă nu există evaluări
- Gastric Secretion-FinalDocument107 paginiGastric Secretion-FinalDr.Gomathi sivakumarÎncă nu există evaluări
- Gi SystemDocument73 paginiGi SystemSeema SachdevaÎncă nu există evaluări
- Digestive SystemDocument58 paginiDigestive SystemseibdÎncă nu există evaluări
- Common Laboratory ProceduresDocument4 paginiCommon Laboratory ProceduresLheidaniel MMM.Încă nu există evaluări
- Comprehensive Notes of The Topic Covered For 4th ExamDocument10 paginiComprehensive Notes of The Topic Covered For 4th ExamZhailyn Joy DumlaoÎncă nu există evaluări
- II. Anatomy and PhysiologyDocument16 paginiII. Anatomy and PhysiologyLee Cel100% (1)
- Case Presentation (NCM 102)Document26 paginiCase Presentation (NCM 102)Ibs LimÎncă nu există evaluări
- Pencernaan FaalDocument82 paginiPencernaan FaalhardianÎncă nu există evaluări
- Digestive SystemDocument9 paginiDigestive SystemJhomar B, Dela CruzÎncă nu există evaluări
- 1 Pud CD UcDocument14 pagini1 Pud CD UcCorpus, Irene Zen P.Încă nu există evaluări
- GI System and Its Disorders (Nurses Perspective)Document23 paginiGI System and Its Disorders (Nurses Perspective)aswathykrishnan73100% (3)
- دمج شباتر البالغين .....Document511 paginiدمج شباتر البالغين .....Abdallah AlasalÎncă nu există evaluări
- Chapter 2 Gastrointestinal SystemDocument11 paginiChapter 2 Gastrointestinal SystemPersonne AnonymeÎncă nu există evaluări
- GI HandoutsDocument9 paginiGI Handoutsjeannine_ledesmaÎncă nu există evaluări
- SN 212Document59 paginiSN 212Daroo D.TÎncă nu există evaluări
- Alimentary and Biliary Conditions 3-1Document249 paginiAlimentary and Biliary Conditions 3-1Mercy KeruboÎncă nu există evaluări
- Digestive SystemDocument3 paginiDigestive SystemDarwin CauilanÎncă nu există evaluări
- The Digestive SystemDocument44 paginiThe Digestive SystemJoy NatividadÎncă nu există evaluări
- Chemically Digested To Small Molecules That AreDocument14 paginiChemically Digested To Small Molecules That AreVarun WadhwaÎncă nu există evaluări
- Glossary Key PointsDocument3 paginiGlossary Key PointsbxyrtbgyxcÎncă nu există evaluări
- Section P - Group 1 E.C.S. - Pediatric Ward Mr. Ralph P. Pilapil, R.N. Clinical InstructorDocument62 paginiSection P - Group 1 E.C.S. - Pediatric Ward Mr. Ralph P. Pilapil, R.N. Clinical InstructorClaudine N SantillanÎncă nu există evaluări
- Learning Objectives:: at The End of This Lecture, You Will Be Able ToDocument119 paginiLearning Objectives:: at The End of This Lecture, You Will Be Able ToMaica LectanaÎncă nu există evaluări
- Stomach: Dr. Aulia Janer Tutor: Dr. Anbiar Manjas, SP.B KBDDocument47 paginiStomach: Dr. Aulia Janer Tutor: Dr. Anbiar Manjas, SP.B KBDardhom122Încă nu există evaluări
- Medical-Surgical Nursing (Gastrointestinal)Document1 paginăMedical-Surgical Nursing (Gastrointestinal)アンナドミニクÎncă nu există evaluări
- Psychiatric NursingDocument32 paginiPsychiatric NursingPinky Cuaresma100% (1)
- Cancer Nursing:: Medical Surgical Nursing:: Review For Nursing Licensure ExaminationDocument7 paginiCancer Nursing:: Medical Surgical Nursing:: Review For Nursing Licensure ExaminationPinky CuaresmaÎncă nu există evaluări
- Genito Urinary SystemDocument8 paginiGenito Urinary SystemPinky CuaresmaÎncă nu există evaluări
- Neuro DisordersDocument11 paginiNeuro DisordersPinky CuaresmaÎncă nu există evaluări
- Musculoskeletal SystemDocument10 paginiMusculoskeletal SystemPinky CuaresmaÎncă nu există evaluări
- What Is A Green School Sinta Rahayu - 4401416068 - P.Bio 1Document5 paginiWhat Is A Green School Sinta Rahayu - 4401416068 - P.Bio 1Lia RistyÎncă nu există evaluări
- Online AssignmentDocument9 paginiOnline AssignmentAnonymous Sodimy5Încă nu există evaluări
- Relative Effect of Particle Size On The Physical Properties of Corn Meal Extrudates: Effect of Particle Size On The Extrusion of Corn MealDocument7 paginiRelative Effect of Particle Size On The Physical Properties of Corn Meal Extrudates: Effect of Particle Size On The Extrusion of Corn MealWilliam Yesid Diaz AvilaÎncă nu există evaluări
- Quiz On Hypertension-22March2013Document5 paginiQuiz On Hypertension-22March2013MEÎncă nu există evaluări
- Biscuits and Candy Manufacturing Industry-787831 PDFDocument73 paginiBiscuits and Candy Manufacturing Industry-787831 PDFdawitÎncă nu există evaluări
- Recipe BookDocument2 paginiRecipe Bookesca_eliÎncă nu există evaluări
- MythicalStrength Random ThoughtsDocument61 paginiMythicalStrength Random Thoughtsbarna284Încă nu există evaluări
- Appeal For DonationDocument3 paginiAppeal For DonationshaheedaazmaÎncă nu există evaluări
- Mother and Child Protection Card (MCP Card)Document40 paginiMother and Child Protection Card (MCP Card)Venkat67% (3)
- Daily Price Monitoring: Retail Prices of Selected Agri-Fishery Commodities in Selected Markets in Metro ManilaDocument3 paginiDaily Price Monitoring: Retail Prices of Selected Agri-Fishery Commodities in Selected Markets in Metro ManilaRio CorralÎncă nu există evaluări
- Basic DialoguesDocument131 paginiBasic DialoguesElizabeth Simão MiguensÎncă nu există evaluări
- Get swole cụ thểDocument34 paginiGet swole cụ thểVi Khuu NguyenÎncă nu există evaluări
- Stern Rams in Antiquity PDFDocument522 paginiStern Rams in Antiquity PDFfoxeosÎncă nu există evaluări
- Class 6 1 PDFDocument4 paginiClass 6 1 PDFBrittomanoharÎncă nu există evaluări
- Grammar Book (Grade 8)Document124 paginiGrammar Book (Grade 8)Vinh NguyenÎncă nu există evaluări
- 2 LP in Creative WritingDocument3 pagini2 LP in Creative WritingMeceri Jane Dacuran SilvioÎncă nu există evaluări
- WIDGB1 - Rtest - Language - 1 - REVISIONDocument5 paginiWIDGB1 - Rtest - Language - 1 - REVISIONSanjaÎncă nu există evaluări
- How To Find Truffles in The ForestDocument4 paginiHow To Find Truffles in The Forestadiomanovic1Încă nu există evaluări
- Sistem: Pengurusan Halal Malaysia - MhmsDocument9 paginiSistem: Pengurusan Halal Malaysia - MhmsAzurah Abdul AzizÎncă nu există evaluări
- Collocations List: Collocations Are Very Common in English, and Learning Them Is Important. ADocument50 paginiCollocations List: Collocations Are Very Common in English, and Learning Them Is Important. AVillMa ABÎncă nu există evaluări
- AMIGOS Business PlanDocument10 paginiAMIGOS Business PlanyakarimÎncă nu există evaluări
- Tree of LifeDocument909 paginiTree of LifeMariza D. KabamaruÎncă nu există evaluări
- Crop Upper Gibe Jimma AbrahamDocument38 paginiCrop Upper Gibe Jimma AbrahamRamon ColonÎncă nu există evaluări
- Unit 6 PastryDocument29 paginiUnit 6 PastryRicardo HarveyÎncă nu există evaluări
- Pilgrimage of The El RocioDocument3 paginiPilgrimage of The El RociopasferacosÎncă nu există evaluări
- The Indian Diet Plan To Lose Weight - My Health Tips PDFDocument15 paginiThe Indian Diet Plan To Lose Weight - My Health Tips PDFRAGHAVENDRAÎncă nu există evaluări
- Coca Cola ProjectDocument96 paginiCoca Cola ProjectAjay KumarÎncă nu există evaluări
- Tirupati Balaji Darshan Short Travel GuideDocument7 paginiTirupati Balaji Darshan Short Travel GuideAvinash SinghÎncă nu există evaluări
- Paleothitic DietDocument7 paginiPaleothitic DietD HernandezÎncă nu există evaluări
- Egg Powder BriefDocument3 paginiEgg Powder Briefhadi wijayaÎncă nu există evaluări