Documente Academic
Documente Profesional
Documente Cultură
Peritonitis
Încărcat de
Dhiya Rahadian0 evaluări0% au considerat acest document util (0 voturi)
14 vizualizări2 paginiperitonitis
Drepturi de autor
© © All Rights Reserved
Formate disponibile
DOCX, PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentperitonitis
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca DOCX, PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
14 vizualizări2 paginiPeritonitis
Încărcat de
Dhiya Rahadianperitonitis
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca DOCX, PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 2
Background
Peritonitis is defined as an inflammation of the serosal membrane that
lines the abdominal cavity and the organs contained therein. The
peritoneum, which is an otherwise sterile environment, reacts to various
pathologic stimuli with a fairly uniform inflammatory response. Depending
on the underlying pathology, the resultant peritonitis may be infectious or
sterile (ie, chemical or mechanical). The abdomen is the second most
common source of sepsis and secondary peritonitis. [1]Intra-abdominal
sepsis is an inflammation of the peritoneum caused by pathogenic
microorganisms and their products. [2] The inflammatory process may be
localized (abscess) or diffuse in nature.
Peritonitis is most often caused by introduction of an infection into the
otherwise sterile peritoneal environment through organ perforation, but it
may also result from other irritants, such as foreign bodies, bile from a
perforated gall bladder or a lacerated liver, or gastric acid from a
perforated ulcer. Women also experience localized peritonitis from an
infected fallopian tube or a ruptured ovarian cyst. Patients may present
with an acute or insidious onset of symptoms, limited and mild disease, or
systemic and severe disease with septic shock.
Peritoneal infections are classified as primary (ie, from hematogenous
dissemination, usually in the setting of an immunocompromised state),
secondary (ie, related to a pathologic process in a visceral organ, such as
perforation or trauma, including iatrogenic trauma), or tertiary (ie,
persistent or recurrent infection after adequate initial therapy). Primary
peritonitis is most often spontaneous bacterial peritonitis (SBP) seen
mostly inpatients with chronic liver disease. Secondary peritonitis is by far
the most common form of peritonitis encountered in clinical practice.
Tertiary peritonitis often develops in the absence of the original visceral
organ pathology.
Infections of the peritoneum are further divided into generalized
(peritonitis) and localized (intra-abdominal abscess). This article focuses
on the diagnosis and management of infectious peritonitis and abdominal
abscesses. An abdominal abscess is seen in the image below.
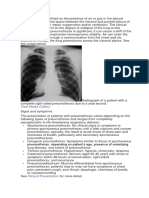
Peritonitis and abdominal sepsis. A 35-year-old man
with a history of Crohn disease presented with pain and swelling in the
right abdomen. In figure A, a thickened loop of terminal ileum is evident
adherent to the right anterior abdominal wall. In figure B, the right anterior
abdominal wall is markedly thickened and edematous, with adjacent
inflamed terminal ileum. In figure C, a right lower quadrant abdominal wall
abscess and enteric fistula are observed and confirmed by the presence
of enteral contrast in the abdominal wall.
The diagnosis of peritonitis is usually clinical. Diagnostic peritoneal
lavage may be helpful in patients who do not have conclusive signs on
physical examination or who cannot provide an adequate history; in
addition, paracentesis should be performed in all patients who do not
have an indwelling peritoneal catheter and are suspected of having SBP,
because results of aerobic and anaerobic bacterial cultures, used in
conjunction with the cell count, are useful in guiding therapy.
The management approach to peritonitis and peritoneal abscesses
targets correction of the underlying process, administration of systemic
antibiotics, and supportive therapy to prevent or limit secondary
complications due to organ system failure.
Early control of the septic source is mandatory and can be achieved
operatively and nonoperatively. Nonoperative interventions include
percutaneous abscess drainage, as well as percutaneous and
endoscopic stent placements. Operative management addresses the
need to control the infectious source and to purge bacteria and toxins.
The type and extent of surgery depends on the underlying disease
process and the severity of intra-abdominal infection.
SOURCE : emedicine.medscape.com
S-ar putea să vă placă și
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (119)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (587)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2219)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (894)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (73)
- Drug Study CISPLATINDocument2 paginiDrug Study CISPLATINCorrine IvyÎncă nu există evaluări
- Celecoxib uses, dosage, side effectsDocument4 paginiCelecoxib uses, dosage, side effectsAbigail LonoganÎncă nu există evaluări
- Dermatology Final Questions (2010-2012Document72 paginiDermatology Final Questions (2010-2012Rashed ShatnawiÎncă nu există evaluări
- AmebiasisDocument16 paginiAmebiasisNagendra NayakÎncă nu există evaluări
- LithiumDocument4 paginiLithiumapi-3797941100% (1)
- Guide to Henoch Schönlein Purpura (HSPDocument2 paginiGuide to Henoch Schönlein Purpura (HSPDhiya RahadianÎncă nu există evaluări
- Hemoptysis Following A Chronic IllnessDocument2 paginiHemoptysis Following A Chronic IllnessDhiya RahadianÎncă nu există evaluări
- Achalasia Treatment and DiagnosisDocument2 paginiAchalasia Treatment and DiagnosisDhiya RahadianÎncă nu există evaluări
- View Media GalleryDocument2 paginiView Media GalleryDhiya RahadianÎncă nu există evaluări
- ParonikiaDocument1 paginăParonikiaDhiya RahadianÎncă nu există evaluări
- SGD LBM 1 THT DhiyaDocument13 paginiSGD LBM 1 THT DhiyaDhiya Rahadian100% (1)
- ParonikiaDocument1 paginăParonikiaDhiya RahadianÎncă nu există evaluări
- My Baby Look JaundiceDocument4 paginiMy Baby Look JaundiceDhiya RahadianÎncă nu există evaluări
- LBM 4Document2 paginiLBM 4Dhiya RahadianÎncă nu există evaluări
- Streptococcal PharyngitisDocument28 paginiStreptococcal PharyngitisDhiya RahadianÎncă nu există evaluări
- 4 Asma Stepwise ApproachDocument1 pagină4 Asma Stepwise ApproachbrianÎncă nu există evaluări
- Daftar Harga Generik dan Non-Generik dari PT Sapta Sari TamaDocument70 paginiDaftar Harga Generik dan Non-Generik dari PT Sapta Sari Tamanaelarizqi0% (1)
- Acetaminophen, ParacetamolDocument2 paginiAcetaminophen, ParacetamolAubrey Unique Evangelista100% (2)
- Invasive Group A Streptococcal Disease Fact SheetDocument2 paginiInvasive Group A Streptococcal Disease Fact SheetCityNewsTorontoÎncă nu există evaluări
- Neurology 40 KochiDocument9 paginiNeurology 40 KochiSrirupa BiswasÎncă nu există evaluări
- DOMINGO - OB RequirmentsDocument10 paginiDOMINGO - OB RequirmentsJick Esteva de VicenteÎncă nu există evaluări
- AntibiotikDocument3 paginiAntibiotikFeny OktariaÎncă nu există evaluări
- Child's Abdominal Pain Admitting ConferenceDocument24 paginiChild's Abdominal Pain Admitting ConferenceRaul MangrobangÎncă nu există evaluări
- Pengiriman Tanggal 23 Mei 2017: No No Faktur Produk QTY HNA ValueDocument20 paginiPengiriman Tanggal 23 Mei 2017: No No Faktur Produk QTY HNA Valuesiti fauziyantiÎncă nu există evaluări
- CVX CodesDocument16 paginiCVX CodesansarÎncă nu există evaluări
- CotrimoxazoleDocument2 paginiCotrimoxazoleKeri AyomiÎncă nu există evaluări
- 10 Communicable DiseasesDocument3 pagini10 Communicable DiseasesPauline de VeraÎncă nu există evaluări
- Dosis Obat Untuk AnakDocument15 paginiDosis Obat Untuk AnakBudi SantosoÎncă nu există evaluări
- Stok 5 April 2021 Ogb Dexa: Stock Product - DescDocument8 paginiStok 5 April 2021 Ogb Dexa: Stock Product - DescBelza ChristianÎncă nu există evaluări
- 5a's 5R's Motivational InterviewingDocument2 pagini5a's 5R's Motivational Interviewingbkano100% (1)
- Infectious or Communicable Diseases: TuberculosisDocument7 paginiInfectious or Communicable Diseases: TuberculosischandraÎncă nu există evaluări
- Daftar Nama ObatDocument5 paginiDaftar Nama ObatGabriyah HamzahÎncă nu există evaluări
- Integrated Management of Childhood Illness: Child Aged 2 Months Up To 5 YearsDocument44 paginiIntegrated Management of Childhood Illness: Child Aged 2 Months Up To 5 YearsJulio Iñigo López100% (22)
- PMSMA Excel FORMATSDocument10 paginiPMSMA Excel FORMATSsri sri100% (1)
- Medication List with Dosages Less Than 40 CharactersDocument6 paginiMedication List with Dosages Less Than 40 CharactersArya WiradewaÎncă nu există evaluări
- No Tanggal No. Kartu Nama Pes Sex Jenis Pes Diagnosa: MastayahDocument33 paginiNo Tanggal No. Kartu Nama Pes Sex Jenis Pes Diagnosa: MastayahIc-tika Siee ChuabbieÎncă nu există evaluări
- Anemia & HemobionDocument56 paginiAnemia & HemobionMar'atus SholikahÎncă nu există evaluări
- CKD 2016Document39 paginiCKD 2016husnaÎncă nu există evaluări
- Essential Drugs PDFDocument363 paginiEssential Drugs PDFdanpmorÎncă nu există evaluări
- Harga ObatDocument21 paginiHarga ObatRizamdhani AptÎncă nu există evaluări