Documente Academic
Documente Profesional
Documente Cultură
ABC of Breast Diseases Breast Cancer
Încărcat de
Heldrian D SuyuthieDrepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
ABC of Breast Diseases Breast Cancer
Încărcat de
Heldrian D SuyuthieDrepturi de autor:
Formate disponibile
ABC ofBreast Diseases
BREAST CANCER
J R C Sainsbury, T J Anderson, D A L Morgan, J M Dixon
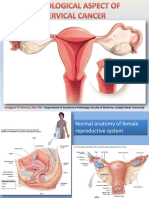
Breast cancers are derived from the epithelial cells that line the
terminal duct lobular unit. Cancer cells that remain within the
basement membrane of the elements of the terminal duct lobular unit
a Wandg the draining duct are classified as in situ or non-invasive. An
invasive breast cancer is one in which there is dissemination of cancer
| g fW4cells
> r Xf
outside the basement membrane of the ducts and lobules into the
surrounding adjacent normal tissue. Both in situ and invasive cancers
have characteristic patterns by which they can be classified.
Carcinoma in situ affecting a breast
lobule.
Classification of invasive breast cancers
The most commonly used classification of invasive breast cancers
Classification of invasive breast divides them into ductal and lobular types. This classification was
cancers based on the belief that ductal carcinomas arose from ducts and
Special types lobular carcinomas from lobules. We now know that invasive ductal
* Tubular * Cribriform * Medullary and lobular breast cancers both arise from the terminal duct lobular
* Mucoid * Papillary * Classic Lobular unit, and this terminology is no longer appropriate. Some tumours
show distinct patterns of growth and cellular morphology, and on this
No special type basis certain types of breast cancer can be identified. Those with
othermmse slyknoed) as NST or NOS (not specific features are called invasive carcinomas of special type, while
* Useful prognostic information can be the remainder are considered to be of no special type.This
gained by grading such cancers classification has clinical relevance in that certain special type tumours
have a much better prognosis than tumours that are of no special type.
I lnvasve carcinomas showing diffuse infiltration through breast tissue: grade I (left), grade 11 (centre), and grade Ill (right).
Tumour differentiation
ugrade Among the cancers of no special type, prognostic information can be
gained by grading the degree of differentiation of the tumour. Degrees
of glandular formation, nuclear pleomorphism, and frequency of
mitoses are scored from 1 to 3. For example, a tumour with many
glands would score 1 whereas a tumour with no glands would score 3.
11 These values are combined and converted into three groups: grade I
_(score
Ill - 3-5), grade II (scores 6 and 7), and grade III (scores 8 and 9).
This derived histological grade-often known as the Bloom and
Richardson grade or the Scarff, Bloom, and Richardson grade after the
originators of this system-is an important predictor of both disease
liarvii
aoudi :AVngIlII
v UvaO fnintr with invaqivo CaZL n:nr-pr
hrnsct
Ivaalve U to t1uu;g free and overall survival.
according to tumour grade.
1150 BMJ VOLUME 309 29 OCTOBER 1994
, 44
:;;:;K Otherfeatures
Other histological features in the primary tumour are also of value in
predicting local recurrence and prognosis.
Lymphatic or vascular invasion-The presence of cancer cells in blood
or lymphatic vessels is a marker of more aggressive disease, and
patienits with this feature are at increased risk of both local and
systemic recurrence.
Extensive in situ component-If more than 25% of the main tumour
mass contains non-invasive disease and there is in situ cancer in the
surrounding breast tissue the cancer is classified as having an extensive
of * in situ component. Patients with such tumours are more likely to
Tumour cells in lymphatic or vascular space. develop local recurrence after breast conserving treatment.
Staging of invasive breast cancers
TNM classification of breast tumours Correlation of UICC (1987) and
TNM classifications of tumours
Ti. Cancer in situ
UICC stage TNM classification
T, s2 cm (Tl. s0.5 cm, Tlb >0.5 cm-1 cm, T,c >1 cm-2 cm)
T2 >2cm-5 cm I Tl, No, Mo
T3 >5cm 11 Tl, Nl, Mo; T2, NO,, Mo
T4a Involvement of chest wall III any T, N23, MO; T3, any N, MO;
T4b Involvement of skin (includes ulceration, direct infiltration, peau T4, any N, MO
d'orange, and satellite nodules) IV any T, any N, M
T4. T4. and T4b together
T4d Inflammatory cancer
No No regional node metastases When an invasive breast cancer is
N, Palpable ipsilateral axillary nodes diagnosed the extent of the disease should be
N2 Fixed ipsilateral axillary nodes assessed and the tumour staged. The two
N3 Ipsilateral internal mammary node involvement (rarely clinically staging classifications in current use are not
detectable)
Mo No evidence of metastasis well suited to breast cancer: the tumour node
M, Distant metastasis (includes ipsilateral supraclavicular nodes) metastases (TNM) system depends on clinical
measurements and clinical assessment of
lymph node status, both of which are
inaccurate, and the International Union
Against Cancer (UICC) system incorporates
the TNM classification. To improve the
TNM system, a separatepathological
classification has recently been added; this
allows tumour size and node status, as
assessed by a pathologist, to be taken into
account. Prognosis in breast cancer relates to
the stage of the disease at presentation.
To ensure that there is no gross evidence of disease all patients with
invasive breast cancer should have a full blood count, liver function
tests, and a chest radiograph. Patients with stage I and stage II disease
have a low incidence of detectable metastatic disease, and in the
absence of abnormal results of liver function tests or specific signs or
II
symptoms they should not undergo further investigations to assess
according to stage of disease.
41 metastatic disease. Patients with bigger or more advanced tumours
should be considered for bone and liver scans if these could lead to a
change in clinical management.
Surgical treatment of localised breast cancer
Most patients will have a combination of local treatments to control
local disease and systemic treatment for any micrometastatic disease.
Local treatments consist of surgery and radiotherapy. Surgery can be
Risk factors for local recurrence of an excision of the tumour with surrounding normal breast tissue
cancer after breast conservation (breast conservation surgery) or a mastectomy.
Relative Certain clinical and pathological factors may influence selection for
Factor risk breast conservation or mastectomy because of their impact on local
Involved margins x3 recurrence after breast conserving therapy. These include an
Extensive in situ component x3 incomplete initial excision, young age, the presence of an extensive in
Patient's age <35 (v age >50) x3 situ component, the presence of lymphatic or vascular invasion, and
Lymphatic or vascular invasion x2 histological grade. Young patients are more to likely localdevelop
recurrence than older patients, but this is probably because young
patients are more likely to have tumours that have an extensive in situ
component, have lymphatic or vascular invasion, and are of high grade.
BMJ voLumE 309 29 OCTOBER 1994 1 151
, 44
:;;:;K Otherfeatures
Other histological features in the primary tumour are also of value in
predicting local recurrence and prognosis.
Lymphatic or vascular invasion-The presence of cancer cells in blood
or lymphatic vessels is a marker of more aggressive disease, and
patienits with this feature are at increased risk of both local and
systemic recurrence.
Extensive in situ component-If more than 25% of the main tumour
mass contains non-invasive disease and there is in situ cancer in the
surrounding breast tissue the cancer is classified as having an extensive
of * in situ component. Patients with such tumours are more likely to
Tumour cells in lymphatic or vascular space. develop local recurrence after breast conserving treatment.
Staging of invasive breast cancers
TNM classification of breast tumours Correlation of UICC (1987) and
TNM classifications of tumours
Ti. Cancer in situ
UICC stage TNM classification
T, s2 cm (Tl. s0.5 cm, Tlb >0.5 cm-1 cm, T,c >1 cm-2 cm)
T2 >2cm-5 cm I Tl, No, Mo
T3 >5cm 11 Tl, Nl, Mo; T2, NO,, Mo
T4a Involvement of chest wall III any T, N23, MO; T3, any N, MO;
T4b Involvement of skin (includes ulceration, direct infiltration, peau T4, any N, MO
d'orange, and satellite nodules) IV any T, any N, M
T4. T4. and T4b together
T4d Inflammatory cancer
No No regional node metastases When an invasive breast cancer is
N, Palpable ipsilateral axillary nodes diagnosed the extent of the disease should be
N2 Fixed ipsilateral axillary nodes assessed and the tumour staged. The two
N3 Ipsilateral internal mammary node involvement (rarely clinically staging classifications in current use are not
detectable)
Mo No evidence of metastasis well suited to breast cancer: the tumour node
M, Distant metastasis (includes ipsilateral supraclavicular nodes) metastases (TNM) system depends on clinical
measurements and clinical assessment of
lymph node status, both of which are
inaccurate, and the International Union
Against Cancer (UICC) system incorporates
the TNM classification. To improve the
TNM system, a separatepathological
classification has recently been added; this
allows tumour size and node status, as
assessed by a pathologist, to be taken into
account. Prognosis in breast cancer relates to
the stage of the disease at presentation.
To ensure that there is no gross evidence of disease all patients with
invasive breast cancer should have a full blood count, liver function
tests, and a chest radiograph. Patients with stage I and stage II disease
have a low incidence of detectable metastatic disease, and in the
absence of abnormal results of liver function tests or specific signs or
II
symptoms they should not undergo further investigations to assess
according to stage of disease.
41 metastatic disease. Patients with bigger or more advanced tumours
should be considered for bone and liver scans if these could lead to a
change in clinical management.
Surgical treatment of localised breast cancer
Most patients will have a combination of local treatments to control
local disease and systemic treatment for any micrometastatic disease.
Local treatments consist of surgery and radiotherapy. Surgery can be
Risk factors for local recurrence of an excision of the tumour with surrounding normal breast tissue
cancer after breast conservation (breast conservation surgery) or a mastectomy.
Relative Certain clinical and pathological factors may influence selection for
Factor risk breast conservation or mastectomy because of their impact on local
Involved margins x3 recurrence after breast conserving therapy. These include an
Extensive in situ component x3 incomplete initial excision, young age, the presence of an extensive in
Patient's age <35 (v age >50) x3 situ component, the presence of lymphatic or vascular invasion, and
Lymphatic or vascular invasion x2 histological grade. Young patients are more to likely localdevelop
recurrence than older patients, but this is probably because young
patients are more likely to have tumours that have an extensive in situ
component, have lymphatic or vascular invasion, and are of high grade.
BMJ voLumE 309 29 OCTOBER 1994 1 151
Breast conservation surgery
Relation between age and local Breast conservation surgery may consist of excision of the tumour
recurrence of cancer after breast with a 1 cm margin of normal tissue (wide local excision) or a more
conservation extensive excision of a whole quadrant of the breast (quadrantectomy).
Age (years) Local recurrence
The wider the excision the lower the recurrence rate but the worse the
after five years cosmetic result. There is no size limit for breast conservation surgery,
<35 17% but adequate excision of lesions over 4 cm produces a poor cosmetic
35-50 12% result in most women; thus breast tends to be limited to lesions of 4
>50 6%
cm or less. There is no age limit for breast conservation.
Factors affecting cosmetic outcome-Wider excisions give poorer
cosmetic results, and excision of any skin overlying the cancer also
Breast cancers suitable for affects the cosmetic result. For this reason only dimpled or retracted
treatment by breast conservation skin overlying a localised breast cancer should be excised. Operations
* Single clinical and mammographic lesion performed in specialist breast units seem to have better cosmetic
* Tumour s4 cm in diameter results than those performed in non-specialist units. Other factors that
* No sign of local advancement (T,, T, <4 influence cosmetic outcome include clearance of axillary nodes and
cm),extensive nodal involvement (No, N1), or delivery of a radiotherapy boost to the tumour bed.
metastases (M0)
* Tumour >4 cm in large breast
Mastectomy
About a third of localised breast cancers are unsuitable for treatment
by breast conservation but can be treated by mastectomy, and some
patients who are suitable for breast conservation surgery opt for
Patients who are best treated by mastectomy. Mastectomy removes the breast tissue with some
mastectomy overlying skin, usually including the nipple. The breast is removed
* Those who prefer treatment by mastectomy from the chest wall muscles (pectoralis major, rectus abdominus, and
* Those for whom breast conservation serratus anterior), which are left intact. Mastectomy should be
treatment would produce an unacceptable combined with some form of axillary surgery.
cosmetic result (includes most central lesions
and carcinomas >4 cm in diameter, although
breast conserving surgery is now possible if
these lesions are successfully treated by
primary systemic therapy) Common complications after mastectomy include formation of seroma,
* Those with either clinical or mammographic infection, and flap necrosis. Collection of fluid under mastectomy flaps
evidence of more than one focus of cancer in after suction drains have been removed (seroma) occurs in a third to a
the breast half of all patients. It is more common after a mastectomy and axillary
node clearance than after mastectomy and node sampling. The seroma
can be aspirated if it is troublesome. Infection after mastectomy is
uncommon, and when it occurs it is usually secondary to flap necrosis.
Occasionally the areas of necrotic skin need to be excised and skin
grafts applied. Most patients treated by mastectomy are suitable for
some form of breast reconstruction, which should ideally be performed
at the same time as the initial mastectomy.
Factors associated with
increased rates of local
recurrence after mastectomy
* Axillary lymph node involvement
* Lymphatic or vascular invasion by cancer
* Grade Ill carcinoma Follow up of patients after surgery
* Tumour >4 cm in diameter (pathological)
Local recurrence after mastectomy is most common in the first two
years and decreases with time. In contrast local recurrence after breast
conservation occurs at a fixed rate each year. Follow up schedules
should take this difference into account. The aim of follow up is to
detect local recurrence while it is treatable or to detect contralateral
disease. Patients with carcinoma of one breast are at high risk of cancer
Follow up schedule after in the other breast, and about 1% a year develop this. All patients
surgery for breast cancer under follow up after breast cancer should, therefore, have
Breast conservation surgery mammography performed regularly (the interval between
mammograms varies from one to two years in different units) on one
Review every six months or both breasts. Mammograms can be difficult to interpret after breast
Mastectomy conservation because scarring from surgery can result in the formation
Review every six months for first two years of a stellate opacity and localised distortion, which can be difficult to
and annually thereafter differentiate from cancer recurrence. Magnetic resonance imaging
seems to be useful in this situation.
1152 BMJ VOLUME 309 29 OCTOBER 1994
S-ar putea să vă placă și
- Topic Viii NeoplasiaDocument6 paginiTopic Viii NeoplasiaMarinelle TumanguilÎncă nu există evaluări
- Neoplasia: Dr. Methaq Mueen Lec.2Document48 paginiNeoplasia: Dr. Methaq Mueen Lec.2bv2328002Încă nu există evaluări
- Pathology of Breast CancerDocument4 paginiPathology of Breast CancerEugene Osei AmoakoÎncă nu există evaluări
- Breast and Lung CancerDocument141 paginiBreast and Lung CancerabdurehmanÎncă nu există evaluări
- 3 - Fudamentals of Neoplasm 2022Document32 pagini3 - Fudamentals of Neoplasm 2022noreentamer20Încă nu există evaluări
- Non Urothelial Carcinoma of BladderDocument15 paginiNon Urothelial Carcinoma of BladderAida EsmeronÎncă nu există evaluări
- BorderlineDocument7 paginiBorderlineAna vargasÎncă nu există evaluări
- Mironov 2007Document18 paginiMironov 2007Alif Dellavia SuciÎncă nu există evaluări
- Diversity of Breast Carcinoma Histological Subtypes and Clinical RelevanceDocument9 paginiDiversity of Breast Carcinoma Histological Subtypes and Clinical RelevanceNGUYEN QUYNHÎncă nu există evaluări
- Adenocarcinoma Borderline OvarioDocument18 paginiAdenocarcinoma Borderline OvarioIsaac MaderoÎncă nu există evaluări
- Update On Nasopharyngeal Carcinoma: Ó Humana 2007Document6 paginiUpdate On Nasopharyngeal Carcinoma: Ó Humana 2007Zakia AjaÎncă nu există evaluări
- Referat Bedah - QuwDocument14 paginiReferat Bedah - QuwSaniaty TuankottaÎncă nu există evaluări
- Oncogenesis Lecture IDocument73 paginiOncogenesis Lecture IValeriiShulypaÎncă nu există evaluări
- Salivary Gland Cancer: From Diagnosis to Tailored TreatmentDe la EverandSalivary Gland Cancer: From Diagnosis to Tailored TreatmentLisa LicitraÎncă nu există evaluări
- Case Analysis DR RinaDocument30 paginiCase Analysis DR RinaCindy PrayogoÎncă nu există evaluări
- 2 NeoplasiaDocument48 pagini2 Neoplasiayadetakebede53Încă nu există evaluări
- Histology of ColorectalDocument18 paginiHistology of ColorectalThomas KlebÎncă nu există evaluări
- NE0PLASIADocument28 paginiNE0PLASIADaniel SutantoÎncă nu există evaluări
- Git ArticleDocument6 paginiGit ArticlePawan SapkotaÎncă nu există evaluări
- The Dualistic Model of Ovarian Carcinogenesis Revisited Revised and ExpandedDocument15 paginiThe Dualistic Model of Ovarian Carcinogenesis Revisited Revised and ExpandedFrederico TimmÎncă nu există evaluări
- Esmo Guia de Ca de Ovario 2012Document8 paginiEsmo Guia de Ca de Ovario 2012henryÎncă nu există evaluări
- Understanding CancerDocument5 paginiUnderstanding CancerEunice Villa CuñadaÎncă nu există evaluări
- Pharma en OncologyDocument14 paginiPharma en Oncologyyaqoob008Încă nu există evaluări
- NeoplasiaDocument31 paginiNeoplasiaAnin PrakashÎncă nu există evaluări
- FIGO 2012 Pathology of CancerDocument14 paginiFIGO 2012 Pathology of CancerFellita Ratri AÎncă nu există evaluări
- Rectal Cancer StagingDocument10 paginiRectal Cancer StagingI G. A. Ratna DewiÎncă nu există evaluări
- Malignant Diseases of BreastDocument70 paginiMalignant Diseases of BreastdranjupradhanÎncă nu există evaluări
- Management of Salivary Gland Tumours: United Kingdom National Multidisciplinary GuidelinesDocument8 paginiManagement of Salivary Gland Tumours: United Kingdom National Multidisciplinary GuidelinesCeriaindriasariÎncă nu există evaluări
- Breast and Lung CancerDocument141 paginiBreast and Lung CancerabdurehmanÎncă nu există evaluări
- Breast CancerDocument3 paginiBreast Cancerlaurie.charlynjaneÎncă nu există evaluări
- Case StudyDocument18 paginiCase StudyKristine Joy RevañoÎncă nu există evaluări
- NATIONAL CANCER CONTROL PROGRAMM 2 (Prakash)Document19 paginiNATIONAL CANCER CONTROL PROGRAMM 2 (Prakash)angayarkanni100% (1)
- CACXDocument34 paginiCACXMax ZealÎncă nu există evaluări
- Staging and Treatment of Breast CancerDocument20 paginiStaging and Treatment of Breast CancerSalim Mwiti NabeaÎncă nu există evaluări
- NCM 109 A3 Rle Ward ClassDocument33 paginiNCM 109 A3 Rle Ward Classdunhill26labanÎncă nu există evaluări
- 03 Chapter 3 PDFDocument5 pagini03 Chapter 3 PDFTuấn HoàngÎncă nu există evaluări
- 212F - Oncology L1 - 2104Document25 pagini212F - Oncology L1 - 2104Tyler LiuÎncă nu există evaluări
- Infodatin IbuDocument39 paginiInfodatin IbuchintyamontangÎncă nu există evaluări
- NeoplasiaDocument150 paginiNeoplasiaDavon Richard Walter Van-VeenÎncă nu există evaluări
- Intl J Gynecology Obste - 2021 - Koskas - Cancer of The Corpus Uteri 2021 UpdateDocument16 paginiIntl J Gynecology Obste - 2021 - Koskas - Cancer of The Corpus Uteri 2021 UpdateGraceAnnSanjorjoÎncă nu există evaluări
- Cc2 - MidtermDocument3 paginiCc2 - MidtermMika SusadaÎncă nu există evaluări
- Prise en Charge Des Tumeurs Des Glandes Salivaires Royaume-Uni Lignes Directrices Nationales MultidisciplinairesDocument8 paginiPrise en Charge Des Tumeurs Des Glandes Salivaires Royaume-Uni Lignes Directrices Nationales MultidisciplinairesMamadou DIENEÎncă nu există evaluări
- Tumors: Benign and Malignant: Cancer Therapy & OncologyDocument3 paginiTumors: Benign and Malignant: Cancer Therapy & OncologyMaria ArifahÎncă nu există evaluări
- Breast Cancer Pa Tho PhysiologyDocument3 paginiBreast Cancer Pa Tho PhysiologyFrancis Carpio100% (1)
- Chapter 6 Neoplasia (2nd Edition)Document42 paginiChapter 6 Neoplasia (2nd Edition)vs7ksgrj8pÎncă nu există evaluări
- G Path-NeoplasiaDocument60 paginiG Path-Neoplasiachouchou124Încă nu există evaluări
- Cancer Bio Lecture 3Document26 paginiCancer Bio Lecture 3snoori2307Încă nu există evaluări
- Carcinoma BreastDocument8 paginiCarcinoma BreastYeshvi s100% (1)
- Tumor FiloidesDocument11 paginiTumor FiloidesRicoÎncă nu există evaluări
- Review Article Phyllodes Tumor of Breast: A Review ArticleDocument10 paginiReview Article Phyllodes Tumor of Breast: A Review ArticleSafira Indriakasia NaskarÎncă nu există evaluări
- (Mater) 6. Kanker ServiksDocument42 pagini(Mater) 6. Kanker ServiksRevi Tamimi0% (2)
- Neoplasia 2, Nursing 2021Document30 paginiNeoplasia 2, Nursing 2021ARAK AldarwishÎncă nu există evaluări
- Cervical CancerDocument3 paginiCervical CancernoblefxÎncă nu există evaluări
- Cytology II: Gynae and Non-Gynae CytologyDocument126 paginiCytology II: Gynae and Non-Gynae Cytologybusiness onlyyouÎncă nu există evaluări
- Lectura 2Document11 paginiLectura 2CristianÎncă nu există evaluări
- Rishika Vijayvargiya Class XII ADocument21 paginiRishika Vijayvargiya Class XII ARajat PorwalÎncă nu există evaluări
- Ca EndometriumDocument10 paginiCa Endometriumoktaviany810Încă nu există evaluări
- Kulliyyah of Nursing Year 1 Problem-Based Learning: Trigger 1Document17 paginiKulliyyah of Nursing Year 1 Problem-Based Learning: Trigger 1Fitri ZulkifliÎncă nu există evaluări
- 2.3.1 Cancer Biology Cheat Sheet: by ViaDocument5 pagini2.3.1 Cancer Biology Cheat Sheet: by Viaimk_mithunÎncă nu există evaluări
- Care For Women: With Ovarian, Cerviacl, Vulvar and Endometrial CancerDocument26 paginiCare For Women: With Ovarian, Cerviacl, Vulvar and Endometrial CancerAhmad JradeenÎncă nu există evaluări
- Partial Mechanical Bowel Resume Dari HariDocument2 paginiPartial Mechanical Bowel Resume Dari HariHeldrian D SuyuthieÎncă nu există evaluări
- A Randomized Controlled Study Comparing A Vessel Sealing System With The Conventional Technique in Axillary Lymph Node Dissection For Primary Breast CancerDocument9 paginiA Randomized Controlled Study Comparing A Vessel Sealing System With The Conventional Technique in Axillary Lymph Node Dissection For Primary Breast CancerHeldrian D SuyuthieÎncă nu există evaluări
- FAST15Document13 paginiFAST15Whinet Jojo TerunaÎncă nu există evaluări
- Journal Reading Brain MetastasisDocument27 paginiJournal Reading Brain MetastasisHeldrian D SuyuthieÎncă nu există evaluări
- Adhesive ObstructionDocument6 paginiAdhesive ObstructionHeldrian D SuyuthieÎncă nu există evaluări
- Abdominal TraumaDocument21 paginiAbdominal TraumaSyifa EnnyÎncă nu există evaluări
- AdhesionsDocument2 paginiAdhesionsHeldrian D SuyuthieÎncă nu există evaluări
- Ethical ClearanceDocument4 paginiEthical ClearanceHeldrian D SuyuthieÎncă nu există evaluări
- Congenital Diaphragmatic HerniaDocument11 paginiCongenital Diaphragmatic HerniaHeldrian D SuyuthieÎncă nu există evaluări
- Transarterial Chemoembolisation2Document15 paginiTransarterial Chemoembolisation2Heldrian D SuyuthieÎncă nu există evaluări
- Lash Lift Waiver and File SheetDocument2 paginiLash Lift Waiver and File SheettiffyoloÎncă nu există evaluări
- Teacher EducationDocument32 paginiTeacher Educationsoumya satheshÎncă nu există evaluări
- Group DR - Script - Allergic Rhinitis (Peanut Allergy) Health EducationDocument10 paginiGroup DR - Script - Allergic Rhinitis (Peanut Allergy) Health EducationKyra Bianca R. FamacionÎncă nu există evaluări
- Physiological Changes Postpartum PeriodDocument2 paginiPhysiological Changes Postpartum PeriodEurielle MioleÎncă nu există evaluări
- Job Chart of Physical Education Teachers - AP GOVTDocument3 paginiJob Chart of Physical Education Teachers - AP GOVTRamachandra Rao100% (1)
- Group1-FINAL-Chapter-1-2-3 (G1)Document46 paginiGroup1-FINAL-Chapter-1-2-3 (G1)Sydney BautistaÎncă nu există evaluări
- 7 Legal Dimensions of Nursing Chapter ReviewDocument2 pagini7 Legal Dimensions of Nursing Chapter ReviewAmy AnonymousÎncă nu există evaluări
- Lista Medicamente OTC Conform Nomenclator ANM 17 Feb2020Document184 paginiLista Medicamente OTC Conform Nomenclator ANM 17 Feb2020Andreea PasolÎncă nu există evaluări
- MOHAN Di. RAJU....... MOHAN Di. RAJU......Document32 paginiMOHAN Di. RAJU....... MOHAN Di. RAJU......Nagaraja ReddyÎncă nu există evaluări
- 2018 MUSE Inspire Conference - Show and Tell SessionsDocument13 pagini2018 MUSE Inspire Conference - Show and Tell SessionsMichele LambertÎncă nu există evaluări
- Food Act 1983Document14 paginiFood Act 1983Shahirah Zubir0% (1)
- V-Gel Cleaning & User GuideDocument3 paginiV-Gel Cleaning & User GuideInstrulife OostkampÎncă nu există evaluări
- MSDS Aceite CastorDocument6 paginiMSDS Aceite CastorwaddydiÎncă nu există evaluări
- The Extent of Influence of Factors On Cigarette Smoking Among TeenagersDocument4 paginiThe Extent of Influence of Factors On Cigarette Smoking Among TeenagersLESTHER DELA CRUZÎncă nu există evaluări
- Diana Barnett Course Critique n5327 RDocument4 paginiDiana Barnett Course Critique n5327 Rapi-308950624Încă nu există evaluări
- Alternatives To Hydrazine MHI PaperDocument5 paginiAlternatives To Hydrazine MHI PaperjycortesÎncă nu există evaluări
- Laparoscopic Appendectomy SurgeryDocument2 paginiLaparoscopic Appendectomy SurgeryNycoÎncă nu există evaluări
- Correlation Between Body Mass Index and Heart Rate in Males and Females of Different Age GroupDocument7 paginiCorrelation Between Body Mass Index and Heart Rate in Males and Females of Different Age GroupAdriel Jian NaldoÎncă nu există evaluări
- The Influence of Music in Horror Games (Final Draft)Document7 paginiThe Influence of Music in Horror Games (Final Draft)Panther LenoXÎncă nu există evaluări
- Resumes For Physical Therapists: Resume Assessment, Diagnosis and TreatmentDocument4 paginiResumes For Physical Therapists: Resume Assessment, Diagnosis and TreatmentSuganya BalachandranÎncă nu există evaluări
- Introduction To Occupational Therapy PDFDocument291 paginiIntroduction To Occupational Therapy PDFMurat Hasan BaşaranÎncă nu există evaluări
- Letters of Intent (Cover Letters)Document6 paginiLetters of Intent (Cover Letters)anca_ramona_s0% (1)
- PREGABALINDocument5 paginiPREGABALINJojenelle R. TepaitÎncă nu există evaluări
- Response To States 4.2 Motion in Limine Character of VictimDocument10 paginiResponse To States 4.2 Motion in Limine Character of VictimLaw of Self DefenseÎncă nu există evaluări
- Lecture in Geriatrics Physical Therapy 1Document27 paginiLecture in Geriatrics Physical Therapy 1S.AÎncă nu există evaluări
- Fasting and Low Carb InfoDocument4 paginiFasting and Low Carb InfoKatrin NovaÎncă nu există evaluări
- General Practitioner Sample Resume WWW - Careerfaqs.com - AuDocument3 paginiGeneral Practitioner Sample Resume WWW - Careerfaqs.com - AuSubhash RitwalÎncă nu există evaluări
- Dpmas 20180126Document2 paginiDpmas 20180126gmejiar5237Încă nu există evaluări
- Fatima's CommissionDocument7 paginiFatima's CommissionSachie Daniela CheungÎncă nu există evaluări
- Arterial Events, Venous Thromboembolism, Thrombocytopenia, and Bleeding After Vaccination With Oxford-Astrazeneca Chadox1-S in Denmark and Norway: Population Based Cohort StudyDocument10 paginiArterial Events, Venous Thromboembolism, Thrombocytopenia, and Bleeding After Vaccination With Oxford-Astrazeneca Chadox1-S in Denmark and Norway: Population Based Cohort StudyFemale calmÎncă nu există evaluări