Documente Academic
Documente Profesional
Documente Cultură
Ischemic Heart Disease: Epidemiology and Global Trends
Încărcat de
Random Commenter0 evaluări0% au considerat acest document util (0 voturi)
11 vizualizări2 paginiIschemic heart disease is caused by an inadequate supply of blood and oxygen to the heart muscle. The most common cause is atherosclerotic disease of the coronary arteries. Risk factors include smoking, hypertension, diabetes, obesity, and high cholesterol. Coronary atherosclerosis develops gradually, reducing blood flow and oxygen supply to the heart. When oxygen demand increases such as during exercise, ischemia can occur, causing chest pain or angina. Prolonged ischemia can damage heart muscle leading to a heart attack.
Descriere originală:
IHD Harrison's
Titlu original
Ischemic Heart Disease
Drepturi de autor
© © All Rights Reserved
Formate disponibile
DOCX, PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentIschemic heart disease is caused by an inadequate supply of blood and oxygen to the heart muscle. The most common cause is atherosclerotic disease of the coronary arteries. Risk factors include smoking, hypertension, diabetes, obesity, and high cholesterol. Coronary atherosclerosis develops gradually, reducing blood flow and oxygen supply to the heart. When oxygen demand increases such as during exercise, ischemia can occur, causing chest pain or angina. Prolonged ischemia can damage heart muscle leading to a heart attack.
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca DOCX, PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
11 vizualizări2 paginiIschemic Heart Disease: Epidemiology and Global Trends
Încărcat de
Random CommenterIschemic heart disease is caused by an inadequate supply of blood and oxygen to the heart muscle. The most common cause is atherosclerotic disease of the coronary arteries. Risk factors include smoking, hypertension, diabetes, obesity, and high cholesterol. Coronary atherosclerosis develops gradually, reducing blood flow and oxygen supply to the heart. When oxygen demand increases such as during exercise, ischemia can occur, causing chest pain or angina. Prolonged ischemia can damage heart muscle leading to a heart attack.
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca DOCX, PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 2
ISCHEMIC HEART DISEASE
Ischemic heart disease (IHD) o Smoking
- Inadequate supply of blood and oxygen o Hypertension
- Imbalance between myocardial oxygen supply and demand o DM
- MOST COMMON CAUSE: atherosclerotic disease of epicardial - Disturb normal functions:
coronal artery o Control of vascular tone inappropriate constriction
o Maintenance of antithrombotic surface thrombus
EPIDEMIOLOGY AND GLOBAL TRENDS formation
Associated w/: o Control of inflammatory cell adhesion abnormal
- Genetic factors interactionis
- High-fat and energy-rich diet - Vulnerable vessel + Vulnerable blood hypercoagulability +
- Smoking hypofibrinolysis
- Sedentary lifestyle Atherosclerosis develops at irregular rates in different segments
Risk factors: segmental reduction in cross-sectional area
- Obesity - Predilection at sites of ↑ turbulence – branch points
- Insulin resistance - Stenosis reduces the diameter by 50% limitation to ↑ flow
- Type 2 DM to meet MVO2
IHD – likely to become most common cause of death by 2020 o Reduced by 80% - blood flow at rest may be reduced
further minor decreases cause ischemia at rest
PATHOPHYSIOLOGY - Segmental atherosclerotic narrowing – most commonly by
For any given level of demand for O2, myocardium will control supply formation of a plaque subject to rupture or erosion of cap
of oxygen-rich blood to prevent underperfusion o Plaque contents upon exposure:
- Determinants of Myocardial O2 demand (MVO2) platelets – activated and aggregate
o Heart rate coagulation cascade is activated
o Contractility - Location – influences quantity of myocardium rendered ischemic
o Wall tension (stress) and severity
Adequate supply requires: Satisfactory O2-carrying capacity of blood o Left main coronary artery and proximal LAD – hazardous
- Determined by: o Collateral vessels – if narrowing develops gradually
o inspired O2 Worsening distal resistance vessels dilate
o pulmonary function - Pressure gradient develops
o Hemoglobin - Resistance vessels maximally dilated blood follow becomes
o Adequate level of coronary blood flow phasic dependent on pressure in coronary artery distal to obstruction
Majority during diastole - Ischemia – precipitated by ↑ in MVO2 precipitated by:
Coronary resistance to flow occurs across 3 sets of arteries o Physiologic vasomotion
- Large epicardial arteries (R1) o Loss of endothelial control
- Prearteriolar vessels (R2) Major determinant
o Pathologic spasm (Pinzmetal’s)
of coronary
- Arterioral and intramyocardial vessels
resistance
(R3) EFFECTS OF ISCHEMIA
Normal coronary circulation is dominated by MVO2 Coronary atherosclerosis – nonuniform ischemia
- Met by ability to vary its resistance (blood flow) - Regional disturbances Segmental hypokinesia, or bulging
- Normal: R2 & R3 demonstrate capacity for dilation in response to: (dyskinesia) ↓ pump function
o Exercise and emotional stress (metabolic regulation) - Poor perfusion of subendocardium – more intense ischemia
o Blood pressure (autoregulation) Ischemia of large portions of ventricle transient LV failure
- Atherosclerosis: ↓ lumen limits ↑ perfusion w/ ↑ demand - If papillary muscle is involved mitral regurgitation (MR) occur
o Reduction severe: ↓ basal state - Transient – angina pectoris
Blood flow also can be limited by: - Prolonged – myocardial necrosis and scarring
- Spasm (Pinzmetal’s angina) Normal myocardium – metabolizes fatty acids (FA) & glucose to CO2
- Thrombi and water
- Coronary emboli - Severe deprivation
- Aortitis o FAs cannot be oxidized
- Congenital abnormalities – L anterior descending coronary artery o Glucose lactate
from pulmonary artery (infants) o ↓ intracellular pH and stores of high-energy phosphates
Myocardial ischemia: o ↓ ATP impaired cell membrane function leakage of K
- ↑ MVO2 when coronary blood flow is limited and uptake of Na + Ca
- d/t left ventricular hypertrophy d/t aortic stenosis - Reversible damage: <=20 minutes of total occlusion w/o collaterals
- severe anemia or presence of carboxyhemoglobin – rarely cause ECG: inversion of T-waves
ischemia but lowers threshold to ischemia - More severe: displacement of ST segment
- Microvascular angina – abnormal constriction or failure of normal Transient T-wave Transient ST- ST-segment
dilation inversion segment depression elevation
non-transmural, patchy More severe
CORONARY ATHEROSCLEROSIS intramyocardial subendocardial transmural ischemia
Epicardial coronary arteries – major site ischemia ischemia
- Major risk factors: Electrical instability
o ↑ LDL - Isolated ventricular premature beats
o ↓ HDL - Ventricular tachy or ventricular fibrillation
ISCHEMIC HEART DISEASE
S-ar putea să vă placă și
- Ischemic Heart DiseaseDocument8 paginiIschemic Heart DiseaseJustine CastilloÎncă nu există evaluări
- Cvspa04 Ihd and MiDocument8 paginiCvspa04 Ihd and MiRobert So JrÎncă nu există evaluări
- Ischemic Heart Disease and Myocardial Infarction: Drs. Syamsudin, M. Biomed Fakultas Farmasi Universitas PancasilaDocument67 paginiIschemic Heart Disease and Myocardial Infarction: Drs. Syamsudin, M. Biomed Fakultas Farmasi Universitas PancasilaPutri RizkiaÎncă nu există evaluări
- Ischemic Heart Disease and Myocardial Infarction: Pathophysiology of Myocardial Ischemia Bio-Med 350 September 2004Document81 paginiIschemic Heart Disease and Myocardial Infarction: Pathophysiology of Myocardial Ischemia Bio-Med 350 September 2004roshamaharaniÎncă nu există evaluări
- Exam 2 Study GuideDocument12 paginiExam 2 Study GuideAlexandria SmithÎncă nu există evaluări
- Week 10 - Hypertension, Atherosclerosis, ArrhythmiaDocument14 paginiWeek 10 - Hypertension, Atherosclerosis, Arrhythmiashivani patel100% (1)
- 29 Coronary Artery Disease and DysrhythmiasDocument3 pagini29 Coronary Artery Disease and DysrhythmiasKrishna Faith P. DelaraÎncă nu există evaluări
- Acute Ischemic Stroke: Etiology, Pathophysiology, Clinical Features, Diagnostics, TreatmentDocument7 paginiAcute Ischemic Stroke: Etiology, Pathophysiology, Clinical Features, Diagnostics, TreatmentAfrah AbdulÎncă nu există evaluări
- Coronary Artery Disease (CAD) : Pathogenesis RFDocument5 paginiCoronary Artery Disease (CAD) : Pathogenesis RFJennyu Yu100% (1)
- Cardiomyopathy Dilated CardiomyopathyDocument5 paginiCardiomyopathy Dilated Cardiomyopathym3d1k100% (1)
- Ischemic Heart DiseaseDocument67 paginiIschemic Heart Diseasealfaz lakhani80% (5)
- Ischemic Heart Disease and Myocardial InfarctionDocument129 paginiIschemic Heart Disease and Myocardial InfarctionEspieglerie EspieglerieÎncă nu există evaluări
- Patol SistkardiovaskularDocument68 paginiPatol SistkardiovaskularfaridaÎncă nu există evaluări
- Syok Kardiogenik Dr. Rani Maliawan, SP JPDocument59 paginiSyok Kardiogenik Dr. Rani Maliawan, SP JPLuh Leni AriniÎncă nu există evaluări
- Wk3 Emergency Medicine Notes Cardiovascular Emergencies & Shock ObjectivesDocument23 paginiWk3 Emergency Medicine Notes Cardiovascular Emergencies & Shock ObjectivesKhandar Yo100% (1)
- Coronary Artery Disease: Arief Santoso, S.farm., AptDocument31 paginiCoronary Artery Disease: Arief Santoso, S.farm., AptDahniarErickyuwslalusmangat TdkbtuhpcartetapcintaAllahÎncă nu există evaluări
- Chapter 9: BLOOD VESSELSDocument18 paginiChapter 9: BLOOD VESSELSangelina buenaÎncă nu există evaluări
- Cardiovascular PathologyDocument182 paginiCardiovascular PathologyPavan chowdaryÎncă nu există evaluări
- Class 17Document46 paginiClass 17Nishani SatiyaseelanÎncă nu există evaluări
- Stroke 1Document69 paginiStroke 1Berk HalilbeyoğluÎncă nu există evaluări
- Vascular Disorder: DR Nur Asyilla Che Jalil Pathology Department PPSP HusmDocument140 paginiVascular Disorder: DR Nur Asyilla Che Jalil Pathology Department PPSP HusmHaziq KamardinÎncă nu există evaluări
- Heart - PathologyDocument22 paginiHeart - Pathologyjmosser100% (1)
- Ischemic Heart DiseaseDocument10 paginiIschemic Heart DiseaseA-sHakour AadenÎncă nu există evaluări
- Chapter 9: BLOOD VESSELSDocument19 paginiChapter 9: BLOOD VESSELSangelina buenaÎncă nu există evaluări
- ATHEROSCLEROSISDocument4 paginiATHEROSCLEROSISMARYHAN M MUKHALALATIÎncă nu există evaluări
- CardiologyDocument4 paginiCardiologyShatha AlgahtaniÎncă nu există evaluări
- Cardio Day 3 TemplateDocument24 paginiCardio Day 3 TemplateMikeÎncă nu există evaluări
- IHD Ema - 2020Document55 paginiIHD Ema - 2020Anastasia ApriliaÎncă nu există evaluări
- Stroke: Abyot From Harrison, DR Belachew and DR Yared HandoutDocument32 paginiStroke: Abyot From Harrison, DR Belachew and DR Yared HandoutashuÎncă nu există evaluări
- (K7) Valvular Heart DiseaseDocument79 pagini(K7) Valvular Heart DiseaseXeniel AlastairÎncă nu există evaluări
- Ajith Kumar P MPT Cardiopulmonary SciencesDocument30 paginiAjith Kumar P MPT Cardiopulmonary SciencesSuhana JahangeerÎncă nu există evaluări
- Ischemic Heart Disease: Joana Marie E. GantuangcoDocument8 paginiIschemic Heart Disease: Joana Marie E. GantuangcoJoana Marie Gantuangco-MaglinteÎncă nu există evaluări
- CVS1 - K8 - Valvular Heart DiseaseDocument79 paginiCVS1 - K8 - Valvular Heart DiseaseDumora FatmaÎncă nu există evaluări
- Patho-The Heart 2Document11 paginiPatho-The Heart 2Isabel CastilloÎncă nu există evaluări
- Textbook Discussion On ST-elevation Myocardial Infarction - GicaroDocument12 paginiTextbook Discussion On ST-elevation Myocardial Infarction - GicaroJica Marie Bandiola GicaroÎncă nu există evaluări
- Athero 2 Dr. Raquid 2021Document93 paginiAthero 2 Dr. Raquid 2021oreaÎncă nu există evaluări
- Heart Failure DujingDocument79 paginiHeart Failure DujingEdward XiamÎncă nu există evaluări
- Shock: Agus Setiyana, M.D. Cardiac Anesthetist Acls Provider Fccs Provider Atls ProviderDocument39 paginiShock: Agus Setiyana, M.D. Cardiac Anesthetist Acls Provider Fccs Provider Atls ProvidersheiraÎncă nu există evaluări
- Infarction PDFDocument24 paginiInfarction PDFAmandeep Kaur ChabbraÎncă nu există evaluări
- Group 3 Cardiovascular ProblemDocument52 paginiGroup 3 Cardiovascular ProblemWARREN WILLIAM PERAN100% (3)
- Diseases of Blood Vessels Dr. Fe A. Bartolome, Maed, FpasmapDocument15 paginiDiseases of Blood Vessels Dr. Fe A. Bartolome, Maed, FpasmapJayesh MahajanÎncă nu există evaluări
- Peripheral Arterial Disease: PathogenesisDocument4 paginiPeripheral Arterial Disease: PathogenesisDarawan MirzaÎncă nu există evaluări
- باثو 2Document35 paginiباثو 2shahadkhaled171Încă nu există evaluări
- Thrombosis: Pgi Ricky G. JalecoDocument34 paginiThrombosis: Pgi Ricky G. JalecoRicky JalecoÎncă nu există evaluări
- Sudden DeathDocument26 paginiSudden DeathAbang AzharÎncă nu există evaluări
- Lecture 6-ShockDocument5 paginiLecture 6-ShockMadiha MadiÎncă nu există evaluări
- CardiomyopathyDocument9 paginiCardiomyopathyMinh Nguyễn Phương HồngÎncă nu există evaluări
- Dr. Judya - PA CardiovasculerDocument101 paginiDr. Judya - PA Cardiovasculerdelia rahmaÎncă nu există evaluări
- Myocardial InfarctionDocument11 paginiMyocardial InfarctionAleena ShajiÎncă nu există evaluări
- Acquired Heart Diseases: Extracorporeal PerfusionDocument7 paginiAcquired Heart Diseases: Extracorporeal PerfusionJenneylyn AbieraÎncă nu există evaluări
- SHOCKDocument24 paginiSHOCKAngela mitaÎncă nu există evaluări
- Hemodynamic Disorders, Thrombosis and ShockDocument40 paginiHemodynamic Disorders, Thrombosis and ShockAndi Tri NugrahaÎncă nu există evaluări
- Seminar2ischemia 180315152816Document124 paginiSeminar2ischemia 180315152816قاسم اليوسفيÎncă nu există evaluări
- Patologicheskaya Anatomia COVID 19 Atlas 86 98.ru - enDocument13 paginiPatologicheskaya Anatomia COVID 19 Atlas 86 98.ru - enkapil pancholiÎncă nu există evaluări
- Cardiogenic Shock and HemodynamicsDocument21 paginiCardiogenic Shock and Hemodynamicsravi_02Încă nu există evaluări
- Book Cardio ConceptDocument29 paginiBook Cardio ConceptJulia Rae Delos SantosÎncă nu există evaluări
- Ischemic Heart Disease and Myocardial InfarctionDocument73 paginiIschemic Heart Disease and Myocardial InfarctionAngelEduardoVillarrealGiraldoÎncă nu există evaluări
- ACS HandoutDocument19 paginiACS HandoutGloriana Julia TeopeÎncă nu există evaluări
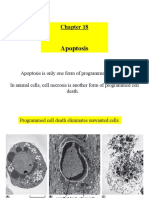
- Chapter 18 - Apoptosis - 112612Document28 paginiChapter 18 - Apoptosis - 112612Anonymous nkR1PhIHÎncă nu există evaluări
- Weeks 3 - 8Document32 paginiWeeks 3 - 8Stefan HutsonÎncă nu există evaluări
- Human Excretory SystemDocument6 paginiHuman Excretory SystemRahul SinghÎncă nu există evaluări
- St. Luke's College of Medicine - William H. Quasha Memorial: AnatomyDocument6 paginiSt. Luke's College of Medicine - William H. Quasha Memorial: AnatomyMavic VillanuevaÎncă nu există evaluări
- Bio BatteryDocument13 paginiBio BatterymukulÎncă nu există evaluări
- Patente Endoesqueleto para Sex Doll SiliconaDocument12 paginiPatente Endoesqueleto para Sex Doll SiliconaGabriel De Jesus100% (1)
- Motivation - BPTDocument7 paginiMotivation - BPTRenukaÎncă nu există evaluări
- Diagnosis & Management of Anaphylactic Shock NewDocument6 paginiDiagnosis & Management of Anaphylactic Shock Newputri auliyahÎncă nu există evaluări
- MIO MediumDocument2 paginiMIO MediumIntan Farida YasminÎncă nu există evaluări
- Intro To Ana Physio RBLDocument69 paginiIntro To Ana Physio RBLHades HadesÎncă nu există evaluări
- Beef Carcass Evaluation, Grading and CutsDocument21 paginiBeef Carcass Evaluation, Grading and CutsMuhammad AsifÎncă nu există evaluări
- Funda 7Document19 paginiFunda 7Akia Cayasan BayaÎncă nu există evaluări
- ZENICADocument72 paginiZENICAVedadÎncă nu există evaluări
- Introduction To Health Care 4th Edition Mitchell Solutions Manual DownloadDocument5 paginiIntroduction To Health Care 4th Edition Mitchell Solutions Manual DownloadMark Prindle100% (20)
- Marieb ch3bDocument25 paginiMarieb ch3bapi-229554503100% (1)
- A&p Lab Ex 38Document6 paginiA&p Lab Ex 38Alex Lee95% (19)
- ADR Common Drug - Induced Organ DisordersDocument45 paginiADR Common Drug - Induced Organ Disorders0009439Încă nu există evaluări
- Physical Assessment Feu NRMFDocument16 paginiPhysical Assessment Feu NRMFJhen Bitco FidelÎncă nu există evaluări
- Apex o GenesisDocument54 paginiApex o GenesisbrahmannaÎncă nu există evaluări
- Mitochondrial Cytopathies in Children and AdultsDocument28 paginiMitochondrial Cytopathies in Children and AdultsmmaitehmdÎncă nu există evaluări
- 200-Protein Quantification BCA™, Modified Lowry and Bradford AssaysDocument5 pagini200-Protein Quantification BCA™, Modified Lowry and Bradford AssaysMusa LooÎncă nu există evaluări
- MRCS Revision Guide Trunk and Thorax by Mazyar Kanani Leanne Harling (Z-LiDocument184 paginiMRCS Revision Guide Trunk and Thorax by Mazyar Kanani Leanne Harling (Z-LiRahmaÎncă nu există evaluări
- Adult Health Final Study GuideDocument5 paginiAdult Health Final Study GuideNurseNancy93100% (1)
- NeuroDocument35 paginiNeuroFlor OMÎncă nu există evaluări
- Zabrina Joana DDocument4 paginiZabrina Joana DEmman BalidoÎncă nu există evaluări
- Drug FeaturesDocument9 paginiDrug FeaturesLeah Claudia de OcampoÎncă nu există evaluări
- Isometric Power Revolution Part2Document86 paginiIsometric Power Revolution Part2Smriti Ichopra100% (15)
- Penyakit Jantung KongenitalDocument30 paginiPenyakit Jantung KongenitalrintiikÎncă nu există evaluări
- GastritisDocument10 paginiGastritisMario100% (2)
- CarbohydratesDocument10 paginiCarbohydratesshajmalikÎncă nu există evaluări