Documente Academic
Documente Profesional
Documente Cultură
ABC of Oral Health Dental Emergencies
Încărcat de
Erfiadi Nur FahmiDrepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
ABC of Oral Health Dental Emergencies
Încărcat de
Erfiadi Nur FahmiDrepturi de autor:
Formate disponibile
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/12352935
ABC of oral health. Dental emergencies
Article in BMJ Clinical Research · October 2000
DOI: 10.1136/bmj.321.7260.559 · Source: PubMed
CITATIONS READS
21 415
3 authors, including:
Crispian Scully
University College London
1,418 PUBLICATIONS 32,277 CITATIONS
SEE PROFILE
Some of the authors of this publication are also working on these related projects:
Oral Epithelial Dysplasia View project
oral cancer View project
All content following this page was uploaded by Crispian Scully on 29 May 2014.
The user has requested enhancement of the downloaded file.
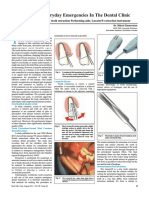
Clinical review
ABC of oral health
Dental emergencies
Graham Roberts, Crispian Scully, Rosemary Shotts
Most oral emergencies relate to pain, bleeding, or orofacial
trauma and should be attended by a dental practitioner.
However, in the absence of access to dental care, a medical
practitioner may be called on to help. Jaw fractures require the
attention of oral or maxillofacial surgeons.
Dental pain
Pulpal pain is spontaneous, strong, often throbbing, and
Orofacial swelling
exacerbated by temperature and outlasts the evoking stimulus. in a patient with
Localisation is poor, and pain tends to radiate to the ipsilateral an acute dental
ear, temple, or cheek. The pain may abate spontaneously, but abscess
the patient should still be referred for dental advice, as the pulp
has probably necrosed, and acute periapical periodontitis
(dental abscess) will probably follow in due course. Endodontics
(root canal treatment) or tooth extraction are required.
Periapical periodontitis pain is spontaneous and severe,
persists for hours, is well localised, and is exacerbated by biting.
The adjacent gum is often tender to palpation. An abscess may
form (“gumboil”), sometimes with facial swelling, fever, and
illness. Fascial space infections are fortunately rare since they
threaten the airway: patients should be referred to a specialist.
In the absence of immediate dental attention it is best to incise a Chronic dental
fluctuant abscess and give antimicrobials (amoxicillin) and abscess (gumboil)
analgesics. The acute situation usually then resolves, but the at a typical site, in
this case related to
abscess will recur, since the necrotic pulp will become the broken molar
re-infected unless the tooth is endodontically treated or
extracted, though a chronic abscess may be asymptomatic apart
from a discharging sinus. Rarely, this may open on to the skin.
x Emergency treatment of dental abscess is
antimicrobials, analgesics, and drainage of a fluctuant
swelling by a dentist
x Dental treatment should then be arranged, or the
abscess will recur
Dental sinus
Bleeding opening on to
skin
Most oral bleeding results from gingivitis (see earlier article) or
trauma, but if it is prolonged consider a bleeding tendency.
Dental indications for urgent admission to hospital
Trauma
After a tooth is extracted, the socket bleeds normally for a few Trauma
minutes but then clots. Since clots are easily disturbed, patients x Middle facial third fractures
x Mandibular fractures unless simple or undisplaced
should be advised not to rinse their mouth, disturb the clot, x Zygomatic fractures where there is danger of ocular damage
chew hard, take hot drinks or alcohol, or exercise for the next
Inflammatory lesions and infections
24 hours. If the socket continues to bleed lie a gauze pad across x Cervical or facial fascial space infection
the socket and ask the patient to bite on it for 15-30 minutes. If x Oral infections where patient is “toxic” or severely
it is still bleeding place Surgicel or another haemostatic agent in immunocompromised
the socket. If the bleeding continues suture the socket and, x Tuberculosis (some)
lastly, consider a bleeding tendency. x Severe viral infections
x Severe vesiculobullous disorders (pemphigus, Stevens-Johnson
syndrome, toxic epidermal necrolysis)
x Emergency care of post-extraction bleeding is to have Blood loss
the patient bite on gauze for 15-30 minutes x Severe or persistent haemorrhage (particularly in patient with a
x Persistent bleeding may require packing the socket with bleeding tendency)
a haemostatic agent or suturing, but it occasionally Others
signifies an unrecognised bleeding tendency x Diabetes with poor control
BMJ VOLUME 321 2 SEPTEMBER 2000 bmj.com 559
Clinical review
Surgical complications
Post-extraction pain
Some pain and swelling after tooth extraction are common but
ease over a few hours. Paracetamol usually provides adequate
analgesia. Pain from complex procedures may last longer and
should be controlled with regularly administered analgesics. If
pain persists or increases the patient should return to the
dentist to exclude pathology (such as dry socket or jaw fracture).
Infection
Localised osteitis (dry socket) occasionally follows an extraction,
typically a lower molar extraction. After two to four days there is
Actinomycosis
usually increasing pain, halitosis, unpleasant taste, an empty
socket, and tenderness. Exclude retained roots, foreign body, jaw
fracture, osteomyelitis, or other pathology, especially if there is
fever, intense pain, or neurological signs such as labial
anaesthesia. Treat by irrigating with warm (50°C) saline or
aqueous chlorhexidine, dressing the socket (several concoctions
are available), and giving analgesics and antimicrobials x Pain increasing after an extraction may indicate
infection or fracture
(metronidazole).
x Radiograph to exclude pathology
Actinomycosis a rare late complication of extraction or jaw x Irrigate and dress the socket, and consider
fracture and usually presents as a chronic purplish swelling. A antimicrobials and analgesics
three week course of penicillin is often indicated.
Antral complications
Loss of tooth or root into the antrum—Give antimicrobials and a
nasal decongestant and locate the object by radiography. A
further operation is required.
Oroantral fistula—Patients should not blow their nose.
Antimicrobials and nasal decongestants help. If it is detected
early, primary closure is possible, but others may need flap
closure by a specialist.
Fractured teeth
Injuries to the primary teeth may be of little consequence with
regard to emergency care, but even seemingly mild injuries can
damage the permanent successors. Upwards of 30% of children
damage their permanent teeth by the age of 15.
Enamel fracture needs no emergency care, but dental
attention should be sought later. More severe injuries affecting Oroantral fistula after extraction of an upper molar.
the dentine should be treated as urgent as there might be The antral floor is often in close proximity to the roots
of maxillary molars and premolars
pulpal infection. Emergency care consists of placing a suitable
dentine lining material on to the fractured dentine, and so
prompt treatment by a dentist within the same working day or
at least by the following morning is required. Fractured roots
require dental advice.
Avulsed teeth
Avulsed permanent anterior teeth can be replanted successfully
in a child, particularly if the root apex is not completely formed
(under 16 years old). Avulsed primary teeth should not be
replanted. The younger the child and the sooner the replantation,
the better the success; teeth replanted within 15 minutes stand a
98% chance of being retained after further dental attention.
Immediate replantation gives the best results. Hold the tooth
by the crown (do not handle root as that could damage the
periodontal ligament). If the tooth is contaminated rinse it with
sterile saline, and if the socket contains a clot remove it with Oral and dental trauma after a skateboarding accident
saline irrigation. Replant the tooth the right way round (ensure
the labial (convex) surface is facing forward) and manually
compress the socket. Splint the tooth; “finger crimping” a foil
milk bottle top is a temporary measure, an alternative is tissue
adhesive. The child should see a dentist within 72 hours.
560 BMJ VOLUME 321 2 SEPTEMBER 2000 bmj.com
Clinical review
If immediate replantation is not possible place tooth in an
isotonic fluid (cool fresh pasteurised or long life milk, saline, or
contact lens fluid). Otherwise, if the child is cooperative, place
tooth in the buccal sulcus and get to a dentist within 30
minutes. Unsuitable and slightly damaging fluids are water
(because of isotonic damage as a result of prolonged exposure),
disinfectants, bleach, and fruit juice. The use of a doxycycline
immersion before reimplantation by the dentist may be helpful
in preventing later external root resorption. x Primary teeth should not be replanted
x Permanent teeth in children can be successfully
Splint the tooth for 7-10 days, with no biting on splinted teeth,
replanted
soft diet, and good oral hygiene. x Hold tooth by crown, keep clean and moist in saline or
Follow up—Root resorption, ankylosis, and tooth milk, replant as soon as possible, and splint
submergence (infraocclusion) are potential complications.
Maxillofacial trauma
Dislocation or subluxation of mandible
This is commonly caused by a blow to the chin when the jaw is
open. The condyles are dislocated forwards and upwards
anterior to the eminence, and the patient gags open.
Fractures must be excluded. Reduction can usually be
achieved by facing the patient and placing the thumb pads over
the lower molars and applying downwards pressure and
simultaneously, with the fingers under the chin, rotating the jaw
backwards and upwards. If muscle spasm prevents reduction
intravenous midazolam may be needed. After reduction, wide
opening of the jaw should be avoided.
Recurrent dislocation is a feature of Ehlers-Danlos and
Marfan’s syndromes.
Jaw fractures
These mainly result from high velocity impact as in road traffic Step deformity of occlusion revealing mandibular
accidents, other accidents, and assaults. fracture
The immediate concern is to preserve the airway. Assess all
traumatised patients along the lines of the advanced trauma life
support scheme (ATLS). Other immediate life threatening
problems include intracranial haemorrhage, severe
haemorrhage from other sites, and cervical spine damage.
During the secondary survey, inspect the head for lacerations
and leakage of cerebrospinal fluid. Radiographs for demonstrating maxillofacial fractures
Associated bleeding may further compromise the airway. Mandibular fracture
Jaw fractures alone, unless associated with a split palate or x Panoramic or
x Bilateral oblique laterals
gunshot wounds, rarely cause severe haemorrhage. Bleeding
x Postero-anterior view of mandible
from a ruptured inferior dental artery usually stops x Occlusal
spontaneously, but may recur if, for example, there is traction
Temporomandibular joint and condyle fracture
on the mandible. Severe maxillofacial bleeding may be x Conventional and high orthopantomogram or
tamponaded with craniofacial fixation. Bleeding can arise from x Reverse Towne’s
fractured nasal bones, in which case nasal packing may be x Consider computed tomography
required. If bleeding recurs the damaged vessel must be ligated. Zygomatic arch fracture
Definitive management of fractures, despite frighteningly x Occipitomental
severe disfigurement, is not an immediate priority, but debris x Submentovertex (exposed for zygomatic arches, not base of skull)
such as fractured teeth, blood, and saliva should be cleared from Middle third fracture
x Occipitomental 30°
the mouth, and the tongue may be controlled by a dorsal
x Occipitomental 10°
suture. An oropharyngeal airway may be required. Involve the x Lateral skull
maxillofacial team early on for treatment planning. x Computed tomography
Intubation may be necessary in presence of substantial head Skull fracture
injury, and inability to intubate may necessitate surgical x Postero-anterior view of skull
cricothyroidotomy, since nasotracheal intubation is x Lateral skull (brow up)
contraindicated. x Submentovertex (exposed for base of skull)
x Computed tomography
The diagnosis of fracture is from the history, pain, swelling,
bruising (haematoma), bleeding (usually intraorally), mobility of Nasal fracture
x Soft tissues lateral view for nasal bones
fragments (and crepitus), deranged occlusion, paraesthesia or
x Occipitomental 30°
anaesthesia of nerves involved, and radiographic signs.
BMJ VOLUME 321 2 SEPTEMBER 2000 bmj.com 561
Clinical review
Mandibular fractures
These are commonly owing to assault and are usually simple
and not associated with serious other injuries or bleeding. If the
symphysis is comminuted the tongue could fall back and
obstruct the airway, and this must be prevented. Simple
undisplaced fractures may occasionally be treated conservatively
with a soft diet if the teeth are not damaged. If the fragments
are excessively mobile, pain will be substantial, and early fixation
is the best management. Most fractures are managed by open
reduction and internal fixation, usually with mini-plates.
Middle third or upper facial skeleton fractures
These commonly arise from severe trauma (particularly road
traffic accidents) and are classified into Le Fort fracture lines:
I—Low level above the nasal floor (swelling of upper lip)
II—Subzygomatic (massive swelling of face: ballooning) (Panda
III
facies)
III—Suprazygomatic (massive swelling of face and cerebrospinal
rhinorrhoea).
There may be airway obstruction, head injury, chest injuries, II
ruptured viscera, and fractured spine and long bones. Most I
middle third fractures are treated by open reduction and
internal fixation with mini-plates.
Zygomatic (malar) fractures
These are typically due to assaults. Orbital features are common Le Fort lines of middle third facial fractures (redrawn
and include depression of cheek, lateral subconjunctival from Scully et al. Oxford Handbook of Dental Patient Care.
Oxford University Press, 1998)
haemorrhage, rim step deformities, restricted eye movements,
changes in visual acuity, variation in pupil size and reactivity,
and, occasionally, enophthalmos or exophthalmos.
Undisplaced uncomplicated fractures need no treatment but
should be reviewed as early as possible within two weeks. For
others, reduction is by elevating from the temporal region
(Gillies approach), an intraoral approach, or open reduction
and internal fixation. Further reading
x Andreasen JO, Andreasen FM. Textbook and colour atlas of traumatic
injuries to the teeth. Copenhagen: Munksgaard, 1994
x The priority in patients with maxillofacial injury is the
x Bishop BG, Donnelly JC. Proposed criteria for classifying potential
airway dental emergencies in Department of Defence military personnel.
x Middle third facial fractures may be associated with Mil Med 1997;162:130-5
cerebrospinal rhinorrhoea x Gilthorpe MS, Wilson RC, Moles DR, Bedi R. Variations in
x Zygomatic fractures may be associated with ocular admissions to hospital for head injury and assault to the head. Part
damage 1: Age and gender. Br J Oral Maxillofac Surg 1999;37:294-300
x The maxillofacial team should be involved at an early x Moles DR, Gilthorpe MS, Wilson RC, Bedi R. Variations in
stage for planning treatment admission to hospital for head injury and assault to the head. Part
2: Ethnic group. Br J Oral Maxillofac Surg 1999;37:301-8
x Muthukrishnan A, Walters H, Douglas PS. An audit of antibiotic
Graham Roberts is professor of paediatric dentistry, Crispian Scully is prescribing by general practitioners in the initial management of
dean, and Rosemary Shotts is honorary lecturer at the Eastman acute dental infection. Dent Update 1996;23:316-8
Dental Institute for Oral Health Care Sciences, University College x Nelson LP, Shusterman S. Emergency management of oral trauma
London, University of London (www.eastman.ucl.ac.uk). in children. Curr Opin Pediatr 1997;9:242-5
x Roberts G, Longhurst P. Oral and dental trauma in children and
The ABC of Oral Health is edited by Crispian Scully
adolescents. Oxford: Oxford University Press, 1996
Crispian Scully is grateful for the advice of Dr Rosemary Toy, general x Sheller B, Williams BJ, Lombardi SM. Diagnosis and treatment of
practitioner, Rickmansworth, Hertfordshire. dental caries-related emergencies in a children’s hospital. Pediatr
Dent 1997;19:470-5
BMJ 2000;321:559-62
Corrections
ABC of oral health: Dental damage, sequelae, and prevention ABC of oral health: Periodontal disease
Two errors occurred in this article by Ruth Holt and colleagues In this article by John Coventry and colleagues (1 July, pp 36-9) the
(24 June, pp 1717-9). First, the picture of tooth erosion (bottom of third picture on page 38 is wrongly labelled as pregnancy epulis. In
p 1717) is upside down. Second, in the table of recommended fact, it shows pyogenic granuloma in a child.
fluoride dietary supplementation for caries prophylaxis in high risk
children (p 1718) the supplementation for children aged > 6 years ABC of oral health: Oral cancer
old in areas with water fluoride levels < 0.3 ppm should have read In this article by Crispian Scully and Stephen Porter (8 July, pp 97-
1 mg/day (not 1 g/day). 100) the picture of carcinoma of the tongue (p 97) is upside down.
562 BMJ VOLUME 321 2 SEPTEMBER 2000 bmj.com
View publication stats
S-ar putea să vă placă și
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (121)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (588)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (895)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (73)
- Case Study Analysis - WeWorkDocument8 paginiCase Study Analysis - WeWorkHervé Kubwimana50% (2)
- S O S Services Alert Level Help Sheet - REFERENCIALESDocument20 paginiS O S Services Alert Level Help Sheet - REFERENCIALESDavid Poma100% (1)
- Anesthesia For Paediatric DentistryDocument18 paginiAnesthesia For Paediatric DentistryErfiadi Nur FahmiÎncă nu există evaluări
- I. Objectives:: Semi-Detailed Lesson Plan in Reading and Writing (Grade 11)Document5 paginiI. Objectives:: Semi-Detailed Lesson Plan in Reading and Writing (Grade 11)Shelton Lyndon CemanesÎncă nu există evaluări
- Business Plan - A TeahouseDocument6 paginiBusiness Plan - A TeahouseJoe DÎncă nu există evaluări
- Odontogenic InfectionsDocument27 paginiOdontogenic InfectionsEmad Hussien Haj-Abdulla100% (2)
- EBM On Harm - Dentistry 2010Document16 paginiEBM On Harm - Dentistry 2010Erfiadi Nur FahmiÎncă nu există evaluări
- Comparison of Nitrous Oxidemidazolam and Nitrous oDocument9 paginiComparison of Nitrous Oxidemidazolam and Nitrous oErfiadi Nur FahmiÎncă nu există evaluări
- Bru X Is M Consensus 2018Document9 paginiBru X Is M Consensus 2018Erfiadi Nur FahmiÎncă nu există evaluări
- ElevatorDocument2 paginiElevatorErfiadi Nur FahmiÎncă nu există evaluări
- Journal of Oral and Maxillofacial Surgery Volume Issue 2017 (Doi 10.1016/j.joms.2017.04.045) Best, Adrian D. de Silva, R.K. Thomson, W.M. Tong, Darryl C. - The Efficacy of Codeine When Added To PDFDocument24 paginiJournal of Oral and Maxillofacial Surgery Volume Issue 2017 (Doi 10.1016/j.joms.2017.04.045) Best, Adrian D. de Silva, R.K. Thomson, W.M. Tong, Darryl C. - The Efficacy of Codeine When Added To PDFErfiadi Nur FahmiÎncă nu există evaluări
- 152 1394 2 PB PDFDocument2 pagini152 1394 2 PB PDFErfiadi Nur FahmiÎncă nu există evaluări
- Inclusion and Exclusion Criteria: Experimental Designs: Preliminary InfoDocument13 paginiInclusion and Exclusion Criteria: Experimental Designs: Preliminary Infoa1savedÎncă nu există evaluări
- Odontogenicinfection 130303003840 Phpapp02Document141 paginiOdontogenicinfection 130303003840 Phpapp02Erfiadi Nur FahmiÎncă nu există evaluări
- Hubungan Pola Asuh Orang Tua Dengan Status Kebersihan Gigi Dan Mulut Siswa Tuna Netra Kelas V Dan VI SDLB A YPAB Surabaya Isnanto Dwi Rahayu Poltekkes SurabayaDocument8 paginiHubungan Pola Asuh Orang Tua Dengan Status Kebersihan Gigi Dan Mulut Siswa Tuna Netra Kelas V Dan VI SDLB A YPAB Surabaya Isnanto Dwi Rahayu Poltekkes SurabayaErfiadi Nur FahmiÎncă nu există evaluări
- Heart Diseases Dental TreatmentDocument2 paginiHeart Diseases Dental TreatmentErfiadi Nur FahmiÎncă nu există evaluări
- Pregnancy Oral HealthcareDocument2 paginiPregnancy Oral HealthcareErfiadi Nur FahmiÎncă nu există evaluări
- Pregnancy Oral HealthcareDocument2 paginiPregnancy Oral HealthcareErfiadi Nur FahmiÎncă nu există evaluări
- Cuentos CADEDocument6 paginiCuentos CADEMäuricio E. González VegaÎncă nu există evaluări
- Wordbank 15 Youtube Writeabout1Document2 paginiWordbank 15 Youtube Writeabout1Olga VaizburgÎncă nu există evaluări
- When I Was A ChildDocument2 paginiWhen I Was A Childapi-636173534Încă nu există evaluări
- Your Bentley Bentayga V8: PresentingDocument9 paginiYour Bentley Bentayga V8: PresentingThomas SeiferthÎncă nu există evaluări
- Ezpdf Reader 1 9 8 1Document1 paginăEzpdf Reader 1 9 8 1AnthonyÎncă nu există evaluări
- Letter of Acceptfor TDocument3 paginiLetter of Acceptfor TCCSÎncă nu există evaluări
- Chanakya: For The Indian Television Series Based On His Life, SeeDocument11 paginiChanakya: For The Indian Television Series Based On His Life, SeeTrinadh CrazyguyÎncă nu există evaluări
- Asme b16.3 (1998) Malleable Iron Threaded FittingsDocument30 paginiAsme b16.3 (1998) Malleable Iron Threaded FittingsMarcos RosenbergÎncă nu există evaluări
- Matokeo CBDocument4 paginiMatokeo CBHubert MubofuÎncă nu există evaluări
- Qcfi Durgapur Chapter: Question & Answers BankDocument13 paginiQcfi Durgapur Chapter: Question & Answers Bankdeepakhishikar24Încă nu există evaluări
- COMMISSIONING COUPLE Aafidavit SANKET DOCTORDocument2 paginiCOMMISSIONING COUPLE Aafidavit SANKET DOCTORYogesh ChaudhariÎncă nu există evaluări
- Silk Road Ensemble in Chapel HillDocument1 paginăSilk Road Ensemble in Chapel HillEmil KangÎncă nu există evaluări
- 1Z0-061 Sample Questions AnswersDocument6 pagini1Z0-061 Sample Questions AnswersLaura JohnstonÎncă nu există evaluări
- 1000 KilosDocument20 pagini1000 KilosAbdullah hayreddinÎncă nu există evaluări
- Pepcoding - Coding ContestDocument2 paginiPepcoding - Coding ContestAjay YadavÎncă nu există evaluări
- Wire Rope TesterDocument4 paginiWire Rope TesterclzagaÎncă nu există evaluări
- Estill Voice Training and Voice Quality Control in Contemporary Commercial Singing: An Exploratory StudyDocument8 paginiEstill Voice Training and Voice Quality Control in Contemporary Commercial Singing: An Exploratory StudyVisal SasidharanÎncă nu există evaluări
- EstoqueDocument56 paginiEstoqueGustavo OliveiraÎncă nu există evaluări
- EC105Document14 paginiEC105api-3853441Încă nu există evaluări
- Portfolio AdityaDocument26 paginiPortfolio AdityaAditya DisÎncă nu există evaluări
- Mang-May-Tinh - 03a.-Dns1 - (Cuuduongthancong - Com)Document52 paginiMang-May-Tinh - 03a.-Dns1 - (Cuuduongthancong - Com)Anh Quân TrầnÎncă nu există evaluări
- T Rex PumpDocument4 paginiT Rex PumpWong DaÎncă nu există evaluări
- Laporan Keuangan TRIN Per Juni 2023-FinalDocument123 paginiLaporan Keuangan TRIN Per Juni 2023-FinalAdit RamdhaniÎncă nu există evaluări
- Name: Mercado, Kath DATE: 01/15 Score: Activity Answer The Following Items On A Separate Sheet of Paper. Show Your Computations. (4 Items X 5 Points)Document2 paginiName: Mercado, Kath DATE: 01/15 Score: Activity Answer The Following Items On A Separate Sheet of Paper. Show Your Computations. (4 Items X 5 Points)Kathleen MercadoÎncă nu există evaluări
- NSTP SlabDocument2 paginiNSTP SlabCherine Fates MangulabnanÎncă nu există evaluări
- Adhesive Film & TapeDocument6 paginiAdhesive Film & TapeJothi Vel MuruganÎncă nu există evaluări