Documente Academic
Documente Profesional
Documente Cultură
Ectopic Pregnancy: A Guide For Patients
Încărcat de
Riany Jade SabrinaTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Ectopic Pregnancy: A Guide For Patients
Încărcat de
Riany Jade SabrinaDrepturi de autor:
Formate disponibile
Ectopic Pregnancy
A Guide for Patients
PATIENT INFORMATION SERIES
Ectopic Pregnancy.indd 1 9/19/14 9:29 AM
Published by the American Society for Reproductive Medicine under the direction
of the Patient Education Committee and the Publications Committee. No portion
herein may be reproduced in any form without written permission. This booklet
is in no way intended to replace, dictate, or fully define evaluation and treatment
by a qualified physician. It is intended solely as an aid for patients seeking general
information on issues in reproductive medicine.
Copyright © 2014 by the American Society for Reproductive Medicine
Ectopic Pregnancy.indd 2 9/19/14 9:29 AM
AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE
ECTOPIC PREGNANCY
A Guide for Patients Revised 2014
A glossary of italicized words is located at the end of this booklet.
INTRODUCTION
The diagnosis of an ectopic pregnancy is usually unexpected and is often emotionally
traumatic. Many women may have only recently discovered they were pregnant
when they receive the diagnosis. Some women diagnosed with an ectopic pregnancy
do not even know they are pregnant and suddenly must think about the possibility
of major surgery or medical treatment. This booklet is designed to provide
information on the diagnosis and treatment of ectopic pregnancy.
Definition
Ectopic pregnancies account for 1% to 2% of all conceptions. An ectopic
pregnancy is an early embryo (fertilized egg) that has implanted outside of
the uterus (womb), the normal site for implantation. In normal conception,
the egg is fertilized by the sperm inside the fallopian tube. The resulting
embryo travels through the tube and reaches the uterus 3 to 4 days later.
However, if the fallopian tube is blocked or damaged and unable to
transport the embryo to the uterus, the embryo may implant in the lining
of the tube, resulting in an ectopic pregnancy. The fallopian tube cannot
support the growing embryo. After several weeks the tube can rupture and
bleed, resulting in a potentially serious situation.
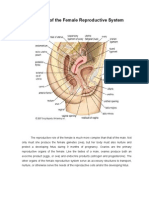
Ninety-five percent of ectopic pregnancies implant in the fallopian tube,
but they also can occur in the cervix, ovary (Fig. 1), or even within the
abdomen (abdominal pregnancy). Abdominal pregnancies are extremely rare
and can progress quite late into the pregnancy before they are discovered.
Fetuses that grow in the abdomen who could survive after birth have been
delivered, on rare occasions, by laparotomy (abdominal surgery).
Women who have ectopic pregnancies, particularly if they have been
attempting to conceive for a long period of time, often ask whether the
pregnancy can be removed from the tube and then transplanted into the
uterus where it might grow normally. Unfortunately, this is not possible
with present medical science.
3
Ectopic Pregnancy.indd 3 9/19/14 9:29 AM
Interstitial Isthmic
Ampullary
Normal intrauterine
(embryo properly
implanted in lining) Ovarian
Cervical
Figure 1. Female reproductive system showing sites of ectopic pregnancy and normal
intrauterine pregnancy.
Causes
Women who already have damaged tubes are more likely to develop an
ectopic pregnancy. In fact, 50% of ectopic pregnancies are associated
with some degree of tubal disease. Fallopian tube damage commonly
results from prior pelvic infection, such as gonorrhea, chlamydia, or other
sexually transmitted infections (STIs). Tubal disease also may occur as a
result of endometriosis, appendicitis, previous pelvic surgery, or exposure
to diethylstilbestrol (DES). The pregnancies of women who conceive with
an IUD in place sometimes occur in the fallopian tube. Women who
conceive after having a tubal ligation for sterilization, reversal of a tubal
ligation, or any other type of tubal surgery also have a higher risk of having
an ectopic pregnancy. Women who conceive as a result of fertility drugs or
in vitro fertilization (IVF) have a slightly higher risk of having an ectopic
pregnancy as well as a combined intrauterine and ectopic pregnancy. For
more information on tubal damage and surgery, refer to the ASRM patient
information booklet titled, Tubal Factor Infertility.
Sometimes, there is no apparent explanation for why an ectopic pregnancy
has occurred. However, it is known that once a woman has had an ectopic
4
Ectopic Pregnancy.indd 4 9/19/14 9:29 AM
pregnancy, she has a higher chance of having another one and should be
monitored carefully if another pregnancy is attempted or suspected.
Symptoms
Delayed or abnormal bleeding can be an early sign of an ectopic pregnancy.
If pregnancy is confirmed, early abnormal levels of human chorionic
gonadotropin (hCG), pelvic pain, and/or irregular bleeding in the first weeks
of pregnancy can indicate an ectopic pregnancy. If a woman knows or
suspects that she is pregnant and has had pelvic or lower abdominal pain,
she should consult her physician, even if the pain decreases in severity or
stops altogether. Additionally, if a woman has any risk factors for an ectopic
pregnancy, including a previous ectopic pregnancy, she should check a home
pregnancy test if her period is delayed and consult her physician as soon as
she is pregnant. Early detection of an ectopic pregnancy may help minimize
the complications associated with ectopic pregnancies and offers the
opportunity for other treatment options. Sometimes an ectopic pregnancy is
suspected when an ultrasound does not show a pregnancy inside the uterus.
Until recently, ectopic pregnancies often were not diagnosed until 6 to 8
weeks into the pregnancy, when a woman was experiencing pelvic pain,
irregular vaginal bleeding, possible internal bleeding, and a tender feeling
in the pelvis. Under these circumstances, this represented a life-threatening
emergency, and major surgery (laparotomy) was required to remove the
pregnancy and control bleeding. Fortunately, most ectopic pregnancies are
now identified much earlier, often before the woman is even aware of an
acute problem. This is largely due to the availability of sensitive hormone
testing and ultrasound examinations.
Diagnosis
The tests that are often used to diagnose an early ectopic pregnancy include
the measurement of hCG and/or progesterone levels in the bloodstream,
ultrasound, laparoscopy, or dilation and curettage (D&C).
Human Chorionic Gonadotropin
In a normal pregnancy, the blood level of hCG, a hormone produced by the
placenta, should double approximately every 48 hours. If this doubling does
not occur, this suggests that the pregnancy may not be healthy. It may mean
a miscarriage or an ectopic pregnancy. Often measurements of hCG blood
levels are repeated to help make the diagnosis.
Progesterone
Progesterone levels in the bloodstream rise very early in the course of
a pregnancy. Low levels of this hormone are frequently associated with
5
Ectopic Pregnancy.indd 5 9/19/14 9:29 AM
an abnormal pregnancy, such as an ectopic pregnancy or an impending
miscarriage. However, progesterone levels alone do not always predict the
location or mean the pregnancy is healthy and are not routinely used to
diagnose ectopic pregnancy.
Ultrasound Examinations
Ultrasound can be used in the first 3 to 5 weeks after conception (as early as
1 to 3 weeks after a missed period) to determine whether or not a pregnancy
is inside the uterine cavity. Transvaginal ultrasound is much more sensitive
than abdominal ultrasound for this purpose. Ultrasound scans also can show
fluid or blood in the abdominal cavity, suggesting bleeding from an ectopic
pregnancy. Sometimes, the use of ultrasound, combined with hCG and/
or progesterone blood level measurements, can confirm the diagnosis of an
ectopic pregnancy without the need for a laparoscopy or D&C. Often, it is
not possible to see an ectopic pregnancy with ultrasound and the diagnosis
is considered when the pregnancy is not seen in the uterus when specific
levels of hCG are also present.
Laparoscopy
In some cases, a laparoscopy is needed to confirm the diagnosis of an ectopic
pregnancy. Sometimes, laparoscopy also can be used to treat the ectopic
pregnancy. Laparoscopy is an outpatient surgical procedure requiring
general anesthesia. A small telescope called a laparoscope is placed into the
abdominal cavity through a small incision (cut) in the navel. If necessary,
the doctor usually can remove the ectopic pregnancy by placing special
instruments through the laparoscope or through small incisions above the
pubic area. An overnight hospital stay usually is not necessary following
laparoscopy. For more information on laparoscopy, refer to the ASRM
patient information booklet titled, Laparoscopy and Hysteroscopy.
Dilation and Curettage (D&C)
If a woman’s blood hormone levels and ultrasounds show that the pregnancy
will end in miscarriage or an embryo that has not successfully attached to
the uterine wall, the physician may choose to gently scrape out the lining
of the uterus. This operation, known as a D&C, can be performed under
anesthesia either in the hospital or as an outpatient procedure. A woman’s
hCG levels will drop sharply following removal of a miscarriage. The
tissues taken from the uterus also are examined carefully by a pathologist.
If pregnancy tissue is seen, an ectopic pregnancy is very unlikely. However,
very rarely a double pregnancy can occur, one in the uterus and the other in
Ectopic Pregnancy.indd 6 9/19/14 9:29 AM
the fallopian tube (called a heterotopic pregnancy). If there is no evidence of
pregnancy tissue or the hCG levels do not drop sharply following a D&C,
the presence of an ectopic pregnancy must be considered.
TREATMENT
Prior to sensitive pregnancy tests and modern pelvic ultrasound, ectopic
pregnancies were usually diagnosed after they ruptured and had caused
internal bleeding. Surgery was the main treatment. Now, doctors can
detect pregnancy by the time a women is due for her menstrual period by
measuring blood hCG levels, and the location of a pregnancy usually can be
determined within 1 to 2 weeks. As a result, ectopic pregnancies often can
be diagnosed very early, even before symptoms develop. This allows some
ectopic pregnancies to be treated safely without the need for surgery.
Observation Alone
Some ectopic pregnancies resolve without treatment and can be managed
by observation alone. This is referred to as “expectant management”
and usually is limited to women with early ectopic pregnancies with no
symptoms and low serum hCG levels (usually <1,000 IU/L) that decrease
without treatment. Treatment of ectopic pregnancy by observation alone
can be used only for women who can dependably return for weekly blood
hCG levels or sooner if symptoms develop. Women being treated with
observation alone should avoid intercourse and strenuous exercise.
When hCG levels are <1,000 IU/L and dropping, and pelvic ultrasound
is unable to determine the location of the pregnancy, these pregnancies are
sometimes referred to as “biochemical pregnancies.” Approximately half are
actually ectopic pregnancies, and the rest are intrauterine pregnancies that
are destined to end as miscarriages. Observation alone will allow the great
majority of these to resolve without incident within a month. If the woman
experiences pain or related symptoms, or the hCG levels do not drop
appropriately or rise, treatment with the medicine methotrexate or surgery
will be necessary.
Medical Treatment
With early diagnosis of an ectopic pregnancy, medical (non-surgical)
treatment often is possible with the drug methotrexate. To be a candidate
for methotrexate treatment, a woman needs to be in stable condition with
no evidence of internal bleeding or severe pain. She also needs to maintain
communication with her physician during the treatment protocol and be
able to return for follow-up blood tests after treatment.
7
Ectopic Pregnancy.indd 7 9/19/14 9:29 AM
Methotrexate is a drug that was initially used to treat certain types of
cancers, some of which are derived from placental tissue. It is very effective
in destroying ectopic pregnancy tissue and allowing it to be reabsorbed by
the body. It can also destroy normal pregnancy tissue. Therefore, it is not
an option for women with a heterotopic pregnancy. Methotrexate is given
as a single intramuscular shot or as a series of shots over several days. Most
early ectopic pregnancies can be successfully treated with methotrexate. This
often leaves the tube open. Success is based largely on the size of the ectopic
pregnancy seen on the ultrasound exam and the level of hCG found on the
blood test. Women with large ectopic pregnancies or rapidly rising and/
or high levels of hCG (>10,000 IU/L) are less likely to respond to single-
dose methotrexate therapy. These women may be considered candidates for
multiple-dose methotrexate regimens or surgical treatment. If methotrexate
is successful, hCG levels should decrease to zero over the next 2 to 6 weeks.
If the hCG levels do not fall, methotrexate treatment may be repeated or the
pregnancy may be removed surgically.
There are no known long-term side effects from use of methotrexate. The
short-term side effects are few. The drug can cause temporary ulcers in the
mouth and other gastrointestinal areas and can cause temporary changes
in liver function. Rare complications include pneumonia. Decreased
platelet production, another rare complication, can cause bleeding within
2 weeks after the injection. Any woman with changes in liver blood tests,
anemia (low blood counts), or platelet disorders cannot take methotrexate.
A woman may have some abdominal pain for a few days due to the
resorption of the ectopic pregnancy. Any severe pain needs to be reported
to her physician. Women should limit sun exposure during treatment, as
methotrexate can cause sensitivity to sunlight and sunburn may occur.
When being treated with methotrexate, women should not drink alcohol or
take vitamins containing folic acid (folate).
Surgical Treatment
Until the last 20 years, ectopic pregnancies usually were treated by total
salpingectomy (removal of the entire tube [Fig. 2]) via laparotomy (major
abdominal surgery). Today, most surgeries for ectopic pregnancies are
performed by laparoscopy. Laparotomy usually is reserved for those ectopic
pregnancies that have ruptured, causing severe internal bleeding, or when
there is extensive scar tissue inside the abdomen and pelvis.
Ectopic Pregnancy.indd 8 9/19/14 9:29 AM
If the ectopic pregnancy is diagnosed early, before the tube ruptures, a
laparoscopic salpingostomy may be performed. In this procedure, the fallopian
tube is opened and the pregnancy tissue is removed while leaving the tube in
place (Fig. 3). The tube then heals on its own. In about 5% to 15% of cases,
some of the ectopic tissue may remain and continue to grow. This may be
treated by additional surgery to remove the tube or by using methotrexate
therapy. A partial salpingectomy (sometimes called a segmental resection, to
remove a middle segment of the tube [Fig. 2]) may be performed when the ends
of the tubes (the fimbriae) appear healthy and the ectopic pregnancy is small. If
only a small portion of the tube is removed, the tube may be rejoined later using
microsurgery. If the fallopian tube is extremely damaged, the ectopic pregnancy is
large, or the woman is bleeding excessively, a total salpingectomy is performed.
In rare cases when the ectopic pregnancy involves the ovary, a portion of the
ovary or the entire ovary may be removed.
Total salpingectomy
Tube containing ectopic pregnancy is
removed
Partial salpingectomy
Only section of tube containing ectopic
pregnancy is removed
Figure 2. Total salpingectomy with removal of the entire fallopian tube (top) and partial
salpingectomy showing removal of a section of the fallopian tube (bottom).Surgery to
rejoin the tube at a later time may be performed.
Ectopic Pregnancy.indd 9 9/19/14 9:29 AM
Fallopian tube
Uterine cavity Uterus
Endometrium
Ovary
Cervix Tube containing
ectopic pregnancy is
Vagina opened and tissue is
removed
Figure 3. In salpingostomy, the fallopian tube is opened and the ectopic pregnancy is
removed.
Operative Laparoscopy Versus Laparotomy for Ectopic Pregnancy
Up until the late 20th century, all gynecologic, reproductive, and tubal
operations were performed by opening the abdomen (called “laparotomy”)
using either a “bikini” or “up and down” skin incision several inches long.
Women usually remained in the hospital 2 to 5 days following surgery
and returned to work in 2 to 6 weeks, depending on the level of physical
activity required. Today, many of these operations can be performed by
“laparoscopy,” using a small telescope with a camera and 2 to 4 smaller
skin incisions approximately one-quarter to one-half inch long. Following
laparoscopy, women generally are able to go home the day of surgery and
recover more quickly, returning to full activities in 3 to 7 days.
Despite the advantages of laparoscopy, not all surgeries for ectopic
pregnancy can be done with this technique. Emergency situations with
extensive internal bleeding or large amounts of intra-abdominal adhesions
(scar tissue) may require immediate laparotomy. Some types of operations
also may be too risky to perform laparoscopically, while in others it is
not clear that laparoscopy yields results as good as those by laparotomy.
Finally, the surgeon’s training, skill, and experience also play a significant
10
Ectopic Pregnancy.indd 10 9/19/14 9:29 AM
role in deciding whether laparoscopy or laparotomy should be used. When
considering a pelvic operation, the patient and doctor should discuss the
pros and cons of performing a laparotomy versus a laparoscopy, including
the surgical risks.
OUTCOME
A woman who has had an ectopic pregnancy has a lower chance of
becoming pregnant again. In addition, her chance of having another ectopic
pregnancy is higher. Fortunately, over half of women who experience
an ectopic pregnancy will have a healthy baby sometime in the future.
Women with 2 or more ectopic pregnancies may have tubal disease and may
want to consider IVF. However, there is still about a 1.5% chance of ectopic
pregnancy with IVF. For more information on IVF, refer to the ASRM
patient information booklet titled Assisted Reproductive Technologies.
Emotional Aspects
Ectopic pregnancy is a physically and emotionally traumatic experience.
In addition to experiencing the loss of a pregnancy, women may fear the
loss of future fertility. Feelings of grief and loss are normal. Sadness, anger,
self-blame, guilt, and depression are part of the grieving process and need
to be acknowledged and expressed. It can be helpful to share these feelings
in a support group, such as RESOLVE or SHARE, or through counseling.
Time is necessary for both physical and emotional healing before attempting
another pregnancy. For more information on these support groups, consult
the Resources section below.
SUMMARY
Ectopic pregnancy refers to any pregnancy implanted outside the uterus,
usually in the fallopian tube. Early diagnosis is often made using sensitive
hormone tests, ultrasound exams, laparoscopy, and/or D&C. Modern
surgical and medical treatments frequently allow women to avoid extensive
surgery and preserve their fallopian tube. Although the risk of having
another ectopic pregnancy is increased, many women will successfully
conceive and have children in the future, either naturally or with the aid of
an assisted reproductive technology such as IVF.
RESOURCES:
AMERICAN FERTILITY ASSOCIATION -- http://www.theafa.org/
RESOLVE -- http://www.resolve.org/
SHARE (Source of Help in Airing and Resolving Experiences) -- http://www.nationalshare.org/
11
Ectopic Pregnancy.indd 11 9/19/14 9:29 AM
GLOSSARY
Abdominal pregnancy. An ectopic (extrauterine) pregnancy that has
implanted on structures in the abdomen other than the uterus, fallopian
tubes, or ovaries. It usually implants on tissue in the abdomen known as the
omentum.
Appendicitis. A condition where the appendix (a tubular structure attached
to the large colon) becomes infected and inflamed and can be associated
with the formation of adhesions in the proximity of the fallopian tube.
Cervix. The lower narrow end of the uterus that connects the uterus to the
vagina.
Diethylstilbestrol (DES). A synthetic hormone formerly given during
pregnancy to prevent miscarriage. Women born from treated pregnancies
can have abnormalities of the reproductive system, including an increased
risk of ectopic pregnancy.
Dilation and curettage (D&C). An outpatient surgical procedure during
which the cervix is dilated and the lining of the uterus is scraped out. The
tissue often is microscopically examined for the presence of abnormality or
pregnancy tissue.
Ectopic pregnancy. A pregnancy that implants outside of the uterus, usually
in the fallopian tube. The tube may rupture or bleed as the pregnancy grows
and present a serious medical situation.
Embryo. The earliest stage of human development arising after the union of
the sperm and egg (fertilization).
Endometriosis. A condition where patches of endometrial-like tissue
develop outside the uterine cavity in abnormal locations such as the ovaries,
fallopian tubes, and abdominal cavity. Endometriosis can grow with
hormonal stimulation, causing pain, inflammation, and scar tissue. It also
may be associated with pelvic pain and infertility.
Fallopian tube. A pair of hollow tubes attached one on each side of
the uterus through which the egg travels from the ovary to the uterus.
Fertilization usually occurs in the fallopian tube. The fallopian tube is the
most common site of ectopic pregnancy.
Fertility drugs. Drugs that stimulate the ovaries to produce mature eggs so
that they can be released at ovulation.
Fimbriae. The flared (finger-like) end of the fallopian tube that sweeps over
the surface of the ovary and helps to direct the egg into the tube.
Human chorionic gonadotropin (hCG). This hormone is produced by the
placenta. Its detection is the basis of most pregnancy tests.
Implantation. The process whereby an embryo embeds in the uterine
lining in order to obtain nutrition and oxygen. Sometimes, an embryo will
implant in areas other than the uterus, such as in a fallopian tube. This is
known as an ectopic pregnancy.
12
Ectopic Pregnancy.indd 12 9/19/14 9:29 AM
In vitro fertilization (IVF). A method of assisted reproduction that
involves combining an egg with sperm in a laboratory dish. If the egg
fertilizes and begins cell division, the resulting embryo is transferred into
the woman’s uterus where it will hopefully implant in the uterine lining and
further develop. IVF may be performed in conjunction with medications
that stimulate the ovaries to produce multiple eggs in order to increase
the chances of successful fertilization and implantation. IVF bypasses the
fallopian tubes and is often the treatment of choice for women who have
badly damaged or absent tubes.
Laparoscope. A thin, lighted, telescope-like viewing instrument that
is usually inserted through the navel into the abdomen to examine the
contents of the pelvic and abdominal cavities. Other small incisions also
may be made, and additional instruments inserted, to facilitate diagnosis
and allow surgical correction of pelvic abnormalities. The laparoscope can be
used as both a diagnostic and operative instrument.
Laparoscopy. The insertion of a long, thin, lighted, telescope-like
instrument called a laparoscope into the abdomen through an incision,
usually in the navel, to visually inspect the organs in the abdominal cavity.
Other small incisions also may be made, and additional instruments
inserted, to facilitate diagnosis and allow surgical correction of
abnormalities. The surgeon can sometimes remove scar tissue and open
closed fallopian tubes during this procedure.
Laparotomy. Major abdominal surgery through an incision in the
abdominal wall.
Methotrexate. A medication that destroys pregnancy-related tissue and
hastens reabsorption of this tissue in a woman with an ectopic pregnancy.
Microsurgery. A type of surgery that uses magnification, meticulous
technique, and fine suture material in order to get precise surgical results.
Microsurgery is important for certain types of tubal surgery in the female, as
well as for vasectomy reversal in the male.
Miscarriage. The naturally occurring expulsion of a nonviable fetus and
placenta from the uterus, also known as spontaneous abortion or pregnancy
loss.
Ovaries. The two female sex glands in the pelvis, located one on each side
of the uterus. The ovaries produce eggs and hormones including estrogen,
progesterone, and androgen.
Partial salpingectomy. An operation in which the section of a fallopian
tube containing an ectopic pregnancy is removed. This procedure
attempts to preserve most of the tube for subsequent reattachment using
microsurgery in order to achieve future fertility.
Pneumonia. Lung inflammation.
Progesterone. A female hormone secreted by the corpus luteum after
ovulation during the second half of the menstrual cycle (luteal phase).
13
Ectopic Pregnancy.indd 13 9/19/14 9:29 AM
It prepares the lining of the uterus (endometrium) for implantation of a
fertilized egg and also allows for complete shedding of the endometrium at
the time of menstruation. In the event of pregnancy, the progesterone level
remains stable beginning a week or so after conception.
Salpingectomy. An operation in which one or both of the fallopian tubes
are removed.
Salpingo-oophorectomy. Removal of a fallopian tube and ovary together.
Salpingostomy. A surgical procedure in which the wall of the fallopian tube
is opened and the ectopic pregnancy is removed. The tubal incision heals
spontaneously.
Sexually transmitted infection (STI). An infection, such as chlamydia or
gonorrhea, which is transmitted by sexual activity. In the female, some STIs
can cause pelvic infections and lead to infertility by damaging the fallopian
tubes and increasing the risk of ectopic pregnancy. In the male, STIs can
cause blockage of the ductal system that transports sperm.
Transvaginal ultrasound. An imaging technique in which a smooth
cylindrical probe that uses sound waves to view organs on a video screen is
placed in the vagina.
Tubal ligation. A surgical procedure in which the fallopian tubes are
clamped, clipped, or cut to prevent pregnancy.
Ulcer. A lesion (sore) on the surface of the skin or on a mucous surface,
usually inflamed. As an occasional side effect of methotrexate therapy,
temporary ulcers may form in the mouth.
Ultrasound. A picture of internal organs produced by high frequency
sound waves viewed as an image on a video screen; used to monitor growth
of ovarian follicles, retrieve eggs, or monitor growth and development of a
fetus. Ultrasound can be performed either abdominally or vaginally.
Uterus (womb). The hollow, muscular female organ in the pelvis in which
an embryo implants and grows during pregnancy. The lining of the uterus,
called the endometrium, produces the monthly menstrual blood flow when
there is no pregnancy.
Let Us Know What You Think
Email your comments on this booklet to asrm@asrm.org.
In the subject line, type “Attention: Patient Education Committee.”
14
Ectopic Pregnancy.indd 14 9/19/14 9:29 AM
15
Ectopic Pregnancy.indd 15 9/19/14 9:29 AM
AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE
1209 MONTGOMERY HIGHWAY
BIRMINGHAM, ALABAMA 35216-2809
(205) 978-5000 • ASRM@ASRM.ORG • WWW.ASRM.ORG
Ectopic Pregnancy.indd 16 9/19/14 9:29 AM
S-ar putea să vă placă și
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (895)
- Induction of Labor in Nullipara Is Associated With An Increased Risk of Cesarean Delivery and Postpartum HemorrhageDocument16 paginiInduction of Labor in Nullipara Is Associated With An Increased Risk of Cesarean Delivery and Postpartum HemorrhageRiany Jade SabrinaÎncă nu există evaluări
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Allergic and Irritant Contact Dermatitis: Pathophysiology and Immunological DiagnosisDocument8 paginiAllergic and Irritant Contact Dermatitis: Pathophysiology and Immunological DiagnosisRiany Jade SabrinaÎncă nu există evaluări
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- TNSS AU1.0 eng-USDocument1 paginăTNSS AU1.0 eng-USRiany Jade SabrinaÎncă nu există evaluări
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- TNSS AU1.0 eng-AUori ReviewDocument1 paginăTNSS AU1.0 eng-AUori ReviewRiany Jade SabrinaÎncă nu există evaluări
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- Occupational Skin Diseases in Construction Workers at A Large Construction SiteDocument3 paginiOccupational Skin Diseases in Construction Workers at A Large Construction SiteRiany Jade SabrinaÎncă nu există evaluări
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (266)
- Literarture ReviewDocument10 paginiLiterarture ReviewRiany Jade SabrinaÎncă nu există evaluări
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (400)
- About My Needs?: Breadwinner, Provider or Pencari Nafkah'Document17 paginiAbout My Needs?: Breadwinner, Provider or Pencari Nafkah'Riany Jade SabrinaÎncă nu există evaluări
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- Accepted Manuscript: Respiratory MedicineDocument33 paginiAccepted Manuscript: Respiratory MedicineRiany Jade SabrinaÎncă nu există evaluări
- Chlamydia Antibody Testing Helps in Identifying Females With Possible Tubal Factor InfertilityDocument6 paginiChlamydia Antibody Testing Helps in Identifying Females With Possible Tubal Factor InfertilityRiany Jade SabrinaÎncă nu există evaluări
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- Current Chlamydia Trachomatis Infection, A Major Cause of InfertilityDocument7 paginiCurrent Chlamydia Trachomatis Infection, A Major Cause of InfertilityRiany Jade SabrinaÎncă nu există evaluări
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (588)
- Effects of Chlamydia Trachomatis Infection On Fertility A Case-Control StudyDocument7 paginiEffects of Chlamydia Trachomatis Infection On Fertility A Case-Control StudyRiany Jade SabrinaÎncă nu există evaluări
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- Zeller 2004Document6 paginiZeller 2004Riany Jade SabrinaÎncă nu există evaluări
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- Maternal Pulse Pressure and The Risk of Postepidural ComplicationsDocument11 paginiMaternal Pulse Pressure and The Risk of Postepidural ComplicationsRiany Jade SabrinaÎncă nu există evaluări
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (74)
- Abstrak CabeDocument1 paginăAbstrak CabeRiany Jade SabrinaÎncă nu există evaluări
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (345)
- Use of Epidural Clonidine For The Management of Analgesia in The Opioid Addicted Parturient On Buprenorphine Maintenance Therapy: An Observational StudyDocument6 paginiUse of Epidural Clonidine For The Management of Analgesia in The Opioid Addicted Parturient On Buprenorphine Maintenance Therapy: An Observational StudyRiany Jade SabrinaÎncă nu există evaluări
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- Ante-Partum Fetal Assessment and Early Neonatal Outcome in Pregnancies Complicated With IugrDocument58 paginiAnte-Partum Fetal Assessment and Early Neonatal Outcome in Pregnancies Complicated With IugrRiany Jade SabrinaÎncă nu există evaluări
- HheheheheDocument6 paginiHheheheheRiany Jade SabrinaÎncă nu există evaluări
- The Age Associations of Blood Pressure, Cholesterol, and GlucoseDocument18 paginiThe Age Associations of Blood Pressure, Cholesterol, and GlucoseRiany Jade SabrinaÎncă nu există evaluări
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- The Depression Anxiety Stress Scale (DASS) : DescriptionDocument1 paginăThe Depression Anxiety Stress Scale (DASS) : DescriptionRiany Jade SabrinaÎncă nu există evaluări
- Hesc 107Document14 paginiHesc 107C. Kesav ReddyÎncă nu există evaluări
- Physiology of Menstruation: TH THDocument7 paginiPhysiology of Menstruation: TH THRainy DaysÎncă nu există evaluări
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2259)
- Condyloma AcuminataDocument79 paginiCondyloma Acuminatayhanne100% (16)
- كامل نساءDocument213 paginiكامل نساءniemand da100% (1)
- Lab Report Bio Experiment 5 (Mouse Dissection)Document14 paginiLab Report Bio Experiment 5 (Mouse Dissection)Hakim SunaeÎncă nu există evaluări
- Catfish RearingDocument109 paginiCatfish RearingKenneth LauÎncă nu există evaluări
- Lesson Plan On Polycystic Ovary Syndrome (Pcos)Document22 paginiLesson Plan On Polycystic Ovary Syndrome (Pcos)N.Subhashini100% (5)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (121)
- Reproductive System ModuleDocument17 paginiReproductive System ModulePATRICIA KAYE RIOÎncă nu există evaluări
- Powerpoint Case Study of MiscarriageDocument25 paginiPowerpoint Case Study of MiscarriageAngel CauilanÎncă nu există evaluări
- Maturity and Spawning of Secutor Insidiator Along The Kerala CoastDocument6 paginiMaturity and Spawning of Secutor Insidiator Along The Kerala CoastAnonymous cXJcwLzEcSÎncă nu există evaluări
- L. Pereira - Embryology - Updates and Highlights On Classic Topics (2012, Intech)Document222 paginiL. Pereira - Embryology - Updates and Highlights On Classic Topics (2012, Intech)Katy AÎncă nu există evaluări
- Endocrine SystemDocument52 paginiEndocrine Systemnurshuhada zainuddinÎncă nu există evaluări
- 12 PraDocument30 pagini12 Praxelivo8277Încă nu există evaluări
- Benign and Malignat Ovarian TumorsDocument67 paginiBenign and Malignat Ovarian TumorsZEMENAY TRUNEHÎncă nu există evaluări
- Cow ReproductiveDocument5 paginiCow Reproductiveastyrafe100% (1)
- Pencitraan Brightness Mode Ultrasonografi Untuk Deteksi Kebuntingan Dan Pengamatan Perkembangan Fetus Kucing (Felis Catus)Document54 paginiPencitraan Brightness Mode Ultrasonografi Untuk Deteksi Kebuntingan Dan Pengamatan Perkembangan Fetus Kucing (Felis Catus)Pa lamÎncă nu există evaluări
- The Menstrual Cycle: Sevag OuzounianDocument20 paginiThe Menstrual Cycle: Sevag OuzounianBijay Kumar MahatoÎncă nu există evaluări
- Reproducrive SystemDocument15 paginiReproducrive SystemEfren GuinumtadÎncă nu există evaluări
- Reproductive System of CockroachDocument3 paginiReproductive System of Cockroachhui_junÎncă nu există evaluări
- Anatomy - B. Rabischong - GRDocument20 paginiAnatomy - B. Rabischong - GRAnonymous UHnQSkxLBDÎncă nu există evaluări
- Anatomy and Physiology Reproductive SystemDocument91 paginiAnatomy and Physiology Reproductive SystemApril BenaventeÎncă nu există evaluări
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- Benign Gynecologic TumorsDocument57 paginiBenign Gynecologic TumorsDexter IanÎncă nu există evaluări
- Anatomy of The Female Reproductive SystemDocument9 paginiAnatomy of The Female Reproductive SystemPinkeyinthecityÎncă nu există evaluări
- Human Reproductive System (Female Reproductive System)Document4 paginiHuman Reproductive System (Female Reproductive System)Jonalyn Brozula Capobres100% (5)
- Science: Role of HormonesDocument16 paginiScience: Role of Hormonescharyl jean cagaÎncă nu există evaluări
- Group 9. Presentation. Animal Form and Function 2Document29 paginiGroup 9. Presentation. Animal Form and Function 2Dat HoangÎncă nu există evaluări
- Adolescence and Puberty PDFDocument318 paginiAdolescence and Puberty PDFjorge torresÎncă nu există evaluări
- ESHRE Guideline - POI 2015 - FINAL - 11122015Document161 paginiESHRE Guideline - POI 2015 - FINAL - 11122015Md ShotonÎncă nu există evaluări
- Chapter 10 - The Endocrinology of Mammalian ReproductionDocument58 paginiChapter 10 - The Endocrinology of Mammalian ReproductionNicole CorreiaÎncă nu există evaluări
- 4 Male and Female Reproductive Organs PPTDocument71 pagini4 Male and Female Reproductive Organs PPTDanica Marie Sibay100% (1)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)De la EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Evaluare: 3 din 5 stele3/5 (1)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDDe la EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDEvaluare: 5 din 5 stele5/5 (2)
- The Age of Magical Overthinking: Notes on Modern IrrationalityDe la EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityEvaluare: 4 din 5 stele4/5 (29)