Documente Academic
Documente Profesional
Documente Cultură
FM1010 Anatomy Learning Objectives
Încărcat de
Jonathan NgDrepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
FM1010 Anatomy Learning Objectives
Încărcat de
Jonathan NgDrepturi de autor:
Formate disponibile
FM1010 Anatomy Learning Objectives
Lecturer: Dr. Kathleen A. Quane
FM1010 Module Content:
Anatomy of nerve (including the autonomic nervous system), muscle, joints, musculoskeletal
system, upper and lower limbs. Histology of the cell, surface epithelium, skin, nerve, muscle,
and connective tissues. Radiological anatomy and medical imaging of upper and lower limbs.
Gametes and fertilisation; general embryology; early development of embryo and
membranes, implantation, placenta. Development of body wall and limbs.
Anatomical Society Core Syllabus
In 2016, the Anatomical Society of Great Britain and Ireland (ASGBI) education committee
produced a revised syllabus describing the core anatomical knowledge that it felt should be
possessed by medical students1. In the UK, the responsibility for “Deciding on the
knowledge, skills and behaviours required of medical graduates” rests with the General
Medical Council (GMC) which publishes its instructions in “Tomorrow’s Doctors” which
identified the ASGBI syllabus as the anatomical knowledge necessary for medical students.
The anatomy teaching at UCC is fully informed by the ASGBI syllabus.
1
Smith CF, Finn GM, Stewart J, et al. The Anatomical Society core regional anatomy
syllabus for undergraduate medicine. J Anat. 2016 Jan;228(1):15-23. doi: 10.1111/joa.12405.
Epub 2015 Nov 27. Review
FM1010 Anatomy Course
The anatomy course is designed to enable you achieve an understanding of (i) the basic
structure of the human body, (ii) the principles underlying its organisation and (iii) the
relationship of structure to function, in particular that of the locomotor system and its
neurological control. It includes the following components:
SYSTEMATIC ANATOMY: The principles underlying the organisation and function of
the various systems.
TOPOGRAPHICAL ANATOMY: Regional and topographical anatomy and dissection of
the limbs, trunk, head and neck.
HISTOLOGY: Histological techniques; cytology; tissues; relationships of structure to
function.
RADIOLOGICAL ANATOMY: Radiological anatomy and medical imaging. Interpretation
of common diagnostic images.
EMBRYOLOGY: The study of the prenatal development of embryos and foetuses.
The term ‘anatomy’ used in the learning outcomes below encompasses the form,
functions, position and relations as well as the neurovascular connections of a given
structure or group of structures.
FM1010 SYSTEMATIC ANATOMY:
Anatomical terminology
Spinal nerve composition: motor, sensory neurons
Joints
Skeletal Muscle
Bones
Autonomic Nervous System
FM1010 Anatomy Learning Objectives KA Quane 1
Anatomical terminology
• Medical graduates should be able to communicate effectively with colleagues and be able to
understand and use anatomical language appropriately. Knowledge of accepted general
anatomical terminology is a prequisite for learning anatomy.
• Define and demonstrate the following basic terms relative to the anatomical position:
medial, median, lateral, proximal, distal, superior, inferior, deep, superficial, palmar, plantar,
anterior/ventral, posterior/ dorsal, cephalic/cranial, rostral, caudal.
• Describe the following basic anatomical planes: axial/transverse/horizontal, sagittal and
coronal.
• Define and demonstrate the basic terms used to describe movement: flexion, extension,
lateral flexion, pronation, supination, abduction, adduction (radial/ ulnar/deviation),
medial/internal and lateral/external rotation, inversion, eversion, plantar flexion, dorsiflexion,
protraction, retraction and circumduction.
.• Define the basic terms somatic and visceral/autonomic when used to describe parts of the
body and nervous systems of the body.
Spinal nerve composition: motor, sensory neurons
• Describe the anatomy of a typical spinal nerve, including its origin from dorsal and ventral
spinal roots, its main motor and cutaneous branches and any autonomic component.
• Define the terms dermatome and myotome.
Joints
• Define the term joint and outline the structural classifications of joints.
• Describe the anatomy of fibrous, cartilaginous (primary and secondary) and synovial joints.
Give examples of each.
• Describe the classification of synovial joints on the basis of shape (plane/gliding, hinge,
saddle, pivot, ellipsoid, ball and socket), giving examples.
• Name and demonstrate the axes of movements (degrees of freedom) at a joint. Define the
terms uniaxial, biaxial and multiaxial joints and give examples of each joint.
• Describe what is meant by the terms ‘close-packed position’ and ‘loose-packed position’.
• Clinical application: arthritis, joint dislocation, joint effusion.
Skeletal Muscle
• Name the layers of connective tissue that are found in and around a muscle fibre and briefly
describe a muscle’s blood and nerve supply.
FM1010 Anatomy Learning Objectives KA Quane 2
• Describe the ways in which muscles attach at origins and insertions.
• Define a muscle fascicle. Describe the classification of muscles based on the arrangements
of muscle fascicles (parallel, convergent, pennate, circular).
• Describe the structure of muscle bellies, tendons, aponeurosis, sesamoid bones, sesamoid
fibrocartilage, bursae and synovial sheaths.
• Describe the criteria used in naming muscles.
• Describe the functional classification of muscles (prime mover, antagonist, fixator,
synergist) and outline the functions of each type.
• Describe the anatomy of the neuromuscular junction,
• Define a motor unit and describe the anatomy of the motor unit.
• Define isometric, isotonic and eccentric contraction.
Bones
• Describe the classification of bones on the basis of shape (long, short, flat, irregular).
• Describe the structure of compact and spongy bone.
• Describe the gross anatomy of a typical long bone.
• Explain how bones withstand tension and compression.
• Outline the categories of bone markings.
• Outline the process of ossification (osteogenesis).
• Briefly describe the process of bone remodelling within the skeleton.
• Clinical application: osteoporosis, bone fractures.
Autonomic Nervous System
• Describe the classification of the nervous system.
• Compare the anatomy of the autonomic & somatic motor systems.
• Outline the differences between the sympathetic and parasympathetic divisions of the
autonomic nervous system.
FM1010 Anatomy Learning Objectives KA Quane 3
• Describe the anatomy of the parasympathetic divisions of the autonomic nervous system
including how it relates to the brain, cranial nerves and the sacral region of the spinal cord.
• Describe the anatomy of the sympathetic divisions of the autonomic nervous system
including how it relates to the spinal cord and spinal nerves.
• Describe the sympathetic function of the adrenal medulla.
FM1010 TOPOGRAPHICAL ANATOMY:
Posterior Triangle of the back
Upper Limb
Lower Limb
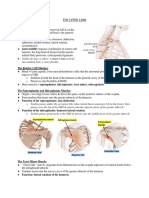
The Posterior Triangle of the Neck.
• Demonstrate the boundaries of the posterior triangle of the neck defined by the sternum,
clavicle, mastoid process, trapezius,and sternocleidomastoid.
• In the posterior triangle, demonstrate the position of the spinal accessory nerve, the roots
and trunks of the brachial plexus, the phrenic nerve, the external jugular vein and subclavian
vessels in relation to penetrating neck trauma.
• Describe the courses of the accessory and phrenic nerves in the neck.
• Apply knowledge of the anatomy of the accessory nerve to a neurological assessment of the
nerve.
• Describe the anatomy of the major structures passing between the neck, and the thorax and
the upper limb. Describe the courses and important relationships
of the subclavian arteries and veins.
• Identify anatomical features on prosections.
Upper Limb
Overview
Medical graduates should be able to describe the innervation, arterial supply, venous and
lymphatic drainage of the structures of the upper limb. They should be able to interpret
relevant standard diagnostic images using a range of modalities, with particular reference to
common sites of fractures. They should be able to explain the factors that influence the
stability of the joints of the upper limb. They should have a working knowledge of surface
anatomy (including the site of major pulse points, e.g. radial), dermatomes and peripheral
nerve distribution. They should be aware of the organisation of the deep fascia of the upper
limb and its clinical relevance to compartment syndromes.
Areas of the Upper Limb
• Describe the boundaries and contents of the axilla, including the major vessels and relevant
parts of the brachial plexus
FM1010 Anatomy Learning Objectives KA Quane 4
Bones of Upper Limb.
• Describe and demonstrate the main anatomical landmarks of the clavicle, scapula, humerus,
radius and ulna. Identify the bones of the wrist and hand and their relative positions, identify
those bones that are commonly injured, e.g. scaphoid.
• Describe the neurovascular structures lying in close relation to the bones and joints of the
upper limb which are at risk of injury following fracture or dislocation. Predict what the
functional effects of such injury might be.
Joints and Muscles of Upper Limb.
• Describe the fascial compartments enclosing the major muscle groups of the upper limb;
explain the functional and clinical importance of those compartments and their contents.
• Describe the anatomy of the pectoral girdle, explain the movements of the pectoral girdle;
identify the muscles and joints responsible for these movements. Name the main attachments
and nerve supply of these muscles.
• Describe the factors that contribute to the movement and stability of the gleno-humeral joint
and explain the functional and clinical consequences of its dislocation.
• Describe the anatomy of the elbow joint. Demonstrate the movements of flexion and
extension. Identify the muscles responsible for these movements. Name the main attachments
and nerve supply of these muscles.
• Describe the anatomy of the radio-ulnar joints. Explain the movements of supination and
pronation; identify the muscles responsible for these movements, name the main attachments
and describe the nerve supply of these muscles.
.
• Describe the anatomy of the wrist. Describe and demonstrate movements at the wrist joints
and name and identify the muscle groups responsible for the movements. Describe the
relative positions of the tendons, vessels and nerves in the region of the wrist in relation to
injuries.
• Name and demonstrate the movements of the fingers and thumb. Describe the position,
function and nerve supply of the muscles and tendons involved in these movements,
differentiating between those in the forearm and those intrinsic to the hand.
• Describe the main types of grip (power, precision and hook) and the role of the muscles and
nerves involved in executing them.
• Describe the position and function of the retinacula of the wrist and the tendon sheaths of
the wrist and hand in order to explain carpal tunnel syndrome and the spread of infection in
tendon sheaths.
Blood Vessels and lymphatics of Upper Limb.
• Describe the origin, course and distribution of the major arteries and their branches that
supply the shoulder, arm, forearm and hand in relation to common sites of injury. Explain the
FM1010 Anatomy Learning Objectives KA Quane 5
importance of anastomoses between the branches. Identify those sites where neurovascular
structures are at particular risk of damage from musculoskeletal injuries.
• Demonstrate the sites at which pulses of the brachial, radial and ulnar arteries may be
located.
• Describe the course of the main veins of the upper limb and contrast the functions of the
deep and superficial veins.
• Identify the common sites of venous access and describe their key anatomical relations.
• Describe the anatomy of the axillary lymph nodes and explain their importance in the
lymphatic drainage of the breast and skin of the trunk and upper limb and in the spread of
tumours
Nerves of Upper Limb.
• Describe the anatomy of the brachial plexus from its origin in the neck to its terminal
branches. Recognise brachial plexus injuries and explain their clinical presentation.
• Describe the origin, course and function of the axillary, radial, musculocutaneous, median
and ulnar nerves in the upper limb.
• Name the major muscles and muscle groups that the axillary, radial, musculocutaneous,
median and ulnar nerves supply, together with their sensory distribution. Predict the
consequences of injury to these nerves and describe how to test their functional integrity.
• Describe the anatomical basis of assessment of: cutaneous sensation in the dermatomes of
the upper limb, motor function, tendon reflexes, and muscle power in the upper limb.
• Describe the dermatomes and peripheral nerve distribution of the upper limb.
Upper Limb Prosections.
• Identify anatomical features on prosections of the upper limb.
Lower Limb
Overview
Medical graduates should be able to describe the innervation, arterial supply, venous and
lymphatic drainage of the structures of the lower limb. They should be able to interpret
relevant standard diagnostic images using a range of modalities, with particular reference to
common sites of fractures (neck and shaft of femur, tibia and fibula). They should be able to
explain the factors that influence the stability of the joints of the lower limb. They should
have a working knowledge of surface anatomy (including major pulse points e.g. femoral),
dermatomes and peripheral nerve distribution, and the functions of major muscle groups and
their innervation in order to perform clinical procedures such as a basic neurological
examination of the lower limb and intramuscular injections. They should be aware of the
organisation of the deep fascia of the lower limb and its clinical relevance to compartment
syndromes.
FM1010 Anatomy Learning Objectives KA Quane 6
Areas of the Lower Limb
• Describe the boundaries and contents of the femoral triangle with particular regard to
arterial blood sampling and catheter placement.
• Describe the relationship between the femoral canal and the inguinal ligament and the
anatomy of femoral hernias.
• Describe the boundaries and contents of the popliteal fossa.
Bones of Lower Limb.
• Describe the osteology and surface landmarks of the pelvis, femur, tibia, fibula and foot.
Demonstrate their palpable and imaging landmarks. Explain how the bones, joints and related
structures are vulnerable to damage and what the consequences of such damage could be.
Joints and Muscles of Lower Limb.
• Describe the fascial compartments enclosing the major muscle groups and explain the
functional importance of these compartments and their contents in relation to compartment
syndrome.
• Describe the anatomy and movements of the hip joint. Summarise the muscles responsible
for these movements, their innervation and attachments.
• Describe the structures responsible for stability of the hip joint.
• Describe the structures at risk from a fracture of the femoral neck or dislocation of the hip
and explain the functional consequences of these injuries.
• Describe the anatomy and movements of the knee joint. Summarise the muscles responsible
for these movements, their innervation and main attachments.
• Describe the close relations of the knee joint, including major bursae and explain which of
these structures may be injured by trauma.
• Identify the factors responsible for maintaining the stability of the knee joint. Describe the
locking mechanism that occurs in full extension. Explain the anatomical basis of tests that
assess the integrity of the cruciate ligaments.
• Describe the anatomy of the ankle and subtalar joints. Explain the movements of plantar
flexion, dorsiflexion, inversion and eversion. Summarise the muscles responsible for these
movements, their innervation and their attachments.
• Describe the factors responsible for stability of the ankle joint, especially the lateral
ligaments, and explain the anatomical basis of ‘sprain’ injuries.
• Describe the arches of the foot and the bony, ligamentous and muscular factors that
maintain them.
FM1010 Anatomy Learning Objectives KA Quane 7
Blood Vessels and lymphatics of Lower Limb.
• Demonstrate the origin, course and branches of the major arteries that supply the gluteal
region, hip, thigh, leg, ankle and foot. Explain the functional significance of anastomoses
between branches of these arteries at the hip and knee.
• Demonstrate the locations at which the femoral, popliteal, posterior tibial and dorsalis pedis
arterial pulses can be palpated.
• Demonstrate the course of the principal veins of the lower limb. Explain the role of the
perforator veins between the superficial and deep veins and the function of the ‘muscle
pump’ for venous return to the heart. Describe the surface landmarks for sites of venous
access that can be used for ‘cutdown’ procedures in emergencies.
• Describe the lymphatic drainage of the lower limb and its relationship to infection and
tumour spread.
Nerves of Lower Limb.
• Outline the origin of the lumbosacral plexus and the formation of its major branches.
• Describe the origin, course and function of the femoral, obturator, sciatic, tibial, common
fibular (peroneal), sural and saphenous nerves and summarise the muscles and muscle groups
that each supplies, as well as their sensory distribution.
• Describe the anatomy of the gluteal region and the course of the sciatic nerve through it.
Explain how to avoid damage to the sciatic nerve when giving intramuscular injections.
• Describe the anatomical bases (nerve root or peripheral nerve) for loss of movements and
reflexes at the knee and ankle resulting from spinal injuries, disc lesions and common
peripheral nerve injuries.
• Describe the dermatomes of the lower limb and perineum that can be used to assess spinal
injuries.
• Describe the peripheral nerve distribution of the lower limb.
Lower Limb Prosections.
• Identify anatomical features on prosections of the lower limb.
FM1010 HISTOLOGY:
Biomolecules, cells, cell membranes
Cytoplasmic organelles
Connective tissue
Muscle
Nerve
Surface epithelium
Skin
FM1010 Anatomy Learning Objectives KA Quane 8
Online Histology (Blue Histology):
Please see ‘Guidelines for Online Histology’ available on ‘Blackboard / FM1010 / Course
Information / Anatomy Folder / Instructions for Histology Online (Blue Histology and
Assignments).’
Online Assignments:
Available on Blackboard / FM1010 / Assignments / Anatomy Pre-Practical Assignments /
relevant practical.
Histology of Biomolecules, cells, cell membranes
• Define the term microscopy and briefly outline how a tissue is prepared for microscopy.
• Define a cell and its major regions.
• Describe the histological structure of a plasma membrane
• Recognise the histological appearance of a plasma membrane.
• Explain how molecules move across the plasma membrane
Histology of Cytoplasmic Organelles
• Outline the structure and function of the nuclear envelope, chromatin and the nucleolus.
• Describe the cytosol.
• Describe the structure and function of endoplasmic reticulum and ribosomes.
• Describe how the Golgi apparatus relates to the rough endoplasmic reticulum.
• Describe the structure and function of lysosomes.
• Outline the structure of mitochondria.
• Outline the structure of the cytoskeleton.
• Recognise the histological appearance of cell organelles.
Histology of Muscle
• Compare and contrast skeletal, cardiac and smooth muscle tissue.
• Describe the microscopic structure of a skeletal muscle fibre/cell.
• Describe the arrangement of the contractile filaments into sacromeres and myofibrils.
• Recognise the histological appearance of skeletal, cardiac and smooth muscle.
Histology of Nerve
• Outline the classification of neurons.
• Describe the structure of neurons.
• Describe the structure of a synapse.
• Describe the functions of the support cells in the CNS and PNS.
• Outline the structural organisation of a typical peripheral nerve.
• Outline the process of myelination in the CNS and PNS.
• Recognise the histological appearance of nerve tissue.
Histology of Connective Tissue
• Describe the classification of connective tissue.
• Outline the cells found in general connective tissue and describe their functions.
• Describe the role of fibres and ground substance in connective tissue.
• Recognise the histological appearance of the different types of connective tissue.
FM1010 Anatomy Learning Objectives KA Quane 9
Histology of Surface Epithelium
• Outline the classification of epithelial tissue.
• Recognise the microscopic appearance of the various types of surface epithelia.
• Describe the ultrastructural features of their apical, lateral and basal surfaces.
• Describe the structure, general location and functional significance of the different types of
surface epithelia.
Histology of Skin
• Recognise the microscopic appearance of the types of skin.
• Outline the cells found in skin and describe their functions.
• Describe the layers found in skin.
• Describe the features of derivatives of the epidermis (Hair, Nails, Glands)
FM1010 RADIOLOGICAL ANATOMY
Interpret standard diagnostic images, e.g. CT, MRI, X-ray and ultrasound of the upper limb
and lower limb, and recognise common abnormalities (lectures and tutorials given by Dept
of Radiology).
FM1010 EMBRYOLOGY
• Describe the key anatomical differences between a neonate, child and adult.
Further learning objectives for embryology will be given at each lecture.
FM1010 Anatomy Learning Objectives KA Quane 10
S-ar putea să vă placă și
- Aplikasi Penggunaan Micro CTDocument7 paginiAplikasi Penggunaan Micro CTZannuraini AZÎncă nu există evaluări
- Medicinal Chemistry—III: Main Lectures Presented at the Third International Symposium on Medicinal ChemistryDe la EverandMedicinal Chemistry—III: Main Lectures Presented at the Third International Symposium on Medicinal ChemistryP. PratesiÎncă nu există evaluări
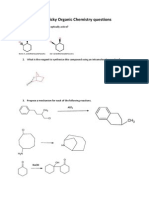
- Real Tricky Organic Chemistry QuestionsDocument3 paginiReal Tricky Organic Chemistry QuestionsABC67% (3)
- Anatomy & Physiology - Nervous SystemDocument5 paginiAnatomy & Physiology - Nervous SystemChristine Marylou PalomoÎncă nu există evaluări
- 2 ThoraxDocument7 pagini2 Thoraxapi-3757921Încă nu există evaluări
- BIO 201 Upper Limbs Muscles of The Upper Limbs Brachial PlexusDocument5 paginiBIO 201 Upper Limbs Muscles of The Upper Limbs Brachial PlexusKelly TrainorÎncă nu există evaluări
- Gross Anatomy of Posterior Compartment of The ThighDocument20 paginiGross Anatomy of Posterior Compartment of The ThighOnah ArinzeÎncă nu există evaluări
- Histology Notes 2Document13 paginiHistology Notes 2Lukas BüchlerÎncă nu există evaluări
- The Midbrain and Important ConnectionsDocument118 paginiThe Midbrain and Important ConnectionsBaguma MichaelÎncă nu există evaluări
- Biochemistry FinalsDocument11 paginiBiochemistry FinalsKc CalderonÎncă nu există evaluări
- Anatomy Part 1 - The Upper LimbDocument27 paginiAnatomy Part 1 - The Upper LimbSolange AcostaÎncă nu există evaluări
- Anatomy: 1. Atlas of Human Anatomy (Netter)Document5 paginiAnatomy: 1. Atlas of Human Anatomy (Netter)Migs MedinaÎncă nu există evaluări
- Hip Joint: Important PointsDocument4 paginiHip Joint: Important PointsNamrah AfzalÎncă nu există evaluări
- PONS: NeuroanatomyDocument20 paginiPONS: NeuroanatomyHassan IlyasÎncă nu există evaluări
- PhysiologyDocument31 paginiPhysiologyraza20100% (1)
- Collateral Ligament Injuries - OrthoInfo - AAOSDocument4 paginiCollateral Ligament Injuries - OrthoInfo - AAOSgermanda yepezÎncă nu există evaluări
- Axillary Artery: Branches First (1 Branch) Second Part (2 Branches) Third (3 Branches) 1 2 4Document14 paginiAxillary Artery: Branches First (1 Branch) Second Part (2 Branches) Third (3 Branches) 1 2 4foster18Încă nu există evaluări
- Peritoneal Anatomy Lecture NotesDocument4 paginiPeritoneal Anatomy Lecture Noteschc300Încă nu există evaluări
- Grip Strength and ElectromyogramDocument8 paginiGrip Strength and ElectromyogramChandra Murali100% (1)
- Ch. 9 Student Packet (ANP 1)Document7 paginiCh. 9 Student Packet (ANP 1)Alex Zhang100% (1)
- Anatomy Forum AbdDoneDocument7 paginiAnatomy Forum AbdDoneMedShare100% (1)
- Sama Notes Upper LimbDocument15 paginiSama Notes Upper LimbMaiUyen Kieu50% (2)
- Chapter 6 Anatomy and PhysiologyDocument4 paginiChapter 6 Anatomy and PhysiologyDiah Mariano0% (1)
- Cranial Nerves DiagramDocument15 paginiCranial Nerves DiagramSpellkingÎncă nu există evaluări
- Types of Knee InjuriesDocument6 paginiTypes of Knee InjuriesSagarÎncă nu există evaluări
- Upper Limb Exercise - LamuDocument2 paginiUpper Limb Exercise - LamuLem A SharÎncă nu există evaluări
- CatPhan 504 ManualDocument32 paginiCatPhan 504 ManualKevin RisoloÎncă nu există evaluări
- AnatomyDocument45 paginiAnatomyrkoppikarÎncă nu există evaluări
- Surface Anatomy Lower Limb PDFDocument10 paginiSurface Anatomy Lower Limb PDFArunprasath SivaramanÎncă nu există evaluări
- Electromyography I PDFDocument13 paginiElectromyography I PDFkeithtrahÎncă nu există evaluări
- Anatomy ExamDocument9 paginiAnatomy ExamFoo FuuÎncă nu există evaluări
- Vertebral Arteries, and Their Divisions. Arteries Fuse To Form The Basilar ArteryDocument6 paginiVertebral Arteries, and Their Divisions. Arteries Fuse To Form The Basilar Arterymurali_bharadwazÎncă nu există evaluări
- Functions of The Musculoskeletal SystemDocument9 paginiFunctions of The Musculoskeletal SystemLinda XueÎncă nu există evaluări
- Lower Limb Lab SheetDocument3 paginiLower Limb Lab SheetKelly TrainorÎncă nu există evaluări
- Gluteal Region, Posterior Compartment of The Thigh and Popliteal FossaDocument4 paginiGluteal Region, Posterior Compartment of The Thigh and Popliteal FossaSteph SantosÎncă nu există evaluări
- Anterior Compartment of Arm & Cubital FossaDocument24 paginiAnterior Compartment of Arm & Cubital FossaSky StoneÎncă nu există evaluări
- Histology Worksheets All in OneDocument15 paginiHistology Worksheets All in OneGabriel ParasÎncă nu există evaluări
- The Axilla: Norah AlmudawiDocument14 paginiThe Axilla: Norah AlmudawiF-med440 imamÎncă nu există evaluări
- Of These Parts of The Body. Example: What Structure Is Above The Eye?)Document4 paginiOf These Parts of The Body. Example: What Structure Is Above The Eye?)Anonymous QexowtfÎncă nu există evaluări
- Acute Inflammation (Vascular Changes) - 1Document33 paginiAcute Inflammation (Vascular Changes) - 1Ramesh KumarÎncă nu există evaluări
- AnaPhy Lesson 6 Muscular SYstemDocument7 paginiAnaPhy Lesson 6 Muscular SYstemLM KishimotoÎncă nu există evaluări
- 2-Physiotherapy For FracturesDocument17 pagini2-Physiotherapy For FracturesJuanitoCabatañaLimIIIÎncă nu există evaluări
- 2016 ANAT2241 Course Manual FinalDocument66 pagini2016 ANAT2241 Course Manual FinalDijattx100% (1)
- Bones of Upper and Lower Limbs - RevisionDocument15 paginiBones of Upper and Lower Limbs - RevisionChess Nuts100% (1)
- Blue Boxes SummaryDocument16 paginiBlue Boxes Summaryridin007Încă nu există evaluări
- Introduction To Radiology: As Clinical AnatomyDocument30 paginiIntroduction To Radiology: As Clinical AnatomyrizsamaruÎncă nu există evaluări
- Ecg Lab Bio350Document13 paginiEcg Lab Bio350Robin Lewis CooperÎncă nu există evaluări
- Mptregulations 2010Document81 paginiMptregulations 2010jayababuÎncă nu există evaluări
- Ecg PrimerDocument38 paginiEcg Primerdrimran570Încă nu există evaluări
- Notes About BiologyDocument81 paginiNotes About BiologyRichard Coffey100% (1)
- Bsci201 Anatomy Class NotesDocument101 paginiBsci201 Anatomy Class NotesSahel UddinÎncă nu există evaluări
- Ankle Joints and LigamentsDocument8 paginiAnkle Joints and LigamentskristinaÎncă nu există evaluări
- St. Luke's College of Medicine - William H. Quasha Memorial: AnatomyDocument4 paginiSt. Luke's College of Medicine - William H. Quasha Memorial: AnatomyMavic VillanuevaÎncă nu există evaluări
- Copy1 TOPANAT EXAM MCQ Nee RevisedDocument125 paginiCopy1 TOPANAT EXAM MCQ Nee Revisedkapil pancholiÎncă nu există evaluări
- HBTRC Neuroanatomy 2014.1 PDFDocument135 paginiHBTRC Neuroanatomy 2014.1 PDFFirah Triple'sÎncă nu există evaluări
- Human Anatomy PhysiologyDocument3 paginiHuman Anatomy PhysiologyHammad AliÎncă nu există evaluări
- 4 EcDocument13 pagini4 EcayushmanaÎncă nu există evaluări
- 1ST YEAR MBBS HAMDARD MSK MD StudyguideDocument24 pagini1ST YEAR MBBS HAMDARD MSK MD StudyguideRania AijazÎncă nu există evaluări
- mbbs1 PDFDocument16 paginimbbs1 PDFSayed Izhar Ullah sÎncă nu există evaluări
- Jill Miller Fascia PDF PDFDocument5 paginiJill Miller Fascia PDF PDFMaria Kiekari100% (1)
- MnemonicDocument33 paginiMnemonicyanot0206Încă nu există evaluări
- Conduction System of The Heart PPT 2Document12 paginiConduction System of The Heart PPT 2intern shipÎncă nu există evaluări
- Gen Bio 2 - Chapter 1Document79 paginiGen Bio 2 - Chapter 1Samantha AcostaÎncă nu există evaluări
- Glossary of Radiology Signs by SystemsDocument2 paginiGlossary of Radiology Signs by SystemsIssa OliverÎncă nu există evaluări
- Trendelenburg PositionDocument2 paginiTrendelenburg PositionCudith LofinciÎncă nu există evaluări
- Low Back Pain SlidesDocument27 paginiLow Back Pain SlidesAviv Aziz Triono100% (1)
- Mcq. of Bone TissueDocument7 paginiMcq. of Bone TissueRishu SinghÎncă nu există evaluări
- HydralazineDocument2 paginiHydralazineShermayne Mallapre HernandezÎncă nu există evaluări
- Introduction To Chiral or Optical IsomersDocument3 paginiIntroduction To Chiral or Optical IsomersSeepana Dayakar100% (1)
- A Uri Culo TherapyDocument322 paginiA Uri Culo Therapyserafim67100% (1)
- Digestive SystemDocument30 paginiDigestive SystemImneil Jeanne Melendres-PerezÎncă nu există evaluări
- Newborn Case StudyDocument9 paginiNewborn Case Studyitsmeaya75% (4)
- Jim Nursing Essay - Chronic Obstructive Pulmonary Disease (COPD) .Document8 paginiJim Nursing Essay - Chronic Obstructive Pulmonary Disease (COPD) .SarahJaneÎncă nu există evaluări
- 1P 2 OB1-Maternal-AnatomyDocument11 pagini1P 2 OB1-Maternal-AnatomyGeevee Naganag VentulaÎncă nu există evaluări
- Bio Abhyasa Deepika PDFDocument93 paginiBio Abhyasa Deepika PDFArogya Raju Pudhota82% (17)
- BASF Chemical Emergency Medical Guidelines - H2SDocument5 paginiBASF Chemical Emergency Medical Guidelines - H2SemilidiverÎncă nu există evaluări
- Adult History and Physical Examination Well Patient Encounter (A Checklist For Medical Students)Document13 paginiAdult History and Physical Examination Well Patient Encounter (A Checklist For Medical Students)Michael Harrison Chopade100% (1)
- Kuliah Sistem UrogenitalDocument25 paginiKuliah Sistem UrogenitalTiradewi BustamiÎncă nu există evaluări
- Nursing Care of A Family Experiencing A Sudden Pregnancy ComplicationDocument5 paginiNursing Care of A Family Experiencing A Sudden Pregnancy ComplicationCrisheila Sarah PiedadÎncă nu există evaluări
- USNI Medication TestDocument8 paginiUSNI Medication Testusni100% (31)
- Blood Transfusion Therapy DefinitionDocument27 paginiBlood Transfusion Therapy DefinitionEvangelin MelvinÎncă nu există evaluări
- AKI Guideline KDIGODocument141 paginiAKI Guideline KDIGOSarah RepinÎncă nu există evaluări
- Computational Models For The Human Body PDFDocument679 paginiComputational Models For The Human Body PDFGuilherme AyresÎncă nu există evaluări
- NICABM Anger Infographic PrintFriendlyDocument3 paginiNICABM Anger Infographic PrintFriendlyShivaprasad PrabhuÎncă nu există evaluări
- Blood ClottingDocument3 paginiBlood Clottingridwan100% (9)
- Toyota 1GR-FE Engine ControlDocument18 paginiToyota 1GR-FE Engine ControlMaster Xeoto89% (9)
- Clinical Laboratory Hematology 3rd Edition Mckenzie Test BankDocument35 paginiClinical Laboratory Hematology 3rd Edition Mckenzie Test Bankgeincupola.06zi100% (28)
- Internal Root Resorption - A ReviewDocument15 paginiInternal Root Resorption - A Reviewjaime097830690% (1)
- Biol 1010 Exam 2 ReviewDocument3 paginiBiol 1010 Exam 2 Reviewapi-302931792Încă nu există evaluări
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDDe la EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDEvaluare: 5 din 5 stele5/5 (3)
- The Age of Magical Overthinking: Notes on Modern IrrationalityDe la EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityEvaluare: 4 din 5 stele4/5 (30)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeDe la EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeEvaluare: 2 din 5 stele2/5 (1)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)De la EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Evaluare: 3 din 5 stele3/5 (1)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionDe la EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionEvaluare: 4 din 5 stele4/5 (404)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsDe la EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsEvaluare: 4 din 5 stele4/5 (4)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisDe la EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisEvaluare: 4.5 din 5 stele4.5/5 (42)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsDe la EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsEvaluare: 5 din 5 stele5/5 (1)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsDe la EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsÎncă nu există evaluări
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedDe la EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedEvaluare: 5 din 5 stele5/5 (81)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsDe la EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsEvaluare: 4.5 din 5 stele4.5/5 (170)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaDe la EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaEvaluare: 4.5 din 5 stele4.5/5 (266)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.De la EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Evaluare: 4.5 din 5 stele4.5/5 (110)
- Why We Die: The New Science of Aging and the Quest for ImmortalityDe la EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityEvaluare: 4 din 5 stele4/5 (5)
- Summary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisDe la EverandSummary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisEvaluare: 5 din 5 stele5/5 (8)
- Empath: The Survival Guide For Highly Sensitive People: Protect Yourself From Narcissists & Toxic Relationships. Discover How to Stop Absorbing Other People's PainDe la EverandEmpath: The Survival Guide For Highly Sensitive People: Protect Yourself From Narcissists & Toxic Relationships. Discover How to Stop Absorbing Other People's PainEvaluare: 4 din 5 stele4/5 (95)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeDe la EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeEvaluare: 4.5 din 5 stele4.5/5 (253)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessDe la EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessEvaluare: 4.5 din 5 stele4.5/5 (328)
- Summary: Thinking, Fast and Slow: by Daniel Kahneman: Key Takeaways, Summary & Analysis IncludedDe la EverandSummary: Thinking, Fast and Slow: by Daniel Kahneman: Key Takeaways, Summary & Analysis IncludedEvaluare: 4 din 5 stele4/5 (61)
- The Obesity Code: Unlocking the Secrets of Weight LossDe la EverandThe Obesity Code: Unlocking the Secrets of Weight LossEvaluare: 4 din 5 stele4/5 (6)
- The Marshmallow Test: Mastering Self-ControlDe la EverandThe Marshmallow Test: Mastering Self-ControlEvaluare: 4.5 din 5 stele4.5/5 (59)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesDe la EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesEvaluare: 4.5 din 5 stele4.5/5 (1412)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryDe la EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryEvaluare: 4 din 5 stele4/5 (45)