Documente Academic
Documente Profesional
Documente Cultură
Atypical Deglutition
Încărcat de
katherineTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Atypical Deglutition
Încărcat de
katherineDrepturi de autor:
Formate disponibile
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/230840935
Atypical deglutition: Diagnosis and interceptive treatment. A clinical study
Article in European Journal of Paediatric Dentistry · September 2012
Source: PubMed
CITATIONS READS
7 1,317
4 authors, including:
Roberta Condo Micaela Costacurta
University of Rome Tor Vergata University of Rome Tor Vergata
41 PUBLICATIONS 197 CITATIONS 29 PUBLICATIONS 374 CITATIONS
SEE PROFILE SEE PROFILE
Cesare Perugia
University of Rome Tor Vergata
22 PUBLICATIONS 107 CITATIONS
SEE PROFILE
All content following this page was uploaded by Roberta Condo on 08 February 2017.
The user has requested enhancement of the downloaded file.
R. Condò, M. Costacurta, C. Perugia,
and in G2 by 0.76 m and an increase of overbite in G1
R. Docimo
by 3.14 mm and in G2 by 0.88 mm. The inclination of
University of Rome “Tor Vergata”, Rome, Italy
the maxillary and mandibular incisors improved, with
Department of Paediatric Dentistry
an inter-incisive angle of 123° in G1 and 124.2° in G2.
Head Prof. Raffaella Docimo
Conclusion The clinical results obtained suggest
that early intervention in atypical deglutition with
e-mail: roberta.condo@uniroma2.it
Habit CorrectorTM is able to produce significant results
in primary dentition and in the first phase of mixed
dentition, rather than in the late phase of mixed denti-
Atypical deglutition: tion.
diagnosis Keywords Atypical deglutition; Habit CorrectorTM;
and interceptive Paediatric patient.
treatment. A clinical
study Introduction
Clinically, atypical deglutition is classified in simple
or complex [Lescano de Ferrer, 2006]. The former
abstract is characterised by contraction of the lips, the chin
muscle and elevator jaw muscles, due to the presence
Aim The aim of this study was to evaluate the of an open bite that forces interposition of the tongue
early treatment of atypical deglutition, by analysing between the dental arches, with the purpose to ensure
the efficacy of the eruptive guide appliance Habit the anterior seal [Sayin, 2006]. The increase in overjet is
CorrectorTM. typical of these cases, due to the vestibular inclination
Materials and methods The pre- and post- of the upper incisors and sometimes lingual inclination
treatment (T1 and T2) cephalometric data of 2 of the lower incisors [Fellus, 2006]. The complex form is
groups of patients (G1 and G2), both consisting of characterised by contraction of labial and facial muscles
25 patients each and treated with Habit CorrectorTM, and of the chin muscle, but not of the elevator muscles
were compared. The first group included 10 males [Störmer, 1999]. In this case, stabilisation of the jaw is
and 15 females, aged between 4 and 7 years old, with guaranteed by the mimic muscles and deglutition takes
average age 6.17 years, and therefore undergoing the place with separate teeth since the tongue totally falls
last phase of primary dentition and the first phase of between the arches and not in a well defined area, as it
mixed dentition. The second group included 12 males occurs in the simple form [Polimeni, 1995].
and 13 females, aged between 8 and 12 years old, The existing relationship between atypical deglutition
with average age 9.19 years old, undergoing the and malocclusion, especially the open bite, is currently
second phase of mixed dentition. The overall duration one of the most debated subject [Maciel CT, 2004;
of the treatment was 12 months. Cristina Tostes Vieira Maciel, 2005].
Results The results showed significant differences The opinions and researches on this topic are fairly
between the two groups, with respect to overbite, conflicting, because some authors state that atypical
overjet, molar relation, inclination of the upper and deglutition causes the open bite, while others believe
lower incisors, position of the jaw. A significant that atypical swallowing is a consequence of it [Maciel,
variation between the two groups at T2 was registered 2005; Fraser, 2006]. In this regard, Proffit underscores
for the maxillomandibular relationships: the increase in that in patients with anterior open bite, as it often
the growth and degree of mandibular protrusion was occurs in children using pacifiers, it is very difficult to
of 4.66° in G1 and 2.44° in G2. Significant changes obtain closure of the mouth to prevent spilling of fluids
were registered for the position or growth of the during swallowing; the position of the tongue between
upper jaw; the upper facial height almost remained the arches and the contraction of the mimic muscles,
unaltered, with 53.34° for G1 and with 53.96° for G2. represent a physiological adaptation with the purpose
A significant variation occurred with the increase in the to restore the anterior seal. Almost every patient with
sagittal relationship between the molars, improved in anterior open bite is affected by this type of deglutition,
G1 by 3.14 mm and in G2 by 2.61 mm. A significant but the contrary is not necessarily true: indeed, the
decrease of overjet was registered in G1 by 1.94 mm tongue is often in anterior position during deglutition,
even in children with good occlusion. Therefore,
European Journal of Paediatric Dentistry vol. 13/2-2012 1
CONDÒ R. et al.
according to the author, the anterior position of the an incisor-to-incisor ratio, which is important to correct
tongue can be considered the result of an open bite the marked overjet and comes with a tight fissure
and not its cause [Proffit W, 2002]. Indeed, the pressure between upper and lower incisors, such to prevent any
exerted by the tongue during swallowing does not last type of vertical pressure of intrusive type during its use;
enough to modify the position of the teeth: its duration this pressure will be instead present in the molar area
is of about one second [Cozza P, 1992]. An average [Bergersen, 1988]. This helps the intrusion of posterior
individual swallows about 1000 times a day for a total teeth and the extrusion of the anterior ones, resulting
of about 1000 seconds of pressure and therefore, it is in the closure of the open bite, caused by the bad habit
certainly not enough to modify the muscular balance [Bergersen, 1988]. The tongue aspect is also different:
[Cozza, 1992]. The tongue, in addition to assuming an a horizontal membrane, located in the lower part of
anterior position during swallowing, keeps the same the device, extends by about 1 cm in anterior-posterio
posture also at rest, causing facial and dentomaxillary direction and its function is to prevent a low posture
changes [Cozza, 1992; Ierando, 1999; Cozza, 1999; of the tongue and therefore help myofunctional re-
Lescano de Ferrer, 2006]. education, together with two small spurs located in
the upper retro-incisive area, proper tongue position
Habit Corrector™ point [Bergersen, 1988]. Finally, two flaps that have a
Habit Corrector™ is a myofunctional removable double function are located in the lower retro-incisive
appliance, used in paediatric age to prevent and area: forward propulsion of the jaw and repositioning
intercept dental and skeletal malocclusions in primary of lower incisors in a vestibular sense in case of lingual
and mixed dentition [Bergersen, 1981]. inclination [Bergersen EO, 1988].
This appliance was conceived by Bergersen E.O. in The treatment with the Habit Corrector™ should be
1987 in order to prevent or correct the consequences started at about 4-5 years of age [Bergersen, 1988].
of an anomalous tongue thrust, to intercept the
occurrence and persistence of the open bite, which
is often clinically associated to atypical deglutition Materials and methods
[Bergersen, 1988]. It was also conceived to re-
educate and correct the majority of bad habits such as Two groups of patients were selected at the
sucking the finger or the pacifier, atypical deglutition, department of Paediatric Dentistry of Azienda
interposition of the tongue at rest and habitual Ospedaliera Policlinico Tor Vergata of Rome, during their
mouth breathing, often present in young patients and first paediatric dental visit: Group G1, composed of 25
responsible for a number of alterations of functional, patients aged between 4 and 7 years of age (10 males
dental and/or skeletal nature as the open bite, cross and 15 females), undergoing the last phase of primary
bite and excessive overjet [Bergersen, 1986]. dentition and first phase of mixed dentition, and Group
Habit Corrector™ is a preformed appliance, patented G2 (12 males and 13 females), also composed of 25
as “U-shaped device”, consisting of inert, extremely patients aged between 8 and 12 years, undergoing the
flexible plastic material which well adapts to the second phase of mixed dentition. The average age of
occlusal anatomy also in some severe cases of dental the sample was 6.37 years for G1 and 9.19 years for G2.
and skeletal malocclusions [Bergersen, 1988]. All patients of both groups showed atypical deglution
The resistance to wear and the remarkable elastic with anterior dentoalveolar open bite.
properties of the construction material, contribute to Inclusion criteria were the following: subject in
render this appliance extremely comfortable also for the last phase of primary dentition, first and second
young patients, in order to help its clinical use and phase of mixed dentition, atypical deglutition, anterior
render the interceptive therapy easy, quick and effective dentoalveolar open bite, dental, skeletal and dental-
[Bergersen, 1988]. skeletal malocclusion of Class I or II, crowding of the
The device is available in two versions. incisive region in the mandibular arch less than 2 mm,
› HC-C (close) or closed version, in the form of a sin- deciduous and permanent overbite less than 2.5 mm
gle block. and deciduous and permanent overjet greater than 2.5
› HC-O (open) or open version, indicated for habitu- mm and less than 7 mm.
al oral breathing patients, composed by two front Exclusion criteria: complete permanent dentition,
parts that are joined at the back [Bergersen, 1988]. agenesis of permanent teeth, actual or compensated
What makes the Habit Corrector™ stand out from Class III malocclusion, deep bite, crowding in the
other similar appliances is its internal morphology, incisive region in the mandibular arch greater than 7
which consists in both arches, of a higher lateral-rear mm, overjet greater than 7 mm, excessive inclination of
part compared to the front part, that contain inserts for upper incisors, facial hyperdivergence (from mandibular
the single teeth at the front and for the molar group at post-rotation), maxillary contraction of basal type and
the back [Bergersen, 1988]. TMJ disorder.
The construction bite, in sagittal terms, is based on The preliminary phase (T1) consisted for both roups
2 European Journal of Paediatric Dentistry vol. 13/2-2012
diagnosis and treatment of Atypical swallowing
in recording the clinical parameters in order to assess period of 12 months.
the presence of bad habits, such as atypical deglutition, With regards to the therapeutic protocol, the
oral breathing or finger and/or pacifier sucking. The following monthly clinical checkups, biannual checkups
radiographic documentation was collected, including and annual radiographic checkups were performed,
orthopantomogram of the dental arches and latero- including orthopantogram of the dental arches and
lateral teleradiography of the skull. The study plaster latero-lateral teleradiography of the skull.
models were recorded and photographs were taken: Patients with oral breathing were requested to
extra-oral documentation with photographs of the initially wear the open version of the HC-O appliance,
face in front view, front view with smile, lateral view, which was then substituted by the closed version HC-C,
lateral view with smile and nasolabial-chin and intra- when the patient was starting to show a good level of
oral profile with photographs in front, lateral, upper adaptation to the appliance (after about two months).
occlusion and lower occlusion view (Fig. 1). The dentoalveolar and skeletal changes between the
The second phase was performed in both groups two groups, at the beginning of the treatment (T1)
after the use of the Habit Corrector™. and at the end (T2), were evaluated by means of the
All patients of both groups were requested to wear Student’s t-test.
the device all night and 2 hours during the day for a The differences associated to a p-value <0.01 were
Fig. 1A-1c M.R. 7 years and
5 months: frontal facial view
(A), lateral view of the face (B)
Latero-lateral teleradiography
of the skull (C).
Fig. 1D Orthopantogram.
Fig. 1E-1G Intraoral
views: left side (E),
frontal (F), right side
(G).
Fig. 1h-1i Occlusal
views: maxillary arch
(H) and mandibular
arch (I).
European Journal of Paediatric Dentistry vol. 13/2-2012 3
CONDÒ R. et al.
taken into consideration as statistically significant of 53.96° in G2. A significant change occurred with the
in the analysis. The parameters of the skeletal and increase of the sagittal relation between molars, which
dental analysis were set in agreement with Ricketts’ improved in G1 by 3.14 mm and in G2 by 2.61 mm.
cephalometric analysis (Table 1). A significant decrease of overjet was registered in G1
by 1.94 mm and in G2 by 0.76 mm and an increase
of overbite in G1 by 3.14 mm and in G2 by 0.88 mm.
Results The inclination of the maxillary and mandibular incisors
improved, with an inter-incisive angle of 123° in G1 and
In the preliminary phase of the study (T1) groups G1 124.2° in G2 (Fig. 2).
and G2 did not show any significant difference between
males and females. Similar initial cephalometric values
of the skeletal and dental analyses were recorded for Discussion
both groups, except for molar relationship values and
inclination values of the incisors, which were negative Different studies showed that the changes associated
in greater number in G1. During the final phase of the to the growth of the paediatric patient are positively
treatment (T2), significant differences were registered influenced by eruptive guide appliance in mixed
between the two groups. Significant values were dentition [Bergersen, 1988; Methenitou, 1990;
found for overbite, overjet, molar relation, inclination of Keski-Nisula, 2008; Janson, 2000; Bergersen, 1966;
upper and lower incisors and jaw position. A significant Bergersen, 1984; Bergersen, 1985].
change among the two groups was registered in the In this study, the results show that the eruptive
maxillomandibular relationships: in particular the increase guidance appliance Habit Corrector™ proved to
in the mandibular growth and degree of mandibular be effective in correcting different aspects in the
protrusion was of 4.66° in G1 and 2.44° in G2. development of the occlusion, such as overjet, overbite,
No significant changes were recorded for the upper open bite and molar relationship.
maxillary growth; the upper facial height almost The changes induced by the eruptive guidance
remained unaltered with a value of 53.34° in G1 and device mainly involved the dentoalveolar region. In
GROUP, TREATMENT TIME G1 T1 G2 T1 G1 T2 G2 T2
AGE (Y,M) 6.37 9.19 6.37 7.4
SKELETAL ANALYSIS
Angle of facial axis (°) 90.08 89.16 89.92 90.08
Profile convexity (mm) 6.68 4.04 5.92 6.68
Maxillary depth angle (°) 90.72 91.16 90.48 90.72
Facial depth angle (°) 83.3 86.72 84.4 83.2
Angle of the position of the mandibular branch (°) 69.96 72.44 74.62 74.88
Position of porion (mm) 43.72 42.2 42.4 43.72
Angle of lower facial height (°) 46.96 47.68 47 46.96
Angle of the upper facial height (°) 53.56 53.28 53.34 53.96
Angle of mandibular plane (°) 24.72 26.08 25.52 24.72
Angle of mandibular arch (°) 32.84 28.36 31.52 32.84
Posterior facial height (mm) 54.24 56.08 53.68 54.24
Mandibular body lenght (mm) 58.36 66.4 63.02 68.84
DENTAL ANALYSIS
Occlusal plane inclination (°) 19.24 21.4 21.78 19.24
interincisal Angle (°) 114.96 125.56 123 124.2
Angle between lower incisor axis and plane A-PO (°) 27.4 23.44 26.44 27.4
Angle between upper incisor axis and plane A-PO (°) 35 31.12 28.5 35
Position of lower incisive than the plane A-PO (mm) 3.26 3.96 1.86 3.26
Position of upper incisive than the plane A-PO (mm) 5.7 4.7 3 5.7 tabLE 1 Average of
Molar relationship (mm) 2.1 0.79 -1.04 2.1 cephalometric values of G1
Overjet (mm) 4.04 2.96 2.1 2.2 and G2 at the beginning
Overbite (mm) -2.12 0.78 1.02 1.66
T1 and at the end T2 of
treatment.
4 European Journal of Paediatric Dentistry vol. 13/2-2012
diagnosis and treatment of Atypical swallowing
any case, the treatment with Habit Corrector™ seems in overjet, the increase in overbite and the mandibular
to significantly improve the mandibular growth from a growth, are significantly obvious during the last phase
skeletal point of view, as shown by the measurement of primary dentition and the first phase of mixed
of the position angle of the mandibular area, improved dentition, rather than during the late phase of mixed
from T1 to T2 of 4.66° in G1 e 2.44° in G2. dentition. This proves that the favourable changes
At the end of the treatment, the patient showed induced by the Habit Corrector™ on the skeletal and
absence of crowding, Class I dental relationship and dentoalveolar components is greater during the early
harmony in the skull-facial growth. After treatment growth phase.
with Habit Corrector™, there was no need for a In addition, differently from previous studies that did
second treatment phase, but only the development of not show particular changes in the inclination of the
the occlusion was followed, until the end of the phase. incisors, this study shows that the more satisfactory
These results underscore to what extent the eruptive results obtained, particularly in patients of group G1,
guide appliance Habit Corrector™ mainly affects are related to promptness of intervention. Indeed the
these parameters during the last phase of dentition treatment of these subjects started during the pre-
and the first phase of mixed dentition, rather than the eruptive phase of the permanent incisors, therefore in
second phase of mixed dentition. These changes in the the last phase of primary dentition and the first phase
occlusion towards a Class I relationship, the decrease of mixed dentition.
Fig. 2A-2c M.R. 8.5 months:
frontal facial view (A), lateral
view of the face (B), latero-
lateral teleradiography of the
skull (C).
Fig. 2D Orthopantogram.
Fig. 2E-2G Intraoral
views: left side (E),
frontal (F), right side
(G).
Fig. 2h-2i Occlusal
views: maxillary arch
(H) and mandibular
arch (I).
European Journal of Paediatric Dentistry vol. 13/2-2012 5
CONDÒ R. et al.
works, how to use it. Funct Orthod. 1984 Sep-Oct;1(3):28-9, 31-5
Conclusion › Bergersen, EO, The Preformed Orthodontic Positioner and Eruption Guidance
Appliance, Northwestern Univ., Chicago, IL, 1981.
The deglutition reflex is fairly unpredictable with › Bertoldi PM, Felfício CM, Matsumoto MA. Effect of the early intervention
regards to maturation times. This creates many of oral habits on the development of dental occlusion. Pro Fono. 2005 Jan-
Apr;17(1):37-44.
difficulties in trying to identify the line between › Cozza P, Mascolo F, Palatella A. Riabilitazione miofunzionale. Esercizi e
physiological and pathological function and therefore schemi pratici. Dental Cadmos 1999, 4: 47-60.
in planning a suitable treatment able to correct its › Cozza P., Fidato R., Germani C., Santoro F., Siciliani G.: La deglutizione
atipica. Mondo ortod. 2: 141-59, 1992.
causes and ensure a normal growth of the maxillofacial › Cristina Tostes Vieira Maciel et al, Etiological aspects of anterior open bite
region. Therefore, all those cases at risk affected by and its implications to the oral functions. Pro-Fono Revista de Atualizicao
child deglutition should be monitored even after Cientifica, 2005 Apr-Dec;17(3):293-302.
eruption of all deciduous teeth, intervening in the first › Fellus P. Tongue disfunction and abnormal development. Orthod Fr. 2006
Mar;77(1):105-12.
teething phase, to avoid the consolidated acquisition of › Fraser C. Tongue thrust and its influence in orthodontics. Int J Orthod
this bad habit. A re-educational therapy in this phase Milwaukee. 2006 Spring;17(1):9-18.
will ensure the normal growth of maxillary bones. › Gottlieb EL, Brazones MM, Malerman AJ, Moskowitz EM, Phipps GS, Sarver
DM. Early orthodontic treatment, part 2. J Clin Orthod. 2004 Mar;38(3):135-
The early treatment during the last phase of primary
54.
dentition and the first phase of mixed dentition by › Ierardo G, Manzon L, Ottolenghi L, Polimeri A. Aspetti clinici e terapeutici
means of an orthodontic-paedodontic eruptive guide della deglutizione atipica. Dental Cadmos 1999,17: 55-83.
appliance, and in particular with Habit Corrector™, › Janson G, Nakamura A, Chiqueto K, Castro R, de Freitas MR, Henriques
JF, Treatment stability with the eruption guidance appliance. Am J Orthod
can be considered a valid means able to restore the Dentofac Orthop 2007, 131(6):717-28.
physiological occlusion and growth [Keski-Nisula, › Janson GR, da Silva CC, Bergersen EO, Henriques JF, Pinzan A, Eruption
2008; Janson, 2007; Bergersen, 1995; Gottlieb, 2004; Guidance Appliance effects in the treatment of Class II, Division 1
Tausche, 2004; Saldarriaga, 2007]. malocclusions. Am J Orthod Dentofac Orthop 2000,117(2):119-29.
› Keski-Nisula K, Hernesniemi R, Heiskanen M, Keski-Nisula L, Varrela
The clinical results obtained suggest that early J, Orthodontic intervention in the early mixed dentition: a prospective,
intervention in atypical deglutition with Habit controlled study on the effects of the eruption guidance appliance. Am J
Corrector™ is able to produce significant results; Orthod Dentofac 2008 133(2):254-60.
› Keski-Nisula K, Keski-Nisula L, Salo H, Voipio K, Varrela J, Dentofacial
this device is deemed valid in order to intercept changes after orthodontic intervention with eruption guidance appliance in
malocclusions (atypical swallowing, open bite). the early mixed dentition. Angle Orthod 2008, 78(2):324-331.
This study represents the first part of clinical › Keski-Nisula K. et al, Occurrence of malocclusion and need of orthodontic
observations that need to be followed-up to evaluate the treatment in early mixed dentition, American Journal of Orthodontic and
Dentofacial Orthopedics, 2003 Dec;124(6):631-8.
possible stabilisation of the result. Indeed, this is a new › Kluemper C. Beemen. E. Hicks, Early Orthodontic Treatment: What Are The
method that is not currently extensively documented in Imperatives?. Clinical Practice, 2000 May;131(5):613-20.
the literature, and therefore it can help the paediatric › Lescano de Ferrer A, Varela de Villalba TB, Effect of the suction-swallowing
dentist to early intercept these malocclusions. action on orofacial development and growth. Rev Fac Cien Med Univ Nac
Cordoba, 2006;63(2 Suppl):33-7.
› Maciel CT, Leite IC. Etiological aspects of anterior open bite and its
implications to the oral functions. Pro Fono. 2005 Apr-Dec;17(3):293-302.
References › Methenitou S, Shein B, Ramanathan G, Bergersen EO, Prevention of
overbite and overjet development in the 3 to 8 year old by controlled
nighttime guidance of incisal eruption: a study of 43 individuals. J Pedod
› American Academy of Pediatric Dentistry. Clinical guideline on management 1990,14(4):219-30.
of the developing dentition in pediatric dentistry. Pediatr Dent. 2004;26(7 › Musich D, Busch MJ. Early orthodontic treatment: current clinical
Suppl):128-31). perspectives. Alpha Omegan, 2007;100(1):17-24.
› Bergersen EO, Orthodontic appliance to correct open-bite tendencies in › Polimeni A., Ottolenghi L., Ierardo G., Manzon L.: Aspetti clinici e terapeutici
children and adults and tongue-thrust in young children. PATENT ID US della deglutizione atipica. Dent. Cadmos 17: 55-78, 15 Nov 1995.
4784605; November 15, 1988. › Proffit W, Ortodonzia contemporanea. 3Ed ; 2002.
› Bergersen EO, Preventive and interceptive orthodontics in the mixed › Saldarriaga JR. Protocol for the treatment of anterior open bite patients: an
dentition with the myofunctional eruption guidance appliance: correction of evaluation. World J Orthod. 2007 Fall;8(3):285-99.
overbite and overjet. J Pedod 1988, 12(3):386-414. › Sayin MO, Akin E, Karaçay S, Bulakbaşi N, Initial effects of the tongue crib on
› Bergersen EO, Preventive eruption guidance in the 5 to 7 year old. J Clinic tongue movements during deglutition: a Cine-Magnetic resonance imaging
Orthod 1995, 29:382-395. study. Angle Orthod. 2006 May;76(3):400-5. Erratum in: Angle Orthod.
› Bergersen EO. A longitudinal study of anterior vertical overbite from eight to 2006 Jul;76(4):125-129.
twenty years of age. Angle Orthod. 1988 Jul;58(3):237-56. › Störmer K, Pancherz H, Electromyography of the perioral and masticatory
› Bergersen EO. The directions of facial growth from infancy to adulthood. muscles in orthodontic patients with atypical swallowing. J Orofac Orthop,
Angle Orthod. 1966 Jan;36(1):18-43. 1999;60(1):13-23.
› Bergersen EO. The eruption guidance myofunctional appliance in the › Tausche E, Luck O, Harzer W. Prevalence of malocclusions in the early
consecutive treatment of malocclusion. Gen Dent. 1986 Jan-Feb;34(1):24-9. mixed dentition and orthodontic treatment need. Eur J Orthod. 2004
› Bergersen EO. The eruption guidance myofunctional appliance: case Jun;26(3):237-44.
selection, timing, motivation, indications and contraindications in its use. › Wong ML, Che Fatimah Awang, Ng LK, Norlian D, Rashidah Dato
Funct Orthod. 1985 Jan-Feb;2(1):17-21, 24-5, 28-33. Burhanudin, Gere MJ. Role of interceptive orthodontics in early mixed
› Bergersen EO. The eruption guidance myofunctional appliances: how it dentition. Singapore Dent J. 2004 Dec;26(1):10-4.
6 European Journal of Paediatric Dentistry vol. 13/2-2012
View publication stats
S-ar putea să vă placă și
- Facial Growth in Man Studied with Metallic ImplantsDocument26 paginiFacial Growth in Man Studied with Metallic Implantstoffe lopezÎncă nu există evaluări
- IMPLANT OCCLUSION GUIDEDocument57 paginiIMPLANT OCCLUSION GUIDEElango2548994% (16)
- Wjo 2 3 Kim1 PDFDocument11 paginiWjo 2 3 Kim1 PDFGoutam NookalaÎncă nu există evaluări
- Smith & Burstone-Mechanic Tooth MovementDocument14 paginiSmith & Burstone-Mechanic Tooth MovementGisselaMaldonadoÎncă nu există evaluări
- Uprighting MolarsDocument7 paginiUprighting MolarsMa Lyn Gabayeron100% (1)
- Ricketts 1982Document20 paginiRicketts 1982JonasMarçalo100% (1)
- Andrews 1972 The Six Keys To Normal OcclusionDocument15 paginiAndrews 1972 The Six Keys To Normal OcclusionMiguelÎncă nu există evaluări
- Andrews 1972 The Six Keys To Normal OcclusionDocument15 paginiAndrews 1972 The Six Keys To Normal OcclusionMiguelÎncă nu există evaluări
- Andrews 1972 The Six Keys To Normal OcclusionDocument15 paginiAndrews 1972 The Six Keys To Normal OcclusionMiguelÎncă nu există evaluări
- Andrews 1972 The Six Keys To Normal OcclusionDocument15 paginiAndrews 1972 The Six Keys To Normal OcclusionMiguelÎncă nu există evaluări
- Facial Danger Zones - Avoiding Nerve Injury in Facial Plastic SurgeryDocument63 paginiFacial Danger Zones - Avoiding Nerve Injury in Facial Plastic Surgeryramarchiori100% (1)
- The Aging EyeDocument53 paginiThe Aging EyeSenthil Kumar50% (2)
- Soft Tissue Cephalometric AnalysisDocument144 paginiSoft Tissue Cephalometric Analysisaparna mohananithaÎncă nu există evaluări
- Combination in Deep-Bite Cases: The Equiplan-Quad HelixDocument3 paginiCombination in Deep-Bite Cases: The Equiplan-Quad HelixrohitÎncă nu există evaluări
- Multiloop PDFDocument10 paginiMultiloop PDFAstrid Carolina HerreraÎncă nu există evaluări
- Ao Catalog ProTorqueDocument2 paginiAo Catalog ProTorqueMuruganandam EswaranÎncă nu există evaluări
- Ricketts Cephalometric Syntesis PDFDocument27 paginiRicketts Cephalometric Syntesis PDFAleeJanyArroÎncă nu există evaluări
- Spradley1981 PDFDocument10 paginiSpradley1981 PDFFernando Ruiz BorsiniÎncă nu există evaluări
- Sequential Piezocision A Novel Approach To Acelerated Orthodontic TreatmentDocument11 paginiSequential Piezocision A Novel Approach To Acelerated Orthodontic TreatmentMargareth BritoÎncă nu există evaluări
- Torque in Orthodontics ReviewDocument3 paginiTorque in Orthodontics ReviewchaitreeÎncă nu există evaluări
- Manual Bio Art 4000sDocument22 paginiManual Bio Art 4000sArchitÎncă nu există evaluări
- Ortodoncia Brackets inDocument17 paginiOrtodoncia Brackets injavierÎncă nu există evaluări
- Evaluation of Corticotomy - Facilitated Orthodontics and Piezocision in Rapid Canine RetractionDocument8 paginiEvaluation of Corticotomy - Facilitated Orthodontics and Piezocision in Rapid Canine RetractionJose CollazosÎncă nu există evaluări
- Clasificacion de Angle Se Usa Realmente - Morton, Katz PDFDocument7 paginiClasificacion de Angle Se Usa Realmente - Morton, Katz PDFLisset MaritzaÎncă nu există evaluări
- ORTHODONTIC BIOPROGRESSIVE SCIENCE SEMINAR PROGRAMDocument5 paginiORTHODONTIC BIOPROGRESSIVE SCIENCE SEMINAR PROGRAMsaberÎncă nu există evaluări
- Maxillary Arch Distalization Using Interradicular Miniscrews and The Lever-Arm ApplianceDocument8 paginiMaxillary Arch Distalization Using Interradicular Miniscrews and The Lever-Arm ApplianceJuan Carlos CárcamoÎncă nu există evaluări
- Laser en OrtodonciaDocument7 paginiLaser en OrtodonciaDiana ElíasÎncă nu există evaluări
- 2024 STAB J of Oral Rehabilitation - 2023 - Manfredini - Standardised Tool For The Assessment of BruxismDocument30 pagini2024 STAB J of Oral Rehabilitation - 2023 - Manfredini - Standardised Tool For The Assessment of Bruxismteodude48100% (1)
- Maxillary Molar Distalization With Modified Trans Palatal Arch and Mini Implants PDFDocument6 paginiMaxillary Molar Distalization With Modified Trans Palatal Arch and Mini Implants PDFSoe San KyawÎncă nu există evaluări
- -PeriodontаI InstrumentationDocument459 pagini-PeriodontаI InstrumentationDANIELA ALEJANDRA VARGAS SANCHEZÎncă nu există evaluări
- Gummy smile correctionDocument8 paginiGummy smile correctionRockey ShrivastavaÎncă nu există evaluări
- SynergyDocument33 paginiSynergyJaisson CenciÎncă nu există evaluări
- Therapeutic Occlusion. From Occlusal Schools of Thought To Evidence-Based DentistryDocument6 paginiTherapeutic Occlusion. From Occlusal Schools of Thought To Evidence-Based DentistryJosephÎncă nu există evaluări
- Correcting The Class II Subdivision MalocclusionDocument2 paginiCorrecting The Class II Subdivision MalocclusionplsssssÎncă nu există evaluări
- MSE 10.1016@j.ajodo.2016.10.025Document11 paginiMSE 10.1016@j.ajodo.2016.10.025Neycer Catpo NuncevayÎncă nu există evaluări
- Sensors 10 00176 Poligono de MasudaDocument27 paginiSensors 10 00176 Poligono de MasudaNATALIA OSORIOÎncă nu există evaluări
- Surgically-Assisted Rapid Palatal Expansion For Management of Transverse Maxillary DeficiencyDocument3 paginiSurgically-Assisted Rapid Palatal Expansion For Management of Transverse Maxillary DeficiencyDaniela CastilloÎncă nu există evaluări
- Complete Clinical Orthodontic Treatment Mechanic by Dr. Antonino SecchiDocument4 paginiComplete Clinical Orthodontic Treatment Mechanic by Dr. Antonino Secchirimarsha nugrafitraÎncă nu există evaluări
- Dental Trauma - An Overview of Its Influence On The Management of Orthodontic Treatment - Part 1.Document11 paginiDental Trauma - An Overview of Its Influence On The Management of Orthodontic Treatment - Part 1.Djoka DjordjevicÎncă nu există evaluări
- Lillian B. MVSS, N.i) .S., XS.," kRORA, ILL: (1786) U-As OneDocument21 paginiLillian B. MVSS, N.i) .S., XS.," kRORA, ILL: (1786) U-As OneDiana Paola FontechaÎncă nu există evaluări
- Elemento II AndrewsDocument8 paginiElemento II AndrewsdbarrioslambÎncă nu există evaluări
- Wolford 1994 - Occlusal Plane Alteration in Orthognathic Surgery, EstheticsDocument13 paginiWolford 1994 - Occlusal Plane Alteration in Orthognathic Surgery, EstheticsBillÎncă nu există evaluări
- Facial Height Index: Case ReportDocument7 paginiFacial Height Index: Case ReportEstefania MontoyaÎncă nu există evaluări
- Biografía Robert Ricketts OrtodonciaDocument3 paginiBiografía Robert Ricketts OrtodonciaPabloÎncă nu există evaluări
- Setting Procedure of The Fully Adjustable SAM 3 Articulator PDFDocument4 paginiSetting Procedure of The Fully Adjustable SAM 3 Articulator PDFortodoncia 2018Încă nu există evaluări
- 8 - Maxillary Expansion in Nongrowing Patients. Conventional, SurgicalDocument11 pagini8 - Maxillary Expansion in Nongrowing Patients. Conventional, SurgicalMariana SantosÎncă nu există evaluări
- EssixDocument5 paginiEssixdent in dentistÎncă nu există evaluări
- Treatment of Brodie SyndromeDocument25 paginiTreatment of Brodie SyndromeAdina Serban100% (1)
- Axis Horizontal Mounting-TamburrinoDocument4 paginiAxis Horizontal Mounting-TamburrinoGabriela RomeroÎncă nu există evaluări
- Tweed1946 ARTICULO INGLES PDFDocument56 paginiTweed1946 ARTICULO INGLES PDFkÎncă nu există evaluări
- Currie Et Al 2017 Angle Orthod PDFDocument14 paginiCurrie Et Al 2017 Angle Orthod PDFplayer osama100% (1)
- Cantilever Springs Force System and ClinicalDocument10 paginiCantilever Springs Force System and Clinicalsolodont1Încă nu există evaluări
- Maintaining Clearly Defined Treatment Objectives:: Case StudyDocument5 paginiMaintaining Clearly Defined Treatment Objectives:: Case StudyAkylai IllanbekovaÎncă nu există evaluări
- Natural Head PositionDocument9 paginiNatural Head PositionPaolaLÎncă nu există evaluări
- Steiner Analysis Cecil CDocument6 paginiSteiner Analysis Cecil Cjeff diazÎncă nu există evaluări
- The Role of Articulators in Orthodontics and Orthognatic SurgeryDocument5 paginiThe Role of Articulators in Orthodontics and Orthognatic SurgeryDr Shivam VermaÎncă nu există evaluări
- TransPalatalArch SIO1995 J.robettaloDocument11 paginiTransPalatalArch SIO1995 J.robettaloutkmangal100% (1)
- Beggs HocevarDocument11 paginiBeggs HocevarAmanjot Bajwa100% (1)
- Análisis de Wits, Iinclinación Del Plano Silla-Nasion en La RelacionesDocument11 paginiAnálisis de Wits, Iinclinación Del Plano Silla-Nasion en La RelacionesRicardo LaraÎncă nu există evaluări
- Miniscrew Assisted Rapid Palatal Expansion (Marpe) - ExpandingHorizons To Achieve An Optimum in Transverse Dimension A ReviewDocument15 paginiMiniscrew Assisted Rapid Palatal Expansion (Marpe) - ExpandingHorizons To Achieve An Optimum in Transverse Dimension A Reviewaa bbÎncă nu există evaluări
- Van BeekDocument4 paginiVan BeekThendral DevanathanÎncă nu există evaluări
- 21 178 1 PBDocument7 pagini21 178 1 PBClinica Dental AdvanceÎncă nu există evaluări
- A Modified Transpalatal Arch With SleeveDocument1 paginăA Modified Transpalatal Arch With Sleeveanasse1Încă nu există evaluări
- Matias AnghileriDocument32 paginiMatias AnghileriSilvia Fernanda Rosa100% (1)
- Asymmetric Deep Bite With A Canted Occlusal Plane - A Case ReportDocument9 paginiAsymmetric Deep Bite With A Canted Occlusal Plane - A Case ReportIacominiGustavoÎncă nu există evaluări
- Biomechanics of Extra-Alveolar Mini-Implant Use in The Infrazygomatic Crest Area For Asymmetrical Correction of Class II Subdivision MalocclusionDocument9 paginiBiomechanics of Extra-Alveolar Mini-Implant Use in The Infrazygomatic Crest Area For Asymmetrical Correction of Class II Subdivision MalocclusionhabeebÎncă nu există evaluări
- Effects of lip bumper therapy on mandibular arch dimensionsDocument13 paginiEffects of lip bumper therapy on mandibular arch dimensionsDominikaSkórka100% (1)
- TrevisiarchDocument20 paginiTrevisiarchkirmani100% (1)
- Understanding Masticatory Function in Unilateral CrossbitesDe la EverandUnderstanding Masticatory Function in Unilateral CrossbitesÎncă nu există evaluări
- Deglucion AtipicaDocument12 paginiDeglucion AtipicakatherineÎncă nu există evaluări
- Guia de ErupcionDocument4 paginiGuia de ErupcionkatherineÎncă nu există evaluări
- Manejo de Sonrisa Gingival KokichDocument5 paginiManejo de Sonrisa Gingival KokichkatherineÎncă nu există evaluări
- Deglucion AtipicaDocument12 paginiDeglucion AtipicakatherineÎncă nu există evaluări
- Sclerostin Injection Enhances Orthodontic Tooth Movement in RatsDocument8 paginiSclerostin Injection Enhances Orthodontic Tooth Movement in RatskatherineÎncă nu există evaluări
- Articulo 1Document8 paginiArticulo 1katherineÎncă nu există evaluări
- Wang2007 Evaluation of Force Degradation Characteristics of Orthodontic Latex Elastics in Vitro and in VivoDocument6 paginiWang2007 Evaluation of Force Degradation Characteristics of Orthodontic Latex Elastics in Vitro and in VivokatherineÎncă nu există evaluări
- Wala RidgeDocument6 paginiWala Ridgekatherine100% (1)
- Comparison of Levels of Inflammatory Mediators Iterleukin 1bDocument9 paginiComparison of Levels of Inflammatory Mediators Iterleukin 1bkatherineÎncă nu există evaluări
- Cytokine Expression Pattern in CompressionDocument8 paginiCytokine Expression Pattern in CompressionkatherineÎncă nu există evaluări
- Activador Andressen y CombinadoDocument5 paginiActivador Andressen y CombinadokatherineÎncă nu există evaluări
- Carriere® MotionTM Elastics ProtocolsDocument2 paginiCarriere® MotionTM Elastics ProtocolsOrtho OrganizersÎncă nu există evaluări
- Molardist PDFDocument5 paginiMolardist PDFLarbiLamecheÎncă nu există evaluări
- Face Shape TransferDocument3 paginiFace Shape Transferapi-580872167Încă nu există evaluări
- Scientific articles on construction faults associated with complete denture complaintsDocument4 paginiScientific articles on construction faults associated with complete denture complaintsLisa Purnia CahyaniÎncă nu există evaluări
- Monster-Mask Cut and PasteDocument6 paginiMonster-Mask Cut and PasteDaphne DermitzÎncă nu există evaluări
- Contemporary Management Pediatric Craniofacial InjuriesDocument8 paginiContemporary Management Pediatric Craniofacial InjuriesTabishur RahmanÎncă nu există evaluări
- BooksDocument11 paginiBooksDentist Bd100% (1)
- Art To The Aid of Technology - Reading Test 1Document2 paginiArt To The Aid of Technology - Reading Test 1chiÎncă nu există evaluări
- The Use of A Removable Orthodontic Appliance For Space Management Combined With Anterior Esthetic Restorations: A Case ReportDocument11 paginiThe Use of A Removable Orthodontic Appliance For Space Management Combined With Anterior Esthetic Restorations: A Case ReportKhaleda ShafiraÎncă nu există evaluări
- Functional Occlusal Rehabilitation of A Mutilated Adult Dentition Caused by A Constricted Chewing PathwayDocument9 paginiFunctional Occlusal Rehabilitation of A Mutilated Adult Dentition Caused by A Constricted Chewing Pathwayjorefe12Încă nu există evaluări
- Maxillofacial TraumaDocument70 paginiMaxillofacial Traumaeman_879_123456Încă nu există evaluări
- Gua Sha Teacher Training Manual 04.06.2021Document150 paginiGua Sha Teacher Training Manual 04.06.2021ady.crocker1Încă nu există evaluări
- SJDS 412562 572Document11 paginiSJDS 412562 572habeebÎncă nu există evaluări
- تشريح العينDocument9 paginiتشريح العينheaveɴÎncă nu există evaluări
- FaceUP Workout Booklet English MassageDocument14 paginiFaceUP Workout Booklet English MassageTania Dorado100% (2)
- 1.6 Sense of SightDocument10 pagini1.6 Sense of SightFidah MadÎncă nu există evaluări
- Diagnosa GigiDocument3 paginiDiagnosa GigiAntika Fitri LestariyaniÎncă nu există evaluări
- Extraction Treatment, Part 2: Guidelines For Making The Extraction DecisionDocument7 paginiExtraction Treatment, Part 2: Guidelines For Making The Extraction DecisionLuis HerreraÎncă nu există evaluări
- Extraocular Muscle InnervationDocument1 paginăExtraocular Muscle InnervationRiski SudaenyÎncă nu există evaluări
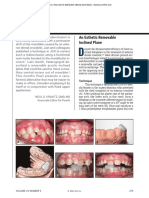
- An Esthetic Removable Inclined Plane - Jco - Pearls - Volume IV Number 5 May 2020 Page 275Document2 paginiAn Esthetic Removable Inclined Plane - Jco - Pearls - Volume IV Number 5 May 2020 Page 275APinhaoFerreiraÎncă nu există evaluări
- Effects of The FrankelDocument5 paginiEffects of The FrankelMatias AnghileriÎncă nu există evaluări
- Tooth Selection in Removablre DentureDocument53 paginiTooth Selection in Removablre Denturejohn mwambuÎncă nu există evaluări
- Diagnosis Dan Tatalaksana Pasien Dengan Insufisiensi Akomodasi - Sri Hudaya WidihasthaDocument13 paginiDiagnosis Dan Tatalaksana Pasien Dengan Insufisiensi Akomodasi - Sri Hudaya WidihasthamalaÎncă nu există evaluări
- Intro +obturators TechDocument26 paginiIntro +obturators Techreem eltyebÎncă nu există evaluări
- 10 Steps To Maximize Success For Veneer PreparationDocument9 pagini10 Steps To Maximize Success For Veneer PreparationMairen RamirezÎncă nu există evaluări
- Orthodontics Part 8 Extractions in OrthodonticsDocument10 paginiOrthodontics Part 8 Extractions in OrthodonticsAdina SerbanÎncă nu există evaluări