Documente Academic
Documente Profesional
Documente Cultură
DISRRUPCION JPediatrNeurosci14294-8463893 - 233038
Încărcat de
Sara IsabelTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
DISRRUPCION JPediatrNeurosci14294-8463893 - 233038
Încărcat de
Sara IsabelDrepturi de autor:
Formate disponibile
[Downloaded free from http://www.pediatricneurosciences.com on Wednesday, April 22, 2020, IP: 190.107.28.
245]
Case Report
Amniotic Band Syndrome Associated with Exencephaly: A Case Report and
Literature Review
Aldo Jose F. da Silva
Division of Pediatric Amniotic band syndrome (ABS) is a rare congenital disease with variable
Abstract
Neurosurgery, Santa
manifestations ranging from simple constriction rings at the extremities to major
Mônica Maternity School
(SMMS), Maceió, Alagoas,
defects such as exencephaly. Here we report the case of a female baby born full
Brazil term (39 weeks) from a 35-year-old primiparous mother by cesarean section.
In addition to the constriction rings at the extremities (fingers), the newborn
presented facial malformations and a cranial anomaly suggestive of exencephaly.
Supportive treatment was chosen because of the poor prognosis, and the child
died 5 months later. Depending on the anomaly associated with ABS and its
complexity, as in our case, genetic studies should be performed whenever
possible, and the parents should be informed about the possibility of recurrences
and incompatibility with life.
Keywords: Abnormalities, amniotic band syndrome, anencephaly, encephalocele,
intrauterine ring constriction
Introduction marriage and no history of teratogenic medication,
diabetes, hypertension, recent infection, or drug
A mniotic band syndrome (ABS) is a rare
congenital disorder with several manifestations
from simple constriction rings to major defects that
exposure during pregnancy. Antenatal ultrasound (28
weeks) led to the diagnosis of frontal encephalocele.
may even lead to miscarriage. Its incidence ranges from On physical examination, the newborn weighed 3500 g
1:200 to 1:500 live births.[1] It affects both sexes equally, and had difficulty in breathing and showed partial
and its frequency is slightly higher in the people of the absence of the skull bones (left parietal, left temporal,
Afro-Caribbean descent.[2] The first report on this type and frontal bones).
of malformation was published in 1685 by Portal. The
Owing to this defect, protruded abnormal brain tissue
first description of its etiopathogenesis was proposed
was covered only by a membrane similar to the dura
by Montgomery in 1832.[3] Although studies by Orioli
mater. There were malformations along the facial
et al.[4] showed that the extremities are more affected
midline, such as bilateral cleft lip and palate and nasal
by this disease, Guzmán-Huerta et al.[5] reported
deformity. Bilateral proptosis was also noted. Changes
craniofacial abnormalities in 78% of the cases and
in the extremities included the following: her right hand
defects of the extremities in 70%. Cranial changes
had hypoplastic second and third fingers conjoined
range from encephalocele to acrania.[6] Exencephaly is
by a fibrous tissue (syndactyly) and left hand had
a type of acrania, with disorganized brain tissue arising
constriction rings around the third and fifth fingers,
from the base of the skull.[7] We report the case of a
newborn with ABS and exencephaly.
Case Report Address for correspondence: Dr. Aldo J. Ferreira da Silva,
Division of Pediatric Neurosurgery,
A female newborn was delivered by a 35-year-old Santa Mônica Maternity School (SMMS),
primigravida mother at term (39 weeks) by a cesarean Maceió, Alagoas, Brazil.
E-mail: neuroajfs@bol.com.br
section. The mother reported a consanguineous
This is an open access journal, and articles are distributed under the terms of the
Access this article online Creative Commons Attribution-NonCommercial-ShareAlike 4.0 License, which allows
Quick Response Code: others to remix, tweak, and build upon the work non-commercially, as long as
Website: appropriate credit is given and the new creations are licensed under the identical terms.
www.pediatricneurosciences.com For reprints contact: reprints@medknow.com
How to cite this article: da Silva AJ. Amniotic band syndrome associated
DOI: 10.4103/jpn.JPN_130_18
with exencephaly: A case report and literature review. J Pediatr Neurosci
2019;14:94-6.
94 © 2019 Journal of Pediatric Neurosciences | Published by Wolters Kluwer - Medknow
[Downloaded free from http://www.pediatricneurosciences.com on Wednesday, April 22, 2020, IP: 190.107.28.245]
da Silva: Amniotic band syndrome associated with exencephaly
with amputation of the distal phalanx of the fourth child died from acquired comorbidities 5 months after
finger. Congenital clubfoot was noted [Figure 1]. birth.
Cranial computed tomography (CT) evidenced a great
amount of protruding malformed brain tissue through
Discussion
the skull bone defect caused by the partial absence ABS comprises a group of anomalies that correspond
of the frontal, left temporal, and left parietal bones, to 1%–2% of the congenital malformations in the
suggesting exencephaly [Figure 2]. general population. This disorder is not hereditary, and
no risk of recurrence is observed.[8]
No other malformations were found. ABS was
diagnosed on the basis of the clinical picture. Its etiology is unknown. Several theories have been
suggested to explain its etiopathogenesis, and the most
Only support treatment was provided because of the accepted ones are as follows: (1) the intrinsic theory
severity of the condition and the poor prognosis, proposed by Streeter in 1930, which establishes that
including feeding via an orogastric tube and congenital constriction is a germplasm defect with
tracheostomy for improved breathing. However, the vascular disruption and change of morphogenesis
during gastrulation, forming the fibrous bands and
causing limb necrosis[1,3,9] and (2) the extrinsic theory
proposed by Torpin in 1965, which associated the
defects of the extremities or limb amputations with
amniotic rupture and compression of the bands.[3]
There are multifactorial and genetic factors that cause
amniotic rupture: direct abdominal trauma, induced
abortion, amniocentesis, maternal exposure to drugs,
bacterial infection of the amniotic membranes, and
oligohydramnios.[8]
According to Higginbottom, there are three mechanisms
that could explain the role of bands in the genesis of
the malformation: (1) interruption of morphogenesis,
(2) deformation due to compression of fetal parts by
the fetus itself or entrapment of fetal parts by the band,
and (3) injury of already formed and developed fetal
parts such as constrictions found in the extremities.[10]
Van Allen et al., in 1987, also contributed with the
theory of vascular disruption, preceded by Kino who
Figure 1: Coronal CT scan, protruding malformed brain tissue conducted experiments in animal models in 1975.[3]
through the skull bone defect caused by the partial absence of the
frontal, left temporal, and left parietal bones (arrows) Hunter et al. proposed another theory based on a
defect or primary deficiency in the ectoderm of the
embryonic disc. The area affected and the severity
of the results varied according to the location of the
defect. In particular, craniofacial abnormalities were
classified as follows: (1) exencephaly/encephalocele
with amniotic connections and without facial cleft;
(2) similar cranial lesions, with facial clefts and with
or without amniotic bands; (3) abdominoschisis and
thoracoabdominoschisis; and (4) limb abnormalities.[3]
Exencephaly is a malformation incompatible with
extrauterine life.[11] This condition is the partial or
complete absence of the calvaria (acrania) associated
Figure 2: Right hand, hypoplastic second and third fingers
conjoined by a fibrous tissue (syndactyly). Left hand, constriction with protrusion of an abnormal brain tissue through
rings around the third and fifth fingers, with amputation of the the defect. Some studies have shown that it is an
distal phalanx of the fourth finger embryological precursor of anencephaly, resulting
Journal of Pediatric Neurosciences ¦ Volume 14 ¦ Issue 2 ¦ April-June 2019 95
[Downloaded free from http://www.pediatricneurosciences.com on Wednesday, April 22, 2020, IP: 190.107.28.245]
da Silva: Amniotic band syndrome associated with exencephaly
from the degeneration of the unprotected brain tissue 3. González ZIR, Padilla FS. Complejo de deformidades
affected by mechanical and chemical trauma when amnióticas, adhesiones, mutilación: interminable debate. Bol
Med Hosp Infant Mex 2015;72:159-68.
exposed to the amniotic fluid.[7,12] 4. Orioli IM, Ribeiro MG, Castilla EE. Clinical and
The diagnosis of ABS is difficult and occurs in only 29%– epidemiological studies of amniotic deformity, adhesion, and
mutilation (ADAM) sequence in a South American (ECLAMC)
50% of cases.[3] The craniofacial deformities are often
population. Am J Med Genet A 2003;118A:135-45.
bizarre, and the internal organ abnormalities are rare.[2] 5. Guzmán-Huerta ME, Muro-Barragán SA, Acevedo-Gallegos S,
Exencephaly may be diagnosed using the measurement Velázquez-Torres B, Gallardo-Gaona JM, Ramírez-Calvo JA,
et al. Amniotic band sequence: prenatal diagnosis, phenotype
of alpha-fetoprotein level in the amniotic fluid and descriptions, and a proposal of a new classification based on
maternal blood. Ultrasound may be used at gestational morphologic findings. Rev Invest Clin 2013;65:300-6.
week 11, which may indicate the absence of bone 6. Dyson RL, Pretorius DH, Budorick NE, Johnson DD,
coverage in the cranial vault.[11,13] Sklansky MS, Cantrell CJ, et al. Three-dimensional ultrasound
in the evaluation of fetal anomalies. Ultrasound Obstet Gynecol
The prognosis of ABS varies according to the 2000;16:321-8.
associated anomalies. In this case, despite the 7. Hendricks SK, Cyr DR, Nyberg DA, Raabe R, Mack LA.
complex anomaly (exencephaly) and poor prognosis, Exencephaly—clinical and ultrasonic correlation to
supportive measures were chosen and the survival anencephaly. Obstet Gynecol 1988;72:898-900.
8. Guzmán-Santos IY, Domínguez-Moreno R, Muñoz-
period was 5 months. The complications from this Delgado M, Martínez-Quintana JD. [Amniotic band syndrome:
disease are severe; therefore, genetic studies should be report of a case]. Ginecol Obstet Mex 2013;81:353-6.
performed whenever possible, and the parents should 9. PardiniJr AG, Santos MA, Freitas AD. Bandas de Constrição
be informed about the potential risk of recurrences Congênitas. Acta Ortop Bras 2001;9:5-12.
and incompatibility with life. 10. Higginbottom MC, Jones KL, Hall BD, Smith DW. The
amniotic band disruption complex - Timing of amniotic
Financial support and sponsorship rupture and variable spectra of consequent defects. J. Pediatr
Nil. 1979;95:544-9.
11. Rohrbach M, Chitayat D, Drake J, Velsher L, Sirkin WL,
Conflicts of interest Blaser S. Prenatal diagnosis of fetal exencephaly associated
There are no conflicts of interest. with amniotic band sequence at 17 weeks of gestation by
fetal magnetic resonance imaging. Fetal Diagn Ther 2007;22:
112-5.
References 12. Machado RA, Brizot ML, Carvalho MH, Waissman AL,
1. Nogueira FCS, Cruz RB, Machado LP, Ramos BLF, Bunduki V, Zugaib M. Sonographic markers of exencephaly
MadureiraJr JL, Pinto RZA. Síndrome da Banda Amniótica: below 10 weeks’ gestation. Prenat Diagn 2005;25:
relato de caso. Rev Bras Ortop 2011;46:56-62. 31-3.
2. Da Silva G, Cammarata SF, Gonzalez-Coira M, Lacruz MA, 13. Tica VI, Beghim M, Tica I, Zaher M, Beghim E. Anencephaly:
Rendon B. Amniotic band syndrome: 3 case reports. Rev Chil pitfalls in pregnancy outcome and relevance of the prenatal
Pediatr 2008;79:172-8. exam. Rom J Morphol Embryol 2009;50:295-7.
96 Journal of Pediatric Neurosciences ¦ Volume 14 ¦ Issue 2 ¦ April-June 2019
S-ar putea să vă placă și
- Nbme Step 1 AnatomyDocument23 paginiNbme Step 1 AnatomyMohsin Farooq100% (12)
- RA 10028 Expanded Breastfeeding Promotion ActDocument3 paginiRA 10028 Expanded Breastfeeding Promotion ActBlgu Lucog100% (4)
- Fat To Fabulous PDFDocument197 paginiFat To Fabulous PDFjjleejustina100% (1)
- Entrepreneurial CompetenciesDocument13 paginiEntrepreneurial Competenciesdharshinee1961Încă nu există evaluări
- Grooming and Personal Hygiene at WorkDocument18 paginiGrooming and Personal Hygiene at WorkJoshua MiñaÎncă nu există evaluări
- Unit 2 Evidence Based Nursing PracticeDocument94 paginiUnit 2 Evidence Based Nursing Practicenoo.wann100% (2)
- Medical TechnologyDocument14 paginiMedical Technologydprincebuchikoy100% (1)
- Thesis On Pre - Marital Sex.Document49 paginiThesis On Pre - Marital Sex.Charmaine Inah Abas Calumpang92% (145)
- Lesson 3 The Self As Cognitive ConstructDocument25 paginiLesson 3 The Self As Cognitive ConstructIvy Canonio Gallardo100% (1)
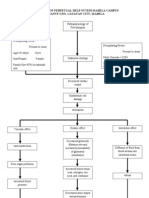
- Pathophysiology of PreeclampsiaDocument1 paginăPathophysiology of PreeclampsiaKristine Alejandro100% (15)
- Topic 1: Before You Begin Evaluate and Prioritise The Needs of A Person With Complex Support IssuesDocument20 paginiTopic 1: Before You Begin Evaluate and Prioritise The Needs of A Person With Complex Support Issuesdefa rey100% (1)
- Amniotic Band Syndrome: A Report of Two Cases and Review of The LiteratureDocument5 paginiAmniotic Band Syndrome: A Report of Two Cases and Review of The LiteratureIzar Handika IlmawanÎncă nu există evaluări
- Constriction Band 2Document5 paginiConstriction Band 2Raudha JanahÎncă nu există evaluări
- Amniotic Band SyndromeDocument5 paginiAmniotic Band SyndromeganotÎncă nu există evaluări
- Espina BífidaDocument18 paginiEspina BífidaDamary Cifuentes ReyesÎncă nu există evaluări
- Art 4Document8 paginiArt 4mariam villalbaÎncă nu există evaluări
- A Cases of Limb Body Wall Syndrome (LBW) : Report and LiteraturereviewDocument5 paginiA Cases of Limb Body Wall Syndrome (LBW) : Report and LiteraturereviewIJAR JOURNALÎncă nu există evaluări
- Amniotic Band Sequence: Consult SeriesDocument2 paginiAmniotic Band Sequence: Consult SeriesRamos Zavala Julio CesarÎncă nu există evaluări
- A Rare Case of Fetal Sirenomelia Malformation in The - 2024 - International JourDocument5 paginiA Rare Case of Fetal Sirenomelia Malformation in The - 2024 - International JourRonald QuezadaÎncă nu există evaluări
- Herman 2012Document20 paginiHerman 2012dewaprasatyaÎncă nu există evaluări
- Case ReportDocument6 paginiCase ReportJellie MendozaÎncă nu există evaluări
- MortalDocument6 paginiMortalazhar naufaldiÎncă nu există evaluări
- Thoracic-Omphalopagus Conjoined Twins A Case Report and Review of The LiteratureDocument3 paginiThoracic-Omphalopagus Conjoined Twins A Case Report and Review of The LiteratureInternational Journal of Innovative Science and Research TechnologyÎncă nu există evaluări
- Files Act Lopezmunoz e 2-5pdf 1524856050Document11 paginiFiles Act Lopezmunoz e 2-5pdf 1524856050Robert ChristevenÎncă nu există evaluări
- Spinal DisDocument32 paginiSpinal DisAkmal Niam FirdausiÎncă nu există evaluări
- Twinpregnancy Bi Chorial Complicatedwithexomphalos of One Twin: Case ReportDocument4 paginiTwinpregnancy Bi Chorial Complicatedwithexomphalos of One Twin: Case ReportIJAR JOURNALÎncă nu există evaluări
- A Rare Case of Limb Body Wall ComplexDocument5 paginiA Rare Case of Limb Body Wall ComplexIvan DavrayÎncă nu există evaluări
- Journal of Pediatric Surgery Case Reports: Moaied A. Hassan, Hasan K. Gatea, Thura K. Ja'afar, Ahmed O. Fahad TDocument3 paginiJournal of Pediatric Surgery Case Reports: Moaied A. Hassan, Hasan K. Gatea, Thura K. Ja'afar, Ahmed O. Fahad TVero MeidyÎncă nu există evaluări
- Lazaroni 16Document4 paginiLazaroni 16adiÎncă nu există evaluări
- Alwahab2017 Article OccipitalMeningoencephaloceleC PDFDocument4 paginiAlwahab2017 Article OccipitalMeningoencephaloceleC PDFOvamelia JulioÎncă nu există evaluări
- Espina Bifida 2022Document7 paginiEspina Bifida 2022Edwin Fabian Paz UrbanoÎncă nu există evaluări
- Brachial Plexus Birth Palsy: An Overview of Early Treatment ConsiderationsDocument7 paginiBrachial Plexus Birth Palsy: An Overview of Early Treatment Considerationsphannghia.ydsÎncă nu există evaluări
- Congenital Orthopedic DeformitiesDocument6 paginiCongenital Orthopedic Deformitiesmamang somayÎncă nu există evaluări
- 87-Article Text-406-1-10-20191202Document16 pagini87-Article Text-406-1-10-20191202Marco Antonio CorreaÎncă nu există evaluări
- C01221215 PDFDocument4 paginiC01221215 PDFratnaharyantiÎncă nu există evaluări
- Amniotic Band SyndromeDocument7 paginiAmniotic Band SyndromeOscar HustorioÎncă nu există evaluări
- Interdisciplinary Neurosurgery: Jimmy Ntimbani, Adrian Kelly, Patrick Lekgwara TDocument4 paginiInterdisciplinary Neurosurgery: Jimmy Ntimbani, Adrian Kelly, Patrick Lekgwara TKunni MardhiyahÎncă nu există evaluări
- Neuroradiological Findings of Trisomy 13 in A Rare Long-Term SurvivorDocument3 paginiNeuroradiological Findings of Trisomy 13 in A Rare Long-Term Survivorchristian roblesÎncă nu există evaluări
- Acog Practice Bullet In: Neural Tube DefectsDocument12 paginiAcog Practice Bullet In: Neural Tube DefectsSILVIA GAONAÎncă nu există evaluări
- Epidemiology of Brachial Plexus Palsy in NewbornsDocument7 paginiEpidemiology of Brachial Plexus Palsy in NewbornsMardyana MardinÎncă nu există evaluări
- Amniotic Band SyndromeDocument7 paginiAmniotic Band SyndromeAdisurosotrionoÎncă nu există evaluări
- 1 s2.0 S1878875020315084 MainDocument6 pagini1 s2.0 S1878875020315084 MainilonaskorinÎncă nu există evaluări
- Anancephaly 2Document3 paginiAnancephaly 2Metta SariÎncă nu există evaluări
- HTTPS:WWW Ncbi NLM Nih gov:pmc:articles:PMC5614933:pdf:fsurg-04-00052Document8 paginiHTTPS:WWW Ncbi NLM Nih gov:pmc:articles:PMC5614933:pdf:fsurg-04-00052Don SarÎncă nu există evaluări
- (23444959 - Romanian Neurosurgery) Shaken Baby Syndrome. Case ReportDocument9 pagini(23444959 - Romanian Neurosurgery) Shaken Baby Syndrome. Case ReportRio M RajagukgukÎncă nu există evaluări
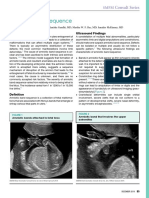
- Journal of Diagnostic Medical Sonography 2010 Moore 286 9Document4 paginiJournal of Diagnostic Medical Sonography 2010 Moore 286 9Hanarisha Putri AzkiaÎncă nu există evaluări
- Branchial Cleft Cyst: A Case Report and Review of LiteratureDocument3 paginiBranchial Cleft Cyst: A Case Report and Review of LiteratureValonia IreneÎncă nu există evaluări
- Common Dysmorphic Syndromes in The NICUDocument12 paginiCommon Dysmorphic Syndromes in The NICUDaniel PuertasÎncă nu există evaluări
- Liu 2016Document2 paginiLiu 2016Anonymous l3X3jf0NPÎncă nu există evaluări
- Ultrasound in The Etiological Assessment of Embryonic Implantation Failures at The Fertilia Medical Clinic in BamakoDocument7 paginiUltrasound in The Etiological Assessment of Embryonic Implantation Failures at The Fertilia Medical Clinic in BamakoIJAR JOURNALÎncă nu există evaluări
- Ultrasound in The Etiological Assessment of Embryonic Implantation Failures at The Fertilia Medical Clinic in BamakoDocument7 paginiUltrasound in The Etiological Assessment of Embryonic Implantation Failures at The Fertilia Medical Clinic in BamakoIJAR JOURNALÎncă nu există evaluări
- Pediatric RehabDocument32 paginiPediatric RehabRainy DaysÎncă nu există evaluări
- Embryofetoscopy A New Old ToolDocument5 paginiEmbryofetoscopy A New Old ToolMiriam ContiÎncă nu există evaluări
- Exencephaly-Anencephaly Sequence: Consult SeriesDocument4 paginiExencephaly-Anencephaly Sequence: Consult SeriesMegaSariDewiÎncă nu există evaluări
- Achondroplasia Case Report: June 2015Document7 paginiAchondroplasia Case Report: June 2015Juodie Lee VaelÎncă nu există evaluări
- Encephalocele Prenatal Diagnosis About A CaseDocument3 paginiEncephalocele Prenatal Diagnosis About A CaseInternational Journal of Innovative Science and Research TechnologyÎncă nu există evaluări
- Birth DefectDocument80 paginiBirth DefectGIRUM BELAYÎncă nu există evaluări
- 2479 ArticleDocument5 pagini2479 Articleclbenitez52Încă nu există evaluări
- 10.1007@s00381 020 04746 9Document12 pagini10.1007@s00381 020 04746 9Alvaro Perez HenriquezÎncă nu există evaluări
- Acquired Infantile Horner Syndrome and Spontaneous Internal Carotid Artery Dissection: A Case Report and Review of LiteratureDocument10 paginiAcquired Infantile Horner Syndrome and Spontaneous Internal Carotid Artery Dissection: A Case Report and Review of LiteratureDanielle SangalangÎncă nu există evaluări
- Pediatric Forensic Pathology: Limits and ControversiesDocument191 paginiPediatric Forensic Pathology: Limits and Controversieschrisr310Încă nu există evaluări
- DiscursoDocument21 paginiDiscursoLeslye SimbañaÎncă nu există evaluări
- A Case of Acrocephalosyndactyly With Low Imperforate AnusDocument3 paginiA Case of Acrocephalosyndactyly With Low Imperforate Anuschristian roblesÎncă nu există evaluări
- First Branchial Cleft AinusDocument5 paginiFirst Branchial Cleft AinusAhmad fayazÎncă nu există evaluări
- Spina Bifida General Dental PracticeDocument5 paginiSpina Bifida General Dental PracticerambuanggieÎncă nu există evaluări
- Ilhan 2018Document3 paginiIlhan 2018akshayajainaÎncă nu există evaluări
- Supposed Otolaryngology Emergency Which Presents Late Bilateral Congenital Choanal AtresiaDocument3 paginiSupposed Otolaryngology Emergency Which Presents Late Bilateral Congenital Choanal AtresiaPaul HartingÎncă nu există evaluări
- Case Leprosy-NewDocument16 paginiCase Leprosy-NewChinta Nur SilmiÎncă nu există evaluări
- Antenatal Detection of CotwinsDocument3 paginiAntenatal Detection of CotwinsSiti Hadijah Aspan, M.PHÎncă nu există evaluări
- Endometriosis Pathogenesis, Clinical Impact and Management: Volume 9: Frontiers in Gynecological EndocrinologyDe la EverandEndometriosis Pathogenesis, Clinical Impact and Management: Volume 9: Frontiers in Gynecological EndocrinologyÎncă nu există evaluări
- HHS Public Access: Testing For N-methyl-D-aspartate Receptor Autoantibodies in Clinical PracticeDocument27 paginiHHS Public Access: Testing For N-methyl-D-aspartate Receptor Autoantibodies in Clinical PracticeSara IsabelÎncă nu există evaluări
- Anti-NMDA Receptor Encephalitis and Vaccination: Molecular SciencesDocument9 paginiAnti-NMDA Receptor Encephalitis and Vaccination: Molecular SciencesSara IsabelÎncă nu există evaluări
- Biomedical Journal: SciencedirectDocument8 paginiBiomedical Journal: SciencedirectSara IsabelÎncă nu există evaluări
- Clinical Characteristics and Prognostic Factors of Children With Anti-N-Methyl-D-Aspartate Receptor EncephalitisDocument9 paginiClinical Characteristics and Prognostic Factors of Children With Anti-N-Methyl-D-Aspartate Receptor EncephalitisSara IsabelÎncă nu există evaluări
- Pediatric Anti-N-Methyl - Aspartate Receptor Encephalitis: A Review With Pooled Analysis and Critical Care EmphasisDocument8 paginiPediatric Anti-N-Methyl - Aspartate Receptor Encephalitis: A Review With Pooled Analysis and Critical Care EmphasisSara IsabelÎncă nu există evaluări
- Early Second-Line Therapy Is Associated With Improved Episodic Memory in anti-NMDA Receptor EncephalitisDocument12 paginiEarly Second-Line Therapy Is Associated With Improved Episodic Memory in anti-NMDA Receptor EncephalitisSara IsabelÎncă nu există evaluări
- European Journal of Paediatric Neurology: SciencedirectDocument5 paginiEuropean Journal of Paediatric Neurology: SciencedirectSara IsabelÎncă nu există evaluări
- Autoimmune Encephalitis in Latin America: A Critical ReviewDocument8 paginiAutoimmune Encephalitis in Latin America: A Critical ReviewSara IsabelÎncă nu există evaluări
- 2019 Article 725Document10 pagini2019 Article 725Sara IsabelÎncă nu există evaluări
- Downard 2017Document15 paginiDownard 2017Sara IsabelÎncă nu există evaluări
- MALFORMACION AnnPediatrCard13181-7027904 - 193119Document3 paginiMALFORMACION AnnPediatrCard13181-7027904 - 193119Sara IsabelÎncă nu există evaluări
- My Competitive AdvantageDocument3 paginiMy Competitive AdvantageAnand ViharÎncă nu există evaluări
- Infographics in Anesthesiology: Complex Information For Anesthesiologists Presented Quickly and ClearlyDocument1 paginăInfographics in Anesthesiology: Complex Information For Anesthesiologists Presented Quickly and ClearlyParvathy R NairÎncă nu există evaluări
- Beeben Russell, Platinum Biologics, Scott Martin, Marcus RusselDocument1 paginăBeeben Russell, Platinum Biologics, Scott Martin, Marcus RusselseenfgÎncă nu există evaluări
- Emergency Trolley GuidelineDocument3 paginiEmergency Trolley GuidelineNur SusiawantyÎncă nu există evaluări
- 4.3 FA2.A MCQ Management Theories Planning - NCM 119 NURSING LEADERSHIP AND MANAGEMENTDocument10 pagini4.3 FA2.A MCQ Management Theories Planning - NCM 119 NURSING LEADERSHIP AND MANAGEMENTGil GanibanÎncă nu există evaluări
- Job Interview QuestionnaireDocument4 paginiJob Interview QuestionnaireFares Salah100% (2)
- Factors That Affect ObedienceDocument2 paginiFactors That Affect ObediencedanieljohnarboledaÎncă nu există evaluări
- DR Batra's Healthcare - WikipediaDocument2 paginiDR Batra's Healthcare - WikipediaRajshekhar ReddyÎncă nu există evaluări
- Monsoon Action PlanDocument8 paginiMonsoon Action PlanViron BaxhiaÎncă nu există evaluări
- Chapter 2 - (Lesson 1 Activity)Document3 paginiChapter 2 - (Lesson 1 Activity)Plain KitchenÎncă nu există evaluări
- Quality Form Oplan Kalusugan Sa Deped Accomplishment Report FormDocument12 paginiQuality Form Oplan Kalusugan Sa Deped Accomplishment Report Formanon_176903314Încă nu există evaluări
- The Great Depression EssaysDocument6 paginiThe Great Depression Essaysafibooxdjvvtdn100% (2)
- Homeroom Guidance Module 1: Self-Analysis: A Step To My ImprovementDocument5 paginiHomeroom Guidance Module 1: Self-Analysis: A Step To My ImprovementJohn Francis Barrios0% (1)
- Academic Reading Practice Test 1Document11 paginiAcademic Reading Practice Test 1Gurpreet DhillonÎncă nu există evaluări
- Turquoise Heart Vector Medical Brochure PDFDocument2 paginiTurquoise Heart Vector Medical Brochure PDFHERNEY LEANDRO PEREZ CADENAÎncă nu există evaluări
- PAR Methods Reader2014 For Web PDFDocument125 paginiPAR Methods Reader2014 For Web PDFPuji Arifianti RamadhanyÎncă nu există evaluări
- Cardioembolic StrokeDocument13 paginiCardioembolic StrokeAzarel JimmyÎncă nu există evaluări
- Amad Uloc Ge15Document4 paginiAmad Uloc Ge15Rolando AmadÎncă nu există evaluări
- Pa RagisDocument11 paginiPa RagisVal FielÎncă nu există evaluări
- Visual Impairments in Young Children: Fundamentals of and Strategies For Enhancing DevelopmentDocument13 paginiVisual Impairments in Young Children: Fundamentals of and Strategies For Enhancing Developmentfadil ahmadiÎncă nu există evaluări